Submitted:
12 February 2025
Posted:
13 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Data Collection
2.3. Instrument
2.4. Data Analysis
3. Results
3.1. Descriptive Statistics
3.2. MANCOVA Results
| Effect | Value | F | Hypothesis df | Error df | Sig. | Partial Eta Squared | |
| Intercept | Pillai's Trace | 0.167 | 4.373 | 9 | 197 | 0.000 | 0.167 |
| Age | Pillai's Trace | 0.027 | 0.609 | 9 | 197 | 0.789 | 0.027 |
| TPSI | Pillai's Trace | 1.342 | 1.197 | 270 | 1845 | 0.022 | 0.149 |
| Severity | Pillai's Trace | 0.042 | 0.962 | 9 | 197 | 0.472 | 0.042 |
| Sex | Pillai's Trace | 0.100 | 2.442 | 9 | 197 | 0.012 | 0.100 |
| TPSI * Severity | Pillai's Trace | 1.036 | 1.026 | 234 | 1845 | 0.386 | 0.115 |
| TPSI * Sex | Pillai's Trace | 0.951 | 0.969 | 225 | 1845 | 0.614 | 0.106 |
| Severity * Sex | Pillai's Trace | 0.077 | 1.822 | 9 | 197 | 0.066 | 0.077 |
| TPSI * Severity * Sex | Pillai's Trace | 0.475 | 0.816 | 126 | 1845 | 0.931 | 0.053 |
3.3. ANCOVA Results
3.4. Partial Kendall Tau Results
3.4.1. All Participants
3.4.2. Men
3.4.3. Women
4. Discussion
4.1. Sex
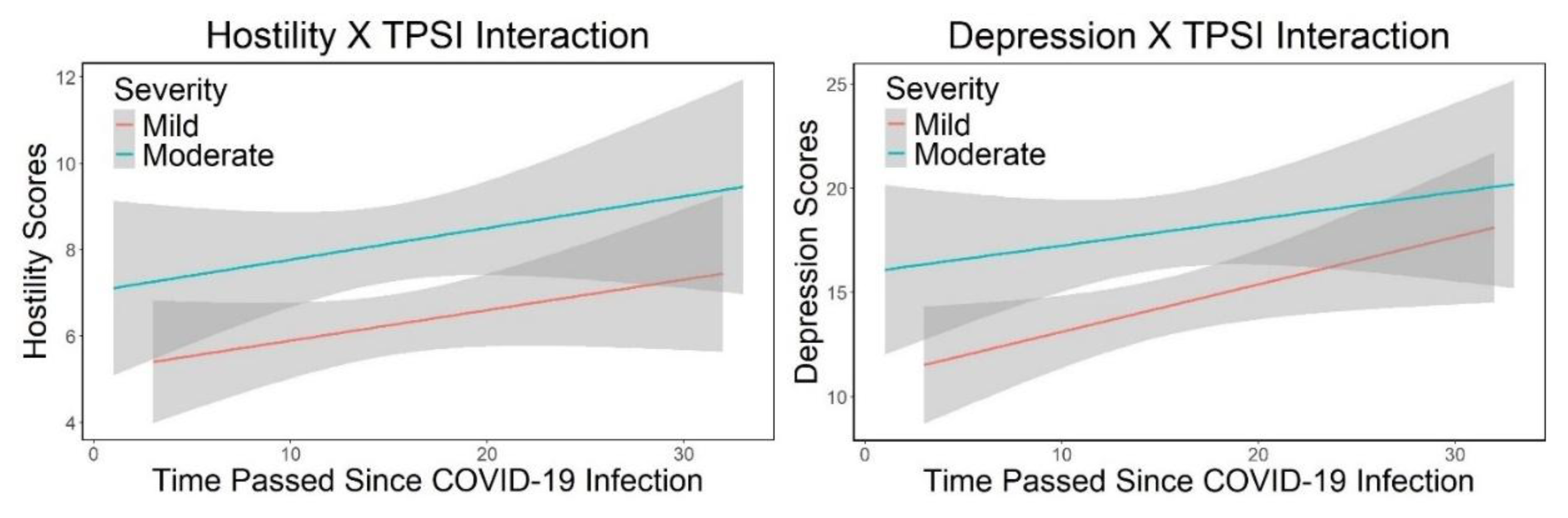
4.2. Time Passed Since COVID-19 Infection (TPSI)
4.3. Severity of COVID-19 Infection
4.4. Strengths
4.5. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| TPSI | Time passed since COVID-19 Infection |
| O-C | Obsessive-Compulsive |
References
- C. Huang et al., “Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China,” The Lancet, vol. 395, no. 10223, pp. 497–506, Feb. 2020, doi: 10.1016/S0140-6736(20)30183-5. [CrossRef]
- H. Solomon et al., “Neuropathological Features of Covid-19,” New England Journal of Medicine, vol. 383, no. 10, pp. 989–992, Sep. 2020, doi: 10.1056/NEJMc2019373. [CrossRef]
- B. Khraisat, A. Toubasi, L. AlZoubi, T. Al-Sayegh, and A. Mansour, “Meta-analysis of prevalence: the psychological sequelae among COVID-19 survivors,” Int J Psychiatry Clin Pract, vol. 26, no. 3, pp. 234–243, Sep. 2022, doi: 10.1080/13651501.2021.1993924. [CrossRef]
- T. Nasserie, M. Hittle, and S. N. Goodman, “Assessment of the Frequency and Variety of Persistent Symptoms Among Patients With COVID-19,” JAMA Netw Open, vol. 4, no. 5, p. e2111417, May 2021, doi: 10.1001/jamanetworkopen.2021.11417. [CrossRef]
