Submitted:
13 January 2025
Posted:
14 January 2025
You are already at the latest version
Abstract
Keywords:
Introduction
Revolutionary Technologies in Implant Dentistry
Magnetic Resonance Imaging (MRI) in Dental Implant Assessment and Optical Coherence Tomography (OCT) for Soft Tissue Evaluation:
Advanced imaging modalities: 3D printing and cone beam CT:
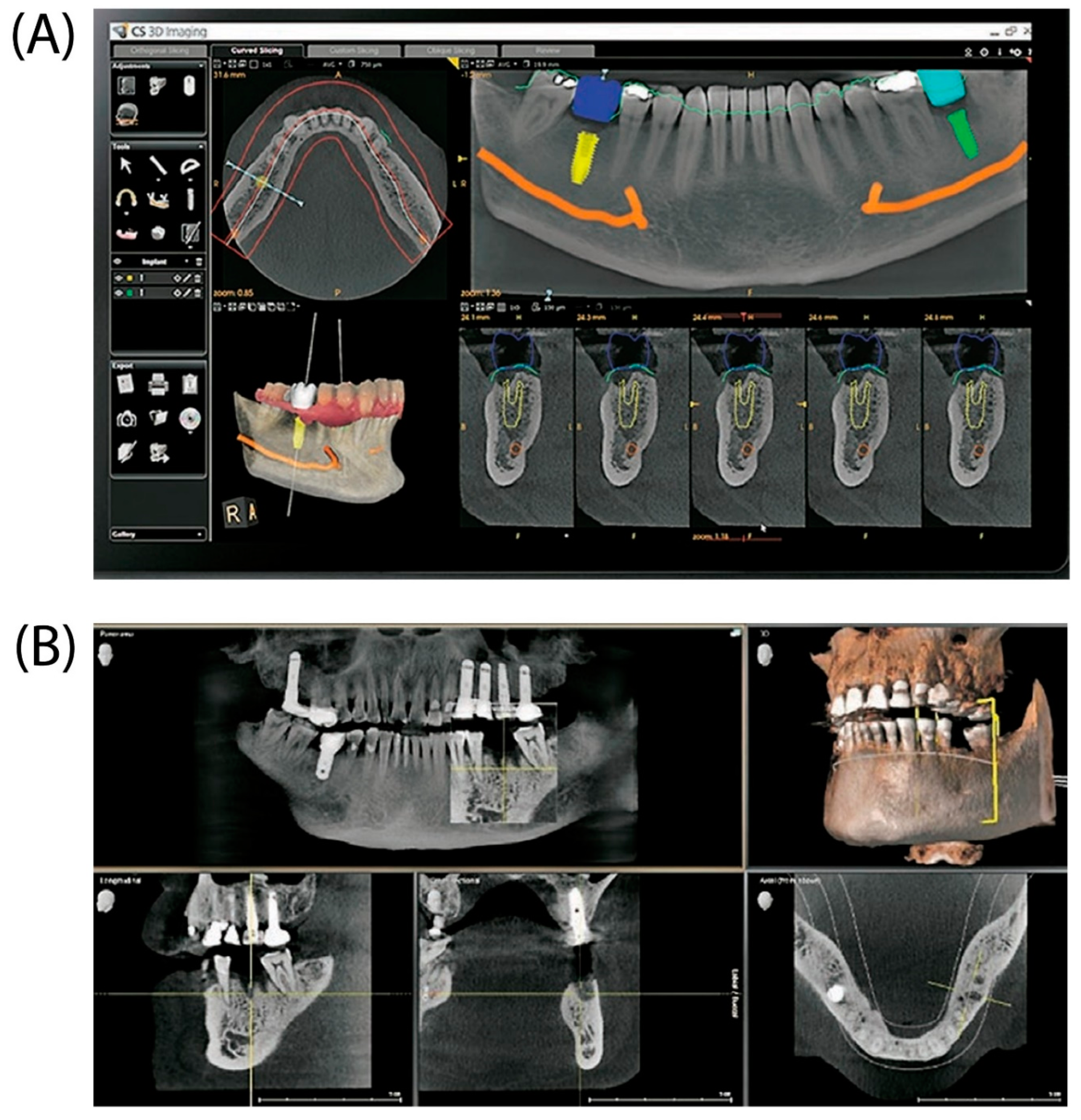
Biomimetic Approaches to Implant Design
