Submitted:
22 January 2025
Posted:
23 January 2025
You are already at the latest version
Abstract
Keywords:
1. Racial Discrimination as a Traumatic Bedrock of Healthcare Avoidance: A Pathway Through Healthcare Institutional Betrayal and Mistrust
1.1. Anticipated Healthcare Avoidance as an Outcome to Prevent
1.2. The BITTEN Model
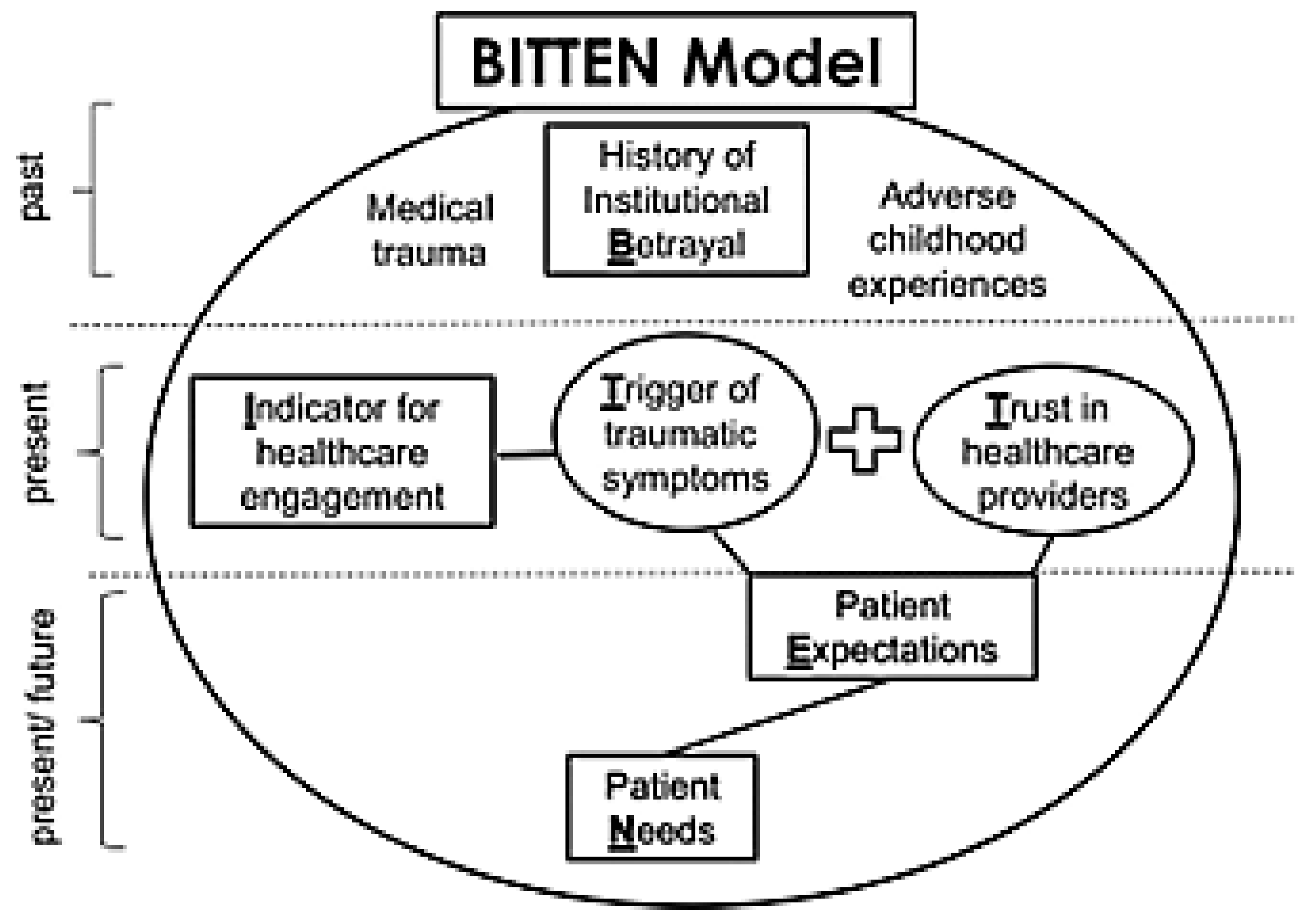
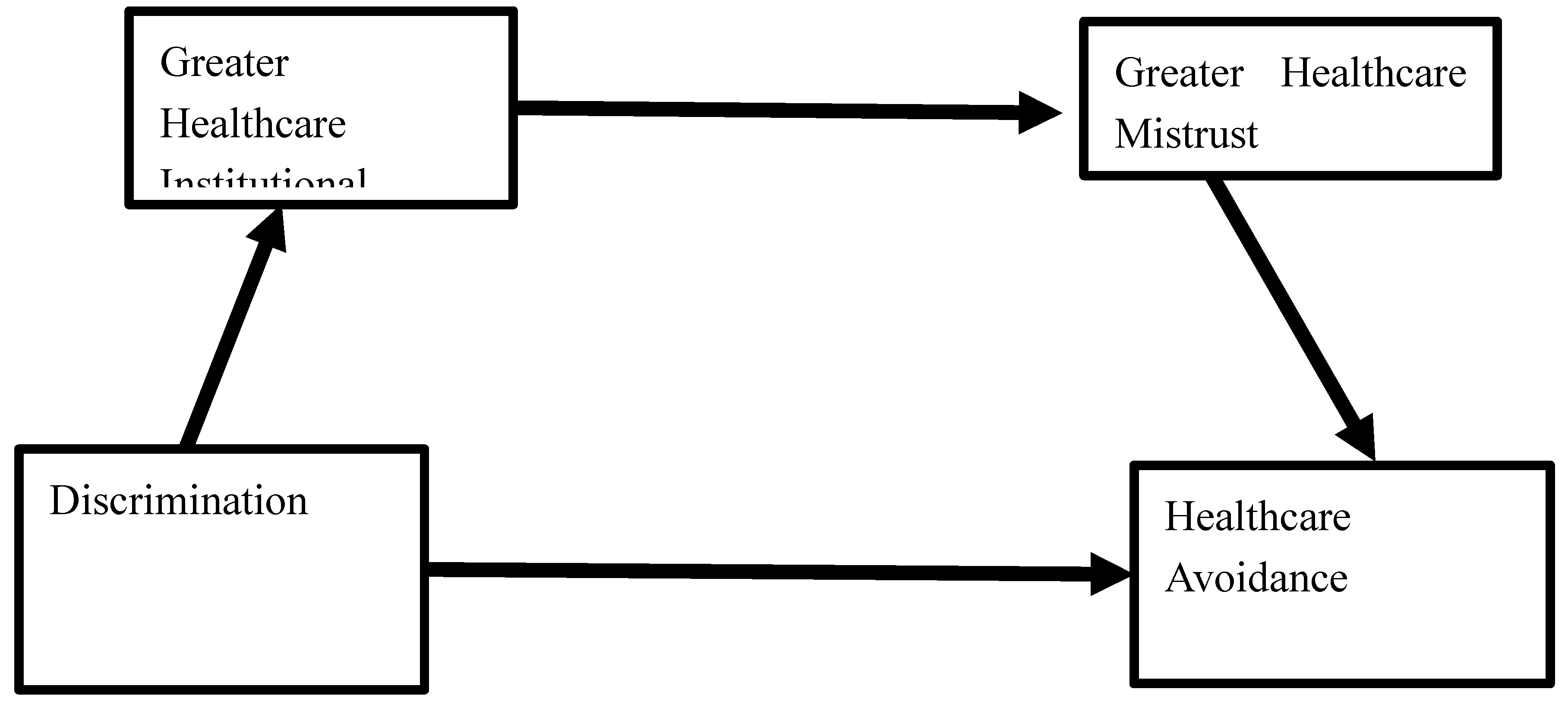
1.3. Healthcare Institutional Betrayal (HIB) as a Mediator
1.4. Reduced Trust as a Mediator
2. Methods
3. Measures
3.1. Demographics
3.2. Racial Discrimination in the Healthcare Setting
3.3. Worst Healthcare Experience
3.4. Healthcare Institutional Betrayal
3.5. Mistrust in the Healthcare System
3.6. Anticipated Healthcare Avoidance (HAV)
4. Preliminary Analyses
5. Primary Analyses
6. Results
6.1. Associations Among the Racial Discrimination, HIB, Healthcare Mistrust, and Anticipated Healthcare Avoidance
6.2. Testing the BITTEN Model to Predicting Anticipated Healthcare Avoidance
7. Discussion
References
- Adams-Clark, A. A., Barnes, M. L., Lind, M. N., Smidt, A., & Freyd, J. J. (2024). Institutional courage attenuates the association between institutional betrayal and trauma symptoms among campus sexual assault survivors. Psychological Trauma: Theory, Research, Practice and Policy. [CrossRef]
- American Psychiatric Association. (2022). Trauma-and Stressor-Related Disorders. In Diagnostic and statistical manual of mental disorders (5th ed., text rev.) . [CrossRef]
- Agarwal, A. K., Gonzales, R. E., Sagan, C., Nijim, S., Asch, D. A., Merchant, R. M., & South, E. C. (2024). Perspectives of Black patients on racism within emergency care. JAMA Health Forum, 5(3), e240046. [CrossRef]
- Alhusen, J. L., Bower, K. M., Epstein, E., & Sharps, P. (2016). Racial discrimination and adverse birth outcomes: An integrative review. Journal of Midwifery & Women’s Health, 61(6), 707–720. [CrossRef]
