Submitted:
30 July 2025
Posted:
11 August 2025
You are already at the latest version
Abstract

Keywords:
1. Introduction
2. Materials and Methods
2.1. Experimental Animals
2.2. Reagents and Materials
2.3. Methods
2.3.1. Animal Model, Grouping, and Treatment
2.3.2. Blood Glucose Measurement
2.3.3. Serum Lipid and Liver Function Analysis
2.3.4. Body Weight and Liver Index Measurement
2.3.5. Histopathological Evaluation of Liver Tissues
2.3.6. Western Blot Analysis of PGC-1α and ERRα in Liver Tissue
2.3.7. Immunofluorescence Double-Staining for PGC-1α and ERRα
2.3.8. ChIP-PCR to Validate PGC-1α Binding to ERRα
2.4. Statistical Analysis
3. Results
3.1. FBG, FINS, and HOMA-IR Levels in Each Group
| Group | FBG (mmol/L) | FINS (mU/L) | HOMA-IR |
|---|---|---|---|
| Control | 5.73 ± 0.61 | 7.75 ± 0.76 | 1.97 ± 0.16 |
| Model | 27.69 ± 2.83* | 17.08 ± 1.69* | 21.02 ± 2.07* |
| E2 | 12.55 ± 1.19# | 10.88 ± 1.41# | 6.07 ± 0.59# |
| E2+siNC | 13.06 ± 1.27a | 10.64 ± 1.03a | 6.18 ± 0.73a |
| E2+siPGC-1α | 29.47 ± 2.90*b | 18.19 ± 1.82*b | 23.82 ± 2.43*b |
3.2. Serum Lipids and Liver Function Indicators
