Submitted:
13 July 2025
Posted:
14 July 2025
You are already at the latest version
Abstract
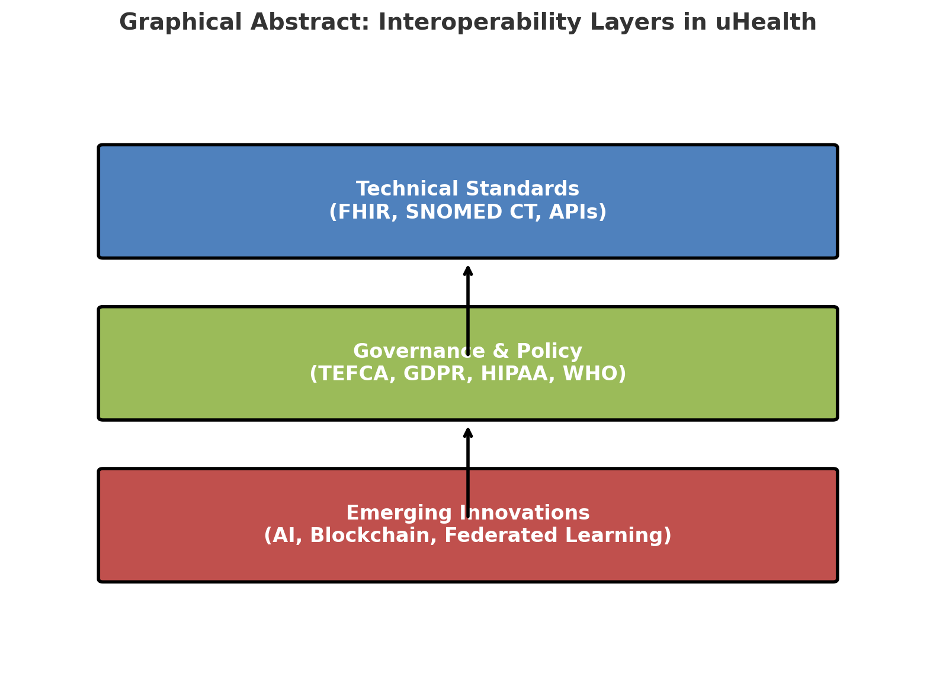
Keywords:
1. Introduction
2. Materials and Methods
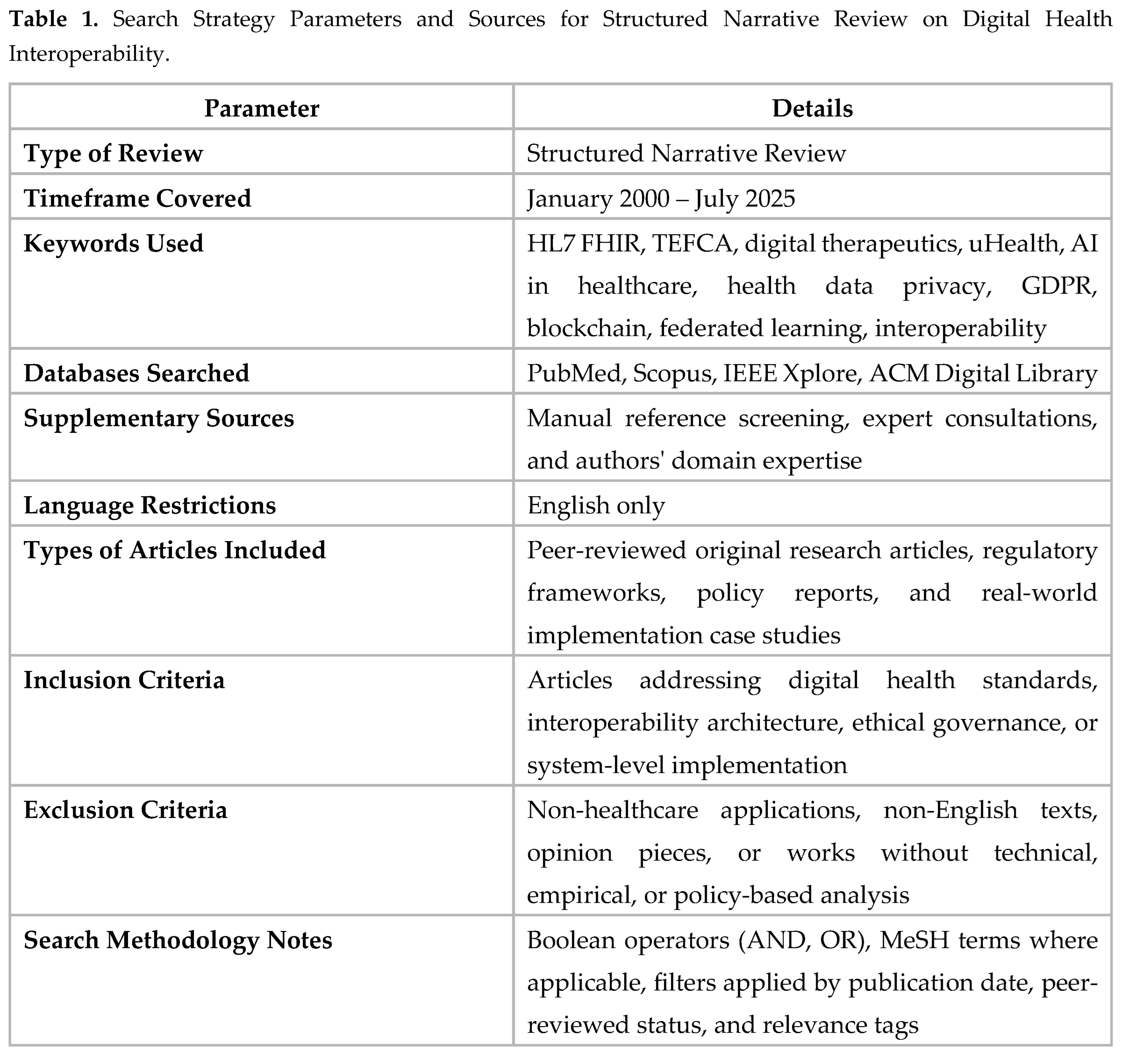
2.1. Search Strategy and Scope
- HL7 FHIR, TEFCA, digital therapeutics, uHealth, artificial intelligence in healthcare, health data privacy, GDPR, blockchain, federated learning, interoperability.
2.2. Eligibility Criteria
- Peer-reviewed publications, policy documents, or implementation frameworks,
- Published between January 2000 and July 2025,
- Written in English,
-
Addressed at least one of the following themes:
- ○
- Interoperability standards (e.g., HL7 FHIR, SMART on FHIR, and SNOMED CT)
- ○
- Evaluation of digital therapeutics, AI-powered systems, or mHealth platforms,
- ○
- Governance and privacy regulations (e.g., HIPAA, GDPR, TEFCA),
- ○
- Ethical, legal, or infrastructural dimensions of scalable digital health.
- Non-healthcare or commercial technology studies,
- Publications not in English,
- Opinion pieces or commentaries lacking technical or policy analysis.
