Submitted:
15 April 2025
Posted:
16 April 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
Study Objectives
2. Methods
2.1. Study Design and Participants
2.2. Ethical Considerations and Recruitment
2.3. Variables and Measurements
- Root mean square of successive differences (rMSSD): A marker of parasympathetic nervous system activity and short-term HRV.
- Percentage of successive RR intervals differing by more than 50 ms (PNN50) and 20 ms (PNN20): Indicators of vagal tone and cardiac autonomic flexibility.
- Low-frequency to high-frequency ratio (LF/HF): Reflects autonomic balance between sympathetic and parasympathetic systems.
- SD1/SD2 ratio: Nonlinear HRV parameter representing autonomic adaptability and resilience.
- Cuestionario para la Evaluación del Síndrome de Quemarse por el Trabajo (CESQT): This tool measures four dimensions of burnout: work engagement (Ilusión por el Trabajo, IT), psychological exhaustion (Desgaste Psíquico, DP), indolence (Indolencia, IN), and guilt (Culpa, CU). This instrument was chosen as the primary burnout measure due to its inclusion of dimensions particularly relevant to healthcare professionals [11].
- Maslach Burnout Inventory (MBI): Assesses emotional exhaustion (EE), depersonalization (DP), and professional inefficacy (PI) [12].
- Professional Quality of Life Scale (ProQOL): Measures compassion satisfaction (CS), secondary traumatic stress (STS), and burnout (BO) [13].
- State-Trait Anxiety Inventory (STAI): Includes two subscales assessing state anxiety (STAI-AE) and trait anxiety (STAI-AR), providing insight into acute and chronic stress levels [14].
2.4. Statistical Analysis
3. Results
3.1. Burnout, Anxiety, and HRV Metrics
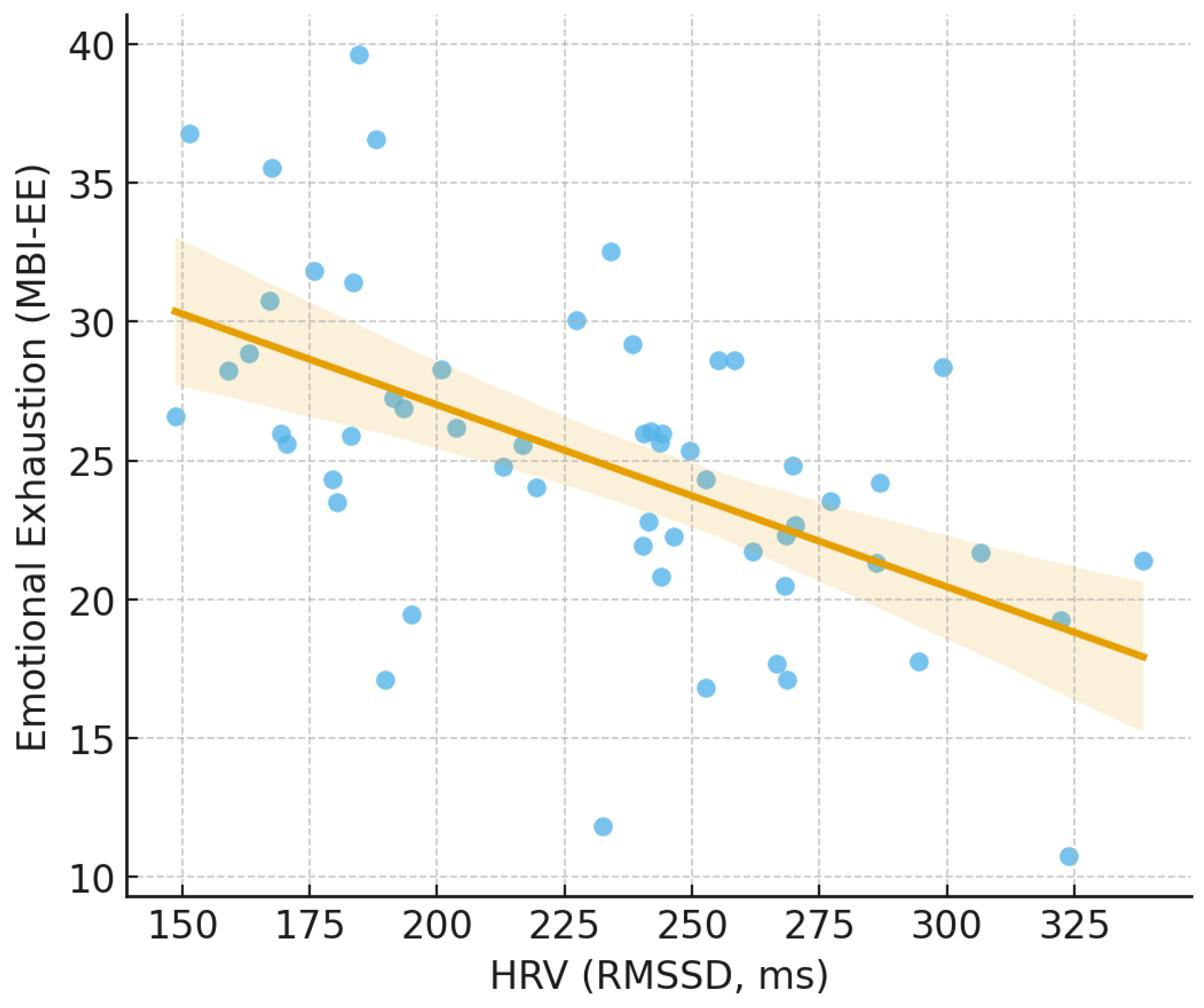
3.2. Correlations Between HRV, Stress, and Burnout
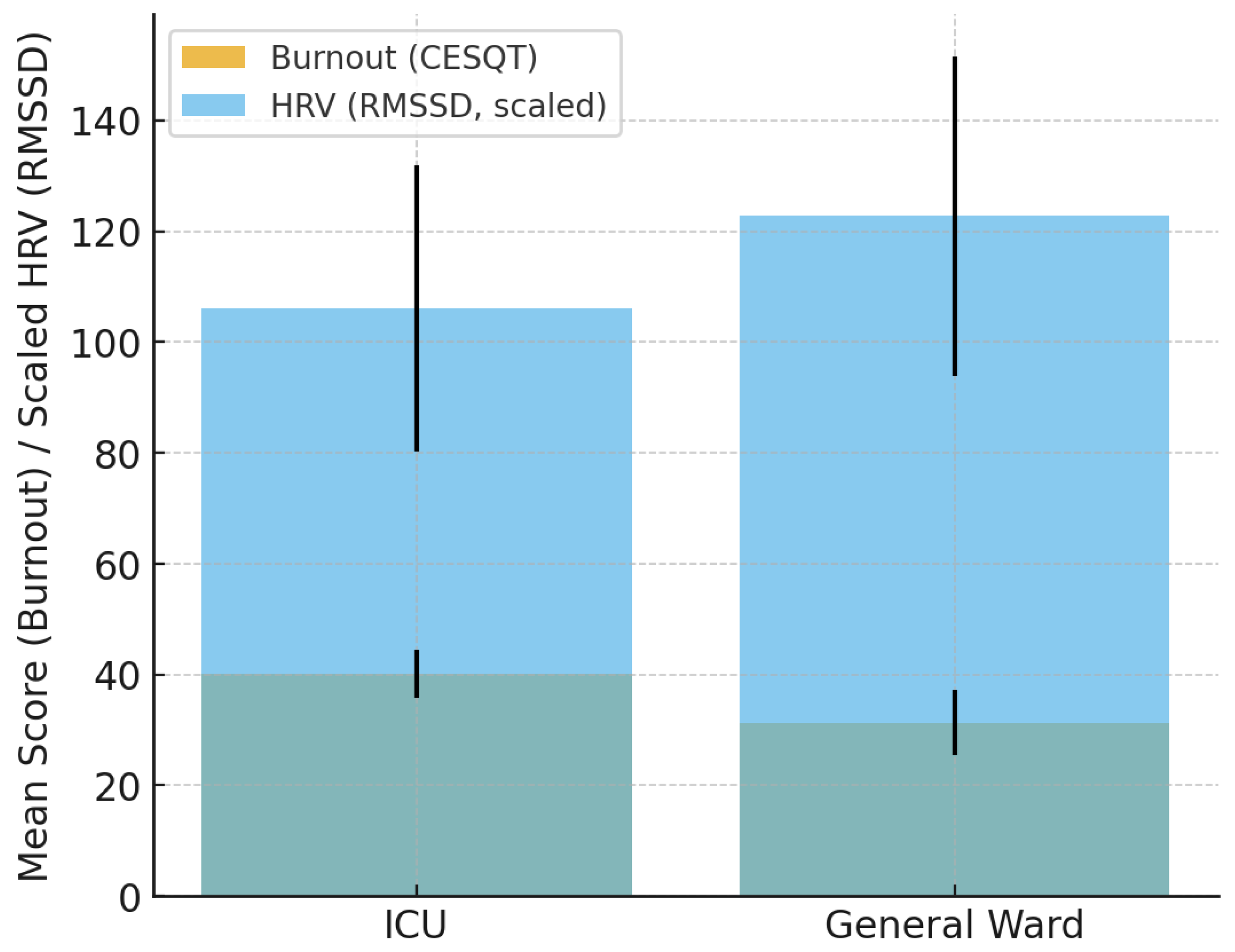
