Submitted:
11 February 2026
Posted:
12 February 2026
You are already at the latest version
Abstract
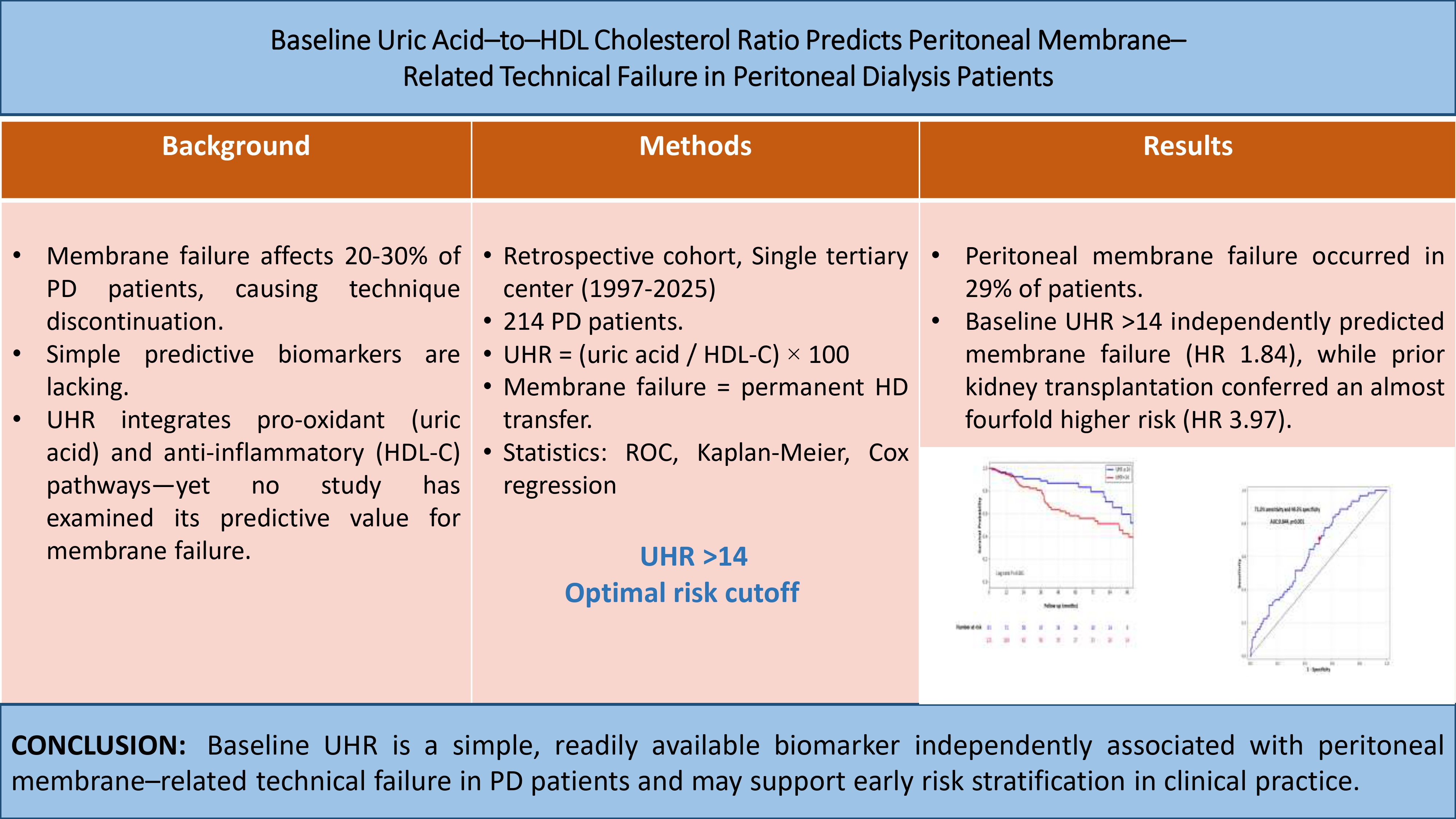
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Data Collection and Laboratory Measurements
2.3. Peritoneal Dialysis Characteristics
2.4. Outcome Definition
2.5. Statistical Analysis
3. Results
3.1. Baseline Characteristics of the Study Population
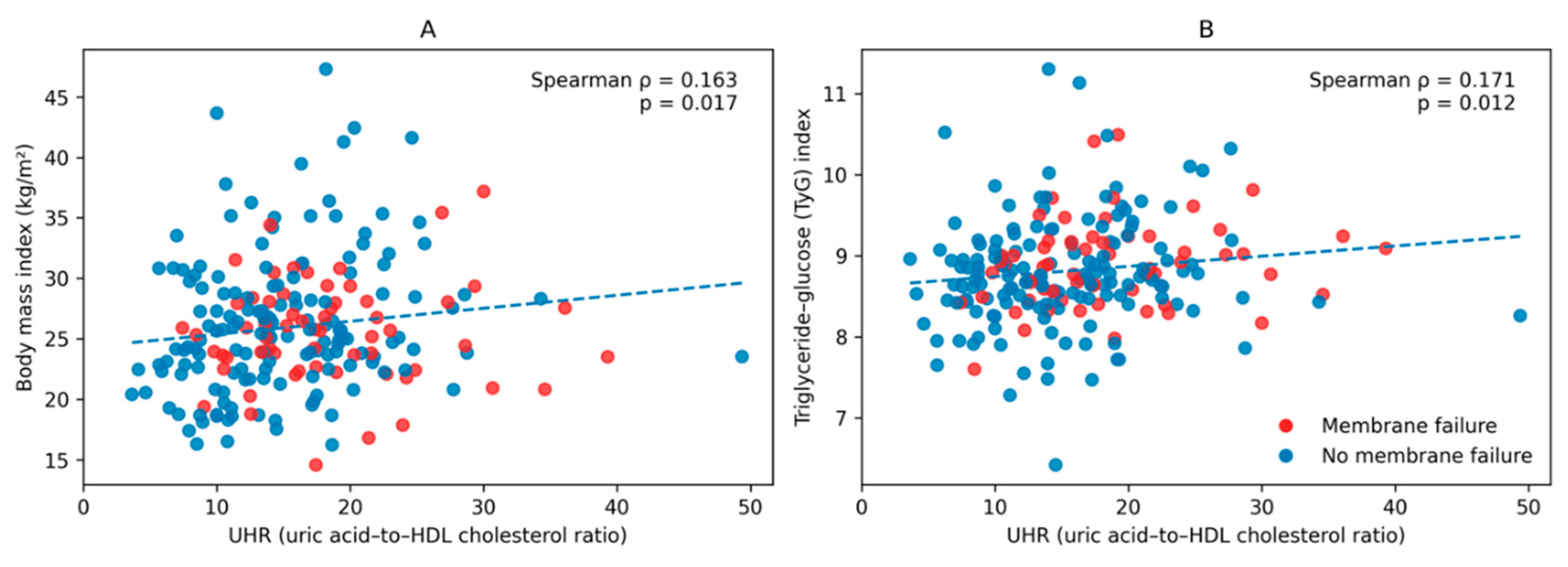
3.2. Correlations Between UHR and Clinical Parameters
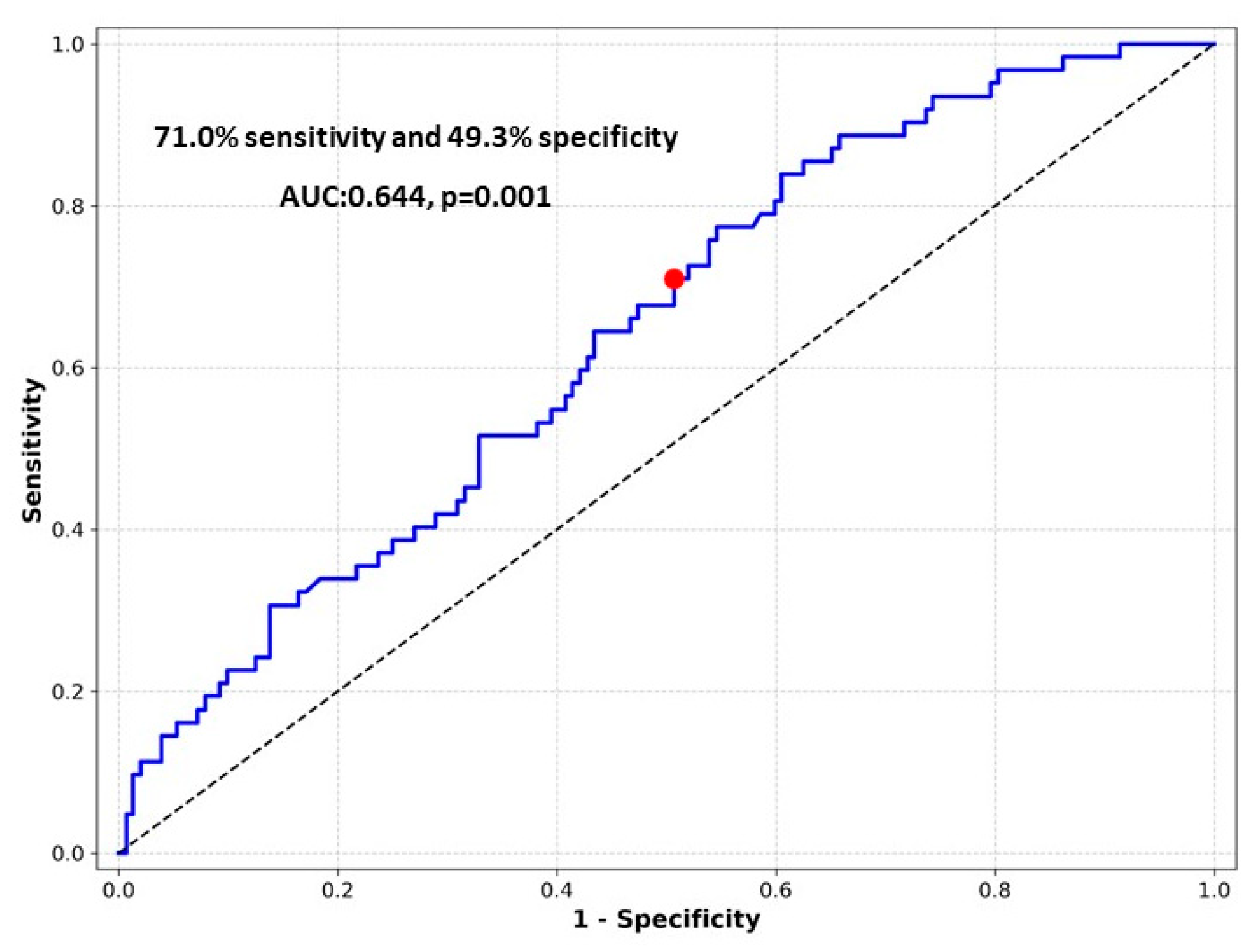
3.3. Diagnostic Performance of UHR for Predicting Membrane Failure
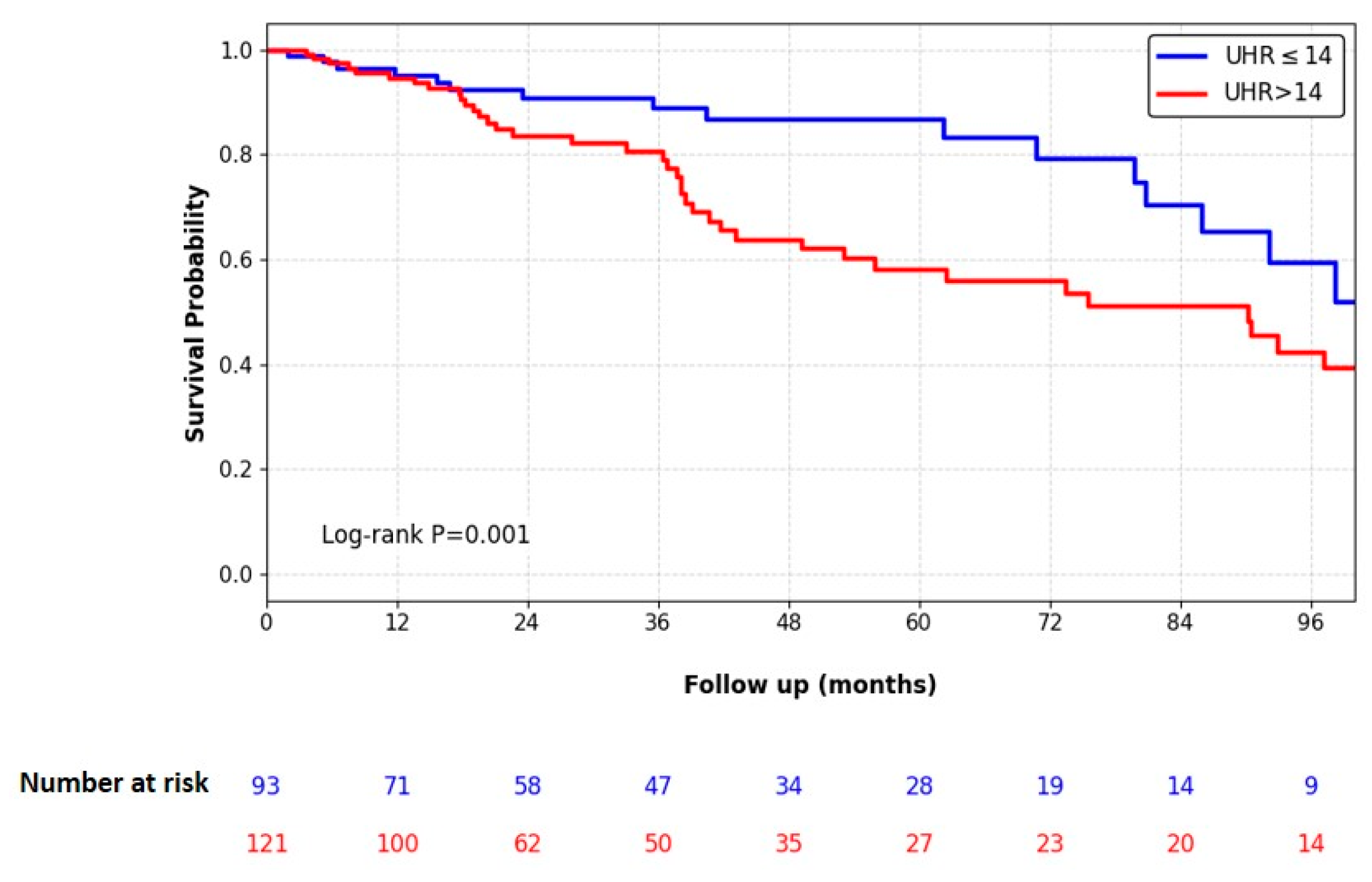
3.4. Survival Analysis and Independent Predictors of Membrane Failure
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bello, A. K.; Okpechi, I. G.; Osman, M. A.; Cho, Y.; Cullis, B.; Htay, H.; Jha, V.; Makusidi, M. A.; McCulloch, M.; Shah, N.; et al. Epidemiology of peritoneal dialysis outcomes. Nat Rev Nephrol. 2022, 18(12), 779–793. [Google Scholar] [CrossRef] [PubMed]
- Bonenkamp, A. A.; van Eck van der Sluijs, A.; Dekker, F. W.; Struijk, D. G.; de Fijter, C. W.; Vermeeren, Y. M.; van Ittersum, F. J.; Verhaar, M. C.; van Jaarsveld, B. C.; Abrahams, A. C. Technique failure in peritoneal dialysis: Modifiable causes and patient-specific risk factors. Perit Dial Int. 2023, 43(1), 73–83. [Google Scholar] [CrossRef]
