Submitted:
13 January 2026
Posted:
14 January 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Statistical Analysis
3. Results
3.1. Population Characteristics
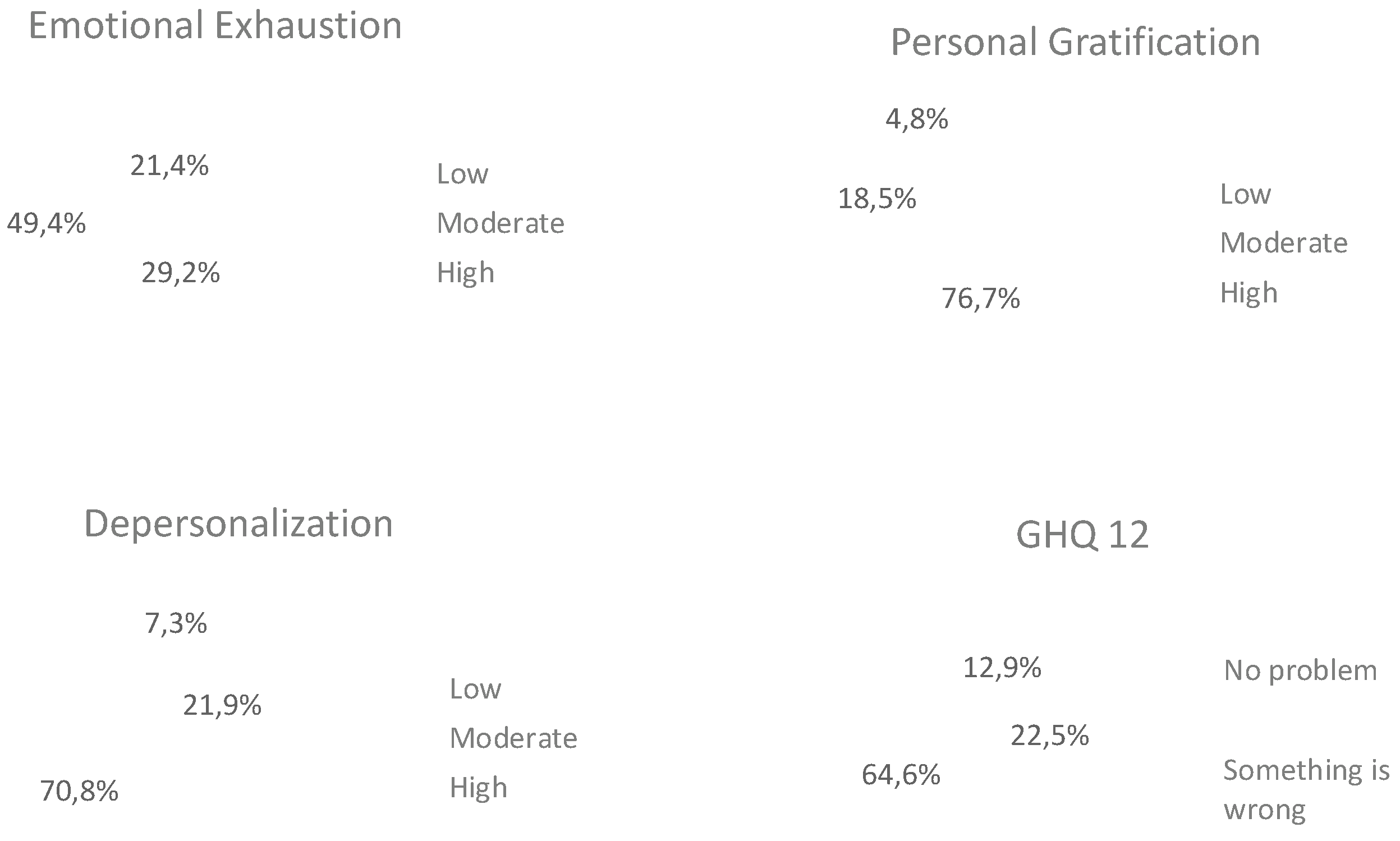
3.2. Burnout Level and Correlation Between Domains
3.3. Graduation Year, Sex, and Specialization
3.4. Burnout Level and General Health Across Different Medical Specialties
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Alcalá-Pacas, A.; Ocaña-Sánchez, M.; Rivera-Arroyo, G.; De Jesús Almanza-Muñoz, J. Síndrome de burnout y rendimiento académico en una escuela de medicina. Rev. Med. Inst. Mex. Seguro Soc. 2017, 43, 13–25.
