Submitted:
18 March 2025
Posted:
19 March 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Ethics Statement
2.2. Data Source
2.3. Study Design
2.4. Statistical Analysis
3. Results
3.1. Predictors of Surgical Intervention and Overall Survival
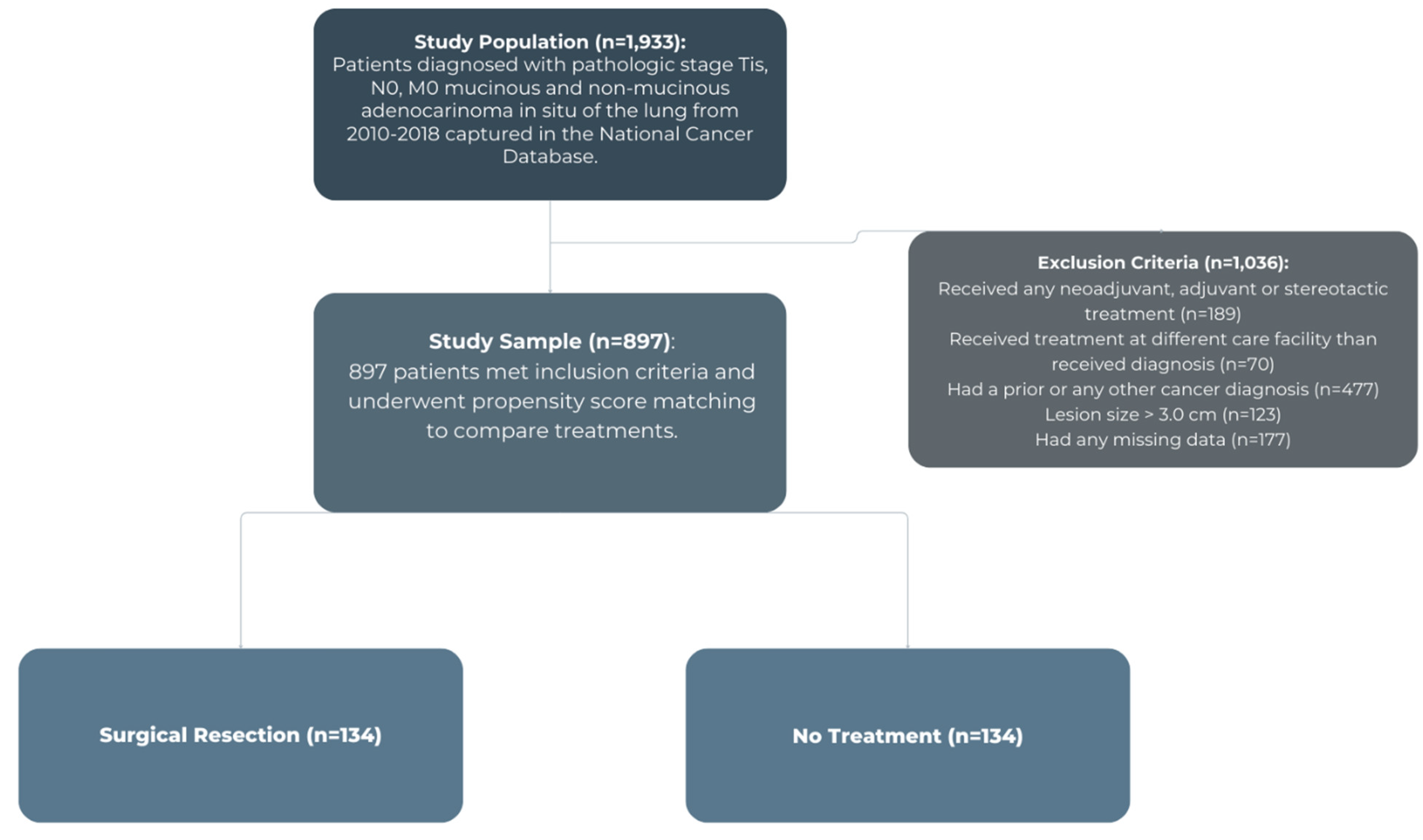
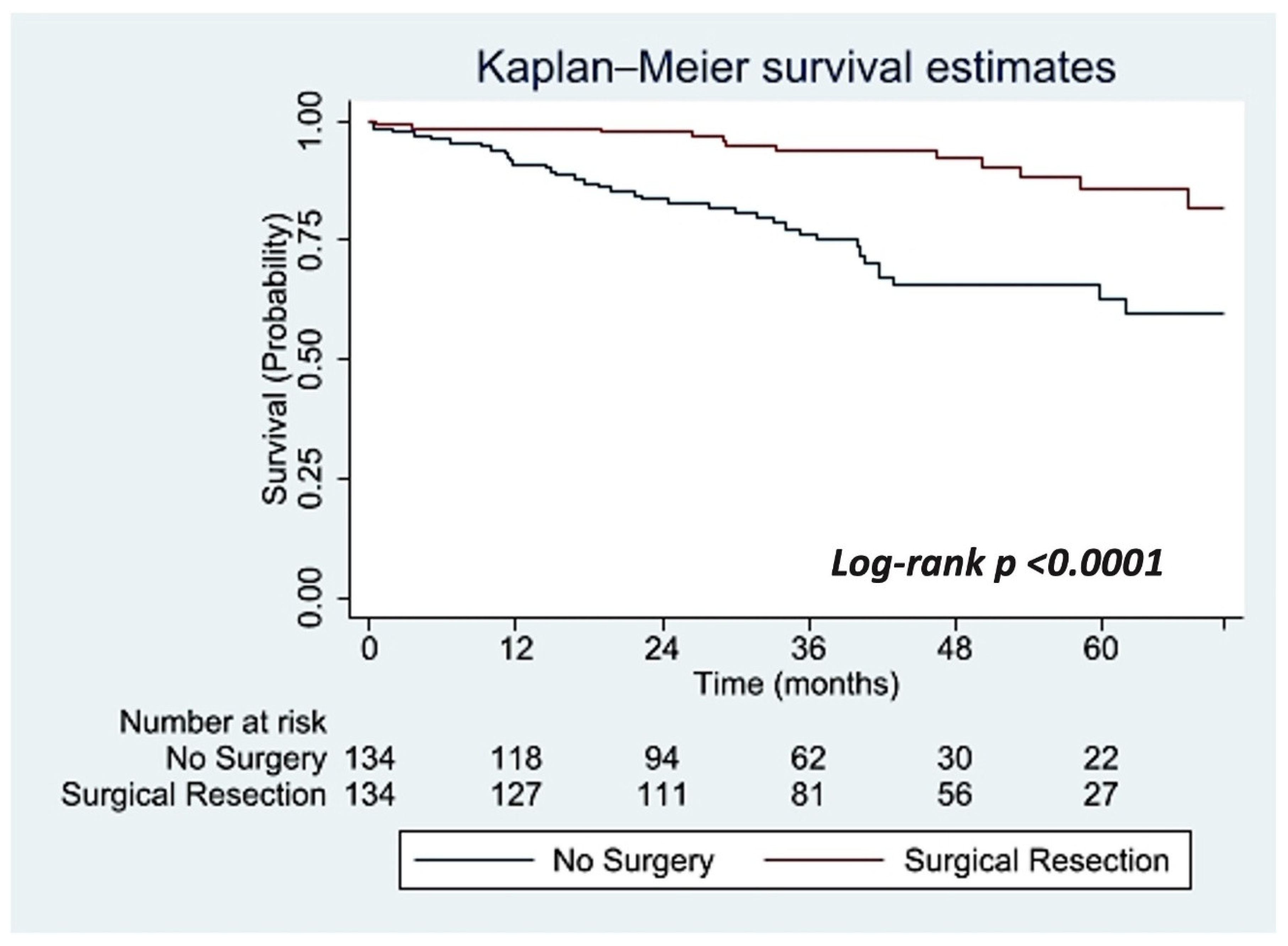
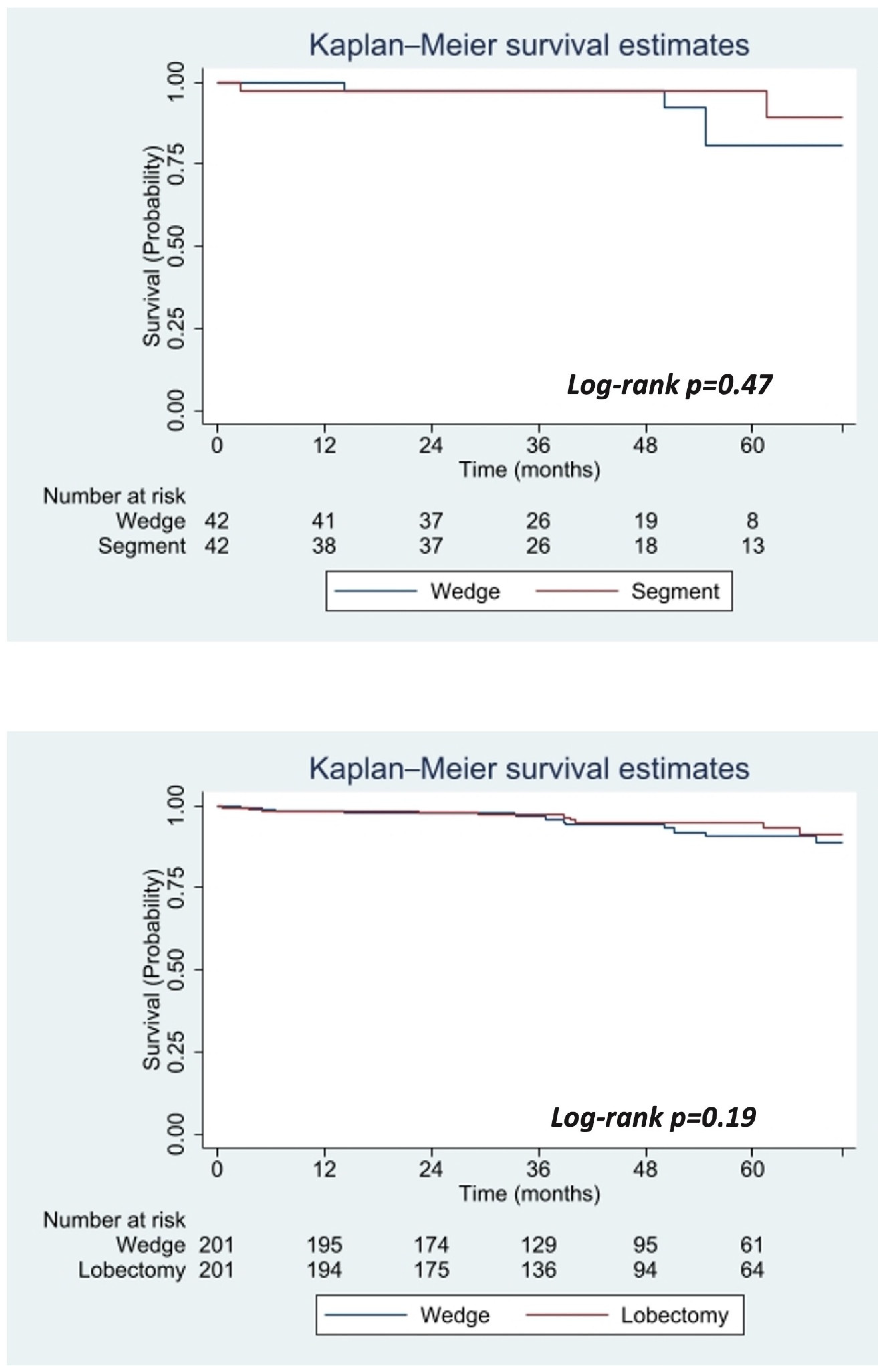
3.2. Propensity Score-Matched Analysis
4. Discussion
5. Conclusion
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| ACS: | American College of Surgeons |
| AIS: | Adenocarcinoma in Situ |
| CDCC: | Charlson Deyo Comorbidity |
| CoC: | Commission on Cancer |
| GGN: | Ground-Glass Nodule |
| ICD-O-3: | International Classification of Diseases for Oncology, 3rd edition |
| NCDB: | National Cancer Database |
| NSCLC: | Non-Small Cell Lung Cancer |
| OS: | Overall Survival |
References
- Du, J. , et al., The novel circular RNA circ-CAMK2A enhances lung adenocarcinoma metastasis by regulating the miR-615-5p/fibronectin 1 pathway. Cell Mol Biol Lett. 2019.
- Travis, W.D. , et al., International association for the study of lung cancer/American thoracic society/European respiratory society international multidisciplinary classification of lung adenocarcinoma. J Thorac Oncol, p: 6(2).
- MacMahon, H. , et al., Guidelines for Management of Incidental Pulmonary Nodules Detected on CT Images: From the Fleischner Society 2017. Radiology, p: 284(1).
