Submitted:
26 November 2025
Posted:
27 November 2025
You are already at the latest version
Abstract
Lactococcus lactis, a safe food-grade lactic acid bacterium, has attracted increasing attention as a live biotherapeutic platform for mucosal vaccine development. Its genetic simplicity, absence of endotoxins, and availability of well-characterized inducible systems have enabled controlled expression and delivery of heterologous antigens and therapeutic molecules. This review highlights recent advances in the use of genetically modified L. lactis for mucosal immunization, focusing on expression technologies, routes of administration, and immune mechanisms relevant to protection or tolerance. Preclinical studies demonstrate its capacity to induce both mucosal and systemic immune responses against diverse pathogens, underscoring its potential as a safe and versatile vaccine chassis. Remaining challenges include regulatory harmonization, biosafety concerns, and the need for standardized manufacturing and evaluation frameworks. Together, these developments position L. lactis as a promising candidate for next-generation mucosal vaccines and live biotherapeutic products.
Keywords:
1. Introduction
2. Advantages of Lactococcus lactis for Its Application in LBPs
3. Conventional Method Used to Express Antigen Expression in L. lactis
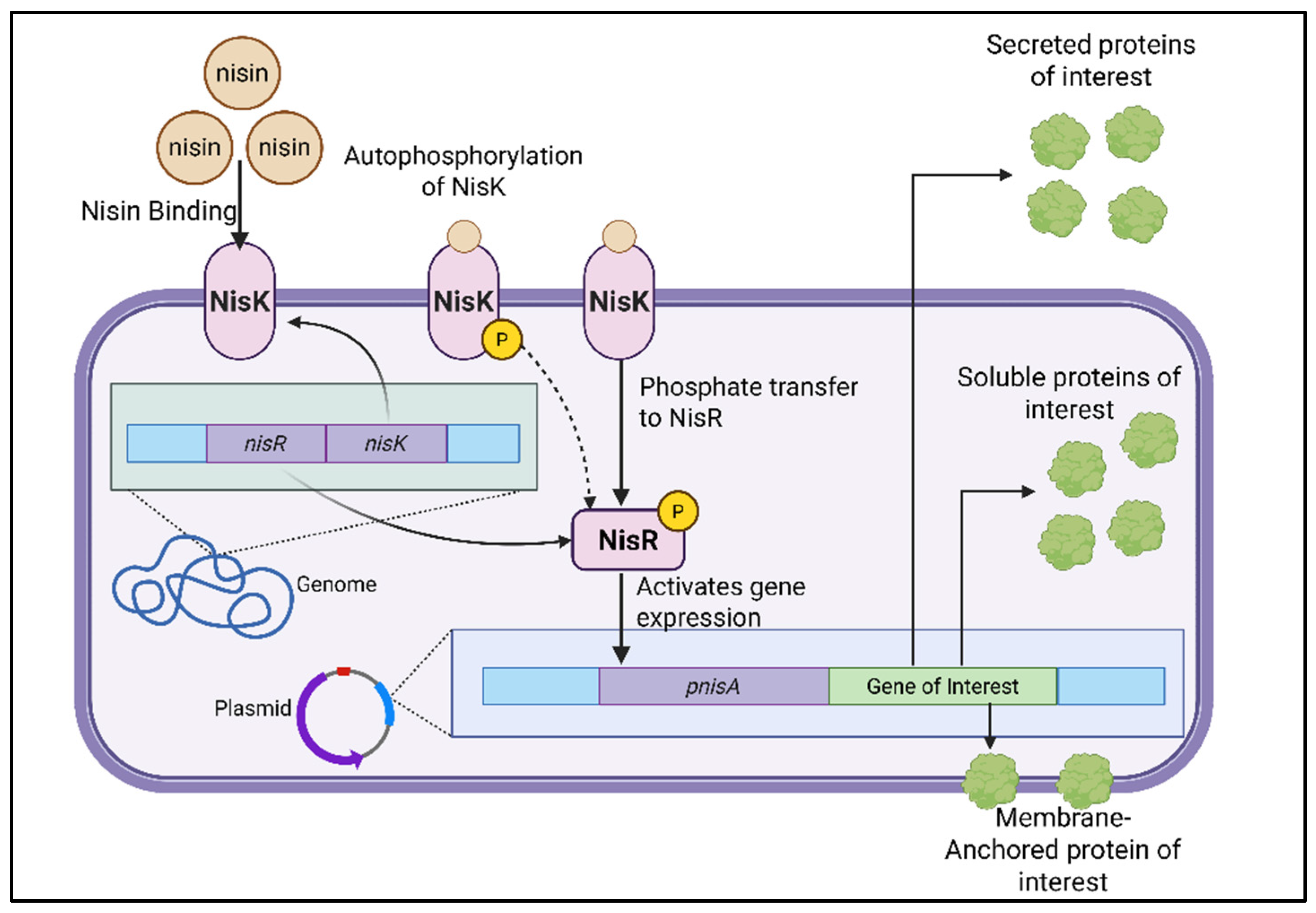
3.1. Nisin-Controlled Gene Expression (NICE)
3.2. Xylose Inducible Expression System (XIES)
3.3. Zinc Induced Systems
3.4. Stress Induces Controlled Expression System (SICE)
4. Routes of Administration
4.1. Oral Administration
4.2. Nasal Administration
4.3. Other Routes od Administration
5. Oral Vaccine Prototypes on L. lactis
5.1. Viral Vaccines
5.2. Bacteria Vaccines
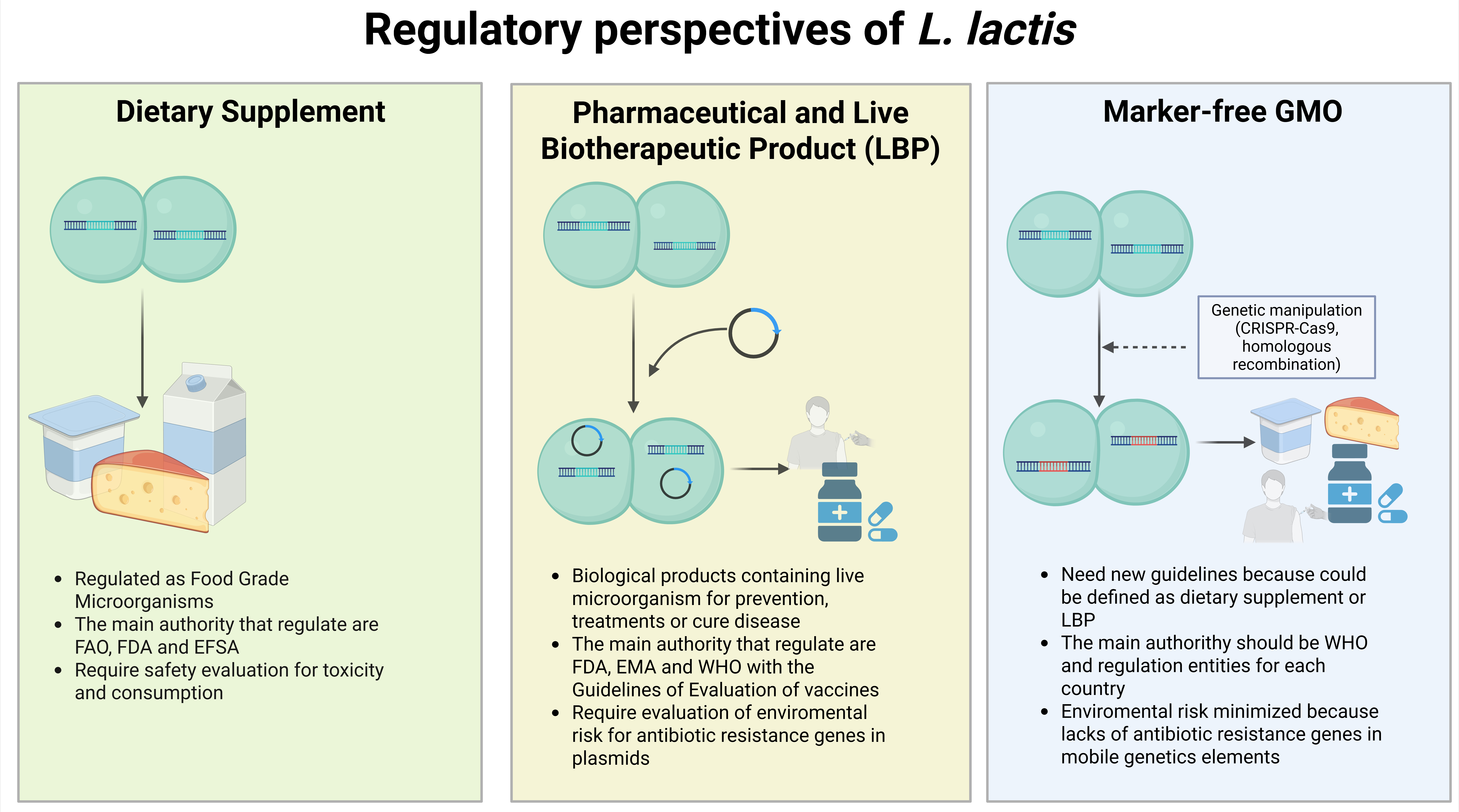
6. Probiotic, Vaccine, or Drug? Regulations, New Technologies, and Solutions
7. Learnings and New Perspectives
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| APCs | Antigen-Presenting Cells |
| BALT | Bronchus-Associated Lymphoid Tissue |
| BAL | Bronchoalveolar Lavage |
| CD | Cluster of Differentiation (CD4, CD8, etc.) |
| CFU | Colony-Forming Units |
| CTL | Cytotoxic T Lymphocyte |
| CTLA-4 | Cytotoxic T-Lymphocyte Antigen 4 |
| DCs | Dendritic Cells |
| EPA | Environmental Protection Agency |
| FDA | Food and Drug Administration |
| GALT | Gut-Associated Lymphoid Tissue |
| GFP | Green Fluorescent Protein |
| GMOs | Genetically Modified Organisms |
| GOALTs | Genital Organ-Associated Lymphoid Tissues |
| GRAS | Generally Recognized As Safe |
| GST | Glutathione-S-Transferase |
| HA | Hemagglutinin |
| HBV | Hepatitis B Virus |
| HBsAg | Hepatitis B Surface Antigen |
| HCR | Highly Conserved Region |
| HIV | Human Immunodeficiency Virus |
| HPV | Human Papillomavirus |
| IL | Interleukin |
| IRCT | Iranian Registry of Clinical Trials |
| LBPs | Live Biotherapeutic Products |
| LPS | Lipopolysaccharide |
| LTB | Heat-Labile Toxin Subunit B |
| MALT | Mucosa-Associated Lymphoid Tissue |
| MHC | Major Histocompatibility Complex |
| NALT | Nasal-Associated Lymphoid Tissue |
| NICE | Nisin-Controlled Gene Expression system |
| OD | Optical Density |
| PnisA | Nisin-Inducible Promoter A |
| PppA | Pneumococcal Protective Protein A |
| PxylT | Xylose-Inducible Promoter |
| BD | Receptor-Binding Domain |
| RPS | Relative Percent Survival |
| SALT | Skin-Associated Lymphoid Tissue |
| SARS | Severe Acute Respiratory Syndrome |
| SICE | Stress-Inducible Controlled Expression system |
| SIgA | Secretory Immunoglobulin A |
