Submitted:
06 June 2025
Posted:
09 June 2025
You are already at the latest version
Abstract
Keywords:
Introduction
Material and Methods
Routine Malaria Data
Geospatial Covariate Data
DHS Variables and Processing
Remotely Sensed Variables
Catchment Population
Computation of Travel Time
Treatment-Seeking Population
Overlapping Catchment Areas
Covariate Extraction
Incidence Model
Model Structure
Dasymetric Disaggregation
Results
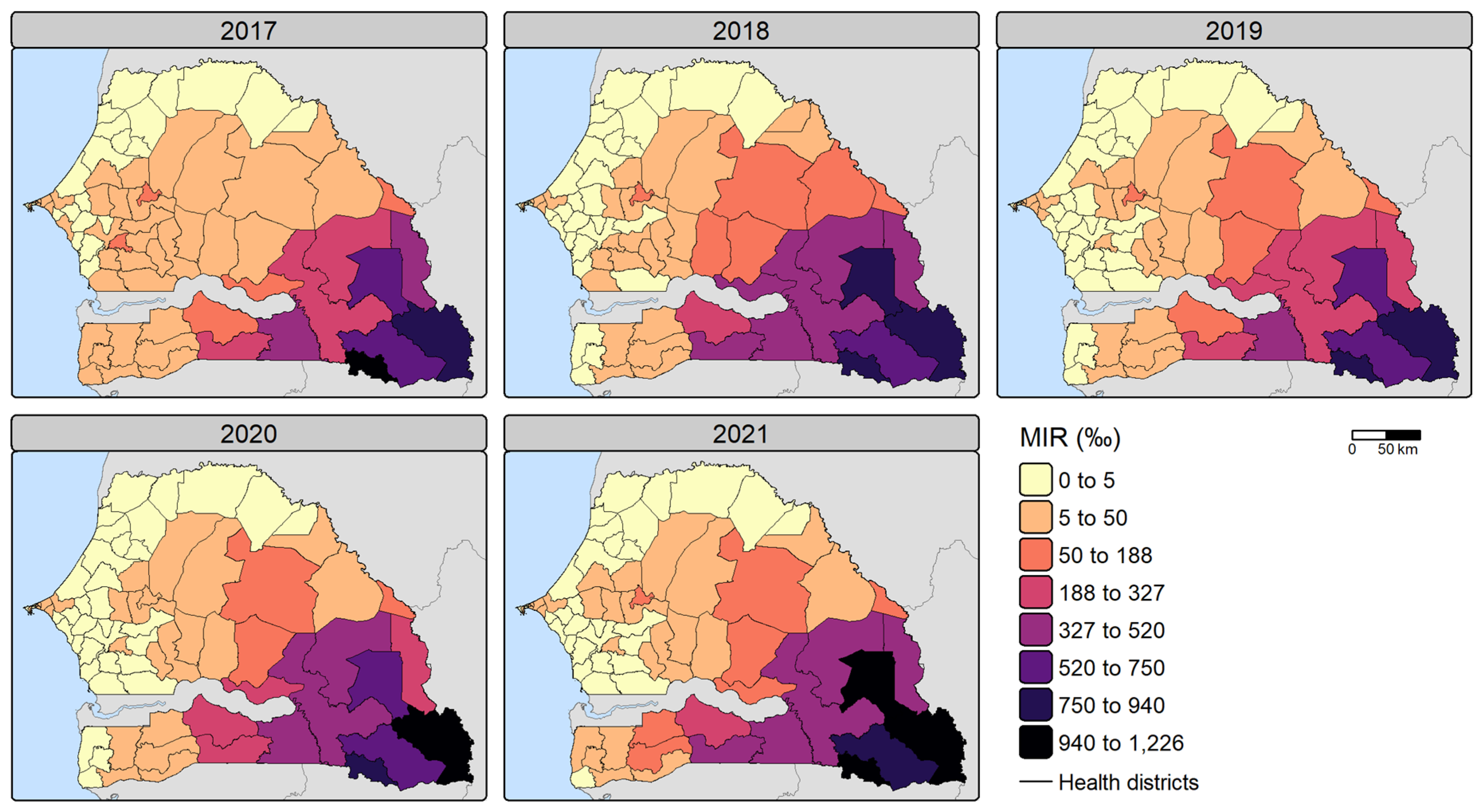
Observed Malaria Incidence
Covariate Selection
Posterior Estimates
Model Parameters
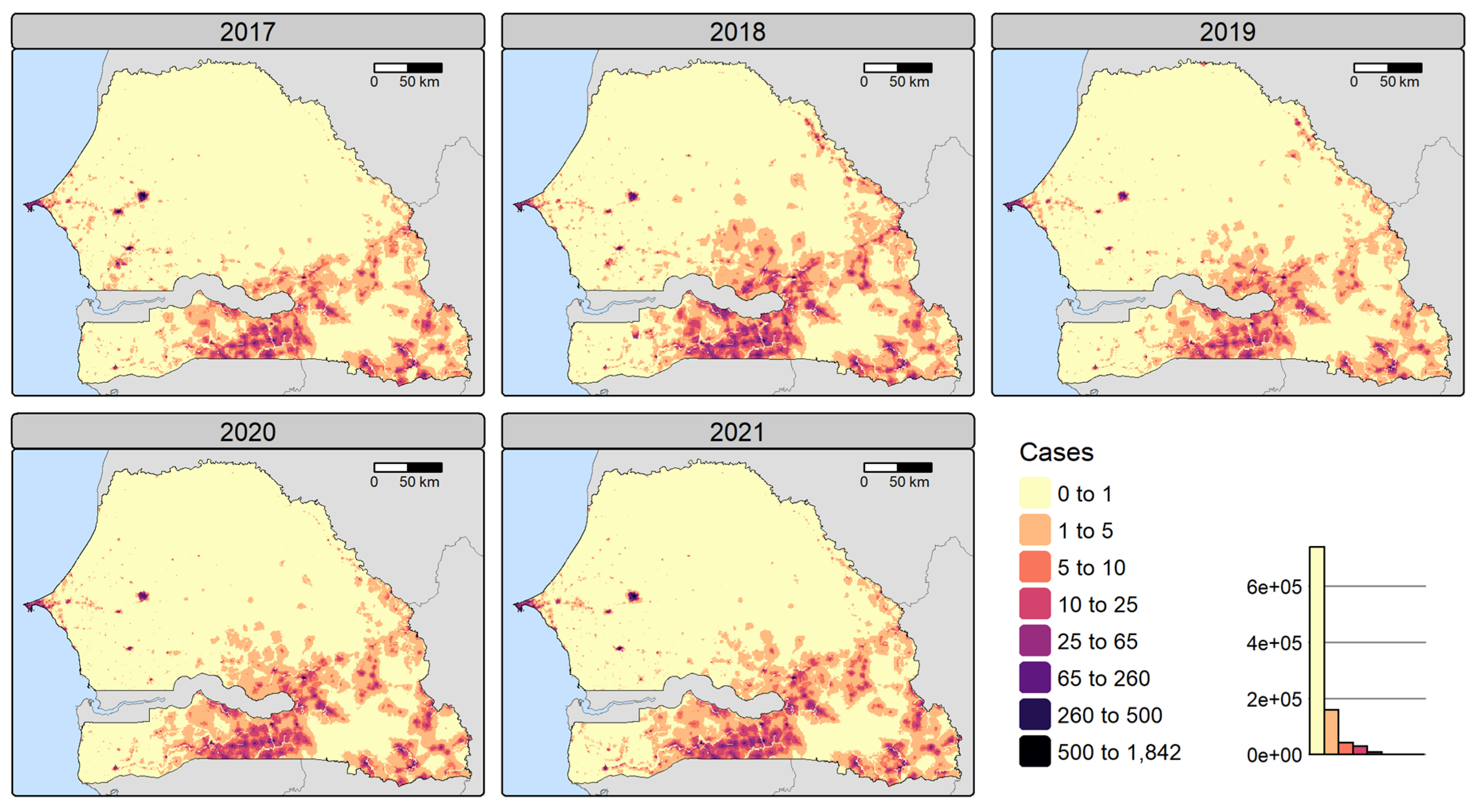
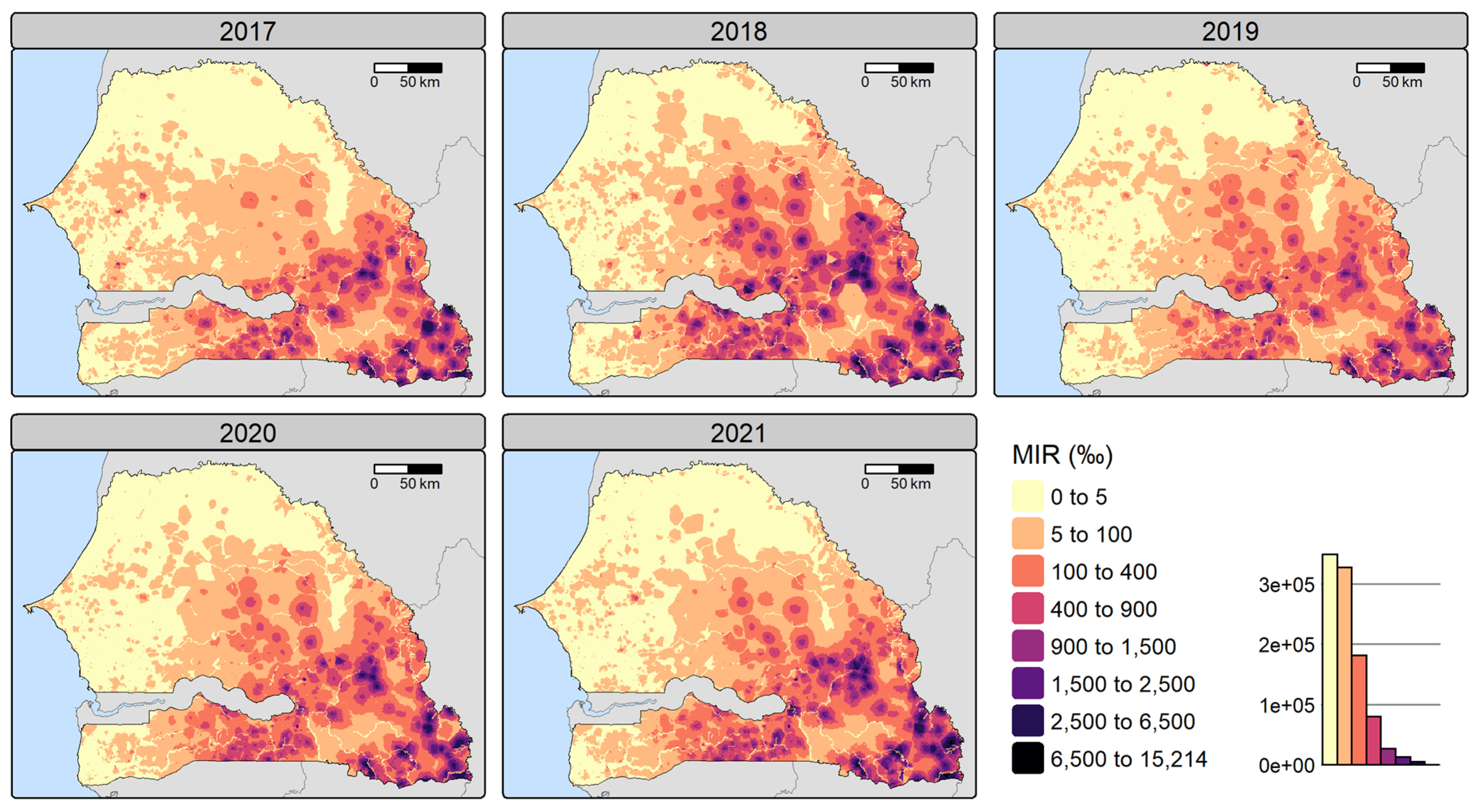
Posterior Malaria Incidence
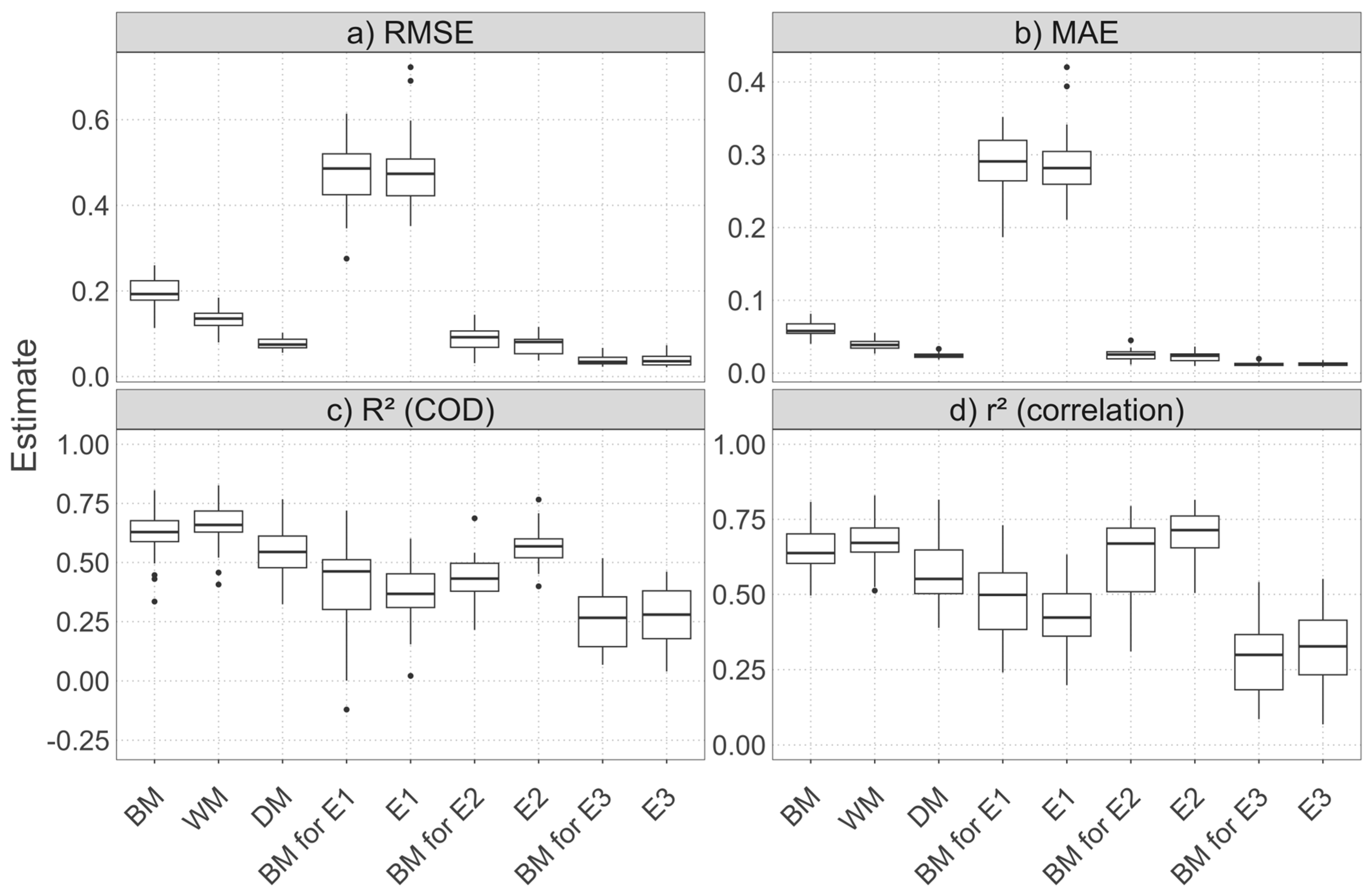
Cross-Validation Performance
Dasymetric Disaggregation
Discussion
Risk Factors Vary by Transmission Level
Temporal Trends in Malaria in Senegal
Spatial Patterns and Fine-Scale Risk Maps
Limitations
Strengths
Supplementary Materials
References
- World Health Organization. World malaria report 2023. Geneva: World Health Organization; 2023.
- Strategic Advisory Group on Malaria Eradication. Malaria eradication: benefits, future scenarios and feasibility. A report of the Strategic Advisory Group on Malaria Eradication. Geneva: World Health Organization; 2020.
- Shretta R, Liu J, Cotter C, Cohen J, Dolenz C, Makomva K, et al. Malaria Elimination and Eradication. In: Holmes KK, Bertozzi S, Bloom BR, Jha P, editors. Major Infectious Diseases. 3rd ed. Washington (DC): The International Bank for Reconstruction and Development / The World Bank; 2017.
- Ndiath M, Faye B, Cisse B, Ndiaye JL, Gomis JF, Dia AT, et al. Identifying malaria hotspots in Keur Soce health and demographic surveillance site in context of low transmission. Malar J. 2014 Nov 24;13(1):453. [CrossRef]
- World Health Organization. Global technical strategy for malaria 2016-2030. Geneva: World Health Organization; 2015. Available online: https://iris.who.int/handle/10665/176712.
