Submitted:
01 August 2025
Posted:
04 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Pressure-Sensing Mats: Principles and Application
2.1. Operating Principle and Applications
2.2. From Individual Sensors to Textile Matrices
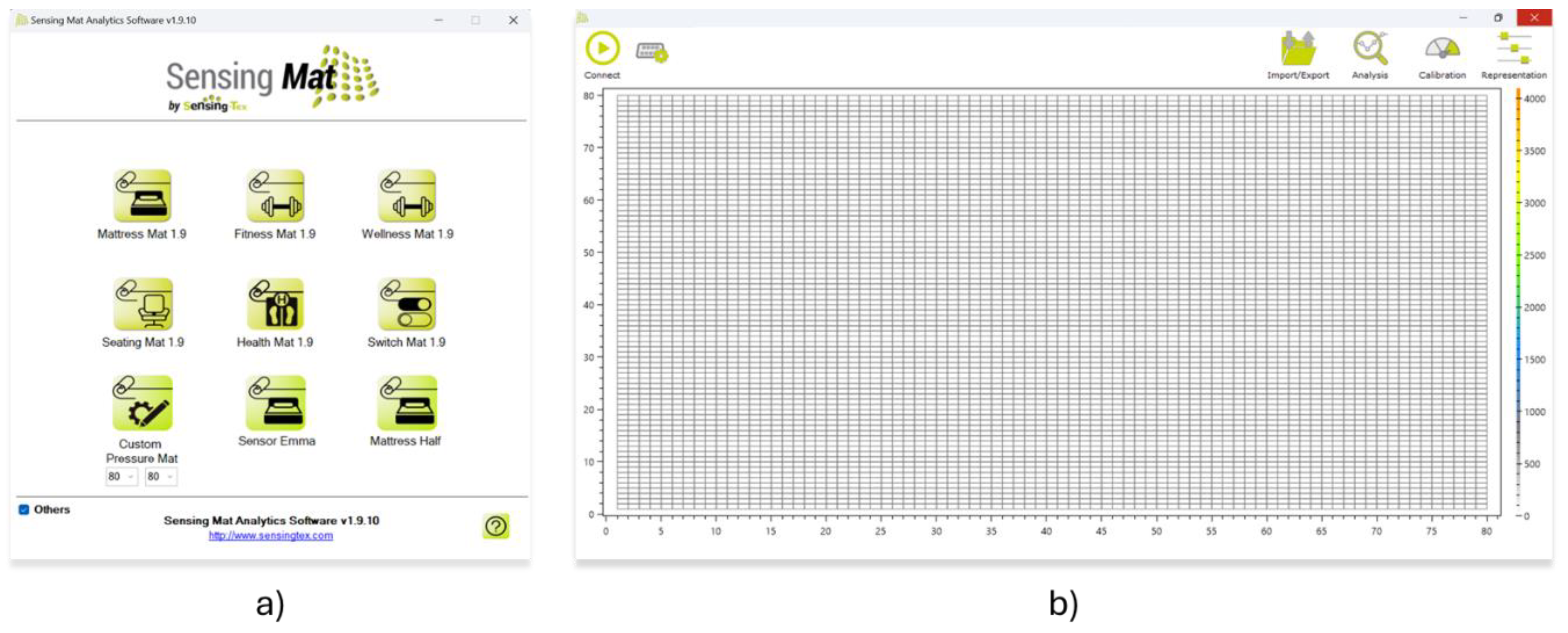
2.3. Data Acquisition System Used in This Study
- Physical Dimensions: 1000 × 1000 mm.
- Sensing Area: 950 × 950 mm
- Matrix Resolution: 80 × 80 sensors, totaling 6,400 measurement points
- Spatial Resolution: Approximately 11.87 mm center-to-center distance between sensors
