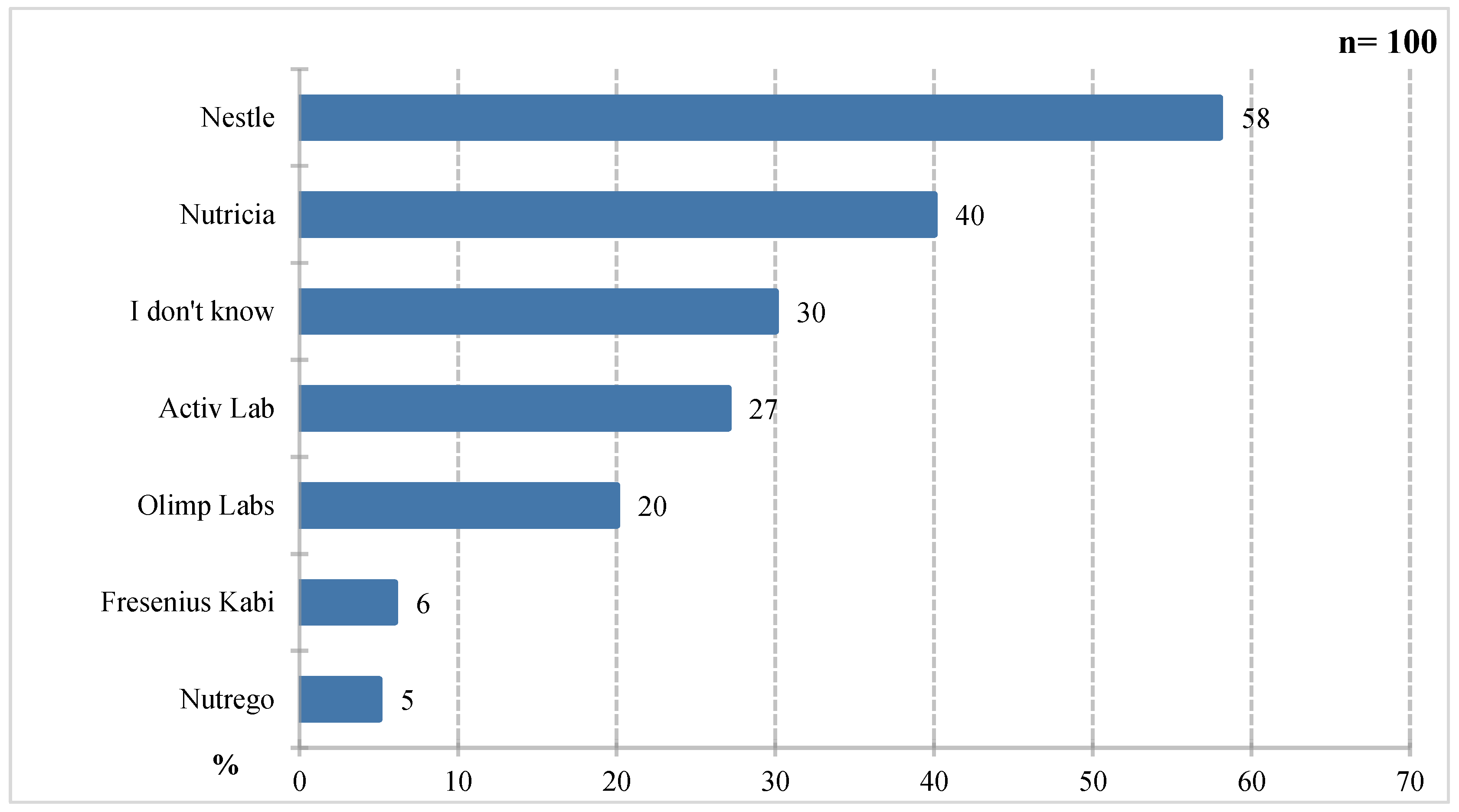1. Introduction
One of the many problems faced by hospitalized patients, especially the elderly, is malnutrition [
1]. Malnutrition, as defined by the WHO, ASPEN, and ESPEN, is an imbalance between the supply and utilization of nutrients. It can involve both deficiency and excess of nutrients, as well as diet-related diseases. Malnutrition is associated with a poorer prognosis, an increased risk of complications, and prolonged hospitalization [
2,
3,
4]. It is a clinical condition resulting from poor nutrition or a disease that causes digestive and malabsorption disorders, or symptoms that negatively affect appetite, resulting in reduced intake of micro and macronutrients [
5,
6]. It is estimated that up to 50% of hospitalized patients may suffer from disease-related malnutrition, and 30% of patients will develop malnutrition during their hospital stay [
7,
8]. According to a review by Salari et al. [2025] malnutrition among older adults worldwide is 18.6%. Malnutrition results in numerous adverse changes in the body, such as changes in body composition (loss of muscle mass and fat tissue) and deterioration of muscle function, including cardiac, renal, and respiratory muscle function [
9]. Gastrointestinal function regresses through impact on the function of the pancreas, intestinal villus, and colon, which can cause diarrhea and further impairment of digestion and absorption [
5]. Malnourished patients have prolonged hospital stays and a higher risk of mortality, poorer response to treatment, impaired wound healing and immune function, and prolonged recovery time after procedures [
10,
11]. Elderly people and those with underlying health conditions (oncology, neurological, and critically ill patients) are particularly at risk [
8,
10]. A key approach to preventing malnutrition is proper assessment of nutritional status, which allows for early detection and mitigation of its progression and negative consequences. Effective tools include scales that include questions about weight loss over a selected period, current body weight, existing diseases, and food consumption.
If malnutrition is detected or is at high risk, appropriate intervention should be initiated. It has been estimated that investing
$1 in nutritional therapy will yield a
$54 return on investment [
12]. Depending on the needs and capabilities, dietary fortification with ONS, enteral nutrition, or parenteral nutrition is used, according to the ESPEN protocol [
13]. If the patient is unable to consume adequate amounts of food, a dietary consultation is recommended to establish an oral diet, possibly supplemented with oral nutritional supplements (ONS). ONS are food for special medical purposes (FSMP), preparations that allow for easy delivery of energy and protein in a small volume. Depending on the disease state, selected preparations may be enriched or omitted with certain essential ingredients. ONS can be classified in various ways. There are hypocaloric (0.5-0.9 kcal/ml), isocaloric (0.9-1.2 kcal/ml), and hypercaloric (1.3-2.4 kcal/ml). Based on their ingredient content, they are classified as high-energy, high-protein and mixed [
14]. Proteins can be in varying degrees of hydrolysis polymeric, oligomeric and monomeric. Many different types allow them to be tailored to specific diseases. Formulations with reduced monosaccharides and saccharose, content, a low glycemic index, and added dietary fiber are intended for diabetics. In liver diseases at risk of encephalopathy, formulas with added branched-chain amino acids (BCAAs), fiber, and medium-chain triglycerides (MCTs) are recommended. For chronic kidney disease, hypercaloric ONS with reduced protein content (approximately 6% of energy) and electrolytes are used [
15]. Immunonutrition is the supply of selected ingredients that modulate the immune response and inflammatory processes [
16]. These preparations contain omega-3 fatty acids, selected amino acids such as glutamine and arginine, nucleotides, and prebiotic fiber. Formulas recommended for patients with difficult-to-heal wounds, ulcers, burns, and pressure sores contain arginine, collagen, and fatty acids, which stimulate repair processes and modulate the immune response [
17,
18]. For patients requiring dialysis, high-energy and high-protein ONS are used. For individuals with cow’s milk protein allergies and vegan, a formula based on plant proteins (soy) is recommended. Single-ingredient products such as protein, fiber, and thickeners are also available [
15].
A lot of scientific data indicates that nutritional support through the use of ONS, along with oral diet fortification, can be crucial as an intervention against malnutrition and disease-related malnutrition [
19,
20,
21,
22,
23,
24]. It is crucial that both healthcare professionals and patients are aware of the potential benefits of using these supplements. Patients often show reluctance to use these supplements due to their non-conventional nature and difficulty persuading them to supplement their diet despite difficulties with swallowing, chewing, or appetite.
The aim of this study was to assess hospitalised patients awareness of foods for special medical purposes (FSMP) and to determine the perception of the dietitian’s role in the hospital treatment process.
