Submitted:
23 January 2026
Posted:
26 January 2026
You are already at the latest version
Abstract

Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Data Source
2.3. Case Ascertainment and Clinical Meaning of ICD-10 Codes
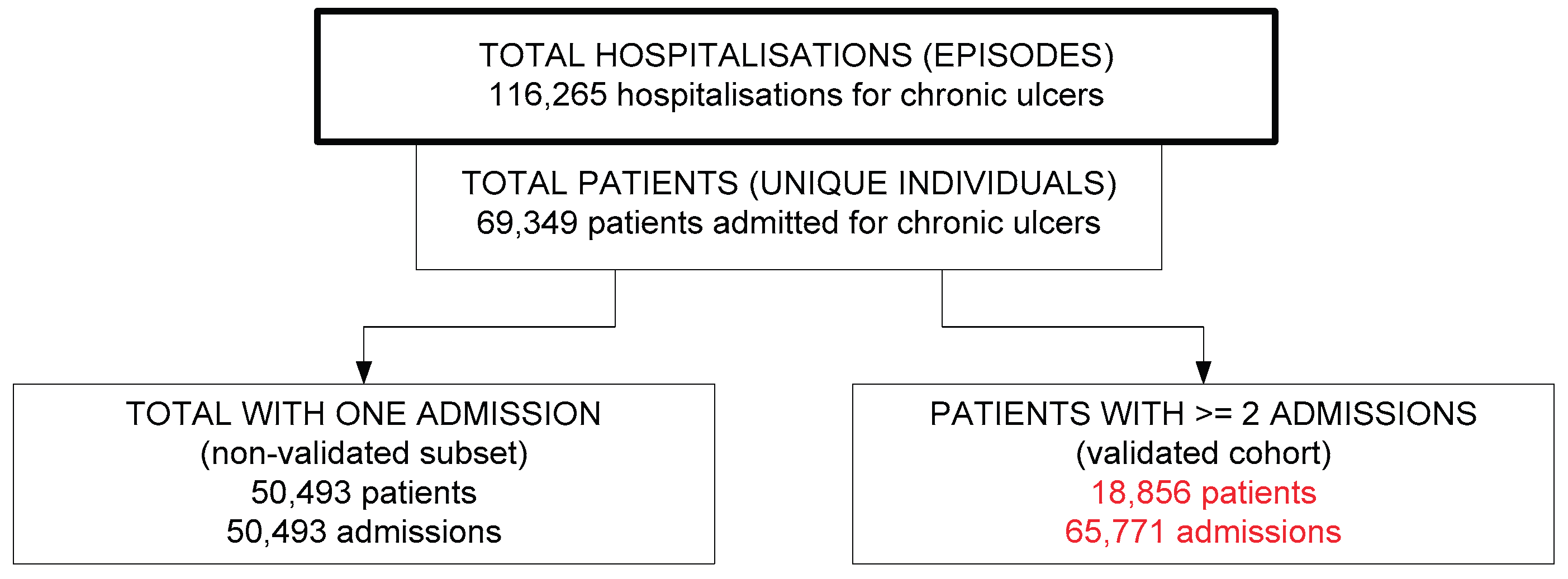
2.4. Validation of Chronicity (≥2 Hospitalisations)
2.5. Handling of Changing Diagnoses Across Admissions
2.6. Outcomes and Epidemiological Definitions
2.7. Statistical Analysis
2.8. Ethical Standards
3. Results
3.1. Study Population, Diagnosis Validation
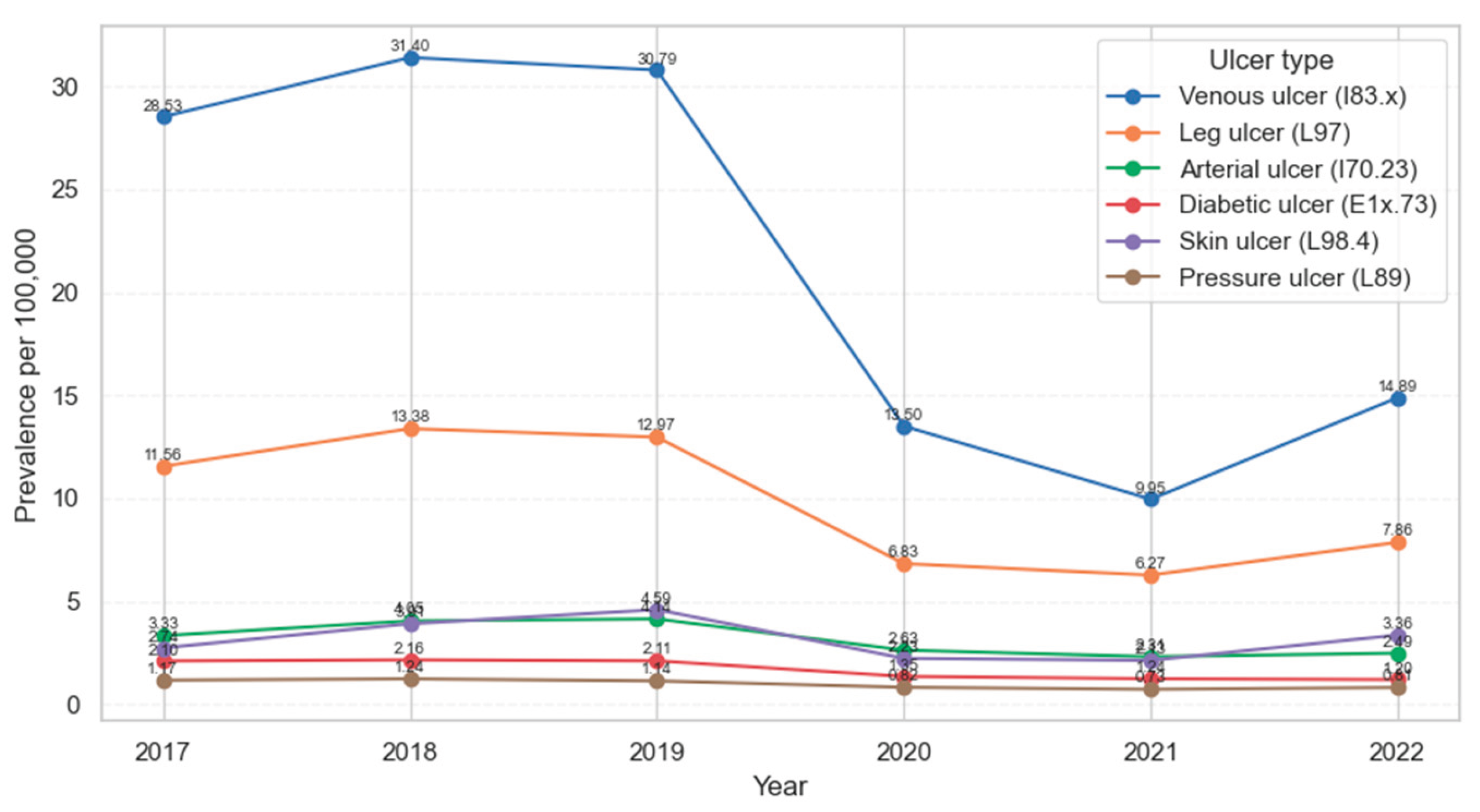
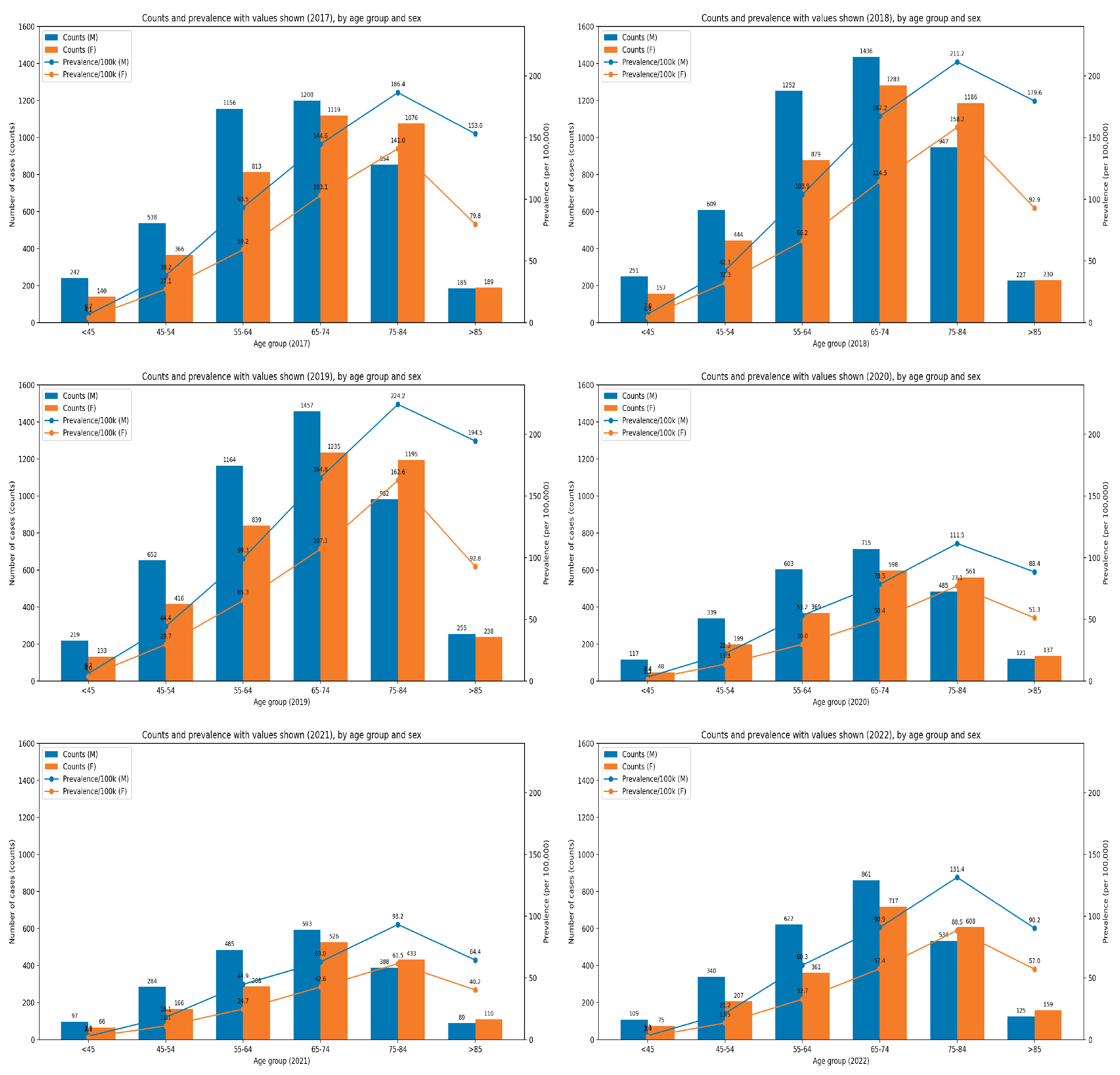
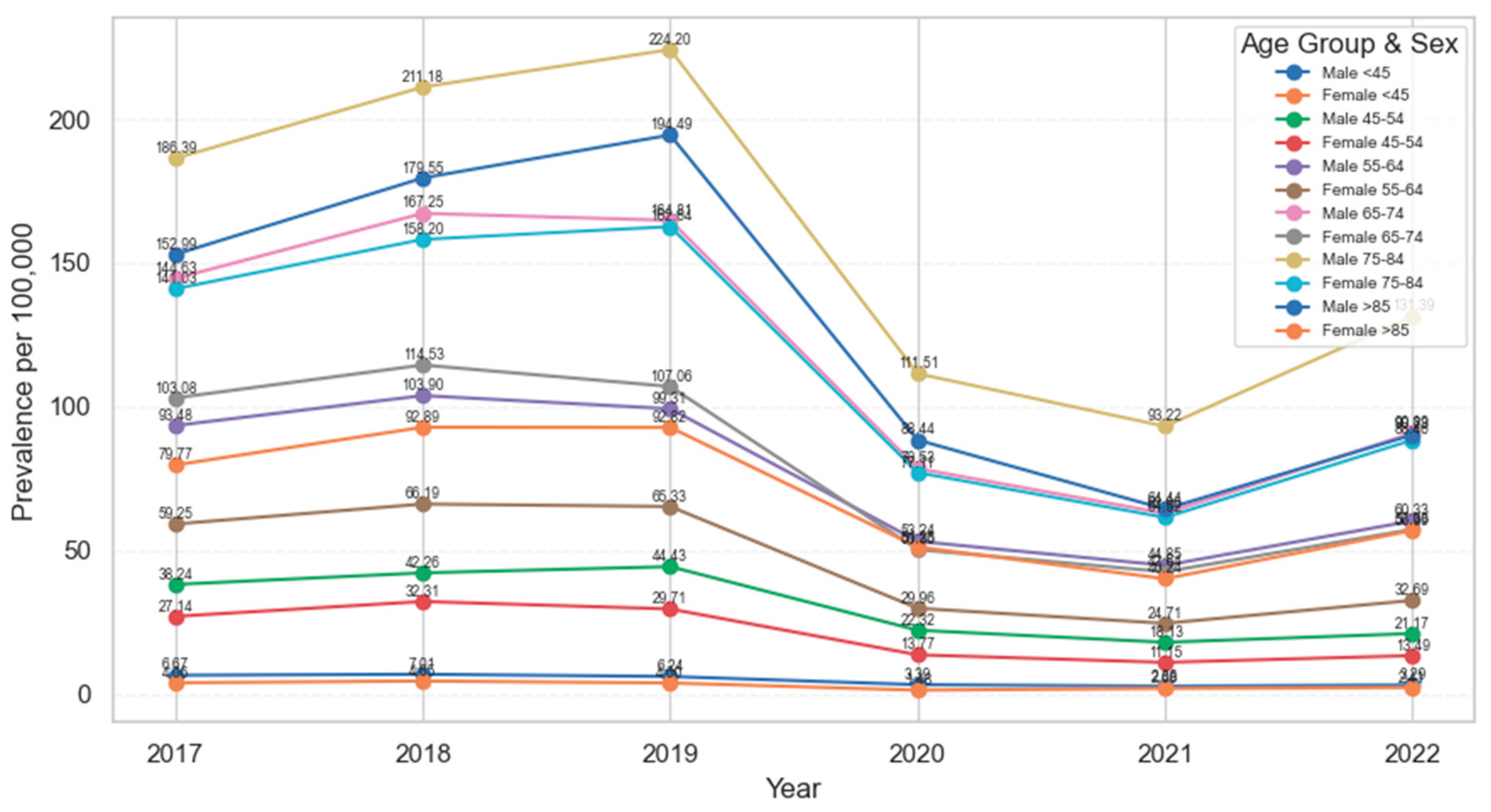
3.2. Epidemiological Study
3.3. Statistical Precision and Robustness of Estimates
4. Discussion
4.1. Key Results
4.2. Interpretation
4.3. Clinical Implications
4.4. Limitations
4.5. Generalizability
5. Conclusions
Acknowledgments
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Nussbaum, S.R.; Carter, M.J.; Fife, C.E.; DaVanzo, J.; Haught, R.; Nusgart, M.; et al. An Economic Evaluation of the Impact, Cost, and Medicare Policy Implications of Chronic Nonhealing Wounds. Value Health 2018, 21, 27–32. [Google Scholar] [CrossRef] [PubMed]
- Sen, C.K. Human Wound and Its Burden: Updated 2022 Compendium of Estimates. Adv. Wound Care 2023, 12, 657–670. [Google Scholar] [CrossRef] [PubMed]