- Benner, A. D., Wang, Y., Shen, Y., Boyle, A. E., Polk, R., & Cheng, Y.-P. (2018). Racial/ethnic discrimination and well-being during adolescence: A meta-analytic review. The American Psychologist, 73(7), 855–883. [CrossRef]
- Bergeron, G., Lundy De La Cruz, N., Gould, L. H., Liu, S. Y., & Levanon Seligson, A. (2020). Association between racial discrimination and health-related quality of life and the impact of social relationships. Quality of Life Research: An International Journal of Quality of Life Aspects of Treatment, Care and Rehabilitation, 29(10), 2793–2805. [CrossRef]
- Birrell, P. J., & Freyd, J. J. (2008). Betrayal trauma: Relational models of harm and healing. Journal of Trauma Practice, 5(1), 49–63. [CrossRef]
- Campbell, R. (2024). Systems-centered care versus survivor-centered care: Reimagining help and healing for sexual assault survivors. Psychology of Violence, 14(6), 379-385. [CrossRef]
- Carter, S. E., Ong, M. L., Simons, R. L., Gibbons, F. X., Lei, M. K., & Beach, S. R. H. (2019). The effect of early discrimination on accelerated aging among African Americans. Health Psychology: Official Journal of the Division of Health Psychology, American Psychological Association, 38(11), 1010–1013. [CrossRef]
- Cave, L., Cooper, M. N., Zubrick, S. R., & Shepherd, C. C. J. (2020). Racial discrimination and child and adolescent health in longitudinal studies: A systematic review. Social Science & Medicine (1982), 250, 112864. [CrossRef]
- Cénat, J. M. (2023). Complex racial trauma: Evidence, theory, assessment, and treatment. Perspectives on Psychological Science: A Journal of the Association for Psychological Science, 18(3), 675–687. [CrossRef]
- Cipollina, R., & Sanchez, D. T. (2023). Racial identity safety cues and healthcare provider expectations. Stigma and Health, 8(2), 159–169. [CrossRef]
