Submitted:
13 July 2025
Posted:
14 July 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
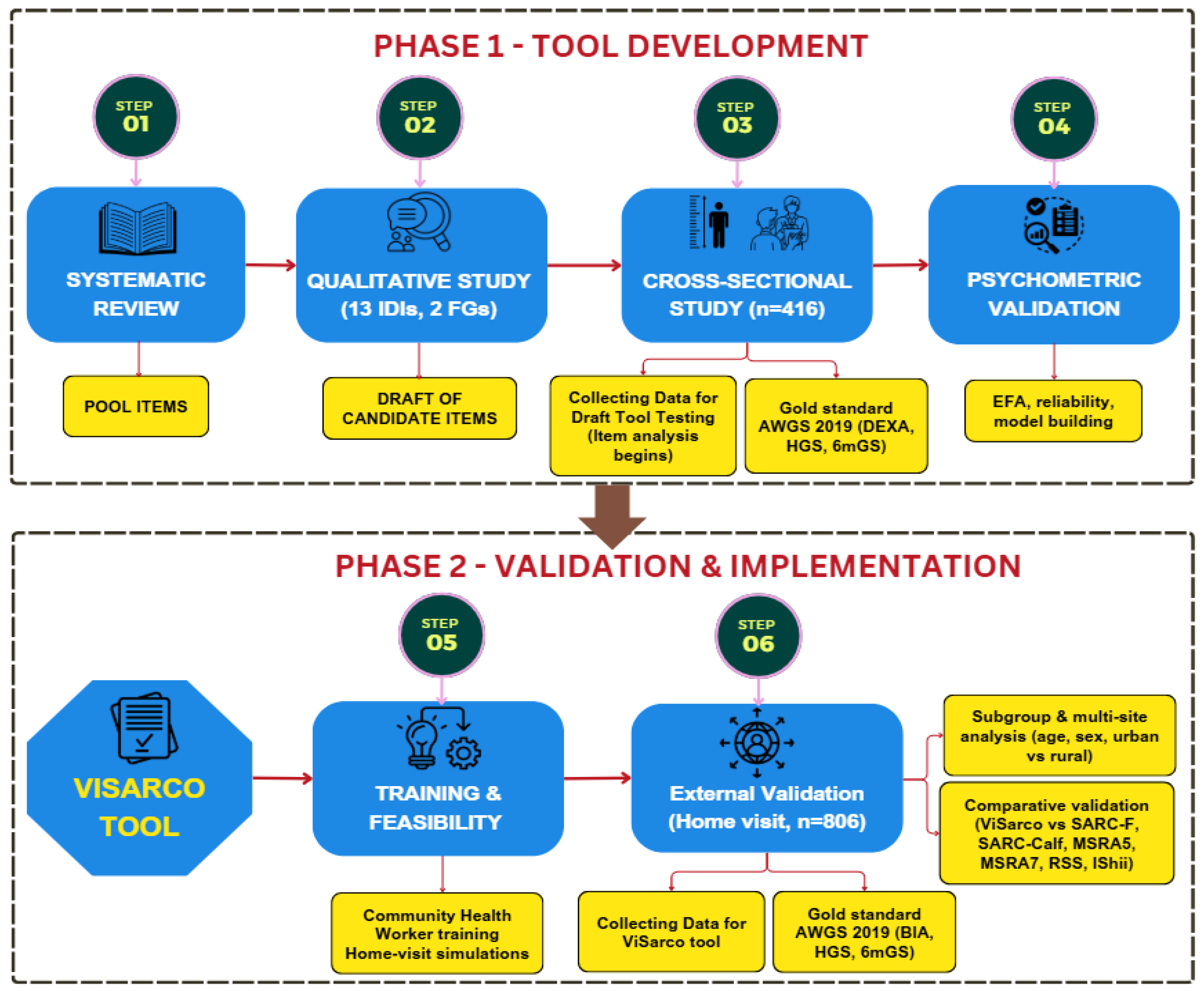
- Phase 1: Instrument Development
2.1. Targeted Literature Review
2.2. Qualitative Needs Assessment
2.3. Cross Sectional Survey
2.4. Psychometric Evaluation and Score Development
- Phase 2: Validation and Implementation
2.5. Training and Feasibility
2.6. External Validation and Comparative Assessment
3. Results
3.1. Item Pool Development Based on Literature Review and Healthcare Provider Insights
- 15 questionnaire items addressing subjective muscle strength, gait speed, muscle mass, physical performance, personal characteristics and lifestyle, and relevant medical history;
- 5 anthropometric measures (BMI, WC, CC, MUAC, and the finger-ring test);
- 6 physical performance tests, including SPPB, TUG, grip strength, chair stand, gait speed, and balance tests.
- 19 modified questionnaire items, revised to binary (Yes/No) formats and adapted based on contextual appropriateness. Items irrelevant to the Vietnamese rural context were excluded (e.g., “climbing stairs” from SARC-F due to one-story homes, “daily milk intake” from MSRA due to uncommon dairy consumption). New items on risk factors were added following provider suggestions.