3. Results and Discussion
As shown in
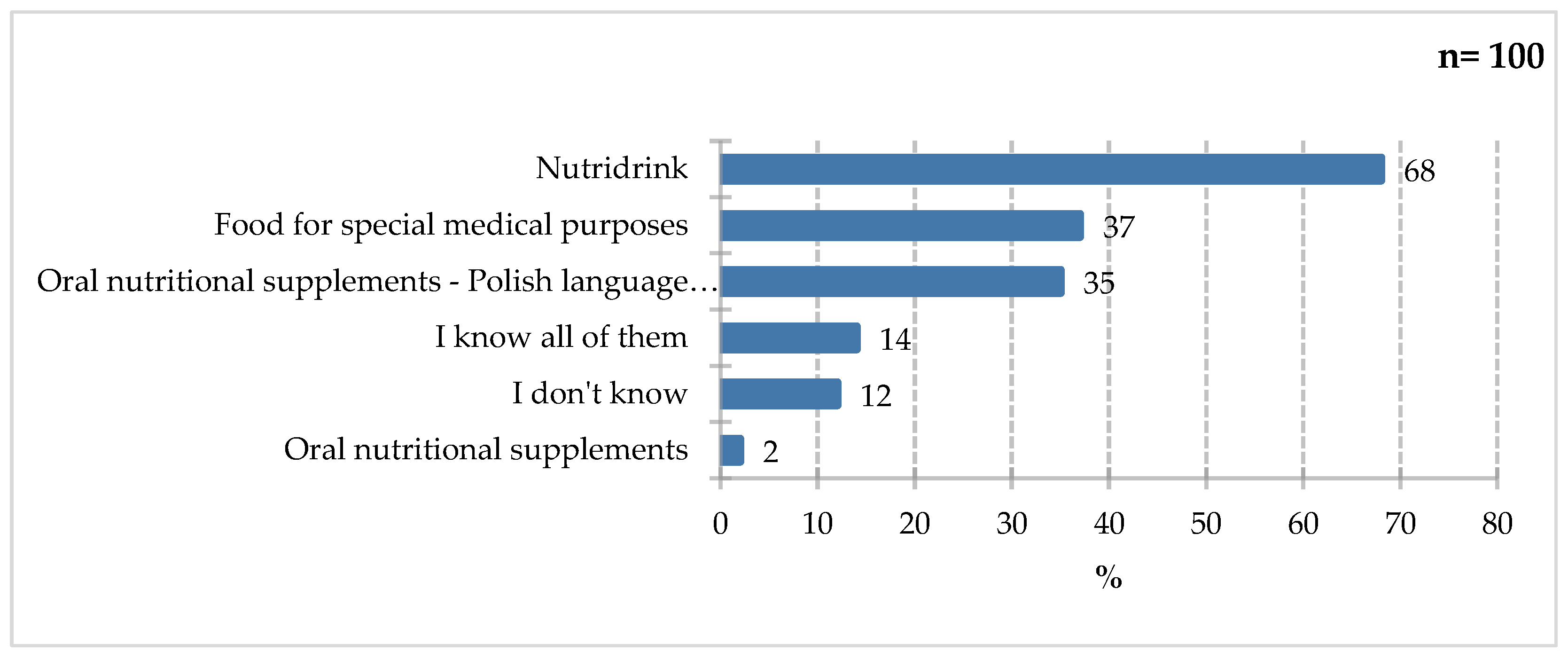
Figure 2 the term “Nutridrink” was most frequently used by survey participants (68%). It is one of the trade names of a product from the leading brand FSMP on the Polish market. It can demonstrates the effectiveness of marketing campaigns on television and social media. Despite respondents’ limited awareness of the product, the generic name ONS is still associated. Slightly fewer respondents indicated familiarity with “foods for special medical purposes” (37%) and oral nutritional supplements (35%) (the survey was conducted in Polish, therefore the translated term and the English version were provided). Less frequently selected were responses regarding familiarity with all of the terms (14%) and unfamiliarity with any of them (12%). The smallest proportion of respondents selected the ONS answer (the untranslated version) (2%).
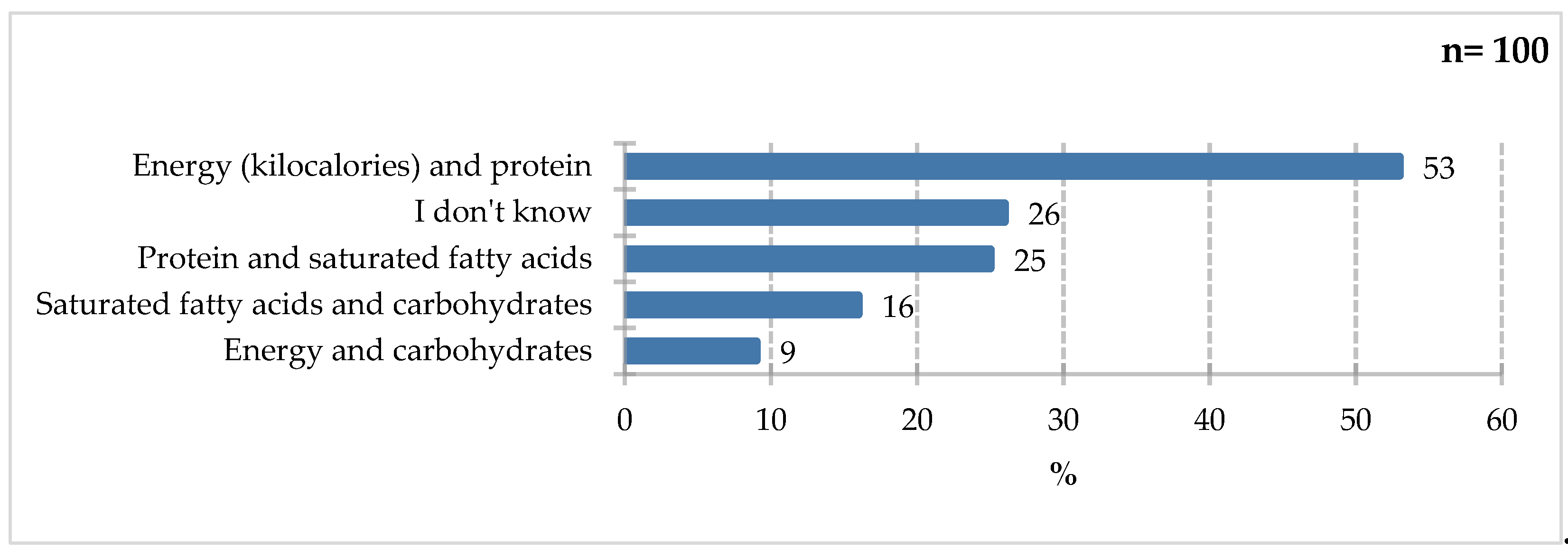
The largest group of respondents would emphasize energy, kilocalories, and protein (53%), indicating an understanding of the role of individual macronutrients in the diet (
Figure 3). Older adults should consume 1.2–1.5 g of protein/kg of body weight/day in acute or chronic conditions, and this intake should be increased to 2.0 g/kg/day in severe conditions or malnutrition. 30 kcal/kg/day is the recommended energy requirement, but other factors should be considered and recommendations should be individualized [
13]. In a review of the ESPEN guidelines, the authors identified varying energy and protein requirements depending on the disease state [
25]. For example, in the intensive care unit, it is recommended to implement enteral nutrition for up to 48 hours or parenteral nutrition between 3 and 7 days. If EN is not possible, the recommended energy requirement is 20–25 kcal/kg of body weight/day and 1.3 g protein/kg of body weight/day [
26]. For geriatric patients 30 kcal/kg of body weight/day is recommended. Oral nutritional support should provide at least 400 kcal, including at least 30 g of protein and at least 1.0 g/kg of body weight [
13]. A significant proportion of respondents indicated protein and saturated fat (25%), as well as saturated fat and carbohydrates (16%). Nine percent of respondents would emphasize energy and simple carbohydrates. Twenty-six percent of respondents declared they did not know the answer to this question.
According to the results in
Figure 4 respondents most frequently cited Nestlé (58%), Nutricia (40%), and Activ Lab (27%). Olimp Labs (20%), Fresenius Kabi (6%), and Nutrego (5%) were mentioned less frequently. Thirty percent of respondents declared they were unaware of any company producing foods for special medical purposes. The high brand awareness of Nestlé and Nutricia may be due to their strong market position, broad product offerings, and active promotional and educational activities. The lower recognition of the remaining companies suggests limited availability to patients or lower marketing expenditures. At the same time, the fact that nearly one-third of respondents were unable to identify any manufacturer indicates the need for further education about foods for special medical purposes among patients. If patients do not recognize the brand, they are likely unfamiliar with the product range, which may limit the possibility of using specific products as the best choice for a given patient.