- Liu, S. , et al., Precise Diagnosis of Intraoperative Frozen Section Is an Effective Method to Guide Resection Strategy for Peripheral Small-Sized Lung Adenocarcinoma. J Clin Oncol.
- Ito, M. , et al., Prediction for prognosis of resected pT1a-1bN0M0 adenocarcinoma based on tumor size and histological status: relationship of TNM and IASLC/ATS/ERS classifications. Lung Cancer.
- Ishida, H. , et al., Distinctive clinicopathological features of adenocarcinoma in situ and minimally invasive adenocarcinoma of the lung: A retrospective study. Lung Cancer.
- Behera, M. , et al., Lung Adenocarcinoma Staging Using the 2011 IASLC/ATS/ERS Classification: A Pooled Analysis of Adenocarcinoma in Situ and Minimally Invasive Adenocarcinoma. Clin Lung Cancer.
- Zhang, Y. , et al., Surgery for pre- and minimally invasive lung adenocarcinoma. J Thorac Cardiovasc Surg. 2020.
- Chen, C. , et al., Cancer-associated fibroblasts, matrix metalloproteinase-9 and lymphatic vessel density are associated with progression from adenocarcinoma in situ to invasive adenocarcinoma of the lung. Oncol Lett. 2020.
- Miyazawa, T. , et al., PD-L1 Expression in Non-Small-Cell Lung Cancer Including Various Adenocarcinoma Subtypes. Ann Thorac Cardiovasc Surg, p: 25(1).
- Boland, J.M. , et al., Adenocarcinoma in situ, minimally invasive adenocarcinoma, and invasive pulmonary adenocarcinoma--analysis of interobserver agreement, survival, radiographic characteristics, and gross pathology in 296 nodules. Hum Pathol.
- Tsubokawa, N. , et al., Prognostic significance of vascular invasion in intermediate-grade subtype of lung adenocarcinoma. Jpn J Clin Oncol. 1015. [Google Scholar]
- Carretta, A. , et al., Prognostic role of positron emission tomography and computed tomography parameters in stage I lung adenocarcinoma. Radiol Oncol.
- Aokage, K. , et al., Influence of Ground Glass Opacity and the Corresponding Pathological Findings on Survival in Patients with Clinical Stage I Non-Small Cell Lung Cancer. J Thorac Oncol.
- Russell, P.A. , et al., Does lung adenocarcinoma subtype predict patient survival? A clinicopathologic study based on the new International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society international multidisciplinary lung adenocarcinoma classification. J Thorac Oncol. 1496. [Google Scholar]
- Bilimoria, K.Y. , et al., The National Cancer Data Base: a powerful initiative to improve cancer care in the United States. Ann Surg Oncol, 2008. 15(3): p. 683-90.
|
Predictors |
Non-Treatment Group | Surgical Group |
P-value | |
|---|---|---|---|---|
| 181 | 716 | |||
| Sex | Male | 73 (40.3%) | 180 (25.1%) | <0.001 |
| Female | 108 (59.7%) | 536 (74.9%) | ||
| Age, mean years (SD) | 72.8 (9.7) | 66.3 (9.7) | <0.001 | |
| Race, n (%) | White | 155 (85.6%) | 597 (83.4%) | 0.86 |
| Black | 13 (7.2%) | 62 (8.7%) | ||
