Submitted:
17 June 2025
Posted:
18 June 2025
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Materials and Methods
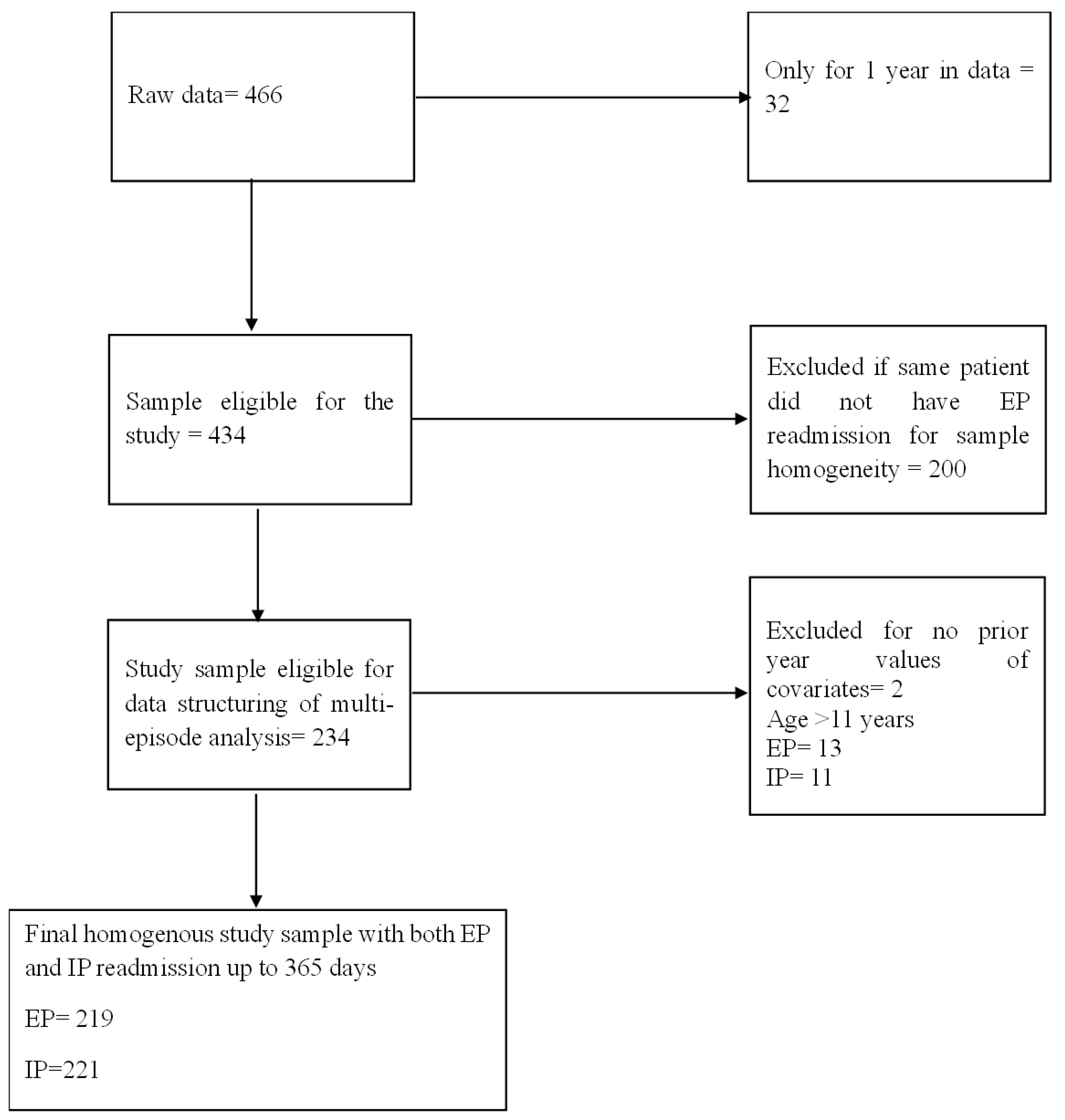
2.1. Study Design and Population
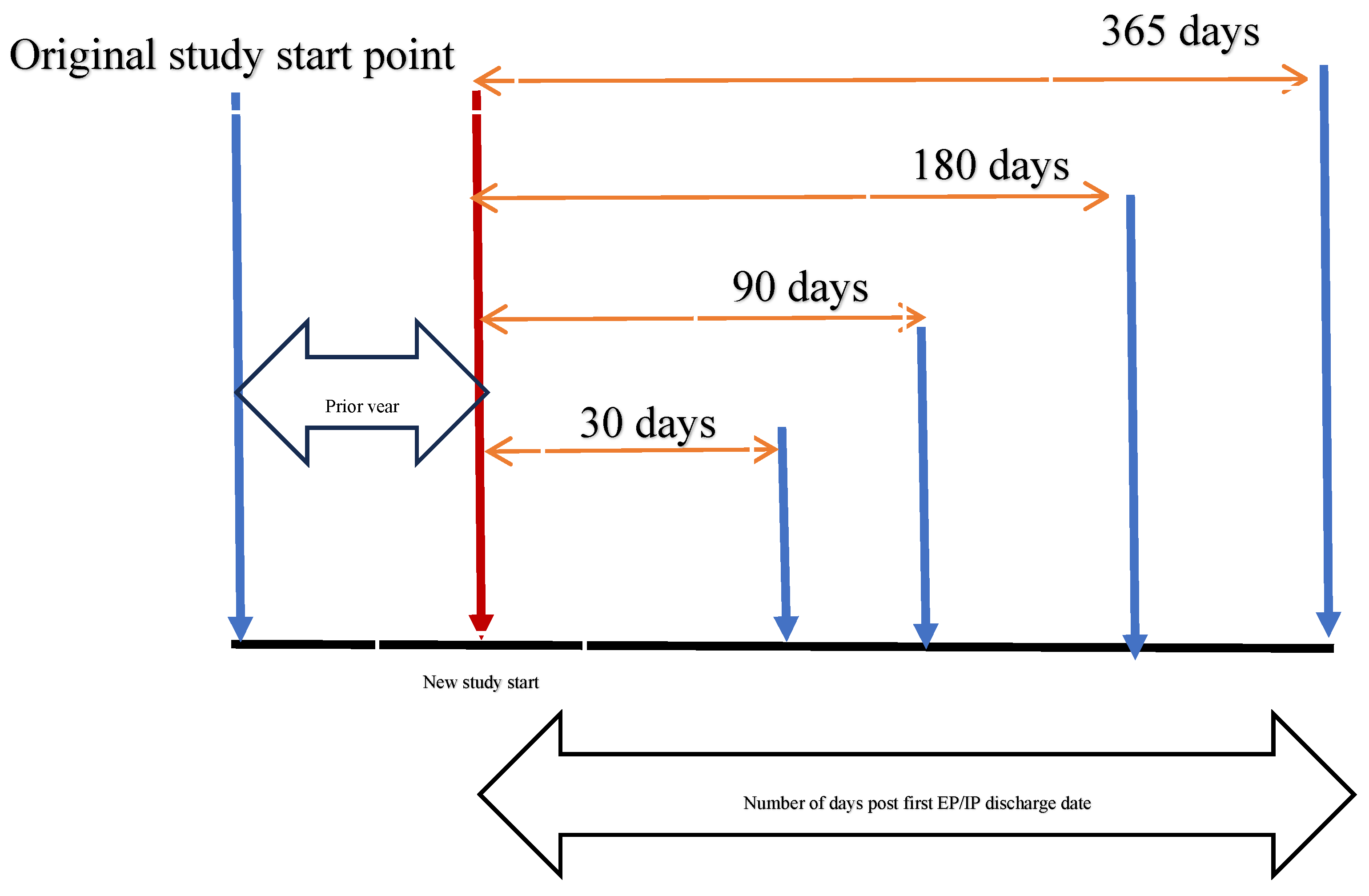
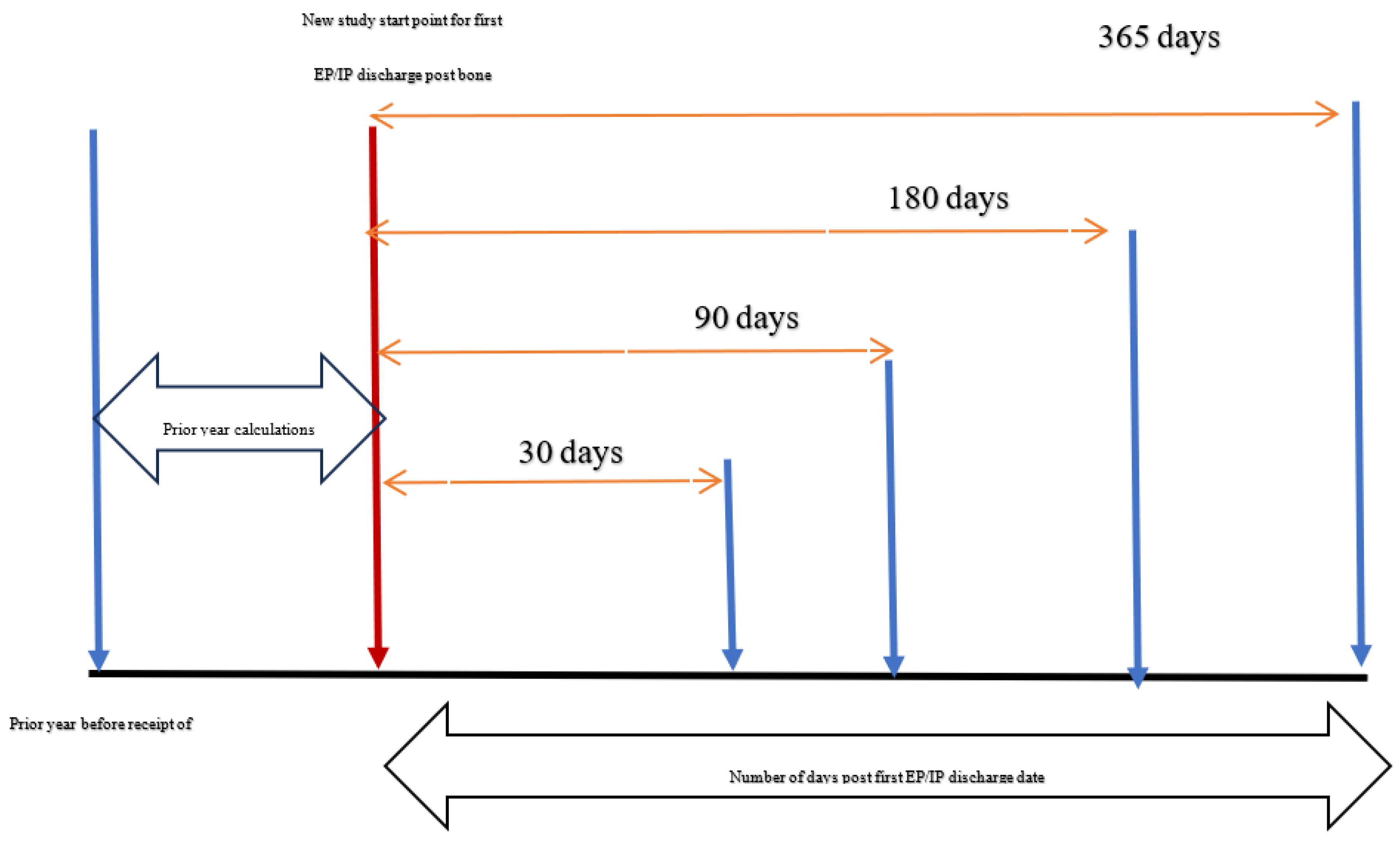
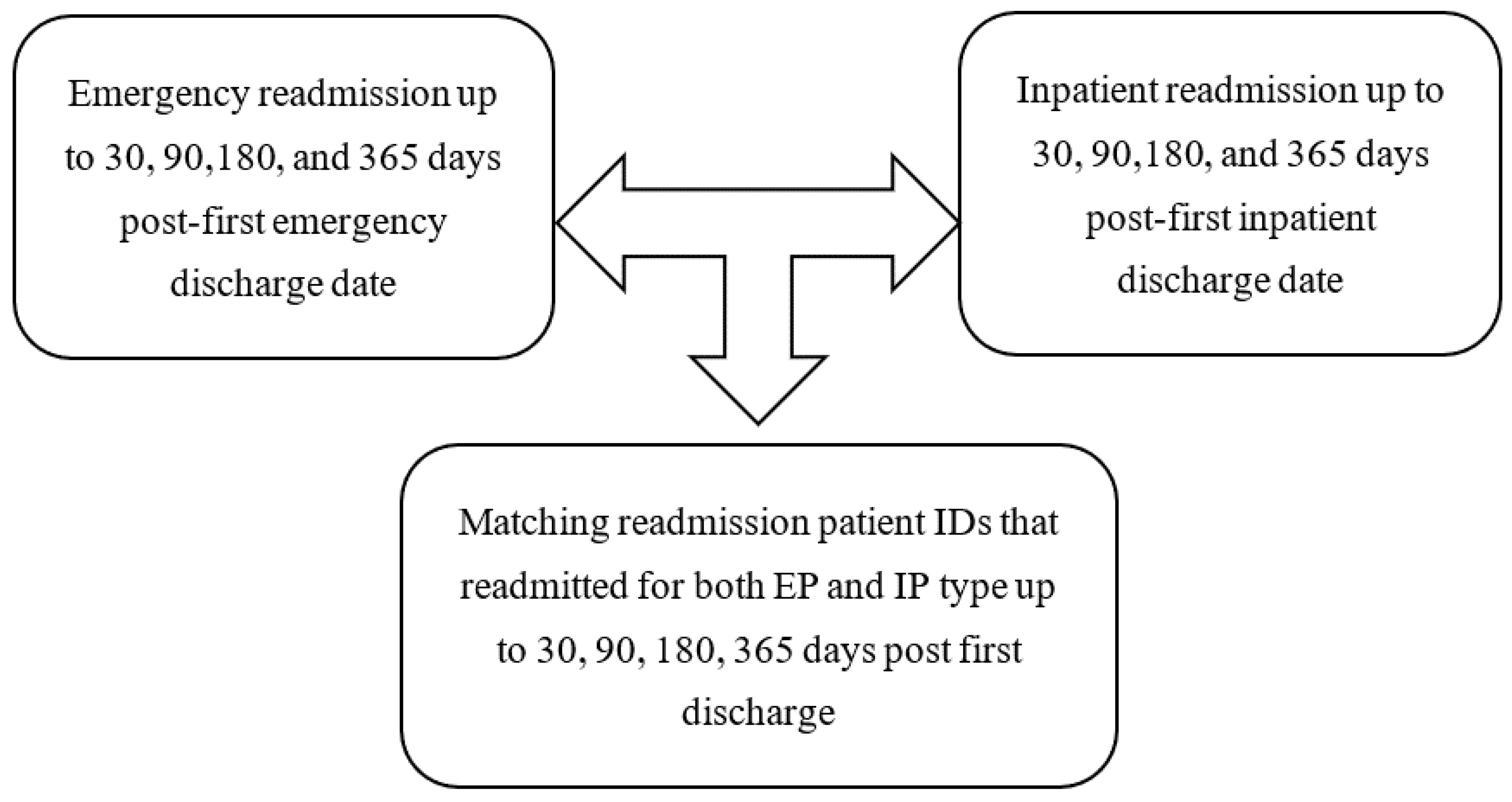
2.2. Data and Data Structure
2.3. Multi-Episode Survival Analysis
2.4. Empirical and Conceptual Model
2.5. Outcome Variable
2.6. Independent Variable
2.7. Covariates
3. Results
3.1. Descriptive Statistics
3.2. Emergency Readmission
3.3. Inpatient Readmission
3.4. Hazards of Emergency Readmission
3.5. Hazards of Inpatient Readmission
4. Discussion
5. Policy Implications
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Diallo, A. B.; Seck, M.; Touré, S. A.; Keita, M.; Bousso, E. S.; Faye, B. F.; Diop, S. Prevalence and Predictive Factors of Sickle Cell Emergencies Readmission in the Clinical Hematology Department of Dakar, Senegal. Anemia, 2024, 2024 (1), 7143716. [CrossRef]
- Kumar, V.; Chaudhary, N.; Achebe, M. M. Epidemiology and Predictors of All-Cause 30-Day Readmission in Patients with Sickle Cell Crisis. Sci Rep, 2020, 10 (1), 2082. [CrossRef]
- Weiss, A. J.; Jiang, H. J. Overview of Clinical Conditions With Frequent and Costly Hospital Readmissions by Payer, 2018. Healthcare Cost and Utilization Project (HCUP) Statistical Briefs, 2021.
- Santiago, L. H.; Vargas, R. B.; Pipolo, D. O.; Pan, D.; Tiwari, S.; Dehghan, K.; Bazargan-Hejazi, S. Predictors of Hospital Readmissions in Adult Patients with Sickle Cell Disease. Am J Blood Res, 2023, 13 (6), 189. [CrossRef]
- Ford, S.; Parikh, J.; Gundala, A.; Vuong, C.; Subramaniam, A.; Hensley, E.; Fernandez, O.; Shah, N. Exploring Differences in Hospital Readmissions in Patients with Sickle Cell Disease By Examining Patterns with MHealth-Acquired Pain and Physiologic Data. Blood, 2024, 144 (Supplement 1), 3898–3898. [CrossRef]
- Santiago, L. H.; Vargas, R. B.; Pipolo, D. O.; Pan, D.; Tiwari, S.; Dehghan, K.; Bazargan-Hejazi, S. Predictors of Hospital Readmissions in Adult Patients with Sickle Cell Disease. Am J Blood Res, 2023, 13 (6), 189. [CrossRef]
