Submitted:
24 February 2026
Posted:
26 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
2.1. Study Design and Cohorts
2.2. Data Collection and Variables
2.3. Patient-Reported Outcomes
2.4. Model Variables
2.5. Statistical Analysis
3. Results
3.1. Patient Characteristics
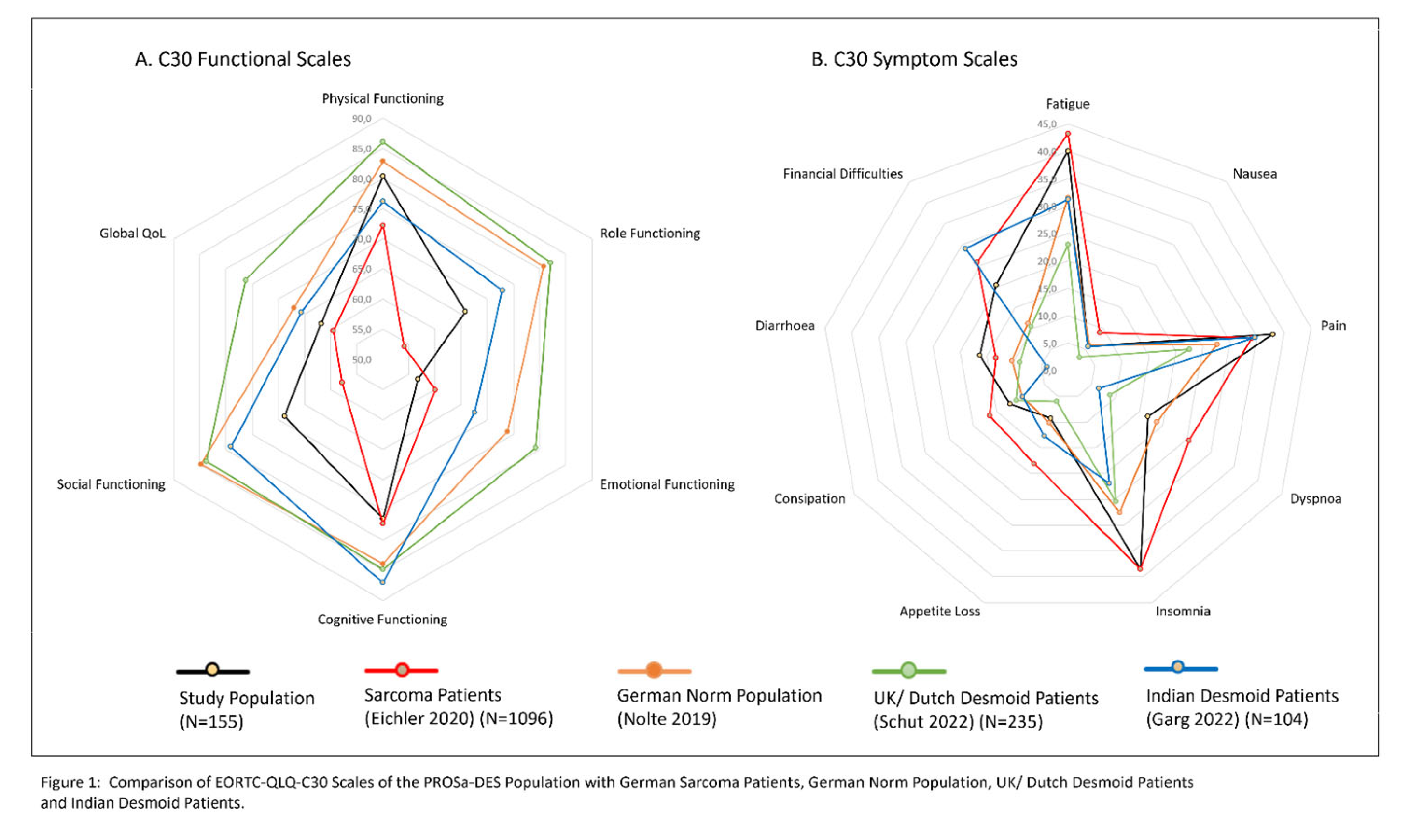
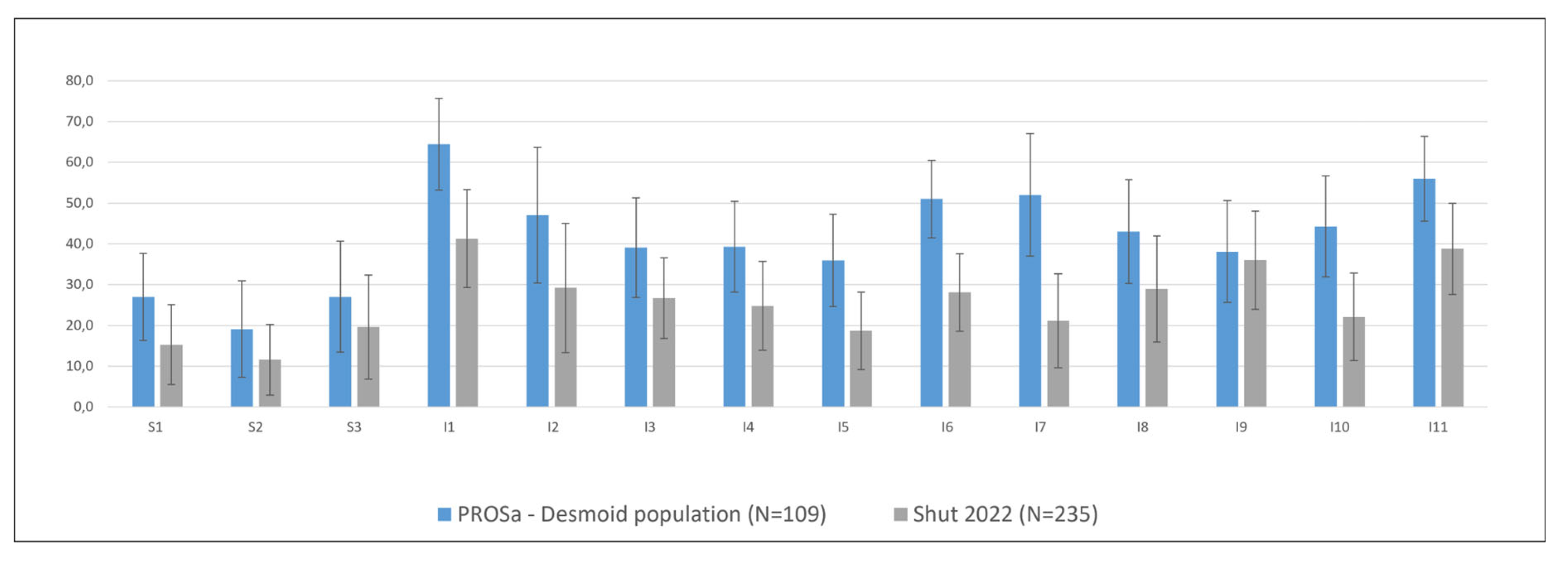
3.2. Quality of Life of Desmoid Patients in Context
3.3. Factors Associated with HRQoL
3.4. Sociodemographic Factors
3.5. Factors Related to the Course of Disease
3.6. Treatment Related Factors
3.7. Tumor Related Factors
4. Discussion
4.1. Quality of Life in Context
4.2. Determinants of HRQoL
4.2.1. Gender
4.2.2. Employment Status
4.3. Disease-Related Factors
4.4. Treatment-Related Factors
4.5. Tumor Location
4.6. Clinical and Psychosocial Implications
4.7. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
AI Disclosure Statement
References
- Hohenberger, P.; Menge, F.; Hohenberger, R.; Kasper, B.; Marx, A.; Haller, F.; Baumgarten, C.; Wardelmann, E.; Jakob, J. Trauma and Sporadic Desmoid Tumor Development: An Approach toward Real Incidence and Aspects of Causality. Cancer 2024, 130, 51–59. [Google Scholar] [CrossRef]
- Lazar, A.J.F.; Tuvin, D.; Hajibashi, S.; Habeeb, S.; Bolshakov, S.; Mayordomo-Aranda, E.; Warneke, C.L.; Lopez-Terrada, D.; Pollock, R.E.; Lev, D. Specific Mutations in the Beta-Catenin Gene (CTNNB1) Correlate with Local Recurrence in Sporadic Desmoid Tumors. Am J Pathol 2008, 173, 1518–1527. [Google Scholar] [CrossRef]
- Trautmann, M.; Rehkämper, J.; Gevensleben, H.; Becker, J.; Wardelmann, E.; Hartmann, W.; Grünewald, I.; Huss, S. Novel Pathogenic Alterations in Pediatric and Adult Desmoid-Type Fibromatosis – A Systematic Analysis of 204 Cases. Sci Rep 2020, 10, 3368. [Google Scholar] [CrossRef] [PubMed]
- Schiessling, S.; Kihm, M.; Ganschow, P.; Kadmon, G.; Büchler, M.W.; Kadmon, M. Desmoid Tumour Biology in Patients with Familial Adenomatous Polyposis Coli. Br J Surg 2013, 100, 694–703. [Google Scholar] [CrossRef] [PubMed]
- Rosa, A.A.; Carolina, A.P.; Marta, A.V.; Francisco, A.; Adriana, F.G.; Natalia, G.; Pablo, L.L.; Cristina, M.F.; Lidia, M.S.; Ulrike, N.; et al. Desmoid Tumors—Experience from a Referral Center, Part 1: Multidisciplinary Review and Practical Recommendations. Cancers 2025, 17, 3470. [Google Scholar] [CrossRef] [PubMed]
- Alman, B.; Attia, S.; Baumgarten, C.; Benson, C.; Blay, J.-Y.; Bonvalot, S.; Breuing, J.; Cardona, K.; Casali, P.G.; Van Coevorden, F.; et al. The Management of Desmoid Tumours: A Joint Global Consensus-Based Guideline Approach for Adult and Paediatric Patients. European Journal of Cancer 2020, 127, 96–107. [Google Scholar] [CrossRef]
