Submitted:
20 February 2026
Posted:
23 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants
2.3. Inclusion and Exclusion Criteria
2.4. Recruitment
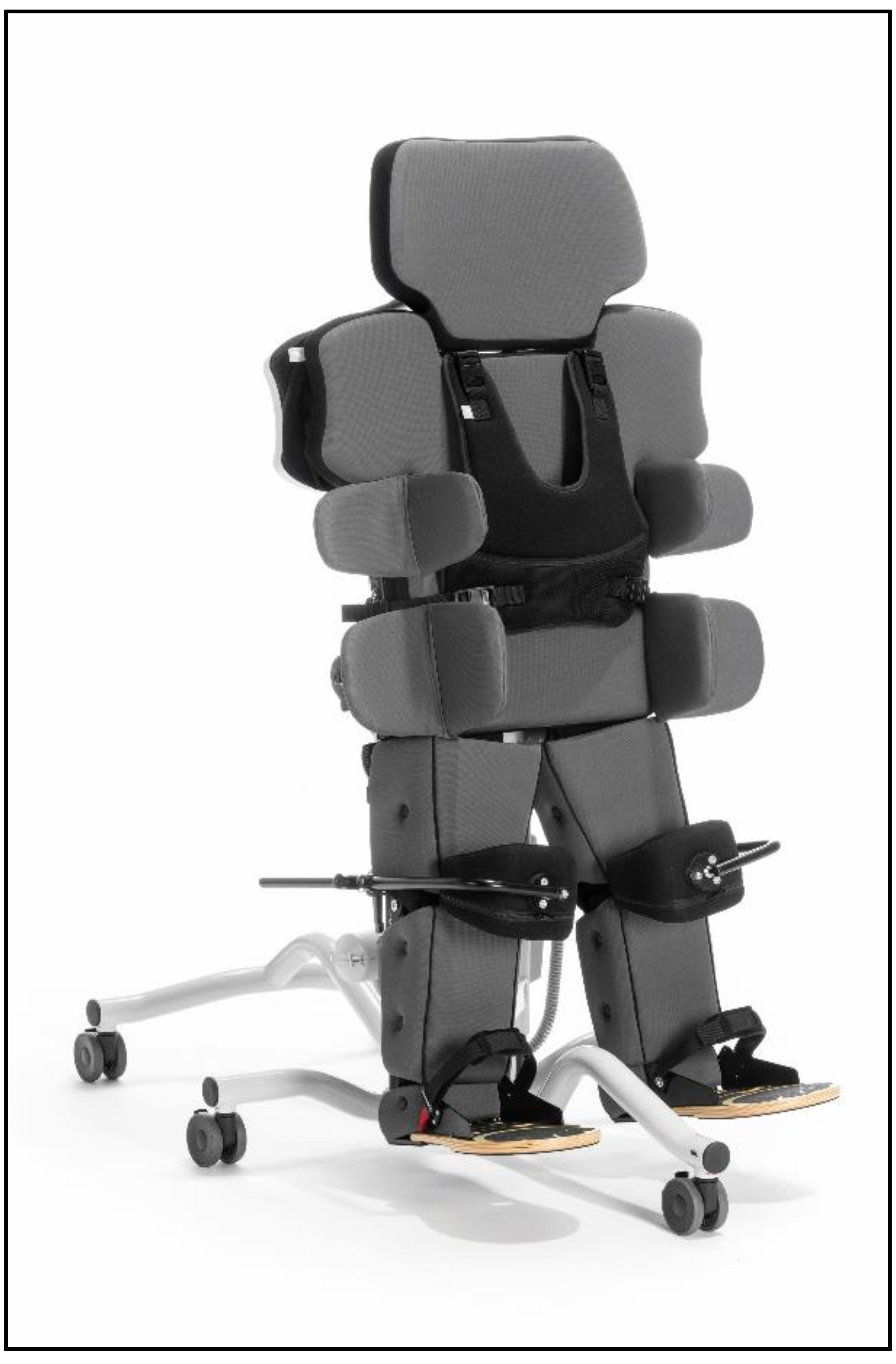
2.5. Equipment and Measurement System
- Verticalization: 0°, 30°, 45°, 60°, 75°, 90°
- Hip/knee flexion: 0°, 15°, 30°, 45°
