Submitted:
27 November 2025
Posted:
28 November 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Data Sources
2.3. Participants and Sample Selection
- Missing data on current ADHD or ASD diagnosis;
- Missing age or age outside the 3–17-year range;
- Missing values on key social determinants of interest (household income category, parental education, neighborhood safety);
- Missing design variables or sampling weights needed for survey analysis.
2.4. Variables and Measures
2.4.1. Outcomes
2.4.2. Predictors: Social Determinants of Health
- Household income was categorized relative to the federal poverty level (FPL) as <100% FPL, 100%–199% FPL, 200%–399% FPL, and ≥400% FPL, based on survey-derived income and family size.
- Parental education was defined as the highest educational attainment of any parent or guardian in the household and grouped as less than high school, high school diploma or equivalent, some college, and bachelor’s degree or higher.
- Health insurance type at the time of the survey was coded as private, public (Medicaid or Children’s Health Insurance Program), or uninsured.
- Food insecurity was defined from caregiver responses indicating that the household sometimes or often could not afford enough food in the past 12 months.
- Neighborhood safety was based on the question asking how safe the caregiver considers the neighborhood for children to play outside, with response options “definitely safe,” “somewhat safe,” and “not at all safe.” For primary analyses, we retained this three-level measure; in regression models, “definitely safe” served as the reference category.
2.4.3. Covariates
- Child age (continuous, in years);
- Sex (male, female);
- Race/ethnicity (non-Hispanic White, non-Hispanic Black, Hispanic, other, or multiracial);
- U.S. Census region (Northeast, Midwest, South, West);
- Family structure (two-parent household, single-parent household, other family arrangement);
- Survey year (2018, 2019, 2020, 2021, 2022, 2023).
2.5. Statistical Analyses
2.6. Ethical Approval
3. Results
3.1. Descriptive Statistics
3.2. Main Outcomes: Prevalence of ADHD and ASD
3.3. Regression Outcomes
3.4. Figures
3.5. Sensitivity Analyses
4. Discussion
4.1. Summary of Key Findings
4.2. Comparison with Existing Literature
4.3. Interpretation of Mechanisms and Implications
4.4. Strengths and Limitations
4.5. Policy Implications and Public Health Relevance
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Arlington, VA: American Psychiatric Association; 2013.
- Thapar, A.; Cooper, M. Attention deficit hyperactivity disorder. Lancet. 2016, 387, 1240–50. [Google Scholar] [CrossRef] [PubMed]
- Lord, C.; Elsabbagh, M.; Baird, G.; Veenstra-VanderWeele, J. Autism spectrum disorder. Lancet. 2018, 392, 508–20. [Google Scholar] [CrossRef] [PubMed]
- Global Burden of Disease Pediatrics Collaboration. Global and national burden of diseases and injuries among children and adolescents. JAMA Pediatr. 2016, 170, 267–87. [Google Scholar] [CrossRef] [PubMed]
- Health Resources and Services Administration; Maternal and Child Health Bureau. National Survey of Children’s Health (NSCH) 2018–2023 Methodology Reports. Rockville, MD: HRSA; 2019–2024.