| Group | TC(mmol/L) | TG(mmol/L) | LDL-C(mmol/L) | ALT(U/L) | AST (U/L) |
|---|---|---|---|---|---|
| Control | 3.56±0.34 | 1.22±0.13 | 0.37±0.04 | 79.50±7.88 | 122.84±13.31 |
| Model | 8.15±0.82* | 3.57±0.36* | 1.12±0.13* | 178.36±17.23* | 267.91±25.48* |
| E2 | 6.04±0.57# | 1.92±0.18# | 0.71±0.09# | 97.13±9.92# | 185.39±19.34# |
| E2+siNC | 6.12±0.63 | 1.99±0.17 | 0.74±0.07 | 99.48±10.06 | 187.66±19.23 |
| E2+siPGC-1α | 8.71±0.89△ | 3.61±0.38△ | 1.16±0.11△ | 180.52±17.94△ | 265.79±25.87△ |
3.3. Body Weight and Liver Index in Each Group
| Group | TC (mmol/L) | TG (mmol/L) | LDL-C (mmol/L) | ALT (U/L) | AST (U/L) |
|---|---|---|---|---|---|
| Control | 3.56 ± 0.34 | 1.22 ± 0.13 | 0.37 ± 0.04 | 79.50 ± 7.88 | 122.84 ± 13.17 |
| Model | 8.15 ± 0.82* | 3.57 ± 0.36* | 1.12 ± 0.13* | 184.36 ± 20.87* | 267.91 ± 25.41* |
| E2 | 6.04 ± 0.57# | 1.92 ± 0.18# | 0.71 ± 0.09# | 97.33 ± 8.72# | 160.98 ± 19.47# |
| E2+siNC | 6.12 ± 0.63a | 1.99 ± 0.17a | 0.73 ± 0.10a | 99.48 ± 6.01a | 162.20 ± 17.39a |
| E2+siPGC-1α | 8.71 ± 0.89*b | 3.61 ± 0.38*b | 1.16 ± 0.11*b | 180.52 ± 17.94*b | 265.79 ± 25.87*b |
| Group | Body weight (g) | Liver/body weight (%) |
|---|---|---|