- Kasper, B.; Raut, C.P.; Gronchi, A. Desmoid Tumors: To Treat or Not to Treat, That Is the Question. Cancer 2020, 126, 5213–5221. [Google Scholar] [CrossRef]
- Schut, A.-R.W.; Lidington, E.; Timbergen, M.J.M.; Younger, E.; van der Graaf, W.T.A.; van Houdt, W.J.; Bonenkamp, J.J.; Jones, R.L.; Grünhagen, D.J.; Sleijfer, S.; et al. Development of a Disease-Specific Health-Related Quality of Life Questionnaire (DTF-QoL) for Patients with Desmoid-Type Fibromatosis. Cancers (Basel) 2022, 14, 709. [Google Scholar] [CrossRef]
- Gounder, M.M.; Maddux, L.; Paty, J.; Atkinson, T.M. Prospective Development of a Patient-reported Outcomes Instrument for Desmoid Tumors or Aggressive Fibromatosis. Cancer 2020, 126, 531–539. [Google Scholar] [CrossRef]
- Gounder, M.M.; Atkinson, T.M.; Bell, T.; Daskalopoulou, C.; Griffiths, P.; Martindale, M.; Smith, L.M.; Lim, A. GOunder/Desmoid Tumor Research Foundation DEsmoid Symptom/Impact Scale (GODDESS©): Psychometric Properties and Clinically Meaningful Thresholds as Assessed in the Phase 3 DeFi Randomized Controlled Clinical Trial. Qual Life Res 2023, 32, 2861–2873. [Google Scholar] [CrossRef]
- Timbergen, M.J.M.; van der Graaf, W.T.A.; Grünhagen, D.J.; Younger, E.; Sleijfer, S.; Dunlop, A.; Dean, L.; Verhoef, C.; van de Poll-Franse, L.V.; Husson, O. Assessing the Desmoid-Type Fibromatosis Patients’ Voice: Comparison of Health-Related Quality of Life Experiences from Patients of Two Countries. Sarcoma 2020, 2020, 2141939. [Google Scholar] [CrossRef] [PubMed]
- Schut, A.-R.W.; de Bruin, L.E.; de Rooij, B.H.; Lidington, E.; Timbergen, M.J.M.; van der Graaf, W.T.A.; van Houdt, W.J.; Bonenkamp, J.J.; Jones, R.L.; Grünhagen, Dirk.J.; et al. Physical Symptom Burden in Patients with Desmoid-Type Fibromatosis and Its Impact on Health-Related Quality of Life and Healthcare Use. Cancer Medicine 2023, 12, 13661–13674. [Google Scholar] [CrossRef] [PubMed]
- Schut, A.-R.W.; Lidington, E.; Timbergen, M.J.M.; Younger, E.; van der Graaf, W.T.A.; van Houdt, W.J.; Bonenkamp, J.J.; Jones, R.L.; Grünhagen, D.J.; Sleijfer, S.; et al. Unraveling Desmoid-Type Fibromatosis-Specific Health-Related Quality of Life: Who Is at Risk for Poor Outcomes. Cancers (Basel) 2022, 14, 2979. [Google Scholar] [CrossRef] [PubMed]
- Garg, V.; Rastogi, S.; Kalra, K.; Bhoriwal, S.; Barwad, A.; Dhamija, E.; Upadhyay, A.; Gamangatti, S. Health-Related Quality of Life (HRQoL), Anxiety, and Depression in Patients with Desmoid Type Fibromatosis. Support Care Cancer 2022, 30, 10089–10098. [Google Scholar] [CrossRef]
