Submitted:
22 December 2024
Posted:
23 December 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Biochemistry
2.3. RFA Procedure
[Power (watts) × Active ablation time (seconds)] / Volume of LN(s) (mL).
2.4. Statistical Analysis:
3. Results
4. Discussion
5. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| TC | Thyroid cancer |
| U/S | Ultrasound |
| CT | Computed tomography |
| MRI | Magnetic resonance imaging |
| WDTC | Well-differentiated thyroid carcinoma |
| PTC | Papillary thyroid carcinoma |
| FTC | Follicular thyroid carcinoma |
| WHO | World Health Organization |
| IEFV | Invasive encapsulated follicular variant |
| OCA | Oncocytic carcinoma |
| MTC | Medullary thyroid carcinoma |
| DHGTC | Differentiated high grade thyroid carcinoma |
| PDTC | Poorly differentiated thyroid carcinoma |
| ATC | Anaplastic thyroid carcinoma |
| SIR | Structural incomplete response |
| RAI | Radioiodine |
| ATA | American Thyroid Association |
| MIT | Minimally invasive treatments |
| RFA | Radiofrequency ablation |
| FNAC | Fine-needle aspiration cytology |
| Tg | Thyroglobulin |
| LN | Lymph node |
| AS | Active surveillance |
| WBS | Whole-body scan |
| FDG | Fludeoxyglucose |
| PET | Positron emission tomography |
| TSH | Thyroid-stimulating hormone |
| FT4 | Free thyroxine |
| Anti-Tgs | Antithyroglobulin antibodies |
| RIA | Radioimmunoassay |
