Submitted:
08 February 2025
Posted:
10 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Gait Assessment Protocol
2.3. Instrumentation & Gait Analysis
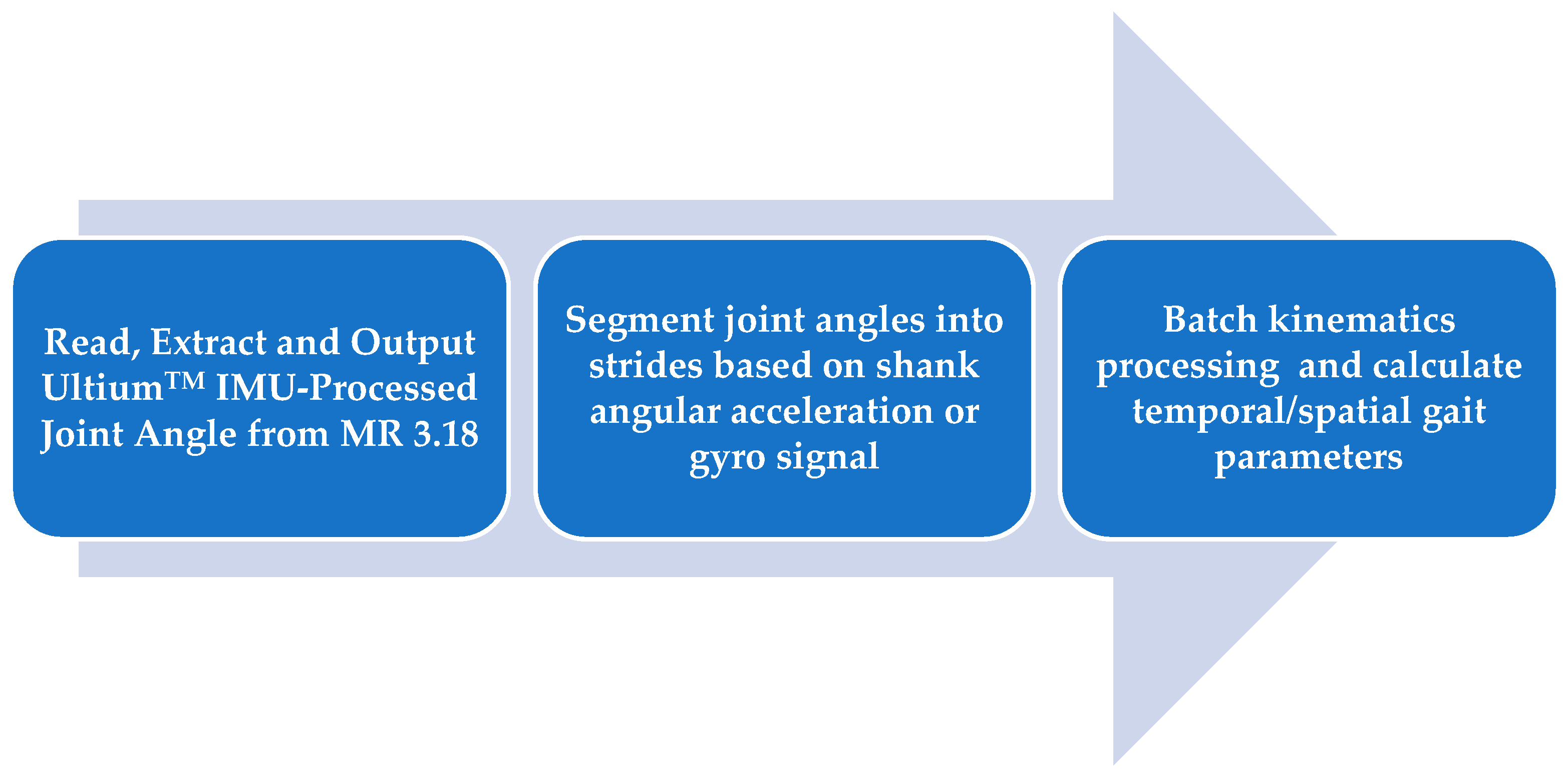
2.4. Data Processing
2.6. Statistical Analysis
- ▪
- XProsthetic is the value of the gait parameter for the prosthetic limb.