| SIP | Surface Immunogenic Protein |
| TcdA | Clostridioides difficile Toxin A |
| TcdB | Clostridioides difficile Toxin B |
| Tregs | Regulatory T Cells |
| Usp45 | Universal Stress Protein 45 (signal peptide) |
| VLPs | Virus-Like Particles |
| WHO | World Health Organization |
| XIES | Xylose-Inducible Expression System |
| ZICE | Zinc-Controlled Expression system |
| Zirex | Zinc-Inducible Regulatory Expression system |
References
- C. Hill et al., “The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic,” Nat Rev Gastroenterol Hepatol, vol. 11, no. 8, pp. 506–514, Aug. 2014. [CrossRef]
- Food and Agriculture Organization of the United Nations and World Health Organization, “Probiotics in food: Health and nutritional properties and guidelines for evaluation,” Rome, 2006. Accessed: Nov. 11, 2025. [Online]. Available: https://openknowledge.fao.org/items/1c836817-9be2-4256-83ae-0b5055039b50.
- M. Naissinger da Silva, B. L. Tagliapietra, V. do A. Flores, and N. S. Pereira dos Santos Richards, “In vitro test to evaluate survival in the gastrointestinal tract of commercial probiotics,” Curr Res Food Sci, vol. 4, pp. 320–325, 2021. [CrossRef]
- M. L. Marco et al., “Health benefits of fermented foods: microbiota and beyond,” Curr Opin Biotechnol, vol. 44, pp. 94–102, Apr. 2017. [CrossRef]
- K. G. de C. Lima, M. F. Kruger, J. Behrens, M. T. Destro, M. Landgraf, and B. D. Gombossy de Melo Franco, “Evaluation of culture media for enumeration of Lactobacillus acidophilus, Lactobacillus casei and Bifidobacterium animalis in the presence of Lactobacillus delbrueckii subsp bulgaricus and Streptococcus thermophilus,” LWT - Food Science and Technology, vol. 42, no. 2, pp. 491–495, Mar. 2009. [CrossRef]
- U. Hynönen and A. Palva, “Lactobacillus surface layer proteins: structure, function and applications,” Appl Microbiol Biotechnol, vol. 97, no. 12, pp. 5225–5243, Jun. 2013. [CrossRef]
- M. Saxelin, S. Tynkkynen, T. Mattila-Sandholm, and W. M. de Vos, “Probiotic and other functional microbes: from markets to mechanisms,” Curr Opin Biotechnol, vol. 16, no. 2, pp. 204–211, Apr. 2005. [CrossRef]
- J. Plaza-Diaz, F. J. Ruiz-Ojeda, M. Gil-Campos, and A. Gil, “Mechanisms of Action of Probiotics,” Advances in Nutrition, vol. 10, pp. S49–S66, Jan. 2019. [CrossRef]
- M. E. Sanders, D. J. Merenstein, G. Reid, G. R. Gibson, and R. A. Rastall, “Probiotics and prebiotics in intestinal health and disease: from biology to the clinic,” Nat Rev Gastroenterol Hepatol, vol. 16, no. 10, pp. 605–616, Oct. 2019. [CrossRef]
- J. Zhou et al., “Programmable probiotics modulate inflammation and gut microbiota for inflammatory bowel disease treatment after effective oral delivery,” Nat Commun, vol. 13, no. 1, p. 3432, Jun. 2022. [CrossRef]
- K. Jin, Y. Huang, H. Che, and Y. Wu, “Engineered Bacteria for Disease Diagnosis and Treatment Using Synthetic Biology,” Microb Biotechnol, vol. 18, no. 1, Jan. 2025. [CrossRef]
- L. G. Bermúdez-Humarán and P. Langella, “Use of Traditional and Genetically Modified Probiotics in Human Health: What Does the Future Hold?,” Microbiol Spectr, vol. 5, no. 5, Sep. 2017. [CrossRef]
- U.S. Food and Drug Administration, “Early Clinical Trials with Live Biotherapeutic Products: Chemistry, Manufacturing, and Control Information. Guidance for Industry,” Silver Spring, MD, Sep. 2003. Accessed: Nov. 11, 2025. [Online]. Available: https://www.fda.gov/regulatory-information/search-fda-guidance-documents/early-clinical-trials-live-biotherapeutic-products-chemistry-manufacturing-and-control-information.