- M. Cai, Y. Xie, E. J. Topol, and Z. Al-Aly, “Three-year outcomes of post-acute sequelae of COVID-19,” Nat Med, vol. 30, no. 6, pp. 1564–1573, Jun. 2024, doi: 10.1038/s41591-024-02987-8. [CrossRef]
- J. Flegr and A. Latifi, “COVID’s long shadow: How SARS-CoV-2 infection, COVID-19 severity, and vaccination status affect long-term cognitive performance and health,” Biol Methods Protoc, vol. 8, no. 1, Jan. 2023, doi: 10.1093/biomethods/bpad038. [CrossRef]
- Latifi and J. Flegr, “Is recovery just the beginning? Persistent symptoms and health and performance deterioration in post-COVID-19, non-hospitalized university students—a cross-sectional study,” Biol Methods Protoc, vol. 8, no. 1, Jan. 2023, doi: 10.1093/biomethods/bpad037. [CrossRef]
- P. Jin, F. Cui, M. Xu, Y. Ren, and L. Zhang, “Altered brain function and structure pre- and post- COVID-19 infection: a longitudinal study,” Neurological Sciences, vol. 45, no. 1, pp. 1–9, Jan. 2024, doi: 10.1007/s10072-023-07236-3. [CrossRef]
- T. Iba, J. H. Levy, C. L. Maier, J. M. Connors, and M. Levi, “Four years into the pandemic, managing COVID-19 patients with acute coagulopathy: what have we learned?,” Journal of Thrombosis and Haemostasis, vol. 22, no. 6, pp. 1541–1549, Jun. 2024, doi: 10.1016/j.jtha.2024.02.013. [CrossRef]
- Latifi and J. Flegr, “Persistent Health and Cognitive Impairments up to Four Years Post-COVID-19 in Young Students: The Impact of Virus Variants and Vaccination Timing,” Biomedicines, vol. 13, no. 1, p. 69, Dec. 2024, doi: 10.3390/biomedicines13010069. [CrossRef]
- S. Kim et al., “Short- and long-term neuropsychiatric outcomes in long COVID in South Korea and Japan,” Nat Hum Behav, vol. 8, no. 8, pp. 1530–1544, Jun. 2024, doi: 10.1038/s41562-024-01895-8. [CrossRef]
- D. LR., “SCL-90-R : administration, scoring and procedures,” Manual II for the R (evised) Version and Other Instruments of the Psychopathology Rating Scale Series, 1983, Accessed: Dec. 25, 2023. [Online]. Available: https://cir.nii.ac.jp/crid/1573387450267334400.