- ▪
- Xintact is the value of the gait parameter for the intact limb.
- ▪
-
The GSI score is used to quantify similarity of movements between limbs, where:
- ❖
- GSI = 0% indicates perfect symmetry (i.e. no difference between prosthetic and intact limbs)
- ❖
- GSI > 0% indicates asymmetry, where
- ❖
- GSI < 0% indicates asymmetry, where
3. Results
3.1. Demographics and Temporal/Spatial
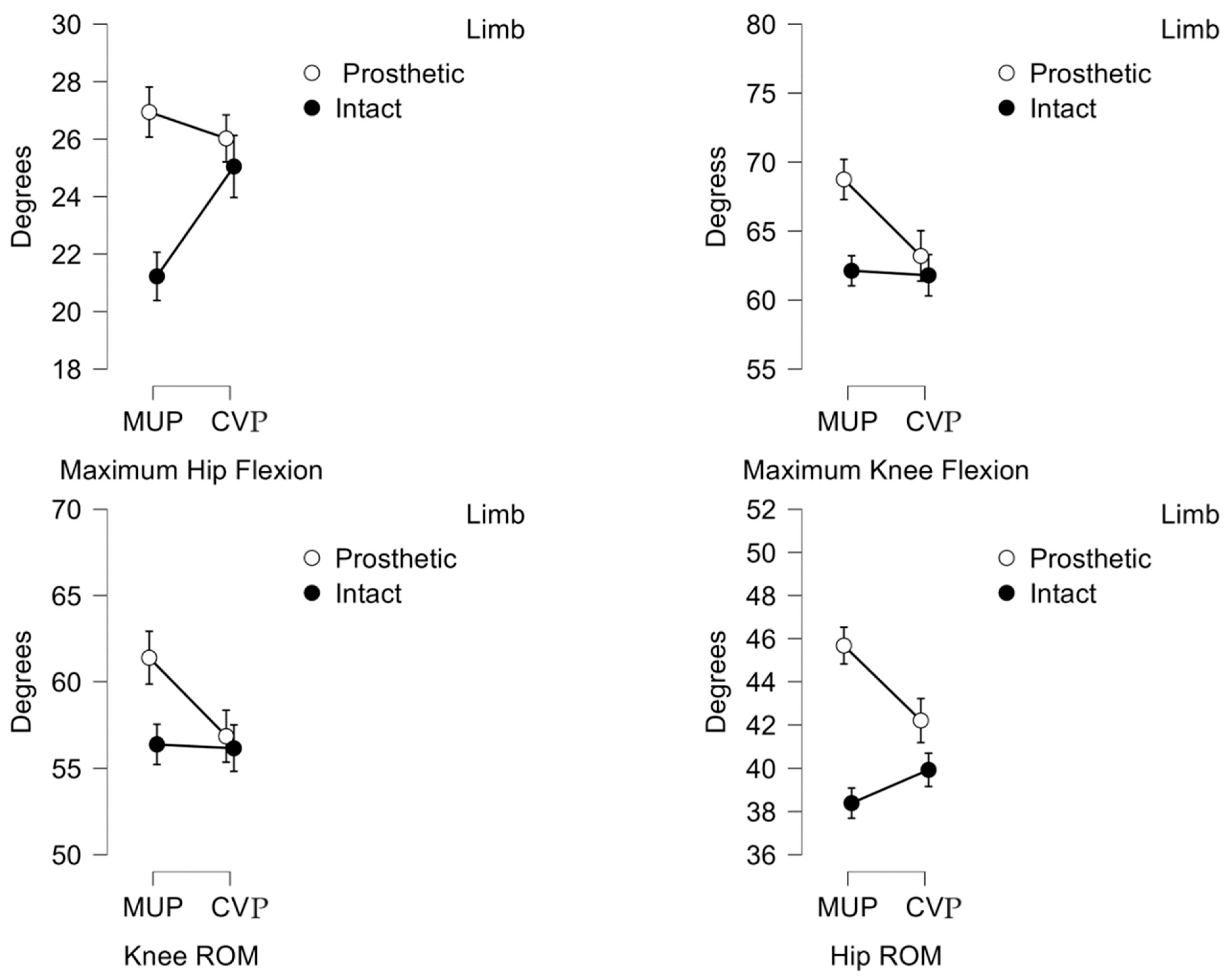
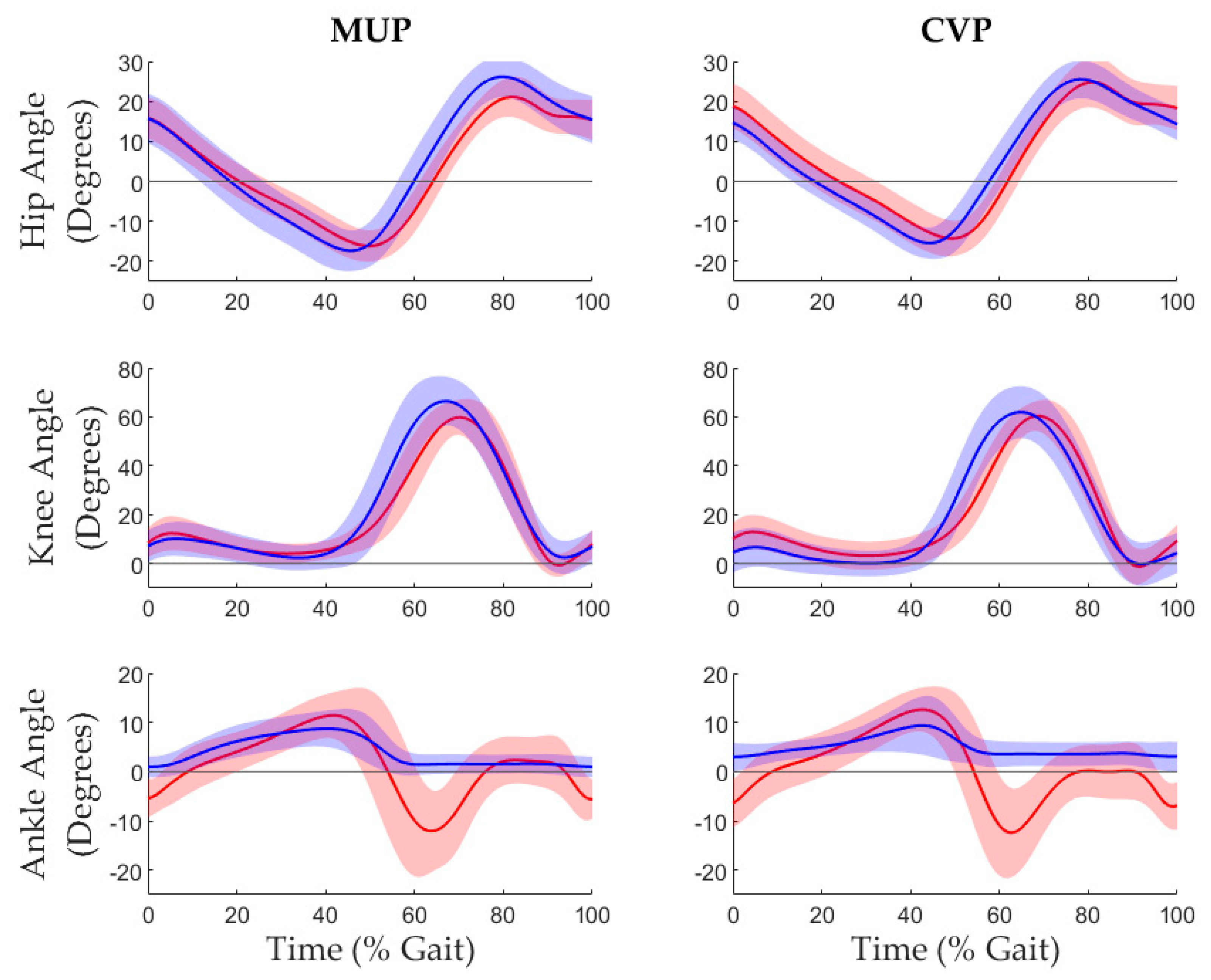
3.2. Kinematics
3.3. Gait Symmetry Index (GSI)
4. Discussion
5. Conclusions and Suggestions
6. Patents
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- M. Marino et al., “Access to prosthetic devices in developing countries: Pathways and challenges,” in 2015 IEEE Global Humanitarian Technology Conference (GHTC), IEEE, Oct. 2015, pp. 45–51. [CrossRef]
- J. Andrysek, “Lower-limb prosthetic technologies in the developing world: A review of literature from 1994-2010,” Dec. 2010. [CrossRef]
- D. Wyss, S. Lindsay, W. L. Cleghorn, and J. Andrysek, “Priorities in lower limb prosthetic service delivery based on an international survey of prosthetists in low- and high-income countries,” Prosthet Orthot Int, vol. 39, no. 2, pp. 102–111, 2015, . [CrossRef]