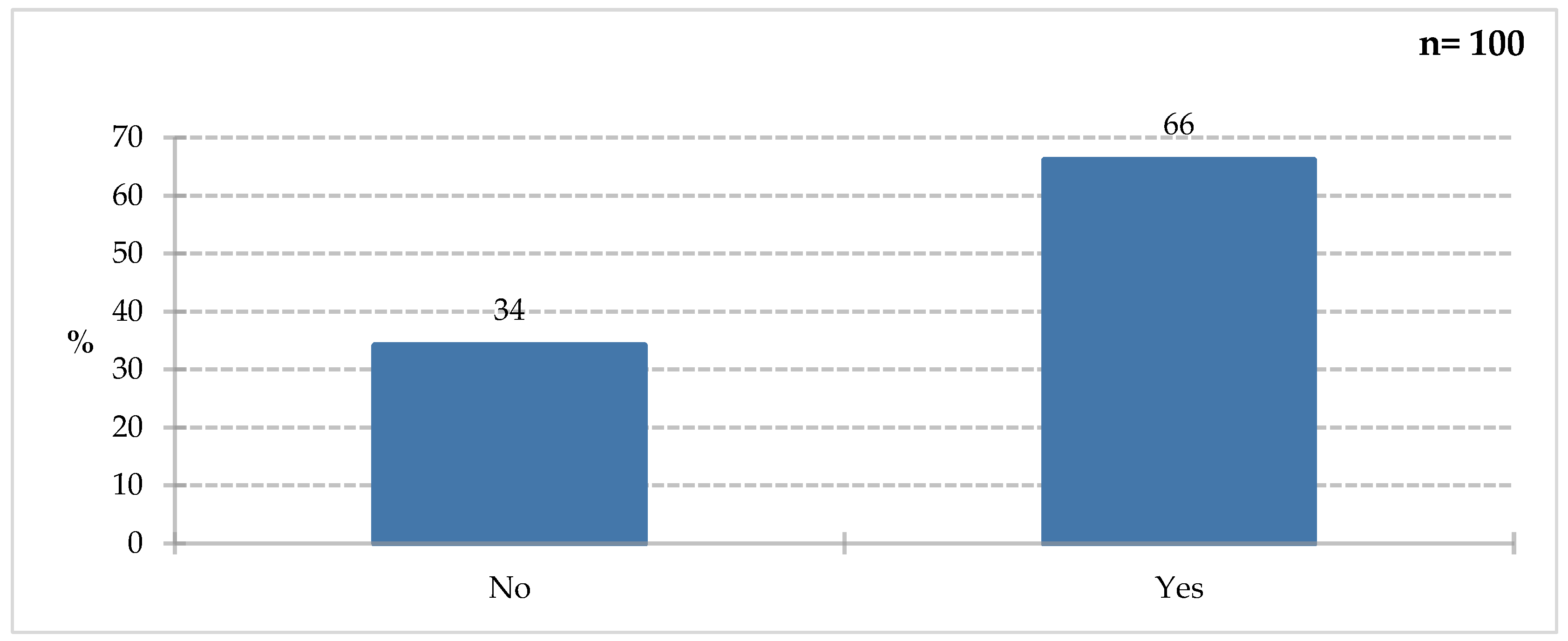
Among all respondents, 66% declared they had knowledge of the purpose of using special medical devices. However, 34% of this study participants provided a negative answer. To verify the correctness of the affirmative answer, the following question (
Figure 6) was asked: „You would use FSMP on people ? (only people who answered yes to the previous question answered)”.
Figure 5.
Percentage of respondents who answered the question100% „Do you know what food for special medical purposes are used for?”.
Figure 5.
Percentage of respondents who answered the question100% „Do you know what food for special medical purposes are used for?”.
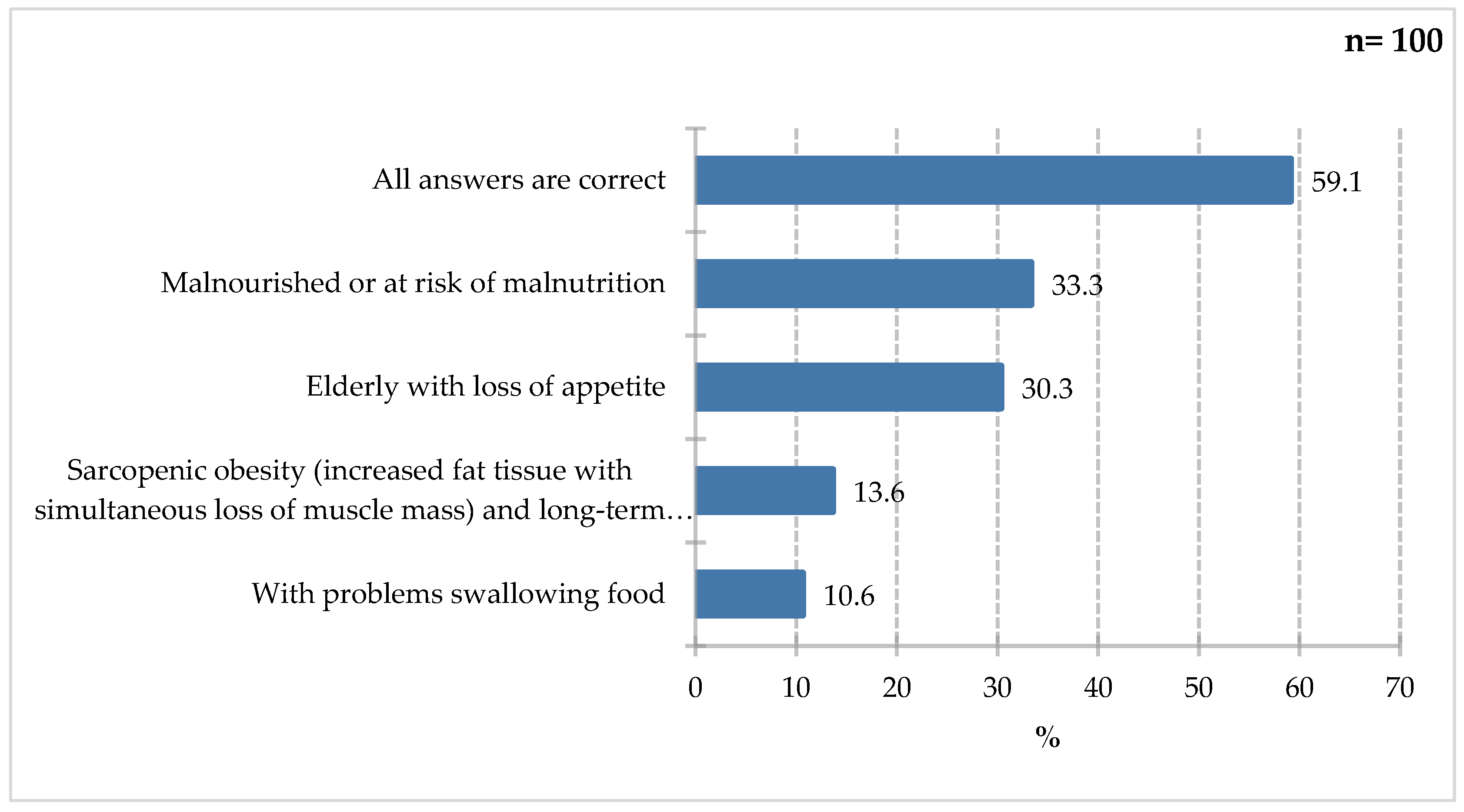
Figure 6.
Percentage of respondents who answered the question 68% „You would use FSMP on people ? (only people who answered yes to the previous question answered)”.
Figure 6.
Percentage of respondents who answered the question 68% „You would use FSMP on people ? (only people who answered yes to the previous question answered)”.
Respondents most frequently indicated the use of special medical purposes in individuals with malnutrition or at risk of malnutrition (33.3%) and in elderly individuals with a lack of appetite (30.3%). Slightly less frequently selected were patients with sarcopenic obesity, characterized by increased body fat combined with loss of muscle mass and long-term hospitalization (13.6%), as well as individuals with swallowing difficulties (10.6%). Furthermore, 59.1% of respondents indicated that all of the above answers were correct, indicating a deeper understanding of the issue of malnutrition in this patient group, as all of the above factors are indications for oral dietary fortification with ONS as the first step towards proper nutritional intervention. Indications for ONS use include:
- perioperative period – patients undergoing major procedures, gastrointestinal surgery, wound healing [
27,
28];
- oncological diseases – insufficient oral intake, prevention of malnutrition [
29];
- elderly patients – Individuals with sarcopenia, frailty syndrome, reduced appetite [
13];
- nephrology, pulmonology, neurology, psychiatry – debilitating, chronic diseases causing reduced intake, appetite disorders, and swallowing disorders [
28].
