Submitted:
19 February 2026
Posted:
26 February 2026
You are already at the latest version
Abstract

Keywords:
1. Introduction
- RQ 1:
- How do perceptions of usefulness and acceptance of Technology Assisted Living (TAL) vary?
- RQ 2:
- How does adoption willingness for Technology Assisted Living (TAL) vary across population groups?
- RQ 3:
- Which adoption barriers and improvement potentials can be identified?
- RQ 4:
- What preferred financing models are reported across stakeholders?
2. Related Work
2.1. Usage and Potential of Technologies to Support Aging in Place:
2.2. Conditions Influencing the Acceptance of Smart Home Health Technology (SHHT) and Technology Assisted Living (TAL)
2.3. Research Gaps in Technology Assisted Living (TAL)-Enabled Tiny Homes
3. Methodology
3.1. NewCareMobil (NCM): Concept and Included Technologies
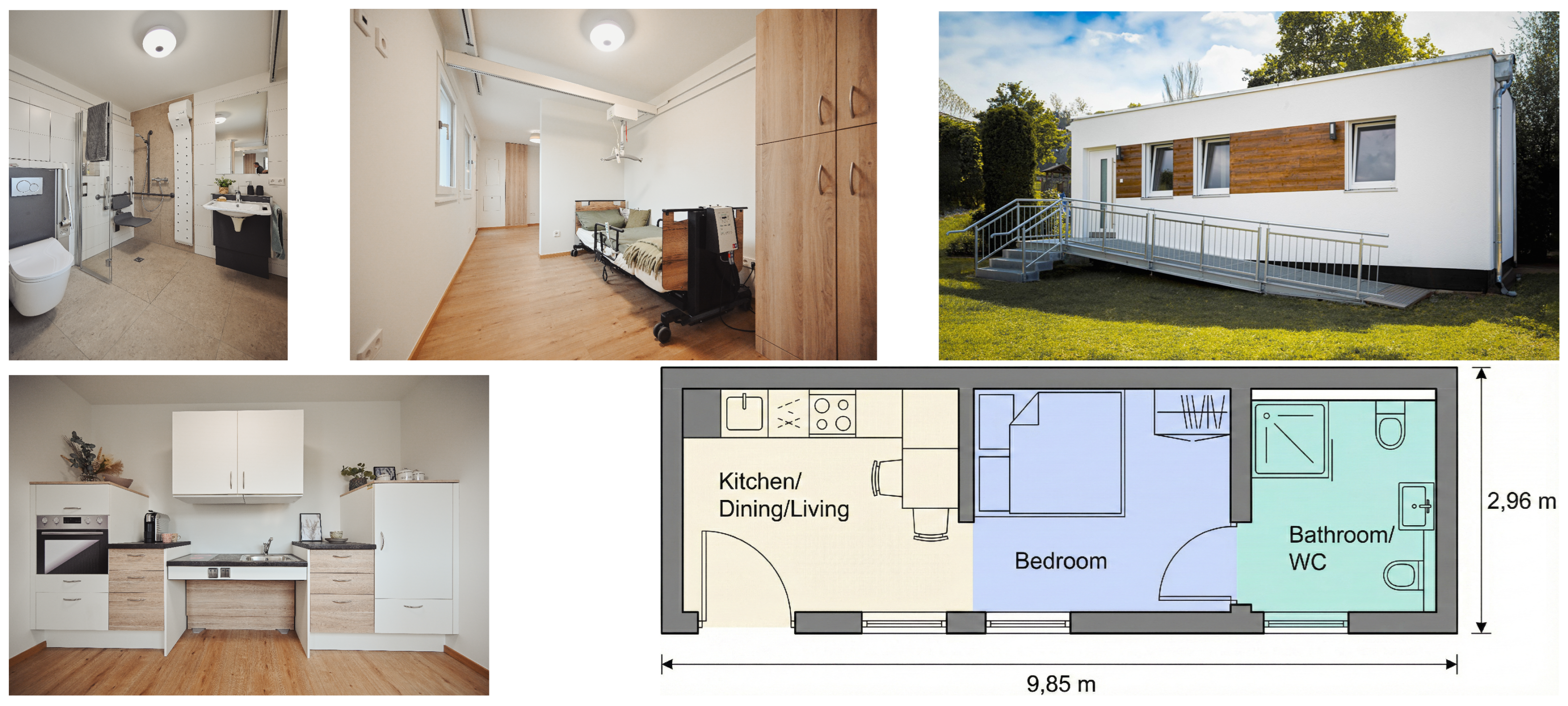
3.2. Multisite Exposure (Public Roadshow)
3.3. Data Collection and Analysis
4. Results
4.1. Perceived Usefulness (PU) of the NCM
4.2. Willingness to Use (WtU) and Reported Barriers
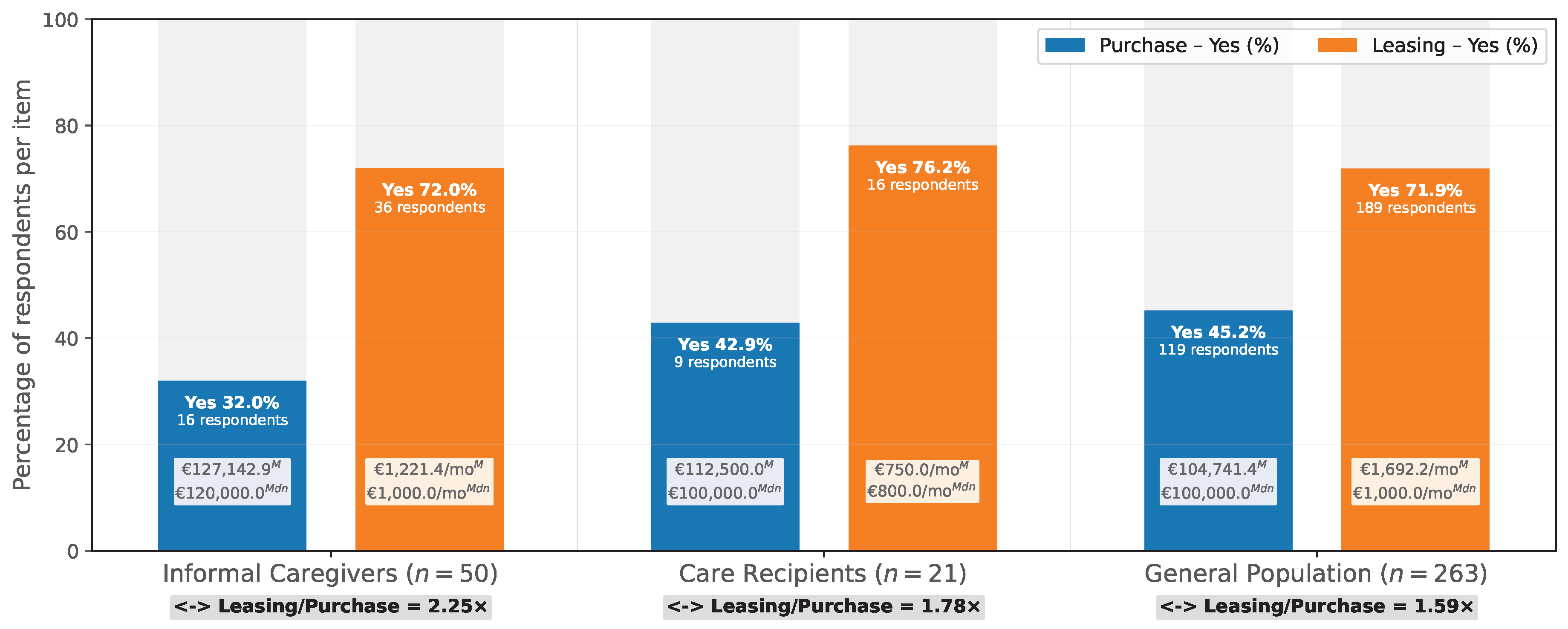
4.3. Willingness to Pay (WtP)
5. Discussion
Limitations:
Contribution:
- RQ 1:
- RQ 2:
- Regardless from costs, a robust willingness to use the NewCareMobile (NCM) was observed, with 90–92% of participants across all groups indicating positive intent.
