Submitted:
08 April 2025
Posted:
08 April 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
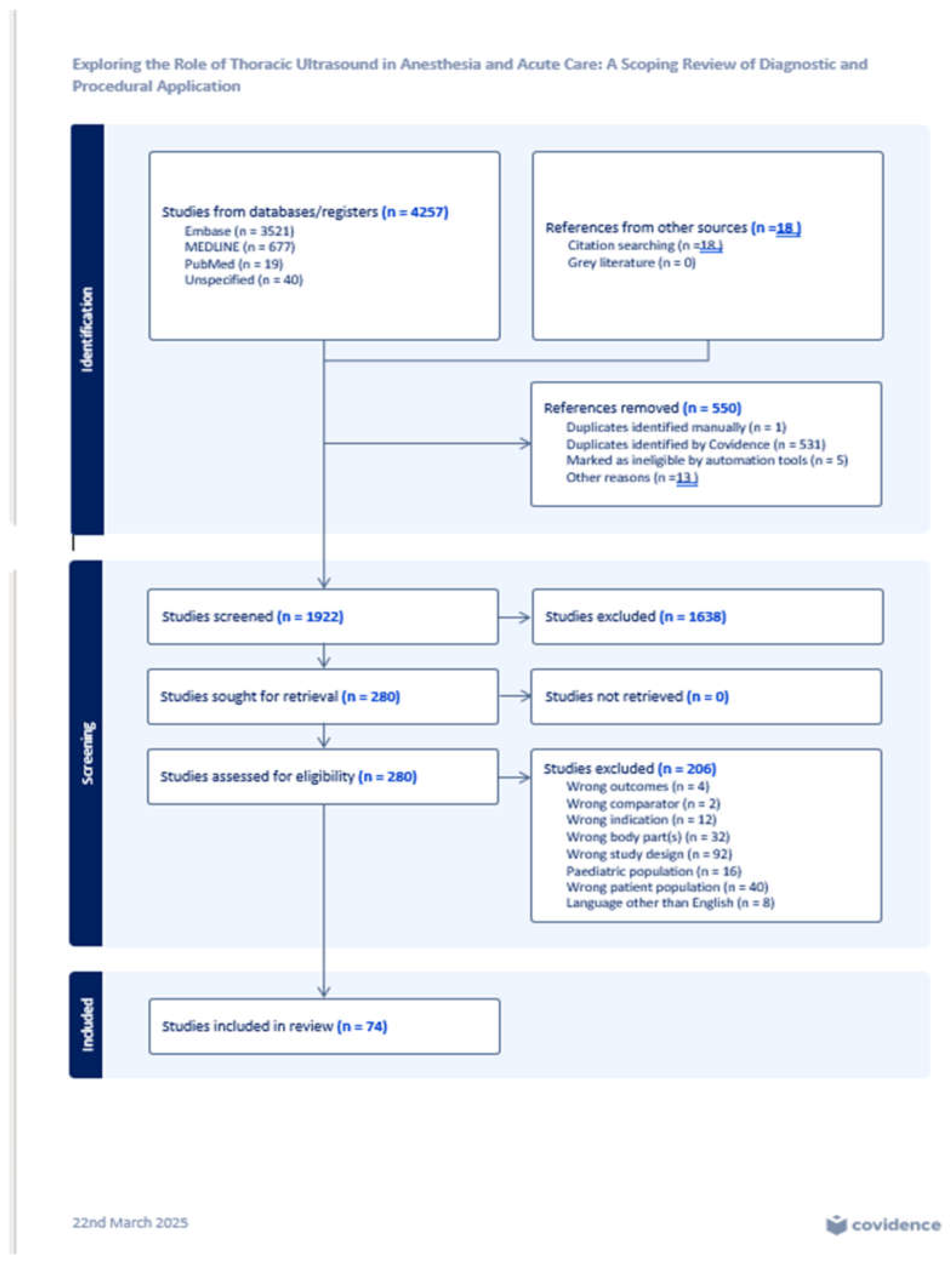
2. Methods
2.1. Search Strategy
2.2. Study Selection
2.3. Bias Assessment
3. Results
3.1. Study Characteristics
3.1.1. Scope of Thoracic Pathologies Assessed
- Pleural effusion
- Pneumothorax
- Pulmonary edema
- Pneumonia
- Acute respiratory distress syndrome
- COVID-19-related lung disease
- Thoracentesis
- Central venous catheter insertion
- Intubation confirmation
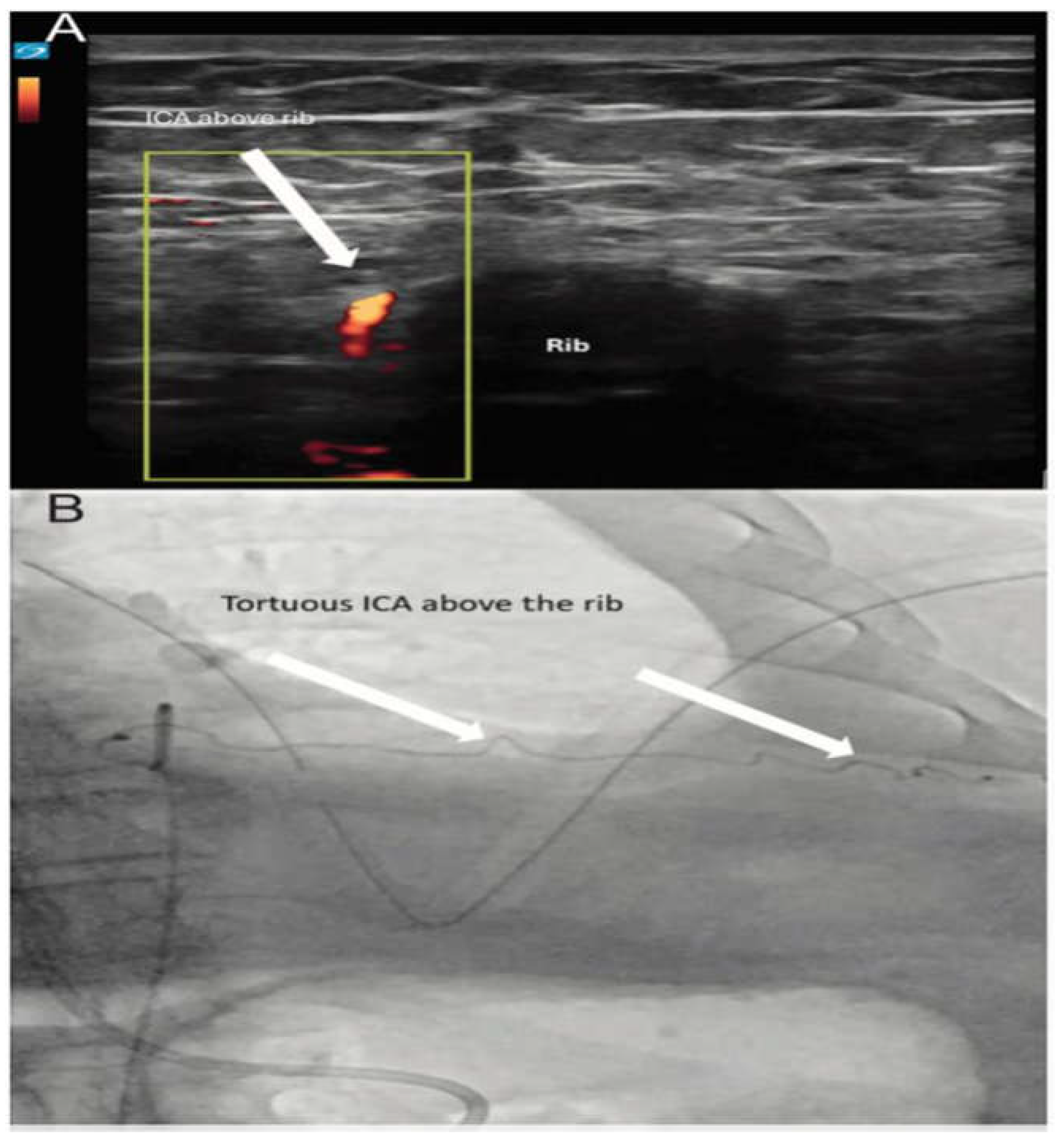
- Intercostal artery localization via Doppler
3.2. Diagnostic Applications
3.3. Procedural Applications
4. Discussion
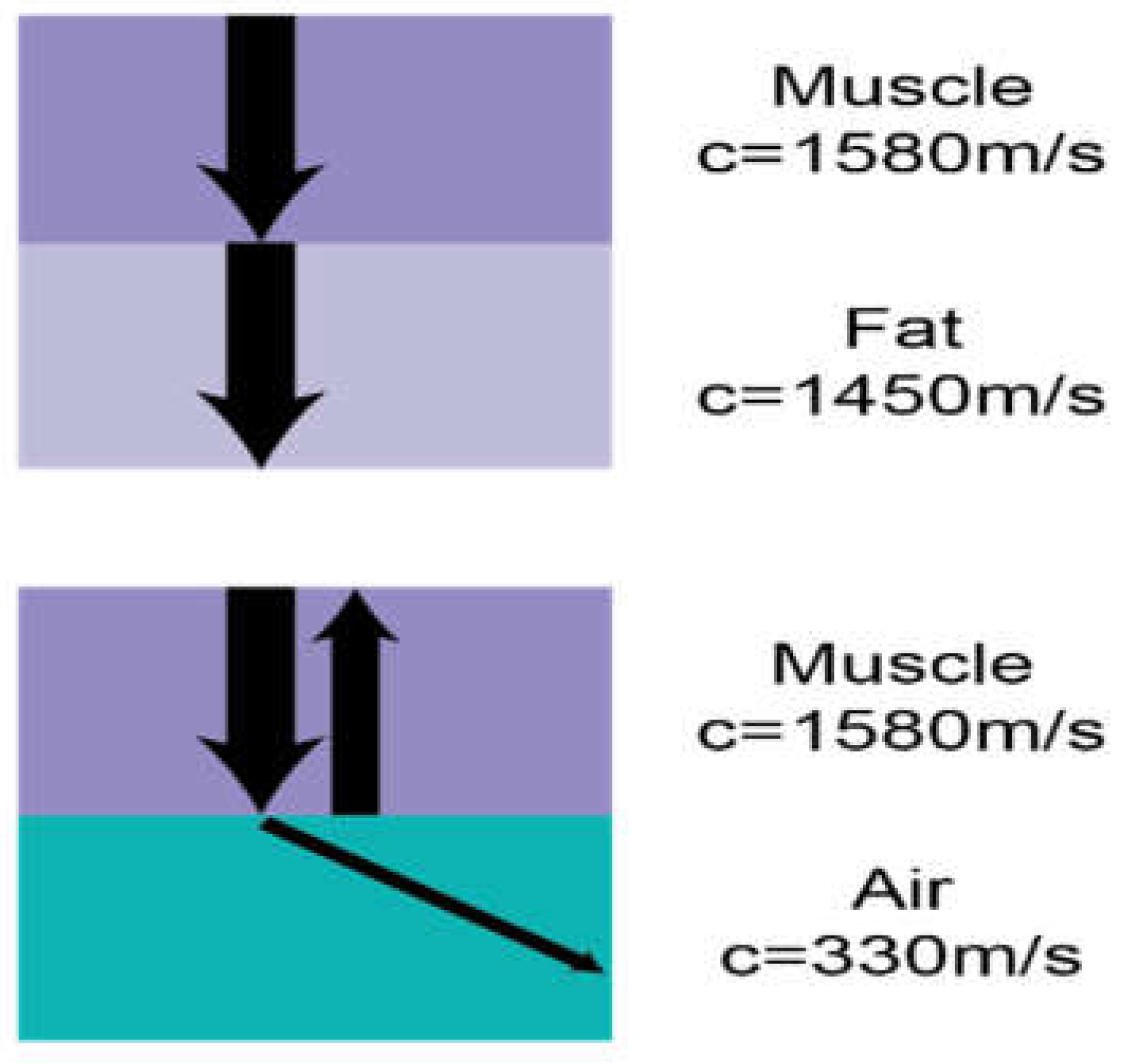
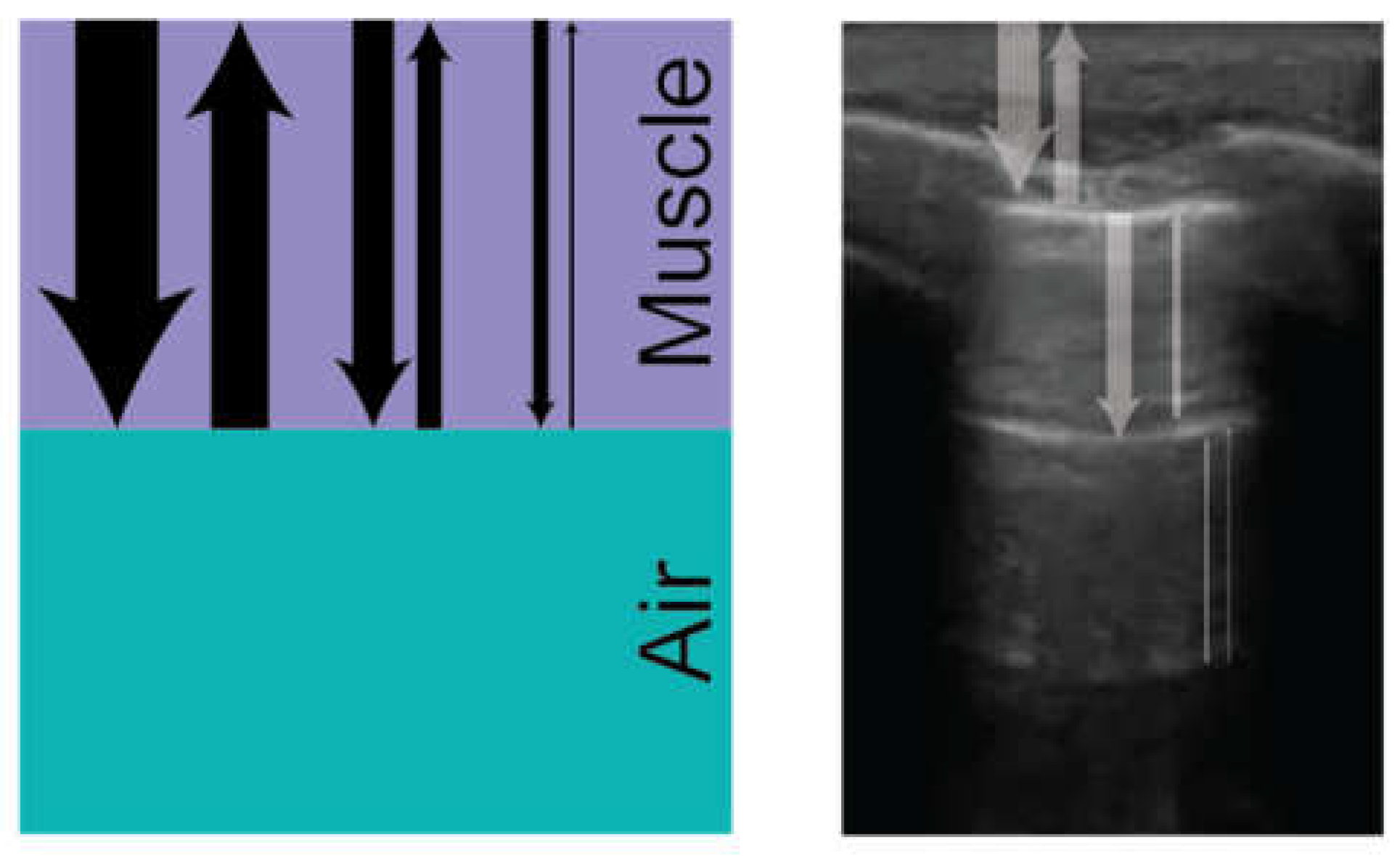
4.1. Physics of Lung Ultrasound
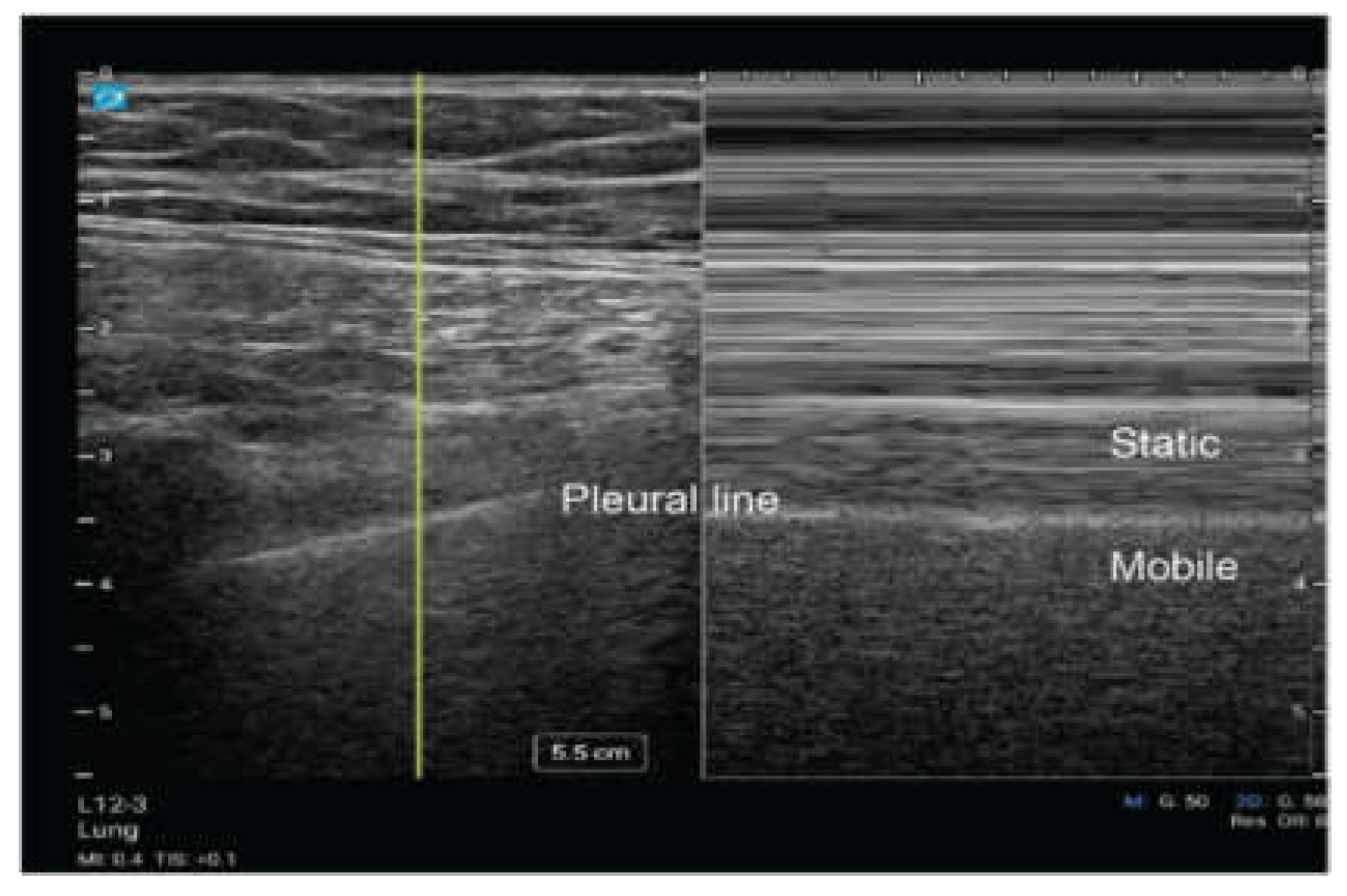
4.2. Normal LUS Findings
A-Lines
Lung Sliding
Lung Pulse
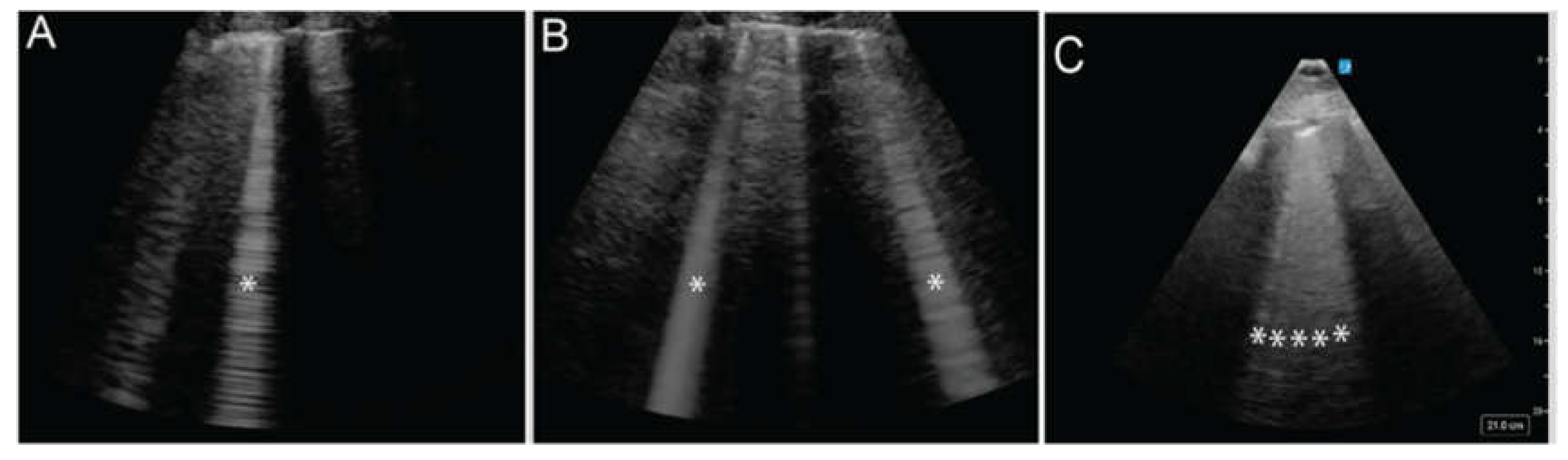
B Lines
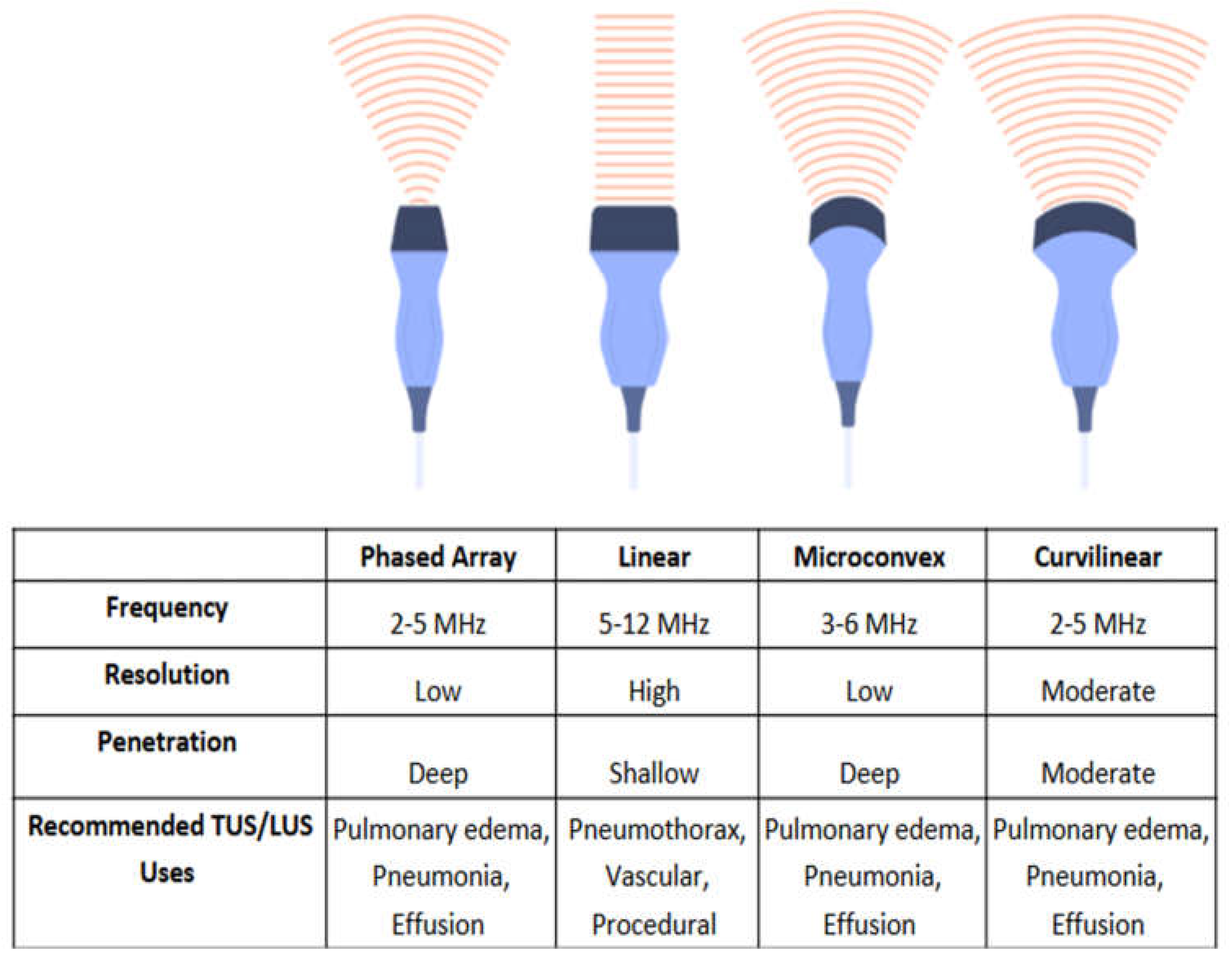
4.3. Ultrasound Machine Configuration
Linear Transducers
Phased-Array Transducers
Curvilinear (Convex) Transducers
Microconvex Transducers