- Zuair, A. Bin; Aldossari, S.; Alhumaidi, R.; Alrabiah, M.; Alshabanat, A. The Burden of Sickle Cell Disease in Saudi Arabia: A Single-Institution Large Retrospective Study. Int J Gen Med, 2023, 16, 161. [CrossRef]
- Cronin, R. M.; Hankins, J. S.; Byrd, J.; Pernell, B. M.; Kassim, A.; Adams-Graves, P.; Thompson, A.; Kalinyak, K.; DeBaun, M.; Treadwell, M. Risk Factors for Hospitalizations and Readmissions among Individuals with Sickle Cell Disease: Results of a U.S. Survey Study. Hematology, 2019, 24 (1), 189. [CrossRef]
- Ballas, S. K.; Lusardi, M. Hospital Readmission for Adult Acute Sickle Cell Painful Episodes: Frequency, Etiology, and Prognostic Significance. Am J Hematol, 2005, 79 (1), 17–25. [CrossRef]
- Alshabanat, A.; Alrabiah, M.; Zuair, A. Bin; Aldossari, S.; Alhumaidi, R. A. Predictive Factors for 30-Day Readmission and Increased Healthcare Utilization in Sickle Cell Disease Patients: A Single-Center Comparative Retrospective Study. Int J Gen Med, 2024, 17, 2065. [CrossRef]
- Weissman, J. S.; Ayanian, J. Z.; Chasan-Taber, S.; Sherwood, M. J.; Roth, C.; Epstein, A. M. Hospital Readmissions and Quality of Care. Med Care, 1999, 37 (5), 490–501. [CrossRef]
- Frei-Jones, M. J.; Field, J. J.; DeBaun, M. R. Multi-Modal Intervention and Prospective Implementation of Standardized Sickle Cell Pain Admission Orders Reduces 30-Day Readmission Rate. Pediatr Blood Cancer, 2009, 53 (3), 401. [CrossRef]
- Hussaini, Z. A. Al; Kanhal, R. Al; Ebrahaimi, F. Al; Shalhoub, M. Al; Asmari, B. Al; Othman, F. Management of Sickle Cell Disease Patients Presenting to the Emergency Department with Vaso-Occlusive Crisis: A Retrospective Study. Int J Res Med Sci, 2024, 12 (1), 8–16. [CrossRef]
- Rushing, M.; Horiuchi, S.; Zhou, M.; Kavanagh, P. L.; Reeves, S. L.; Snyder, A.; Paulukonis, S. Emergency Department 30-Day Emergency Department Revisits among People with Sickle Cell Disease: Variations in Characteristics. Pediatr Blood Cancer, 2024, 71 (10), e31188. [CrossRef]
- Brodsky, M. A.; Rodeghier, M.; Sanger, M.; Byrd, J.; McClain, B.; Covert, B.; Roberts, D. O.; Wilkerson, K.; DeBaun, M. R.; Kassim, A. A. Risk Factors for 30-Day Readmission in Adults with Sickle Cell Disease. American Journal of Medicine, 2017, 130 (5), 601.e9-601.e15. [CrossRef]