- D. LR, “SCL-90 : an outpatient psychiatric rating scale-preliminary report,” Psychopharmacol Bull, vol. 9, pp. 13–28, 1973, doi: 10.15064/JJPM.53.4_334. [CrossRef]
- F. Akhavan Abiri and M. R. Shairi, “Validity and Reliability of Symptom Checklist-90-Revised (SCL-90-R) and Brief Symptom Inventory-53 (BSI-53),” Clinical Psychology and Personality, vol. 17, no. 2, pp. 169–195, Sep. 2020, doi: 10.22070/CPAP.2020.2916. [CrossRef]
- R. E. Hamlin et al., “Sex differences and immune correlates of Long Covid development, symptom persistence, and resolution,” Sci Transl Med, vol. 16, no. 773, Nov. 2024, doi: 10.1126/scitranslmed.adr1032. [CrossRef]
- Gorenshtein, L. Leibovitch, T. Liba, S. Stern, and Y. Stern, “Gender Disparities in Neurological Symptoms of Long COVID: A Systematic Review and Meta-Analysis,” Neuroepidemiology, pp. 1–15, Aug. 2024, doi: 10.1159/000540919. [CrossRef]
- J. Matta et al., “Depressive symptoms and sex differences in the risk of post-COVID-19 persistent symptoms: a prospective population-based cohort study,” Nature Mental Health, vol. 2, no. 9, pp. 1053–1061, Jul. 2024, doi: 10.1038/s44220-024-00290-6. [CrossRef]
- Y. Zhang, V. M. Chinchilli, P. Ssentongo, and D. M. Ba, “Association of Long COVID with mental health disorders: a retrospective cohort study using real-world data from the USA,” BMJ Open, vol. 14, no. 2, p. e079267, Feb. 2024, doi: 10.1136/bmjopen-2023-079267. [CrossRef]
- J. D. Bremner, S. J. Russo, R. Gallagher, and N. M. Simon, “Acute and long-term effects of COVID-19 on brain and mental health: A narrative review,” Brain Behav Immun, vol. 123, pp. 928–945, Jan. 2025, doi: 10.1016/j.bbi.2024.11.007. [CrossRef]
- Rodríguez Onieva, C. A. Soto Castro, V. García Morales, M. Aneri Vacas, and A. Hidalgo Requena, “Long COVID: Factors influencing persistent symptoms and the impact of gender,” Medicina de Familia. SEMERGEN, vol. 50, no. 5, p. 102208, Jul. 2024, doi: 10.1016/j.semerg.2024.102208. [CrossRef]
- Skevaki, C. D. Moschopoulos, P. C. Fragkou, K. Grote, E. Schieffer, and B. Schieffer, “Long COVID: Pathophysiology, current concepts, and future directions,” Journal of Allergy and Clinical Immunology, Dec. 2024, doi: 10.1016/j.jaci.2024.12.1074. [CrossRef]