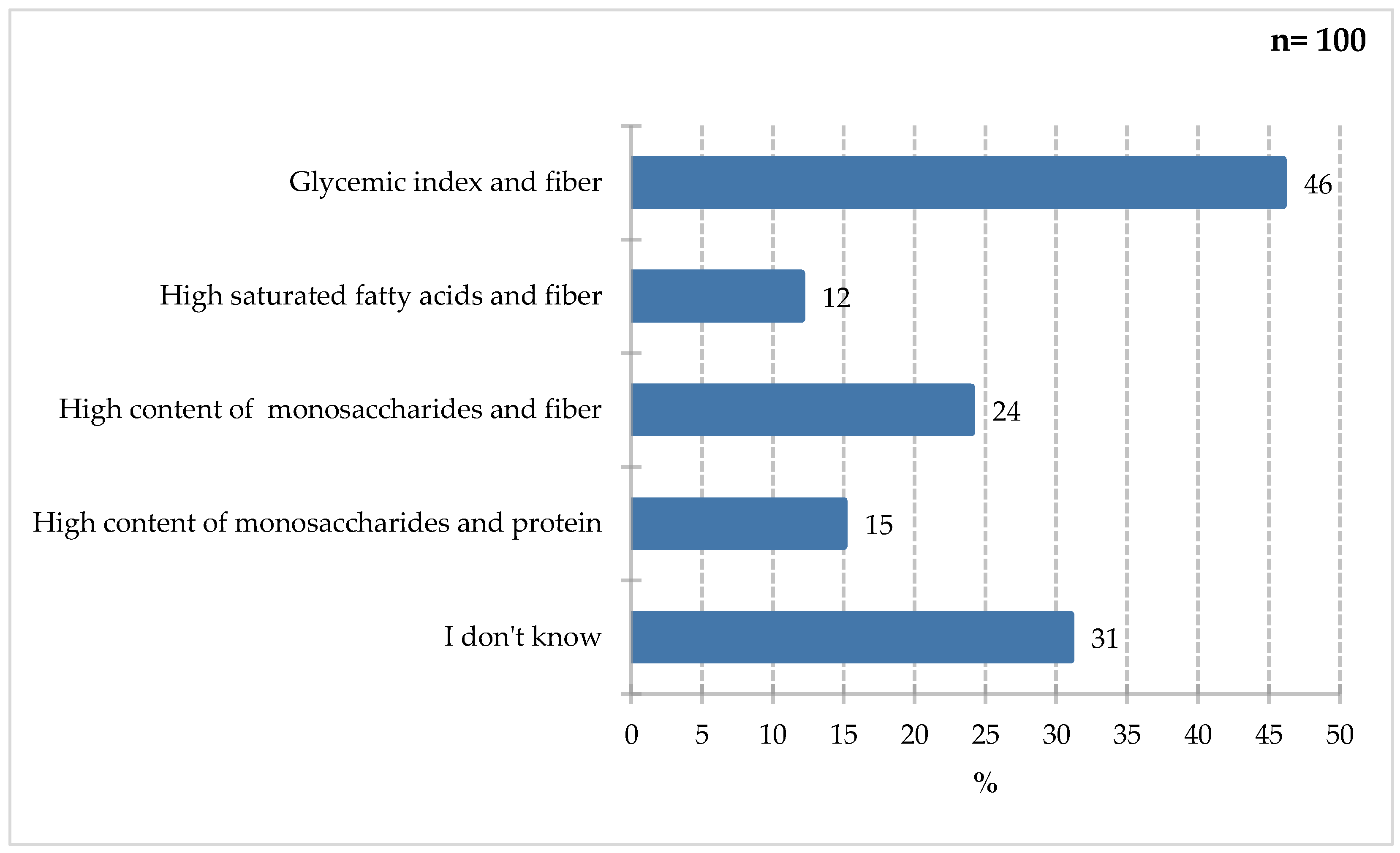
The results of the
Figure 7 indicate that respondents most frequently selected the glycemic index and fiber response (46%). Fewer participants indicated high simple sugar and fiber content (24%), high simple sugar and protein content (15%), and high saturated fat and fiber content (12%). Thirty-one percent of respondents declared a lack of knowledge in this area. Diabetes is a disease affecting a growing part of society. It often coexists with other conditions and carries complications such as e.g., diabetic foot and prolonged hospital stays. Patients with the disease, as well as others at increased risk, should be aware of the ingredients to look out for, which will also facilitate the decision-making process of selecting ONS for patients with glycemic disorders. According to the Polish recommendations [2025], it is necessary to pay attention to the glycemic load and index of a meal, and to consume adequate macronutrients, including fiber-rich carbohydrates (minimum 25 g/day or 15 g of fiber/1000 kcal of diet) [
30]. Limiting the consumption of simple sugars, especially added and free sugars, is crucial, in favor of low-calorie sweeteners. Attention has also been paid to the supply and quality of fats – limiting saturated fats to 10% of the diet’s energy value, in favor of plant-based fats [
30].
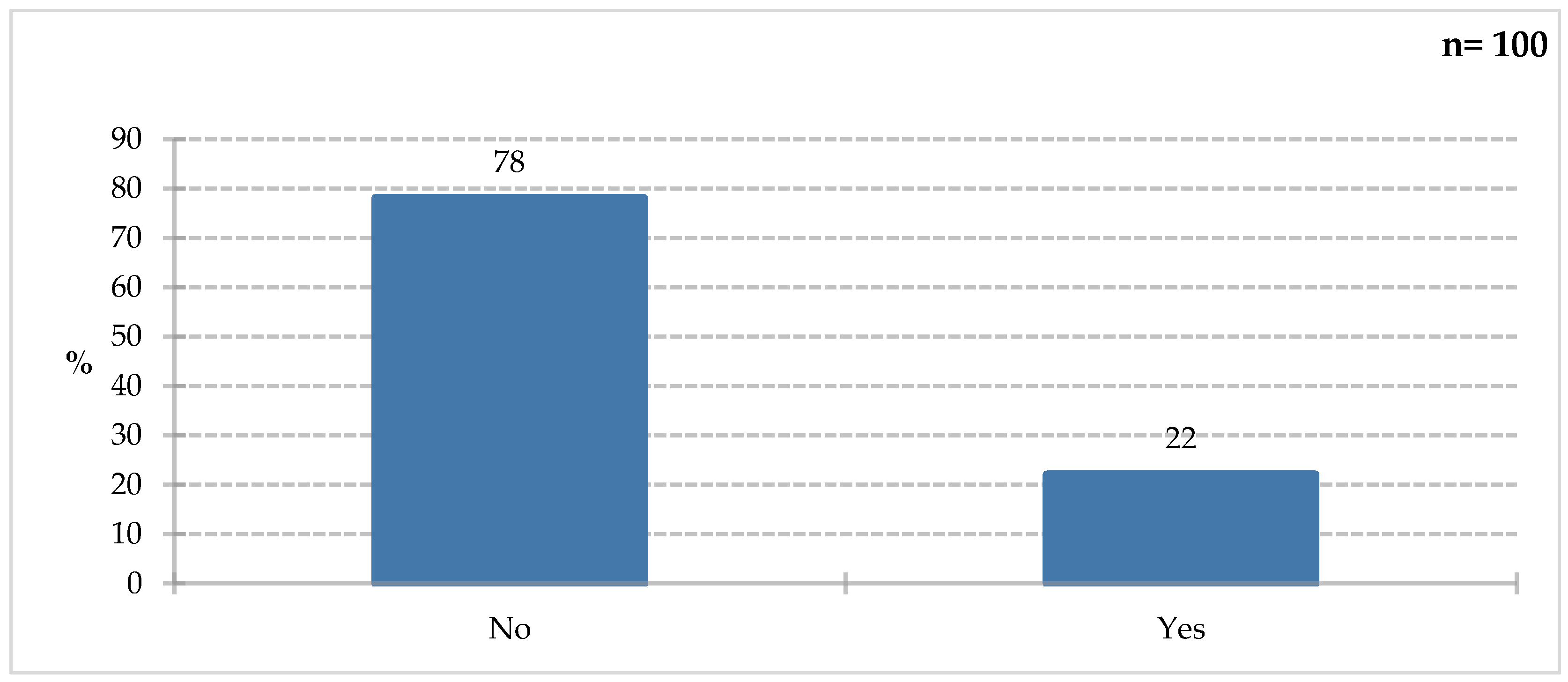
The majority of respondents (78%) were unfamiliar with immunomodulatory ingredients; only 22% of survey participants declared they were familiar with them (
Figure 8). To confirm their knowledge, they were asked to list them in the next question (
Figure 9).
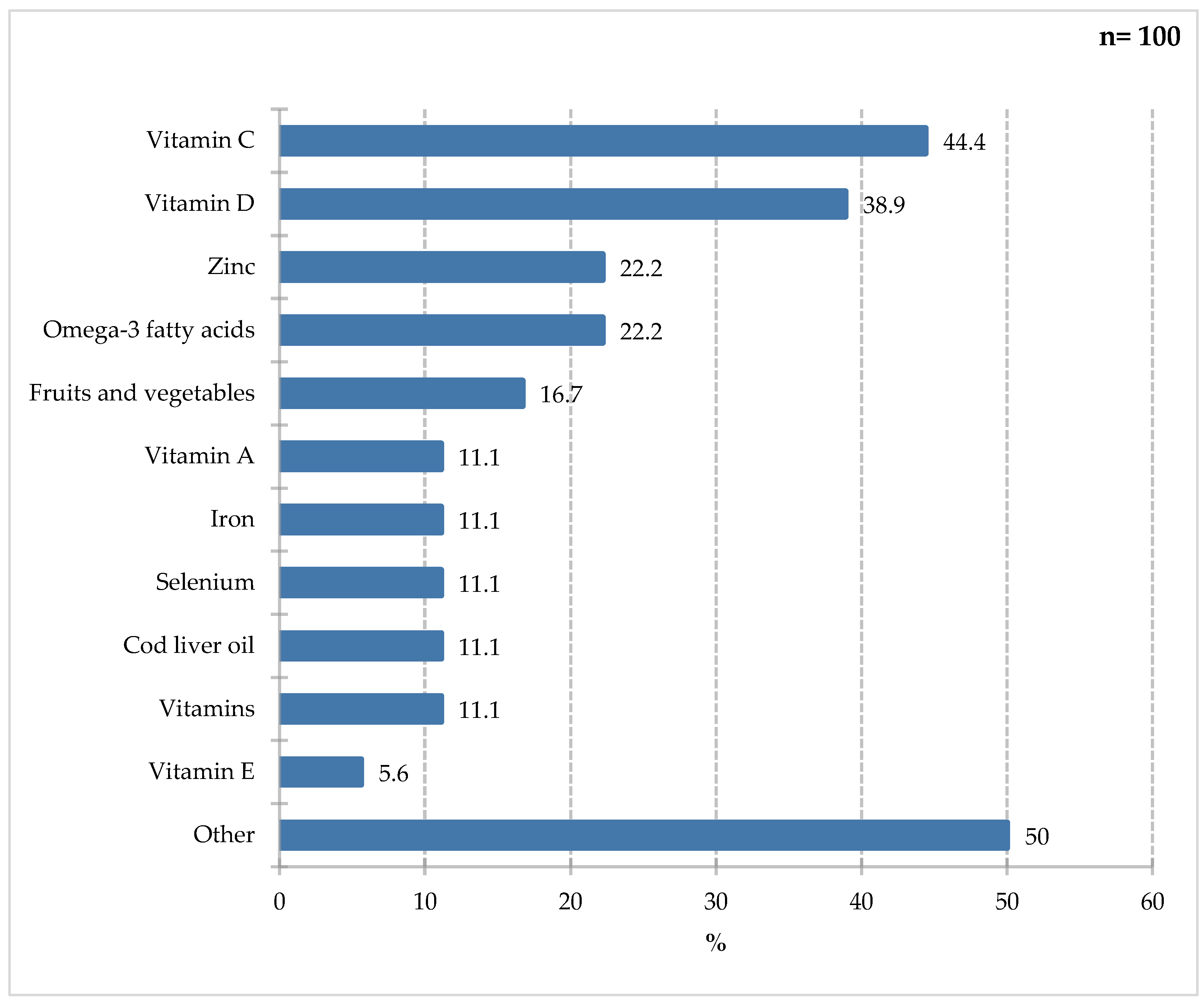
A large proportion of the responding group mentioned vitamin C (44.4%) and vitamin D (38.9%), with slightly smaller groups highlighting ingredients such as omega-3 fatty acids, and zinc (22.2%), selenium iron, and vitamin A. Finally, the “other” category, selected by 50% of study participants, included less relevant responses such as elderberry, the aforementioned fruits or vegetables, but also vitamin E, probiotics, and vitamin E, which fall into this category. Vitamin C, as a cofactor of many enzymes and an one of the important antioxidant, can have immunomodulatory effects. Adequate dietary levels of vitamin C reduce C-reactive protein levels. By stimulating neutrophil migration, it improves wound healing. Studies indicate that vitamin C supplementation may shorten the duration of infection [
28,
31,
32,
33]. The action of vitamin D is widely described in the literature. It influences the secretion of cytokines (IL− 12, IL− 2, IFN−γ) by macrophages, regulates gene expression and cell differentiation [
28,
34]. There is a correlation between the activity of B and T lymphocytes and antigen-presenting cells and vitamin D. It inhibits the secretion of c-reactive protein and IL-6 [
35].
