Submitted:
17 March 2025
Posted:
19 March 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
- Clinical variables: Age group (< 60 years and ≥ 60 years), Gender (male and female), Classic symptoms, Mechanical ventilation, RT-PCR result (positive or negative), Smoking and former smoking, Presence of comorbidities, subdivided into the main conditions: diabetes mellitus, systemic arterial hypertension, obesity, and chronic obstructive pulmonary disease.
- Radiological findings: CXR pattern (positive or negative for COVID-19), Disease extent on CXR (mild/moderate or severe), Type of opacity found (type 1, 2, or 3), Pulmonary involvement (unilateral or bilateral), Symmetry (symmetric or asymmetric), Transverse axis alterations (peripheral or non-peripheral) and Longitudinal axis alterations (without or with predominance).
- Clinical outcome: Asymptomatic, Symptomatic and Death.
- Asymptomatic vs. symptomatic,
- Asymptomatic vs. death,
- Symptomatic vs. death.
2.1. Image Analysis
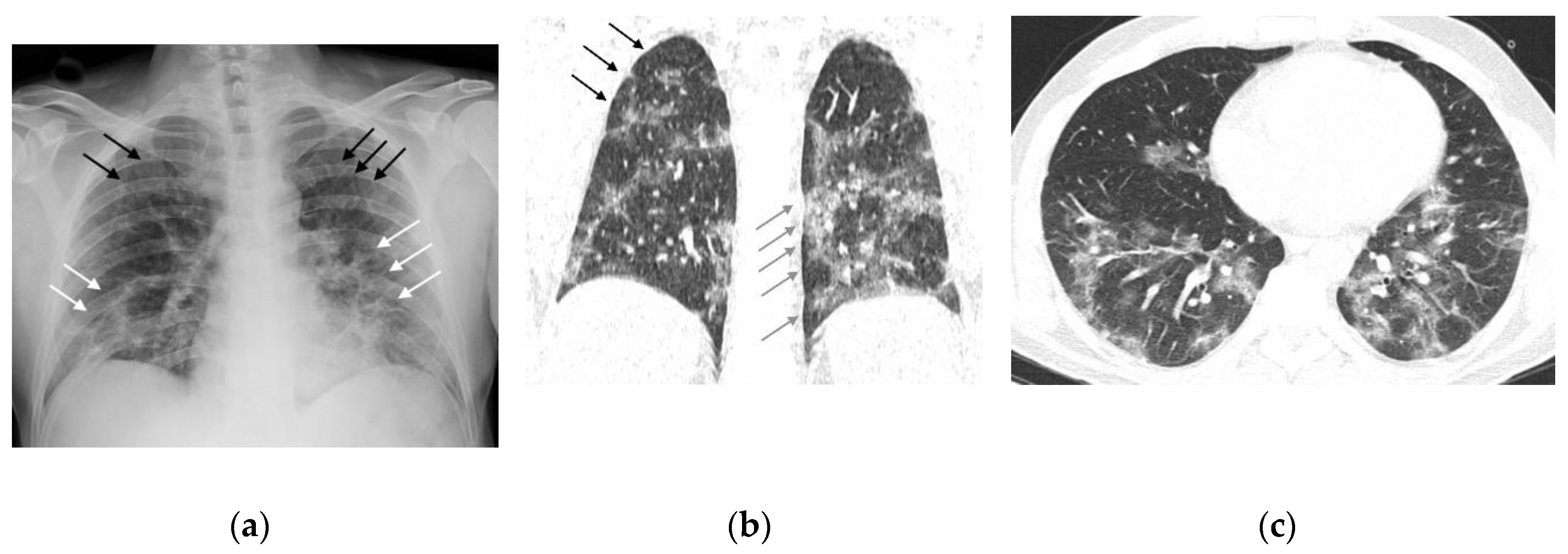
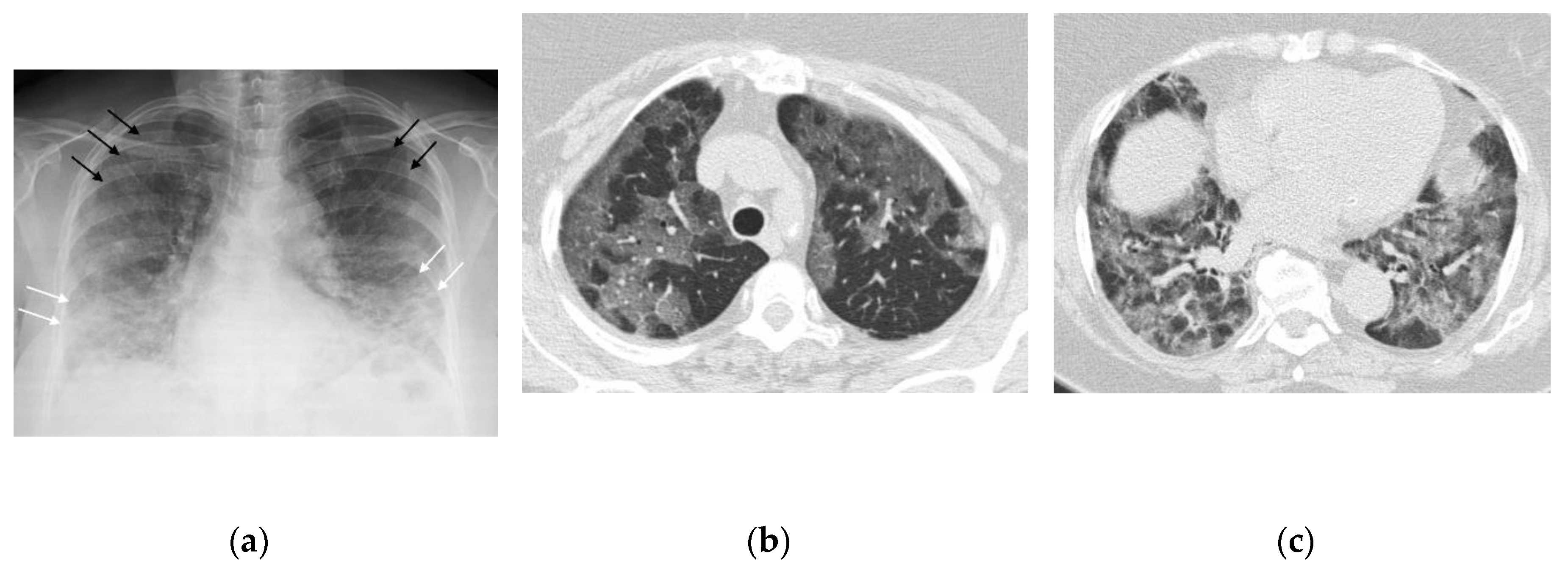
- Typical: Multifocal peripheral or central areas without a clear definition of vascular structure contours (opacity type 1) or a significant and variable increase in parenchymal density with a hazy appearance (opacity type 2); consolidations (opacity type 3) may be present but are associated with one of the other opacities.
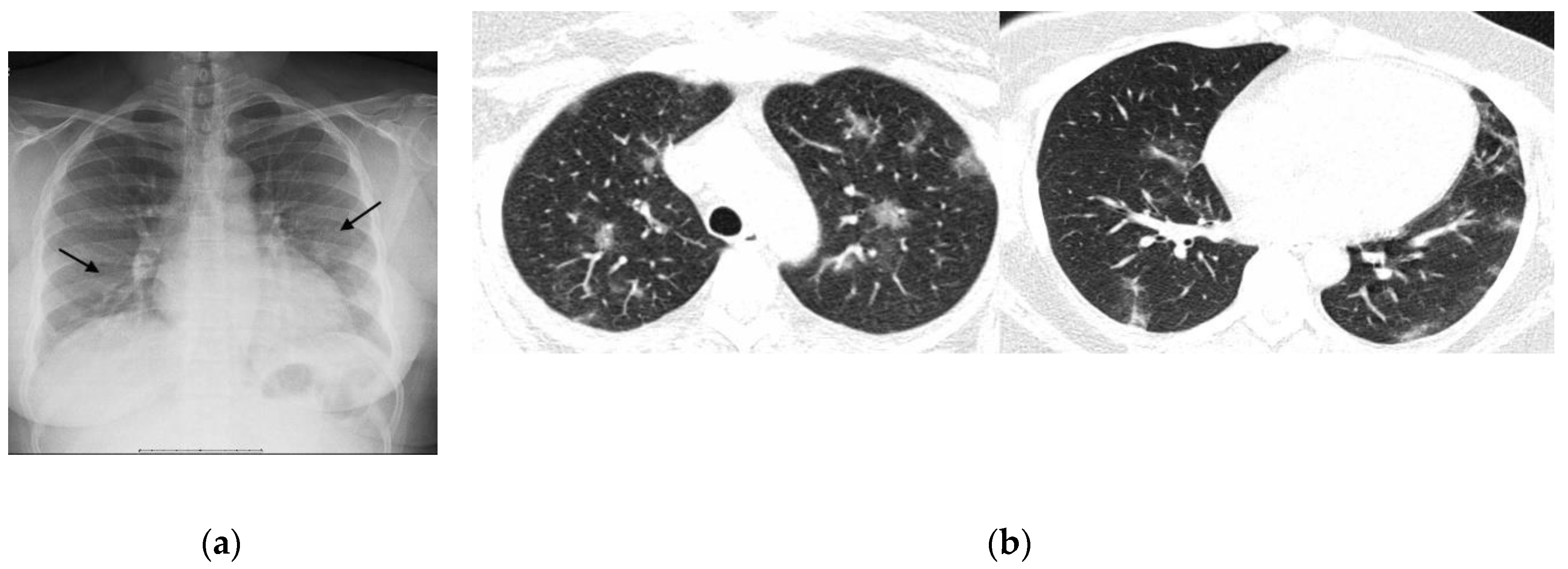
- Possible: Opacities without a multifocal pattern or opacities type 1 and 2 in only one lobe or the upper thirds of the lungs.