- Optimized Pressure Range: At the specific request of this project, the mats were calibrated for optimal performance with weights ranging from 5 to 10 kg, corresponding to the target infant population
- Measurement Resolution: The internal analogue-to-digital converter (ADC) operates at 12 bits, providing 4096 distinct pressure levels per sensor
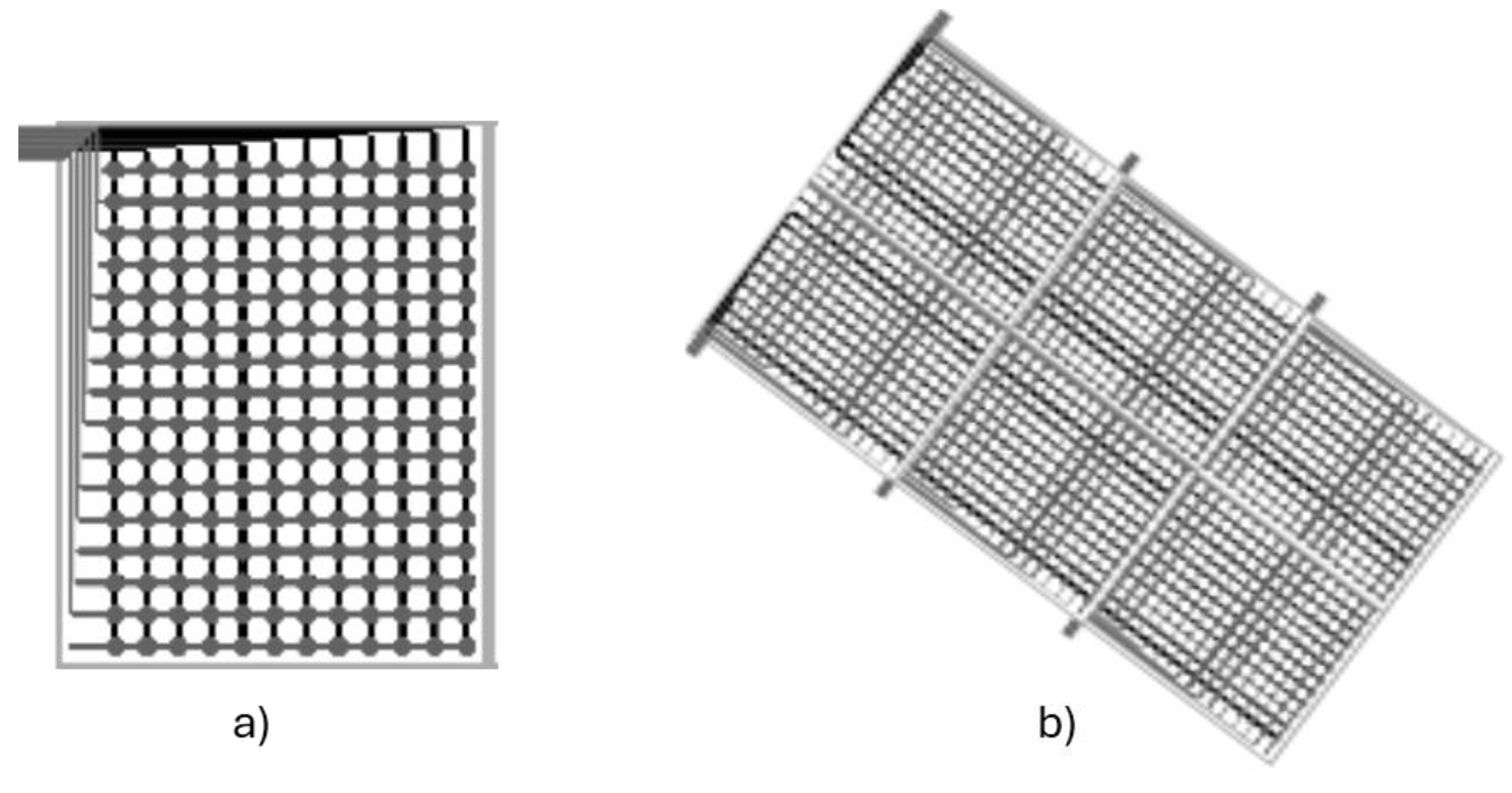
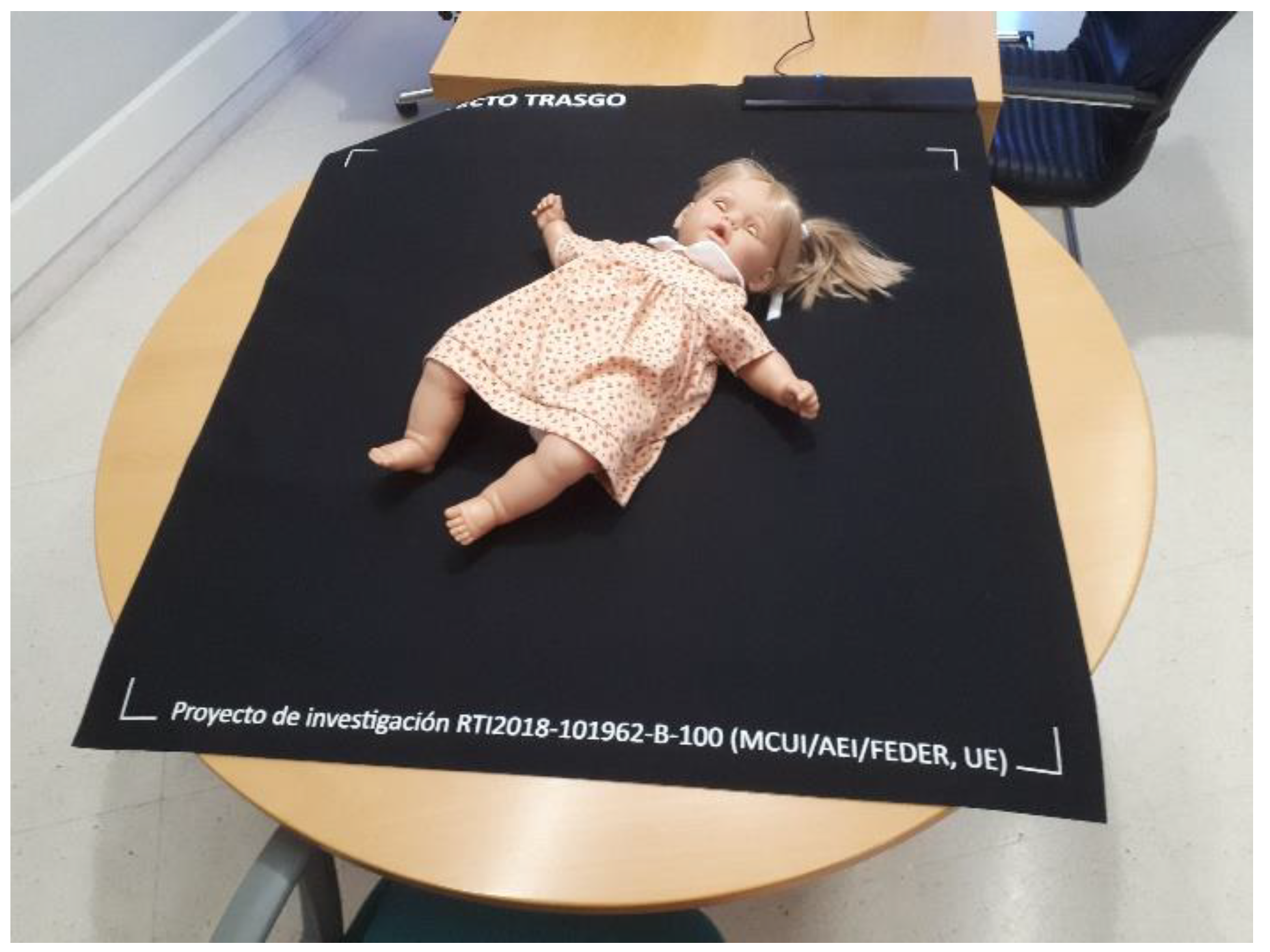
- Materials: Neoprene top layer and anti-slip base (see Figure 4)
