Submitted:
28 January 2026
Posted:
29 January 2026
You are already at the latest version
Abstract
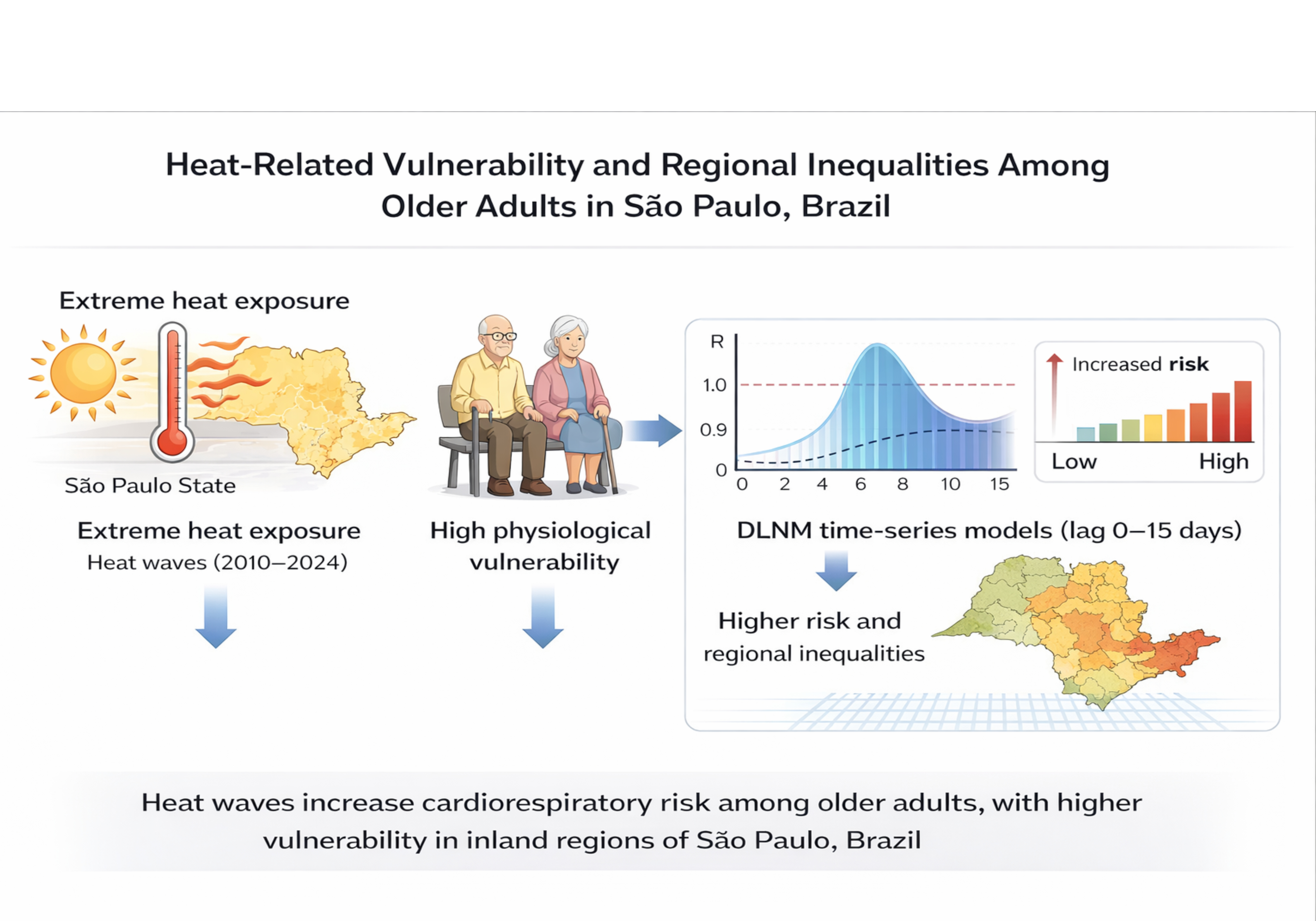
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Ethical Approval
2.2. Study Area and RHDs
2.3. Sociodemographic, Sanitation, and Health System Variables
2.4. Climate Data and Definition of Heat Waves
2.5. Mortality and Hospitalization Data
2.6. Statistical Analysis
2.7. Heat Wave–Health Linkage
2.8. Construction of the Climate Vulnerability Index
2.9. Data Availability, Code, and Use of Artificial Intelligence
3. Results
3.1. Climate Patterns and Heat Wave Occurrence
3.2. Sociodemographic and Health System Context
3.3. Cardiorespiratory Morbidity and Mortality Among Older Adults
3.4. Effect of Heat Waves on Cardiorespiratory Mortality
3.5. Climate Vulnerability Index for Older Adults
4. Discussion
5. Limitations
Ethics Statement
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Meade, R.D.; Akerman, A.P.; Notley, S.R.; McGinn, R.; Poirier, P.; Gosselin, P.; Kenny, G.P. Physiological Factors Characterizing Heat-Vulnerable Older Adults: A Narrative Review. Environ. Int. 2020, 144, 105909. [Google Scholar] [CrossRef]
- Yu, W.; Mengersen, K.; Wang, X.; Ye, X.; Guo, Y.; Pan, X.; Tong, S. Daily Average Temperature and Mortality among the Elderly: A Meta-Analysis and Systematic Review of Epidemiological Evidence. Int. J. Biometeorol. 2012, 56, 569–581. [Google Scholar] [CrossRef]
