Submitted:
06 February 2026
Posted:
06 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Overview and Setting
2.2. Recruitment
2.2. Data Collection
2.3. Mental Health Reports
2.4. Follow-Up Survey
2.5. Analyses
2.6. Research Ethics
3. Results
3.1. Participant Demographics
3.2. Mental Disorder Symptom Prevalence
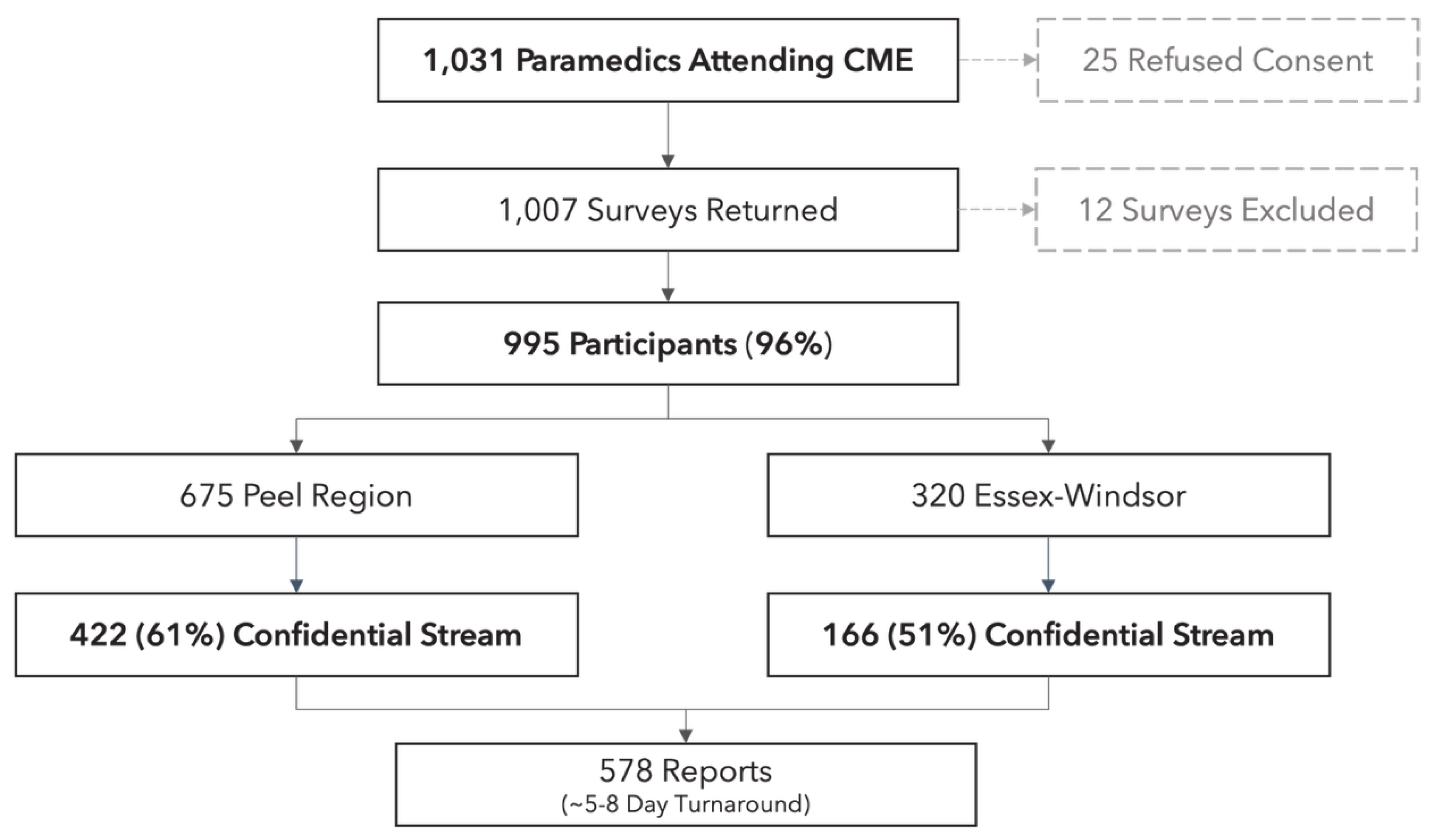
3.3. Delivery of Mental Health Reports
3.4. Follow-Up Survey Responses
3.5. Survey Comments
4. Discussion
4.1. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ACP | Advanced Care Paramedic |
| ANOVA | Analysis of Variance |
| AUDIT | Alcohol Use Disorders Identification Test |
| CAD | Canadian Dollars |
| CME | Continuing Medical Education |
| EW-EMS | Essex-Windsor Emergency Medical Services |
| GAD | Generalized Anxiety Disorder |
| GAD-7 | 7-Item Generalized Anxiety Disorder Scale |
| ISI | Insomnia Severity Index |
| MDD | Major Depressive Disorder |
| NNT | Number Needed to Treat |
| OR | Odds Ratio |
| PCP | Primary Care Paramedic |
| PCL-5 | Posttraumatic Stress Disorder Checklist for DSM-5 |
| PHQ-9 | 9-Item Patient Health Questionnaire |
| PRPS | Peel Regional Paramedic Services |
| PSP | Public Safety Personnel |
| PTSD | Posttraumatic Stress Disorder |
| PTSI | Post-Traumatic Stress Injuries |
| RCMP | Royal Canadian Mounted Police |
| SD | Standard Deviation |
| SPSS | Statistical Package for the Social Sciences |
| WHO | World Health Organization |
| 2SLGBTQI | Two Spirit, Lesbian, Gay, Bisexual, Transgender, Queer/Questioning, Intersex, and additional gender identities |
References
- Public Health Agency of Canada. Federal framework on post-traumatic stress disorder (PTSD): Report to Parliament 2025. 2025.
- Public Safety Canada. Evaluation of the initiatives to address post-traumatic stress injuries (PTSI) among public safety officers. 2023. [Google Scholar]
- Carleton, R.N.; Afifi, T.O.; Taillieu, T.; Turner, S.; Krakauer, R.; Anderson, G.S.; MacPhee, R.S.; Ricciardelli, R.; Cramm, H.A.; Groll, D.; et al. Exposures to potentially traumatic events among public safety personnel in Canada. Canadian Journal of Behavioural Science / Revue canadienne des sciences du comportement 2019, 51, 37–52. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; Duranceau, S.; LeBouthillier, D.M.; Sareen, J.; Ricciardelli, R.; MacPhee, R.; Groll, D.; et al. Mental disorder symptoms among public safety personnel in Canada. Can J Psychiatry 2018, 63, 54–64. [Google Scholar] [CrossRef]
- Tavares, W.; Kaas-Mason, S.; Spearen, C.; Kedzierski, N.; Watts, J.; Moran, P.; Leyenaar, M.S. Redesigning paramedicine systems in Canada with “IMPACC”. Paramedicine 2024. [Google Scholar] [CrossRef]
- Li, K.; Frumkin, A.; Bi, W.G.; Magrill, J.; Newton, C. Biopsy of Canada's family physician shortage. Fam Med Community Health 2023, 11. [Google Scholar] [CrossRef]
