Submitted:
10 May 2025
Posted:
12 May 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. CT-Guided PBD Localization Procedure
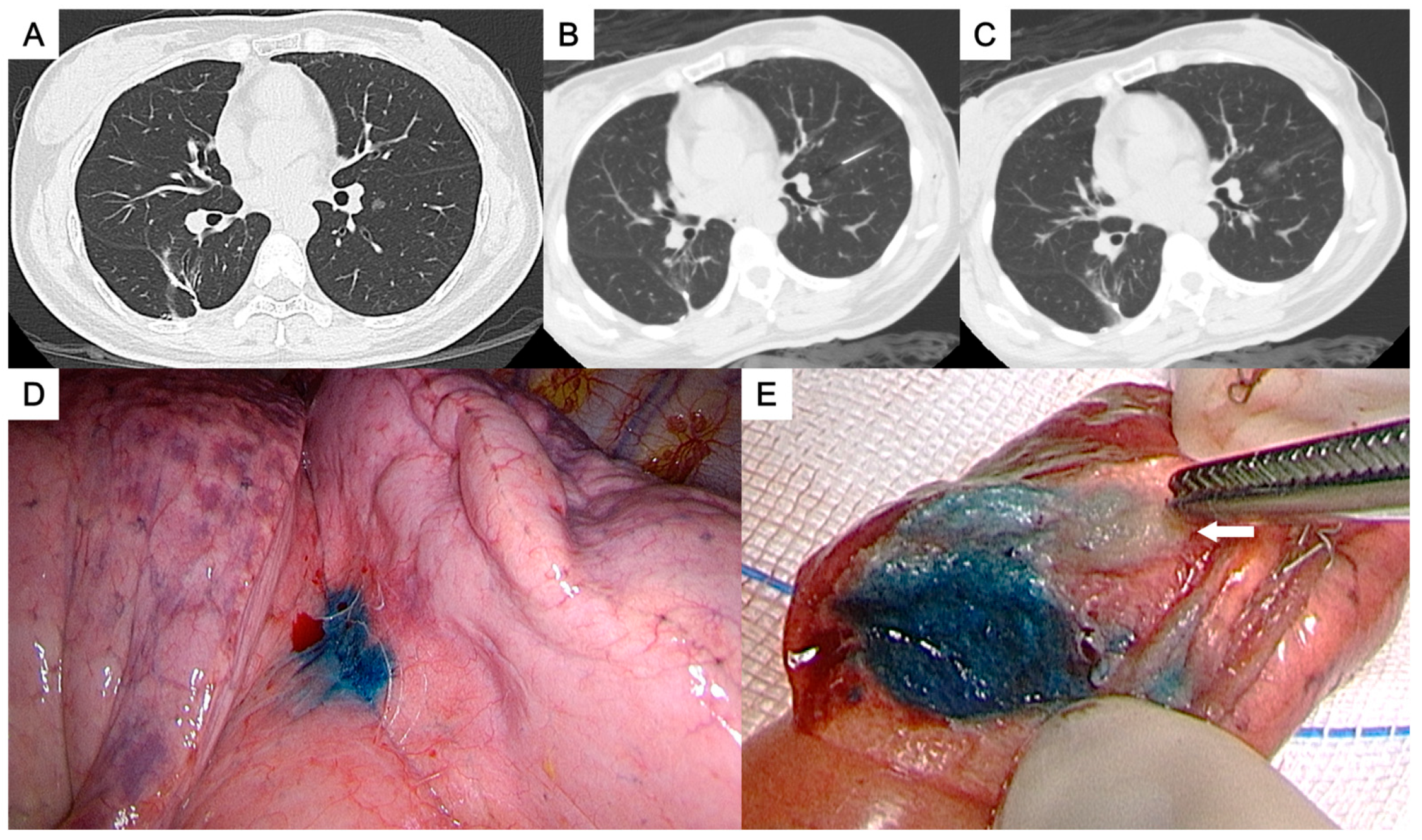
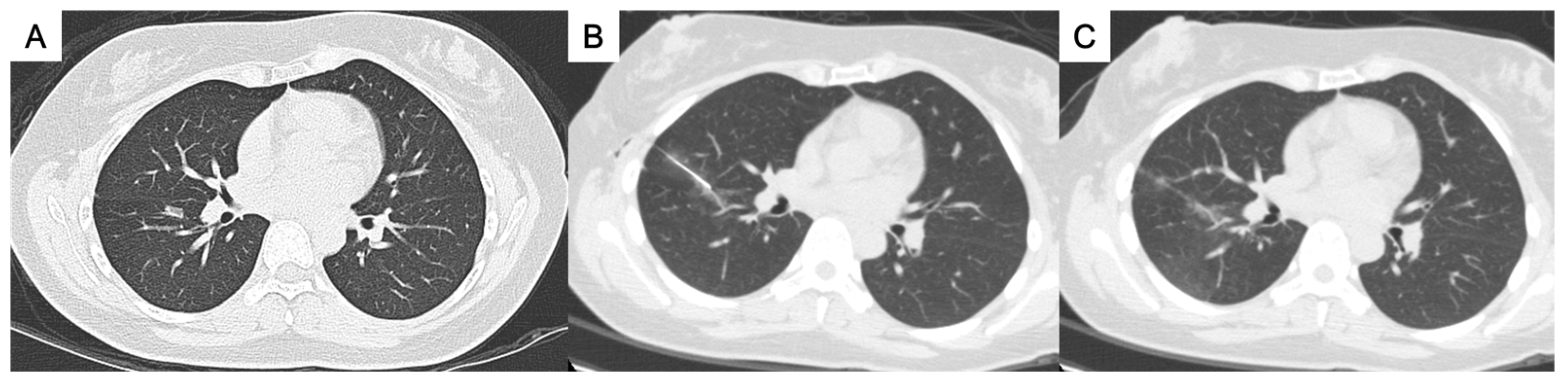
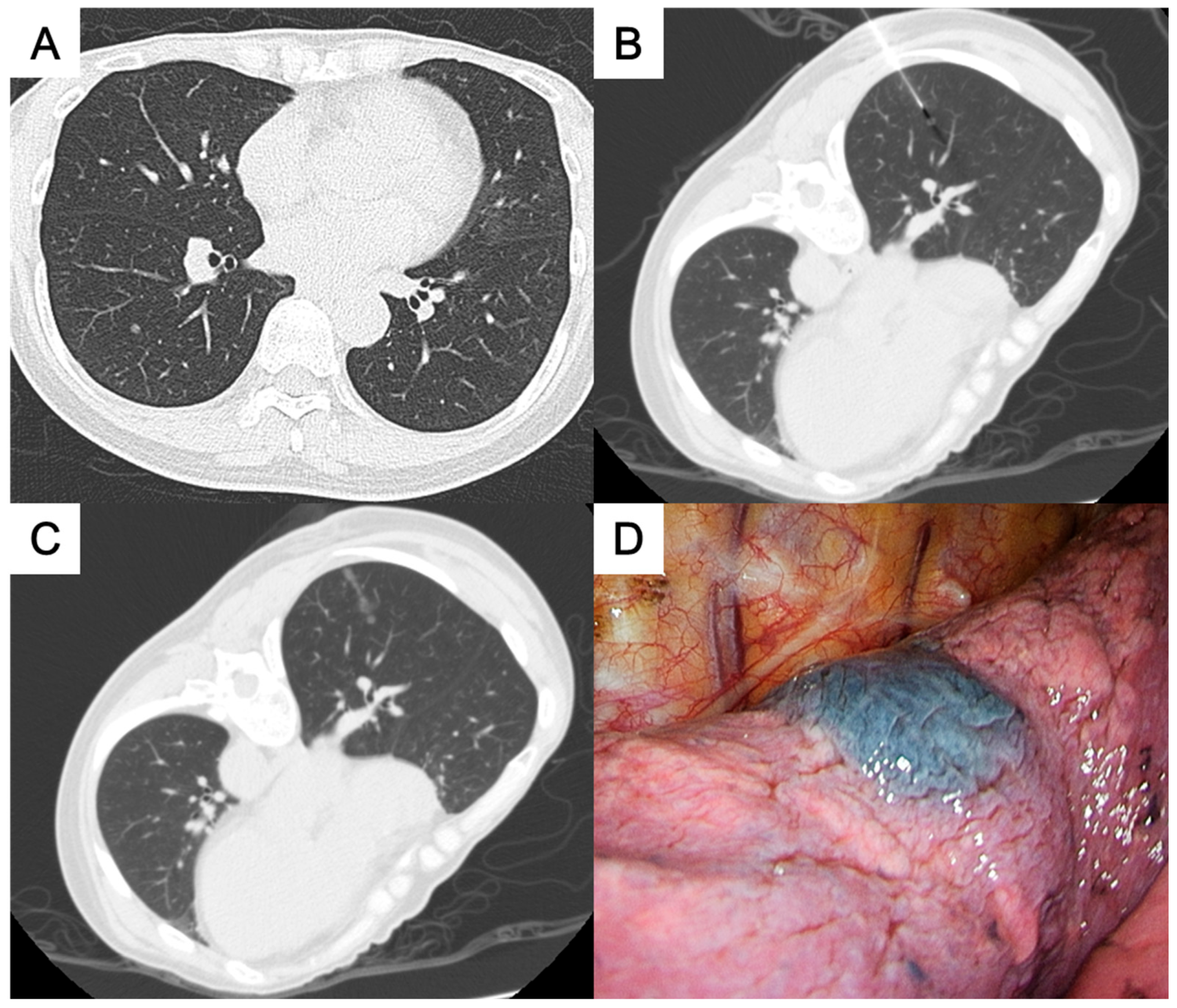
- For the perifissural nodules (Figure 1), we