- 5 anthropometric measures, all anthropometric measurements were chosen by PHC providers due to their simplicity, speed, and availability of measuring devices, with the finger-ring test presented in two response options for feasibility testing.
- 2 retained physical performance tests (chair stand test and balance test), while grip strength, gait speed, SPPB, and TUG were excluded due to their requirement for specialized tools, space, or prolonged testing time.
3.2. Cross-Sectional Assessment and Early Validation of ViSarco
3.2.1. Selection of Candidate Variables via Univariate Logistic Regression
3.2.2. Preliminary Factor Structure Exploration Using EFA
- KMO (Kaiser–Meyer–Olkin)
- Overall MSA = 0.73 (> 0.70) ⇒ the data were eligible for EFA.
- Each item had MSA > 0.60
- Bartlett’s test for sphericity
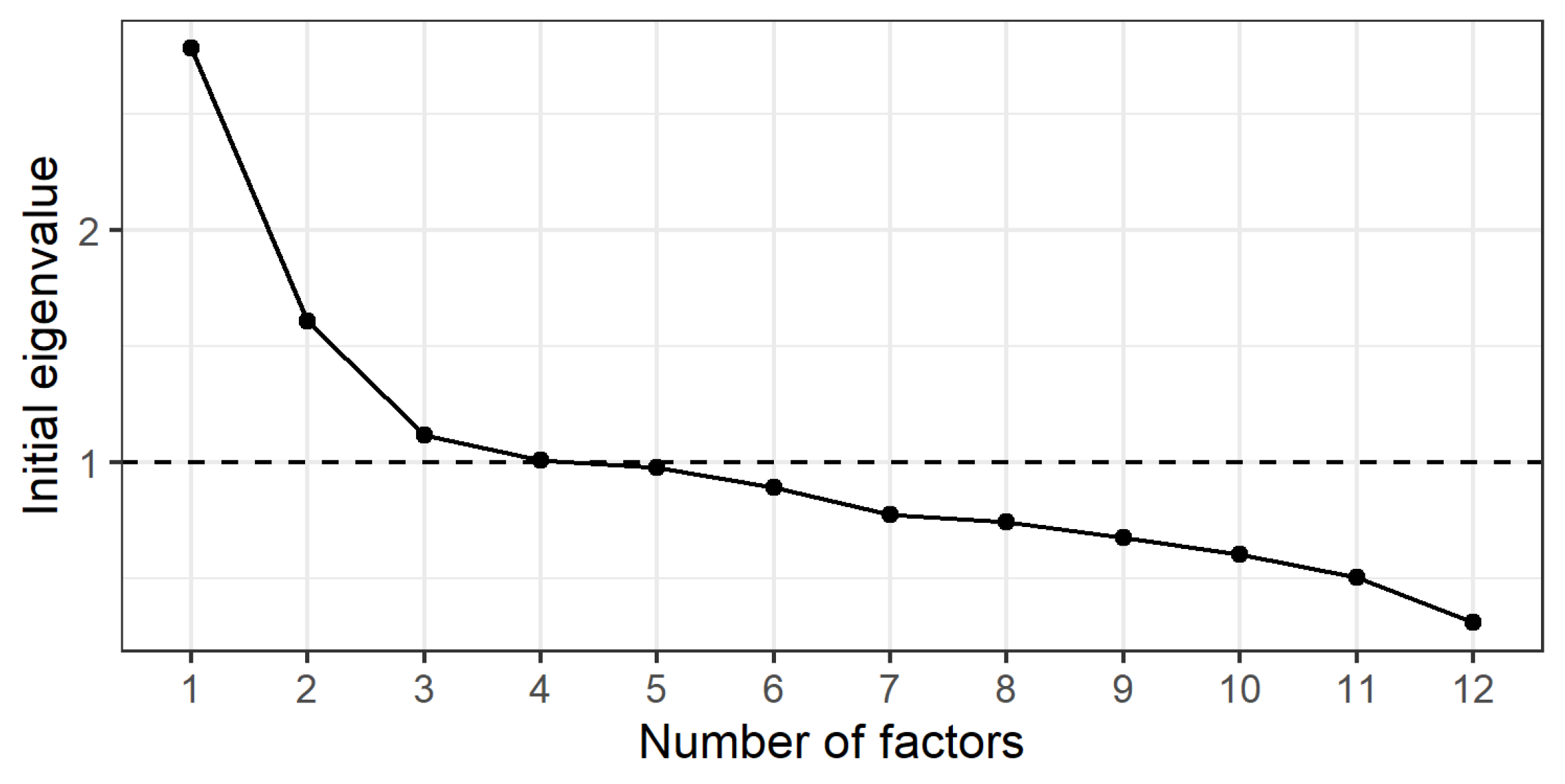
- Parallel analysis suggests that three factors should be extracted.
- Scree plot and eigenvalues analysis results support this choice.
- Since the sample size in our study is approximately 400, we choose a factor loading cutoff of 0.3.
- EFA and factor interpretation
- Apply factor analysis with minres method and varimax rotation on 3 factors.
