Submitted:
05 April 2025
Posted:
08 April 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Literature Review
- Theoretical Frameworks
- Nexus Between Economic Inequality and Healthcare Access
3. Methodology
- Estimation Technique
4. Results and discussion
- Summary Descriptive Statistics
- Correlation Matrix
| VARIABLES | PHC | GIN | GPC | GIN*GHE | PPD | GHE |
|---|---|---|---|---|---|---|
| PHC | 1.000 | |||||
| GIN | 0.203 | 1.000 | ||||
| 0.000 | ||||||
| GPC | 0.836 | 0.248 | 1.000 | |||
| 0.000 | 0.000 | |||||
| GIN*GHE | 0.066 | 0.020 | 0.139 | 1.000 | ||
| -0.219 | -0.706 | -0.010 | ||||
| PPD | 0.421 | 0.264 | 0.464 | 0.030 | 1.000 | |
| 0.000 | 0.000 | 0.000 | -0.581 | |||
| GHE | 0.390 | 0.308 | 0.338 | 0.118 | 0.116 | 1.000 |
| 0.000 | 0.000 | 0.000 | -0.028 | -0.032 |
- Regression Results and Discussion of Findings
- Discussion of Study Findings
| VARIABLES | PHC | PHC |
|---|---|---|
| GIN | -0.0030*** | -0.003*** |
| (0.0011) | (0.001) | |
| GPC | 0.0002*** | -0.078** |
| (5.751) | (0.037) | |
| GHE | 0.0313*** | 0.002** |
| (0.0065) | (0.001) | |
| GIN*GHE | 0.002** | |
| (0.001) | ||
| PPD | 0.0002*** | 0.000*** |
| (5.5810) | (0.000) | |
| Constant | 0.0852* | 0.153*** |
| (0.0437) | (0.044) | |
| Observations | 360 | 360 |
| Number of countries | 15 | 15 |
| R-squared | 0.731 | 0.904 |
| Wald Chi2 | 2011.83*** | 493.89*** |
- Robust Results
| VARIABLES | PHC | PHC |
|---|---|---|
| GIN | -0.001** | -0.003*** |
| (0.001) | (0.001) | |
| GPC | 0.000** | -0.078** |
| (0.000) | (0.038) | |
| GHE | 0.006* | 0.002** |
| (0.014) | (0.001) | |
| GIN*GHE | 0.000*** | |
| (0.000) | ||
| PPD | 0.000*** | -0.0030*** |
| (0.000) | (0.00110) | |
| Constant | 0.044* | 0.153*** |
| (0.046) | (0.054) | |
| Observations | 360 | 360 |
| Number of Countries | 15 | 15 |
| Wald Chi2 | 1242.02*** | 417.48*** |
5. Conclusion, Policy Implications, and Limitations
Declaration of AI use
Acknowledgements
Conflicts of Interest
References
- Aglina, M., Agbejule, A., & Nyamuame, G. Y. (2016). Policy framework on energy access and key development indicators: ECOWAS interventions and the case of Ghana. Energy Policy, 97, 332–342. [CrossRef]
- Ahmed, S., & Mahapatro, S. (2023). Inequality in Healthcare Access at the Intersection of Caste and Gender. Contemporary Voice of Dalit, 15, 75–85. [CrossRef]
- Aiyar, S., & Ebeke, C. (2020). Inequality of opportunity, inequality of income, and economic growth. World Development. [CrossRef]
- Al-Hanawi, M. K., Chirwa, G., Kamninga, T., & Manja, L. P. (2020). Effects of Financial Inclusion on Access to Emergency Funds for Healthcare in the Kingdom of Saudi Arabia. Journal of Multidisciplinary Healthcare, 13, 1157–1167. [CrossRef]
- Alimi, O., Ajide, K., & Isola, W. (2019). Environmental quality and health expenditure in ECOWAS. Environment, Development and Sustainability, 22, 5105–5127. [CrossRef]
- Aluko, O., & Ibrahim, M. (2020). Institutions and financial development in ECOWAS. Journal of Sustainable Finance & Investment, 11, 187–198. [CrossRef]
- Ametoglo, M., Guo, P., & Wonyra, K. O. (2018). Regional Integration and Income Inequality in ECOWAS Zone. Journal of Economic Integration. [CrossRef]
- Arruda, N. M., Maia, A. G., & Alves, L. C. (2018). [Inequality in access to health services between urban and rural areas in Brazil: A disaggregation of factors from 1998 to 2008]. Cadernos de Saude Publica, 34 6. [CrossRef]