- Sampling Frequency: Data acquisition was performed via the USB interface. Although the manufacturer specifies a rate of 5 Hz, empirical measurements taken from the captured data revealed an effective sampling rate between 10 and 11 Hz
3. Data Collection
3.1. Data Obtained
- Pressure imprint file, capturing the data recorded by the mat
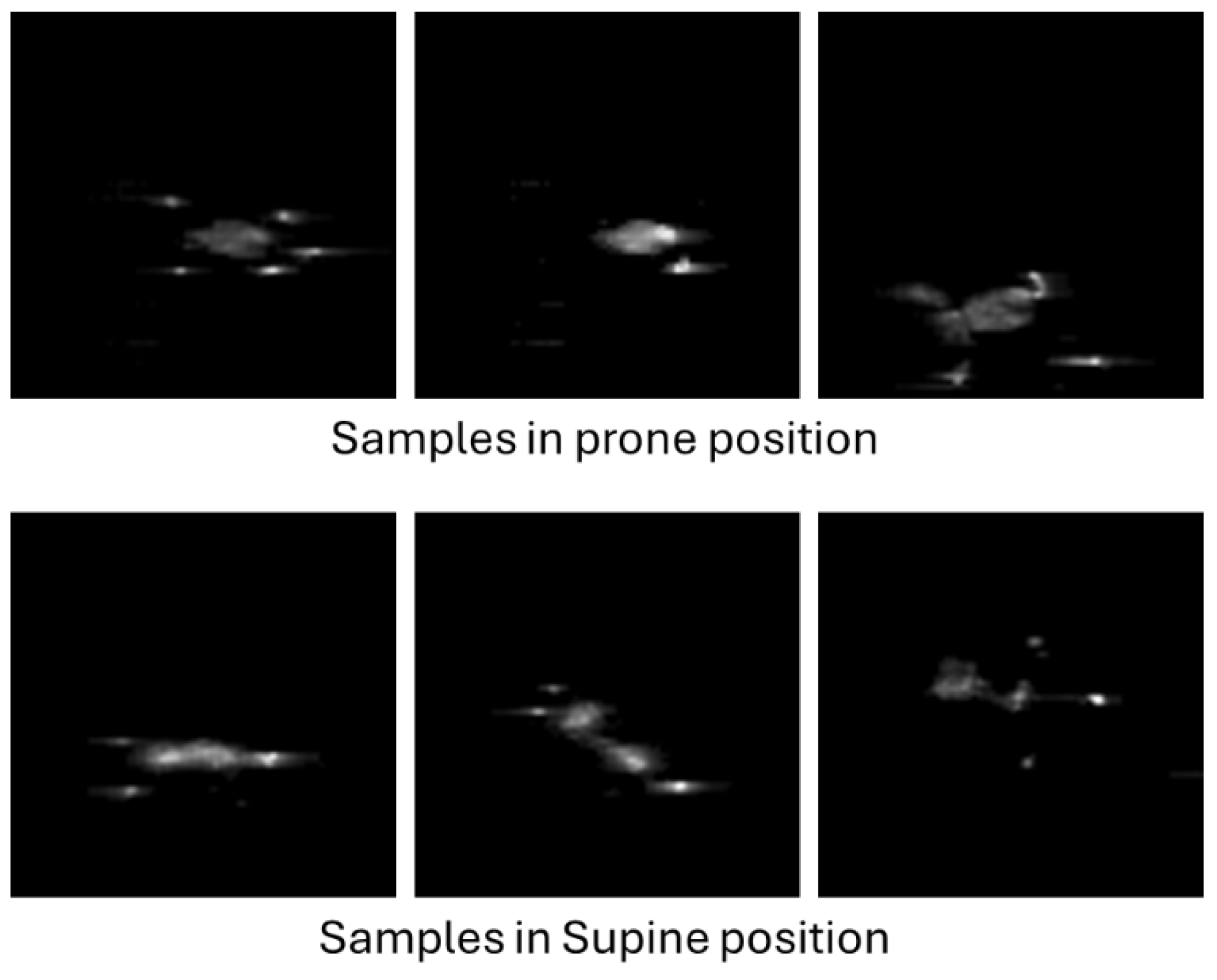
- Timestamp and position annotation file, marking the time intervals during which the infant remained in each posture (prone or supine)
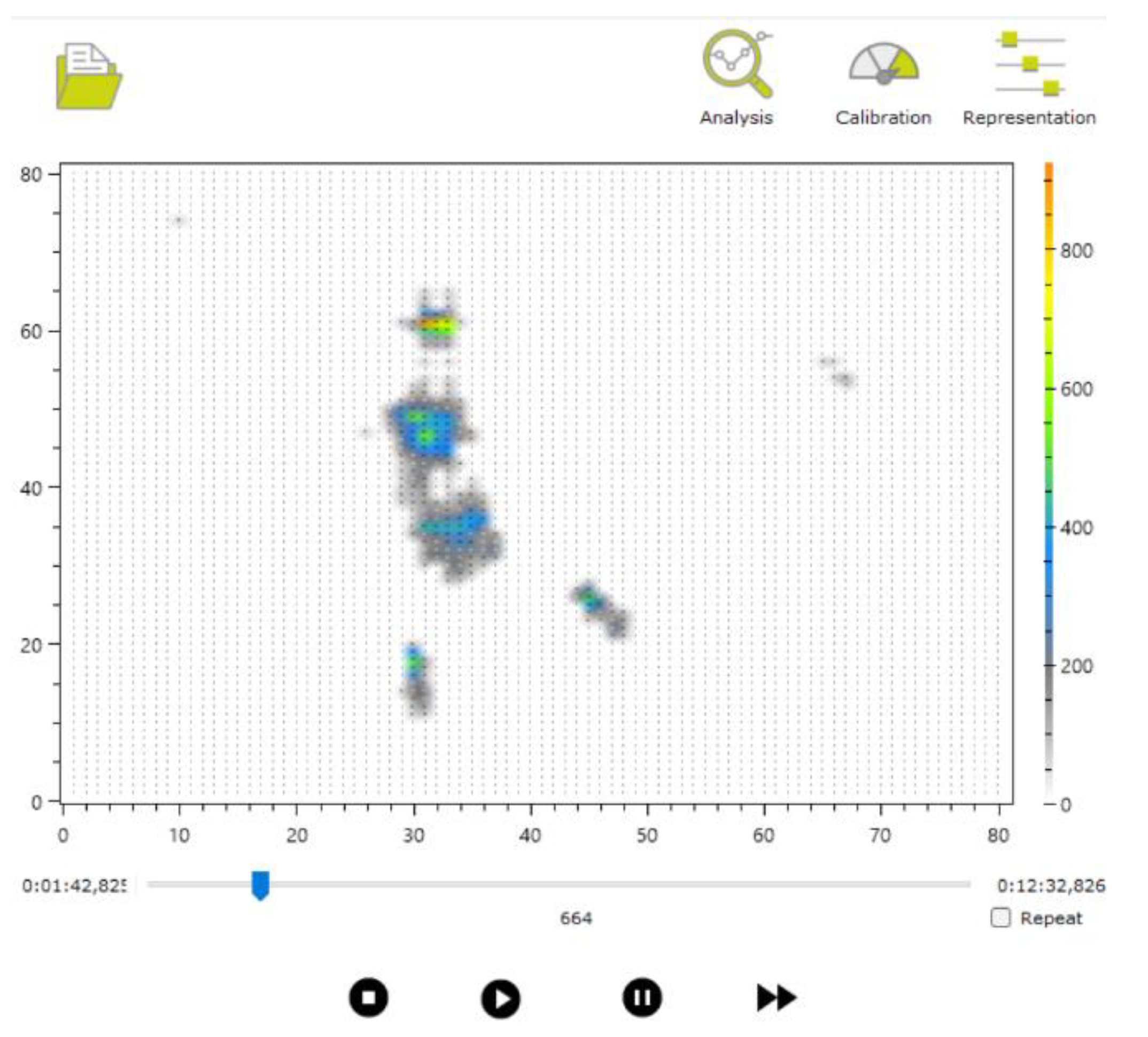
3.1.1. Pressure Imprint File
- dateTime: timestamp in ISO 8601 format [28]