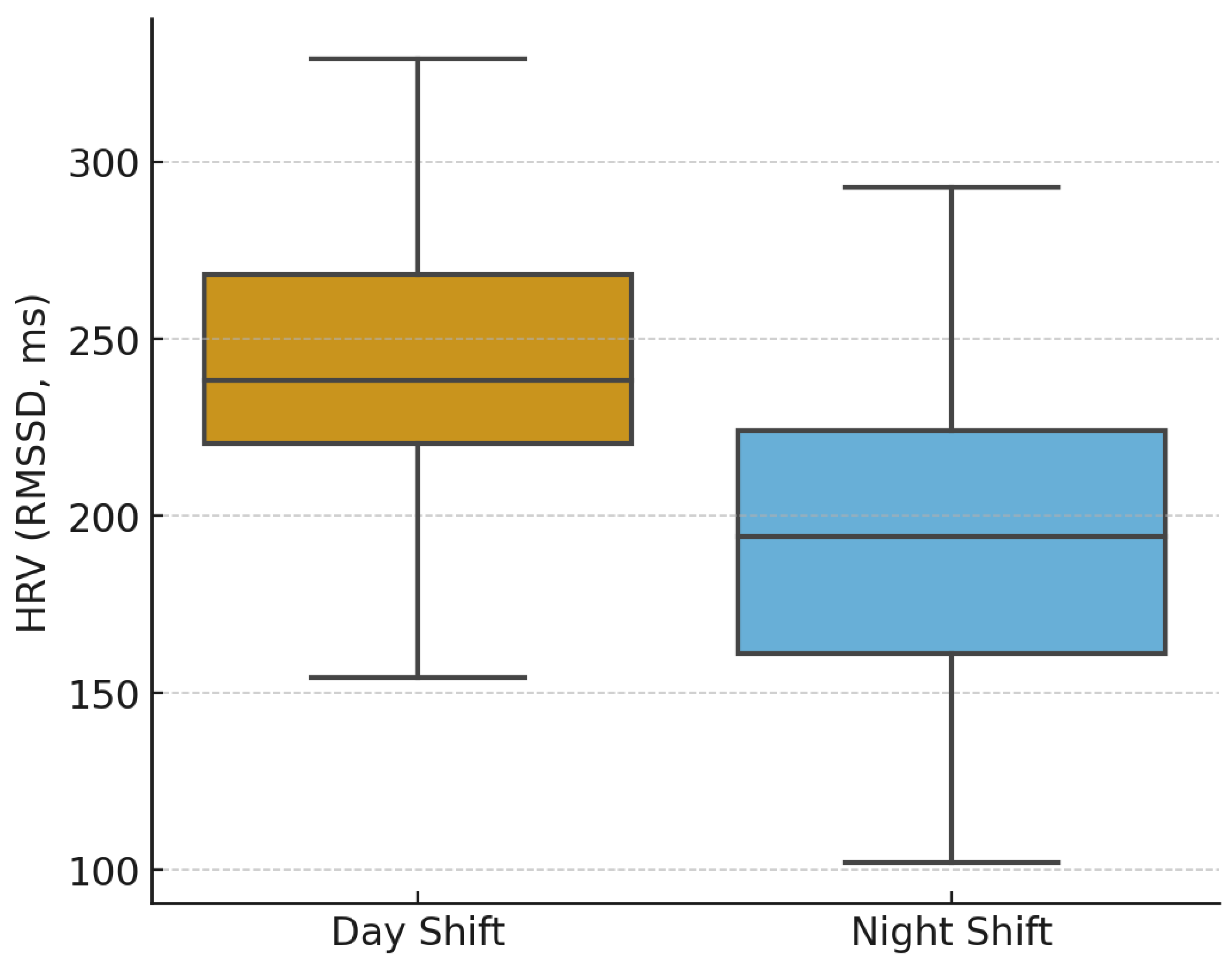
3.3. Workplace and Shift-Related Differences in HRV and Burnout
3.4. Predictive Model for Burnout Risk
4. Discussion
4.1. Implications for Occupational Health and Clinical Practice
4.2. Limitations and Future Directions
5. Conclusion
Funding
Authors’ Contributions
Data Availability
Biometric Data
Acknowledgments
Competing interests:
Appendix A
- Cuestionario para la Evaluación del Síndrome de Quemarse por el Trabajo (CESQT)
- Maslach Burnout Inventory (MBI)
- Professional Quality of Life Scale (ProQOL)
- State-Trait Anxiety Inventory (STAI)
List of abbreviations
References
- Nagle E, Griskevica I, Rajevska O, Ivanovs A, Mihailova S, Skruzkalne I. Factors affecting healthcare workers burnout and their conceptual models: scoping review. BMC psychology. 2024. p. 637. [CrossRef]
- Antonsdottir I, Rushton CH, Nelson KE, Heinze KE, Swoboda SM, Hanson GC. Burnout and moral resilience in interdisciplinary healthcare professionals. J Clin Nurs. 2022;31: 196–208. [CrossRef]
- Soares JP, Lopes RH, De Souza Mendonça PB, Vieira Silva CRD, Martins Rodrigues CCF, De Castro JL. Use of the Maslach Burnout Inventory Among Public Health Care Professionals: Protocol for a Scoping Review. JMIR Research Protocols. JMIR Publications Inc.; 2022. [CrossRef]
- Umaña Ruiz C, Gómez Ortiz V, Gil-Monte PR, Gil-Laorden P, Camacho SS. Psychometric properties of the SBI, Professional Disenchantment version (SBI-DP), in a multi-occupational Colombian sample. Rev Latinoam Psicol. 2023;55: 253–262. [CrossRef]
- Dalmeida KM, Masala GL. Hrv features as viable physiological markers for stress detection using wearable devices. Sensors. 2021;21. [CrossRef]
- Järvelin-Pasanen S, Sinikallio S, Tarvainen MP. Heart rate variability and occupational stress-systematic review.