- M. Marino et al., “Access to prosthetic devices in developing countries: Pathways and challenges,” in 2015 IEEE Global Humanitarian Technology Conference (GHTC), IEEE, Oct. 2015, pp. 45–51. [CrossRef]
- J. S. Jensen, W. Raab, J. Fisk, C. Hartz, A. Saldana, and C. Harte, “Quality of polypropylene sockets for trans-tibial prostheses in low-income countries,” Prosthet Orthot Int, vol. 30, no. 1, pp. 45–59, Apr. 2006, . [CrossRef]
- J. S. Jensen, R. Nilsen, and J. Zeffer, “Quality benchmark for trans-tibial prostheses in low-income countries,” Prosthet Orthot Int, vol. 29, no. 1, pp. 53–58, Apr. 2005, . [CrossRef]
- H. V. Vo, B. N. Nguyen, T. T. Le, C. T. McMahan, E. M. O’Brien, and R. K. Kunz, “The novel design of the mercer universal prosthesis,” in IFMBE Proceedings, Springer Verlag, 2018, pp. 197–204. [CrossRef]
- A. A. Arora, B. E. Nguyen, T. E. Le, B. Lian, L. X. Webb, and H. V Vo, “Harvard Medical Student Review Issue 4 | HMSR RESEARCH Clinical Using 2D Gait Motion Analysis to Evaluate the Mercer Universal Prosthetic Device in a Vietnamese Population,” 2018.
- A. Courtney, M. S. Orendurff, and A. Buis, “Effect of alignment perturbations in a trans-tibial prosthesis user: A pilot study,” J Rehabil Med, vol. 48, no. 4, pp. 396–401, Apr. 2016, . [CrossRef]
