Submitted:
29 January 2025
Posted:
30 January 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
- To evaluate whether Apolipoproteins and their ratios serve as superior diagnostic and prognostic markers for CAD risk assessment compared to the traditional lipid profile;
- To compare the diagnostic accuracy of Apolipoproteins and the ApoB/ ApoA-I ratio with traditional lipid parameters in predicting the severity of coronary artery disease.
2. Materials and Methods
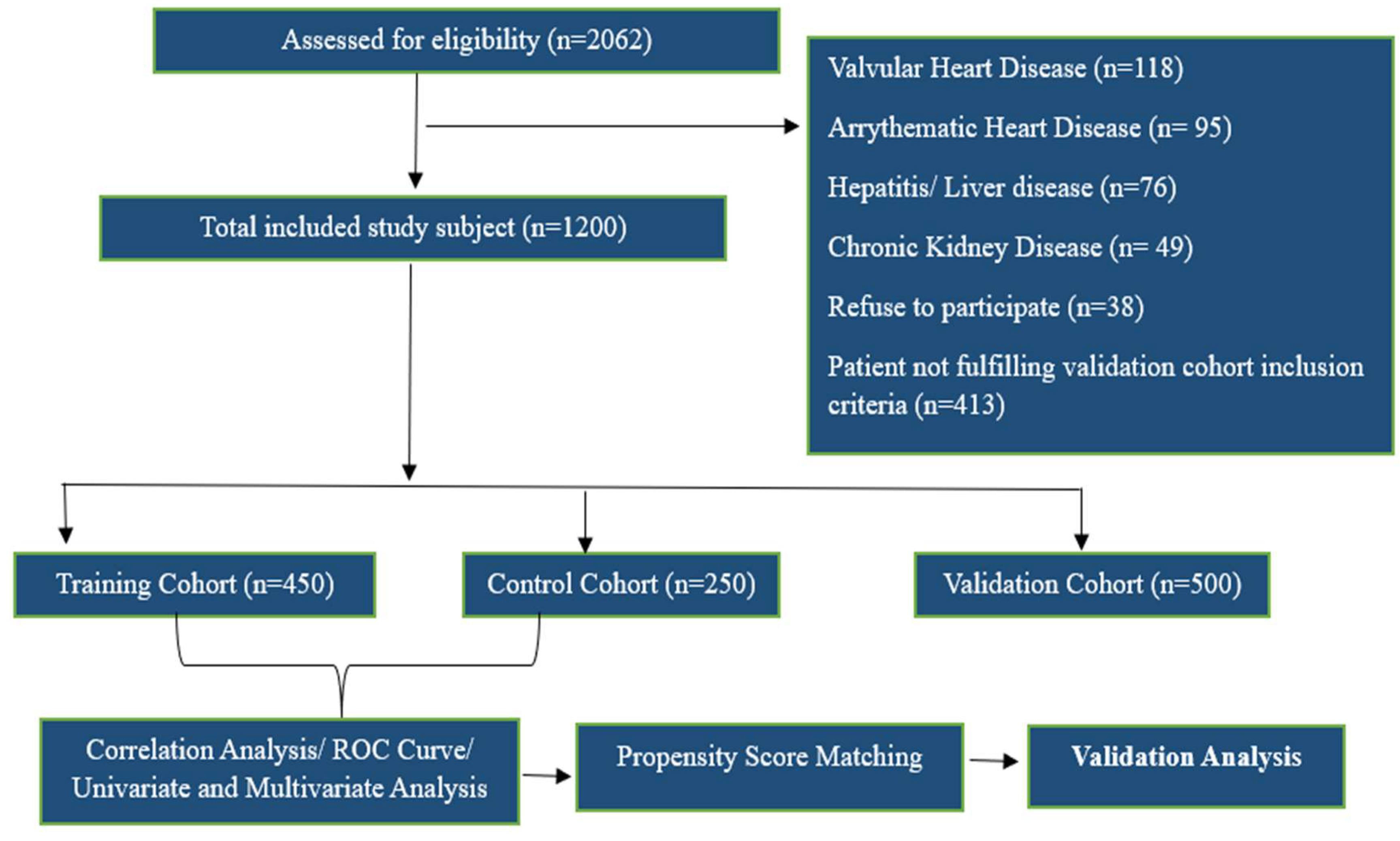
2.1. Study Design & Data Collection
2.2. Laboratory Workup
2.3. Coronary Angiography
2.4. Statistical Analysis
3. Results
3.1. Overview of Demographic and Clinical Characteristics of Participants
3.2. Demographic & Biochemical Characteristics of Validation Cohort
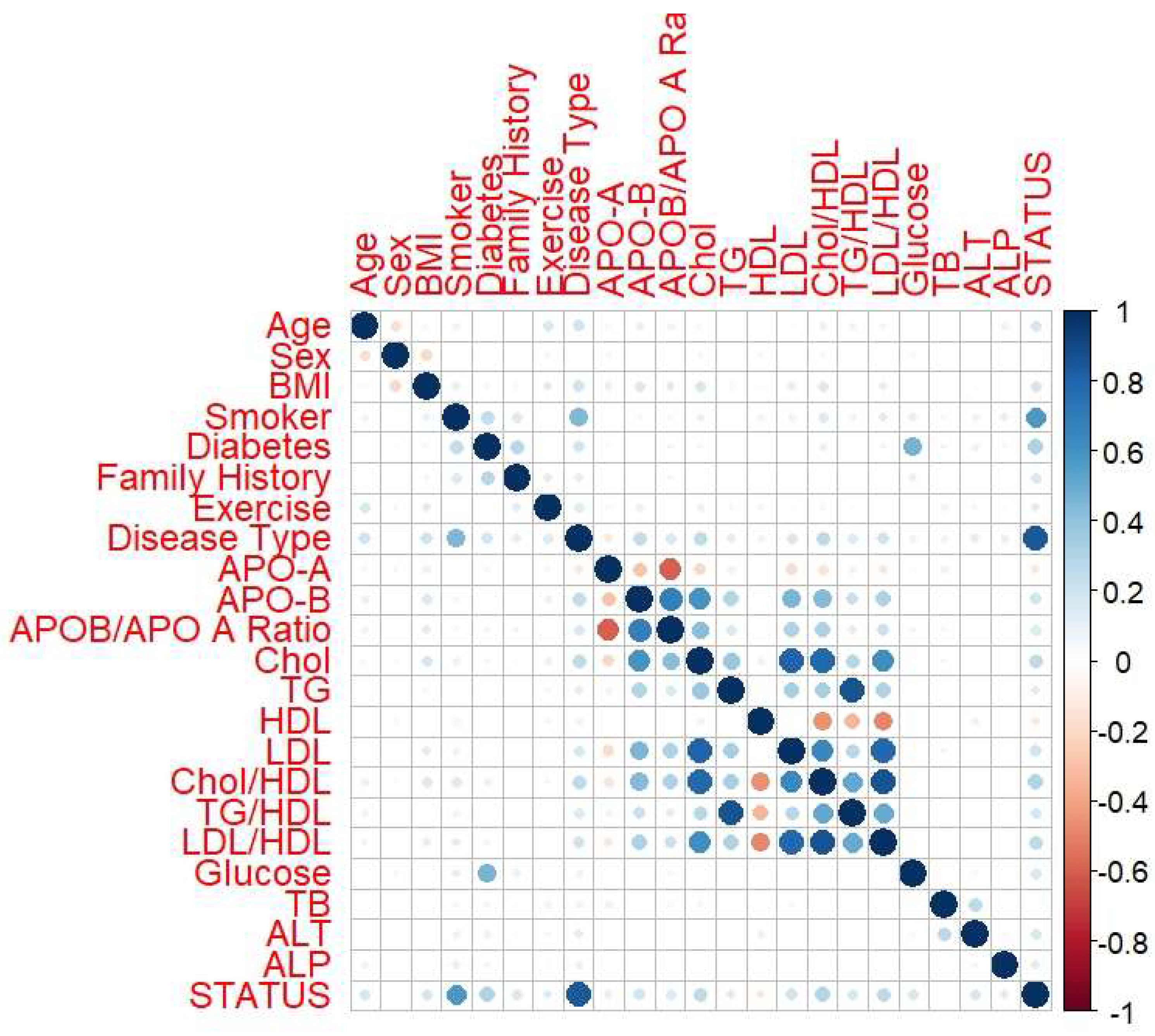
3.3. Correlation Analysis Between Biochemical and Descriptive Parameters
3.4. Univariate and Multivariate Analysis (Post PSM)
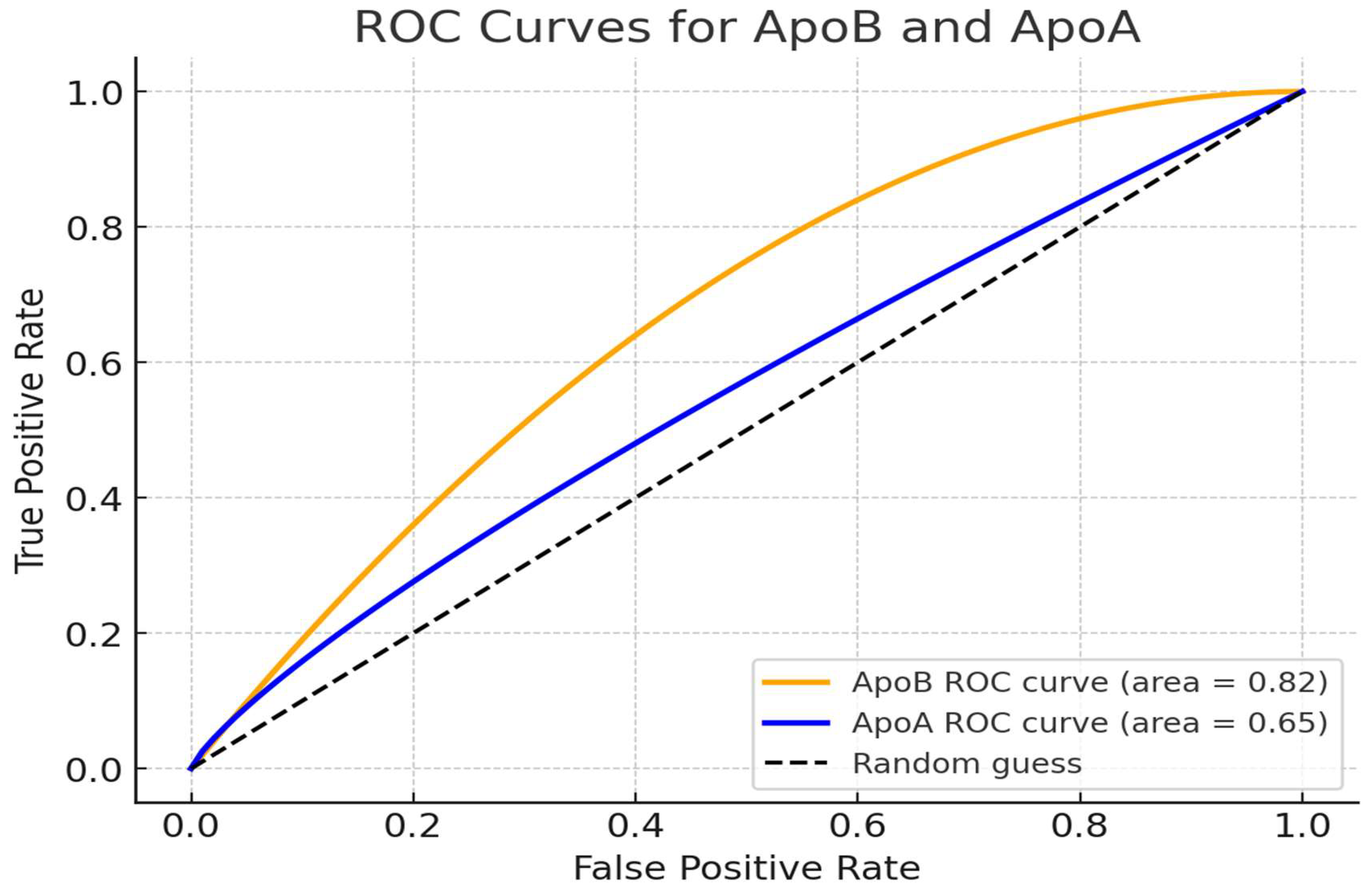
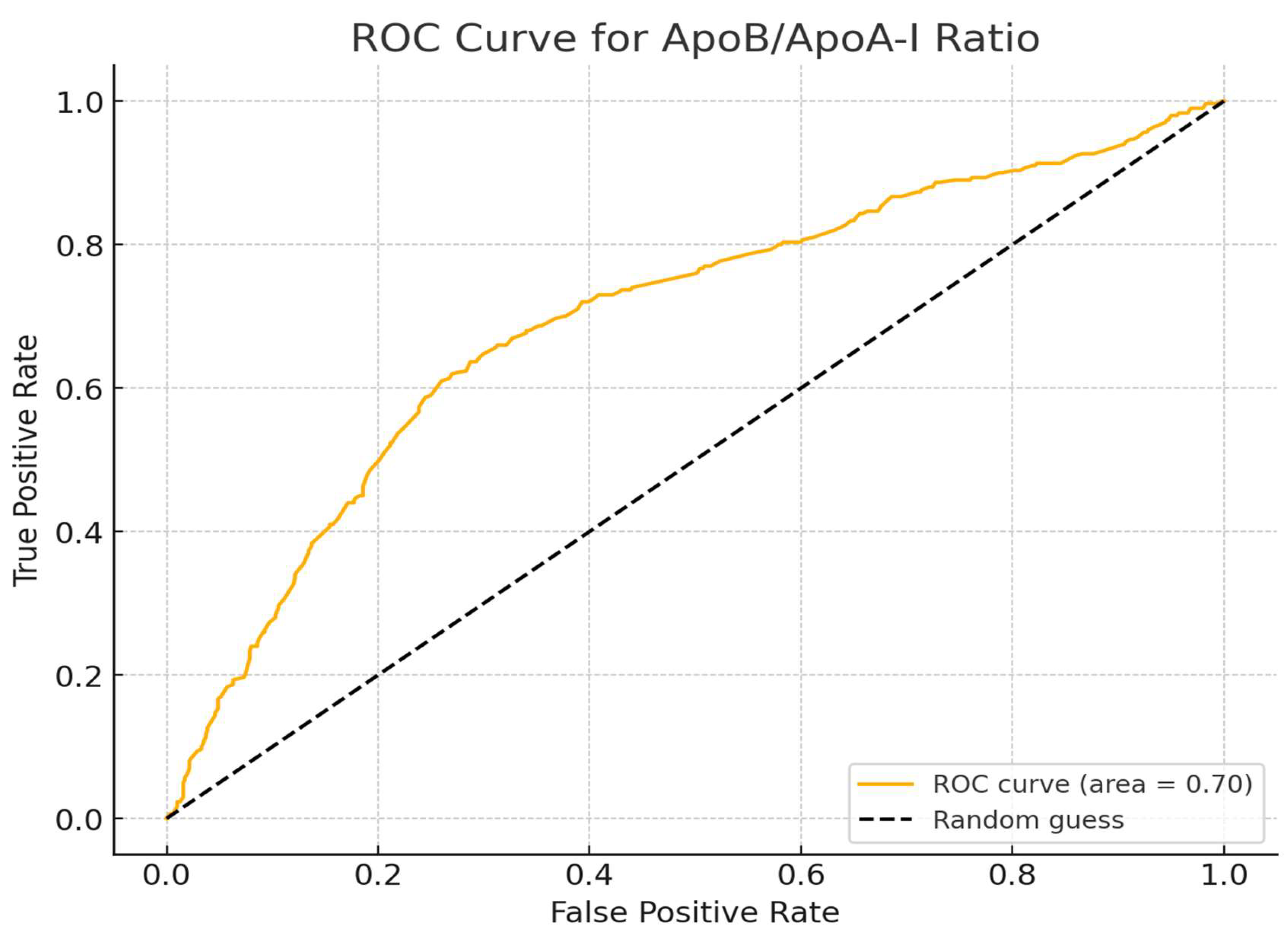
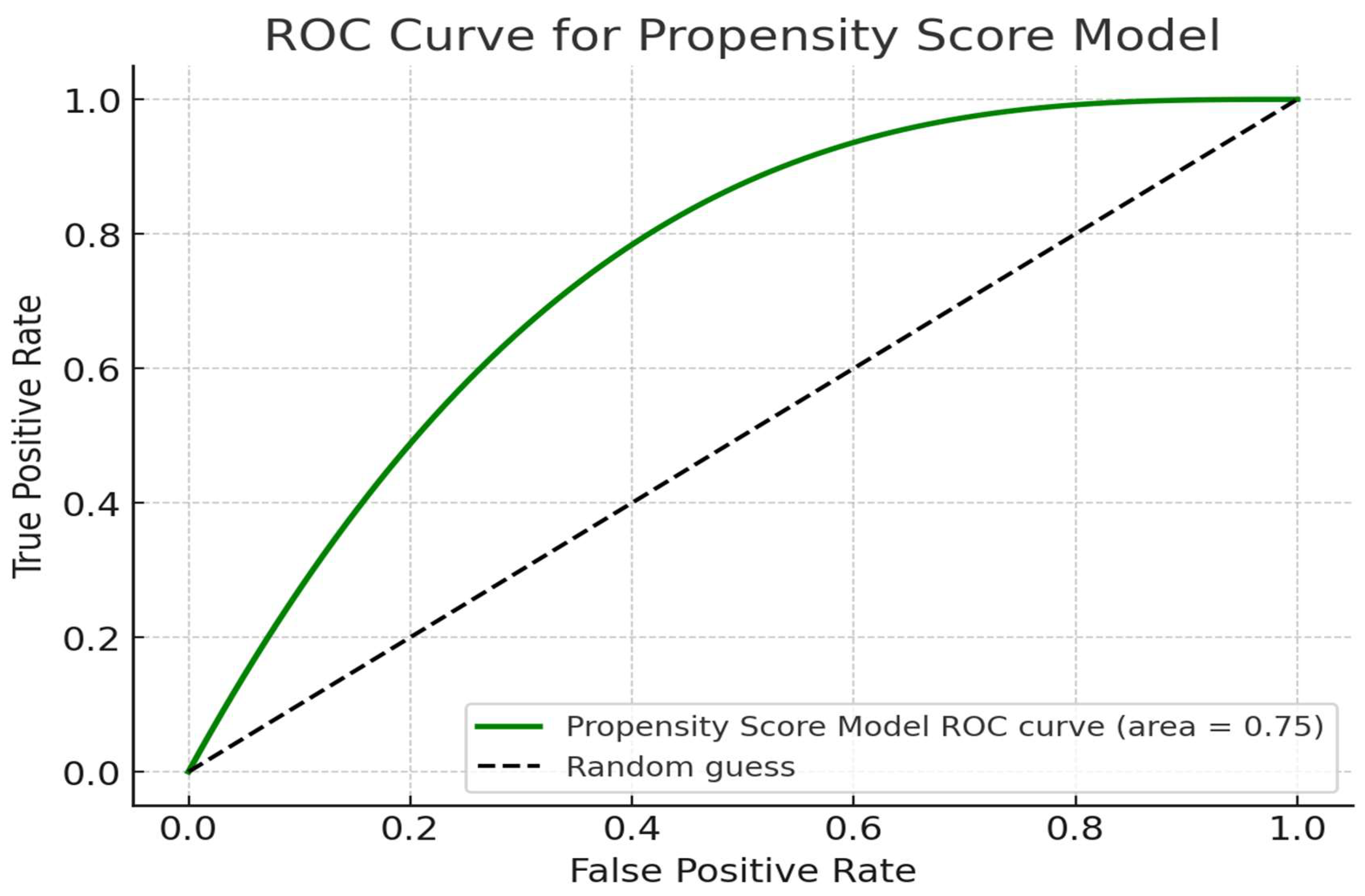
3.5. Analysis of ROC Curve for ApoA-I, ApoB, and ApoB/ApoA-I Ratio
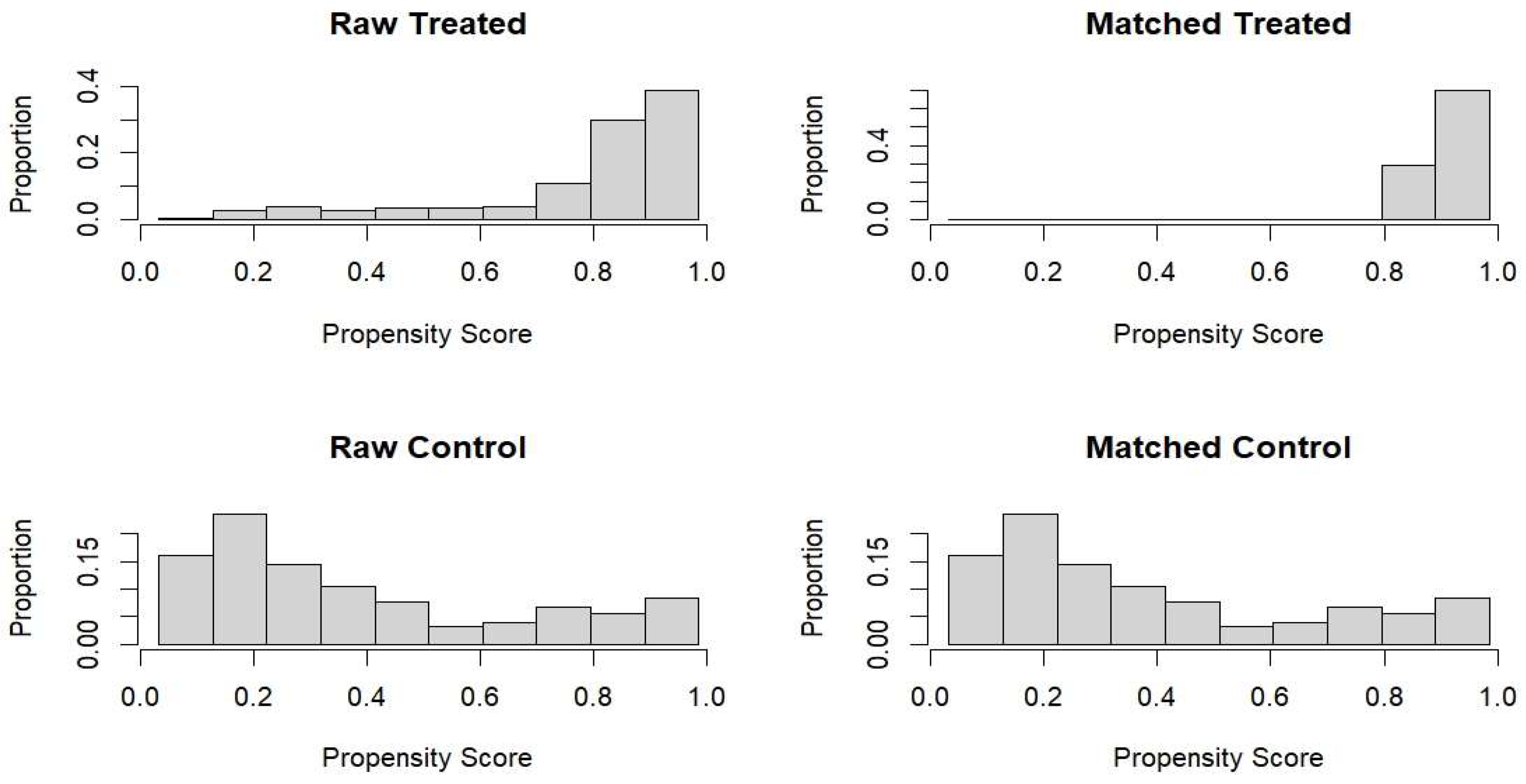
3.6. Effectiveness of Propensity Score Matching and Predictive Accuracy of the Model
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CAD | Coronary Artery Disease |
| LDL | Low-density lipoproteins |
| MI | Myocardial infarction |
| HDL | High-density lipoproteins |