- D’Anna, L. H., Hansen, M., Mull, B., Canjura, C., Lee, E., & Sumstine, S. (2018). Social discrimination and health care: A multidimensional framework of experiences among a low-income multiethnic sample. Social Work in Public Health, 33(3), 187–201. [CrossRef]
- Doshi, R. P., Aseltine, R. H., Sabina, A. B., & Graham, G. N. (2017). Racial and ethnic disparities in preventable hospitalizations for chronic disease: Prevalence and risk factors. Journal of Racial and Ethnic Health Disparities, 4(6), 1100–1106. [CrossRef]
- Flanagin, A., Frey, T., Christiansen, S. L., & AMA Manual of Style Committee. (2021). Updated guidance on the reporting of race and ethnicity in medical and science journals. JAMA, 326(7), 621–627. [CrossRef]
- Freyd, J. J., & Smidt, A. M. (2019). So you want to address sexual harassment and assault in your organization? Training is not enough; Education is necessary. Journal of Trauma & Dissociation, 20(5), 489–494. [CrossRef]
- Gómez, J. M. (2022). Gender, campus sexual violence, cultural betrayal, institutional betrayal, and institutional support in US ethnic minority college students: A descriptive study. Violence Against Women, 28(1), 93-106. [CrossRef]
- Hackett, R. A., Ronaldson, A., Bhui, K., Steptoe, A., & Jackson, S. E. (2020). Racial discrimination and health: A prospective study of ethnic minorities in the United Kingdom. BMC Public Health, 20(1), 1652. [CrossRef]
- Hall, O. T., Jordan, A., Teater, J., Dixon-Shambley, K., McKiever, M. E., Baek, M., Garcia, S., Rood, K. M., & Fielin, D. A. (2022). Experiences of racial discrimination in the medical setting and associations with medical mistrust and expectations of care among Black patients seeking addiction treatment. Journal of Substance Abuse Treatment, 133, 108551. [CrossRef]
- Hausmann, L. R., Kressin, N. R., Hanusa, B. H., & Ibrahim, S. A. (2010). Perceived racial discrimination in health care and its association with patients’ healthcare experiences. Ethnicity & disease, 20(1), 40-47. https://www.jstor.org/stable/48668251.
