Submitted:
12 November 2025
Posted:
14 November 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. Local Context
1.2. Rationale and Aim
1.3. Hypothesis and Research Question
2. Materials and Methods
2.1. Study Design and Ethical Approval
2.2. Study Population and Sample Selection
- Children aged 1–18 years,
- Diagnosed and treated for dental trauma during the study period, and
- Complete documentation of demographic, diagnostic, and treatment data.
2.3. Data Extraction and Calibration
2.4. Variables and Diagnostic Criteria
- Demographic variables: age, gender, and governorate of residence.
- Health status: classified as healthy or special healthcare needs (SHCN). SHCN categories followed Almonaqel’s classification [25]: neurological disorders, sensory impairments, behavioural disabilities, medical disabilities, and developmental/congenital impairments. SHCN status was confirmed through medical documentation provided by caregivers and verified by the supervising pediatric dentist.
- Behavioural assessment: rated according to the Frankl Behaviour Rating Scale (definitely negative, negative, positive, definitely positive).
- Occlusion type: assessed using Angle’s classification and primary molar relationships (flush terminal plane, distal step, mesial step).
- Caries experience: recorded as dmft/DMFT indices following WHO criteria [26].
- Previous history of trauma: yes/no, based on caregiver report and previous record review.
- Apex status: classified radiographically as open or closed, according to Gill et al. [27].
- Etiological and situational variables: time between trauma and dental visit, place of injury (home, school, street, etc.), and cause (falls, traffic accidents, collisions, fights).
- 1.
- Fracture-related injuries (enamel fracture, enamel–dentin fracture, complicated crown fracture, crown–root fracture, root fracture).
- 2.
- Luxation-related injuries (concussion, subluxation, extrusive, lateral, and intrusive luxation, avulsion).
2.5. Data Management and Quality Control
2.6. Statistical Analysis
- Chi-square tests (χ2) for categorical variable comparisons,
- Independent-samples t tests and ANOVA with Bonferroni post hoc for continuous variables, and
- Binary logistic regression to identify independent predictors of TDIs (dependent variable: injury presence = yes/no).
2.7. Methodological Considerations
3. Results
3.1. TDIs Prevalence and the Associated Risk Factors of the Sample