- Åström, D.O.; Forsberg, B.; Rocklöv, J. Heat Wave Impact on Morbidity and Mortality in the Elderly Population: A Review of Recent Studies. Maturitas 2011, 69, 99–105. [Google Scholar] [CrossRef]
- Liu, J.; Varghese, B.M.; Hansen, A.; Zhang, Y.; Driscoll, T.; Morgan, G.; Dear, K.; Gourley, M.; Capon, A.; Bi, P. Heat Exposure and Cardiovascular Health Outcomes: A Systematic Review and Meta-Analysis. Lancet Planet. Health 2022, 6, e484–e495. [Google Scholar] [CrossRef] [PubMed]
- Cheng, J.; Xu, Z.; Bambrick, H.; Prescott, V.; Wang, N.; Zhang, Y.; Su, H.; Tong, S.; Hu, W. Cardiorespiratory Effects of Heatwaves: A Systematic Review and Meta-Analysis of Global Epidemiological Evidence. Environ. Res. 2019, 177, 108610. [Google Scholar] [CrossRef] [PubMed]
- Climate Change 2014: Impacts, Adaptation, and Vulnerability; Intergovernmental Panel on Climate Change, Ed.; Fifth Assessment Report (AR5), Working Group II; 5th Assessment Report (AR5) – Working Group II.; Field, C. B. Barros, V. R. Dokken, D. J. Mach, K. J. Mastrandrea, M. D. Bilir, T. E. Chatterjee, M. Ebi, K. L. Estrada, Y. O. Genova, R. C. Girma, B. Kissel, E. S. Levy, A. N. MacCracken, S. Mastrandrea, P. R. White, L. L. Cambridge, United Kingdom. 2014; ISBN 978-1-107-05807-1.