- Rubio-López A, Sierra-Puerta T, Navas AR. Integrating Heart Rate Variability and Psychometric Assessments to Evaluate Stress and Burnout in ICU Nursing Staff: A Pilot Study.
- Folkard S, Folkard S, Marek T, Noworol C. Health, well-being and burnout of ICU nurses on 12- and 8-h shifts. Work Stress. 1996;10: 251–256. [CrossRef]
- Andrade-Méndez B, Arias-Torres DO, Gómez-Tovar LO. Alarm Fatigue in the Intensive Care Unit: Relevance and Response Time. Enferm Intensiva. 2020;31: 147–153. [CrossRef]
- Liaw SY, Sutini, Chua WL, Tan JZ, Levett-Jones T, Ashokka B, et al. Desktop Virtual Reality Versus Face-to-Face Simulation for Team-Training on Stress Levels and Performance in Clinical Deterioration: a Randomised Controlled Trial. J Gen Intern Med. 2023;38: 67–73. [CrossRef]
- Umaña Ruiz C, Gómez Ortiz V, Gil-Monte PR, Gil-Laorden P, Camacho SS. Psychometric properties of the SBI, Professional Disenchantment version (SBI-DP), in a multi-occupational Colombian sample. Rev Latinoam Psicol. 2023;55: 253–262. [CrossRef]
- Bravo DM, Suárez-Falcón JC, Bianchi JM, Segura-Vargas MA, Ruiz FJ. Psychometric properties and measurement invariance of the maslach burnout inventory–general survey in Colombia. Int J Environ Res Public Health. 2021;18. [CrossRef]
- Dwyer M, Alt M, Brooks J, Katz H, Poje A. Burnout and Compassion Satisfaction: Survey Findings of Healthcare Employee Wellness During COVID-19 Pandemic using ProQOL. Kans J Med. 2021;14: 121–127. [CrossRef]
- Sangrà PS, Ribeiro TC, Esteban-Sepúlveda S, Pagès EG, Barbeito BL, Llobet JA, et al. Mental health assessment of Spanish frontline healthcare workers during the SARS-CoV-2 pandemic. Med Clin (Barc). 2022;159: 268–277. [CrossRef]
- Meredith LS, Bouskill K, Chang J, Larkin J, Motala A, Hempel S. Predictors of burnout among US healthcare providers: a systematic review. BMJ Open. 2022;12. [CrossRef]
- Thielmann B, Hartung J, Böckelmann I. Objective assessment of mental stress in individuals with different levels of effort reward imbalance or overcommitment using heart rate variability: a systematic review. Systematic Reviews. BioMed Central Ltd; 2022. [CrossRef]
