Submitted:
15 February 2026
Posted:
16 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Patients Selection and Surgical Indications
2.3. Preoperative Assessment
- Clinical Evaluation: Detailed medical history and physical examination, including assessment of the frequency of infections, severity of obstructive sleep apnea, and hearing impairment.
- Flexible Fiberoptic Nasopharyngoscopy: This was used to assess the degree of adenoid hypertrophy, graded on a scale of 1 to 4 (grade 1 being minimal and grade 4 representing complete obstruction of the nasopharynx).
- Audiometric and Tympanometric Assessments: Audiometry was performed to evaluate hearing loss, with behavioral audiometry used for children under 5 years of age. Tympanometry was used to assess middle ear function, particularly in cases of recurrent otitis media [8].
- Preoperative Blood Work: Routine preoperative tests were conducted to assess the child’s general health and to rule out any contraindications for surgery.
2.4. Surgical Procedures
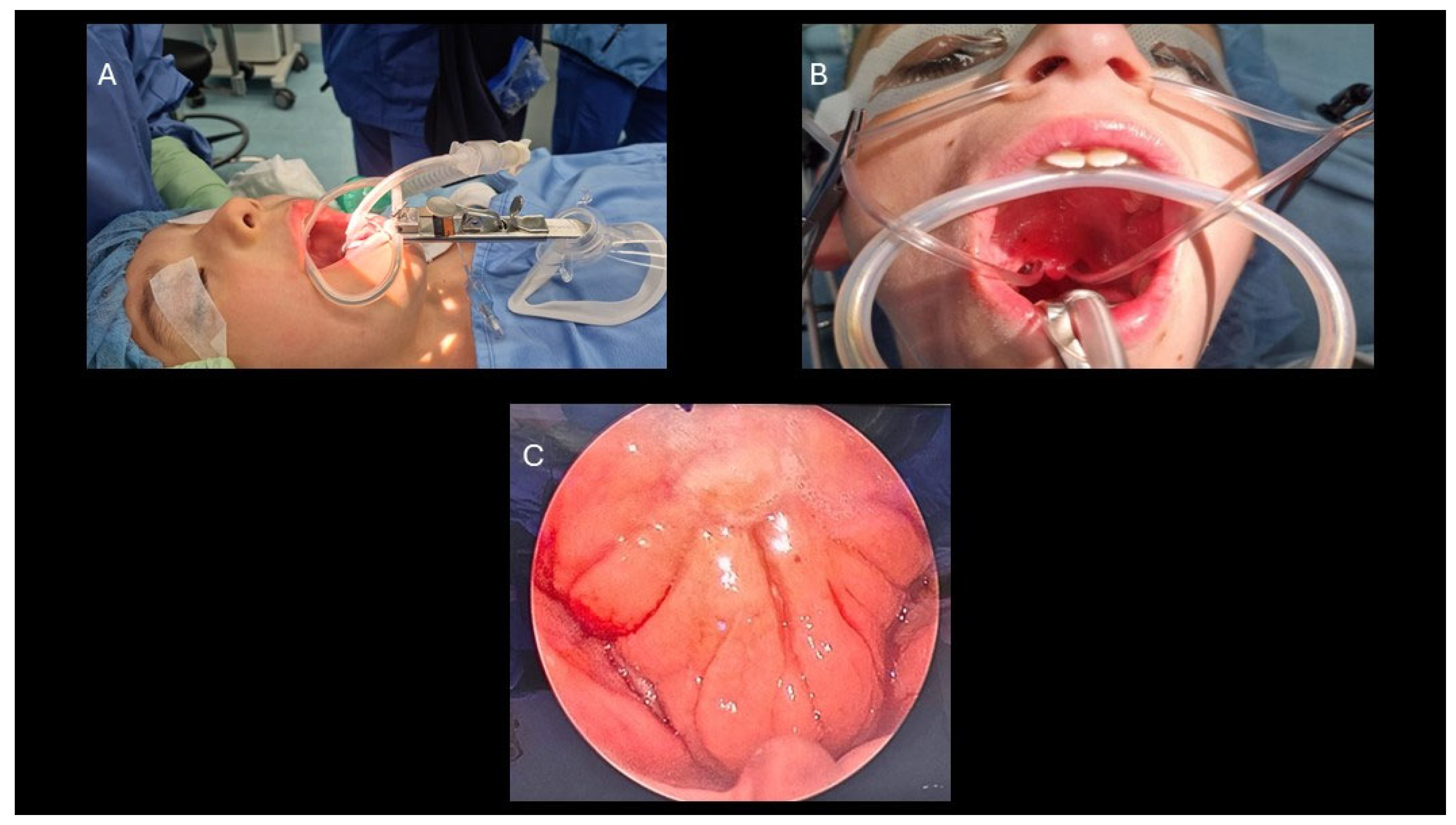
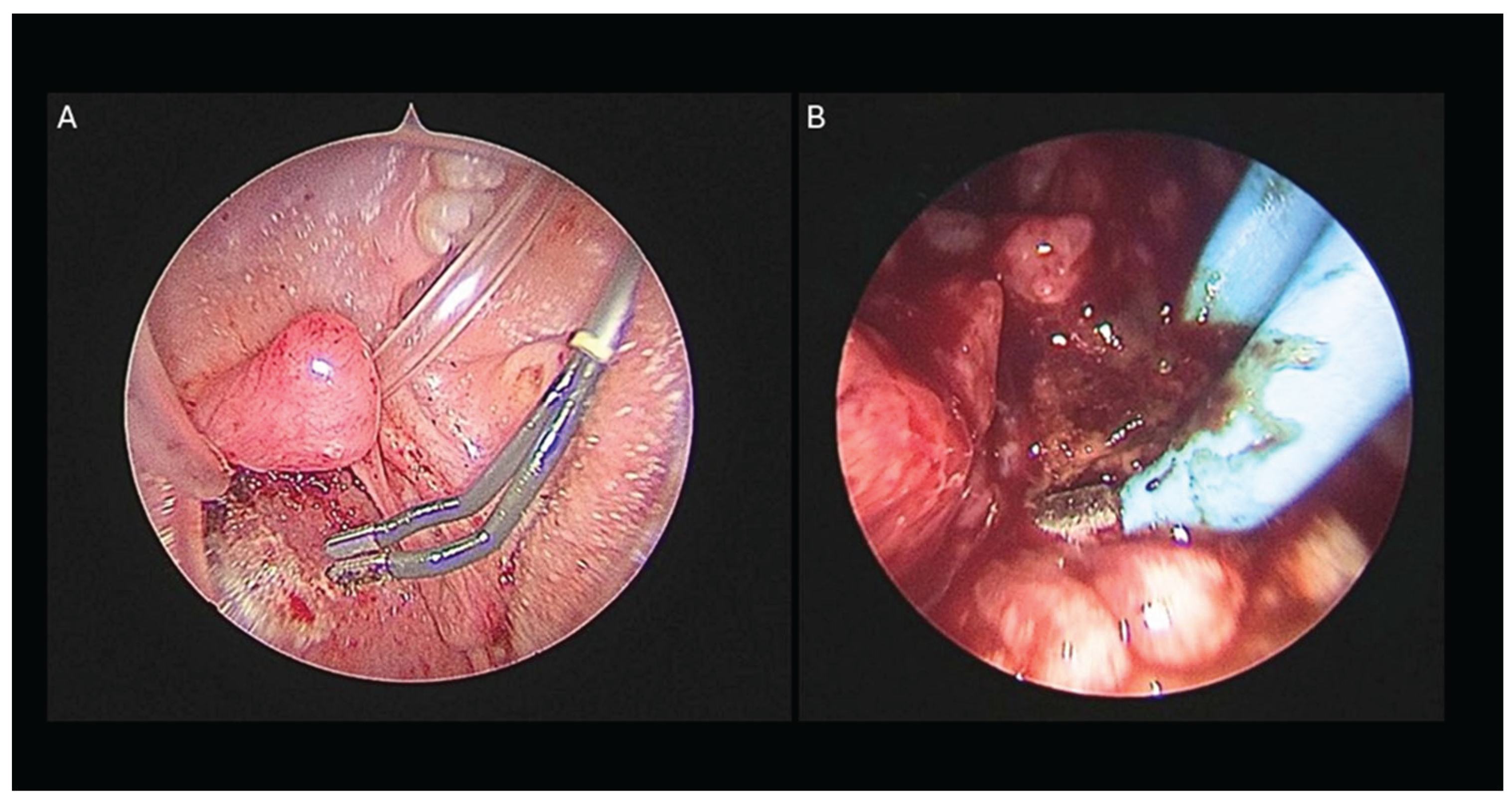
- Adenoidectomy: Adequate retraction of the soft palate was considered essential to ensure full visualization and access to the adenoids. This was achieved using two Nelaton nasal catheters, one placed in each nasal cavity, retrieved through the oropharynx and secured externally with a Klemmer clamp (Figure 1B). Before adenoid removal, a preliminary endoscopic evaluation of the nasopharynx was performed with a 45° 4-mm endoscope introduced through the oral cavity (Figure 1C). Adenoidectomy was carried out using a Negus curette, which allowed gentle curettage of the adenoid tissue from the nasopharyngeal wall . During curettage, minor bleeding from the surgical site was controlled by gentle packing of the nasopharynx with gauze to achieve hemostasis. If bleeding persisted despite manual compression, an endoscopic approach was adopted to allow more precise visualization and control. A 45° 4-mm nasal endoscope was introduced through the mouth to inspect the nasopharynx and identify bleeding vessels, which were then coagulated using diathermy (Figure 2A–B) [10].