| RIC | Rawalpindi Institute of Cardiology |
| NSTEMI | Non-ST-elevation myocardial infarction |
| PSM | Propensity score matching |
| AUC | Area under curve |
| ROC | Receiver operating characteristic |
| AMORIS | Apolipoprotein-related Mortality Risk |
References
- Adam, A. M.; Rehan, A.; Waseem, N.; Iqbal, U.; Saleem, H.; Godil, A. Prevalence of Conventional Risk Factors and Evaluation of Baseline Indices Among Young and Elderly Patients with Coronary Artery Disease. J. Clin. Diagn. Res. 2017, 11, 34–39. [Google Scholar] [CrossRef] [PubMed]
- Charla, E.; Mercer, J.; Maffia, P.; Nicklin, S. A. Extracellular vesicle signaling in atherosclerosis. Cell. Signal. 2020, 75, 109751. [Google Scholar] [CrossRef] [PubMed]
- Młynarska, E.; Czarnik, W.; Fularski, P.; Hajdys, J.; Majchrowicz, G.; Stabrawa, M.; Franczyk, B. From Atherosclerotic Plaque to Myocardial Infarction—The Leading Cause of Coronary Artery Occlusion. Int. J. Mol. Sci. 2024, 25, 7295. [Google Scholar] [CrossRef] [PubMed]
- Psaltopoulou, T.; Hatzis, G.; Papageorgiou, N.; Androulakis, E.; Briasoulis, A.; Tousoulis, D. Socioeconomic status and risk factors for cardiovascular disease: impact of dietary mediators. Hellenic J. Cardiol. 2017, 58, 32–42. [Google Scholar] [CrossRef]
- Velilla, T. A.; Guijarro, C.; Ruiz, R. C.; Piñero, M. R.; Marcos, J. V.; Pérez, A. P.; Soto, A. B. Consensus document for lipid profile determination and reporting in Spanish clinical laboratories. What parameters should a basic lipid profile include? Neurol. Perspect. 2023, 3, 100126. [Google Scholar] [CrossRef]