- Dong, X.; Wu, H.; Ye, H.; Yi, C.; Diao, X.; Liu, R.; Mao, H.; Huang, F.; Yu, X.; Yang, X. Incidence and Risk Factors Associated with Technique Failure in the First Year of Peritoneal Dialysis: A Single Center Retrospective Cohort Study in Southern China. BMC Nephrol. 2022, 23(1), 207. [Google Scholar] [CrossRef]
- Ito, Y.; Sun, T.; Tawada, M.; Kinashi, H.; Yamaguchi, M.; Katsuno, T.; Kim, H.; Mizuno, M.; Ishimoto, T. Pathophysiological Mechanisms of Peritoneal Fibrosis and Peritoneal Membrane Dysfunction in Peritoneal Dialysis. Int J Mol Sci. 2024, 25(16), 8607. [Google Scholar] [CrossRef]
- Morelle, J.; Stachowska-Pietka, J.; Öberg, C.; Gadola, L.; La Milia, V.; Yu, Z.; Lambie, M.; Mehrotra, R.; de Arteaga, J.; Davies, S. ISPD recommendations for the evaluation of peritoneal membrane dysfunction in adults: Classification, measurement, interpretation and rationale for intervention. Perit Dial Int. 2021, 41(4), 352–372. [Google Scholar] [CrossRef]
- Baroni, G; Schuinski, A; de Moraes, TP; Meyer, F; Pecoits-Filho, R. Inflammation and the peritoneal membrane: causes and impact on structure and function during peritoneal dialysis. Mediators Inflamm. 2012, 2012, 912595. [Google Scholar] [CrossRef]
- Krediet, RT. Aging of the Peritoneal Dialysis Membrane. Front Physiol. 2022, 13, 885802. [Google Scholar] [CrossRef]
- Piarulli, P.; Vizzardi, V.; Alberici, F.; Riva, H.; Aramini, M.; Regusci, L.; Cippà, P.; Bellasi, A. Peritoneal dialysis discontinuation: to the root of the problem. J Nephrol. 2023, 36(7), 1763–1776. [Google Scholar] [CrossRef] [PubMed]