- pressureMatrix: an 80 × 80 pressure matrix, where each element represents the integer value recorded by each sensor, though presented in the file as a decimal
| Text Box 1. Example of JSON File Exported by the Manufacturer's Application |
 |
3.1.2. Annotation File
|
Text Box 2. Example of an Annotation File Indicating Start and End Points for Supine and Prone Positions. |
 |
4. Data Analysis
5. Image Analysis
5.1. Image Preprocessing
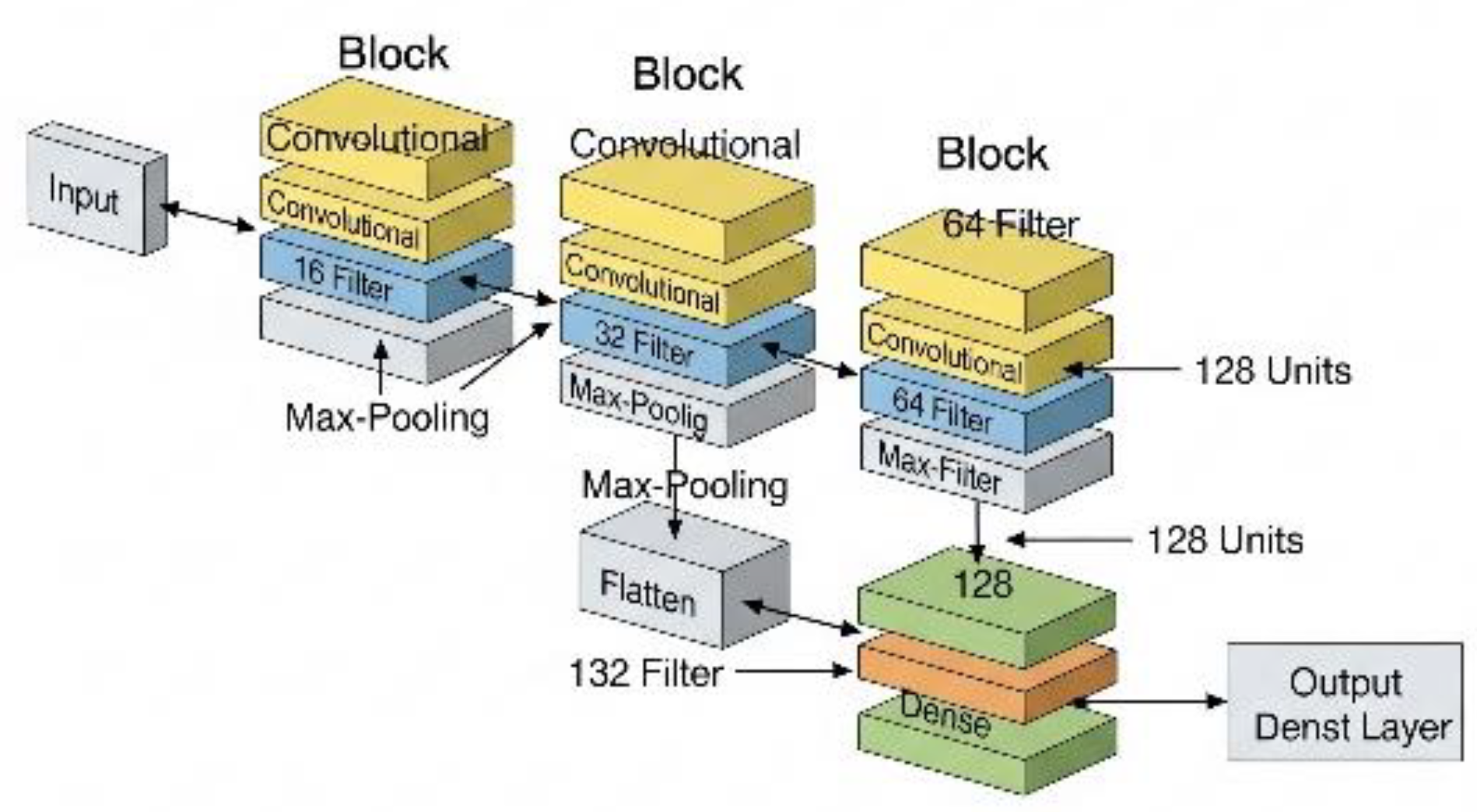
6. Neural Network Architecture
| Text Box 3. Example Code Defining the CNN Used |