| Asian | 10 (5.5%) | 46 (6.4%) | ||
| Other | 3 (1.7%) | 9 (1.3%) | ||
| Insurance Status n (%) | Uninsured | 2 (1.1%) | 10 (1.4%) | 0.002 |
| Private | 33 (18.2%) | 235 (32.8%) | ||
| Medicaid | 7 (3.9%) | 30 (4.2%) | ||
| Medicare | 132 (72.9%) | 431 (60.2%) | ||
| Other | 7 (3.9%) | 10 (1.4%) | ||
| Annual Income n (%) | <$40,227 | 22 (13.9%) | 80 (12.6%) | 0.55 |
| $40,227-50,353 | 33 (20.9%) | 116 (18.3%) | ||
| $50,354-63,332 | 39 (24.7%) | 140 (22.1%) | ||
| >$63,332 | 64 (40.5%) | 297 (46.9%) | ||
| Education Percentage Without High School Diploma, n (%) | >17.6% | 26 (16.3%) | 105 (16.6%) | 0.15 |
| 10.9-17.5% | 43 (26.9%) | 143 (22.6%) | ||
| 6.3-10.8% | 52 (32.5%) | 175 (27.6%) | ||
| <6.3% | 39 (24.4%) | 211 (33.3%) | ||
| Facility Type, n (%) | Community Cancer Facility | 7 (3.9%) | 24 (3.4%) | 0.024 |
| Comprehensive Cancer Facility | 84 (46.7%) | 247 (34.8%) | ||
| Academic/Research Facility | 57 (31.7%) | 291 (41.0%) | ||
| Integrated Network Facility | 32 (17.8%) | 148 (20.8%) | ||
| Distance from Facility, mean miles (SD) | 30.1 (107.9) | 52.6 (237.6) | 0.24 | |
| Year of Diagnosis, n (%) | 2010 | 1 (0.6%) | 4 (0.6%) | 0.064 |
| 2011 | 2 (1.1%) | 7 (1.0%) | ||
| 2012 | 7 (3.9%) | 39 (5.4%) | ||
| 2013 | 12 (6.6%) | 53 (7.4%) | ||
| 2014 | 12 (6.6%) | 97 (13.5%) | ||
| 2015 | 21 (11.6%) | 120 (16.8%) | ||
| 2016 | 31 (17.1%) | 105 (14.7%) | ||
| 2017 | 48 (26.5%) | 158 (22.1%) | ||
| 2018 | 47 (26.0%) | 133 (18.6%) | ||
| CDCC Score, n (%) | 0 | 93 (51.4%) | 419 (58.5%) | 0.16 |
| 1 | 54 (29.8%) | 205 (28.6%) | ||
| 2 | 25 (13.8%) | 64 (8.9%) | ||
| 3 | 9 (5.0%) | 28 (3.9%) | ||
| Tumor Size, mean size in mm (SD) | 16.7 (6.8) | 13.1 (6.2) | <0.001 |
|
PREDICTORS |
ODDS RATIO (95% CI, P-VALUE) |
HAZARDS RATIO (95% CI, P-VALUE) |
|
|---|---|---|---|
| >SURGERY (REFERENCE NO TREATMENT) | NA | 0.25 (0.16-0.40, <0.001) | |
| SEX (MALE VS FEMALE) | 1.86 (1.23-2.80, 0.003) | 0.55 (0.36-0.84, 0.005) | |
| AGE (PER YEAR) | 0.92 (0.90-0.95, <0.001) | 1.05 (1.02-1.08, 0.001) | |
| RACE (REFERENCE WHITE) | Black | 1.52 (0.68-3.38, 0.31) | 2.08 (1.08-3.98, 0.03) |
| Asian | 1.10 (0.50--2.46, 0.80) | 0.52 (0.15-1.78, 0.30) | |
| Other | 0.74 (0.16-3.55, 0.71) | 2.89 (0.16-52.45,0.47) | |
| INSURANCE STATUS (REFERENCE UNINSURED) | Private | 2.38 (0.41-13.73, 0.33) | 0.99 (0.12-8.08, 0.99) |
| Medicaid | 1.33 (0.19-9.36, 0.78) | 1.31 (0.13-12.78, 0.82) | |
| Medicare | 3.3 (0.57-19.44, 0.18) | 1.07 (0.13-8.78, 0.06) | |
| Other | 1.75 (0.19-16.44, 0.63) | 2.01 (0.17-24.02, 0.58) | |
| ANNUAL INCOME (REFERENCE <40,227) | $40,227-50,353 | 1.38 (0.68-2.81, 0.38) | 0.55 (0.27-1.14, 0.11) |
| $50,354-63,332 | 1.64 (0.79-3.42, 0.19) | 0.68 (0.34-1.38, 0.29) | |
| >$63,332 | 1.68 (0.78-3.60, 0.18) | 0.73 (0.35-1.50, 0.39) | |
| EDUCATION PERCENTAGE WITHOUT HIGH SCHOOL DIPLOMA (REFERENCE <17.6%) | 10.9-17.5% | 0.56 (0.30-1.07, 0.08) | 0.91 (0.46-1.79, 0.79) |