2.3. Thematic Organization and Analysis
- Technical Standards and APIs,
- Data Governance and Legal Frameworks,
- Real-World Implementation and Use Cases.
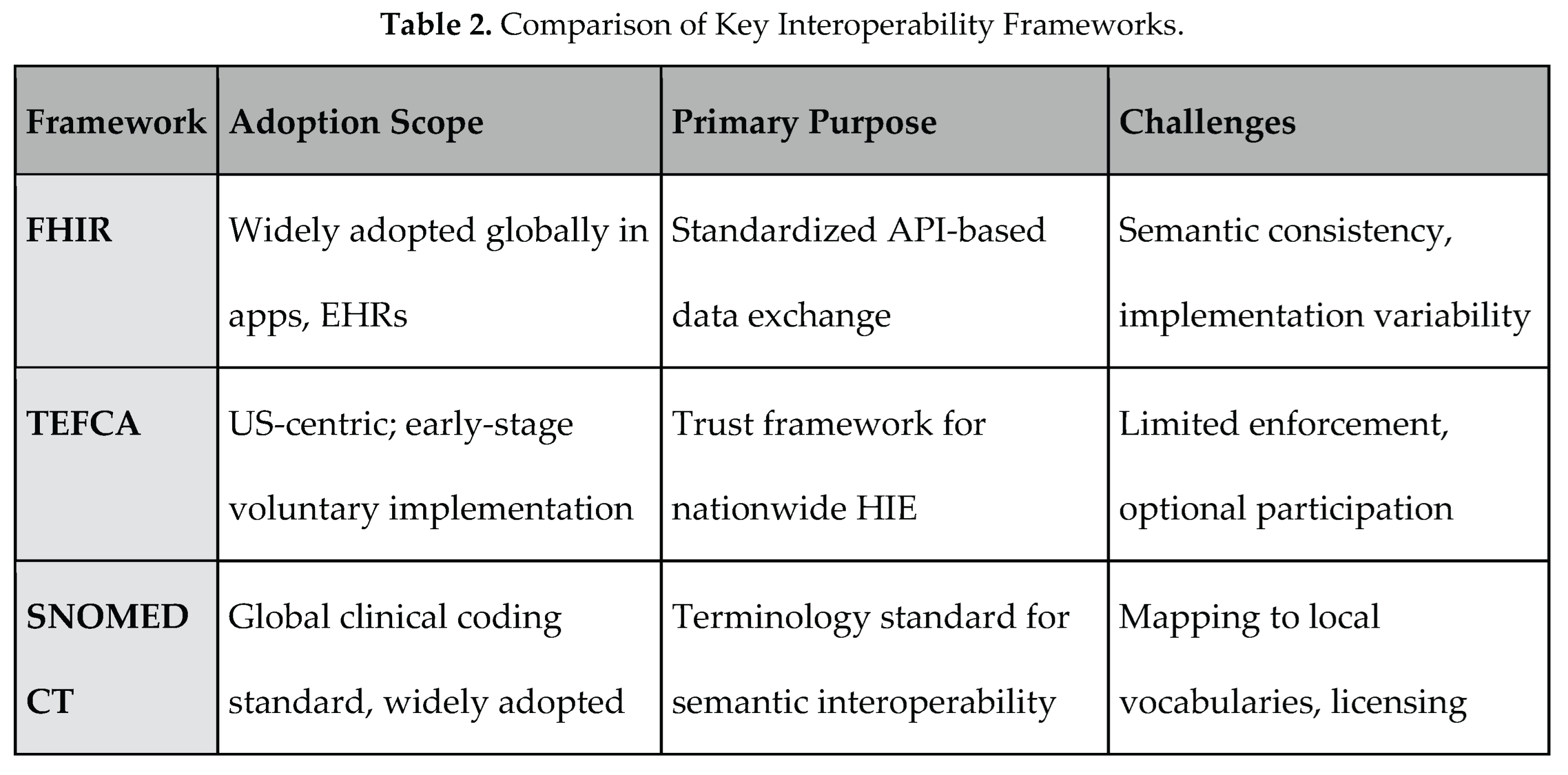
3. Technical Interoperability Frameworks
3.1. Interoperability as a Foundational Pillar
3.2. HL7 FHIR and SMART on FHIR
3.3. Syntactic vs. Semantic Interoperability
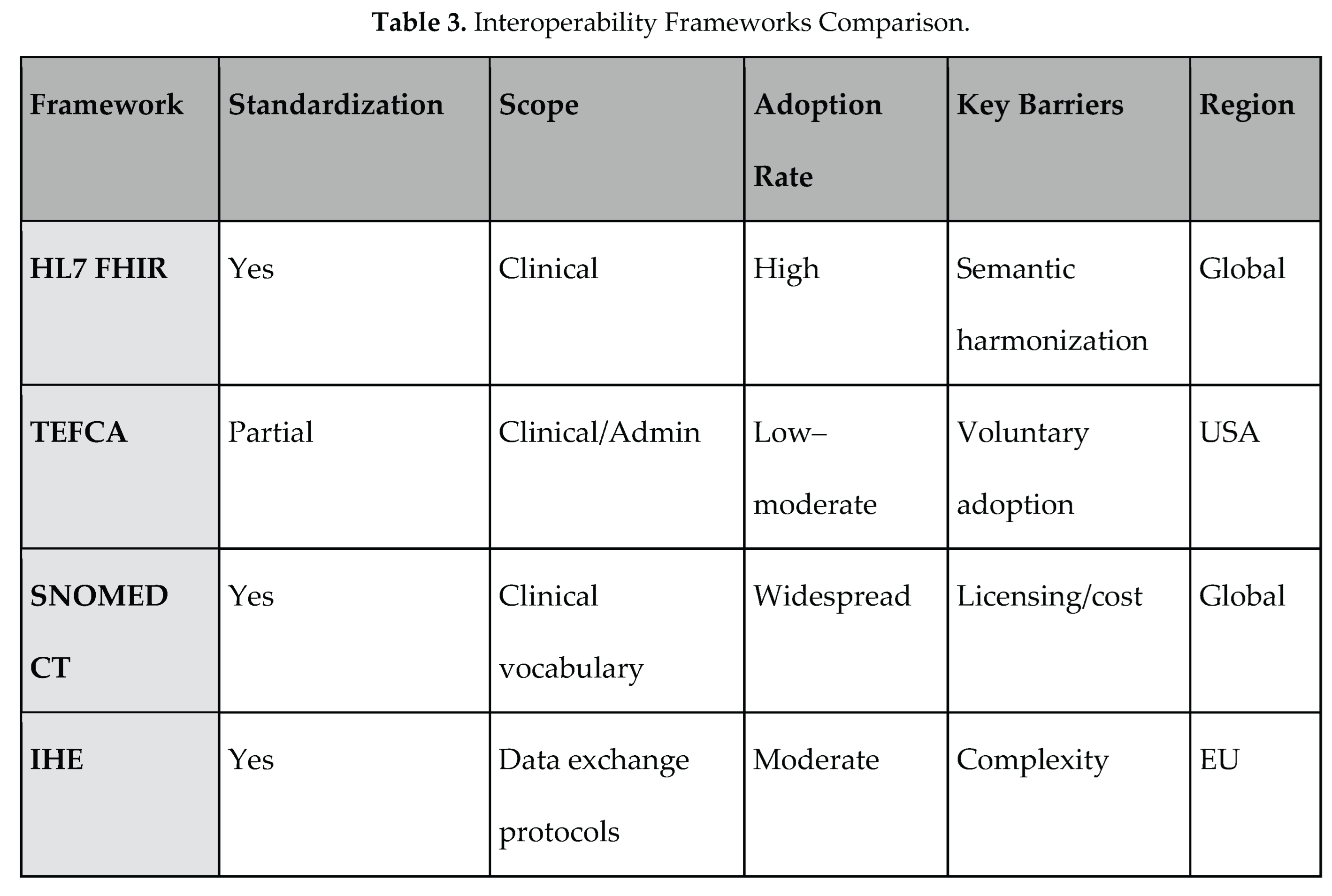
4. Governance and Policy Models
4.1. TEFCA (U.S. Trust Framework)
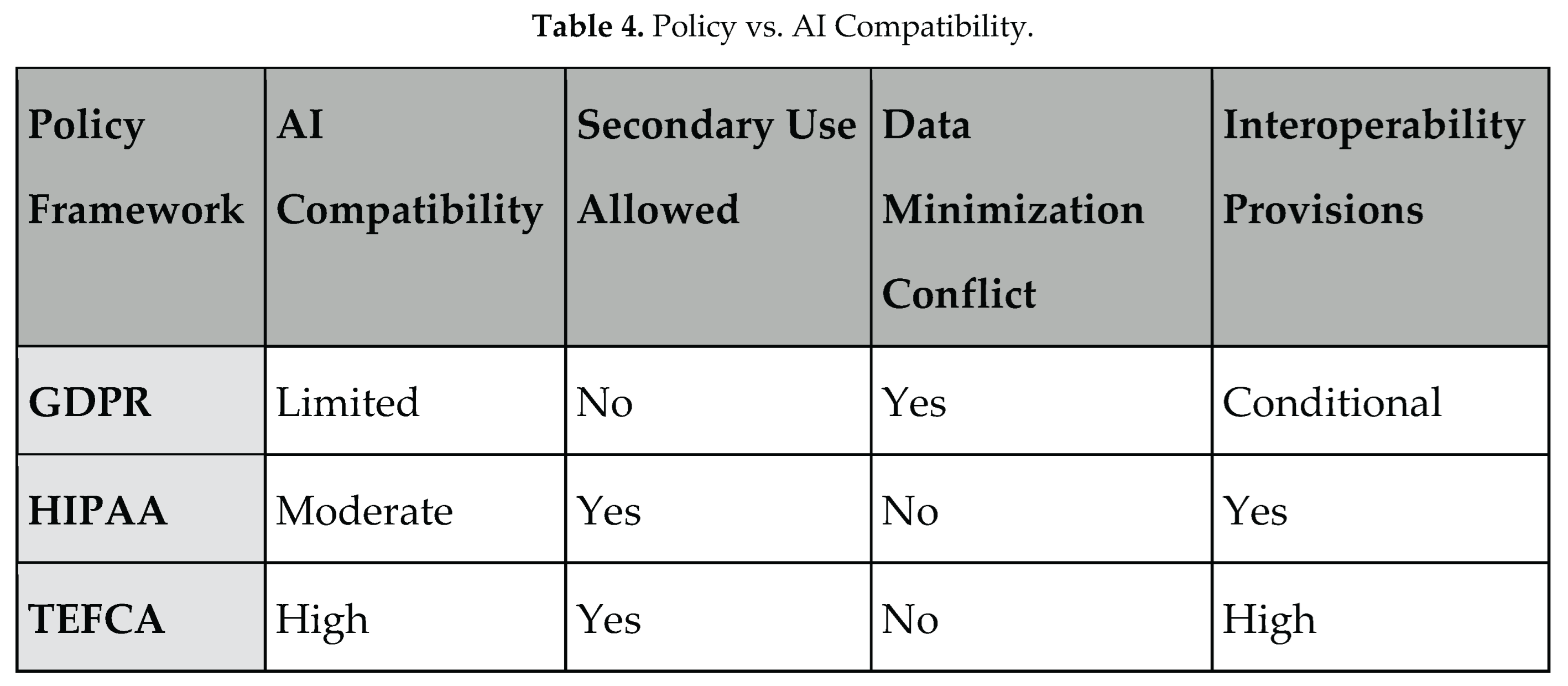
4.2. HIPAA, GDPR, and International Contrasts
4.3. WHO Global Strategy on Digital Health
