Submitted:
28 February 2025
Posted:
03 March 2025
You are already at the latest version
Abstract
The aging of the population and, consequently, dementias represent a priority for global public health. This door-to-door epidemiological study was conducted in a small agricultural community with no migratory flows in the past few decades in Campania. The aim was to identify lifestyles that may be either favourable to the development of dementia. A total of 206 participants were recruited from 502 individuals aged 60 and over. The residents were assessed using the Montreal Cognitive Assessment (MoCA) and Cognitive Reserve Index questionnaire. Regarding the factors associated with cognitive decline, there was a statistically significant association between older age and impairment in MoCA scores. Additionally, a statistically significant association was found between altered MoCA scores and weight loss over the past six months (p < 0.048). A statistically significant association was found between altered MoCA scores and the perception of cognitive deficit (p < 0.029). In conclusion, in our homogeneous community, a low prevalence of cognitive decline was observed, with cognitive reserve playing an important protective role, while advanced age, weight loss, and subjective cognitive deficit were identified as risk factors. Additionally, a low prevalence of cognitive deficits emerged, which may be associated with the habits and lifestyle of the inhabitants.
Keywords:
1. Introduction
- Determining whether cognitive reserve acts as a protective factor against cognitive decline.
- Examining the factors contributing to cognitive decline in the rural municipality of Comiziano.
2. Materials and Methods
3. Results
3.1. Results and Statistical Analysis
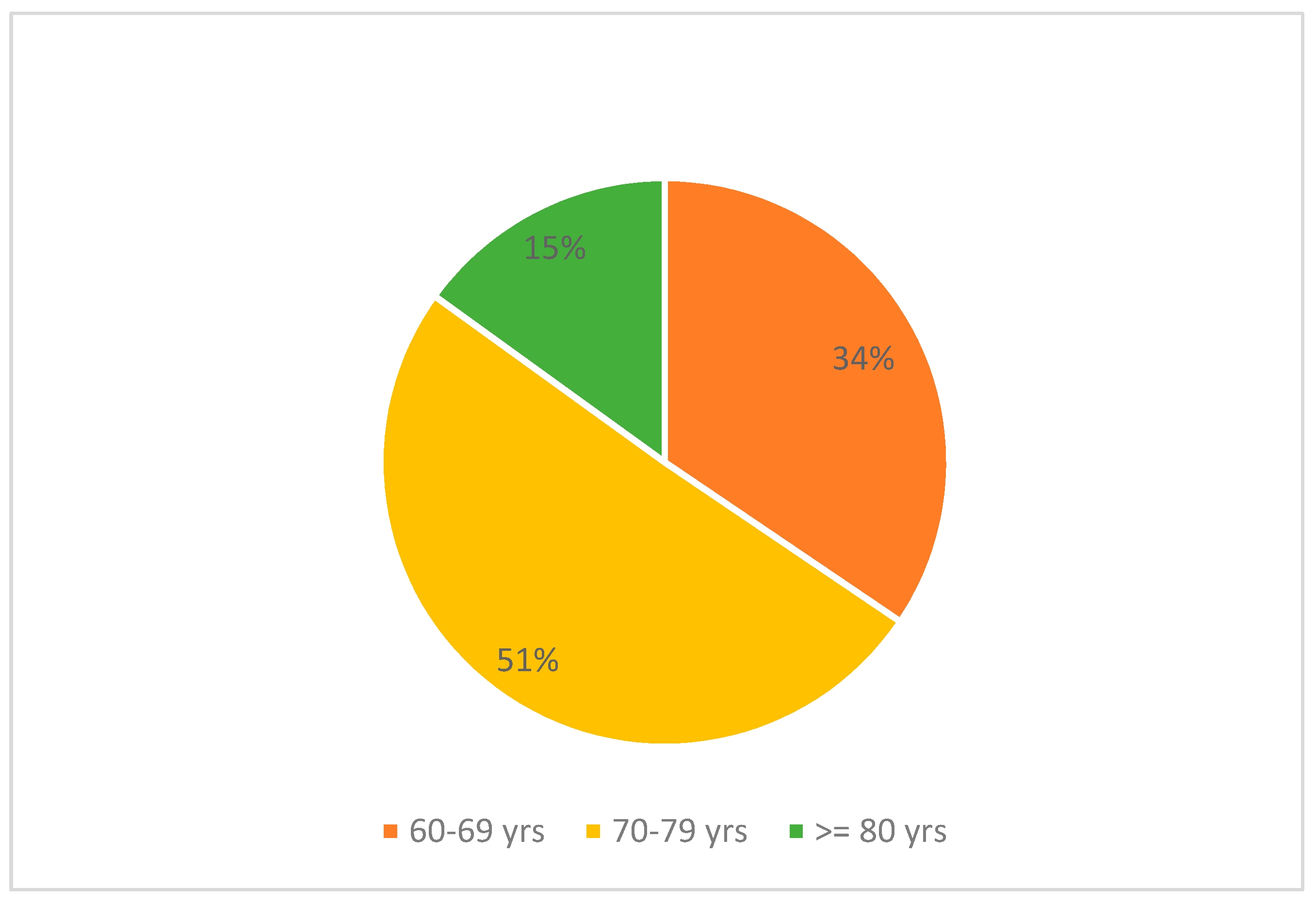
- We recruited 206 individuals over the age of 60, of whom 51.9% were women. The average age of the participants was 72 ± 6.77 years (Figure 1), and the average level of education was 9.45 ± 4.85 years (Figure 2). The average BMI was 27.7 ± 4.22 kg/m²; 36.4% reported having lost weight in the over the past six months. 10.7% felt they had a cognitive deficit. 83% of the participants had comorbidities (Table 1; Table 2). The average score on the MoCA, corrected for age and education, was 21.7 ± 3.57. The mean total CRIq score was 93.9 ± 18.8. (Table 3)
- We considered two populations: one with a normal MoCA score corrected for age and education (>17.54) and another that includes both the altered MoCA (<15.5) and borderline MoCA (15.5–17.54), as the latter also require further in-depth testing.
