Submitted:
13 February 2026
Posted:
18 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Model Overview
Bone Segment Geometry
Osteotomy Conditions
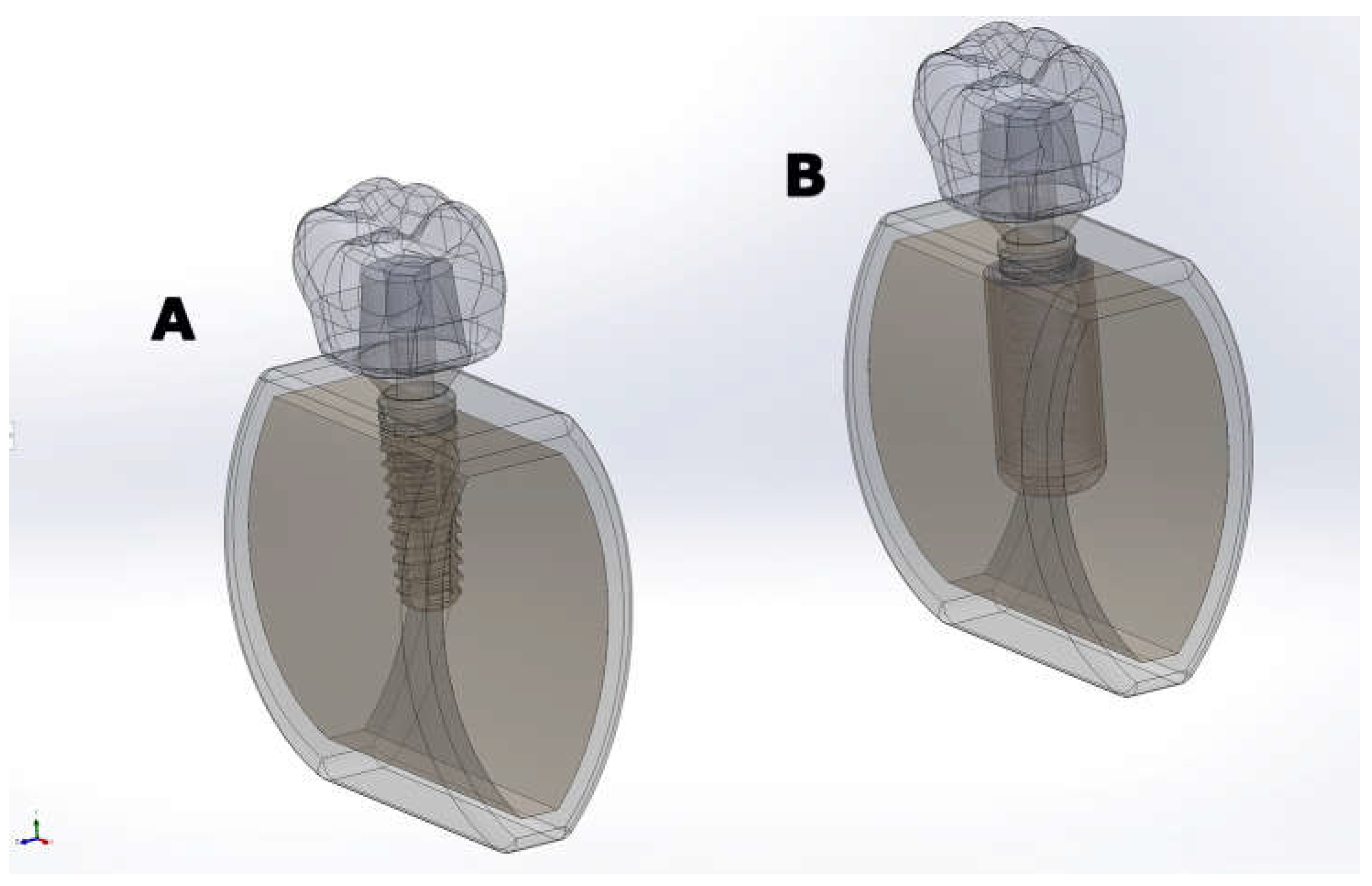
Implant–Restoration Assembly
Material Properties
Meshing and Convergence
Contact Definitions and Boundary Conditions
Loading Conditions
Outcome Measures and Strain Post-Processing
3. Results
3.1. Cortical Bone Strain Outcomes
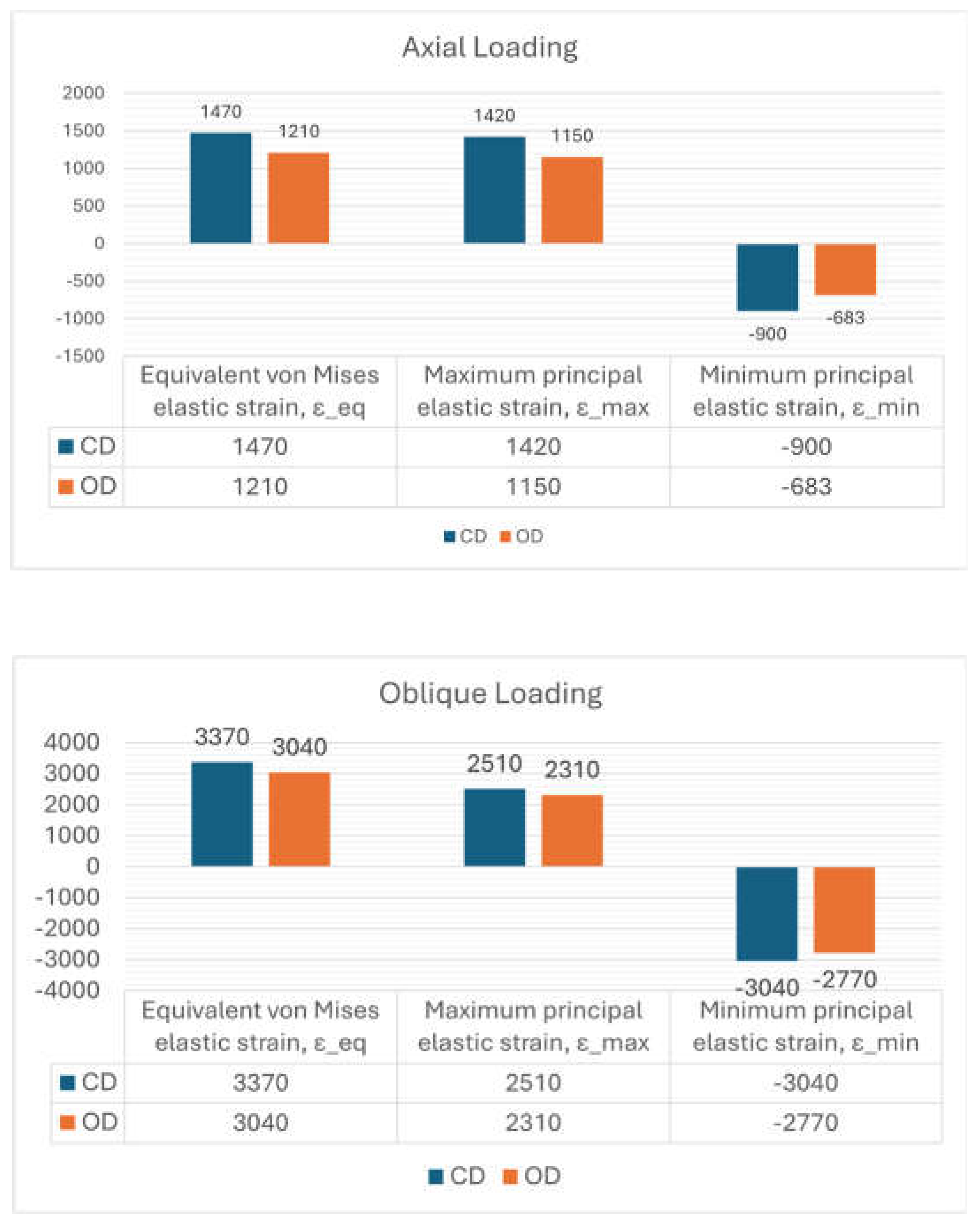
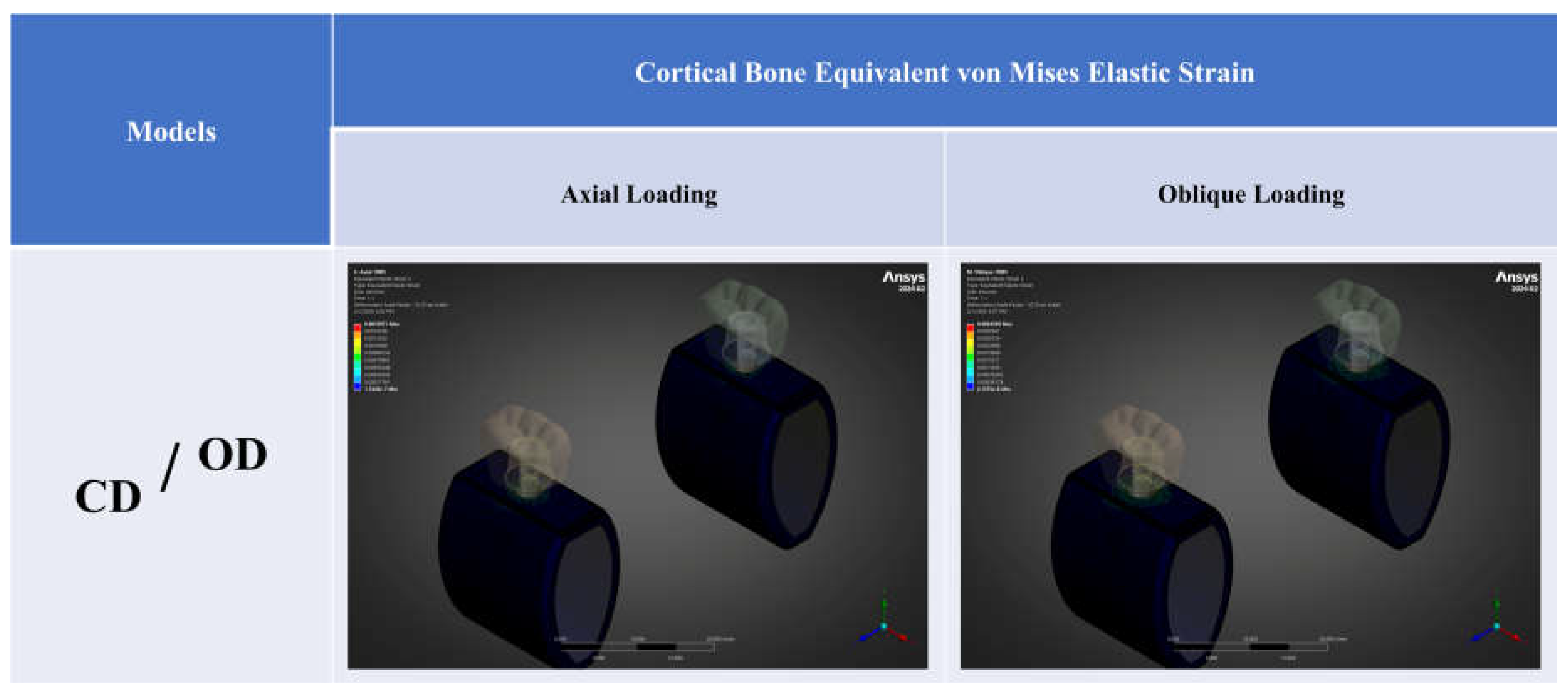
3.2. Equivalent (von Mises) Elastic Strain
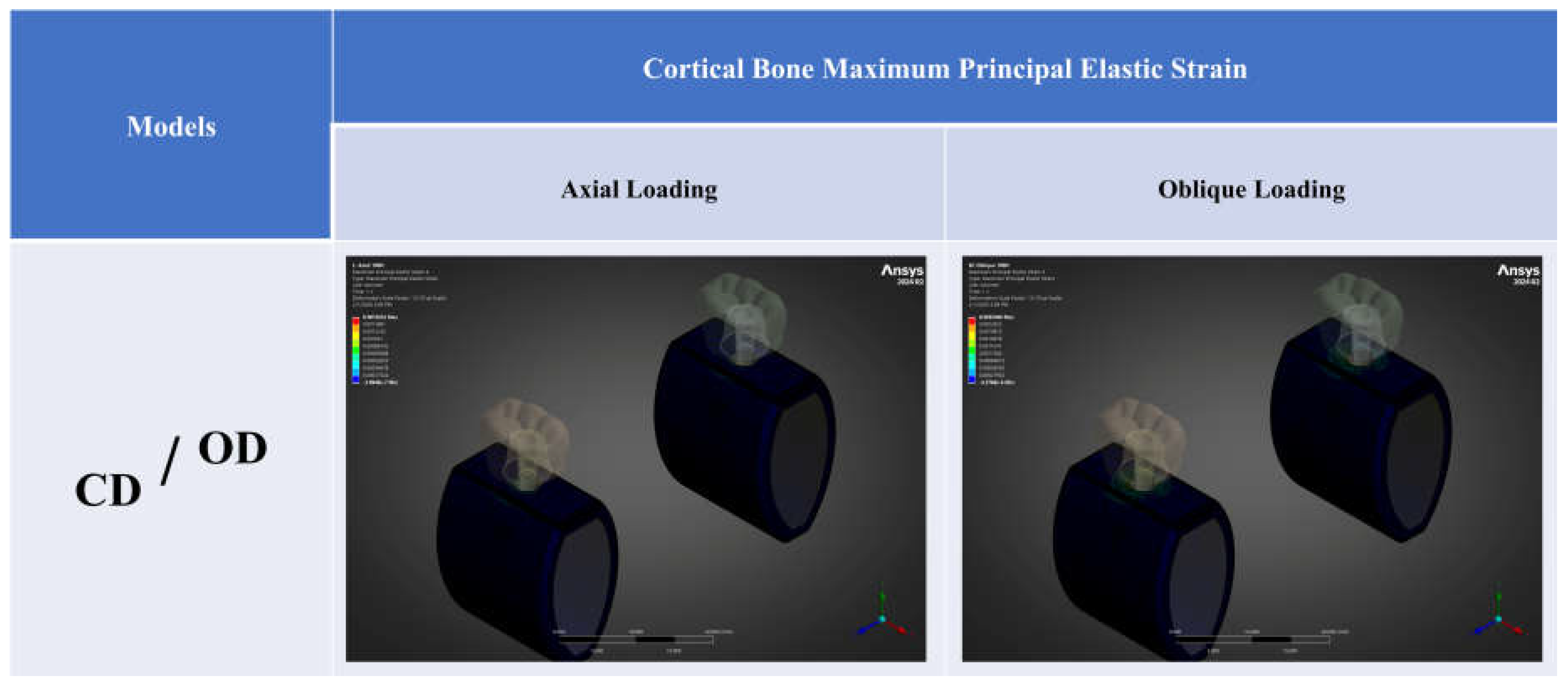
3.3. Maximum Principal (Tensile) Elastic Strain
3.4. Minimum Principal (Compressive) Elastic Strain
4. Discussion
Mechanostat-Informed Interpretation of Peri-Implant Strain Magnitudes
Relationship to the Osseodensification Evidence Base
Why the Crestal Cortical Region Is a Critical Area in Low-Density Cancellous Bone
Clinical Implications and Cautious Translation
Limitations and Future Research Directions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| BMD | Bone mineral density |
| CD | Conventional drilling |
| D1–D4 | Cancellous bone density classes (Lekholm & Zarb classification) |
| FEA | Finite element analysis |
| ISQ | Implant stability quotient |
| MRONJ | Medication-related osteonecrosis of the jaw |
| OD | Osseodensification |
| ROI | Region of interest |
| εeq | Equivalent (von Mises) elastic strain |
| εmax | Maximum principal (tensile) elastic strain |
| εmin | Minimum principal (compressive) elastic strain |
| µε | Microstrain (10−6 strain) |
References