- Eichler, M.; Hentschel, L.; Singer, S.; Hornemann, B.; Richter, S.; Hofbauer, C.; Hohenberger, P.; Kasper, B.; Andreou, D.; Pink, D.; et al. Health Related Quality of Life over Time in German Sarcoma Patients. An Analysis of Associated Factors - Results of the PROSa Study. Frontiers in Endocrinology 2023, 14. [Google Scholar] [CrossRef]
- Aaronson, N.K.; Ahmedzai, S.; Bergman, B.; Bullinger, M.; Cull, A.; Duez, N.J.; Filiberti, A.; Flechtner, H.; Fleishman, S.B.; de Haes, J.C. The European Organization for Research and Treatment of Cancer QLQ-C30: A Quality-of-Life Instrument for Use in International Clinical Trials in Oncology. J. Natl. Cancer Inst. 1993, 85, 365–376. [Google Scholar] [CrossRef]
- Nolte, S.; Liegl, G.; Petersen, M.A.; Aaronson, N.K.; Costantini, A.; Fayers, P.M.; Groenvold, M.; Holzner, B.; Johnson, C.D.; Kemmler, G.; et al. General Population Normative Data for the EORTC QLQ-C30 Health-Related Quality of Life Questionnaire Based on 15,386 Persons across 13 European Countries, Canada and the Unites States. European Journal of Cancer 2019, 107, 153–163. [Google Scholar] [CrossRef]
- Eichler, M.; Hentschel, L.; Richter, S.; Hohenberger, P.; Kasper, B.; Andreou, D.; Pink, D.; Jakob, J.; Singer, S.; Grützmann, R.; et al. The Health-Related Quality of Life of Sarcoma Patients and Survivors in Germany—Cross-Sectional Results of a Nationwide Observational Study (PROSa). Cancers 2020, 12, 3590. [Google Scholar] [CrossRef]
- Eichler, M.; Singer, S.; Hentschel, L.; Richter, S.; Hohenberger, P.; Kasper, B.; Andreou, D.; Pink, D.; Jakob, J.; Grützmann, R.; et al. The Association of Health-Related Quality of Life and 1-Year-Survival in Sarcoma Patients—Results of a Nationwide Observational Study (PROSa). Br J Cancer 2022, 1–9. [Google Scholar] [CrossRef]
- Cocks, K.; King, M.T.; Velikova, G.; Martyn St-James, M.; Fayers, P.M.; Brown, J.M. Evidence-Based Guidelines for Determination of Sample Size and Interpretation of the European Organisation for the Research and Treatment of Cancer Quality of Life Questionnaire Core 30. JCO 2011, 29, 89–96. [Google Scholar] [CrossRef]
- Bektas, M.; Bell, T.; Khan, S.; Tumminello, B.; Fernandez, M.M.; Heyes, C.; Oton, A.B. Desmoid Tumors: A Comprehensive Review. Adv Ther 2023, 40, 3697–3722. [Google Scholar] [CrossRef]
- Husson, O.; Younger, E.; Dunlop, A.; Dean, L.; Strauss, D.C.; Benson, C.; Hayes, A.J.; Miah, A.; Van Houdt, W.; Zaidi, S.; et al. Desmoid Fibromatosis through the Patients’ Eyes: Time to Change the Focus and Organisation of Care? Support Care Cancer 2019, 27, 965–980. [Google Scholar] [CrossRef] [PubMed]