- United Nations. Global indicator framework for the Sustainable Development Goals and targets of the 2030 Agenda for Sustainable Development. 2023.
- Aheto JMK. Mapping under-five child malaria risk that accounts for environmental and climatic factors to aid malaria preventive and control efforts in Ghana: Bayesian geospatial and interactive web-based mapping methods. Malar J. 2022 Dec 15;21(1):384. [CrossRef]
- Aheto JMK, Duah HO, Agbadi P, Nakua EK. A predictive model, and predictors of under-five child malaria prevalence in Ghana: How do LASSO, Ridge and Elastic net regression approaches compare? Prev Med Rep. 2021 Sep 1;23:101475. [CrossRef]
- Semakula M, Niragire F, Faes C. Spatio-Temporal Bayesian Models for Malaria Risk Using Survey and Health Facility Routine Data in Rwanda. Int J Environ Res Public Health. 2023 Feb 28;20(5):4283. [CrossRef]
- Adigun AB, Gajere EN, Oresanya O, Vounatsou P. Malaria risk in Nigeria: Bayesian geostatistical modelling of 2010 malaria indicator survey data. Malar J. 2015 Apr 14;14(1):156. [CrossRef]
- Ibeji JU, Mwambi H, Iddrisu AK. Bayesian spatio-temporal modelling and mapping of malaria and anaemia among children between 0 and 59 months in Nigeria. Malar J. 2022 Nov 1;21(1):311. [CrossRef]
- Ejigu BA. Geostatistical analysis and mapping of malaria risk in children of Mozambique. Carvalho LH, editor. PLOS ONE. 2020 Nov 9;15(11):e0241680. [CrossRef]
- Giardina F, Franke J, Vounatsou P. Geostatistical modelling of the malaria risk in Mozambique: effect of the spatial resolution when using remotely-sensed imagery. Geospatial Health [Internet]. 2015 Nov 26;10(2). [CrossRef]
- Giardina F, Gosoniu L, Konate L, Diouf MB, Perry R, Gaye O, et al. Estimating the Burden of Malaria in Senegal: Bayesian Zero-Inflated Binomial Geostatistical Modeling of the MIS 2008 Data. PLOS ONE. 2012 Mar 5;7(3):e32625. [CrossRef]
- Ssempiira J, Kissa J, Nambuusi B, Mukooyo E, Opigo J, Makumbi F, et al. Interactions between climatic changes and intervention effects on malaria spatio-temporal dynamics in Uganda. Parasite Epidemiol Control. 2018 Aug;3(3):e00070. [CrossRef]