- Virzì, G. M.; Mattiotti, M.; Milan Manani, S.; Gnappi, M.; Tantillo, I.; Corradi, V.; de Cal, M.; Giuliani, A.; Carta, M.; Giavarina, D.; et al. Peritoneal NGAL: a reliable biomarker for PD-peritonitis monitoring. J Nephrol. 2023, 36, 2139–2141. [Google Scholar] [CrossRef] [PubMed]
- Zoccali, C; Mallamaci, F. Uric acid in chronic kidney disease: the quest for causality continues. Nephrol Dial Transplant. 2018, 33(2), 193–195. [Google Scholar] [CrossRef]
- Luo, Q; Xia, X; Li, B; Lin, Z; Yu, X; Huang, F. Serum uric acid and cardiovascular mortality in chronic kidney disease: a meta-analysis. BMC Nephrol. 2019, 20(1), 18. [Google Scholar] [CrossRef]
- Xia, X; He, F; Wu, X; Peng, F; Huang, F; Yu, X. Relationship between serum uric acid and all-cause and cardiovascular mortality in patients treated with peritoneal dialysis. Am J Kidney Dis. 2014, 64(2), 257–264. [Google Scholar] [CrossRef] [PubMed]
- Rysz, J; Gluba-Brzózka, A; Rysz-Górzyńska, M; Franczyk, B. The Role and Function of HDL in Patients with Chronic Kidney Disease and the Risk of Cardiovascular Disease. Int J Mol Sci. 2020, 21(2), 601. [Google Scholar] [CrossRef] [PubMed]
- Yazdi, F; Baghaei, MH; Baniasad, A; Naghibzadeh-Tahami, A; Najafipour, H; Gozashti, MH. Investigating the relationship between serum uric acid to high-density lipoprotein ratio and metabolic syndrome. Endocrinol Diabetes Metab. 2022, 5(1), e00311. [Google Scholar] [CrossRef]
