Submitted:
19 March 2026
Posted:
23 March 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Method
Result
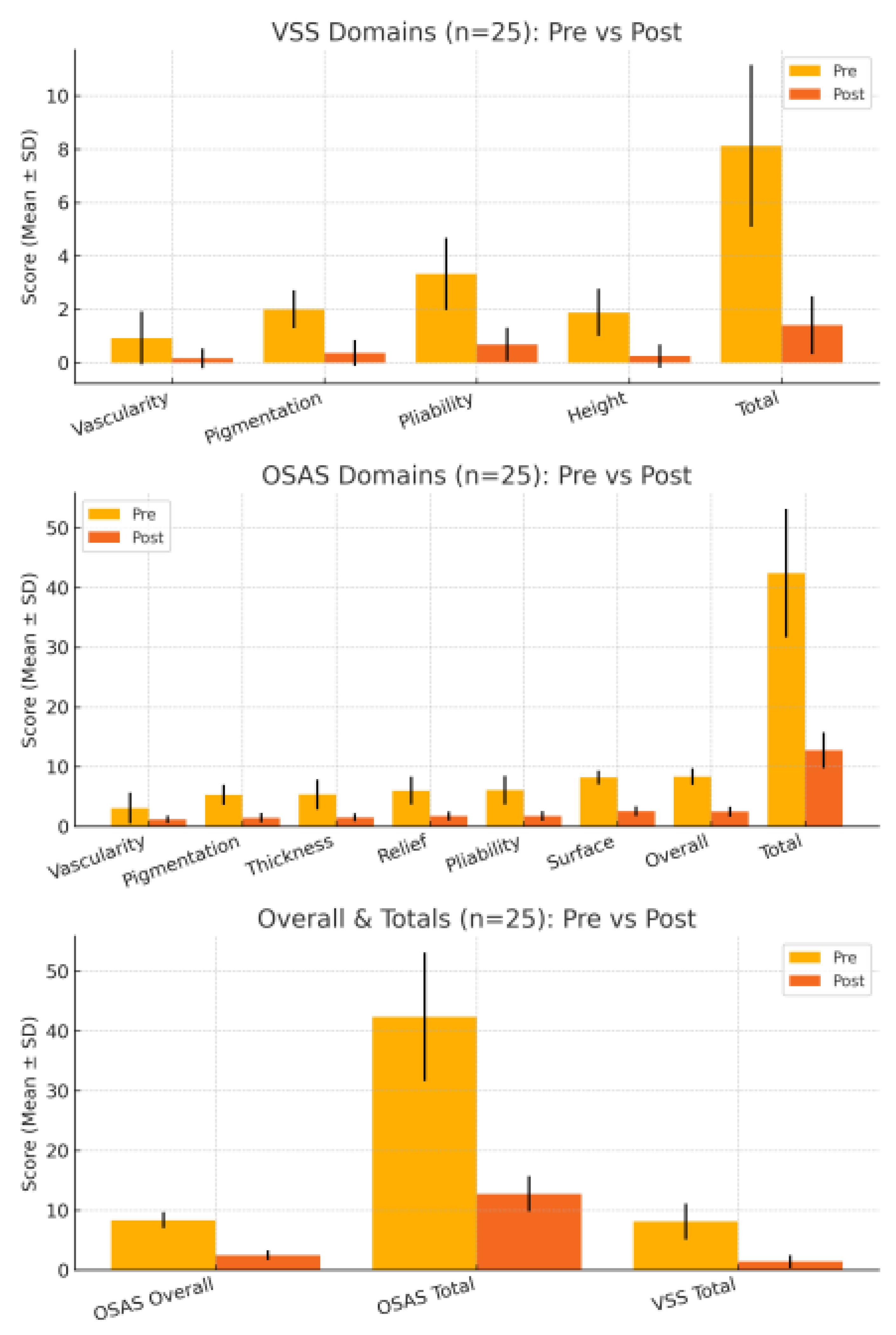
| Parameter | Pre Mean ± SD | Post Mean ± SD | Mean Diff | t-value | p-value |
| Vascularity | 3.08 ± 2.58 | 1.20 ± 0.65 | 1.88 | 4.301 | P < 0.001 |
| Pigmentation | 5.32 ± 1.68 | 1.48 ± 0.77 | 3.84 | 13.668 | P < 0.001 |
| Thickness | 5.36 ± 2.48 | 1.52 ± 0.65 | 3.84 | 9.436 | P < 0.001 |
| Relief | 6.00 ± 2.33 | 1.76 ± 0.72 | 4.24 | 11.163 | P < 0.001 |