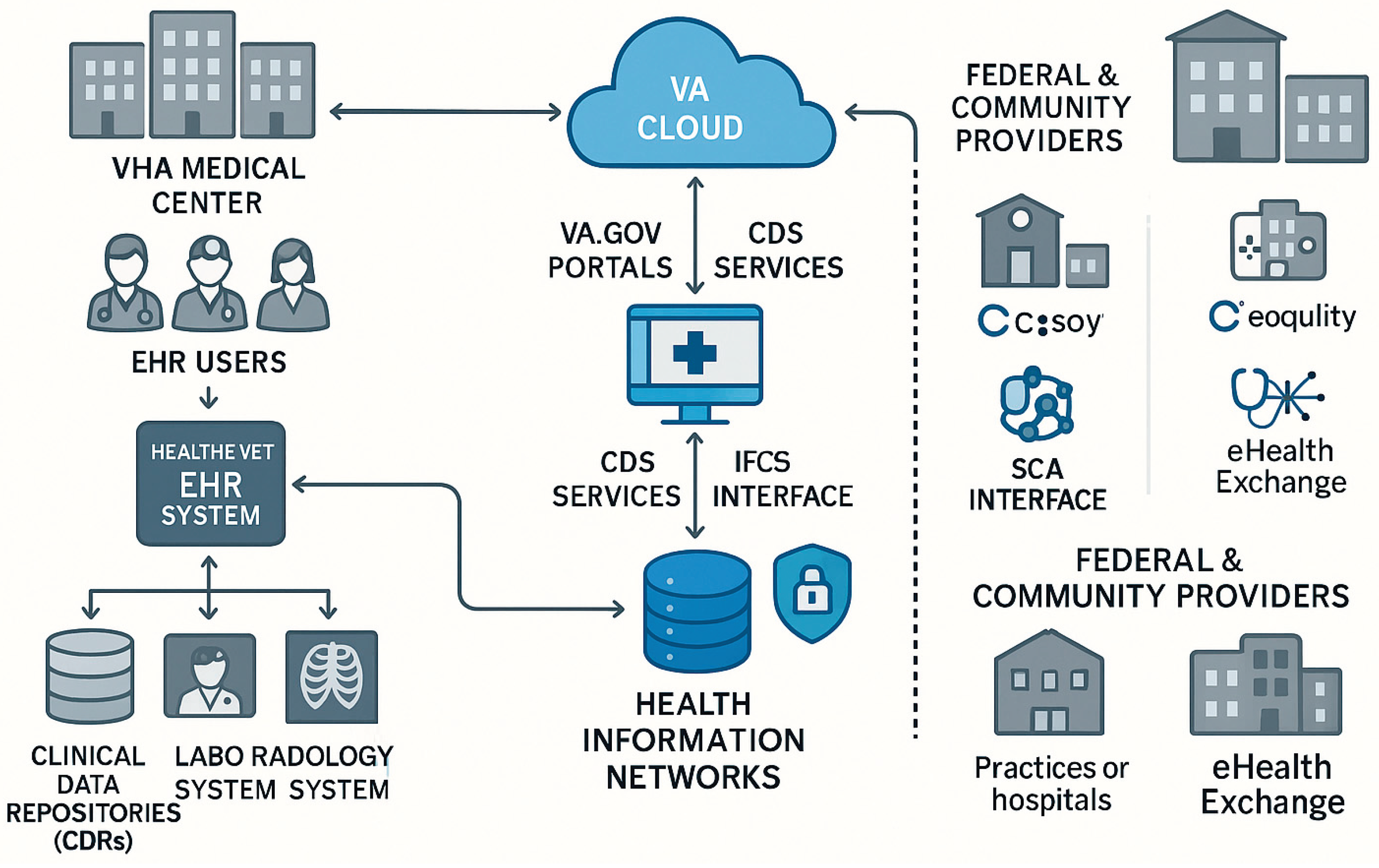
5. Case Study: Veterans Health Administration (VHA)
5.1. Goals and Results of Interoperability
5.2. Implementation Failures and Limitations
6. Emerging Technologies for Interoperability
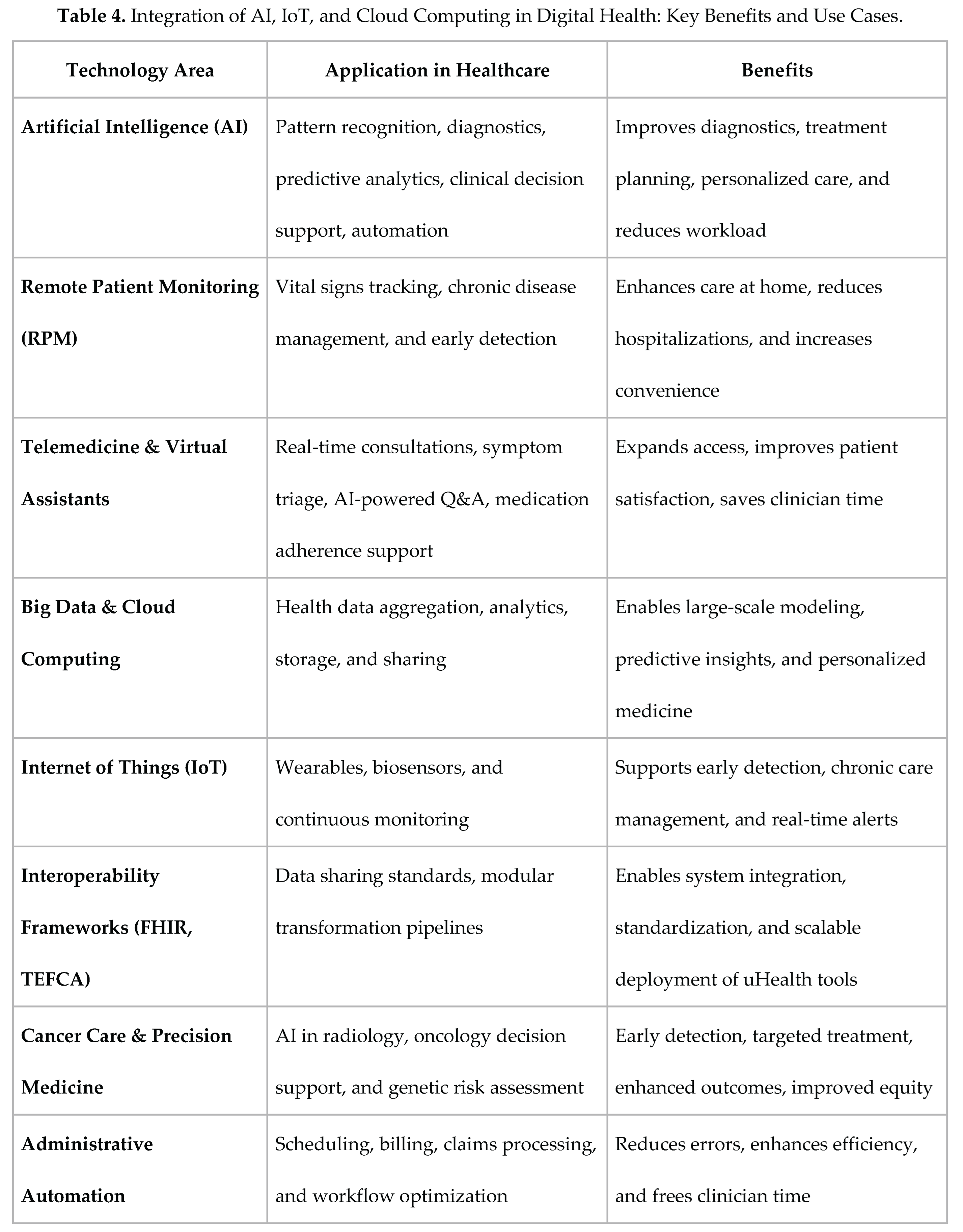
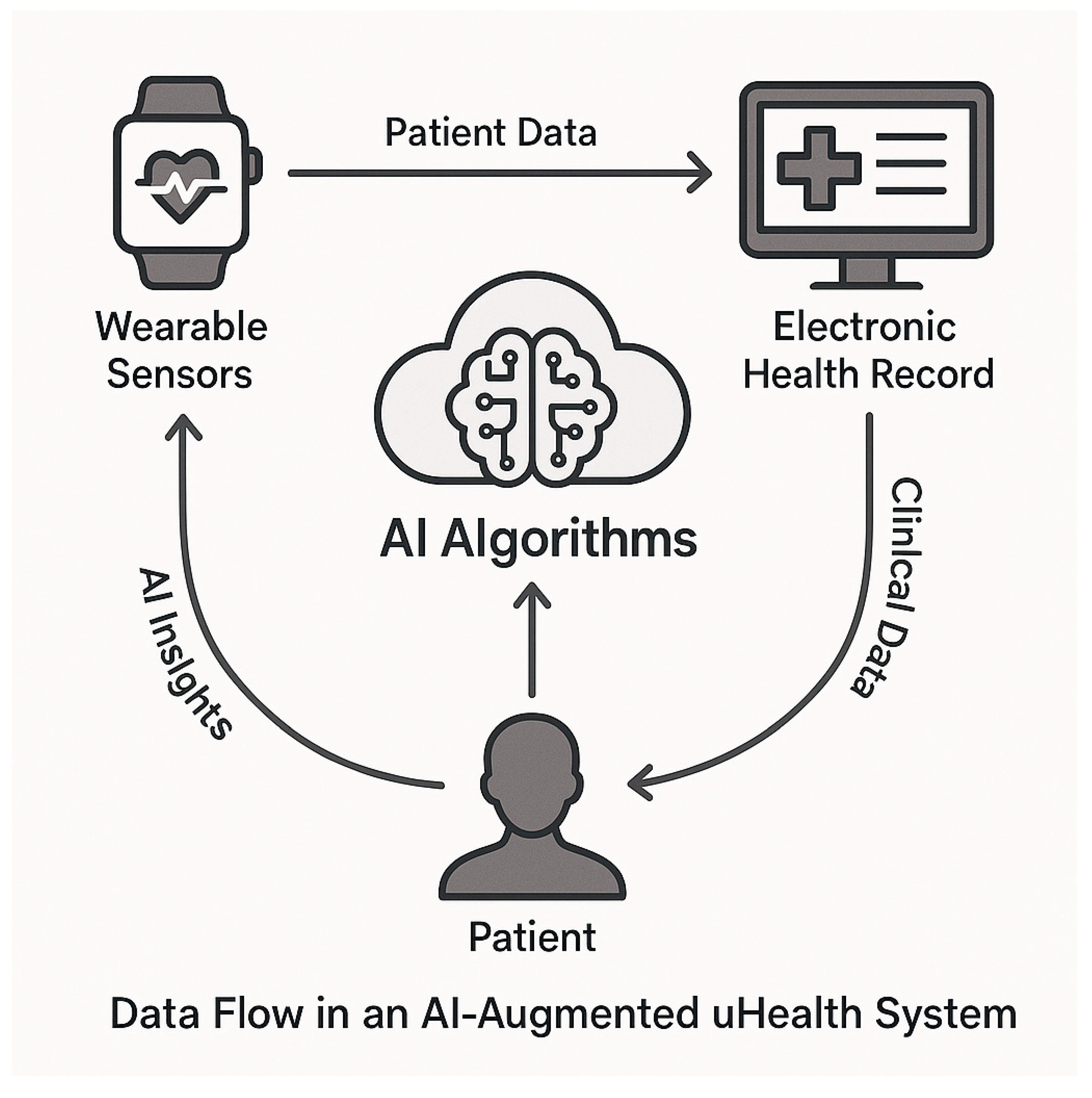
6.1. AI/ML and NLP for Data Harmonization

6.2. Blockchain and Distributed Ledgers
Blockchain
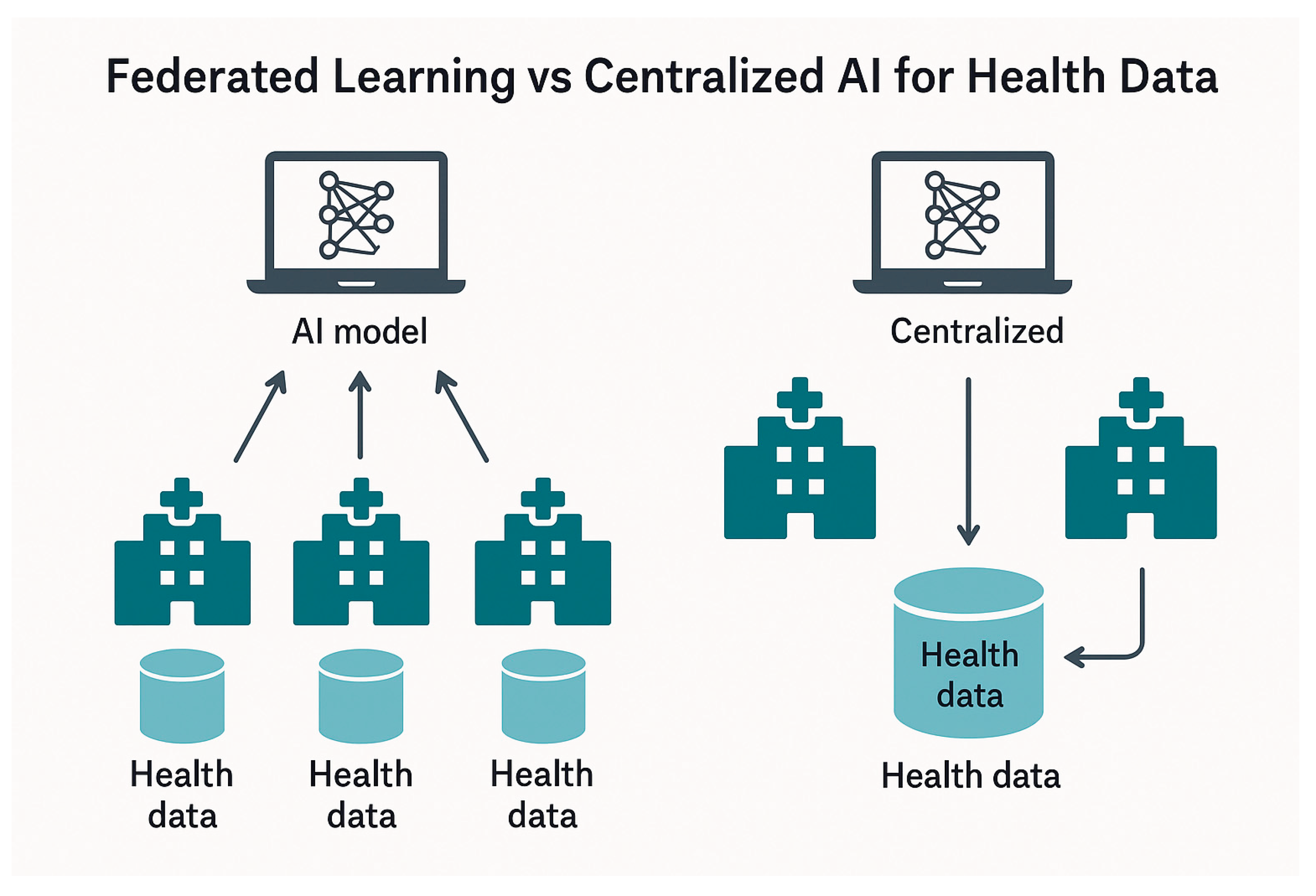
6.3. Federated Learning and Zero Trust Architectures
7. Implementation Challenges
7.1. Technical Barriers
7.2. Policy and Regulatory Gaps
7.3. Constraints on Equity and Access
7.4. Ethical Governance and Global Equity
7.5. Stakeholder Adoption Barriers
8. Policy Evaluation and Recommendations
8.1. TEFCA: Aspirations vs. Adoption
8.2. GDPR: Innovation vs Data Minimization
8.3. WHO Digital Health Strategy
8.4. Actionable Governance Models
9. Conclusion and Future Directions
- Module-based, right-aware architectures that flexibly adjust to diverse requirements within the health system and protect the rights of individuals.
- Rigorous clinical validation of AI-directed interventions to ensure generalizability to diverse demographic and institutional settings.
- Mass investment by LMICs, particularly in rural or underserved regions, where interoperability does not work today.
- Federated and zero-trust analytics architectures enable decentralized learning without loss of data sovereignty or security.
10. Limitations and Future Research
- Conduct comparative evaluations of interoperability implementations across diverse health systems, particularly in LMICs;
- Explore modular, low-resource architectures for HL7 FHIR adoption that are culturally and contextually appropriate
- The scalability and moral appropriateness of AI software on federated and zero-trust architectures are experimentally validated.