- Ramadan, M.; Alnashri, Y.; Ilyas, A.; Batouk, O.; Alsheikh, K. A.; Alhelabi, L.; Alghnam, S. A. Assessment of Opioid Administration Patterns Following Lower Extremity Fracture among Opioid-Naïve Inpatients: Retrospective Multicenter Cohort Study. Ann Saudi Med, 2022, 42 (6), 366–376. [CrossRef]
- Tawhari, M.; Alhamadh, M.; Alhabeeb, A.; Ureeg, A.; Alghnam, S.; Alhejaili, F.; Alnasser, L. A.; Sayyari, A. Establishing the Kidney DIsease in the National GuarD (KIND) Registry: An Opportunity for Epidemiological and Clinical Research in Saudi Arabia. BMC Nephrol, 2024, 25 (1), 1–11. [CrossRef]
- Amorim, L. D. A. F.; Cai, J. Modelling Recurrent Events: A Tutorial for Analysis in Epidemiology. Int J Epidemiol, 2015, 44 (1), 324–333. [CrossRef]
- Trujols, J.; Guàrdia, J.; Peró, M.; Freixa, M.; Siñol, N.; Tejero, A.; Pérez de los Cobos, J. Multi-Episode Survival Analysis: An Application Modelling Readmission Rates of Heroin Dependents at an Inpatient Detoxification Unit. Addictive Behaviors, 2007, 32 (10), 2391–2397. [CrossRef]
- Liu, S. W.; Singer, S. J.; Sun, B. C.; Camargo, C. A. A Conceptual Model for Assessing Quality of Care for Patients Boarding in the Emergency Department: Structure-Process-Outcome. Acad Emerg Med, 2011, 18 (4), 430. [CrossRef]
- Bejanyan, N.; Bolwell, B. J.; Lazaryan, A.; Rybicki, L.; Tench, S.; Duong, H.; Andresen, S.; Sobecks, R.; Dean, R.; Pohlman, B.; et al. Risk Factors for 30-Day Hospital Readmission Following Myeloablative Allogeneic Hematopoietic Cell Transplantation (Allo-HCT). Biology of Blood and Marrow Transplantation, 2012, 18 (6), 874–880. [CrossRef]
- Shulman, D. S.; London, W. B.; Guo, D.; Duncan, C. N.; Lehmann, L. E. Incidence and Causes of Hospital Readmission in Pediatric Patients after Hematopoietic Cell Transplantation. Biology of Blood and Marrow Transplantation, 2015, 21 (5), 913–919. [CrossRef]
