3. Results
During the 9 years, 604 patients were classified as MCVs. Demographic details can be found in
Table 1 (Ethnicity/Gender/Count/Percentage of Total Patients/Average Age). The majority of patients were male (74.5%), while females comprised 25.5% of the study population. The average age of all patients was 42.2 years, with females tending to be older on average (49.0 years) compared to males (39.9 years).
In terms of ethnic distribution, the largest group was “Other” (49.5% of males, 12.4% of females), with a significant proportion identifying as Hispanic origin. Among males in “Other”, 35.3% were Hispanic, while 11.6% were non-Hispanic. White patients made up 8.8% of males and 5.6% of females, with an average age of 43.6 years and 53.1 years, respectively. The Asian subgroup accounted for 7.9% of males and 5.0% of females, with older average ages in the female group (56.6 years) compared to males (45.2 years). Black patients represented a smaller portion of the sample, with 3.97% of males and 0.5% of females, averaging 39.9 and 28.8 years, respectively. A minor percentage of patients identified as Native Hawaiian or Other Pacific Islander (0.33% for both males and females), with average ages ranging from 32.5 to 50.7 years.
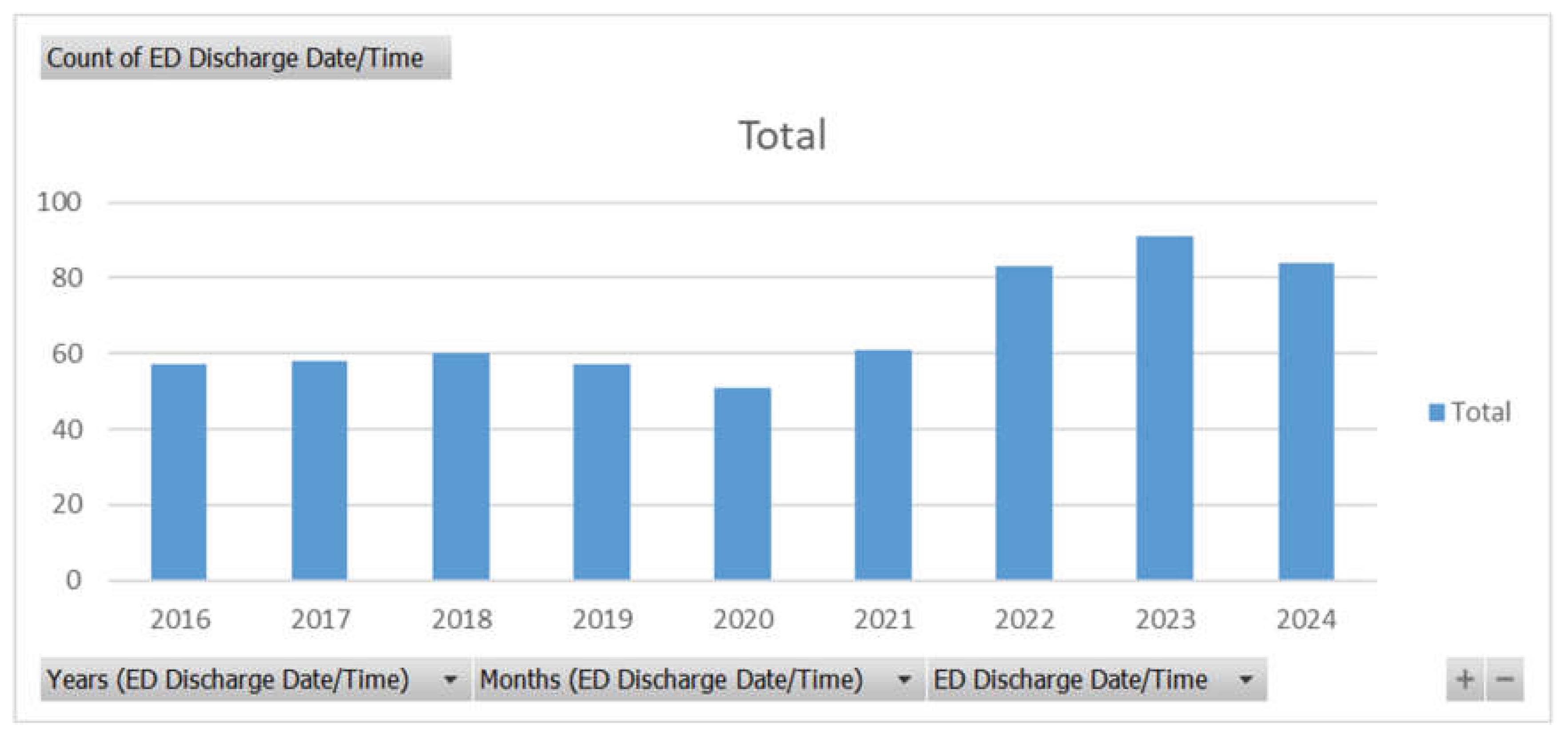
Figure 1.