| IRMA | Immunoradiometric Assay |
| D5W | Dextrose 5% in water |
| E/V | Energy applied per unit volume |
| SSU | Short stay unit |
| SD | Standard deviation |
| IQR | Interquartile range |
| RAI-A-T | RAI ablation treatment |
| TNM | Tumor, node, metastasis |
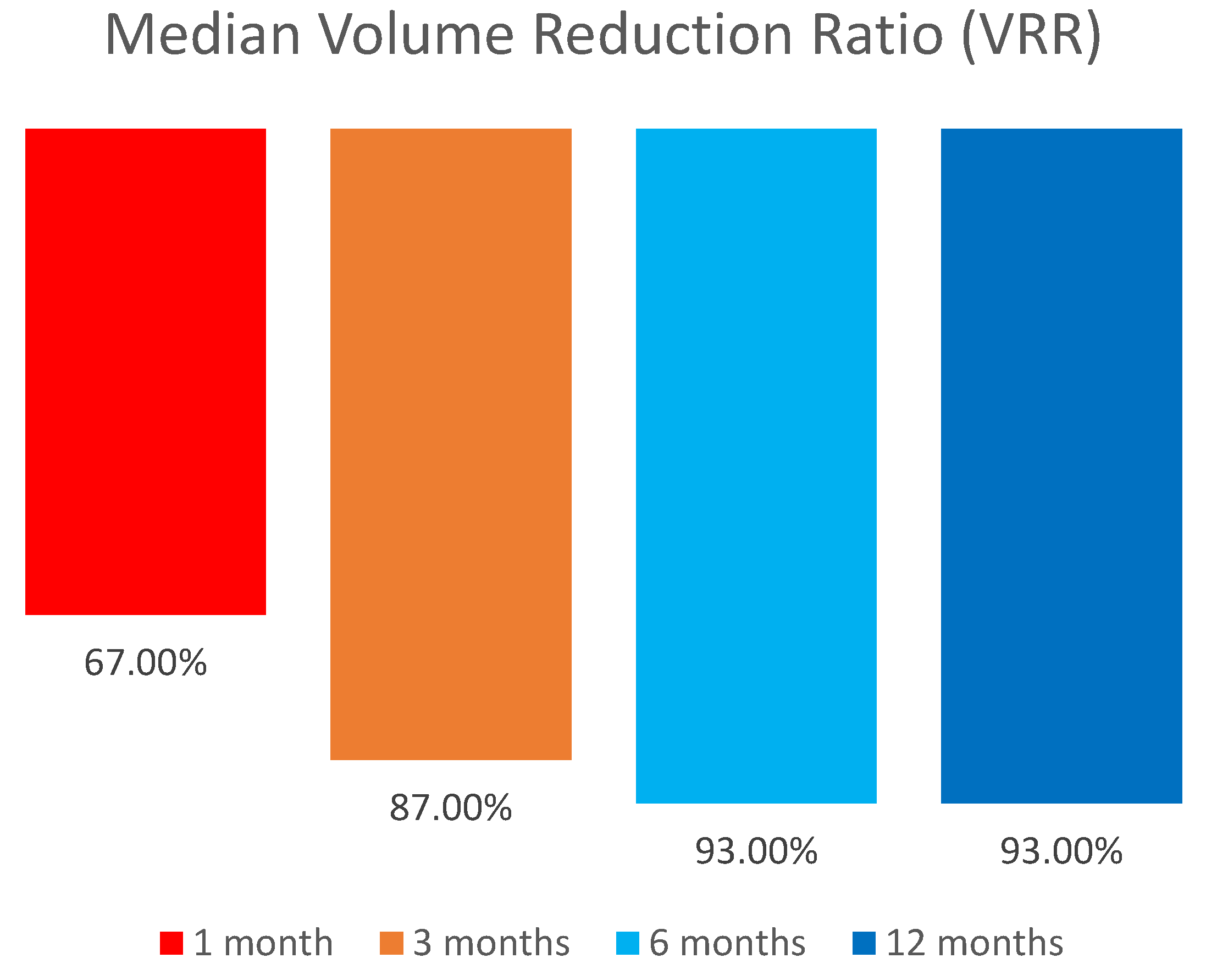
| VRR | Volume reduction ratio |
| URL | Upper reference limit |
| TKI | Tyrosine kinase inhibitor |
| RECIST | Response Evaluation Criteria in Solid Tumors |
References
- NIH National Cancer Insitute Surveillance, Epidemiology, and End Results Program. Cancer Stat Facts: Thyroid Cancer, 2024.
- Seib, C.D.; Sosa, J.A. Evolving Understanding of the Epidemiology of Thyroid Cancer. Endocrinol Metab Clin North Am 2019, 48, 23–35. [Google Scholar] [CrossRef] [PubMed]
- Vaccarella, S.; Franceschi, S.; Bray, F.; Wild, C.P.; Plummer, M.; Dal Maso, L. Worldwide Thyroid-Cancer Epidemic? The Increasing Impact of Overdiagnosis. N Engl J Med 2016, 375, 614–617. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Dal Maso, L.; Vaccarella, S. Global Trends in Thyroid Cancer Incidence and the Impact of Overdiagnosis. Lancet Diabetes Endocrinol 2020, 8, 468–470. [Google Scholar] [CrossRef] [PubMed]
- Key Statistics for Thyroid Cancer. Available online: https://www.cancer.org/cancer/types/thyroid-cancer/about/key-statistics.html (accessed on 10 March 2024).
