Submitted:
01 December 2025
Posted:
09 December 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Study Design and Setting
Study Population
Data Collection and Study Variables
Outcomes
Statistical Analysis
Ethical Approval
3. Results
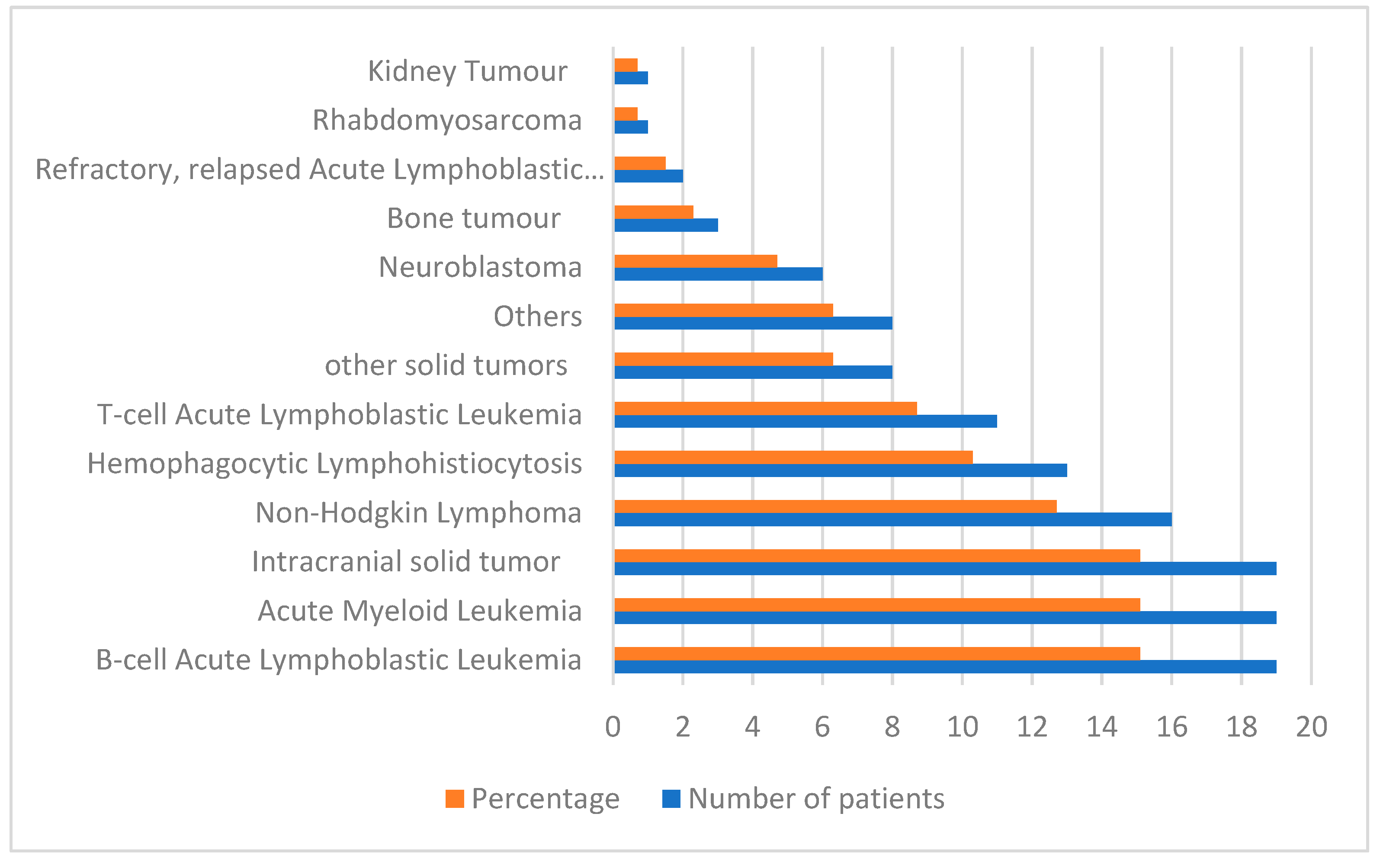
Incidence and Characteristics of PICU Admission
PICU Interventions and Organ Dysfunction
- Mechanical ventilation was required in 35% of patients.