 |
|
Text Box 4. Result of the CNN Generation Code Compilation. |
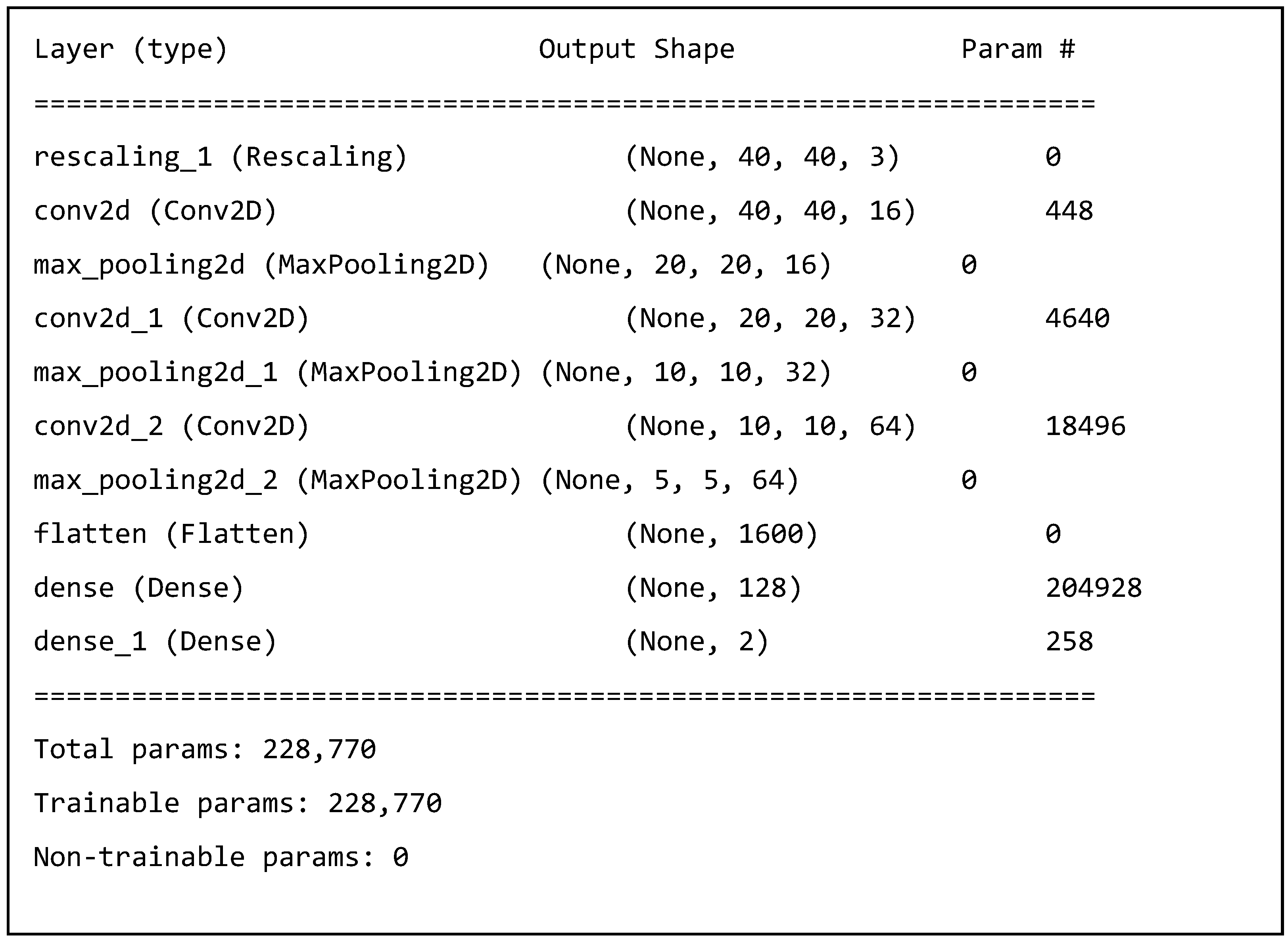 |
6.1. Model Training
|
Text Box 5. Definition of the Number of Epochs and CNN Training. |
 |
|
Text Box 6. Output of the CNN Training for Each Epoch. |
 |
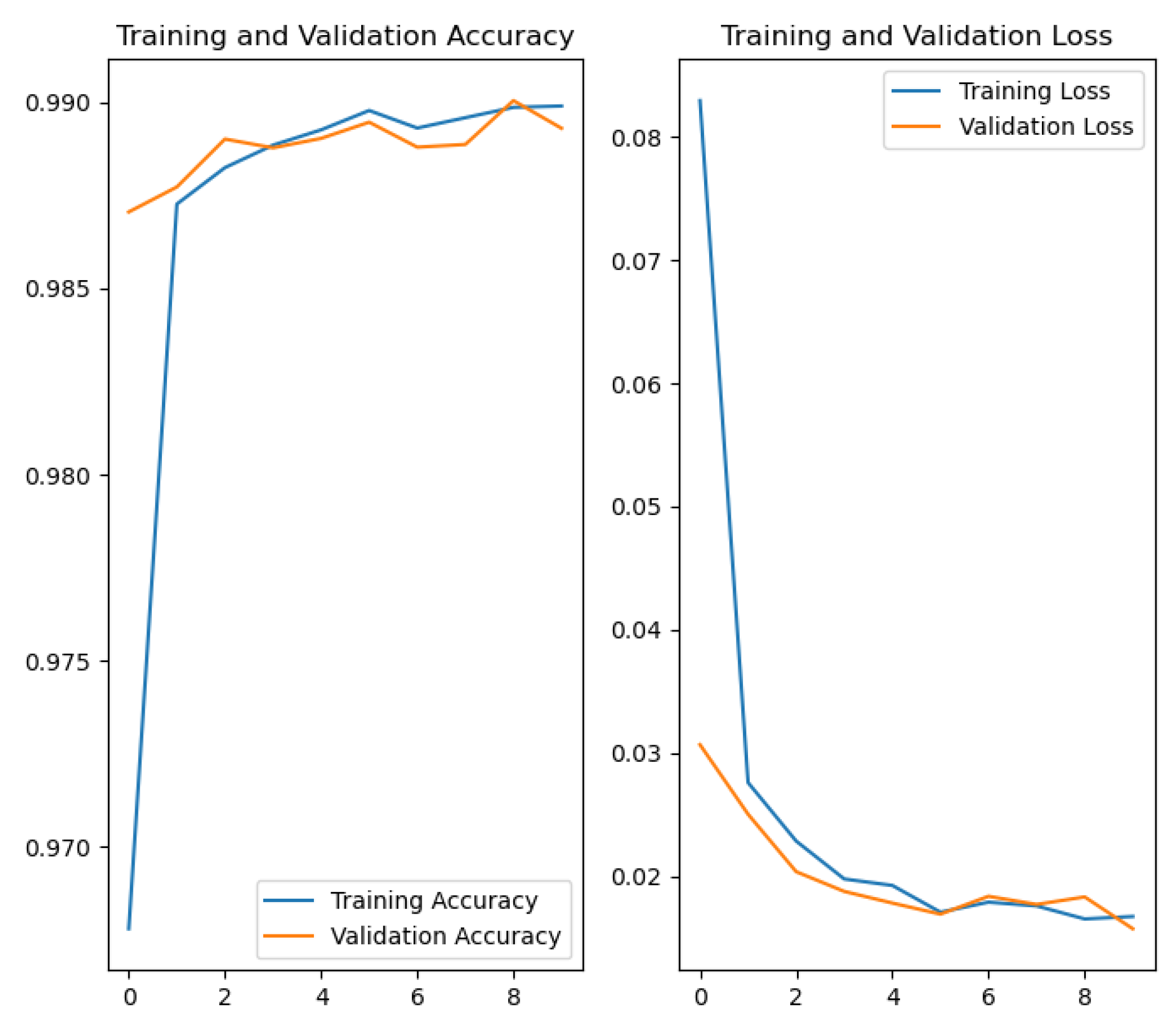
6.2. Training Results
- The graph on the left shows the evolution of accuracy. From the earliest epochs, the model achieves high accuracy, exceeding 97% in both training and validation. From there, both curves continue to rise and stabilize above 99%.