| Pliability | 6.08 ± 2.41 | 1.76 ± 0.83 | 4.32 | 11.316 | P < 0.001 |
| Surface | 8.20 ± 1.15 | 2.56 ± 0.82 | 5.64 | 23.777 | P < 0.001 |
| Overall | 8.36 ± 1.35 | 2.48 ± 0.82 | 5.88 | 19.852 | P < 0.001 |
| Total Score | 42.40 ± 10.75 | 12.76 ± 2.96 | 29.64 | 16.417 | P < 0.001 |
| Table | Parameter | Pre Mean ± SD | Post Mean ± SD | Mean Diff | t-value | p-value |
| VSS | Vascularity | 0.92 ± 1.00 | 0.16 ± 0.37 | 0.76 | 3.919 | P < 0.001 |
| VSS | Pigmentation | 2.00 ± 0.71 | 0.36 ± 0.49 | 1.64 | 12.859 | P < 0.001 |
| VSS | Pliability | 3.32 ± 1.35 | 0.68 ± 0.63 | 2.64 | 11.475 | P < 0.001 |
| VSS | Height | 1.88 ± 0.88 | 0.24 ± 0.44 | 1.64 | 12.859 | P < 0.001 |
| VSS | Total | 8.12 ± 3.03 | 1.40 ± 1.08 | 6.72 | 13.483 | P < 0.001 |
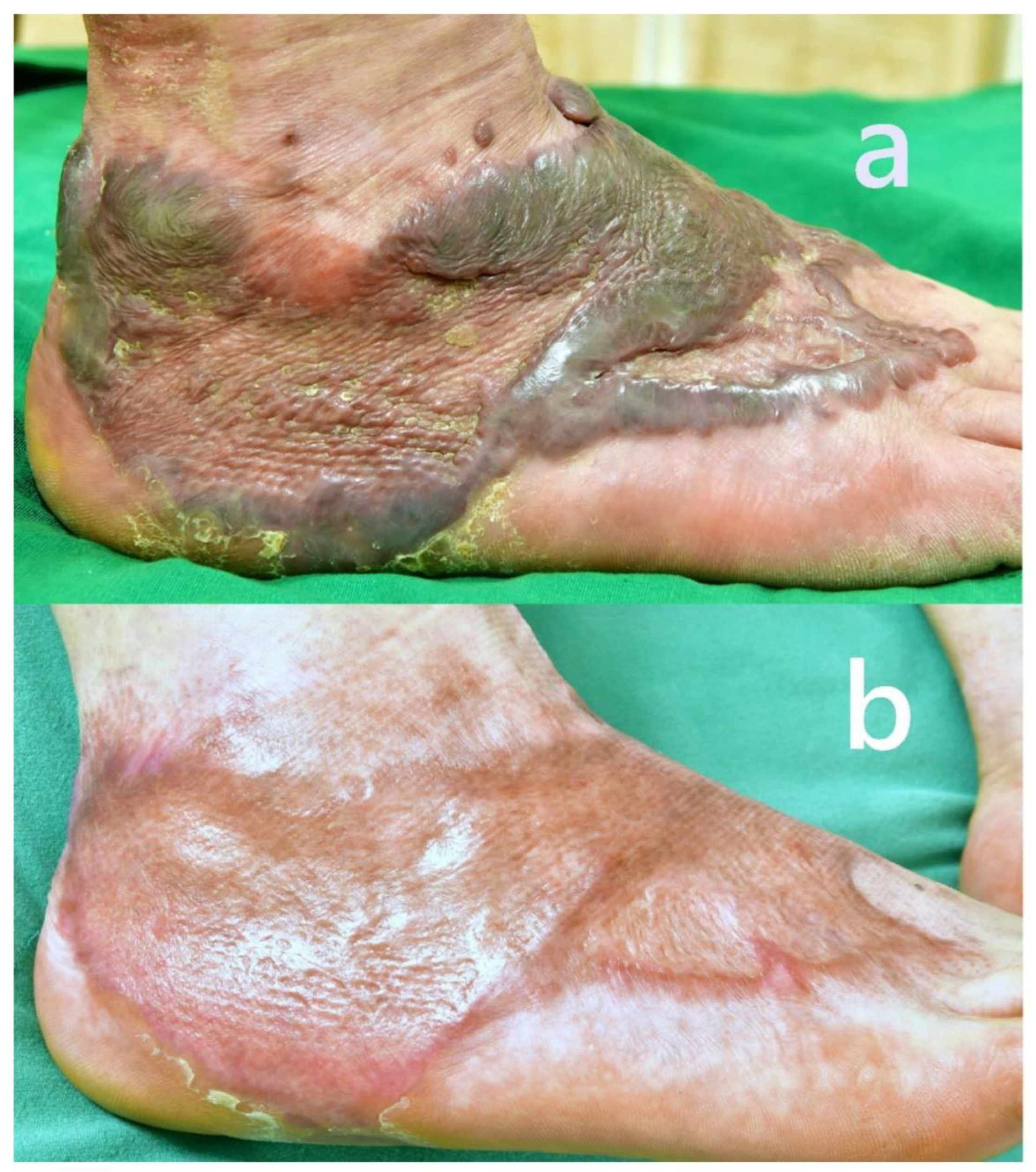
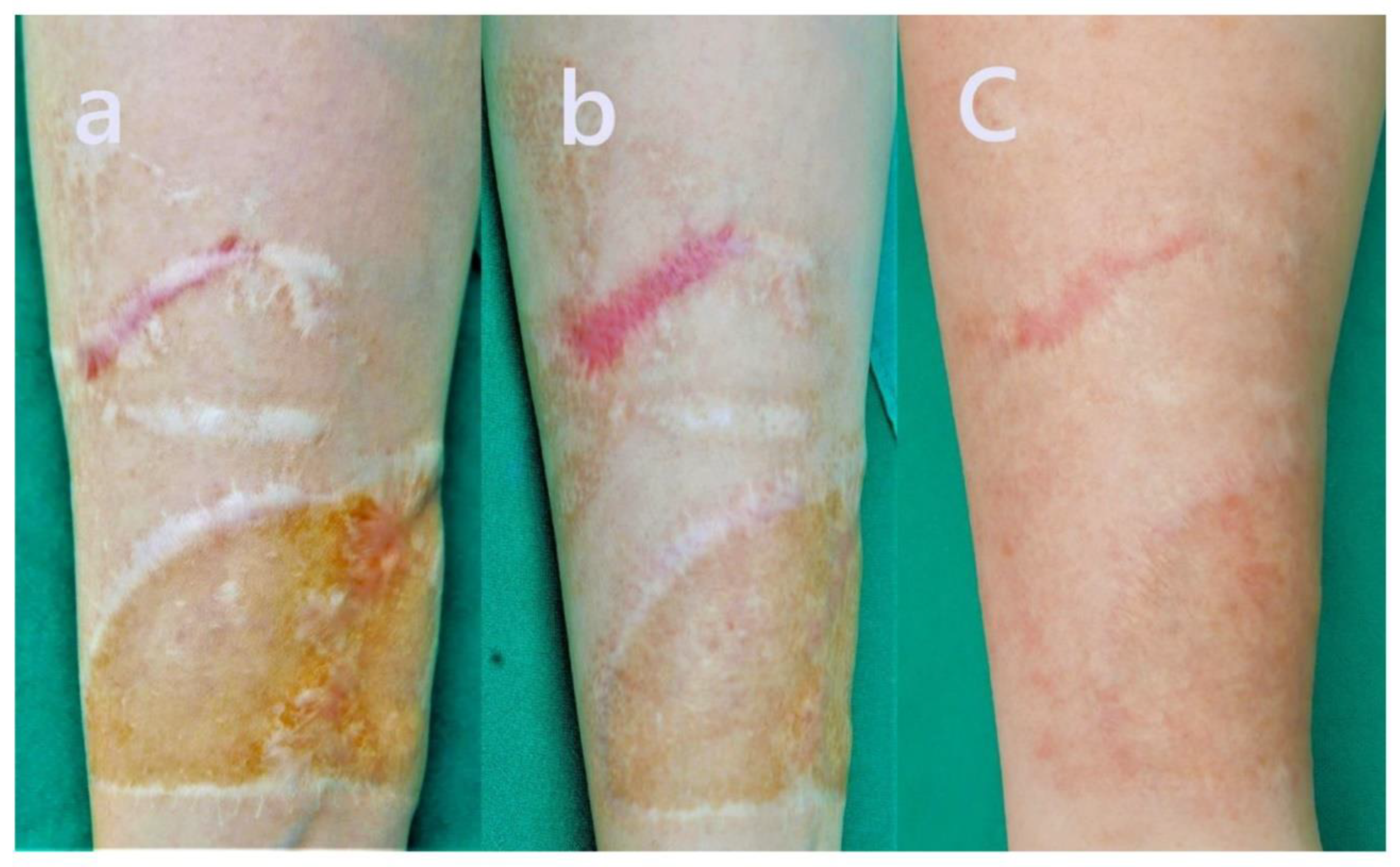
2.1. Case 1
- The pigmentation of the scar significantly normalized. The previously dark violaceous and reddish discoloration diminished, blending more seamlessly with the surrounding skin.