- Ssempiira J, Nambuusi B, Kissa J, Agaba B, Makumbi F, Kasasa S, et al. Geostatistical modelling of malaria indicator survey data to assess the effects of interventions on the geographical distribution of malaria prevalence in children less than 5 years in Uganda. PLOS ONE. 2017 Apr 4;12(4):e0174948. [CrossRef]
- Bennett A, Yukich J, Miller JM, Keating J, Moonga H, Hamainza B, et al. The relative contribution of climate variability and vector control coverage to changes in malaria parasite prevalence in Zambia 2006–2012. Parasit Vectors. 2016 Aug 5;9(1):431. [CrossRef]
- Taylor BM, Andrade-Pacheco R, Sturrock H, Hamainza B, Silumbe K, Miller J, et al. Malaria Risk Mapping Using Routine Health System Incidence Data in Zambia. arXiv; 2021. [CrossRef]
- Danwang C, Khalil É, Achu D, Ateba M, Abomabo M, Souopgui J, et al. Fine scale analysis of malaria incidence in under-5: hierarchical Bayesian spatio-temporal modelling of routinely collected malaria data between 2012-2018 in Cameroon. Sci Rep. 2021 Jun 1;11. [CrossRef]
- Cleary E, Hetzel MW, Siba PM, Lau CL, Clements ACA. Spatial prediction of malaria prevalence in Papua New Guinea: a comparison of Bayesian decision network and multivariate regression modelling approaches for improved accuracy in prevalence prediction. Malar J. 2021 Jun 13;20(1):269. [CrossRef]
- McMahon A, Mihretie A, Ahmed AA, Lake M, Awoke W, Wimberly MC. Remote sensing of environmental risk factors for malaria in different geographic contexts. Int J Health Geogr. 2021 Jun 13;20(1):28. [CrossRef]
- Asori M, Musah A, Odei J, Morgan AK, Zurikanen I. Spatio-temporal assessment of hotspots and seasonally adjusted environmental risk factors of malaria prevalence. Appl Geogr. 2023 Nov 1;160:103104. [CrossRef]
- Rousseau R. A geographical perspective on ticks and associated disease risk in Belgium. Université cathologique de Louvain; 2023.