3.2. Caries Indices and Oral Health Correlates
3.3. Injury Characteristics and Treatment
3.4. Distribution by Age, Health Status, and Etiology
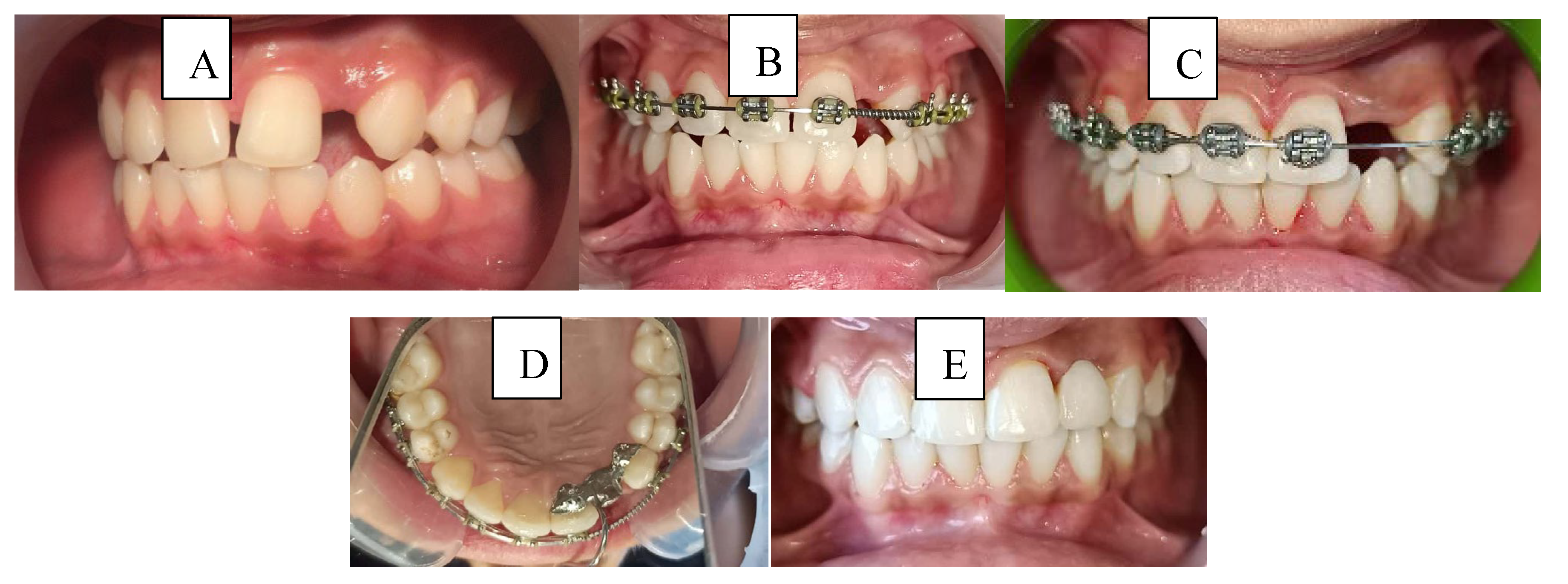
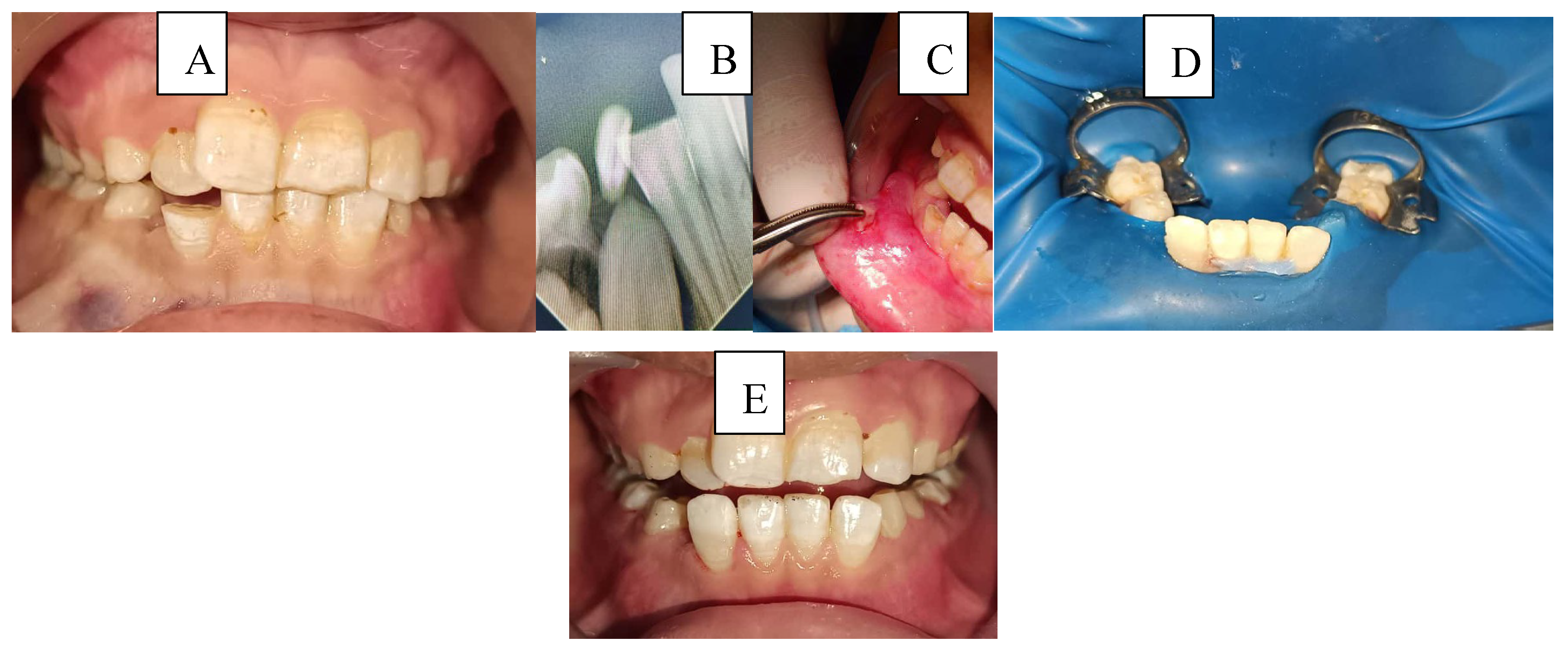
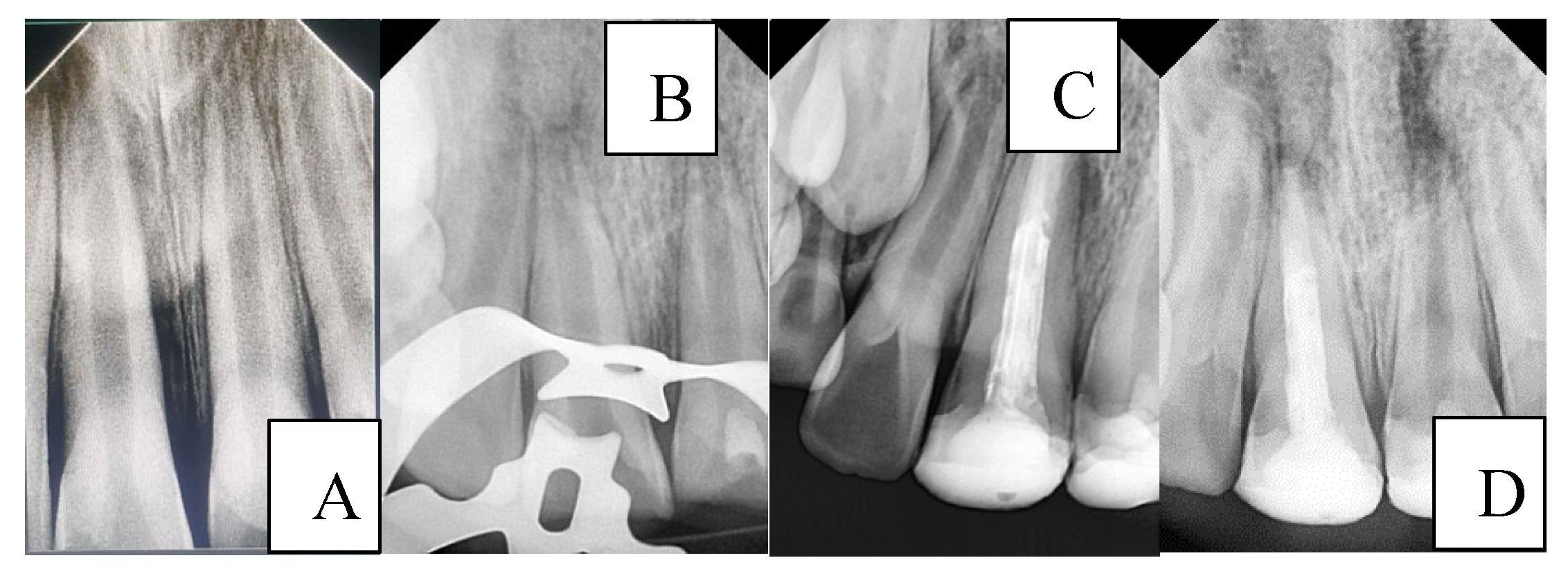
3.5. Illustrative Clinical Cases
3.6. TDI Risk Factors According to the Age Classification
3.7. TDIs’ Risk Factors According to the Number of Traumatized Teeth
4. Discussion
4.1. Overview and Key Findings
4.2. Global Comparisons
4.3. Sociopolitical and Environmental Context
4.4. Clinical Implications
4.5. Preventive and Policy Implications
- 1.
-
School-based Programs
- ○
- Introduce injury-prevention curricula that include dental first-aid education (e.g., management of avulsed teeth, proper storage media).
- ○
- Teachers and school nurses should receive annual first-responder training, supported by the Ministries of Education and Health.
- 2.
-
Parental and Community Education
- ○
- Launch nationwide awareness campaigns on dental trauma prevention and early care—via television, social media, and community centers.
- ○
- Encourage the use of mouthguards during sports activities and promote safer play environments.
- 3.
-
Health System Strengthening
- ○
- ntegrate dental trauma management protocols within emergency departments and pediatric hospitals.
- ○
- Establish a national TDI registry and reporting system to monitor incidence, guide resource allocation, and evaluate interventions.
- 4.
-
Urban and Infrastructure Planning
- ○
- Advocate for child-safe environments through collaboration between the Ministry of Housing, local municipalities, and NGOs.
- ○
- Encourage the use of shock-absorbent materials (e.g., rubberized flooring) in schools and playgrounds, replacing hard marble or stone surfaces prevalent in Damascus (Syrian) homes.
4.6. Limitations
4.7. Summary
5. Conclusions
Call to Action
- Establish a national TDI surveillance registry,
- Implement school-based first-aid and mouthguard education programs, and
- Promote safe urban design with shock-absorbent flooring in schools and playgrounds.
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Liu, F.; Wu, T.-T.; Lei, G.; Fadlelseed, A.F.A.; Xie, N.; Wang, D.-Y.; Guo, D.Q.-Y. Worldwide tendency and perspectives in traumatic dental injuries: A bibliometric analysis over two decades (1999–2018). Dent. Traumatol. 2020, 36, 489–497. [Google Scholar] [CrossRef]