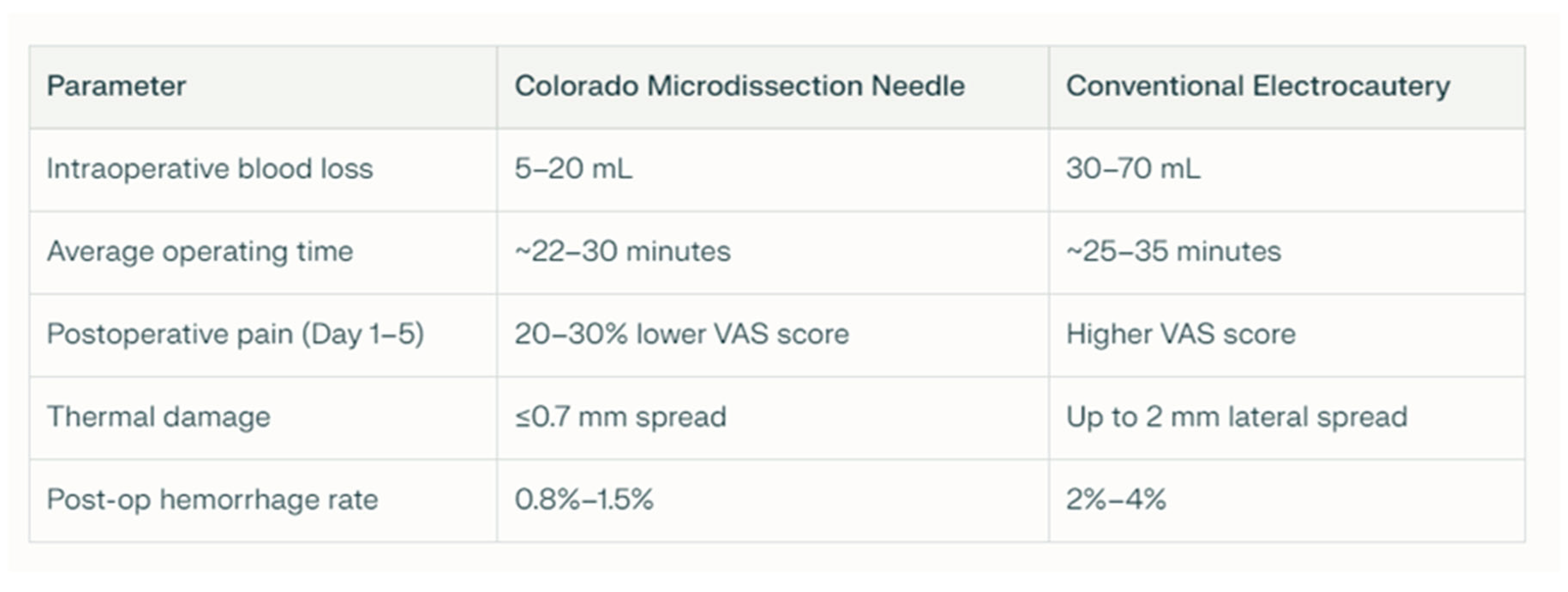
- Tonsillectomy: Tonsillectomy was performed using several techniques, including cold steel dissection, monopolar or bipolar electrocautery, laser dissection, and radiofrequency-based methods. The choice of technique depended on the surgeon’s experience, patient characteristics, and the available equipment. In our center, monopolar electrocautery dissection using the Colorado microdissection needle was the preferred technique. This method uses high-frequency electrical current to cut and coagulate tissue through a fine tungsten-coated tip (5 µm), allowing precise dissection and controlled thermal spread [9]. The tonsil was dissected by carefully separating it from the surrounding pharyngeal tissues, including the muscular layer, blood vessels, and mucosa, with particular attention to preserving the palatopharyngeal and levator veli palatini muscles. Hemostasis was achieved with gauze compression and electrocautery of small bleeding vessels. In most cases, sutures were not required in the tonsillar bed, which was left to heal by secondary intention. The technique was designed to minimize thermal injury, preserve the tonsillar pillars, and deliberately leave a small cuff of tissue at the inferior pole, which was then coagulated using bipolar forceps to reduce the risk of bleeding near the tongue base [11].