- Maheshwari, G.; Gupta, S.; Sagar, S.; Tripathi, S.; Kisaka, T. Chronic Wounds: Magnitude, Socioeconomic Burden and Consequences. Wounds Asia 2021, 4, 8–14. [Google Scholar]
- Frykberg, R.G.; Banks, J. Challenges in the Treatment of Chronic Wounds. Adv. Wound Care 2015, 4, 560–582. [Google Scholar] [CrossRef]
- Kolimi, P.; Narala, S.; Nyavanandi, D.; Youssef, A.A.A.; Dudhipala, N. Innovative Treatment Strategies to Accelerate Wound Healing: Trajectory and Recent Advancements. Cells 2022, 11, 2439. [Google Scholar] [CrossRef]
- Herberger, K.; Rustenbach, S.J.; Grams, L.; Münter, K.C.; Schäfer, E.; Augustin, M. Quality-of-care for leg ulcers in the metropolitan area of Hamburg – a community-based study. J. Eur. Acad. Dermatol. Venereol. 2012, 26, 495–502. [Google Scholar] [CrossRef]
- Ţânţu, M.; Belu, E.; Bobescu, E.; Armean, S.M.; Armean, P.; Constantin, M.M.; Domnariu, C.D. Role of angiotensin converting enzyme (ACE) inhibitors in hypertension and cardiovascular protection management. Farmacia 2014, 62(3), 443–451. Available online: https://farmaciajournal.com/issue-articles/role-of-angiotensin-converting-enzyme-ace-inhibitors-in-hypertension-and-cardiovascular-protection-management.
- Guest, J.F.; Ayoub, N.; McIlwraith, T.; Uchegbu, I.; Gerrish, A.; Weidlich, D.; et al. Health economic burden that different wound types impose on the UK’s National Health Service. Int. Wound J. 2017, 14, 322–330. [Google Scholar] [CrossRef] [PubMed]
