Submitted:
04 July 2025
Posted:
07 July 2025
You are already at the latest version
Abstract
Keywords:
0. Scope of the study
1. Introduction
- Attempt to obtain the minimum case possible for all variables by assuming that all schemes to reduce demand will simultaneously achieve 100% success. See point #8.
- Use simplistic age-based forecasts for admissions based on a single year. Use more than 8 years of data (preferably 15 years), to follow the trend in each year of age. Then take the trend into the future with multiple probable scenarios along with the observed (past) uncertainty associated with demand.
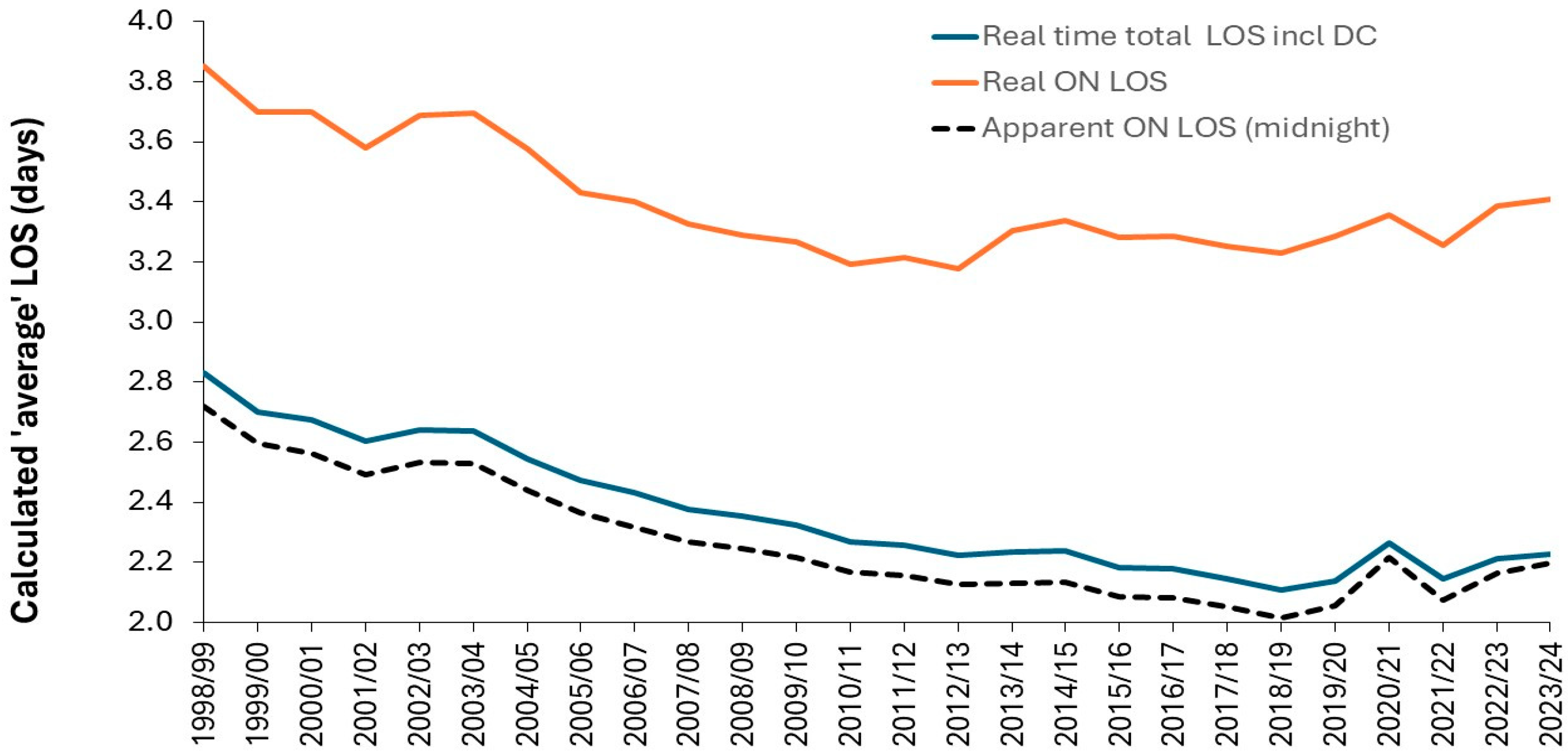
- Calculate average length of stay (LOS) based on midnight stays, always use real time data. Midnight LOS will consistently underestimate the real LOS [3].
- Assume that LOS is a constant, rather than a variable with confidence intervals, and assume that LOS decreases ad-infinitum. Most trends in LOS decrease toward an asymptote.
- Focus exclusively on those HRG/DRGs which show above average LOS. These will generally be matched by other HRG/DRGs with lower-than-average LOS. These arise due to the ambiguities in the local clinical coding process compared to that applying to the national average. This includes how doctors record diagnoses and the depth of local coding with complications and existing conditions affecting health. Local LOS is subject to sampling error as it is a small subset of national data [27].
- Use annual averages for admissions and LOS. Many conditions show seasonality due to multiple causes and LOS can also show seasonal variation.
- Assume that lower LOS means better care or that lower LOS makes large savings in costs. For pediatrics it is the volatility in admissions which dominates bed demand not the calculated LOS – this directly contradicts the accepted dogma that reduction in LOS is one of the key ingredients to reducing bed demand. Reducing LOS only benefits a steady state system or the baseline bed demand which lies beneath the volatile changes, see I.6,9 in S1.
- Make simplistic models comprising all the variables and proposed schemes to reduce admissions and LOS. An alternative is to use Monte Carlo simulation (including seasonality) which will show the full range of probable outcomes. This is a subset of operational research [19,20,21]. The alternative is to use past data to illustrate the sources of variability – upon which Monte Carlo simulation will be based but without the full nuances of the real world. Hence simultaneous variation in admissions and LOS imply that the actual trend in occupied bed days is a preferred approach.