- Asante, A., Wasike, W., & Ataguba, J. (2020). Health Financing in Sub-Saharan Africa: From Analytical Frameworks to Empirical Evaluation. Applied Health Economics and Health Policy, 18, 743–746. [CrossRef]
- Asaria, M. , Ali, S., Doran, T., Ferguson, B., Fleetcroft, R., Goddard, M., Goldblatt, P., Laudicella, M., Raine, R., & Cookson, R. (2016). How a universal health system reduces inequalities: Lessons from England. Journal of Epidemiology and Community Health, 70, 637–643. [CrossRef]
- Ataguba, J. (2021). The Impact of Financing Health Services on Income Inequality in an Unequal Society: The Case of South Africa. Applied Health Economics and Health Policy, 19, 721–733. [CrossRef]
- Bai, J., Choi, S., & Liao, Y. (2019). Feasible generalized least squares for panel data with cross-sectional and serial correlations. Empirical Economics, 60, 309–326. [CrossRef]
- Bai, Q., Ke, X., Huang, L., Liu, L., Xue, D., & Bian, Y. (2022). Finding flaws in the spatial distribution of health workforce and its influential factors: An empirical analysis based on Chinese provincial panel data, 2010–2019. Frontiers in Public Health, 10. [CrossRef]
- Behera, D. K., & Dash, U. (2019). Effects of economic growth towards government health financing of Indian states: An assessment from a fiscal space perspective. Journal of Asian Public Policy, 12, 206–227. [CrossRef]
- Bognini, J., Samadoulougou, S., Ouédraogo, M., Kangoye, T. D., Malderen, C. V., Tinto, H., & Kirakoya-Samadoulougou, F. (2021). Socioeconomic inequalities in curative healthcare-seeking for children under five before and after the free healthcare initiative in Sierra Leone: Analysis of population-based survey data. International Journal for Equity in Health, 20. [CrossRef]
- Brinda, E., Attermann, J., Gerdtham, U., & Enemark, U. (2016). Socio-economic inequalities in health and health service use among older adults in India: Results from the WHO Study on Global AGEing and adult health survey. Public Health, 141, 32–41. [CrossRef]
- Choi, S. (2018). Experiencing Financial Hardship Associated With Medical Bills and Its Effects on Health Care Behavior: A 2-Year Panel Study. Health Education & Behavior, 45, 616–624. [CrossRef]
- Cui, B., Boisjoly, G., Serra, B., & El-geneidy, A. (2022). Modal equity of accessibility to healthcare in Recife, Brazil. Journal of Transport and Land Use. [CrossRef]
- Dickman, S. L., Himmelstein, D., & Woolhandler, S. (2017). Inequality and the health-care system in the USA. The Lancet, 389, 1431–1441. [CrossRef]
- Donahoe, J., & Mcguire, T. (2020). The vexing relationship between socioeconomic status and health. Israel Journal of Health Policy Research, 9. [CrossRef]
- Dwivedi, R., & Pradhan, J. (2017). Does equity in healthcare spending exist among Indian states? Explaining regional variations from national sample survey data. International Journal for Equity in Health, 16. [CrossRef]
- Erlangga, D., Powell-Jackson, T., Balabanova, D., & Hanson, K. (2023). Determinants of government spending on primary healthcare: A global data analysis. BMJ Global Health, 8. [CrossRef]
- Falco, P. R. D., Hodgson, L. T. F., McConnell, J. M., Ahmed, P. A. K., & De, R. (2023). Assessing the Human Rights Framework on Private Health Care Actors and Economic Inequality. Health and Human Rights, 25, 125–139.