- Hoell, A.; Kourmpeli, E.; Dressing, H. Work-related posttraumatic stress disorder in paramedics in comparison to data from the general population of working age. A systematic review and meta-analysis. Front Public Health 2023, 11, 1151248. [Google Scholar] [CrossRef]
- Chan, S.C.; Jenkins, J.L.; Zhang, A.; Everly, G.S., Jr.; Roemer, E.C.; Hsu, E.B.; Han, G.; Sharma, R.; Asenso, E., Jr.; Bidmead, D.; et al. Incidence, Prevalence, and Severity of Mental Health Issues Among Emergency Medical Service Clinicians: A Systematic Review and Meta-Analysis. The Journal of emergency medicine 2025, 79, 427–442. [Google Scholar] [CrossRef]
- McGlynn, C.; Choudhury, A. Mental Health Safety Challenges Among Pre-Hospital Emergency Medical Service Providers: A Scoping Review. IISE Trans Occup Ergon Hum Factors 2025, 1–32. [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; LeBouthillier, D.M.; Duranceau, S.; Sareen, J.; Ricciardelli, R.; MacPhee, R.S.; Groll, D.; et al. Suicidal ideation, plans, and attempts among public safety personnel in Canada. Canadian Psychology/Psychologie canadienne 2018, 59, 220–231. [Google Scholar] [CrossRef]
- Angehrn, A.; Teale Sapach, M.J.N.; Ricciardelli, R.; MacPhee, R.S.; Anderson, G.S.; Carleton, R.N. Sleep Quality and Mental Disorder Symptoms among Canadian Public Safety Personnel. Int J Environ Res Public Health 2020, 17. [Google Scholar] [CrossRef] [PubMed]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; El-Gabalawy, R.; Sareen, J.; Asmundson, G.J.G. Chronic pain among public safety personnel in Canada. Canadian Journal of Pain 2017, 1, 237–246. [Google Scholar] [CrossRef] [PubMed]
- Carleton, R.N.; Afifi, T.O.; Taillieu, T.; Turner, S.; El-Gabalawy, R.; Sareen, J.; Asmundson, G.J.G. Anxiety-related psychopathology and chronic pain comorbidity among public safety personnel. J Anxiety Disord 2018, 55, 48–55. [Google Scholar] [CrossRef]
- Edgelow, M.; Brar, S.; Fecica, A. Worker's compensation usage and return to work outcomes for Ontario public safety personnel with mental stress injury claims: 2017–2021. Frontiers in Organizational Psychology 2023, 1. [Google Scholar] [CrossRef]
- Agarwal, G.; Pirrie, M.; Angeles, R.; Marzanek, F.; Paterson, J.M.; Nguyen, F.; Thabane, L. Community Paramedicine Program in Social Housing and Health Service Utilization: A Cluster Randomized Clinical Trial. JAMA Netw Open 2024, 7, e2441288. [Google Scholar] [CrossRef]
- Agarwal, G.; Angeles, R.; Brar, J.; Pirrie, M.; Marzanek, F.; McLeod, B.; Thabane, L. Effectiveness of the community paramedicine at home (CP@home) program for frequent users of emergency medical services in Ontario: a randomized controlled trial. BMC Health Serv Res 2024, 24, 1462. [Google Scholar] [CrossRef] [PubMed]