- Zorge, N.E.; Scheerders, E.R.Y.; Dudink, K.; Oudshoorn, C.; Polinder-Bos, H.A.; Waalboer-Spuij, R.; et al. A prospective, multicentre study to assess frailty in elderly patients with leg ulcers (GERAS study). J. Eur. Acad. Dermatol. Venereol. 2023, 37, 428–435. [Google Scholar] [CrossRef]
- Kreft, D.; Keiler, J.; Grambow, E.; Kischkel, S.; Wree, A.; Doblhammer, G. Prevalence and Mortality of Venous Leg Diseases of the Deep Veins: An Observational Cohort Study Based on German Health Claims Data. Angiology 2020, 71, 452–464. [Google Scholar] [CrossRef]
- Järbrink, K.; Ni, G.; Sönnergren, H.; Schmidtchen, A.; Pang, C.; Bajpai, R.; et al. Prevalence and incidence of chronic wounds and related complications: A protocol for a systematic review. Syst. Rev. 2016, 5, 152. [Google Scholar] [CrossRef]
- Furtunescu, F.; Minca, D.G.; Vasile, A.; Domnariu, C. Alcohol consumption impact on premature mortality in Romania. Rom. J. Leg. Med. 2009, 17(4), 296–302. [Google Scholar] [CrossRef]
- Domnariu, C.; Andreea, I.; Furtunescu, F. Influence of family modelling on children’s healthy eating behaviour. Rev. Cercet. Interv. Soc. 2013, 41, 77–95. Available online: https://www.rcis.ro/en/section1/84-volumul-412013iunie/904-influence-of-family-modelling-on-childrens-healthy-eating-behaviour.html.