- Zablotsky, B.; Black, L.I.; Maenner, M.J.; et al. Prevalence and trends of developmental disability in U.S. children, 2009–2017. Pediatrics. 2019, 144, e20190811. [Google Scholar] [CrossRef]
- Braveman, P.; Gottlieb, L. The social determinants of health: It’s time to consider the causes of the causes. Public Health Rep. 2014, 129 (Suppl 2), 19–31. [Google Scholar] [CrossRef]
- Shonkoff, J.P.; Garner, A.S. The lifelong effects of early childhood adversity and toxic stress. Pediatrics. 2012, 129, e232–46. [Google Scholar] [CrossRef]
- Pascoe, J.M.; Wood, D.L.; Duffee, J.H.; Kuo, A. Mediators and adverse effects of child poverty in the U.S. Pediatrics. 2016, 137, e20160340. [Google Scholar] [CrossRef]
- McLaughlin, K.A.; Sheridan, M.A.; Nelson, C.A. Biological sensitivity to context. Dev Psychopathol. 2017, 29, 1771–9. [Google Scholar]
- Danielson, M.L.; Bitsko, R.H.; Ghandour, R.M.; et al. ADHD prevalence and diagnosis patterns in U.S. children. J Clin Child Adolesc Psychol. 2018, 47, 199–212. [Google Scholar] [CrossRef]
- Caye, A.; Swanson, J.M.; Thapar, A.; et al. Life outcomes of ADHD: A systematic review. World Psychiatry. 2016, 15, 195–208. [Google Scholar]
- Kingsbury, M.; Weeks, M.; MacKinnon, N.; et al. Neighborhood influences on childhood mental health. Psychol Med. 2015, 45, 2733–47. [Google Scholar]
- Jaffee, S.R.; Christian, C.W. The biological embedding of childhood adversity. Child Dev. 2014, 85, 189–204. [Google Scholar]
- Mandell, D.S.; Novak, M.M.; Zubritsky, C.D. Factors associated with the age of autism diagnosis among minority children. Pediatrics. 2005, 116, e148–55. [Google Scholar] [CrossRef]