- Y. Cherni, S. Laurendeau, M. Robert, and K. Turcot, “The Influence of Transtibial Prosthesis Type on Lower-Body Gait Adaptation: A Case Study,” Int J Environ Res Public Health, vol. 20, no. 1, Jan. 2023, . [CrossRef]
- T. Kobayashi, M. S. Orendurff, and D. A. Boone, “Dynamic alignment of transtibial prostheses through visualization of socket reaction moments,” Prosthet Orthot Int, vol. 39, no. 6, pp. 512–516, Dec. 2015, . [CrossRef]
- C. W. J. Chen et al., “Evaluation of an instrument-assisted dynamic prosthetic alignment technique for individuals with transtibial amputation,” Prosthet Orthot Int, vol. 40, no. 4, pp. 475–483, Aug. 2016, . [CrossRef]
- T. Kobayashi, M. S. Orendurff, M. Zhang, and D. A. Boone, “Effect of transtibial prosthesis alignment changes on out-of-plane socket reaction moments during walking in amputees,” J Biomech, vol. 45, no. 15, pp. 2603–2609, Oct. 2012, . [CrossRef]
- H. Hashimoto, T. Kobayashi, F. Gao, M. Kataoka, M. S. Orendurff, and K. Okuda, “The effect of transverse prosthetic alignment changes on socket reaction moments during gait in individuals with transtibial amputation,” Gait Posture, vol. 65, pp. 8–14, Sep. 2018, . [CrossRef]
- M. S. Zahedi, W. D. Spence, S. E. Solomonidis, and J. P. Paul, “Alignment of lower-limb prostheses.,” J Rehabil Res Dev, vol. 23, no. 2, pp. 2–19, Apr. 1986, [Online]. Available: http://www.ncbi.nlm.nih.gov/pubmed/3723422.