- Penel, N.; Bonvalot, S.; Le Deley, M.-C.; Italiano, A.; Tlemsani, C.; Pannier, D.; Leguillette, C.; Kurtz, J.-E.; Toulmonde, M.; Thery, J.; et al. Pain in Desmoid-Type Fibromatosis: Prevalence, Determinants and Prognosis Value. Int J Cancer 2023, 153, 407–416. [Google Scholar] [CrossRef] [PubMed]
- Gounder, M.; Ratan, R.; Alcindor, T.; Schöffski, P.; van der Graaf, W.T.; Wilky, B.A.; Riedel, R.F.; Lim, A.; Smith, L.M.; Moody, S.; et al. Nirogacestat, a γ-Secretase Inhibitor for Desmoid Tumors. N Engl J Med 2023, 388, 898–912. [Google Scholar] [CrossRef] [PubMed]
- van Eck, I.; den Hollander, D.; Desar, I.M.E.; Soomers, V.L.M.N.; van de Sande, M.A.J.; de Haan, J.J.; Verhoef, C.; Vriens, I.J.H.; Bonenkamp, J.J.; van der Graaf, W.T.A.; et al. Unraveling the Heterogeneity of Sarcoma Survivors’ Health-Related Quality of Life Regarding Primary Sarcoma Location: Results from the SURVSARC Study. Cancers 2020, 12, 3083. [Google Scholar] [CrossRef]
- Timbergen, M.J.M.; van der Graaf, W.T.A.; Grünhagen, D.J.; Younger, E.; Sleijfer, S.; Dunlop, A.; Dean, L.; Verhoef, C.; van de Poll-Franse, L.V.; Husson, O. Assessing the Desmoid-Type Fibromatosis Patients’ Voice: Comparison of Health-Related Quality of Life Experiences from Patients of Two Countries. Sarcoma 2020, 2020, 2141939. [Google Scholar] [CrossRef]
- Ingley, K.M.; Klein, R.; Theobalds, N.; Burtenshaw, S.; Abdul Razak, A.R.; Chen, B.; Xu, W.; Gladdy, R.; Li, M.; Gupta, A.A. High Prevalence of Persistent Emotional Distress in Desmoid Tumor. Psychooncology 2020, 29, 311–320. [Google Scholar] [CrossRef]
- Schwarz, R.; Hinz, A. Reference Data for the Quality of Life Questionnaire EORTC QLQ-C30 in the General German Population. European Journal of Cancer 2001, 37, 1345–1351. [Google Scholar] [CrossRef]
- Eichler, M.; Hentschel, L.; Singer, S.; Hornemann, B.; Hohenberger, P.; Kasper, B.; Andreou, D.; Pink, D.; Jakob, J.; Arndt, K.; et al. Distress in Soft-Tissue Sarcoma and Gastrointestinal Stromal Tumours Patients—Results of a German Multicentre Observational Study (PROSa). Psycho-Oncology 2022, 31, 1700–1710. [Google Scholar] [CrossRef]
- Singer, S.; Szalai, C.; Briest, S.; Brown, A.; Dietz, A.; Einenkel, J.; Jonas, S.; Konnopka, A.; Papsdorf, K.; Langanke, D.; et al. Co-Morbid Mental Health Conditions in Cancer Patients at Working Age – Prevalence, Risk Profiles, and Care Uptake. Psycho-Oncology 2013, 22, 2291–2297. [Google Scholar] [CrossRef]
- Gutiérrez-Rojas, L.; Porras-Segovia, A.; Dunne, H.; Andrade-González, N.; Cervilla, J.A. Prevalence and Correlates of Major Depressive Disorder: A Systematic Review. Braz J Psychiatry 2020, 42, 657–672. [Google Scholar] [CrossRef]