- There was a marked reduction in scar thickness and protrusion. The previously elevated, nodular keloidal margins flattened considerably, resulting in a more even surface contour.
- The texture of the skin improved noticeably. The rough, scaly, and irregular surface observed before treatment became smoother, with improved elasticity and a healthy sheen.
- Subjective symptoms, including persistent itching and pain, were fully relieved. The patient reported no discomfort during rest or ambulation following treatment.
- Functional recovery was also observed. The initial gait disturbance caused by contracture and scar tightness around the ankle was resolved.
2.2. Case 2
- Scar thickness and firmness reduced noticeably, showing a smoother and more uniform texture.
- Skin tone normalized, with reduced redness and the demarcation blended with the surrounding tissue.
- Pain and itching completely resolved.
- Wrist flexibility and range of motion improved significantly.
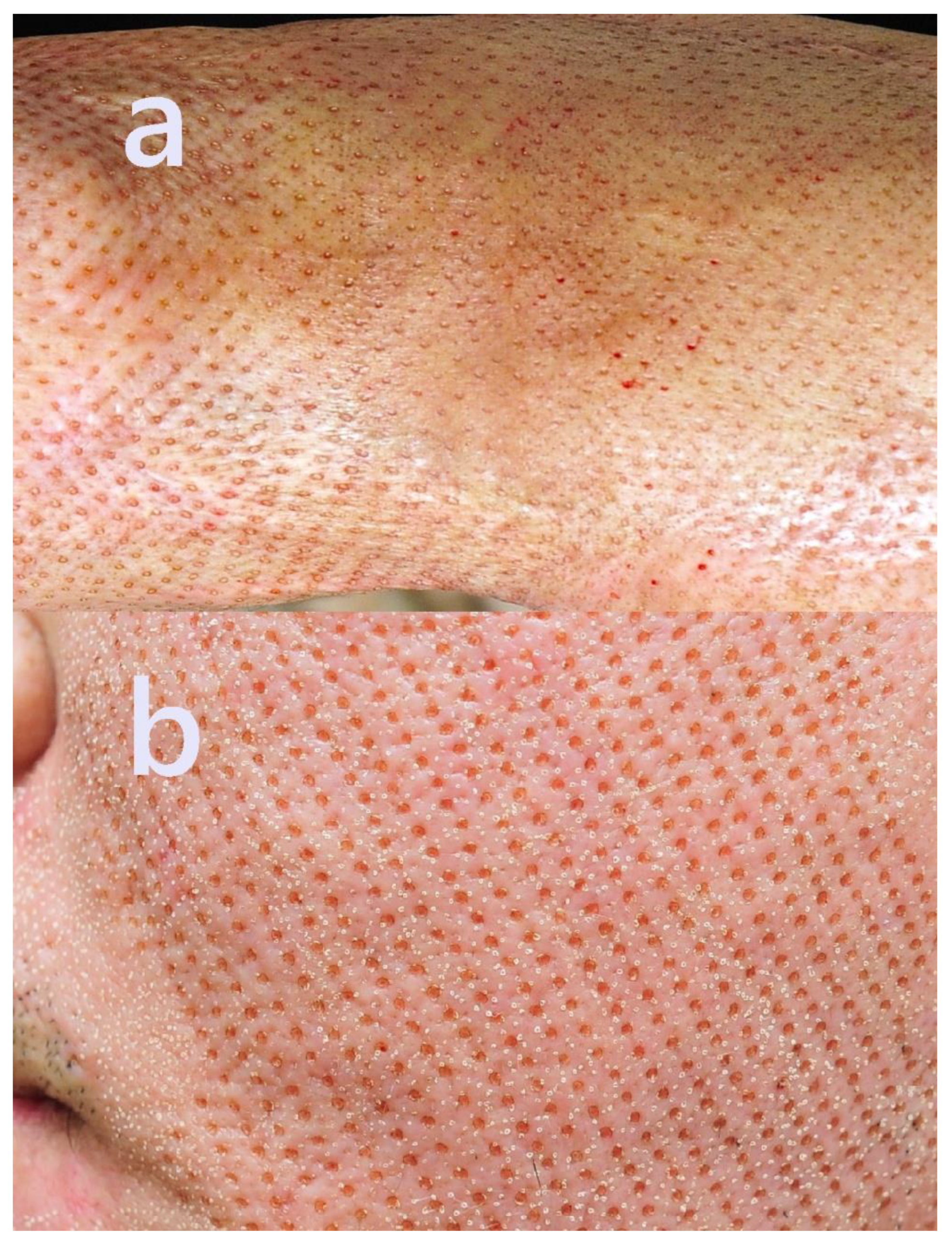
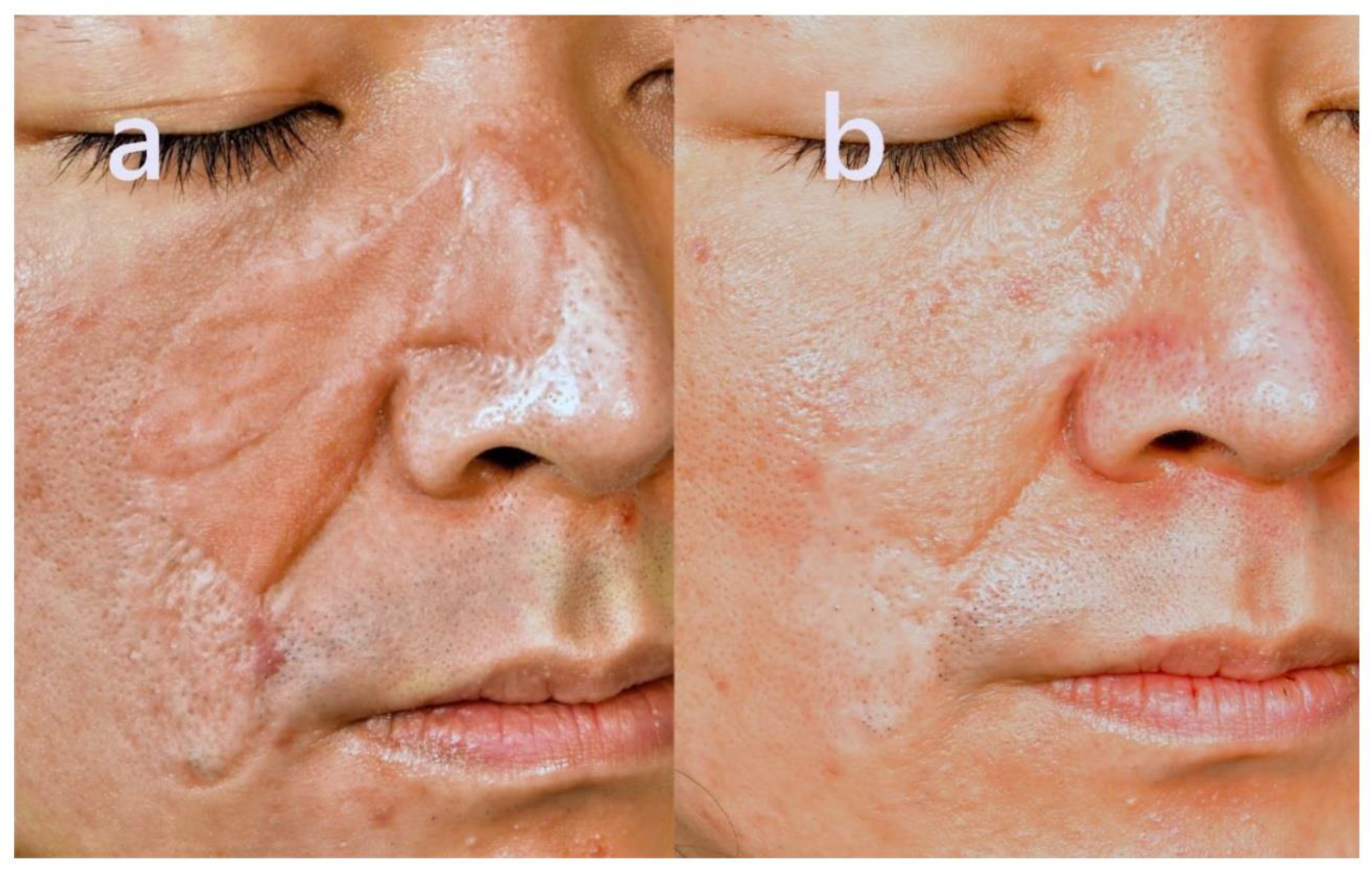
2.3. Case 3
- The scar surface became significantly flatter and less fibrotic, with a marked improvement in contour integration and reduced skin tension.
- The hard, bumpy texture softened, and the demarcation lines visibly blended.
- The color of the scar blended more harmoniously with the adjacent skin.
- Overall facial symmetry improved, with perioral movement appearing more natural.
2.4. Case 4
- The surface texture of the scar normalized significantly, with a marked reduction in rigidity and a more uniform appearance.
- The hyperpigmented areas and keratotic features largely resolved, reflecting substantial improvement in both pigmentation and overall color uniformity.
- Elevated, hypopigmented suture lines at the scar margins became less prominent and blended more seamlessly into adjacent tissue.