introduced the needle by the shortest way from the chest wall to the nodule and injected the PBD in the subpleural area. There is an alternative transfissural approach (Figure 2) to avoid pulmonary vessels, scapula, and ribs, with the dye retention in the subpleural area.
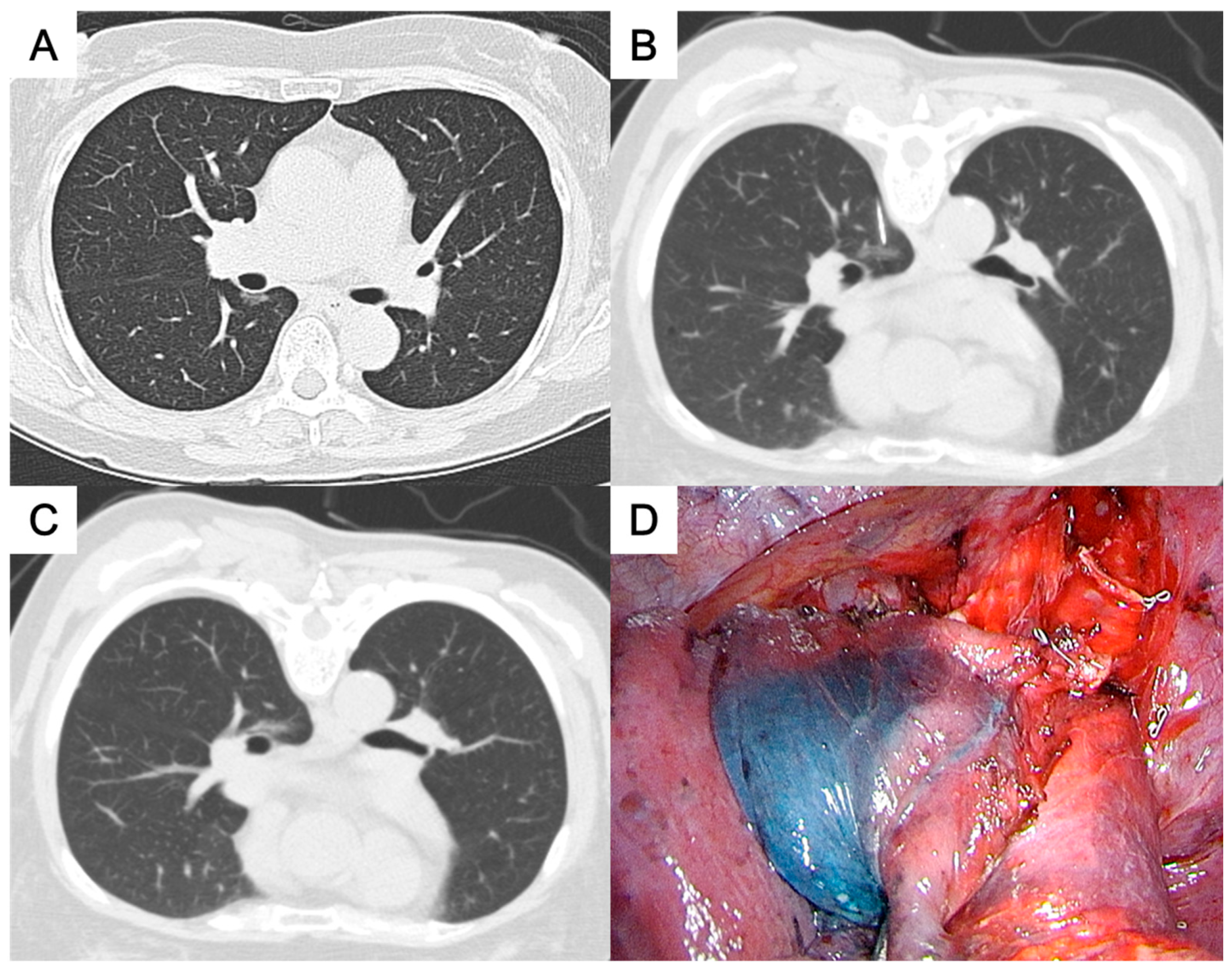
- For the paravertebral nodules (Figure 3), we introduced the needle by paraspinal approach from posterior chest wall with the tip placed within 1 cm to the nodule. PBD was then injected while withdraw the needle, leaving the dye retention in the needle pathway till the subpleural area.