| Control | 22.47 ± 2.34a | 4.08 ± 0.39a |
| Model | 27.08 ± 2.81* | 6.30 ± 0.56* |
| E2 | 22.54 ± 2.17# | 4.32 ± 0.41# |
| E2+siNC | 23.11 ± 2.06a | 4.37 ± 0.44a |
| E2+siPGC-1α | 28.23 ± 2.93*b | 6.71 ± 0.74*b |
3.4. Histopathological Changes in Liver Tissues
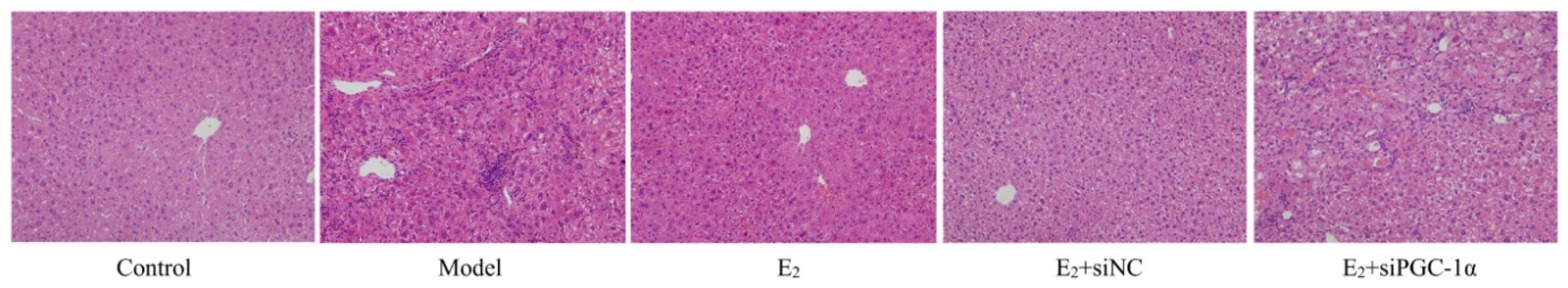
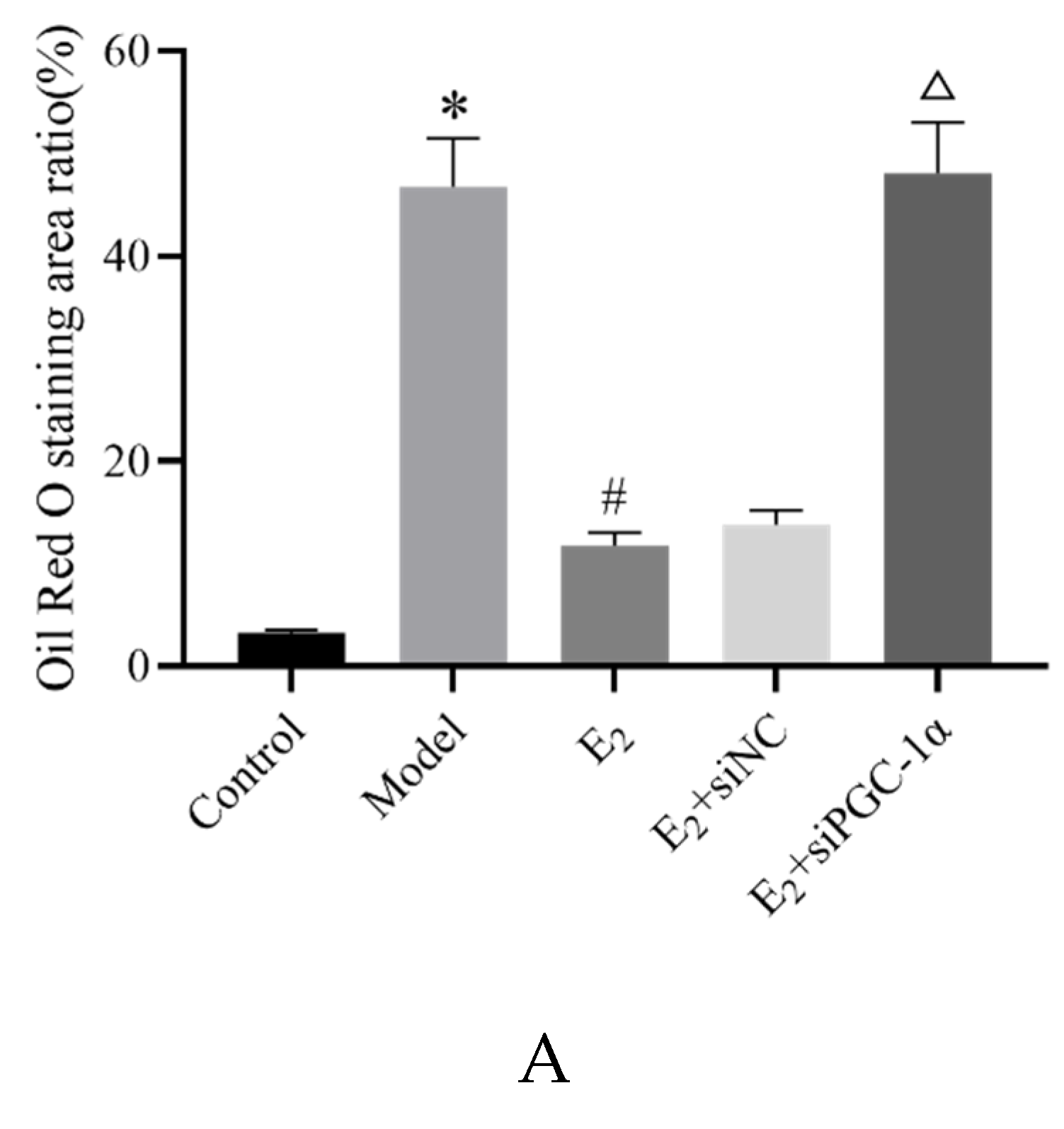
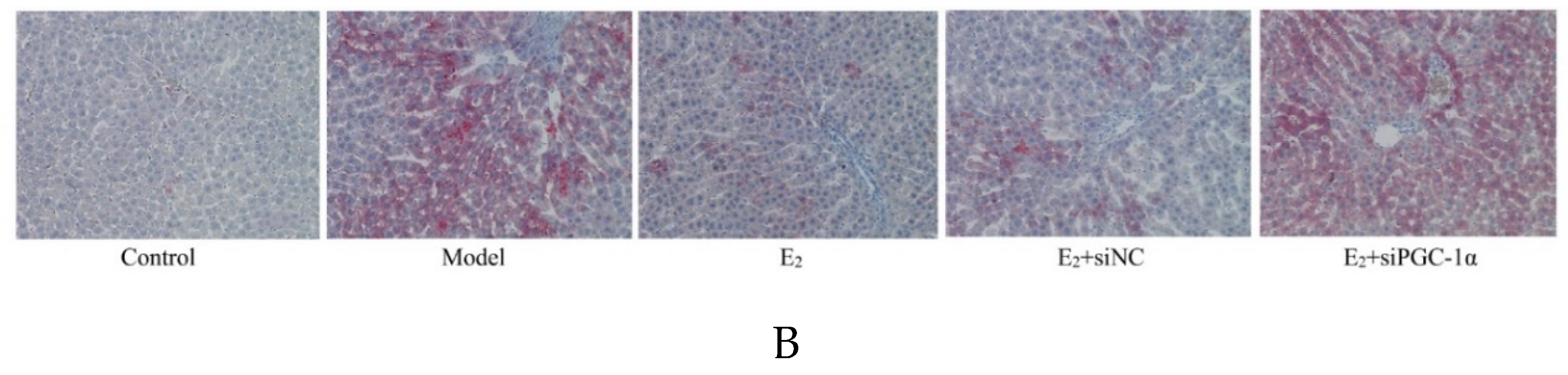
3.5. Protein Expression of the PGC-1α/ERRα Signaling Axis in Liver Tissues
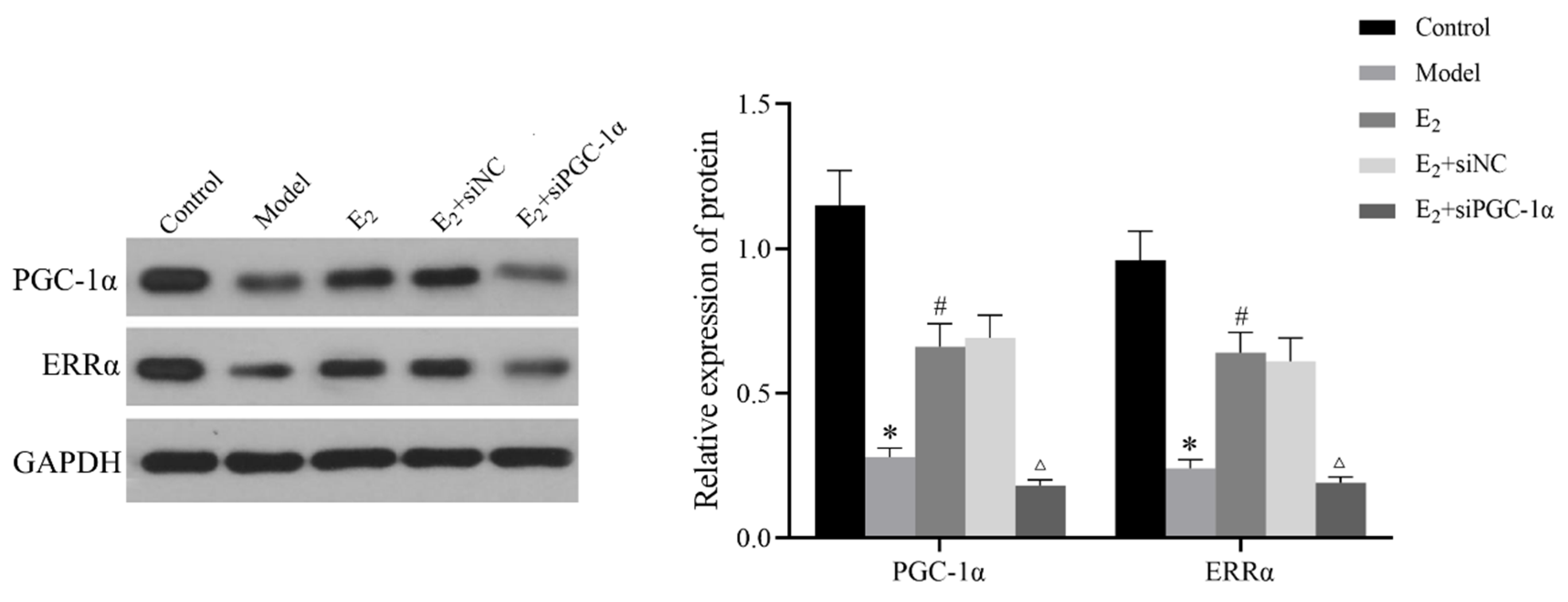
3.6. Interaction Between PGC-1α and ERRα
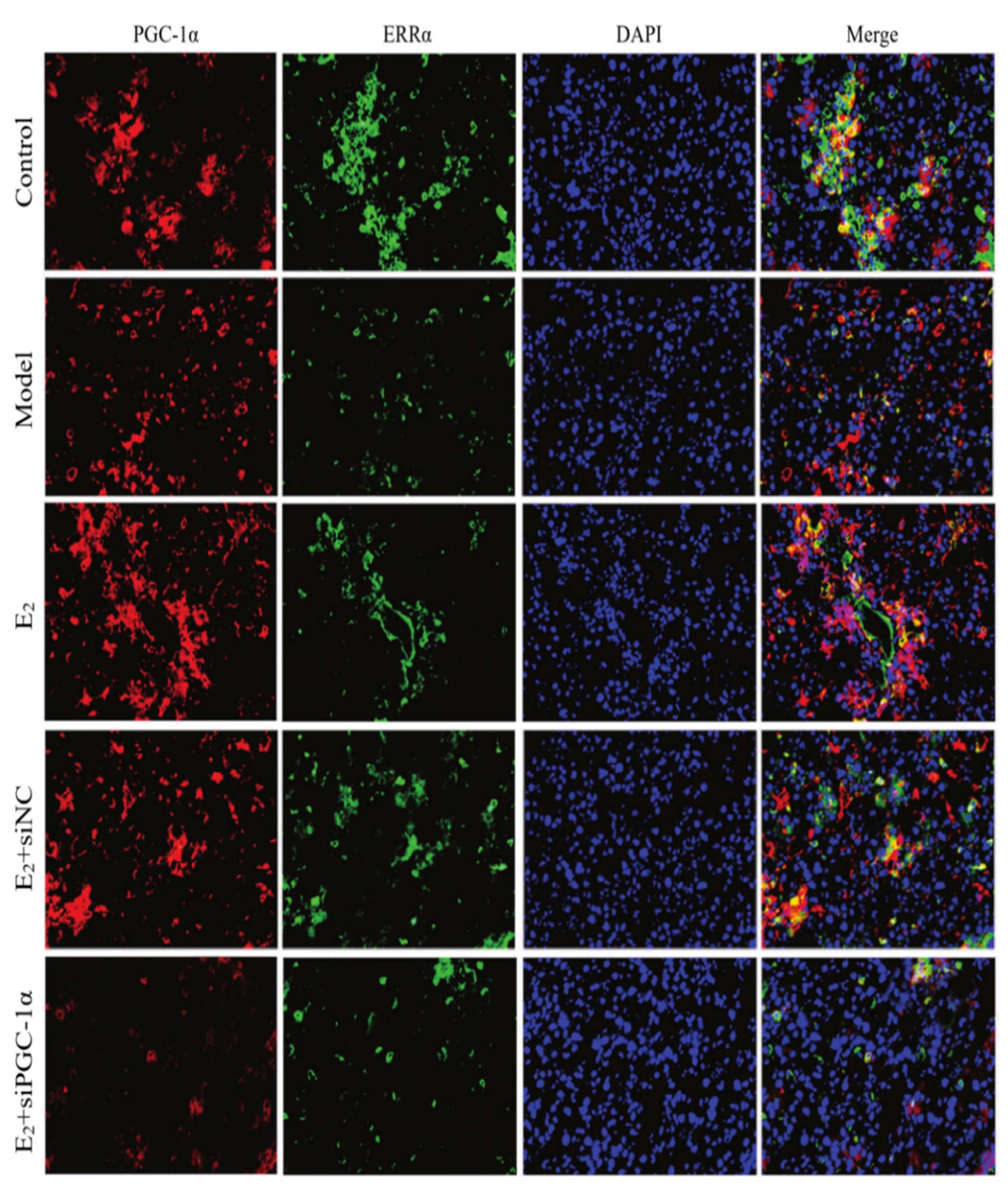
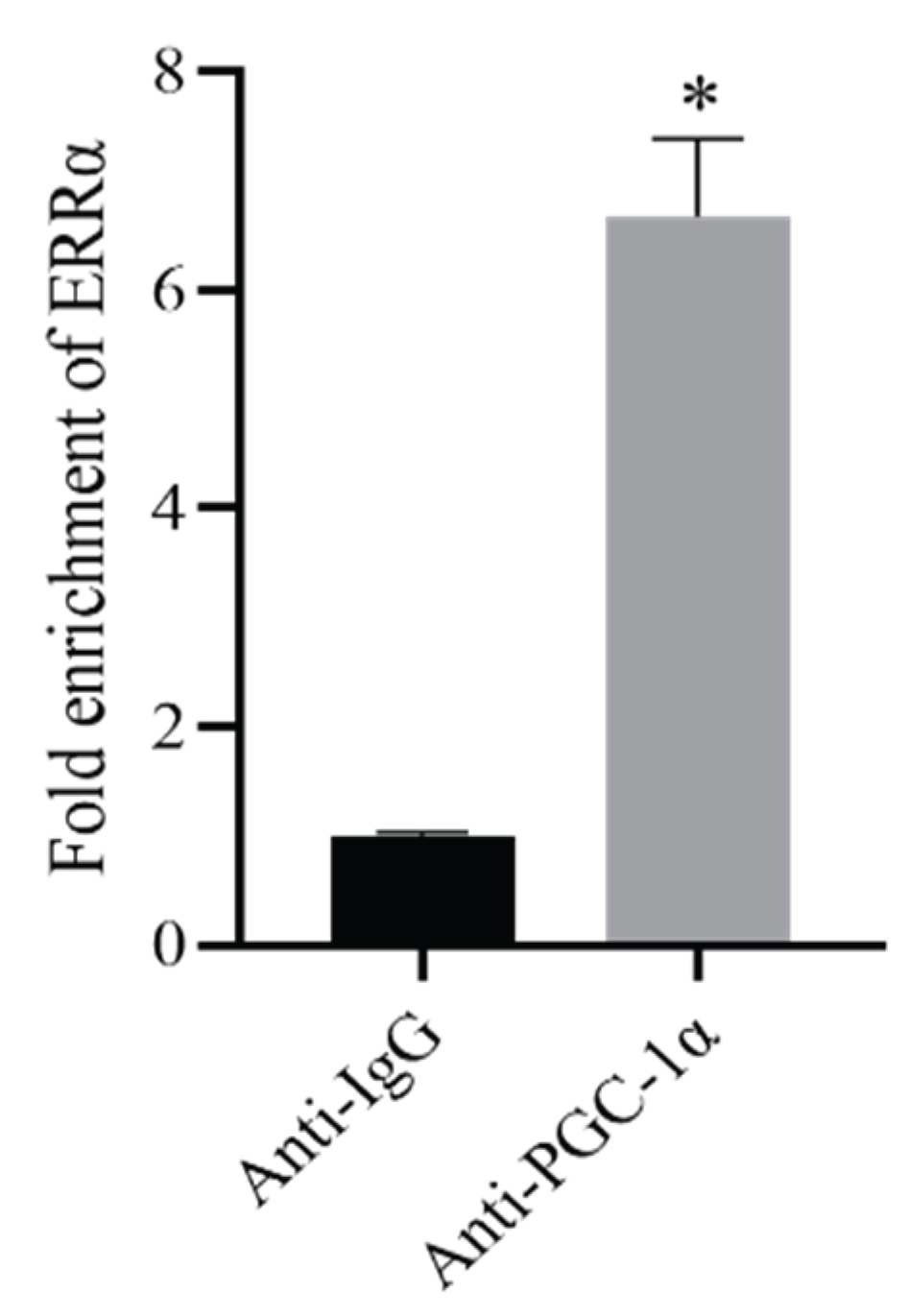
4. Discussion
Institutional Review Board Statement
References
- Bonnefond A, Florez JC, Loos RJF, et al. Dissection of type 2 diabetes: a genetic perspective. Lancet Diabetes Endocrinol 2025, 13, 149–164. [Google Scholar] [CrossRef] [PubMed]
- Younossi ZM, Golabi P, Price JK, et al. The global epidemiology of nonalcoholic fatty liver disease and nonalcoholic steatohepatitis among patients with type 2 diabetes. Clin Gastroenterol Hepatol 2024, 22, 1999–2010.e8. [Google Scholar] [CrossRef] [PubMed]