- Examine clinician adoption and usability patterns within system changes using mixed-method designs
- Develop sound assessment frameworks that account for the real-world impact on health equity and result from interoperability reforms.
Author Contributions
Funding
Ethical Statement
Ethical Compliance
Informed Consent Statement
Ethical Statements
Data Availability Statement
Conflict of Interest
References
- Gazzarata, R.; Almeida, J.; Lindsköld, L.; Cangioli, G. HL7 Fast Healthcare Interoperability Resources (HL7 FHIR) in Digital Healthcare Ecosystems for Chronic Disease Management: Scoping Review. Int. J. Med. Inform. 2024, 185, 105507. [CrossRef]
- Abernethy, A.P.; Adams, L.E.; Barrett, M.; Bechtel, C.; Brennan, P.; Butte, A.J.; et al. The Promise of Digital Health: Then, Now, and the Future. NAM Perspect. 2022, 6(22). [CrossRef]
- Sharma, A.; Harrington, R.A.; McClellan, M.; Turakhia, M.P.; Eapen, Z.J.; Steinhubl, S.R.; et al. Using Digital Health Technology to Better Generate Evidence and Deliver Evidence-Based Care. J. Am. Coll. Cardiol. 2018, 71(23), 2680. [CrossRef]
- Alawiye, T.R. The Impact of Digital Technology on Healthcare Delivery and Patient Outcomes. E-Health Telecommun. Syst. Netw. 2024, 13(2), 13. [CrossRef]
- Sinha, R.K. The Role and Impact of New Technologies on Healthcare Systems. Discov. Health Syst. 2024, 3(1). [CrossRef]
- Elysee, G.; Herrin, J.; Horwitz, L.I. An Observational Study of the Relationship between Meaningful Use-Based Electronic Health Information Exchange, Interoperability, and Medication Reconciliation Capabilities. Medicine (Baltimore) 2017, 96(41), e8274. [CrossRef]
- Armoundas, A.A.; Ahmad, F.S.; Bennett, D.A. Data Interoperability for Ambulatory Monitoring of Cardiovascular Disease: A Scientific Statement from the American Heart Association. Circ. Genom. Precis. Med. 2024. [CrossRef]
- Salunkhe, V. Transforming Healthcare Research with Interoperability: The Role of FHIR and SMART on FHIR. In Handbook of Research on Healthcare Administration and Management; IGI Global: Hershey, PA, USA, 2024. [CrossRef]
- Barker, W.; Chang, W.; Everson, J.; Gabriel, M. The Evolution of Health Information Technology for Enhanced Patient-Centric Care in the United States: Data-Driven Descriptive Study. J. Med. Internet Res. 2024. [CrossRef]
- Abbasi, A.B.; Layden, J.; Gordon, W.; Gregurick, S. A Unified Approach to Health Data Exchange: A Report from the US DHHS. JAMA 2025. [CrossRef]
- Zhang, X.; Saltman, R. Impact of Electronic Health Record Interoperability on Telehealth Service Outcomes. JMIR Med. Inform. 2022, 10(1), e31837. https://medinform.jmir.org/2022/1/e31837/.
- Nyangena, J.; Rajgopal, R.; Ombech, E.; Oloo, E.; Luchetu, H.; Wambugu, S.; et al. Maturity Assessment of Kenya's Health Information System Interoperability Readiness. BMJ Health Care Inform. 2021, 28(1). [CrossRef]
- Aziz, S.U.A.; Askari, M.; Shah, S.N. Standards for Digital Health. In Handbook of eHealth Standards; Elsevier BV, 2020; p. 231. [CrossRef]
- Torab-Miandoab, A.; Samad-Soltani, T.; Jodati, A.; Rezaei-Hachesu, P. Interoperability of Heterogeneous Health Information Systems: A Systematic Literature Review. BMC Med. Inform. Decis. Mak. 2023, 23, 15. [CrossRef]
- Enticott, J.; Johnson, A.; Teede, H. Learning Health Systems Using Data to Drive Healthcare Improvement and Impact: A Systematic Review. BMC Health Serv. Res. 2021, 21(1), 200. [CrossRef]
- McMurry, A.J.; Gottlieb, D.I.; Miller, T.A.; Jones, J.R.; Atreja, A.; Crago, J.; et al. Cumulus: A Federated Electronic Health Record-Based Learning System Powered by Fast Healthcare Interoperability Resources and Artificial Intelligence. J. Am. Med. Inform. Assoc. 2024, 31(8), 1638–1647. [CrossRef]
- Szarfman, A.; Levine, J.G.; Tonning, J.M.; Weichold, F.; Bloom, J.C.; Soreth, J.M.; et al. Recommendations for Achieving Interoperable and Shareable Medical Data in the USA. Commun. Med. 2022, 2(1). [CrossRef]
- Mandel, J.C.; Kreda, D.A.; Mandl, K.D.; Kohane, I.S.; Ramoni, R.B. SMART on FHIR: A Standards-Based, Interoperable Apps Platform for Electronic Health Records. J. Am. Med. Inform. Assoc. 2016, 23(5), 899–908. [CrossRef]
- Apple Inc. Using HealthKit to Access Clinical Records with FHIR. Developer Documentation 2023. https://developer.apple.com/documentation/healthkit.
- Tabari, P.; Costagliola, G.; De Rosa, M. State-of-the-Art Fast Healthcare Interoperability Resources (FHIR)-Based Data Model and Structure Implementations: Systematic Scoping Review. JMIR Med. Inform. 2024, 12(1), e58445. [CrossRef]
- D’Amore, J.D.; Sittig, D.F.; Ness, R.B.; et al. App-Enabled EHRs: Benefits and Challenges of SMART on FHIR Apps. J. Med. Syst. 2018, 42(9), 165. [CrossRef]
- Bodenreider, O. The Unified Medical Language System (UMLS): Integrating Biomedical Terminology. Nucleic Acids Res. 2004, 32(Database issue), D267–D270. [CrossRef]
- Schadow, G.; Mead, C.N.; McDonald, C.J. The HL7 Reference Information Model Under Scrutiny. Stud. Health Technol. Inform. 2001, 84(Pt 1), 133–137. https://pubmed.ncbi.nlm.nih.gov/17108519/.
- Giannangelo, K.; Millar, J. Mapping SNOMED CT to ICD-10. Stud. Health Technol. Inform. 2012, 180, 83–87. https://pubmed.ncbi.nlm.nih.gov/22874157/.
- Fung, K.W.; Xu, J.; Bodenreider, O. The New International Classification of Diseases 11th Edition: A Comparative Review with ICD-10 and ICD-10-CM. J. Am. Med. Inform. Assoc. 2020, 27(5), 738–746. [CrossRef]
- Martínez-Costa, C.; Menárguez-Tortosa, M.; Fernández-Breis, J.T. An Ontology-Based Approach for Representing Clinical Information in SNOMED CT and FHIR. J. Biomed. Semant. 2015, 6, 35. [CrossRef]
- U.S. Office of the National Coordinator for Health IT (ONC). Trusted Exchange Framework and Common Agreement (TEFCA) Overview. Available online: https://www.healthit.gov/tefca (accessed on 11 July 2025).