- Lim, H.; Devesa, S.S.; Sosa, J.A.; Check, D.; Kitahara, C.M. Trends in Thyroid Cancer Incidence and Mortality in the United States, 1974-2013. JAMA 2017, 317, 1338. [Google Scholar] [CrossRef]
- Fagin, J.A.; Wells, S.A. Biologic and Clinical Perspectives on Thyroid Cancer. N Engl J Med 2016, 375, 1054–1067. [Google Scholar] [CrossRef]
- Younis, E. Oncogenesis of Thyroid Cancer. Asian Pac J Cancer Prev 2017, 18, 1191–1199. [Google Scholar] [CrossRef]
- Juhlin, C.C.; Mete, O.; Baloch, Z.W. The 2022 WHO Classification of Thyroid Tumors: Novel Concepts in Nomenclature and Grading. Endocrine-Related Cancer 2023, 30. [Google Scholar] [CrossRef]
- Baloch, Z.W.; Asa, S.L.; Barletta, J.A.; Ghossein, R.A.; Juhlin, C.C.; Jung, C.K.; LiVolsi, V.A.; Papotti, M.G.; Sobrinho-Simões, M.; Tallini, G.; et al. Overview of the 2022 WHO Classification of Thyroid Neoplasms. Endocrine Pathology 2022, 33, 27–63. [Google Scholar] [CrossRef]
- Survival Rates for Thyroid Cancer. Available online: https://www.cancer.org/cancer/types/thyroid-cancer/detection-diagnosis-staging/survival-rates.html (accessed on 11 March 2024).
- Megwalu, U.C.; Moon, P.K. Thyroid Cancer Incidence and Mortality Trends in the United States: 2000–2018. Thyroid 2022, 32, 560–570. [Google Scholar] [CrossRef]
- Henke, L.E.; Pfeifer, J.D.; Baranski, T.J.; DeWees, T.; Grigsby, P.W. Long-Term Outcomes of Follicular Variant vs Classic Papillary Thyroid Carcinoma. Endocr Connect 2018, 7, 1226–1235. [Google Scholar] [CrossRef]
- Matsuura, D.; Yuan, A.; Wang, L.; Ranganath, R.; Adilbay, D.; Harries, V.; Patel, S.; Tuttle, M.; Xu, B.; Ghossein, R.; et al. Follicular and Hurthle Cell Carcinoma: Comparison of Clinicopathological Features and Clinical Outcomes. Thyroid 2022, 32, 245–254. [Google Scholar] [CrossRef] [PubMed]
- Wu, M.-H.; Lee, Y.-Y.; Lu, Y.-L.; Lin, S.-F. Risk Factors and Prognosis for Metastatic Follicular Thyroid Cancer. Front. Endocrinol. 2022, 13. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.Y.; Won, J.-K.; Lee, S.-H.; Park, D.J.; Jung, K.C.; Sung, M.-W.; Wu, H.-G.; Kim, K.H.; Park, Y.J.; Hah, J.H. Changes of Clinicopathologic Characteristics and Survival Outcomes of Anaplastic and Poorly Differentiated Thyroid Carcinoma. Thyroid 2016, 26, 404–413. [Google Scholar] [CrossRef] [PubMed]
- Harahap, A.S.; Roren, R.S.; Imtiyaz, S. A Comprehensive Review and Insights into the New Entity of Differentiated High-Grade Thyroid Carcinoma. Curr Oncol 2024, 31, 3311–3328. [Google Scholar] [CrossRef] [PubMed]
- Bible, K.C.; Kebebew, E.; Brierley, J.; Brito, J.P.; Cabanillas, M.E.; Clark, T.J.; Di Cristofano, A.; Foote, R.; Giordano, T.; Kasperbauer, J.; et al. 2021 American Thyroid Association Guidelines for Management of Patients with Anaplastic Thyroid Cancer. Thyroid 2021, 31, 337–386. [Google Scholar] [CrossRef]
- Haugen, B.R.; Alexander, E.K.; Bible, K.C.; Doherty, G.M.; Mandel, S.J.; Nikiforov, Y.E.; Pacini, F.; Randolph, G.W.; Sawka, A.M.; Schlumberger, M.; et al. 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid 2016, 26, 1–133. [Google Scholar] [CrossRef]