- D. Barberio, “Navigating regulatory and analytical challenges in live biotherapeutic product development and manufacturing,” Frontiers in Microbiomes, vol. 3, Aug. 2024. [CrossRef]
- S. Pan, J.-C. Hsu, K.-T. Hung, and C.-J. Ho, “Regulatory framework and challenges for live biotherapeutic products in Taiwan,” J Food Drug Anal, vol. 33, no. 2, pp. 97–105, Jun. 2025. [CrossRef]
- M. R. Charbonneau, V. M. Isabella, N. Li, and C. B. Kurtz, “Developing a new class of engineered live bacterial therapeutics to treat human diseases,” Nat Commun, vol. 11, no. 1, p. 1738, Apr. 2020. [CrossRef]
- J. L. Owen, B. Sahay, and M. Mohamadzadeh, “New generation of oral mucosal vaccines targeting dendritic cells,” Curr Opin Chem Biol, vol. 17, no. 6, pp. 918–924, 2013. [CrossRef]
- J. E. Vela Ramirez, L. A. Sharpe, and N. A. Peppas, “Current state and challenges in developing oral vaccines,” Adv Drug Deliv Rev, vol. 114, pp. 116–131, 2017. [CrossRef]
- A. A. L. Song, L. L. A. In, S. H. E. Lim, and R. A. Rahim, “A review on Lactococcus lactis: From food to factory,” Microb Cell Fact, vol. 16, no. 1, pp. 1–15, 2017. [CrossRef]
- A. Bolotin et al., “The Complete Genome Sequence of the Lactic Acid Bacterium Lactococcus lactis ssp. lactis IL1403,” Genome Res, vol. 11, no. 5, pp. 731–753, May 2001. [CrossRef]
- D. M. Linares, J. Kok, and B. Poolman, “Genome Sequences of Lactococcus lactis MG1363 (Revised) and NZ9000 and Comparative Physiological Studies,” J Bacteriol, vol. 192, no. 21, pp. 5806–5812, Nov. 2010. [CrossRef]
- L. G. Bermúdez-Humarán, “Lactococcus lactis as a live vector for mucosal delivery of therapeutic proteins,” Hum Vaccin, vol. 5, no. 4, pp. 264–267, 2009. [CrossRef]
- K. H. Schleifer, J. Kraus, C. Dvorak, R. Kilpper-Bälz, M. D. Collins, and W. Fischer, “Transfer of Streptococcus lactis and Related Streptococci to the Genus Lactococcus gen. nov.,” Syst Appl Microbiol, vol. 6, no. 2, pp. 183–195, Sep. 1985. [CrossRef]
- M. J. Gasson, “Plasmid complements of Streptococcus lactis NCDO 712 and other lactic streptococci after protoplast-induced curing,” J Bacteriol, vol. 154, no. 1, pp. 1–9, Apr. 1983. [CrossRef]
- B. Daniel, S. Poiret, V. Dennin, D. Boutillier, and B. Pot, “Bioluminescence imaging study of spatial and temporal persistence of Lactobacillus plantarum and Lactococcus lactis in living mice,” Appl Environ Microbiol, vol. 79, no. 4, pp. 1086–1094, 2013. [CrossRef]
- T. Vesa, P. Pochart, and P. Marteau, “Pharmacokinetics of Lactobacillus plantarum NCIMB 8826, Lactobacillus fermentum KLD, and Lactococcus lactis MG 1363 in the human gastrointestinal tract,” 2000. [CrossRef]
- T. D. Wallace, S. Bradley, N. D. Buckley, and J. M. Green-Johnson, “Interactions of Lactic Acid Bacteria with Human Intestinal Epithelial Cells: Effects on Cytokine Production,” J Food Prot, vol. 66, no. 3, pp. 466–472, Mar. 2003. [CrossRef]
- B. P. Frossard, L. Steidler, and P. A. Eigenmann, “Oral administration of an IL-10–secreting Lactococcus lactis strain prevents food-induced IgE sensitization,” Journal of Allergy and Clinical Immunology, vol. 119, no. 4, pp. 952–959, Apr. 2007. [CrossRef]
- X. Peng et al., “Production and delivery of Helicobacter pylori NapA in Lactococcus lactis and its protective efficacy and immune modulatory activity,” Sci Rep, vol. 8, no. 1, p. 6435, Apr. 2018. [CrossRef]
- S. Taghinezhad-S, H. Keyvani, L. G. Bermúdez-Humarán, G. G. G. Donders, X. Fu, and A. H. Mohseni, “Twenty years of research on HPV vaccines based on genetically modified lactic acid bacteria: an overview on the gut-vagina axis,” Cellular and Molecular Life Sciences, vol. 78, no. 4, pp. 1191–1206, 2021. [CrossRef]
- M. Bahey-El-Din, P. G. Casey, B. T. Griffin, and C. G. M. Gahan, “Lactococcus lactis-expressing listeriolysin O (LLO) provides protection and specific CD8+ T cells against Listeria monocytogenes in the murine infection model,” Vaccine, vol. 26, no. 41, pp. 5304–5314, Sep. 2008. [CrossRef]
- K. K. Yam, P. Pouliot, M. M. N’diaye, S. Fournier, M. Olivier, and B. Cousineau, “Innate inflammatory responses to the Gram-positive bacterium Lactococcus lactis,” Vaccine, vol. 26, no. 22, pp. 2689–2699, May 2008. [CrossRef]
- M. Medina, E. Vintiñi, J. Villena, R. Raya, and S. Alvarez, “Lactococcus lactis as an adjuvant and delivery vehicle of antigens against pneumococcal respiratory infections,” Bioeng Bugs, vol. 1, no. 5, pp. 313–325, 2010. [CrossRef]
- I. Mierau and M. Kleerebezem, “10 years of the nisin-controlled gene expression system (NICE) in Lactococcus lactis,” Appl Microbiol Biotechnol, vol. 68, no. 6, pp. 705–717, Oct. 2005. [CrossRef]
- P. G. de Ruyter, O. P. Kuipers, M. M. Beerthuyzen, I. van Alen-Boerrigter, and W. M. de Vos, “Functional analysis of promoters in the nisin gene cluster of Lactococcus lactis,” J Bacteriol, vol. 178, no. 12, pp. 3434–3439, Jun. 1996. [CrossRef]
- Food and Drug Administration, “Nisin Preparation; Affirmation of GRAS Status as a Direct Human Food Ingredient,” Washington, DC, Apr. 1988. Accessed: Nov. 11, 2025. [Online]. Available: https://hfpappexternal.fda.gov/scripts/fdcc/index.cfm?set=FinalRules&id=53FR11247.