- Twenty-six out of 206 (12.6%) subjects had an impaired or borderline MoCA, corrected for age and education.
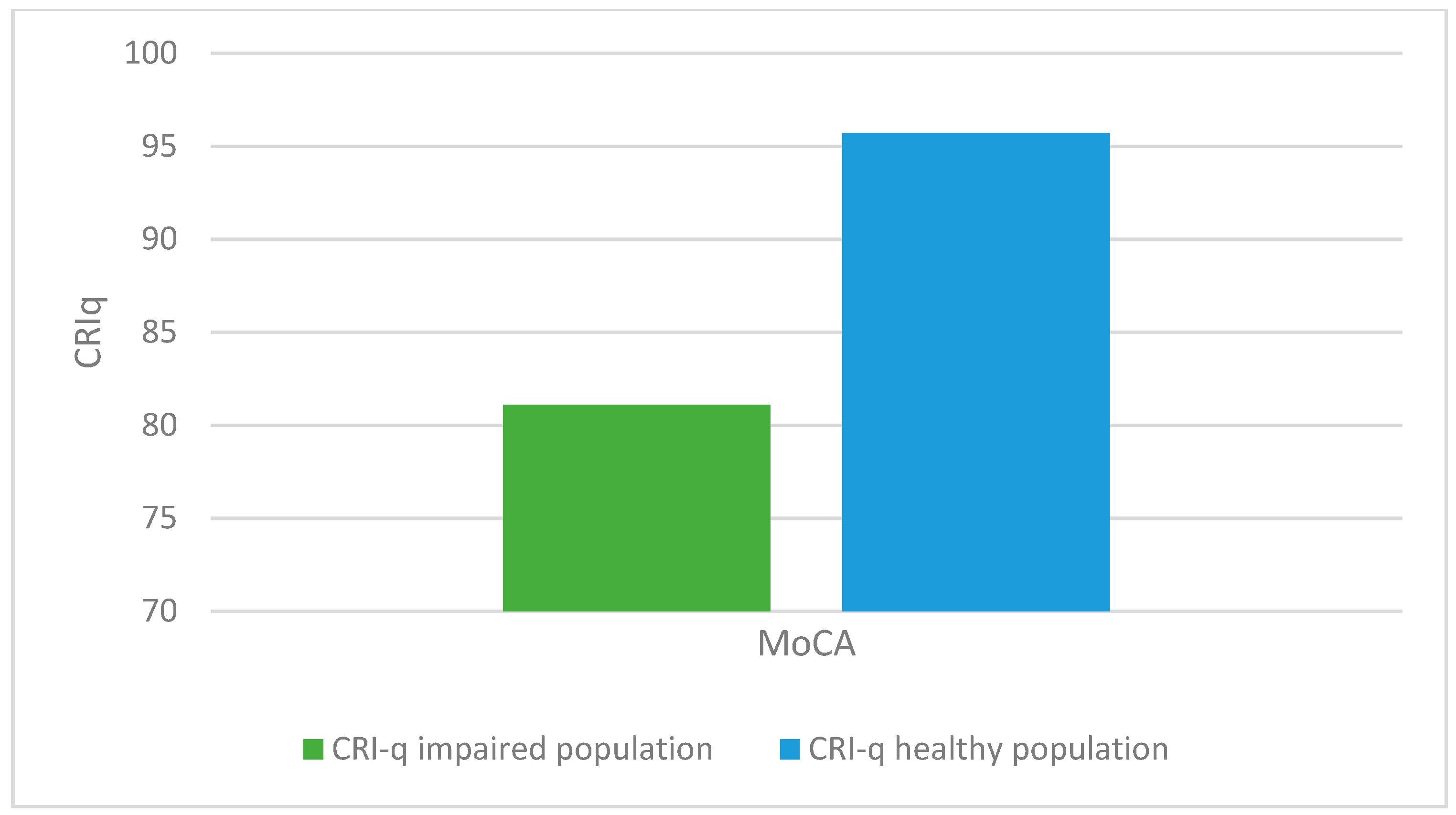
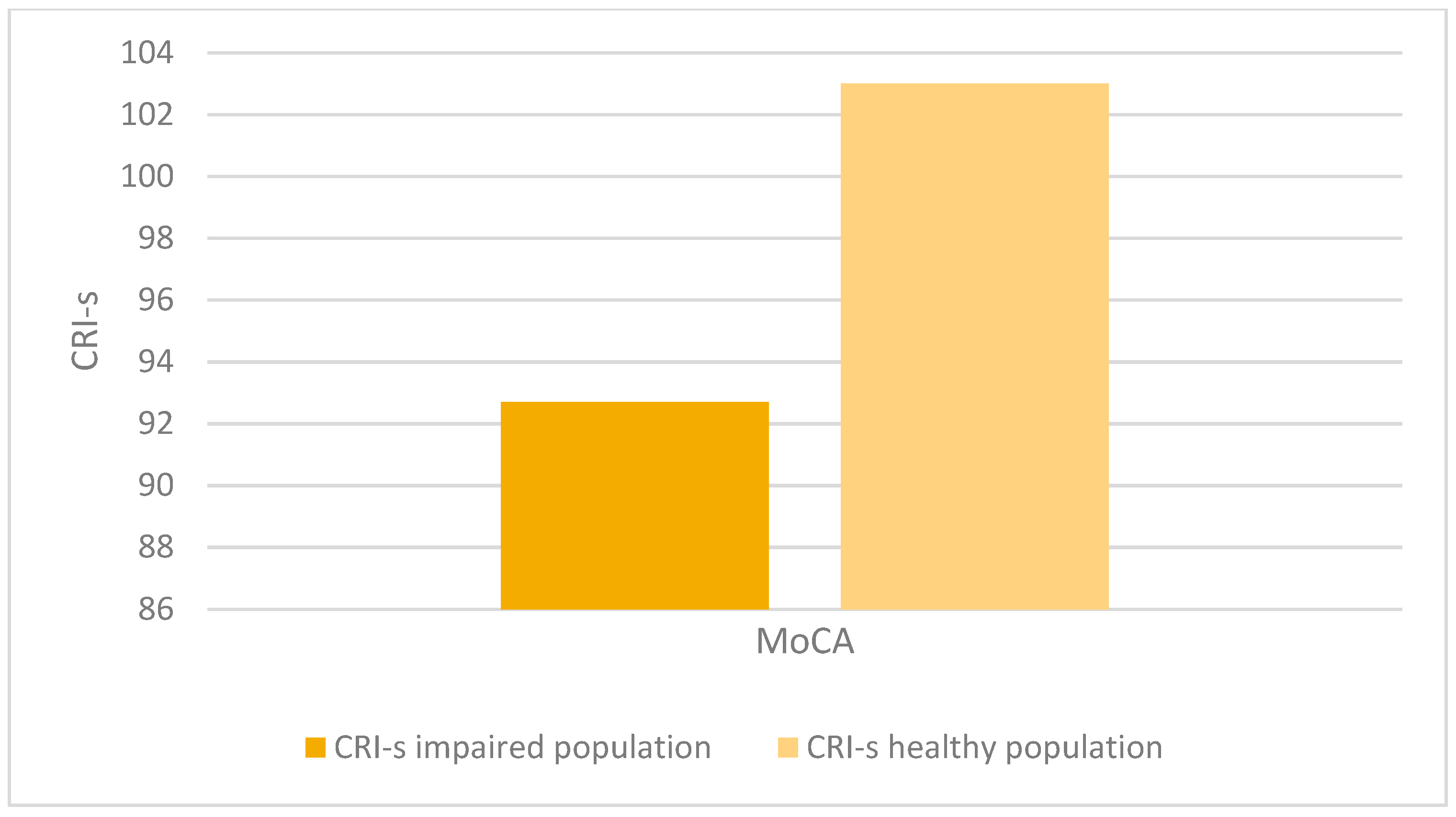
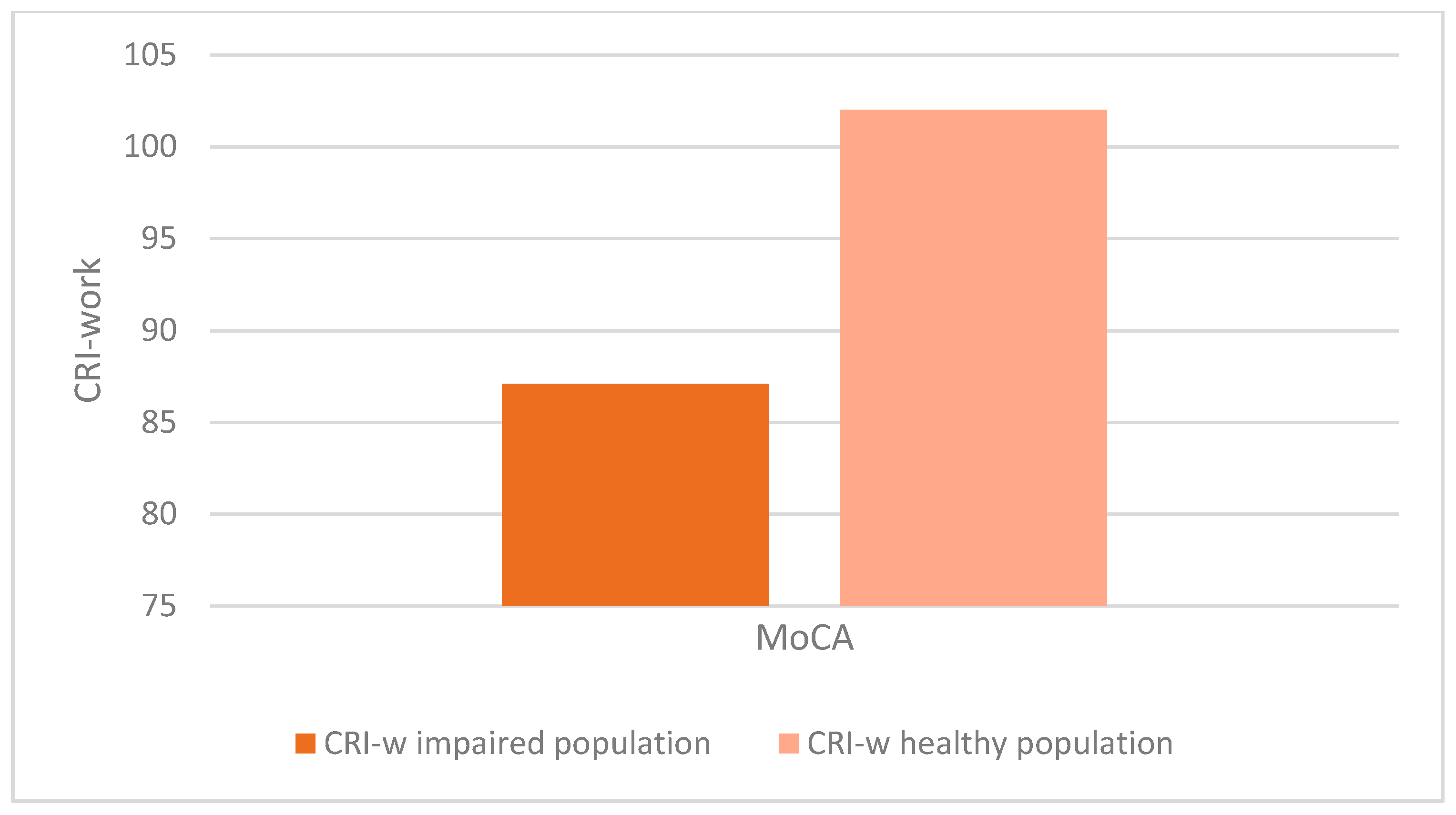
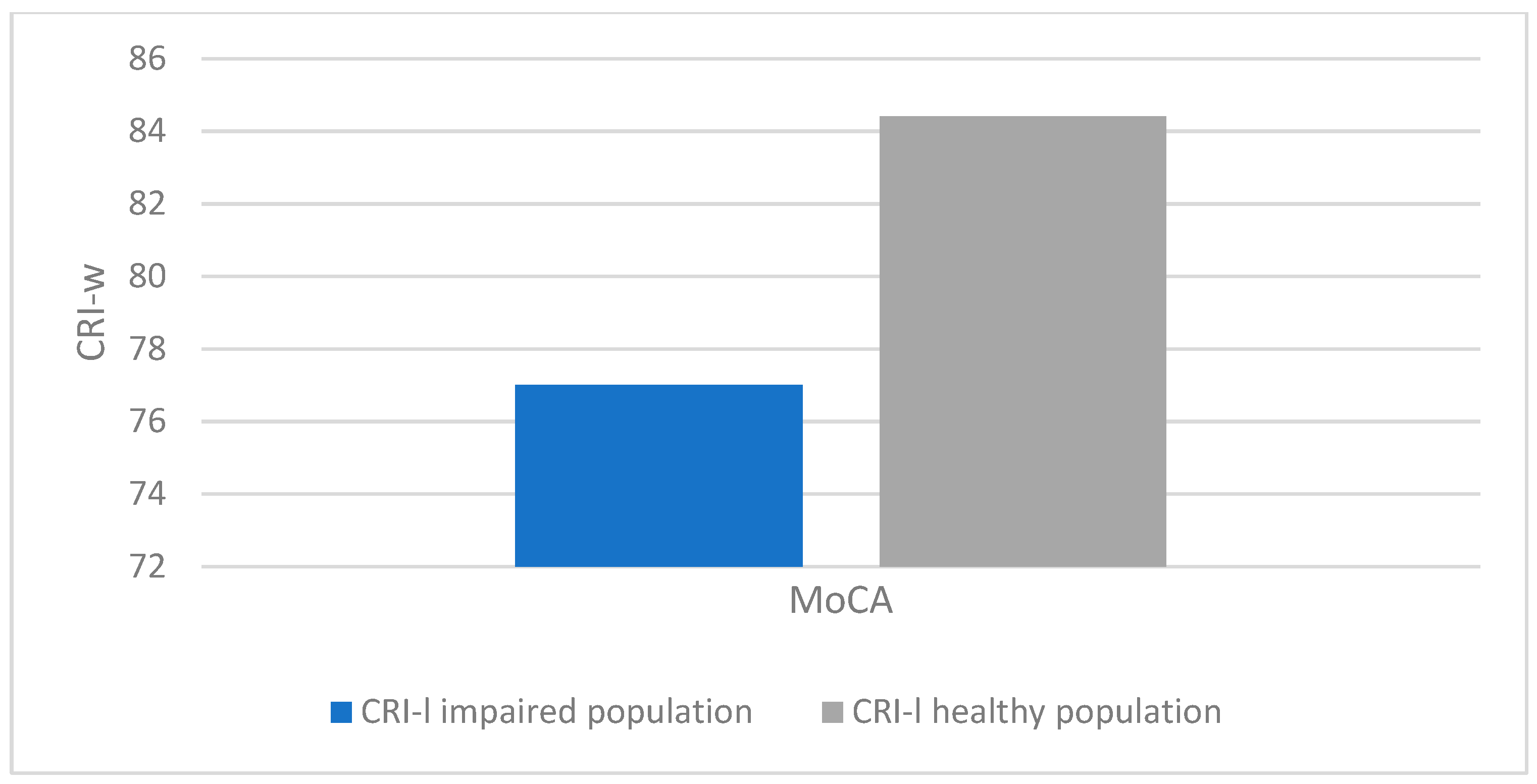
- There was a statistically significant association between altered MoCA scores (corrected for age and education) and lower CRIq scores (impaired population: µ = 81.1; σ = 15.5; healthy population: µ = 95.7; σ = 18.5; p < 0.001), which was also confirmed in CRI items: School (impaired population: µ = 92.7; σ = 11.5; healthy population: µ = 102.6; σ = 14.5; p < 0.003), Work (impaired population: µ = 87.1; σ = 16.2; healthy population: µ = 102.1; σ = 24.5; p < 0.008), Leisure-time (impaired population: µ = 77; σ = 15.2; healthy population: µ = 84.4; σ = 13.7; p < 0.03), as confirmed by the Kruskal-Wallis test (Figure 3, Figure 4, Figure 5 and Figure 6).