- Inotropic support was administered to 30% of patients.
- A smaller proportion required renal replacement therapy.
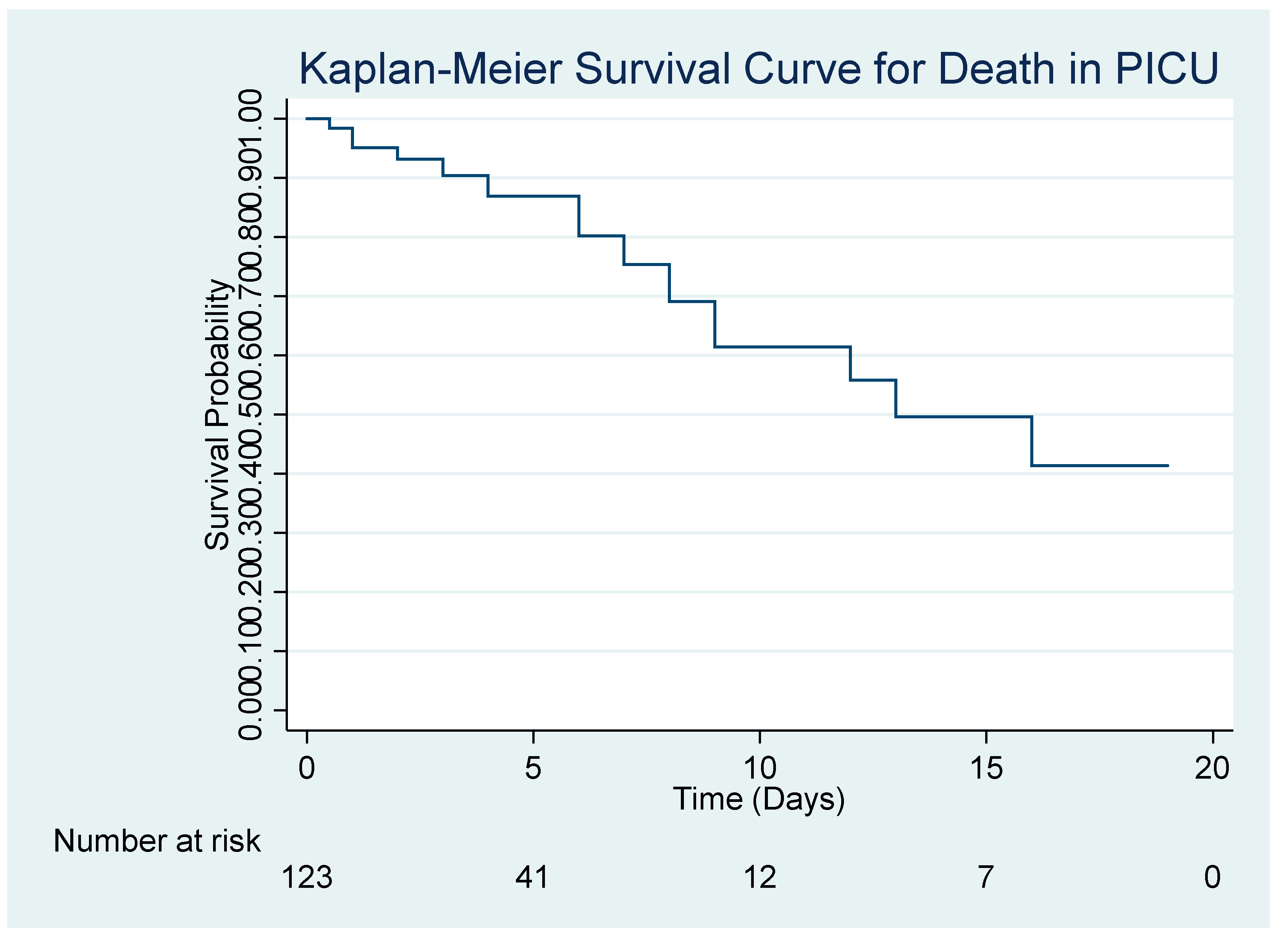
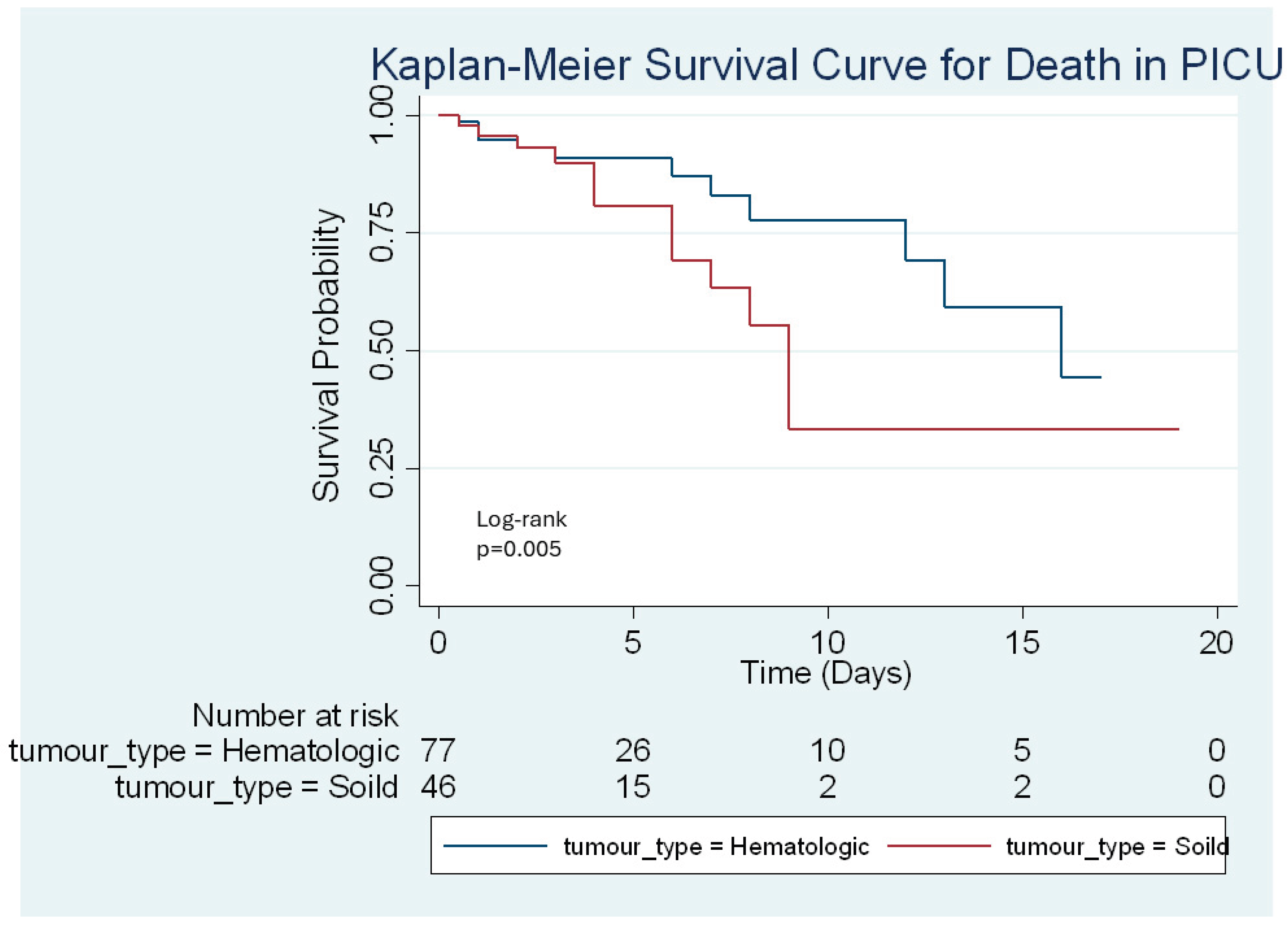
Study Outcomes
- A higher prevalence of comorbidities (48% vs. 26%; p = 0.039)
- Greater need for mechanical ventilation (76% vs. 25%; p < 0.001)
- Increased use of inotropic support (52% vs. 24%; p = 0.008)
Predictors of Mortality
- Comorbidities (HR: 2.10; 95% CI: 1.00–4.40)
- Prior therapeutic interventions before PICU admission (HR: 2.70; 95% CI: 1.04–6.9)
- Mechanical ventilation (HR: 3.0; 95% CI: 1.22–7.39)
- Prior therapeutic interventions remained a strong independent predictor of mortality (HR: 3.19; 95% CI: 1.24–8.19).