- Holder-Dixon, A. R., Adams, O. R., Cobb, T. L., Goldberg, A. J., Fikslin, R. A., Reinka, M. A., Gesselman, A. N., & Price, D. M. (2022). Medical avoidance among marginalized groups: The impact of the COVID-19 pandemic. Journal of Behavioral Medicine, 45(5), 760–770. [CrossRef]
- Kannan, V. D., & Veazie, P. J. (2014). Predictors of avoiding medical care and reasons for avoidance behavior. Medical Care, 52(4), 336–345. [CrossRef]
- Kcomt, L., Gorey, K. M., Barrett, B. J., & McCabe, S. E. (2020). Healthcare avoidance due to anticipated discrimination among transgender people: A call to create trans-affirmative environments. SSM - Population Health, 11, 100608. [CrossRef]
- Kirkinis, K., Pieterse, A. L., Martin, C., Agiliga, A., & Brownell, A. (2021). Racism, racial discrimination, and trauma: A systematic review of the social science literature. Ethnicity & Health, 26(3), 392–412. [CrossRef]
- Kondrath, S. R., Brandt, E. A. B., Campbell, K., Chamberlin, E. S., Dordal, P., East, R., Fantus, S., Frankfurt, S. B., Golden, K. B., Griffin, B. J., Harris, J. I., Hiltner, R. K., Holman, C. S., McGuire, A., & Usset, T. J. (2024). Moral injury and institutional betrayal among cis women and sexual and gender minorities. Current Treatment Options in Psychiatry, 11(4), 265–278. [CrossRef]
- McGuigan, R. D., & Wilkinson, J. M. (2015). Obesity and healthcare avoidance: A systematic review. AIMS Public Health, 2(1), 56. [CrossRef]
- Mohottige, D., Davenport, C. A., Bhavsar, N., Schappe, T., Lyn, M. J., Maxson, P., Johnson, F., Planey, A. M., McElroy, L. M., Wang, V., Cabacungan, A. N., Ephraim, P., Lantos, P., Peskoe, S., Lunyera, J., Bentley-Edwards, K., Diamantidis, C. J., Reich, B., & Boulware, L. E. (2023). Residential structural racism and prevalence of chronic health conditions. JAMA Network Open, 6(12), e2348914. [CrossRef]
- Pellowski, J. A., Price, D. M., Allen, A. M., Eaton, L. A., & Kalichman, S. C. (2017). The differences between medical trust and mistrust and their respective influences on medication beliefs and ART adherence among African Americans living with HIV. Psychology & Health, 32(9), 1127–1139. [CrossRef]
- Porter, E. F., Mendoza, M. P., Deng, M., Horwitz, S. D., Soltys, M. A., & Hattery, A. J. (2024). Institutional betrayal and race in the civil legal system: A latent class analysis with survivors of intimate partner violence. Race and Justice, 1-24. [CrossRef]
- Rastegar, P. J., & Langhinrichsen-Rohling, J. (2024). Understanding college students’ healthcare avoidance: From early maladaptive schemas, through healthcare institutional betrayal and betrayal trauma appraisal of worst healthcare experiences. Healthcare, 12(11), 1126. [CrossRef]
- Richie, F. J. (2023). Repair Following Healthcare Institutional Betrayal (Doctoral dissertation, The University of North Carolina at Charlotte).