5. Procedural Uses of Thoracic Ultrasound
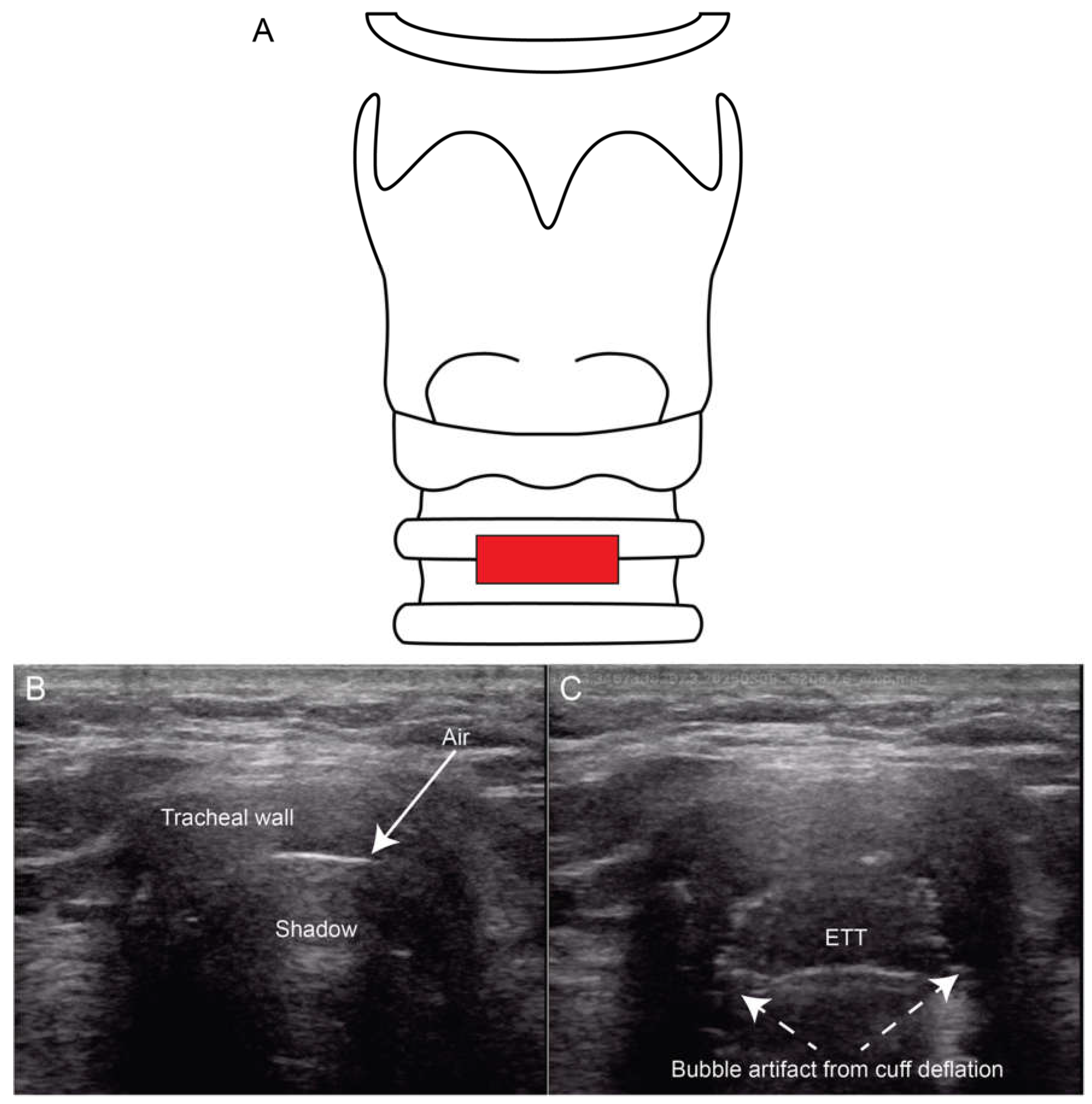
5.1. Intubation Assessment
Future Directions
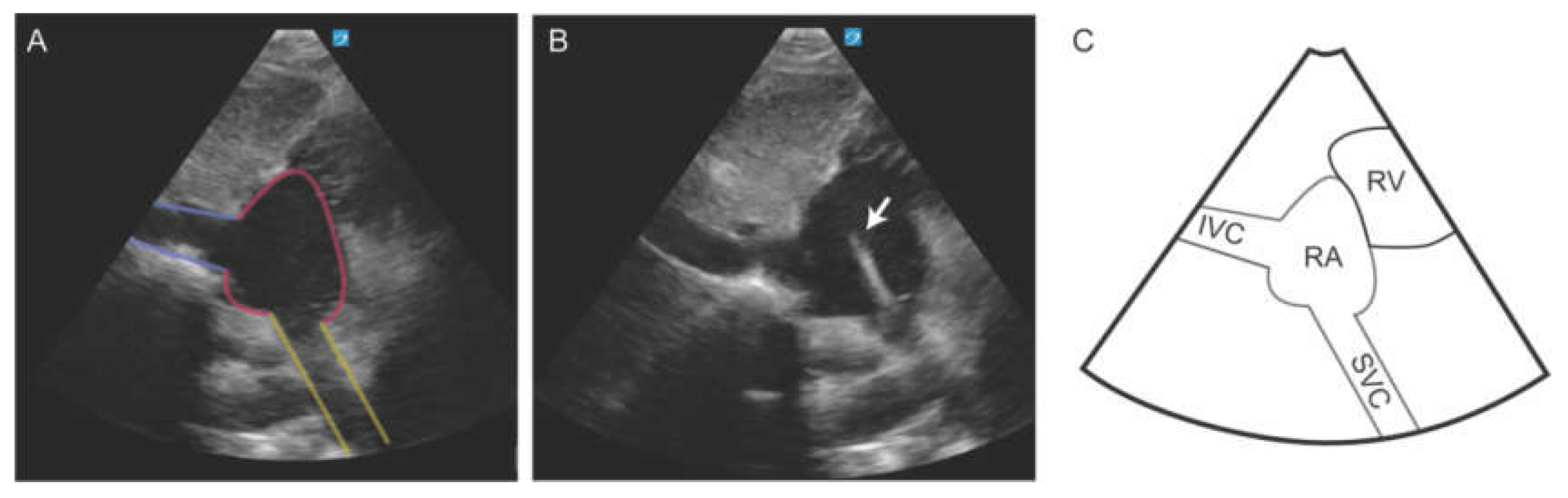
5.2. Central Venous Catheter Placement
Future Directions
5.3. Thoracentesis and Percutaneous Chest Tube Placement
6. Diagnostic uses of LUS
6.1. Pneumothorax
6.2. Pulmonary Edema
6.3. Pneumonia and Empyema
6.4. Pleural Effusion
| Condition | Modality | Sensitivity | Specificity | +LR | Notes |
|---|---|---|---|---|---|
| Pulmonary Edema | LUS | 97% | 98% | 48.5 | Bedside; detects B-lines |
| CXR | 75% | 83% | 4.4 | Limited in early disease | |
| CT | — | — | — | Reference standard | |
| Pleural Effusion | LUS | 91% | 92% | 11.4 | Continuous; bedside |
| CXR | 42% | 81% | 2.2 | Requires upright film | |
| CT | — | — | — | Reference standard | |
| Pneumonia | LUS | 93.4% | 97.7% | 40.6 | Dynamic air bronchograms; high accuracy |
| CXR | 75% | 72% | 2.7 | Lower sensitivity for patchy shadowing | |
| CT | — | — | — | Reference standard | |
| Pneumothorax | LUS | 87% | 99% | 87.0 | Lung point 100% specific |
| CXR | 52% | 100% | ∞ | Misses small PTX | |