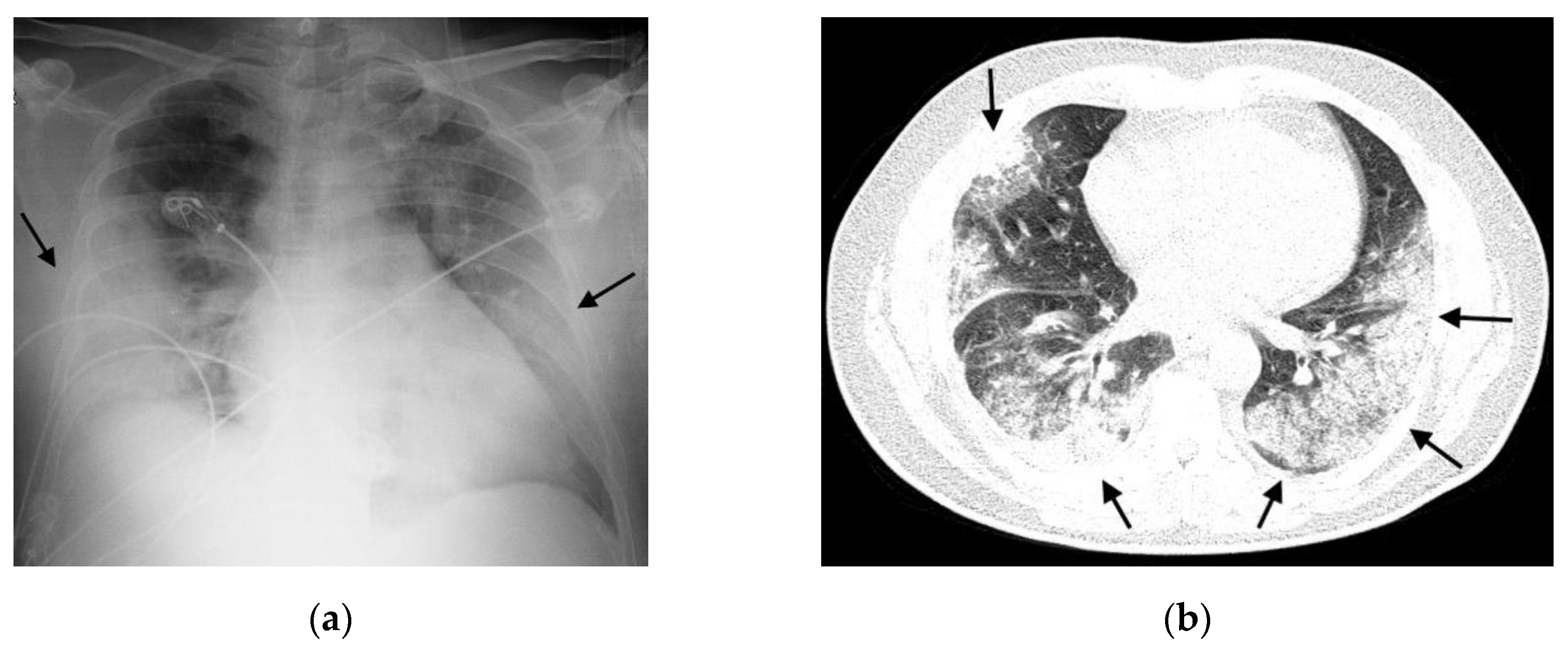
- Atypical: Absence of typical or possible patterns, along with the presence of one or more of the following findings: cavities or isolated lobar/segmental consolidation (resembling bacterial pneumonia); micronodules; signs of pulmonary congestion and pleural effusions; or extensive pleural effusions.