- Miranda, S.A.; Arnaldo, S.I. Causas del síndrome de burnout en médicos: revisión sistemática de la literatura y análisis bibliométrico; Universidad Internacional del Ecuador: Quito, Ecuador, 2019.
- Muku, M.I.; Tonce, Y. Pengaruh pengawasan dan job burnout terhadap kinerja pegawai pada Badan Pendapatan Daerah Kabupaten Sikka. J. Ekon. Manaj. Pariwisata Perhotelan 2023. [CrossRef]
- Apriana, I.; Edris, M.; Sutono, S. Pengaruh beban kerja dan burnout terhadap kinerja pegawai dengan kepuasan kerja sebagai variabel intervening. J. Studi Manaj. Bisnis 2022, 1, 14-32. [CrossRef]
- O’Connor, K.; Neff, D.; Pitman, S. Burnout in mental health professionals: A systematic review and meta-analysis of prevalence and determinants. Eur. Psychiatry 2018, 53, 74–99. [CrossRef]
- McCormack, H.; MacIntyre, T.; O’Shea, D.; Herring, M.; Campbell, M. The prevalence and cause(s) of burnout among applied psychologists: A systematic review. Front. Psychol. 2018, 9, 1897. [CrossRef]
- De Hert, S. Burnout in healthcare workers: Prevalence, impact and preventative strategies. Local Reg. Anesth. 2020, 13, 171–183. [CrossRef]
- West, C.P.; Dyrbye, L.N.; Shanafelt, T.D. Physician burnout: Contributors, consequences and solutions. J. Intern. Med. 2018, 283, 516–529. [CrossRef]
- Epstein, R.; Privitera, M. Doing something about physician burnout. Lancet 2016, 388, 2216–2217. [CrossRef]
- Țăranu, S.; Ilie, A.; Turcu, A.; Ștefăniu, R.; Sandu, I.; Pîslaru, A.; Alexa, I.; Sandu, C.; Rotaru, T.; Alexa-Stratulat, T. Factors associated with burnout in healthcare professionals. Int. J. Environ. Res. Public Health 2022, 19, 14701. [CrossRef]
- Meredith, L.; Bouskill, K.; Chang, J.; Larkin, J.; Motala, A.; Hempel, S. Predictors of burnout among U.S. healthcare providers: A systematic review. BMJ Open 2022, 12, e054243. [CrossRef]
- Dubale, B.W.; Friedman, L.E.; Chemali, Z.; Denninger, J.W.; Mehta, D.H.; Alem, A.; Fricchione, G.L.; Dossett, M.L.; Gelaye, B. Systematic review of burnout among healthcare providers in sub-Saharan Africa. BMC Public Health 2019, 19, 1247. [CrossRef]
- Peterson, U.; Demerouti, E.; Bergström, G.; Samuelsson, M.; Åsberg, M.; Nygren, Å. Burnout and physical and mental health among Swedish healthcare workers. J. Adv. Nurs. 2008, 62, 84–95. [CrossRef]
- Alzailai, N.; Barriball, K.L.; Xyrichis, A. Impact of, and mitigation measures for, burnout in frontline healthcare workers during disasters: A mixed-method systematic review. Worldviews Evid. Based Nurs. 2023, 20, 133-141. [CrossRef]
- Chemali, Z.; Ezzeddine, F.L.; Gelaye, B.; Dossett, M.L.; Salameh, J.; Bizri, M.; Dubale, B.; Fricchione, G. Burnout among healthcare providers in the complex environment of the Middle East: A systematic review. BMC Public Health 2019, 19, 1337. [CrossRef]