- Filetti, S.; Durante, C.; Hartl, D.; Leboulleux, S.; Locati, L.D.; Newbold, K.; Papotti, M.G.; Berruti, A. Thyroid Cancer: ESMO Clinical Practice Guidelines for Diagnosis, Treatment and Follow-Up. Annals of Oncology 2019, 30, 1856–1883. [Google Scholar] [CrossRef]
- Haddad, R.I.; Bischoff, L.; Ball, D.; Bernet, V.; Blomain, E.; Busaidy, N.L.; Campbell, M.; Dickson, P.; Duh, Q.; Ehya, H.; et al. Thyroid Carcinoma, Version 2.2022, NCCN Clinical Practice Guidelines in Oncology. Journal of the National Comprehensive Cancer Network 2022, 20, 925–951. [Google Scholar] [CrossRef]
- Pacini, F.; Fuhrer, D.; Elisei, R.; Handkiewicz-Junak, D.; Leboulleux, S.; Luster, M.; Schlumberger, M.; Smit, J.W. 2022 ETA Consensus Statement: What Are the Indications for Post-Surgical Radioiodine Therapy in Differentiated Thyroid Cancer? Eur Thyroid J 2021, 11, e210046. [Google Scholar] [CrossRef]
- Sapuppo, G.; Tavarelli, M.; Belfiore, A.; Vigneri, R.; Pellegriti, G. Time to Separate Persistent from Recurrent Differentiated Thyroid Cancer: Different Conditions with Different Outcomes. Journal of Clinical Endocrinology and Metabolism 2018, 104, 258–265. [Google Scholar] [CrossRef]
- Mauri, G.; Hegedüs, L.; Bandula, S.; Cazzato, R.L.; Czarniecka, A.; Dudeck, O.; Fugazzola, L.; Netea-Maier, R.; Russ, G.; Wallin, G.; et al. European Thyroid Association and Cardiovascular and Interventional Radiological Society of Europe 2021 Clinical Practice Guideline for the Use of Minimally Invasive Treatments in Malignant Thyroid Lesions. European Thyroid Journal 2021, 10, 185–197. [Google Scholar] [CrossRef] [PubMed]
- Cavalheiro, B.G.; Shah, J.P.; Randolph, G.W.; Medina, J.E.; Tufano, R.P.; Zafereo, M.; Hartl, D.M.; Nixon, I.J.; Guntinas-Lichius, O.; Vander Poorten, V.; et al. Management of Recurrent Well-Differentiated Thyroid Carcinoma in the Neck: A Comprehensive Review. Cancers 2023, 15, 923. [Google Scholar] [CrossRef] [PubMed]
- Jasim, S.; Patel, K.N.; Randolph, G.; Adams, S.; Cesareo, R.; Condon, E.; Henrichsen, T.; Itani, M.; Papaleontiou, M.; Rangel, L.; et al. American Association of Clinical Endocrinology Disease State Clinical Review: The Clinical Utility of Minimally Invasive Interventional Procedures in the Management of Benign and Malignant Thyroid Lesions. Endocrine Practice 2022, 28, 433–448. [Google Scholar] [CrossRef] [PubMed]
- Malandrino, P.; Latina, A.; Marescalco, S.; Spadaro, A.; Regalbuto, C.; Fulco, R.A.; Scollo, C.; Vigneri, R.; Pellegriti, G. Risk-Adapted Management of Differentiated Thyroid Cancer Assessed by a Sensitive Measurement of Basal Serum Thyroglobulin. The Journal of Clinical Endocrinology & Metabolism 2011, 96, 1703–1709. [Google Scholar] [CrossRef]