- The reduced skin thickness alleviated wrist movement discomfort, improving flexibility.
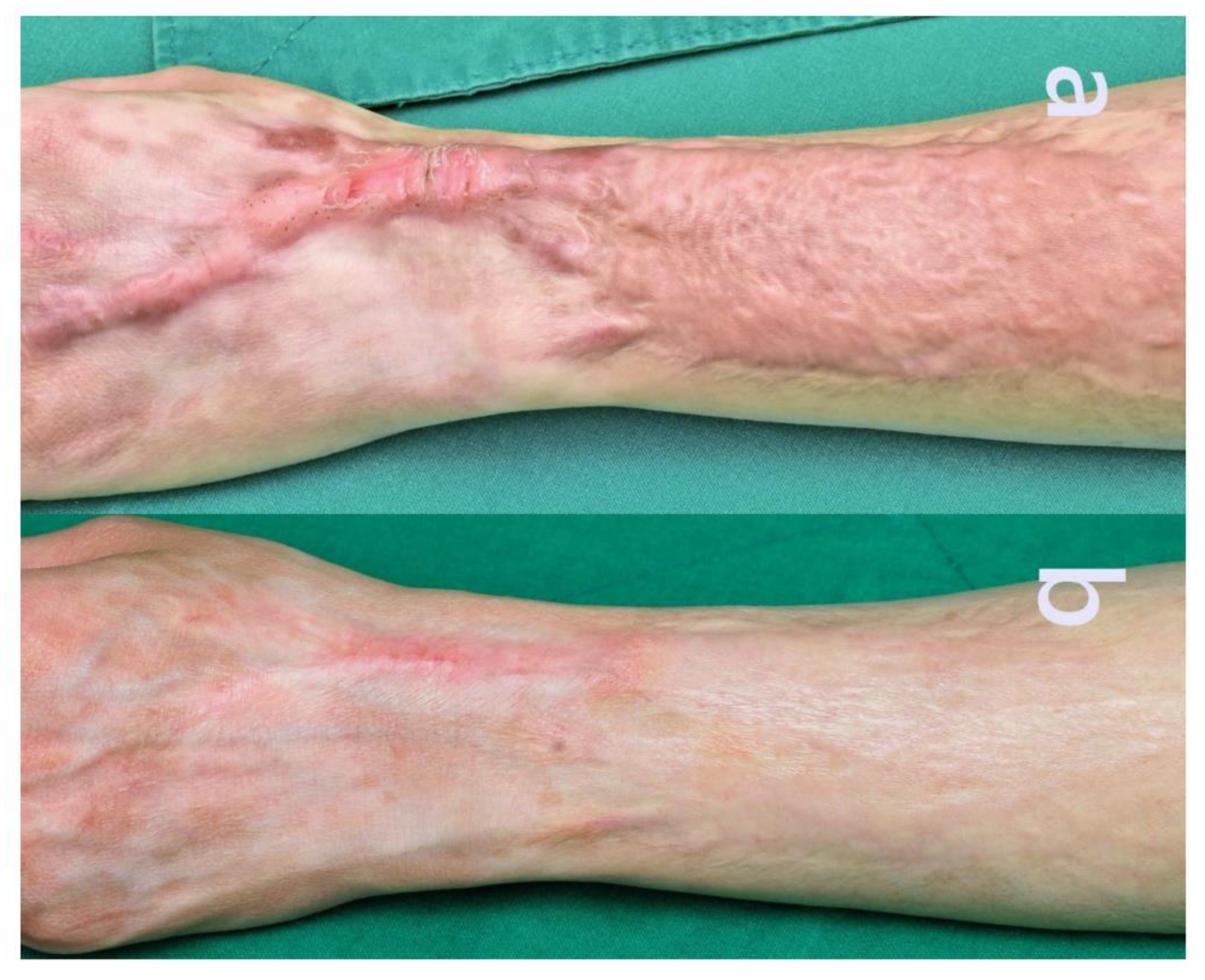
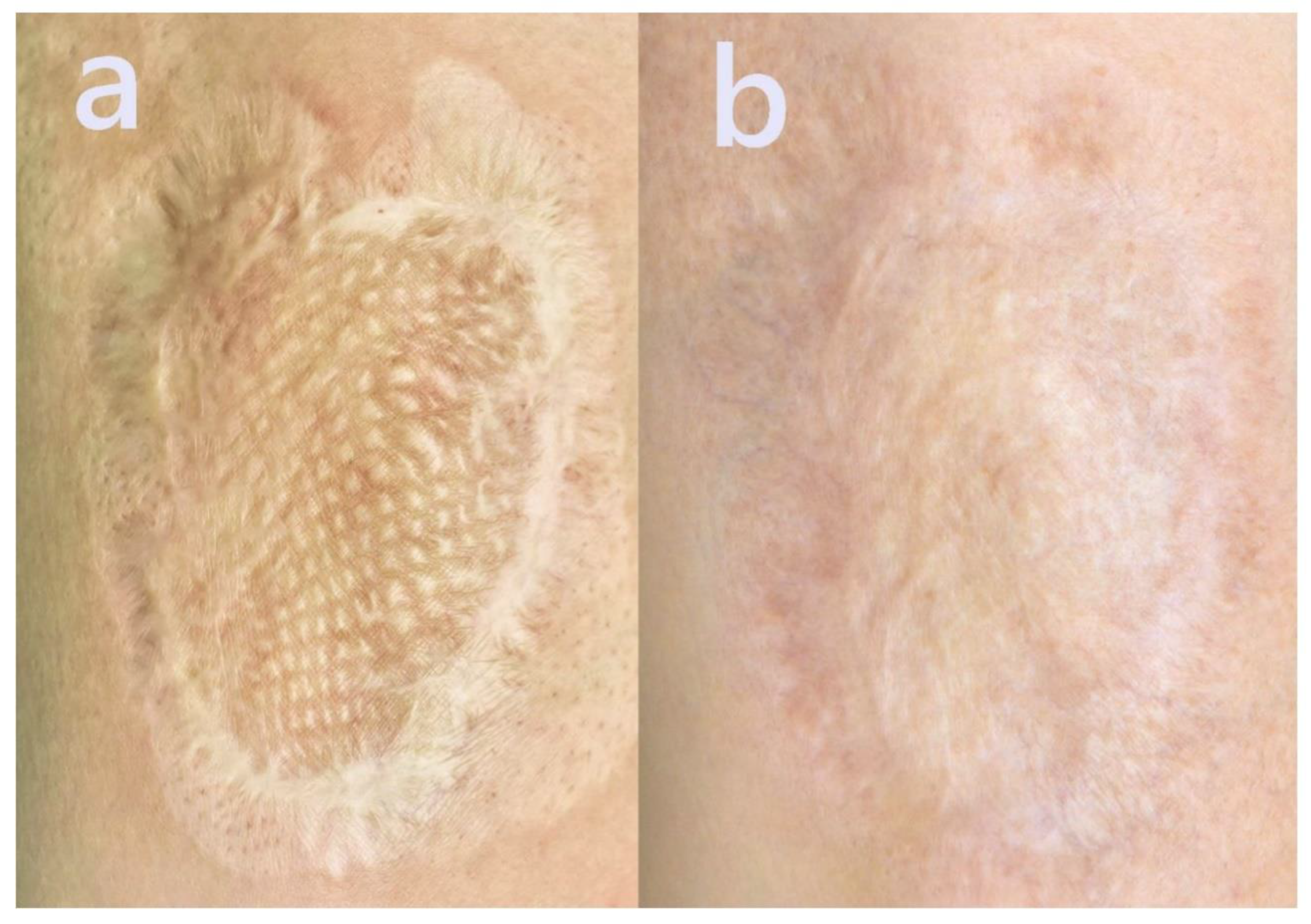
2.5. Case 5
- Scar thickness and stiffness were markedly reduced, resulting in a significantly flatter and less fibrotic surface. Mesh-pattern ridges characteristic of split-thickness grafts became less visible, indicating dermal remodeling and integration with surrounding tissue.
- The previously elevated and indurated texture softened, leading to smoother surface contours and improved tactile quality.
- Scar color transitioned toward a more natural skin tone, demonstrating pigment normalization and better chromatic blending with adjacent skin.
- Scar boundaries became less defined, suggesting successful contour integration and edge softening.
- Overall cosmetic appearance improved, enhancing patient satisfaction and restoring a more natural visual skin landscape.
Discussion
Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Aleman Paredes, K.; et al. Comparative outcomes of graft types in burn reconstruction: A systematic review. Cureus 2024, 16, e54277. [Google Scholar] [PubMed]
- Harrison, CA; MacNeil, S. The mechanism of skin graft contraction: An update. Burns 2008, 34, 153–163. [Google Scholar] [CrossRef] [PubMed]
- Baumann, ME; et al. FXCO2 therapy of existing burn scars in a porcine model. Burns Open. 2019, 3, 89–95. [Google Scholar] [CrossRef]
- Zhuang, Z; Li, Y; Wei, X. Intralesional triamcinolone for keloids/hypertrophic scars: Systematic review. Burns 2021, 47(5), 987–998. [Google Scholar] [CrossRef] [PubMed]
- Leszczynski, R; et al. Laser therapy for hypertrophic and keloid scars. Cochrane Database Syst Rev. 2022, (9), CD011642. [Google Scholar] [CrossRef] [PubMed]
- Lee, SJ; et al. Combination laser-cision and pinhole CO2 for hypertrophic burn scars. Lasers Surg Med. 2014, 46, 380–384. [Google Scholar] [CrossRef] [PubMed]
- Whang, SW; et al. Burn scars treated by pinhole method using a carbon dioxide laser. J Dermatol 2006, 33, 869–872. [Google Scholar] [CrossRef] [PubMed]
- Li, J; et al. Dual-scan CO2 protocol in split-thickness graft contraction (red Duroc pig). Burns Trauma. 2021, 9, tkab048. [Google Scholar] [CrossRef] [PubMed]
- Cox, C; et al. CO2 resurfacing for scars of the hand/upper extremity. Scars Burn Heal. 2022, 8, 20595131211047694. [Google Scholar] [CrossRef] [PubMed]
- Klifto, KM; Asif, M; Hultman, CS. Laser management of hypertrophic burn scars: Review. Burns Trauma 2020, 8, tkz003. [Google Scholar] [CrossRef] [PubMed]
- Shirakami, E; Yamakawa, S; Hayashida, K. Strategies to prevent hypertrophic scars: Molecular evidence. Burns Trauma. 2020, 8, tkz004. [Google Scholar] [CrossRef] [PubMed]
- Poetschke, J; Gauglitz, GG. Hyperpigmented Scar. In Textbook on Scar Management; Springer, 2020; pp. 505–507. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