- The graph on the right displays the loss progression. Initially, the loss decreases rapidly, as is typical during the early learning phases. It then stabilizes, progressively falling below a value of 0.02.
7. Autonomous System
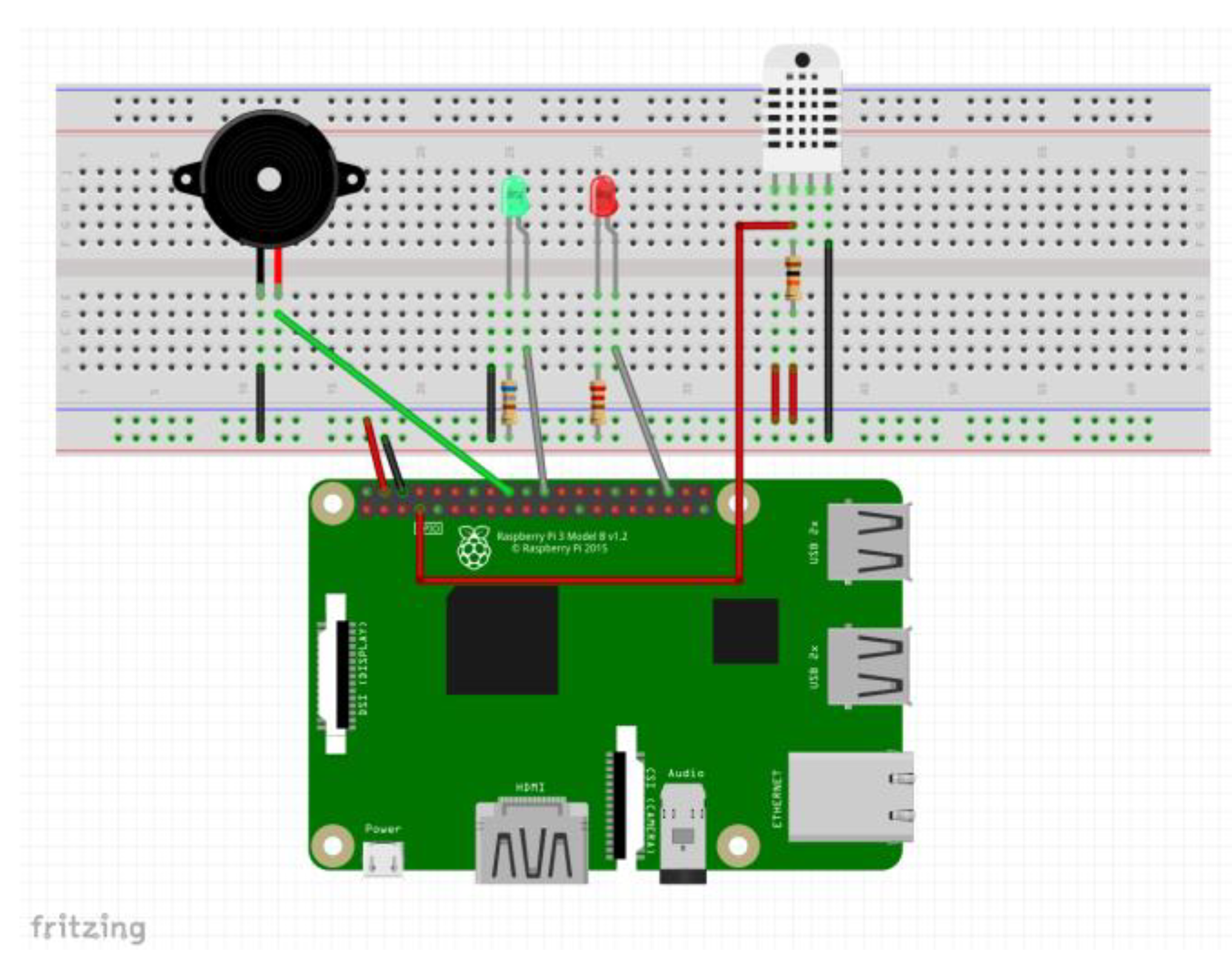
7.1. Hardware and System Environment
7.2. Data Acquisition from the Mattress
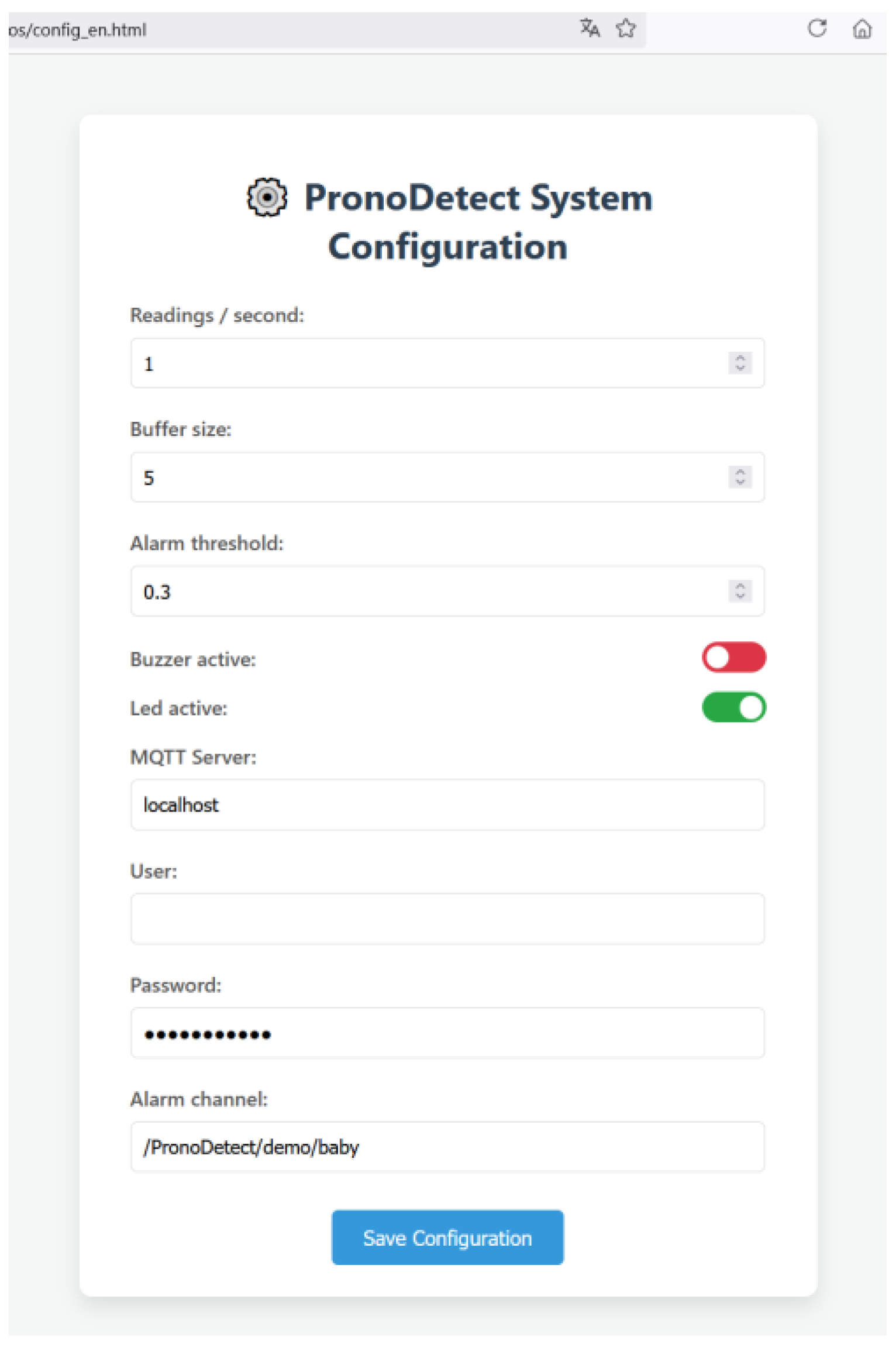
7.3. System Operation
7.4. Decision Logic and Buffer System
- A value of 1 is entered if the prone position is detected.