- Regarding the factors associated with cognitive decline, there was a statistically significant association between older age and impairment in MoCA scores corrected for age and education (impaired population: µ = 75.08; σ = 7.15; healthy population: µ = 71.59; σ = 6.62; p < 0.014).
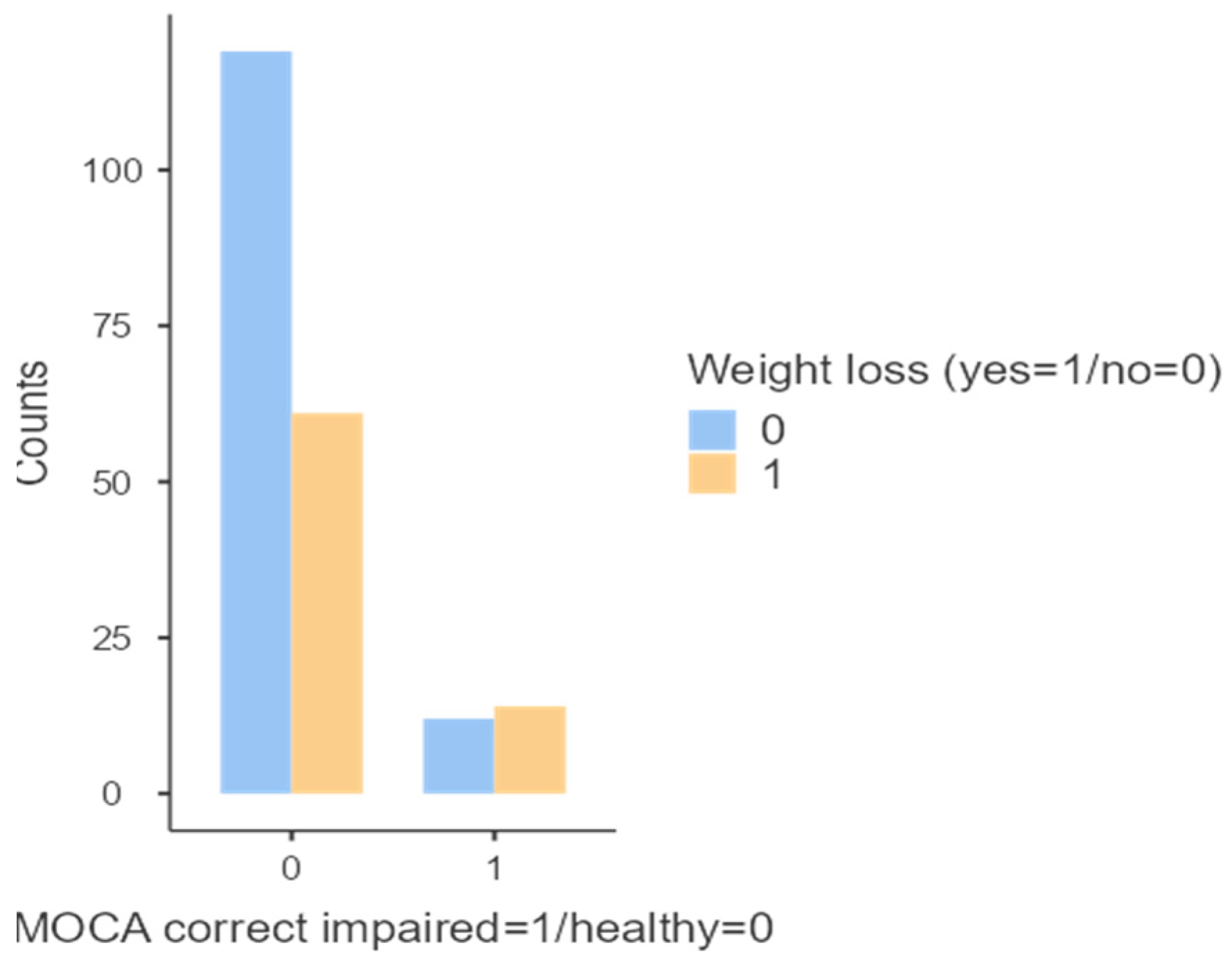
- Additionally, a statistically significant association was found between altered MoCA scores, corrected for age and education, and weight loss over the past six months (p < 0.048; Figure 7).