| CT | — | — | — | Reference standard | |
| ARDS | LUS | 77–100% | 61–100% | Variable | Ranges reflect different phenotyping methods |
| CXR | 65.5–69.4% | — | — | Moderate overlap with LUS | |
| CT | — | — | — | Reference standard |
Complicated Parapneumonic Effusion, Empyema and Hemothorax
| Condition | Definition | Suggestive Sonographic Features |
|---|---|---|
| Empyema | Accumulation of purulent fluid within the pleural space | Complex septations, echogenic material, pleural thickening, plankton sign |
| Parapneumonic Effusion | Pleural fluid collection that develops in association with pneumonia | Complex septations, pleural thickening |
| Hemothorax | Accumulation of blood within the pleural space | Echogenic material, plankton sign |
Future Directions
6.5. Acute Respiratory Distress Syndrome (ARDS)
Future Directions
6.6. COVID-19
LUS vs CXR in COVID-19
LUS vs CT in COVID-19
Future Directions
7. Limitations
8. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| APE | Acute Pulmonary Edema. |
| ARDS | Acute Respiratory Distress Syndrome. |
| B-lines | Vertical, hyperechoic reverberation artifacts indicating interstitial syndrome. |
| CAJ | Cavoatrial Junction. |
| CDI | Color Doppler Imaging. |
| CEUS | Contrast-Enhanced Ultrasound. |
| CVC | Central Venous Catheter. |
| CXR | Chest X-Ray. |
| DIVOT | Direct Visualization of the Thoracic Space. |
| DOAJ | Directory of Open Access Journals. |
| ED | Emergency Department. |
| ETT | Endotracheal Tube. |
| EVLW | Extravascular Lung Water. |
| ICA | Intercostal Artery. |
| ICC | Intraclass Correlation Coefficient. |
| ICU | Intensive Care Unit. |
| ILD | Interstitial Lung Disease. |
| IRB | Institutional Review Board. |
| IV | Intravenous. |
| LUS | Lung Ultrasound. |
| M-mode | Motion Mode. |
| MDPI | Multidisciplinary Digital Publishing Institute. |
| OSF | Open Science Framework. |
| POCUS | Point-of-Care Ultrasound. |
| PRISMA-ScR | Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews. |
| QLUSS | Quantitative Lung Ultrasound Scoring System. |
| RA | Right Atrium. |
| SVC | Superior Vena Cava. |
| TLA | Three Letter Acronym. |
| TRUE | Tracheal Rapid Ultrasound Exam. |
| TUS | Thoracic Ultrasound. |
References