- Yaseen, R. I.; El-Leboudy, M. H.; El-Deeb, H. M. The relation between ApoB/ApoA-1 ratio and the severity of coronary artery disease in patients with acute coronary syndrome. Egypt. Heart J. 2021, 73, 1–9. [Google Scholar] [CrossRef]
- Aggarwal, J.; Kathariya, M. G.; Verma, P. K. LDL-C, NON-HDL-C and APO-B for cardiovascular risk assessment: looking for the ideal marker. Indian Heart J. 2021, 73, 544–548. [Google Scholar] [CrossRef] [PubMed]
- Walldius, G. The apoB/apoA-I ratio is a strong predictor of cardiovascular risk. In Lipoproteins in Health and Diseases; InTech: 2012, pp. 95–148.
- Behbodikhah, J.; Ahmed, S.; Elyasi, A.; Kasselman, L. J.; De Leon, J.; Glass, A. D.; Reiss, A. B. Apolipoprotein B and cardiovascular disease: biomarker and potential therapeutic target. Metabolites 2021, 11, 690. [Google Scholar] [CrossRef]
- Liting, P.; Guoping, L.; Zhenyue, C. Apolipoprotein B/apolipoprotein A1 ratio and non-high-density lipoprotein cholesterol. Herz 2015, 40, 1. [Google Scholar] [CrossRef]
- Welsh, C.; Celis-Morales, C. A.; Brown, R.; Mackay, D. F.; Lewsey, J.; Mark, P. B.; Welsh, P. Comparison of conventional lipoprotein tests and apolipoproteins in the prediction of cardiovascular disease: data from UK Biobank. Circulation 2019, 140, 542–552. [Google Scholar] [CrossRef]