- Xuan, Y.; Zhang, W.; Wang, Y.; Wang, B.; Xia, F.; Zhang, K.; Li, Q.; Wang, N.; Lu, Y. Association Between Uric Acid to HDL Cholesterol Ratio and Diabetic Complications in Men and Postmenopausal Women. Diabetes Metab Syndr Obes. 2023, 16, 167–177. [Google Scholar] [CrossRef]
- Liu, R.; Peng, Y.; Wu, H.; Diao, X.; Ye, H.; Huang, X.; Yi, C.; Mao, H.; Huang, F.; Yu, X.; et al. Uric acid to high-density lipoprotein cholesterol ratio predicts cardiovascular mortality in patients on peritoneal dialysis. Nutr Metab Cardiovasc Dis. 2021, 31(2), 561–569. [Google Scholar] [CrossRef]
- Kocak, MZ; Aktas, G; Erkus, E; Sincer, I; Atak, B; Duman, T. Serum uric acid to HDL-cholesterol ratio is a strong predictor of metabolic syndrome in type 2 diabetes mellitus. Rev Assoc Med Bras (1992) 2019, 65(1), 9–15. [Google Scholar] [CrossRef]
- Simental-Mendía, LE; Rodríguez-Morán, M; Guerrero-Romero, F. The product of fasting glucose and triglycerides as surrogate for identifying insulin resistance in apparently healthy subjects. Metab Syndr Relat Disord. 2008, 6(4), 299–304. [Google Scholar] [CrossRef] [PubMed]
- Wen, S; Arakawa, H; Tamai, I. Uric acid in health and disease: From physiological functions to pathogenic mechanisms. Pharmacol Ther. 2024, 256, 108615. [Google Scholar] [CrossRef]