- Beshara M, Bittner EA, Goffi A, Berra L, Chang MG. Nuts and bolts of lung ultrasound: utility, scanning techniques, protocols, and findings in common pathologies. Crit Care. 2024;28(1):328. [CrossRef]
- Volpicelli G, Elbarbary M, Blaivas M, et al. International evidence-based recommendations for point-of-care lung ultrasound. In: Intensive Care Medicine. Vol 38. ; 2012:577-591. [CrossRef]
- Piette E, Daoust R, Denault A. Basic concepts in the use of thoracic and lung ultrasound. Curr Opin Anaesthesiol. 2013;26(1):20-30. [CrossRef]
- Lichtenstein DA. Lung ultrasound in the critically ill. Ann Intensive Care. 2014;4(1):1. [CrossRef]
- Li R, Liu H, Qi H, et al. Lung ultrasound assessment of acute respiratory distress syndrome caused by coronavirus disease 2019: An observational study. Hong Kong Journal of Emergency Medicine. 2021;28(1):8-14. [CrossRef]
- Andrade H, Jackson E, Brenner D, Haouili M. Exploring the Role of Thoracic Ultrasound in Anesthesia and Acute Care: A Scoping Review of Diagnostic and Procedural Application. OSF. Published online March 30, 2025. Accessed March 29, 2025. osf.io/5taq3.