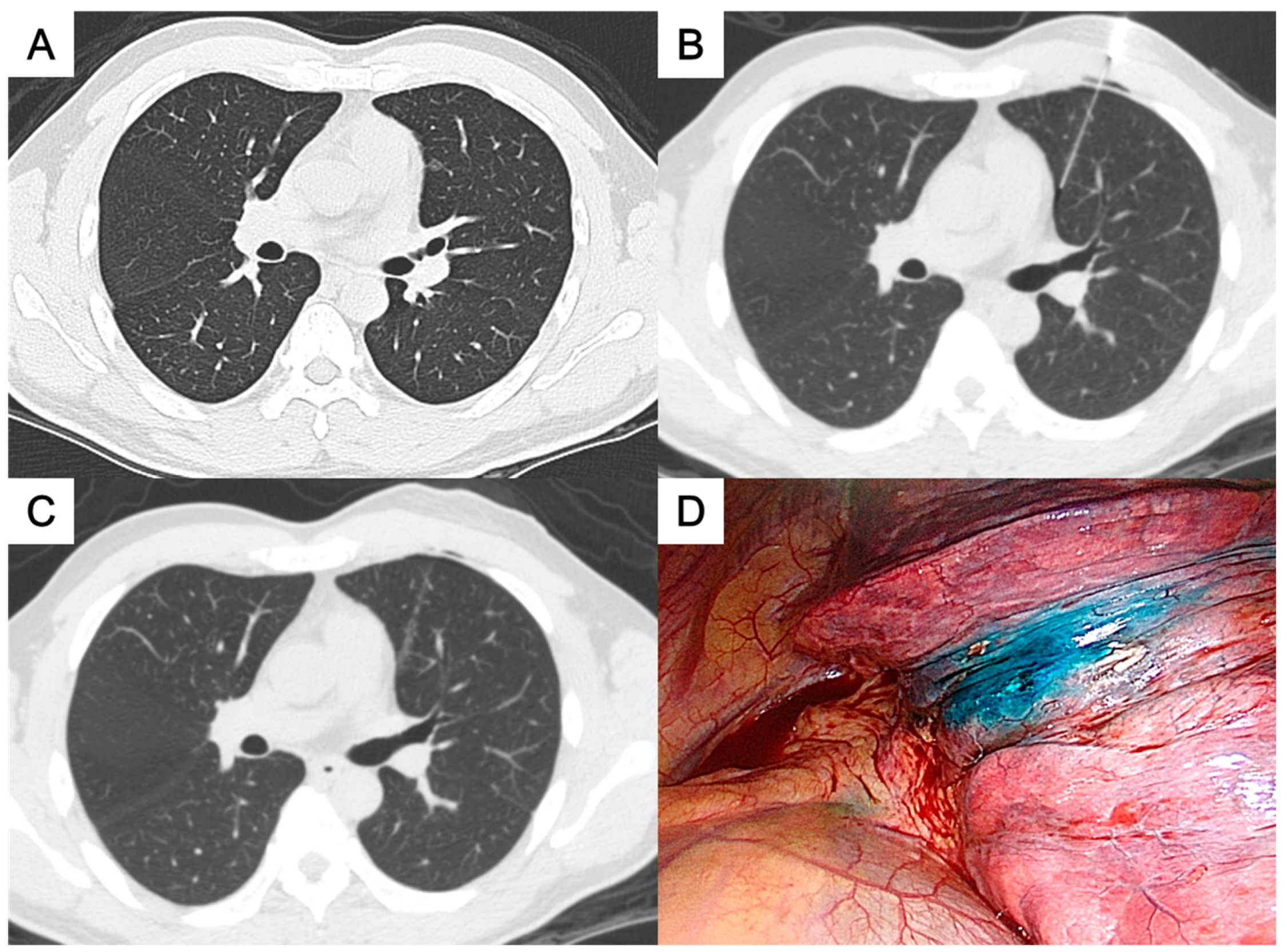
- For the paramediastinal nodules (Figure 4), we approached the nodule by the shortest way from the chest wall to the nodule, with the needle tip placed within 1 cm and relative medial side to the nodule. We then injected the PBD with the dye retention in the subpleural area.