Biomaterial Innovations in Implant Dentistry
Biocompatible Materials for Dental Implants:
Novel Coatings for Dental Implant Surfaces
Tissue Engineering Approaches in Implant Dentistry
Advanced Implant Materials and Surface Engineering
Nanomaterials for Enhanced Osseointegration:
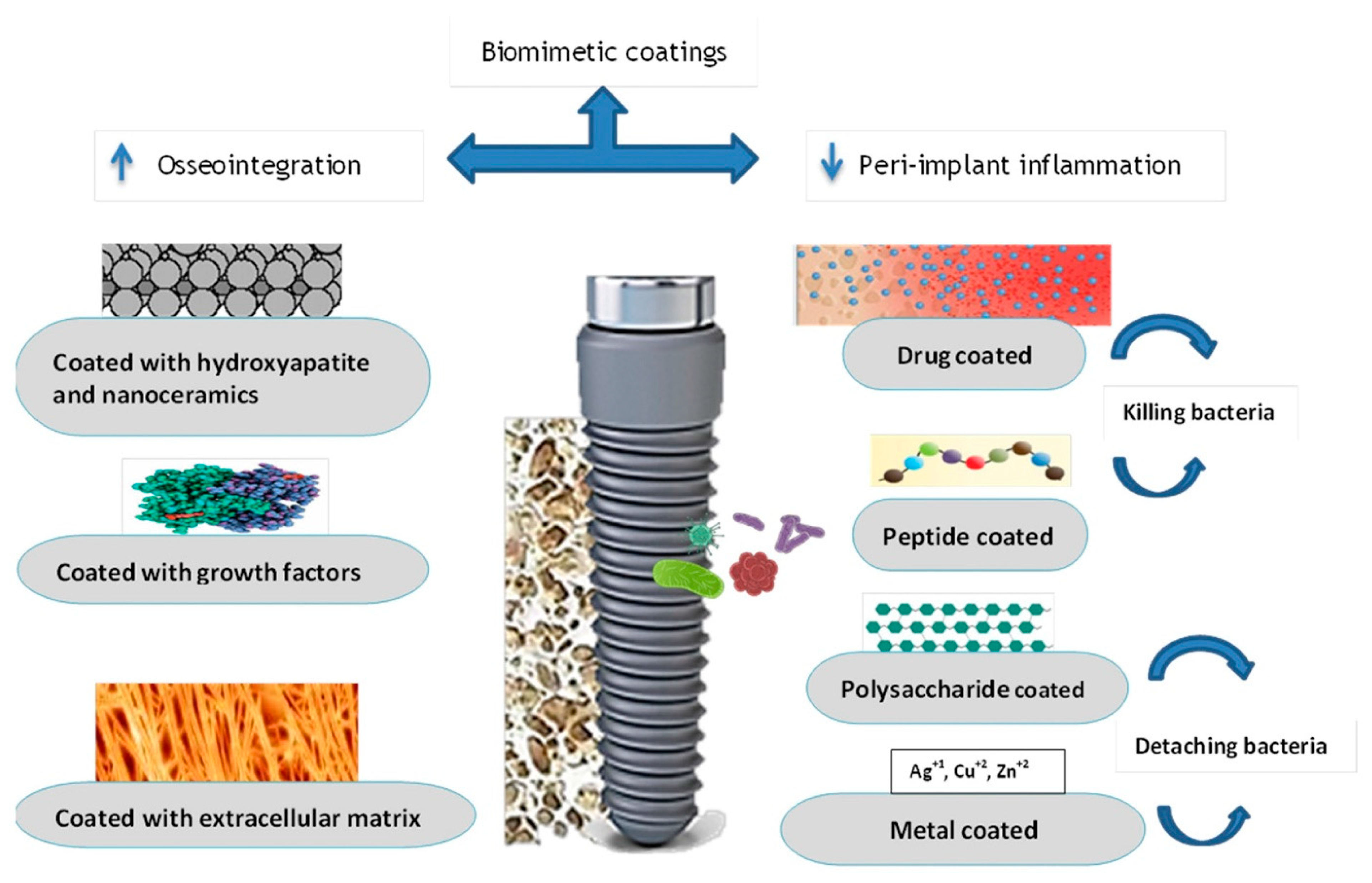
Bioactive Coatings and Surface Modifications
- Promotion of proper cell differentiation for new bone formation.