- Isaacson, BM; Jeyapalina, S. Osseointegration: a review of the fundamentals for assuring cementless skeletal fixation. Orthopedic Research and reviews 2014, 2014(6), 55–65. [Google Scholar] [CrossRef]
- Mukhopadhaya, J; Bhadani, JS. Fixation Failure in Osteoporotic Bone: A Review of Complications and Outcomes. Indian J Orthop. 2025, 59(3), 389–404. [Google Scholar] [CrossRef] [PubMed]
- Tandon, V; Franke, J; Kalidindi, KKV. Advancements in osteoporotic spine fixation. J Clin Orthop Trauma. 2020, 11(5), 778–85. [Google Scholar] [CrossRef] [PubMed]
- Sözen, T; Özışık, L; Başaran, N. An overview and management of osteoporosis. Eur J Rheumatol. 2017, 4(1), 46–56. [Google Scholar] [CrossRef] [PubMed]
- Shen, Y; Huang, X; Wu, J; Lin, X; Zhou, X; Zhu, Z; et al. The Global Burden of Osteoporosis, Low Bone Mass, and Its Related Fracture in 204 Countries and Territories, 1990-2019. Front Endocrinol (Lausanne) 2022, 13, 882241. [Google Scholar] [CrossRef]
- Sànchez-Riera, L; Wilson, N; Kamalaraj, N; Nolla, JM; Kok, C; Li, Y; et al. Osteoporosis and fragility fractures. Best Pract Res Clin Rheumatol. 2010, 24(6), 793–810. [Google Scholar] [CrossRef]
- de Medeiros, F; Kudo, GAH; Leme, BG; Saraiva, PP; Verri, FR; Honório, HM; et al. Dental implants in patients with osteoporosis: a systematic review with meta-analysis. Int J Oral Maxillofac Surg. 2018, 47(4), 480–91. [Google Scholar] [CrossRef]
- Lemos, CAA; de Oliveira, AS; Faé, DS; Oliveira, H; Del Rei Daltro Rosa, CD; Bento, VAA; et al. Do dental implants placed in patients with osteoporosis have higher risks of failure and marginal bone loss compared to those in healthy patients? A systematic review with meta-analysis. Clin Oral Investig. 2023, 27(6), 2483–93. [Google Scholar] [CrossRef]