2. Materials and Methods
2.1. Sources of Data
2.2. Additional Data from English Hospitals
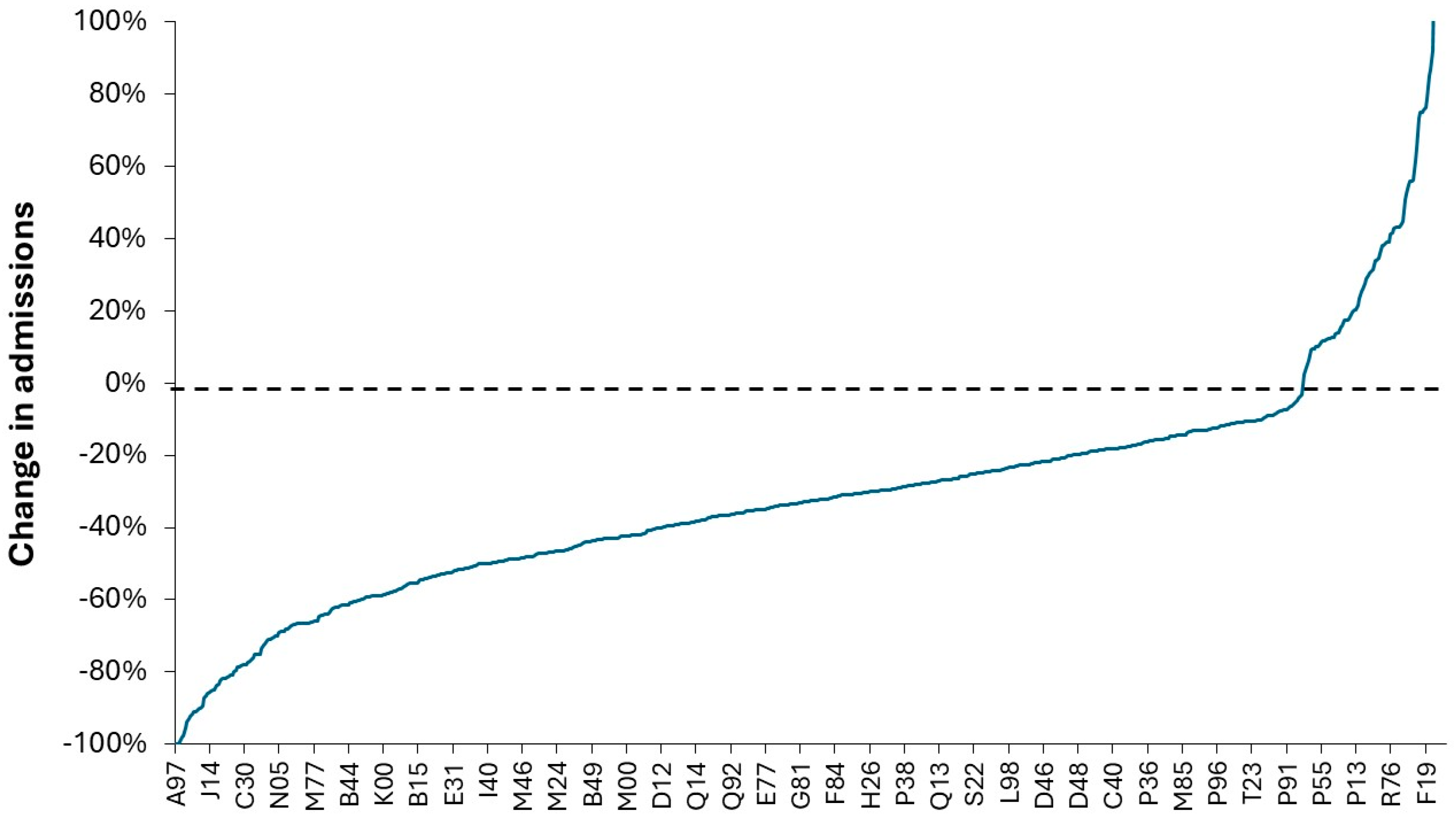
2.3. Analysis of Admissions During the First Year of COVID-19
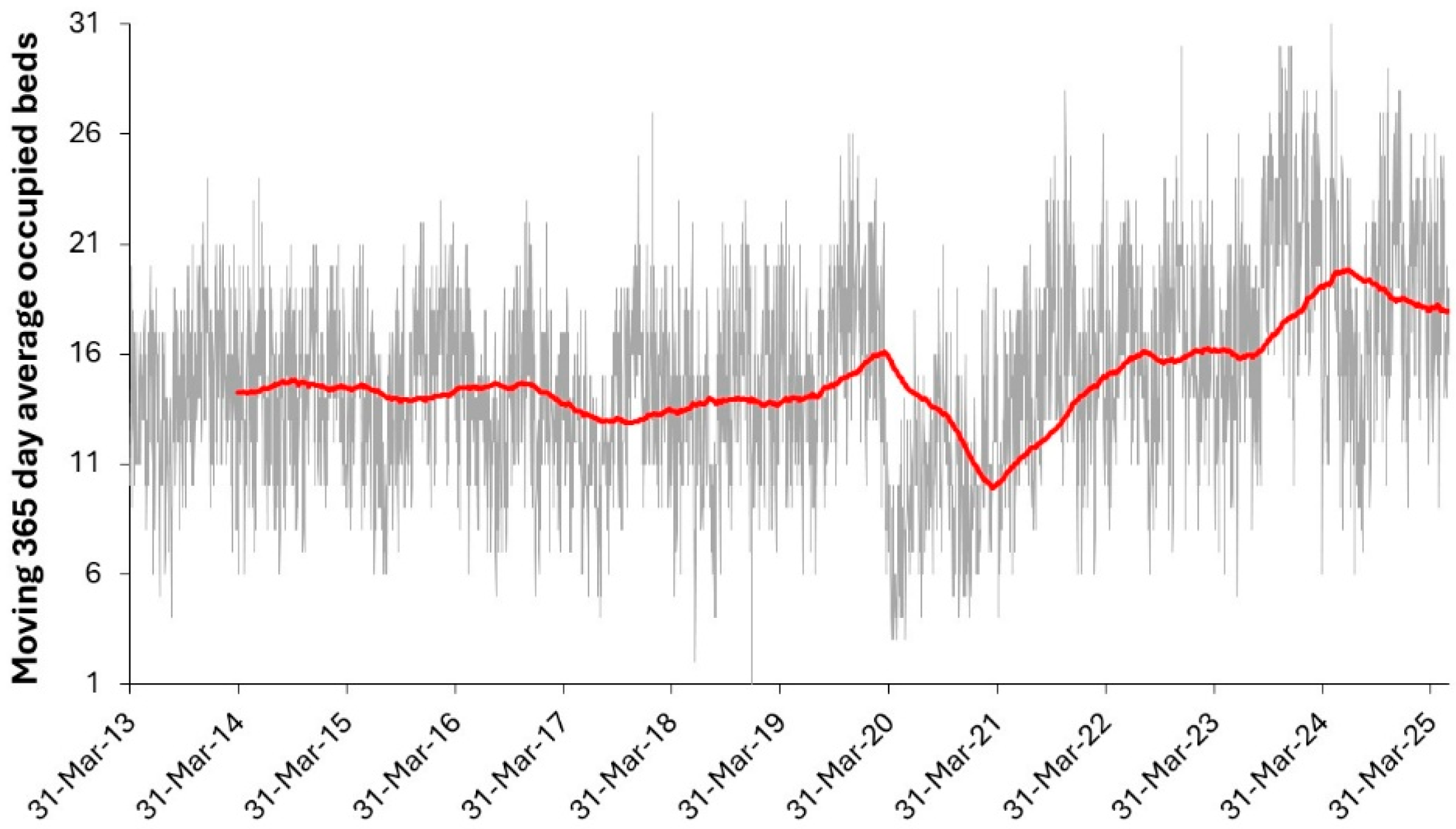
2.4. Analysis of Daily Occupied beds to Simuate a Worst Year
2.5. Analysis of Periods of Maximum Pediatric Deaths
2.6. Estimating Total Occupied Beds for Children in England
3. Results
3.1. Defining Pediatric Admissions, Beds and Bed Pool Size
3.1.2. Defining a bed pool
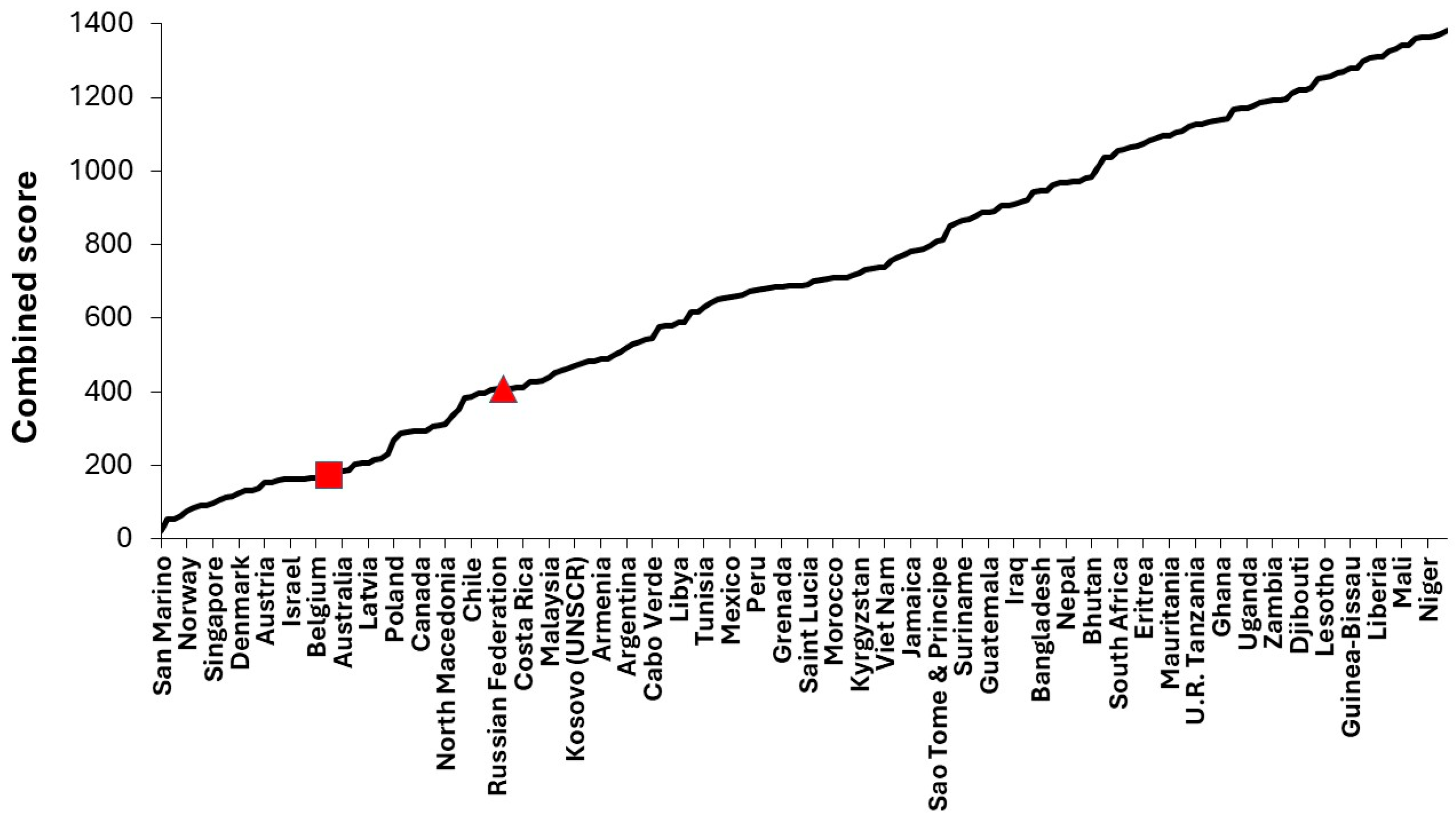
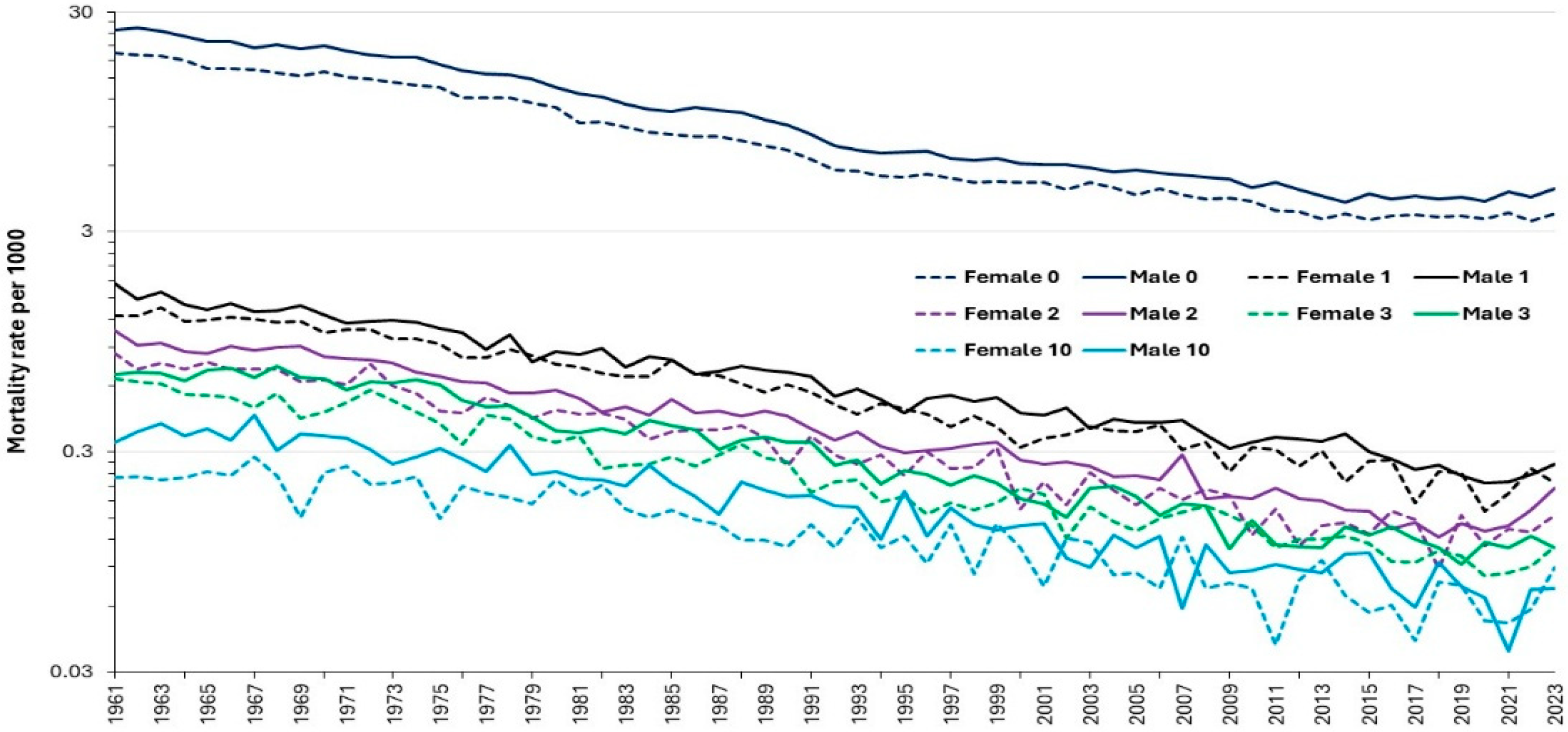
3.2. Ranking Countries by Childhood Mortality
3.3. Is Our Current Bed Supply Sufficient?
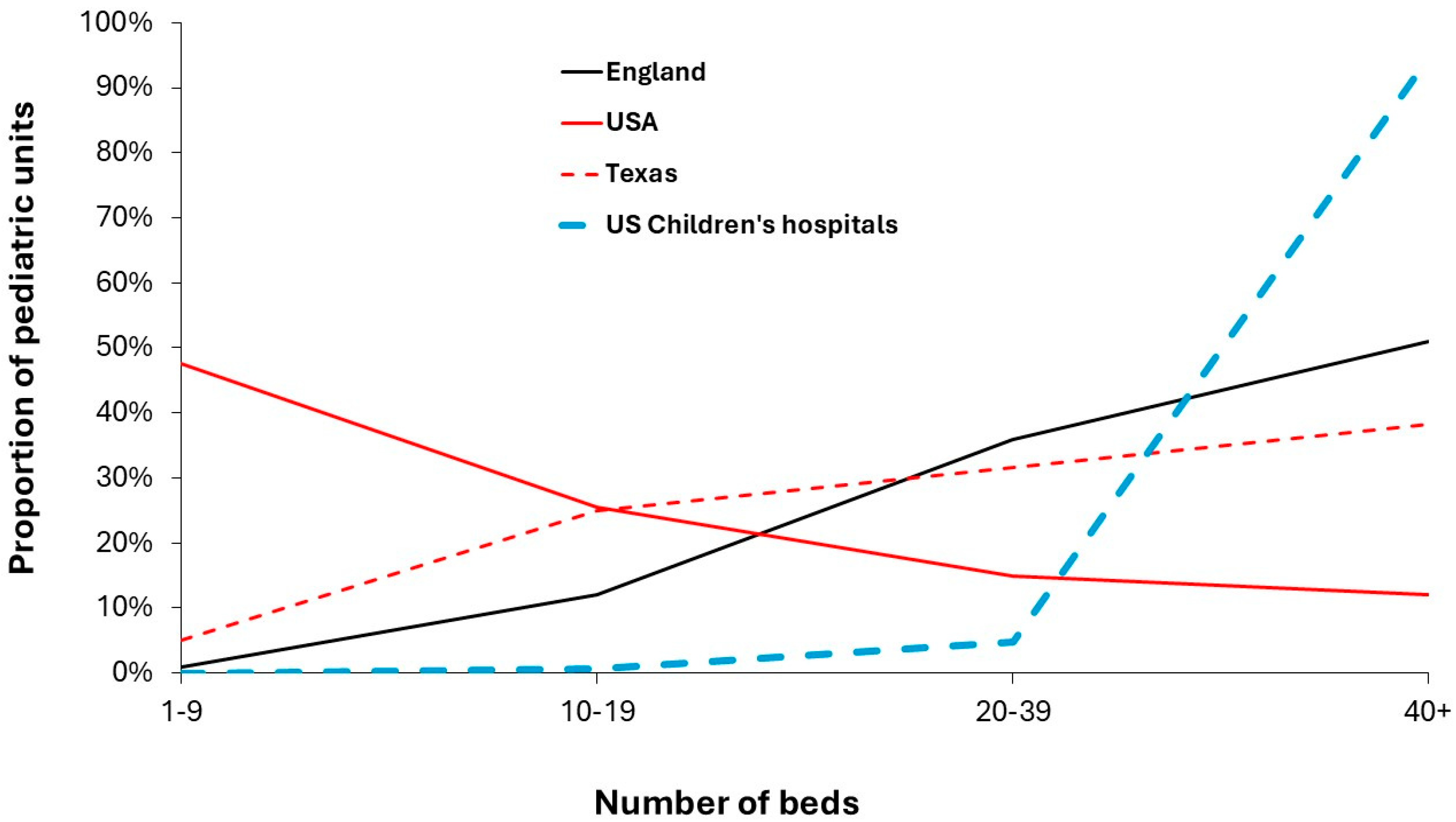