- They can be synthesized or manufactured without requiring extraction from allografts.
- It is resorbable in response to osteogenic activity.
- Prevent implant loss due to coating delamination.
- A lack of host immunological responses.
- The material remains chemically stable until implant insertion.
- Be cost-effective.
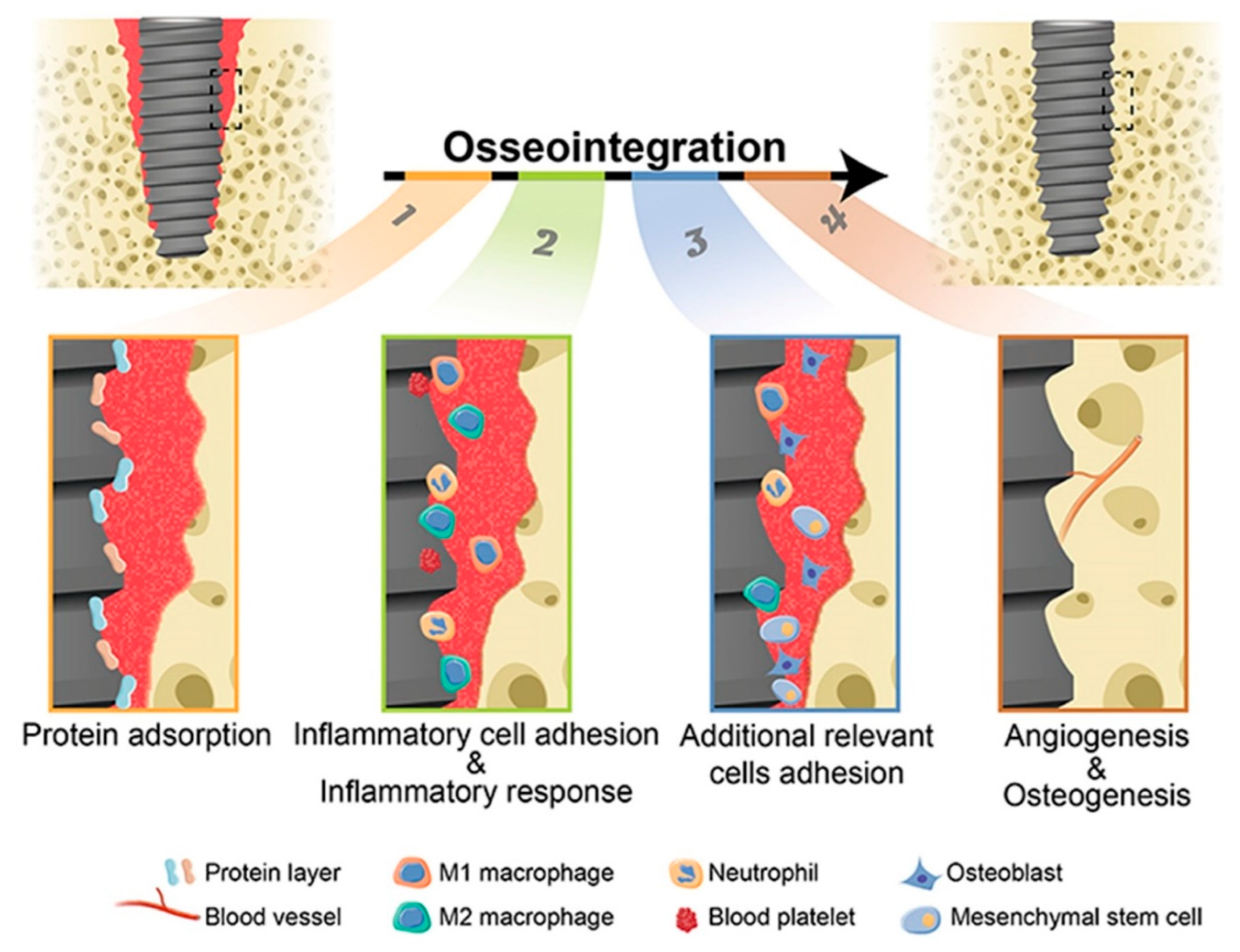
Coating to Improve Osseointegration
Biocompatible Alternatives: Zirconia and Polymer-based Implants:
Conclusion
List of Abbreviations
| Abbreviation | Full Form |
| ALP | Alkaline Phosphatase |
| BMP(s) | Bone Morphogenetic Protein(s) |
| BDWT | Bone Density Within the Threads |
| BIC | Bone-Implant Contact |
| BG | Bioactive Glass |
| BM-MSCs | Bone Marrow-Derived Mesenchymal Stem Cells |
| CBCT | Cone Beam Computed Tomography |
| CNDs | Carbon Nanodots |
| CNFs | Carbon Nanofibers |
| CNTs | Carbon Nanotubes |
| DICOM | Digital Imaging and Communications in Medicine |
| DPSCs | Dental Pulp Stem Cells |
| ECM | Extracellular Matrix |
| FGF | Fibroblast Growth Factor |
| GO | Graphene Oxide |
| HA | Hydroxyapatite |
| MRI | Magnetic Resonance Imaging |
| MSCs | Mesenchymal Stem Cells |
| ND | Nanocrystalline Diamond |