- No significant differences were observed in BMI (p = 0.680) or between genders (p = 0.142) (Table 4).
- No significant differences were found regarding the presence (p = 0.371) or type of comorbidities between the two populations (Normal MoCA corrected for age and education / altered and borderline MoCA). (Table 5)
- A statistically significant association was found between altered MoCA scores and the perception of cognitive deficit (p < 0.029).
- The prevalence of individuals with impaired or borderline MoCA scores in the total population was 12.6% (26/206).
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AD | Alzheimer’s disease |
| SCD | Subjective cognitive decline |
| MCI | Mild cognitive impairment |
| MoCA | Montreal Cognitive Assessment |
| BMI | Body mass index |
| MMSE | Mini Mental State Examination |
| CR | Cognitive reserve |
| CRIq | Cognitive Reserve Index questionnaire |
| CRI-E | Cognitive Reserve Index Education |
| CRI-W | Cognitive Reserve Index Work |
| CRI-L | Cognitive Reserve Index Leisure |
| BR | Brain reserve |
| Vad | Vascular dementia |
References
- Cummings J, Aisen PS, DuBois B, et al. Drug development in Alzheimer’s disease: the path to 2025. Alzheimers Res Ther. 2016; 8:39. Published 2016 Sep 20. [CrossRef]
- GBD 2019 Dementia Forecasting Collaborators. Estimation of the global prevalence of dementia in 2019 and forecasted prevalence in 2050: an analysis for the Global Burden of Disease Study 2019. Lancet Public Health. 2022; 7(2): E105-E125. [CrossRef]
- Jack CR, Jr, Knopman DS, Jagust WJ, et al. Tracking pathophysiological processes in Alzheimer’s disease: an updated hypothetical model of dynamic biomarkers. Lancet Neurol. 2013;12(2):207–216. [CrossRef]
- Scheltens P, Blennow K, Breteler MM, et al. Alzheimer’s disease. Lancet. 2016;388(10043):505-517. [CrossRef]
- Dubois, Bruno et al. “Advancing research diagnostic criteria for Alzheimer’s disease: the IWG-2 criteria.” The Lancet. Neurology vol. 13,6 (2014): 614-29. [CrossRef]
- Dubois B, Feldman HH, Jacova C, et al. Research criteria for the diagnosis of Alzheimer’s disease: revising the NINCDS-ADRDA criteria. Lancet Neurol. 2007;6(8):734-746. [CrossRef]
- Dubois B, Feldman HH, Jacova C, et al. Revising the definition of Alzheimer’s disease: a new lexicon. Lancet Neurol. 2010;9(11):1118-1127. [CrossRef]
- McKhann GM, Knopman DS, Chertkow H, et al. The diagnosis of dementia due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 2011;7(3):263-269. [CrossRef]
- Jessen F, Amariglio RE, van Boxtel M, et al. A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer’s disease. Alzheimers Dement. 2014;10(6):844-852. [CrossRef]
- Jessen F, Amariglio RE, Buckley RF, et al. The characterisation of subjective cognitive decline. Lancet Neurol. 2020;19(3):271-278. [CrossRef]
- National Institute on Aging. What causes Alzheimer’s disease. Avail- able at: https://www.nia.nih.gov/health/what- causes- Alzheimers- disease. Accessed December 18, 2021; 2022 Alzheimer’s disease facts and figures. Alzheimers Dement. 2022; 18(4):700-789. [CrossRef]
- Mayeux R, Saunders AM, Shea S, et al. Utility of the apolipoprotein E genotype in the diagnosis of Alzheimer’s disease. Alzheimer’s Disease Centers Consortium on Apolipoprotein E and Alzheimer’s Disease [published correction appears in N Engl J Med 1998 Apr 30; 338(18):1325]. N Engl J Med. 1998; 338(8):506-511. [CrossRef]
- Loy CT, Schofield PR, Turner AM, Kwok JB. Genetics of dementia. Lancet. 2014; 383(9919):828-840. https://doi.org/10.1016/S0140-6736(13)60630-3; Allwright M, Mundell HD, McCorkindale AN, et al. Ranking the risk factors for Alzheimer’s disease; findings from the UK Biobank study. Aging Brain. 2023; 3:100081. Published 2023 Jun 17. [CrossRef]
- Wolters FJ, van der Lee SJ, Koudstaal PJ, et al. Parental family history of dementia in relation to subclinical brain disease and dementia risk. Neurology. 2017; 88(17):1642-1649. [CrossRef]
- Risk Reduction of Cognitive Decline and Dementia: WHO Guidelines. Geneva: World Health Organization; 2019; Baumgart M, Snyder HM, Carrillo MC, Fazio S, Kim H, Johns H. Summary of the evidence on modifiable risk factors for cognitive decline and dementia: A population-based perspective. Alzheimers Dement. 2015;11(6):718-726. [CrossRef]
- Blazer DG, Yaffe K, Liverman CT, Committee on the Public Health Dimensions of Cognitive Aging; Board on Health Sciences Policy; Institute of Medicine, eds. Cognitive Aging: Progress in Understanding and Opportunities for Action. Washington (DC): National Academies Press (US); July 21, 2015. N: Washington (DC).
