Submitted:
09 January 2026
Posted:
09 January 2026
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Hypothesis
3. Methods
4. Results
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| T2DM | Type 2 Diabetes |
| REM | Rapid Eye Movement |
| OSA | Obstructive Sleep Apnea |
| BMI | Body Mass Index |
References
- Centers for Disease Control and Prevention. National Diabetes Statistics Report . 15 May 2024. Available online: https://www.cdc.gov/diabetes/php/data-research/index.html (accessed on 6 June 2024).
- Xu, G.; Liu, B.; Sun, Y.; Du, Y.; Snetselaar, L.G.; Hu, F.B.; Bao, W. Prevalence of diagnosed type 1 and type 2 diabetes among US adults in 2016 and 2017: Population based study. BMJ 2018, 362, k1497. [Google Scholar] [CrossRef] [PubMed]
- Punjabi, N.M.; Shahar, E.; Redline, S.; Gottlieb, D.J.; Givelber, R.; Resnick, H.E. & Sleep Heart Health Study Investigators Sleep-disordered breathing, glucose intolerance, and insulin resistance: The Sleep Heart Health Study. American journal of epidemiology 2004, 160(6), 521–530. [Google Scholar] [CrossRef] [PubMed]
- Pham, L.V.; Jun, J.; Polotsky, V.Y. Obstructive sleep apnea. In Handbook of Clinical Neurology; 2022; Volume 189, pp. 105–136. [Google Scholar] [CrossRef] [PubMed]
- Mitra, A.K.; Bhuiyan, A.R.; Jones, E.A. Association and Risk Factors for Obstructive Sleep Apnea and Cardiovascular Diseases: A Systematic Review. Diseases 2021, 9(4), 88. [Google Scholar] [CrossRef]
- Kurnool, S.; McCowen, K.C.; Bernstein, N.A.; Malhotra, A. Sleep Apnea, Obesity, and Diabetes - an Intertwined Trio. Current diabetes reports 2023, 23(7), 165–171. [Google Scholar] [CrossRef]
- Xu, H.; Liang, C.; Zou, J.; Yi, H.; Guan, J.; Gu, M.; Feng, Y.; Yin, S. Interaction between obstructive sleep apnea and short sleep duration on insulin resistance: A large-scale study: OSA, short sleep duration and insulin resistance. Respiratory research 2020, 21(1), 151. [Google Scholar] [CrossRef]
- Aronsohn, R.S.; Whitmore, H.; Van Cauter, E.; Tasali, E. Impact of untreated obstructive sleep apnea on glucose control in type 2 diabetes. American journal of respiratory and critical care medicine 2010, 181(5), 507–513. [Google Scholar] [CrossRef]
- Muraki, I.; Wada, H.; Tanigawa, T. Sleep apnea and type 2 diabetes. Journal of diabetes investigation 2018, 9(5), 991–997. [Google Scholar] [CrossRef]
- Rutters, F.; Nefs, G. Sleep and Circadian Rhythm Disturbances in Diabetes: A Narrative Review. Diabetes, metabolic syndrome and obesity: Targets and therapy 2022, 15, 3627–3637. [Google Scholar] [CrossRef]
- Pamidi, S.; Tasali, E. Obstructive sleep apnea and type 2 diabetes: Is there a link? Frontiers in neurology 2012, 3, 126. [Google Scholar] [CrossRef]