Count of ED Discharge Patients related to MVCs from 2016 to 2024.
Figure 1.
Count of ED Discharge Patients related to MVCs from 2016 to 2024.
Out of a total of 602 patients, the number of ED discharge patients has increased in the previous years compared to before 2021. There is a drop in ED discharges in 2020, which might suggest the effect COVID had in reducing motor vehicle travel. However, before COVID, ED discharge patients were much less than in the years after COVID. This might suggest a shift in injury severity, practices in the ED, or an increase in vehicle traffic and unsafe motor vehicle travel.
Table 2.
This table represents the length of stay in the ED, ICU, and other units in the hospital. The average AIS head score and ISS score are reflected, with a distribution of trauma type.
Table 2.
This table represents the length of stay in the ED, ICU, and other units in the hospital. The average AIS head score and ISS score are reflected, with a distribution of trauma type.
| Hospital Stays |
Total |
Average |
Percentage |
| Days |
7799.00 |
13.04 |
|
| |
|
|
|
| Hours |
187662.84 |
104.61 |
100.00% |
| ED hours |
6295.25 |
10.53 |
3.35% |
| ICU hours |
67768.32 |
113.32 |
36.11% |
| Other hours |
113599.28 |
189.97 |
60.53% |
| |
|
|
|
| ED/HOSPITAL Initial Gcs Total |
6727.00 |
11.25 |
|
| |
|
|
|
| Injury Severity Score (ISS) |
13505.00 |
22.58 |
|
| |
|
|
|
| AIS Head |
2217.00 |
3.71 |
|
| |
|
|
|
| Trauma Type |
598.00 |
|
100.00% |
| Blunt |
597.00 |
|
99.83% |
| Penetrating |
1.00 |
|
0.17% |
Among the cohort, a total of 7,799 hospital days were recorded, with an average length of stay (LOS) of 13.04 days per patient. The majority of time spent in the hospital was distributed as follows: 60.53% in other inpatient units (113,599.28 hours), 36.11% in the ICU (67,768.32 hours), and only 3.35% in the Emergency Department (ED) (6,295.25 hours). This suggests that most patients required prolonged care beyond the ED, with a substantial portion requiring intensive care services. Patients presented with a total initial Glasgow Coma Scale (GCS) score sum of 6,727, averaging 11.25, indicating a moderately impaired level of consciousness at presentation. The average Injury Severity Score (ISS) was 22.58, consistent with severe trauma. The Abbreviated Injury Scale (AIS) Head score averaged 3.71, indicating that head injuries were common and generally moderate to severe. Out of 598 total trauma cases, 99.83% were blunt trauma, while only 0.17% were penetrating injuries, reflecting the predominance of MVCs and similar blunt-force mechanisms.
Table 3.
Patient Mortality and Discharge Disposition following Motor Vehicle Collisions.
Table 3.
Patient Mortality and Discharge Disposition following Motor Vehicle Collisions.