- Tansir, G.; Sharma, A.; Biswas, B.; Sah, S.N.; Roy, S.; Deo, S.V.S.; Agarwala, S.; Khan, S.A.; Bakhshi, S.; Pushpam, D. A Real-World Study on the Clinicopathological Profile, Treatment Outcomes and Health-Related Quality of Life, Anxiety and Depression among Patients with Desmoid Tumor at Two Tertiary Care Centers in India. Front Oncol 2024, 14, 1382856. [Google Scholar] [CrossRef]
- Alman, B.; Attia, S.; Baumgarten, C.; Benson, C.; Blay, J.-Y.; Bonvalot, S.; Breuing, J.; Cardona, K.; Casali, P.G.; van Coevorden, F.; et al. The Management of Desmoid Tumours: A Joint Global Consensus-Based Guideline Approach for Adult and Paediatric Patients. European Journal of Cancer 2020, 127, 96–107. [Google Scholar] [CrossRef]
- Gounder, M.M.; Mahoney, M.R.; Van Tine, B.A.; Ravi, V.; Attia, S.; Deshpande, H.A.; Gupta, A.A.; Milhem, M.M.; Conry, R.M.; Movva, S.; et al. Sorafenib for Advanced and Refractory Desmoid Tumors. N Engl J Med 2018, 379, 2417–2428. [Google Scholar] [CrossRef]
- Toulmonde, M.; Pulido, M.; Ray-Coquard, I.; Andre, T.; Isambert, N.; Chevreau, C.; Penel, N.; Bompas, E.; Saada, E.; Bertucci, F.; et al. Pazopanib or Methotrexate-Vinblastine Combination Chemotherapy in Adult Patients with Progressive Desmoid Tumours (DESMOPAZ): A Non-Comparative, Randomised, Open-Label, Multicentre, Phase 2 Study. Lancet Oncol 2019, 20, 1263–1272. [Google Scholar] [CrossRef]
| Variable | Complete Dataset | PROSa-Desmoid | PROSa | |||
|---|---|---|---|---|---|---|
| Value | N | % | N | % | N | % |
| All | 155 | 109 | 70.3 | 46 | 29.7 | |
| Age Groups | ||||||
| 18-35 | 45 | 29.6 | 29 | 26.9 | 16 | 36.4 |
| 36-55 | 74 | 48.7 | 57 | 52.8 | 17 | 38.6 |
| > 55 | 33 | 21.7 | 22 | 20.4 | 11 | 25 |
| Age (mean. SD) | 45.0 | 14.3 | 45.7 | 14.1 | 43.4 | 14.8 |
| Gender | ||||||
| female | 108 | 69.7 | 76 | 69.7 | 32 | 69.6 |
| male | 45 | 29 | 31 | 28.4 | 14 | 30.4 |
| diverse | 2 | 1.3 | 2 | 1.8 | 0 | 0 |
| Time since diagnosis | ||||||
| 0-<5 year | 64 | 41.6 | 29 | 26.6 | 35 | 77.8 |
| 5-<10 year | 34 | 22.1 | 31 | 28.4 | 3 | 6.7 |
| > 10 years | 56 | 36.4 | 49 | 45 | 7 | 15.6 |
| Time since diagnosis (mean. SD) | 7.9 | 6.4 | 9.5 | 6.1 | 4.0 | 5.4 |
| Time since treatment | ||||||
| in treatment | 17 | 17.9 | ||||
| 0-<5 years | 28 | 25.7 | ||||
| 5-<10 years | 30 | 31.6 | ||||
| more than 10 years | 20 | 21.1 | ||||
| Time since treatment (mean. SD) | 5.8 | 4.7 | ||||
| Medical lines | ||||||
| 0 to 1 | 83 | 53.5 | ||||
| 2 or more | 23 | 14.8 | ||||
| unknown | 3 | 1.9 | ||||
| Recurrence after Surgery | ||||||
| no | 52 | 33.5 | 33 | 30.3 | 19 | 41.3 |
| yes | 60 | 38.7 | 43 | 39.4 | 17 | 37 |
| unknown or no OP | 43 | 27.7 | 33 | 30.3 | 10 | 21.7 |
| Tumor Location | ||||||