- Glendor, U. Epidemiology of traumatic dental injuries–a 12-year review of the literature. Dent. Traumatol. 2008, 24, 603–611. [Google Scholar] [CrossRef]
- Petti, S.; Glendor, U.; Andersson, L. World traumatic dental injury prevalence and incidence, a meta-analysis—One billion living people have had traumatic dental injuries. Dent. Traumatol. 2018, 34, 71–86. [Google Scholar] [CrossRef] [PubMed]
- Magno, M.B.; de Paiva Cabral Tristão, S.K.; Jural, L.A.; Aguiar Sales Lima, S.O.; Coqueiro, R.D.S.; Maia, L.C.; Pithon, M.M. Does dental trauma influence the social judgment and motivation to seek dental treatment by children and adolescents? Development, validation, and application of an instrument for the evaluation of traumatic dental injuries and their consequences. Int. J. Paediatr. Dent. 2019, 29, 474–488. [Google Scholar] [CrossRef] [PubMed]
- Verma, S.K.; Jha, A.K.; Prakash, O.; Ekram, S.; Tigga, C.; Noorani, M.K.; Mehta, V.; Meto, A.; Meto, A.; Fiorillo, L.; et al. Impact of dental and orofacial trauma on oral health-related quality of life in adults: A systematic review. Chin. J. Traumatol. 2024, 27, 249–253. [Google Scholar] [CrossRef]
- da Silva, R.L.C.; Dias Ribeiro, A.P.; Almeida, J.C.F.; Sousa, S.J.L.; Garcia, F.C.P. Impact of dental treatment and the severity of traumatic dental injuries on the quality of life of Brazilian schoolchildren. Dent. Traumatol. 2021, 37, 562–567. [Google Scholar] [CrossRef]
- Zengin, A.Z.; Celenk, P.; Sumer, A.P.; Cankaya, S. Evaluation of traumatic dental injuries in a group of Turkish population. Niger. J. Clin. Pract. 2015, 18, 86–89. [Google Scholar] [CrossRef]
- Alshammary, F.; Alhur, T.; Alshammari, K.N.; Siddiqui, A.A.; Abideen, M.Z.U.; Alghaythi, K.S.; Ilyas, M.; Alam, M.K. Prevalence and Risk Factors of Dental Trauma in Ha’il, Saudi Arabia. J. Contemp. Dent. Pract. 2022, 23, 628–633. [Google Scholar]
- Andreasen, J.O.; Andreasen, F.M. Classification, etiology and epidemiology. In Textbook and Color Atlas of Traumatic Injuries to the Teeth, 5th ed.; Wiley Blackwell: Hoboken, NJ, USA, 2019; pp. 252–282. [Google Scholar]
- Magno, M.B.; Nadelman, P.; Leite, K.L.F.; Ferreira, D.M.; Pithon, M.M.; Maia, L.C. Associations and risk factors for dental trauma: A systematic review of systematic reviews. Community Dent. Oral. Epidemiol. 2020, 48, 447–463. [Google Scholar] [CrossRef] [PubMed]
- Tewari, N.; Mathur, V.P.; Siddiqui, I.; Morankar, R.; Verma, A.R.; Pandey, R.M. Prevalence of traumatic dental injuries in India: A systematic review and meta-analysis. Indian J. Dent. Res. 2020, 31, 601–614. [Google Scholar] [CrossRef] [PubMed]