- I. Mierau, K. Olieman, J. Mond, and E. J. Smid, “Optimization of the Lactococcus lactis nisin-controlled gene expression system NICE for industrial applications,” Microb Cell Fact, vol. 4, no. 1, p. 16, Dec. 2005. [CrossRef]
- A. P. KUIPERS, M. M. BEERTHUYZEN, R. J. SIEZEN, and W. M. DE VOS, “Characterization of the nisin gene cluster nisABTCIPR of Lactococcus lactis,” Eur J Biochem, vol. 216, no. 1, pp. 281–291, Aug. 1993. [CrossRef]
- A. P. Kuipers, P. G. G. A. de Ruyter, M. Kleerebezem, and W. M. de Vos, “Quorum sensing-controlled gene expression in lactic acid bacteria,” J Biotechnol, vol. 64, no. 1, pp. 15–21, Sep. 1998. [CrossRef]
- MoBiTec GmbH, “NICE expression system: Handbook for Lactococcus lactis expression system,” Goettingen, Mar. 2015. Accessed: Nov. 11, 2025. [Online]. Available: https://www.mobitec.com/media/mobitec/old_content/NICE_Expression_System-Handbook.pdf.
- S. Bakari, F. André, D. Seigneurin-Berny, M. Delaforge, N. Rolland, and A. Frelet-Barrand, “Lactococcus lactis: Recent Developments in Functional Expression of Membrane Proteins,” in Membrane Proteins Production for Structural Analysis, New York, NY: Springer New York, 2014, pp. 107–132. [CrossRef]
- A. Miyoshi, E. Jamet, J. Commissaire, P. Renault, P. Langella, and V. Azevedo, “A xylose-inducible expression system for Lactococcus lactis,” FEMS Microbiol Lett, vol. 239, no. 2, pp. 205–212, Oct. 2004. [CrossRef]
- Y. Miwa, “Evaluation and characterization of catabolite-responsive elements (cre) of Bacillus subtilis,” Nucleic Acids Res, vol. 28, no. 5, pp. 1206–1210, Mar. 2000. [CrossRef]
- M. van Asseldonk, W. M. de Vos, and G. Simons, “Functional analysis of the Lactococcus lactis usp45 secretion signal in the secretion of a homologous proteinase and a heterologous α-amylase,” Mol Gen Genet, vol. 240, no. 3, pp. 428–434, Sep. 1993. [CrossRef]
- I. Poquet, S. D. Ehrlich, and A. Gruss, “An Export-Specific Reporter Designed for Gram-Positive Bacteria: Application to Lactococcus lactis,” J Bacteriol, vol. 180, no. 7, pp. 1904–1912, Apr. 1998. [CrossRef]
- B. P. de Castro, M. M. Drumond, V. L. Batista, A. Nunes, P. Mancha-Agresti, and V. Azevedo, “Vector Development Timeline for Mucosal Vaccination and Treatment of Disease Using Lactococcus lactis and Design Approaches of Next Generation Food Grade Plasmids,” Front Microbiol, vol. 9, Aug. 2018. [CrossRef]
- B. Llull and I. Poquet, “New Expression System Tightly Controlled by Zinc Availability in Lactococcus lactis,” Appl Environ Microbiol, vol. 70, no. 9, pp. 5398–5406, Sep. 2004. [CrossRef]
- D. Mu, M. Montalb�n-L�pez, Y. Masuda, and O. P. Kuipers, “Zirex: a Novel Zinc-Regulated Expression System for Lactococcus lactis,” Appl Environ Microbiol, vol. 79, no. 14, pp. 4503–4508, Jul. 2013. [CrossRef]
- X. Xu, L. Zhang, Y. Cui, J. Kong, and T. Guo, “Development of Zn2+-controlled expression system for lactic acid bacteria and its application in engineered probiotics,” Synth Syst Biotechnol, vol. 9, no. 1, pp. 152–158, Mar. 2024. [CrossRef]
- B. Benbouziane et al., “Development of a Stress-Inducible Controlled Expression (SICE) system in Lactococcus lactis for the production and delivery of therapeutic molecules at mucosal surfaces,” J Biotechnol, vol. 168, no. 2, pp. 120–129, Oct. 2013. [CrossRef]
- H. M. Fischer, M. Babst, T. Kaspar, G. Acuña, F. Arigoni, and H. Hennecke, “One member of a gro-ESL-like chaperonin multigene family in Bradyrhizobium japonicum is co-regulated with symbiotic nitrogen fixation genes.,” EMBO J, vol. 12, no. 7, pp. 2901–2912, Jul. 1993. [CrossRef]
- S. M. Kristoffersen, S. Ravnum, N. J. Tourasse, O. A. Økstad, A.-B. Kolstø, and W. Davies, “Low Concentrations of Bile Salts Induce Stress Responses and Reduce Motility in Bacillus cereus ATCC 14570,” J Bacteriol, vol. 189, no. 14, pp. 5302–5313, Jul. 2007. [CrossRef]
- B. Jacouton et al., “Anti-tumoral Effects of Recombinant Lactococcus lactis Strain Secreting IL-17A Cytokine,” Front Microbiol, vol. 9, Jan. 2019. [CrossRef]
- U. Müh, A. G. Pannullo, D. S. Weiss, and C. D. Ellermeier, “A Xylose-Inducible Expression System and a CRISPR Interference Plasmid for Targeted Knockdown of Gene Expression in Clostridioides difficile,” J Bacteriol, vol. 201, no. 14, Jul. 2019. [CrossRef]
- C. Kiyono and S. Fukuyama, “NALT- versus PEYER’S-patch-mediated mucosal immunity,” Nat Rev Immunol, vol. 4, no. 9, pp. 699–710, Sep. 2004. [CrossRef]
- J. Holmgren and C. Czerkinsky, “Mucosal immunity and vaccines,” Nat Med, vol. 11, no. S4, pp. S45–S53, Apr. 2005. [CrossRef]
- R. Anggraeni, I. D. Ana, and H. Wihadmadyatami, “Development of mucosal vaccine delivery: an overview on the mucosal vaccines and their adjuvants,” Clin Exp Vaccine Res, vol. 11, no. 3, p. 235, 2022. [CrossRef]
- N. Qiao, G. Du, X. Zhong, and X. Sun, “Recombinant lactic acid bacteria as promising vectors for mucosal vaccination,” Exploration, vol. 1, no. 2, Oct. 2021. [CrossRef]
- K. W.-Y. Kwong et al., “Oral Vaccines: A Better Future of Immunization,” Vaccines (Basel), vol. 11, no. 7, p. 1232, Jul. 2023. [CrossRef]
- S. J. Challacombe, D. Rahman, and D. T. O’Hagan, “Salivary, gut, vaginal and nasal antibody responses after oral immunization with biodegradable microparticles,” Vaccine, vol. 15, no. 2, pp. 169–175, Feb. 1997. [CrossRef]
- K. Szatraj, A. K. Szczepankowska, and M. Chmielewska-Jeznach, “Lactic acid bacteria — promising vaccine vectors: possibilities, limitations, doubts,” J Appl Microbiol, vol. 123, no. 2, pp. 325–339, Aug. 2017. [CrossRef]
- E. Wambre and D. Jeong, “Oral Tolerance Development and Maintenance,” Immunol Allergy Clin North Am, vol. 38, no. 1, pp. 27–37, Feb. 2018. [CrossRef]