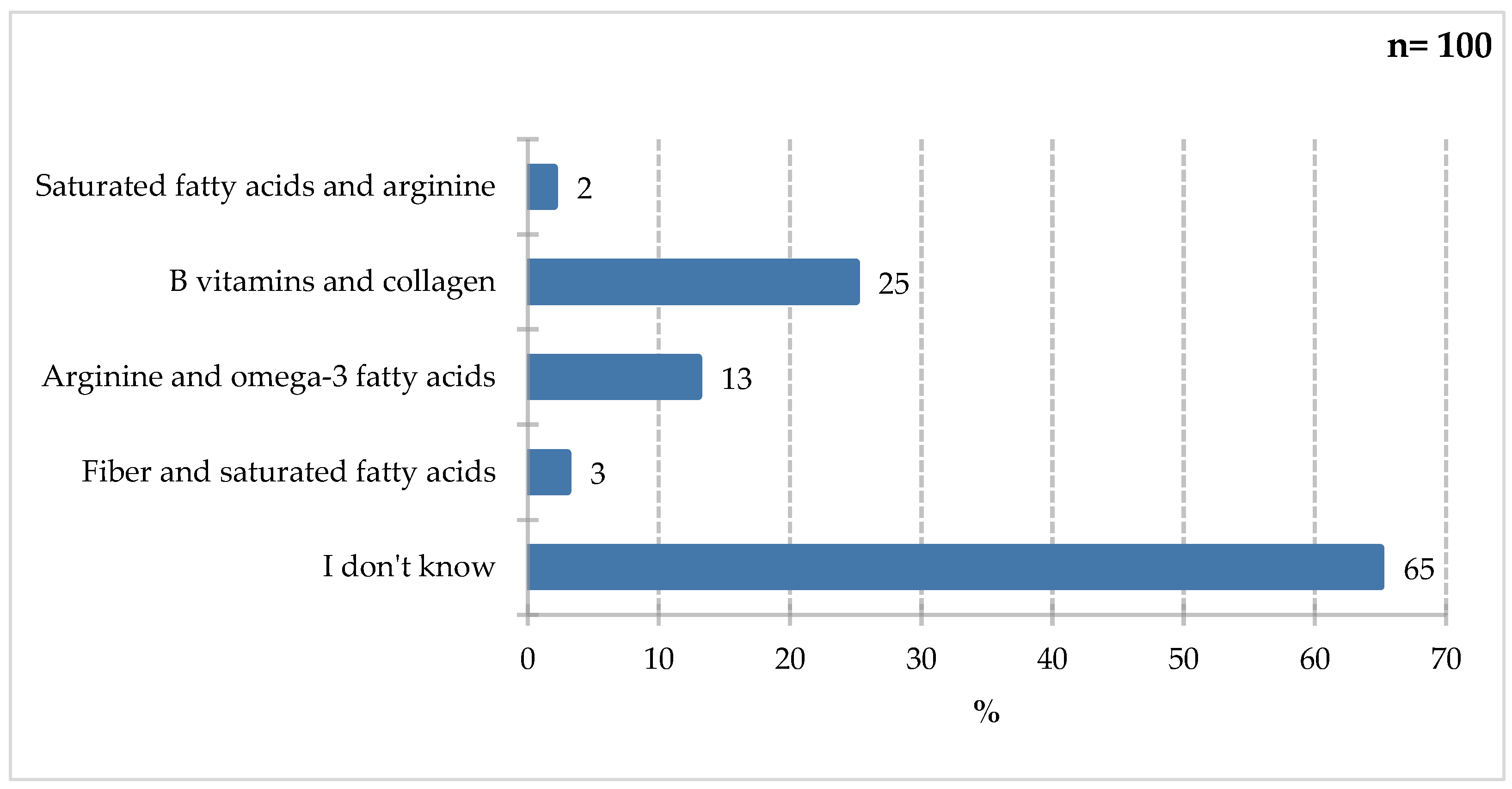
As shown in the
Figure 10 respondents most frequently indicated B-group vitamins and collagen (25%). Less frequently selected were arginine and omega-3 fatty acids (13%), fiber and saturated fatty acids (3%), and saturated fatty acids and arginine (2%). A significant proportion of respondents (65%) declared they did not know the answer to this question. A literature review by Arribas-López et al. [2021] indicated a positive effect of arginine and glutamine supplementation on wound healing or related parameters [
36]. In turn, patients supplemented with arginine, vitamin C, and zinc showed a clinically significant improvement in pressure ulcer healing [
37]. A study by Cheshmeh et al. [2021] also found a beneficial effect of arginine on pressure ulcer healing. Arginine and its metabolites improve wound healing through metabolism and nitric oxide (NO) synthesis, but attention is also drawn to the addition of other components, such as an adequate supply of calories and protein [
38]. Elahi et al. [2012], in a review on the effects of fish oil, including omega-3 fatty acids, described various mechanisms and effects on the healing of stage 1 pressure ulcers. They indicated the formation of blood vessels in the ulcer, shortened hospital stays in surgical patients, and stimulation of cytokine activity [
40]. In turn, in patients in the intensive care unit, the use of fish oil locally as dressings has a beneficial effect in preventing pressure ulcer development [
41]. According to the review by Dospra et al. [2024] supplementation with eicosapentaenoic acid (EPA) in the postoperative period may contribute to reducing the risk of infection, supporting the wound healing process and shortening the recovery time of patients [
42].