- Sora, F.; Chiusolo, P.; Laurenti, L.; Innocenti, I.; Autore, F.; Giammarco, S.; Metafuni, E.; Alma, E.; Di Giovanni, A.; Sica, S.; et al. Days Alive Outside Hospital and Readmissions in Patients Undergoing Allogeneic Transplants from Identical Siblings or Alternative Donors. Mediterr J Hematol Infect Dis, 2020, 12 (1), e2020055. [CrossRef]
- Spring, L.; Li, S.; Soiffer, R. J.; Antin, J. H.; Alyea, E. P.; Glotzbecker, B. Risk Factors for Readmission after Allogeneic Hematopoietic Stem Cell Transplantation and Impact on Overall Survival. Biology of Blood and Marrow Transplantation, 2015, 21 (3), 509–516. [CrossRef]
- Debaun, M. R.; Frei-Jones, M. J.; Field, J. J. Risk Factors for Hospital Readmission within 30-Days: A New Quality Measure for Children with Sickle Cell Disease. Pediatr Blood Cancer, 2009, 52 (4), 481. [CrossRef]
- Cronin, R. M.; Hankins, J. S.; Byrd, J.; Pernell, B. M.; Kassim, A.; Adams-Graves, P.; Thompson, A.; Kalinyak, K.; DeBaun, M.; Treadwell, M. Risk Factors for Hospitalizations and Readmissions among Individuals with Sickle Cell Disease: Results of a U.S. Survey Study. Hematology, 2019, 24 (1), 189. [CrossRef]
- Kidwell, K.; Albo, C.; Pope, M.; Bowman, L.; Xu, H.; Wells, L.; Barrett, N.; Patel, N.; Allison, A.; Kutlar, A. Characteristics of Sickle Cell Patients with Frequent Emergency Department Visits and Hospitalizations. PLoS One, 2021, 16 (2), e0247324. [CrossRef]
- Krumholz, H. M.; Wang, K.; Lin, Z.; Dharmarajan, K.; Horwitz, L. I.; Ross, J. S.; Drye, E. E.; Bernheim, S. M.; Normand, S.-L. T. Hospital-Readmission Risk — Isolating Hospital Effects from Patient Effects. New England Journal of Medicine, 2017, 377 (11), 1055–1064. [CrossRef]
- Singh, S.; Lin, Y. L.; Nattinger, A. B.; Kuo, Y. F.; Goodwin, J. S. Variation in Readmission Rates by Emergency Departments and Emergency Department Providers Caring for Patients After Discharge. J Hosp Med, 2015, 10 (11), 705. [CrossRef]
| Patient ID | Treatment | Tstart | Tstop | Status | Age | Prior year crisis episodes | Prior year total emergency visits | Other study covariates |
|---|---|---|---|---|---|---|---|---|
| 1 | 0 | 0 | 90 | 0 | 5 | 15 | 37 | |
| 2 | 1 | 0 | 45 | 1 | 9 | 4 | 12 | |
| 3 | 1 | 0 | 50 | 1 | 2 | 20 | 23 | |
| 3 | 1 | 50 | 75 | 1 | 2 | 20 | 23 | |