- Moradi, H; Vaziri, ND; Kashyap, ML; Said, HM; Kalantar-Zadeh, K. Role of HDL dysfunction in end-stage renal disease: a double-edged sword. J Ren Nutr. 2013, 23(3), 203–206. [Google Scholar] [CrossRef]
- Johnson, D. W.; Hawley, C. M.; McDonald, S. P.; Brown, F. G.; Rosman, J. B.; Wiggins, K. J.; Bannister, K. M.; Badve, S. V. Superior survival of high transporters treated with automated versus continuous ambulatory peritoneal dialysis. Nephrol Dial Transplant. 2010, 25(6), 1973–1979. [Google Scholar] [CrossRef] [PubMed]
- Perl, J; Dong, J; Rose, C; Jassal, SV; Gill, JS. Is dialysis modality a factor in the survival of patients initiating dialysis after kidney transplant failure? Perit Dial Int. 2013, 33(6), 618–628. [Google Scholar] [CrossRef] [PubMed]
- Badve, S. V.; Hawley, C. M.; McDonald, S. P.; Mudge, D. W.; Rosman, J. B.; Brown, F. G.; Johnson, D. W.; ANZDATA Registry PD Working Committee. Effect of previously failed kidney transplantation on peritoneal dialysis outcomes in the Australian and New Zealand patient populations. Nephrol Dial Transplant. 2006, 21(3), 776–783. [Google Scholar] [CrossRef]
- Heldal, T. F.; Åsberg, A.; Ueland, T.; Reisæter, A. V.; Pischke, S. E.; Mollnes, T. E.; Aukrust, P.; Reinholt, F.; Hartmann, A.; Heldal, K.; et al. Systemic inflammation early after kidney transplantation is associated with long-term graft loss: a cohort study. Front Immunol. 2023, 14, 1253991. [Google Scholar] [CrossRef]