- A value of -1 is entered if supine is detected.
- A value of 0 is entered if no presence is detected on the mattress.
7.5. Alert System and Additional Sensors
- 1.
- Local notifications:
- A red LED is activated to indicate the alarm state.
- A buzzer is available, which is disabled by default but can be configured to emit an audible signal.
- 2.
- Remote notifications:
- A notification system using the MQTT protocol [40] is provided, allowing integration with monitoring platforms or mobile devices.
7.6. Remote Communication via MQTT
8. Discussion of Results and Conclusions
- The incorporation of new sensors to enrich the collected data, such as a depth camera.
- Integration with IoT platforms or connected healthcare systems.
- Expansion of the model to other tasks related to sleep analysis, such as phase detection or abnormal movement identification.
- Enhancement of the alarm system, adapting it to personalized scenarios based on each environment or user type.
Abbreviations
| SIDS | Sudden Infant Death Syndrome |
| CNN | Convolutional Neural Network |
| MQTT | Message Queuing Telemetry Transport |
| HAR | Human Activity Recognition |
| ADC | Analogue-to-Digital Converter |
| USB | Universal Serial Bus |
| SDK | Software Development Kit |
| JSON | JavaScript Object Notation |
| PNG | Portable Network Graphics |
| SMOTE | Synthetic Minority Over-sampling Technique |
| API | Application Programming Interface |
| AIMS | Accuracy of the Alberta Infant Motor Scale |
References
- Bajanowski, T.; Vege, Å.; Byard, R.W.; et al. Sudden infant death syndrome (SIDS)—standardised investigations and classification: Recommendations. Forensic Sci. Int. 2007, 165, 129–143. [Google Scholar] [CrossRef]
- Bouvier-Colle, M.H.; Inizan, J.; Michel, E. Postneonatal mortality, sudden infant death syndrome: Factors preventing the decline of infant mortality in France from 1979 to 1985. Paediatr. Perinat. Epidemiol. 1989, 3, 256–267. [Google Scholar] [CrossRef]
- Centers for Disease Control (CDC). Seasonality in sudden infant death syndrome—United States, 1980–1987. MMWR Morb. Mortal. Wkly. Rep. 1990, 39, 891–895. [Google Scholar]
- Almansoor, B.A.; Almaiman, W.A. Sudden infant death syndrome. Int. J. Adv. Med. 2023, 10, 340. [Google Scholar] [CrossRef]
- Rodrigues, L.; De Souza, A.V.; Del Risco Sánchez, O.; Carmona, E.V. Knowledge, attitudes and practice on sudden infant death: Study protocol of a scoping review. BMJ Open 2024, 14. [Google Scholar] [CrossRef]
- Douglas, A.S.; Gupta, R.; Helms, P.J.; Jolliffe, I.T. Month of birth as an independent variable in the sudden infant death syndrome. Paediatr. Perinat. Epidemiol. 1997, 11, 57–66. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, E.A.; Krous, H.F. Sudden unexpected death in infancy: A historical perspective. J. Paediatr. Child Health 2015, 51, 108–112. [Google Scholar] [CrossRef] [PubMed]
- Tappin, D.; Mitchell, E.A.; Carpenter, J.; Hauck, F.; Allan, L. Bed-sharing is a risk for sudden unexpected death in infancy. Arch. Dis. Child. 2023, 108, 79–80. [Google Scholar] [CrossRef]
- Kim, T.H.; Lee, H.; Woo, S.; et al. Prenatal and postnatal factors associated with sudden infant death syndrome: An umbrella review of meta-analyses. World J. Pediatr. 2024, 20, 451–460. [Google Scholar] [CrossRef]
- Mehboob, R.; Kurdi, M.; Ahmad, M.; et al. Comprehensive analysis of genes associated with sudden infant death syndrome. Front. Pediatr. 2021, 9, 742225. [Google Scholar] [CrossRef]
- Lakhoo DP, Blake HA, Chersich MF, Nakstad B, Kovats S. The Effect of High and Low Ambient Temperature on Infant Health: A Systematic Review. Int J Environ Res Public Health. 2022, 19, 9109. [CrossRef]
- Ruiz Botia, I.; Cassanello Peñarroya, P.; Díez Izquierdo, A.; Martínez Sánchez, J.M.; Balaguer Santamaria, A. Síndrome de muerte súbita del lactante: ¿siguen las familias las recomendaciones? An. Pediatr. (Engl. Ed.) 2020, 92, 222–228. [Google Scholar] [CrossRef]
- Jullien, S. Sudden infant death syndrome prevention. BMC Pediatr. 2021, 21 (Suppl 1), 320. [Google Scholar] [CrossRef] [PubMed]
- Bharati, V. An efficient edge deep learning computer vision system to prevent sudden infant death syndrome. In Proceedings of the 2021 IEEE International Conference on Smart Computing (SMARTCOMP), Irvine, CA, USA, 23–25 August 2021; pp. 286–291. [Google Scholar] [CrossRef]
- Al-Nashash, H.; Lvov, B. Sudden infant death syndrome detector. Technol. Health Care 1997, 5, 461–469. [Google Scholar] [CrossRef]
- Kinney, H.C.; Thach, B.T. The sudden infant death syndrome. N. Engl. J. Med. 2009, 361, 795–805. [Google Scholar] [CrossRef] [PubMed]
- Glinge, C.; Rossetti, S.; Oestergaard, L.B.; et al. Risk of sudden infant death syndrome among siblings of children who died of sudden infant death syndrome in Denmark. JAMA Netw. Open 2023, 6, e2252724. [Google Scholar] [CrossRef]
- Burke, M.J.; Downes, R. A fuzzy logic based apnoea monitor for SIDS risk infants. J. Med. Eng. Technol. 2006, 30, 397–411. [Google Scholar] [CrossRef]
- McInnes, E.; Jammali-Blasi, A.; Bell-Syer, S.E.; Dumville, J.C.; Middleton, V.; Cullum, N. Support surfaces for pressure ulcer prevention. Cochrane Database Syst. Rev. 2015, 2015, CD001735. [Google Scholar] [CrossRef]
- Meaume, S.; Marty, M. Pressure ulcer prevention using an alternating-pressure mattress overlay: the MATCARP project. J. Wound Care 2018, 27, 488–494. [Google Scholar] [CrossRef] [PubMed]
- Cohen-McFarlane, M.; Green, J.; Goubran, R.; Knoefel, F. Monitoring congestive heart failure using pressure-sensitive mats. In Proceedings of the 2016 IEEE International Symposium on Medical Measurements and Applications (MeMeA), Benevento, Italy, 15–18 May 2016; pp. 1–6. [Google Scholar] [CrossRef]
- Interlink Electronics, Inc. Available online: https://www.interlinkelectronics.com/force-sensing-resistor (accessed on 20 July 2025).