- Gualano, M.R.; Sinigaglia, T.; Lo Moro, G.; Rousset, S.; Cremona, A.; Bert, F.; Siliquini, R. The burden of burnout among healthcare professionals of intensive care units and emergency departments during the COVID-19 pandemic: A systematic review. Int. J. Environ. Res. Public Health 2021, 18, 8172. [CrossRef]
- Ghahramani, S.; Lankarani, K.B.; Yousefi, M.; Heydari, K.; Shahabi, S.; Azmand, S. A systematic review and meta-analysis of burnout among healthcare workers during COVID-19. Front. Psychiatry 2021, 12, 758849. [CrossRef]
- Tan, B.Y.Q.; Kanneganti, A.; Lim, L.J.H.; Tan, M.; Chua, Y.X.; Tan, L.; Sia, C.H.; Denning, M.; Goh, E.T.; Purkayastha, S.; et al. Burnout and associated factors among healthcare workers in Singapore during the COVID-19 pandemic. J. Am. Med. Dir. Assoc. 2020, 21, 1751–1758.e5. [CrossRef]
- Lasalvia, A.; Amaddeo, F.; Porru, S.; Carta, A.; Tardivo, S.; Bovo, C.; Ruggeri, M.; Bonetto, C. Levels of burn-out among healthcare workers during the COVID-19 pandemic and associated factors. BMJ Open 2021, 11, e045127. [CrossRef]
- Civita, M.; Laurita, E.; Di Stefano, C.; Gervasoni, M.; Viotti, S.; Zucchi, S. Physicians and nurses’ burnout in emergency departments of North West Italy. Intern. Emerg. Med. 2021, 16, 1381–1385. [CrossRef]
- Lupo, R.; Iezzi, A.; Conte, L.; Santoro, P.; Carvello, M.; Artioli, G.; Calabrò, A.; Caldararo, C.; Botti, S.; Carriero, M. Work environment and related burnout levels among healthcare workers in Southern Italy. Acta Biomed. 2021, 92, e11307. [CrossRef]
- Brera, A.; Arrigoni, C.; Dellafiore, F.; Odone, A.; Magon, A.; Nania, T.; Pittella, F.; Palamenghi, L.; Barello, S.; Caruso, R. Burnout syndrome and its determinants among healthcare workers during COVID-19 in Italy. Med. Lav. 2021, 112, 306–319. [CrossRef]
- Di Trani, M.; Mariani, R.; Ferri, R.; De Berardinis, D.; Frigo, M. From resilience to burnout in healthcare workers during the COVID-19 emergency. Front. Psychol. 2021, 12, 646435. [CrossRef]
- De Wit, K.; Tran, A.; Clayton, N.; et al. A longitudinal survey on Canadian emergency physician burnout. Ann. Emerg. Med. 2024, 83, 576–584. [CrossRef]
- Burns, K.E.A.; Duffett, M.; Kho, M.E.; et al. A guide for the design and conduct of self-administered surveys of clinicians. CMAJ 2008, 179, 245–252.
- Maslach, C.; Jackson, S.E.; Leiter, M.P. Maslach Burnout Inventory Manual, 3rd ed.; Consulting Psychologists Press: Palo Alto, CA, USA, 1996.
- Goldberg, D.P.; Gater, R.; Sartorius, N.; et al. The validity of two versions of the GHQ in general health care. Psychol. Med. 1997, 27, 191–197. [CrossRef]
- Italy. Decree-Law No. 18 of 17 March 2020; Gazzetta Ufficiale della Repubblica Italiana, General Series No. 110, 29 April 2020.