- Folayan, A., Fatt, Q. K., Cheong, M., & Su, T. T. (2024). Healthcare cost coverage inequality and its impact on hypertension and diabetes: A five-year follow-up study in a Malaysian rural community. Health Science Reports, 7. [CrossRef]
- Gomez-Gonzalez, J. E., & Reyes, N. R. (2017). Patterns of global health financing and potential future spending on health. The Lancet, 389, 1955–1956. [CrossRef]
- Gong, S., Gao, Y., Zhang, F., Mu, L., Kang, C., & Liu, Y. (2021). Evaluating healthcare resource inequality in Beijing, China, based on an improved spatial accessibility measurement. Transactions in GIS, 25, 1504–1521. [CrossRef]
- Gordon, T. , Booysen, F., & Mbonigaba, J. (2020). Socio-economic inequalities in the multiple dimensions of access to healthcare: The case of South Africa. BMC Public Health, 20. [CrossRef]
- Gugushvili, A. , & Reeves, A. (2021). How democracy alters our view of inequality—And what it means for our health. Social Science & Medicine, 283. [CrossRef]
- Hailu, A. , Gebreyes, R., & Norheim, O. (2021). Equity in public health spending in Ethiopia: A benefit incidence analysis. Health Policy and Planning, 36, 4–13. [CrossRef]
- Harikrishnan, K. , & Hiremath, G. (2024). Inequality in Public Provision of Healthcare: Do Fiscal Transfers Matter? Journal of Public Affairs. [CrossRef]
- Hunter, B. M. , & Murray, S. (2019). Deconstructing the Financialization of Healthcare. Development and Change. [CrossRef]
- Iheonu, C. O. , Asongu, S., Odo, K. O., & Ojiem, P. K. (2020). Financial sector development and Investment in selected countries of the Economic Community of West African States: Empirical evidence using heterogeneous panel data method. Financial Innovation, 6. [CrossRef]
- Jakovljevic, M. , Pallegedara, A., Vinayagathasan, T., & Kumara, A. S. (2022). Editorial: Inequality in healthcare utilization and household spending in developing countries. Frontiers in Public Health, 10. [CrossRef]
- Johar, M., Soewondo, P., Pujisubekti, R., Satrio, H. K., & Adji, A. (2018). Inequality in access to health care, health insurance and the role of supply factors. Social Science & Medicine, 213, 134–145. [CrossRef]
- Kamdar, D. , Hossein, Y., Al-Alewi, T., Abdulrahim, N., & Kayyali, R. (2024). Exploring experiences and perspectives of inclusivity amongst community pharmacists in their practice: A survey study. International Journal of Pharmacy Practice. [CrossRef]
- Kaur, S. , Kiran, R., & Sharma, R. (2024). Healthcare Expenditure, Health Outcomes and Economic Growth: A Study of BRICS Countries. Millennial Asia. [CrossRef]
- Langnel, Z., Amegavi, G. B., Donkor, P., & Mensah, J. (2021). Income inequality, human capital, natural resource abundance, and ecological footprint in ECOWAS member countries. Resources Policy, 74. [CrossRef]
- Li, C. , Tang, C., & Wang, H. (2020). Investigating the association of health system characteristics and health care utilization: A multilevel model in China's aging population. Journal of Global Health, 10. [CrossRef]
- Lokossou, V. K. , Atama, N. C., Nzietchueng, S., Koffi, B. Y., Iwar, V., Oussayef, N., Umeokonkwo, C. D., Behravesh, C. B., Sombie, I., Okolo, S., & Ouendo, E.-M. (2021). Operationalizing the ECOWAS regional one health coordination mechanism (2016–2019): Scoping review on progress, challenges and way forward. One Health, 13, 100291. [CrossRef]
- Maduekwe, M. , Morris, E., Greene, J., & Healey, V. (2019). Gender Equity and Mainstreaming in Renewable Energy Policies—Empowering Women in the Energy Value Chain in the Economic Community of West African States (ECOWAS). Current Sustainable/Renewable Energy Reports, 6, 13–21. [CrossRef]
- Manasseh, C. O. , Ihedimma, G. I., Abada, F. C., Nwakoby, I. C., Njoku, B., Kesuh, J. T., Okeke, C. G., Alio, F., & Onwumere, J. (2019). DID GLOBAL FINANCIAL CRISIS WORSEN OIL PRICE VOLATILITY AND BANKING SECTOR NEXUS IN SELECTED ECOWAS AND G-7 MEMBER COUNTRIES? International Journal of Energy Economics and Policy. [CrossRef]