- RQ 3:
- RQ 4:
- The leasing preference in all participants underscores the need for models tailored to pension-based incomes and the temporary TAL-needs [30].
6. Outlook
Supplementary Materials
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Statistisches Bundesamt. Pflegebedürftige in Deutschland. Press release, 2024. Press Release PD24_478_224, Acc.: 2026-01-16.
- Institut für Demoskopie Allensbach (IfD). Indiv. Strategien zur Bewältigung des Pflegefalls, 2022. Acc.: 2026-02-01.
- BMFSFJ. Living at home longer, 2019. Acc.: 2026-02-01.
- Pfnür, A.; Lachenmayer, F.; Bachtal, Y.; Voll, K. So wohnen wir in Zukunft, 2023.
- Facchinetti, G.; Petrucci, G.; Albanesi, B.; de Marinis, M.G.; Piredda, M. Can Smart Home technologies Help Older Adults Manage Their Chronic Condition? IJERPH 2023, 20. [CrossRef]
- Peek, S.T.M.; Wouters, E.J.M.; van Hoof, J.; Luijkx, K.G.; Boeije, H.R.; Vrijhoef, H.J.M. Factors influencing acceptance of technol. for aging in place: a Syst. Rev. Int. journal of medical informatics 2014, 83, 235–248. [CrossRef]
- Borelli, E.; Paolini, G.; Antoniazzi, F.; Barbiroli, M.; Benassi, F.; Chesani, F.; Chiari, L.; Fantini, M.; Fuschini, F.; Galassi, A.; et al. HABITAT: An IoT Solution for Independent Elderly. Sensors 2019, 19. [CrossRef]
- Wick, J.Y. Aging in Place: Our House Is a Very, Very, Very Fine House. The Consultant Pharmacist 2017, 32, 566–574. [CrossRef]
- Moreno, A.; Scola, M.C.; Sun, H.; Durce, H.; Couve, C.; Acevedo, K.; Gutman, G.M. A Syst. Rev. of gerontechnologies to support aging in place among community-dwelling older adults & their family caregivers. Frontiers in psychology 2023, 14, 18. [CrossRef]
- Shafei, I.; Khadka, J.; Balasubramanian, M. Smart homes: pioneering age-friendly Environ. in China for enhanced health & quality of life. Frontiers in public health 2024, 12, 1346963. [CrossRef]
- Dolman, A.; Kaliappan, S.; Zhou, Y.; Palleti, D.; Marquard, J.; Lee, S.I.; Karkar, R.; Jimison, H.B. A Syst. Rev. of unmet needs of older adults in home settings & their implications for novel technol. solutions. Innovation in aging 2025, 9, 14–23. [CrossRef]
- Tian, Y.J.A.; Felber, N.A.; Pageau, F.; Schwab, D.R.; Wangmo, T. Benefits & barriers associated with the use of smart home health technol. in the care of older persons: a Syst. Rev. BMC geriatrics 2024, 24, 152. [CrossRef]
- Cha, S.M. A Syst. Rev. of Home Modifications for Aging in Place in Older Adults. Healthcare 2025, 13. [CrossRef]
- Dubbeldam, R.; Stemplewski, R.; Pavlova, I.; Cyma-Wejchenig, M.; Lee, S.; Esser, P.; Bentlage, E.; Alcan, V.; Çevik, Ö.S.; Epiphaniou, E.; et al. Technol.-Assisted Physical Activity Interventions for Older People in Their Home-Based Environ.: Scoping Rev. JMIR aging 2025, 8, 25. [CrossRef]
- Moreno, J.A.; Durce, H.; Cifuentes, C.; Múnera, M.; Acevedo-Benítez, K.; Couve, C.; Scola, M.C.; Gutman, G.M. Technol.-assisted home support of community-dwelling older adults living with dementia & their family caregivers: A ten-year Syst. Rev. Gerontechnol. 2024, 24, 1–29. [CrossRef]