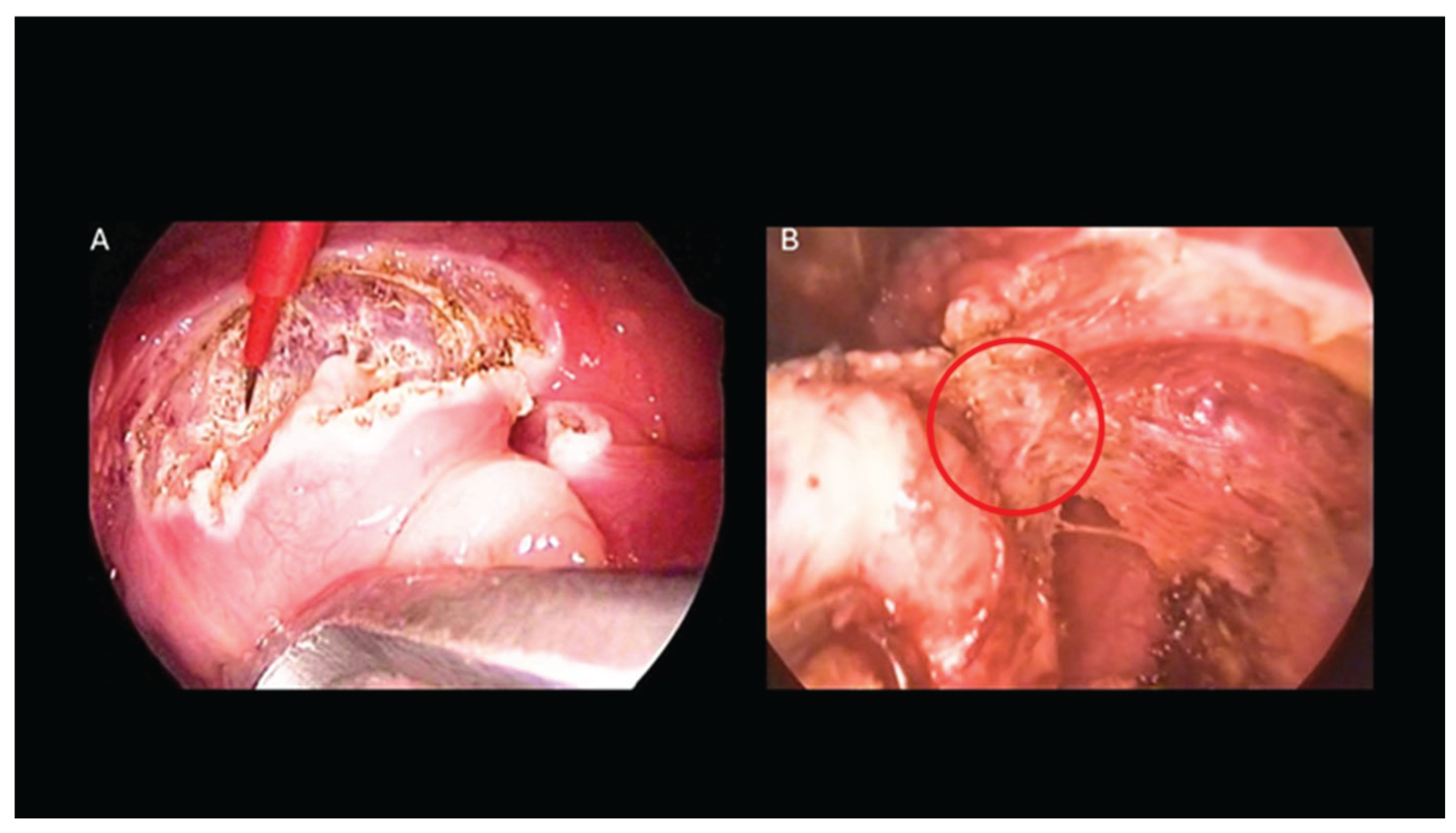
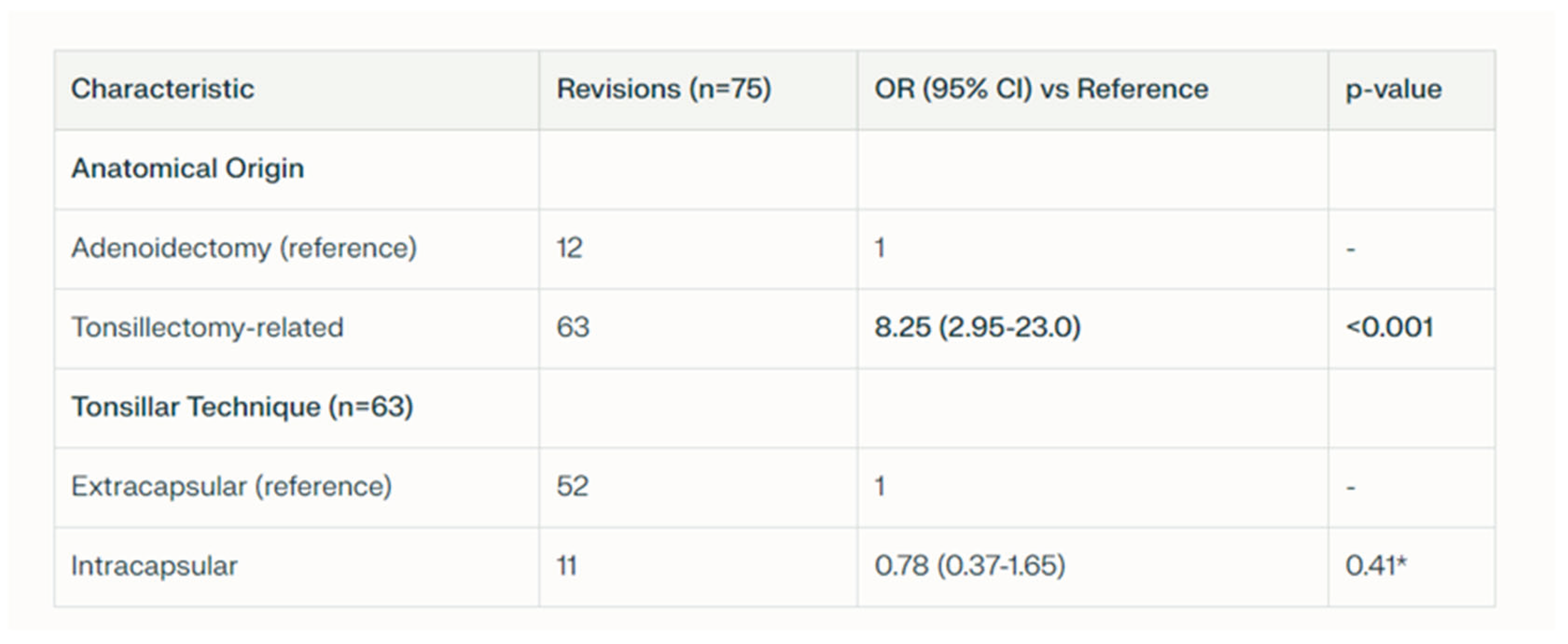
- Extracapsular vs. Intracapsular Techniques: Tonsillectomy was performed using either an extracapsular or an intracapsular approach, chosen according to the clinical indication and patient profile. In the extracapsular technique, the tonsil was completely removed along with its fibrous capsule (Figure 3A–B). In the intracapsular technique, a small portion of tonsillar tissue was intentionally left in situ to facilitate healing and reduce the risk of postoperative hemorrhage. Intracapsular tonsillectomy is associated with lower postoperative bleeding rates, faster recovery, and reduced pain, although it carries a risk of tonsillar regrowth. In accordance with international guidelines, extracapsular dissection was typically preferred for patients with chronic or recurrent tonsillitis refractory to medical therapy, whereas the intracapsular approach was mainly used in children with OSA, for whom complete tonsillar removal is not mandatory, and in patients at increased risk of bleeding or in need of more rapid recovery (e.g., children with Down syndrome) [11].
- Endoscopic tympanic paracentesis and transtympanic drainage placement are performed in conjunction with adenotonsillar surgery when indicated by audiometric findings. The use of the endoscopic approach allows for enhanced visualization of the tympanic membrane, facilitating the detection of any abnormalities and optimizing the procedure. This technique is aimed at improving middle ear ventilation, thereby addressing underlying dysfunctions and contributing to better postoperative outcomes [8].
- Postoperative Care: All patients were monitored just after surgery in the post-anesthesia care unit (PACU) and after a period of observation they go in the Pediatric unit and discharged according to the type of surgery:
- Adenoidectomy: Patients were usually discharged on the same day. Postoperative home care included topical antibiotic nasal drops for 7 days and 7 days of home rest.
- Tonsillectomy/Adenotonsillectomy: Patients were admitted for at least one night of observation. Postoperative management included a beta-lactam antibiotic—most commonly amoxicillin, administered twice daily for 7 days—home rest, and adherence to a soft, cool diet for 15 days to promote healing and reduce discomfort [12].