- SS Loadings (Sum of squared loadings) show that all three factors have significant contributions to the diagnosis of muscular dystrophy, in which Factor 1 explains the largest change. Variance ratio shows the percentage of change in the data that each factor explains, Cumulative variance shows the total variance explained by the factors up to that factor, Chi-Square test with p-value less than 0.05, This shows that the model with 3 factors is suitable and sufficient to explain the data structure.
- Uniquenesses column shows that variables 5, 6, 9, 12 are highly independent, not clearly explained by the factors. Therefore, we will eliminate these 4 items from ViSarco's candidate items, leaving 8 items to be included in the next analysis steps.
| No | Items | Uniquenesses | Factor 1 | Factor 2 | Factor 3 |
|---|---|---|---|---|---|
| 1 | BMI_Vn threshold | 0,40 | 0.67 | 0.34 | |
| 2 | Waist_Vn threshold | 0,18 | 0.90 | ||
| 3 | CC_Vn threshold | 0,48 | 0.70 | ||
| 4 | Feeling muscle strength vs. peers (weaker) | 0,72 | 0.52 | ||
| 5 | 70 years and older | 0,91 | |||
| 6 | Hospitalizations last year | 0,92 | |||
| 7 | Weight loss last year | 0,77 | 0.46 | ||
| 8 | Gender male | 0,79 | 0.45 | ||
| 9 | >=3 chronic diseases | 0,94 | |||
| 10 | Ring finger | 0,73 | 0.43 | ||
| 11 | AC_Vn threshold | 0,66 | 0.47 | 0.31 | |
| 12 | Balance test_tandem stand | 0,92 | |||
| SS loading | 1.77 | 1.00 | 0.84 | ||
| Proportion Var | 0,15 | 0,08 | 0,07 | ||
| CumulativeVar | 0,15 | 0,23 | 0,30 | ||
| The chi square statistic is 48.56 on 33 degrees of freedom. The p-value is 0.0395 | |||||
3.2.3. Internal Consistency and Reliability of Extracted Factors
| Measure/Item | Cronbach's Alpha 95% CI | Alpha if Item Deleted | Average_r | r.cor | ICC |
|---|---|---|---|---|---|
| Overall Factor 1 (4 items) | 0.73 (0.68-0.77) | 0.4 | 0.71-0.73 | ||
| Gender male | 0.77 | 0.4 | |||
| BMI_Vn | 0.61 | 0.73 | |||
| Waist_Vn | 0.56 | 0.81 | |||
| AC_Vn | 0.70 | 0.55 | |||
| Overall Factor 2 (2 items) | 0.52 (0.43-0.61) | 0.35 | 0.51-0.52 | ||
| CC_Vn | 0.35 | 0.49 | |||
| Ring finger | 0.35 | 0.49 | |||
| Overall Factor 3 (2 items) | 0.36 (0.24-0.48) | 0.22 | 0.33-0.36 | ||
| Feeling muscle strength vs. peers | 0.26 | 0.37 | |||
| Weight loss last year | 0.19 | 0.37 |
3.3. Selection of the Optimal Model from Candidate Items
3.4. Weight Assignment and Optimal Cutpoint Identification for the ViSarco Tool
| Var X | OR | AUC | Sen | Spec | Youden’s | PLR | NLR |
|---|---|---|---|---|---|---|---|
| Total score | 2.65 | 0.832 | - | - | - | - | - |
| Cutpoint ≥ 1 | 10.00 | 0.696 | 0.916 | 0.478 | 0.394 | 1.754 | 0.175 |
| Cutpoint ≥ 2 | 11.10 | 0.769 | 0.772 | 0.766 | 0.538 | 3.302 | 0.297 |
| Cutpoint ≥ 3 | 15.05 | 0.766 | 0.637 | 0.896 | 0.533 | 6.099 | 0.405 |
| Cutpoint ≥ 4 | 14.56 | 0.691 | 0.433 | 0.950 | 0.383 | 8.694 | 0.597 |
3.5. Assessing External Validity of the ViSarco Tool by Subgroup and Site
| Sample | AUC (cutpoint ≥2) | Sen | Spec | PLR | NLR | Accuracy |