- Mechanical ventilation also remained independently associated with increased mortality (HR: 3.02; 95% CI: 1.16–7.60).
- PRISM score was not independently associated with mortality.
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| ALL | Acute Lymphoblastic Leukemia |
| AML | Acute Myeloid Leukemia |
| CI | Confidence Interval |
| ED HLH HR IQR KASCH KM NHL PRISM WHO |
Emergency Department Hemophagocytic Lymphohistiocytosis Hazard Ratio Interquartile Range King Abdullah Specialized Children’s Hospital Kaplan-Meier Non-Hodgkin Lymphoma Pediatric Risk of Mortality World Health Organization |
References
- Saudi Cancer Registry. Cancer Incidence Report Saudi Arabia. 2014. [Google Scholar]
- SEER Program Research Data, 1973–2017.
- Dalton, H.J.; Slonim, A.D.; Pollack, M.M. Multicenter outcome of pediatric oncology patients requiring intensive care. Pediatr. Hematol. Oncol. 2003, 20, 643–649. [Google Scholar] [CrossRef] [PubMed]
- Rosenman, M.B.; Vik, T.; Hui, S.L.; Breitfeld, P.P. Hospital resource utilization in childhood cancer. J. Pediatr. Hematol. Oncol. 2005, 27, 295–300. [Google Scholar] [CrossRef] [PubMed]
- Demaret, P.; Pettersen, G.; Hubert, P.; Teira, P.; Emeriaud, G. Critically ill pediatric hemato-oncology patients: epidemiology and PICU transfer strategy. Ann. Intensive Care 2012, 2, 14. [Google Scholar] [CrossRef] [PubMed]
- Zinter, M.S.; DuBois, S.G.; Spicer, A.; Matthay, K.; Sapru, A. Pediatric cancer type predicts critical care needs and mortality. Intensive Care Med. 2014, 40, 1536–1544. [Google Scholar] [CrossRef] [PubMed]
- Pollack, M.M.; et al. The ideal time interval for severity-of-illness assessment. Pediatr. Crit. Care Med. 2013, 14, 448–453. [Google Scholar] [CrossRef] [PubMed]
- Wösten-van Asperen, R.M.; et al. PICU mortality of children with cancer: systematic review and meta-analysis. Crit. Rev. Oncol. Hematol. 2019, 142, 153–163. [Google Scholar] [CrossRef] [PubMed]
- AlAbdullah, H.; et al. Post-HSCT outcomes in PICU: Saudi experience. Hematol. Oncol. Stem Cell Ther. 2024, 17, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Eschke, A.; et al. Clinical pathways for high-risk pediatric oncology patients. Front. Oncol. 2022, 12, 1033993. [Google Scholar]
- Hallahan, A.R.; et al. Improved outcomes of children with malignancy in PICU. Crit. Care Med. 2000, 28, 3718–3721. [Google Scholar] [CrossRef] [PubMed]
- Quintana, J.H.; et al. Mortality risk factors in hematologic neoplasms admitted to ICU. Curr. Oncol. 2025, 32, 132. [Google Scholar] [CrossRef] [PubMed]
- Ben Abraham, R.; et al. Predictors of outcome in PICU patients with malignancy. J. Pediatr. Hematol. Oncol. 2002, 24, 23–26. [Google Scholar] [CrossRef] [PubMed]
- Tamburro, R.F.; et al. Outcomes for oncology and HSCT patients requiring ventilation. Pediatr. Crit. Care Med. 2008, 9, 270–277. [Google Scholar] [CrossRef] [PubMed]