- McGuire, F. , Vijayasingham, L., Vassall, A., Small, R., Webb, D., Guthrie, T., & Remme, M. (2019). Financing intersectoral action for health: A systematic review of co-financing models. Globalization and Health, 15. [CrossRef]
- Miller, S. , & Startz, R. (2018). Feasible generalized least squares using support vector regression. Economics Letters. [CrossRef]
- Molla, A. , & Chi, C. (2017). Who pays for healthcare in Bangladesh? An analysis of progressivity in health systems financing. International Journal for Equity in Health, 16. [CrossRef]
- Moundigbaye, M., Messemer, C., Parks, R. W., & Reed, W. R. (2020). Bootstrap methods for inference in the Parks model. Economics, 14. [CrossRef]
- Mulcahy, P. , Mahal, A., McPake, B., Kane, S., Ghosh, P., & Lee, J. (2021). Is there an association between public spending on health and choice of healthcare providers across socioeconomic groups in India? - Evidence from a national sample. Social Science & Medicine. [CrossRef]
- Mulenga, A., & Ataguba, J. (2017). Assessing income redistributive effect of health financing in Zambia. Social Science & Medicine, 189, 1–10. [CrossRef]
- Nwoko, K. C. (2021). ECOWAS responses to the COVID-19 pandemic under its peace and security architecture. South African Journal of International Affairs, 28, 29–46. [CrossRef]
- Oburota, C. , & Olaniyan, O. (2020). Health care financing and income inequality in Nigeria. International Journal of Social Economics. [CrossRef]
- Olaniyan, T. O. , Ijaiya, M. A., & Kolapo, F. T. (2022). Remittances, Financial Sector Development, Institutions and Economic Growth in the ECOWAS Region. Migration Letters. [CrossRef]
- Palacios, A. , Espinola, N., & Rojas-Roque, C. (2020). Need and inequality in the use of health care services in a fragmented and decentralized health system: Evidence for Argentina. International Journal for Equity in Health, 19. [CrossRef]
- Rahman, M. , Khanam, R., & Rahman, M. (2018). Health care expenditure and health outcome nexus: New evidence from the SAARC-ASEAN region. Globalization and Health, 14. [CrossRef]
- Ridge, L., Dickson, V., & Stimpfel, A. W. (2019). The Occupational Health of Nurses in the Economic Community of West African States: A Review of the Literature. Workplace Health & Safety, 67, 554–564. [CrossRef]
- Rivillas, J. C. , Devia-Rodriguez, R., & Ingabire, M.-G. (2020). Measuring socioeconomic and health financing inequality in maternal mortality in Colombia: A mixed methods approach. International Journal for Equity in Health, 19. [CrossRef]
- Saito, E., Gilmour, S., Yoneoka, D., Gautam, G. S., Rahman, M. M., Shrestha, P., & Shibuya, K. (2016). Inequality and inequity in healthcare utilization in urban Nepal: A cross-sectional observational study. Health Policy and Planning, 31, 817–824. [CrossRef]
- Seddon, J., & Currie, W. (2017). Healthcare financialisation and the digital divide in the European Union: Narrative and numbers. Inf. Manag., 54, 1084–1096. [CrossRef]
- Shaltynov, A. , Rocha, J., Jamedinova, U., & Myssayev, A. (2022). Assessment of primary healthcare accessibility and inequality in north-eastern Kazakhstan. Geospatial Health, 17 1. [CrossRef]
- Shamu, S., January, J., & Rusakaniko, S. (2017). Who benefits from public health financing in Zimbabwe? Towards universal health coverage. Global Public Health, 12, 1169–1182. [CrossRef]
- Sheinman, I., & Terentieva, S. (2015). International comparison of the effectiveness of fiscal and insurance models of healthcare financing. Economic Policy, 6. https://consensus.app/papers/international-comparison-of-the-effectiveness-of-fiscal-sheinman-terentieva/e7d8f276f07651b18d7a918e3b4b98b1/.