| OCT | Optical Coherence Tomography |
| PDGF | Platelet-Derived Growth Factor |
| PDLSCs | Periodontal Ligament Stem Cells |
| PEEK | Polyether-Ether-Ketone |
| PRF | Platelet-Rich Fibrin |
| PRP | Platelet-Rich Plasma |
| TGF-β | Transforming Growth Factor-Beta |
| TiO2 | Titanium Dioxide |
| VISA | Vancomycin-Intermediate Staphylococcus aureus |
| VEGF | Vascular Endothelial Growth Factor |
| Y-TZP | Yttria-Stabilized Tetragonal Zirconia Polycrystal |
References
- Alghamdi HS, Jansen JA. The development and future of dental implants. Dent Mater J. 2020 Mar 31;39(2):167-172. doi: 10.4012/dmj.2019-140. Epub 2020 Jan 22.PMID: 31969548.
- Alamoudi A. Nanoengineering and Surface Modifications of Dental Implants. Cureus. 2024 Jan 2;16(1):e51526. doi: 10.7759/cureus.51526. PMID: 38304686; PMCID: PMC10833059.
- Zhu, G., Wang, G., & Li, J. J. (2021). Advances in implant surface modifications to improve osseointegration. Materials Advances, 2(21), 6901-6927. [CrossRef]
- Zhang Y, Gulati K, Li Z, Di P, Liu Y. Dental Implant Nano-Engineering: Advances, Limitations and Future Directions. Nanomaterials (Basel). 2021 Sep 24;11(10):2489. doi: 10.3390/nano11102489. PMID: 34684930; PMCID: PMC8538755.