- Alabdulsalam, M.K.; et al. Clinical profiles and mortality risk factors in pediatric pulmonary hemorrhage. Ann. Saudi Med. 2025, 45, 235–242. [Google Scholar] [CrossRef] [PubMed]
| Clinical variables |
Total N=126 |
| Age, years (median [IQR]) | 6 (3-10) |
| Age categories | |
| <1 year | 11 (8.7) |
| 1–4 years | 46 (36.5) |
| >4 years | 69 (54.7) |
| Gender | |
| Male | 51 (40.4) |
| Female | 75 (59.5) |
| Sources of PICU admission | |
| Oncology ward | 72 (57.1) |
| Emergency department | 33 (26.1) |
| Others | 21 (16.6) |
| Presence of comorbidities | |
| No | 87 (69.0) |
| Yes | 39 (30.9) |
| Associated comorbidity (n=39) | |
| Genetic disease | 9 (7.1) |
| CNS disease | 6 (4.7) |
| Renal disease | 5 (3.9) |
| Gastrointestinal disease | 1 (0.7) |
| Rheumatological disease | 1 (0.7) |
| Immunological disease | 3 (2.3) |
| Endocrine disease | 2 (1.5) |
| Others | 12 (9.5) |
| Therapeutic interventions prior PICU admission | |
| No | 37 (29.3) |
| Yes | 89 (70.6) |
| Type of treatment received (n=89) | |
| Chemotherapy alone | 64 (71.9) |
| Chemotherapy + radiotherapy | 7 (7.8) |
| Chemotherapy + radiotherapy + Surgery | 5 (5.6) |
| Chemotherapy + Surgery | 4 (4.4) |
| Chemotherapy + targeted therapy | 3 (3.3) |
| Steroids | 2 (2.2) |
| Others | 4 (4.4) |
| Reason for admission | |
| Respiratory failure | 27 (21.4) |
| Sepsis | 52 (41.2) |
| Neurological deterioration | 7 (5.5) |
| Renal impairment | 2 (1.5) |
| Disease-related complication | 10 (7.9) |
| Therapy-related complication | 3 (2.3) |
| Disease progression | 5 (3.9) |
| Others | 20 (15.8) |
| Diagnosis of patients | ||||
| Outcome | Total (%) |
Hematologic malignancies 80 (63.4) |
Solid tumors 46 (36.5) |
P-value |
| Survival status | 0.183 | |||
| Survival | 101 (80.1) | 67 (83.7) | 34 (73.9) | |
| Non-survival | 25 (19.8) | 13 (16.2) | 12 (26.1) | |
| If non-survival | 0.848 | |||
| During the PICU admission | 13 (52.0) | 7 (53.8) | 6 (50.0) | |
| After to the PICU admission | 12 (48.0) | 6 (46.1) | 6 (50.0) | |
| Presence of organ failure during PICU admission | 0.778 | |||
| No | 76 (60.3) | 49 (61.2) | 27 (58.7) | |
| Yes | 50 (39.6) | 31 (38.7) | 19 (41.3) | |
| Number of organ failure during PICU admission* | 0.458 | |||
| 1 organ failure | 34 (68.0) | 20 (64.5) | 14 (73.6) | |
| 2 organ failure | 10 (20.0) | 5 (16.1) | 5 (26.3) | |
| 3 organ failure | 2 (4.0) | 2 (6.4) | 0 | |
| 4 organ failure | 1 (2.0) | 1 (3.2) | 0 | |
| 5 organ failure | 3 (6.0) | 3 (9.6) | 0 | |
| Mechanical ventilation use | 0.168 | |||
| No | 81 (64.2) | 55 (68.7) | 26 (56.5) | |
| Yes | 45 (35.7) | 25 (31.2) | 20 (43.4) | |
| Duration if MV used in days (median [IQR]) | 3 (2–7) | 5 (2–11) | 3 (1.5–4) | 0.244 |
| Positive inotropic support | 0.450 | |||