- Shah SG, Ahmed A, Ahmed A, Ikram K, Mirza A, Ahmed S, et al. Assessment of Occupational Based Stress and Internal Coherence Related with Quality of Life Through Heartrate Variability (HRV) - A Cross Sectional Study. Journal of Health and Rehabilitation Research. 2024;4: 1591–1596. [CrossRef]
- Hu Z, Cao X, Jing P, Zhang B, Shi Y, Siegrist J, et al. Work stress and changes in heart rate variability among employees after first acute coronary syndrome: a hospital-based longitudinal cohort study. Front Public Health. 2024;12. [CrossRef]
- Tomes C, Schram B, Orr R. Relationships Between Heart Rate Variability, Occupational Performance, and Fitness for Tactical Personnel: A Systematic Review. Frontiers in Public Health. Frontiers Media S.A.; 2020. [CrossRef]
- Dall’ora C, Ejebu OZ, Ball J, Griffiths P. Shift work characteristics and burnout among nurses: cross-sectional survey. Occup Med (Chic Ill). 2023;73: 199–204. [CrossRef]
- Varghese B, Joseph CM, Al- Akkam AAA, AL-Balawi RMOAM, Swallmeh E, Singh K. Nurse’s experience working 12-hour shift in a tertiary level hospital in Qatar: a mixed method study. BMC Nurs. 2023;22. [CrossRef]
- Carvalho SP, Correa F, En Macau E, Santos L Dos, En E, Biomed M, et al. Stress Level of Critical Care Nurses: Evaluation by Heart Rate Variability Mini Review Open Access. Biomed J Sci &Tech Res. 4. [CrossRef]
- Tsou MT, Pai TP, Chiang TM, Huang WH, Lin HM, Lee SC. Burnout and metabolic syndrome among different departments of medical center nurses in Taiwan-Cross-sectional study and biomarker research. J Occup Health. 2021;63. [CrossRef]
- Wilton AR, Sheffield K, Wilkes Q, Chesak S, Pacyna J, Sharp R, et al. The Burnout PRedictiOn Using Wearable aNd ArtIficial IntelligEnce (BROWNIE) study: a decentralized digital health protocol to predict burnout in registered nurses. BMC Nurs. 2024;23. [CrossRef]
- Danhof-Pont MB, van Veen T, Zitman FG. Biomarkers in burnout: A systematic review. Journal of Psychosomatic Research. 2011. pp. 505–524. [CrossRef]