- K. Sakai, S. Tarutani, T. Okamura, H. Yoneda, T. Kawasaki, and M. Takeda, “Comparing personality traits of healthcare workers with and without long COVID: Cross-sectional study,” Psychiatry and Clinical Neurosciences Reports, vol. 3, no. 4, Dec. 2024, doi: 10.1002/pcn5.70017. [CrossRef]
- C. E. Gebhard et al., “Impact of sex and gender on post-COVID-19 syndrome, Switzerland, 2020,” Eurosurveillance, vol. 29, no. 2, Jan. 2024, doi: 10.2807/1560-7917.ES.2024.29.2.2300200. [CrossRef]
- R. Van Cleve et al., “Risk of developing long COVID based on acute COVID-19 severity,” J Public Health (Bangkok), Nov. 2024, doi: 10.1007/s10389-024-02364-2. [CrossRef]
- S. Kananian, A. Nemani, and U. Stangier, “Risk and protective factors for the severity of long COVID – A network analytic perspective,” J Psychiatr Res, vol. 178, pp. 291–297, Oct. 2024, doi: 10.1016/j.jpsychires.2024.08.031. [CrossRef]
- F. Couto Amendola et al., “A Two-Year cohort study examining the impact of cytokines and chemokines on cognitive and psychiatric outcomes in Long-COVID-19 patients,” Brain Behav Immun, vol. 124, pp. 218–225, Feb. 2025, doi: 10.1016/j.bbi.2024.12.006. [CrossRef]
- U. Bonnet and J. Kuhn, “Serotonin deficiency and psychiatric long COVID: both caused specifically by the virus itself or an adaptive general stress response?,” Eur Arch Psychiatry Clin Neurosci, Feb. 2024, doi: 10.1007/s00406-024-01769-0. [CrossRef]
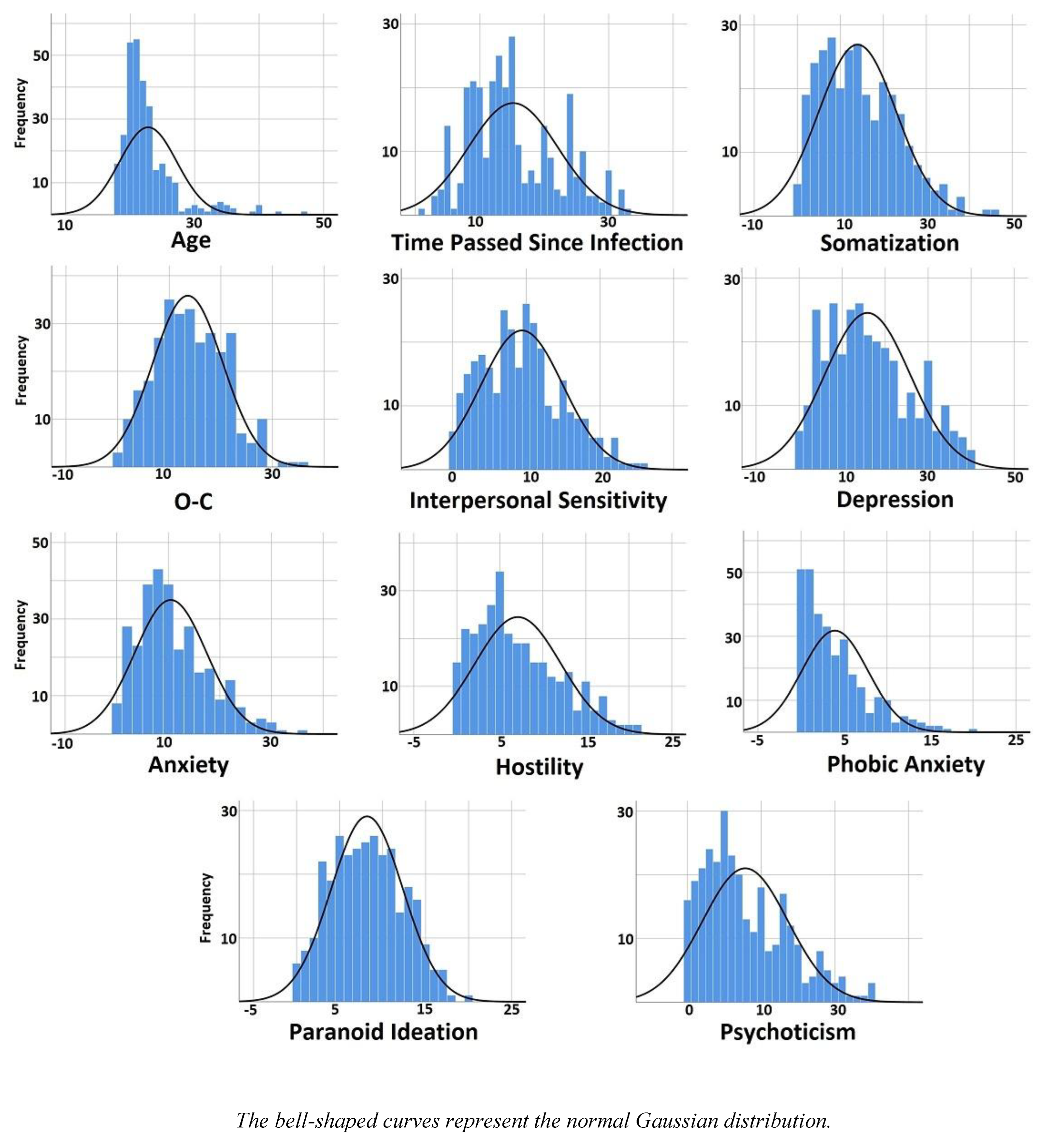
| Skewness | |||||
| N | Mean | Std. Deviation | Statistic | Std. Error | |
| Age | 305 | 22.80 | 4.438 | 2.315 | 0.140 |
| TPSI | 305 | 15.18 | 6.921 | 0.529 | 0.140 |
| Somatization | 305 | 14.01 | 9.052 | 0.641 | 0.140 |
| O-C | 305 | 13.59 | 6.795 | 0.285 | 0.140 |
| Interpersonal Sensitivity | 305 | 9.42 | 5.573 | 0.468 | 0.140 |
| Depression | 305 | 15.90 | 9.925 | 0.457 | 0.140 |
| Anxiety | 305 | 10.45 | 6.959 | 0.813 | 0.140 |
| Hostility | 305 | 7.10 | 4.967 | 0.664 | 0.140 |
| Phobic Anxiety | 305 | 3.95 | 3.830 | 1.304 | 0.140 |
| Paranoid Ideation | 305 | 8.19 | 4.184 | 0.162 | 0.140 |
| Psychoticism | 305 | 7.85 | 5.795 | 0.794 | 0.140 |