- Shapiro, J; Schiff, J; Perl, J. Peritoneal dialysis and kidney transplantation: Your questions answered. Perit Dial Int. 2025, 45(3), 142–152. [Google Scholar] [CrossRef] [PubMed]
| Total n=214 |
Non- failure n=152 (71%) |
Failure n=62 (29%) |
p value | |
|---|---|---|---|---|
| Sex (female) | 101 (47.2) | 75 (49.3) | 26 (41.9) | 0.325 |
| Age (years) | 48.2±17.3 | 49.4±17.2 | 45.2±17.5 | 0.112 |
| BMI | 25.3 (22.5-28.7) | 25.2 (22.5-29.3) | 25.5 (22.7-28.0) | 0.288 |
| DM | 58 (27.1) | 46 (30.3) | 12 (19.4) | 0.103 |
| HT | 182 (85.0) | 131 (86.2) | 51 (82.3) | 0.465 |
| CAD | 39 (18.2) | 28 (18.4) | 11 (17.7) | 0.907 |
| Smoking | 34 (15.9) | 25 (16.4) | 9 (14.5) | 0.726 |
| KT history before PD | 12 (5.6) | 6 (3.9) | 6 (9.7) | 0.098 |
|
PD choice Mandatory |
20 (9.3) |
15 (9.9) |
5 (8.1) |
0.681 |
| Previous hernia history | 35 (16.4) | 23 (15.1) | 12 (19.4) | 0.449 |
|
Laboratoryvalues Hemoglobin (g/dl) Albumin (g/dl) CRP (mg/dl) PTH (pg/ml) LDL-Cholesterol |
11.0±1.8 3.8 (3.4-4.1) 3.0 (3.0-9.6) 276 (173-529) 106 (85-135) |
11.1±1.7 3.9 (3.5-4.1) 4.1 (3.0-10.2) 302 (174-553) 107 (83-135) |
10.6±2.0 3.7 (3.3-4.1) 3.0 (3.0-7.0) 247 (169-449) 105 (89-134) |
0.176 0.108 0.349 0.372 0.911 |
| UHR | 14.8 (11.1-19.3) | 14.0 (10.3-18.8) | 17.3 (13.7-21.6) | 0.001 |
| TyG Index | 8.8 (8.5-9.2) | 8.7 (8.4-9.1) | 8.9 (8.5-9.2) | 0.192 |
| Baseline RRF (yes) | 199 (93.9) | 143 (94.1) | 56 (90.3) | 0.329 |