| 3 | 1 | 75 | 90 | 0 | 2 | 20 | 23 | |
| 4 | 0 | 0 | 10 | 1 | 6 | 2 | 40 | |
| 4 | 0 | 10 | 30 | 0 | 6 | 2 | 40 |
| Emergency type readmission | ||||
|---|---|---|---|---|
| Mean | SD | Min | Max | |
| Age | 5.86 | 2.70 | 1.58 | 11 |
| Prior year | ||||
| Total crisis episodes | 1.82 | 3.35 | 0 | 24 |
| Total complications | 0.33 | 0.54 | 0 | 2 |
| Prior year visits | ||||
| Total prior year OP visits | 8.12 | 8.21 | 0 | 75 |
| Total prior year EP visits | 1.64 | 3.17 | 0 | 37 |
| Total prior year IP visits | 2.29 | 3.48 | 0 | 34 |
| Seasonal visits | ||||
| Total Spring | 0.84 | 1.39 | 0.00 | 17 |
| Total Summer | 0.52 | 0.75 | 0.00 | 4 |
| Total Autumn | 0.74 | 0.92 | 0.00 | 6 |
| Total nurses and physicians | 37956.21 | 19722.60 | 17185 | 73635 |
| N | 234 | |||
| Emergency type readmission | |||
|---|---|---|---|
| Frequency | Percent | Cumulative | |
| Medication | |||
| No Hydroxy Urea | 41 | 17.5% | 17.5 |
| Hydroxy Urea | 193 | 82.5% | 100.0 |
| CCI score | |||
| 0 | 221 | 94.4% | 94.4 |
| 1 | 13 | 5.6% | 100.0 |
| Region | |||
| Central | 101 | 43.2% | 43.2 |
| East | 83 | 35.5% | 78.6 |
| West & South | 50 | 21.4% | 100.0 |
| Healthcare facility | |||
| AHSA | 43 | 2.1% | 18.38 |
| IABFH | 38 | 18.0% | 34.62 |
| KAMC-J | 52 | 1.3% | 56.84 |
| KAMC-R | 97 | 22.7% | 98.29 |
| PMBAH | 4 | 36.8% | 100 |
| Gender | |||
| Female | 101 | 43.2% | 43.2 |
| Male | 133 | 56.8% | 100.0 |
| Treatment | |||
| No Bone Marrow | 205 | 87.6% | 87.61 |
| Bone Marrow | 29 | 12.4% | 100 |
| N | 234 | ||
| Inpatient type readmission | ||||
|---|---|---|---|---|
| Mean | SD | Min | Max | |
| Age | 5.86 | 2.70 | 1.58 | 11 |
| Prior year | ||||
| Total crisis episodes | 1.53 | 2.41 | 0 | 16 |
| Total complications | 0.33 | 0.54 | 0 | 2 |
| Prior year visits | ||||
| Total prior year OP visits | 7.15 | 4.54 | 0 | 30 |
| Total prior year EP visits | 1.33 | 1.70 | 0 | 8 |
| Total prior year IP visits | 2.29 | 3.48 | 0 | 34 |
| Seasonal visits | ||||
| Total Spring | 0.81 | 1.03 | 0.00 | 7 |
| Total Summer | 0.62 | 0.85 | 0.00 | 5 |
| Total Autumn | 0.78 | 0.85 | 0.00 | 4 |
| Total nurses and physicians | 37956.21 | 19722.60 | 17185 | 73635 |