- Aromataris E, Porritt K, Pilla B, Jordan Z. JBI Manual for Evidence Synthesis. (Aromataris E, Lockwood C, Porritt K, Pilla B, Jordan Z, eds.). JBI; 2024. [CrossRef]
- Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19-32. [CrossRef]
- Pierrakos C, Smit MR, Pisani L, et al. Lung Ultrasound Assessment of Focal and Non-focal Lung Morphology in Patients With Acute Respiratory Distress Syndrome. Front Physiol. 2021;12:730857. [CrossRef]
- Frankel HL, Kirkpatrick AW, Elbarbary M, et al. Guidelines for the appropriate use of bedside general and cardiac ultrasonography in the evaluation of critically ill patients-part I: General ultrasonography. Crit Care Med. 2015;43(11):2479-2502. [CrossRef]
- American College of Emergency Physicians. Emergency ultrasound guidelines. Ann Emerg Med. 2009;53(4):550-570. [CrossRef]
- Kanai M, Sekiguchi H. Avoiding vessel laceration in thoracentesis: A role of vascular ultrasound with color Doppler. Chest. 2015;147(1):e5-e7. [CrossRef]
- Aldrich JE. Basic physics of ultrasound imaging. Crit Care Med. 2007;35(Suppl):S131-S137. [CrossRef]
- Feldman MK, Katyal S, Blackwood MS. US artifacts. Radiographics. 2009;29(4):1179-1189. [CrossRef]
- Buttar S, Cooper D, Olivieri P, et al. Air and its Sonographic Appearance: Understanding the Artifacts. Journal of Emergency Medicine. 2017;53(2):241-247. [CrossRef]
- Prada G, Vieillard-Baron A, Martin AK, et al. Tracheal, Lung, and Diaphragmatic Applications of M-Mode Ultrasonography in Anesthesiology and Critical Care. J Cardiothorac Vasc Anesth. 2021;35(1):310-322. [CrossRef]
- Lichtenstein DA, Lascols N, Prin S, Mezière G. The “lung pulse”: an early ultrasound sign of complete atelectasis. Intensive Care Med. 2003;29(12):2187-2192. [CrossRef]
- Dietrich CF, Mathis G, Blaivas M, et al. Lung B-line artefacts and their use. J Thorac Dis. 2016;8(6):1356-1365. [CrossRef]
- Johannessen Ø, Reite FU, Bhatnagar R, Øvrebotten T, Einvik G, Myhre PL. Lung Ultrasound to Assess Pulmonary Congestion in Patients with Acute Exacerbation of COPD. International Journal of COPD. 2023;18:693-703. [CrossRef]
- Nakao S, Vaillancourt C, Taljaard M, Nemnom MJ, Woo MY, Stiell IG. Diagnostic Accuracy of Lung Point-Of-Care Ultrasonography for Acute Heart Failure Compared With Chest X-Ray Study Among Dyspneic Older Patients in the Emergency Department. Journal of Emergency Medicine. 2021;61(2):161-168. [CrossRef]
- Matthias I, Panebianco NL, Maltenfort MG, Dean AJ, Baston C. Effect of Machine Settings on Ultrasound Assessment of B-lines. Journal of Ultrasound in Medicine. 2021;40(10):2039-2046. [CrossRef]
- Yen JT, Nguyen MM, Lou Y, Shin JS, Chen Y, Tarnoff HL. Gated Transmit and Fresnel-Based Receive Beamforming with a Phased Array for Low-Cost Ultrasound Imaging. IEEE Trans Ultrason Ferroelectr Freq Control. 2021;68(6):2183-2192. [CrossRef]
- Zhang Z, Chen R, Wang B, et al. Development of a KNN Ceramic-Based Lead-Free Linear Array Ultrasonic Transducer. IEEE Trans Ultrason Ferroelectr Freq Control. 2018;65(11):2113-2120. [CrossRef]
- Rizzatto G. Ultrasound Transducers. Vol 27.; 1998.
- Chou HC, Tseng WP, Wang CH, et al. Tracheal rapid ultrasound exam (T.R.U.E.) for confirming endotracheal tube placement during emergency intubation. Resuscitation. 2011;82(10):1279-1284. [CrossRef]
- Gildea TH, Anderson KL, Niknam KR, et al. The utility of color doppler to confirm endotracheal tube placement: A pilot study. Western Journal of Emergency Medicine. 2020;21(4):870-875. [CrossRef]
- Gottlieb M, Burns K, Holladay D, Chottiner M, Shah S, Gore SR. Impact of endotracheal tube twisting on the diagnostic accuracy of ultrasound for intubation confirmation. American Journal of Emergency Medicine. 2020;38(7):1332-1334. [CrossRef]
- Pfeiffer P, Bache S, Isbye DL, Rudolph SS, Rovsing L, Børglum J. Verification of endotracheal intubation in obese patients - Temporal comparison of ultrasound vs. auscultation and capnography. Acta Anaesthesiol Scand. 2012;56(5):571-576. [CrossRef]
- Sahu AK, Bhoi S, Aggarwal P, et al. Endotracheal Tube Placement Confirmation by Ultrasonography: A Systematic Review and Meta-Analysis of more than 2500 Patients. Journal of Emergency Medicine. 2020;59(2):254-264. [CrossRef]
- Hoffmann B, Gullett JP, Hill HF, et al. Bedside ultrasound of the neck confirms endotracheal tube position in emergency intubations. Ultraschall in der Medizin. 2014;35(5):451-458. [CrossRef]
- Karacabey S, Sanri E, Gencer EG, Guneysel O. Tracheal ultrasonography and ultrasonographic lung sliding for confirming endotracheal tube placement: Speed and Reliability. American Journal of Emergency Medicine. 2016;34(6):953-956. [CrossRef]
- Park SC, Ryu JH, Yeom SR, Jeong JW, Cho SJ. Confirmation of endotracheal intubation by combined ultrasonographic methods in the emergency department. EMA - Emergency Medicine Australasia. 2009;21(4):293-297. [CrossRef]
- Chou HC, Chong KM, Sim SS, et al. Real-time tracheal ultrasonography for confirmation of endotracheal tube placement during cardiopulmonary resuscitation. Resuscitation. 2013;84(12):1708-1712. [CrossRef]
- Practice Guidelines for Central Venous Access 2020: An Updated Report by the American Society of Anesthesiologists Task Force on Central Venous Access. Anesthesiology. 2020;132(1):8-43. [CrossRef]
- Brindley PG, Deschamps J, Milovanovic L, Buchanan BM. Are routine chest radiographs still indicated after central line insertion? A scoping review. J Intensive Care Soc. 2024;25(2):190-207. [CrossRef]
- Fragou M, Gravvanis A, Dimitriou V, et al. Real-time ultrasound-guided subclavian vein cannulation versus the landmark method in critical care patients: A prospective randomized study. Crit Care Med. 2011;39(7):1607-1612. [CrossRef]
- Koratala A. The Subcostal Bicaval View. NephroPOCUS.