- Shrivastava, S. , Shrivastava, P., & Ramasamy, J. (2016). Inequality in Health for Women, Infants, and Children: An Alarming Public Health Concern. International Journal of Preventive Medicine, 7. [CrossRef]
- Sulemana, M., & Dramani, J. B. (2020). Effect of financial sector development and institutions on economic growth in SSA. Does the peculiarities of regional blocs matter? Journal of Sustainable Finance & Investment, 12, 1102–1124. [CrossRef]
- Tandon, A., & Reddy, K. (2021). Redistribution and the health financing transition. Journal of Global Health, 11. [CrossRef]
- Tong, Y. , Tan, C.-H., Sia, C., Shi, Y., & Teo, H. (2022). Rural-Urban Healthcare Access Inequality Challenge: Transformative Roles of Information Technology. MIS Quarterly. [CrossRef]
- Umar, U. H. , Baita, A. J., Hamadou, I., & Abduh, M. (2024). Digital finance and SME financial inclusion in Africa. African Journal of Economic and Management Studies. [CrossRef]
- Uneke, C. J. , Sombie, I., Johnson, E., Uneke, B. I., & Okolo, S. (2020). Promoting the use of evidence in health policymaking in the ECOWAS region: The development and contextualization of an evidence-based policymaking guidance. Globalization and Health. [CrossRef]
- Usman, M. , Ma, Z., Zafar, M. W., Haseeb, A., & Ashraf, R. U. (2019). Are Air Pollution, Economic and Non-Economic Factors Associated with Per Capita Health Expenditures? Evidence from Emerging Economies. International Journal of Environmental Research and Public Health, 16. [CrossRef]
