Submitted:
04 September 2025
Posted:
05 September 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Case Report
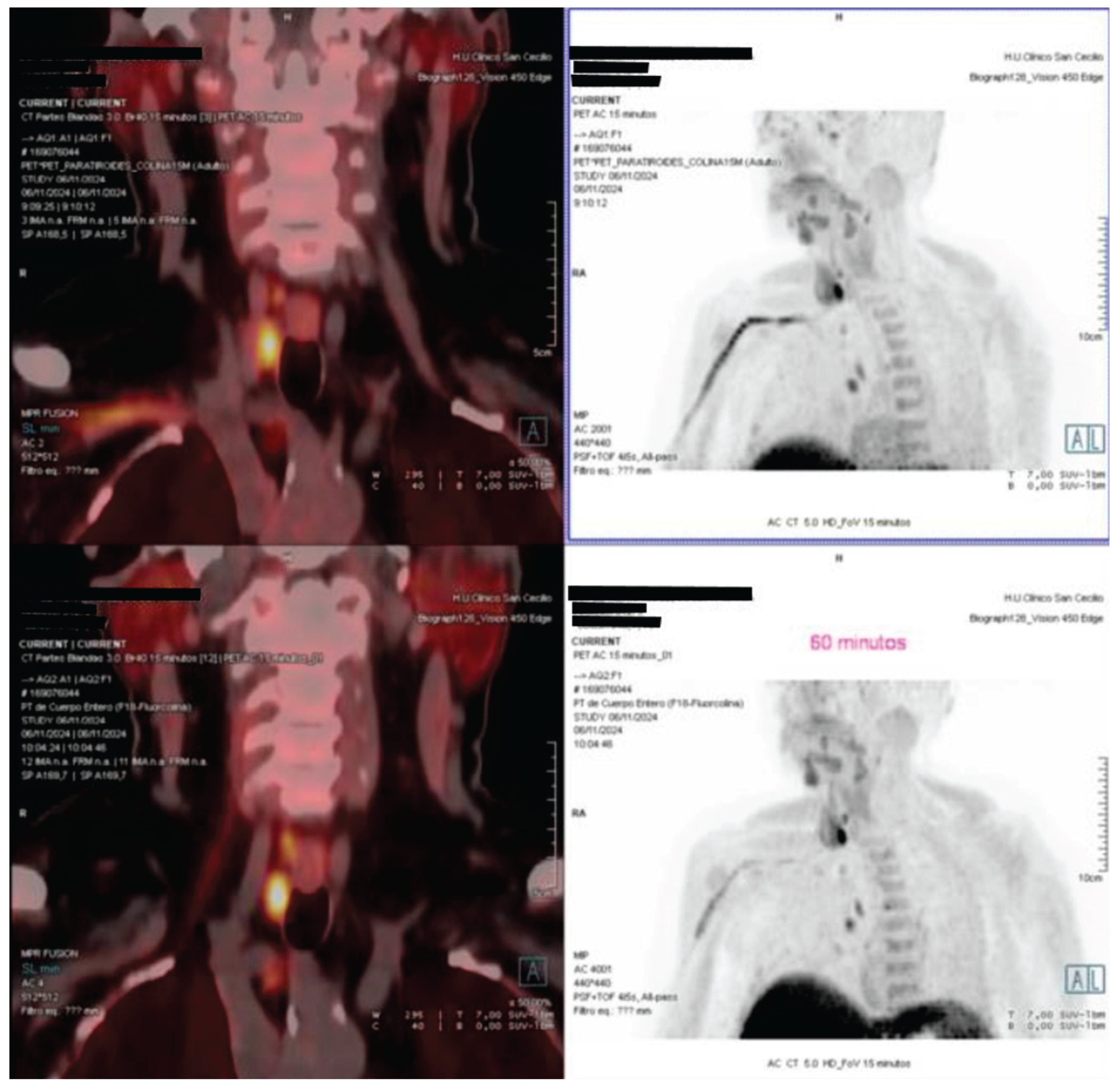
3. Discussion
3.1. Pathophysiology of Hypophosphatemia in Primary Hyperparathyroidism
3.2. Clinical Relevance of Chronic Hypophosphatemia
3.3. Diagnostic Approach to Hypophosphatemia
3.4. Treatment of Hypophosphatemia and Therapeutic Implications in PHPT
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Bilezikian, J.P.; Khan, A.A.; Silverberg, S.J.; Fuleihan, G.E.-H.; Marcocci, C.; Minisola, S.; et al. Evaluation and management of primary hyperparathyroidism: Summary statement and guidelines from the fifth international workshop. J Bone Miner Res [Internet]. 2020, 37, 2293–314. [Google Scholar] [CrossRef]
- Minisola, S.; Gianotti, L.; Bhadada, S.; Silverberg, S.J. Classical complications of primary hyperparathyroidism. Best Pract Res Clin Endocrinol Metab. 2018, 32, 791–803. [Google Scholar] [CrossRef] [PubMed]
- Eufrazino, C.; Veras, A.; Bandeira, F. Epidemiology of primary hyperparathyroidism and its non-classical manifestations in the city of Recife, Brazil. Clin Med Insights Endocrinol Diabetes [Internet]. 2013, 6, 69–74. [Google Scholar] [CrossRef]
- Silva, B.C.; Cusano, N.E.; Bilezikian, J.P. Primary hyperparathyroidism. Best Pract Res Clin Endocrinol Metab [Internet]. 2024, 38, 101247. [Google Scholar] [CrossRef]
- Khan, A.A.; Hanley, D.A.; Rizzoli, R.; Bollerslev, J.; Young, J.E.M.; Rejnmark, L.; et al. Primary hyperparathyroidism: review and recommendations on evaluation, diagnosis, and management. A Canadian and international consensus. Osteoporos Int [Internet]. 2017, 28, 1–19. [Google Scholar] [CrossRef]
- Wagner, C.A. The basics of phosphate metabolism. Nephrol Dial Transplant. 2024, 39, 190–201. [Google Scholar] [CrossRef]
- Aljuraibah, F.; Bacchetta, J.; Brandi, M.L.; Florenzano, P.; Javaid, M.K.; Mäkitie, O.; Raimann, A.; Rodriguez, M.; Siggelkow, H.; Tiosano, D.; Vervloet, M.; Wagner, C.A. An Expert Perspective on Phosphate Dysregulation With a Focus on Chronic Hypophosphatemia. J Bone Miner Res. 2022, 37, 12–20. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Tebben, P.J. Hypophosphatemia: a practical guide to evaluation and management. Endocr Pract. 2022, 28, 1091–1099. [Google Scholar] [CrossRef] [PubMed]
- Florenzano, P.; Cipriani, C.; Roszko, K.L.; Fukumoto, S.; Collins, M.T.; Minisola, S.; Pepe, J. Approach to patients with hypophosphataemia. Lancet Diabetes Endocrinol. 2020, 8, 163–174. [Google Scholar] [CrossRef] [PubMed]
- Puente Ruiz, N.; Valero Díaz de Lamadrid, M.C.; Riancho, J.A. Etiology of hypophosphatemia in adults. Med Clin (Barc). 2025, 164, 30–37. [Google Scholar] [CrossRef] [PubMed]