|---|---|---|---|---|---|---|
| Total (n = 806) | 0.77 (0.74-0.80) | 0.72 | 0.82 | 3.93 | 0.34 | 0.78 |
| Age (years old) | ||||||
| 60 – 69 (n=543) | 0.75 (0.71-0.79) | 0.67 | 0.83 | 3.94 | 0.39 | 0.78 |
| 70 – 79 (n=229) | 0.79 (0.74-0.84) | 0.79 | 0.79 | 3.81 | 0.27 | 0.79 |
| ≥ 80 (n=34) | 0.73 (0.58-0.89) | 0.75 | 0.71 | 2.63 | 0.35 | 0.74 |
| Gender | ||||||
| Male (n=261) | 0.79 (0.74-0.84) | 0.88 | 0.70 | 2.91 | 0.17 | 0.78 |
| Female (n=545) | 0.75 (0.71-0.79) | 0.63 | 0.87 | 4.72 | 0.43 | 0.78 |
| Area | ||||||
| Rural (n=355) | 0.75 (0.71-0.80) | 0.76 | 0.75 | 3.05 | 0.32 | 0.75 |
| Urban (n=451) | 0.77 (0.72-0.81) | 0.68 | 0.86 | 4.76 | 0.38 | 0.80 |
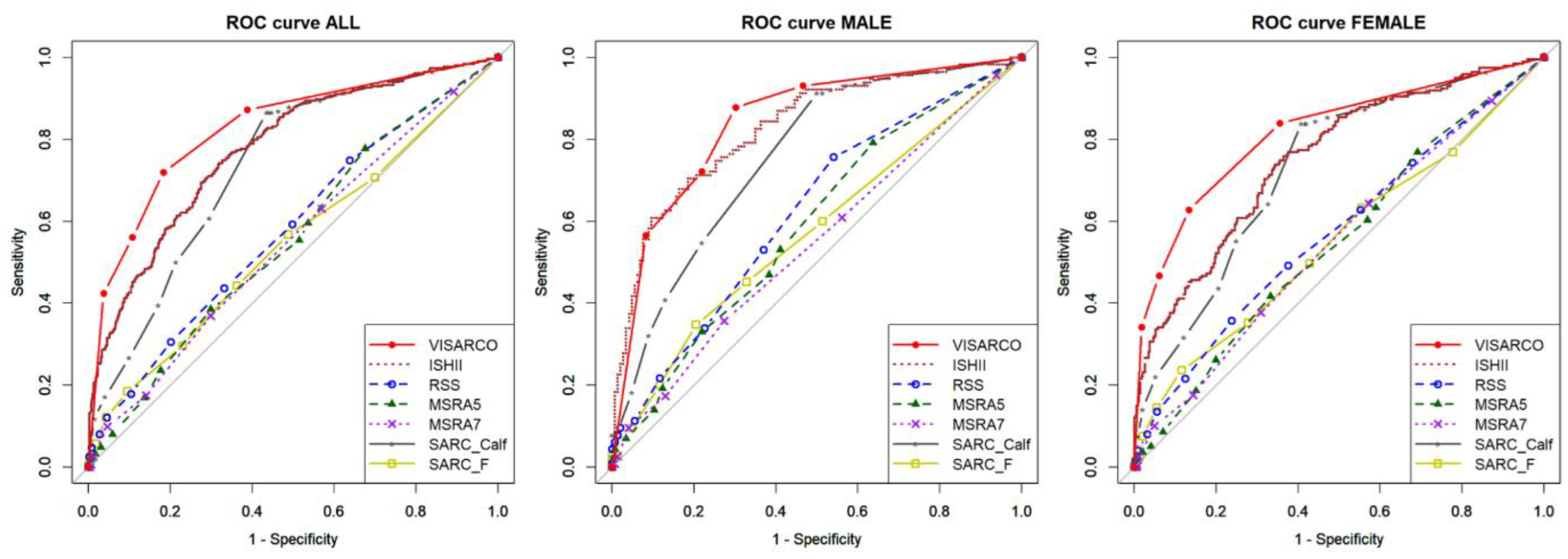
3.6. Comparison of ViSarco with Existing Sarcopenia Screening Tools
| Sample (n= 806) | AUC (total score) | AUC (cutpoint) | sen | spec | PLR | NLR | Accuracy | |
|---|---|---|---|---|---|---|---|---|
|
SARC-F (cutpoint ≥ 4) |
All | 0.55 (0.51-0.59) | 0.53 (0.50-0.56) | 0.29 | 0.77 | 1.29 | 0.91 | 0.59 |
| Male | 0.57 (0.51-0.64) | 0.54 (0.50-0.59) | 0.20 | 0.88 | 1.72 | 0.91 | 0.58 | |
| Female | 0.55 (0.50-0.60) | 0.54 (0.50-0.58) | 0.35 | 0.72 | 1.27 | 0.90 | 0.59 | |
|
SARC-Calf (cutpoint ≥ 11) |
All | 0.74 (0.70-0.77) | 0.64 (0.61-0.68) | 0.50 | 0.79 | 2.34 | 0.64 | 0.67 |
| Male | 0.76 (0.70-0.81) | 0.64 (0.59-0.69) | 0.41 | 0.87 | 3.14 | 0.68 | 0.67 | |
| Female | 0.73 (0.69-0.77) | 0.65 (0.61-0.69) | 0.55 | 0.75 | 2.22 | 0.60 | 0.68 | |
|
RSS (cutpoint ≤14) |
All | 0.58 (0.54-0.62) | 0.55 (0.52-0.58) | 0.31 | 0.80 | 1.52 | 0.87 | 0.61 |
| Male | 0.62 (0.55-0.69) | 0.55 (0.50-0.60) | 0.22 | 0.88 | 1.88 | 0.89 | 0.59 | |
| Female | 0.57 (0.52-0.62) | 0.56 (0.52-0.60) | 0.36 | 0.76 | 1.50 | 0.84 | 0.61 | |
|
MSRA5 (cutpoint < 45) |
All | 0.56 (0.52-0.60) | 0.54 (0.51-0.58) | 0.39 | 0.70 | 1.29 | 0.88 | 0.58 |
| Male | 0.59 (0.52-0.66) | 0.56 (0.50-0.61) | 0.33 | 0.78 | 1.51 | 0.86 | 0.58 | |
| Female | 0.55 (0.50-0.60) | 0.54 (0.50-0.58) | 0.42 | 0.67 | 1.25 | 0.87 | 0.58 | |
|
MSRA7 (cutpoint < 30) |
All | 0.55 (0.51-0.59) | 0.54 (0.50-0.57) | 0.37 | 0.70 | 1.24 | 0.90 | 0.57 |
| Male | 0.55 (0.48-0.61) | 0.54 (0.48-0.60) | 0.35 | 0.73 | 1.30 | 0.89 | 0.56 | |
| Female | 0.55 (0.50-0.60) | 0.53 (0.49-0.58) | 0.38 | 0.69 | 1.21 | 0.90 | 0.57 | |
|
Ishii (male ≤ 105, female ≤ 120) |
All | 0.78 (0.74-0.81) | 0.68 (0.65-0.71) | 0.86 | 0.49 | 1.69 | 0.28 | 0.64 |
| Male | 0.83 (0.78-0.88) | 0.67 (0.62-0.71) | 0.93 | 0.40 | 1.56 | 0.17 | 0.63 | |
| Female | 0.75 (0.71-0.80) | 0.67 (0.64-0.71) | 0.82 | 0.52 | 1.73 | 0.34 | 0.63 | |
|
ViSarco (cutpoint ≥ 2) |
All | 0.83 (0.80-0.86) | 0.77 (0.74-0.80) | 0.72 | 0.82 | 3.93 | 0.34 | 0.78 |
| Male | 0.84 (0.79-0.89) | 0.79 (0.74-0.84) | 0.88 | 0.70 | 2.91 | 0.17 | 0.78 | |
| Female | 0.82 (0.78-0.85) | 0.75 (0.71-0.79) | 0.63 | 0.87 | 4.72 | 0.43 | 0.78 | |
4. Discussion
4.1. Effectiveness and Feasibility of ViSarco in Primary Care Settings
4.2. Comparison with Previous Tools
4.3. Strengths and Limitations of the Study