- Liptak, G.S.; Benzoni, L.B.; Mruzek, D.W.; et al. Disparities in the diagnosis of autism in children from minority communities. Pediatrics. 2008, 122, e120–6. [Google Scholar]
- Bitsko, R.H.; Holbrook, J.R.; Ghandour, R.M.; et al. Epidemiology and impact of ASD and ADHD among U.S. children. J Dev Behav Pediatr. 2018, 39, 732–41. [Google Scholar]
- Maenner, M.J.; Shaw, K.A.; Bakian, A.V.; et al. Prevalence of autism spectrum disorder among children aged 8 years—ADDM Network, 11 Sites, United States, 2018. MMWR Surveill Summ. 2021, 70, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Sheridan, M.A.; McLaughlin, K.A. Dimensions of childhood adversity and neural development. Curr Opin Pediatr. 2014, 26, 667–73. [Google Scholar]
- Visser, S.N.; Danielson, M.L.; Bitsko, R.H.; et al. Trends in ADHD diagnosis and treatment patterns. J Am Acad Child Adolesc Psychiatry. 2014, 53, 34–46. [Google Scholar] [CrossRef]
- Archer, K.J.; Lemeshow, S. Goodness-of-fit tests for logistic regression using survey design–adjusted procedures. Stata J. 2006, 6, 97–105. [Google Scholar] [CrossRef]
- Lambert, S.F.; Brown, T.L.; Phillips, C.M.; Ialongo, N.S. Neighborhood disadvantage and child mental health trajectories. Dev Psychol. 2004, 40, 635–49. [Google Scholar]
- Kalb, L.G.; Stuart, E.A.; Freedman, B.; Zablotsky, B. Race and ASD diagnosis timing in U.S. children. Intellect Dev Disabil. 2020, 58, 328–39. [Google Scholar]
- Durkin, M.S.; Maenner, M.J.; Baio, J.; et al. Autism and developmental disabilities among children by race/ethnicity. Am J Public Health. 2017, 107, 1818–26. [Google Scholar] [CrossRef]
- McDonnell, C.G.; Bradley, C.; Zuckerman, K.; et al. Barriers to early ASD diagnosis across pediatric populations. Acad Pediatr. 2019, 19, 909–17. [Google Scholar]