- Diniz, F.R.; Gonçalves, F.L.T.; Sheridan, S. Heat Wave and Elderly Mortality: Historical Analysis and Future Projection for Metropolitan Region of São Paulo, Brazil. Atmosphere 2020, 11, 933. [Google Scholar] [CrossRef]
- Silveira, I.H.; Cortes, T.R.; Bell, M.L.; Junger, W.L. Effects of Heat Waves on Cardiovascular and Respiratory Mortality in Rio de Janeiro, Brazil. PLOS ONE 2023, 18, e0283899. [Google Scholar] [CrossRef]
- Paim, J.; Travassos, C.; Almeida, C.; Bahia, L.; Macinko, J. The Brazilian Health System: History, Advances, and Challenges. Lancet Lond. Engl. 2011, 377, 1778–1797. [Google Scholar] [CrossRef]
- Bigoni, A.; Malik, A.M.; Tasca, R.; Carrera, M.B.M.; Schiesari, L.M.C.; Gambardella, D.D.; Massuda, A. Brazil’s Health System Functionality amidst of the COVID-19 Pandemic: An Analysis of Resilience. Lancet Reg. Health Am. 2022, 10, 100222. [Google Scholar] [CrossRef]
- Macinko, J.; Harris, M.J. Brazil’s Family Health Strategy - Delivering Community-Based Primary Care in a Universal Health System. N. Engl. J. Med. 2015, 372, 2177–2181. [Google Scholar] [CrossRef]
- Paschoalotto, MAC; Passador, CS; Passador, JL; Oliveira, LR; Lopes, JEF; Dantas, MK. A Regionalização Do SUS: Proposta de Avaliação de Desempenho Dos Departamentos Regionais de Saúde do Estado de São Paulo [Regionalization of the Brazilian Unified Health System: a performance evaluation proposal for the Regional Health Departments of São Paulo State]. Saúde Soc. São Paulo (in Portuguese). 2018, 27, 80–93. [Google Scholar] [CrossRef]
- de Araújo, C.S.P.; Silva, J.R.I.; Almeida, C.D.G.C. de Total Precipitation and Air Temperature Data Obtained from ERA5-Land Reanalysis: Validation and Accuracy. Rev. Caatinga 2025, 38, e12578–e12578. [Google Scholar] [CrossRef]
- Silva, N. de S.; Alves, J.M.B.; da Silva, E.M.; Sousa, G.M. de Ocorrência de Ondas de Calor com Dados de Reanálises em áreas do Nordeste, Amazônia e Centro-Sudeste do Brasil [Occurrence of heat waves based on reanalysis data in areas of Northeastern, Amazonian and Central-Southeastern Brazil]. Rev. Bras. Meteorol. (in Portuguese). 2023, 37, 441–451. [Google Scholar] [CrossRef]
- Firpo, M.Â.F.; Sansigolo, C.A.; Assis, S.V. de Climatologia e variabilidade sazonal do número de ondas de calor e de frio no Rio Grande do Sul associadas ao ENOS [Climatology and seasonal variability of the number of heat and cold waves in Rio Grande do Sul associated with ENSO]. Rev. Bras. Meteorol. (in Portuguese). 2012, 27, 95–106. [Google Scholar] [CrossRef]
- Saldanha, R. de F.; Bastos, R.R.; Barcellos, C. Microdatasus: pacote para download e pré-processamento de microdados do Departamento de Informática do SUS (DATASUS) [Microdatasus: an R package for downloading and preprocessing microdata from the Brazilian Unified Health System database (DATASUS)]. Cad. Saúde Pública (in Portuguese). 2019, 35, e00032419. [Google Scholar] [CrossRef]
- Gasparrini, A.; Armstrong, B.; Kenward, M.G. Distributed Lag Non-Linear Models. Stat. Med. 2010, 29, 2224–2234. [Google Scholar] [CrossRef]
- Climate Change 2001: Impacts, Adaptation, and Vulnerability.; Contribution of Working Group II to the Third Assessment Report of the Intergovernmental Panel on Climate Change.; Cambridge University Press.: Cambridge, United Kingdom., 2001.
- Estoque, R.C.; Ishtiaque, A.; Parajuli, J.; Athukorala, D.; Rabby, Y.W.; Ooba, M. Has the IPCC’s Revised Vulnerability Concept Been Well Adopted? Ambio 2023, 52, 376–389. [Google Scholar] [CrossRef]
- Pan American Health Organization (PAHO) / World Health Organization (WHO) Mudanças Climáticas e Saúde No Envelhecimento: Desafios e Estratégias Adaptativas [Climate change and health in ageing: challenges and adaptive strategies]; Washington, DC: OPAS/OMS, 2025; (in Portuguese).