2.5. Complication Monitoring
2.6. Emergency Support
2.7. Statistical Analysis
3. Results
3.1. Surgical Volume and Demographics
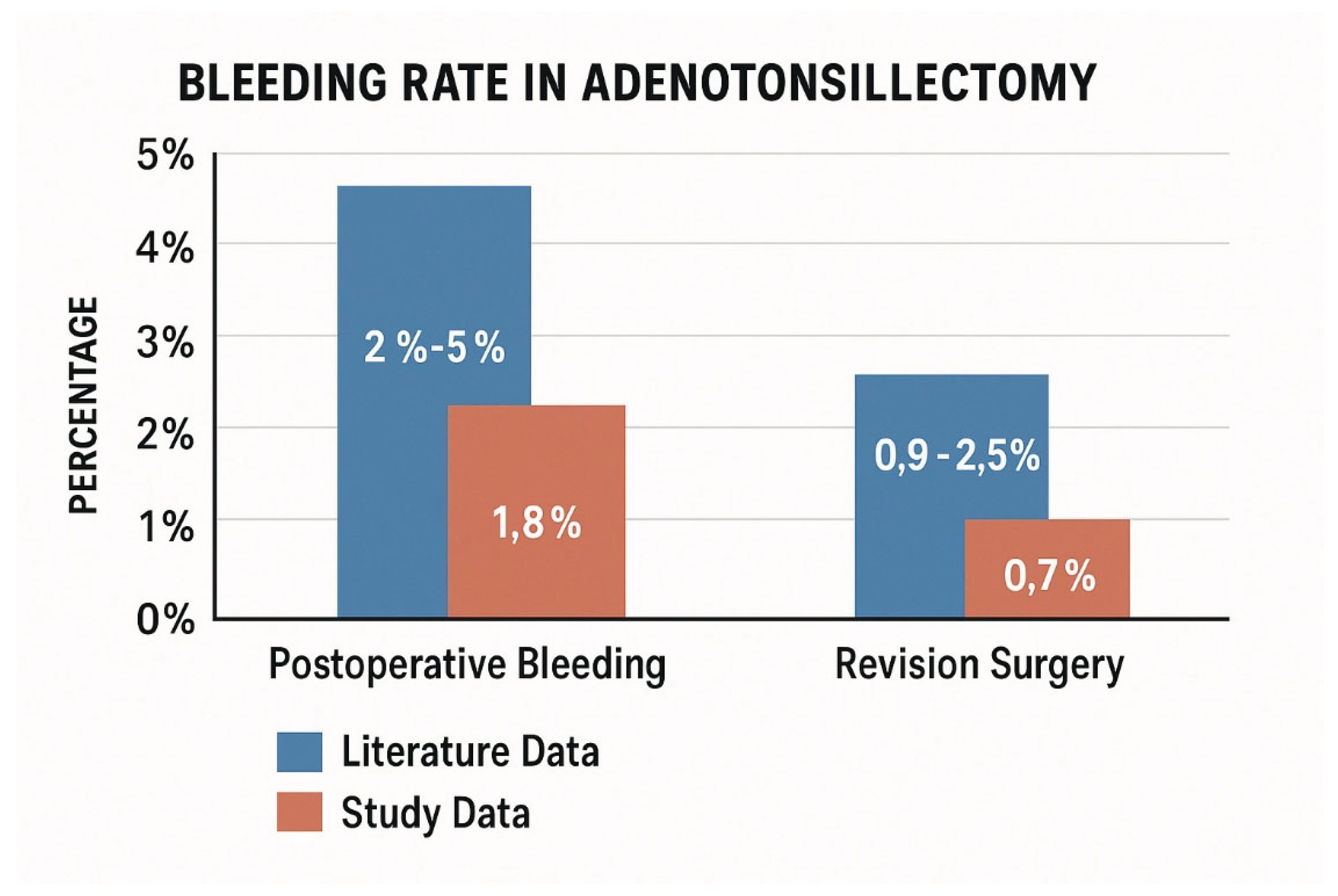
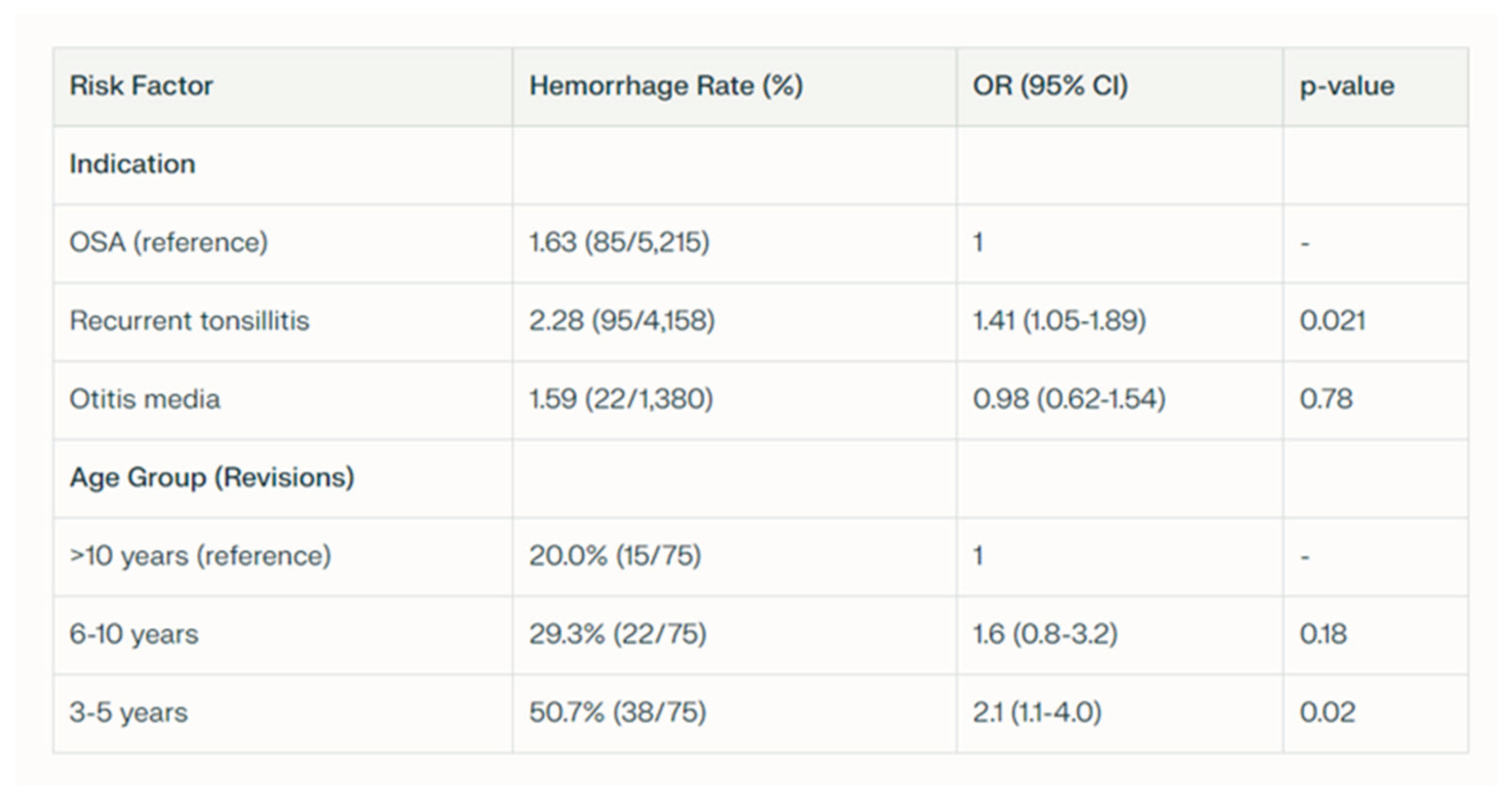
3.2. Postoperative Hemorrhage Rates
3.3. Complication Comparison with Literature
4. Discussion
4.1. Postoperative Hemorrhage and Surgical Revision
4.2. Pain Management and Recovery
4.3. Multidisciplinary and Psychological Support
- 94% reported "significantly reduced parental anxiety"
- 89% noted "improved child cooperation" in the operating room
4.4. The Importance of Inter-Hospital Collaboration in Otolaryngology within the Modena Province
4.5. Limitations and Future Directions
5. Conclusions
5.1. List of Abbreviations
Author Contributions
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bohr C, Shermetaro C. Tonsillectomy and Adenoidectomy. [Updated 2023 Jun 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK536942/.
- Della Vecchia L, Passali FM, Coden E. Complications of adenotonsillectomy in pediatric age. Acta Biomed. 2020;91(1-S):48-53. doi:10.23750/abm.v91i1-S.9256.