- M. S. Pinzur, W. Cox, J. Kaiser, T. Morris, A. Patwardhan, and L. Vrbos, “The effect of prosthetic alignment on relative limb loading in persons with trans-tibial amputation: a preliminary report.,” J Rehabil Res Dev, vol. 32, no. 4, pp. 373–7, Nov. 1995, Accessed: Jan. 30, 2023. [Online]. Available: http://www.ncbi.nlm.nih.gov/pubmed/8770802.
- C. Siddhardh Muvvala, J. Kethar, S. Ganapathy, and B. Reed Henderson High School, “Implementation of Prosthetics in Underdeveloped Countries.” [Online]. Available: www.JSR.org.
- S. Park and S. Yoon, “Validity evaluation of an inertial measurement unit (IMU) in gait analysis using statistical parametric mapping (SPM),” Sensors, vol. 21, no. 11, Jun. 2021, . [CrossRef]
- K. Berner, J. Cockcroft, L. D. Morris, and Q. Louw, “Concurrent validity and within-session reliability of gait kinematics measured using an inertial motion capture system with repeated calibration,” J Bodyw Mov Ther, vol. 24, no. 4, pp. 251–260, Oct. 2020, . [CrossRef]
- M. Al-Amri, K. Nicholas, K. Button, V. Sparkes, L. Sheeran, and J. L. Davies, “Inertial measurement units for clinical movement analysis: Reliability and concurrent validity,” Sensors (Switzerland), vol. 18, no. 3, Mar. 2018, . [CrossRef]
- Z. Aftab and R. Shad, “Estimation of gait parameters using leg velocity for amputee population,” PLoS One, vol. 17, no. 5 May, May 2022, . [CrossRef]
- Z. Aftab, “Assessing the validity of dual-minima algorithm for heel-strike and toe-off prediction for the amputee population,” 2021, . [CrossRef]
- J. Love et al., “JASP: Graphical statistical software for common statistical designs,” J Stat Softw, vol. 88, no. 1, 2019, . [CrossRef]
- S. Holm, “Board of the Foundation of the Scandinavian Journal of Statistics A Simple Sequentially Rejective Multiple Test Procedure A Simple Sequentially Rejective Multiple Test Procedure,” 1979.
- Y. Chang et al., “Changes in Spatiotemporal Parameters and Lower Limb Coordination During Prosthetic Gait Training in Unilateral Transfemoral Amputees,” International Journal of Precision Engineering and Manufacturing, vol. 23, no. 3, pp. 361–373, Mar. 2022, . [CrossRef]
- I. Kova~, V. Medved, and L. Ostoji}, “Spatial, Temporal and Kinematic Characteristics of Traumatic Transtibial Amputees’ Gait,” 2010.