- Schwei, R. J., Johnson, T., Matthews, A. K., & Jacobs, E. A. (2017). Perceptions of negative health care experiences and self-reported health behavior change in three racial and ethnic groups. Ethnicity & Health, 22(2), 156–168. [CrossRef]
- Selwyn, C. N., Lathan, E. C., Richie, F., Gigler, M. E., & Langhinrichsen-Rohling, J. (2021). Bitten by the system that cared for them: Towards a trauma-informed understanding of patients’ healthcare engagement. Journal of Trauma & Dissociation, 22(5), 636-652. [CrossRef]
- Simon, K. A., Driver, R., Rathus, T., Cole, A., Kalinowski, J., Watson, R. J., & Eaton, L. A. (2024). HIV information avoidance, HIV stigma, and medical mistrust among Black sexual minority men in the Southern United States: Associations with HIV testing. AIDS and Behavior, 28(1), 12–18. [CrossRef]
- Slaughter-Acey, J. C., Sneed, D., Parker, L., Keith, V. M., Lee, N. L., & Misra, D. P. (2019). Skin tone matters: Racial microaggressions and delayed prenatal care. American Journal of Preventive Medicine, 57(3), 321–329. [CrossRef]
- Smith, C. P., & Freyd, J. J. (2013). Dangerous safe havens: Institutional betrayal exacerbates sexual trauma. Journal of Traumatic Stress, 26(1), 119–124. [CrossRef]
- Smith, K. T., Monti, D., Mir, N., Peters, E., Tipirneni, R., & Politi, M. C. (2018). Access is necessary but not sufficient: Factors influencing delay and avoidance of health care services. MDM Policy & Practice, 3(1), 2381468318760298. [CrossRef]
- Spleen, A. M., Lengerich, E. J., Camacho, F. T., & Vanderpool, R. C. (2014). Health care avoidance among rural populations: Results from a nationally representative survey. The Journal of Rural Health, 30(1), 79–88. [CrossRef]
- Tamaian, A., Anstey, H., Kokokyi, S., & Klest, B. (2024). The impact of discrimination and institutional Betrayal on Canadian University Students’ Mental Health. Journal of Trauma & Dissociation, 25(2), 185-201. [CrossRef]
- Tamaian, A., & Klest, B. (2017). Institutional betrayal in the Canadian medical system: Reliability and validity of a self-report questionnaire. Journal of Aggression, Maltreatment & Trauma, 27(7), 703–719. [CrossRef]
- Thomas, M. D., Michaels, E. K., Reeves, A. N., Okoye, U., Price, M. M., Hasson, R. E., Chae, D. H., & Allen, A. M. (2019). Differential associations between everyday versus institution-specific racial discrimination, self-reported health, and allostatic load among Black women: Implications for clinical assessment and epidemiologic studies. Annals of Epidemiology, 35, 20-28.e3. [CrossRef]
- Villarose, L. (2022). Under the skin: The hidden toll of racism on American lives and on the health of our nation. New York: Doubleday. ISBN: 9780385544887.