- Wang, M. , & Tao, C. (2019). Research on the Efficiency of Local Government Health Expenditure in China and Its Spatial Spillover Effect. Sustainability. [CrossRef]
- Weinrich, A. (2023). Regional citizenship regimes from within: Unpacking divergent perceptions of the ECOWAS citizenship regime. The Journal of Modern African Studies, 61, 117–138. [CrossRef]
- Woldemichael, A. , Takian, A., Sari, A. A., & Olyaeemanesh, A. (2019). Availability and inequality in accessibility of health centre-based primary healthcare in Ethiopia. PLoS ONE, 14. [CrossRef]
- Yamada, T., Chen, C.-C., Murata, C., Hirai, H., Ojima, T., Kondo, K., & Harris, J. R. (2015). Access Disparity and Health Inequality of the Elderly: Unmet Needs and Delayed Healthcare. International Journal of Environmental Research and Public Health, 12, 1745–1772. [CrossRef]
- Yang, F., Katumba, K., & Griffin, S. (2021). Incorporating health inequality impact into economic evaluation in low- and middle-income countries: A systematic review. Expert Review of Pharmacoeconomics & Outcomes Research, 22, 17–25. [CrossRef]
- Yang, J. , Zhong, Q., Liao, Z., Pan, C., & Fan, Q. (2023). Socioeconomic deprivation, medical services accessibility, and income-related health inequality among older Chinese adults: Evidence from a national longitudinal survey from 2011 to 2018. Family Practice. [CrossRef]