- Menezes, J.A.; Confalonieri, U.; Madureira, A.P.; Duval, I. de B.; dos Santos, R.B.; Margonari, C. Mapping Human Vulnerability to Climate Change in the Brazilian Amazon: The Construction of a Municipal Vulnerability Index. PLoS ONE 2018, 13, e0190808. [Google Scholar] [CrossRef]
- Zhao, Q.; Li, S.; Coelho, M.S.Z.S.; Saldiva, P.H.N.; Hu, K.; Arblaster, J.M.; Nicholls, N.; Huxley, R.R.; Abramson, M.J.; Guo, Y. Geographic, Demographic, and Temporal Variations in the Association between Heat Exposure and Hospitalization in Brazil: A Nationwide Study between 2000 and 2015. Environ. Health Perspect. 2019, 127, 017001. [Google Scholar] [CrossRef] [PubMed]
- Kephart, J.L.; Sánchez, B.N.; Moore, J.; Schinasi, L.H.; Bakhtsiyarava, M.; Ju, Y.; Gouveia, N.; Caiaffa, W.T.; Dronova, I.; Arunachalam, S.; et al. City-Level Impact of Extreme Temperatures and Mortality in Latin America. Nat. Med. 2022, 28, 1700–1705. [Google Scholar] [CrossRef]
- Arsad, F.S.; Hod, R.; Ahmad, N.; Ismail, R.; Mohamed, N.; Baharom, M.; Osman, Y.; Radi, M.F.M.; Tangang, F. The Impact of Heatwaves on Mortality and Morbidity and the Associated Vulnerability Factors: A Systematic Review. Int. J. Environ. Res. Public. Health 2022, 19, 16356. [Google Scholar] [CrossRef]
- Fernandez-Medina, R.D.; Peixoto, E.M.; Rodrigues, D.; Said, R.; Holanda, C.A.; Freire, C. da S.; de Almeida, A.M.; de Carvalho Cardoso, S.C.; Sergio Ribeiro, M.; de Mello, C.M.B.; et al. Excess Mortality Associated with Extreme Heat in Rio de Janeiro, Brazil, 2023. Rev. Panam. Salud Pública 2025, 49, e76. [Google Scholar] [CrossRef] [PubMed]