- Z. Chen et al., “FOXP3 and RORγt: Transcriptional regulation of Treg and Th17,” Int Immunopharmacol, vol. 11, no. 5, pp. 536–542, May 2011. [CrossRef]
- D. A. A. Vignali, L. W. Collison, and C. J. Workman, “How regulatory T cells work,” Nat Rev Immunol, vol. 8, no. 7, pp. 523–532, Jul. 2008. [CrossRef]
- L. Qin et al., “Unraveling the role of Ctla-4 in intestinal immune homeostasis through a novel Zebrafish model of inflammatory bowel disease,” Elife, vol. 13, May 2025. [CrossRef]
- M. Jutel et al., “IL-10 and TGF-β cooperate in the regulatory T cell response to mucosal allergens in normal immunity and specific immunotherapy,” Eur J Immunol, vol. 33, no. 5, pp. 1205–1214, May 2003. [CrossRef]
- A. Taylor, J. Verhagen, K. Blaser, M. Akdis, and C. A. Akdis, “Mechanisms of immune suppression by interleukin-10 and transforming growth factor-β: the role of T regulatory cells,” Immunology, vol. 117, no. 4, pp. 433–442, Apr. 2006. [CrossRef]
- C. H. Uhlig et al., “Characterization of Foxp3+CD4+CD25+ and IL-10-Secreting CD4+CD25+ T Cells during Cure of Colitis,” The Journal of Immunology, vol. 177, no. 9, pp. 5852–5860, Nov. 2006. [CrossRef]
- L. M. Williams, G. Ricchetti, U. Sarma, T. Smallie, and B. M. J. Foxwell, “Interleukin-10 suppression of myeloid cell activation — a continuing puzzle,” Immunology, vol. 113, no. 3, pp. 281–292, Nov. 2004. [CrossRef]
- S.-G. Park et al., “T Regulatory Cells Maintain Intestinal Homeostasis by Suppressing γδ T Cells,” Immunity, vol. 33, no. 5, pp. 791–803, Nov. 2010. [CrossRef]
- Y.-J. Heo et al., “IL-10 suppresses Th17 cells and promotes regulatory T cells in the CD4+ T cell population of rheumatoid arthritis patients,” Immunol Lett, vol. 127, no. 2, pp. 150–156, Jan. 2010. [CrossRef]
- D. Jankovic, D. G. Kugler, and A. Sher, “IL-10 production by CD4+ effector T cells: a mechanism for self-regulation,” Mucosal Immunol, vol. 3, no. 3, pp. 239–246, May 2010. [CrossRef]
- K. G. Schmetterer and W. F. Pickl, “The IL–10/STAT3 axis: Contributions to immune tolerance by thymus and peripherally derived regulatory T-cells,” Eur J Immunol, vol. 47, no. 8, pp. 1256–1265, Aug. 2017. [CrossRef]
- A. Chaudhry et al., “CD4 + Regulatory T Cells Control T H 17 Responses in a Stat3-Dependent Manner,” Science (1979), vol. 326, no. 5955, pp. 986–991, Nov. 2009. [CrossRef]
- C. E. Konkel and W. Chen, “Balancing acts: the role of TGF-β in the mucosal immune system,” Trends Mol Med, vol. 17, no. 11, pp. 668–676, Nov. 2011. [CrossRef]
- C. Massagué, “TGFβ signalling in context,” Nat Rev Mol Cell Biol, vol. 13, no. 10, pp. 616–630, Oct. 2012. [CrossRef]
- M. J. Barnes, T. Griseri, A. M. F. Johnson, W. Young, F. Powrie, and A. Izcue, “CTLA-4 promotes Foxp3 induction and regulatory T cell accumulation in the intestinal lamina propria,” Mucosal Immunol, vol. 6, no. 2, pp. 324–334, Mar. 2013. [CrossRef]
- C. S. K. Walker, “Treg and CTLA-4: Two intertwining pathways to immune tolerance,” J Autoimmun, vol. 45, pp. 49–57, Sep. 2013. [CrossRef]
- C. E. Rudd, A. Taylor, and H. Schneider, “CD28 and CTLA-4 coreceptor expression and signal transduction,” Immunol Rev, vol. 229, no. 1, pp. 12–26, May 2009. [CrossRef]
- S. Van Coillie, B. Wiernicki, and J. Xu, “Molecular and Cellular Functions of CTLA-4,” 2020, pp. 7–32. [CrossRef]
- B. C. Lo et al., “Microbiota-dependent activation of CD4 + T cells induces CTLA-4 blockade–associated colitis via Fcγ receptors,” Science (1979), vol. 383, no. 6678, pp. 62–70, Jan. 2024. [CrossRef]
- Y. Onishi, Z. Fehervari, T. Yamaguchi, and S. Sakaguchi, “Foxp3 + natural regulatory T cells preferentially form aggregates on dendritic cells in vitro and actively inhibit their maturation,” Proceedings of the National Academy of Sciences, vol. 105, no. 29, pp. 10113–10118, Jul. 2008. [CrossRef]
- J. D. Fontenot, M. A. Gavin, and A. Y. Rudensky, “Foxp3 programs the development and function of CD4+CD25+ regulatory T cells,” Nat Immunol, vol. 4, no. 4, pp. 330–336, Apr. 2003. [CrossRef]
- V. K. Hench and L. Su, “Regulation of IL-2 gene expression by Siva and FOXP3 in human T cells,” BMC Immunol, vol. 12, no. 1, p. 54, Dec. 2011. [CrossRef]
- Y. Wang, M. Nag, J. L. Tuohy, K. De Paris, and J. E. Fogle, “T Regulatory Cell Induced Foxp3 Binds the IL2, IFN γ, and TNF α Promoters in Virus-Specific CD8 + T Cells from Feline Immunodeficiency Virus Infected Cats,” AIDS Res Hum Retroviruses, vol. 34, no. 3, pp. 269–276, Mar. 2018. [CrossRef]
- Y. Wu et al., “FOXP3 Controls Regulatory T Cell Function through Cooperation with NFAT,” Cell, vol. 126, no. 2, pp. 375–387, Jul. 2006. [CrossRef]
- N. Lycke, “Recent progress in mucosal vaccine development: potential and limitations,” Nat Rev Immunol, vol. 12, no. 8, pp. 592–605, Aug. 2012. [CrossRef]
- E. Ramvikas, M. Arumugam, S. R. Chakrabarti, and K. S. Jaganathan, “Nasal Vaccine Delivery,” in Micro and Nanotechnology in Vaccine Development, Elsevier, 2017, pp. 279–301. [CrossRef]
- C. R. Neutra and P. A. Kozlowski, “Mucosal vaccines: the promise and the challenge,” Nat Rev Immunol, vol. 6, no. 2, pp. 148–158, Feb. 2006. [CrossRef]
- J. Persson et al., “Nasal Immunization Confers High Avidity Neutralizing Antibody Response and Immunity to Primary and Recurrent Genital Herpes in Guinea Pigs,” Front Immunol, vol. 7, Dec. 2016. [CrossRef]
- E.-L. Johansson, L. Wassén, J. Holmgren, M. Jertborn, and A. Rudin, “Nasal and Vaginal Vaccinations Have Differential Effects on Antibody Responses in Vaginal and Cervical Secretions in Humans,” Infect Immun, vol. 69, no. 12, pp. 7481–7486, Dec. 2001. [CrossRef]