- Tufano, R.P.; Clayman, G.; Heller, K.S.; Inabnet, W.B.; Kebebew, E.; Shaha, A.; Steward, D.L.; Tuttle, R.M. Management of Recurrent/Persistent Nodal Disease in Patients with Differentiated Thyroid Cancer: A Critical Review of the Risks and Benefits of Surgical Intervention Versus Active Surveillance. Thyroid 2015, 25, 15–27. [Google Scholar] [CrossRef]
- Orloff, L.A.; Noel, J.E.; Stack, B.C.; Russell, M.D.; Angelos, P.; Baek, J.H.; Brumund, K.T.; Chiang, F.Y.; Cunnane, M.B.; Davies, L.; et al. Radiofrequency Ablation and Related Ultrasound-Guided Ablation Technologies for Treatment of Benign and Malignant Thyroid Disease: An International Multidisciplinary Consensus Statement of the American Head and Neck Society Endocrine Surgery Section with the Asia Pacific Society of Thyroid Surgery, Associazione Medici Endocrinologi, British Association of Endocrine and Thyroid Surgeons, European Thyroid Association, Italian Society of Endocrine Surgery Units, Korean Society of Thyroid Radiology, Head & Neck 2022, 44, 633–660. [Google Scholar] [CrossRef]
- Dupuy, D.E.; Monchik, J.M.; Decrea, C.; Pisharodi, L. Radiofrequency Ablation of Regional Recurrence from Well-Differentiated Thyroid Malignancy. Surgery 2001, 130, 971–977. [Google Scholar] [CrossRef]
- van Dijk, S.P.J.; Coerts, H.I.; Gunput, S.T.G.; van Velsen, E.F.S.; Medici, M.; Moelker, A.; Peeters, R.P.; Verhoef, C.; van Ginhoven, T.M. Assessment of Radiofrequency Ablation for Papillary Microcarcinoma of the Thyroid: A Systematic Review and Meta-Analysis. JAMA Otolaryngol Head Neck Surg 2022, 148, 317–325. [Google Scholar] [CrossRef]
- Zhao, Q.; Tian, G.; Kong, D.; Jiang, T. Meta-Analysis of Radiofrequency Ablation for Treating the Local Recurrence of Thyroid Cancers. Journal of Endocrinological Investigation 2016, 39, 909–916. [Google Scholar] [CrossRef]
- Chegeni, H.; Ebrahiminik, H.; Mosadegh Khah, A.; Malekzadeh, H.; Abbasi, M.; Molooghi, K.; Fadaee, N.; Kargar, J. Ultrasound-Guided Radiofrequency Ablation of Locally Recurrent Thyroid Carcinoma. CardioVascular and Interventional Radiology 2022, 45, 677–684. [Google Scholar] [CrossRef]
- Ahmad, S.; Aljammal, J.; Orozco, I.; Raashid, S.; Zulfiqar, F.; Nikravan, S.P.; Hussain, I. Radiofrequency Ablation of Cervical Thyroid Cancer Metastases—Experience of Endocrinology Practices in the United States. Journal of the Endocrine Society 2023, 7, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Baek, J.H.; Lim, H.K.; Ahn, H.S.; Baek, S.M.; Choi, Y.J.; Choi, Y.J.; Chung, S.R.; Ha, E.J.; Hahn, S.Y.; et al. 2017 Thyroid Radiofrequency Ablation Guideline: Korean Society of Thyroid Radiology. Korean Journal of Radiology 2018, 19, 632. [Google Scholar] [CrossRef] [PubMed]
- Chung, S.R.; Baek, J.H.; Choi, Y.J.; Lee, J.H. Ten-Year Outcomes of Radiofrequency Ablation for Locally Recurrent Papillary Thyroid Cancer. Korean Journal of Radiology 2024, 25, 851. [Google Scholar] [CrossRef]
- Yang, Z.; Yan, L.; Xiao, J.; Li, W.; Li, X.; Li, Y.; Zhang, M.; Luo, Y. Long-Term Results of Radiofrequency Ablation for Locally Recurrent Papillary Thyroid Carcinoma. International Journal of Hyperthermia 2023, 40. [Google Scholar] [CrossRef]