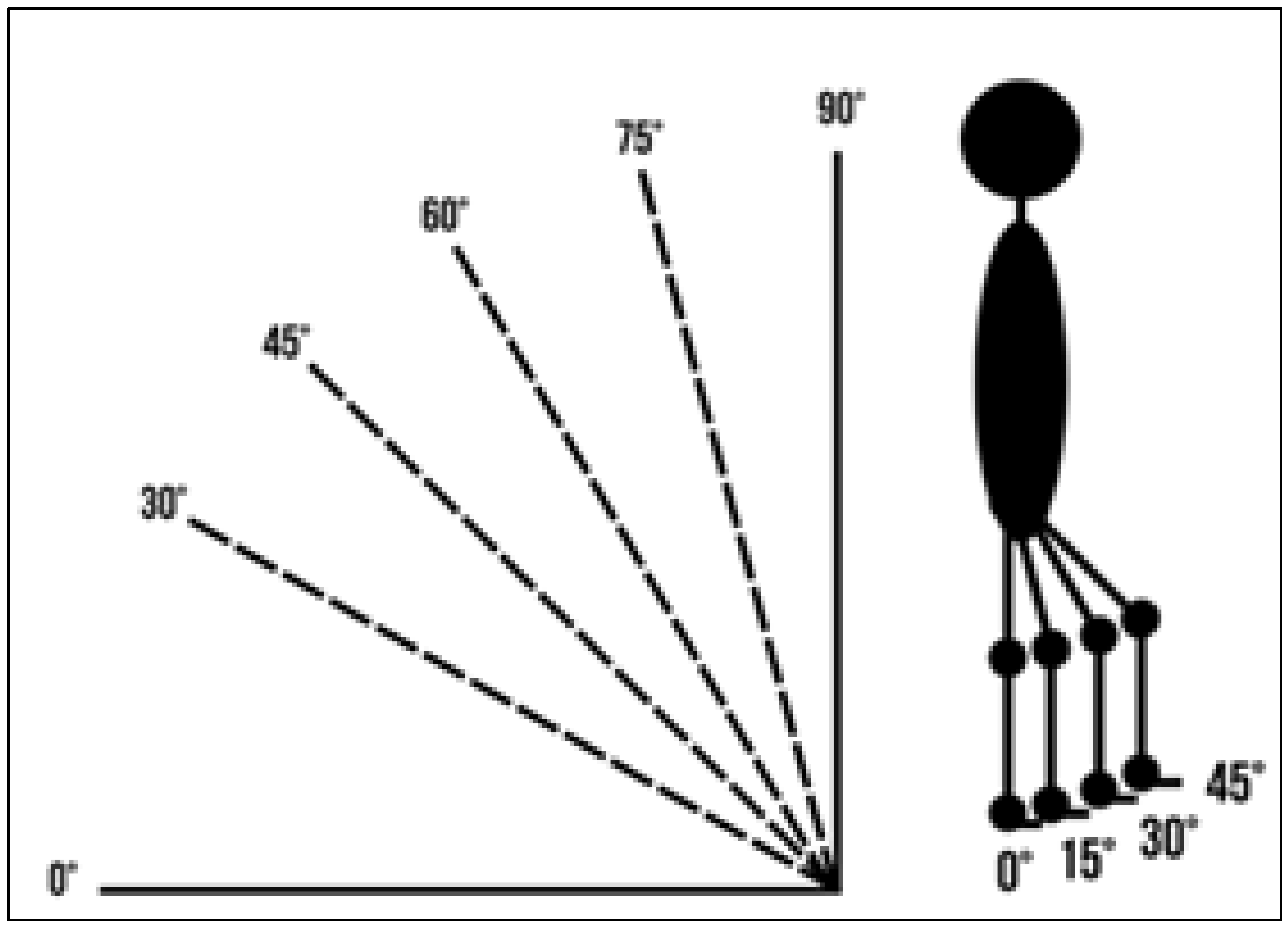

2.6. Procedure
| Position | Hip flexion angle | Knee flexion angle | Verticalization angles |
| 1 | 0° | 0° | 0°, 30°, 45°, 60°, 75°, 90° |
| 2 | 15° | 15° | 0°, 30°, 45°, 60°, 75°, 90° |
| 3 | 30° | 30° | 0°, 30°, 45°, 60°, 75°, 90° |
| 4 | 45° | 45° | 0°, 30°, 45°, 60°, 75°, 90° |