3.4. The Size of Pediatric Units in the USA and England
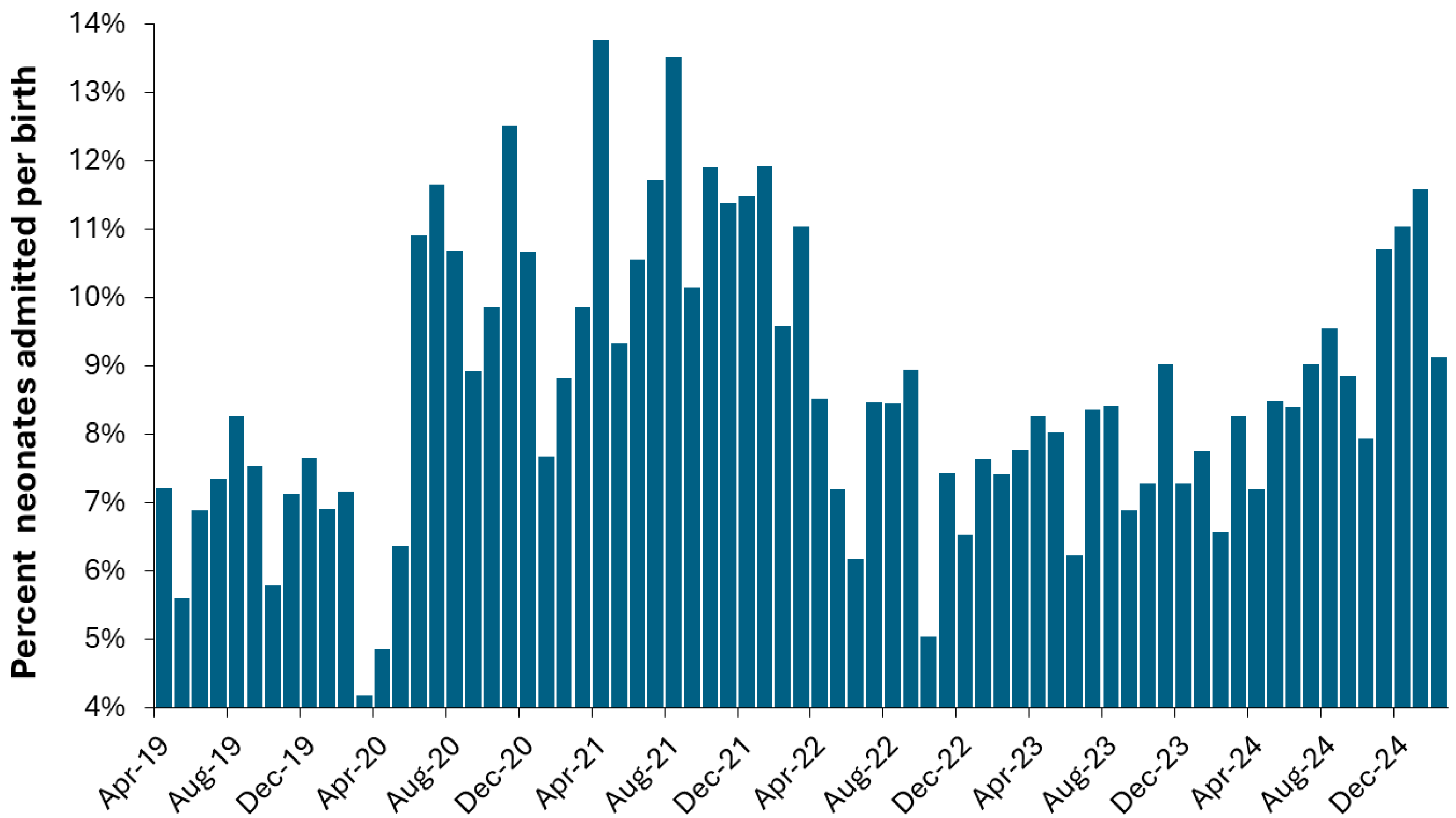
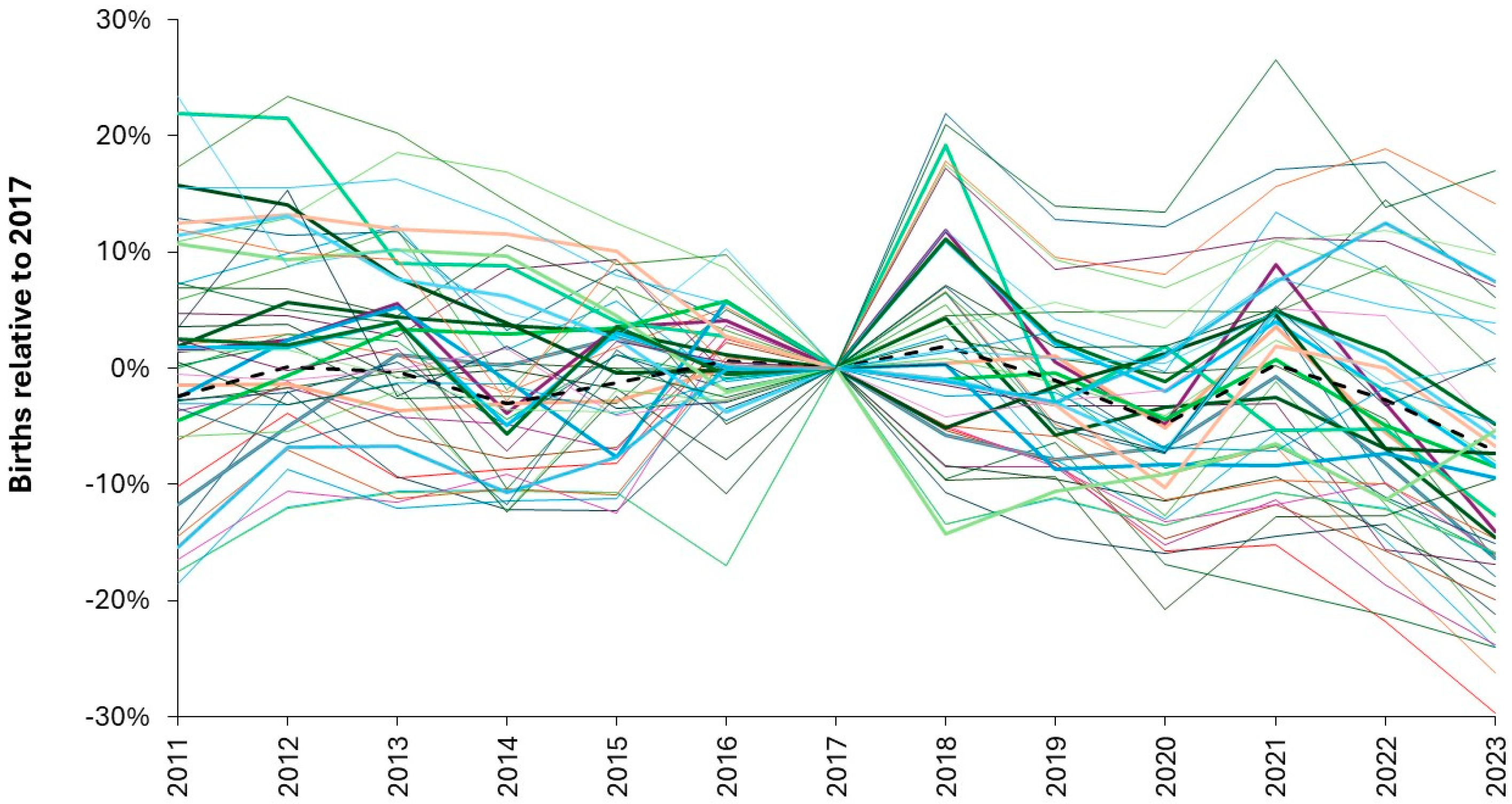
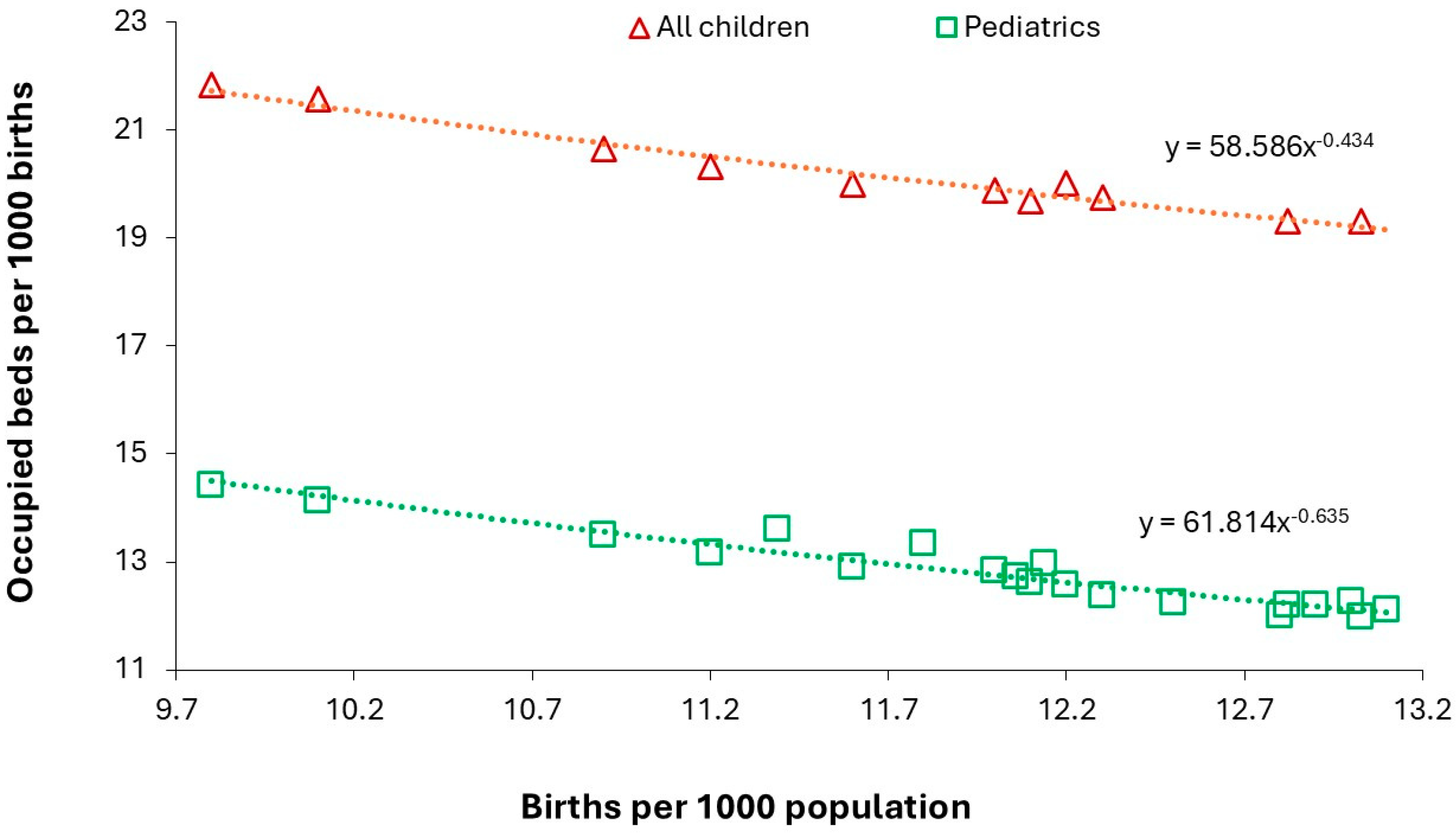
3.5. Using Births to Forecast Pediatric and Neonatal Admissions
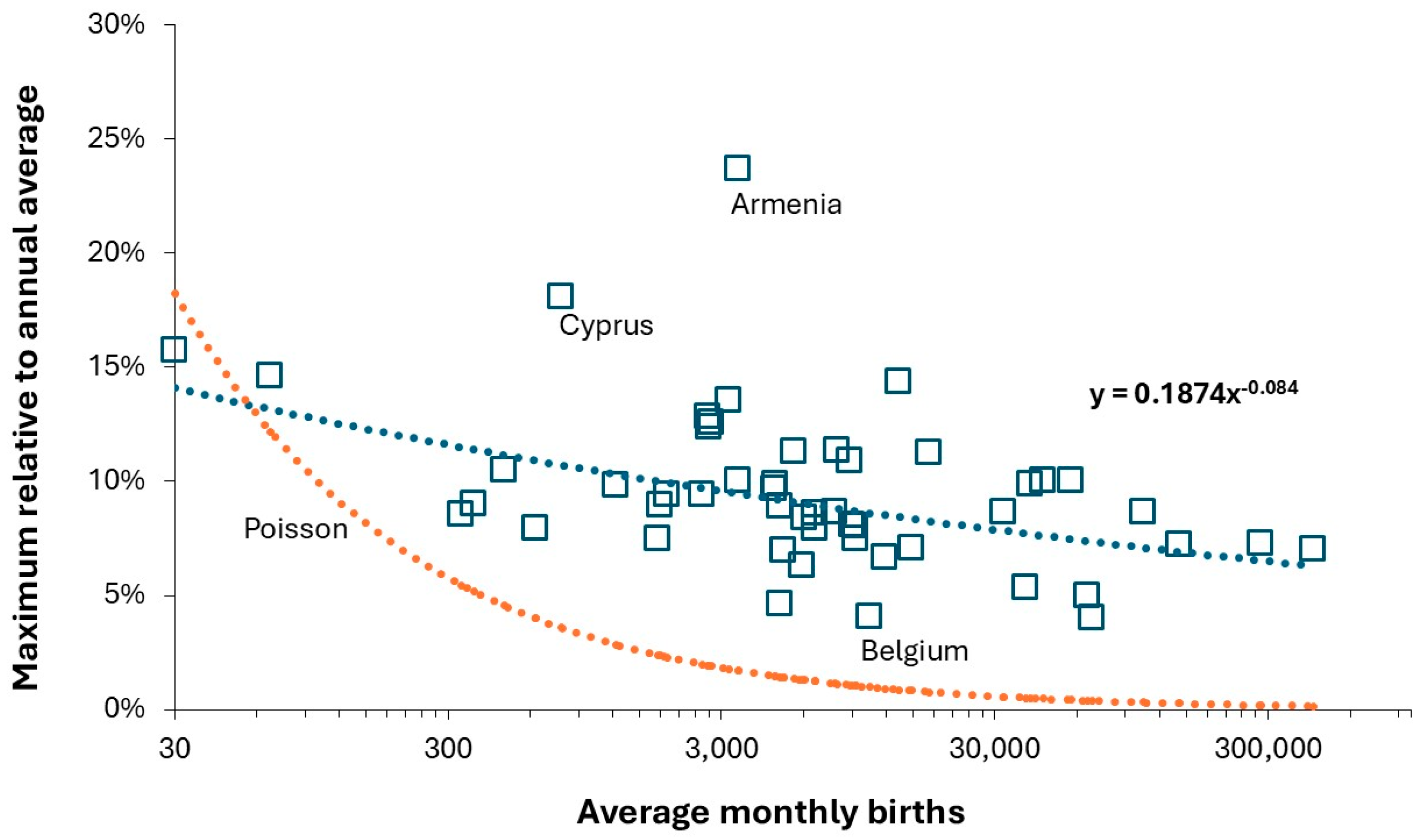
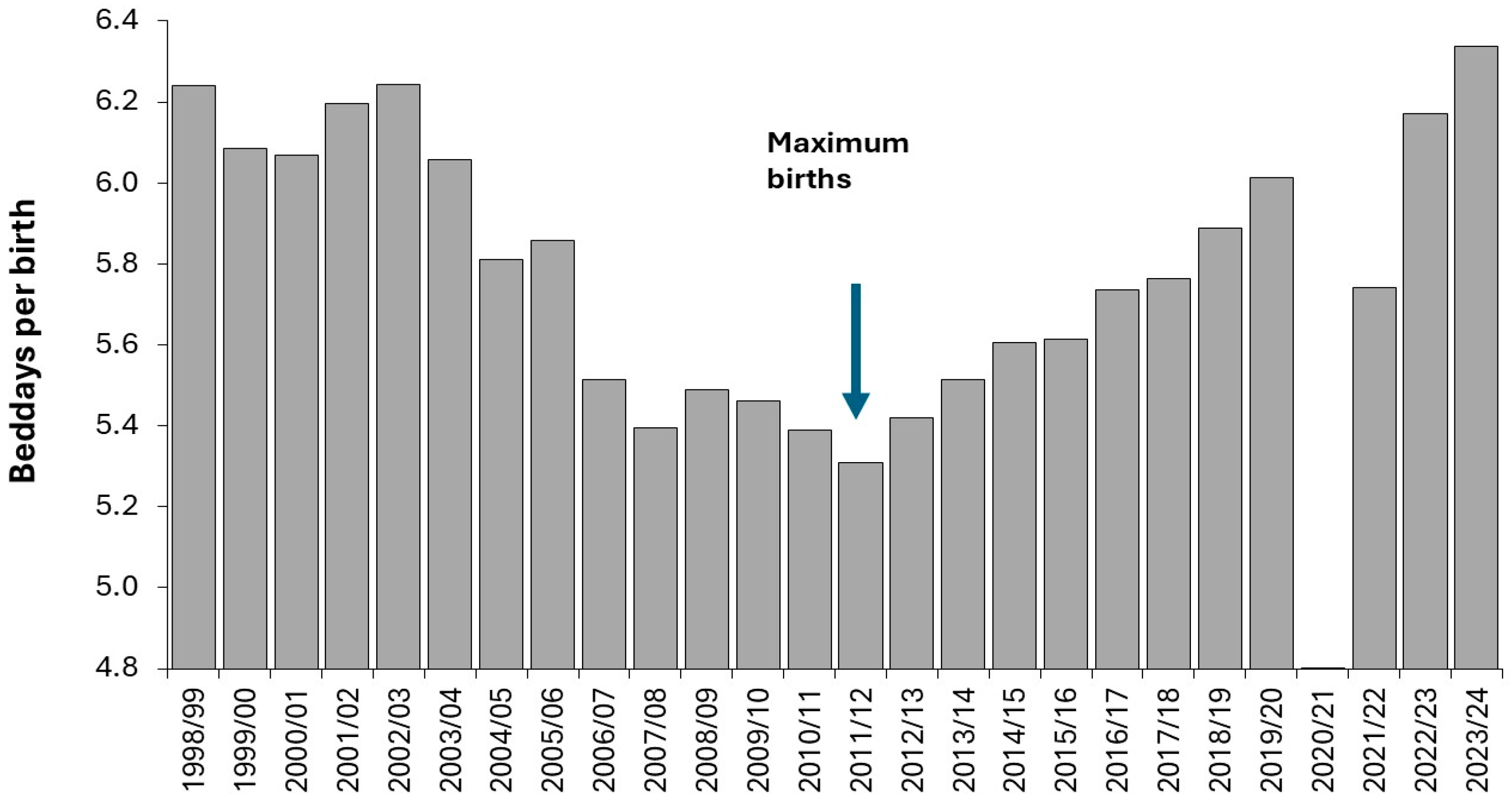
3.6. High Births and Capacity Shocks
3.7. The Dilemma Regarding Forecasting Future Births
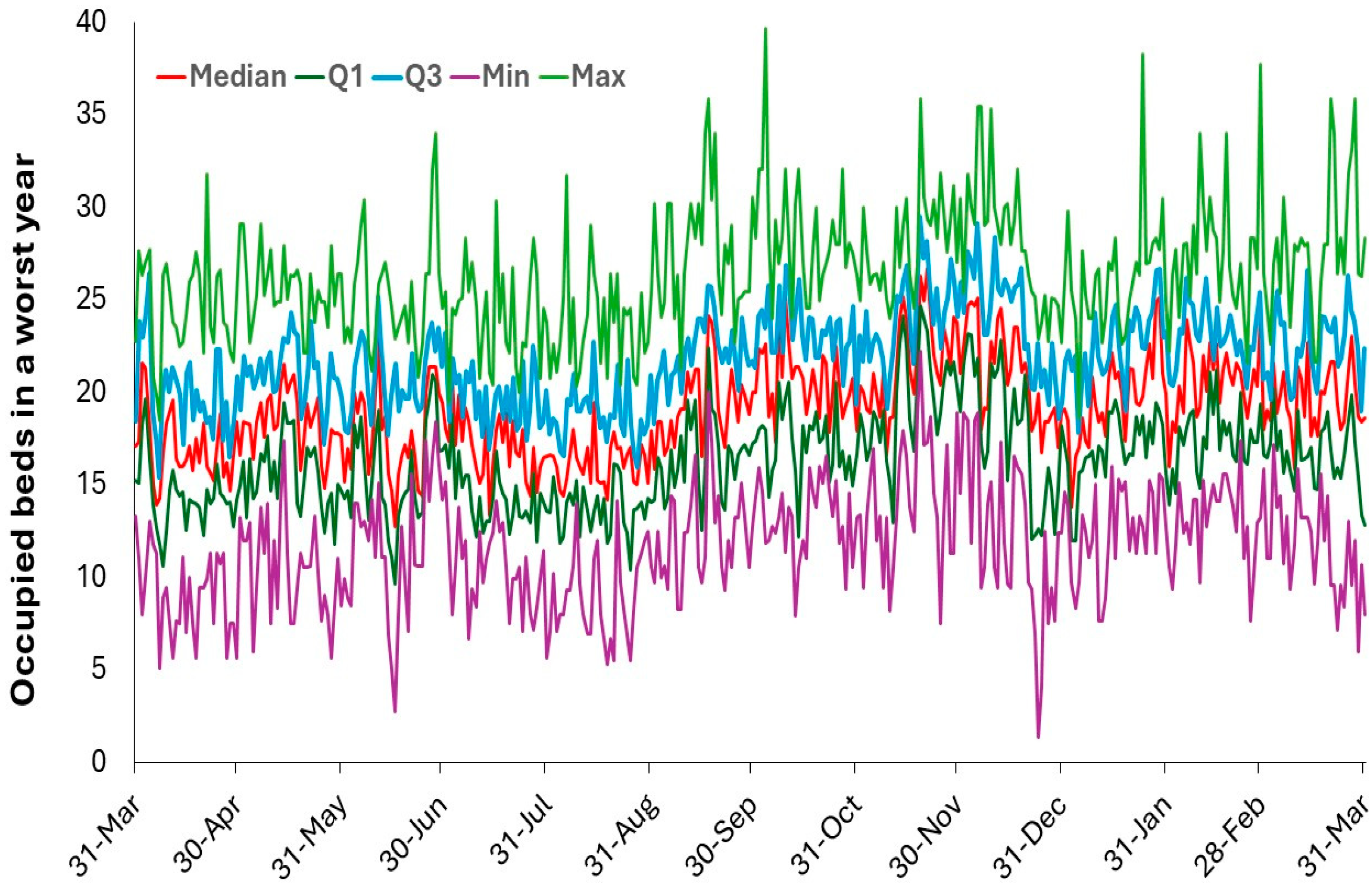
3.8. Using Past Daily Bed Occupancy to Quantify Seasonality and Staffing
3.9. Nearness-to-Death in Pediatric Bed Demand
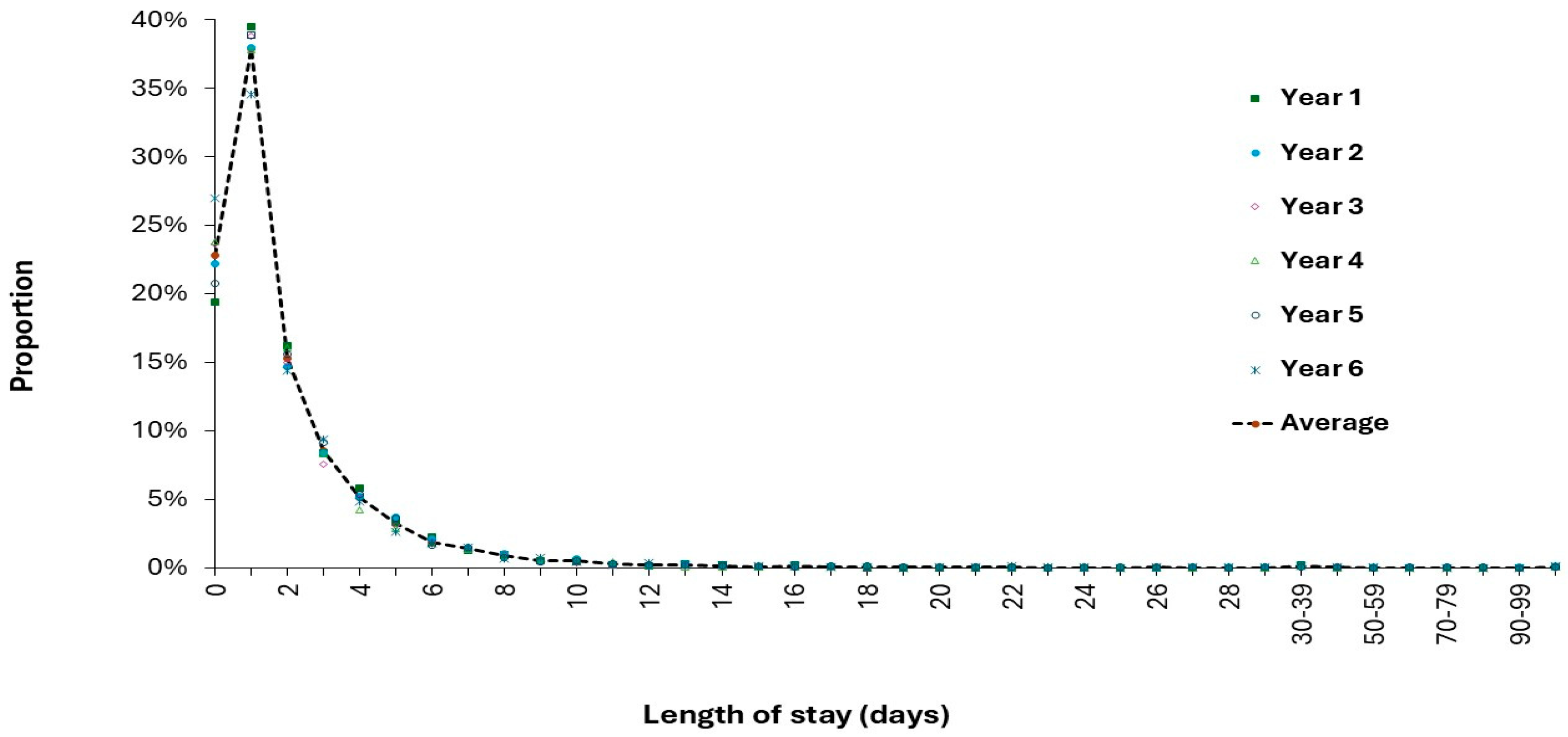
3.10. Pediatric Length of Stay (LOS) and the Benchmarking Fallacy
3.10.1. Different Calculations for Average LOS Give Different Answers