| Lower extremity (incl hip/ pelvis) | 48 | 31 | 32 | 29.4 | 16 | 34.8 |
| Shoulder & upper extremity | 12 | 7.7 | 8 | 7.3 | 4 | 8.7 |
| Trunk (thoracic wall & back) | 27 | 17.4 | 20 | 18.3 | 7 | 15.2 |
| Abdominal wall | 17 | 11 | 17 | 15.6 | 0 | 0 |
| Intra-abdominal | 36 | 23.2 | 24 | 22 | 12 | 26.1 |
| Head & neck | 8 | 5.2 | 7 | 6.4 | 1 | 2.2 |
| not defined/ multifocal | 7 | 4.5 | 1 | 0.9 | 6 | 13 |
| Received treatments | ||||||
| surgery only | 30 | 27.5 | ||||
| ST only | 14 | 12.8 | ||||
| ST + surgery | 19 | 17.4 | ||||
| ST + RT + surgery | 21 | 19.3 | ||||
| none (W&W) | 7 | 6.4 | ||||
| all other | 18 | 16.5 | ||||
| Education | ||||||
| basic/ medium | 58 | 37.7 | 36 | 33 | 22 | 48.9 |
| high | 96 | 62.3 | 73 | 67 | 23 | 51.1 |
| Status Employment | ||||||
| employed | 114 | 73.5 | 78 | 71.6 | 36 | 78.3 |
| unemployed. disability pension | 17 | 11 | 14 | 12.8 | 3 | 6.5 |
| retirement pension | 15 | 9.7 | 12 | 11 | 3 | 6.5 |
| other | 9 | 5.8 | 5 | 4.6 | 4 | 8.7 |
| Desmoid-Type Fibromatosis Quality of Life Questionnaire (DTF QoL) | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Symptom Scales B (p) |
Impact Scales B (p) |
|||||||||||||
| W1 Emotional consequences |
W2 Physical consequences |
W3 Pain and discomfort |
1 Concerns Condition |
2 Job & Education |
3 Doctor–patient relationship |
4 Effect of DTF on relationships |
5 Physical limitations and consequences |
6 Diagnostic and treatment trajectory |
7 Parenting and fertility |
8 Body image and sensation |
9 Supportive care |
10 Concerns around treatment and its consequences |
11 Unpredictable course and nature of DTF |
|
| Age Groups | ||||||||||||||
| 18-35 years (ref) | ||||||||||||||
| 36-55 years | / | / | / | -1,2 (0,81) |
/ | / | / | / | / |
-43,2 (0,00) |
2,5 (0,65) |
/ | / | / |
| > 55 years | / | / | / | -11,3 (0,07) |
/ | / | / | / | / | -6,5 (0,40) |
-8,5 (0,22) |
/ | / | / |
| Gender* | ||||||||||||||
| woman (ref) | ||||||||||||||
| men |
-11,9 (<,01) |
-12,2 (<,01) |
-15,7 (<,01) |
-10,4 (0,03) |
/ |
-17,6 (<,001) |
-19,2 (<,001) |
-13,5 (<,01) |
-13,0 (<,001) |
-26,6 (<,001) |
-14,7 (<,01) |
-16,3 (<,001) |
-15,4 (<,01) |
-14,9 (<,001) |
| Time since treatment | ||||||||||||||
| In treatment (ref) | ||||||||||||||
| 0–<5 years | / | / | / | / | / | / | / | / | / | / | / | / | / | / |
| 5–<10 years | / | / | / | / | / | / | / | / | / | / | / | / | / | / |
| >10 years | / | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Time since diagnosis | ||||||||||||||
| 0–<5 years (ref.) | ||||||||||||||
| 5–<10 years | / |
11,5 (0,03) |
/ | / | / | / | / | / | / | / | / | -6,1 (0,31) |
/ | / |
| >10 years | / | 1,7 (0,73) |