- Ito, N.; Hidaka, N.; Kato, H. The pathophysiology of hypophosphatemia. Best Pract Res Clin Endocrinol Metab. 2024, 38, 101851. [Google Scholar] [CrossRef] [PubMed]
- Michigami, T.; Kawai, M.; Yamazaki, M.; Ozono, K. Phosphate as a signaling molecule and its sensing mechanism. Physiol Rev 2018, 98, 2317–2348. [Google Scholar] [CrossRef] [PubMed]
- Michigami, T. Advances in understanding of phosphate homeostasis and related disorders. Endocr J. 2022, 69, 881–896. [Google Scholar] [CrossRef] [PubMed]
- Walton, J.; Gray, T.K. Absorption of inorganic phosphate in the human small intestine. Clin Sci (London). 1979, 56, 407–412. [Google Scholar] [CrossRef] [PubMed]
- Labonté, E.D.; Carreras, C.W.; Leadbetter, M.R.; Kozuka, K.; Kohler, J.; Koo-McCoy, S.; He, L.; Dy, E.; Black, D.; Zhong, Z.; Langsetmo, I.; Spencer, A.G.; Bell, N.; Deshpande, D.; Navre, M.; Lewis, J.G.; Jacobs, J.W.; Charmot, D. Gastrointestinal Inhibition of Sodium-Hydrogen Exchanger 3 Reduces Phosphorus Absorption and Protects against Vascular Calcification in CKD. J Am Soc Nephrol. 2015, 26, 1138–49. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Castellano, E.; Attanasio, R.; Boriano, A.; Pellegrino, M.; Borretta, G. Serum phosphate: a neglected test in the clinical management of primary hyperparathyroidism. J Clin Endocrinol Metab. 2022, 107, e612–e618. [Google Scholar] [CrossRef] [PubMed]
- Hassani, S.; Afkhamizadeh, M.; Teimouri, A.; Najaf Najafi, M.; Vazifeh Mostaan, L.; Mohebbi, M. Evaluation of serum level of FGF23 and 1,25(OH)₂D₃ in primary hyperparathyroidism patients before and after parathyroidectomy. Int J Gen Med 2020, 13, 289–295. [Google Scholar] [CrossRef]
- Schaefer, B.; Tobiasch, M.; Wagner, S.; Glodny, B.; Tilg, H.; et al. Hypophosphatemia after intravenous iron therapy: comprehensive review of clinical findings and recommendations for management. Bone. 2022, 154, 116202. [Google Scholar] [CrossRef]
- Wilson, R.; MukherjeeRoy, N.; Gattineni, J. The role of fibroblast growth factor 23 in regulation of phosphate balance. Pediatr Nephrol. 2024, 39, 3439–3451. [Google Scholar] [CrossRef] [PubMed]
- Shimada, T.; Hasegawa, H.; Yamazaki, Y.; Muto, T.; Hino, R.; Takeuchi, Y.; et al. FGF-23 is a potent regulator of vitamin D metabolism and phosphate homeostasis. J Bone Miner Res. 2004, 19, 429–435. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.; Ma, T.; Yu, X.; Su, T. Severe hypophosphatemia as the initial presentation of renal Fanconi's syndrome and distal renal tubular acidosis related to zoledronic acid: a case report and literature review. Kidney Blood Press Res 2023, 48, 18–27. [Google Scholar] [CrossRef] [PubMed]