- Abdel Malak, C.; Chakar, C.; Romanos, A.; Rachidi, S. Prevalence and Etiological Factors of Dental Trauma among 12- and 15-Year-Old Schoolchildren of Lebanon: A National Study. ScientificWorldJournal 2021, 2021, 5587431. [Google Scholar] [CrossRef] [PubMed]
- Martin, A.G.; Shivashakarappa, P.G.; Adimoulame, S.; Sundaramurthy, N.; G, E. Prevalence, Etiology, and Risk Factors of Traumatic Dental Injuries in Children with Special Needs of Puducherry. Int. J. Clin. Pediatr. Dent. 2022, 15, 104–108. [Google Scholar] [CrossRef] [PubMed]
- Glendor, U. Aetiology and risk factors related to traumatic dental injuries—A review of the literature. Dent. Traumatol. 2009, 25, 19–31. [Google Scholar] [CrossRef] [PubMed]
- Born, C.D.; Jackson, T.H.; Koroluk, L.D.; Divaris, K. Traumatic dental injuries in preschool-age children: Prevalence and risk factors. Clin. Exp. Dent. Res. 2019, 5, 151–159. [Google Scholar] [CrossRef]
- Council, O. Guideline on management of acute dental trauma. Dent. Traumatol. 2009, 1. [Google Scholar]
- Levin, L.; Day, P.F.; Hicks, L.; O’Connell, A.; Fouad, A.F.; Bourguignon, C.; Abbott, P.V. International Association of Dental Traumatology guidelines for the management of traumatic dental injuries: General introduction. Dent. Traumatol. 2020, 36, 309–313. [Google Scholar] [CrossRef]
- Fouad, A.F.; Abbott, P.V.; Tsilingaridis, G.; Cohenca, N.; Lauridsen, E.; Bourguignon, C.; O’Connell, A.; Flores, M.T.; Day, P.F.; Hicks, L.; et al. International Association of Dental Traumatology guidelines for the management of traumatic dental injuries: 2. Avulsion of permanent teeth. Dent. Traumatol. 2020, 36, 331–342. [Google Scholar] [CrossRef]
- Marcenes, W.; al Beiruti, N.; Tayfour, D.; Issa, S. Epidemiology of traumatic injuries to the permanent incisors of 9-12-year-old schoolchildren in Damascus, Syria. Endod. Dent. Traumatol. 1999, 15, 117–123. [Google Scholar] [CrossRef]
- Alshayeb, L.; Al-Shiekh, M.N.; Dashash, M. Prevalence and Risk Factors of Traumatic Dental Injuries among Conflict-Affected Schoolchildren in Syria (2023–2024). J. Epidemiol. Glob. Health 2025, 15, 1–10. [Google Scholar] [CrossRef]
- Dashash, M.; Omar, K. CRISIS criteria for effective continuous education in traumatic dental injuries during syrian crisis. Am. J. Health Res. 2016, 4, 1–6. [Google Scholar]