- Ng, I. Making the transition from medical student to junior doctor. J. R. Coll. Physicians Edinb. 2024, 54, 316-318. [CrossRef]
- Dobretsova, E.; Arshukova, I.; Dugina, T. New generation of medical students: What are they looking for? Eur. J. Public Health 2020, 30 (Suppl. 5). [CrossRef]
- Michalik, B.; Kulbat, M.; Domagała, A. Factors affecting young doctors’ choice of medical specialty. PLoS ONE 2024, 19, e0297927. [CrossRef]
- Hoff, T.; Lee, D.R. Burnout and physician gender: What do we know? Med. Care 2021, 59, 711–720. [CrossRef]
- Yeluru, H.; Newton, H.L.; Kapoor, R. Physician burnout through the female lens. Front. Public Health 2022, 10, 880061. [CrossRef]
- Spataro, B.M.; Tilstra, S.A.; Rubio, D.M.; McNeil, M.A. Sex differences in burnout and coping in internal medicine trainees. J. Womens Health 2016, 25, 1147–1152. [CrossRef]
- Daruvala, R.; Ghosh, M.; Fratazzi, F.; et al. Emotional exhaustion in cancer clinicians. Indian J. Med. Paediatr. Oncol. 2019, 40, 111–120. [CrossRef]
- Qamar, M.K.; Shaikh, B.T.; Kumar, R.; Qamar, A.K. Gender difference of burnout in physicians. J. Coll. Physicians Surg. Pak. 2024, 34, 620–622. [CrossRef]
- Thakur, S.; Chauhan, V.; Galwankar, S.; et al. Gender disparities and burnout among emergency physicians. West. J. Emerg. Med. 2025, 26, 338–346. [CrossRef]
- Kilic, R.; Nasello, J.A.; Melchior, V.; Triffaux, J.M. Academic burnout among medical students. Public Health 2021, 198, 187–195. [CrossRef]
- Stanetić, K.; Petrović, V.; Marković, B.; Stanetić, B. Stress and burnout among primary healthcare physicians. Acta Med. Acad. 2019, 48, 159–166. [CrossRef]
- Gelaw, Y.M.; Hanoch, K.; Adini, B. Burnout and resilience among health professionals in Ethiopia. Front. Public Health 2023, 11, 1118450. [CrossRef]
- Hewitt, D.B.; Ellis, R.J.; Hu, Y.Y.; Cheung, E.O.; Moskowitz, J.T.; Agarwal, G.; Bilimoria, K.Y. Evaluating the association of multiple burnout definitions and thresholds with prevalence and outcomes. JAMA Surg. 2020, 155, 1043–1049. [CrossRef]
- Rodrigues, H.; Cobucci, R.; Oliveira, A.; et al. Burnout syndrome among medical residents. PLoS ONE 2018, 13, e0206840. [CrossRef]
- Etheridge, J.C.; Evans, D.; Zhao, L.; et al. Trends in surgeon burnout. J. Am. Coll. Surg. 2023, 236, 253–265. [CrossRef]
- Low, Z.X.; Yeo, K.A.; Sharma, V.K.; et al. Prevalence of burnout in medical and surgical residents. Int. J. Environ. Res. Public Health 2019, 16, 1479. [CrossRef]
- Stehman, C.R.; Testo, Z.; Gershaw, R.S.; Kellogg, A.R. Burnout, dropout, suicide in emergency medicine. West. J. Emerg. Med. 2019, 20, 485–494. [CrossRef]
- Williamson, K.; Lank, P.M.; Cheema, N.; Hartman, N.; Lovell, E.O. Comparing burnout instruments in emergency medicine residents. J. Grad. Med. Educ. 2018, 10, 532–536. [CrossRef]
- Sharaf, A.M.; Abdulla, I.H.; Alnatheer, A.M.; et al. Emotional intelligence and burnout in otorhinolaryngology residents. Front. Public Health 2022, 10, 851408. [CrossRef]
| Participant characteristics | ||
|---|---|---|
| Sex n (%) | Male | 184 (51.69) |
| Female | 172 (48.31) | |
| Age mean, SD (range) | 34.16 ± 9.2 (25-66) | |
| Marital status n (%) | Single or not cohabiting | 208 (58.43) |
| Married or cohabiting | 148 (41.57) | |
| 0 | 289 (81.18) | |
| Number of Children n (%) | 1 | 27 (7.58) |
| 2 | 35 (9.83) | |
| ≥3 | 5 (1.40) | |
| ≤40 | 93 (26.12) | |
| Working Hours n (%) | 41-50 | 163 (45.79) |
| 51-60 | 100 (28.09) | |
| Services area | 92 (25.92) | |
| Medical Specialization Areas n (%) | Medical area | 152 (42.82) |
| Surgical area | 111 (31.27) |