- Negative: No findings indicative of pulmonary diseases.
3. Results
3.1. Associations Between Clinical and Radiographic Variables and Outcomes (Asymptomatic, Symptomatic, and Death)
3.2. Influence of Comorbidities on Radiographic Changes
3.3. Influence of Age on Outcome
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
Abbreviations
| AP | Anteroposterior |
| CAAE | Certificate of Presentation for Ethical Appreciation |
| COVID-19 | Coronavirus Disease 2019 |
| CT | Computed tomography |
| CXR | Chest X-ray |
| DM | Diabetes mellitus |
| HUPE | Pedro Ernesto University Hospital |
| IQR | Interquartile range |
| PA | Posteroanterior |
| RT-PCR | Reverse transcription-polymerase chain reaction |
| SAH | Systemic arterial hypertension |
| SARS-CoV-2 | Severe Acute Respiratory Syndrome Coronavirus 2 |
| WHO | World Health Organization |
References
- Pereira, I.D.R.; Soares, O.A.B. Análise de casos de COVID-19 no Hospital Central do Exército (HCE) durante a pandemia com ênfase nos aspectos tomográficos. Brasil, 2020. Trabalho de Conclusão de Curso (Curso de Aperfeiçoamento de Oficiais Médicos) – Escola de Saúde do Exército. Available online: http://bdex.eb.mil.br/jspui/handle/123456789/8160 (accessed on 2 July 2024).
- World Health Organization. Clinical Management of COVID-19. 2020. Available online: https://www.who.int/news-room/detail/29-06-2020-covidtimeline (accessed on 2 July 2024).
- Brasil. Ministério da Saúde. Protocolo de manejo clínico para o novo coronavírus (2019-nCoV). Brasília: MS, 2020. Available online: https://portaldeboaspraticas.iff.fiocruz.br/biblioteca/protocolo-de-manejo-clinico-para-o-novo-coronavirus2019-ncov/ (accessed on 2 July 2024).
- Perlman, S.; McIntosh, K. Mandell, Douglas and Bennett's principles and practice of Infectious Diseases. 2020, p. 2072–2080.
- Bosch, B.J.; Van Der Zee, R.; Haan, C.A.M.; Rottier, P.J.M. The coronavirus spike protein is a class I virus fusion protein: structural and functional characterization of the fusion core complex. J. Virol. 2003, 77, 8801–8811. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Liu, Q.; Guo, D. Emerging coronaviruses: genome structure, replication, and pathogenesis. J. Med. Virol. 2020, 92, 418–423. [Google Scholar] [PubMed]
- Giovagnoni, A.; Agostini, A. Diagnosi radiologica e prevenzione della diffusione di COVID-19 nei Dipartimenti di Radiologia. 2020. Available online: https://www.sirm.org/wp-content/uploads/2020/03/SIRM-Covid-19.pdf (accessed on 2 July 2024).