- Teckchandani, T.A.; Shields, R.E.; Andrews, K.L.; Nisbet, J.; Afifi, T.O.; Asmundson, G.J.G.; Maguire, K.Q.; Jamshidi, L.; Neary, J.P.; Krätzig, G.P.; et al. Monthly Mental Health Self-Monitoring and Positive Changes in Mental Health Disorder Symptoms Scores Among Royal Canadian Mounted Police Cadets. International Journal of Cognitive Behavioral Therapy 2025, 18, 425–454. [Google Scholar] [CrossRef]
- Handley, K.; Carleton, R.N.; Deschênes, A.A.; Devlin, J.; Kamkar, K.; Lee, V.; Mackoff, R.; Martin-Doto, C.A.; Shields, N.; Stockdale, K.; et al. Safeguard programs and mandatory mental health checks in Canadian police agencies: history, trends, and future directions. Journal of Community Safety and Well-Being 2025, 10, 38–42. [Google Scholar] [CrossRef]
- Corthesy-Blondin, L.; Genest, C.; Dargis, L.; Bardon, C.; Mishara, B.L. Reducing the impacts of exposure to potentially traumatic events on the mental health of public safety personnel: A rapid systematic scoping review. Psychol Serv 2022, 19, 80–94. [Google Scholar] [CrossRef] [PubMed]
- Newell, C.J.; Ricciardelli, R.; Czarnuch, S.M.; Martin, K. Police staff and mental health: barriers and recommendations for improving help-seeking. Police Practice and Research 2021, 23, 111–124. [Google Scholar] [CrossRef]
- Howe, E.; Czarnuch, S.; Ricciardelli, R.; Leduc, N. Exploring Canadian Public Safety Communicator Mental Health Help-Seeking Behaviors. New Solut 2025, 10482911251326648. [Google Scholar] [CrossRef]
- Ricciardelli, R.; Carleton, R.N.; Mooney, T.; Cramm, H. “Playing the system”: Structural factors potentiating mental health stigma, challenging awareness, and creating barriers to care for Canadian public safety personnel. Health 2020, 24, 259–278. [Google Scholar] [CrossRef]
- Ricciardelli, R.; Andres, E.; Kaur, N.; Czarnuch, S.; Carleton, R.N. Fit for public safety: Informing attitudes and practices tied to the hiring of public safety personnel. Journal of Workplace Behavioral Health 2019, 35, 14–36. [Google Scholar] [CrossRef]
- Donnelly, E.A.; Bradford, P.; Davis, M.; Hedges, C.; Klingel, M. Predictors of posttraumatic stress and preferred sources of social support among Canadian paramedics. Cjem 2016, 18, 205–212. [Google Scholar] [CrossRef]
- Blevins, C.A.; Weathers, F.W.; Davis, M.; Witte, T.K.; Domino, J.L. The posttraumatic stress disorder checklist for DSM-5 (PCL-5): Development and initial psychometric evaluation. Journal of Traumatic Stress 2015, 28, 489–498. [Google Scholar] [CrossRef]
- Kroenke, K.; Spitzer, R.L.; Williams, J. The PHQ-9: Validity of a brief depression severity measure. J Gen Intern Med 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.; Löwe, B. A brief measure for assessing generalized anxiety disorder. Arch Intern Med 2006, 1666, 1092–1097. [Google Scholar] [CrossRef]