- Yeung, A. W. K., AlHadidi, A., Vyas, R., Bornstein, M. M., Watanabe, H., & Tanaka, R. (2024). Nonionizing diagnostic imaging modalities for visualizing health and pathology of periodontal and peri-implant tissues. Periodontology 2000, 95(1), 87–101. [CrossRef]
- Spagnuolo, G., & Soltani, P. (2024). Magnetic Resonance Imaging in Digital Dentistry: The Start of a New Era. Prosthesis, 6(4), 798–802. [CrossRef]
- Putra, R. H., Yoda, N., Astuti, E. R., & Sasaki, K. (2021). Potential Imaging Capability of Optical Coherence Tomography as Dental Optical Probe: A Mini-Review. Applied Sciences, 11(22), 11025. [CrossRef]
- Ali, S., Gilani, S. B. S., Shabbir, J., Almulhim, K. S., Bugshan, A., & Farooq, I. (2021). Optical coherence tomography’s current clinical medical and dental applications: a review. F1000Research, 10, 310. [CrossRef]
- Janjua, O. S., Jeelani, W., Khan, M. I., Qureshi, S. M., Shaikh, M. S., Zafar, M. S., & Khurshid, Z. (2023c). Use of Optical Coherence Tomography in Dentistry. International Journal of Dentistry, 2023, 1–10. [CrossRef]
- Saini, R. S., Bavabeedu, S. S., Quadri, S. A., Gurumurthy, V., Kanji, M. A., Kuruniyan, M. S., Binduhayyim, R. I. H., Avetisyan, A., & Heboyan, A. (2024). Impact of 3D imaging techniques and virtual patients on the accuracy of planning and surgical placement of dental implants: A systematic review. Digital Health, 10. [CrossRef]
- Jurić, B., & Matijaš, T. (2023). Uloga CBCT-a u području dentalne implantologije. RadiološKi Vjesnik, 47(1), 16–27. [CrossRef]
- Blum, I. R. (2024). Implant Dentistry: A journey from the beginnings to what has become an established discipline. Primary Dental Journal, 13(3), 2–3. [CrossRef]
- Cruz, M. B., Silva, N., Marques, J. F., Mata, A., Silva, F. S., & Caramês, J. (2022). Biomimetic Implant Surfaces and Their Role in Biological Integration—A Concise Review. Biomimetics, 7(2), 74. [CrossRef]
- Sotova, C., Yanushevich, O., Kriheli, N., Grigoriev, S., Evdokimov, V., Kramar, O., Nozdrina, M., Peretyagin, N., Undritsova, N., Popelyshkin, E., & Peretyagin, P. (2023). Dental Implants: Modern Materials and Methods of Their Surface Modification. Materials, 16(23), 7383. [CrossRef]
- Pabst, A., Asran, A., Lüers, S., Laub, M., Holfeld, C., Palarie, V., Thiem, D. G. E., Becker, P., Hartmann, A., Heimes, D., Al-Nawas, B., & Kämmerer, P. W. (2022). Osseointegration of a New, Ultrahydrophilic and Nanostructured Dental Implant Surface: A Comparative In Vivo Study. Biomedicines, 10(5), 943. [CrossRef]
- Al-Zubaidi, S. M., Madfa, A. A., Mufadhal, A. A., Aldawla, M. A., Hameed, O. S., & Yue, X. (2020). Improvements in Clinical Durability From Functional Biomimetic Metallic Dental Implants. Frontiers in Materials, 7. [CrossRef]
- Mechanical, chemical and biological aspects of titanium and titanium alloys in implant dentistry. (2018, February 1). PMID: 29460522.