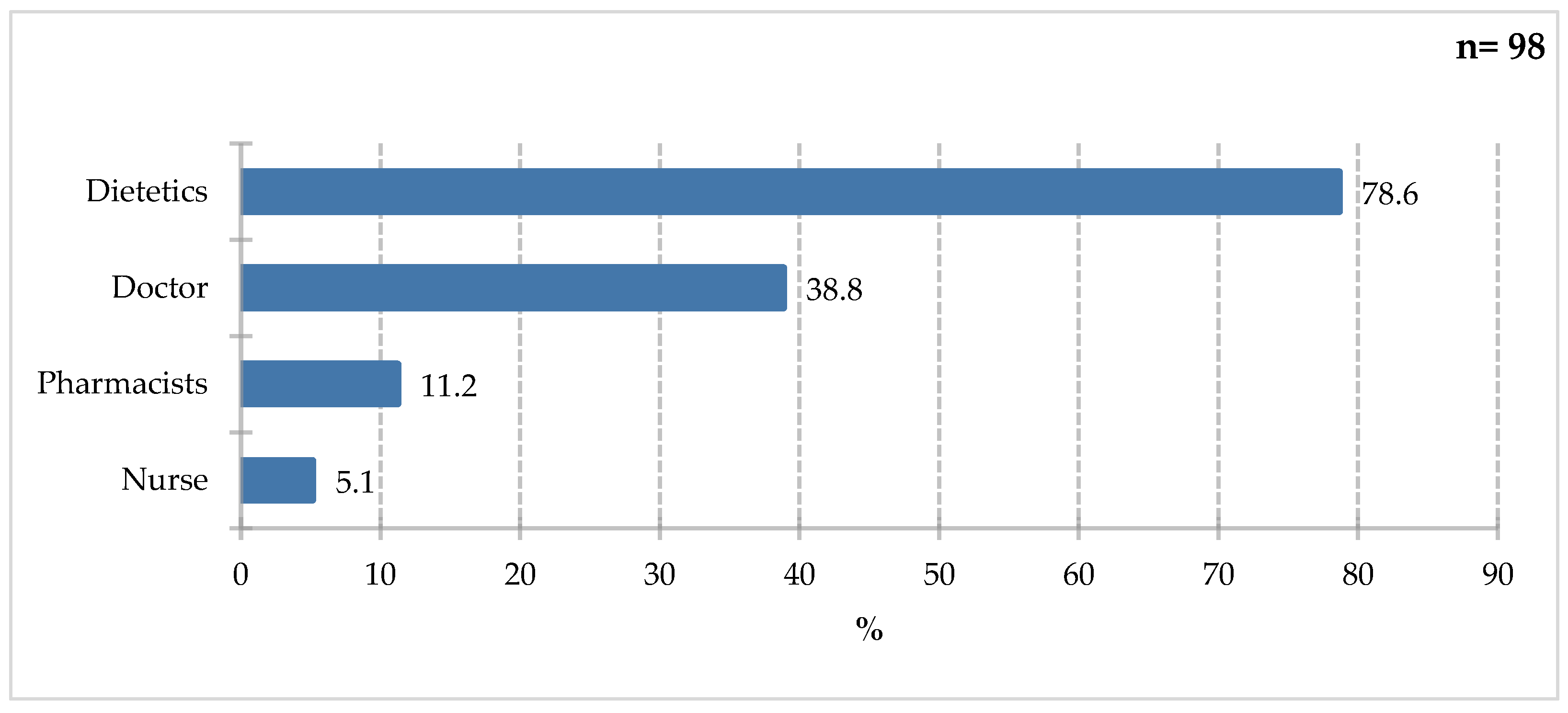
Survey participants most often cited a dietitian (78.6%) as the specialist they would seek advice on selecting special medical supplies. Physicians (38.8%) and pharmacists (11.2%) were significantly less likely to choose one. Nurses were cited by 5.1% of respondents (
Figure 11). Although, by law, only a physician can prescribe ONS for a hospitalized patient, a dietitian can be an important part of the process. Patient responses also indicate a growing trust in this professional group.
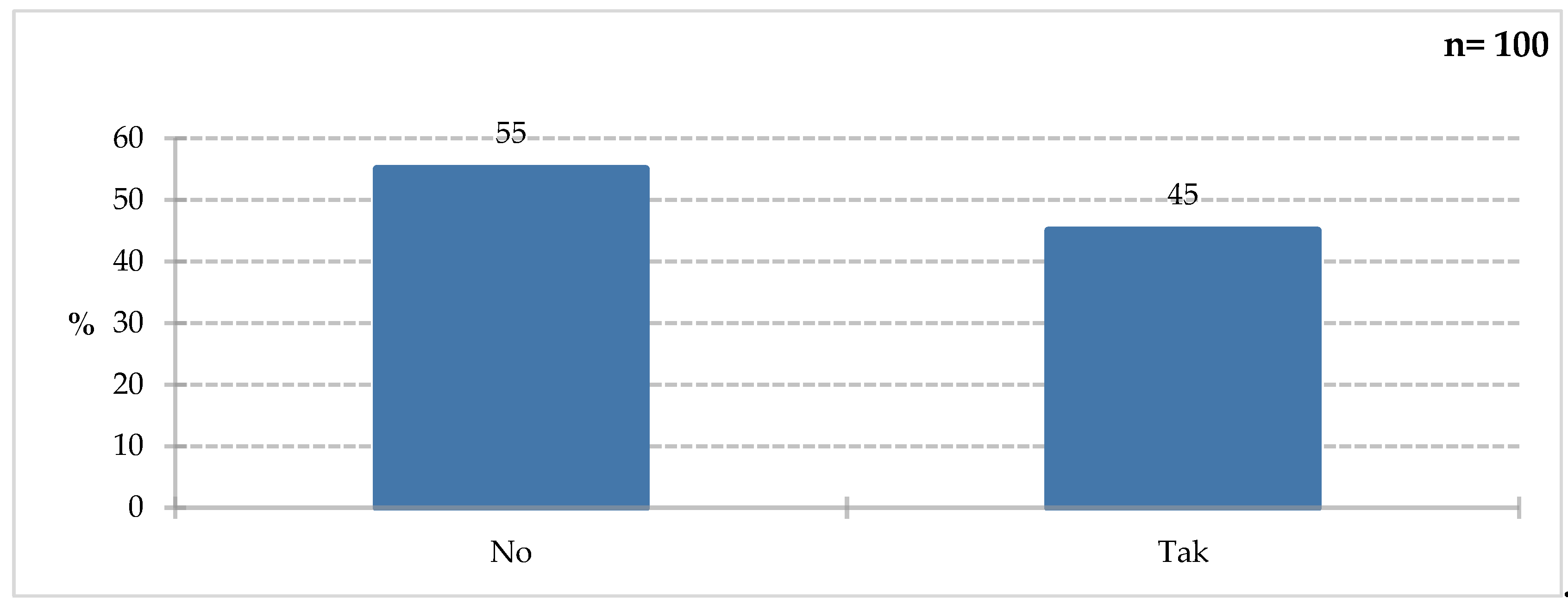
Forty-five percent of respondents confirmed that they had experience with this type of food during their hospital stay (
Figure 12).
Figure 12.
Percentage of respondents who answered the question100% „Have you ever use food for special medical purposes during your hospitalization?”.
Figure 12.
Percentage of respondents who answered the question100% „Have you ever use food for special medical purposes during your hospitalization?”.
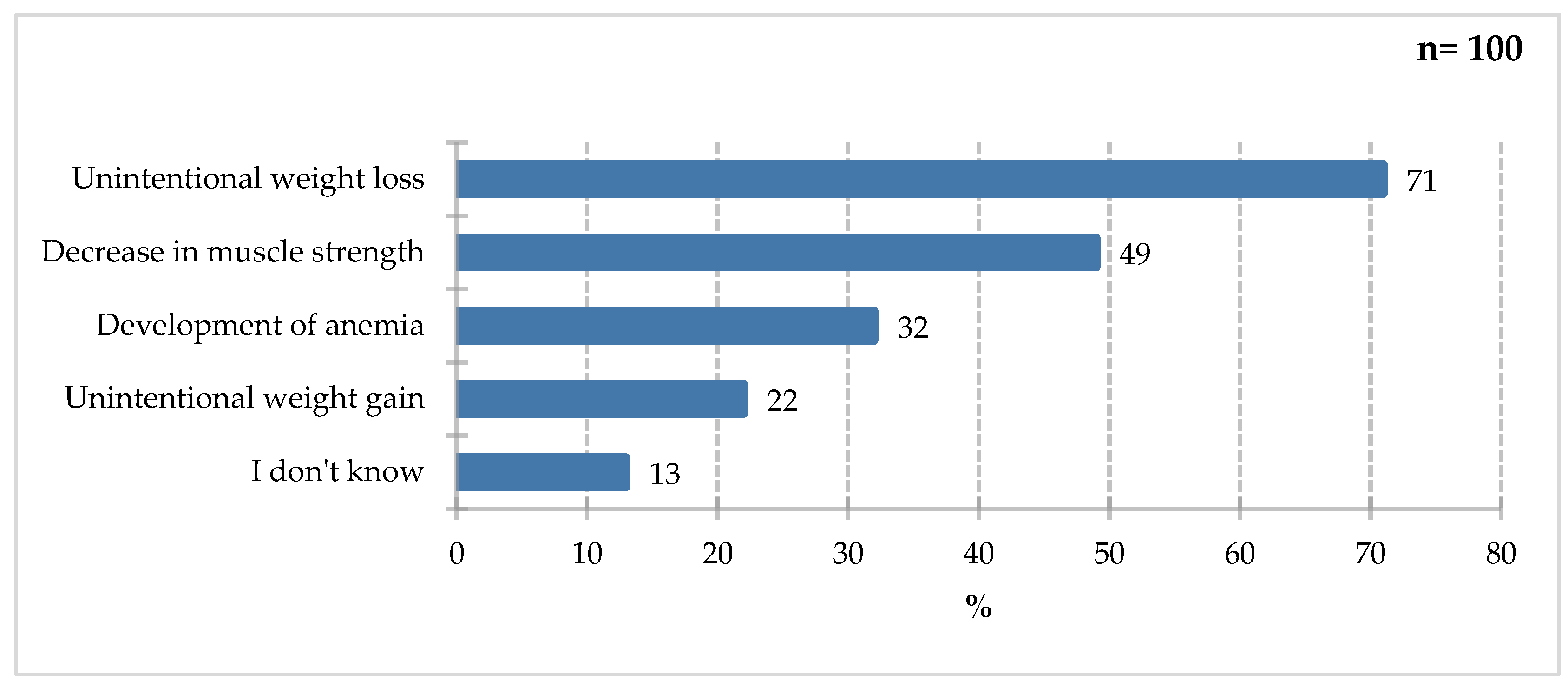
Figure 13.
Percentage of respondents who answered the question 100% „Which of the following symptoms would you notice as risk factors for malnutrition?”.
Figure 13.
Percentage of respondents who answered the question 100% „Which of the following symptoms would you notice as risk factors for malnutrition?”.