- W. Herzog, B. M. Nigg, L. J. Read, and E. Olsson, “Asymmetries in ground reaction force patterns in normal human gait.,” Med Sci Sports Exerc, vol. 21, no. 1, pp. 110–4, Feb. 1989, . [CrossRef]
- K. De Pauw et al., “Prosthetic gait of unilateral lower-limb amputees with current and novel prostheses: A pilot study: Kinetics and kinematics of prosthetic gait,” Clinical Biomechanics, vol. 71, pp. 59–67, Jan. 2020, . [CrossRef]
- S. Laing, N. Lythgo, J. Lavranos, and P. V. S. Lee, “Transtibial Prosthetic Socket Shape in a Developing Country: A study to compare initial outcomes in Pressure Cast hydrostatic and Patella Tendon Bearing designs,” Gait Posture, vol. 58, pp. 363–368, Oct. 2017, . [CrossRef]
- S. Laing, P. V. S. Lee, J. Lavranos, and N. Lythgo, “The functional, spatio-temporal and satisfaction outcomes of transtibial amputees with a hydrocast socket following an extended usage period in an under-resourced environment,” Gait Posture, vol. 66, pp. 88–93, Oct. 2018, . [CrossRef]
- P. V. S. Lee, N. Lythgo, S. Laing, J. Lavranos, and N. H. Thanh, “10Pressure casting technique for transtibial prosthetic socket fit in developing countries,” J Rehabil Res Dev, vol. 51, no. 1, pp. 101–110, 2014, . [CrossRef]
- H. Bateni and S. J. Olney, “Effect of the Weight of Prosthetic Components on the Gait of Transtibial Amputees,” 2004. [Online]. Available: http://journals.lww.com/jpojournal.
- J. S. Jensen, R. Nilsen, J. Zeffer, J. Fisk, and C. Hartz, “Clinical field testing of vulcanized rubber feet for trans-tibial amputees in tropical low-income countries,” Prosthet Orthot Int, vol. 30, no. 2, pp. 195–212, Aug. 2006, . [CrossRef]
- X. Zhang, G. Fiedler, and Z. Liu, “Evaluation of gait variable change over time as transtibial amputees adapt to a new prosthesis foot,” Biomed Res Int, vol. 2019, 2019, . [CrossRef]
- T. Schmalz, M. Bellmann, E. Proebsting, and S. Blumentritt, “Effects of Adaptation to a Functionally New Prosthetic Lower-Limb Component: Results of Biomechanical Tests Immediately after Fitting and after 3 Months of Use.” [Online]. Available: http://journals.lww.com/jpojournal.
- S. F. Ray, S. R. Wurdeman, and K. Z. Takahashi, “Prosthetic energy return during walking increases after 3 weeks of adaptation to a new device,” J Neuroeng Rehabil, vol. 15, no. 1, Jan. 2018, . [CrossRef]
- B. J. Darter, E. D. Syrett, K. B. Foreman, E. Kubiak, and S. Sinclair, “Changes in frontal plane kinematics over 12-months in individuals with the Percutaneous Osseointegrated Prosthesis (POP),” PLoS One, vol. 18, no. 2 February, Feb. 2023, . [CrossRef]
- C. Barnett et al., “Kinematic gait adaptations in unilateral transtibial amputees during rehabilitation,” Prosthet Orthot Int, vol. 33, no. 2, pp. 135–147, 2009, . [CrossRef]

| Sex | 19 Male / 1 Female | |
| Age | 60.4 ± 8.08 year | |
| Height | 1.60 ± 0.07 m | |
| Prosthetic Mass | Conventional (CVP) | 1.55 ± 0.35 kg |