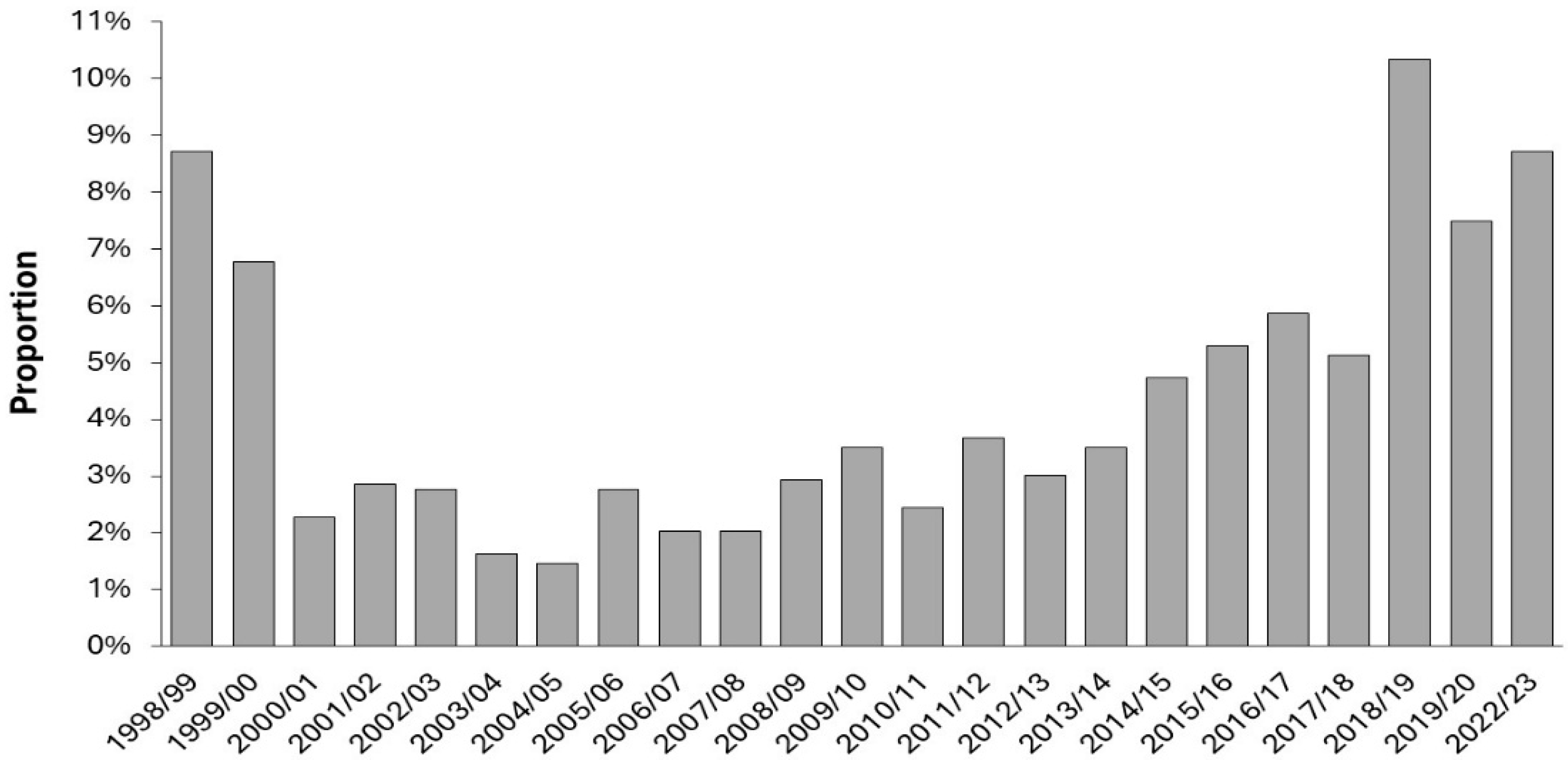
3.10.2. Trends in Pediatric LOS in England
3.10.3. Average LOS from a Single Year is Subject to Sampling Error
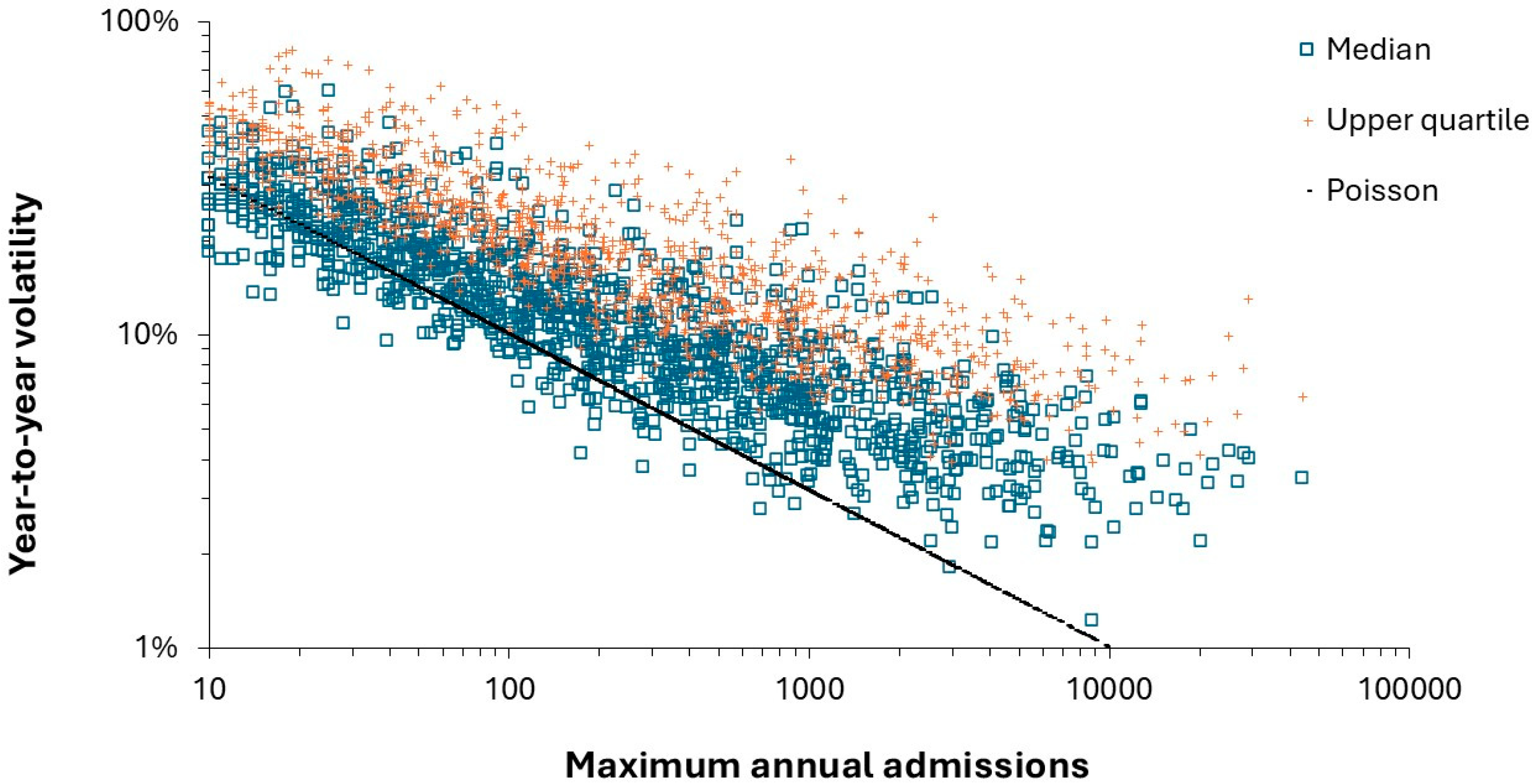
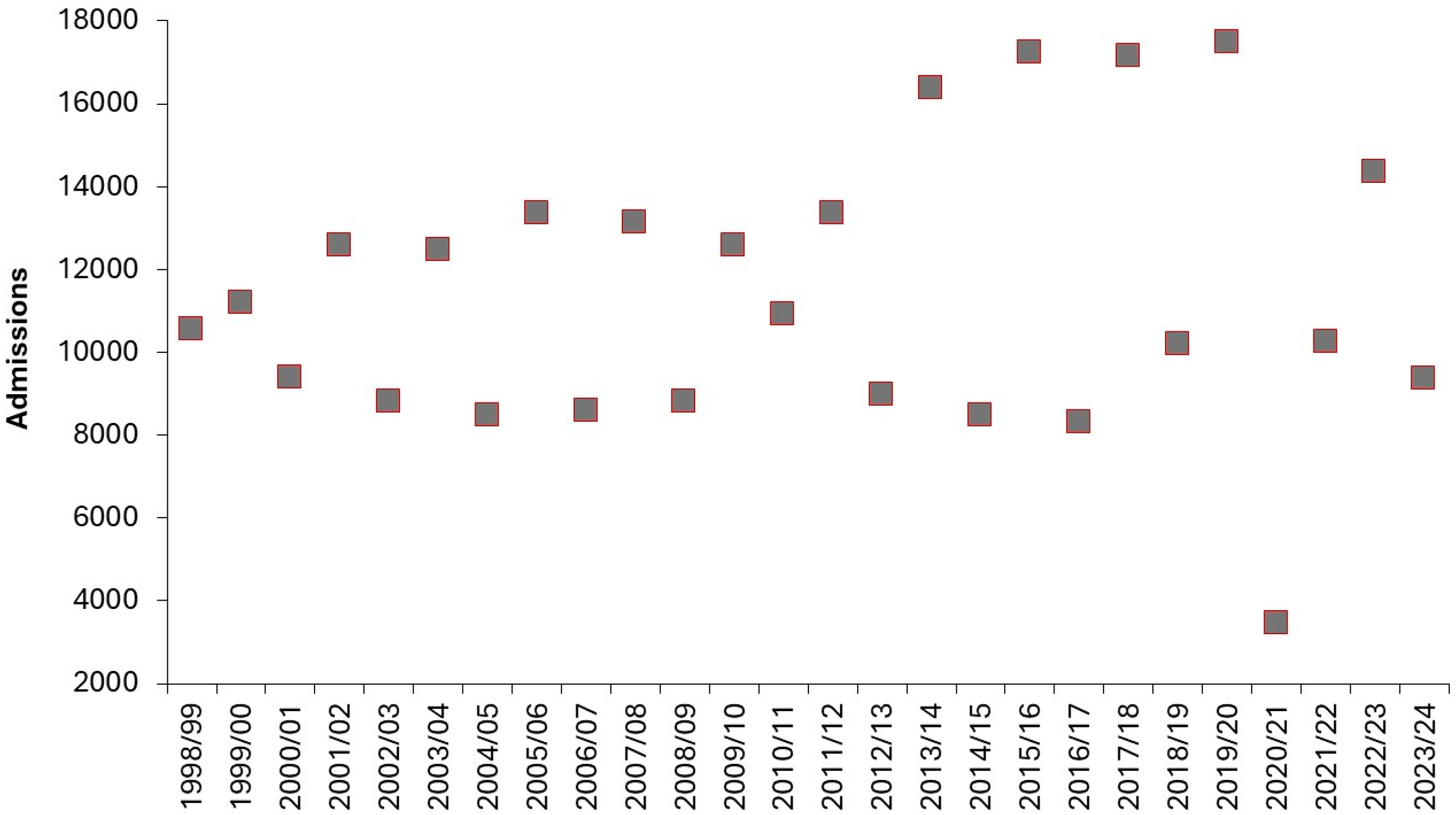
3.11. Pediatric Demand is Intrinsically Unstable (Volatile)
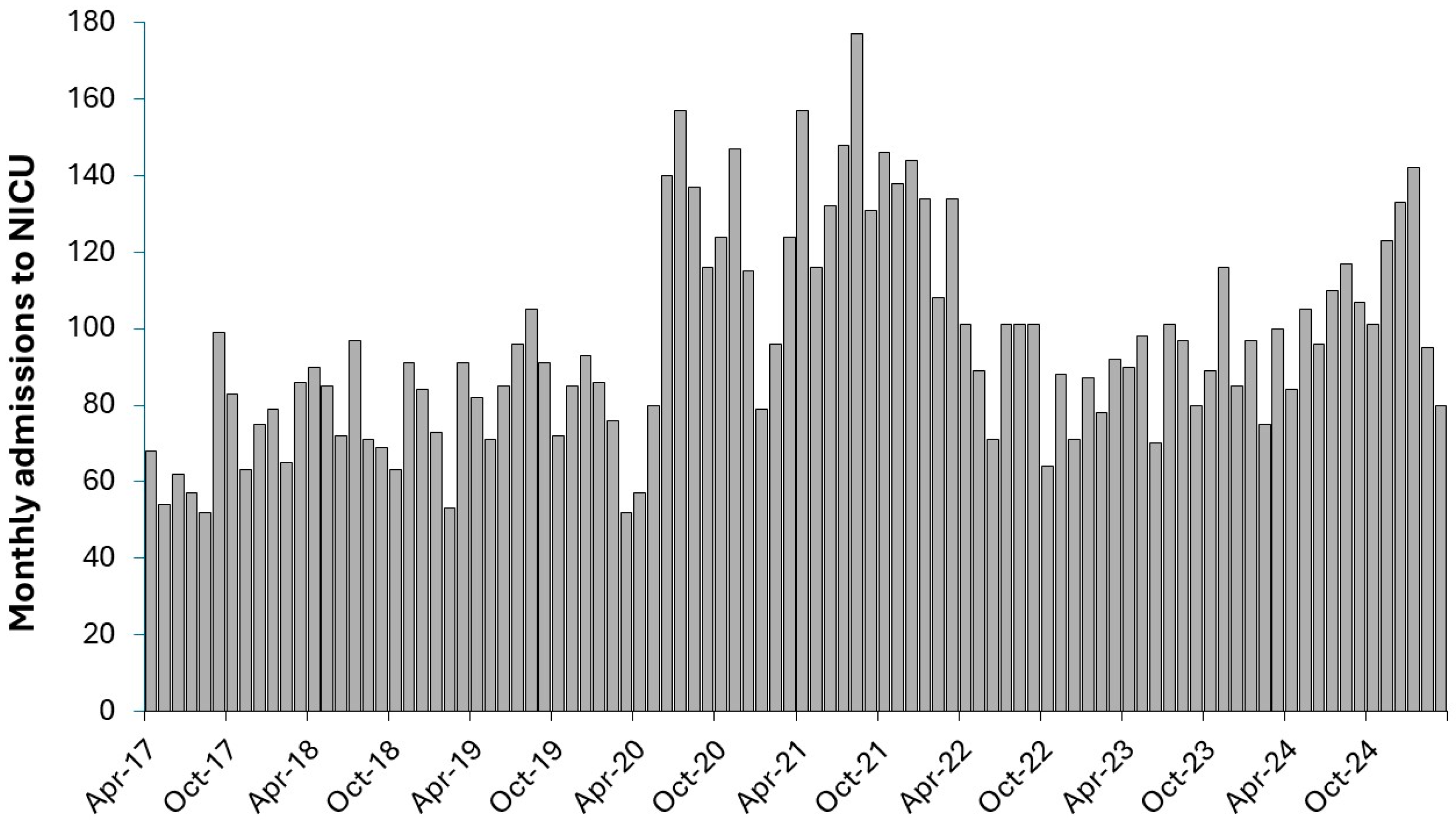
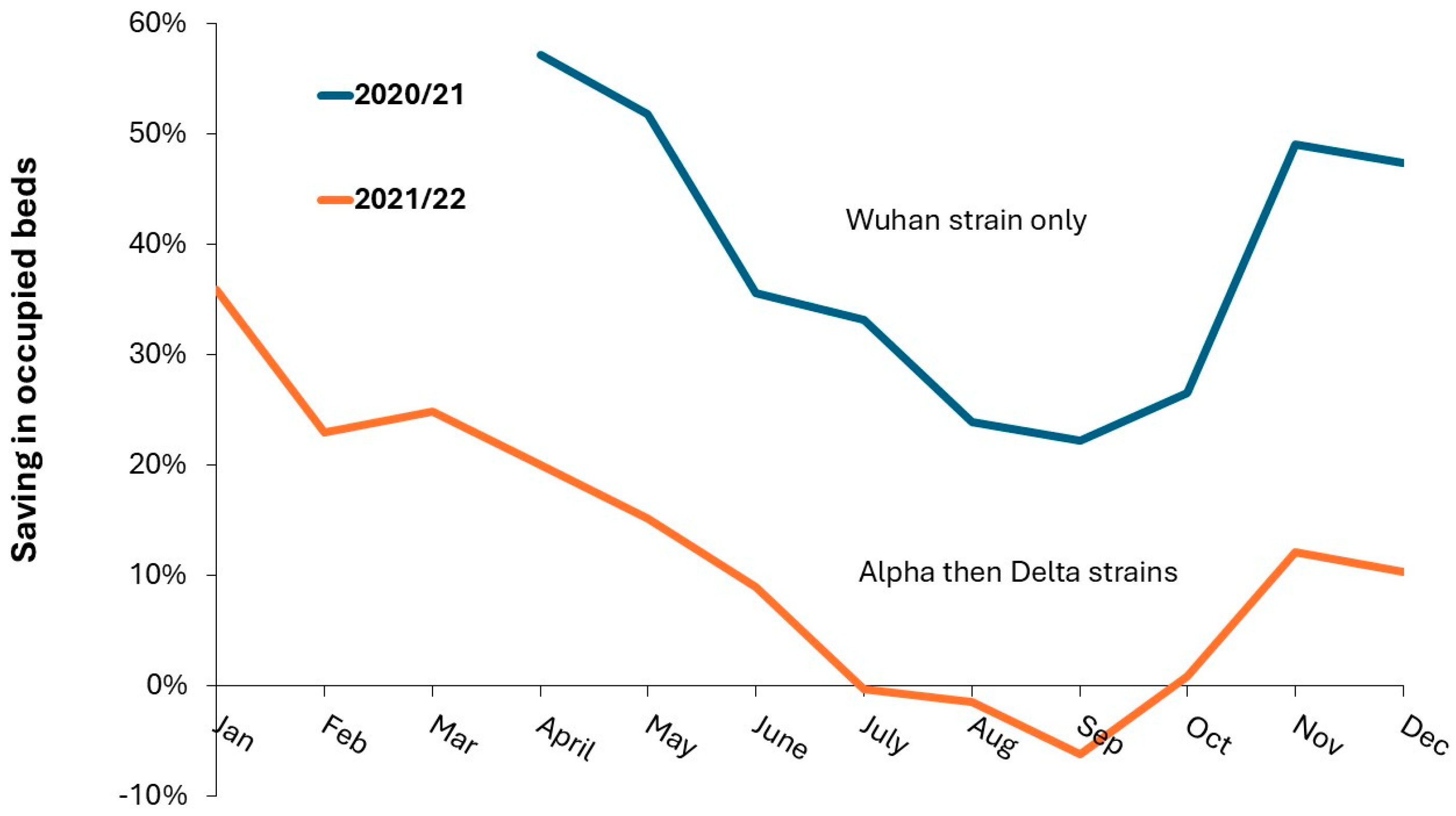
3.12. Effect of COVID-19 on Pediatric Admissions and Occupied Beds
- Different strains of COVID-19 have divergent single-year-of-age profiles in their degree of infectiousness and their deleterious effects, see G.6, G.7in S1.
- COVID-19 strains exert powerful effects on the range of prevailing pathogens via pathogen interference, see G.6 in S1.