- Mach, F.; Baigent, C.; Catapano, A. L.; Koskinas, K. C.; Casula, M.; Badimon, L.; Wiklund, O. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk. Eur. Heart J. 2020, 41, 111–188. [Google Scholar] [CrossRef]
- Ridker, P. M.; Rifai, N.; Cook, N. R.; Bradwin, G.; Buring, J. E. Non–HDL cholesterol, apolipoproteins AI and B100, standard lipid measures, lipid ratios, and CRP as risk factors for cardiovascular disease in women. JAMA 2005, 294, 326–333. [Google Scholar] [CrossRef] [PubMed]
- Writing Committee Members; Lawton, J. S.; Tamis-Holland, J. E.; Bangalore, S.; Bates, E. R.; Beckie, T. M.; Zwischenberger, B. A. 2021 ACC/AHA/SCAI guideline for coronary artery revascularization. J. Am. Coll. Cardiol. 2022, 79, e21–e129. [Google Scholar] [CrossRef]
- Tian, M.; Li, R.; Shan, Z.; Wang, D. W.; Jiang, J.; Cui, G. Comparison of Apolipoprotein B/A1 ratio, Framingham risk score and TC/HDL-c for predicting clinical outcomes in patients undergoing percutaneous coronary intervention. Lipids Health Dis. 2019, 18, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Ivert, T.; Malmström, H.; Hammar, N.; Carlsson, A. C.; Wändell, P. E.; Holzmann, M. J.; Walldius, G. Cardiovascular events in patients under age fifty with early findings of elevated lipid and glucose levels–The AMORIS study. PLoS ONE 2018, 13, e0201972. [Google Scholar] [CrossRef]