/ | / | / | / | / | / | / | / | / | -8,9 (0,12) |
/ | / |
| No of ST lines | ||||||||||||||
| 0 or 1 line (ref.) | ||||||||||||||
| ≥2 lines | 7,3 (0,11) |
/ |
19,0 (<,01) |
7,7 (0,14) |
12,3 (0,09) |
/ | 5,5 (0,24) |
8,4 (0,09) |
/ | / |
15,3 (<,01) |
/ | 9,7 (0,07) |
13,9 (<,01) |
| Recurrence* | ||||||||||||||
| no (ref.) | ||||||||||||||
| yes | / | / | / | / | / | / | / | / | / | -13,3 (0,10) |
/ |
-11,4 (0,03) |
/ | / |
| Tumor location* | ||||||||||||||
| Lower extremity (incl hip/ pelvis) (ref.) |
||||||||||||||
| Upper extremity | / |
-17,2 (0,02) |
6,3 (0,46) |
/ | / | / | / | / | / |
-46,5 (<,01) |
/ | / |
-24,3 (<,01) |
/ |
| Trunk (thoracic wall & back) |
/ |
-13,0 (0,02) |
-10,1 (0,12) |
/ | / | / | / | / | / | -17,2 (0,09) |
/ | / | -7,0 (0,23) |
/ |
| Abdominal wall | / |
-16,0 (<,01) |
-12,4 (0,07) |
/ | / | / | / | / | / | -10,2 (0,29) |
/ | / |
-14,1 (0,02) |
/ |
| Intra-abdominal | / | -10,6 (0,06) |
-8,2 (0,20) |
/ | / | / | / | / | / | 1,2 (0,90) |
/ | / | -7,7 (0,19) |
/ |
| Head & Neck | / |
-18,2 (0,02) |
-4,3 (0,64) |
/ | / | / | / | / | / | -30,5 (0,06) |
/ | / |
-26,6 (<,01) |
/ |
| Received treatments* | ||||||||||||||
| Surgery and/ or ST (ref.) |
||||||||||||||
| ST + RT + surgery | / |
11,9 (0,02) |
9,9 (0,09) |
7,3 (0,18) |
/ | / | / |
11,8 (0,02) |
7,4 (0,10) |
/ | 9,1 (0,13) |
/ |
11,5 (0,03) |
6,8 (0,16) |
| Education | ||||||||||||||
| basic/ medium (ref.) | ||||||||||||||
| high | / | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Status Employment* | ||||||||||||||
| employed (ref.) | ||||||||||||||
| unemployed, disability pension |
26,0 (<,001) |
26,7 (<,001) |
16,9 (0,01) |
/ |
44,5 (<,001) |
/ |
25,4 (<,001) |
20,9 (<,001) |
/ | / | / | / |
18,8 (<,01) |
/ |
| retirement pension | 5,8 (0,33) |
11,3 (0,05) |
-1,1 (0,87) |
/ | 16,8 (0,20) |
/ | 5,0 (0,40) |
9,4 (0,13) |
/ | / | / | / | -1,5 (0,83) |
/ |
| European Organisation for Research and Treatment of Cancer Quality of Life Core Questionnaire (EORTC QLQ-C30) | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Functional Scales B (p) |
Symptom Scales B (p) |
||||||||||||||
| PF (N=109) | RF (N=109) | EF (N=154) | CF (N=109) | SF (N=154) | Global QoL (N=107) | FA (N=109) | NV (N=151) | Pain (N=109) | Dyspnea (N=153) | Insomnia (N=154) | Appetite Loss (N=155) | Constipation (N=154) | Diarrhea (N=109) | Financial Diff (N=152) | |
| Age Groups | |||||||||||||||
| 18-35 years (ref) | |||||||||||||||
| 36-55 years | / | / | / | / | / | / | / | -6.1 (0.01) | / | -7.6 (0.11) | / | / | / | / | / |
| > 55 years | / | / | / | / | / | / | / | -12.6 (<.001) | / | -0.5 (0.94) | / | / | / | / | / |