- Yu, J., & Meng, S. (2022). Impacts of the Internet on Health Inequality and Healthcare Access: A Cross-Country Study. Frontiers in Public Health, 10. [CrossRef]
- Zhang, J., Gallifant, J., Pierce, R. L., Fordham, A., Teo, J., Celi, L., & Ashrafian, H. (2023). Quantifying digital health inequality across a national healthcare system. BMJ Health & Care Informatics, 30. [CrossRef]
- Zhao, P., Li, S., & Liu, D. (2020). Unequable spatial accessibility to hospitals in developing megacities: New evidence from Beijing. Health & Place, 65, 102406–102406. [CrossRef]
- Zouri, S. (2020). Business cycles, bilateral trade and financial integration: Evidence from Economic Community of West African States (ECOWAS). International Economics. [CrossRef]
| Codes | Variables | Obs. | Mean | Max. | Min. | Std. Dev. | Skewness | Kurtosis |
|---|---|---|---|---|---|---|---|---|
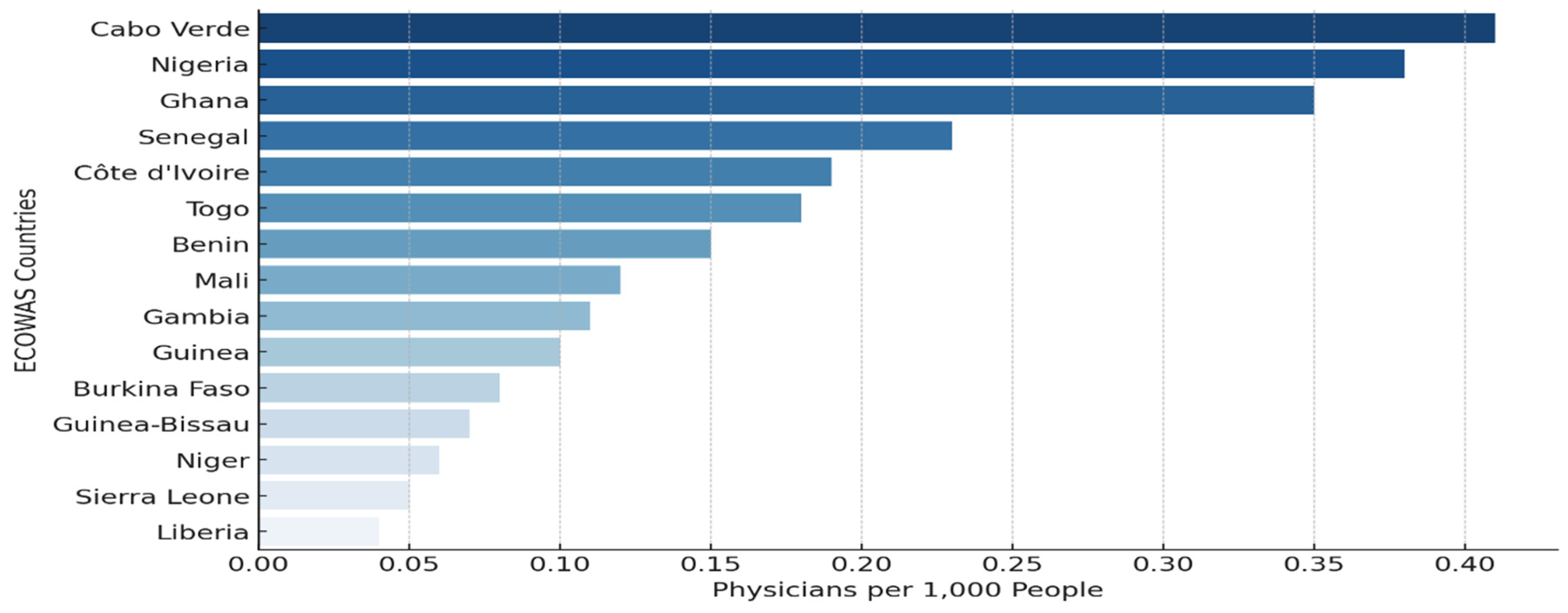
| PHC | Physicians (per 1,000 people) | 360 | 0.135 | 0.487 | 0.025 | 0.124 | 1.676 | 4.841 |
| PPD | Population density | 360 | 87.173 | 260.861 | 9.493 | 55.041 | 0.823 | 3.317 |
| GHE | Government health expenditure | 360 | 1.156 | 2.953 | 0.417 | 0.675 | 1.302 | 4.112 |
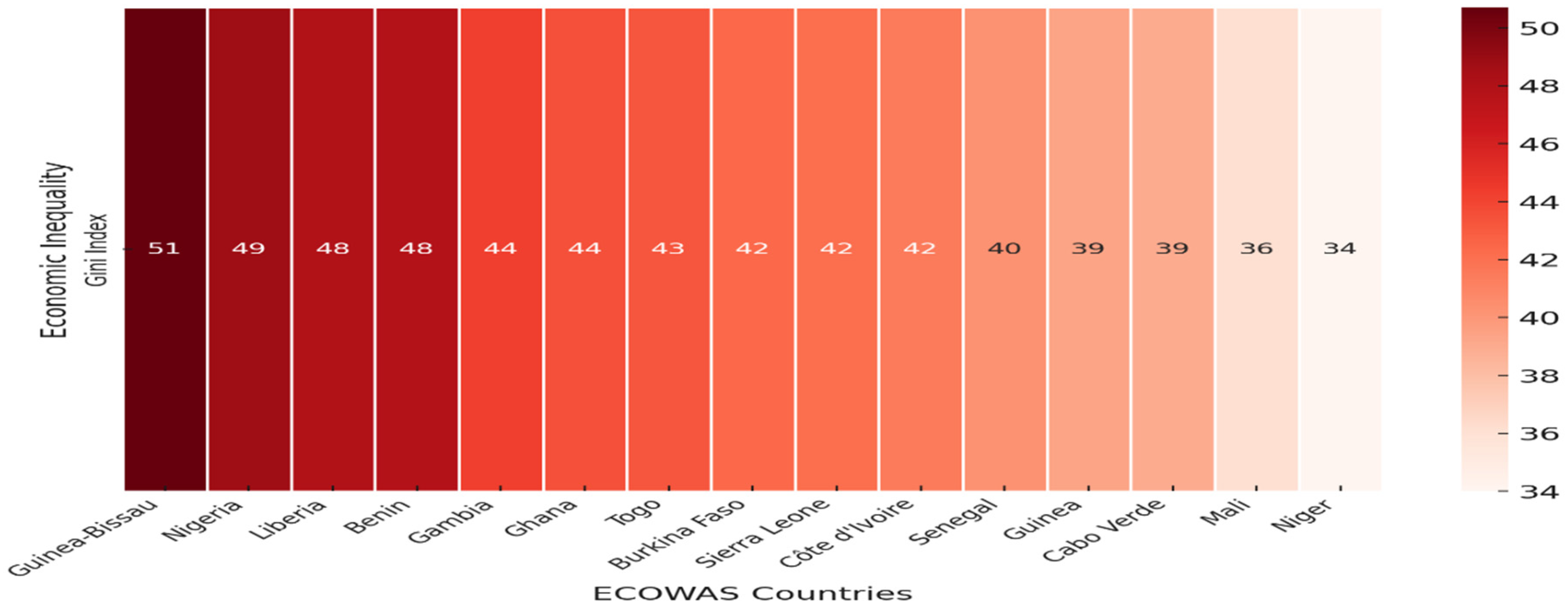
| GIN | Gini index | 360 | 39.365 | 52.500 | 29.600 | 4.108 | 0.315 | 2.879 |
| GPC | GDP per capita (constant 2015 US$) | 360 | 1088.286 | 2679.550 | 460.032 | 671.322 | 1.233 | 3.201 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