- Available online: https://pne.agenas.it/ospedaliera/indicatori?noso=orl (accessed on 18/06/2025).
- Mahant S, Keren R, Localio R, et al. Complications in pediatric tonsillectomy and adenoidectomy. JAMA Otolaryngol Head Neck Surg. 2016;142(9):893-899. doi:10.1001/jamaoto.2016.1444.
- Jones P, Walker D, Harris G, et al. Management of Postoperative Hemorrhage After Adenotonsillectomy in Children. Int J Pediatr Otorhinolaryngol. 2021;143:110689. https://doi.org/10.1016/j.ijporl.2021.110689.
- Taylor R, Chen A. Postoperative Hemorrhage Rates in Pediatric Tonsillectomy: A Meta-Analysis. Laryngoscope. 2015;125(2):543-550. https://doi.org/10.1002/lary.24751.
- Randall DA. Current Indications for Tonsillectomy and Adenoidectomy. J Am Board Fam Med. 2020 Nov-Dec;33(6):1025-1030. doi: 10.3122/jabfm.2020.06.200038. PMID: 33219085.
- Marchioni D, Mattioli F, Alicandri-Ciufelli M, et al. Endoscopic Evaluation of Middle Ear Ventilation Route Blockage. Am J Otolaryngol. 2010; 31(6):453-466.