- Seo, DD; Borke, JL. Medication-Related Osteonecrosis of the Jaw–2024 Update. Oral Health Dental Sci. 2024, 8(1), 1–6. [Google Scholar] [CrossRef]
- Andersen, SWM; Hindocha, NV; Poulsen, I; Schliephake, H; Jensen, SS. Medication-Related Osteonecrosis of the Jaws in Patients on Antiresorptive Medication With Dental Implants. A Scoping Review. Clin Oral Implants Res. 2025, 36(10), 1173–201. [Google Scholar] [CrossRef]
- Ruggiero, SL; Dodson, TB; Aghaloo, T; Carlson, ER; Ward, BB; Kademani, D. American Association of Oral and Maxillofacial Surgeons’ Position Paper on Medication-Related Osteonecrosis of the Jaws-2022 Update. J Oral Maxillofac Surg. 2022, 80(5), 920–43. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, D; Sennerby, L; Jagger, D; Meredith, N. A comparison of two methods of enhancing implant primary stability. Clin Implant Dent Relat Res. 2004, 6(1), 48–57. [Google Scholar] [CrossRef] [PubMed]
- Huwais, S; Meyer, EG. A Novel Osseous Densification Approach in Implant Osteotomy Preparation to Increase Biomechanical Primary Stability, Bone Mineral Density, and Bone-to-Implant Contact. Int J Oral Maxillofac Implants 2017, 32(1), 27–36. [Google Scholar] [CrossRef] [PubMed]
- Trisi, P; Berardini, M; Falco, A; Podaliri Vulpiani, M. New Osseodensification Implant Site Preparation Method to Increase Bone Density in Low-Density Bone: In Vivo Evaluation in Sheep. Implant Dent. 2016, 25(1), 24–31. [Google Scholar] [CrossRef]