- Heyer, K.; Herberger, K.; Protz, K.; Glaeske, G.; Augustin, M. Epidemiology of chronic wounds in Germany: Analysis of statutory health insurance data. Wound Repair Regen. 2016, 24, 434–442. [Google Scholar] [CrossRef]
- Berenguer Pérez, M.; López-Casanova, P.; Sarabia Lavín, R.; González De La Torre, H.; Verdú-Soriano, J. Epidemiology of venous leg ulcers in primary health care: Incidence and prevalence in a health centre—A time series study (2010–2014). Int. Wound J. 2019, 16, 256–265. [Google Scholar] [CrossRef] [PubMed]
- Díaz-Herrera, M.Á.; Martínez-Riera, J.R.; Verdú-Soriano, J.; Capillas-Pérez, R.M.; Pont-García, C.; Tenllado-Pérez, S.; et al. Multicentre Study of Chronic Wounds Point Prevalence in Primary Health Care in the Southern Metropolitan Area of Barcelona. J. Clin. Med. 2021, 10, 797. [Google Scholar] [CrossRef] [PubMed]
- Furtado, K.A.X.; Infante, P.; Sobral, A.; Gaspar, P.; Eliseu, G.; Lopes, M. Prevalence of acute and chronic wounds – with emphasis on pressure ulcers – in integrated continuing care units in Alentejo, Portugal. Int. Wound J. 2020, 17, 1002–1010. [Google Scholar] [CrossRef]
- Probst, S.; Saini, C.; Gschwind, G.; Stefanelli, A.; Bobbink, P.; Pugliese, M.; et al. Prevalence and incidence of venous leg ulcers—A systematic review and meta-analysis. Int. Wound J. 2023, 20, 3906–3921. [Google Scholar] [CrossRef] [PubMed]
- Margolis, D.J.; Bilker, W.; Santanna, J.; Baumgarten, M. Venous leg ulcer: Incidence and prevalence in the elderly. J. Am. Acad. Dermatol. 2002, 46, 381–386. [Google Scholar] [CrossRef]
- Homs-Romero, E.; Romero-Collado, A.; Verdú, J.; Blanch, J.; Rascón-Hernán, C.; Martí-Lluch, R. Validity of Chronic Venous Disease Diagnoses and Epidemiology Using Validated Electronic Health Records From Primary Care: A Real-World Data Analysis. J. Nurs. Scholarsh. 2021, 53, 296–305. [Google Scholar] [CrossRef]
- Bondor, C.I.; Veresiu, I.A.; Florea, B.; Vinik, E.J.; Vinik, A.I.; Gavan, N.A. Epidemiology of Diabetic Foot Ulcers and Amputations in Romania: Results of a Cross-Sectional Quality of Life Questionnaire Based Survey. J. Diabetes Res. 2016, 2016, 5439521. [Google Scholar] [CrossRef]
- Feodor, T.; Baila, S.; Mitea, I.A.; Branisteanu, D.E.; Vittos, O. Epidemiology and clinical characteristics of chronic venous disease in Romania. Exp. Ther. Med. 2019, 17, 1097–1105. [Google Scholar] [CrossRef]
- Sima, D.I.; Bondor, C.I.; Vereşiu, I.A.; Gâvan, N.A.; Borzan, C.M. Hospitalisation Costs of Lower Limb Ulcerations and Amputations in Patients with Diabetes in Romania. Int. J. Environ. Res. Public Health 2021, 18, 2230. [Google Scholar] [CrossRef]
- Taroi, M.; Gligorea, I.; Fleacă, R.; Vecerzan, L.; Prihoi, A.; Domnariu, C.D. Profiling Patients with Chronic Ulcers Using K-Means Clustering and Analysis of the Impact on the Consumption of Medical Resources: Retrospective Study on Hospitalised Patients in Romania. J. Clin. Med. 2025, 14, 6252. [Google Scholar] [CrossRef]
- Rusu, E.; Coman, H.; Coșoreanu, A.; Militaru, A.M.; Popescu-Vâlceanu, H.C.; Teodoru, I.; et al. Incidence of Lower Extremity Amputation in Romania: A Nationwide 5-Year Cohort Study, 2015–2019. Medicina 2023, 59, 1199. [Google Scholar] [CrossRef] [PubMed]
- Mihaila, R.G.; Nedelcu, L.; Fratila, O.; Retzler, L.; Domnariu, C.; Cipaian, R.C.; Rezi, E.C.; Beca, C.; Deac, M. Effects of simvastatin in patients with viral chronic hepatitis C. Hepato-gastroenterology 2011, 58, 1296–1300. [Google Scholar] [CrossRef]
- Tanasescu, D.; Sabau, D.; Moisin, A.; Gherman, C.; Fleaca, R.; Bacila, C.; et al. Risk assessment of amputation in patients with diabetic foot. Exp. Ther. Med. 2023, 25, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Ion, N.; Fleaca, S.; Bocea, B.A.; Mohor, C.; Roman, M.; Alexandru-Florin, D.; et al. Key factors influencing orthopaedic operating room contamination: Impact of human activity and Staphylococcus epidermidis prevalence. J. Exp. Orthop. 2025, 12. [Google Scholar] [CrossRef]
- World Health Organization. International Statistical Classification of Diseases and Related Health Problems (10th Revision) - ICD-10 Version:2019. Available online: https://icd.who.int/browse10/2019/en.
- Centers for Disease Control and Prevention (CDC). Principles of Epidemiology in Public Health Practice, 3rd ed.; An Introduction to Applied Epidemiology and Biostatistics; U.S. Department of Health and Human Services: Atlanta, GA, USA, 2006; Available online: https://www.cdc.gov/csels/dsepd/ss1978/lesson3/index.html.
- Association of Schools of Public Health in the European Region (ASPHER). How to Count Illness, 2021, Second Edition. Available online: https://www.aspher.org.
- National Institute of Statistics (INSSE). TEMPO-Online Time Series: POP105A — Resident Population on 1 January by Age and Sex. Available online: http://statistici.insse.ro/tempoins/index.jsp?page=tempo3&lang=ro&ind=POP105A.