| N | 234 | |||
| Inpatient type readmission | |||
|---|---|---|---|
| Frequency | Percent | Cumulative | |
| Medication | |||
| No Hydroxy Urea | 41 | 17.5% | 17.5 |
| Hydroxy Urea | 193 | 82.5% | 100.0 |
| CCI score | |||
| 0 | 221 | 94.4% | 94.4 |
| 1 | 13 | 5.6% | 100.0 |
| Region | |||
| Central | 101 | 43.2% | 43.2 |
| East | 83 | 35.5% | 78.6 |
| West & South | 50 | 21.4% | 100.0 |
| Healthcare facility | |||
| AHSA | 43 | 18.4% | 18.38 |
| IABFH | 38 | 16.2% | 34.62 |
| KAMC-J | 52 | 22.2% | 56.84 |
| KAMC-R | 97 | 41.5% | 98.29 |
| PMBAH | 4 | 1.7% | 100 |
| Gender | |||
| Female | 101 | 43.2% | 43.2 |
| Male | 133 | 56.8% | 100.0 |
| Treatment | |||
| No Bone Marrow | 205 | 87.6% | 87.61 |
| Bone Marrow | 29 | 12.4% | 100 |
| N | 234 | ||
| Days post first Emergency discharge | ||||
|---|---|---|---|---|
| 30 | 90 | 180 | 365 | |
| Hazards ratio (95% CI) | Hazards ratio (95% CI) | Hazards ratio (95% CI) | Hazards ratio (95% CI) | |
| Treatment: Reference is Bone Marrow | ||||
| Control | 1.017 | 2.637 | 4.56*** | 6.38*** |
| (0.24-4.25) | (0.72-9.36) | (1.65-12.57) | (2.26-18.01) | |
| CCI scores: Reference is 0 | ||||
| 1 | 2.734 | 1.102 | 0.774 | 0.853 |
| (0.58-12.79) | (0.27-4.53) | (0.24-2.51) | (0.31-2.31) | |
| Total complications | 0.79 | 1.6 | 1.95*** | 2.02*** |
| (0.32-1.94) | (0.90-2.83) | (1.30-2.93) | (1.40-2.89) | |
| Healthcare Facility name: Reference KAMC-R | ||||
| AHSA | 0.508 | 0.98 | 0.927 | 1.157 |
| (0.13-2.05) | (0.29-3.32) | (0.29-3.00) | (0.44-3.05) | |
| IABFH | 0.24* | 0.529 | 0.46 | 0.752 |
| (0.05-1.24) | (0.15-1.82) | (0.14-1.46) | (0.31-1.80) | |
| PMBAH | 0.00*** | 1.834 | 1.883 | 2.127 |
| (0.00-0.01) | (0.22-15.02) | (0.31-11.52) | 0.58-7.85) | |
| KAMCJ | 1.525 | 1.842 | 1.027 | 1.027 |
| (0.30-7.83) | (0.51-6.59) | (0.24-4.47) | (0.25-4.23) | |
| Total prior year emergency visits | 0.963 | 1.19** | 1.11* | 1.15*** |
| (0.73-1.28) | (1.01-1.40) | (0.10-1.24) | (1.05-1.26) | |
| Seasons of Readmission visit | ||||
| Spring | 1.213 | 0.805 | 0.944 | 0.876 |
| (0.30-4.88) | (0.38-1.70) | (0.50-1.78) | (0.50-1.55) | |