- Nagendrababu, V.; Duncan, H.F.; Fouad, A.F.; Kirkevang, L.L.; Parashos, P.; Pigg, M.; Vaeth, M.; Jayaraman, J.; Suresh, N.; Arias, A.; et al. PROBE 2023 guidelines for reporting observational studies in endodontics: A consensus-based development study. Int. Endod. J. 2023, 56, 308–317. [Google Scholar] [CrossRef] [PubMed]
- Organization, W.H. Oral Health Surveys: Basic Methods; World Health Organization: Geneva, Switzerland, 2013. [Google Scholar]
- Almonaqel, M.B.; Makieh, R.E. Health status and visit reasons for children attending the Pediatric Dentistry department in damascus university, damascus, Syria: A retrospective study. Saudi Dent. J. 2024, 36, 1025–1030. [Google Scholar] [CrossRef]
- Gill, I.; Mittal, S.; Kumar, T.; Keshav, V. Open Apex and its Management: Review Article. J. Pharm. Bioallied. Sci. 2024, 16 (Suppl. S1), S31–S34. [Google Scholar] [CrossRef] [PubMed]
- Petti, S.; Andreasen, J.O.; Glendor, U.; Andersson, L. NA0D—The new Traumatic Dental Injury classification of the World Health Organization. Dent. Traumatol. 2022, 38, 170–174. [Google Scholar] [CrossRef]
- Habal, W.; Alkattan, R.; Hajeer, M.Y.; Alkhouli, M.; Al-Nerabieah, Z.; Habal, T.; Awawdeh, M. Impact of Syrian Conflict on the Oral Health of Adolescents: A Cross-Sectional Study. Cureus 2024, 16, e54613. [Google Scholar] [CrossRef]
- Petti, S.; Glendor, U.; Andersson, L. World traumatic dental injury prevalence and incidence, a meta-analysis-One billion living people have had traumatic dental injuries. Dent. Traumatol. 2018, 34, 71–86. [Google Scholar] [CrossRef]
- Goswami, M.; Aggarwal, T. Prevalence of Traumatic Dental Injuries among 1- to 14-year-old Children: A Retrospective Study. Int. J. Clin. Pediatr. Dent. 2021, 14, 467–470. [Google Scholar] [CrossRef]
- Eyuboglu, O.; Yilmaz, Y.; Zehir, C.; Sahin, H. A 6-year investigation into types of dental trauma treated in a paediatric dentistry clinic in Eastern Anatolia region, Turkey. Dent. Traumatol. 2009, 25, 110–114. [Google Scholar] [CrossRef]
- Oldin, A.; Lundgren, J.; Nilsson, M.; Norén, J.G.; Robertson, A. Traumatic dental injuries among children aged 0–17 years in the BITA study—A longitudinal Swedish multicenter study. Dent. Traumatol. 2015, 31, 9–17. [Google Scholar] [CrossRef]
- Ogunmayowa, O.; Baker, C. Neighborhood risk factors for sports and recreational injuries: A systematic review of studies applying multilevel modeling techniques. Inj. Epidemiol. 2022, 9, 6. [Google Scholar] [CrossRef] [PubMed]