- National Institute of Statistics (INSSE). TEMPO-Online Time Series: POP106A — Resident Population on 1 July by Age and Sex. Available online: http://statistici.insse.ro/tempoins/index.jsp?page=tempo3&lang=ro&ind=POP106A.
- F. Vladu, A.; Badau, D.; Daina, L.G.; Domnariu, H.P.; Daina, C.M. Importance of hospital performance indicators in contracting and financing medical services in surgical wards. Cureus 2024, 16, 8. [Google Scholar] [CrossRef]
- Rogers, L.C.; Armstrong, D.G.; Capotorto, J.; Fife, C.E.; Garcia, J.R.; Gelly, H.; et al. ound Center Without Walls: The New Model of Providing Care During the COVID-19 Pandemic. Wounds 2020, 32, 178–185. Available online: https://pmc.ncbi.nlm.nih.gov/articles/PMC8356413/.
- Probst, S.; Weller, C.D.; Bobbink, P.; Saini, C.; Pugliese, M.; Skinner, M.B.; et al. Prevalence and incidence of venous leg ulcers—a protocol for a systematic review. Syst. Rev. 2021, 10, 148. [Google Scholar] [CrossRef] [PubMed]
- Kennerly, S.M.; Sharkey, P.D.; Horn, S.D.; Alderden, J.; Yap, T.L. Nursing Assessment of Pressure Injury Risk with the Braden Scale Validated against Sensor-Based Measurement of Movement. Healthcare 2022, 10, 2330. [Google Scholar] [CrossRef] [PubMed]
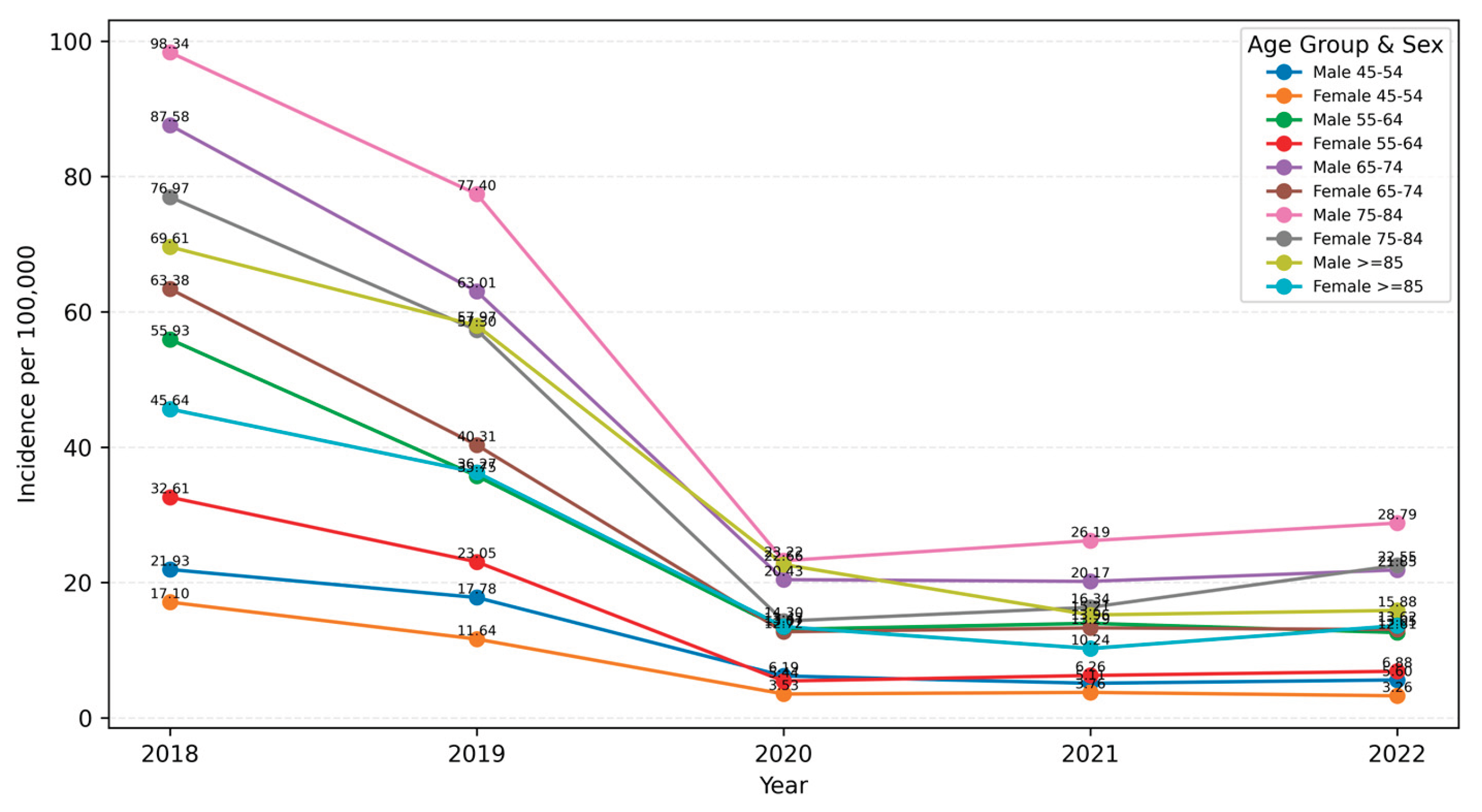
| Age group | Sex | Ulcer category / number (percent) | |||||
|---|---|---|---|---|---|---|---|
| L89 | E1x.73 | I70.23 | I83.x | L97 | L98.4 | ||
| <45 | men | 58 (6.85%) | 26 (2.18%) | 14 (0.66%) | 283 (2.76%) | 113 (3.41%) | 74 (6.68%) |
| women | 23 (2.72%) | 6 (0.50%) | 8 (0.37%) | 165 (1.61%) | 64 (1.93%) | 93 (8.40%) | |
| 45–54 | men | 51 (6.02%) | 139 (11.68%) | 117 (5.48%) | 731 (7.12%) | 237 (7.15%) | 104 (9.39%) |
| women | 26 (3.07%) | 17 (1.43%) | 25 (1.17%) | 587 (5.72%) | 174 (5.25%) | 93 (8.40%) | |
| 55–64 | men | 95 (11.22%) | 317 (26.64%) | 419 (19.63%) | 1238 (12.06%) | 466 (14.05%) | 143 (12.92%) |
| women | 56 (6.61%) | 78 (6.55%) | 89 (4.17%) | 1095 (10.67%) | 315 (9.50%) | 124 (11.20%) | |