- Lockdowns, including school closures, during the pandemic only acted to reduce the transmission of the prevailing pathogens – only when they were in place. Note all lockdown measures were removed toward the end of the 2021/22 financial year [100]
3.13. Benchmarking International Pediatric Bed Demand
3.14. Obtaining a Long-Term Local Overview
4. Discussion
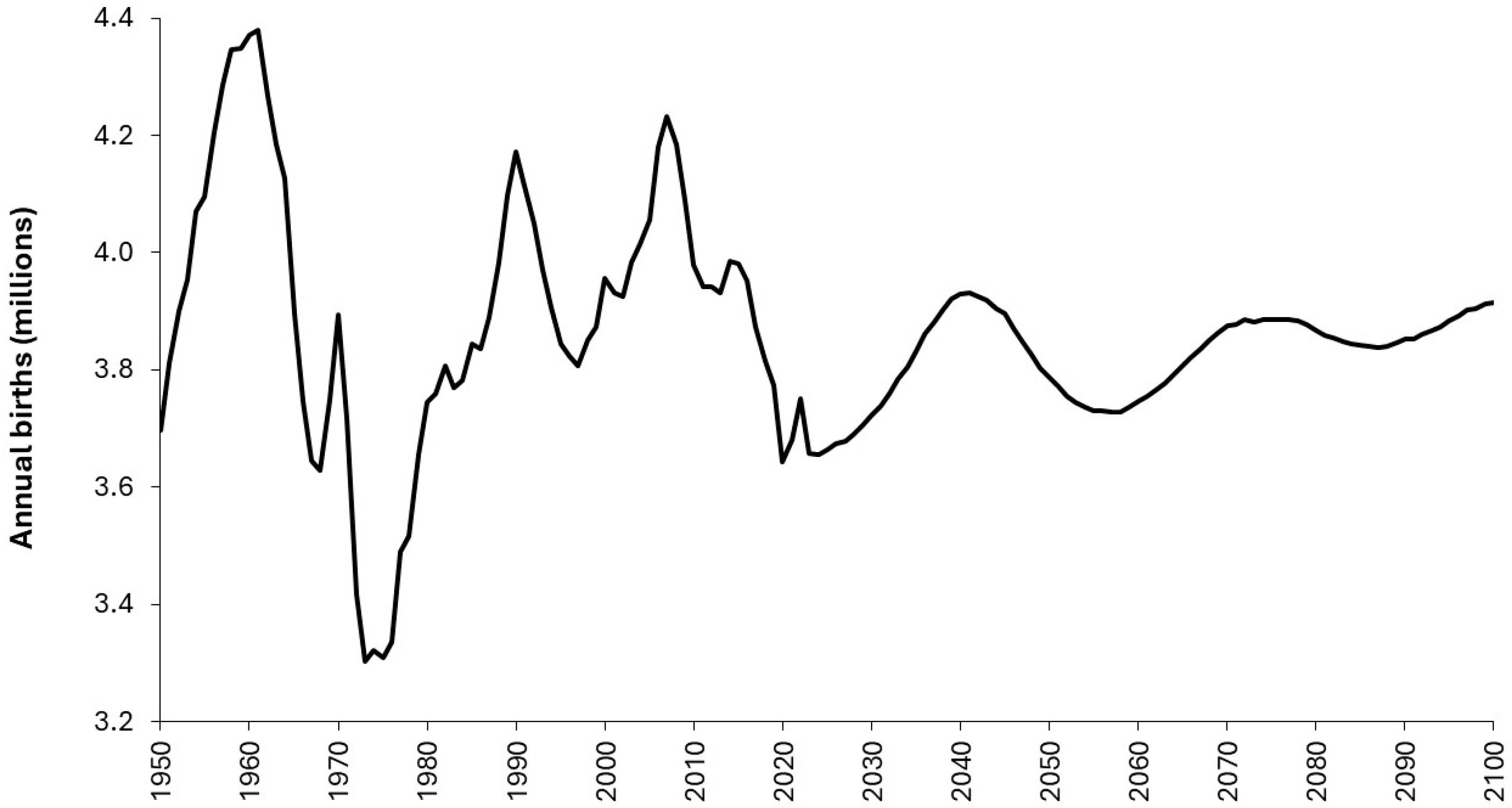
4.1. The Fundamental Role of the Trends in Births
4.2. Variable Seasonality in Births
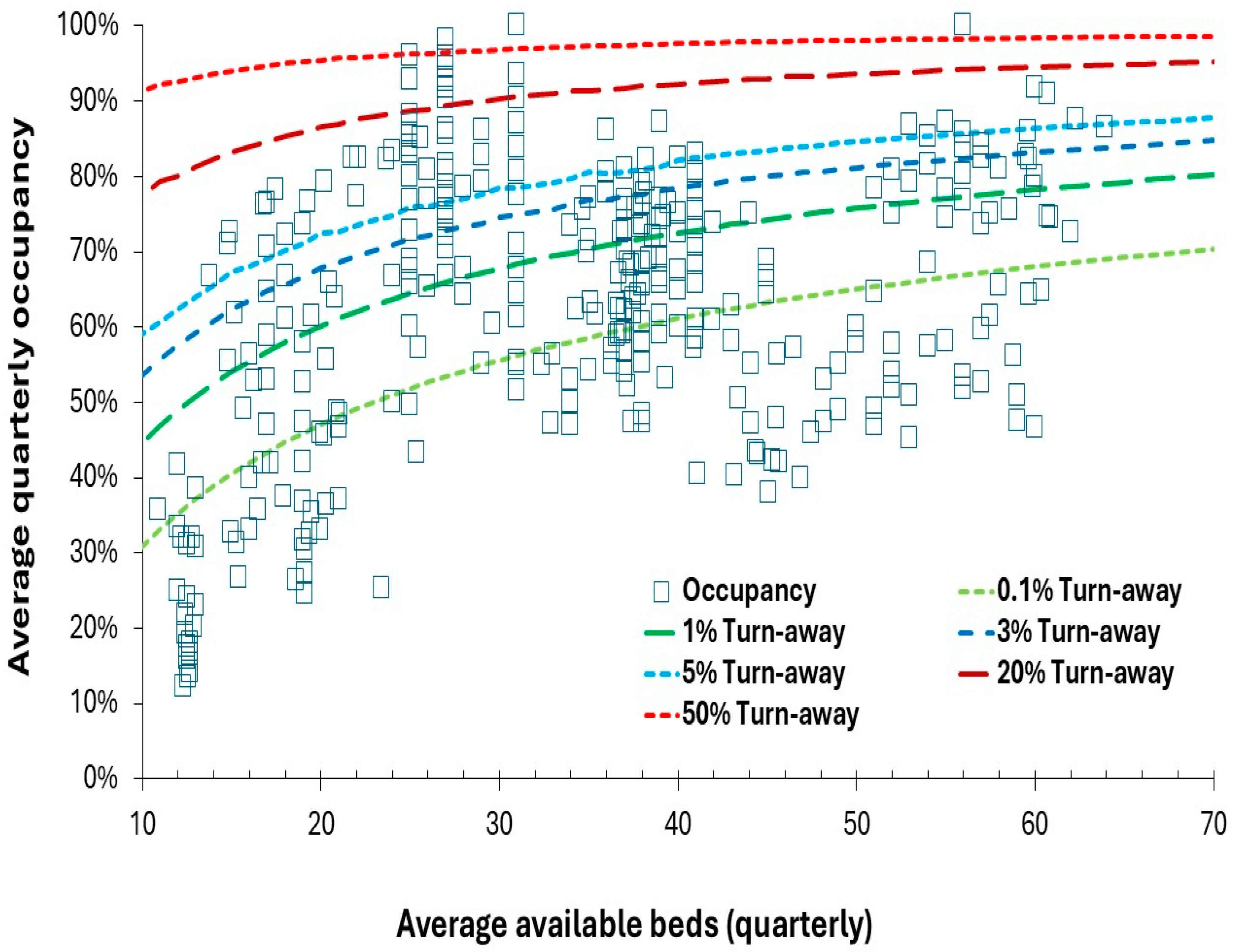
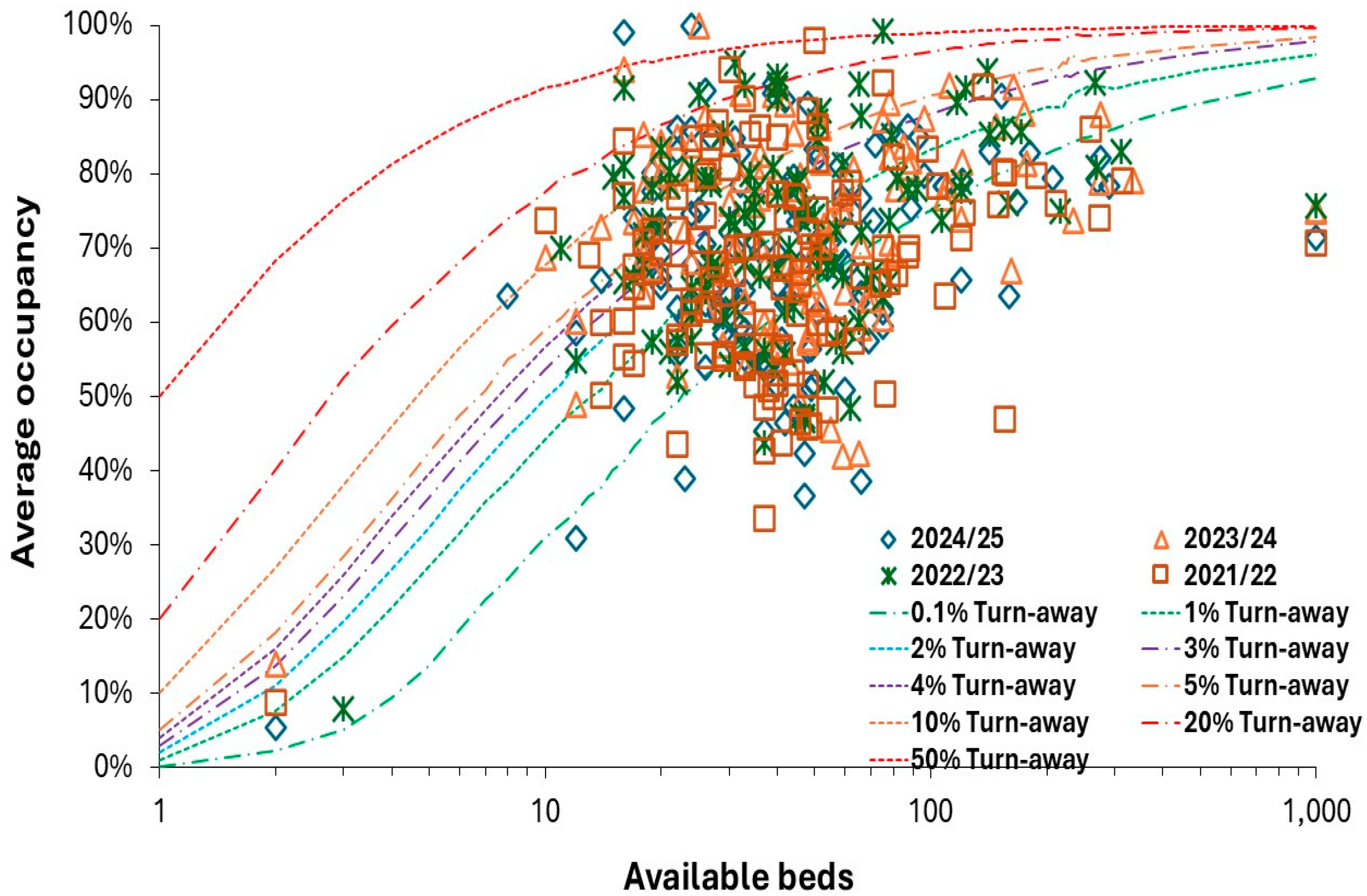
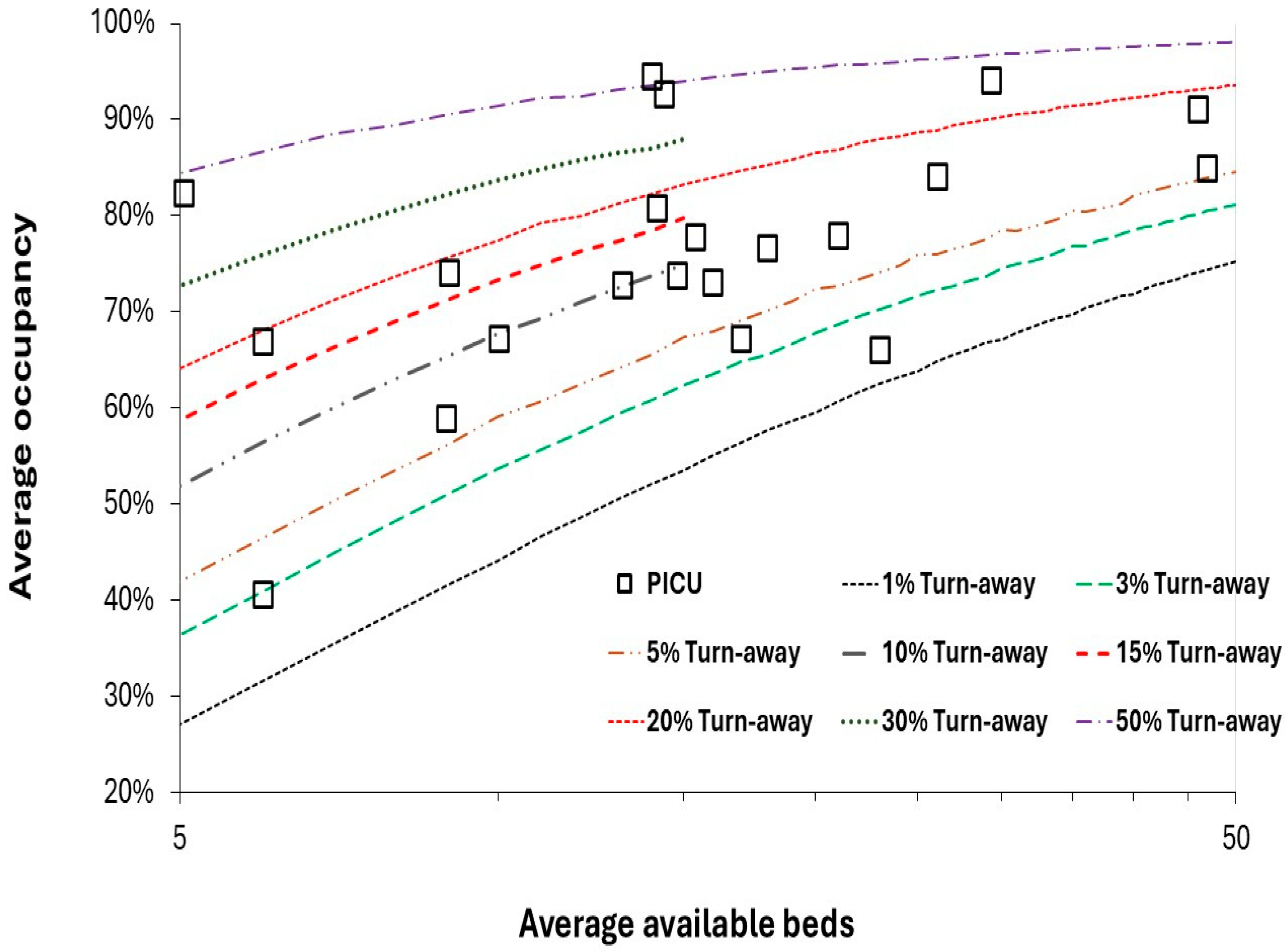
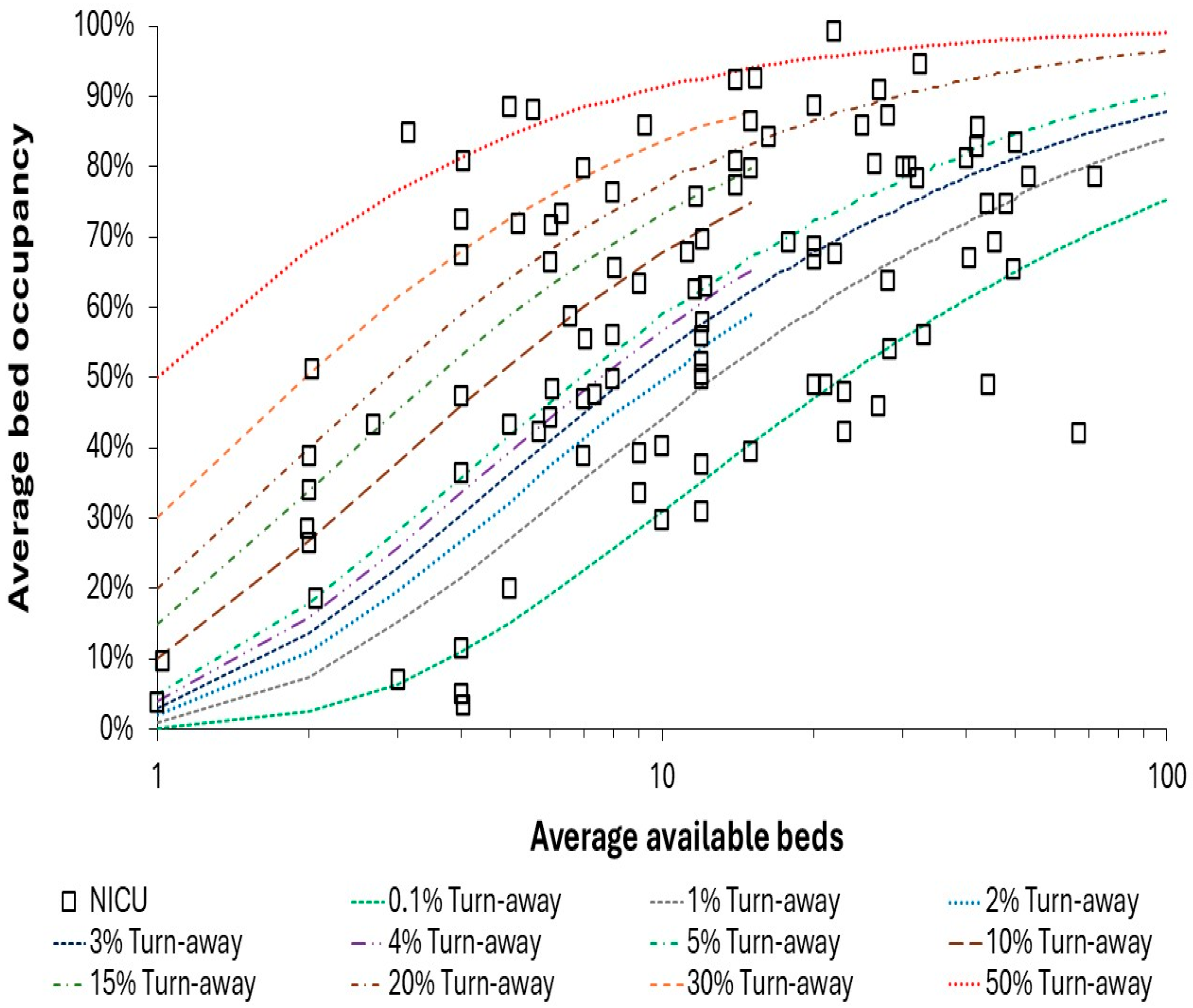
4.3. Unit Size (Beds), Occupancy and Turn-Away
4.4. Poisson Variation is a Hard Taskmaster Especially to the Small Unit
4.5. Benchmarking LOS
4.6. The Illusionary Effect of LOS on Costs
The Fixed Costs Dilemma
4.7. Changes in Pediatric Admissions During the First 12-Months of COVID-19
4.8. Hidden Roles for Pathogens in Childhood Illness
4.5. Using Profiles in Bed Demand to Inform Staffing
4.9. Factors Contributing to the Recent Pediatric Capacity Crisis in England and the USA
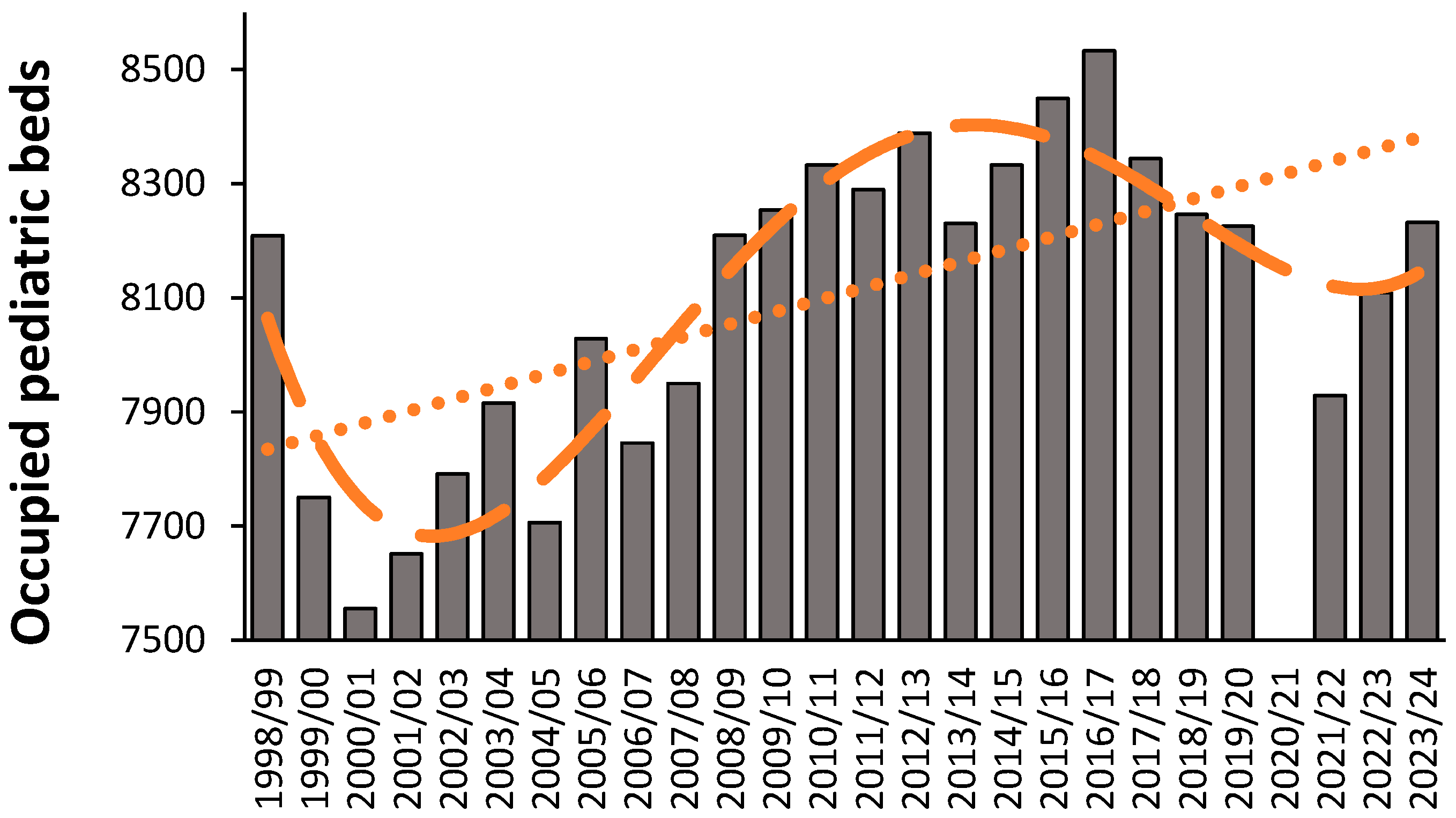
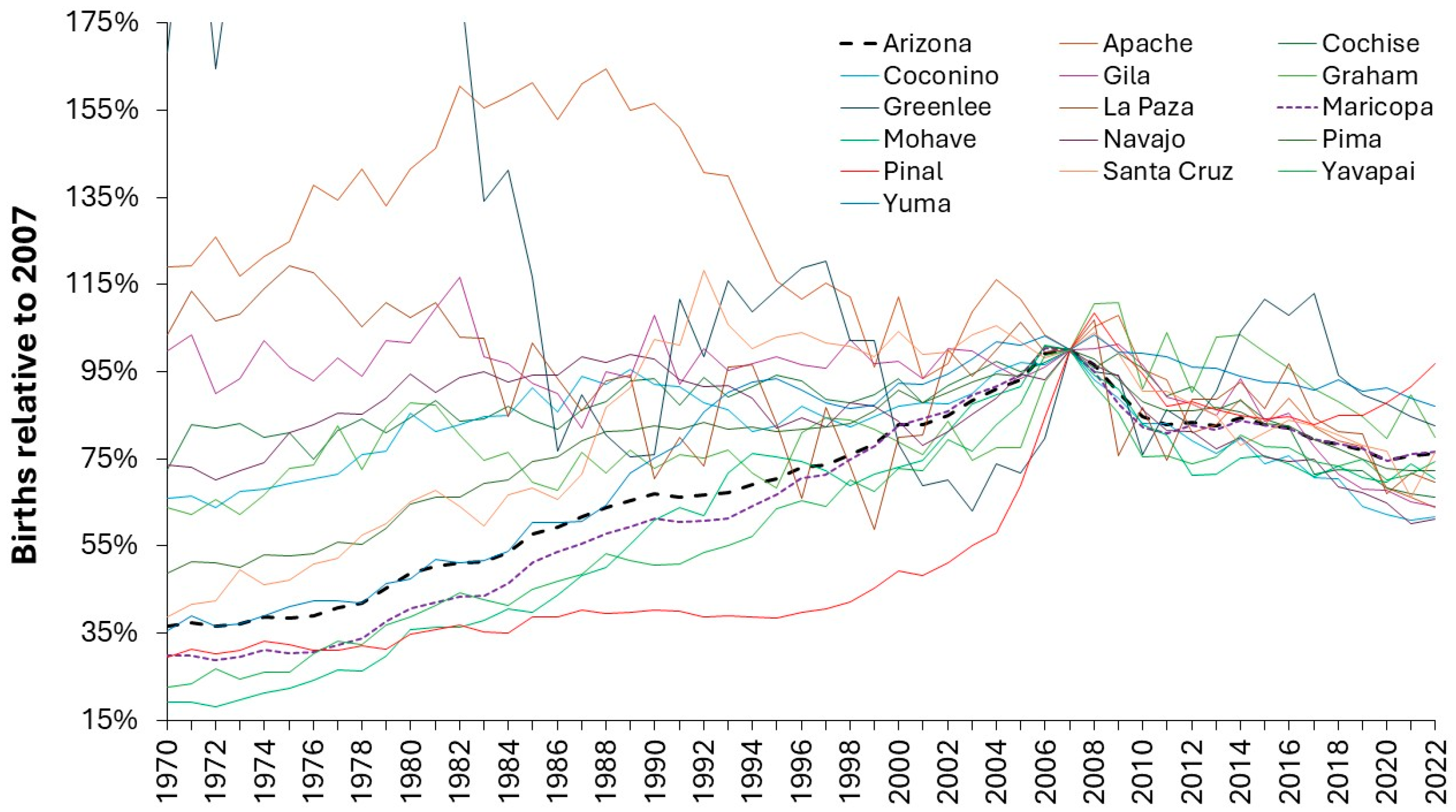
- Planners in the USA seemingly ignored or were completely unaware of the long-term cycle in births shown in Figure 8. This was a by-product of the lack of national oversight for a free-market system having conflicting objectives, i.e. market share at the expense of economy of scale and profit ahead of overall patient care thus delivering a postcode lottery.