- Y. LI, X. LI, H. LIU, S. ZHUANG, J. YANG, and F. ZHANG, “Intranasal immunization with recombinant Lactococci carrying human papillomavirus E7 protein and mouse interleukin-12 DNA induces E7-specific antitumor effects in C57BL/6 mice,” Oncol Lett, vol. 7, no. 2, pp. 576–582, Feb. 2014. [CrossRef]
- E. F. Pacini et al., “Nasal immunization with a L. lactis-derived trans-sialidase antigen plus c-di-AMP protects against acute oral T. cruzi infection,” Vaccine, vol. 40, no. 15, pp. 2311–2323, Apr. 2022. [CrossRef]
- T. Ebensen, R. Libanova, K. Schulze, T. Yevsa, M. Morr, and C. A. Guzmán, “Bis-(3′,5′)-cyclic dimeric adenosine monophosphate: Strong Th1/Th2/Th17 promoting mucosal adjuvant,” Vaccine, vol. 29, no. 32, pp. 5210–5220, Jul. 2011. [CrossRef]
- J. Tai, M. Han, D. Lee, I.-H. Park, S. H. Lee, and T. H. Kim, “Different Methods and Formulations of Drugs and Vaccines for Nasal Administration,” Pharmaceutics, vol. 14, no. 5, p. 1073, May 2022. [CrossRef]
- H. Kleanthous et al., “Rectal and Intranasal Immunizations with Recombinant Urease Induce Distinct Local and Serum Immune Responses in Mice and Protect against Helicobacter pylori Infection,” Infect Immun, vol. 66, no. 6, pp. 2879–2886, Jun. 1998. [CrossRef]
- H. M. VanBenschoten and K. A. Woodrow, “Vaginal delivery of vaccines,” Adv Drug Deliv Rev, vol. 178, p. 113956, Nov. 2021. [CrossRef]
- R. Levit et al., “Use of genetically modified lactic acid bacteria and bifidobacteria as live delivery vectors for human and animal health,” Gut Microbes, vol. 14, no. 1, Dec. 2022. [CrossRef]
- A. H. Mohseni, V. Razavilar, H. Keyvani, M. R. Razavi, and R. A. Khavari-Nejad, “Oral immunization with recombinant Lactococcus lactis NZ9000 expressing human papillomavirus type 16 E7 antigen and evaluation of its immune effects in female C57BL/6 mice,” J Med Virol, vol. 91, no. 2, pp. 296–307, Feb. 2019. [CrossRef]
- A. H. Mohseni, S. Sedigheh Taghinezhad, and H. Keyvani, “The First Clinical Use of a Recombinant Lactococcus lactis Expressing Human Papillomavirus Type 16 E7 Oncogene Oral Vaccine: A phase I safety and immunogenicity trial in healthy women volunteers,” Mol Cancer Ther, vol. 19, no. 2, pp. 717–727, 2020. [CrossRef]
- H. Prudden et al., “Experimental Medicine for HIV Vaccine Research and Development,” Vaccines (Basel), vol. 11, no. 5, p. 970, May 2023. [CrossRef]
- V. Chamcha, A. Jones, B. R. Quigley, J. R. Scott, and R. R. Amara, “Oral Immunization with a Recombinant Lactococcus lactis –Expressing HIV-1 Antigen on Group A Streptococcus Pilus Induces Strong Mucosal Immunity in the Gut,” The Journal of Immunology, vol. 195, no. 10, pp. 5025–5034, Nov. 2015. [CrossRef]
- K. Q. Xin et al., “Immunogenicity and protective efficacy of orally administered recombinant Lactococcus lactis expressing surface-bound HIV Env,” Blood, vol. 102, no. 1, pp. 223–228, Jul. 2003. [CrossRef]
- World Health Organization, “Influenza update n° 509,” World Health Organization. Accessed: Nov. 11, 2025. [Online]. Available: https://www.who.int/publications/m/item/influenza-update-n--509.
- H. Lei, Y. Xu, J. Chen, X. Wei, and D. Man-Kit Lam, “Immunoprotection against influenza H5N1 virus by oral administration of enteric-coated recombinant Lactococcus lactis mini-capsules,” 2010. [CrossRef]
- H. Lei, T. Gao, and Q. Cen, “Cross-protective immunity of the haemagglutinin stalk domain presented on the surface of Lactococcus lactis against divergent influenza viruses in mice,” 2020. [CrossRef]
- Q. Zhang, J. Zhong, and L. Huan, “Expression of hepatitis B virus surface antigen determinants in Lactococcus lactis for oral vaccination,” Microbiol Res, vol. 166, no. 2, pp. 111–120, Feb. 2010. [CrossRef]
- R. N. Umami, R. I. Anwar, H. Murtiyaningsih, and A. Z. Mustopa, “Cloning and Expression of HBcAg Using Food Grade Vector pNZ8149 in Lactococcus Lactis for the Development of HBV Therapeutic Vaccine,” in Proceedings of the 1st International Conference for Health Research – BRIN (ICHR 2022), Dordrecht: Atlantis Press International BV, 2023, pp. 833–846. [CrossRef]
- H. Pei et al., “Expression of SARS-coronavirus nucleocapsid protein in Escherichia coli and Lactococcus lactis for serodiagnosis and mucosal vaccination,” Appl Microbiol Biotechnol, vol. 68, no. 2, pp. 220–227, Jul. 2005. [CrossRef]
- A. Xuan, J. Park, J. H. Yoo, and E. B. Kim, “Oral Immunization of Mice with Cell Extracts from Recombinant Lactococcus lactis Expressing SARS-CoV-2 Spike Protein,” Curr Microbiol, vol. 79, no. 6, Jun. 2022. [CrossRef]
- V. Yurina, O. Rahayu Adianingsih, and N. Widodo, “Oral and intranasal immunization with food-grade recombinant Lactococcus lactis expressing high conserved region of SARS-CoV-2 spike protein triggers mice’s immunity responses,” Vaccine X, vol. 13, p. 100265, Apr. 2023. [CrossRef]
- S. Guo et al., “The recombinant Lactococcus lactis oral vaccine induces protection against C. difficile spore challenge in a mouse model,” Vaccine, vol. 33, no. 13, pp. 1586–1595, 2015. [CrossRef]
- Y.-C. Lee, M. P. Dore, and D. Y. Graham, “Diagnosis and Treatment of Helicobacter pylori Infection,” Annu Rev Med, vol. 73, no. 1, pp. 183–195, Jan. 2022. [CrossRef]
- M. H. Lee, Y. Roussel, M. Wilks, and S. Tabaqchali, “Expression of Helicobacter pylori urease subunit B gene in Lactococcus lactis MG1363 and its use as a vaccine delivery system against H. pylori infection in mice,” Vaccine, vol. 19, no. 28–29, pp. 3927–3935, Jul. 2001. [CrossRef]
- M. R. Aliramaei, M. R. Khorasgani, M. R. Rahmani, S. H. Zarkesh Esfahani, and R. Emamzadeh, “Expression of Helicobacter pylori CagL gene in Lactococcus lactis MG1363 and evaluation of its immunogenicity as an oral vaccine in mice,” Microb Pathog, vol. 142, p. 103926, May 2020. [CrossRef]