- Daniels CE, Ryu JH. Improving the safety of thoracentesis. Curr Opin Pulm Med. 2011;17(4):232-236. [CrossRef]
- Cantey EP, Walter JM, Corbridge T, Barsuk JH. Complications of thoracentesis: Incidence, risk factors, and strategies for prevention. Curr Opin Pulm Med. 2016;22(4):378-385. [CrossRef]
- Gordon CE, Feller-Kopman D, Balk EM, Smetana GW. Pneumothorax following thoracentesis: a systematic review and meta-analysis. Arch Intern Med. 2010;170(4):332-339. [CrossRef]
- Havelock T, Teoh R, Laws D, Gleeson F, BTS Pleural Disease Guideline Group. Pleural procedures and thoracic ultrasound: British Thoracic Society Pleural Disease Guideline 2010. Thorax. 2010;65 Suppl 2:ii61-76. [CrossRef]
- Salamonsen M, Ellis S, Paul E, Steinke K, Fielding D. Thoracic ultrasound demonstrates variable location of the intercostal artery. Respiration. 2012;83(4):323-329. [CrossRef]
- Koyanagi T, Kawaharada N, Kurimoto Y, et al. Examination of intercostal arteries with transthoracic Doppler sonography. Echocardiography. 2010;27(1):17-20. [CrossRef]
- Chan KK, Joo DA, McRae AD, et al. Chest ultrasonography versus supine chest radiography for diagnosis of pneumothorax in trauma patients in the emergency department. Cochrane Database of Systematic Reviews. 2020;2020(7). [CrossRef]
- DeMasi S, Parker MS, Joyce M, Mulligan K, Feeser S, Balderston JR. Thoracic point-of-care ultrasound is an accurate diagnostic modality for clinically significant traumatic pneumothorax. Academic Emergency Medicine. 2023;30(6):653-661. [CrossRef]
- Santorelli JE, Chau H, Godat L, Casola G, Doucet JJ, Costantini TW. Not so FAST—Chest ultrasound underdiagnoses traumatic pneumothorax. Journal of Trauma and Acute Care Surgery. 2022;92(1):44-48. [CrossRef]
- Lichtenstein D, Goldstein I, Mourgeon E, Cluzel P, Grenier P, Rouby JJ. CLINICAL INVESTIGATIONS Comparative Diagnostic Performances of Auscultation, Chest Radiography, and Lung Ultrasonography in Acute Respiratory Distress Syndrome.; 2004. http://www.anesthesiology.org.
- Tierney DM, Huelster JS, Overgaard JD, et al. Comparative Performance of Pulmonary Ultrasound, Chest Radiograph, and CT Among Patients With Acute Respiratory Failure∗. Crit Care Med. 2020;48(2):151-157. [CrossRef]
- Maw AM, Hassanin A, Ho PM, et al. Diagnostic Accuracy of Point-of-Care Lung Ultrasonography and Chest Radiography in Adults With Symptoms Suggestive of Acute Decompensated Heart Failure: A Systematic Review and Meta-analysis. JAMA Netw Open. 2019;2(3):e190703. [CrossRef]
- Picano E, Pellikka PA. Ultrasound of extravascular lung water: A new standard for pulmonary congestion. Eur Heart J. 2016;37(27):2097-2104. [CrossRef]
- Brusasco C, Santori G, Bruzzo E, et al. Quantitative lung ultrasonography: A putative new algorithm for automatic detection and quantification of B-lines. Crit Care. 2019;23(1). [CrossRef]
- File TM, Ramirez JA. Community-Acquired Pneumonia. O’Malley PG, ed. New England Journal of Medicine. 2023;389(7):632-641. [CrossRef]
- Reissig A, Copetti R, Mathis G, et al. Lung ultrasound in the diagnosis and follow-up of community-acquired pneumonia: A prospective, multicenter, diagnostic accuracy study. Chest. 2012;142(4):965-972. [CrossRef]
- Hew M, Corcoran JP, Harriss EK, Rahman NM, Mallett S. The diagnostic accuracy of chest ultrasound for CT-detected radiographic consolidation in hospitalised adults with acute respiratory failure: a systematic review. [CrossRef]
- Xirouchaki N, Magkanas E, Vaporidi K, et al. Lung ultrasound in critically ill patients: Comparison with bedside chest radiography. Intensive Care Med. 2011;37(9):1488-1493. [CrossRef]
- Shen-Wagner J, Gamble C, MacGilvray P. Pleural Effusion: Diagnostic Approach in Adults. Am Fam Physician. 2023;108(5):464-475.
- Hansell L, Milross M, Delaney A, Tian DH, Ntoumenopoulos G. Lung ultrasound has greater accuracy than conventional respiratory assessment tools for the diagnosis of pleural effusion, lung consolidation and collapse: a systematic review. J Physiother. 2021;67(1):41-48. [CrossRef]
- Shen KR, Bribriesco A, Crabtree T, et al. The American Association for Thoracic Surgery consensus guidelines for the management of empyema. J Thorac Cardiovasc Surg. 2017;153(6):e129-e146. [CrossRef]
- Jacoby RC, Battistella FD. Hemothorax. Semin Respir Crit Care Med. 2001;22(6):627-630. [CrossRef]