- Bastien, C.H.; Vallières, A.; Morin, C.M. Validation of the insomnia severity index as an outcome measure for insomnia research. Sleep Medicine 2001, 2, 297–307. [Google Scholar] [CrossRef]
- Saunders, J.B.; Aasland, O.G.; Fabor, T.F.; De La Fuente, J.R.; Grant, M. Development of the alcohol use disorders identification test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption-II. Addiction 1993, 88, 791–804. [Google Scholar] [CrossRef] [PubMed]
- Statistics Canada. Survey on COVID-19 and mental health, February to May 2023. 2023. [Google Scholar]
- Mausz, J.; Donnelly, E.A.; Moll, S.; Harms, S.; McConnell, M. Mental Disorder Symptoms and the Relationship with Resilience among Paramedics in a Single Canadian Site. Int J Environ Res Public Health 2022, 19. [Google Scholar] [CrossRef]
- Wortmann, J.H.; Jordan, A.H.; Weathers, F.W.; Resick, P.A.; Dondanville, K.A.; Hall-Clark, B.; Foa, E.B.; Young-McCaughan, S.; Yarvis, J.S.; Hembree, E.A.; et al. Psychometric analysis of the PTSD Checklist-5 (PCL-5) among treatment-seeking military service members. Psychol Assess 2016, 28, 1392–1403. [Google Scholar] [CrossRef] [PubMed]
- McAlister, F.A. The "number needed to treat" turns 20--and continues to be used and misused. CMAJ 2008, 179, 549–553. [Google Scholar] [CrossRef] [PubMed]
- Vaismoradi, M.; Turunen, H.; Bondas, T. Content analysis and thematic analysis: Implications for conducting a qualitative descriptive study. Nursing and Health Sciences 2013, 15, 398–405. [Google Scholar] [CrossRef]
- Charmaz, K. The logic of grounded theory coding practices and initial coding. In Constructing Grounded Theory, 2nd ed.; Seaman, J., Ed.; Sage Publications: London, 2014; pp. 109–137. [Google Scholar]
- Charmaz, K. Focused coding and beyond. In Constructing Grounded Theory, 2nd ed.; Seaman, J., Ed.; Sage Publications: London, 2014; pp. 138–161. [Google Scholar]
- Singh, J.; Poon, D.E.; Alvarez, E.; Anderson, L.; Verschoor, C.P.; Sutton, A.; Zendo, Z.; Piggott, T.; Apatu, E.; Churipuy, D.; et al. Burnout among public health workers in Canada: a cross-sectional study. BMC Public Health 2024, 24, 48. [Google Scholar] [CrossRef]
- de Wit, K.; Tran, A.; Clayton, N.; Seeburruth, D.; Lim, R.K.; Archambault, P.M.; Chan, T.M.; Rang, L.C.F.; Gray, S.; Ritchie, K.; et al. A Longitudinal Survey on Canadian Emergency Physician Burnout. Annals of emergency medicine 2024, 83, 576–584. [Google Scholar] [CrossRef]
- Gajjar, J.; Pullen, N.; Li, Y.; Weir, S.; Wright, J.G. Impact of the COVID-19 pandemic upon self-reported physician burnout in Ontario, Canada: evidence from a repeated cross-sectional survey. BMJ Open 2022, 12, e060138. [Google Scholar] [CrossRef]
- Sporer, C. Burnout in emergency medical technicians and paramedics in the USA. International Journal of Emergency Services 2021, 10, 366–389. [Google Scholar] [CrossRef]