| Mortality |
Count of Patients |
Count of Signs of Life |
| Arrived with NO signs of life |
35 |
5.79% |
| Died as full code |
34 |
5.63% |
| Died unknown |
1 |
0.17% |
| Arrived with signs of life |
569 |
94.21% |
| blank |
1 |
0.17% |
| Died after withdrawal of care |
13 |
2.15% |
| Died as full code |
44 |
7.28% |
| Died with care, not begun DNR/DNI |
6 |
0.99% |
| Discharged to Home or Self-care (Routine Discharge) |
308 |
50.99% |
| Home with services |
20 |
3.31% |
| Homeless/Shelter |
1 |
0.17% |
| Hospice |
2 |
0.33% |
| Inpatient Psych Care |
1 |
0.17% |
| Inpatient Rehabilitation |
33 |
5.46% |
| Left AMA |
10 |
1.66% |
| Met brain death criteria |
17 |
2.81% |
| New placement at Skilled Nursing Facility |
13 |
2.15% |
| Other Acute Care Hospital Emergency Department |
14 |
2.32% |
| Other Acute Care Hospital In-Patient |
11 |
1.82% |
| Other Health Care Facility |
5 |
0.83% |
| Police Custody/Jail/Prison |
5 |
0.83% |
| Spinal Cord Injury Rehabilitation |
2 |
0.33% |
| Sub-Acute Inpatient Rehabilitation |
19 |
3.15% |
| Traumatic Brain Rehabilitation |
44 |
7.28% |
Among the 604 patients included in this analysis, 35 patients (5.79%) arrived at the hospital with no signs of life. Of these, 34 (5.63%) were confirmed deceased as full code, and 1 patient (0.17%) had an unknown cause of death. The majority of patients, 569 (94.21%), arrived with signs of life. Among this group, 63 patients (10.42%) died during hospitalization, with 44 (7.28%) dying as full code, 13 (2.15%) following the withdrawal of care, and 6 (0.99%) categorized as DNR/DNI, where care was not initiated. Seventeen patients (2.81%) met brain death criteria. Regarding discharge disposition, 308 patients (50.99%) were discharged home or to self-care, while 20 (3.31%) required home services. A small number of patients were discharged to alternative facilities or care pathways, including 33 (5.46%) to inpatient rehabilitation, 19 (3.15%) to sub-acute inpatient rehabilitation, and 44 (7.28%) to traumatic brain rehabilitation centers. Additionally, 13 patients (2.15%) were transferred to skilled nursing facilities, 14 (2.32%) to other acute care hospital emergency departments, and 11 (1.82%) to other acute care hospital inpatient units. Smaller proportions of patients were discharged to hospice, inpatient psychiatric care, other healthcare facilities, correctional facilities, or specialized rehabilitation centers. These findings highlight that while the majority of patients survived their injuries, a significant proportion required specialized or prolonged care, and mortality remained notable among those arriving with or without signs of life.
Table 4.
Regression Analysis: Helmet Use and Length of Stay.
Table 4.
Regression Analysis: Helmet Use and Length of Stay.
| Regression Statistics |
|
|
|
|
|
| Multiple R |
0.02898106 |
|
|
|
|
|
| R Square |
0.000839902 |
|
|
|
|
|
| Adjusted R Square |
-0.003032812 |
|
|
|
|
|
| Standard Error |
12.82906425 |
|
|
|
|
|
| Observations |
260 |
|
|
|
|
|
| ANOVA |
|
|
|
|
|
|
| |
df |
SS |
MS |
F |
Significance F |
|
| Regression |
1 |
35.69465009 |
35.69465009 |
0.216876836 |
0.641822872 |
|
| Residual |
258 |
42462.9015 |
164.5848895 |
|
|
|
| Total |
259 |
42498.59615 |
|
|
|
|
| |
Coefficients |
Standard Error |
t Stat |
P-value |
Lower 95% |
Upper 95% |
| Intercept |
8.678947368 |
0.930718143 |
9.325000741 |
5.21918E-18 |
6.846175912 |
10.51171882 |
| Helmet |
0.835338346 |
1.793724887 |
0.465700371 |
0.641822872 |
-2.696867187 |
4.367543879 |
A linear regression analysis was conducted to examine the relationship between helmet use and the outcome of interest across 260 observations. The model demonstrated a very low R-squared value of 0.00084, indicating that helmet use accounted for less than 1% of the variance in the length of stay. The overall regression model was not statistically significant, F(1, 258) = 0.217, p = 0.642. The coefficient for helmet use was 0.84 (p = 0.642), with a 95% confidence interval ranging from -2.70 to 4.37, suggesting no significant association between helmet use and the length of stay measured. The intercept was significant at 8.68 (p < 0.001), indicating the estimated length of stay when helmet use is absent. These findings suggest that helmet use, within this sample, did not significantly impact the measured outcome.
Table 5.
Regression Analysis: Helmet Use and Injury Severity Score.
Table 5.