- Hagenlocher M, Kienberger S, Lang S, Blaschke T. Implications of Spatial Scales and Reporting Units for the Spatial Modelling of Vulnerability to Vector-Borne Diseases. In 2014. p. 197–206.
- Openshaw S. The modifiable areal unit problem. In: Concepts and Techniques in Modern Geography. Norwhich: Geo Books; 1984.
- Ijumba JN, Lindsay SW. Impact of irrigation on malaria in Africa: paddies paradox. Med Vet Entomol. 2001 Mar;15(1):1–11. [CrossRef]
- Boyce MR, Katz R, Standley CJ. Risk Factors for Infectious Diseases in Urban Environments of Sub-Saharan Africa: A Systematic Review and Critical Appraisal of Evidence. Trop Med Infect Dis. 2019 Sep 29;4(4):123. [CrossRef]
- Morlighem C, Chaiban C, Georganos S, Brousse O, Van Lipzig NPM, Wolff E, et al. Spatial Optimization Methods for Malaria Risk Mapping in Sub-Saharan African Cities Using Demographic and Health Surveys. GeoHealth. 2023 Oct;7(10):e2023GH000787. [CrossRef]
- Morlighem C, Chaiban C, Georganos S, Brousse O, Van de Walle J, van Lipzig NPM, et al. The Multi-Satellite Environmental and Socioeconomic Predictors of Vector-Borne Diseases in African Cities: Malaria as an Example. Remote Sens. 2022 Jan;14(21):5381. [CrossRef]
- Mitchell CL, Ngasala B, Janko MM, Chacky F, Edwards JK, Pence BW, et al. Evaluating malaria prevalence and land cover across varying transmission intensity in Tanzania using a cross-sectional survey of school-aged children. Malar J. 2022 Mar 9;21(1):80. [CrossRef]
- Bates I, Fenton C, Gruber J, Lalloo D, Lara AM, Squire SB, et al. Vulnerability to malaria, tuberculosis, and HIV/AIDS infection and disease. Part 1: determinants operating at individual and household level. Lancet Infect Dis. 2004 May;4(5):267–77. [CrossRef]
- Cairns ME, Walker PGT, Okell LC, Griffin JT, Garske T, Asante KP, et al. Seasonality in malaria transmission: implications for case-management with long-acting artemisinin combination therapy in sub-Saharan Africa. Malar J. 2015 Aug 19;14(1):321. [CrossRef]
- Birkmann J, Cardona OD, Carreño ML, Barbat AH, Pelling M, Schneiderbauer S, et al. Framing vulnerability, risk and societal responses: the MOVE framework. Nat Hazards. 2013 Jun;67(2):193–211. [CrossRef]
- Croft TN, Marshall AMJ, Allen CK. Guide to DHS Statistics 7. Rockville, Maryland, USA: ICF International; 2018.
- Sturrock HJW, Bennett AF, Midekisa A, Gosling RD, Gething PW, Greenhouse B. Mapping Malaria Risk in Low Transmission Settings: Challenges and Opportunities. Trends Parasitol. 2016;32(8):635–45. [CrossRef]
- Yekutiel P. Problems of epidemiology in malaria eradication. Bull World Health Organ. 1960;22(6):669–83.
- Ozodiegwu ID, Ambrose M, Battle KE, Bever C, Diallo O, Galatas B, et al. Beyond national indicators: adapting the Demographic and Health Surveys’ sampling strategies and questions to better inform subnational malaria intervention policy. Malar J. 2021 Mar 1;20(1):122. [CrossRef]
- Alegana VA, Okiro EA, Snow RW. Routine data for malaria morbidity estimation in Africa: challenges and prospects. BMC Med. 2020 Jun 3;18(1):121. [CrossRef]
- Arambepola R, Keddie SH, Collins EL, Twohig KA, Amratia P, Bertozzi-Villa A, et al. Spatiotemporal mapping of malaria prevalence in Madagascar using routine surveillance and health survey data. Sci Rep. 2020 Oct 22;10(1):18129. [CrossRef]
- Epstein A, Namuganga JF, Nabende I, Kamya EV, Kamya MR, Dorsey G, et al. Mapping malaria incidence using routine health facility surveillance data in Uganda. BMJ Glob Health. 2023 May 1;8(5):e011137. [CrossRef]
- Kang SY, Amratia P, Dunn J, Vilay P, Connell M, Symons T, et al. Fine-scale maps of malaria incidence to inform risk stratification in Laos. Malar J. 2024 Jun 25;23(1):196. [CrossRef]
- Alegana VA, Atkinson PM, Lourenço C, Ruktanonchai NW, Bosco C, Erbach-Schoenberg E zu, et al. Advances in mapping malaria for elimination: fine resolution modelling of Plasmodium falciparum incidence. Sci Rep. 2016 Jul 13;6(1):29628. [CrossRef]
- Stevens FR, Gaughan AE, Linard C, Tatem AJ. Disaggregating Census Data for Population Mapping Using Random Forests with Remotely-Sensed and Ancillary Data. PLOS ONE. 2015 févr;10(2):e0107042. [CrossRef]
- Yankey O, Utazi CE, Nnanatu CC, Gadiaga AN, Abbot T, Lazar AN, et al. Disaggregating census data for population mapping using a Bayesian Additive Regression Tree model. Appl Geogr. 2024 Nov 1;172:103416. [CrossRef]
- PNLP. Bulletin Epidemiologique annuel 2022 du Paludisme au Sénégal. 2022.
- Visée C, Morlighem C, Linard C, Faty A, Henry S, Dujardin S. Addressing bias in national population density models: Focusing on rural Senegal. PLOS ONE. 2024 Nov 12;19(11):e0310809. [CrossRef]
- PNLP. Bulletin Epidemiologique annuel 2023 du Paludisme au Sénégal. 2023.