- Bergamo, ETP; Zahoui, A; Barrera, RB; Huwais, S; Coelho, PG; Karateew, ED; Bonfante, EA. Osseodensification effect on implants primary and secondary stability: Multicenter controlled clinical trial. Clin Implant Dent Relat Res. 2021, 23(3), 317–28. [Google Scholar] [CrossRef]
- Frost, HM. Bone’s mechanostat: a 2003 update. Anat Rec A Discov Mol Cell Evol Biol. 2003, 275(2), 1081–101. [Google Scholar] [CrossRef]
- Sugiyama, T; Meakin, LB; Browne, WJ; Galea, GL; Price, JS; Lanyon, LE. Bones’ adaptive response to mechanical loading is essentially linear between the low strains associated with disuse and the high strains associated with the lamellar/woven bone transition. J Bone Miner Res. 2012, 27(8), 1784–93. [Google Scholar] [CrossRef]
- Marques, FC; Boaretti, D; Walle, M; Scheuren, AC; Schulte, FA; Müller, R. Mechanostat parameters estimated from time-lapsed in vivo micro-computed tomography data of mechanically driven bone adaptation are logarithmically dependent on loading frequency. Front Bioeng Biotechnol. 2023, 11, 1140673. [Google Scholar] [CrossRef]
- Fontes Pereira, J; Costa, R; Nunes Vasques, M; Salazar, F; Mendes, JM; Infante da Câmara, M. Osseodensification: An Alternative to Conventional Osteotomy in Implant Site Preparation: A Systematic Review. J Clin Med. 2023, 12(22). [Google Scholar] [CrossRef]
- Meslier, QA; Shefelbine, SJ. Using Finite Element Modeling in Bone Mechanoadaptation. Curr Osteoporos Rep. 2023, 21(2), 105–16. [Google Scholar] [CrossRef]
- Premnath, K; Sridevi, J; Kalavathy, N; Nagaranjani, P; Sharmila, MR. Evaluation of stress distribution in bone of different densities using different implant designs: a three-dimensional finite element analysis. J Indian Prosthodont Soc. 2013, 13(4), 555–9. [Google Scholar] [CrossRef]