Regression Analysis: Helmet Use and Injury Severity Score.
| Regression Statistics |
|
|
|
|
|
| Multiple R |
0.084340862 |
|
|
|
|
|
| R Square |
0.007113381 |
|
|
|
|
|
| Adjusted R Square |
0.003279842 |
|
|
|
|
|
| Standard Error |
12.50303003 |
|
|
|
|
|
| Observations |
261 |
|
|
|
|
|
| ANOVA |
|
|
|
|
|
|
| |
df |
SS |
MS |
F |
Significance F |
|
| Regression |
1 |
290.0726135 |
290.0726135 |
1.85556503 |
0.174321005 |
|
| Residual |
259 |
40488.37183 |
156.32576 |
|
|
|
| Total |
260 |
40778.44444 |
|
|
|
|
| |
Coefficients |
Standard Error |
t Stat |
P-value |
Lower 95% |
Upper 95% |
| Intercept |
19.8 |
0.907065134 |
21.82864191 |
1.22713E-60 |
18.01383858 |
21.58616142 |
| Helmet |
2.369014085 |
1.739120014 |
1.36219126 |
0.174321005 |
-1.055601146 |
5.793629315 |
A linear regression analysis was conducted to evaluate the relationship between helmet use and Injury Severity Score (ISS) among 261 patients. The model produced a low R² value of 0.0071, indicating that helmet use explained less than 1% of the variance in ISS. The overall regression was not statistically significant, F(1, 259) = 1.86, p = 0.17. The regression coefficient for helmet use was 2.37 (SE = 1.74), suggesting that helmet use was associated with an estimated increase of 2.37 points in ISS; however, this effect was not statistically significant (p = 0.17). The 95% confidence interval for the helmet coefficient ranged from -1.06 to 5.79, crossing zero, further indicating no reliable effect. The intercept was 19.80 (SE = 0.91, p < .001), representing the expected ISS when helmet use was absent. These results suggest that, within this sample, helmet use was not a significant predictor of injury severity as measured by ISS.
Table 6.
Regression Analysis: Helmet Use and Mortality.
Table 6.
Regression Analysis: Helmet Use and Mortality.
| Regression Statistics |
|
|
|
|
|
| Multiple R |
0.041703506 |
|
|
|
|
|
| R Square |
0.001739182 |
|
|
|
|
|
| Adjusted R Square |
-0.002115106 |
|
|
|
|
|
| Standard Error |
0.324486507 |
|
|
|
|
|
| Observations |
261 |
|
|
|
|
|
| ANOVA |
|
|
|
|
|
|
| |
df |
SS |
MS |
F |
Significance F |
|
| Regression |
1 |
0.047510999 |
0.047510999 |
0.451233023 |
0.502348714 |
|
| Residual |
259 |
27.27049666 |
0.105291493 |
|
|
|
| Total |
260 |
27.31800766 |
|
|
|
|
| |
Coefficients |
Standard Error |
t Stat |
P-value |
Lower 95% |
Upper 95% |
| Intercept |
0.110526316 |
0.023540725 |
4.695110874 |
4.32421E-06 |
0.06417073 |
0.156881901 |
| Helmet |
0.030318755 |
0.045134737 |
0.671738806 |
0.502348714 |
-0.058559016 |
0.119196525 |
A linear regression analysis was performed to examine the relationship between helmet use and mortality in motor vehicle crashes. The model explained very little of the variance in mortality (R² = 0.0017), with an adjusted R² of -0.0021, indicating that helmet use was not a meaningful predictor of mortality in this sample of 261 observations. The overall regression was not statistically significant (F(1, 259) = 0.45, p = 0.50). The coefficient for helmet use was positive but not significant (β = 0.03, SE = 0.045, t = 0.67, p = 0.50), suggesting no evidence of an association between helmet use and mortality after controlling for the intercept. The intercept was significant (β = 0.11, p < 0.001), representing the baseline mortality level when helmet use is absent.
Table 7.
Regression Analysis: Blood Alcohol Concentration and Injury Severity Score.
Table 7.
Regression Analysis: Blood Alcohol Concentration and Injury Severity Score.