- Anghel, I.; Cioara, T.; Moldovan, D.; Antal, M.; Pop, C.D.; Salomie, I.; Pop, C.B.; Chifu, V.R. Smart Environ. & Social Robots for Age-Friendly Integr. Care Services. IJERPH 2020, 17. [CrossRef]
- Engelhardt, S.; Kardas, L.; Kastl, A.; Lüftl, K.; Nick, C.; Rauner, Y. DeinHaus 4.0 Oberbayern. In Digitale Technik für ambulante Pflege & Therapie II; Weber, K.; Haug, S.; Lauer, N.; Mohr, C.; Pfingsten, A.; Raptis, G.; Bahr, G., Eds.; transcript: Bielefeld, 2023; Vol. 3, Regensburger Beiträge zur Digitalisierung des Gesundheitswesens, pp. 29–42. [CrossRef]
- Perez, A.J.; Siddiqui, F.; Zeadally, S.; Lane, D. A Rev. of IoT systems to enable independence for the elderly & disabled individuals. IoT 2023, 21, 100653. [CrossRef]
- Dogra, S.; Dunstan, D.W.; Sugiyama, T.; Stathi, A.; Gardiner, P.A.; Owen, N. Active Aging & Public Health: Evidence, Implications, & Opportunities. Annual Rev. of public health 2022, 43, 439–459. [CrossRef]
- Cahill, J.; McLoughlin, S.; Wetherall, S. The Design of New Technol. Supporting Wellbeing, Independence & Social Participation, for Older Adults Domiciled in Residential Homes &/or Assisted Living Communities. Technologies 2018, 6, 18. [CrossRef]
- Elske, A. Technol. Acceptance Models in Health Informatics. Studies in health technology and informatics 2019, 263, 64–71. [CrossRef]
- Venkatesh, V.; Thong, J.Y.L.; Xu, X. Consumer Acceptance & Use of IT: Extending the UTAUT. MIS Quarterly 2012, 36, 157–178. [CrossRef]
- Alnajim, R.; Alkhalifah, A. Exploring Factors Affecting the Adoption of IoT in Healthcare: A Syst. Lit. Rev. Healthcare 2025, 13. [CrossRef]
- Fakhimi, M.M.; Hughes, A.; Gustavson, A.M. Human-centered design for smart home technol.: a framework for aging & mental health. Frontiers in digital health 2025, 7, 5. [CrossRef]
- Pirzada, P.; Wilde, A.; Doherty, G.H.; Harris-Birtill, D. Ethics & acceptance of smart homes for older adults. Informatics for health & social care 2022, 47, 10–37. [CrossRef]
- Malden, S.; McGill, K.; Guthrie, B.; Frost, H.; Shenkin, S.D.; Ezike, A.; Bareham, B.K.; Mercer, S.W.; Pearce, C.; Wilson, C.; et al. Patient & Carer-Related Facilitators & Barriers to the Adoption of Assistive technol. for the Care of Older Adults: Syst. Rev. JMIR aging 2025, 8, 20. [CrossRef]
- Wilson, A.B.; Villodas, M.L.; Mahadevan, T.; Bosman, E.; Swaine, J.; Gilmore, J.H.; Bowman, L.; Money-Garman, A. Tiny homes-big movement: building a permanent & affordable housing option for people with severe mental illness. Frontiers in public health 2025, 13, 7. [CrossRef]
- Wong, A.; Chen, J.; Dicipulo, R.; Weiss, D.; Sleet, D.A.; Francescutti, L.H. Combatting Homelessness in Canada: Applying Lessons Learned from Six Tiny Villages to the Edmonton Bridge Healing Program. IJERPH 2020, 17. [CrossRef]
- Jackson, A.; Callea, B.; Stampar, N.; Sanders, A.; de Los Rios, A.; Pierce, J. Exploring Tiny Homes as an Affordable Housing Strategy to Ameliorate Homelessness: A Case Study of the Dwellings in Tallahassee, FL. IJERPH 2020, 17. [CrossRef]