- Nicholson, J. W. (2020). Titanium Alloys for Dental Implants: A review. Prosthesis, 2(2), 100–116. [CrossRef]
- Chaturvedi, T. P. (2009). An overview of the corrosion aspect of dental implants (titanium and its alloys). Indian Journal of Dental Research, 20(1), 91. [CrossRef]
- Lin, H., Yin, C., & Mo, A. (2021). Zirconia based dental biomaterials: structure, mechanical properties, biocompatibility, surface modification, and applications as implant. Frontiers in Dental Medicine, 2. [CrossRef]
- Qu, Y., & Liu, L. (2021). Zirconia Materials for Dental Implants: A Literature review. Frontiers in Dental Medicine, 2. [CrossRef]
- Chopra, D., Jayasree, A., Guo, T., Gulati, K., & Ivanovski, S. (2021). Advancing dental implants: Bioactive and therapeutic modifications of zirconia. Bioactive Materials, 13, 161–178. [CrossRef]
- Jaafar, A., Hecker, C., Árki, P., & Joseph, Y. (2020). Sol-Gel derived hydroxyapatite coatings for titanium implants: A review. Bioengineering, 7(4), 127. [CrossRef]
- Kim, J., Kang, I., Cheon, K., Lee, S., Park, S., Kim, H., & Han, C. (2021). Stable sol–gel hydroxyapatite coating on zirconia dental implant for improved osseointegration. Journal of Materials Science Materials in Medicine, 32(7). [CrossRef]
- Baheti, W., Lv, S., Mila, N., Ma, L., ·Amantai, D., Sun, H., & He, H. (2023). Graphene/hydroxyapatite coating deposit on titanium alloys for implant application. Journal of Applied Biomaterials & Functional Materials, 21, 228080002211481. [CrossRef]
- Arcos, D., & Vallet-Regí, M. (2020). Substituted hydroxyapatite coatings of bone implants. Journal of Materials Chemistry B, 8(9), 1781–1800. [CrossRef]
- Hammami, I., Gavinho, S. R., Pádua, A. S., Sá-Nogueira, I., Silva, J. C., Borges, J. P., Valente, M. A., & Graça, M. P. F. (2023). Bioactive Glass Modified with Zirconium Incorporation for Dental Implant Applications: Fabrication, Structural, Electrical, and Biological Analysis. International Journal of Molecular Sciences, 24(13), 10571. [CrossRef]
- Lung, C. Y. K., Abdalla, M. M., Chu, C. H., Yin, I., Got, S., & Matinlinna, J. P. (2021). A Multi-Element-Doped porous bioactive glass coating for implant applications. Materials, 14(4), 961. [CrossRef]
- Sergi, R., Bellucci, D., & Cannillo, V. (2020). A comprehensive review of bioactive glass coatings: state of the art, challenges and future perspectives. Coatings, 10(8), 757. [CrossRef]
- Fiorillo, L., Cervino, G., Galindo-Moreno, P., Herford, A. S., Spagnuolo, G., & Cicciù, M. (2021). Growth factors in oral tissue Engineering: New perspectives and current therapeutic options. BioMed Research International, 2021, 1–11. [CrossRef]
- Stramandinoli-Zanicotti, R., Sassi, L., Rebelatto, C., Boldrine-Leite, L., Brofman, P., & Carvalho, A. (2020). The effect of bone marrow-derived stem cells associated with platelet-rich plasma on the osseointegration of immediately placed implants. Journal of Clinical and Experimental Dentistry, e8–e13. [CrossRef]
- He, P., Zhang, Q., Motiwala, F. I., Shanti, R. M., Chang, B. M., & Le, A. D. (2021). Potential application of dental stem cells in regenerative reconstruction of oral and maxillofacial tissues: a narrative review. Frontiers of Oral and Maxillofacial Medicine, 4, 14. [CrossRef]
- Ma, Y., Wang, S., Wang, H., Chen, X., Shuai, Y., Wang, H., Mao, Y., & He, F. (2023). Mesenchymal stem cells and dental implant osseointegration during aging: from mechanisms to therapy. Stem Cell Research & Therapy, 14(1). [CrossRef]
- Sayed, M. E., Mugri, M. H., Almasri, M. A., Al-Ahmari, M. M., Bhandi, S., Madapusi, T. B., Varadarajan, S., Raj, A. T., Reda, R., Testarelli, L., & Patil, S. (2021). Role of stem cells in Augmenting dental implant osseointegration: a Systematic review. Coatings, 11(9), 1035. [CrossRef]