| No | 88 (69.8) | 54 (67.5) | 34 (73.9) | |
| Yes | 38 (30.1) | 26 (32.5) | 12 (26.1) | |
| Duration of inotropes use, days (median [IQR]) | 2 (2–4) | 2 (1–3) | 2 (2–5) | 0.443 |
| Use of dialysis during PICU admission | 0.139 | |||
| No | 118 (93.6) | 73 (91.2) | 45 (97.8) | |
| Yes | 8 (6.3) | 7 (8.7) | 1 (2.1) | |
| Duration of dialysis use | 3 (2.5–7) | 3 (2–7) | - | - |
| Pediatric Risk Score for Mortality (PRISM) | 15 (11–24) | 15 (12–26) | 15 (9–23) | 0.146 |
| PICU length of stay in days (median [IQR]) | 3 (2–7) | 3 (2-7) | 3 (2–7) | 0.930 |
| Variables |
Total N=126 |
Survival | p-value | |
| Survival N=101 | Non-survival N=25 | |||
| Age | 6 (3–10) | 7 (3–10) | 3.7 (2.9–9) | 0.285 |
| Gender | 0.957 | |||
| Male | 51 (40.4) | 41 (40.5) | 10 (40.0) | |
| Female | 75 (59.5) | 60 (59.4) | 15 (60.0) | |
| Presence of comorbidities | 0.039 | |||
| No | 87 (69.0) | 74 (73.2) | 13 (52.0) | |
| Yes | 39 (30.9) | 27 (26.7) | 12 (48.0) | |
| Therapeutic interventions prior PICU | 0.511 | |||
| No | 37 (29.3) | 31 (30.6) | 6 (24.0) | |
| Yes | 89 (70.6) | 70 (69.3) | 19 (76.0) | |
| Diagnosis of Patients_ recategorized | 0.183 | |||
| Hematologic malignancies | 80 (63.4) | 67 (66.3) | 13 (52.0) | |
| Solid tumors | 46 (36.5) | 34 (33.6) | 12 (48.0) | |
| Presence of organ failure during PICU admission | 0.063 | |||
| No | 76 (60.3) | 65 (64.3) | 11 (44.0) | |
| Yes | 50 (39.6) | 36 (35.6) | 14 (56.0) | |
| Mechanical ventilation use | <0.001 | |||
| No | 81 (64.2) | 75 (74.2) | 6 (24.0) | |
| Yes | 45 (35.7) | 26 (25.7) | 19 (76.0) | |
| Positive inotropic support | 0.008 | |||
| No | 88 (69.8) | 76 (72.2) | 12 (48.0) | |
| Yes | 38 (30.1) | 25 (24.7) | 13 (52.0) | |
| Length of stay in PICU, days | 3 (2–7) | 3 (2–7) | 6 (2–8) | 0.25 |
| Variables | HR (95% CI) | p-value | HR (95% CI)* | p-value |
| Age | 0.99 (0.90–1.10) | 0.977 | - | |
| Gender | ||||
| Male | 1 | |||
| Female | 1.10 (0.49–2.47) | 0.805 | ||
| Presence of comorbidities | ||||
| No | 1 | |||
| Yes | 2.10 (1.00–4.40) | 0.048 | 1.95 (0.89–4.22) | 0.091 |
| Therapeutic interventions prior PICU | ||||
| No | 1 | |||
| Yes | 2.70 (1.04–6.95) | 0.039 | 3.19 (1.24–8.19) | 0.016 |
| Diagnosis of Patients recategorized | ||||
| Hematologic malignancies | 1 | |||
| Solid tumors | 2.15 (0.95–4.87) | 0.066 | ||
| Presence of organ failure during PICU admission | ||||
| No | 1 | |||
| Yes | 1.27 (0.57–2.81) | 0.554 | ||
| Mechanical ventilation use | ||||
| No | 1 | |||
| Yes | 3.00 (1.22–7.39) | 0.016 | 2.97 (1.16–7.60) | 0.023 |
| Positive inotropic support | ||||
| No | 1 | |||
| Yes | 1.48 (0.66–3.30) | 0.350 | ||
| Pediatric Risk Score for Mortality (PRISM) | 1.04 (1.00–1.08) | 0.022 | 1.02 (0.98–1.06) | 0.262 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