2.7. Data Processing
2.8. Statistical Analysis
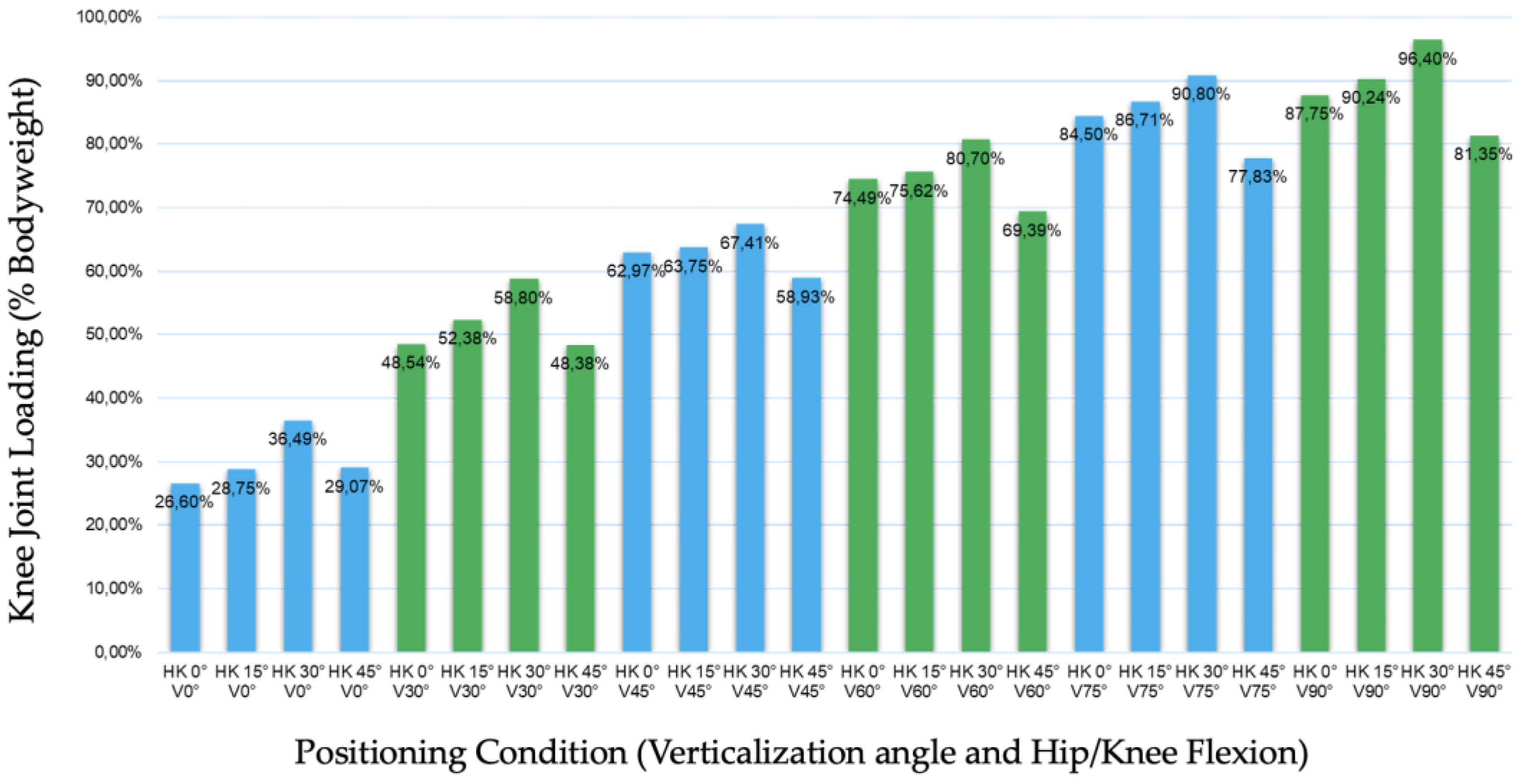
3. Results
4. Discussion
4.1. Clinical Implications
- Children and adolescents with hip/knee flexion contractures were able to achieve clinically meaningful plantar loading within the tested configurations.