- Paraschou EM, Shalit A, Paschou SA. Non-alcoholic fatty liver disease in patients with type 2 diabetes: diagnostic and therapeutic considerations. Hormones (Athens) 2024, 23, 415–417. [Google Scholar] [CrossRef] [PubMed]
- Guo X, Yin X, Liu Z, et al. Non-alcoholic fatty liver disease (NAFLD) pathogenesis and natural products for prevention and treatment. Int J Mol Sci 2022, 23, 15489. [Google Scholar] [CrossRef]
- Targher G, Corey KE, Byrne CD, et al. The complex link between NAFLD and type 2 diabetes mellitus - mechanisms and treatments. Nat Rev Gastroenterol Hepatol 2021, 18, 599–612. [Google Scholar] [CrossRef]
- Mauvais-Jarvis F, Lindsey SH. Metabolic benefits afforded by estradiol and testosterone in both sexes: clinical considerations. J Clin Invest 2024, 134, e180073. [Google Scholar] [CrossRef]
- Zhang Y, Liu M, Yu D, et al. 17β-estradiol ameliorates postoperative cognitive dysfunction in aged mice via miR-138-5p/SIRT1/HMGB1 pathway. Int J Neuropsychopharmacol 2024, 27, pyae054. [Google Scholar] [CrossRef]
- Galmés-Pascual BM, Martínez-Cignoni MR, Morán-Costoya A, et al. 17β-estradiol ameliorates lipotoxicity-induced hepatic mitochondrial oxidative stress and insulin resistance. Free Radic Biol Med 2020, 150, 148–160. [CrossRef]