- Lahens, B; Neiva, R; Tovar, N; Alifarag, AM; Jimbo, R; Bonfante, EA; et al. Biomechanical and histologic basis of osseodensification drilling for endosteal implant placement in low density bone. An experimental study in sheep. J Mech Behav Biomed Mater. 2016, 63, 56–65. [Google Scholar] [CrossRef] [PubMed]
- Pisarciuc, C; Dan, I; Cioară, R. The Influence of Mesh Density on the Results Obtained by Finite Element Analysis of Complex Bodies. Materials (Basel) 2023, 16(7). [Google Scholar] [CrossRef] [PubMed]
- Falcinelli, C; Valente, F; Vasta, M; Traini, T. Finite element analysis in implant dentistry: State of the art and future directions. Dent Mater. 2023, 39(6), 539–56. [Google Scholar] [CrossRef] [PubMed]
- Frost, HM. Bone “mass” and the “mechanostat”: a proposal. Anat Rec. 1987, 219(1), 1–9. [Google Scholar] [CrossRef]
- Lahens, B; Lopez, CD; Neiva, RF; Bowers, MM; Jimbo, R; Bonfante, EA; et al. The effect of osseodensification drilling for endosteal implants with different surface treatments: A study in sheep. J Biomed Mater Res B Appl Biomater. 2019, 107(3), 615–23. [Google Scholar] [CrossRef]
- Turner, CH. Three rules for bone adaptation to mechanical stimuli. Bone 1998, 23(5), 399–407. [Google Scholar] [CrossRef]
- Warden, SJ; Hurst, JA; Sanders, MS; Turner, CH; Burr, DB; Li, J. Bone adaptation to a mechanical loading program significantly increases skeletal fatigue resistance. J Bone Miner Res. 2005, 20(5), 809–16. [Google Scholar] [CrossRef]