- Remuzzi, A.; Remuzzi, G. COVID-19 and Italy: what next? Lancet 2020, 395, 1225–1228. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar]
- Hui, D.S.; Azhar, E.I.; Madani, T.A.; Ntoumi, F.; Koch, R.; Dar, O.; et al. The continuing 2019-nCoV epidemic threat of novel coronaviruses to global health: The latest 2019 novel coronavirus outbreak in Wuhan, China. Int. J. Infect. Dis. 2020, 91, 264–266. [Google Scholar]
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Ou, C.Q.; He, J.X.; et al. Clinical characteristics of coronavirus disease 2019 in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar]
- Pecho-Silva, S.; Navarro-Solsol, A.C.; Taype-Rondan, A.; Torres-Valencia, J.; Arteaga-Livias, K.; Herriman, D.A.; et al. Pulmonary ultrasound in the diagnosis and monitoring of coronavirus disease (COVID-19): a systematic review. Ultrasound Med. Biol. 2021, 47, 1997–2005. [Google Scholar] [CrossRef]
- Lopes, A.J.; Mafort, T.T.; Da Costa, C.H.; Rufino, R.; De Cássia Firmida, M.; Kirk, K.M.; et al. Comparison Between Lung Ultrasound and Computed Tomographic Findings in Patients With COVID-19 Pneumonia. J. Ultrasound Med. 2021, 41, 1391–1399. [Google Scholar]
- Zhao, Y.; Xiang, C.; Wang, S.; Peng, C.; Zou, Q.; Hu, J. Radiology department strategies to protect radiologic technologists against COVID-19: experience from Wuhan. Eur. J. Radiol. 2020, 127, 108996. [Google Scholar]
- Ai, T.; Yang, Z.; Hou, H.; Zhan, C.; Chen, C.; Lv, W.; et al. Correlation of Chest CT and RT-PCR Testing for Coronavirus Disease 2019 (COVID-19) in China: A Report of 1014 Cases. Radiology 2020, 296, E32–E40. [Google Scholar]
- Kim, H.; Hong, H.; Yoon, S.H. Diagnostic performance of CT and reverse transcriptase-polymerase chain reaction for coronavirus disease 2019: a meta-analysis. Radiology 2020, 296, E145–E155. [Google Scholar] [CrossRef]
- Song, F.; Shi, N.; Shan, F.; Zhang, Z.; Shen, J.; Lu, H.; et al. Emerging 2019 Novel Coronavirus (2019-nCoV) Pneumonia. Radiology 2020, 295, 210–217. [Google Scholar] [CrossRef]
- Pan, F.; Ye, T.; Sun, P.; Gui, S.; Liang, B.; Li, L.; et al. Time Course of Lung Changes at Chest CT during Recovery from Coronavirus Disease 2019 (COVID-19). Radiology 2020, 295, 715–721. [Google Scholar] [PubMed]
- De Jaegere, T.M.H.; Krdzalic, J.; Fasen, B.; Kwee, R.M. Radiological Society of North America Chest CT Classification System for Reporting COVID-19 Pneumonia: interobserver variability and correlation with reverse-transcription polymerase chain reaction. Radiol. Cardiothorac. Imaging 2020, 2, e200213. [Google Scholar]
- Hope, M.D.; Raptis, C.A.; Shah, A.; Hammer, M.M.; Henry, T.S. A role for CT in COVID-19? What data really tell us so far. Lancet 2020, 395, 1189–1190. [Google Scholar]
- Bandirali, M.; Sconfienza, L.M.; Serra, R.; Brembilla, R.; Albano, D.; Pregliasco, F.E.; et al. Chest radiograph findings in asymptomatic and minimally symptomatic quarantined patients in Codogno, Italy during COVID-19 pandemic. Radiology 2020, 295, E7–E8. [Google Scholar] [CrossRef] [PubMed]
- Choi, H.; Qi, X.; Yoon, S.H.; Park, S.J.; Lee, K.H.; Kim, J.Y.; et al. Extension of coronavirus disease 2019 (COVID-19) on chest CT and implications for chest radiograph interpretation. Radiol. Cardiothorac. Imaging 2020, 2, e200107. [Google Scholar] [CrossRef]