- Clinically relevant plantar loading levels (>70% of body weight) were observed at moderate verticalization angles (~60°) in this cohort [3].
- Individual adjustment of the standing system to the child’s anatomical alignment and available range of motion may help optimize plantar loading while supporting safe foot weight-bearing.
- When prescribing and adjusting standing devices, both the achievable verticalization angle and existing movement restrictions should be systematically considered to facilitate effective foot weight-bearing through optimized plantar loading.
4.2. Strengths and Limitations
4.3. Future Research
5. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Vitrikas, K.; Dalton, H.; Breish, D. Cerebral palsy: An overview. Am. Fam. Physician 2020, 101, 213–220. [Google Scholar] [PubMed]
- Caulton, J.M.; Ward, K.A.; Alsop, C.W.; Dunn, G.; Adams, J.E.; Mughal, M.Z. A randomised controlled trial of standing programme on bone mineral density in non-ambulant children with cerebral palsy. Arch. Dis. Child. 2004, 89, 131–135. [Google Scholar] [CrossRef] [PubMed]
- Paleg, G.S.; Smith, B.A.; Glickman, L.B. Systematic review and evidence-based clinical recommendations for dosing of pediatric supported standing programs. Pediatr. Phys. Ther. 2013, 25, 232–247. [Google Scholar] [CrossRef] [PubMed]
- Uddenfeldt Wort, U.; Nordmark, E.; Wagner, P.; Düppe, H.; Westbom, L. Fractures in children with cerebral palsy: A total population study. Dev. Med. Child Neurol. 2013, 55, 821–826. [Google Scholar] [CrossRef] [PubMed]
- Hind, K.; Burrows, M. Weight-bearing exercise and bone mineral accrual in children and adolescents: A review of controlled trials. Bone 2007, 40, 14–27. [Google Scholar] [CrossRef] [PubMed]
- Neuroorthopädie: Disability Management; Strobl, W., Schikora, N., Pitz, E., Abel, C., Eds.; Springer: Berlin, Germany, 2020. [Google Scholar]
- Döderlein, L. Infantile Zerebralparese: Diagnostik, konservative und operative Therapie, 2nd ed.; Springer: Berlin, Germany, 2015. [Google Scholar]
- Kecskemethy, H.H.; Herman, D.; May, R.; Paul, K.; Bachrach, S.J.; Henderson, R.C. Quantifying weight bearing while in passive standers and a comparison of standers. Dev. Med. Child Neurol. 2008, 50, 520–523. [Google Scholar] [CrossRef] [PubMed]
- Herman, D.; May, R.; Vogel, L.; Johnson, J.; Henderson, R.C. Quantifying weight-bearing by children with cerebral palsy while in passive standers. Pediatr. Phys. Ther. 2007, 19, 283–287. [Google Scholar] [CrossRef] [PubMed]
- Paleg, G.; Altizer, W.; Malone, R.; Ballard, K.; Kreger, A. Inclination, hip abduction, orientation, and tone affect weight-bearing in standing devices. J. Pediatr. Rehabil. Med. 2021, 14, 433–441. [Google Scholar] [CrossRef] [PubMed]
- McLean, L.J.; Paleg, G.S.; Livingstone, R.W. Supported-standing interventions for children and young adults with non-ambulant cerebral palsy: A scoping review. Dev. Med. Child Neurol. 2022, 64, 754–772. [Google Scholar] [CrossRef] [PubMed]
- Glickman, L.B.; Geigle, P.R.; Paleg, G.S. A systematic review of supported standing programs. J. Pediatr. Rehabil. Med. 2010, 3, 197–213. [Google Scholar] [CrossRef] [PubMed]