- For the deep parenchymal nodules (Figure 5), the needle pathway was made by the shortest way from the chest wall to the nodule, while avoiding bony structures. After confirming the needle tip placed within 1 cm to the nodule, the PBD was injected while needle retraction until the subpleural area. The dye was then deposit in the needle pathway.
2.2. Video-Assisted Thoracoscopic Surgery (VATS ) After Localization
2.3. Statistical Analysis
3. Results
3.1. Clinical and Radiological Features
3.2. Localization Parameters, Complications, and Surgical Results
3.3. Pathological Reports
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CT | Computer Tomography |
| PBD | Patent Blue Dye |
| VATS | Video-Assisted Thoracoscopic Surgery |
| BMI | Body Mass Index |
| RUL | Right Upper Lobe |
| RML | Right Middle Lobe |
| RLL | Right Lower Lobe |
| LUL | Left Upper Lobe |
| LLL | Left Lower Lobe |
| MIA | Minimally Invasive Adenocarcinoma |
| AIS | Adenocarcinoma In Situ |
| AAH | Atypical Adenomatous Hyperplasia |
References
- Krochmal, R.; Arias, S.; Yarmus, L.; Feller-Kopman, D.; Lee, H. Diagnosis and management of pulmonary nodules. Expert Rev Respir Med 2014, 8, 677-691. [CrossRef]
- Suzuki, K.; Nagai, K.; Yoshida, J.; Ohmatsu, H.; Takahashi, K.; Nishimura, M.; Nishiwaki, Y. Video-Assisted Thoracoscopic Surgery for Small Indeterminate Pulmonary Nodules. Chest 1999, 115, 563-568. [CrossRef]
- McDermott, S.; Fintelmann, F.J.; Bierhals, A.J.; Silin, D.D.; Price, M.C.; Ott, H.C.; Shepard, J.-A.O.; Mayo, J.R.; Sharma, A. Image-guided Preoperative Localization of Pulmonary Nodules for Video-assisted and Robotically Assisted Surgery. RadioGraphics 2019, 39, 1264-1279. [CrossRef]
- Ichinose, J.; Kohno, T.; Fujimori, S.; Harano, T.; Suzuki, S. Efficacy and Complications of Computed Tomography-Guided Hook Wire Localization. The Annals of Thoracic Surgery 2013, 96, 1203-1208. [CrossRef]
- Hsu, H.-H.; Shen, C.-H.; Tsai, W.-C.; Ko, K.-H.; Lee, S.-C.; Chang, H.; Huang, T.-W. Localization of nonpalpable pulmonary nodules using CT-guided needle puncture. World Journal of Surgical Oncology 2015, 13. [CrossRef]
- Lizza, N.; Eucher, P.; Haxhe, J.-P.; De Wispelaere, J.-F.; Johnson, P.M.; Delaunois, L. Thoracoscopic resection of pulmonary nodules after computed tomographic–guided coil labeling. The Annals of Thoracic Surgery 2001, 71, 986-988. [CrossRef]
- Liu, L.; Zhang, L.J.; Chen, B.; Cao, J.M.; Lu, G.M.; Yuan, L.; Li, K.; Xu, J. Novel CT-guided coil localization of peripheral pulmonary nodules prior to video-assisted thoracoscopic surgery: a pilot study. Acta Radiologica 2014, 55, 699-706. [CrossRef]
- Lenglinger, F.X.; Schwarz, C.D.; Artmann, W. Localization of pulmonary nodules before thoracoscopic surgery: value of percutaneous staining with methylene blue. American Journal of Roentgenology 1994, 163, 297-300. [CrossRef]
- McConnell, P.I.; Feola, G.P.; Meyers, R.L. Methylene blue–stained autologous blood for needle localization and thoracoscopic resection of deep pulmonary nodules. Journal of Pediatric Surgery 2002, 37, 1729-1731. [CrossRef]