- Yoon, S.H.; Lee, K.H.; Kim, J.Y.; Lee, Y.K.; Ko, H.; Kim, K.H.; et al. Chest Radiographic and CT Findings of the 2019 Novel Coronavirus Disease (COVID-19): Analysis of nine patients treated in Korea. Korean J. Radiol. 2020, 21, 494–500. [Google Scholar]
- Litmanovich, D.E.; Chung, M.; Kirkbride, R.K.; Kicska, G.; Kanne, J.P. Review of chest radiograph findings of COVID-19 pneumonia and suggested reporting language. J. Thorac. Imaging 2020, 35, 219–227. [Google Scholar]
- Toussie, D.; Voutsinas, N.; Finkelstein, M.; Cedillo, M.A.; Manna, S.; Maron, S.Z.; et al. Clinical and chest radiography features determine patient outcomes in young and middle age adults with COVID-19. Radiology 2020, 297, E197–E206. [Google Scholar]
- Vancheri, S.G.; Savietto, G.; Ballati, F.; Maggi, A.; Canino, C.; Bortolotto, C.; et al. Radiographic findings in 240 patients with COVID-19 pneumonia: time-dependence after the onset of symptoms. Eur. Radiol. 2020, 30, 6161–6169. [Google Scholar]
- Parekh, M.; Donuru, A.; Balasubramanya, R.; Kapur, S. Review of the Chest CT differential diagnosis of ground-glass opacities in the COVID Era. Radiology 2020, 297, E289–E302. [Google Scholar] [PubMed]
- Simpson, S.; Kay, F.U.; Abbara, S.; Bhalla, S.; Chung, J.H.; Chung, M.; et al. Radiological Society of North America Expert Consensus Statement on Reporting Chest CT Findings Related to COVID-19. J. Thorac. Imaging 2020, 35, 219–227. [Google Scholar] [PubMed]
- Kirkpatrick, J.N.; Swaminathan, M.; Adedipe, A.; Garcia-Sayan, E.; Hung, J.; Kelly, N.; et al. American Society of Echocardiography COVID-19 Statement Update: Lessons Learned and Preparation for Future Pandemics. J. Am. Soc. Echocardiogr. 2023, 36, 1127–1139. [Google Scholar] [PubMed]
- Hochhegger, B.; Zanon, M.; Altmayer, S.; Mandelli, N.S.; Stüker, G.; Mohammed, T.L.; et al. COVID-19 mimics on chest CT: a pictorial review and radiologic guide. Br. J. Radiol. 2021, 94, 20200703. [Google Scholar]
- Torres, P.P.T.; Irion, K.L.; Marchiori, E. COVID-19: radiografia de tórax na predição de desfecho clínico. J. Bras. Pneumol. 2020, 46, e20200464. [Google Scholar]
- Alencar, J.R.M.; Taumaturgo, I.C.B. A importância da utilização de exames radiológicos no diagnóstico da Covid-19. Braz. J. Dev. 2021, 7, 66545–66554. [Google Scholar]
- Rosenthal, N.; Cao, Z.; Gundrum, J.; Sianis, J.; Safo, S. Risk factors associated with in-hospital mortality in a US National Sample of Patients with COVID-19. JAMA Netw. Open 2020, 3, e2020352. [Google Scholar]
- Capone, D.; Capone, R.; Pereira, A.C.H.; Bruno, L.P.; Visconti, N.R.G.R.; Jansen, J.M. Diagnóstico por imagem na pneumonia por COVID-19. Pulmão RJ 2020, 29, 22–27. [Google Scholar]
- Feitoza, T.M.O.; Chaves, A.M.; Muniz, G.T.S.; Da Cruz, M.C.C.; Junior, I.F.C. Comorbidades e COVID-19: uma revisão integrativa. Rev. Interfaces 2020, 8, 711–723. [Google Scholar]
- Abate, S.M.; Checkol, Y.A.; Mantefardoc, B. Prevalence and risk factors of mortality among hospitalized patients with COVID-19: A systematic review and Meta-analysis. Ann. Med. Surg. 2021, 64, 102204. [Google Scholar]