| 65–74 | men | 102 (12.04%) | 294 (24.71%) | 616 (28.87%) | 1367 (13.32%) | 554 (16.71%) | 159 (14.36%) |
| women | 117 (13.81%) | 120 (10.08%) | 211 (9.89%) | 1734 (16.90%) | 461 (13.90%) | 129 (11.65%) | |
| 75–84 | men | 79 (9.33%) | 102 (8.57%) | 335 (15.70%) | 1045 (10.18%) | 326 (9.83%) | 74 (6.68%) |
| women | 144 (17.00%) | 69 (5.80%) | 192 (9.00%) | 1524 (14.85%) | 446 (13.45%) | 73 (6.59%) | |
| ≥85 | men | 29 (3.42%) | 14 (1.18%) | 55 (2.58%) | 235 (2.29%) | 67 (2.02%) | 23 (2.08%) |
| women | 67 (7.91%) | 8 (0.67%) | 53 (2.48%) | 258 (2.51%) | 93 (2.80%) | 18 (1.63%) | |
| Total 18856 | 847 | 1190 | 2134 | 10262 | 3316 | 1107 | |
| year/population | I83.x | L97 | I70.23 | E1x.73 | L98.4 | L89 | TOTAL | |
|
2017 / 15,939,431 |
n | 4547 | 1842 | 531 | 335 | 436 | 187 | 7878 |
| % | 57.72 | 23.38 | 6.74 | 4.25 | 5.53 | 2.37 | 100 | |
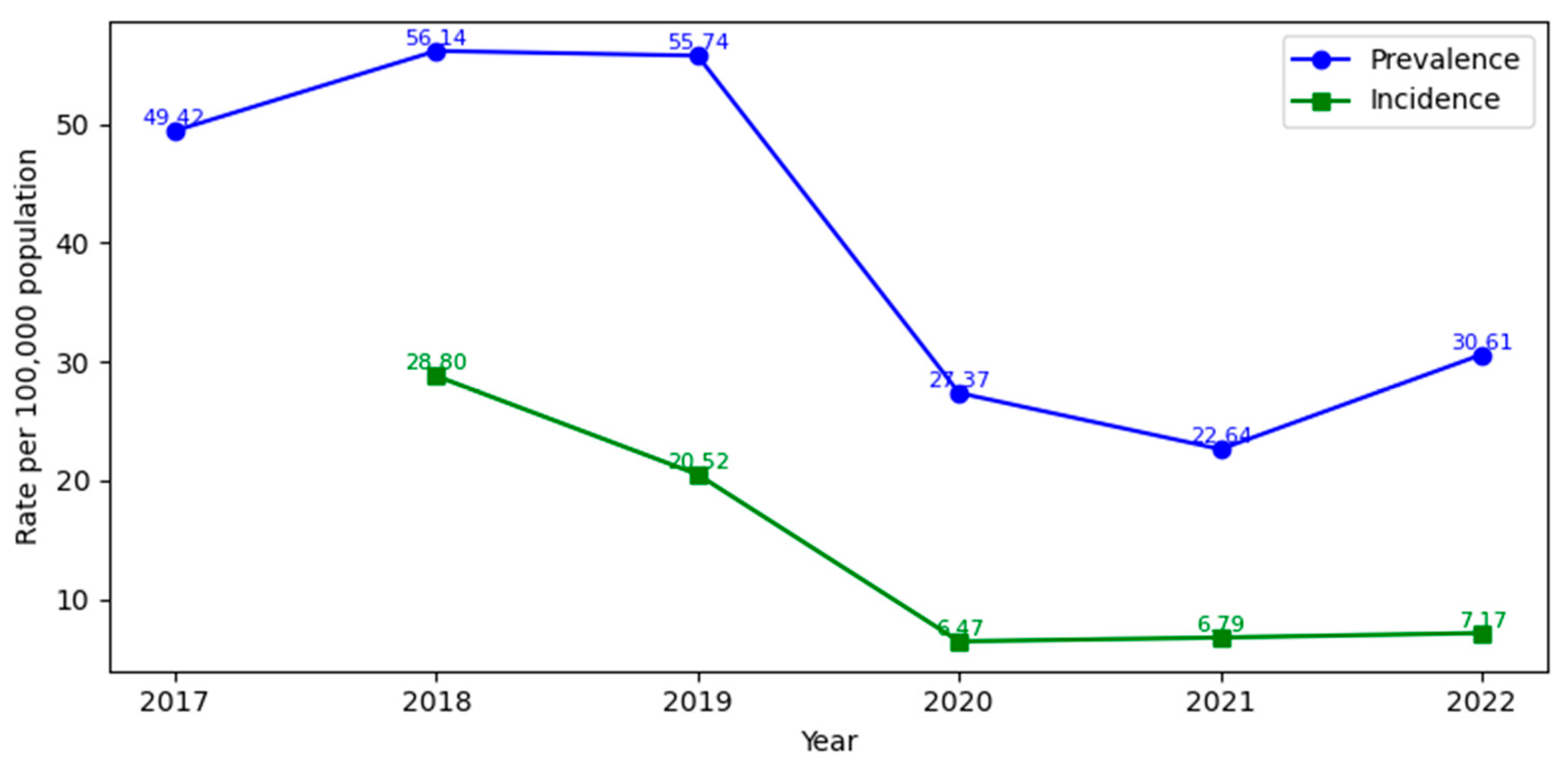
| prevalence | 28.53 | 11.56 | 3.33 | 2.1 | 2.74 | 1.17 | 49.42 | |
| 95% CI | 27.7–29.36 | 11.03–12.08 | 3.05–3.61 | 1.88–2.33 | 2.48–2.99 | 1.01–1.34 | 48.33–50.52 | |
|
2018 / 15,856,123 |
n | 4979 | 2122 | 642 | 342 | 620 | 196 | 8901 |
| % | 55.94 | 23.84 | 7.21 | 3.84 | 6.97 | 2.2 | 100 | |
| prevalence | 31.4 | 13.38 | 4.05 | 2.16 | 3.91 | 1.24 | 56.14 | |
| 95% CI | 30.53–32.27 | 12.81–13.95 | 3.74–4.36 | 1.93–2.39 | 3.6–4.22 | 1.06–1.41 | 54.97–57.3 | |
|
2019 / 15,759,889 |
n | 4853 | 2044 | 653 | 332 | 724 | 179 | 8785 |
| % | 55.24 | 23.27 | 7.43 | 3.78 | 8.24 | 2.04 | 100 | |
| prevalence | 30.79 | 12.97 | 4.14 | 2.11 | 4.59 | 1.14 | 55.74 | |
| 95% CI | 29.93–31.66 | 12.41–13.53 | 3.83–4.46 | 1.88–2.33 | 4.26–4.93 | 0.97–1.3 | 54.58–56.91 | |
|
2020 / 15,683,675 |
n | 2118 | 1071 | 412 | 212 | 350 | 129 | 4292 |
| % | 49.35 | 24.95 | 9.6 | 4.94 | 8.15 | 3.01 | 100 | |
| prevalence | 13.5 | 6.83 | 2.63 | 1.35 | 2.23 | 0.82 | 27.37 | |
| 95% CI | 12.93–14.08 | 6.42–7.24 | 2.37–2.88 | 1.17–1.53 | 2.0–2.47 | 0.68–0.96 | 26.55–28.18 | |
|
2021 / 15,571,548 |
n | 1550 | 977 | 360 | 193 | 332 | 113 | 3525 |
| % | 43.97 | 27.72 | 10.21 | 5.48 | 9.42 | 3.21 | 100 | |