- Nomura K, Kinoshita S, Mizusaki N, et al. Adaptive gene expression of alternative splicing variants of PGC-1α regulates whole-body energy metabolism. Mol Metab, 2024, 86, 101968. [Google Scholar] [CrossRef]
- Nakadai T, Shimada M, Ito K, et al. Two target gene activation pathways for orphan ERR nuclear receptors. Cell Res 2023, 33, 165–183. [Google Scholar] [CrossRef]
- El Kebbaj R, Andreoletti P, El Hajj HI, et al. Argan oil prevents down-regulation induced by endotoxin on liver fatty acid oxidation and gluconeogenesis and on peroxisome proliferator-activated receptor gamma coactivator-1α, (PGC-1α), peroxisome proliferator-activated receptor α (PPARα) and estrogen related receptor α (ERRα). Biochim Open, 2015, 1, 51–59. [Google Scholar] [CrossRef]
- Guo T, Yan W, Cui X, et al. Liraglutide attenuates type 2 diabetes mellitus-associated non-alcoholic fatty liver disease by activating AMPK/ACC signaling and inhibiting ferroptosis. Mol Med 2023, 29, 132. [Google Scholar] [CrossRef]
- Tian Y, Hong X, Xie Y, et al. 17β-Estradiol (E2) upregulates the ERα/SIRT1/PGC-1α signaling pathway and protects mitochondrial function to prevent bilateral oophorectomy (OVX)-induced nonalcoholic fatty liver disease (NAFLD). Antioxidants (Basel) 2023, 12, 2100. [Google Scholar] [CrossRef]
- Zhao X, An X, Yang C, et al. The crucial role and mechanism of insulin resistance in metabolic disease. Front Endocrinol (Lausanne), 2023, 14, 1149239. [Google Scholar] [CrossRef] [PubMed]
- Portincasa P, Khalil M, Mahdi L, et al. Metabolic dysfunction-associated steatotic liver disease: from pathogenesis to current therapeutic options. Int J Mol Sci 2024, 25, 5640. [Google Scholar] [CrossRef]
- Muzurović EM, Volčanšek Š, Tomšić KZ, et al. Glucagon-like peptide-1 receptor agonists and dual glucose-dependent insulinotropic polypeptide/glucagon-like peptide-1 receptor agonists in the treatment of obesity/metabolic syndrome, prediabetes/diabetes and non-alcoholic fatty liver disease-current evidence. J Cardiovasc Pharmacol Ther, 2022, 27, 10742484221146371. [Google Scholar] [CrossRef]
- Xiao X, Kennelly JP, Feng AC, et al. Aster-B-dependent estradiol synthesis protects female mice from diet-induced obesity. J Clin Invest 2024, 134, e173002. [Google Scholar] [CrossRef]