- Wager, K.A.; Lee, F.W.; Glaser, J.P. Health Care Information Systems: A Practical Approach for Health Care Management, 5th ed.; Jossey-Bass: Hoboken, NJ, USA, 2022; p. 83; ISBN 9781119853879.
- Holmgren, A.J.; Adler-Milstein, J.; Apathy, N.C. Electronic Health Record Documentation Burden Crowds Out Health Information Exchange Use by Primary Care Physicians. Health Aff. (Millwood) 2024, 43(11). [CrossRef]
- Cohen, I.G.; Mello, M.M. HIPAA and Protecting Health Information in the 21st Century. JAMA 2018, 320(3), 231–232. [CrossRef]
- Szarfman, A.; Levine, J.G.; Tonning, J.M.; et al. Recommendations for Achieving Interoperable and Shareable Medical Data in the USA. Commun. Med. 2022, 2(1). [CrossRef]
- Rigas, E.S.; Lagakis, P.; Karadimas, M.; Logaras, E. Semantic Interoperability for an AI-Based Applications Platform for Smart Hospitals Using HL7 FHIR. Comput. Methods Programs Biomed. 2024, 240, 107138. https://www.sciencedirect.com/science/article/pii/S0164121224001389.
- Marfoglia, A.; Nardini, F.; Arcobelli, V.A.; Moscato, S. Towards Real-World Clinical Data Standardization: A Modular FHIR-Driven Transformation Pipeline to Enhance Semantic Interoperability in Healthcare. Comput. Methods Programs Biomed. 2025, 238, 107095. https://www.sciencedirect.com/science/article/pii/S0010482525000952.
- Zhang, X. Healthcare Regulation and Governance: Big Data Analytics and Healthcare Data Protection; Jefferson Digital Commons, 2020. Available online: https://jdc.jefferson.edu/cgi/viewcontent.cgi?article=1003&context=jscpssp (accessed on 11 July 2025).
- Konnoth, C. AI and Data Protection Law in Health. In Research Handbook on Health, AI and the Law; Solaiman, B., Cohen, I.G., Eds.; Edward Elgar: Cheltenham, UK, 2024; pp. 111–129.
- Gilbert, S.; Mathias, R.; Schönfelder, A.; Wekenborg, M.; Steinigen-Fuchs, J.; Dillenseger, A.; et al. A Roadmap for Safe, Regulation-Compliant Living Labs for AI and Digital Health Development. Sci. Adv. 2025, 11(20). [CrossRef]
- Amar, F.; April, A.; Abran, A. Electronic Health Record and Semantic Issues Using Fast Healthcare Interoperability Resources: Systematic Mapping Review. J. Med. Internet Res. 2024, 26(1), e45209. https://www.jmir.org/2024/1/e45209/.
- World Health Organization. Global Strategy on Digital Health 2020–2025; WHO: Geneva, Switzerland, 2021. Available online: https://www.who.int/publications/i/item/9789240020924 (accessed on 11 July 2025).
- Ricciardi Celsi, L.; Zomaya, A.Y. Perspectives on Managing AI Ethics in the Digital Age. Information 2025, 16(4), 318. [CrossRef]
- Dhinakaran, D.; Edwin Raja, S.; Ramathilagam, A.; Vennila, G.; Alagulakshmi, A. Ethical and Legal Challenges with IoT in Home Digital Twins. MethodsX 2025, 14, 103409. [CrossRef]
- Watson, A.; Collins, L.A.; Danan, R.; Walsh, E.; Sarkhel, K.K. Use of EHR to Support Pilot Aeromedical Certification. U.S. Dept. of Transportation [Internet] 2024 [cited 2025 Jul]. Available online: . [CrossRef]
- Topol, E.J. High-Performance Medicine: The Convergence of Human and Artificial Intelligence. Nat. Med. 2019, 25(1), 44–56. [CrossRef]
- Gilbert, S.; Mathias, R.; Schönfelder, A.; Wekenborg, M.; Steinigen-Fuchs, J.; Dillenseger, A.; et al. A Roadmap for Safe, Regulation-Compliant Living Labs for AI and Digital Health Development. Sci. Adv. 2025, 11(20). [CrossRef]
- Braunstein, M.L. Health Informatics on FHIR: How HL7's API is Transforming Healthcare; Springer: Cham, Switzerland, 2022. Available online: https://onesearch.nihlibrary.ors.nih.gov/permalink/01NIH_INST/15et3fj/alma991001345887304686 (accessed on 11 July 2025).
- Snyder, M.E.; Nguyen, K.A.; Patel, H.; Sanchez, S.L. Clinicians’ Use of Health Information Exchange Technologies for Medication Reconciliation in the U.S. Department of Veterans Affairs: A Qualitative Analysis. BMC Health Serv. Res. 2024, 24(1), 1–10. [CrossRef]
- Denney, K.B. Assessing Clinical Software User Needs for Improved Clinical Decision Support Tools [Internet]; Walden Dissertations and Doctoral Studies, 2015 [cited 2025 Jul]. Available online: https://scholarworks.waldenu.edu/dissertations/2562.
- Sarkar, I.N. Transforming Health Data to Actionable Information: Recent Progress and Future Opportunities in Health Information Exchange. Yearb. Med. Inform. 2022, 31(1), 203–214. [CrossRef]
- Laster, R.J. Improving the Department of Veterans Affairs Medical Centers Electronic Health Record Implementation [Internet]; Walden Dissertations and Doctoral Studies, 2024 [cited 2025 Jul]. Available online: https://scholarworks.waldenu.edu/dissertations/12228.
- Holmgren, A.J.; Esdar, M.; Hüsers, J.; Coutinho-Almeida, J. Health Information Exchange: Understanding the Policy Landscape and Future of Data Interoperability. Yearb. Med. Inform. 2023, 32(1), 184–194. [CrossRef]
- Wu, S.; Roberts, K.; Datta, S.; et al. Deep Learning in Clinical Natural Language Processing: A Methodical Review. J. Am. Med. Inform. Assoc. 2020, 27(3), 457–470. [CrossRef]
- Singhal, K.; Azizi, S.; Tu, T.; et al. Large Language Models Encode Clinical Knowledge. Nature 2023, 620(7974), 172–180. [CrossRef]
- Roberts, M.; Driggs, D.; Thorpe, M.; et al. Common Pitfalls and Recommendations for Using Machine Learning to Detect and Prognosticate for COVID-19 Using Chest Radiographs and CT Scans. Nat. Mach. Intell. 2021, 3(3), 199–217. [CrossRef]
- Goel, I.; Bhaskar, Y.; Kumar, N.; et al. Role of AI in Empowering and Redefining the Oncology Care Landscape: Perspective from a Developing Nation. Front. Digit. Health 2025, 7, 1550407. [CrossRef]
- Varnosfaderani, S.M.; Forouzanfar, M. The Role of AI in Hospitals and Clinics: Transforming Healthcare in the 21st Century. Bioengineering 2024, 11(4), 337. [CrossRef]
- Pathak, Y.; Greenleaf, W.; Metman, L.V.; et al. Digital Health Integration with Neuromodulation Therapies: The Future of Patient-Centric Innovation in Neuromodulation. Front. Digit. Health 2021, 3, 618959. [CrossRef]
- Hryciw, B.N.; Fortin, Z.; Ghossein, J.; Kyeremanteng, K. Doctor-Patient Interactions in the Age of AI: Navigating Innovation and Expertise. Front. Med. 2023, 10, 1241508. [CrossRef]
- Sheller, M.J.; Reina, G.A.; Edwards, B.; et al. Federated Learning in Medicine: Facilitating Multi-Institutional Collaborations without Sharing Patient Data. Sci. Rep. 2020, 10, 12598. [CrossRef]
- Gupta, A.; Dogar, M.E.; Zhai, E.S.; et al. Innovative Telemedicine Approaches in Different Countries: Opportunity for Adoption, Leveraging, and Scaling-Up. Telemed. Med. Today 2019, 5. [CrossRef]
- Linn, L.A.; Koo, M.B. Blockchain for Health Data and Its Potential Use in Health IT and Health Care-Related Research. ONC White Paper [Internet] 2016 [cited 2025 Jul]. Available online: https://www.healthit.gov/sites/default/files/11-74-ablockchainforhealthcare.pdf.