- Lebeaut, A.; Zegel, M.; Leonard, S.J.; Healy, N.A.; Anderson-Fletcher, E.A.; Vujanovic, A.A. COVID-19-Related Medical Vulnerability and Mental Health Outcomes Among US First Responders. J Occup Environ Med 2023, 65, e283–e289. [Google Scholar] [CrossRef]
- Ebben, R.H.A.; Woensdregt, T.; Wielenga-Meijer, E.; Pelgrim, T.; de Lange, A.; Berben, S.A.A.; Vloet, L.C.M. The impact of COVID-19 on the mental health and well-being of ambulance care professionals: A rapid review. PLoS One 2023, 18, e0287821. [Google Scholar] [CrossRef] [PubMed]
- Soto-Camara, R.; Garcia-Santa-Basilia, N.; Onrubia-Baticon, H.; Cardaba-Garcia, R.M.; Jimenez-Alegre, J.J.; Reques-Marugan, A.M.; Molina-Oliva, M.; Fernandez-Dominguez, J.J.; Matellan-Hernandez, M.P.; Morales-Sanchez, A.; et al. Psychological Impact of the COVID-19 Pandemic on Out-of-Hospital Health Professionals: A Living Systematic Review. J Clin Med 2021, 10. [Google Scholar] [CrossRef] [PubMed]
- Piotrowski, A.; Makarowski, R.; Predoiu, R.; Predoiu, A.; Boe, O. Resilience and Subjectively Experienced Stress Among Paramedics Prior to and During the COVID-19 Pandemic. Front Psychol 2021, 12, 664540. [Google Scholar] [CrossRef]
- Statistics Canada. Survey on COVID-19 and mental health, February to May 2021. 2021. [Google Scholar]
- Shields, R.E.; Teckchandani, T.A.; Asmundson, G.J.G.; Nisbet, J.; Krakauer, R.L.; Andrews, K.L.; Maguire, K.Q.; Jamshidi, L.; Afifi, T.O.; Lix, L.M.; et al. Daily survey participation and positive changes in mental health symptom scores among Royal Canadian Mounted Police Cadets. Front Psychol 2023, 14, 1145194. [Google Scholar] [CrossRef] [PubMed]
- Moghimi, E.; Knyahnytska, Y.; Omrani, M.; Nikjoo, N.; Stephenson, C.; Layzell, G.; Frederic Simpson, A.I.; Alavi, N. Benefits of Digital Mental Health Care Interventions for Correctional Workers and Other Public Safety Personnel: A Narrative Review. Front Psychiatry 2022, 13, 921527. [Google Scholar] [CrossRef] [PubMed]
- Krakauer, R.L.; Stelnicki, A.M.; Carleton, R.N. Examining Mental Health Knowledge, Stigma, and Service Use Intentions Among Public Safety Personnel. Front Psychol 2020, 11, 949. [Google Scholar] [CrossRef]
- Kaur, N.; Ricciardelli, R.; Fletcher, A.; Carleton, R.N. ‘You are safe. You are not alone:’ gender and Social Support Coping (SSC) in public safety personnel. Journal of Gender Studies 2021, 1–16. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; Vaughan, A.D.; Anderson, G.S.; Ricciardelli, R.; MacPhee, R.S.; Cramm, H.A.; Czarnuch, S.; et al. Mental health training, attitudes toward support, and screening positive for mental disorders. Cogn Behav Ther 2019, 49, 1–19. [Google Scholar] [CrossRef]
- Edgelow, M.; Legassick, K.; Novecosky, J.; Fecica, A. Return to Work Experiences of Ontario Public Safety Personnel with Work-Related Psychological Injuries. J Occup Rehabil 2023, 33, 796–807. [Google Scholar] [CrossRef]