- Stephenson, J.A.; Mahfouz, A.; Rathinam, S.; Nakas, A.; Bajaj, A. A Simple and Safe Technique for CT Guided Lung Nodule Marking prior to Video Assisted Thoracoscopic Surgical Resection Revisited. Lung Cancer International 2015, 2015, 1-3. [CrossRef]
- Chen, J.-R.; Tseng, Y.-H.; Lin, M.-W.; Chen, H.-M.; Chen, Y.-C.; Chen, M.-C.; Lee, Y.-F.; Chen, J.-S.; Chang, Y.-C. Safety and efficacy of computed tomography-guided dye localization using patent blue V for single lung nodule for video-assisted thoracoscopic surgery: a retrospective study. Annals of Translational Medicine 2019, 7, 28-28. [CrossRef]
- Lin, M.-W.; Tseng, Y.-H.; Lee, Y.-F.; Hsieh, M.-S.; Ko, W.-C.; Chen, J.-Y.; Hsu, H.-H.; Chang, Y.-C.; Chen, J.-S. Computed tomography-guided patent blue vital dye localization of pulmonary nodules in uniportal thoracoscopy. The Journal of Thoracic and Cardiovascular Surgery 2016, 152, 535-544.e532. [CrossRef]
- Wang, Y.-Z.; Boudreaux, J.P.; Dowling, A.; Woltering, E.A. Percutaneous localisation of pulmonary nodules prior to video-assisted thoracoscopic surgery using methylene blue and TC-99. European Journal of Cardio-Thoracic Surgery 2010, 37, 237-238. [CrossRef]
- Choi, B.G.; Kim, H.H.; Kim, B.S.; Kim, K.T.; Shinn, K.S.; Moon, S.W. Pulmonary nodules: CT-guided contrast material localization for thoracoscopic resection. Radiology 1998, 208, 399-401. [CrossRef]
- Lee, N.K.; Park, C.M.; Kang, C.H.; Jeon, Y.K.; Choo, J.Y.; Lee, H.-J.; Goo, J.M. CT-Guided Percutaneous Transthoracic Localization of Pulmonary Nodules Prior to Video-Assisted Thoracoscopic Surgery Using Barium Suspension. Korean Journal of Radiology 2012, 13, 694. [CrossRef]
- Bellomi, M.; Veronesi, G.; Trifirò, G.; Brambilla, S.; Bonello, L.; Preda, L.; Casiraghi, M.; Borri, A.; Paganelli, G.; Spaggiari, L. Computed Tomography-Guided Preoperative Radiotracer Localization of Nonpalpable Lung Nodules. The Annals of Thoracic Surgery 2010, 90, 1759-1764. [CrossRef]
- Zuo, T.; Shi, S.; Wang, L.; Shi, Z.; Dai, C.; Li, C.; Zhao, X.; Ni, Z.; Fei, K.; Chen, C. Supplement CT-Guided Microcoil Placement for Localising Ground-glass Opacity (GGO) Lesions at “Blind Areas” of the Conventional Hook-Wire Technique. Heart, Lung and Circulation 2017, 26, 696-701. [CrossRef]
- Ko, K.-H.; Huang, T.-W.; Lee, S.-C.; Chang, W.-C.; Gao, H.-W.; Hsu, H.-H. A simple and efficient method to perform preoperative pulmonary nodule localization: CT-guided patent blue dye injection. Clinical Imaging 2019, 58, 74-79. [CrossRef]
- Chiang, H.; Chen, L.-K.; Hsieh, W.-P.; Tang, Y.-X.; Lo, C.-Y. Complications during CT-Guided Lung Nodule Localization: Impact of Needle Insertion Depth and Patient Characteristics. Diagnostics 2023, 13, 1881. [CrossRef]
- Tsai, T.-M.; Chiang, X.-H.; Liao, H.-C.; Tsou, K.-C.; Lin, M.-W.; Chen, K.-C.; Hsu, H.-H.; Chen, J.-S. Computed tomography-guided dye localization for deeply situated pulmonary nodules in thoracoscopic surgery. Annals of Translational Medicine 2019, 7, 31-31. [CrossRef]