- Habib, H.; Haroon, Z. H.; Aamir, M.; Bibi, A.; Javed, H.; Jaffer, S. R. Association of Apolipoprotein B and Triglyceride Levels with Coronary Artery Disease. Pak. Armed Forces Med. J. 2022, 72, 1641–45. [Google Scholar] [CrossRef]
- Tamang, H. K.; Timilsina, U.; Singh, K. P.; Shrestha, S.; Raman, R. K.; Panta, P.; Dahal, C. Apo B/Apo AI ratio is statistically a better predictor of cardiovascular disease (CVD) than conventional lipid profile: a study from Kathmandu Valley, Nepal. J. Clin. Diagn. Res. 2014, 8, 34. [Google Scholar]
- Sniderman, A. D.; Islam, S.; Yusuf, S.; McQueen, M. J. Is the superiority of apoB over non–HDL-C as a marker of cardiovascular risk in the INTERHEART study due to confounding by related variables? J. Clin. Lipidol. 2013, 7, 626–631. [Google Scholar] [CrossRef] [PubMed]
- Tsimihodimos, V.; Gazi, I.; Kostara, C.; Tselepis, A. D.; Elisaf, M. Plasma lipoproteins and triacylglycerol are predictors of small, dense LDL particles. Lipids 2007, 42, 403–409. [Google Scholar] [CrossRef]
- Chien, K. L.; Hsu, H. C.; Su, T. C.; Chen, M. F.; Lee, Y. T.; Hu, F. B. Apolipoprotein B and non-high density lipoprotein cholesterol and the risk of coronary heart disease in Chinese. J. Lipid Res. 2007, 48, 2499–2505. [Google Scholar] [CrossRef] [PubMed]
- Landmesser, U.; McGinniss, J.; Steg, P. G.; Bhatt, D. L.; Bittner, V. A.; Diaz, R.; ODYSSEY OUTCOMES Investigators. Achievement of ESC/EAS LDL-C treatment goals after an acute coronary syndrome with statin and alirocumab. Eur. J. Prev. Cardiol. 2022, 29, 554–562. [Google Scholar] [CrossRef]