| Baseline weekly Kt/V | 2.25±0.76 | 2.31±0.76 | 2.12±0.76 | 0.081 |
|
PET category Low - Low average High average - High |
112 (52.3) 102 (47.7) |
86 (56.6) 66 (43.4) |
26 (41.9) 36 (58.1) |
0.052 |
|
PD modality CAPD APD |
151 (70.6) 63 (29.4) |
99 (65.1) 53 (34.9) |
52 (83.9) 10 (16.1) |
0.006 |
| Assisted PD | 22 (10.3) | 15 (9.9) | 7 (11.3) | 0.756 |
| Any peritonitis episodes at follow-up, n (%) | 74 (34.6) | 52 (34.2) | 22 (35.5) | 0.859 |
| PD duration (months) | 31.0 (15.0-61.5) | 27.7 (13.8-54.1) | 38.3 (17.8-80.8) | 0.036 |
| Univariate, HR (%95 CI) | p value | Multivariate, HR (%95 CI) | p value | |
|---|---|---|---|---|
| Age | 1.002 (0.987–1.018) | 0.771 | ||
| Male sex | 1.748 (1.045–2.924) | 0.033 | 1.562 (0.918-2.658) | 0.100 |
| BMI | 0.994 (0.944-1.046) | 0.815 | ||
| DM | 1.371 (0.714-2.631) | 0.343 | ||
| Transplantation before PD | 3.677 (1.561-8.662) | 0.003 | 3.971 (1.668-9.455) | 0.002 |
| PD mandatory | 0.689 (0.275-1.729) | 0.428 | ||
| RRF (yes) | 1.006 (0.430-2.355) | 0.988 | ||
| PD modality (APD) | 1.258 (0.611–2.590) | 0.533 | ||
| Baseline PET category (High/High-average) | 1.533 (0.912–2.576) | 0.107 | ||
| Any peritonitis episodes | 0.758 (0.443–1.297) | 0.312 | ||
| TGI | 1.369 (0.911-2.056) | 0.131 | ||
| UHR > 14 | 1.971 (1.134–3.424) | 0.016 | 1.836 (1.040-3.241) | 0.036 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