- Sturrock HJ, Cohen JM, Keil P, Tatem AJ, Le Menach A, Ntshalintshali NE, et al. Fine-scale malaria risk mapping from routine aggregated case data. Malar J. 2014 Nov 3;13(1):421. [CrossRef]
- ANSD [Sénégal], ICF. Sénégal : Enquête Démographique et de Santé Continue (EDS-Continue 2017). Rockville, Maryland, USA: ANSD and ICF; 2018.
- Cameron E, Young AJ, Twohig KA, Pothin E, Bhavnani D, Dismer A, et al. Mapping the endemicity and seasonality of clinical malaria for intervention targeting in Haiti using routine case data. Rodriguez-Barraquer I, Franco E, White N, editors. eLife. 2021 Jun 1;10:e62122. [CrossRef]
- Gueye D, Ly A, Gueye B, Ndour P, Fullman N, Liu P, et al. A consolidated and geolocated facility list in Senegal from triangulating secondary data. Sci Data. 2024 Jan 24;11. [CrossRef]
- Maina J, Ouma PO, Macharia PM, Alegana VA, Mitto B, Fall IS, et al. A spatial database of health facilities managed by the public health sector in sub Saharan Africa. Sci Data. 2019 Jul 25;6(1):134. [CrossRef]
- Corsi D, Neuman M, Finlay J, Subramanian S. Demographic and Health Surveys: a profile. Int J Epidemiol. 2012;41(6):1602–13. [CrossRef]
- Karger DN, Conrad O, Böhner J, Kawohl T, Kreft H, Soria-Auza RW, et al. Climatologies at high resolution for the earth’s land surface areas. Sci Data. 2017 Sep 5;4(1):170122. [CrossRef]
- Wan Z, Hook S, Hulley, G. MODIS/Terra Land Surface Temperature/Emissivity Daily L3 Global 1km SIN Grid V061 [dataset]. NASA EOSDIS Land Processes DAAC; 2021. [CrossRef]
- Wan Z, Hook S, Hulley, G. MODIS/Aqua Land Surface Temperature/Emissivity Daily L3 Global 1km SIN Grid V061 [dataset]. NASA EOSDIS Land Processes DAAC; 2021. [CrossRef]
- Simonetti D, Pimple U, Langner A, Marelli A. Pan-tropical Sentinel-2 cloud-free annual composite datasets. Data Brief. 2021 Dec;39:107488. [CrossRef]
- Brown CF, Brumby SP, Guzder-Williams B, Birch T, Hyde SB, Mazzariello J, et al. Dynamic World, Near real-time global 10 m land use land cover mapping. Sci Data. 2022 Jun 9;9(1):251. [CrossRef]
- Farr TG, Rosen PA, Caro E, Crippen R, Duren R, Hensley S, et al. The Shuttle Radar Topography Mission. Rev Geophys. 2007;45(2):RG2004.
- Morlighem C, Nnanatu CC, Visée C, Fall A, Linard C. Spatial interpolation of health and demographic variables: Predicting malaria indicators with and without covariates. PLOS ONE. 2025 mai;20(5):e0322819. [CrossRef]
- Rue H, Martino S, Chopin N. Approximate Bayesian inference for latent Gaussian models by using integrated nested Laplace approximations. J R Stat Soc Ser B Stat Methodol. 2009;71(2):319–92. [CrossRef]
- Gomez-Rubio V. Bayesian inference with INLA. New York: Chapman and Hall/CRC; 2020. 330 p.
- ANSD [Sénégal], ICF. Sénégal: Enquête Démographique et de Santé Continue (EDS-Continue) 2023. Rockville, Maryland, USA: ANSD and ICF; 2024. Available online: https://dhsprogram.com/publications/publication-FR390-DHS-Final-Reports.cfm.
- Dixit A, Lee MC, Goettsch B, Afrane Y, Githeko AK, Yan G. Discovering the cost of care: consumer, provider, and retailer surveys shed light on the determinants of malaria health-seeking behaviours. Malar J. 2016 Mar 22;15(1):179. [CrossRef]
- Alegana VA, Wright JA, Pentrina U, Noor AM, Snow RW, Atkinson PM. Spatial modelling of healthcare utilisation for treatment of fever in Namibia. Int J Health Geogr. 2012 Feb 15;11(1):6. [CrossRef]
- Tobler, W. Three Presentations On Geographical Analysis And Modeling: Non-isotropic Geographic Modeling; Speculations on the Geometry of Geography; and Global Spatial Analysis. Technical Report 93-1. National Center for Geographic Information and Analysis; 1993.
- Macharia PM, Ray N, Gitonga CW, Snow RW, Giorgi E. Combining school-catchment area models with geostatistical models for analysing school survey data from low-resource settings: Inferential benefits and limitations. Spat Stat. 2022 Oct 1;51:100679. [CrossRef]
- WorldPop (www.worldpop.org - School of Geography and Environmental Science, University of Southampton; Department of Geography and Geosciences, University of Louisville; Departement de Geographie, Universite de Namur), Center for International Earth Science Information Network (CIESIN), Columbia University. Global High Resolution Population Denominators Project - Funded by The Bill and Melinda Gates Foundation (OPP1134076). 2018. [CrossRef]
- WorldPop (www.worldpop.org - School of Geography and Environmental Science, University of Southampton; Department of Geography and Geosciences, University of Louisville; Departement de Geographie, Universite de Namur), Center for International Earth Science Information Network (CIESIN), Columbia University. Global High Resolution Population Denominators Project - Funded by The Bill and Melinda Gates Foundation (OPP1134076). 2018. [CrossRef]
- Macharia, P. Approaches to defining health facility catchment areas in sub-Saharan Africa.
- Macharia PM, Ray N, Giorgi E, Okiro EA, Snow RW. Defining service catchment areas in low-resource settings. BMJ Glob Health. 2021 Jul 22;6(7):e006381. [CrossRef]
- Ndione, B. Migration au Sénégal: profil national 2018. Sénégal: Agence Nationale de la Statistique et de la Démographie du Sénégal (ANSD); 2018.
- Blangiardo M, Cameletti M. Spatial and Spatio-temporal Bayesian Models with R-INLA. Wiley; 2015.
- Blangiardo M, Cameletti M, Baio G. A tutorial in spatial and spatio-temporal models with R-INLA.