- Yuan, L.; Wei, Y.; Li, J. Smart pressure e-mat for human sleeping posture and dynamic activity recognition. IEEE J. Sel. Areas Sensors 2024, 1. [Google Scholar] [CrossRef]
- Sensing Tex, Inc. Available online: https://sensingtex.com/ (accessed on 20 July 2025).
- Sensing Tex. Presentation of Sensing Tex Products and Features. Available online: http://sensingtex.com/wp-content/uploads/2018/02/DATA-SHEET_Switch_Sensor_Tex_english_rev_11.pdf (accessed on 20 July 2025).
- Walker, D.M.; Tolentino, V.R. White coat versus no white coat: the pediatrician’s dilemma. Ambul. Pediatr. 2007, 7, 201–202. [Google Scholar] [CrossRef]
- JSON. Available online: https://www.json.org (accessed on 20 July 2025).
- ISO 8601. Available online: https://www.iso.org/iso-8601-date-and-time-format.html (accessed on 20 July 2025).
- de Albuquerque, P.L.; Lemos, A.; Guerra, M.Q.; Eickmann, S.H. Accuracy of the Alberta Infant Motor Scale (AIMS) to detect developmental delay of gross motor skills in preterm infants: A systematic review. Dev. Neurorehabil. 2015, 18, 15–21. [Google Scholar] [CrossRef] [PubMed]
- Fuentefria, R.D.N.; Silveira, R.C.; Procianoy, R.S. Motor development of preterm infants assessed by the Alberta Infant Motor Scale: Systematic review article. J. Pediatr. (Rio J.) 2017, 93, 328–342. [Google Scholar] [CrossRef]
- Ko, J.; Lim, H.K. Motor development comparison between preterm and full-term infants using Alberta Infant Motor Scale. Int. J. Environ. Res. Public Health 2023, 20, 3819. [Google Scholar] [CrossRef]
- Syrengelas, D.; Kalampoki, V.; Kleisiouni, P.; et al. Alberta Infant Motor Scale (AIMS) performance of Greek preterm infants: Comparisons with full-term infants of the same nationality and impact of prematurity-related morbidity factors. Phys. Ther. 2016, 96, 1102–1108. [Google Scholar] [CrossRef]
- Wu, Z. Application of CNN classic model in modern image processing. J. Adv. Eng. Technol. 2024, 1, 1–6. [Google Scholar] [CrossRef]
- Jiang, Z. Several applications of convolutional neural networks in medical imaging. Trans. Comput. Sci. Intell. Syst. Res. 2024, 7, 200–205. [Google Scholar] [CrossRef]
- Izadkhah, H. Medical image processing: An insight to convolutional neural networks. In Elsevier eBooks; 2022; pp. 175–213. [CrossRef]
- Song, X. Exploration and research of convolutional neural networks in image recognition. Appl. Comput. Eng. 2025, 121, 58–65. [Google Scholar] [CrossRef]
- Liu, T. Application of convolutional neural networks in image classification and applications of improved convolutional neural networks. Appl. Comput. Eng. 2024, 81, 56–62. [Google Scholar] [CrossRef]
- Fernández, A.; Garcia, S.; Herrera, F.; Chawla, N.V. SMOTE for learning from imbalanced data: Progress and challenges, marking the 15-year anniversary. J. Artif. Intell. Res. 2018, 61, 863–905. [Google Scholar] [CrossRef]
- Pradipta, G.A.; Wardoyo, R.; Musdholifah, A.; Sanjaya, I.N.H.; Ismail, M. SMOTE for handling imbalanced data problem: A review. In Proceedings of the 2021 Sixth International Conference on Informatics and Computing (ICIC), Semarang, Indonesia, 10–11 November 2021; pp. 1–8. [Google Scholar] [CrossRef]
- MQTT Protocol. Available online: https://mqtt.org/ (accessed on 20 July 2025).
- Waveshare. Temperature and Humidity Sensor DHT22. Available online: https://www.waveshare.com/wiki/DHT22_Temperature-Humidity_Sensor (accessed on 20 July 2025).
- Eclipse Mosquito. Available online; https://mosquitto.org/. (accessed on 20 July 2025).
- MyMQTT Android and IOS Application. Available online: https://mymqtt.app/en (accessed on 20 July 2025).
- IoT MQTT Panel IOS Application. Available online: https://apps.apple.com/pl/app/iot-mqtt-panel/id6466780124 (accessed on 20 July 2025).
- IoT MQTT Panel Android Application. Available online: https://play.google.com/store/apps/details?id=snr.lab.iotmqttpanel.prod (accessed on 20 July 2025).
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