- The DRG payments relating to the 50% of pediatric patients covered by Medicaid is not weighted to account for higher costs in smaller units thereby precipitating a flood of unit and bed closures as demonstrated in Figure S13.2 in Supplementary material S13. This would have been compounded by falling births in the downward part of the cycle from 2008 onward, as in Figure 8.
- The exceedingly small size of units in the USA implied a catastrophe guaranteed to occur.
- The issue of capacity planning has been overly influenced by the opinions of politicians and ensuing policy hubris, namely, England had far too many hospital beds, that length of stay was far too high, and that admissions would be diverted into community care. The latter was repeatedly promised but never properly materialized [2].
- These opinions were reinforced by the imposition of Treasury rules for ‘affordability’ imposed upon largely Private Finance Initiative (PFI) new hospital construction from early 1990 onward [2]. The only way to achieve ‘affordability’ was to fiddle the assumptions in the business case thereby reinforcing the opinions of politicians. No one in the NHS was allowed to question what was being imposed upon the NHS.
- Allocation of capital funding is highly regulated and competes for funds against other national priorities. Hence there were virtually no new NHS capital projects following the 2008 financial crash. Both revenue and capital funding in England, collected from general taxation, is not hypothecated and thereby creates regular periods of financial crisis during which many of the promised community schemes were cut.
- As in the USA, the HRG payments are not adjusted to the size of the unit [3].
- As in the USA, the natural cycle in births was completely ignored [2.3].
4.10. The Fixed Costs Dilemma, Transparency in Costs and Population-Based Funding
5. Key Recommendations
- Although the USA and UK have the most extreme examples of cyclic birth trends this does not imply that all areas within these countries will follow the same patterns [3]. Health departments should insist that statistical agencies prepare a wider range of birth forecasts which can include those based on TFR, three-parameter models, and other pragmatic local approaches detailed in this and the previous study [3]. They must ensure that the potential range of births is communicated to all regional health authorities and hospitals. Hospitals should have contingency plans to deal with anticipated periods of higher births [3] and deal with surges in demand.
- The ideal position is that pregnancy, childbirth, neonatal and pediatric care be free of charge and funded from hypothecated state general taxation. For-profit health insurance with its inherent high transaction costs, and temptation to maximize profits is incompatible with care delivered to those who are unable, by virtue of childhood, to earn money. The USA appears to exemplify this requirement with disturbingly poor childhood mortality across all age bands.
- It must be clearly understood that small maternity/neonatal/pediatric will suffer from unavoidable high capital and staff costs per admission and that these costs will be further distorted by the allocation of shared overhead costs as was discussed previously [3].
- The USA appears to have a gross excess of specialist children’s hospitals and pediatric units driven partly by competition for market share and low population density in particular states. With 45% of pediatric units having 9 or fewer beds, and 25% with fewer than 5 beds [43] the inevitable outcome can only be a very expensive form of chaos. It is recommended that no town or smaller city should have more than 1 maternity/neonatal/pediatric unit – in order to gain the benefits of economy of scale and to ensure that the relevant teams have an appropriate level of experience as reflected in the weighted pediatric readiness score (WPRS) for the associated ED or pediatric assessment unit [126], or in higher procedure volumes per surgeon [Aguilera].
- Given the very high childhood mortality in the USA, it is suggested that State governments intervene to promote rationalization among the 45% of pediatric units with fewer than 9 beds. A minimum size of 10 beds is suggested, and preferably up to 30 beds. State governments may need to operate pediatric units in remote locations where such rationalization is not possible. One possibility is that one hospital focuses on maternity while another focusses on pediatrics. Both will then benefit from higher economy of scale. Dare it be said, please America act for the sake of your children.
- High pediatric inpatient occupancy (and related turn-away) are known to be associated with delays to admission and poor patient outcomes such as hospital acquired infection rates [28,114,162]. Such studies are usually conducted at large units where bed occupancy is used as an (incorrect) proxy for turn-away - although the bed occupancy rate is also a proxy measure for busyness. An upper limit on turn-away should be stipulated for pediatric units. Given the fact that many units operate at an annual or quarterly turn-away less than 0.1%, it is suggested that no unit should operate at >5% turn-away in the worst quarter. An upper limit for turn-away would also partly correct issues associated with high bed occupancy (busyness) – see #7 below.
- Pediatric bed demand is highly seasonal including particularly high years. The bed planning calculation is therefore one regarding available floor space rather than a fixed number of beds. The floor space simply provides the opportunity to flex the number of available beds which will range from sleeping cots for the youngest through to single rooms or separate wards for the oldest children. Such flexibility is profoundly important for staffing, which dictates against small units. A method was presented to estimate the required numbers of full-time and on-call staff to minimize total staff costs. It is recognized that units situated in small towns and remote areas will struggle to implement such flexibility unless on-call staff can be redeployed from elsewhere.
- The inherent volatility in pediatric bed demand implies that the actual trends in occupied beds become the benchmark rather than futile attempts to separately forecast admissions and LOS – which are both part of the inherent volatility.
6. Policy and Funding Implications
7. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgements
Conflicts of Interest
Acknowledgments
Appendix A
| Country | Births (monthly) | Maximum | Month |
|---|---|---|---|
| Ukraine | 40,504 | 9.8% | February/July |
| Azerbaijan | 13,390 | 14.4% | February/July |
| Norway | 4,911 | 8.9% | June |
| Andorra | 67 | 14.6% | June |
| Finland | 4,907 | 4.6% | July |
| Denmark | 5,068 | 7.0% | July |
| Sweden | 9,320 | 7.5% | July |
| Montenegro | 630 | 7.9% | July |
| Czechia | 9,335 | 8.0% | July |
| Belarus | 9,017 | 8.1% | July |
| Bulgaria | 6,030 | 8.4% | July |
| Latvia | 1,801 | 8.9% | July |
| Lithuania | 2,554 | 9.4% | July |
| Estonia | 1,233 | 9.8% | July |
| Luxembourg | 484 | 10.5% | July |
| Greece | 8,832 | 10.9% | July |
| Romania | 17,227 | 11.3% | July |
| Liechtenstein | 29 | 15.7% | July |
| Belgium | 10,506 | 4.0% | July/September |
| Slovenia | 1,763 | 7.5% | July/September |
| Poland | 32,469 | 8.6% | July/September |
| France | 68,466 | 4.0% | September |
| United Kingdom | 65,537 | 5.0% | September |
| Spain | 38,856 | 5.4% | September |
| Ireland | 5,908 | 6.3% | September |
| European Free Trade Association | 11,891 | 6.6% | September |
| European Union (28 countries) | 439,105 | 7.0% | September |
| Netherlands | 14,945 | 7.0% | September |
| Russia | 142,609 | 7.2% | September |
| Austria | 6,579 | 8.0% | September |
| Malta | 336 | 8.6% | September |
| Switzerland | 6,576 | 8.6% | September |
| Hungary | 7,806 | 8.7% | September |
| Turkey | 105,223 | 8.7% | September |
| Iceland | 375 | 9.0% | September |
| Macedonia | 1,908 | 9.4% | September |
| Georgia | 4,708 | 9.7% | September |
| Slovakia | 4,743 | 9.9% | September |
| Croatia | 3,459 | 10.0% | September |
| Germany | 57,116 | 10.0% | September |
| Italy | 45,124 | 10.0% | September |
| Serbia | 5,561 | 11.3% | September |
| Portugal | 7,923 | 11.3% | September |
| Bosnia and Herzegovina | 2,841 | 14.8% | September |
| Moldova | 3,204 | 13.5% | September |
| Kosovo | 2,757 | 14.0% | September |
| Albania | 4,187 | 19.6% | September |
| Cyprus | 779 | 18.1% | September |
| Armenia | 3,446 | 23.7% | September |
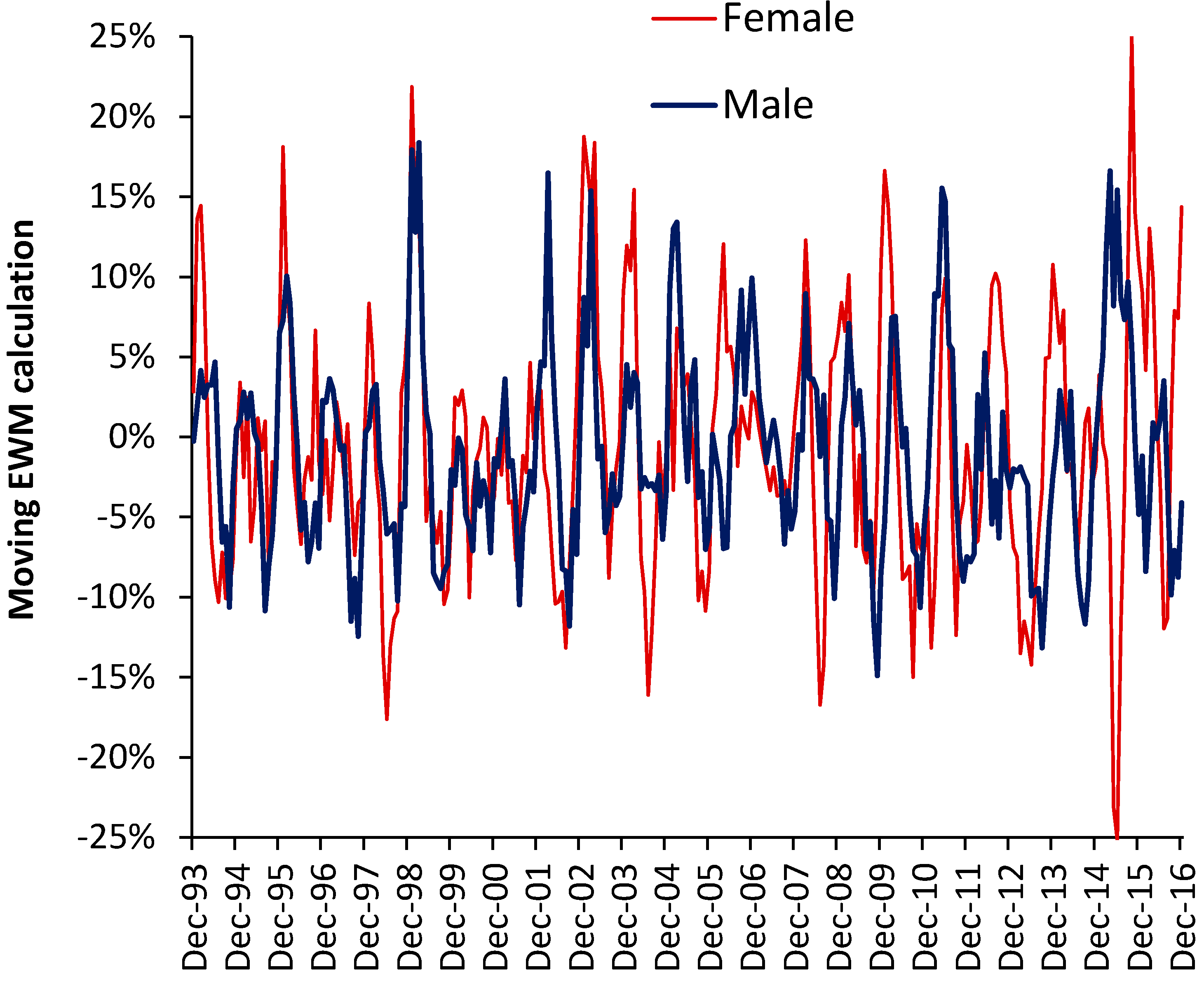
| Age | Female | Male | ||
|---|---|---|---|---|
| Max | When | Max | When | |
| 0 | 25% | Oct-15 | 18% | Mar-99 |
| 1 | 70% | May-16 | 77% | May-07 |
| 2 | 182% | Mar-14 | 129% | Mar-15 |
| 3 | 178% | Apr-03 | 170% | Mar-03 |
| 4 | 200% | Apr-06 | 143% | Dec-13 |
| 5 | 150% | Aug-12 | 143% | Dec-10 |
| 6 | 162% | Jun-06 | 180% | Feb-10 |
| 7 | 200% | Jul-16 | 167% | Jun-08 |
| 8 | 367% | Oct-09 | 150% | Jun-12 |
| 9 | 329% | Jan-08 | 220% | Apr-14 |
| 10 | 340% | Jun-12 | 240% | May-08 |
| 11 | 180% | Mar-15 | 200% | Jul-14 |
| 12 | 256% | Apr-11 | 113% | Jan-11 |
| 13 | 227% | Nov-09 | 220% | Apr-12 |
| 14 | 153% | Mar-11 | 92% | Jun-11 |
| 15 | 122% | Aug-05 | 100% | Jul-06 |
| 16 | 129% | Feb-14 | 82% | Nov-16 |
| 17 | 110% | May-15 | 82% | Apr-99 |
| 18 | 96% | Feb-00 | 46% | Aug-95 |
| 19 | 100% | Dec-97 | 41% | Aug-13 |
References
- Jones, R.P. Addressing the Knowledge Deficit in Hospital Bed Planning and Defining an Optimum Region for the Number of Different Types of Hospital Beds in an Effective Health Care System. Int. J. Environ. Res. Public Health 2023, 20, 7171. [Google Scholar] [CrossRef] [PubMed]
- Jones, R.P. A New Approach for Understanding International Hospital Bed Numbers and Application to Local Area Bed Demand and Capacity Planning. Int. J. Environ. Res. Public Health 2024, 21, 1035. [Google Scholar] [CrossRef]
- Jones, R.P. Capacity Planning (Capital, Staff and Costs) of Inpatient Maternity Services: Pitfalls for the Unwary. Int. J. Environ. Res. Public Health 2025, 22, 87. [Google Scholar] [CrossRef]
- Raftery, A.; Ševčíková, H. Probabilistic population forecasting: Short to very long-term. Int J Forecasting. 2023, 39(1), 73–97. [Google Scholar] [CrossRef] [PubMed]
- Lee, R. Forecasting Population in an Uncertain World: Approaches, New Uses, and Troubling Limitations. Population and Development Review. 2025. [CrossRef]
- Keilman, N. Uncertain population forecasts. Nature. 2001, 412, 490–491. [Google Scholar] [CrossRef] [PubMed]
- Caro-Barrera, J.; García-Moreno, G.; Pérez-Priego, M. Projecting Spanish fertility at regional level: A hierarchical Bayesian approach. PLoS One. 2022, 17(10), e0275492. [Google Scholar] [CrossRef]
- Kallis, C,; Maslova, E,; Morgan, A. ; Sinha, T.; Roberts,; G.; van der Valk, R.; Quint, J.; Tran, T. Recent trends in asthma diagnosis, preschool wheeze diagnosis and asthma exacerbations in English children and adolescents: a SABINA Jr study. Thorax 2023, 78, 1175–1180.
- Turner, P.; Conrado, A.; Kalis, C.; O’Rourke, E.; Haider, S.; Ullah, A.; et al. Time trends in the epidemiology of food allergy in England: an observational analysis of Clinical Practice Research Datalink data. The Lancet Public Health. 2024, 9(9), e664 - e673.
- Steliarova-Foucher, E.; Fidler, M.; Colombet, M.; Lacour, B.; Kaatsch, P.; Piñeros, M.; et al. Changing geographical patterns and trends in cancer incidence in children and adolescents in Europe, 1991–2010 (Automated Childhood Cancer Information System): a population-based study. The Lancet Oncology. 2018, 19(9), 1159 – 1169.
- Marshak, A.; Venkat, A.; Young, H.; Naumova, E. How Seasonality of Malnutrition Is Measured and Analyzed. Int J Environ Res Public Health. 2021, 18(4), 828. [Google Scholar] [CrossRef]
- Naumova, EN. Mystery of seasonality: getting the rhythm of nature. J Public Health Policy. 2006, 27(1), 2–12. [Google Scholar] [CrossRef]
- Dopico, X.; Evangelou, M.; Ferreira, R.; et al. Widespread seasonal gene expression reveals annual differences in human immunity and physiology. Nat Commun. 2015, 6, 7000. [Google Scholar] [CrossRef] [PubMed]
- Fleming, D.; Norbury, C.; Crombie, D. Annual and seasonal variation in the incidence of common diseases. Royal College of General Practitioners, Occasional paper 53, 91. ISBN 0 85084 161 5. Printed by Arrowsmith Ltd, Bristol. 19 October.