- Heffner, J.E.; Rozenfeld, Y.; Kai, M.; Stephens, E.A.; Brown, L.K. Prevalence of diagnosed sleep apnea among patients with type 2 diabetes in primary care. Chest 2012, 141(6), 1414–1421. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. 8. Pharmacologic Approaches to Glycemic Treatment: Standards of Medical Care in Diabetes-2018. Diabetes care 2018, 41 Suppl 1, S73–S85. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.W.; He, S.J.; Feng, X.; Cheng, J.; Luo, Y.T.; Tian, L.; Huang, Q. Metformin: A review of its potential indications. Drug design, development and therapy 2017, 11, 2421–2429. [Google Scholar] [CrossRef]
- Le, S.; Lee, G.C. Emerging Trends in Metformin Prescribing in the United States from 2000 to 2015. Clinical drug investigation 2019, 39(8), 757–763. [Google Scholar] [CrossRef] [PubMed]
- Foretz, M.; Guigas, B.; Viollet, B. Metformin: Update on mechanisms of action and repurposing potential. Nature reviews. Endocrinology 2023, 19(8), 460–476. [Google Scholar] [CrossRef]
- Susilawati, E.; Levita, J.; Susilawati, Y.; Sumiwi, S.A. Review of the Case Reports on Metformin, Sulfonylurea, and Thiazolidinedione Therapies in Type 2 Diabetes Mellitus Patients. Medical sciences 2023, 11(3), 50. [Google Scholar] [CrossRef]
- Wiwanitkit, S.; Wiwanitkit, V. Metformin and insomnia: An interesting story. Diabetes & metabolic syndrome 2011, 5(3), 160. [Google Scholar]
- Yoda, K.; Inaba, M.; Hamamoto, K.; Yoda, M.; Tsuda, A.; Mori, K.; Imanishi, Y.; Emoto, M.; Yamada, S. Association between poor glycemic control, impaired sleep quality, and increased arterial thickening in type 2 diabetic patients. PloS one 2015, 10(4), e0122521. [Google Scholar] [CrossRef]
- Abdelmaksoud, A.A.; Salah, N.Y.; Ali, Z.M.; Rashed, H.R.; Abido, A.Y. Disturbed sleep quality and architecture in adolescents with type 1 diabetes mellitus: Relation to glycemic control, vascular complications and insulin sensitivity. Diabetes research and clinical practice 2021, 174, 108774. [Google Scholar] [CrossRef]
- Pallayova, M.; Donic, V.; Gresova, S.; Peregrim, I.; Tomori, Z. Do differences in sleep architecture exist between persons with type 2 diabetes and nondiabetic controls? Journal of diabetes science and technology 2010, 4(2), 344–352. [Google Scholar] [CrossRef]
- Chen, D.M.; Taporoski, T.P.; Alexandria, S.J.; Aaby, D.A.; Beijamini, F.; Krieger, J.E.; von Schantz, M.; Pereira, A.C.; Knutson, K.L. Altered sleep architecture in diabetes and prediabetes: Findings from the Baependi Heart Study. Sleep 2024, 47(1), zsad229. [Google Scholar] [CrossRef]
- Varma, M.; Eghbali, M.; Hung, D.; Sahai, A. Effect of insulin on sleep architecture in diabetic patients with sleep apnea. Sleep Medicine 2024, 115, S252. [Google Scholar] [CrossRef]
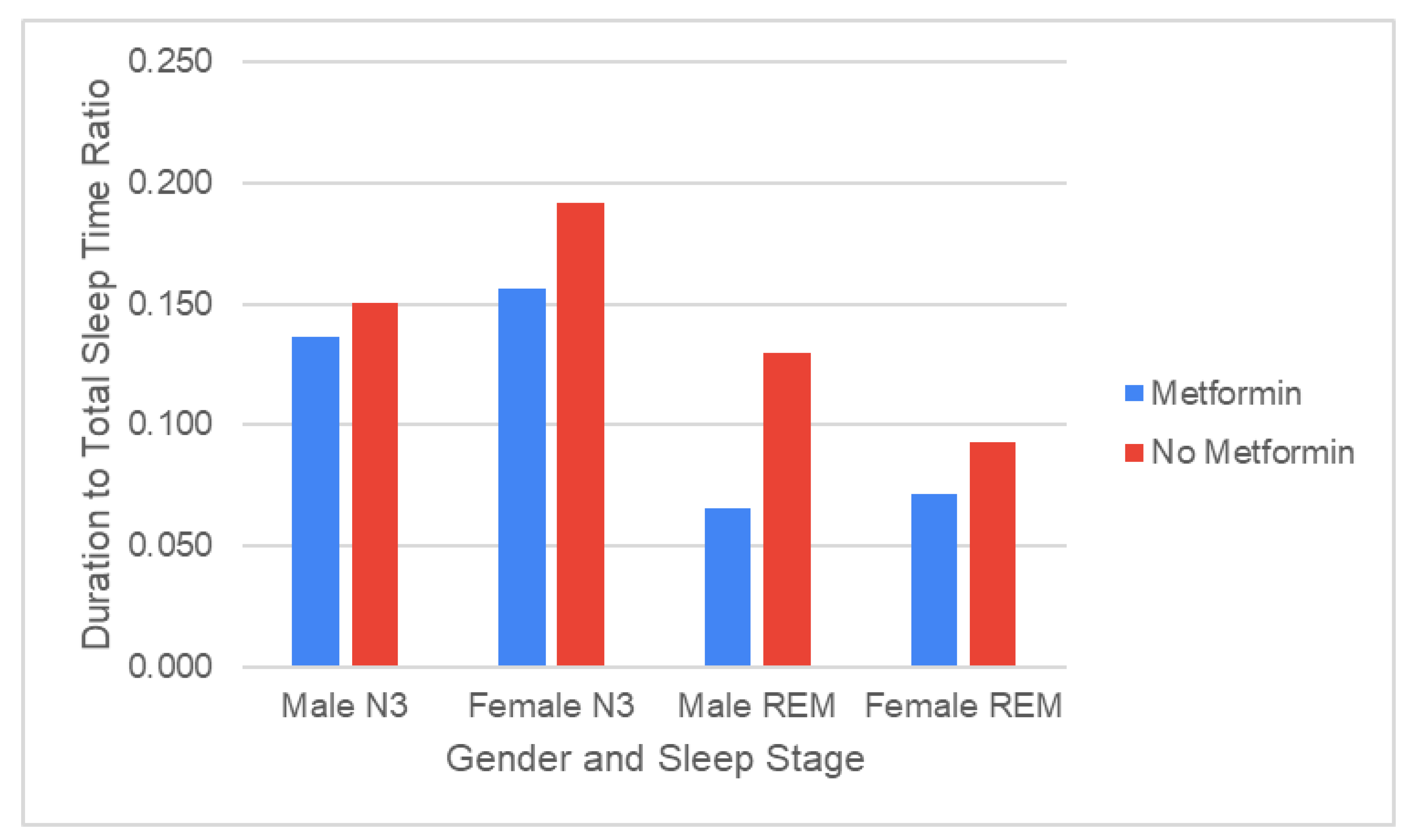
- Baranski, T.; Eghbali, M.; Sahai, A.; Varma, M. Gender differences in sleep architecture of diabetic patients on metformin with sleep apnea: An analysis of polysomnography studies. Sleep Medicine 2024, 115 Suppl. 1, S106. [Google Scholar] [CrossRef]
- Henson, J.; Covenant, A.; Hall, A.P.; Herring, L.; Rowlands, A.V.; Yates, T.; Davies, M.J. Waking Up to the Importance of Sleep in Type 2 Diabetes Management: A Narrative Review. Diabetes care 2024, 47(3), 331–343. [Google Scholar] [CrossRef] [PubMed]