- Beydoun MA, Beydoun HA, Gamaldo AA, Teel A, Zonderman AB, Wang Y. Epidemiologic studies of modifiable factors associated with cognition and dementia: systematic review and meta-analysis. BMC Public Health. 2014; 14:643. Published 2014 Jun 24. [CrossRef]
- Lewis CR, Talboom JS, De Both MD, et al. Smoking is associated with impaired verbal learning and memory performance in women more than men. Sci Rep. 2021;11(1):10248. Published 2021 May 13. https://doi.org/10.1038/s41598-021-88923-z; Arnold SE, Arvanitakis Z, Macauley-Rambach SL, et al. Brain insulin resistance in type 2 diabetes and Alzheimer disease: concepts and conundrums. Nat Rev Neurol. 2018;14(3):168-181. [CrossRef]
- Gottesman RF, Schneider AL, Zhou Y, et al. Association Between Midlife Vascular Risk Factors and Estimated Brain Amyloid Deposition. JAMA. 2017;317(14):1443-1450. [CrossRef]
- Kivimäki M, Luukkonen R, Batty GD, et al. Body mass index and risk of dementia: Analysis of individual-level data from 1.3 million individuals. Alzheimers Dement. 2018;14(5):601-609. [CrossRef]
- Nasreddine ZS, Phillips NA, Bédirian V, Charbonneau S, Whitehead V, Collin I, Cummings JL, Chertkow H. Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc. 2005 Apr;53(4):695-9. https://doi.org/10.1111/j.1532-5415.2005.53221. x. Erratum in: J Am Geriatr Soc. 2019 Sep;67(9):1991. [CrossRef] [PubMed]
- Nucci M, Mapelli D, Mondini S. Cognitive Reserve Index questionnaire (CRIq): a new instrument for measuring cognitive reserve. Aging Clin Exp Res. 2012 Jun;24(3):218-26. Epub 2011 Jun 20. [CrossRef] [PubMed]
- Santangelo G, Siciliano M, Pedone R, Vitale C, Falco F, Bisogno R, Siano P, Barone P, Grossi D, Santangelo F, Trojano L. Normative data for the Montreal Cognitive Assessment in an Italian population sample. Neurol Sci. 2015 Apr;36(4):585-91. Epub 2014 Nov 8. [CrossRef] [PubMed]
- Stern, Y. Cognitive reserve in ageing and Alzheimer’s disease. Lancet Neurol. 2012 Nov;11(11):1006-12. [CrossRef] [PubMed] [PubMed Central]
- Serra L, Cercignani M, Petrosini L, Basile B, Perri R, Fadda L, Spanò B, Marra C, Giubilei F, Carlesimo GA, Caltagirone C, Bozzali M. Neuroanatomical correlates of cognitive reserve in Alzheimer disease. Rejuvenation Res. 2011 Apr;14(2):143-51. Epub 2011 Jan 4. [CrossRef] [PubMed]
- Herring A, Ambrée O, Tomm M, Habermann H, Sachser N, Paulus W, Keyvani K. Environmental enrichment enhances cellular plasticity in transgenic mice with Alzheimer-like pathology. Exp Neurol. 2009 Mar;216(1):184-92. Epub 2008 Dec 11. [CrossRef] [PubMed]
- Connell E, Le Gall G, Pontifex MG, Sami S, Cryan JF, Clarke G, Müller M, Vauzour D. Microbial-derived metabolites as a risk factor of age-related cognitive decline and dementia. Mol Neurodegener. 2022 Jun 17;17(1):43. [CrossRef] [PubMed] [PubMed Central]