- Damiani, M.; Dixon, J. Managing the pressure. Emergency hospital admissions in London, 1997-2001. King’s Fund, 2001. ISBN 1 85717 461 5. King’s Fund Publishing, London.
- Chen, Z.; Tsui, J.; Cai, J.; Su, S.; Viboud, C.; du Plessis, L.; Lemey, P.; Kraemer, M.; Yu, H. Disruption of seasonal influenza circulation and evolution during the 2009 H1N1 and COVID-19 pandemics in Southeastern Asia. Nat Commun. 2025, 16, 475. [Google Scholar] [CrossRef]
- National Academies of Sciences, Engineering, and Medicine. Pivotal Interfaces of Environmental Health and Infectious Disease Research to Inform Responses to Outbreaks, Epidemics, and Pandemics: Proceedings of a Workshop—in Brief. Washington, DC: The National Academies Press. 2021. [CrossRef]
- Wu, X.; Lu, Y. ; Zhou,S. ; Chen, L.; Xu, B. Impact of climate change on human infectious diseases: Empirical evidence and human adaptation. Environ Internat. 2016, 86, 14–23. [Google Scholar] [CrossRef]
- Green, L. Capacity Planning and Management in Hospitals. In: Brandeau, M.L., Sainfort, F., Pierskalla, W.P. (eds) Operations Research and Health Care. International Series in Operations Research & Management Science. 2005, vol 70. Springer, Boston, MA. [CrossRef]
- Harper, P.; Shahani, A. Modelling for the planning and management of bed capacities in hospitals. Journal of the Operational Research Society. [CrossRef]
- Kuntz, L.; Scholtes, S.; Vera, A. Incorporating efficiency in hospital-capacity planning in Germany. Eur J Health Econ, 2007; 8, 213–223. [Google Scholar] [CrossRef]
- Kimes, D.; Levine, E.; Timmins, S.; Weiss, S.; Bollinger, M.; Blaisdell, C. Temporal dynamics of emergency department and hospital admissions of pediatric asthmatics. Environmental Research. 2004, 94(1), 7–17. [Google Scholar] [CrossRef] [PubMed]
- Ramgopal, S.; Dunnick, J.; Siripong, N.; Conti, K.; Gaines, B.; Zuckerbraun, N. Seasonal, Weather, and Temporal Factors in the Prediction of Admission to a Pediatric Trauma Center. World J. Surg. 2019, 43: 2211-2217 1. [CrossRef]
- Xirasagar, S. , Lin, HC. & Liu, TC. Seasonality in pediatric asthma admissions: the role of climate and environmental factors. Eur J Pediatr. 2006, 165, 747–752. [Google Scholar] [CrossRef]
- Lipsett, S.; Monuteaux, M.; Fine, A. Seasonality of Common Pediatric Infectious Diseases. Pediatric Emergency Care. 2021, 37(2), 82–85. [Google Scholar] [CrossRef] [PubMed]
- Farmer, R.; Emami, J. Models for forecasting hospital bed requirements in the acute sector. J Epidemiol Community Health. 1990, 44, 307–312. [Google Scholar] [CrossRef]
- Altman, D.; Bland, J. ; Uncertainty and sampling error. BMJ. 7064. [Google Scholar] [CrossRef]
- Kaier, K.; Mutters, N.; Frank, U. Bed occupancy rates and hospital-acquired infections—should beds be kept empty? Clinical Microbiology and Infection. 2012, 18(10), 941–945. [Google Scholar] [CrossRef]
- Payne, G.; Laporte, A.; Deber, R.; Coyte, P. Counting backward to health care’s future: Using time-to-death modleing to identify changes in end-of-life morbidity and the impact of aging on health care expenditures. Milbank Q. 2007, 85, 213–257. [Google Scholar] [CrossRef]
- Busse, R.; Krauth, C.; Schwartz, F. Use of acute hospital beds does not increase as the population ages: Results from a seven year cohort study in Germany. J. Epidemiol. Community Health 2002, 56, 289–293. [Google Scholar] [CrossRef]
- Hanlon, P.; Walsh, D.; Whyte, B.; Scott, S.; Lightbody, P.; Gilhooly, M. Hospital use by an ageing cohort: an investigation into the association between biological, behavoural and social risk markers and subsequent hospital utilization. J Public Health Med. 1998, 20(4), 467–476. [Google Scholar] [CrossRef]
- Feudtner, C.; DiGiuseppe, D.; Neff, J. Hospital care for children and young adults in the last year of life: a population-based study. BMC Med. 2003, 1, 3. [Google Scholar] [CrossRef] [PubMed]
- Ananth, P.; Melvin, P.; Feudtner, C.; Wolfe, J.; Berry, J. Hospital Use in the Last Year of Life for Children With Life-Threatening Complex Chronic Conditions. Pediatrics. 2015, 136(5), 938–46. [Google Scholar] [CrossRef] [PubMed]
- PDepartment of Health and Social Care. Palliative and end of life care factsheet: Patterns of care England 2023, Version 4. Published 4 March 2025. Available online: Palliative and end of life care factsheet: Patterns of care, England 2023 (Accessed on 5 March 2025).
- Dixon, T.; Shaw, T.; Frankel, S.; Ebrahim, S. Hospital admissions, age, and death: retrospective cohort study. BMJ. 2004, 328(7451), 1288–1292. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.; Pedroza, C.; Avritscher, E. ; Mosquera,R. ; Tyson, J. Evaluation of negative binomial and zero-inflated negative binomial models for the analysis of zero-inflated count data: application to the telemedicine for children with medical complexity trial. Trials. 2023, 24, 613. [Google Scholar] [CrossRef]
- Zhu, H.; Lakkis, H. Sample size calculation for comparing two negative binomial rates. Statist. Med. 2014, 33, 376–387. [Google Scholar] [CrossRef]
- GBD 2021 Fertility and Forecasting Collaborators. Global fertility in 204 countries and territories, 1950-2021, with forecasts to 2100: a comprehensive demographic analysis for the Global Burden of Disease Study 2021. The Lancet. 2024. [CrossRef]
- Jones, E.; Taylor, B.; Rudge, G.; MacArthur, C.; Jyothish, D.; Simkiss, D.; Cummins, C. Hospitalisation after birth of infants: cross sectional analysis of potentially avoidable admissions across England using hospital episode statistics. BMC Pediatr. 2018, 18, 390. [Google Scholar] [CrossRef]
- Montoro-Pérez, N.; Richart-Martínez, M.; Montejano-Lozoya, R. Factors associated with the inappropriate use of the pediatric emergency department. A systematic review. J Pediatric Nursing. 2023, 69, 38–46. [Google Scholar] [CrossRef]
- Bunting, C.; Clery, A.; McGrath-Lone, L.; Liu, M.; Kendall, S.; Bedford, H.; Cavallaro, F.; Saloniki, E.; Harron, K.; Woodman, J. How does health visiting in the first year of life vary by family characteristics? A longitudinal analysis of administrative data. J Public Health (Oxf). 2025, 47(1), 82–89. [Google Scholar] [CrossRef] [PubMed]
- Greve, P. Pediatrics: A unique and volatile risk. J Healthc Risk Mgmt. 2011, 31, 19–29. [Google Scholar] [CrossRef]
- Roberts, A.; Blunt, I.; Bardsley, M. Distance from home to emergency care. Available online: QualityWatch_FocusOnDistanceFromHomeToEmergencyCare.pdf (Accessed on 25 March 2025).
- Cushing, A.; Bucholz, E.; Chien, A.; Rauch, D.; Michelson, K. Availability of Pediatric Inpatient Services in the United States. Pediatrics. 2021, 148(1), e2020041723. [Google Scholar] [CrossRef] [PubMed]
- UN Inter-agency Group for Child Mortality Estimation (IGME). Available online: CME Info - Child Mortality Estimates (Accessed on 6 May 2025).
- National Centre for Health Statistics. Infant mortality rates by State. Available online: Stats of the States -Infant Mortality (Accessed on 29 April 2025).
- World Bank Group. Hospital beds per 1,000 population. Available online: https://data.worldbank.org/indicator/sh.med.beds.zs (accessed on 11 April 2025).
- NHS England Digital. Hospital admitted patient care activity. Available online: Hospital Admitted Patient Care Activity - NHS England Digital (Accessed on 6 May 2025).
- NHS England. Urgent and emergency care daily situation reports. Available online: Statistics » Urgent and Emergency Care Daily Situation Reports (Accessed on 6 May 2025).
- NHS England. Beds available overnight. Available online: https://www.england.nhs.uk/statistics/statistical-work-areas/bed-availability-and-occupancy-kh03/ (accessed on 5 April 2024).
- Department of Health. Hospital statistics: Inpatient and day case activity. Available online: Hospital statistics: inpatient and day case activity 2023/24 | Department of Health (Accessed on 6 May 2025).
- UNECE. Total live births by sex. Available online: Total Live Births by Sex, Measurement, Country and Year. UNECE Statistical Database (Accessed on 10 May 2025).
- Database earth. Population births in United States of America. Available online: Population Births in United States of America 1950-2025 Future Projections (Accessed on 6 May 2025).
- Arizona Department of Health Services. Population health and vital statistics. Available online: ADHS | Various Health Statistics (Accessed on 9 Mat 2025).
- Hawaii Health. Number of births per year. Available online: Birth Data – Hawai'i Health Data Warehouse(Accessed on 28 April 2025).
- EUROSTAT. Live births (total) by month. Available online: [demo_fmonth] Live births (total) by month (Accessed on 6 May 2025).
- Australian Bureau of Statistics. Births, Australia. Available online: Births, Australia, 2023 | Australian Bureau of Statistics (Accessed on 10 May 2025).
- Office for National Statistics. Deaths occurring by single year of age, by sex, year and month of death, for usual residents of England and Wales: 1993 to 2016. Available online: Deaths occurring by single year of age, by sex, year and month of death, for usual residents of England and Wales: 1993 to 2014 - Office for National Statistics and also Deaths occurring by single year of age, by sex, year and month of death, for usual residents of England and Wales, 2015 to 2016 (Accessed on 6 May 2025).
- Office for National Statistics. Deaths and population estimates by sex and single year of age, England and Wales, 1961 to 2023. Available online: Deaths and population estimates for England and Wales, 1961 to 2023, by single year of age - Office for National Statistics (Accessed on 10 May 2025).
- Australian Institute for Health and Welfare. Average length of stay. Appendix removal. Available online: https://www.aihw.gov.au/hospitals/topics/admitted-patient-care/length-of-stay (accessed on 9 June 2025).
- Wikipedia. List of children’s hospitals in the United States. Available online: List of children's hospitals in the United States - Wikipedia (Accessed on 9 June 2025).
- Personal communication with Dr Kenneth Michelson, Lurie Children’s Hospital, Chicago, USA.
- Texas Health and Human Services. Hospitals: Directory of general and special hospitals. Available online: https://www.hhs.texas.gov/providers/health-care-facilities-regulation/hospitals-general-hospitals (accessed on 12 June 2025).
- Intensive Care Society. Understanding intensive care staffing, occupancy and capacity. Available online: Intensive Care Society | Understanding Intensive Care Staffing, Occupancy and Capacity (Accessed on 29 April 2025).
- DeLia, D. Annual Bed Statistics Give a Misleading Picture of Hospital Surge Capacity. Annals of Emergency Medicine. 2006, 48(4), 384-388.e2. [CrossRef]
- Adams, L. Exploring the Concept of Surge Capacity" OJIN: The Online Journal of Issues in Nursing; 2009, 14(2). T: Exploring the Concept of Surge Capacity | OJIN.
- Riahi, V.; Boyle, J.; Hassanzadeh, H.; Yoon, J.; Diouf, I.; Khanna, S.; Samadbeik, M.; Sullivan, C.; Bosley, E.; Staib, A.; Lind, J. Do Midnight Censuses Accurately Portray Hospital Bed Occupancy? Stud Health Technol Inform. 2024, 24, 318:36–41. [Google Scholar] [CrossRef]
- Hindery, R.; UCSF Epidemiologist Describes Similarities between Swine Flu and 1918 Killer. University of California, 22 September 2009. Available online: https://www.ucsf.edu/news/2009/09/101057/ucsf-epidemiologist-describes-similarities-between-swine-flu-and-1918-killer (accessed on 1 June 2025).
- Wikipedia. List of countries by system of government. Available online: List of countries by system of government - Wikipedia (Accessed on 13 May 2025).
- Brunn, M.; Kratz, T.; Padget, M.; Clément, M.; Smyrl, M. Why are there so many hospital beds in Germany? Health Serv Manage Res. 2023, 36(1), 75–81. [Google Scholar] [CrossRef]
- Tikkanen, R.; Osborn, R.; Mossialos, E.; Djordjevic, A.; Wharton, G.; International health care system profiles; Australia. The Commonwealth Fund, June 5 2020. Available online: Australia | International Health Care System Profiles | Commonwea lth Fund (Accessed on 13 May 2025).
- Australian Institute of Health and Welfare. Health system overview. Available online: https://www.aihw.gov.au/reports/australias-health/health-system-overview (accessed on 5 April 2025).
- Leyenaar, J.; Ralston, S. ; Shieh, M-S. ; Pekow, P.; Mangione-Smith, R.; Lindenauer, P. Epidemiology of pediatric hospitalizations at general hospitals and freestanding children's hospitals in the United States. J. Hosp. Med. 2016, 11, 743–749. [Google Scholar] [CrossRef]
- American Hospital Association. Fast Facts on U.S. hospitals, 2025. Available online: Fast-Facts-on-USHospitals-2025.pdf (Accessed on 26 April 2025).
- National Centre for Health Statistics. State and National Provisional Birth Counts. Available online: https://www.cdc.gov/nchs/nvss/vsrr/provisional-tables.htm (accessed on 26 June 2025).
- United States Census Bureau. County population totals: 2020-2024. Available online: https://www.census.gov/data/datasets/time-series/demo/popest/2020s-counties-total.html.
- Office for National Statistics. Population estimates for the UK, England, Wales, Scotland and Northern Ireland: mid-2023. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/populationandmigration/populationestimates/bulletins/annualmidyearpopulationestimates/mid2023 (accessed on 26 June 2025).
- The Leapfrog Group. State of maternity care in U.S. hospitals. Available online: https://www.leapfroggroup.org/state-maternity-care-us-hospitals-leapfrog-group-2025-report-trends (accessed on 26 June 2025).
- McDaniel, C.; Ralston, D.; Freyleue, S.; Seryozhenkov, E. ; Peled, A,; Amaravadi, H.; Malla, N.; Leyenaar, J. Identifying Inpatient Pediatric Services Across National Datasets. JAMA Netw Open. 2025 Jun 2;8(6):e2513527. [CrossRef]
- Pineda, R,; Knudsen, K. ; Breault, C.; Rogers, E., Ed.; Mack W.; Fernandez-Fernandez, A. NICUs in the US: levels of acuity, number of beds, and relationships to population factors. J Perinatol. 2023, 43(6), 796-805. [Google Scholar] [CrossRef]
- Michelson, K.; Wells, A.; Bucholz, E. National Trends in Pediatric Inpatient Capacity. JAMA Pediatr. 2025, 179(2), 208–209. [Google Scholar] [CrossRef] [PubMed]
- Horvat, C.; Hamilton, M.; Hall, M.; McGuire, J.; Mink, R. Child Health Needs and the Pediatric Critical Care Medicine Workforce: 2020–2040. Pediatrics. 2024, 153 (Suppl 2), e2023063678G. [Google Scholar] [CrossRef]
- Li, J.; Baker, A.; D’Ambrosi, G.; Monuteaux, M. ; Chung. M. A Statewide Assessment of Pediatric Emergency Care Surge Capabilities. Pediatrics 2023, 151 (4), e2022059459. 10.1542/peds. 2022. [Google Scholar]
- McDaniel, C.; Hall, M.; Berry, J. Hospitalization Patterns for Rural-Residing Children from 2002 to 2017. Acad Pediatr. 2025, 25(1), 102554. [Google Scholar] [CrossRef]
- Bongiorno, D.; Ravicz, M.; Nadeau, N.; Michelson, K.; Alpern, E.; Myers, S.; Samuels-Kalow, M. Pediatric capacity crisis: A framework and strategies to prepare for a pediatric surge. JACEP Open. 2024, 5(1), e13093. [Google Scholar] [CrossRef]
- Greenbury, S.; Longford, N. ; Ougham K,; Angelini, E. ; Battersby, C.; Uthaya, S.; Modi, N. Changes in neonatal admissions, care processes and outcomes in England and Wales during the COVID-19 pandemic: a whole population cohort study. BMJ Open 2021, 11, e054410. [Google Scholar] [CrossRef]
- van Hasselt,T. ; Gale, C.; Battersby, C.; On behalf of the United Kingdom Neonatal Collaborative and the Paediatric Critical Care Society Study Group (PCCS-SG), et al. Paediatric intensive care admissions of preterm children born <32 weeks gestation: a national retrospective cohort study using data linkage. Archives of Disease in Childhood - Fetal and Neonatal Edition 2024, 109, 265–271.
- Gamber, R.; Blonsky, H.; McDowell, M.; Lakshminrusimha, S. Declining birth rates, increasing maternal age and neonatal intensive care unit admissions. J Perinatol. 2024, 44(2), 203–208. [Google Scholar] [CrossRef]
- Schwartz, J.; Spix, C.; Wichmann, H.; Malin, E. Air pollution and acute respiratory illness in five German communities. Environ Res. 1991, 56(1), 1–14. [Google Scholar] [CrossRef]
- D'Amato, G.; Annesi-Maesano, I.; Urrutia-Pereira, M.; Del Giacco, S.; Rosario Filho, N.; Chong-Neto, H.; Solé, D.; Ansotegui, I.; et al. Thunderstorm allergy and asthma: state of the art. Multidiscip Respir Med. 2021, 16(1), 806. [Google Scholar] [CrossRef] [PubMed]
- Provenzano, S.; Roth, S.; Sager, L. Air Pollution and Respiratory Infectious Diseases. Environ Resource Econ. 2024, 87, 1127–1139. [Google Scholar] [CrossRef]
- Tran, H.; Tsai, F.; Lee, Y.; Chang, J.; Chang, L.; Chang, T.; Chung, K.; Kuo, H.; Lee, K.; Chuang, K.; Chuang, H. The impact of air pollution on respiratory diseases in an era of climate change: A review of the current evidence. Sci Total Environ. 2023, 898, 166340. [Google Scholar] [CrossRef]
- Traidl-Hoffmann C, Kasche A, Menzel A, Jakob T, Thiel M, Ring J, Behrendt H. Impact of pollen on human health: more than allergen carriers? Int Arch Allergy Immunol. 2003, 131(1), 1–13. [CrossRef] [PubMed]
- Congdon, P. Spatiotemporal Frameworks for Infectious Disease Diffusion and Epidemiology. Int J Environ Res Public Health. 2016, 13(12), 1261. [Google Scholar] [CrossRef]
- Psistaki, K.; Paschalidou, A.; McGregor, G. Weather patterns and all-cause mortality in England, UK. Int J Biometeorol. 2020, 64, 123–136 (2020). [Google Scholar] [CrossRef]
- Paschalidou, A.; Kassomenos, P.; McGregor, G. Analysis of the synoptic winter mortality climatology in five regions of England: Searching for evidence of weather signals. Science Total Environ. 2017, 598, 432–444. [Google Scholar] [CrossRef]
- Vasilevski, V.; Mekonnen, A.; Peeters, A.; et al. Healthcare related barriers and enablers for weight management among pregnant women with overweight and obesity: a rapid scoping review. BMC Pregnancy Childbirth 2025, 25, 252. [Google Scholar] [CrossRef]
- Leddy, M.; Power, M.; Schulkin, J. The impact of maternal obesity on maternal and fetal health. Rev Obstet Gynecol. 2008, 1(4), 170–8. [Google Scholar]
- Godfrey, K.; Reynolds, R.; Prescott, S.; Nyirenda, M.; Jaddoe, V.; Eriksson, J.; Broekman, B. Influence of maternal obesity on the long-term health of offspring. Lancet Diabetes Endocrinol. 2017, 5(1), 53–64. [Google Scholar] [CrossRef] [PubMed]
- WikipediA. COVID-19 lockdown in the United Kingdom. Available online: COVID-19 lockdown in the United Kingdom - Wikipedia (Accessed on 21 April 2025).