- Xu, R.; Zhao, Q.; Coelho, M.S.Z.S.; Saldiva, P.H.N.; Abramson, M.J.; Li, S.; Guo, Y. Socioeconomic Inequality in Vulnerability to All-Cause and Cause-Specific Hospitalisation Associated with Temperature Variability: A Time-Series Study in 1814 Brazilian Cities. Lancet Planet. Health 2020, 4, e566–e576. [Google Scholar] [CrossRef] [PubMed]
- dos Santos, D.M.; Libonati, R.; Garcia, B.N.; Geirinhas, J.L.; Salvi, B.B.; Silva, E.L. e; Rodrigues, J.A.; Peres, L.F.; Russo, A.; Gracie, R.; et al. Twenty-First-Century Demographic and Social Inequalities of Heat-Related Deaths in Brazilian Urban Areas. PLOS ONE 2024, 19, e0295766. [Google Scholar] [CrossRef]
- Gronlund, C.J. Racial and Socioeconomic Disparities in Heat-Related Health Effects and Their Mechanisms: A Review. Curr. Epidemiol. Rep. 2014, 1, 165–173. [Google Scholar] [CrossRef]
- Neves, J.M.; Garcia, K.K.S.; Oliveira, B.F.A.; Horta, M.A. Too Hot to Ignore: The Escalating Health Impact of Heatwaves in Brazil. Int. J. Environ. Res. Public. Health 2025, 22, 1451. [Google Scholar] [CrossRef]
- Watts, N.; Adger, W.N.; Agnolucci, P.; Blackstock, J.; Byass, P.; Cai, W.; Chaytor, S.; Colbourn, T.; Collins, M.; Cooper, A.; et al. Health and Climate Change: Policy Responses to Protect Public Health. The Lancet 2015, 386, 1861–1914. [Google Scholar] [CrossRef]
- Deering, S. Clinical Public Health, Climate Change, and Aging. Can. Fam. Physician 2023, 69, 233–235. [Google Scholar] [CrossRef] [PubMed]
- Berry, P.; Enright, P.M.; Shumake-Guillemot, J.; Villalobos Prats, E.; Campbell-Lendrum, D. Assessing Health Vulnerabilities and Adaptation to Climate Change: A Review of International Progress. Int. J. Environ. Res. Public. Health 2018, 15, 2626. [Google Scholar] [CrossRef]
- Ansah, E.W.; Amoadu, M.; Obeng, P.; Sarfo, J.O. Health Systems Response to Climate Change Adaptation: A Scoping Review of Global Evidence. BMC Public Health 2024, 24, 2015. [Google Scholar] [CrossRef]