| Characteristic | Category | Weighted % | 95% CI |
|---|---|---|---|
| Sex | Male | 51.2 | 50.4–52.0 |
| Female | 48.8 | 48.0–49.6 | |
| Race/Ethnicity | Non-Hispanic White | 50.8 | 49.6–52.0 |
| Non-Hispanic Black | 13.6 | 12.9–14.3 | |
| Hispanic | 24.1 | 23.1–25.1 | |
| Other/Multiracial | 11.5 | 10.8–12.2 | |
| Household Income (% FPL) | <100% FPL | 19.7 | 18.6–20.8 |
| 100–199% FPL | 25.4 | 24.2–26.6 | |
| 200–399% FPL | 31.8 | 30.4–33.2 | |
| ≥400% FPL | 23.1 | 22.0–24.3 | |
| Parental Education | <High school | 9.5 | 8.8–10.2 |
| High school diploma | 29.1 | 28.0–30.3 | |
| Some college | 27.6 | 26.4–28.8 | |
| Bachelor’s or higher | 33.8 | 32.4–35.2 | |
| Insurance Type | Private | 54.2 | 53.0–55.4 |
| Public | 38.5 | 37.2–39.8 | |
| Uninsured | 7.3 | 6.8–7.9 | |
| Neighborhood Safety | Definitely safe | 70.1 | 69.1–71.2 |
| Somewhat safe | 25.8 | 24.7–26.9 | |
| Not safe | 4.1 | 3.7–4.6 | |
| Food Insecurity | Yes | 10.8 | 10.1–11.6 |
| No | 89.2 | 88.4–90.0 |
| Determinant | Category | ADHD % (95% CI) | ASD % (95% CI) |
|---|---|---|---|
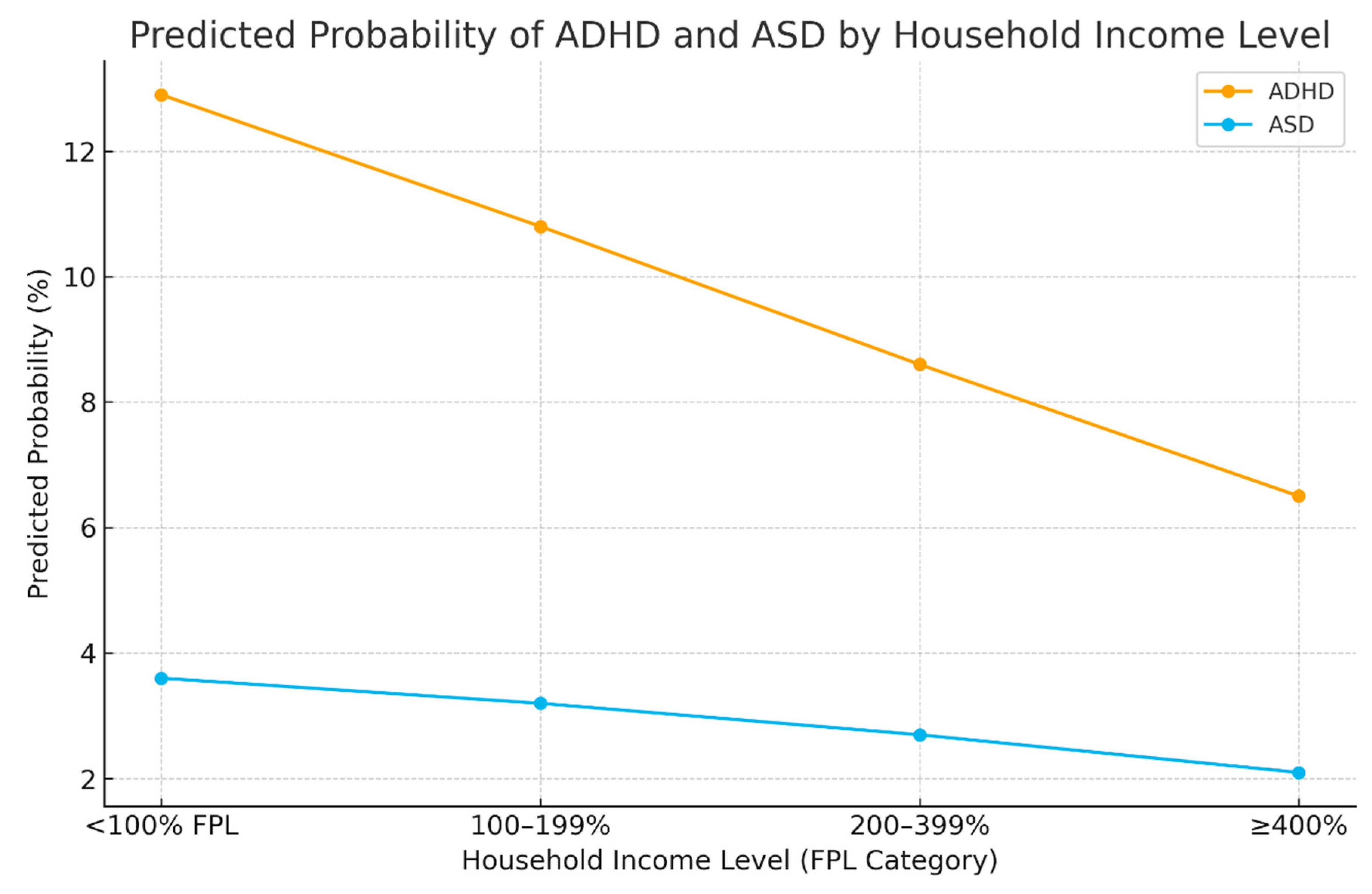
| Household Income (% FPL) | <100% FPL | 13.4 (12.1–14.7) | 3.8 (3.1–4.5) |
| 100–199% FPL | 10.8 (9.8–11.8) | 3.2 (2.6–3.8) | |
| 200–399% FPL | 8.6 (7.8–9.4) | 2.7 (2.3–3.1) | |
| ≥400% FPL | 6.2 (5.6–6.8) | 2.0 (1.7–2.3) | |
| Parental Education | <High school | 14.6 (12.8–16.4) | 3.9 (3.1–4.7) |
| High school diploma | 11.2 (10.1–12.3) | 3.3 (2.7–3.9) | |
| Some college | 9.0 (8.1–9.9) | 2.7 (2.3–3.1) | |
| Bachelor’s or higher | 6.8 (6.1–7.5) | 2.1 (1.8–2.4) | |
| Insurance Type | Private | 8.1 (7.5–8.7) | 2.4 (2.1–2.7) |
| Public | 13.2 (12.0–14.4) | 3.8 (3.2–4.4) | |