- Friedman M, Salapatas AM, Bonzelaar LB. Microdissection needle tonsillectomy: a review of surgical outcomes. Laryngoscope. 2009;119(3):620-627. doi:10.1002/lary.20107.
- Walker J, Thompson P, Brown L, et al. Minimizing Risk of Hemorrhage in Pediatric Tonsillectomy: A Review of Surgical Techniques. Laryngoscope Investig Otolaryngol. 2020;5(2):189-193. https://doi.org/10.1002/lio2.388.
- Peterson J, Stewart C. The Colorado Microdissection Needle in Pediatric Adenotonsillectomy: Outcomes and Benefits. Int J Pediatr Otorhinolaryngol. 2017;95:63-67. https://doi.org/10.1016/j.ijporl.2017.02.021.
- Mitchell RB. Adenotonsillectomy and adenoidectomy in children: the impact of surgical technique on postoperative outcomes. Laryngoscope. 2017;127(9):2185-2190. doi:10.1002/lary.26569.
- Cheng, S., Englesakis, M., Park, S. et al. Optimizing pain management in pediatric tonsillectomy: the role of NSAIDs. J Anesth 2025. https://doi.org/10.1007/s00540-025-03552-4.
- Smith J, Brown P, Lee A, et al. Postoperative Hemorrhage in Pediatric Adenotonsillectomy: A Review. J Surg Res. 2019;56(2):128-134. https://doi.org/10.1016/j.jss.2018.12.005.
- IBM Corp. IBM SPSS Statistics for Windows, Version 25.0. Armonk, NY: IBM Corp; 2017.
- Demir UL, İnan HC. The Impact of Comorbid Diseases on Postoperative Complications in Children after Adenotonsillectomy: Is It a Myth? Turk Arch Otorhinolaryngol. 2020 Sep;58(3):141-148. doi: 10.5152/tao.2020.5502.
- Perkins JN, Liang C, Gao D, Shultz L, Friedman NR. Risk of post-tonsillectomy hemorrhage by clinical diagnosis. Laryngoscope. 2012 Oct;122(10):2311-5. doi: 10.1002/lary.23421.
- Hoddeson EK, Gourin CG. Adult tonsillectomy: current indications and outcomes. Otolaryngol Head Neck Surg. 2009 Jan;140(1):19-22. doi: 10.1016/j.otohns.2008.09.023.
- Achar P, Sharma RK, De S, Donne AJ. Does primary indication for tonsillectomy influence post-tonsillectomy haemorrhage rates in children? Int J Pediatr Otorhinolaryngol. 2015 Feb;79(2):246-50. doi: 10.1016/j.ijporl.2014.12.022.
- Mitchell RB, Pereira KD, Friedman NR; Clinical Practice Guideline: Tonsillectomy in Children (Update). Otolaryngol Head Neck Surg. 2019;160(1 Suppl):S1-S42. doi:10.1177/0194599818801757.
- Bhattacharyya N. Adenotonsillectomy complications: a meta-analysis. Otolaryngol Head Neck Surg. 2015;152(4):623-632. doi:10.1177/0194599814567110.
- Mitchell RB. Adenotonsillectomy and adenoidectomy in children: the impact of surgical technique on postoperative outcomes. Laryngoscope. 2017;127(9):2185-2190. doi:10.1002/lary.26569.
- Acevedo JL, Shah RK, Brietzke SE. Systematic review of complications of tonsillotomy versus tonsillectomy. Otolaryngol Head Neck Surg. 2012;146(6):841-848. doi:10.1177/0194599812439017.
- Ramadan HK, Miller RH. Tonsillectomy and adenoidectomy: a review of surgical techniques and complications. Int J Pediatr Otorhinolaryngol. 1997;40(3):237-251. doi:10.1016/s0165-5876(97)00028-2.
- Rideout B, Dobson D, Glover P, Lemire J. Tonsillectomy using the Colorado microdissection needle. South Med J. 2004;97(3):289–292.pubmed.ncbi.nlm.nih+1.
- Al-Qahtani AS. Post-tonsillectomy hemorrhage. Monopolar microdissection needle vs cold dissection. Saudi Med J. 2012;33(1):50–54.applications.emro.who+1.
- Perkins JN, Duffy VK, Schubert W, et al. Microdissection needle tonsillectomy and postoperative pain in children. Arch Otolaryngol Head Neck Surg. 2003;129(11):1285–1289.jamanetwork.
- Chandra RV, Prasad K, Rani VV, et al. Comparing the outcomes of incisions made by Colorado microdissection needle, electrosurgery tip, and surgical blade. J Indian Soc Periodontol. 2016;20(6):36–41.
 |
 |
 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