- Public Health Scotland. Acute hospital activity and NHS beds information (annual)Year ending 31 March 2024. Available online: https://publichealthscotland.scot/publications/acute-hospital-activity-and-nhs-beds-information-annual/acute-hospital-activity-and-nhs-beds-information-annual-year-ending-31-march-2024/ (accessed on 12 June 2025).
- Romaniuk, A. A three parameter model for birth projections. Population Studies. 1973, 27(3), 467–478. [Google Scholar] [CrossRef] [PubMed]
- McDonald, P.; Kippen, R. Forecasting births. Feature Article, ABS Catalogue Number 2051.0, Australian Bureau of Statistics, Canberra, 2011. Available online: http://www.abs.gov.au/ausstats/abs@.nsf/mf/2051.0 (accessed on 11 April 2025).
- Hosseini, M.; McDonald, P. Projecting births in Iran using a three-parameter model. Available online: www.humanfertility.org/file/getdocument/docs/symposium2/pmcdonald.pdf (accessed on 20 March 2025).
- Shevchuk,P. Reconstruction of birth structure by parity of birth and age of mother in Ukraine in 1995–1998. Demog Social Econ. 2015, 1, 113–125.
- Hoem, J.; Madsen, D.; Nielsen, J. ; Ohlsen, E-M.; Hansen, H.; Rennermalm, B. Experiments in Modelling Recent Danish Fertility Curves. Demography, 1981, 18(2), 231-244.
- José Rafael Caro-Barrera, María de los Baños García-Moreno García & Manuel Pérez-Priego. Projecting Spanish fertility at regional level: A hierarchical Bayesian approach. PLOS ONE. 2022, 17(10), e0275492.
- Srivastava, U.; Singh, K.; Pandey, A.; Narayan, N. Experiments in modeling recent Indian fertility pattern. Scientific Reports. 2021, 11, 1. [Google Scholar] [CrossRef] [PubMed]
- Bobak, M.; Gjonca, A. The seasonality of live birth is strongly influenced by socio-demographic factors, Human Reproduction 2001, 16(7), 1512–1517. [CrossRef]
- Dahlberg, J.; Andersson, G. Changing seasonal variation in births by sociodemographic factors: a population-based register study, Human Reproduction Open. 2018,2018(4), hoy015. [CrossRef]
- Rojansky, N.; Brzezinski, A.; Schenker, J. Seasonality in human reproduction: an update, Human Reproduction. 1992, 7(6), 735–745. [CrossRef]
- Lowell, W.; Davis, G. The light of life: Evidence that the sun modulates human lifespan. Medical Hypotheses. 208, 70(3), 501-507. [CrossRef]
- Martinez, M. The calendar of epidemics: Seasonal cycles of infectious diseases. PLoS Pathog. 2018; 14(11), e1007327. [CrossRef]
- Hillier, D.; Parry, G.; Shannon, M.; Stack, A. The Effect of Hospital Bed Occupancy on Throughput in the Pediatric Emergency Department. Ann Emerg Med. 2009, 53(6), 767-776 e3. [CrossRef]
- Clarke, A. Why are we trying to reduce length of stay? Evaluation of the costs and benefits of reducing time in hospital must start from the objectives that govern change. Qual Health Care. 1996, 5(3), 172–179. [Google Scholar] [CrossRef]
- Taheri, P.; Butz, D.; Greenfield, L. Length of stay has minimal impact on the cost of hospital admission. J Amer Coll Surgeons 2000, 191(2), 123–130. [Google Scholar] [CrossRef]
- Evans, J.; Kobewka, D.; Thavorn, K.; D'Egidio, G.; Rosenberg, E.; Kyeremanteng, K. The impact of reducing intensive care unit length of stay on hospital costs: evidence from a tertiary care hospital in Canada. Can J Anaesth. 2018, 65(6), 627–635. [Google Scholar] [CrossRef]
- Dranove, D. Economies of scale in non-revenue producing cost centers: Implications for hospital mergers. J Health Econ, 1998, 17(1), 69-83. [CrossRef]
- Giancotti, M.; Guglielmo, A.; Mauro, M. Efficiency and optimal size of hospitals: Results of a systematic search. PLoS One. 2017, 12(3), e0174533. [Google Scholar] [CrossRef]
- Beulieu, N.; Hoicks, A.; Chernew, M. Hospital Capital Expenditures Associated With Prices And Hospital Expansion Or Withering, 2010–19. Health Affairs. 2025; 44. [Google Scholar] [CrossRef]
- McRae, S.; Brunner, J.; Bard, J. Analyzing economies of scale and scope in hospitals by use of case mix planning. Health Care Manag Sci. 2020, 23(1), 80–101. [Google Scholar] [CrossRef]
- Freeman, M.; Savva, M.; Scholtes, S. Economies of Scale and Scope in Hospitals: An Empirical Study of Volume Spillovers. Management Science. 2021, 67(2), 673–697. [Google Scholar] [CrossRef]
- Møller, J.; Sørensen, M.; Hardahl, C. Prediction of risk of acquiring urinary tract infection during hospital stay based on machine-learning: A retrospective cohort study. PLOS ONE 2021, 16(3), e0248636. [Google Scholar] [CrossRef] [PubMed]
- Aguilera, C.; Kalam, K.; Chesney, K.; Donoho, D. The Relationship Between Procedural Volume, Hospital Quality, and Postoperative Mortality in Pediatric Neurosurgery: Review of the literature. World Neurosurgery, 2024, 182, e764–e771. [Google Scholar] [CrossRef]
- Husk, K.; Berry, V.; Tozer, R.; Skipwith, G.; Radmore, R.; Ball, S.; Ukoumunne, O.; Logan, S. Interventions for reducing unplanned paediatric admissions: an observational study in one hospital: BMJ Paediatrics Open 2018;2:e000235.
- Jyotsna, K.; Sharan, S.; Kishore, S.; Prakash, J. The Various Scoring Systems in Pediatric Intensive Care Units: A Prospective Observational Study. Cureus. 2023, 15(5), e39679. [Google Scholar] [CrossRef]
- Gold, D.; Mihalov, L.; Cohen, D. Evaluating the Pediatric Early Warning Score (PEWS) System for Admitted Patients in the Pediatric Emergency Department. Acad Emerg Med. 2014, 21(11), 1249–1256. [Google Scholar] [CrossRef] [PubMed]
- ÓhAiseadha’, C.; Mannix, M.; Saunders, J.; Philip, R. Bed Utilisation in an Irish Regional Paediatric Unit - A Cross-Sectional Study Using the Paediatric Appropriateness Evaluation Protocol (PAEP). Int J Health Policy Manag. 2016, 5(11), 643–652. [Google Scholar] [CrossRef]
- Harper, J.; Coyle, A.; Tam, C.; Skakum, M.; Ragheb, M.; Wilson, L.; Lê, M.; Klassen, T.; Aregbesola, A. Readiness of emergency departments for pediatric patients and pediatric mortality: a systematic review. CMAJ Open. 2023, 11(5), E956–E968. [Google Scholar] [CrossRef]
- Laposata, M. Diagnostic error in the United States: A summary of the report of a national Academy of medicine Committee. Trans Am Clin Climatol Assoc. 2022, 132, 194–201. [Google Scholar]
- Waltraud, F.; Vilen, L.; Konitzer, M. Diagnoses by general practitioners: Accuracy and reliability. International Journal of Forecasting. 209, 25(4), 784-793. [CrossRef]
- Yoon, H.; Gerdes, L.; Beigel, F.; Sun, Y.; Kövilein, J.; Wang, J.; Kuhlmann, T.; Flierl-Hecht, A. ; Haller, D, et al. Multiple sclerosis and gut microbiota: Lachnospiraceae from the ileum of MS twins trigger MS-like disease in germfree transgenic mice-An unbiased functional study. Proc Natl Acad Sci U S A. 2025, 122(18), e2419689122. [CrossRef]
- Liu, Y.; Johnston, C.; Jarousse, N.; Fletcher, S.; Iqbal, S. Association between herpes simplex virus type 1 and the risk of Alzheimer’s disease: a retrospective case–control study. BMJ Open. 2025, 15, e093946. [Google Scholar] [CrossRef]
- Nemeth, K.; Bayraktar, R.; Ferracin, M.; et al. Non-coding RNAs in disease: from mechanisms to therapeutics. Nat Rev Genet. 2024, 25, 211–232. [Google Scholar] [CrossRef]
- Loganathan, T.; Doss, C. Non-coding RNAs in human health and disease: potential function as biomarkers and therapeutic targets. Functional & integrative genomics. 2023, 23(1), 33.
- Li, C.; Ni, Y.; Xu, H.; Xiang, Q.; Zhao, Y.; Zhan, J.; He, J.; Li, S.; Liu, Y. Roles and mechanisms of exosomal non-coding RNAs in human health and diseases. Signal transduction and targeted therapy. 2021, 6(1), 383. [Google Scholar] [CrossRef] [PubMed]
- Bhatti GK, Khullar N, Sidhu IS, Navik US, Reddy AP, Reddy PH, Bhatti JS. Emerging role of non-coding RNA in health and disease. Metabolic brain disease. 2021, 36, 1119–1134.
- Paloviita, P.; Vuoristo, S. The non-coding genome in early human development – Recent advancements. Seminars in Cell & Developmental Biology. 2022, 131, 4–13. [Google Scholar] [CrossRef]
- González-Moyotl, N. , Huesca-Gómez, C. , Torres-Paz, Y.E. et al. Paediatrics congenital heart disease is associated with plasma miRNAs. Pediatr Res. 2024, 96, 1220–1227. [Google Scholar] [CrossRef]
- Tingö, L; Ahlberg, E; Johansson, L; Pedersen, S. ; Chawla, K.; Sætrom, P.; Cione, E.; Simpson, M. Non-coding RNAs in human breast milk: a systematic review. Frontiers in immunology. 2021, 12, 725323.
- Liang, J.; Liu, X.; Chen, X.; Song, X.; Li, W.; Huang, Y. Emerging roles of non-coding RNAs in childhood asthma. Frontiers in Pharmacology. 2022 ;13:856104. 17 May.
- Zhang, X.; Zhang, X.; Feng, S.; Wang, X.; Guo, B.; Liu, J.; Xu, D.; Liu, F. The Specific microRNA Profile and Functional Networks for Children with Allergic Asthma. J Asthma Allergy. 2022, 15, 1179–1194. [Google Scholar] [CrossRef] [PubMed]
- Wang, P.; Zhang, H.; Zhao, W.; Dai, N. Silencing of long non-coding RNA KCNQ1OT1 alleviates LPS-induced lung injury by regulating the miR-370-3p/FOXM1 axis in childhood pneumonia. BMC Pulmonary Medicine. 2021, 21, 1–3. [Google Scholar] [CrossRef]
- Li, S.; Cui, H.; Lu, H.; Zheng, S.; Yuan, C. Advances in noncoding RNA in children allergic rhinitis. International Forum of Allergy & Rhinology 2024, 14(8), 1350-1362.
- Zhang, S.; Gao, J.; Liu, C. The Role of Non-Coding RNAs in Neurodevelopmental Disorders. Front Genet. 2019, 20(10), 1033. [Google Scholar] [CrossRef]
- Chen, S.; Deng, X.; Sheng, H.; Rong, Y.; Zheng, Y.; Zhang, Y.; Lin, J. Noncoding RNAs in pediatric brain tumors: Molecular functions and pathological implications. Mol Ther Nucleic Acids. 2021, 26, 417–431. [Google Scholar] [CrossRef]
- Wang, Q.; Zhao, C.; Du, Q.; et al. Non-coding RNA in infantile hemangioma. Pediatr Res 2024, 96, 1594–1602. [Google Scholar] [CrossRef]
- Pathania, A.; Prathipati, P.; Pandey, M.; Byrareddy, S.; Coulter, D.; Gupta, S.; Challagundla, K. The emerging role of non-coding RNAs in the epigenetic regulation of pediatric cancers. Semin Cancer Biol. 2022, 83, 227–241. [Google Scholar] [CrossRef]
- Pasławska M, Grodzka A, Peczyńska J, Sawicka B, Bossowski AT. Role of miRNA in Cardiovascular Diseases in Children-Systematic Review. Int J Mol Sci. 2024, 25(2), 956. https, //doi.org/10.3390/ijms25020956.
- Wang, H.; Wu, X.; Chen, Y.; Hou, F.; Zhu, K.; Jiang, Q.; Xiao, P.; Zhang, Q. ; Xiang, Z; Fan, Y. ; Xie, X.; Li, L; Song, R. Combining multi-omics approaches to prioritize the variant-regulated functional long non-coding RNAs in autism spectrum disorder. Asian J Psychiatr. 2023, 80, 103357. [Google Scholar] [CrossRef]
- Salloum-Asfar, S.; Elsayed, A.; Elhag, S.; Abdulla, S. Circulating non-coding RNAs as a signature of autism spectrum disorder symptomatology. International Journal of Molecular Sciences. 2021, 22(12), 6549. [Google Scholar] [CrossRef] [PubMed]
- Maligianni, I.; Yapijakis, C.; Bacopoulou, F.; Chrousos, G. The potential role of exosomes in child and adolescent obesity. Children. 2021, 8(3), 196. [Google Scholar] [CrossRef] [PubMed]
- Drury, R.; Pollard, A.; O'Connor, D. The effect of H1N1 vaccination on serum miRNA expression in children: A tale of caution for microRNA microarray studies. PLoS One. 2019, 14(8), e0221143. [Google Scholar] [CrossRef] [PubMed]
- Zhou, R.; Joshi, P.; Katsushima, K.; Liang, W.; Liu, W.; Goldenberg, N.; Dover, G.; Perera, R. The Emerging Field of Noncoding RNAs and Their Importance in Pediatric Diseases. J Pediatr. 2020, 221S, S11–S19. [Google Scholar] [CrossRef]
- McKee, M. What are the lessons learnt by countries that have had dramatic reductions of their hospital bed capacity? World Health Organization Regional Office for Europe, Copenhagen, Denmark (2003) 21 pp.
- Bhattacharjee, N. ; Global fertility in 204 countries and territories, 1950–2021, with forecasts to 2100: a comprehensive demographic analysis for the Global Burden of Disease Study 2021. The Lancet. 2024, 403(10440), 2057 – 2099. [CrossRef]
- Wells, J.; Shah, A.; Gillis, H.; Gustafson, S.; Powell, C.; Krasaelap, A.; Hanna, S.; Hoefert, J.; Bigelow, A.; et al. Tiny patients, huge impact: a call to action. Front Public Health. 2024, 12, 1423736. [Google Scholar] [CrossRef]
- Bai G, Zare H. Hospital Cost Structure and the Implications on Cost Management During COVID-19. J Gen Intern Med. 2020 Sep;35(9):2807-2809. doi: 10.1007/s11606-020-05996-8.Mechanic, R. Implementing Administrative Benchmarks In The Medicare Shared Savings Program: Opportunities and Challenges. Health Affairs: Forefront 2025, 10.1377/forefront.20250522.694566.
- First Focus on Children. U.S. child poverty in 2023. Available online: https://poverty.ucdavis.edu/faq/what-current-poverty-rate-united-states#:~:text=The%20official%20poverty%20rate%20is%2011.1%20percent%2C%20based,rate%20nor%20the%20number%20differed%20significantly%20from%202022. (accessed on 2 July 2025).
- Ryan, A.; Whaley, C.; Brown, E.; Radhakrishnan, E.; Murray, R. Rhode Island’s Affordability Standards Led to Hospital Price Reductions and Lower Insurance Premiums. Health Affairs 2025, 44(5), 597–605. [Google Scholar] [CrossRef]
- Mechanic, R. Implementing administrative benchmarks in the Medicare shared savings program: Opportunities and challenges. Health Affairs. 2025. [CrossRef]
- Ahyow, L.; Lambert, P.; Jenkins, D.; Neal, K.; Tobin, M. Bed Occupancy Rates and Hospital-Acquired Clostridium difficile Infection: A Cohort Study. Infection Control & Hospital Epidemiology. 2013, 34(10), 1062-1069. [CrossRef]

| Consultant Specialty | Proportion children |
|---|---|
| Dental Medicine Specialties | 50% |
| Sports & Exercise Medicine | 60% |
| Clinical Genetics | 71% |
| Clinical Neurophysiology | 75% |
| Orthodontics | 79% |
| Special Care Dentistry | 82% |
| Audiological Medicine | 92% |
| Paediatric Cardiology | 92% |
| Surgical Dentistry | 95% |
| Paediatric Surgery | 99% |
| Paediatric Neurology | 99% |
| Paediatric Dentistry | 100% |
| Paediatrics | 100% |
| Year | Average occupied beds |
|---|---|
| 2020/21 | 13.2 |
| 2023/24 | 14.9 |
| 2021/22 | 16.1 |
| 2017/18 | 18.5 |
| 2019/20 | 18.5 |
| 2024/25 | 18.7 |
| 2013/14 | 18.8 |
| 2022/23 | 19.1 |
| 2015/16 | 19.4 |
| 2018/19 | 19.7 |
| 2014/15 | 20.0 |
| 2016/17 | 21.6 |
| Year | Admissions | Admissions (13+ days) | Occ-upied Beds | Occupied Beds (13+ days) | LOS | LOS (13+ days) | % 0 day |
|---|---|---|---|---|---|---|---|
| Year 1 | 4079 | 61 | 24.5 | 4.8 | 2.2 | 28.6 | 19% |
| Year 2 | 3644 | 63 | 24.1 | 6.8 | 2.4 | 39.2 | 22% |
| Year 3 | 4147 | 44 | 22.7 | 4.0 | 2.0 | 33.0 | 24% |
| Year 4 | 3207 | 35 | 18.7 | 4.2 | 2.1 | 43.5 | 24% |
| Year 5 | 3354 | 44 | 19.7 | 3.9 | 2.1 | 32.3 | 21% |
| Year 6 | 3610 | 56 | 21.0 | 5.0 | 2.1 | 32.7 | 27% |
| Average | 3674 | 50.5 | 21.8 | 4.8 | 2.2 | 34.9 | 23% |
|
STDEV as % |
378 (±10%) | 11.1 (±22%) | 2.4 (±11%) | 1.1 (±23%) | 0.1 (±5%) | 5.5 (±16%) | 3% (±13%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).