- Wang, J. C., Dalke, K. B., Nachnani, R., Baratz, A. B., & Flatt, J. D. (2023). Medical mistrust mediates the relationship between nonconsensual intersex surgery and healthcare avoidance among intersex adults. Annals of Behavioral Medicine, 57(12), 1024–1031. [CrossRef]
- Williams, D. R., Yu, Y., Jackson, J. S., & Anderson, N. B. (1997). Racial differences in physical and mental health: Socio-economic status, stress, and discrimination. Journal of health psychology, 2(3), 335-351. [CrossRef]
- Yearby, R. (2018). Racial disparities in health status and access to healthcare: The continuation of inequality in the United States due to structural racism. The American Journal of Economics and Sociology, 77(3–4), 1113–1152. [CrossRef]
- Zhang, D., Li, G., Shi, L., Martin, E., Chen, Z., Li, J., Chen, L., Li, Y., Wen, M., Chen, B., Li, H., Su, D., & Han, X. (2022). Association between racial discrimination and delayed or forgone care amid the COVID-19 pandemic. Preventive Medicine, 162, 107153. [CrossRef]
| N | % | |
|---|---|---|
| 472 | ||
| Race* | ||
| White | 84 | 17.8 |
| Black/AA/Afro-Caribbean | 173 | 36.7 |
| East Asian | 50 | 10.6 |
| South Asian | 64 | 13.6 |
| American Indian/Alaskan Native | 12 | 2.5 |
| Native Hawaiian/Pacific Islander | 6 | 1.3 |
| Middle Eastern/Arab/N. African | 25 | 5.3 |
| Multiracial | 64 | 13.6 |
| Identity Not listed (Other) | 46 | 9.7 |
| Prefer not to answer | 18 | 3.8 |
| Ethnicity | ||
| Hispanic/Latino | 139 | 29.4 |
| Not Hispanic/Latino | 322 | 68.2 |
| Prefer not to answer | 11 | 2.3 |
| Gender Identity | ||
| Woman | 308 | 65.3 |
| Man | 145 | 30.7 |
| Gender Minority | 16 | 3.4 |
| Prefer not to say | 3 | 0.6 |
| Sexual Orientation | ||
| Straight/Heterosexual | 352 | 74.6 |
| Sexual Minority | 108 | 22.9 |
| Prefer not to answer | 12 | 2.5 |
| Year in College | ||
| Freshmen | 212 | 44.9 |
| Sophomore | 153 | 32.4 |
| Junior | 70 | 14.8 |
| Senior | 34 | 7.2 |
| Graduate Student | 1 | 0.2 |
| Other | 2 | 0.4 |
| N | Min-Max | M (SD) | |
|---|---|---|---|
| Racial Discrimination in Healthcare | 462 | 1.0 - 12.0 | 4.20 (2.18) |
| Healthcare Institutional Betrayal (HIB) | 458 | 0.0 - 12.0 | 2.94 (2.90) |
| Healthcare Mistrust Appraisal | 469 | 6.0 - 51.0 | 31.63 (9.40) |
| Anticipated Healthcare Avoidance | 463 | 2.0 - 15.0 | 7.56 (3.21) |
| Age in years | 455 | 18.0 - 62.0 | 19.74 (3.96) |
| 1 | 2 | 3 | 4 | 5 | ||
|---|---|---|---|---|---|---|
| 1. | Healthcare Avoidance | |||||
| 2. | Racial Discrimination | 0.32*** | - | |||
| 3. | Healthcare Inst. Betrayal | 0.48*** | 0.40*** | - | ||
| 4. | Healthcare Mistrust | 0.45*** | 0.33*** | 0.58*** | - | |
| 5. | Sexual Minority Status | 0.13** | 0.09 | 0.18*** | 0.21*** | - |
| Step 1 | Step 2 | Final Model | |||||||
|---|---|---|---|---|---|---|---|---|---|
| M1 (HIB) | M2 (Mistrust) | Y(HAV) | |||||||
| Antecedent | b | SE | p | b | SE | p | b | SE | p |
| X (Discrimination) | .53 | .06 | .00 | .58 | .19 | .00 | .17 | .07 | .01 |
| M1 (HIB) | ? | ? | ? | 1.69 | 0.14 | .00 | .33 | .57 | .00 |
| M2 (Mistrust) | ? | ? | ? | ? | ? | ? | .08 | .02 | .00 |
| Men | -.06 | .28 | .83 | -1.46 | .82 | .75 | -.47 | .29 | .10 |
| Gender Minority | -1.48 | .81 | .07 | 1.19 | 2.35 | .61 | 2.19 | .82 | .01 |
| Sexual Minority | 1.15 | .32 | .00 | 1.85 | .93 | .05 | -.18 | .33 | .58 |
| Constant | .53 | .31 | .09 | 24.18 | .91 | .00 | 3.59 | .52 | .00 |
| R2 | R2 | R2 | |||||||
| .18 | .37 | .31 | |||||||
| F (4,432) = 23.96 p = .00 |
F (5,431) = 50.95 p = .00 |
F (6,430) = 32.04 p = .00 |
|||||||
| F (4,432) = 23.96 p = .00 |
F (5,431) = 50.95 p = .00 |
||||||||
| F (4,432) = 23.96 p = .00 |
F (5,431) = 50.95 p = .00 |
||||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