The largest share of study participants would report unintentional weight loss (71%). Decreased muscle strength (49%) and the development of anemia (32%) were also frequently mentioned. Unintentional weight gain (22%) and lack of knowledge on the subject (13%) were less frequently mentioned. Underweight in adults is defined as a BMI below 18.5. Consequences of insufficient dietary intake include impaired function, negative impact on muscle mass and fitness, sarcopenia, and the development of anemia. Unintentional weight gain can lead to overweight and obesity, but it does not correlate with an increased risk of underweight, which does not exclude the occurrence of sarcopenia and qualitative malnutrition in excess body weight [
43].
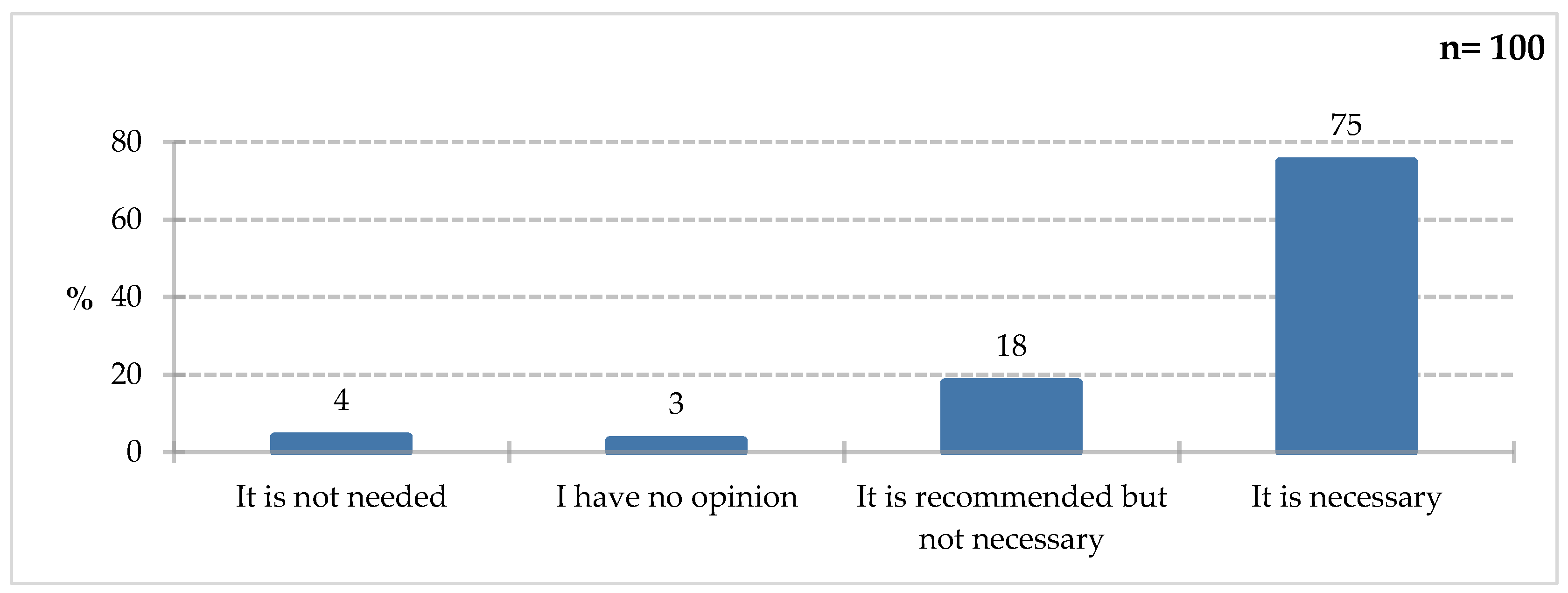
Respondents most often believed that collaboration with a dietitian on hospital wards was necessary (75%). It was recommended, but not essential, according to 18% of respondents; only 4% declared it unnecessary, while 3% had no opinion on the matter (
Figure 14). It’s encouraging that patients are beginning to understand the role of nutrition and the need for interdisciplinary collaboration. Dietitians in hospitals play a role as important as other medical professionals, assessing nutritional status, providing nutritional education to patients, fortifying a natural diet, and collaborating with the interdisciplinary team to determine nutritional treatment. According to a 2018 report, the role of dietitians in hospitals is still misunderstood. In the audited facilities, nutritional education was lacking, with each dietitian serving between 76 and 740 patients, and additional duties unrelated to their competencies were assigned, such as warehouseman, kitchen assistant, or archivist [
44]. This may be due to the lack of regulations regarding the scope of duties and competences of the dietitian. Bator [2017] assessed the nutritional knowledge of healthcare workers, and the results were clear: the staff’s knowledge was insufficient and the dietitian should be responsible for providing nutritional education to patients [
45]. Folwarski and Wernio [2023] clearly described the benefits of employing a dietitian in hospitals, such as improved detection of malnutrition and shorter hospital stays, as well as significant savings due to the accuracy of nutritional intervention tailored to the patient’s condition and needs [
12]. Mogiłko and Zarzeczny [2024], in turn, emphasize the dietitian’s important role in the prehabilitation process, as one of the new but crucial tasks in patient care. This includes the selection of individualized nutritional recommendations, assessment of nutritional status, and continuous monitoring of outcomes [
46].
Figure 14.
Percentage of respondents who answered the question 100% „How do you assess the need for cooperation with a dietitian in hospital wards?”.
Figure 14.
Percentage of respondents who answered the question 100% „How do you assess the need for cooperation with a dietitian in hospital wards?”.
Figure 15.
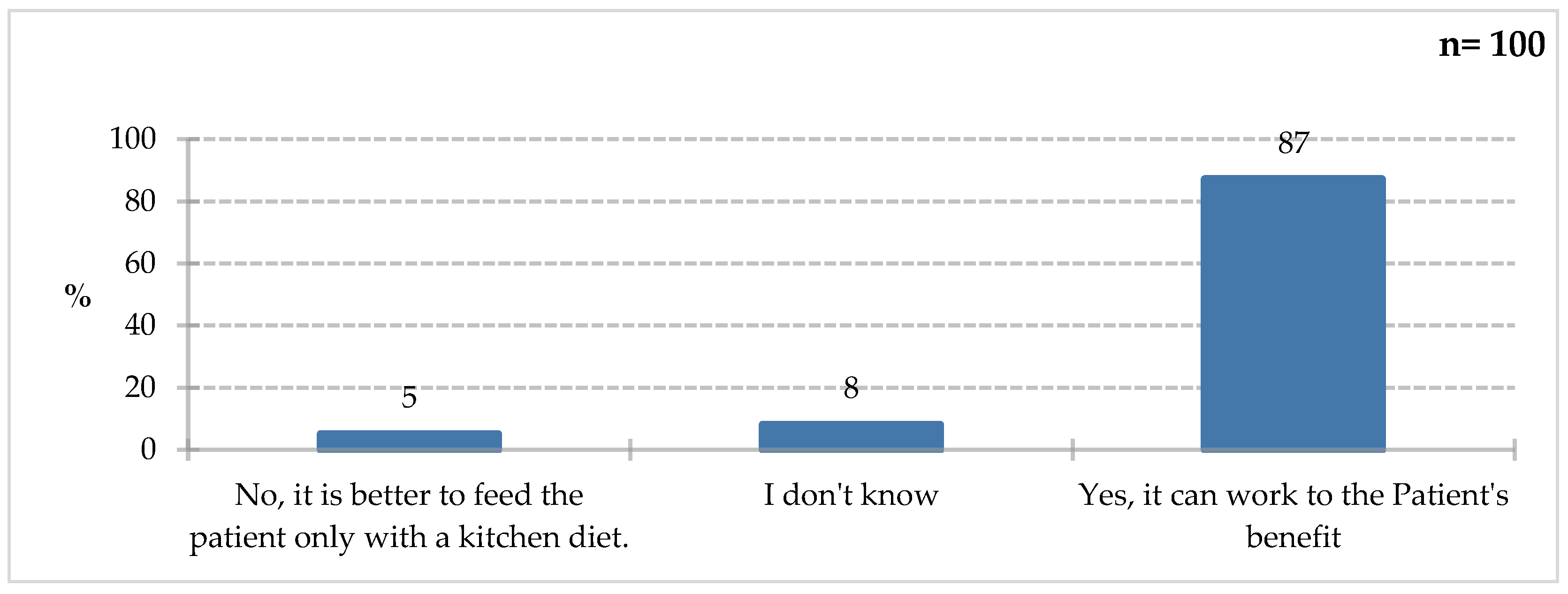
Percentage of respondents who answered the question 100% „Do you think that the use of FSMP purposes can be an important measure to improve or maintain the nutritional status of hospitalized patients?”.
Figure 15.
Percentage of respondents who answered the question 100% „Do you think that the use of FSMP purposes can be an important measure to improve or maintain the nutritional status of hospitalized patients?”.
The vast majority of respondents (87%) agreed that the use of foods for special medical purposes can be a significant step towards improving or maintaining the nutritional status of hospitalized patients, pointing to the potential benefits for these patients. As previously indicated, ONS are used in many medical conditions. It is worth noting that 13% of respondents either lack knowledge on this topic or believe that a traditional kitchen diet is sufficient. This indicates the need for educational initiatives.
Table 2.