- Lindgren F, Rue H, Lindström J. An Explicit Link between Gaussian Fields and Gaussian Markov Random Fields: The Stochastic Partial Differential Equation Approach. J R Stat Soc Ser B Stat Methodol. 2011 Sep 1;73(4):423–98. [CrossRef]
- Utazi CE, Thorley J, Alegana VA, Ferrari MJ, Takahashi S, Metcalf CJE, et al. High resolution age-structured mapping of childhood vaccination coverage in low and middle income countries. Vaccine. 2018 Mar 14;36(12):1583–91. [CrossRef]
- Craig MH, Snow RW, le Sueur D. A climate-based distribution model of malaria transmission in sub-Saharan Africa. Parasitol Today Pers Ed. 1999 Mar;15(3):105–11. [CrossRef]
- Frimpong A, Kwabena Forkuo E, Matthew Osei Jnr E. The effect of land use land cover types on MODIS land surface temperature in Ghana. Cogent Eng. 2024 Dec 31;11(1):2411865. [CrossRef]
- Diop A, Ndiaye F, Sturm-Ramirez K, Konate L, Senghor M, Diouf EH, et al. Urban malaria vector bionomics and human sleeping behavior in three cities in Senegal. Parasit Vectors. 2023 Sep 19;16:331. [CrossRef]
- Dlamini SN, Fall IS, Mabaso SD. Bayesian Geostatistical Modeling to Assess Malaria Seasonality and Monthly Incidence Risk in Eswatini. J Epidemiol Glob Health. 2022 Sep 1;12(3):340–61. [CrossRef]
- Kabaria CW, Molteni F, Mandike R, Chacky F, Noor AM, Snow RW, et al. Mapping intra-urban malaria risk using high resolution satellite imagery: a case study of Dar es Salaam. Int J Health Geogr. 2016 Dec;15(1):26. [CrossRef]
- Pourtois JD, Tallam K, Jones I, Hyde E, Chamberlin AJ, Evans MV, et al. Climatic, land-use and socio-economic factors can predict malaria dynamics at fine spatial scales relevant to local health actors: Evidence from rural Madagascar. PLOS Glob Public Health. 2023 févr;3(2):e0001607. [CrossRef]
- Krefis AC, Schwarz NG, Nkrumah B, Acquah S, Loag W, Oldeland J, et al. Spatial Analysis of Land Cover Determinants of Malaria Incidence in the Ashanti Region, Ghana. PLOS ONE. 2011 Mar 23;6(3):e17905. [CrossRef]
- Oldenburg CE, Guerin PJ, Berthé F, Grais RF, Isanaka S. Malaria and Nutritional Status Among Children With Severe Acute Malnutrition in Niger: A Prospective Cohort Study. Clin Infect Dis. 2018 Sep 14;67(7):1027–34. [CrossRef]
- Protopopoff N, Bortel WV, Speybroeck N, Geertruyden JPV, Baza D, D’Alessandro U, et al. Ranking Malaria Risk Factors to Guide Malaria Control Efforts in African Highlands. PLOS ONE. 2009 Nov 25;4(11):e8022. [CrossRef]
- Diallo AM, Ridde V. Climate change and resilience of the Senegalese health system in the face of the floods in Keur Massar. Int J Health Plann Manage. 2024;39(6):1840–59. [CrossRef]
- Ndiaye F, Diop A, Chabi J, Sturm-Ramirez K, Senghor M, Diouf EH, et al. Distribution and dynamics of Anopheles gambiae s.l. larval habitats in three Senegalese cities with high urban malaria incidence. PLOS ONE. 2024 mai;19(5):e0303473. [CrossRef]
- Georganos S, Brousse O, Dujardin S, Linard C, Casey D, Milliones M, et al. Modelling and mapping the intra-urban spatial distribution of Plasmodium falciparum parasite rate using very-high-resolution satellite derived indicators. Int J Health Geogr. 2020 Dec;19(1):38. [CrossRef]
- Dolo A, Modiano D, Maiga B, Daou M, Dolo G, Guindo H, et al. Difference in susceptibility to malaria between two sympatric ethnic groups in Mali. Am J Trop Med Hyg. 2005 Mar;72(3):243–8. [CrossRef]
- Bolad A, Farouk SE, Israelsson E, Dolo A, Doumbo OK, Nebié I, et al. Distinct interethnic differences in immunoglobulin G class/subclass and immunoglobulin M antibody responses to malaria antigens but not in immunoglobulin G responses to nonmalarial antigens in sympatric tribes living in West Africa. Scand J Immunol. 2005 Apr;61(4):380–6. [CrossRef]
- Seck MC, Thwing J, Fall FB, Gomis JF, Deme A, Ndiaye YD, et al. Malaria prevalence, prevention and treatment seeking practices among nomadic pastoralists in northern Senegal. Malar J. 2017 Dec;16(1):413. [CrossRef]
- Cissé B, Ba EH, Sokhna C, NDiaye JL, Gomis JF, Dial Y, et al. Effectiveness of Seasonal Malaria Chemoprevention in Children under Ten Years of Age in Senegal: A Stepped-Wedge Cluster-Randomised Trial. PLoS Med. 2016 Nov;13(11):e1002175. [CrossRef]
- Sy O, Niang EHA, Ndiaye M, Konaté L, Diallo A, Ba ECC, et al. Entomological impact of indoor residual spraying with pirimiphos-methyl: a pilot study in an area of low malaria transmission in Senegal. Malar J. 2018 Feb 5;17(1):64. [CrossRef]
- PNLP. Bulletin Epidemiologique annuel 2018 du Paludisme au Sénégal. 2018.
- World Health Organization. World malaria report 2019. Geneva: World Health Organization; 2019. Available online: https://iris.who.int/handle/10665/330011.
- PNLP. Bulletin Epidemiologique annuel 2019 du Paludisme au Sénégal. 2019.
- PNLP. Bulletin Epidemiologique annuel 2020 du Paludisme au Sénégal. 2020.
- World Health Organization. World Malaria Report 2020: 20 Years of Global Progress and Challenges. Geneva: World Health Organization; 2020.
- Seydou, A. Who wants COVID-19 vaccination? In 5 West African countries, hesitancy is high, trust low. Afrobarometer; 2021. Report No.: Dispatch No. 432. Available online: https://www.afrobarometer.org/wp-content/uploads/2022/02/ad432-covid-19_vaccine_hesitancy_high_trust_low_in_west_africa-afrobarometer-8march21.pdf.
- Sulemane N, Armocida B, Valente M, Formenti B, Barigazzi S, Ussai S, et al. Vaccines Hesitancy in Africa: how the COVID-19 pandemic may affect malaria vaccination campaigns. J Prev Med Hyg. 2022 Apr 26;63(1):E1–E1. [CrossRef]
- World Health Organization. World malaria report 2024: addressing inequity in the global malaria response. Geneva: World Health Organization; 2024.
- Brousse O, Georganos S, Demuzere M, Dujardin S, Lennert M, Linard C, et al. Can we use local climate zones for predicting malaria prevalence across sub-Saharan African cities? Environ Res Lett. 2020 Dec 15;15(12):124051.
- United Nations, Department of Economic and Social Affairs, Population Division. World Urbanization Prospects: The 2018 Revision (ST/ESA/SER.A/420). New York: United Nations; 2019.
- Sokhna C, Mboup BM, Sow PG, Camara G, Dieng M, Sylla M, et al. Communicable and non-communicable disease risks at the Grand Magal of Touba: The largest mass gathering in Senegal. Travel Med Infect Dis. 2017 Sep 1;19:56–60. [CrossRef]
- Sokhna C, Goumballa N, Hoang VT, Mboup BM, Dieng M, Sylla AB, et al. Senegal’s Grand Magal of Touba: Syndromic Surveillance during the 2016 Mass Gathering. Am J Trop Med Hyg. 2020 Feb;102(2):476–82. [CrossRef]
- World Health Organization. World malaria report 2021. Geneva: World Health Organization; 2021. Available online: https://apps.who.int/iris/handle/10665/350147.