- Peever, J.; Fuller, P.M. The Biology of REM Sleep. Current biology: CB 2017, 27(22), R1237–R1248. [Google Scholar] [CrossRef]
- Varma, M.; Eghbali, M.; Hung, D.; Sahai, A. FRI636 sleep architecture in diabetic patients with sleep apnea on metformin. Journal of the Endocrine Society 2023, 7 Supplement_1, A459–A460. [Google Scholar] [CrossRef]
- Lapierre, O.; Montplaisir, J.; Lamarre, M.; Bedard, M.A. The effect of gamma-hydroxybutyrate on nocturnal and diurnal sleep of normal subjects: Further considerations on REM sleep-triggering mechanisms. Sleep 1990, 13(1), 24–30. [Google Scholar] [CrossRef]
- Moser, D.; Anderer, P.; Gruber, G.; Parapatics, S.; Loretz, E.; Boeck, M.; Kloesch, G.; Heller, E.; Schmidt, A.; Danker-Hopfe, H.; et al. Sleep classification according to AASM and Rechtschaffen & Kales: Effects on sleep scoring parameters. Sleep 2009, 32(2), 139–149. [Google Scholar] [CrossRef]
- Durak, B.; Gunduz Gurkan, C.; Özol, D.; Saraç, S. The Effect of Type-2 Diabetes Mellitus on Sleep Architecture and Sleep Apnea Severity in Patients With Obstructive Sleep Apnea Syndrome. Cureus 2024, 16(5), e61215. [Google Scholar] [CrossRef]
- Shahveisi, K.; Jalali, A.; Moloudi, M.R.; Moradi, S.; Maroufi, A.; Khazaie, H. Sleep Architecture in Patients With Primary Snoring and Obstructive Sleep Apnea. Basic and clinical neuroscience 2018, 9(2), 147–156. [Google Scholar] [CrossRef]
- Yanto, T.A.; Huang, I.; Kosasih, F.N.; Lugito, N.P.H. Nightmare and Abnormal Dreams: Rare Side Effects of Metformin? Case reports in endocrinology 2018, 2018, 7809305. [Google Scholar] [CrossRef] [PubMed]
- Voloshyna, D.; Sandhu, Q.I.; Khan, S.; Bseiso, A.; Mengar, J.; Nayudu, N.; Kumar, R.; Khemani, D.; Usama, M. An Unusual Association Between Metformin and Nightmares: A Case Report. Cureus 2022, 14(9), e28974. [Google Scholar] [CrossRef] [PubMed]
- Modi, B.; Suravajjala, D.P.; Case, J.; Velumani, P. Metformin-induced nightmares: An uncommon event. Cureus 2024, 16(7). [Google Scholar] [CrossRef] [PubMed]
- Sakurai, T.; Amemiya, A.; Ishii, M.; Matsuzaki, I.; Chemelli, R.M.; Tanaka, H.; Williams, S.C.; Richardson, J.A.; Kozlowski, G.P.; Wilson, S.; et al. Orexins and orexin receptors: A family of hypothalamic neuropeptides and G protein- coupled receptors that regulate feeding behavior. Cell 1998, 92(4), 573–585. [Google Scholar] [CrossRef]
- Toor, B.; Ray, L.B.; Pozzobon, A.; Fogel, S.M. Sleep, Orexin and Cognition. Frontiers of neurology and neuroscience 2021, 45, 38–51. [Google Scholar] [CrossRef]
- St-Onge, M.P.; Cherta-Murillo, A.; Darimont, C.; Mantantzis, K.; Martin, F.P.; Owen, L. The interrelationship between sleep, diet, and glucose metabolism. Sleep medicine reviews 2023, 69, 101788. [Google Scholar] [CrossRef]
- Funato, H.; Tsai, A.L.; Willie, J.T.; Kisanuki, Y.; Williams, S.C.; Sakurai, T.; Yanagisawa, M. Enhanced orexin receptor-2 signaling prevents diet-induced obesity and improves leptin sensitivity. Cell metabolism 2009, 9(1), 64–76. [Google Scholar] [CrossRef]