| RHDs | Proportion of older adults (60 years, %) | Mean HDI | Water supply coverage (%) | Sewerage coverage (%) | Primary care coverage (%) ¹ | Health human resources index² | Per capita public health expenditure index³ |
|---|---|---|---|---|---|---|---|
| I – Greater São Paulo | 16 | 0.760 | 98.5 | 94.0 | 2.27 | 1.26 | 2.73 |
| II – Araçatuba | 19 | 0.740 | 95.0 | 92.6 | 2.98 | 3.09 | 2.71 |
| III – Araraquara | 17.8 | 0.743 | 95.1 | 95.0 | 2.36 | 3.00 | 2.79 |
| IV – Baixada Santista | 18.7 | 0.759 | 91.7 | 77.2 | 1.87 | 3.09 | 3.24 |
| V – Barretos | 18.2 | 0.742 | 97.9 | 97.8 | 2.60 | 3.23 | 2.78 |
| VI – Bauru | 17.8 | 0.732 | 95.5 | 93.5 | 2.41 | 3.03 | 2.41 |
| VII – Campinas | 17.1 | 0.757 | 95.4 | 91.1 | 2.32 | 2.81 | 3.18 |
| VIII – Franca | 17 | 0.737 | 97.7 | 97.4 | 3.06 | 3.38 | 2.35 |
| IX – Marília | 19.2 | 0.736 | 95.2 | 94.2 | 2.76 | 2.86 | 2.67 |
| X – Piracicaba | 17.4 | 0.756 | 96.7 | 96.2 | 2.45 | 3.24 | 2.75 |
| XI – Presidente Prudente | 19.6 | 0.736 | 93.1 | 90.4 | 3.23 | 3.39 | 2.44 |
| XII – Registro | 20.6 | 0.703 | 75.1 | 62.9 | 2.79 | 2.63 | 2.74 |
| XIII – Ribeirão Preto | 16.6 | 0.743 | 97.3 | 96.7 | 2.34 | 3.03 | 2.74 |
| XIV – São João da Boa Vista | 19.1 | 0.747 | 95.2 | 92.8 | 2.27 | 2.53 | 2.75 |
| XV – São José do Rio Preto | 20.1 | 0.743 | 96.0 | 94.0 | 2.90 | 2.27 | 2.63 |
| XVI – Sorocaba | 16.7 | 0.717 | 91.2 | 81.8 | 2.23 | 3.02 | 2.51 |
| XVII – Taubaté | 17.2 | 0.735 | 94.1 | 88.7 | 2.33 | 2.42 | 2.85 |
| RHDs | CV hospitalizations (x 1,000) | Respiratory hospitalizations (x 1,000) | CV deaths (x 1,000) | Respiratory deaths (x 1,000) |
|---|---|---|---|---|