- ElKarmi, R.F.; Hamdan, M.A.; Rajab, L.D.; Abu-Ghazaleh, S.B.; Sonbol, H.N. Prevalence of traumatic dental injuries and associated factors among preschool children in Amman, Jordan. Dent. Traumatol. 2015, 31, 487–492. [Google Scholar] [CrossRef] [PubMed]
- Agouropoulos, A.; Pavlou, N.; Kotsanti, M.; Gourtsogianni, S.; Tzanetakis, G.; Gizani, S. A 5-year data report of traumatic dental injuries in children and adolescents from a major dental trauma center in Greece. Dent. Traumatol. 2021, 37, 631–638. [Google Scholar] [CrossRef]
- Kramer, P.F.; Pereira, L.M.; Ilha, M.C.; Borges, T.S.; Freitas, M.P.M.; Feldens, C.A. Exploring the impact of malocclusion and dentofacial anomalies on the occurrence of traumatic dental injuries in adolescents. Angle Orthod. 2017, 87, 816–823. [Google Scholar] [CrossRef] [PubMed]
- Alsayed Tolibah, Y.; Bshara, N.; Aljabban, O.; Abbara, M.T.; Alhaji, M.; Almasri, I.A.; Baghdadi, Z.D. Randomized Trial of Bioceramic Apical Barrier Methods in Necrotic Immature Incisors: Effects on Pain, Extrusion, and Procedure Duration. Children 2025, 12, 1423. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Alsayed Tolibah, Y.; Bshara, N.; Abbara, M.T.; Alhaji, M.; Aljabban, O.; Ahmad, I.A.; Baghdadi, Z.D. Root Development Following Bioceramic Material Application in Immature Permanent Teeth: A Case Series With 24-Month Follow-U. Case Rep. Dent. 2025, 2025, 1530438. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Baghdadi, Z.D. Crown fractures: New concepts, materials, and techniques. Compend. Contin. Educ. Dent. 2000, 21, 831 832, 834, 836 passim; quiz 851. [Google Scholar] [PubMed]
- UNICEF Middle East; North Africa Regional Office. Humanitarian Situation Report: Middle East & North Africa (Jan–Dec 2023); UNICEF MENA: Amman, Jordan, 2023; p. 2. [Google Scholar]
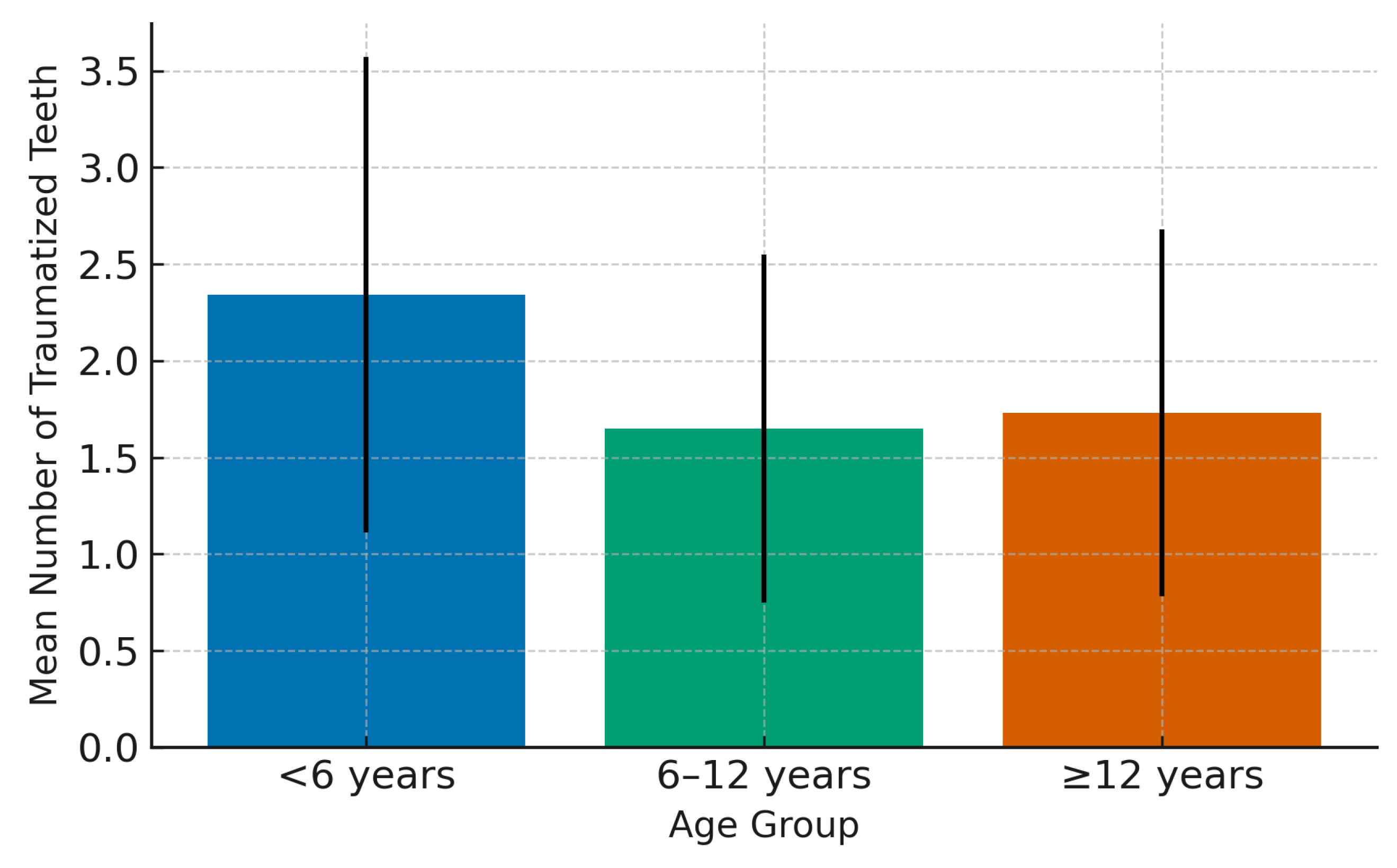
| Variable | With Injuries (n=301) | No Injuries (n=2415) | TDI Prevalence (%) | p-value |
|---|---|---|---|---|
| Gender (Male/Female) | 213/88 | 1323/1092 | 13.9/7.5 | <0.001 |
| Age group (<6/6–12/≥12) | 32/165/104 | 441/1507/467 | 6.8/8.4/18.2 | <0.001 |
| Health status (Healthy/SHCN) | 273/28 | 2169/246 | 11.8/10.2 | 0.631 |
| Frankl’s behaviour (Neg/Pos) | 104/197 | 1125/1290 | 8.1/17.6 | <0.001 |
| Previous trauma (Yes/No) | 17/284 | 53/2354 | 24.3/10.8 | <0.001 |
| Occlusion (Class I/II/III) | 212/53/6 | 1447/309/146 | 12.8/14.6/4.0 | <0.001 |
| Note: SHCN = special healthcare needs. Bold p-values indicate significant associations (p < 0.05). | ||||