- Yokota-Nakagi N, Omoto S, Tazumi S, et al. Estradiol replacement improves high-fat diet-induced insulin resistance in ovariectomized rats. Physiol Rep 2022, 10, e15193. [Google Scholar] [CrossRef]
- Lv Y, Zhang S, Weng X, et al. Estrogen deficiency accelerates postmenopausal atherosclerosis by inducing endothelial cell ferroptosis through inhibiting NRF2/GPX4 pathway. FASEB J 2023, 37, e22992. [Google Scholar] [CrossRef]
- Hong W, Zeng X, Wang H, et al. PGC-1α loss promotes mitochondrial protein lactylation in acetaminophen-induced liver injury via the LDHB-lactate axis. Pharmacol Res, 2024, 205, 107228. [Google Scholar] [CrossRef]
- Cheng D, Zhang M, Zheng Y, et al. α-Ketoglutarate prevents hyperlipidemia-induced fatty liver mitochondrial dysfunction and oxidative stress by activating the AMPK-pgc-1α/Nrf2 pathway. Redox Biol, 2024, 74, 103230. [Google Scholar] [CrossRef]
- Billon C, Schoepke E, Avdagic A, et al. A synthetic ERR agonist alleviates metabolic syndrome. J Pharmacol Exp Ther 2024, 388, 232–240. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