- Da Silva, A.L.O.; Moreira, J.C.; Martins, S.R. COVID-19 e tabagismo: uma relação de risco. Cad. Saúde Pública 2020, 36, e00072020. [Google Scholar]
- Mogami, R. Comparison between lung ultrasound and computed tomographic findings in patients with COVID-19 pneumonia. J. Ultrasound Med. 2021, 40, 1391–1399. [Google Scholar]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar]
- Wong, H.Y.F.; Lam, H.Y.S.; Fong, A.H.; Leung, S.T.; Chin, T.W.; Lo, C.S.Y.; et al. Frequency and distribution of chest radiographic findings in COVID-19 positive patients. Radiology 2019, 296, E72–E78. [Google Scholar]
- Baratella, E.; Crivelli, P.; Marrocchio, C.; Bozzato, A.M.; Vito, A.; Madeddu, G.; et al. Gravidade do comprometimento pulmonar em radiografias de tórax de pacientes infectados por SARS-coronavirus-2 como possível ferramenta para prever a evolução clínica: análise retrospectiva observacional da relação entre dados radiológicos, clínicos e laboratoriais. J. Bras. Pneumol. 2020, 46, e20200226. [Google Scholar]
- George, P.M.; Barratt, S.L.; Condliffe, R.; Desai, S.R.; Devaraj, A.; Forrest, I.; et al. Respiratory follow-up of patients with COVID-19 pneumonia. Thorax 2020, 75, 1009–1016. [Google Scholar]
| Variable | Total Sample | Asymptomatic | Symptomatic | Death | p valor | ||||
|---|---|---|---|---|---|---|---|---|---|
| n | % | N | % | n | % | n | % | ||
| Age group | |||||||||
| ≥ 60 years | 35 | 54.7 | 8 | 33.3 | 8 | 44.4 | 19 | 86.4 | 0.001 |
| < 60 years | 29 | 45.3 | 16 | 66.7 | 10 | 55.6 | 3 | 13.6 | |
| Gender | |||||||||
| Male | 33 | 51.6 | 14 | 58.3 | 8 | 44.4 | 11 | 50 | 0.66 |
| Female | 31 | 48.4 | 10 | 41.7 | 10 | 55.6 | 11 | 50 | |
| Comorbidities | |||||||||
| Yes | 44 | 83 | 17 | 85 | 10 | 62.5 | 17 | 100 | 0.010 |
| No | 9 | 17 | 3 | 15 | 6 | 37.5 | 0 | 0 | |
| Diabetes mellitus | |||||||||
| Yes | 11 | 20.8 | 3 | 15 | 3 | 18.8 | 5 | 29.4 | 0.64 |
| No | 42 | 79.2 | 17 | 85 | 13 | 81.3 | 12 | 70.6 | |
| Obesity | |||||||||
| Yes | 3 | 5.7 | 1 | 5 | 1 | 6.3 | 1 | 5.9 | 0.99 |
| No | 50 | 94.3 | 19 | 95 | 15 | 93.8 | 16 | 94.1 | |
| Systemic arterial hypertension | |||||||||
| Yes | 23 | 43.4 | 7 | 35 | 6 | 37.5 | 10 | 58.8 | 0.29 |
| No | 30 | 56.6 | 13 | 65 | 10 | 62.5 | 7 | 41.2 | |
| Chronic obstructive pulmonary disease | |||||||||
| Yes | 1 | 1.9 | 0 | 0 | 0 | 0 | 1 | 5.9 | 0.62 |
| No | 52 | 98.1 | 20 | 100 | 16 | 100 | 16 | 94.1 | |
| Smoking | |||||||||
| Yes | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | NA |
| No | 53 | 100 | 20 | 100 | 16 | 100 | 17 | 100 | |
| Former smoking | |||||||||
| Yes | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | NA |
| No | 53 | 100 | 20 | 100 | 16 | 100 | 17 | 100 | |
| Classic symptoms | |||||||||
| Yes | 43 | 74.1 | 15 | 65.2 | 14 | 82.4 | 14 | 77.8 | 0.52 |
| No | 15 | 25.9 | 8 | 34.8 | 3 | 17.6 | 4 | 22.2 | |
| Mechanical ventilation | |||||||||
| Yes | 6 | 9.7 | 0 | 0 | 2 | 11.8 | 4 | 19 | 0.065 |
| No | 56 | 90.3 | 24 | 100 | 15 | 88.2 | 17 | 81 | |
| PCR result | |||||||||
| Yes | 42 | 65.6 | 14 | 58.3 | 14 | 77.8 | 14 | 63.6 | 0.41 |
| No | 22 | 34.4 | 10 | 41.7 | 4 | 22.2 | 8 | 36.4 | |
| Variable | Total Sample | Asymptomatic | Symptomatic | Death | p valor | ||||
|---|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | n | % | ||
| CXR Pattern | |||||||||