- Lucas TCD, Nandi AK, Chestnutt EG, Twohig KA, Keddie SH, Collins EL, et al. Mapping Malaria by Sharing Spatial Information Between Incidence and Prevalence Data Sets. J R Stat Soc Ser C Appl Stat. 2021 Jun 1;70(3):733–49. [CrossRef]
- Taylor BM, Andrade-Pacheco R, Sturrock HJW. Continuous Inference for Aggregated Point Process Data. J R Stat Soc Ser A Stat Soc. 2018 Oct 1;181(4):1125–50. [CrossRef]
- ANSD [Sénégal], ICF. Sénégal : Enquête sur les indicateurs du paludisme (EIPS) 2020-2021. Rockville, Maryland, USA: ANSD and ICF; 2022.
- Erbach-Schoenberg E, Alegana V, Sorichetta A, Linard C, Lourenço C, Ruktanonchai N, et al. Dynamic denominators: The impact of seasonally varying population numbers on disease incidence estimates. Popul Health Metr. 2016 Oct 12;14:35. [CrossRef]
- Ihantamalala FA, Herbreteau V, Rakotoarimanana FMJ, Rakotondramanga JM, Cauchemez S, Rahoilijaona B, et al. Estimating sources and sinks of malaria parasites in Madagascar. Nat Commun. 2018 Dec;9(1):3897. [CrossRef]
- Tatem AJ, Huang Z, Narib C, Kumar U, Kandula D, Pindolia DK, et al. Integrating rapid risk mapping and mobile phone call record data for strategic malaria elimination planning. Malar J. 2014 Dec;13(1):52. [CrossRef]
- Lucas TCD, Nandi AK, Keddie SH, Chestnutt EG, Howes RE, Rumisha SF, et al. Improving disaggregation models of malaria incidence by ensembling non-linear models of prevalence. Spat Spatio-Temporal Epidemiol. 2022 Jun 1;41:100357. [CrossRef]
| Category | Variables | Date | Spatial resolution | Source |
| Climate & weather | Precipitation | Climatic average over 1988-2018 | 1000 m | CHELSA [54] (https://chelsa-climate.org/) |
| Day land surface temperature (LST), night LST | Annual (2017-2021) | 1000 m | MODIS [55,56] (http://modis.gsfc.nasa.gov/) | |
| Vector-habitat | Normalized difference moisture index (NDMI) | Annual (2017-2021) | 10 m | Computed from Sentinel-2 L1C composites of the Joint Research Centre (JRC) [57] (https://forobs.jrc.ec.europa.eu/sentinel/sentinel2_composite) |
| Land use and land cover: water, trees, flooded vegetation, cropland, grassland, bare land, shrubland, built-up | Annual (2017-2021) | 10 m | Dynamic World by Google and the World Resources Institute [58] (https://dynamicworld.app/) | |
| Elevation | 2000 | 30 m | US Geological Survey [59] (http://eros.usgs.gov/elevation-products) | |
| Susceptibility | Access to basic sanitation service, proportion of Fula, stunting in children | Annual (2017-19/20 avail.; stunting: 2020-21 proj., others: 2021 proj.) | Survey clusters | The DHS Program |
| Lack of resilience | Distance to major roads | 2023 | 100 m | OpenStreetMap (www.openstreetmap.org) |
| Walking-only travel time to health facilities | Annual (2017-2021) | 1000 m | Walking time is computed using elevation, land use, roads and rivers (see Section Computation of travel time) | |
| Ownership of insecticide-treated nets, literacy rate in women | Annual (2017-20 avail.; 2021 proj.) | Survey clusters | The DHS Program |
| Data source | Land and road type | Walking speed (km/h) |
| Dynamic World LULC | Built up | 5 |
| Trees | 3.5 | |
| Shrubland | 4.5 | |
| Cropland | 3.5 | |
| Grassland | 4 | |
| Bare ground | 5 | |
| Flooded vegetation | 0 | |
| Water bodies | 0 | |
| OpenStreetMap | Rivers | 0 |
| Roads | 5 |
| Model name | Description | Number of facilities |
| Benchmark model (BM) |
|
1472 (1389) |
| Wet season model (WM) |
|
1472 (1389) |
| Dry season model (DM) |
|
1472 (1389) |
| Endemicity 1 model (E1) |
|
217 (216) |
| Endemicity 2 model (E2) |
|
373 (328) |
| Endemicity 3 model (E3) |
|
882 (845) |
| Category | Variable | BM | WM | DM | E1 | E2 | E3 | Number of models |
| Climate & weather | Precipitation | (⨯) | ⨯ | (⨯) | 3 | |||
| Day LST | ⨯ | ⨯ | ⨯ | ⨯ | 4 | |||
| Night LST | ⨯ | ⨯ | 2 | |||||
| Vector-habitat | NDMI | ⨯ | (⨯) | 2 | ||||
| Prop. of bare land | (⨯) | ⨯ | ⨯ | 3 | ||||
| Prop. of built-up | ⨯ | ⨯ | ⨯ | ⨯ | ⨯ | ⨯ | 6 | |
| Prop. of cropland | (⨯) | (⨯) | ⨯ | 3 | ||||
| Prop. of flooded vegetation | ⨯ | (⨯) | 2 | |||||
| Prop. of shrubland | ⨯ | ⨯ | 2 | |||||
| Prop. of trees | ⨯ | ⨯ | 2 | |||||
| Prop. of water | ⨯ | 1 | ||||||
| Elevation | ⨯ | ⨯ | 2 | |||||
| Susceptibility | Access to basic sanitation | ⨯ | ⨯ | ⨯ | ⨯ | 4 | ||
| Prop. of Fula | ⨯ | 1 | ||||||
| Stunting in children | ⨯ | ⨯ | ⨯ | ⨯ | ⨯ | ⨯ | 6 | |
| Lack of resilience | Distance to major roads | ⨯ | ⨯ | ⨯ | ⨯ | 4 | ||
| Walking time to health facilities | ⨯ | ⨯ | ⨯ | ⨯ | ⨯ | ⨯ | 6 | |