- Strengths.
- Limitations
4.4. Clinical Practice and Future Research
5. Conclusion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| BMI | Body Mass Index |
| CC | Calf Circumference |
| AC | Arm Circumference |
| WC | Waist Circumference |
| WWI | The Weight-Adjusted Waist Index |
| AWGS 2019 | The Asian Working Group For Sarcopenia 2019 |
| ROC | Receiver Operating Characteristic |
| AUC | Area Under The Curve |
| BIA | Bioelectrical Impedance Analysis |
| DEXA | Dual-Energy X-ray Absorptiometry |
| HGS | Handgrip strength |
| 6mGS | 6-meter Gait Speed |
References
- Anker, S.D.; Morley, J.E.; von Haehling, S. Welcome to the ICD-10 code for sarcopenia. J Cachexia Sarcopenia Muscle 2016, 7, 512-514. [CrossRef]
- Gao, Q.; Hu, K.; Yan, C.; Zhao, B.; Mei, F.; Chen, F.; Zhao, L.; Shang, Y.; Ma, Y.; Ma, B. Associated Factors of Sarcopenia in Community-Dwelling Older Adults: A Systematic Review and Meta-Analysis. Nutrients 2021, 13, 4291.
- Beaudart, C.; Zaaria, M.; Pasleau, F.; Reginster, J.Y.; Bruyère, O. Health Outcomes of Sarcopenia: A Systematic Review and Meta-Analysis. PLoS One 2017, 12, e0169548. [CrossRef]
- Bruyère, O.; Beaudart, C.; Ethgen, O.; Reginster, J.-Y.; Locquet, M. The health economics burden of sarcopenia: a systematic review. Maturitas 2019, 119, 61-69. [CrossRef]
- Yuan, S.; Larsson, S. Epidemiology of sarcopenia: Prevalence, risk factors, and consequences. Metabolism: Clinical and Experimental 2023. [CrossRef]
- Liu, J.; Zhu, Y.; Tan, J.K.; Ismail, A.H.; Ibrahim, R.; Hassan, N.H. Factors Associated with Sarcopenia among Elderly Individuals Residing in Community and Nursing Home Settings: A Systematic Review with a Meta-Analysis. Nutrients 2023, 15. [CrossRef]
- Darvishi, A.; Hemami, M.R.; Shafiee, G.; Daroudi, R.; Mohseni, M.; Shekarabi, F.H.; Heshmat, R. Sarcopenia screening strategies in older people: a cost effectiveness analysis in Iran. BMC Public Health 2021, 21, 926. [CrossRef]
- Sousa, A.S.; Guerra, R.S.; Fonseca, I.; Pichel, F.; Ferreira, S.; Amaral, T.F. Financial impact of sarcopenia on hospitalization costs. Eur J Clin Nutr 2016, 70, 1046-1051. [CrossRef]
- Pinedo-Villanueva, R.; Westbury, L.D.; Syddall, H.E.; Sanchez-Santos, M.T.; Dennison, E.M.; Robinson, S.M.; Cooper, C. Health Care Costs Associated With Muscle Weakness: A UK Population-Based Estimate. Calcif Tissue Int 2019, 104, 137-144. [CrossRef]
- Darvishi, A.; Shafiee, G.; Balajam, N.Z.; Hemami, M.R.; Ostovar, N.; Heshmat, R. Cost-effectiveness analysis of sarcopenia management interventions in Iran. BMC Public Health 2023, 23, 819. [CrossRef]
- Beaudart, C.; Alcazar, J.; Aprahamian, I.; Batsis, J.A.; Yamada, Y.; Prado, C.M.; Reginster, J.Y.; Sanchez-Rodriguez, D.; Lim, W.S.; Sim, M.; et al. Health outcomes of sarcopenia: a consensus report by the outcome working group of the Global Leadership Initiative in Sarcopenia (GLIS). Aging Clin Exp Res 2025, 37, 100. [CrossRef]