| Gender* | |||||||||||||||
| woman (ref) | |||||||||||||||
| men | 13.1 (<.001) | / | 16.2 (<.001) | / | / | 12.4 (<.01) | / | / | -23.2 (<.001) | / | / | / | / | / | / |
| Time since treatment | |||||||||||||||
| In treatment (ref) | |||||||||||||||
| 0–<5 years | / | / | / | 2.3 (0.77) |
/ | -3.9 (0.46) | -4.3 (0.60) | / | / | / | / | / | / | / | / |
| 5–<10 years | / | / | / | 6.2 (0.42) |
/ | -0.9 (0.87) | -6.2 (0.45) | / | / | / | / | / | / | / | / |
| >10 years | / | / | / | 20.0 (0.02) | / | 7.7 (0.19) |
-17.9 (0.04) | / | / | / | / | / | / | / | / |
| Time since diagnosis | |||||||||||||||
| 0–<5 years (ref.) | |||||||||||||||
| 5–<10 years | / | / | / | / | / | / | / | 2.2 (0.41) |
/ | / | -3.5 (0.60) | / | / | 3.5 (0.62) |
/ |
| >10 years | / | / | / | / | / | / | / | -3.1 (0.19) | / | / | -12.2 (0.03) | / | / | -10.7 (0.09) | / |
| No. of ST lines | |||||||||||||||
| 0 or 1 line (ref.) | |||||||||||||||
| ≥2 lines | / | / | / | / | / | / | / | / | 12.0 (0.07) | / | / | / | / | 13.4 (0.04) | / |
| Recurrence* | |||||||||||||||
| no (ref.) | |||||||||||||||
| yes | / | / | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Tumor location* | |||||||||||||||
| Lower extremity (incl hip/ pelvis) (ref.) | |||||||||||||||
| Upper extremity | 9.9 (0.13) |
/ | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Trunk (thoracic wall & back) | 12.8 (0.01) | / | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Abdominal wall | 11.4 (0.03) | / | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Intra-abdominal | 1.8 (0.71) |
/ | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Head & Neck | 5.5 (0.42) |
/ | / | / | / | / | / | / | / | / | / | / | / | / | / |
| Received treatments* | |||||||||||||||
| surgery and/ or ST (ref.) | |||||||||||||||
| ST + RT + surgery | -15.3 (<.001) | -12.9 (0.07) | / | / | / | -9.6 (0.02) | 12.1 (0.07) | / | 13.9 (0.04) | / | / | / | / | / | / |
| Education | |||||||||||||||
| basic/ medium (ref.) | |||||||||||||||
| high | / | / | / | / | / | / | / | / | / | / | / | / | 8.4 (0.05) |
-8.8 (0.15) | / |
| Status Employment* | |||||||||||||||
| employed (ref.) | |||||||||||||||
| unemployed, disability pension | -27.4 (<.001) | -33.0 (<.001) | -23.8 (<.001) | -34.9 (<.001) | -40.3 (<.001) | -25.3 (<.001) | 31.8 (<.001) | 15.3 (<.001) | 33.5 (<.001) | 12.7 (0.07) | 39.6 (<.001) | 14.3 (<.01) | / | / | 48.5 (<.001) |
| retirement pension | -4.4 (0.41) | -10.0 (0.25) | 2.9 (0.68) |
-5.2 (0.51) | -6.9 (0.38) | -3.5 (0.52) | 1.7 (0.83) |
6.8 (0.12) |
-0.6 (0.94) | 9.7 (0.26) |
8.7 (0.31) |
3.8 (0.46) |
/ | / | 10.5 (0.18) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