- Ramanan, M.; Tabah, A.; Affleck, J.; Edwards, F.; White, K.C.; Attokaran, A.; Laupland, K. Hypophosphataemia in Critical Illness: A Narrative Review. J Clin Med. 2024, 13, 7165. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Knochel, J.P.; Barcenas, C.; Cotton, J.R.; Fuller, T.J.; Haller, R.; Carter, N.W. Hypophosphatemia and rhabdomyolysis. J Clin Invest. 1978, 62, 1240–1246. [Google Scholar] [CrossRef] [PubMed]
- Mughal, M.Z. Ricketts. Curr Osteoporos Rep. 2011, 9, 291–299. [Google Scholar] [CrossRef] [PubMed]
- Beck-Nielsen, S.S.; Mughal, Z.; Haffner, D.; Nilsson, O.; Levtchenko, E.; Ariceta, G.; de Lucas Collantes, C.; Schnabel, D.; Jandhyala, R.; Mäkitie, O. FGF23 and its role in X-linked hypophosphatemia-related morbidity. Orphanet J Rare Dis. 2019, 14, 58. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Linglart, A.; Biosse-Duplan, M.; Briot, K.; Chaussain, C.; Esterle, L.; Guillaume-Czitrom, S.; et al. Therapeutic management of hypophosphatemic rickets from infancy to adulthood. Endocr Connect. 2014, 3, R13–R30. [Google Scholar] [CrossRef] [PubMed]
- Lecoq, A.L.; Brandi, M.L.; Linglart, A.; Kamenický, P. Management of X-linked hypophosphatemia in adults. Metabolism. 2020, 103 (Suppl), 154049. [Google Scholar] [CrossRef] [PubMed]
- Lin, X.; Li, S.; Zhang, Z.; Yue, H. Clinical and genetic characteristics of 153 Chinese patients with X-linked hypophosphatemia. Front Cell Dev Biol. 2021, 9, 617738. [Google Scholar] [CrossRef] [PubMed]
- Laurent, M.R.; De Schepper, J.; Trouet, D.; Godefroid, N.; Boros, E.; Heinrichs, C.; et al. Consensus recommendations for the diagnosis and management of X-linked hypophosphatemia in Belgium. Front Endocrinol (Lausanne). Erratum in: Front Endocrinol (Lausanne). 2021, 12, 686401. 2021, 12, 641543. [Google Scholar] [CrossRef] [PubMed]
- Seefried, L.; Smyth, M.; Keen, R.; Harvengt, P. Burden of disease associated with X-linked hypophosphataemia in adults: a systematic literature review. Osteoporos Int. 2021, 32, 7–22. [Google Scholar] [CrossRef] [PubMed]
- Soehle, M.; Casey, A.T. Cervical spinal cord compression attributable to a calcified intervertebral disc in a patient with X-linked hypophosphatemic rickets: case report and review of the literature. Neurosurgery. 2002, 51, discussion 242–243. [Google Scholar] [CrossRef] [PubMed]
- García Martín, A.; Varsavsky, M.; Cortés Berdonces, M.; Ávila Rubio, V.; Alhambra Expósito, M.R.; Novo Rodríguez, C.; Rozas Moreno, P.; Romero Muñoz, M.; Jódar Gimeno, E.; Rodríguez Ortega, P.; Muñoz Torres, M. Phosphate disorders and clinical management of hypophosphatemia and hyperphosphatemia. Endocrinol Nutr (Engl Ed). 2019, 66, 383–395. [Google Scholar] [CrossRef] [PubMed]
- Emmens, J.E.; de Borst, M.H.; Boorsma, E.M.; Damman, K.; Navis, G.; van Veldhuisen, D.J.; et al. Assessment of proximal tubular function by tubular maximum phosphate reabsorption capacity in heart failure. Clin J Am Soc Nephrol. 2022, 17, 228–239. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