- Kato, H.; Oizumi, H.; Suzuki, J.; Hamada, A.; Watarai, H.; Nakahashi, K.; Sadahiro, M. Thoracoscopic wedge resection and segmentectomy for small-sized pulmonary nodules. Journal of Visualized Surgery 2017, 3, 66-66. [CrossRef]
- Lin, C.-W.; Ko, H.-J.; Yang, S.-M.; Chen, Y.-C.; Ko, W.-C.; Huang, H.-C.; Chen, J.-S.; Chang, Y.-C. Computed tomography-guided dual localization with microcoil and patent blue vital dye for deep-seated pulmonary nodules in thoracoscopic surgery. Journal of the Formosan Medical Association 2019, 118, 979-985. [CrossRef]
| Value N(%) or mean (range) | |
| Age (years), Mean (range) | 57.4(32–74) |
| Sex | |
| Male | 11 (22.0%) |
| Female | 39 (78.0%) |
| Smoking status | |
| Never | 39 (78.0%) |
| Current or former | 11 (22.0%) |
| BMI, Mean (range) | 23 (17.4–29.7) |
| Nodular size (mm), Mean (range) | 10.3 (4.7–21.0) |
| Pulmonary lobe | |
| RUL | 16 (32.0%) |
| RML | 1 (2.0%) |
| RLL | 11 (22.0%) |
| LUL | 16 (32.0%) |
| LLL | 6 (12.0%) |
| Nodule attenuation | |
| Ground-glass opacity | 40 (80.0%) |
| Part solid | 4 (8.0%) |
| Solid | 6 (12.0%) |
| N(%) or mean (range) | |
| Nodule localization category | |
| Perifissural nodules | 13 (26.0%) |
| Paravertebral nodules | 20 (40%) |
| Paramediastinal nodules | 4 (8%) |
| Deep parenchymal nodules | 13 (26.0%) |
| Transfissural puncture | 11 (22.0%) |
| Nodular depth (mm) | 16.1 (0.1–52.2) |
| Needle pathway length (cm) | 7.7 (4.5–11.7) |
| Distance between the nodule and the dye (mm) | Median: 0.6; Mean: 1.6; Range (0–13.5) |
| Procedure time (minute) | 16 (8–26) |
| Time interval from localization to surgery (minute) | Median: 139; Mean: 270; Range (57–2641) |
| Complications | |
| Pneumothorax | 24 (48.0%) |
| Asymptomatic | 24 (48.0%) |
| Symptomatic | 0 (0.0%) |
| Focal parenchymal hemorrhage | 4 (8.0%) |
| Hemothorax | 0 (0.0%) |
| Hemoptysis | 0 (0.0%) |
| Allergic reaction | 0 (0.0%) |
| Failed marking on the visceral pleura | 0 (0.0%) |
| Surgical procedure | |
| Wedge resection | 25 (50.0%) |
| Segmentectomy | 19 (38.0%) |
| Lobectomy | 6 (12.0%) |
| OR (95% CI) | p value | |
| Smoking status | 1.60 (0.20–12.68) | 0.658 |
| BMI | 0.87 (0.67–1.13) | 0.294 |
| Nodular size (mm) | 1.24 (0.97–1.57) | 0.085 |
| Pulmonary lobes | 1.33 (0.78–2.27) | 0.301 |
| Attenuation of nodule | 1.75 (0.50–6.12) | 0.378 |
| Localization type | 1.81 (0.58–5.62) | 0.304 |
| Transfissural puncture | 3.24 (0.36–28.91) | 0.293 |
| Nodular depth (mm) | 0.93 (0.86–1.01) | 0.080 |
| Needle pathway length (cm) | 0.86 (0.51–1.50) | 0.637 |
| N (%) | |
| Malignant and premalignant lesions | 48 (96.0%) |
| Invasive adenocarcinoma | 35 (70.0%) |
| MIA | 6 (12.0%) |
| AIS | 4 (8.0%) |
| Squamous cell carcinoma | 1 (2.0%) |
| AAH | 2 (4.0%) |
| Metastasis | 0 (0%) |
| Benign lesions | |
| Chronic granulomatous inflammation | 2 (4%) |
| Fibrosis | 0 (0%) |
| Intrapulmonary lymph node | 0 (0%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