- Guang, Y.; Luo, Y.; Zhang, Y.; Zhang, M.; Li, N.; Zhang, Y.; Tang, J. Efficacy and Safety of Percutaneous Ultrasound Guided Radiofrequency Ablation for Treating Cervical Metastatic Lymph Nodes from Papillary Thyroid Carcinoma. Journal of Cancer Research and Clinical Oncology 2017, 143, 1555–1562. [Google Scholar] [CrossRef]
- Suh, C.H.; Baek, J.H.; Choi, Y.J.; Lee, J.H. Efficacy and Safety of Radiofrequency and Ethanol Ablation for Treating Locally Recurrent Thyroid Cancer: A Systematic Review and Meta-Analysis. Thyroid 2016, 26, 420–428. [Google Scholar] [CrossRef]
- Chung, S.R.; Suh, C.H.; Baek, J.H.; Park, H.S.; Choi, Y.J.; Lee, J.H. Safety of Radiofrequency Ablation of Benign Thyroid Nodules and Recurrent Thyroid Cancers: A Systematic Review and Meta-Analysis. International Journal of Hyperthermia 2017, 33, 1–35. [Google Scholar] [CrossRef]
- Shin, J.E.; Baek, J.H.; Lee, J.H. Radiofrequency and Ethanol Ablation for the Treatment of Recurrent Thyroid Cancers. Current Opinion in Oncology 2013, 25, 14–19. [Google Scholar] [CrossRef]
- Shin, J.H.; Baek, J.H.; Ha, E.J.; Lee, J.H. Radiofrequency Ablation of Thyroid Nodules: Basic Principles and Clinical Application. International Journal of Endocrinology 2012, 2012, 1–7. [Google Scholar] [CrossRef]
- Bremner, F. Apraclonidine Is Better Than Cocaine for Detection of Horner Syndrome. Front Neurol 2019, 10, 55. [Google Scholar] [CrossRef]
- Bouvet, C.; Barres, B.; Kwiatkowski, F.; Batisse-Lignier, M.; Chafai El Alaoui, M.; Kauffmann, P.; Cachin, F.; Tauveron, I.; Kelly, A.; Maqdasy, S. Re-Treatment With Adjuvant Radioactive Iodine Does Not Improve Recurrence-Free Survival of Patients With Differentiated Thyroid Cancer. Front. Endocrinol. 2019, 10. [Google Scholar] [CrossRef] [PubMed]
- Cadena-Piñeros, E.; Escobar, J.V.; Carreño, J.A.; Rojas, J.G. Second Adjuvant Radioiodine Therapy after Reoperation for Locoregionally Persistent or Recurrent Papillary Thyroid Carcinoma. World J Nucl Med 2022, 21, 290–295. [Google Scholar] [CrossRef] [PubMed]
- Lamartina, L.; Borget, I.; Mirghani, H.; Al Ghuzlan, A.; Berdelou, A.; Bidault, F.; Deandreis, D.; Baudin, E.; Travagli, J.-P.; Schlumberger, M.; et al. Surgery for Neck Recurrence of Differentiated Thyroid Cancer: Outcomes and Risk Factors. J Clin Endocrinol Metab 2017, 102, 1020–1031. [Google Scholar] [CrossRef]
- Chen, W.C.; Chou, C.K.; Chang, Y.H.; Chiang, P.L.; Lim, L.S.; Chi, S.Y.; Luo, S.D.; Lin, W.C. Efficacy of Radiofrequency Ablation for Metastatic Papillary Thyroid Cancer with and without Initial Biochemical Complete Status. Frontiers in Endocrinology 2022, 13. [Google Scholar] [CrossRef]
- Suh, C.H.; Baek, J.H.; Choi, Y.J.; Lee, J.H. Efficacy and Safety of Radiofrequency and Ethanol Ablation for Treating Locally Recurrent Thyroid Cancer: A Systematic Review and Meta-Analysis. Thyroid 2016, 26, 420–428. [Google Scholar] [CrossRef]