| All Participants | |||||||||
| Tau Partial Correlation Coefficients | |||||||||
| Somatization | O-C | Interpersonal Sensitivity | Depression | Anxiety | Hostility | Phobic Anxiety | Paranoid Ideation | Psychoticism | |
| Age | 0.026 | 0.091* | 0.005 | 0.059 | 0.032 | 0.033 | 0.02 | 0.027 | 0.03 |
| TPSI | 0.028 | 0.077* | 0.089* | 0.109** | 0.099* | 0.09* | -0.012 | 0.098* | 0.036 |
| Severity | 0.206*** | 0.159*** | 0.125** | 0.14*** | 0.17*** | 0.156*** | 0.085* | 0.131** | 0.168*** |
| Sex | -0.224*** | -0.121** | -0.092* | -0.115** | -0.151*** | -0.064 | -0.052 | -0.017 | 0.024 |
| P-values | |||||||||
| Age | 0.503 | 0.018 | 0.905 | 0.125 | 0.411 | 0.389 | 0.603 | 0.483 | 0.43 |
| TPSI | 0.459 | 0.044 | 0.021 | 0.004 | 0.01 | 0.02 | 0.755 | 0.01 | 0.346 |
| Severity | 0.000 | 0.000 | 0.001 | 0.000 | 0.000 | 0.000 | 0.027 | 0.001 | 0.000 |
| Sex | 0.000 | 0.002 | 0.017 | 0.003 | 0.000 | 0.095 | 0.179 | 0.652 | 0.527 |
| Men | |||||||||
| Tau Partial Correlation Coefficients | |||||||||
| Age | 0.007 | 0.068 | -0.018 | 0.033 | -0.002 | 0.006 | -0.024 | 0.009 | 0.02 |
| TPSI | 0.031 | 0.068 | 0.039 | 0.076 | 0.072 | 0.127* | 0.003 | 0.107 | 0.02 |
| Severity | 0.186** | 0.181** | 0.174** | 0.149** | 0.15** | 0.122* | 0.097 | 0.117* | 0.183** |
| P-values | |||||||||
| Age | 0.897 | 0.219 | 0.747 | 0.552 | 0.968 | 0.91 | 0.658 | 0.872 | 0.724 |
| TPSI | 0.581 | 0.22 | 0.479 | 0.172 | 0.196 | 0.022 | 0.961 | 0.053 | 0.718 |
| Severity | 0.001 | 0.001 | 0.002 | 0.007 | 0.007 | 0.028 | 0.08 | 0.035 | 0.001 |
| Women | |||||||||
| Tau Partial Correlation Coefficients | |||||||||
| Age | 0.003 | 0.083 | 0.005 | 0.061 | 0.03 | 0.04 | 0.038 | 0.036 | 0.025 |
| TPSI | 0.037 | 0.087 | 0.139* | 0.154** | 0.13* | 0.061 | -0.018 | 0.094 | 0.06 |
| Severity | 0.23*** | 0.14* | 0.071 | 0.128* | 0.17** | 0.192*** | 0.066 | 0.145** | 0.157** |
| P-values | |||||||||
| Age | 0.957 | 0.126 | 0.932 | 0.255 | 0.582 | 0.459 | 0.482 | 0.5 | 0.637 |
| TPSI | 0.499 | 0.109 | 0.01 | 0.005 | 0.017 | 0.259 | 0.734 | 0.082 | 0.271 |
| Severity | 0.000 | 0.01 | 0.191 | 0.018* | 0.002 | 0.000 | 0.222 | 0.008 | 0.004 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