- A. R. Narciso, R. Dookie, P. Nannapaneni, S. Normark, and B. Henriques-Normark, “Streptococcus pneumoniae epidemiology, pathogenesis and control,” Nat Rev Microbiol, vol. 23, no. 4, pp. 256–271, Apr. 2025. [CrossRef]
- A. Y.-H. Thong, R. Pawankar, H.-S. Park, and A. H. Abdul Latiff, “Evaluating immune responses to pneumococcal vaccines,” Asia Pac Allergy, vol. 13, no. 3, pp. 127–131, Sep. 2023. [CrossRef]
- M. T. El Hussein and H. Saleh, “Pneumonia Vaccines in Primary Care: Evidence-Based Recommendations for Clinical Practice,” The Journal for Nurse Practitioners, vol. 21, no. 9, p. 105510, Oct. 2025. [CrossRef]
- T. Chandler, S. Furmanek, R. Carrico, D. Balcom, F. Arnold, and J. Ramirez, “23-Valent Pneumococcal Polysaccharide Vaccination Does Not Prevent Community-Acquired Pneumonia Hospitalizations Due to Vaccine-Type Streptococcus pneumoniae,” Microorganisms, vol. 10, no. 3, p. 560, Mar. 2022. [CrossRef]
- A. Chen et al., “Effect and cost-effectiveness of pneumococcal conjugate vaccination: a global modelling analysis,” Lancet Glob Health, vol. 7, no. 1, pp. e58–e67, Jan. 2019. [CrossRef]
- Centers for Disease Control and Prevention, “Current CDC Vaccine Price List,” U.S. Department of Health and Human Services.
- A. Vintiñi, J. Villena, S. Alvarez, and M. Medina, “Administration of a probiotic associated with nasal vaccination with inactivated Lactococcus lactis -PppA induces effective protection against pneumoccocal infection in young mice,” Clin Exp Immunol, vol. 159, no. 3, pp. 351–362, Jan. 2010. [CrossRef]
- World Health Organization, “WHO preferred product characteristics for vaccines against enterotoxigenic Escherichia coli (ETEC),” Geneva, Jun. 2021. Accessed: Nov. 11, 2025. [Online]. Available: https://www.who.int/publications/i/item/who-preferred-product-characteristics-for-vaccines-against-enterotoxigenic-escherichia-coli.
- H. Ahmadi Rouzbahani, S. L. Mousavi Gargari, S. Nazarian, and S. Abdollahi, “Protective Immunity Against Enterotoxigenic Escherichia coli by Oral Vaccination of Engineered Lactococcus lactis,” Curr Microbiol, vol. 78, no. 9, pp. 3464–3473, Sep. 2021. [CrossRef]
- K. A. Qureshi et al., “Brucellosis: epidemiology, pathogenesis, diagnosis and treatment–a comprehensive review,” Ann Med, vol. 55, no. 2, Dec. 2023. [CrossRef]
- L. E. Samartino and F. M. Enright, “Pathogenesis of abortion of bovine brucellosis,” Comp Immunol Microbiol Infect Dis, vol. 16, no. 2, pp. 95–101, Apr. 1993. [CrossRef]
- T. Jamil, F. Melzer, J. Njeru, H. El-Adawy, H. Neubauer, and G. Wareth, “Brucella abortus: Current Research and Future Trends,” Curr Clin Microbiol Rep, vol. 4, no. 1, pp. 1–10, Mar. 2017. [CrossRef]
- L. A. Ribeiro et al., “Production and Targeting of the Brucella abortus Antigen L7/L12 in Lactococcus lactis : a First Step towards Food-Grade Live Vaccines against Brucellosis,” Appl Environ Microbiol, vol. 68, no. 2, pp. 910–916, Feb. 2002. [CrossRef]
- A. S. Pontes et al., “Induction of Partial Protection in Mice after Oral Administration of Lactococcus lactis Producing Brucella abortus L7/L12 Antigen,” J Drug Target, vol. 11, no. 8–10, pp. 489–493, Jan. 2003. [CrossRef]
- S. Rioux, D. Martin, H. W. Ackermann, J. Dumont, J. Hamel, and B. R. Brodeur, “Localization of surface immunogenic protein on group B streptococcus,” Infect Immun, vol. 69, no. 8, pp. 5162–5165, 2001. [CrossRef]
- D. Martin et al., “Protection from group B streptococcal infection in neonatal mice by maternal immunization with recombinant Sip protein,” Infect Immun, vol. 70, no. 9, pp. 4897–4901, 2002. [CrossRef]
- B. R. Brodeur et al., “Identification of group B streptococcal sip protein, which elicits cross-protective immunity,” Infect Immun, vol. 68, no. 10, pp. 5610–5618, 2000. [CrossRef]
- D. A. Diaz-Dinamarca et al., “Mucosal vaccination with lactococcus lactis-secreting surface immunological protein induces humoral and cellular immune protection against group b streptococcus in a murine model,” Vaccines (Basel), vol. 8, no. 2, Jun. 2020. [CrossRef]
- K. Y. Wong et al., “Recombinant lactococcal-based oral vaccine for protection against Streptococcus agalactiae infections in tilapia (Oreochromis niloticus),” Fish Shellfish Immunol, vol. 149, p. 109572, Jun. 2024. [CrossRef]
- S. Taghinezhad-S, A. H. Mohseni, H. Keyvani, and V. Razavilar, “Protection against human papillomavirus type 16-induced tumors in C57BL/6 mice by mucosal vaccination with Lactococcus lactis NZ9000 expressing E6 oncoprotein,” Microb Pathog, vol. 126, pp. 149–156, Jan. 2019. [CrossRef]
- S. Taghinezhad-S, A. H. Mohseni, H. Keyvani, and M. R. Razavi, “Phase 1 Safety and Immunogenicity Trial of Recombinant Lactococcus lactis Expressing Human Papillomavirus Type 16 E6 Oncoprotein Vaccine,” Mol Ther Methods Clin Dev, vol. 15, pp. 40–51, Dec. 2019. [CrossRef]
- Md. Rokon-Uz-Zaman et al., “Detection of antimicrobial resistance genes in Lactobacillus spp. from poultry probiotic products and their horizontal transfer among Escherichia coli,” Vet Anim Sci, vol. 20, p. 100292, Jun. 2023. [CrossRef]
- S. Tao, H. Chen, N. Li, T. Wang, and W. Liang, “The Spread of Antibiotic Resistance Genes In Vivo Model,” Canadian Journal of Infectious Diseases and Medical Microbiology, vol. 2022, pp. 1–11, Jul. 2022. [CrossRef]
- M. Bahey-El-Din, “Lactococcus lactis-based vaccines from laboratory bench to human use: An overview,” Vaccine, vol. 30, no. 4, pp. 685–690, 2012. [CrossRef]
- World Health Organization, “Annex 1 WHO guidelines on nonclinical,” no. 927, 2005, Accessed: Nov. 11, 2025. [Online]. Available: https://www.who.int/publications/m/item/annex1-nonclinical.p31-63.