- Hägglund, G.; Lauge-Pedersen, H.; Wagner, P. Characteristics of children with hip displacement in cerebral palsy. BMC Musculoskelet. Disord. 2007, 8, 101. [Google Scholar] [CrossRef] [PubMed]
- Larnert, P.; Risto, O.; Hägglund, G.; Wagner, P. Hip displacement in relation to age and gross motor function in children with cerebral palsy. J. Child. Orthop. 2014, 8, 129–134. [Google Scholar] [CrossRef] [PubMed]
- Novak, I.; Morgan, C.; Fahey, M.; Finch-Edmondson, M.; Galea, C.; Hines, A.; Langdon, K.; Mc Namara, M.; Paton, M.C.B.; Popat, H.; et al. State of the Evidence Traffic Lights 2019: Systematic Review of Interventions for Preventing and Treating Children with Cerebral Palsy. Curr. Neurol. Neurosci. Rep. 2020, 20, 3. [Google Scholar] [CrossRef] [PubMed]
- Paleg, G.S.; Williams, S.A.; Livingstone, R.W. Supported Standing and Supported Stepping Devices for Children with Non-Ambulant Cerebral Palsy: An Interdependence and F-Words Focus. Int. J. Environ. Res. Public Health 2024, 21, 669. [Google Scholar] [CrossRef] [PubMed]
- Martinsson, C.; Himmelmann, K. Effect of weight-bearing in abduction and extension on hip stability in children with cerebral palsy. Pediatr. Phys. Ther. 2011, 23, 150–157. [Google Scholar] [CrossRef] [PubMed]
- Turner, C.; Pavalko, F. Mechanotransduction and functional response of the skeleton to physical stress: The mechanisms and mechanics of bone adaptation. J. Orthop. Sci. 1998, 3, 346–355. [Google Scholar] [CrossRef] [PubMed]




| Inclusion criteria | Exclusion criteria |
| Diagnosis of cerebral palsy (CP) | Other neurological disease |
| GMFCS Level IV or V | GMFCS Level I-III |
| Regular participation in supported standing therapy | Absence of regular standing therapy |
| Age 4-18 years | Age <4 years or > 18 years |
| Lack of compliance or inability to follow study procedures | |
| Botulinum toxin injections to the lower extremities within the previous 6 months | |
| Orthopaedic surgery of the lower extremities within the previous 6 months | |
| Acute illness at the time of assessment | |
| Acute pain affecting standing tolerance or foot weight-bearing |
| Hip/Knee Flexion | Verticalization | Mean (%BW) | SD | 95% CI |
| 0° (n=21) | 0° | 26.60 | 16.14 | 19.25–33.95 |
| 30° | 48.54 | 12.74 | 42.74–54.34 | |
| 45° | 62.97 | 11.86 | 57.57–68.37 | |
| 60° | 74.49 | 14.23 | 68.01–80.97 | |
| 75° | 84.50 | 17.67 | 76.46–92.54 | |
| 90° | 87.79 | 20.56 | 78.43–97.15 | |
| 15° (n=23) | 0° | 28.75 | 13.81 | 22.79–34.71 |
| 30° | 52.38 | 13.33 | 46.62–58.14 | |
| 45° | 63.75 | 13.06 | 58.11–69.39 | |
| 60° | 75.62 | 14.66 | 69.29–81.95 | |
| 75° | 86.71 | 18.56 | 78.69–94.73 | |
| 90° | 90.24 | 17.99 | 82.47–98.01 | |
| 30° (n=23) | 0° | 36.49 | 18.14 | 28.65–44.33 |
| 30° | 58.80 | 16.49 | 51.68–65.92 | |
| 45° | 67.41 | 18.10 | 59.59–75.23 | |
| 60° | 80.70 | 17.86 | 72.98–88.42 | |
| 75° | 90.80 | 17.27 | 83.34–98.26 | |
| 90° | 96.40 | 19.48 | 87.98–104.82 | |
| 45° (n=25) | 0° | 29.07 | 9.08 | 25.32–32.82 |
| 30° | 48.38 | 11.55 | 43.61–53.15 | |
| 45° | 58.93 | 13.25 | 53.46–64.40 | |
| 60° | 69.39 | 17.20 | 62.29–76.49 | |
| 75° | 77.83 | 19.19 | 69.91–85.75 | |
| 90° | 81.35 | 21.65 | 72.41–90.29 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