| Predictor Variable | B | SE | Wald | OR (95% CI) | p-value |
|---|---|---|---|---|---|
| Gender (Male) | 0.834 | 0.137 | 37.262 | 2.30 (1.76–3.01) | <0.001 |
| Age (Increasing) | -0.570 | 0.138 | 17.064 | 0.56 (0.43–0.74) | <0.001 |
| Behaviour (Frankl) | -0.140 | 0.090 | 2.415 | 0.87 (0.73–1.04) | 0.120 |
| Previous trauma | 0.017 | 0.120 | 0.019 | 1.02 (0.80–1.29) | 0.889 |
| Angle’s classification | 0.095 | 0.059 | 2.574 | 1.10 (0.98–1.23) | 0.109 |
| Model χ2 = 62.45, p < 0.001; Nagelkerke R2 = 0.118; Hosmer–Lemeshow test p = 0.47; Overall classification accuracy = 78.2%. OR = odds ratio; CI = confidence interval. | |||||
| Index | With Injuries (Mean ± SD) | No Injuries (Mean ± SD) | Mean Difference (95% CI) | p-value |
|---|---|---|---|---|
| dmft (Primary) | 1.96 ± 2.15 | 5.92 ± 3.79 | -3.96 (-4.35, --3.57) | <0.001 |
| DMFT (Permanent) | 2.94 ± 2.33 | 5.57 ± 4.00 | -2.63 (-3.05, -2.21) | <0.001 |
| DMFT + dmft (Mixed) | 4.45 ± 2.82 | 5.51 ± 3.44 | -1.06 (-1.45, -0.67) | <0.001 |
| Variable | Permanent teeth (n = 430) | Primary teeth (n = 91) | Notes/p-value |
|---|---|---|---|
| Apex status—open | 40.1% | – | 40.1% overall open apex rate |
| Most affected teeth | #11 (36.1%), #21 (32.4%) | #51 (5.4%), #61 (5.0%) | — |
| Complicated crown fracture | 39.1% | 9.9% | Most frequent type overall |
| Avulsion | 4.9% | 25.3% | p < 0.001 (primary > permanent) |
| Healthy/Reversible pulpitis | 22.0%/29.6% | 16.4%/6.0% | — |
| Asymptomatic apical periodontitis | 32.1% | 17.9% | — |
| >one month delay | 45.3% | 45.1% | 45% delayed overall |
| Restorations | 26.1% | 1.9% | |
| Re-bonding fractured segment | 1.2% | — | |
| Traditional root canal treatment | 7.7% | 1.7% | |
| Apexogenesis | 7.8% | 0.3% | |
| Apical barrier, Regeneration | 18.3%, 2.7% | — | — |
| Note: Percentages refer to teeth within each dentition grouBold values indicate major categories. p < 0.05 is considered significant. | |||
| Variables | Age Classification | p-value | |||||
|---|---|---|---|---|---|---|---|
| <6 | 6–<12 | 12≤ | Total | ||||
| Gender | Male | N | 15 | 121 | 77 | 213 | 0.007 a |
| % of Total | 5.0% | 40.2% | 25.6% | 70.8% | |||
| Female | N | 17 | 44 | 27 | 88 | ||
| % of Total | 5.6% | 14.6% | 9.0% | 29.2% | |||
| Total | N | 32 | 165 | 104 | 301 | ||
| % of Total | 10.6% | 54.8% | 34.6% | 100.0% | |||
| Health status | Healthy | N | 22 | 157 | 94 | 273 | <0.001 a |
| % of Total | 7.3% | 52.2% | 31.2% | 90.7% | |||