| I – Greater São Paulo | 397.5 | 206.2 | 290.3 | 141.6 |
| II – Araçatuba | 21.7 | 22.7 | 9.1 | 7.7 |
| III – Araraquara | 22.4 | 16.0 | 10.0 | 7.0 |
| IV – Baixada Santista | 26.9 | 15.0 | 33.6 | 13.7 |
| V – Barretos | 10.0 | 11.1 | 5.5 | 4.1 |
| VI – Bauru | 47.6 | 40.5 | 22.5 | 16.3 |
| VII – Campinas | 78.5 | 63.9 | 52.1 | 33.6 |
| VIII – Franca | 15.0 | 14.0 | 8.6 | 6.2 |
| IX – Marília | 38.2 | 31.2 | 16.3 | 10.7 |
| X – Piracicaba | 23.0 | 14.8 | 16.2 | 11.2 |
| XI – Presidente Prudente | 27.9 | 21.1 | 10.8 | 7.5 |
| XII – Registro | 5.7 | 4.2 | 4.2 | 2.2 |
| XIII – Ribeirão Preto | 36.7 | 28.9 | 17.2 | 11.7 |
| XIV – São João da Boa Vista | 25.6 | 23.8 | 12.7 | 8.1 |
| XV – São José do Rio Preto | 58.6 | 51.9 | 21.4 | 17.5 |
| XVI – Sorocaba | 47.6 | 47.3 | 28.5 | 19.9 |
| XVII – Taubaté | 54.9 | 33.6 | 26.4 | 17.5 |
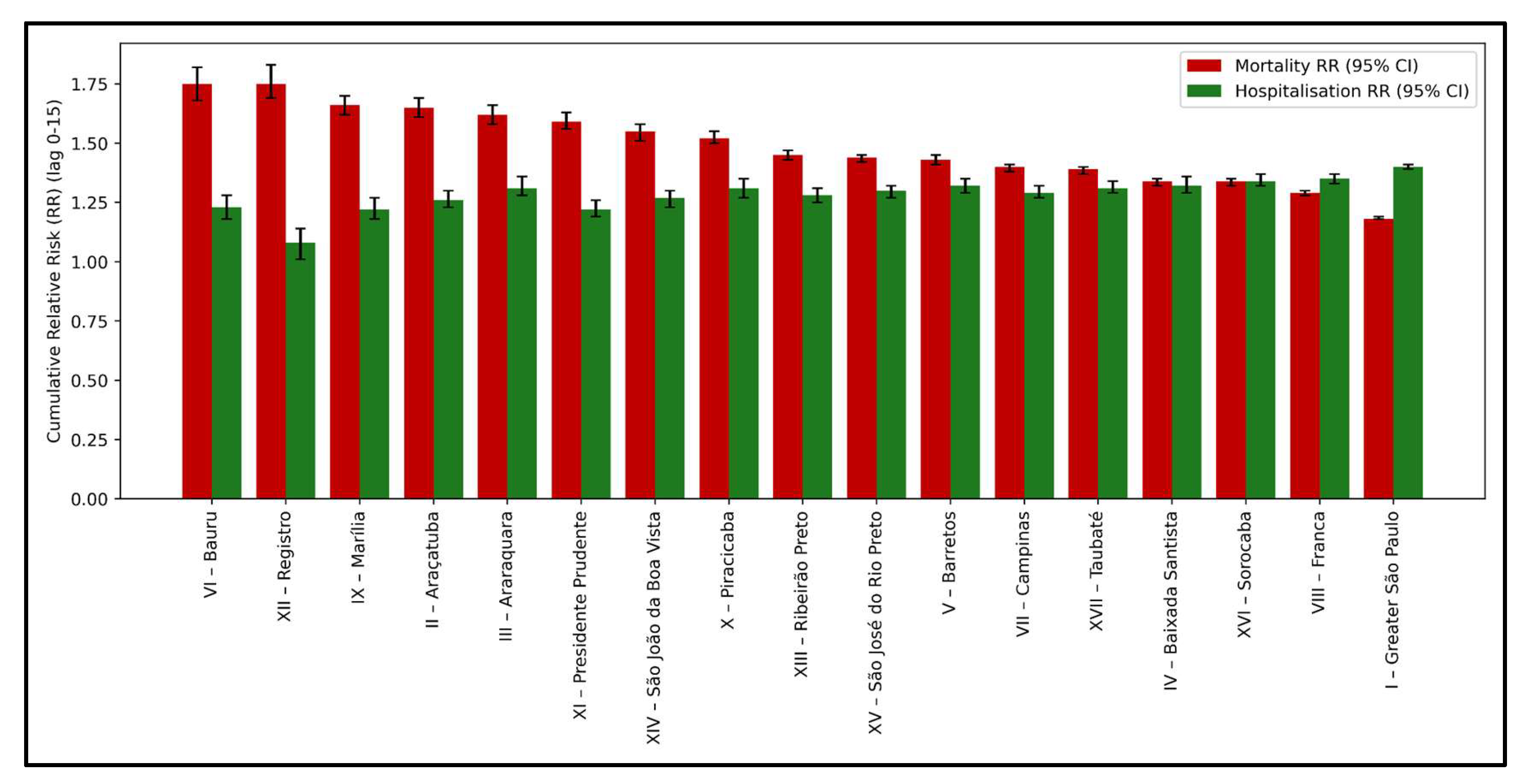
| RHDs | Mortality RR (95% CI) | Hospitalization RR (95% CI) |
|---|---|---|
| I – Greater São Paulo | 1.18 (1.18–1.19) | 1.40 (1.39–1.41) |
| II – Araçatuba | 1.65 (1.61–1.69) | 1.26 (1.23–1.30) |
| III – Araraquara | 1.62 (1.58–1.66) | 1.31 (1.28–1.36) |
| IV – Baixada Santista | 1.34 (1.32–1.35) | 1.32 (1.29–1.36) |
| V – Barretos | 1.43 (1.41–1.45) | 1.32 (1.29–1.35) |
| VI – Bauru | 1.75 (1.68–1.82) | 1.23 (1.18–1.28) |
| VII – Campinas | 1.40 (1.38–1.41) | 1.29 (1.27–1.32) |
| VIII – Franca | 1.29 (1.28–1.30) | 1.35 (1.33–1.37) |
| IX – Marília | 1.66 (1.62–1.70) | 1.22 (1.18–1.27) |
| X – Piracicaba | 1.52 (1.50–1.55) | 1.31 (1.27–1.35) |
| XI – Presidente Prudente | 1.59 (1.56–1.63) | 1.22 (1.19–1.26) |
| XII – Registro | 1.75 (1.69–1.83) | 1.08 (1.01-1.14) |
| XIII – Ribeirão Preto | 1.45 (1.43–1.47) | 1.28 (1.25–1.31) |