- Glumac, B. Tiny portable home: Measuring the rental preferences. Cities 2021, 116, 103279. [CrossRef]
| 1 | Based on prior experiences [17] and accessibility standards (e.g., www.readyhome.de). |
| Category | Representative technologiesi | Diffusionii | Studies |
|---|---|---|---|
| Communication & Social Interaction |
Videocalls, digital companions, voice assistants, social robots, chatbots, games | + | [9,10,11,12] |
| Emergency & safety |
Fall detection, alarm buttons, motion & door sensors, smart lights, stove guard | 0 | [7,8,9,12,13] |
| Health monitoring |
Wearables, Vital sign & Sleep tracking, health data transmission, telemedicine | 0 | [7,9,10,12,13] |
| Information & Documentation |
Medication intake reminders, electronic health records, assistive interfacesiii | + | [9,14] |
| Daily life support | lifting aids, adjustability, service-robots | - | [10,13,15,16] |
| Activity enhancing | fitness & walking aids, activity tracking | o | [14] |
| Integrated Solutions |
Combined Technology Assisted Living (TAL) platforms, IoT-based SHHT, AI-supported environments | - | [7,10,12,13,17] |
| Start to End | Exhibition venuei | Length | Pop.ii | Visitorsiii | |
|---|---|---|---|---|---|
| 05th May | – 09th May | D-93444 Bad Kötzting | 5 days | 7,421 | 220 |
| 12th May | – 30th May | D-84307 Eggenfelden | 9 days | 14,277 | 438 |
| 16th Jun | – 18th Jun | D-84095 Furth (Landshut) | 3 days | 3,679 | 159 |
| 21st Jul | – 24th Jul | D-85049 Ingolstadt | 4 days | 140,717 | 258 |
| 29th Sep | – 02nd Oct | D-85399 Hallbergmoos | 4 days | 11,681 | 153 |
| 10th Oct | – 10th Oct | D-94469 Deggendorf | 1 day | 35,044 | 200 |
| 13th Oct | – 17th Oct | D-95652 Waldsassen | 4 days | 6,698 | 118 |
| 19th Oct | – 19th Oct | D-93138 Lappersdorf | 1 day | 13,472 | 449 |
| 20th Oct | – 22nd Oct | D-93059 Regensburg | 3 days | 151,208 | 166 |
| 10th Nov | – 14th Nov | D-91054 Erlangen | 4 days | 120,301 | 1,475 |
| 15th Nov | – 15th Nov | D-94469 Deggendorf | 1 day | 35,044 | 29 |
| Total exhibition length and visitor counts: | 39 days | 3,665 | |||
| Informal caregivers ()i | Care recipients ()ii | ||
|---|---|---|---|
| Yes, relief trough tech & tiny-home concept i | 98.3% | Yesiii | 100.0% |
| No relief perceived | 1.7% | No | 0.0% |
| Technology Helpfulness (), in% | Affected Area (), in% | ||
|---|---|---|---|
| No AT was helpful | 0.6% | Bathroom | 71.0% |
| One AT was helpful | 34.3% | Living & sleeping | 69.2% |
| More than two ATs helpful | 21.3% | Kitchen | 46.7% |
| More than three ATs helpful | 43.8% | ||
| Question | Group | Yes, n (%) | No, n (%) | Total (N) |
|---|---|---|---|---|
| Can you imagine using the NCM? (dichotomized) |
Care recipients | 22 (91.7%) | 2 (8.3%) | 24 |
| Healthcare workers | 94 (91.3%) | 9 (8.7%) | 103 | |
| General population | 179 (90.4%) | 19 (9.6%) | 198 | |
| Informal caregivers | 52 (89.7%) | 6 (10.3%) | 58 | |
| 347 (90.6%) | 36 (9.4%) | 383 | ||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