- Bijukumar, D. R., McGeehan, C., & Mathew, M. T. (2018). Regenerative Medicine Strategies in Biomedical implants. Current Osteoporosis Reports, 16(3), 236–245. [CrossRef]
- Bandyopadhyay, A., Mitra, I., Goodman, S. B., Kumar, M., & Bose, S. (2022). Improving biocompatibility for next generation of metallic implants. Progress in Materials Science, 133, 101053. [CrossRef]
- Marin, E., & Lanzutti, A. (2023). Biomedical Applications of Titanium Alloys: A Comprehensive Review. Materials, 17(1), 114. [CrossRef]
- Accioni, F., Vázquez, J., Merinero, M., Begines, B., & Alcudia, A. (2022). Latest Trends in Surface Modification for Dental Implantology: Innovative Developments and Analytical Applications. Pharmaceutics, 14(2), 455. [CrossRef]
- Cooper, L. F., & Shirazi, S. (2021). Osseointegration—the biological reality of successful dental implant therapy: a narrative review. Frontiers of Oral and Maxillofacial Medicine, 4, 39. [CrossRef]
- Wieszczycka, K., Staszak, K., Woźniak-Budych, M. J., Litowczenko, J., Maciejewska, B. M., & Jurga, S. (2021). Surface functionalization – The way for advanced applications of smart materials. Coordination Chemistry Reviews, 436, 213846. [CrossRef]
- Ahlawat, J., Asil, S. M., Barroso, G. G., Nurunnabi, M., & Narayan, M. (2020). Application of carbon nano onions in the biomedical field: recent advances and challenges. Biomaterials Science, 9(3), 626–644. [CrossRef]
- Kang MS, Lee JH, Hong SW, Lee JH, Han D-W. Nanocomposites for Enhanced Osseointegration of Dental and Orthopedic Implants Revisited: Surface Functionalization by Carbon Nanomaterial Coatings. Journal of Composites Science. 2021; 5(1):23. [CrossRef]
- Abdulghafor, M. A., Mahmood, M. K., Tassery, H., Tardivo, D., Falguiere, A., & Lan, R. (2023). Biomimetic coatings in implant dentistry: A quick update. Journal of Functional Biomaterials, 15(1), 15.[https://www.mdpi.com/2079-4983/15/1/15.
- Mahmud, S., Rahman, M., Kamruzzaman, M., Khatun, H., Ali, M. O., & Haque, M. M. (2023). Recent developments in hydroxyapatite coating on magnesium alloys for clinical applications. The results in Engineering, 17, 101002. [CrossRef]
- Mysore, T. H. M., Patil, A. Y., Hegde, C., Sudeept, M., Kumar, R., Soudagar, M. E. M., & Fattah, I. (2024). Apatite insights: From synthesis to biomedical applications. European Polymer Journal, 112842. [CrossRef]
- Liu, M., Liu, Y., & Luo, F. (2023). The role and mechanism of platelet-rich fibrin in alveolar bone regeneration. Biomedicine & Pharmacotherapy, 168, 115795. [CrossRef]
- Khaohoen, A., Sornsuwan, T., Chaijareenont, P., Poovarodom, P., Rungsiyakull, C., & Rungsiyakull, P. (2023). Biomaterials and Clinical Application of Dental Implants in Relation to Bone Density—A Narrative Review. Journal of Clinical Medicine, 12(21), 6924. [CrossRef]
- Reda, R., Zanza, A., Galli, M., De Biase, A., Testarelli, L., & Di Nardo, D. (2022). Applications and Clinical Behavior of BioHPP in Prosthetic Dentistry: A Short Review. Journal of Composites Science, 6(3), 90. [CrossRef]
- Lo Giudice, R., Sindoni, A., Tribst, J. P. M., Dal Piva, A. M. D. O., Lo Giudice, G., Bellezza, U., ... & Famà, F. (2022). Evaluation of zirconia and high performance polymer abutment surface roughness and stress concentration for implant-supported fixed dental prostheses. Coatings, 12(2), 238.[https://www.mdpi.com/2079-6412/12/2/238].
- Özcan, M., Volpato, C. A. M., Hian, L., Karahan, B. D., & Cesar, P. F. (2022). Graphene for zirconia and titanium composites in dental implants: significance and predictions. Current Oral Health Reports, 9(3), 66-74.[https://link.springer.com/article/10.1007/s40496-022-00310-3.

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