| XIV – São João da Boa Vista | 1.55 (1.51–1.58) | 1.27 (1.23–1.30) |
| XV – São José do Rio Preto | 1.44 (1.42–1.45) | 1.30 (1.27–1.32) |
| XVI – Sorocaba | 1.34 (1.32–1.35) | 1.34 (1.32–1.37) |
| XVII – Taubaté | 1.39 (1.37–1.40) | 1.31 (1.29–1.34) |
| RHD | Sensitivity (0.65) ¹ | Adaptive Capacity (0.35) ² | Index³ | Classification |
|---|---|---|---|---|
| I Greater São Paulo | 0.25 | 0.136 | 0.386 | Low |
| II Araçatuba | 0.44 | 0.088 | 0.528 | High |
| III Araraquara | 0.43 | 0.118 | 0.548 | High |
| IV Baixada Santista | 0.34 | 0.148 | 0.488 | Moderate |
| V Barretos | 0.37 | 0.086 | 0.456 | Low |
| VI Bauru | 0.42 | 0.142 | 0.562 | High |
| VII Campinas | 0.29 | 0.097 | 0.39 | Low |
| VIII Franca | 0.28 | 0.087 | 0.367 | Low |
| IX Marília | 0.42 | 0.113 | 0.533 | High |
| X Piracicaba | 0.37 | 0.087 | 0.457 | Low |
| XI Presidente Prudente | 0.40 | 0.088 | 0.488 | Moderate |
| XII Registro | 0.40 | 0.257 | 0.657 | High |
| XIII Ribeirão Preto | 0.29 | 0.116 | 0.406 | Low |
| XIV São João da Boa Vista | 0.41 | 0.133 | 0.543 | High |
| XV São José do Rio Preto | 0.42 | 0.103 | 0.522 | Moderate |
| XVI Sorocaba | 0.29 | 0.203 | 0.493 | Moderate |
| XVII Taubaté | 0.31 | 0.154 | 0.464 | Moderate |
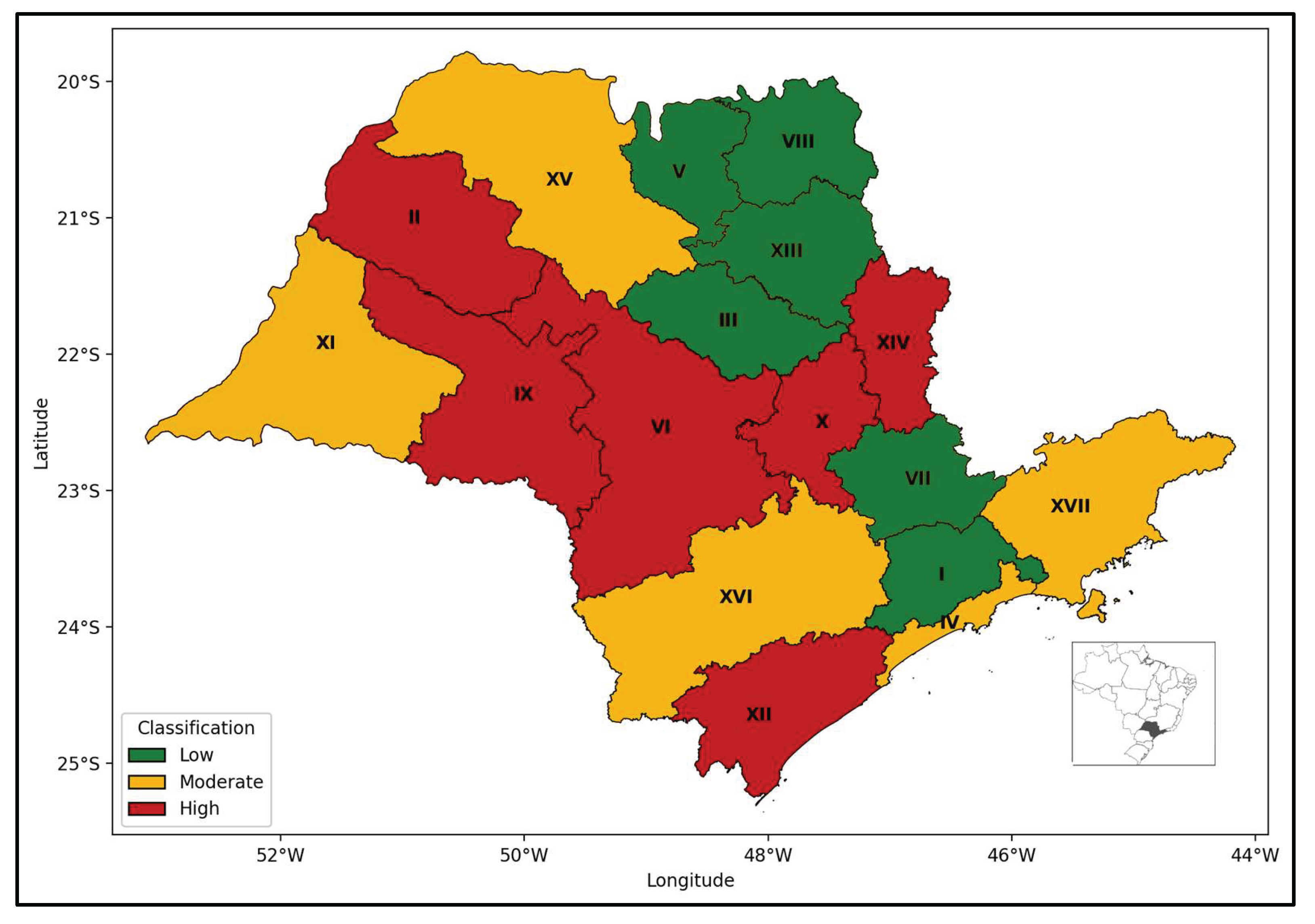
| Vulnerability category | Index range | Count of RHDs (%) |
RHDs |
|---|---|---|---|
| Low | ≤ 0.459 | 6 (35.3%) | Greater São Paulo,Campinas, Franca, Piracicaba, Ribeirão Preto, Barretos |
| Moderate | > 0.459–≤ 0.526 | 5 (29.4%) | Baixada Santista, Presidente Prudente, São José do Rio Preto, Sorocaba, Taubaté |
| High | > 0.526 | 6 (35.3%) | Araçatuba, Araraquara, Bauru, Marília, São João da Boa Vista, Registro |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