| SHCN | N | 10 | 8 | 10 | 28 | ||
| % of Total | 3.3% | 2.7% | 3.3% | 9.3% | |||
| Total | N | 32 | 165 | 104 | 301 | ||
| % of Total | 10.6% | 54.8% | 34.6% | 100.0% | |||
| Previous traumatic injury | No | N | 29 | 160 | 95 | 284 | 0.094 a |
| % of Total | 9.6% | 53.2% | 31.6% | 94.4% | |||
| Yes | N | 3 | 5 | 9 | 17 | ||
| % of Total | 1.0% | 1.7% | 3.0% | 5.6% | |||
| Total | N | 32 | 165 | 104 | 301 | ||
| % of Total | 10.6% | 54.8% | 34.6% | 100.0% | |||
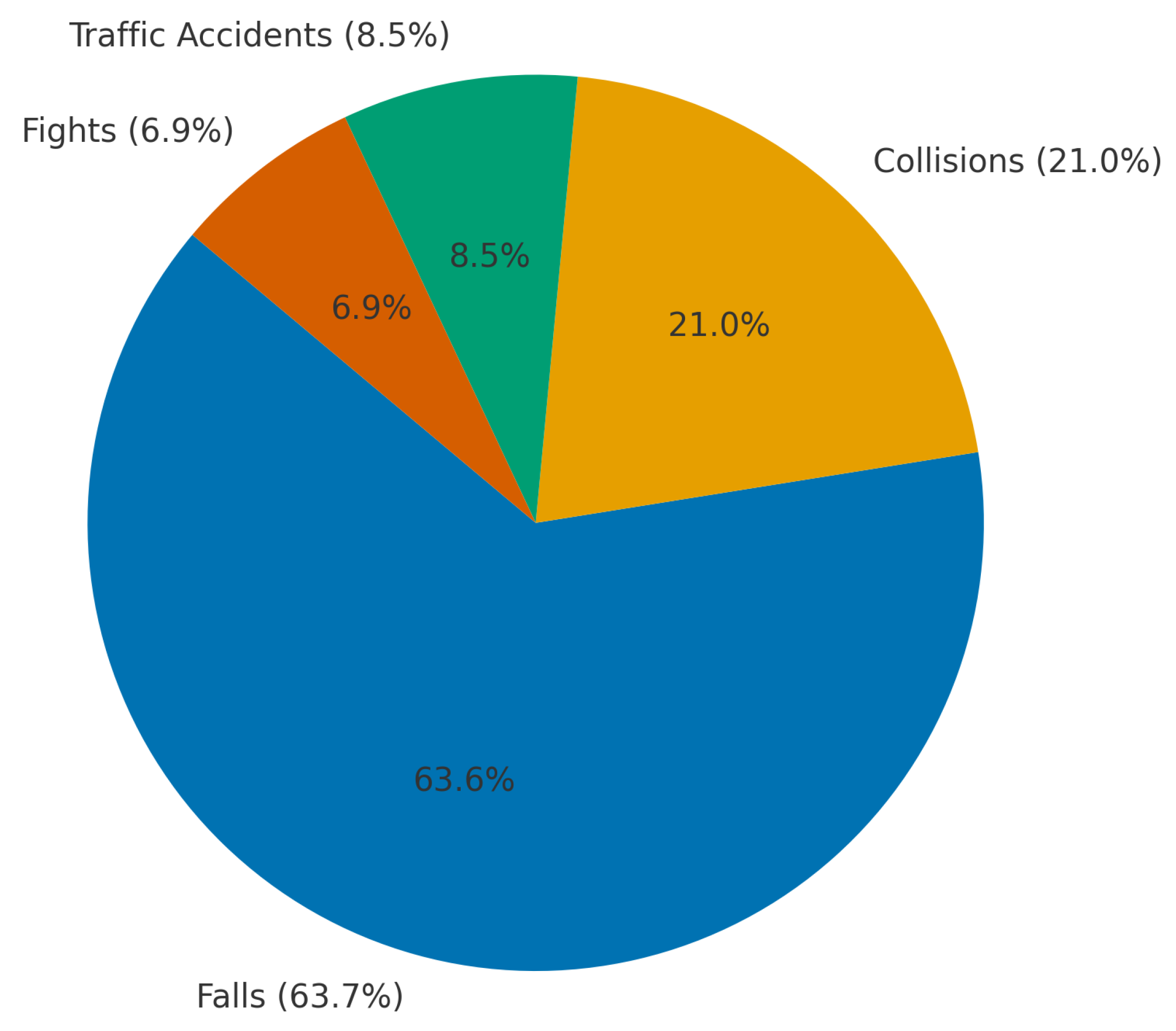
| Cause | Falls | N | 20 | 130 | 60 | 210 | <0.001 a |
| % of Total | 6.7% | 43.3% | 20.0% | 70.0% | |||
| Traffic accident | N | 5 | 5 | 5 | 15 | ||
| % of Total | 1.7% | 1.7% | 1.7% | 5.0% | |||
| Collisions with objects | N | 6 | 27 | 22 | 55 | ||
| % of Total | 2.0% | 9.0% | 7.3% | 18.3% | |||
| Fight | N | 1 | 2 | 17 | 20 | ||
| % of Total | 0.3% | 0.7% | 5.7% | 6.7% | |||
| Total | N | 32 | 164 | 104 | 300 | ||
| % of Total | 10.7% | 54.7% | 34.7% | 100.0% | |||
| |||||||
| variables | Number of traumatized teeth | p-value | |||
|---|---|---|---|---|---|
| N | Mean | SD | |||
| Gender | Male | 213 | 1.71 | .955 | 0.305 a |
| Female | 88 | 1.84 | 1.027 | ||
| Health status | Healthy | 273 | 1.66 | .918 | <0.001 a |
| SHCN | 28 | 2.61 | 1.133 | ||
| Place | Home | 148 | 1.74 | .897 | 0.469 b |
| Street | 46 | 1.98 | 1.483 | ||
| School | 62 | 1.65 | .812 | ||
| Sport | 19 | 1.79 | .855 | ||
| Garden | 25 | 1.64 | .700 | ||
| Total | 300 | 1.75 | .978 | ||
| Age | <6 | 32 | 2.34 | 1.234 | 0.001 b |
| 6–<12 | 165 | 1.65 | .903 | ||
| 12 ≤ | 104 | 1.73 | .947 | ||
| Total | 301 | 1.75 | .977 | ||
| Cause | Falls | 210 | 1.59 | .760 | <0.001 b |
| Traffic accident | 15 | 2.93 | 1.944 | ||
| Collision with objects | 55 | 2.04 | 1.105 | ||
| Fight | 20 | 1.80 | .894 | ||
| Total | 300 | 1.75 | .978 | ||
| |||||
| Age | Mean Difference | Std. Error | p-value a | |
|---|---|---|---|---|
| <6 | 6–<12 | .695 | .185 | .001 |
| 12 ≤ | .613 | .194 | .005 | |
| 6–<12 | 12 ≤ | -.082 | .120 | 1.000 |
| Cause | Mean Difference | Std. Error | p-value a | |
| Falls | Traffic accident | -1.343 | .248 | 0.000 |
| Collisions with objects | -.446 | .141 | 0.010 | |
| Fight | -.210 | .217 | 1.000 | |
| Traffic accident | Collisions with objects | .897 | .270 | 0.006 |
| Fight | 1.133 | .317 | 0.002 | |
| Collisions with objects | Fight | .236 | .242 | 1.000 |
| ||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