| Number of covariates | 9 | 10 | 8 | 9 | 9 | 8 | / |
| Variable | Benchmark (BM) | Wet season (WM) | Dry season (DM) | ||||||
| Mean | 2.5% quant. | 97.5% quant. | Mean | 2.5% quant. | 97.5% quant. | Mean | 2.5% quant. | 97.5% quant. | |
| ) | -3.61 | -4.40 | -2.82 | -4.00 | -4.72 | -3.28 | -4.37 | -5.12 | -3.62 |
| Day LST | -0.37 | -0.50 | -0.23 | -0.34 | -0.48 | -0.19 | - | - | - |
| Night LST | 0.26 | 0.15 | 0.37 | 0.24 | 0.13 | 0.36 | - | - | - |
| Prop. of bare land | - | - | - | 0.003 | -0.08 | 0.07 | - | - | - |
| Prop. of built-up | 0.57 | 0.52 | 0.62 | 0.51 | 0.44 | 0.58 | 0.63 | 0.58 | 0.67 |
| Prop. of cropland | 0.02 | -0.03 | 0.07 | - | - | - | 0.04 | -0.01 | 0.10 |
| Prop. of flooded vegetation | - | - | - | -0.10 | -0.16 | -0.05 | - | - | - |
| Prop. of shrubland | - | - | - | -0.11 | -0.19 | -0.02 | - | - | - |
| Prop. of trees | 0.11 | 0.05 | 0.17 | - | - | - | 0.15 | 0.09 | 0.22 |
| Elevation | - | - | - | - | - | - | -0.13 | -0.23 | -0.03 |
| Access to basic sanitation | 0.23 | 0.16 | 0.30 | 0.25 | 0.18 | 0.32 | 0.18 | 0.11 | 0.25 |
| Stunting in children | 0.26 | 0.17 | 0.35 | 0.29 | 0.20 | 0.37 | 0.25 | 0.16 | 0.33 |
| Distance to major roads | -0.19 | -0.25 | -0.13 | -0.12 | -0.18 | -0.06 | -0.13 | -0.19 | -0.07 |
| Walking time to health facilities | -0.35 | -0.41 | -0.28 | -0.34 | -0.41 | -0.28 | -0.38 | -0.45 | -0.31 |
| Precision of uncorrelated random variations ( | 1.12 | 1.08 | 1.17 | 1.17 | 1.13 | 1.22 | 1.09 | 1.05 | 1.13 |
| ) | 2.16a | 1.71 | 2.73 | 2.22b | 1.74 | 2.76 | 2.01c | 1.59 | 2.53 |
| SD of spatially correlated variations ( | 2.78 | 2.22 | 3.46 | 2.53 | 2.00 | 3.10 | 2.57 | 2.06 | 3.19 |
| ) | 0.99 | 0.98 | 0.99 | 0.98 | 0.97 | 0.99 | 0.99 | 0.98 | 0.99 |
| Variable | Endemicity 1 | Endemicity 2 | Endemicity 3 | ||||||
| Mean | 2.5% quant. | 97.5% quant. | Mean | 2.5% quant. | 97.5% quant. | Mean | 2.5% quant. | 97.5% quant. | |
| ) | -1.24 | -2.20 | -0.32 | -5.98 | -7.24 | -4.72 | -4.56 | -5.44 | -3.67 |
| Precipitation | 0.45 | -0.06 | 0.96 | 1.64 | 0.95 | 2.34 | 0.17 | -0.05 | 0.38 |
| Day LST | -1.60 | -2.08 | -1.12 | - | - | - | -0.14 | -0.26 | -0.02 |
| NDMI | -0.50 | -0.70 | -0.30 | 0.17 | -0.08 | 0.42 | - | - | - |
| Prop. of bare land | - | - | - | 0.22 | 0.09 | 0.35 | -0.08 | -0.15 | -0.02 |
| Prop. of built-up | 0.43 | 0.28 | 0.58 | 0.63 | 0.52 | 0.75 | 0.53 | 0.46 | 0.60 |
| Prop. of cropland | - | - | - | 0.35 | 0.20 | 0.50 | - | - | - |
| Prop. of flooded vegetation | 1.15 | -0.22 | 2.53 | - | - | - | - | - | - |
| Prop. of shrubland | -0.38 | -0.50 | -0.26 | - | - | - | - | - | - |
| Prop. of water | -1.23 | -1.76 | -0.69 | - | - | - | - | - | - |
| Elevation | - | - | - | -0.58 | -0.95 | -0.21 | - | - | - |
| Access to basic sanitation | - | - | - | - | - | - | 0.18 | 0.09 | 0.27 |
| Prop. of Fula | - | - | - | -0.31 | -0.59 | -0.04 | - | - | - |
| Stunting in children | 0.40 | 0.26 | 0.54 | 0.32 | 0.09 | 0.54 | 0.25 | 0.14 | 0.37 |
| Distance to major roads | - | - | - | - | - | - | -0.21 | -0.28 | -0.14 |
| Walking time to health facilities | -0.23 | -0.30 | -0.16 | -1.84 | -2.17 | -1.51 | -0.36 | -0.45 | -0.27 |
| Precision of uncorrelated random variations ( | 2.27 | 2.05 | 2.50 | 1.02 | 0.95 | 1.10 | 1.15 | 1.09 | 1.20 |
| ) | 1.74a | 1.13 | 2.57 | 0.91b | 0.59 | 1.40 | 2.17c | 1.59 | 2.87 |
| SD of spatially correlated variations ( | 1.58 | 1.10 | 2.21 | 1.80 | 1.31 | 2.46 | 2.46 | 1.83 | 3.21 |
| ) | 0.97 | 0.95 | 0.99 | 0.97 | 0.94 | 0.99 | 0.98 | 0.96 | 0.99 |
| Random CV | RMSE | MAE | R² (COD) | r² (corr.) |
| Benchmark (BM) | 0.20 | 0.06 | 0.62 | 0.65 |
| BM for E1 | 0.47 | 0.29 | 0.40 | 0.48 |
| BM for E2 | 0.09 | 0.03 | 0.43 | 0.60 |
| BM for E3 | 0.04 | 0.01 | 0.26 | 0.29 |
| Wet season (WM) | 0.13 | 0.04 | 0.65 | 0.67 |
| Dry season (DM) | 0.08 | 0.02 | 0.54 | 0.56 |
| Endemicity 1 (E1) | 0.48 | 0.29 | 0.37 | 0.43 |
| Endemicity 2 (E2) | 0.08 | 0.02 | 0.57 | 0.69 |
| Endemicity 3 (E3) | 0.04 | 0.01 | 0.27 | 0.32 |
| Temporal block CV | RMSE | MAE | R² (COD) | r² (corr.) |
| Benchmark (BM) | 0.17 | 0.05 | 0.70 | 0.75 |
| BM for E1 | 0.41 | 0.25 | 0.55 | 0.65 |
| BM for E2 | 0.09 | 0.03 | 0.44 | 0.63 |
| BM for E3 | 0.04 | 0.01 | 0.19 | 0.30 |
| Wet season (WM) | 0.13 | 0.04 | 0.66 | 0.77 |
| Dry season (DM) | 0.07 | 0.02 | 0.63 | 0.66 |
| Endemicity 1 (E1) | 0.41 | 0.24 | 0.55 | 0.64 |
| Endemicity 2 (E2) | 0.08 | 0.03 | 0.49 | 0.68 |
| Endemicity 3 (E3) | 0.04 | 0.01 | 0.20 | 0.31 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