- Vazirani, A.A.; O’Donoghue, O.; Brindley, D.; Meinert, E. Blockchain Vehicles for Efficient Medical Record Management. Blockchain Healthc. Today 2019, 2(1). [CrossRef]
- Williams, E.; Kienast, M.; Medawar, E.; Reinelt, J.; Merola, A.; Klopfenstein, S.; et al. A Standardized Clinical Data Harmonization Pipeline for Scalable AI Application Deployment (FHIR-DHP): Validation and Usability Study. JMIR Med. Inform. 2023, 11, e43847. https://medinform.jmir.org/2023/1/e43847.
- Vukotich, G. Healthcare and Cybersecurity: Taking a Zero Trust Approach. Health Serv. Insights 2023, 16, 11786329231187826. [CrossRef]
- Ndlovu, K.; Scott, R.E.; Mars, M. Interoperability Opportunities and Challenges in Linking mHealth Applications and eRecord Systems: Botswana as an Exemplar. BMC Med. Inform. Decis. Mak. 2021, 21, 1–9. [CrossRef]
- Mulukuntla, S. Interoperability in Electronic Medical Records: Challenges and Solutions for Seamless Healthcare Delivery. EIJMHS 2015, 1(1), 12–20. https://eijmhs.com/index.php/mhs/article/view/214.
- Ciecierski-Holmes, T.; Kahn, T.; Sharma, R.; Mejía, A.; Ravi, N. Artificial Intelligence in Low- and Middle-Income Countries: A Systematic Scoping Review. NPJ Digit. Med. 2022, 5, 104. https://www.nature.com/articles/s41746-022-00700-y.
- Kaushik, A.; Barcellona, C.; Mandyam, N.K.; Tan, S.Y. Challenges and Opportunities for Data Sharing Related to Artificial Intelligence Tools in Health Care in Low- and Middle-Income Countries: Systematic Review. J. Med. Internet Res. 2025, 27(1), e58338. https://www.jmir.org/2025/1/e58338/.
- World Health Organization. Assessing the Enabling Environment for Digital Health: A Guidance Tool for Countries with Limited Infrastructure; WHO: Geneva, Switzerland, 2023. Available online: https://cdn.who.int/media/docs/default-source/digital-health-documents/global-initiative-on-digital-health_executive-summary-31072023.pdf?sfvrsn=5282e32f_1 (accessed on 11 July 2025).
- Ahmed, S.; Bhattacharyya, S.; Jafri, A.; Essar, M.Y.; Beiersmann, C.; Mathur, A.; et al. Strengthening Primary Health Care through Digital Platforms: Closing the Universal Health Coverage Gap. Healthcare 2024, 13(9), 1060. https://www.mdpi.com/2227-9032/13/9/1060.
- World Health Organization. Ethics and Governance of Artificial Intelligence for Health: WHO Guidance; WHO: Geneva, Switzerland, 2021. Available online: https://iris.who.int/bitstream/handle/10665/341996/9789240029200-eng.pdf (accessed on 11 July 2025).
- Ho, C.W.L. Equitable Artificial Intelligence in Global Health: Benefit Sharing and Governance. Front. Public Health 2022, 10, 768977. https://www.frontiersin.org/articles/10.3389/fpubh.2022.768977/full.
- Aerts, A.; Bogdan-Martin, D. Leveraging Data and AI to Deliver on the Promise of Digital Health. Int. J. Med. Inform. 2021, 150, 104456. [CrossRef]
- Bernardi, L.; Ferrer, M.; Arias, J.; Castagna, D.; Ismailova, K. Human-Centered Design in Digital Health: Best Practices for Clinician Engagement in Digital Transformation. Digit. Health 2023, 9, 1–14. [CrossRef]
- Gomis-Pastor, M.; Berdún, J.; Borrás-Santos, A. Clinical Validation of Digital Healthcare Solutions: State of the Art, Challenges and Opportunities. Healthcare 2024, 12(11), 1057. https://www.mdpi.com/2227-9032/12/11/1057.
- Adler-Milstein, J.; Worzala, C.; Dixon, B.E. Future Directions for Health Information Exchange. In Advances in Health Informatics; Elsevier: Amsterdam, The Netherlands, 2023. [CrossRef]
- Hussein, R.; Griffin, A.C.; Pichon, A. A Guiding Framework for Creating a Comprehensive Strategy for mHealth Data Sharing, Privacy, and Governance in Low-and Middle-Income Countries (LMICs). J. Am. Med. Inform. Assoc. 2023, 30(4), 787–794. [CrossRef]
- Kaushik, A.; Barcellona, C.; Mandyam, N.K.; Tan, S.Y. Challenges and Opportunities for Data Sharing Related to Artificial Intelligence Tools in Health Care in Low-and Middle-Income Countries: Systematic Review. J. Med. Internet Res. 2025, 27(1), e58338. https://www.jmir.org/2025/1/e58338.
- Faridoon, A.; Kechadi, M.T. Healthcare Data Governance, Privacy, and Security—A Conceptual Framework. In AI for Smart Healthcare Systems; Springer: Cham, Switzerland, 2024. [CrossRef]
- Swathi, N.L.; Kavitha, S.; Karpakavalli, M. Healthcare Information Systems Management; IGI Global: Hershey, PA, USA, 2025. Available online: https://www.igi-global.com/viewtitle.aspx?titleid=357954 (accessed on 11 July 2025).
- Kim, H.; Kwon, I.H.; Chul, W. Future and Development Direction of Digital Healthcare. Healthc. Inform. Res. 2021, 27(2), 95. [CrossRef]
- Thacharodi, A.; Singh, P.; Meenatchi, R.; Ahmed, Z.; Kumar, R.R.S.; Neha, V.; et al. Revolutionizing Healthcare and Medicine: The Impact of Modern Technologies for a Healthier Future—A Comprehensive Review. Health Care Sci. 2024, 3(5), 329. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