| Positive | 44 | 68.8 | 18 | 75 | 10 | 55.6 | 16 | 72.7 | 0.36 |
| Negative | 20 | 31.3 | 6 | 25 | 8 | 44.4 | 6 | 27.3 | |
| Disease Extent on CXR | |||||||||
| Mild/Moderate | 20 | 42.6 | 10 | 55.6 | 2 | 20 | 8 | 42.1 | 0.21 |
| Severe | 27 | 57.4 | 8 | 44.4 | 8 | 80 | 11 | 57.9 | |
| Type 1 Opacities | |||||||||
| Yes | 18 | 37.5 | 11 | 57.9 | 3 | 30 | 4 | 21.1 | 0.056 |
| No | 30 | 62.5 | 8 | 42.1 | 7 | 70 | 15 | 78.9 | |
| Type 2 Opacities | |||||||||
| Yes | 34 | 70.8 | 10 | 52.6 | 9 | 90 | 15 | 78.9 | 0.099 |
| No | 14 | 29.2 | 9 | 47.4 | 1 | 10 | 4 | 21.1 | |
| Type 3 Opacities | |||||||||
| Yes | 18 | 37.5 | 3 | 15.8 | 6 | 60 | 9 | 47.4 | 0.028 |
| No | 30 | 62.5 | 16 | 84.2 | 4 | 40 | 10 | 52.6 | |
| Lung Involvement | |||||||||
| Unilateral | 4 | 8.5 | 3 | 16.7 | 0 | 0 | 1 | 5.3 | 0.42 |
| Bilateral | 43 | 91.5 | 15 | 83.3 | 10 | 100 | 18 | 94.7 | |
| Presence of Symmetry | |||||||||
| Symmetric | 14 | 29.8 | 5 | 27.8 | 3 | 30 | 6 | 31.6 | 0.99 |
| Asymmetric | 33 | 70.2 | 13 | 72.2 | 7 | 70 | 13 | 68.4 | |
| Transverse Axis Alterations | |||||||||
| Peripheral | 4 | 8.5 | 3 | 16.7 | 1 | 10 | 0 | 0 | 0.19 |
| Non-peripheral | 43 | 91.5 | 15 | 83.3 | 9 | 90 | 19 | 100 | |
| Longitudinal Axis Alterations | |||||||||
| Without predominance | 23 | 48.9 | 7 | 38.9 | 6 | 60 | 10 | 52.6 | 0.56 |
| With predominance | 24 | 51.1 | 11 | 61.1 | 4 | 40 | 9 | 47.4 | |
| Variable | Total Sample | With Comorbidities | Without Comorbidities | p valor | ||||
|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | |||
| CXR pattern | ||||||||
| Positive | 35 | 66 | 29 | 65.9 | 6 | 66.7 | 0.64 | |
| Negative | 18 | 34 | 15 | 34.1 | 3 | 33.3 | ||
| Disease extent on CXR | ||||||||
| Mild/Moderate | 17 | 44.7 | 13 | 40.6 | 4 | 66.7 | 0.23 | |
| Severe | 21 | 55.3 | 19 | 59.4 | 2 | 33.3 | ||
| Type 1 opacities | ||||||||
| Yes | 13 | 34.2 | 10 | 31.3 | 3 | 50 | 0.33 | |
| No | 25 | 65.8 | 22 | 68.8 | 3 | 50 | ||
| Type 2 opacities | ||||||||
| Yes | 28 | 73.7 | 23 | 71.9 | 5 | 83.3 | 0.49 | |
| No | 10 | 26.3 | 9 | 28.1 | 1 | 16.7 | ||
| Type 3 opacities | ||||||||
| Yes | 15 | 39.5 | 13 | 40.6 | 2 | 33.3 | 0.56 | |
| No | 23 | 60.5 | 19 | 59.4 | 4 | 66.7 | ||
| Lung involvement | ||||||||
| Unilateral | 3 | 7.9 | 3 | 9.4 | 0 | 0 | 0.59 | |
| Bilateral | 35 | 92.1 | 29 | 90.6 | 6 | 100 | ||
| Presence of symmetry | ||||||||
| Symmetric | 11 | 28.9 | 7 | 21.9 | 4 | 66.7 | 0.046 | |
| Asymmetric | 27 | 71.1 | 25 | 78.1 | 2 | 33.3 | ||
| Transverse axis alterations | ||||||||
| Peripheral | 4 | 10.5 | 4 | 12.5 | 0 | 0 | 0.49 | |
| Non-peripheral | 34 | 89.5 | 28 | 87.5 | 6 | 100 | ||
| Longitudinal axis alterations | ||||||||
| Without predominance | 18 | 47.4 | 15 | 46.9 | 3 | 50 | 0.62 | |
| With predominance | 20 | 52.6 | 17 | 53.1 | 3 | 50 | ||
| Sample | n | mean | SD | Median | IQR | Minimum | Maximum |
|---|---|---|---|---|---|---|---|
| Total | 64 | 58.3 | 18.7 | 62 | 41 - 73 | 19 | 96 |
| Asymptomatic | 24 | 50.8 | 18.4 | 50 | 36 – 70 | 25 | 84 |
| Symptomatic | 18 | 55 | 18.8 | 58 | 39 – 70 | 19 | 96 |
| Death | 22 | 69 | 14.1 | 73 | 63 – 77 | 25 | 91 |
| Alive | 42 | 52.6 | 18.5 | 52 | 37 - 70 | 19 | 96 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