| Regression Statistics |
|
|
|
|
|
| Multiple R |
0.014229126 |
|
|
|
|
|
| R Square |
0.000202468 |
|
|
|
|
|
| Adjusted R Square |
-0.001805158 |
|
|
|
|
|
| Standard Error |
10.97887658 |
|
|
|
|
|
| Observations |
500 |
|
|
|
|
|
| ANOVA |
|
|
|
|
|
|
| |
df |
SS |
MS |
F |
Significance F |
|
| Regression |
1 |
12.15596746 |
12.15596746 |
0.100849494 |
0.750945686 |
|
| Residual |
498 |
60026.79403 |
120.535731 |
|
|
|
| Total |
499 |
60038.95 |
|
|
|
|
| |
Coefficients |
Standard Error |
t Stat |
P-value |
Lower 95% |
Upper 95% |
| Intercept |
21.38403956 |
0.593634461 |
36.02223414 |
8.6128E-141 |
20.21770279 |
22.55037632 |
| ETOH Level |
0.001388116 |
0.004371081 |
0.317568093 |
0.750945686 |
-0.007199918 |
0.00997615 |
A linear regression was conducted to assess the association between ETOH Level and Injury Severity Score (ISS) in 500 cases. The model explained a negligible amount of variance in ISS (R² = 0.0002), with an adjusted R² of -0.0018, indicating that ETOH level did not meaningfully predict injury severity. The overall regression was not statistically significant (F(1, 498) = 0.10, p = 0.75). The coefficient for ETOH level was positive but not statistically significant (β = 0.0014, SE = 0.0044, t = 0.32, p = 0.75), suggesting no evidence of an association between ETOH level and injury severity in this sample. The intercept was significant (β = 21.38, p < 0.001), representing the average injury severity score when ETOH level is zero. In conclusion, ETOH level was not a significant predictor of injury severity in this dataset.
Table 8.
Regression Analysis: ETOH Level and Hospital Length of Stay.
Table 8.
Regression Analysis: ETOH Level and Hospital Length of Stay.
| Regression Statistics |
|
|
|
|
|
| Multiple R |
0.051681003 |
|
|
|
|
|
| R Square |
0.002670926 |
|
|
|
|
|
| Adjusted R Square |
0.000660182 |
|
|
|
|
|
| Standard Error |
27.05380799 |
|
|
|
|
|
| Observations |
498 |
|
|
|
|
|
| ANOVA |
|
|
|
|
|
|
| |
df |
SS |
MS |
F |
Significance F |
|
| Regression |
1 |
972.2139861 |
972.2139861 |
1.328327175 |
0.249658193 |
|
| Residual |
496 |
363026.6294 |
731.908527 |
|
|
|
| Total |
497 |
363998.8434 |
|
|
|
|
| |
Coefficients |
Standard Error |
t Stat |
P-value |
Lower 95% |
Upper 95% |
| Intercept |
15.89969566 |
1.464958994 |
10.85333837 |
9.08876E-25 |
13.02140534 |
18.77798598 |
| ETOH Level |
-0.012445909 |
0.010798765 |
-1.15253077 |
0.249658193 |
-0.033662872 |
0.008771054 |
A linear regression analysis was conducted to evaluate the relationship between ETOH level and hospital length of stay (LOS) in 498 patients. The model explained a very small portion of the variance in LOS (R² = 0.0027), with an adjusted R² of 0.0007, suggesting minimal explanatory power. The regression model was not statistically significant (F(1, 496) = 1.33, p = 0.25). The coefficient for ETOH level was negative but not statistically significant (β = -0.012, SE = 0.011, t = -1.15, p = 0.25), indicating no meaningful association between ETOH level and hospital LOS. The intercept was statistically significant (β = 15.90, p < 0.001), representing the expected LOS when ETOH level is zero. In summary, ETOH level was not a significant predictor of hospital length of stay in this dataset.
Table 9.
Regression Analysis: ETOH Level and Mortality.
Table 9.
Regression Analysis: ETOH Level and Mortality.
| Regression Statistics |
|
|
|
|
|
| Multiple R |
0.027908509 |
|
|
|
|
|
| R Square |
0.000778885 |
|
|
|
|
|
| Adjusted R Square |
-0.00123162 |
|
|
|
|
|
| Standard Error |
0.334916813 |
|
|
|
|
|
| Observations |
499 |
|
|
|
|
|
| ANOVA |
|
|
|
|
|
|
| |
df |
SS |
MS |
F |
Significance F |
|
| Regression |
1 |
0.043455219 |
0.043455219 |
0.387407518 |
0.533950731 |
|
| Residual |
497 |
55.74812795 |
0.112169272 |
|
|
|
| Total |
498 |
55.79158317 |
|
|
|
|
| |
Coefficients |
Standard Error |
t Stat |
P-value |
Lower 95% |
Upper 95% |
| Intercept |
0.12193493 |
0.018109157 |
6.733330088 |
4.59084E-11 |
0.086354989 |
0.15751487 |
| ETOH Level |
8.317E-05 |
0.000133623 |
0.622420692 |
0.533950731 |
-0.000179366 |
0.000345706 |
A linear regression analysis was performed to examine the relationship between ETOH level and the outcome variable in a sample of 499 observations. The model accounted for a negligible portion of the variance (R² = 0.0008), with an adjusted R² of -0.0012, indicating no meaningful predictive power. The regression was not statistically significant (F(1, 497) = 0.39, p = 0.53). The coefficient for ETOH level was extremely small and not statistically significant (β = 0.000083, SE = 0.000134, t = 0.62, p = 0.53), suggesting no association between ETOH level and the outcome. The intercept was statistically significant (β = 0.122, p < 0.001), representing the expected value of the outcome when ETOH level is zero. In conclusion, ETOH level was not a significant predictor of the outcome in this dataset.