- Penz M, Wekenborg MK, Pieper L, Beesdo-Baum K, Walther A, Miller R, et al. The Dresden Burnout Study: Protocol of a prospective cohort study for the bio-psychological investigation of burnout. Int J Methods Psychiatr Res. 2018;27. [CrossRef]
- Cohen C, Pignata S, Bezak E, Tie M, Childs J. Workplace interventions to improve well-being and reduce burnout for nurses, physicians and allied healthcare professionals: a systematic review. BMJ Open. 2023;13. [CrossRef]
- Orosz A, Federspiel A, Eckert A, Seeher C, Dierks T, Tschitsaz A, et al. Exploring the effectiveness of a specialized therapy programme for burnout using subjective report and biomarkers of stress. Clin Psychol Psychother. 2021;28: 852–861. [CrossRef]
- Alameri F, Aldaheri N, Almesmari S, Basaloum M, Albeshr NA, Simsekler MCE, et al. Burnout and Cardiovascular Risk in Healthcare Professionals During the COVID-19 Pandemic. Front Psychiatry. 2022;13. [CrossRef]
- Marković S, Kostić O, Terzić-Supic Z, Tomic Mihajlovic S, Milovanović J, Radovanovic S, et al. Exposure to Stress and Burnout Syndrome in Healthcare Workers, Expert Workers, Professional Associates, and Associates in Social Service Institutions. Medicina (Lithuania). 2024;60. [CrossRef]
| Variable | Total (%) | ICU (%) | General Ward (%) |
|---|---|---|---|
| Job Role | |||
| Nurse (DUE) | 54.4 | ||
| Assistant Nurse (TCAE) | 45.6 | ||
| Work Unit | |||
| ICU | 52.6 | ||
| General Ward | 47.4 | ||
| Work Shift | |||
| Day shift | 56.1 | ||
| Night shift | 43.9 | ||
| Shift Duration | |||
| 8 hours | 49.1 | ||
| 12 hours | 50.9 | ||
| Mental Health Conditions | |||
| Anxiety | 36.8 | 43.33 | 29.63 |
| Depression | 10.5 | 6.67 | 14.81 |
| Suicidal Ideation | 28.1 | 30.0 | 25.93 |
| Medication Use | |||
| Anxiolytics | 26.3 | 16.67 | 37.04 |
| Antidepressants | 19.3 | 26.67 | 11.11 |
| Lifestyle Factors | |||
| Regular Physical Activity | 31.6 | 13.33 | 18.52 |
| Smokers | 21.1 | 66.67 | 74.07 |
| Caffeine Consumption | 78.9 | 13.33 | 11.11 |
| Variable | Total (Mean ± SD) |
ICU (Mean ± SD) |
General Ward (Mean ± SD) |
|---|---|---|---|
| RMSSD (ms) | 229.77 ± 104.86 | 210.33 ± 117.69 | 251.37 ± 85.52 |
| PNN50 (%) | 59.14 ± 28.67 | 48.87 ± 28.91 | 70.56 ± 24.1 |
| LF/HF Ratio | 0.89 ± 1.24 | 1.23 ± 1.62 | 0.52 ± 0.34 |