- Maheshwari, A.; Maheshwari, G. Aging Population in Vietnam: Challenges, Implications, and Policy Recommendations. International Journal of Aging 2024, 2, e1. [CrossRef]
- Châu, N.T.Q.; Linh, N.T.; Chinh, P.T.T. Khẩu phần ăn và thực trạng suy mòn cơ của người cao tuổi tại một trung tâm chăm sóc người cao tuổi tại Hà Nội năm 2023. Tạp chí Dinh dưỡng và Thực phẩm 2023, 19, 92-101.
- Pham, L.-A.T.; Nguyen, B.T.; Huynh, D.T.; Nguyen, B.-M.L.T.; Tran, P.-A.N.; Van Vo, T.; Bui, H.-H.T.; Thai, T.T. Community-based prevalence and associated factors of sarcopenia in the Vietnamese elderly. Scientific Reports 2024, 14, 17. [CrossRef]
- Trần, G.H.; Ngô, L.P.; Đỗ, A.T.; Lê, T.K.O.; Lê, T.K.D.; Nguyễn, T.H. Tình hình sarcopenia và một số yếu tố liên quan ở người cao tuổi huyện Phong Điền thành phố Cần Thơ năm 2024. Tạp chí Y Dược học Cần Thơ 2025, 184-190. [CrossRef]
- Cruz-Jentoft, A.J.; Baeyens, J.P.; Bauer, J.M.; Boirie, Y.; Cederholm, T.; Landi, F.; Martin, F.C.; Michel, J.P.; Rolland, Y.; Schneider, S.M.; et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing 2010, 39, 412-423. [CrossRef]
- Fielding, R.A.; Vellas, B.; Evans, W.J.; Bhasin, S.; Morley, J.E.; Newman, A.B.; Abellan van Kan, G.; Andrieu, S.; Bauer, J.; Breuille, D.; et al. Sarcopenia: an undiagnosed condition in older adults. Current consensus definition: prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc 2011, 12, 249-256. [CrossRef]
- Chen, L.K.; Woo, J.; Assantachai, P.; Auyeung, T.W.; Chou, M.Y.; Iijima, K.; Jang, H.C.; Kang, L.; Kim, M.; Kim, S.; et al. Asian Working Group for Sarcopenia: 2019 Consensus Update on Sarcopenia Diagnosis and Treatment. J Am Med Dir Assoc 2020, 21, 300-307.e302. [CrossRef]
- Dung, V.; Thi Mai Lan, N.; Thu Trang, V.; Xuan Cu, T.; Minh Thien, L.; Sy Thu, N.; Dinh Man, P.; Minh Long, D.; Trong Ngo, P.; Minh Nguyet, L. Quality of life of older adults in nursing homes in Vietnam. Health Psychol Open 2020, 7, 2055102920954710. [CrossRef]
- Giang, L. The Aging population in Viet Nam: Current status, prognosis, and possible policy responses; 2011.
- Adulkasem, N.; Ekasame, V.; Pojchong, C.; Apichat, A.; and Unnanuntana, A. Evaluation of the Diagnosis Accuracy of the AWGS 2019 Criteria for “Possible Sarcopenia” in Thai Community-Dwelling Older Adults. Clinical Interventions in Aging 2025, 20, 425-433. [CrossRef]
- Health, T.M.o. Decision 1588/QD-BYT 2020 professional document Guidelines for health management of the elderly. 2020.
- Health, T.M.o. Decision 5904/QD-BYT 2019 document on Guidelines for diagnosing non-communicable diseases at commune health stations. 2019.
- Nguyen, H.T.; Suwanbamrung, C.; Wattanapisit, A.; Satheannoppakao, W.; Nguyen, T.; Truong, N.T.; Ha, G.H.; Huynh, D.T.N.; Le, C.N. Cultural Contexts Meet Clinical Precision: A Systematic Review and Meta-Analysis of Sarcopenia Screening Tools in Global Aging Communities. Journal of Posthumanism 2025, 5, 1735-1769. [CrossRef]
- Pallant, J. SPSS Survival Manual: A Step by Step Guide to Data Analysis Using SPSS, 4th Edition ed.; Allen & Unwin, Berkshire, 2011.