- Zuber, V.; Gill, D.; Ala-Korpela, M.; Langenberg, C.; Butterworth, A.; Bottolo, L.; Burgess, S. High-throughput multivariable Mendelian randomization analysis prioritizes apolipoprotein B as key lipid risk factor for coronary artery disease. Int. J. Epidemiol. 2021, 50, 893–901. [Google Scholar] [CrossRef]
| Parameter | Control (Mean ± SD) |
Training Cohort (Mean ± SD) | p-value | |
|---|---|---|---|---|
| Baseline Characteristics | ||||
| Age (years) | 51.25 ± 13.0 | 55.48 ± 10.4 | < 0.001 | |
| BMI (kg/m²) | 23.98 ± 3.4 | 25.46 ± 4.1 | 0.005 | |
| Smoker (%) | 24% | 82.20% | < 0.001 | |
| Exercise (%) | 18% | 20% | 0.03 | |
| Diabetes (%) | 30% | 61.30% | 0.001 | |
| Family History (%) | 44% | 60.89% | 0.001 | |
| Biochemical parameters | ||||
| ApoA-I (g/L) | 1.12 ± 0.34 | 0.95 ± 0.33 | 0.045 | |
| ApoB (g/L) | 1.0 ± 0.40 | 1.32 ± 0.54 | < 0.001 | |
| ApoB/A-I Ratio | 1.06 ± 0.95 | 1.76 ± 0.97 | < 0.001 | |
| Cholesterol (mg/dL) | 148.16 ± 48.6 | 183.69 ± 57.81 | 0.04 | |
| Triglycerides (mg/dL) | 167.34 ± 80.9 | 199.19 ± 97.94 | 0.03 | |
| HDL (mg/dL) | 36.04 ± 7.08 | 33.16 ± 8.21 | 0.001 | |
| LDL (mg/dL) | 94.78 ± 27.94 | 116.26 ± 38.87 | 0.001 | |
| Chol/HDL Ratio | 4.27 ± 1.50 | 5.79 ± 2.27 | 0.001 | |
| TG/HDL Ratio | 4.8 ± 2.46 | 6.36 ± 3.96 | 0.002 | |
| LDL/HDL Ratio | 2.72 ± 0.93 | 3.66 ± 1.52 | 0.002 | |