| SD1/SD2 Ratio | 0.83 ± 0.23 | 0.77 ± 0.26 | 0.89 ± 0.16 |
| CESQT – Burnout Index | 35.42 ± 5.06 | 36.43 ± 5.34 | 34.3 ± 4.57 |
| CESQT – Work Engagement (IT) | 9.82 ± 1.39 | 9.8 ± 1.49 | 9.85 ± 1.29 |
| CESQT – Psychological Exhaustion (DP) | 13.93 ± 2.45 | 14.17 ± 2.53 | 13.67 ± 2.37 |
| CESQT – Indolence (IN) | 11.32 ± 3.78 | 12.07 ± 4.08 | 10.48 ± 3.3 |
| CESQT – Guilt (CU) | 1.86 ± 1.43 | 1.67 ± 0.76 | 2.07 ± 1.92 |
| MBI – Emotional Exhaustion | 23.02 ± 8.73 | 25.33 ± 8.47 | 20.44 ± 8.43 |
| MBI – Depersonalization | 7.7 ± 4.0 | 8.63 ± 3.92 | 6.67 ± 3.9 |
| MBI – Personal Accomplishment | 25.18 ± 5.08 | 24.07 ± 4.99 | 26.41 ± 4.99 |
| STAI – State Anxiety | 42.86 ± 10.24 | 45.33 ± 10.53 | 40.11 ± 9.35 |
| STAI – Trait Anxiety | 32.21 ± 8.88 | 33.1 ± 9.44 | 31.22 ± 8.26 |
| HRV Parameter | Burnout/Stress Variable | Mean ± SD (HRV) | Mean ± SD (Burnout) | Spearman’s ρ | P Value |
|---|---|---|---|---|---|
| RMSSD | Depression | 229.77 ± 104.86 | 10.50 ± 2.80 | -0.281 | 0.034 |
| RMSSD | Suicidal Ideation | 229.77 ± 104.86 | 28.10 ± 5.20 | -0.297 | 0.025 |
| LF/HF | Emotional Exhaustion | 0.89 ± 1.24 | 23.02 ± 8.72 | 0.324 | 0.014 |
| SD1/SD2 | Indolence | 0.83 ± 0.23 | 11.32 ± 3.78 | -0.316 | 0.017 |
| Poincaré Area | Depersonalization | 15.30 ± 4.50 | 9.13 ± 4.98 | -0.281 | 0.034 |
| Comparison | Higher in | Mean ± SD (Higher Group) | Mean ± SD (Lower Group) | p-Value |
|---|---|---|---|---|
| RMSSD (ICU vs. Ward) | Ward | 210.50 ± 98.30 | 245.20 ± 110.70 | 0.037 |
| Emotional Exhaustion (ICU vs. Ward) | Ward | 25.80 ± 7.90 | 20.60 ± 8.40 | 0.041 |
| Burnout Index (Night vs. Day Shift) | Day Shift | 37.10 ± 4.20 | 33.40 ± 5.10 | 0.028 |
| HRV LF/HF Ratio (Night vs. Day Shift) | Day Shift | 1.02 ± 0.89 | 0.78 ± 0.65 | 0.039 |
| PNN50 (12h vs. 8h Shift) | 12h Shift | 62.30 ± 9.80 | 55.70 ± 11.20 | 0.044 |
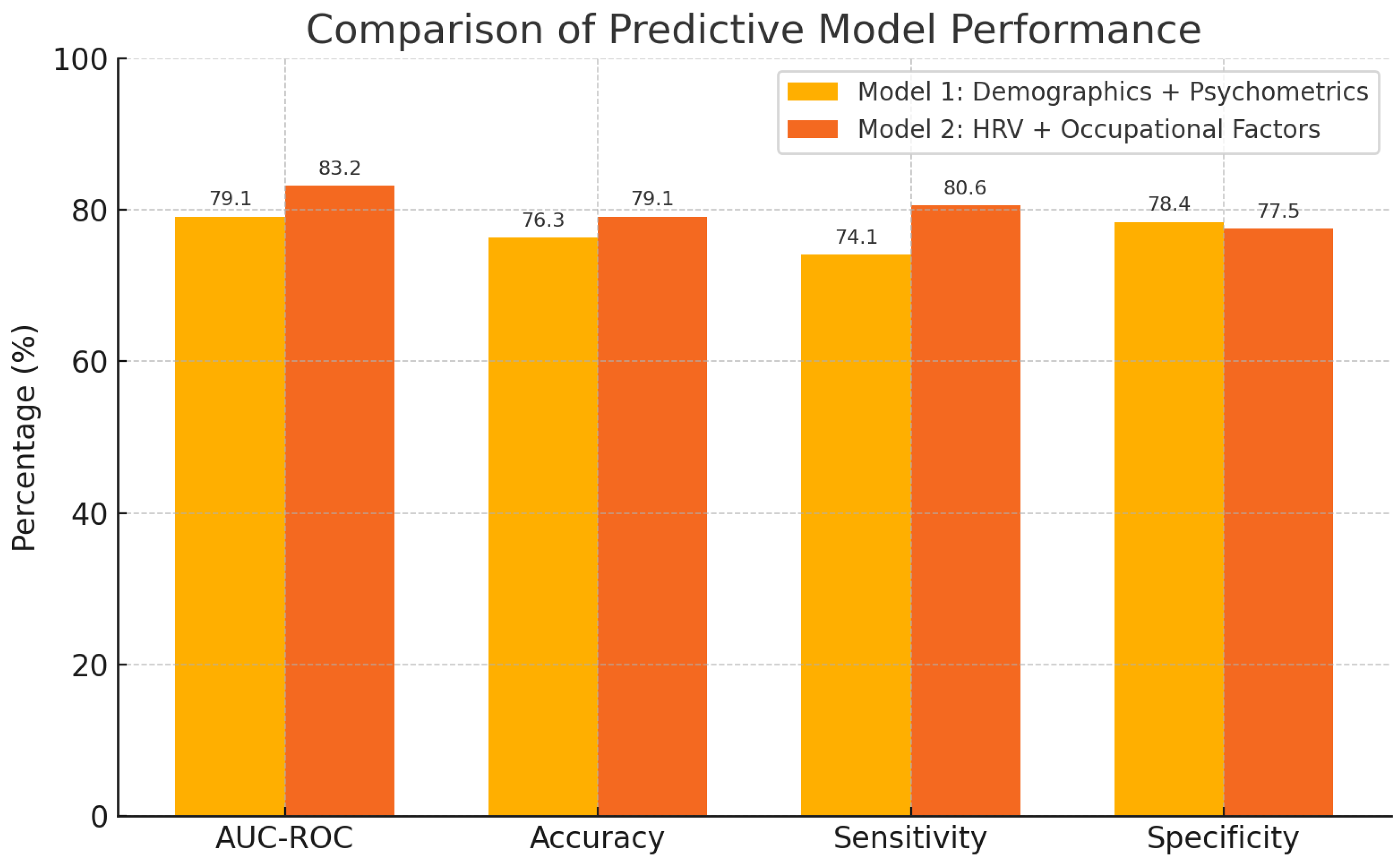
| Metric | Model 1 | Model 2 |
|---|---|---|
| AUC-ROC | 0.791 | 0.832 |
| Accuracy (%) | 76.3 | 79.1 |
| Sensitivity (%) | 74.1 | 80.6 |
| Specificity (%) | 78.4 | 77.5 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