| Uninsured | 10.5 (8.4–12.6) | 2.6 (1.8–3.4) | |
| Neighborhood Safety | Definitely safe | 8.9 (8.3–9.5) | 2.5 (2.2–2.8) |
| Somewhat safe | 12.5 (11.3–13.7) | 3.4 (2.8–4.0) | |
| Not safe | 15.8 (13.0–18.6) | 4.4 (3.0–5.8) | |
| Food Insecurity | Yes | 14.9 (13.2–16.6) | 4.1 (3.4–4.9) |
| No | 8.8 (8.3–9.3) | 2.7 (2.4–3.0) |
| Determinant | Category | ADHD aOR (95% CI) | ASD aOR (95% CI) |
|---|---|---|---|
| Household Income (% FPL) | <100% FPL | 2.11 (1.82–2.46) | 1.73 (1.32–2.28) |
| 100–199% FPL | 1.69 (1.46–1.95) | 1.32 (1.04–1.67) | |
| 200–399% FPL | 1.28 (1.12–1.45) | 1.14 (0.92–1.40) | |
| ≥400% FPL (ref) | 1.00 | 1.00 | |
| Parental Education | <High school | 1.83 (1.52–2.20) | 1.46 (1.12–1.91) |
| High school diploma | 1.42 (1.26–1.60) | 1.28 (1.01–1.63) | |
| Some college | 1.21 (1.07–1.36) | 1.10 (0.88–1.37) | |
| Bachelor’s or higher (ref) | 1.00 | 1.00 | |
| Insurance Type | Public | 1.37 (1.20–1.55) | 1.21 (0.98–1.49) |
| Uninsured | 1.18 (0.95–1.47) | 1.05 (0.72–1.52) | |
| Private (ref) | 1.00 | 1.00 | |
| Neighborhood Safety | Somewhat safe | 1.31 (1.15–1.50) | 1.24 (0.97–1.59) |
| Not safe | 1.94 (1.51–2.49) | 1.79 (1.21–2.64) | |
| Definitely safe (ref) | 1.00 | 1.00 | |
| Food Insecurity | Yes | 1.88 (1.60–2.21) | 1.61 (1.18–2.19) |
| No (ref) | 1.00 | 1.00 | |
| Child Sex | Male | 2.39 (2.12–2.68) | 3.84 (3.13–4.72) |
| Female (ref) | 1.00 | 1.00 | |
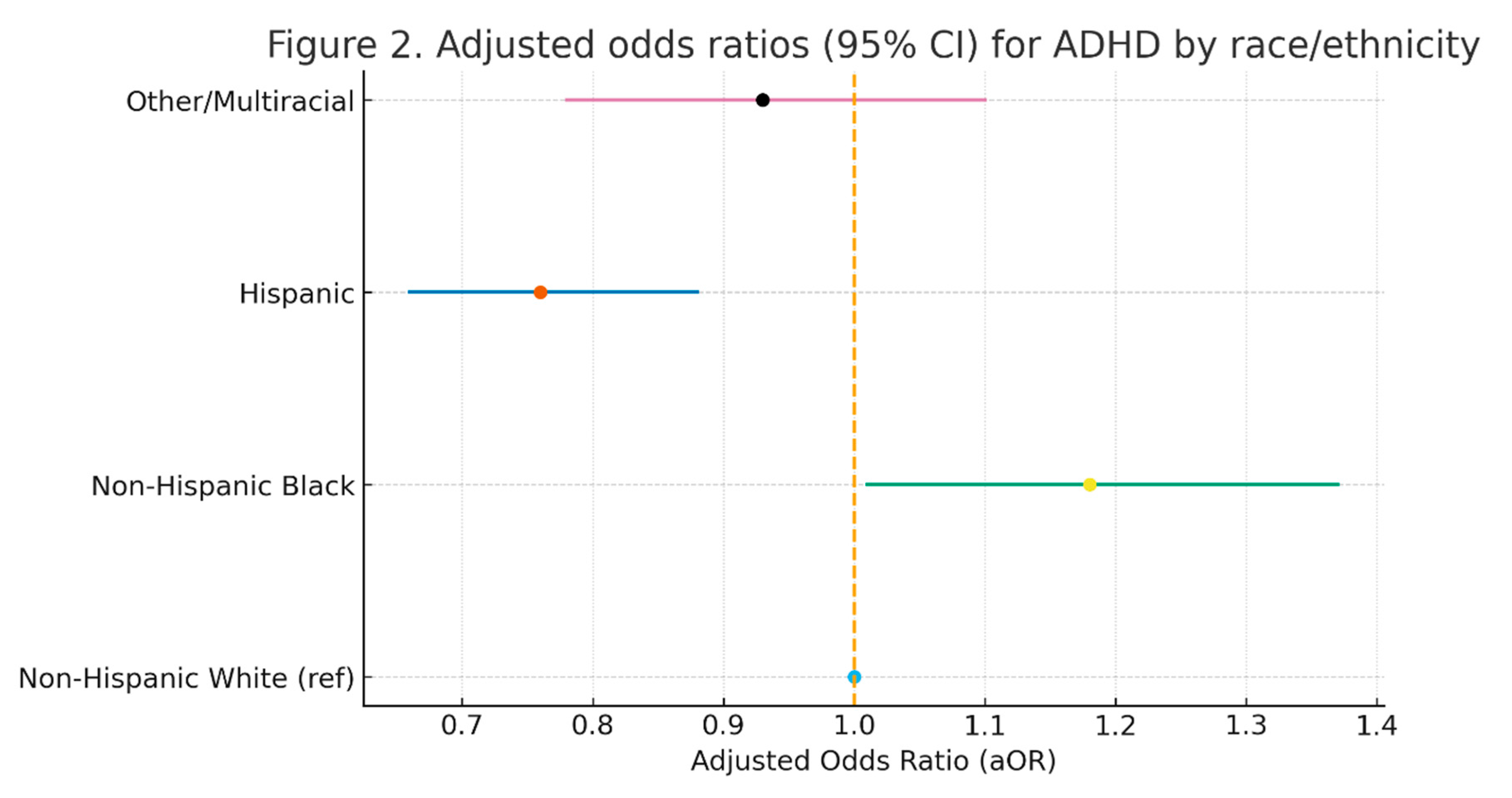
| Race/Ethnicity | Non-Hispanic Black | 1.18 (1.01–1.37) | 0.64 (0.51–0.80) |
| Hispanic | 0.76 (0.66–0.88) | 0.59 (0.47–0.73) | |
| Other/Multiracial | 0.93 (0.78–1.10) | 0.82 (0.64–1.06) | |
| Non-Hispanic White (ref) | 1.00 | 1.00 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