| Glucose (mg/dL) | 127.8 ± 60.2 | 150.74 ± 72.46 | 0.001 | |
| T.Bilirubin (mg/dL) | 0.59 ± 0.32 | 0.66 ± 0.43 | 0.040 | |
| ALT (U/L) | 37.05 ± 21.9 | 69.89 ± 128.31 | 0.03 | |
| ALP (U/L) | 91.18 ± 27.4 | 98.56 ± 43.34 | 0.04 | |
| Parameter | Control Cohort (Mean ± SD) | Validation Cohort (Mean ± SD) | p-value | |
|---|---|---|---|---|
| Baseline Characteristics | ||||
| Age (years) | 51.25 ± 13.0 | 53.75 (12.64) | 0.143 | |
| BMI (kg/m²) | 23.98 ± 3.4 | 26.14 (4.33) | 0.000 | |
| Smoker (%) | 24% | 60.00% | 0.000 | |
| Exercise (%) | 18% | 10% | 0.101 | |
| Diabetes (%) | 30% | 54.67% | 0.000 | |
| Family History (%) | 44% | 64.29% | 0.002 | |
| CAD Type | (DVCAD: 38.33, TVCAD: 33.33, SVCAD: 28.33] | 0.00% | N/A | |
| Biochemical parameters | ||||
| ApoA-I (g/L) | 1.12 ± 0.34 | 0.88 (0.32) | 0.000 | |
| ApoB (g/L) | 1.0 ± 0.40 | 1.44 (0.55) | 0.000 | |
| ApoB/A-I Ratio | 1.06 ± 0.95 | 2.06 (1.76) | 0.000 | |
| Cholesterol (mg/dL) | 148.16 ± 48.6 | 192.25 (62.25) | 0.000 | |
| Triglycerides (mg/dL) | 167.34 ± 80.9 | 206.51 (103.98) | 0.002 | |
| HDL (mg/dL) | 36.04 ± 7.08 | 32.65 (6.53) | 0.000 | |
| LDL (mg/dL) | 94.78 ± 27.94 | 125.30 (46.43) | 0.000 | |
| Chol/HDL Ratio | 4.27 ± 1.50 | 6.15 (2.60) | 0.000 | |
| TG/HDL Ratio | 4.8 ± 2.46 | 6.69 (4.31) | 0.000 | |
| LDL/HDL Ratio | 2.72 ± 0.93 | 4.02 (1.94) | 0.000 | |
| Glucose (mg/dL) | 127.8 ± 60.2 | 151.34 (80.90) | 0.015 | |