| 6.3-10.8% | 0.67 (0.34-1.31, 0.24) | 1.03 (0.51-2.08, 0.93) | |
| <6.3% | 0.92 (0.43-1.98, 0.83) | 1.04 (0.47-2.32, 0.91) | |
| FACILITY TYPE (REFERENCE COMMUNITY CANCER FACILITY) | Comprehensive Cancer Facility | 0.56 (0.20-1.56, 0.27) | 0.75 (0.26-2.18, 0.60) |
| Academic/Research Facility | 0.71 (0.25-1.99, 0.51) | 0.62 (0.21-1.84, 0.39) | |
| Integrated Network Facility | 0.76 (0.25-2.28, 0.63) | 0.97 (0.32-2.96, 0.96) | |
| DISTANCE FROM FACILITY (PER MILE) | 1.00 (0.99-1.01, 0.52) | 1.01 (0.99-1.01, 0.55) | |
| YEAR OF DIAGNOSIS (PER YEAR) | 0.84 (0.75-0.94, 0.003) | 1.05 (0.93-1.20, 0.42) | |
| CDCC SCORE (REFERENCE 0) | 1 | 0.90 (0.57-1.42, 0.65) | 1.35 (0.83-2.19, 0.22) |
| 2 | 0.69 (0.38-1.27, 0.24) | 2.18 (0.25-3.81, 0.06) | |
| 3 | 0.90 (0.38-2.21, 0.84) | 1.21 (0.48-3.08, 0.69) | |
| PREDICTORS |
Non-Treatment Group |
Surgical Group |
|
| TUMOR SIZE (PER MM) | 0.94 (0.91-0.97, <0.001) | 1.00 (0.97-1.03, 0.95) |
|
Predictors |
Non-Treatment Group |
Surgical Group |
Absolute Standardized Difference (%) | |
|---|---|---|---|---|
| 134 | 134 | |||
| Female Sex, n (%) | 85 (63.4%) | 82 (61.2%) | 4.8 | |
| Age, years (SD) | 71.8 (9.5) | 72.2 (7.8) | 3.9 | |
| Race, n (%) | White | 112 (83.6%) | 107 (79.9%) | 6.1 |
| Black | 10 (7.5%) | 13 (9.7%) | 8.3 | |
| Asian | 10 (7.5%) | 11 (8.2%) | 3.1 | |
| Other | 2 (1.5%) | 3 (2.2%) | 6.2 | |
| Insurance Status, n (%) | Uninsured | 1 (0.7%) | 4 (3.0%) | 2.6 |
| Private | 29 (21.6%) | 26 (19.4%) | 5.2 | |
| Medicaid | 4 (3.0%) | 4 (3.0%) | <0.1 | |
| Medicare | 96 (71.6%) | 97 (72.4%) | 1.6 | |
| Other | 4 (3.0%) | 3 (2.2%) | <0.1 | |
| Annual Income, n (%) | <$40,227 | 18 (13.4%) | 20 (14.9%) | 4.6 |
| $40,227-50,353 | 27 (20.1%) | 30 (22.4%) | 5.6 | |
| $50,354-63,332 | 33 (24.6%) | 34 (25.4%) | 1.8 | |
| >$63,332 | 56 (41.8%) | 50 (37.3%) | 9.1 | |
| Education Percentage Without High School Diploma, n (%) | >17.6% | 24 (17.9%) | 26 (19.4%) | 4.2 |
| 10.9-17.5% | 32 (23.9%) | 30 (22.4%) | 3.5 | |
| 6.3-10.8% | 42 (31.3%) | 50 (37.3%) | 11 | |
| <6.3% | 36 (26.9%) | 28 (20.9%) | 10.2 | |
| Facility Type, n (%) | Community Cancer Facility | 5 (3.7%) | 3 (2.2%) | 8.4 |
| Comprehensive Cancer Facility | 62 (46.3%) | 59 (44.0%) | 4.6 | |
| Academic/Research Facility | 46 (34.3%) | 49 (36.6%) | 4.7 | |
| Integrated Network Facility | 21 (15.7%) | 23 (17.2%) | 3.8 | |
| Distance from Facility, mean miles (SD) | 31.1 (116.7) | 36.4 (201.4) | 2.8 | |
| CDCC Score, n (%) | 0 | 69 (51.5%) | 69 (51.5%) | <0.1 |
| 1 | 38 (28.4%) | 37 (27.6%) | 1.6 | |
| 2 | 18 (13.4%) | 19 (14.2%) | 2.3 | |
| 3 | 9 (6.7%) | 9 (6.7%) | <0.1 | |
| Year of Diagnosis, (IQR) | 2014 (2011,2017) | 2014 (2011,2017) | 9.4 | |
| Tumor Size, mm (SD) | 16.1 (6.8) | 16.6 (7.2) | 6.7 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