- Piedmont, R.; Hyland, M. Inter-Item Correlation Frequency Distribution Analysis: A Method for Evaluating Scale Dimensionality. Educational and Psychological Measurement - EDUC PSYCHOL MEAS 1993, 53, 369-378. [CrossRef]
- Seidell, J.C.; Kahn, H.S.; Williamson, D.F.; Lissner, L.; Valdez, R. Report from a Centers for Disease Control and Prevention Workshop on Use of Adult Anthropometry for Public Health and Primary Health Care. The American Journal of Clinical Nutrition 2001, 73, 123-126. [CrossRef]
- Ha, T.; McNamara, M.; Melo, L.; Frost, E.; Moore, G. Filling the gap between evidence, policy and practice: are 45 and Up Study researchers planning for impact? Public Health Research & Practice 2023, 33, e45.
- Trevethan, R. Response: Commentary: Sensitivity, Specificity, and Predictive Values: Foundations, Pliabilities, and Pitfalls in Research and Practice. Frontiers in Public Health 2020, Volume 7 - 2019. [CrossRef]
- Ben-Haim, Y.; Dacso, C.C. Interpreting PPV and NPV of Diagnostic Tests with Uncertain Prevalence. Rambam Maimonides Med J 2024, 15. [CrossRef]
- Dekker - van Doorn, C.; Wauben, L.; van Wijngaarden, J.; Lange, J.; Huijsman, R. Adaptive design: adaptation and adoption of patient safety practices in daily routines, a multi-site study. BMC Health Services Research 2020, 20, 426. [CrossRef]
- Carlfjord, S.; Lindberg, M.; Bendtsen, P.; Nilsen, P.; Andersson, A. Key factors influencing adoption of an innovation in primary health care: a qualitative study based on implementation theory. BMC Family Practice 2010, 11, 60. [CrossRef]
- Luo, S.; Chen, X.; Hou, L.; Yue, J.; Liu, X.; Xia, X.; Dong, B.; Cao, L. The accuracy of body mass index and calf circumference values when assessing sarcopenia in a multi-ethnic cohort of middle-aged and older adults: West China health and aging trend study results. Heliyon 2023, 9, e15027. [CrossRef]
- Wang, B.; Nong, C.; Zhang, J.; Deng, L.; Li, W.; Zhang, X.; Liu, P. Prevalence and associated body composition factors of sarcopenia in community-dwelling older adults. European Journal of Medical Research 2024, 29, 598. [CrossRef]
- Sun, G.; French, C.R.; Martin, G.R.; Younghusband, B.; Green, R.C.; Xie, Y.-g.; Mathews, M.; Barron, J.R.; Fitzpatrick, D.G.; Gulliver, W.; et al. Comparison of multifrequency bioelectrical impedance analysis with dual-energy X-ray absorptiometry for assessment of percentage body fat in a large, healthy population1–3. The American Journal of Clinical Nutrition 2005, 81, 74-78. [CrossRef]
- Van Ancum, J.M.; Meskers, C.G.M.; Reijnierse, E.M.; Yeung, S.S.Y.; Jonkman, N.H.; Trappenburg, M.C.; Pijnappels, M.; Maier, A.B. Lack of Knowledge Contrasts the Willingness to Counteract Sarcopenia Among Community-Dwelling Adults. Journal of Aging and Health 2019, 32, 787-794. [CrossRef]
- Xie, W.Q.; Xiao, G.L.; Hu, P.W.; He, Y.Q.; Lv, S.; Xiao, W.F. Possible sarcopenia: early screening and intervention-narrative review. Ann Palliat Med 2020, 9, 4283-4293. [CrossRef]
- Won, C.W. Management of Sarcopenia in Primary Care Settings. Korean J Fam Med 2023, 44, 71-75. [CrossRef]
- Crosignani, S.; Sedini, C.; Calvani, R.; Marzetti, E.; Cesari, M. Sarcopenia in primary care: screening, diagnosis, management. J Frailty Aging 2021, 10, 226-232. [CrossRef]
| No. | Candidate Items | OR | p_OR | AUC (95% CI) | p_AUC |
|---|---|---|---|---|---|
| I.1 | Trouble moving in room | 0.89 | 0.56 | 0.51(0.47-0.56) | 0.28 |