- Szmukler-Moncler, S; Salama, H; Reingewirtz, Y; Dubruille, JH. Timing of loading and effect of micromotion on bone-dental implant interface: review of experimental literature. J Biomed Mater Res. 1998, 43(2), 192–203. [Google Scholar] [CrossRef]
- Szmukler-Moncler, S; Piattelli, A; Favero, GA; Dubruille, JH. Considerations preliminary to the application of early and immediate loading protocols in dental implantology. Clin Oral Implants Res. 2000, 11(1), 12–25. [Google Scholar] [CrossRef]
- Koc, D; Dogan, A; Bek, B. Bite force and influential factors on bite force measurements: a literature review. Eur J Dent. 2010, 4(2), 223–32. [Google Scholar] [CrossRef]
- Mathur, VP; Atif, M; Duggal, I; Tewari, N; Duggal, R; Chawla, A. Reporting guidelines for in-silico studies using finite element analysis in medicine (RIFEM). Comput Methods Programs Biomed. 2022, 216, 106675. [Google Scholar] [CrossRef]
| Material | Modulus of elasticity (GPa) | Poisson’s ratio (ν) |
|---|---|---|
| Cortical bone | 14.8 | 0.30 |
| Cancellous bone D1 | 9.5 | 0.30 |
| Cancellous bone D2 | 5.5 | 0.30 |
| Cancellous bone D3 | 1.6 | 0.30 |
| Cancellous bone D4 | 0.69 | 0.30 |
| Titanium (implant, abutment) | 110 | 0.35 |
| Zirconia | 210 | 0.33 |
| Strain measure (cortical bone) |
Axial loading | Oblique loading | ||||
|---|---|---|---|---|---|---|
| CD (µε) | OD (µε) | Δ% | CD (µε) | OD (µε) | Δ% | |
| Equivalent von Mises elastic strain, εeq | 1470 | 1210 | -17.7% | 3370 | 3040 | -9.8% |
| Maximum principal elastic strain, εmax | 1420 | 1150 | -19.0% | 2510 | 2310 | -8.0% |
| Minimum principal elastic strain, εmin | -900 | -683 | -24.1% | -3040 | -2770 | -8.9% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