- Kim KY, Ha J, Lee JY, Kim E. Weight loss and risk of dementia in individuals with versus without obesity. Alzheimers Dement. 2023 Dec;19(12):5471-5481. Epub 2023 May 22. [CrossRef] [PubMed]
- Emmerzaal TL, Kiliaan AJ, Gustafson DR. 2003-2013: a decade of body mass index, Alzheimer’s disease, and dementia. J Alzheimers Dis. 2015;43(3):739-55. [CrossRef] [PubMed]
- Mooldijk SS, de Crom TOE, Ikram MK, Ikram MA, Voortman T. Adiposity in the older population and the risk of dementia: The Rotterdam Study. Alzheimers Dement. 2023 May;19(5):2047-2055. Epub 2022 Nov 29. [CrossRef] [PubMed]
- Gu X, Shi Z, Liu S, Guan Y, Lu H, Zhang Y, Zhang M, Liu S, Yue W, Wu H, Wang X, Zhang Y, Ji Y. Incidence and risk factors of dementia and the primary subtypes in northern rural China. Medicine (Baltimore). 2021 Apr 2;100(13):e25343. [CrossRef] [PubMed] [PubMed Central]
- Spada RS, Stella G, Calabrese S, Bosco P, Anello G, Guéant-Rodriguez RM, Romano A, Benamghar L, Guéant JL. Prevalence of dementia in mountainous village of Sicily. J Neurol Sci. 2009 Aug 15;283(1-2):62-5. Epub 2009 Mar 4. [CrossRef] [PubMed]
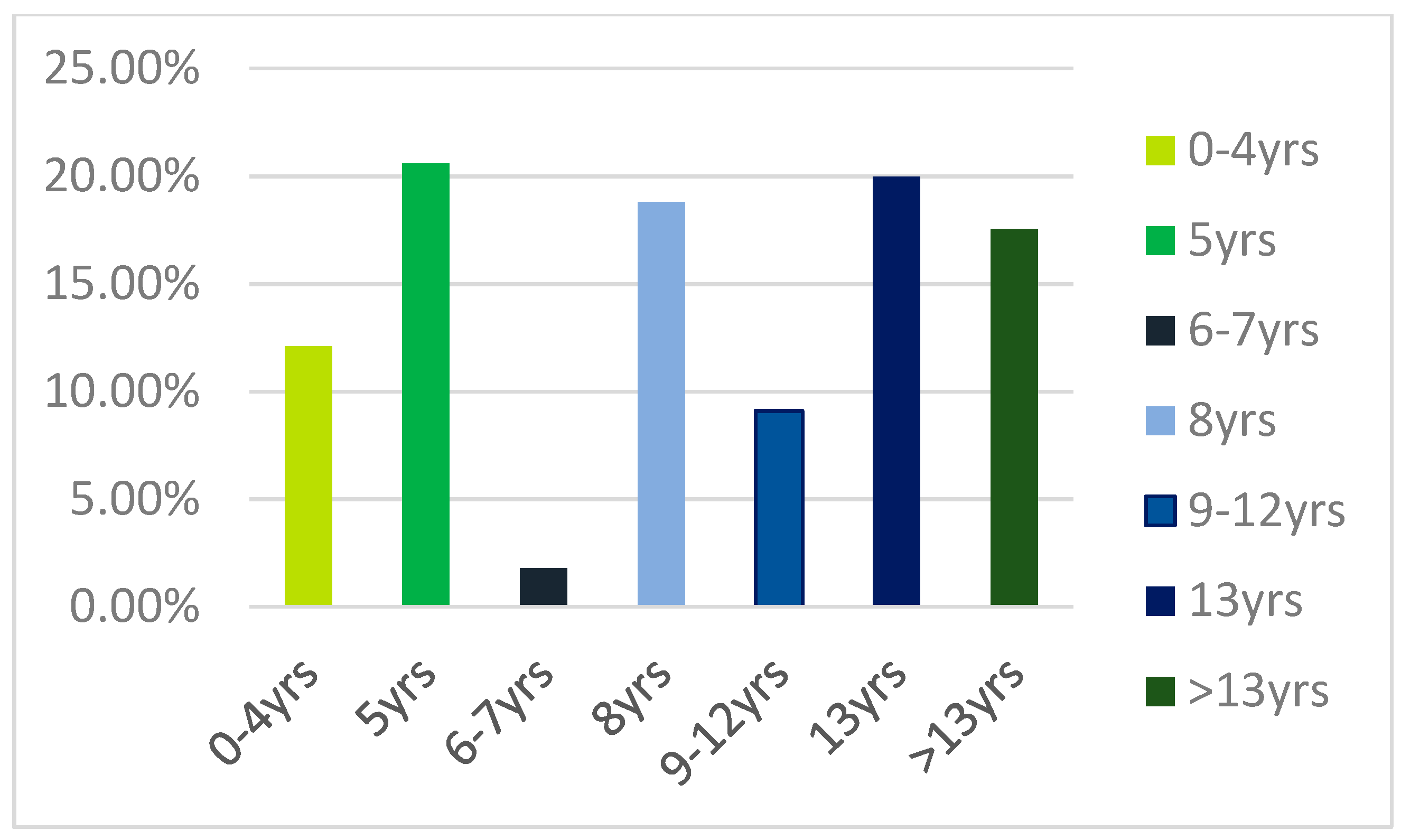
| General Characteristics of the Population | Values |
| Age (mean and standard deviation) | 72 ± 6.77 |
| Schooling (mean and standard deviation) | 9.45 ± 4.85 |
| Body Mass Index (mean and standard deviation) | 27.7 ± 4.22 |
| Weight loss in the last 6 months (percentage) | 36.4% |
| Subjective cognitive deficit (percentage) | 10.7% |
| Presence of comorbidities (percentage) | 83% |
| Types of Comorbidities | Frequency |
| Cardiovascular (percentage) | 60.6% |
| Respiratory (percentage) | 1.8% |
| Endocrine-metabolic (percentage) | 47.3% |
| Gastrointestinal and hepatic (percentage) | 4.2% |
| Musculoskeletal (percentage) | 3.6% |
| Oncological (percentage) | 4.8% |
| Genito-urinary (percentage) | 9.1% |
| Psychiatric and nervous central system (percentage) | 17.6% |
| Tests | Average of Scores |
| MoCA correct for age and education (mean value and standard deviation) | 21.7±3.57 |
| CRI-q (mean value and standard deviation) | 93.9±18.8 |
| CRI-school* (mean value and standard deviation) | 101±14.5 |
| CRI-work* (mean value and standard deviation) | 100± 24 |
| CRI-leisure* (mean value and standard deviation) | 83.5±14.1 |
| Factors | p-Value |
| Sex | 0.142 |
| Weight loss | 0.048 |
| Subjective cognitive decline | 0.029 |
| Presence of comorbidities | 0.371 |
| Types of Comorbidities | p-Value |
| Cardiovascular | 0.192 |
| Respiratory | 0.504 |
| Endocrine-metabolic | 0.664 |
| Gastrointestinal and hepatic | 0.899 |
| Musculoskeletal | 0.341 |
| Oncological | 0.268 |
| Genito-urinary | 0.460 |
| Psychiatric and nervous central system | 0.850 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