Table 10.
Table of Primary Payor Source by ED Disposition.
Table 10.
Table of Primary Payor Source by ED Disposition.
| Table of Primary Payor Source by ED Disposition |
Table of Primary Payor Source by ED Disposition |
| Primary Payor Source(Primary Payor Source) |
ED Disposition(ED Disposition) |
| Admitted |
Died in ED |
Died on Arrival |
Died within 15 minutes |
Discharged to Home or Self-care (Routine Discharge) |
Not Applicable |
Transferred to Another Hospital Emergency Dept. |
Total |
| |
1 |
0 |
0 |
0 |
0 |
0 |
0 |
. |
| unk |
7 |
5 |
4 |
2 |
0 |
0 |
4 |
22 |
| Auto |
16 |
0 |
0 |
0 |
0 |
0 |
0 |
16 |
| Blue Cross |
11 |
0 |
1 |
0 |
0 |
0 |
0 |
12 |
| Commercial |
97 |
0 |
1 |
1 |
1 |
0 |
4 |
104 |
| Corrections |
2 |
0 |
0 |
0 |
0 |
0 |
0 |
2 |
| HMO |
1 |
0 |
0 |
0 |
0 |
0 |
0 |
1 |
| Managed Care |
4 |
0 |
0 |
0 |
0 |
0 |
0 |
4 |
| Medicaid |
150 |
2 |
5 |
0 |
3 |
0 |
1 |
161 |
| Medicare |
26 |
2 |
1 |
0 |
0 |
0 |
0 |
29 |
| No Fault |
104 |
0 |
2 |
1 |
1 |
0 |
3 |
111 |
| None |
43 |
3 |
5 |
2 |
2 |
1 |
0 |
56 |
| Other Govmt |
3 |
0 |
0 |
0 |
0 |
0 |
0 |
3 |
| Other |
40 |
5 |
1 |
4 |
1 |
0 |
1 |
52 |
| Self Pay |
16 |
3 |
3 |
0 |
0 |
0 |
1 |
23 |
| Workers Comp |
7 |
0 |
0 |
0 |
0 |
0 |
0 |
7 |
| Total |
527 |
20 |
23 |
10 |
8 |
1 |
14 |
603 |
| Frequency Missing = 1 |
| Statistic |
DF |
Value |
Prob |
| WARNING: 88% of the cells have expected counts less |
| Than 5. Chi-Square may not be a valid test. |
| Chi-Square |
84 |
158.9329 |
<.0001 |
| Likelihood Ratio Chi-Square |
84 |
124.8594 |
0.0026 |
| Mantel-Haenszel Chi-Square |
1 |
1.0929 |
0.2958 |
| Phi Coefficient |
|
0.5134 |
|
| Contingency Coefficient |
|
0.4567 |
|
| Cramer's V |
|
0.2096 |
|
| Fisher's Exact Test |
| Table Probability (P) |
<.0001 |
| Monte Carlo Estimate for the Exact Test |
| Pr <= P |
<.0001 |
| 99% Lower Conf Limit |
<.0001 |
| 99% Upper Conf Limit |
0.0005 |
| |
|
| Number of Samples |
10000 |
| Initial Seed |
610796875 |
A contingency analysis was performed to examine the association between Primary Payor Source and Emergency Department (ED) Disposition in 603 patients. The overall relationship between payor source and ED disposition was found to be statistically significant. The chi-square test revealed a significant association between payor type and ED disposition (χ²(84) = 158.93, p < .0001). However, 88% of the cells had expected counts less than 5, indicating that the assumptions for the chi-square test were not fully met. To account for this, Fisher’s Exact Test using Monte Carlo simulation was conducted, which also showed a statistically significant association (p < .0001, 99% CI: <.0001 to 0.0005). The strength of association was small to moderate, as reflected by Cramer's V = 0.21. These findings suggest that a patient's primary payor source is significantly associated with their ED disposition, though the strength of this association is limited.