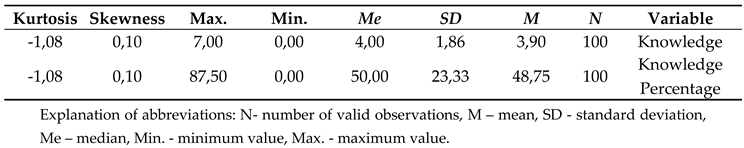
Knowledge of study participants - basic descriptive statistics.
Table 2.
Knowledge of study participants - basic descriptive statistics.
In the knowledge test regarding foods for special medical purposes, participants scored an average of 3.90 (SD = 1.867) points out of 8 possible points. The mean percentage score was 48.75% (SD = 23.33). The interpretation of participants’ knowledge is presented in the graph (<25% - lack of knowledge, <50% - low level of knowledge, <75% - average level of knowledge, >=75% - high level of knowledge).
Figure 16.
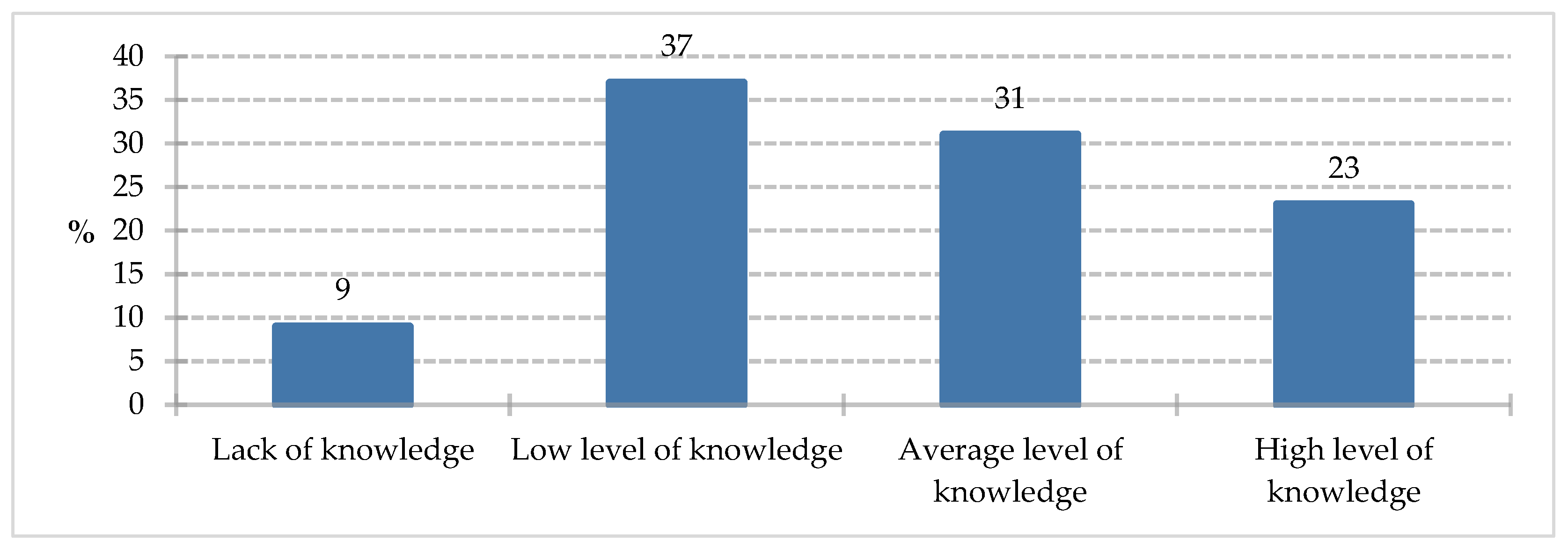
Distribution of knowledge among study participants.
Figure 16.
Distribution of knowledge among study participants.
Respondents most often demonstrated a low level of knowledge in the test (37%). An average level of knowledge was recorded for 31% of study participants. A high level of knowledge was achieved by 23% of respondents, and a lack of knowledge in the area under study was noted by 9% of participants.
To determine the direction and strength of the relationship between age and knowledge about specialty foods, Spearman’s monotonic correlation coefficient was used. The results of the analysis are presented in
Table 3.
The results of the Spearman’s rho correlation analysis indicate a significant correlation between age and knowledge about special-purpose foods, rho = -0.32, p = 0.001, n = 98 - the strength of the correlation turned out to be moderate, the direction of the correlation turned out to be negative - with increasing age, the level of knowledge about special-purpose foods decreases significantly.
The observed negative association between age and knowledge of foods for special medical purposes is clinically relevant, particularly in the context of geriatric care. Older patients are at the highest risk of disease-related malnutrition, sarcopenia, and functional decline, while simultaneously demonstrating lower awareness of available nutritional interventions. These findings highlight the need for targeted, age-adapted nutritional education strategies in hospital settings, with particular emphasis on geriatric patients, for whom simplified communication, repeated counseling, and close cooperation with dietitians may be crucial elements of effective malnutrition prevention and lifecare. Such an approach aligns with the concept of lifecare, emphasizing not only the provision of nutritional support, but also patient-centered education as an integral component of comprehensive malnutrition management in older adults.
The most important descriptive statistics regarding knowledge, broken down by gender, are presented in the table (
Table 4).
The Shapiro-Wilk test was used to test the normality of the residual distribution. The results are presented in
Table 5.
The results of the Shapiro-Wilk test indicate a non-normal distribution of residuals for the knowledge level variable.
The table presents the results of the analysis of equality of variance for the ‘Knowledge’ variable, conducted using Leven’s test (
Table 6).
The results of the Leven’s test indicate that the variances of the compared groups were unequal for the ‘Knowledge’ variable.
The Mann-Withney test was used to analyze the significance of differences in knowledge levels (dependent variable) while taking into account gender (independent variable). The results are presented in
Table 7.
The results of the study, using the Mann-Withney test, suggest that the level of knowledge does not differ statistically significantly between women and men.
Basic descriptive statistics regarding knowledge, broken down by comorbidities, are presented in
Table 8.
The Shapiro-Wilk test was used to test the normality of the residual distribution. The results are presented in
Table 9.
Data analysis, conducted using the Shapiro-Wilk test, revealed a non-normal distribution of residuals for the knowledge level variable. Levene’s test was used to analyze the equality of variances for the ‘Knowledge’ variable.
Table 10.
‘Knowledge’ - Leven’s test results (equality of variances).
Table 10.
‘Knowledge’ - Leven’s test results (equality of variances).
| p |
df2 |
df1 |
|
F |
Variable |
| 0,047 |
98 |
1 |
* |
4,06 |
Knowledge |
The results of the study, based on Leven’s test, indicate a lack of equality of variances between the compared groups in terms of knowledge level.
The Mann-Withney test was used to analyze the significance of differences in knowledge level (dependent variable) while taking into account the presence of comorbidities (independent variable). The obtained results are presented in
Table 11.
The Mann-Withney test did not reveal any significant differences in the level of knowledge between people with comorbidities and those without them.
Numerous studies confirm the effectiveness of FSMP in various physiological conditions and individual diseases. The use of ONS for at least 7 days in patients in the preoperative period for gastrointestinal procedures reduces the incidence of infections and the length of hospitalization [
19]. A literature review by Tangvik et al. [2020] examined the effects of ONS supplementation in patients with dementia on daily dietary intake, nutritional status, and cognitive and functional function, focusing on malnourished patients. ONS consumption had a positive effect on nutritional status, daily protein and energy intake, but no correlation was detected with improved cognitive or functional function. One study included 65-year-olds classified as at moderate to high risk of malnutrition using the Malnutrition Universal Screening Tool (MUST). Participants were divided into two groups: control and treatment for 180 days. The control group received two servings per day of ONS containing beta-hydroxy-beta-methylbutyrate with dietary counseling or the treatment group received two servings per day of a placebo supplement with dietary counseling. The results clearly established that ONS supplemented with HMB and vitamin D, along with dietary counseling, significantly improved nutritional and functional outcomes in older adults at risk of malnutrition compared with placebo supplementation combined with dietary counseling [
11]. Liu et al. [2021] analyzed 22 studies of ONS consumption in patients undergoing hemodialysis (HD) or peritoneal dialysis (PD), who are at high risk of malnutrition due to their disease. The ONS group had significantly higher serum albumin levels, body mass index (BMI), and handgrip strength (HGS) from the beginning to the end of the intervention. No significant differences were observed between groups in terms of lean body mass, phase angle, C-reactive protein concentration, and serum phosphorus and potassium levels. The effectiveness of ONS in elderly patients with anorexia has also been assessed. Their use has been shown to improve appetite to some extent and have a beneficial effect on body weight and food intake. Researchers also suggest a reduction in the incidence of pressure sores and diarrhea, as well as lower treatment costs, but these data should be comprehensively studied [
22]. Benefits of ONS consumption have also been observed in malnourished children in developing countries, particularly on growth and weight gain. Adequate nutritional status in children characteristically improves motor and cognitive function in adolescents [
23]. Baldwin et al. [2021] suggest that the effects of ONS consumption in selected patient groups should be further investigated, given the unclear benefits of their use, based on 22 literature reviews [
24]. Therefore, actions aimed at expanding and shaping the knowledge and awareness of hospitalized patients, but also their medical caregivers, are becoming a priority.
The study’s limitations include the small number of respondents. Interpretation problems were initially caused by questions that respondents answered multiple times.