| prevalence | 9.95 | 6.27 | 2.31 | 1.24 | 2.13 | 0.73 | 22.64 | |
| 95% CI | 9.46–10.45 | 5.88–6.67 | 2.07–2.55 | 1.06–1.41 | 1.9–2.36 | 0.59–0.86 | 21.89–23.38 | |
|
2022 / 15,412,147 |
n | 2295 | 1212 | 383 | 185 | 518 | 125 | 4718 |
| % | 48.64 | 25.69 | 8.12 | 3.92 | 10.98 | 2.65 | 100 | |
| prevalence | 14.89 | 7.86 | 2.49 | 1.2 | 3.36 | 0.81 | 30.61 | |
| 95% CI | 14.28–15.5 | 7.42–8.31 | 2.24–2.73 | 1.03–1.37 | 3.07–3.65 | 0.67–0.95 | 29.74–31.49 | |
| Year / population | I83.x | L97 | I70.23 | E1x.73 | L98.4 | L89 | TOTAL | |
| 2018 / | n | 2362 | 1029 | 418 | 223 | 396 | 139 | 4567 |
| 15,856,123 | % | 51.72 | 22.53 | 9.15 | 4.88 | 8.67 | 3.04 | 100 |
| incidence | 14.9 | 6.49 | 2.64 | 1.41 | 2.5 | 0.88 | 28.8 | |
| 95% CI | 14.3–15.5 | 6.09–6.89 | 2.38–2.89 | 1.22–1.59 | 2.25–2.74 | 0.73–1.02 | 27.97–29.64 | |
| 2019 / | n | 1517 | 740 | 357 | 174 | 328 | 118 | 3234 |
| 15,759,889 | % | 46.91 | 22.88 | 11.04 | 5.38 | 10.14 | 3.65 | 100 |
| incidence | 9.63 | 4.7 | 2.27 | 1.1 | 2.08 | 0.75 | 20.52 | |
| 95% CI | 9.14–10.11 | 4.36–5.03 | 2.03–2.5 | 0.94–1.27 | 1.86–2.31 | 0.61–0.88 | 19.81–21.23 | |
| 2020 / | n | 348 | 240 | 180 | 79 | 91 | 76 | 1014 |
| 15,683,675 | % | 34.32 | 23.67 | 17.75 | 7.79 | 8.97 | 7.5 | 100 |
| incidence | 2.22 | 1.53 | 1.15 | 0.5 | 0.58 | 0.48 | 6.47 | |
| 95% CI | 1.99–2.45 | 1.34–1.72 | 0.98–1.32 | 0.39–0.61 | 0.46–0.7 | 0.38–0.59 | 6.07–6.86 | |
| 2021 / | n | 343 | 272 | 173 | 72 | 124 | 74 | 1058 |
| 15,571,548 | % | 32.42 | 25.71 | 16.35 | 6.81 | 11.72 | 6.99 | 100 |
| incidence | 2.2 | 1.75 | 1.11 | 0.46 | 0.8 | 0.48 | 6.79 | |
| 95% CI | 1.97–2.44 | 1.54–1.95 | 0.95–1.28 | 0.36–0.57 | 0.66–0.94 | 0.37–0.58 | 6.39–7.2 | |
| 2022 / | n | 386 | 250 | 145 | 69 | 187 | 68 | 1105 |
| 15,412,147 | % | 34.93 | 22.62 | 13.12 | 6.24 | 16.92 | 6.15 | 100 |
| incidence | 2.5 | 1.62 | 0.94 | 0.45 | 1.21 | 0.44 | 7.17 | |
| 95% CI | 2.25–2.75 | 1.42–1.82 | 0.79–1.09 | 0.34–0.55 | 1.04–1.39 | 0.34–0.55 | 6.75–7.59 | |