| Parameter | All Sites | Peel Region | Essex-Windsor | ||||
| Overall | Men | Women | Overall | Men | Women | ||
| Age (Mean [SD]) | 36.1 (9.1) | 35.9 (8.7) | 36.4 (8.7) | 35.0 (8.6)* | 36.4 (9.8) | 37.6 (10.1) | 34.7 (9.0) |
| Confidential Stream | 588 (59.0) | 422 (62.5) | 246 (36.4) | 172 (25.4) | 166 (51.8) † | 107 (56.0) | 57 (44.5)* |
| Race (White) | 719 (72.9) | 437 (65.4) | 254 (61.8) | 182 (71.3)* | 282 (88.6) † | 162 (85.2) | 120 (93.7)* |
| In a Relationship | 732 (73.5) | 491 (72.8) | 316 (76.3) | 174 (67.4)* | 241 (75.7) | 152 (80.4) | 89 (68.9)* |
| 2SLGBTQI+ | 71 (7.1%) | 48 (7.1) | 19 (4.5) | 27 (10.4)** | 23 (7.2) | 8 (4.2) | 15 (11.6)* |
| Education Certificate Diploma Undergraduate Graduate |
46 (4.6) 583 (58.5) 331 (33.2) 26 (2.6) |
23 (3.4) 340 (50.5) 282 (41.9) 24 (3.5) |
19 (4.6) 218 (52.7) 157 (38.0) 15 (3.6) |
4 (1.5) 121 (46.8) 124 (48) 9 (3.4) |
23 (7.2) 242 (76.3) 49 (15.4) † 2 (0.6) |
14 (7.4) 145 (76.7) 28 (14.8) 1 (0.5) |
9 (7.0) 97 (75.7) 21 (16.4) 1 (0.7) |
| Full-Time Employment | 729 (73.2) | 505 (74.9) | 306 (73.9) | 197 (76.3) | 224 (70.) | 139 (72.7) | 85 (65.8) |
| Current Role Front-Line Leadership CP |
920 (92.4) 56 (5.6) 63 (6.3) |
633 (94) 32 (4.7) 27 (4.0) |
382 (92.4) 26 (6.2) 10 (2.4) |
249 (96.5) 6 (2.3)* 17 (6.5)* |
286 (90.5) 24 (7.6) 36 (113) † |
166 (88.2) 18 (10.7) 18 (9.4) |
120 (93.7) 6 (4.6) 18 (14.2) |
| Clinical Certification PCP ACP |
733 (73.6) 256 (25.7) |
462 (68.6) 211 (31.3) |
264 (63.6) 151 (36.3) |
198 (76.4)** 60 (23.2) |
275 (85.9) 45 (14.0) † |
154 (80.6) 37 (19.3) |
121 (93.7)** 8 (6.2) |
| Experience (Mean [SD]) Recruit Early Career Mid-Career Senior Career |
11 (8.7) 154 (15.5) 167 (16.8) 540 (54.2) 128 (12.9) |
10.4 (8.1) 104 (15.6) 119 (17.8) 372 (55.8) 71 (10.6) |
10.8 (8.2) 57 (13.9) 76 (18.5) 237 (57.8) 40 (9.7) |
9.9 (7.9) 47 (18.3) 43 (16.7) 135 (52.7) 31 (12.1) |
12.1 (9.7) † 50 (15.6) 48 (15.0) 165 (51.6) 57 (17.8) † |
13.0 (10.1) 22 (11.5) 27 (14.1) 102 (53.4) 40 (20.9) |
10.7 (8.9) 28 (21.7) 21 (16.2)* 63 (48.4)* 17 (13.1) |
| Question | All Sites | Peel Region | Essex-Windsor |
| The report was useful in helping you make decisions about your mental health (mean [SD]) | 5.6 (1.1) | 5.5 (1.1) | 5.7 (1.0) |
| The information in the report was consistent with how you felt about your mental health (mean [SD]) | 5.8 (0.9) | 5.9 (0.9) | 5.7 (0.9) |
| Did you access any of the resources provided with your report? (n [%]) | Yes = 30 (13.5%) | Yes = 23 (14.8%) | Yes = 7 (10.6%) |
| Did you contact a mental health professional because of your report? (n [%]) | Yes = 33 (14.9%) | Yes = 24 (15.4%) | Yes = 9 (13.6%) |
| Do you intend to contact a mental health professional in the future because of your report? (n [%]) | Yes = 75 (33.9%) | Yes = 57 (36.7%) | Yes = 18 (27.2%) |