| Summer | 1.19 | 0.786 | 0.753 | 0.783 |
| (0.28-5.02) | (0.37-1.68) | (0.40-1.43) | (0.44-1.40) | |
| Autumn | 0.947 | 0.44* | 0.59* | 0.62* |
| (0.26-3.47) | (0.20-1.00) | (0.31-1.10) | (0.36-1.07) | |
| Medication: No Hydroxyurea | ||||
| Hydroxyurea | 0.93 | 1.449 | 1.75* | 1.492 |
| (0.34-2.55) | (0.62-3.40) | (0.92-3.32) | (0.87-2.56) | |
| Total prior year crisis episodes | 0.95 | 0.86* | 1.001 | 0.998 |
| (0.77-1.17) | (0.73-1.00) | (0.91-1.10) | (0.91-1.10) | |
| Gender:Reference is Female | ||||
| Male | 1.574 | 1.509 | 1.289 | 1.24 |
| (0.75-3.32) | (0.91-2.51) | (0.88-1.90) | (0.88-1.75) | |
| Regions of Saudi Arabia: Central | ||||
| East | 1.161 | 1.72 | 2.14 | 1.737 |
| (0.13-10.35) | (0.32-9.30) | (0.53-8.62) | (0.56-5.42) | |
| West and South | 0.363 | 0.555 | 0.934 | 0.894 |
| (0.04-3.07) | (0.12-2.57) | (0.19-4.52) | (0.21-3.89) | |
| Age | 0.976 | 1.012 | 1.019 | 0.99 |
| (0.84-1.13) | (0.92-1.12) | (0.94-1.10) | (0.92-1.06) | |
| Total prior year IP visits | 0.991 | 0.966 | 0.938 | 0.927 |
| (0.83-1.19) | (0.85-1.10) | (0.85-1.04) | (0.85-1.01) | |
| Total prior year OP visits | 0.93* | 0.956 | 0.98 | 0.988 |
| (0.86-1.00) | (0.90-1.01) | (0.94-1.02) | (0.95-1.03) | |
| Total nurses and physicians | 1 | 1 | 1.00** | 1.00** |
| (1.00-1.00) | (1.00-1.00) | (1.00-1.00) | (1.00-1.00) | |
| N | 215 | 216 | 216 | 215 |
| p value: *** 1%, ** 5%, *10% | ||||
| Inpatient Department Visits Rate of readmissions | |||||
|---|---|---|---|---|---|
| Days post first Inpatient discharge | |||||
| 30 | 90 | 180 | 365 | ||
| Hazards ratio (95% CI) | Hazards ratio (95% CI) | Hazards ratio (95% CI) | Hazards ratio (95% CI) | ||
| Treatment: Reference is Bone Marrow | |||||
| Control | 0.06*** | 0.14*** | 0.13*** | 0.18*** | |
| (0.01-0.24) | (0.06-0.31) | (0.07-0.26) | (0.09-0.33) | ||
| CCI scores: Reference is 0 | |||||
| 1 | 1.129 | 1.142 | 0.762 | 0.693 | |
| (0.21-6.19) | (0.42-3.11) | (0.27-2.14) | (0.24-1.96) | ||
| Total complications | 0.604 | 0.696 | 0.795 | 0.895 | |
| (0.22-1.65) | (0.39-1.24) | (0.52-1.21) | (0.62-1.29) | ||
| Healthcare Facility name: Reference KAMC-R | |||||
| AHSA | 5.879 | 1.665 | 2.426 | 2.343 | |