| Year / population | I83.x | L97 | I70.23 | E1x.73 | L98.4 | L89 | TOTAL | |
|
2017 15896137 |
n | 4 | 3 | 6 | 3 | 0 | 23 | 39 |
| % | 10.26 | 7.69 | 15.38 | 7.69 | 0.00 | 58.97 | 100 | |
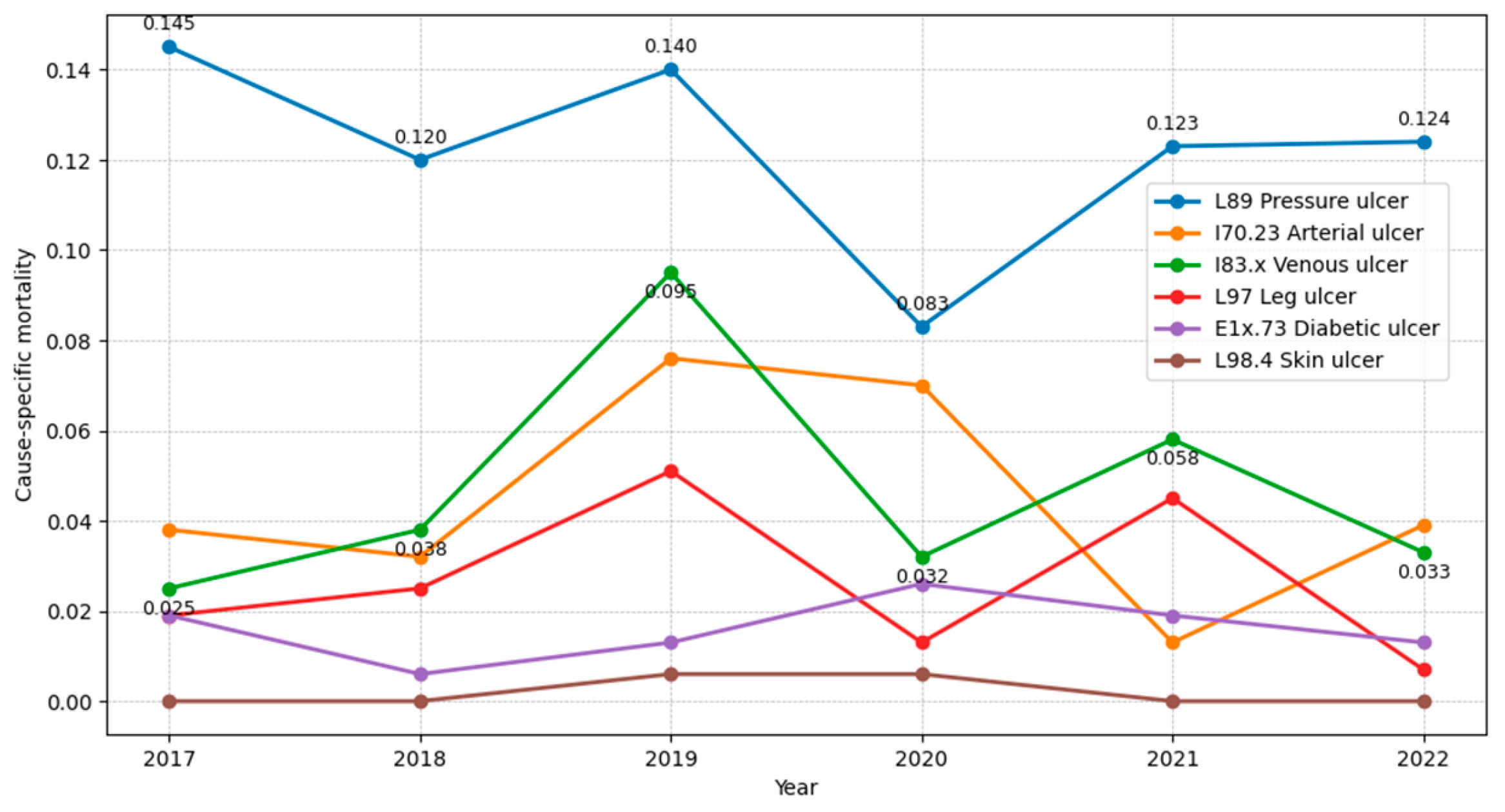
| mortality | 0.025 | 0.019 | 0.038 | 0.019 | 0.000 | 0.145 | 0.245 | |
| 95% CI | 0.007–0.064 | 0.004–0.055 | 0.014–0.082 | 0.004–0.055 | 0.000–0.023 | 0.092–0.217 | 0.174–0.335 | |
| 2018 15803757 | n | 6.00 | 4.00 | 5.00 | 1.00 | 0.00 | 19.00 | 35 |
| % | 17.14 | 11.43 | 14.29 | 2.86 | 0.00 | 54.29 | 100 | |
| mortality | 0.038 | 0.025 | 0.032 | 0.006 | 0.000 | 0.120 | 0.221 | |
| 95% CI | 0.014–0.083 | 0.007–0.065 | 0.010–0.074 | 0.000–0.035 | 0.000–0.023 | 0.072–0.188 | 0.154–0.308 | |
| 2019 15721399 | n | 15.00 | 8.00 | 12.00 | 2.00 | 1.00 | 22.00 | 60 |
| % | 25.00 | 13.33 | 20.00 | 3.33 | 1.67 | 36.67 | 100 | |
| mortality | 0.095 | 0.051 | 0.076 | 0.013 | 0.006 | 0.140 | 0.382 | |
| 95% CI | 0.053–0.157 | 0.022–0.100 | 0.039–0.133 | 0.002–0.046 | 0.000–0.035 | 0.088–0.212 | 0.291–0.491 | |
| 2020 15617687 | n | 5.00 | 2.00 | 11.00 | 4.00 | 1.00 | 13.00 | 36 |
| % | 13.89 | 5.56 | 30.56 | 11.11 | 2.78 | 36.11 | 100 | |
| mortality | 0.032 | 0.013 | 0.070 | 0.026 | 0.006 | 0.083 | 0.231 | |
| 95% CI | 0.010–0.075 | 0.002–0.046 | 0.035–0.126 | 0.007–0.066 | 0.000–0.036 | 0.044–0.142 | 0.161–0.319 | |
| 2021 15429205 | n | 9.00 | 7.00 | 2.00 | 3.00 | 0.00 | 19.00 | 40 |
| % | 22.50 | 17.50 | 5.00 | 7.50 | 0.00 | 47.50 | 100 | |
| mortality | 0.058 | 0.045 | 0.013 | 0.019 | 0.000 | 0.123 | 0.259 | |
| 95% CI | 0.027–0.111 | 0.018–0.093 | 0.002–0.047 | 0.004–0.057 | 0.000–0.024 | 0.074–0.192 | 0.185–0.353 | |
| 2022 15309736 | n | 5.00 | 1.00 | 6.00 | 2.00 | 0.00 | 19.00 | 33 |
| % | 15.15 | 3.03 | 18.18 | 6.06 | 0.00 | 57.58 | 100 | |
| mortality | 0.033 | 0.007 | 0.039 | 0.013 | 0.000 | 0.124 | 0.216 | |
| 95% CI | 0.011–0.07 | 0.000–0.036 | 0.014–0.085 | 0.002–0.047 | 0.000–0.024 | 0.075–0.194 | 0.148–0.303 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