- Wang T, Du G, Fang L, Bai Y, Liu Z, Wang L. Value of ultrasonography in determining the nature of pleural effusion: Analysis of 582 cases. Medicine (United States). 2022;101(33):E30119. [CrossRef]
- Lane AB, Petteys S, Ginn M, Nations JA. Clinical importance of echogenic swirling pleural effusions. Journal of Ultrasound in Medicine. 2016;35(4):843-847. [CrossRef]
- Yamada A, Taiji R, Nishimoto Y, et al. Pictorial Review of Pleural Disease: Multimodality Imaging and Differential Diagnos. Radiographics. 2024;44(4). [CrossRef]
- Yang L, Wang K, Li W, Liu D. Chest ultrasound is better than CT in identifying septated effusion of patients with pleural disease. Sci Rep. 2024;14(1):11964. [CrossRef]
- Staub LJ, Biscaro RRM, Kaszubowski E, Maurici R. Chest ultrasonography for the emergency diagnosis of traumatic pneumothorax and haemothorax: A systematic review and meta-analysis. Injury. 2018;49(3):457-466. [CrossRef]
- See KC, Ong V, Tan YL, Sahagun J, Taculod J. Chest radiography versus lung ultrasound for identification of acute respiratory distress syndrome: a retrospective observational study. Crit Care. 2018;22(1):203. [CrossRef]
- Copetti R, Soldati G, Copetti P. Chest sonography: A useful tool to differentiate acute cardiogenic pulmonary edema from acute respiratory distress syndrome. Cardiovasc Ultrasound. 2008;6. [CrossRef]
- Cammarota G, Bruni A, Morettini G, et al. Lung ultrasound to evaluate aeration changes in response to recruitment maneuver and prone positioning in intubated patients with COVID-19 pneumonia: preliminary study. Ultrasound Journal. 2023;15(1). [CrossRef]
- Boero E, Schreiber A, Rovida S, Vetrugno L, Blaivas M. The role of lung ultrasonography in COVID-19 disease management. JACEP Open. 2020;1(6):1357-1363. [CrossRef]
- Aguersif A, Sarton B, Bouharaoua S, et al. Lung Ultrasound to Assist ICU Admission Decision-Making Process of COVID-19 Patients with Acute Respiratory Failure. Crit Care Explor. 2022;4(6):E0719. [CrossRef]
- Heldeweg MLA, Lopez Matta JE, Haaksma ME, et al. Lung ultrasound and computed tomography to monitor COVID-19 pneumonia in critically ill patients: a two-center prospective cohort study. Intensive Care Medicine Experimental. 2021;9(1). [CrossRef]
- Giovannetti G, De Michele L, De Ceglie M, et al. Lung ultrasonography for long-term follow-up of COVID-19 survivors compared to chest CT scan. Respir Med. 2021;181. [CrossRef]
- Ramos Hernández C, Tilve Gomez A, Sánchez Fernández A, et al. Multicentre study on the accuracy of lung ultrasound in the diagnosis and monitoring of respiratory sequelae in the medium and long term in patients with COVID-19. Front Med (Lausanne). 2023;10:1199666. [CrossRef]
| Term | Definition |
|---|---|
| A-lines | Horizontal, hyperechoic lines from reverberation artifact, indicating air filled lungs and helping exclude interstitial syndromes or pulmonary edema. Can be seen in pneumothorax. |
| Lung Sliding | Shimmering movement of the pleural line seen in 2D and M-mode ("sandy beach" pattern), confirming lung ventilation and reducing the likelihood of pneumothorax. |
| Lung Pulse | Subtle pleural movement due to cardiac motion, seen in low or absent ventilation states (e.g., low tidal volume, regional hypoventilation). |
| B-lines | Vertical, hyperechoic artifacts that move with lung sliding and obliterate A-lines. Scattered B-lines can be normal, but ≥3 per window suggests alveolar-interstitial syndrome. |
| Step | Description |
|---|---|
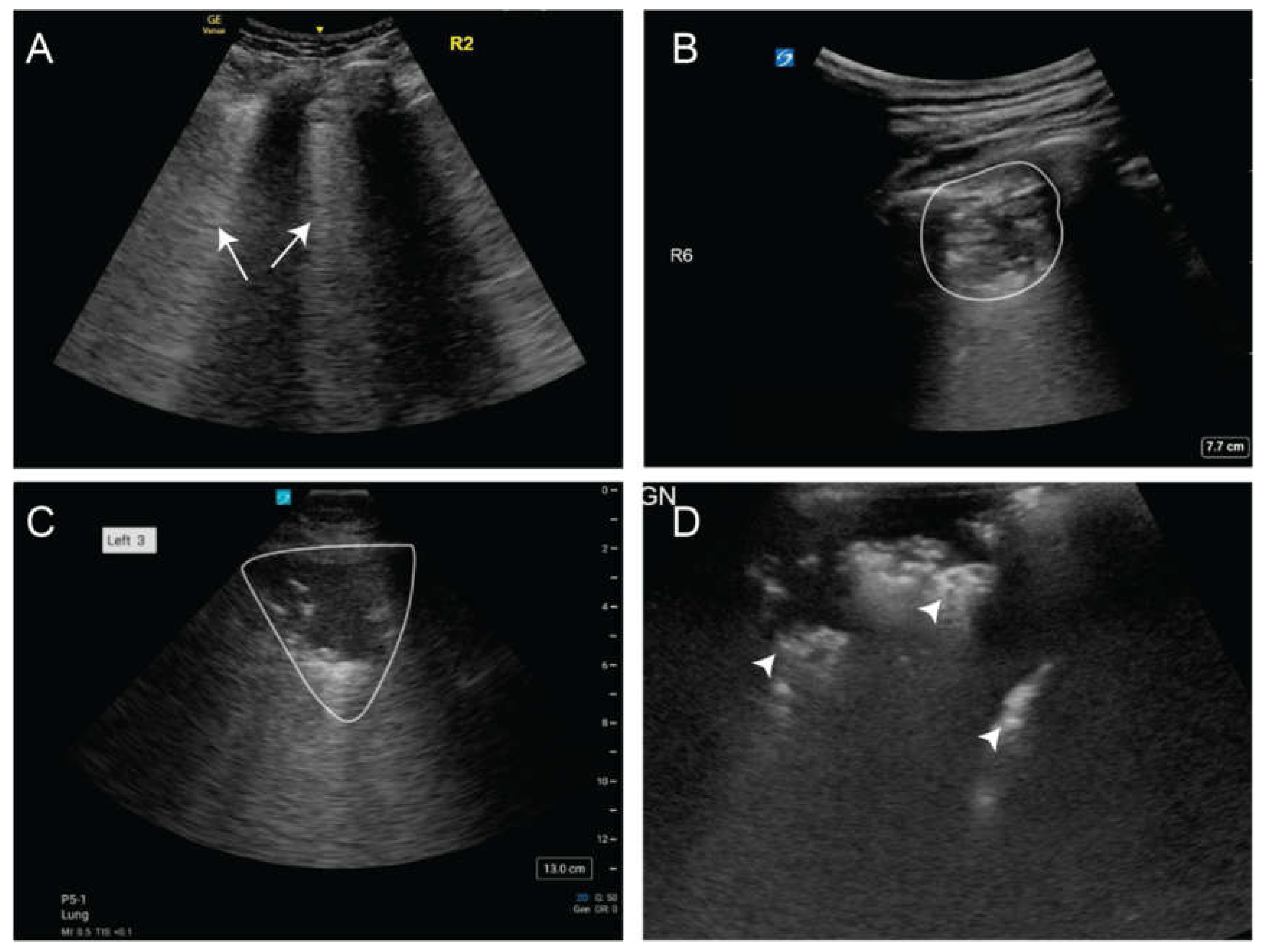
| Identification | A phased array transducer was used to locate the pleural effusion, lung parenchyma, and diaphragm. |
| Marking | A skin marking pen was used to mark the selected site. |
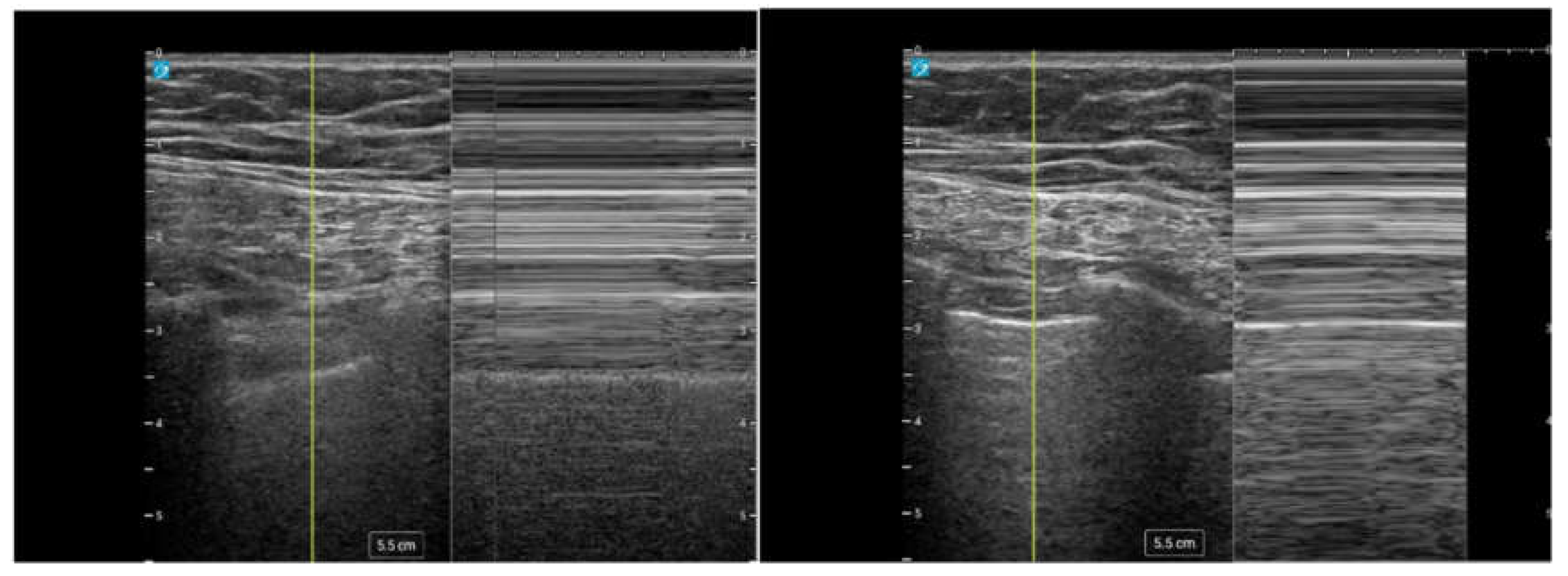
| Intercostal Space Assessment | A high-frequency linear transducer was used to visualize the target intercostal space and adjacent ribs. Zoom was activated to enhance visualization. |
| Doppler Imaging | Color Doppler imaging (CDI) was applied, scanning from the inferior border of the superior rib to the superior border of the inferior rib. The flow scale was adjusted until pulsatile activity of the intercostal artery (ICA) was identified. |
| Confirmation and Final Assessment | CDI was used to confirm findings and assess additional low-flow vessels in the planned procedural field. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