| Mercer Universal (MUP) | 1.31 ± 0.16 kg | |
| Descriptive Statistics: Mean (Std) | 2 Factors Repeated ANOVA | ||||||
| MUP | CVP | p-value | |||||
| Prosthetic | Intact | Prosthetic | Intact | Device*Limb | Device | Limb | |
| Stride Time (s) | 1.26 (0.15) | 1.26 (0.15) | 1.24 (0.13) | 1.24 (0.13) | 0.171 | 0.086 | 0.641 |
| Stance Time (s) | 0.65 (0.12) | 0.61 (0.05) | 0.61 (0.09) | 0.63 (0.06) | 0.287 | <0.001** | <0.001** |
| Swing Time (s) | 0.71 (0.14) | 0.55 (0.03) | 0.67 (0.12) | 0.57 (0.03) | 0.785 | 0.003** | <0.001** |
| Speed (m/s) | 0.68 (0.19) | 0.69 (0.20) | 0.72 (0.13) | 0.72 (0.13) | 0.590 | 0.378 | 0.276 |
| Stride Length (m) | 0.86 (0.21) | 0.86 (0.20) | 0.87 (0.10) | 0.89 (0.10) | 0.419 | 0.696 | 0.348 |
| Step Length (m) | 0.44 (0.12) | 0.45 (0.14) | 0.42 (0.10) | 0.48 (0.09) | 0.120 | 0.752 | 0.265 |
| Descriptive Statistics: Mean (Std) | 2 Factors Repeated ANOVA | ||||||
| MUP | CVP | p-value | |||||
| Prosthetic | Intact | Prosthetic | Intact | Device*Limb | Device | Limb | |
| Hip Extension (0) | -18.6 (4.1) | -17.1(3.) | -16.1 (3.5) | -14.8 (4.7) | 0.786 | 0.013* | 0.092 |
| Knee Extension (0) | -0.4 (6.2) | -1.4(4.5) | -3.2 (5.8) | -1.5 (7.2) | 0.459 | 0.301 | 0.230 |
| Ankle Plantarflex (0) | 0.3 (2.2) | -17.6 (7.7) | 1.9 (2.9) | -15.1 (7.0) | 0.435 | 0.011* | <0.001** |
| Hip Flexion (0) | 26.9 (4.8) | 21.2 (4.9) | 26.03 (4.5) | 25.1 (6.1) | 0.013 | 0.039* | 0.008 |
| Knee Flexion (0) | 68.4 (9.3) | 62.0(5.8) | 63.2 (9.3) | 61.6 (6.3) | 0.025 | 0.016* | 0.067 |
| Ankle Dorsiflex (0) | 9.3 (4.1) | 12.8 (4.4) | 10.1 (6.2) | 13.7 (4.4) | 0.929 | 0.281 | 0.004* |
| Hip ROM (0) | 45.5 (5.3) | 38.2 (4.1) | 42.1 (6.1) | 39.8 (4.3) | 0.014* | 0.124 | <0.001** |
| Knee ROM (0) | 68.8 (10.6) | 63.1 (5.6) | 66.3 (8.6) | 63.0 (6.5) | 0.033* | 0.024* | 0.168 |
| Ankle ROM (0) | 8.9 (3.5) | 30.3 (6.4) | 8.2 (7.7) | 28.8 (5.7) | 0.675 | 0.305 | <0.001** |
| Mean GSI (SEM) |
Paired t-test p < 0.05 |
|||
| MUP | CVP | |||
| Hip Extension (0) | 9.1 (4.9) | 11.1 (7.9) | .780 | |
| Knee Extension (0) | 18.7 (19.4) | 25.1 (23.0) | .806 | |
| Ankle Plantarflexion (0) | -163.4 (46.0) | -267.9 (61.3) | .013* | |
| Hip Flexion (0) | 24.2 (5.5) | 5.2 (5.) | .012* | |
| Knee Flexion (0) | 9.7 (2.8) | 1.7 (4.2) | .026* | |
| Ankle Dorsiflexion (0) | -32.9 (10.9) | -36.4 (12.2) | .738 | |
| Hip ROM (0) | 17.1 (2.9) | 5.1 (3.5) | .014* | |
| Knee ROM (0) | 7.8 (3.6) | 0.6 (4.0) | .044* | |
| Ankle ROM (0) | -109.2 (6.5) | -120.4 (10.3) | .323 | |
| Mean GSI (SEM) |
Paired t-test p < 0.05 |
||
| MUP | CVP | ||
| Stride Duration (s)
Stance Duration (s) Swing Duration (s) Speed (m/s) Stride Length (m) Step Length (m) |
0.5 (0.2) -7.8 (1.4) 9.4 (1.6) -1.2 (1.3) -0.3 (1.4) -0.8 (8.4) |
-0.2 (0.4) -10.2 (1.8) 10.2 (1.8) -0.7 (0.8) -1.6 (0.9) -14.9 (8.0) |
0.120 0.185 0.838 0.747 0.473 0.135 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