| I.2 | Walks faster than peers | 1.13 | 0.52 | 0.52(0.46-0.56) | 0.26 |
| I.3 | Struggles to lift 5 kg | 1.43 | 0.08 | 0.54(0.49-0.59) | 0.04 |
| I.4 | Struggles to stand up | 1.11 | 0.58 | 0.51(0.47-0.56) | 0.29 |
| I.5 | Falls in the past year | 1.15 | 0.60 | 0.51(0.47-0.54) | 0.30 |
| I.6 | Wring out towels or clothes | 1.33 | 0.23 | 0.52(0.48-0.56) | 0.12 |
| I.7 | Feeling muscle strength vs. peers (weaker) | 1.93 | 0.003 | 0.57(0.53-0.61) | 0.001 |
| I.8 | 70 years and older | 2.16 | <0.001 | 0.59(0.54-0.63) | <0.001 |
| I.9 | Walking ability | 1.15 | 0.48 | 0.52(0.47-0.57) | 0.24 |
| I.10 | Protein intake frequency | 1.07 | 0.81 | 0.5(0.47-0.54) | 0.41 |
| I.11 | Enough 3 meals | 0.87 | 0.54 | 0.51(0.47-0.55) | 0.27 |
| I.12 | Hospitalizations last year | 1.88 | 0.008 | 0.55(0.51-0.59) | 0.004 |
| I.13 | Weight loss last year | 1.89 | 0.01 | 0.55(0.51-0.59) | 0.06 |
| 1.14 | Gender male | 2.17 | <0.001 | 0.58(0.54-0.63) | <0.001 |
| 1.15 | >=3 chronic diseases | 1.99 | 0.01 | 0.55(0.51-0.58) | <0.001 |
| I.16 | Smoking | 1.31 | 0.34 | 0.52(0.48-0.55) | 0.17 |
| I.17 | Drinks alcohol | 0.78 | 0.57 | 0.50(0.48-0.52) | 0.44 |
| I.18 | Daily sleep hours. | 1.21 | 0.38 | 0.52(0.48-0.56) | 0.19 |
| I.19 | Follow a diet | 1.29 | 0.33 | 0.52(0.48-0.55) | 0.16 |
| I.20 | Ring finger | 3.29 | <0.001 | 0.64(0.60-0.69) | <0.001 |
| I.21 | BMI_Vn threshold | 13.1 | <0.001 | 0.77(0.73-0.81) | <0.001 |
| I.22 | Waist_Vn threshold | 5.23 | <0.001 | 0.69(0.65-0.74) | <0.001 |
| I.23 | AC_Vn threshold | 5.41 | <0.001 | 0.70(0.65-0.74) | <0.001 |
| I.24 | CC_Vn threshold | 4.60 | <0.001 | 0.68(0.64-0.73) | <0.001 |
| I.25 | 5-CST | 1.35 | 0.13 | 0.54(0.49-0.58) | 0.07 |
| I.26 | Balance test_feet together stand | 5511049 | 0.98 | 0.51(0.50-0.52) | 0.02 |
| I.27 | Balance test_semi-tandem stand | 2.34 | 0.05 | 0.52(0.50-0.55) | 0.02 |
| I.28 | Balance test_tandem stand | 1.65 | 0.03 | 0.54(0.50-0.59) | 0.02 |
| Items | PIP (%) | Post-mean β (SD) | Model 1 | Model 2 | Model 3 | Model 4 | Model 5 |
|---|---|---|---|---|---|---|---|
| BMI_Vn | 100 | 0.44(0.05) | 0.43 | 0.49 | 0.42 | 0.42 | 0.41 |
| Waist_Vn | 4 | 0.001(0.01) | . | . | . | . | 0.03 |
| AC_Vn | 85.6 | 0.12(0.06) | 0.14 | . | 0.14 | 0.14 | 0.13 |
| Ring finger | 6.9 | 0.004(0.02) | . | . | . | 0.05 | . |
| CC_Vn | 100 | 0.19(0.04) | 0.18 | 0.21 | 0.18 | 0.17 | 0.19 |
| Feeling muscle strength vs. peers | 8.3 | 0.004(0.02) | . | . | 0.06 | . | . |
| Weight loss last year | 0.0 | 0.00(0.00) | . | . | . | . | . |
| nVar | 3 | 2 | 4 | 4 | 4 | ||
| r2 | 0.36 | 0.34 | 0.36 | 0.36 | 0.36 | ||
| BIC | -164.83 | -161.76 | -160.66 | -160.31 | -159.19 | ||
| Post prob | 0.67 | 0.14 | 0.08 | 0.07 | 0.04 |
| Step | Variable | R² | Adj. R² | Beta | Std. Beta | SE | t | p |
|---|---|---|---|---|---|---|---|---|
| 0 | Base Mode | 0.000 | 0.000 | 0.17 | - | 0.03 | 5.23 | <0.001 |
| 1 | BMI_Vn (+) | 0.302 | 0.301 | 0.43 | 0.43 | 0.05 | 9.27 | <0.001 |
| 2 | CC_Vn (+) | 0.342 | 0.338 | 0.18 | 0.18 | 0.04 | 4.32 | <0.001 |
| 3 | AC_Vn (+) | 0.356 | 0.351 | 0.13 | 0.13 | 0.05 | 3.02 | 0.003 |
| Items | OR | 95% CI | Regression coefficient | Assigned score* | Score |
|---|---|---|---|---|---|
| BMI_Vn threshold | 8.18 | (4.87-14.04) | 2.10 | 2.84 | 2 |
| AC_Vn threshold | 2.10 | (1.26-3.47) | 0.74 | 1.00 | 1 |
| CC_Vn threshold | 2.81 | (1.73-4.58) | 1.03 | 1.39 | 1 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