| Variables | GHQ 12 | Emotional Exhaustion | Depersonalization | Gratification |
|---|---|---|---|---|
| GHQ 12 | 1.000 | |||
| Emotional Exhaustion | 0.588* | 1.000 | ||
| (0.000) | ||||
| Depersonalization | 0.373* | 0.591* | 1.000 | |
| (0.000) | (0.000) | |||
| Gratification | -0.207* | -0.020 | 0.013 | 1.000 |
| (0.000) | (0.706) | (0.811) |
| Emotional Exhaustion | ||||
|
Graduation before 2020 Graduation after 2020 |
Low | Moderate | High | p-value |
| 32 (42.11) | 42 (40.38) | 87 (49.43) | 0.19 | |
| 44 (57.89) | 62 (59.62) | 89 (50.57) | ||
| Depersonalization | ||||
| Low | Moderate | High | p-value | |
| Graduation before 2020 | 12 (46.15) | 35 (44.87) | 114 (45.24) | 0.97 |
| Graduation after 2020 | 14 (7.18) | 43 (55.13) | 138 (54.76) | |
| Gratification | ||||
| Low | Moderate | High | p-value | |
| Graduation before 2020 | 109 (39.93) | 40 (60.61) | 12 (70.59) | p<0.01 |
| Graduation after 2020 | 164 (60.07) | 26 (39.39) | 29 (41) | |
| GHQ 12 | ||||
| No problem | Something is wrong | I need help | p-value | |
| Graduation before 2020 | 23 (50) | 32 (40) | 106 (46.09) | p=0.97 |
| Graduation after 2020 | 23 (50) | 48 (60) | 124 (53.91) |
| Emotional Exhaustion | ||||
|
Male Female |
Low | Moderate | High | p-value |
| 42 (55.26) | 61 (58.65) | 81 (46.02) | 0.09 | |
| 34 (44.74) | 43 (41.35) | 95 (53.98) | ||
| Depersonalization | ||||
| Low | Moderate | High | p-value | |
| Male | 12 (46.15) | 35 (44.87) | 114 (45.24) | 0.97 |
| Female | 14 (7.18) | 43 (55.13) | 138 (54.76) | |
| Gratification | ||||
| Low | Moderate | High | p-value | |
| Male | 109 (39.93) | 40 (60.61) | 12 (70.59) | p<0.01 |
| Female | 164 (60.07) | 26 (39.39) | 29 (41) | |
| GHQ 12 | ||||
| No problem | Something is wrong | I need help | p-value | |
| Male | 29 (63.04) | 44 (55) | 111 (48.26) | p=0.05 |
| Female | 17 (36.96) | 36 (45) | 119 (51.74) |
| Emotional Exhaustion | ||||
| Medical Surgery |
Low | Moderate | High | p-value |
| 32 (42.67) | 39 (37.50) | 81 (46.02) | p=0.025 (services vs surgery) | |
| 18 (24) | 32 (30.77) | 61 (34.66) | p=0.78 (clinical vs surgery) | |
| Services | 25 (33.3) | 33 (31.73) | 34 (19.32) | p=0.079 (clinical vs services) |
| Depersonalization | ||||
| Low | Moderate | High | p-value | |
| Medical | 6 (23.08) | 26 (33.77) | 120 (47.62) | p=0.01 (services vs surgery) |
| Surgery | 6 (23.08) | 22 (28.57) | 83 (32.94) | p=0.73 (clinical vs surgery) |
| Services | 14 (53.85) | 29 (37.66) | 49 (19.44) | p<0.001 (clinical vs services) |
| Gratification | ||||
| Low | Moderate | High | p-value | |
| Medical | 115 (42.28) | 30 (45.45) | 7 (41.18) | p=0.04 (services vs surgery) |
| Surgery | 79 (29.04) | 24 (36.36) | 8 (47.06) | p=0.54 (clinical vs surgery) |
| Services | 78 (28.68) | 12 (18.18) | 2 (11.76) | p=0.24 (clinical vs services) |
| GHQ 12 | ||||
| No problem | Something is wrong | I need help | p-value | |
| Medical | 16 (35.56) | 34 (42.50) | 102 (44.35) | p=0.59 (services vs surgery) |
| Surgery | 17 (36.96) | 36 (45) | 119 (51.74) | p=0.92 (clinical vs surgery) |
| Services | 15 (33.33) | 22 (27.50) | 55 (23.91) | p=0.34 (clinical vs services) |
| MBI | Low-level burnout | Moderate burnout | High-level burnout |
|---|---|---|---|
| Emotional Exhaustion | Total score of 17 or less | Total score between 18 and 29 (inclusive) | Total score over 30 |
| Depersonalization | Total score of 5 or less | Total score between 6 and 11 (inclusive) | Total score of 12 or greater |
| Gratification | Total score of 33 or less | Total score between 34 and 39 (inclusive) | Total score greater than 40 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