- Cai, X.J.; Lister, C.A.; Buckingham, R.E.; Pickavance, L.; Wilding, J.; Arch, J.R.; Wilson, S.; Williams, G. Down-regulation of orexin gene expression by severe obesity in the rats: Studies in Zucker fatty and zucker diabetic fatty rats and effects of rosiglitazone. Brain research. Molecular brain research 2000, 77(1), 131–137. [Google Scholar] [CrossRef]
- Mogavero, M.P.; Godos, J.; Grosso, G.; Caraci, F.; Ferri, R. Rethinking the Role of Orexin in the Regulation of REM Sleep and Appetite. Nutrients 2023, 15(17), 3679. [Google Scholar] [CrossRef]
- Zarifkar, M.; Noshad, S.; Shahriari, M.; Afarideh, M.; Khajeh, E.; Karimi, Z.; Ghajar, A.; Esteghamati, A. Inverse Association of Peripheral Orexin-A with Insulin Resistance in Type 2 Diabetes Mellitus: A Randomized Clinical Trial. The review of diabetic studies: RDS 2017, 14, 301–310. [Google Scholar] [CrossRef]
- Lendner, J.D.; Niethard, N.; Mander, B.A.; van Schalkwijk, F.J.; Schuh-Hofer, S.; Schmidt, H.; Knight, R.T.; Born, J.; Walker, M.P.; Lin, J.J.; et al. Human REM sleep recalibrates neural activity in support of memory formation. Science advances 2023, 9(34), eadj1895. [Google Scholar] [CrossRef]
- Espiritu, J.R. Aging-related sleep changes. Clinics in geriatric medicine 2008, 24(1), 1-v. [Google Scholar] [CrossRef]
- Casagrande, M.; Forte, G.; Favieri, F.; Corbo, I. Sleep Quality and Aging: A Systematic Review on Healthy Older People, Mild Cognitive Impairment and Alzheimer’s Disease. International journal of environmental research and public health 2022, 19(14), 8457. [Google Scholar] [CrossRef]
- Lok, R.; Qian, J.; Chellappa, S.L. Sex differences in sleep, circadian rhythms, and metabolism: Implications for precision medicine. Sleep medicine reviews 2024, 75, 101926. [Google Scholar] [CrossRef]
- Morssinkhof, M.W.L.; van der Werf, Y.D.; van den Heuvel, O.A.; van den Ende, D.A.; van der Tuuk, K.; den Heijer, M.; Broekman, B.F.P. Influence of sex hormone use on sleep architecture in a transgender cohort. Sleep 2023, 46(11), zsad249. [Google Scholar] [CrossRef]
- Naufel, M.F.; Frange, C.; Andersen, M.L.; Girão, M.J.B.C.; Tufik, S.; Beraldi Ribeiro, E.; Hachul, H. Association between obesity and sleep disorders in postmenopausal women. Menopause 2018, 25(2), 139–144. [Google Scholar] [CrossRef]
- Messineo, L.; Bakker, J.P.; Cronin, J.; Yee, J.; White, D.P. Obstructive sleep apnea and obesity: A review of epidemiology, pathophysiology and the effect of weight-loss treatments. Sleep medicine reviews Advance online publication. 2024, 78, 101996. [Google Scholar] [CrossRef]
- Sever, O.; Kezirian, E.J.; Gillett, E.; Davidson Ward, S.L.; Khoo, M.; Perez, I.A. Association between REM sleep and obstructive sleep apnea in obese and overweight adolescents. Sleep & breathing = Schlaf & Atmung 2019, 23(2), 645–650. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