| T.Bilirubin (mg/dL) | 0.59 ± 0.32 | 0.69 (0.46) | 0.06 | |
| ALT (U/L) | 37.05 ± 21.9 | 77.46 (170.30) | 0.014 | |
| ALP (U/L) | 91.18 ± 27.4 | 98.49 (57.87) | 0.224 | |
| Variables | OR | 95% CI (Lower - Upper) |
Std. Error | T value | p-value |
|---|---|---|---|---|---|
| APO-A | 0.19 | 0.13 - 0.27 | 0.19 | -7.48 | 7.40E-14 |
| APO-B | 3.1 | 2.47 - 3.88 | 0.14 | 8.01 | 1.13E-15 |
| APOB/APO A | 1.65 | 1.35 - 2.02 | 0.10 | 3.74 | 0.000198 |
| Cholesterol | 0.99 | 0.98 - 1.00 | 0.00 | -2.70 | 0.00691 |
| Triglycerides | 1 | 0.98 - 1.01 | 0.00 | -0.98 | 0.32659 |
| LDL | 1.01 | 1.00 - 1.02 | 0.00 | 1.93 | 0.05403 |
| LDL/HDL | 1.56 | 1.42 - 1.70 | 0.05 | 8.10 | 5.52E-16 |
| GLUCOSE | 1 | 0.98 - 1.01 | 0.00 | 0.18 | 0.8597 |
| ALT | 1.00 | 1.0 - 1.01 | 0.00 | 2.88 | 0.00402 |
| Variables | OR | 95% CI (Lower - Upper) |
Std. Error | T value | p-value |
|---|---|---|---|---|---|
| APO-A | 0.25 | 0.12 - 0.52 | 0.31 | -4.43 | 9.58E-06 |
| APO-B | 2.94 | 2.34 - 3.7 | 0.23 | 4.75 | 1.99E-06 |
| APOB/APO A | 0.86 | 0.74 - 1.02 | 0.10 | -1.85 | 0.06376 |
| Cholesterol | 0.99 | 0.98 - 1.0 | 0.00 | -2.70 | 0.00691 |
| Triglycerides | 1.00 | 0.98 - 1.0 | 0.00 | -0.98 | 0.32659 |
| LDL | 1.01 | 1 - 1.03 | 0.00 | 1.93 | 0.05403 |
| LDL/HDL | 1.36 | 1.18 - 1.57 | 0.09 | 3.27 | 0.00108 |
| GLUCOSE | 1.0 | 0.98 - 1.01 | 0.00 | 0.18 | 0.8597 |
| ALT | 1.0 | 1 - 1.01 | 0.00 | 2.88 | 0.00402 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