- European Parliament; Council of the European Union, Regulation (EC) No 1829/2003 of the European Parliament and of the Council of 22 September 2003 on genetically modified food and feed. European Union: https://eur-lex.europa.eu/eli/reg/2003/1829/oj/eng, 2003, pp. 1–23.
- V. Venugopalan, K. A. Shriner, and A. Wong-Beringer, “Regulatory Oversight and Safety of Probiotic Use,” Emerg Infect Dis, vol. 16, no. 11, pp. 1661–1665, Nov. 2010. [CrossRef]
- T. Guo, Y. Xin, Y. Zhang, X. Gu, and J. Kong, “A rapid and versatile tool for genomic engineering in Lactococcus lactis,” Microb Cell Fact, vol. 18, no. 1, p. 22, Dec. 2019. [CrossRef]
- X. Song et al., “Single-plasmid systems based on CRISPR-Cas9 for gene editing in Lactococcus lactis,” J Dairy Sci, vol. 104, no. 10, pp. 10576–10585, Oct. 2021. [CrossRef]
- Y. Zhou et al., “Construction of a food-grade gene editing system based on CRISPR-Cas9 and its application in Lactococcus lactis NZ9000,” Biotechnol Lett, vol. 45, no. 8, pp. 955–966, Aug. 2023. [CrossRef]
- J. B. Divya and K. M. Nampoothiri, “Encapsulated Lactococcus lactis with enhanced gastrointestinal survival for the development of folate enriched functional foods,” Bioresour Technol, vol. 188, pp. 226–230, Jul. 2015. [CrossRef]
- D. Dusso and C. J. Salomon, “Solving the delivery of Lactococcus lactis : Improved survival and storage stability through the bioencapsulation with different carriers,” J Food Sci, vol. 88, no. 4, pp. 1495–1505, Apr. 2023. [CrossRef]
- S. Dey and S. Sankaran, “Engineered bacterial therapeutics with material solutions,” Trends Biotechnol, vol. 42, no. 12, pp. 1663–1676, Dec. 2024. [CrossRef]
- C. Lee, “Biocontainment strategies for live lactic acid bacteria vaccine vectors,” Bioeng Bugs, vol. 1, no. 1, pp. 75–77, Jan. 2010. [CrossRef]
| System | Inductor | Advantages | Disadvantages | Ref. |
| NICE | Nisin | -Tight, dose-dependent control -High expression levels -Well-characterized and widely used -Suitable for secretion or surface display |
-Requires addition of nisin (non-food-grade inducer in some contexts) -Possible background expression -Limited in complex media containing nisin inhibitors |
[34,35,37,38] |
| XIES | Xylose | - Food-grade, no antibiotics or peptides - Cost-effective inducer - Direct link between metabolism and expression |
- Requires strains able to metabolize xylose - Slower induction during exponential growth - Lower maximal expression than NICE |
[42,54] |
| Zinc Repressible System | Zinc depletion or chelation (EDTA) | - Tight repression and gradual induction - Food-grade and environmentally responsive - Ideal for metal-dependent regulation studies |
- Requires precise control of Zn²⁺ concentration - Chelation can disturb cell physiology - Lower expression yield than NICE |
[47] |
| Zirex | Zn2+ | - Strong induction (~80% of NICE) - Very low basal expression - Dual-promoter compatibility (can combine with NICE) - Suitable for metalloenzyme production |
- Requires fine-tuning of zinc concentration - May vary between strains - Still less standardized than NICE |
[48] |
| ZICE | Zn2+ | Completely food grade (GRAS) - No basal expression |
Lower expression than NICE (45 – 60%) | [49] |
| SICE | host-related stress (heat, acidity, bile salts) through the groESL promoter |
Auto-regulated and self-limiting - Activation during host transit (in situ expression) - No external inducer required - High biosafety potential |
- Variable induction due to stress conditions - Episomal plasmid may be unstable |
[50] |
| Pathogen | Antigen | Route of administration | Response | Reference |
| HPV | E7 Oncoprotein | Oral | Induced E7-specific IgG antibodies and activation of CD4⁺ T cells; demonstrated therapeutic potential confirmed in early-phase clinical trials | [99,100,135] |
| HIV | Gag–T3 pilus fusion; V2–V4 Env loop | Oral | Increased Gag-specific IgG and IgA in serum, feces, and vaginal secretions; activation of dendritic cells in Peyer’s patches; limited CD8⁺ T-cell response | [101,102,103] |
| Influenza A | Hemagglutinin (HA) and HA-stalk fusion | Oral | Induced strong serum IgG and mucosal IgA responses; conferred complete protection in mice and cross-protection among influenza subtypes | [105,106] |
| HBV | PreS region or central HBsAg fragments ± IFN-γ | Oral | Elicited serum IgG and intestinal IgA; co-expression of IFN-γ enhanced the humoral response. | [107,108] |
| SARS | Nucleocapsid (N) protein; RBD; HCR (S2 subunit) | Oral / Intranasal | Induced anti-SARS-CoV-2 IgG and IgA responses; activated CD4⁺ and CD8⁺ T cells; stronger NALT response via intranasal route; developed under food-grade conditions | [109,110,111] |
| C. difficile | Toxin fragments TcdA, TcdB | Oral | Elicited high IgG and IgA levels with toxin-neutralizing activity; improved animal survival and reduced intestinal pathology | [112] |
| H. pylori | UreB; NapA; CagL | Oral | Induced antigen-specific IgG and mucosal IgA; promoted a Th1/Th17 cytokine profile associated with protection | [29,114,115] |
| S. pneumoniae | Pneumococcal protective protein A (PppA) | Oral / intranasal | Increased IgA and IgG in bronchoalveolar lavage and serum; conferred protection against serotypes 3 and 14; promoted Th1-dominant response with moderate Th2/Th17 activity | [122] |
| E. coli | Heat-labile toxin subunit B (LTB) | Oral / subcutaneous | Induced intestinal IgA and serum IgG; demonstrated in vitro toxin neutralization; provided protection in the rabbit ileal loop assay. | [124] |
| Brucella abortus | Ribosomal protein L7/L12 | Oral | Induced fecal IgA indicating local response; no systemic IgG detected; secretion improved with Usp45 and LEISS pro-peptide; anchored form enhanced mucosal delivery | [128] |
| C. difficile | Toxin fragments TcdA, TcdB | Oral | Elicited high IgG and IgA levels with toxin-neutralizing activity; improved animal survival and reduced intestinal pathology | [112] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