| (0.54-63.48) | (0.49-5.70) | (0.71-8.23) | (0.81-6.78) | ||
| IABFH | 5.636 | 1.397 | 2.399 | 1.963 | |
| (0.43-74.12) | (0.37-5.22) | (0.73-7.93) | (0.71-5.46) | ||
| PMBAH | 0.00*** | 0.00*** | 0*** | 0 | |
| (0.00-0.01) | (0.00-0.01) | (0.00-0.01) | (0.00-0.01) | ||
| KAMCJ | 9.90*** | 2.50** | 2.43* | 2.56** | |
| (1.80-54.30) | (1.06-5.91) | (0.97-6.08) | (1.22-5.40) | ||
| Total prior year emergency visits | 1.166 | 1.129 | 1.16** | 1.14** | |
| (0.81-1.67) | (0.95-1.35) | (1.01-1.33) | (1.01-1.29) | ||
| Seasons of Readmission visit | |||||
| Spring | 0.262 | 0.38** | 0.607 | 0.843 | |
| (0.05-1.48) | (0.16-0.90) | (0.33-1.12) | (0.52-1.37) | ||
| Summer | 1.005 | 1.339 | 1.289 | 1.165 | |
| (0.31-3.26) | (0.67-2.67) | (0.70-2.37) | (0.69-1.97) | ||
| Autumn | 0.695 | 0.671 | 0.827 | 0.776 | |
| (0.23-2.13) | (0.33-1.36) | (0.46-1.47) | (0.46-1.30) | ||
| Medication: No Hydroxyurea | |||||
| Hydroxyurea | 0.593 | 1.065 | 0.986 | 1.048 | |
| (0.14-2.47) | (0.47-2.40) | (0.55-1.77) | (0.65-1.70) | ||
| Total prior year crisis episodes | 1.064 | 1.003 | 0.969 | 0.989 | |
| (0.81-1.40) | (0.88-1.14) | (0.87-1.08) | (0.90-1.08) | ||
| Gender:Reference is Female | |||||
| Male | 0.779 | 0.833 | 0.894 | 0.895 | |
| (0.35-1.75) | (0.50-1.37) | (0.60-1.32) | (0.64-1.26) | ||
| Regions of Saudi Arabia: Central | |||||
| East | 0.244 | - | 0.30* | 0.47 | |
| (0.01-8.71) | - | (0.09-1.08) | (0.15-1.45) | ||
| West and South | 0.265 | - | 0.504 | 0.42* | |
| (0.02-3.10) | - | (0.17-1.46) | (0.17-1.04) | ||
| Age | 0.94 | 0.994 | 0.98 | 0.959 | |
| (0.78-1.14) | (0.90-1.10) | (0.90-1.06) | (0.89-1.03) | ||
| Total prior year IP visits | 1.043 | 1.10* | 1.11** | 1.11*** | |
| (0.86-1.26) | (1.00-1.21) | (1.02-1.20) | (1.03-1.20) | ||
| Total prior year OP visits | 1.032 | 1.033 | 1.035 | 1.023 | |
| (0.90-1.18) | (0.94-1.13) | (0.97-1.11) | (0.96-1.09) | ||
| Total nurses and physicians | 1 | 1 | 1 | 1 | |
| (1.00-1.00) | (1.00-1.00) | (1.00-1.00) | (1.00-1.00) | ||
| N | 220 | 219 | 220 | 221 | |
| p value: *** 1%, ** 5%, *10% | |||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