| Theme | N | Description | Sample Quotes |
| Already Receiving Care | 30 | Participant descriptions of existing relationships with practitioners from whom they are accessing mental health care | “(The report) was essentially a confirmation of what I already knew. Fortunately, I have a good therapist I am seeing already” “I shared the report with my current (mental healthcare provider). We discussed it. They agreed with (the content) and how it was representative of where I am with my mental health” “I have been receiving mental health support since our benefits increased. This survey was great. … Thank you for taking care of us.” “I suspected I could benefit from therapy. I have a provider but have not had a session in a while. I have since gone back for regular visits.” |
| Gaining Insight | 16 | Comments from the participants about how the mental health reports provided them actionable insights into their mental health and well-being | “This was very informative and a good self-reflection. Thank you” “Interesting to see what you learn about yourself when you are forced to do some introspection. Maybe some habits aren’t healthy” “As a new paramedic who is just starting her career, I wanted to understand my risk factors and be proactive about my mental health.” “I have been thinking about seeing a professional for some time and this will be one of the things that eventually leads me to it.” “My results informed me that I was at severe risk for insomnia … I (saw) my family doctor. I’m now medicated to help me sleep and I’m feeling clearer every day” “The report was eye opening for me. Despite feeling well mentally, I’ve since been in contact with a psychologist. I’ve also encouraged others to do the same. Thank you for doing this.” |
| Expressing Support for the Research | 29 | Expressions of gratitude and support for the research. Some participants also commented that the survey should be more in-depth or offered regularly as a form of “mental health check-in” |
“Great idea to conduct (this) survey and share its findings with the participants” “Please continue doing this important work” “Thanks so much for looking into our minds, hearts, and souls” “Thank you for improving mental health support in (our service)” “It was a great experience to finally sit down and reflect on my own mental health with some sort of screening tool/assessment and not just wonder what my mental health status might be.” “Thank you for the report. Taken well to heart” “I wish studies like this were regularly conducted in our line of work as the benefits are immeasurable” “I think this would be a good screening tool for all employees to take and have follow-up if needed” |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