- Yang, Z.; Zhang, M.; Yan, L.; Xiao, J.; Li, Y.; Li, X.; Luo, Y. Value of Radiofrequency Ablation for Treating Locally Recurrent Thyroid Cancer: A Systematic Review and Meta-Analysis for 2-Year Follow-Up. Endocrine 2024, 85, 1066–1074. [Google Scholar] [CrossRef]
- Chung, S.R.; Baek, J.H.; Choi, Y.J.; Sung, T.-Y.; Song, D.E.; Kim, T.Y.; Lee, J.H. Efficacy of Radiofrequency Ablation for Recurrent Thyroid Cancer Invading the Airways. European Radiology 2021, 31, 2153–2160. [Google Scholar] [CrossRef]
- Bischoff, L.A.; Ganly, I.; Fugazzola, L.; Buczek, E.; Faquin, W.C.; Haugen, B.R.; McIver, B.; McMullen, C.P.; Newbold, K.; Rocke, D.J.; et al. Molecular Alterations and Comprehensive Clinical Management of Oncocytic Thyroid Carcinoma: A Review and Multidisciplinary 2023 Update. JAMA Otolaryngol Head Neck Surg 2024, 150, 265–272. [Google Scholar] [CrossRef]
- Lamartina, L.; Grani, G.; Durante, C.; Borget, I.; Filetti, S.; Schlumberger, M. Follow-up of Differentiated Thyroid Cancer - What Should (and What Should Not) Be Done. Nat Rev Endocrinol 2018, 14, 538–551. [Google Scholar] [CrossRef]
- Kim, C.; Lee, J.H.; Choi, Y.J.; Kim, W.B.; Sung, T.Y.; Baek, J.H. Complications Encountered in Ultrasonography-Guided Radiofrequency Ablation of Benign Thyroid Nodules and Recurrent Thyroid Cancers. European Radiology 2017, 27, 3128–3137. [Google Scholar] [CrossRef]
- Wijaya, T.D.; Saputri, K.M.; Purwanto, D.J. Second Order Horner Syndrome Concurrent with Brachial Plexus Injury Following Thyroid Radiofrequency Ablation: A Case Report. Acta Neurologica Indonesia 2024, 2. [Google Scholar] [CrossRef]
- Carsote, M.; Nistor, C.-E.; Popa, F.L.; Stanciu, M. Horner’s Syndrome and Lymphocele Following Thyroid Surgery. Journal of Clinical Medicine 2023, 12, 474. [Google Scholar] [CrossRef] [PubMed]
- Hu, X.; Zhang, X.; Gan, H.; Yu, D.; Sun, W.; Shi, Z. Horner Syndrome as a Postoperative Complication after Minimally Invasive Video-Assisted Thyroidectomy: A Case Report. Medicine (Baltimore) 2017, 96, e8888. [Google Scholar] [CrossRef] [PubMed]
| Patients (age/sex) |
ATA risk classification |
T N M |
Histology | No of surg. |
No of RAI- A-T (mCi) |
Disease | Lesion/ Loc. |
Largest diam. (mm) |
Time (mo-nths) |
|---|---|---|---|---|---|---|---|---|---|
| Pt No1 (27/F) |
low | T2 N0 M0 |
PTC (classical variant) |
1 | 1 (150) | R | LN / III LN / IV |
12.1 11.5 |
51 |
| Pt No2 (45/M) |
intermediate | T3b N0 M0 |
OCA widely invasive |
3 | 3 (300) | R | TIS / VI TIS / VI |
13.9 9.6 |
34 |
| TIS / VI | 12.8 | 66 | |||||||
| Pt No3 (69/F) |
intermediate | T3b N1b M0 |
FTC with trabecular/ insular/ solid patterns |
1 | 2 (220) | R | LN / IV TIS / VI |
10.6 8.8 |
39 |
| LN / IV LN / IV |
7.9* 6.6* |
65 | |||||||
| Pt No4 (17/M) |
intermediate | T1a(m) N1 M0 |
PTC (classical variant) |
1 | 1 (90) | P | LN / IV | 8 | 3 |
| Pt No5 (45/F) |
intermediate | T3b(m) N0 M0 |
PTC (classical variant) |
1 | 0 (0) | P | LN / IV LN / IV |
11.5 9.7 |
3 |
| Pt No6 (50/F) | intermediate | T3b N1a M0 |
PTC (classical variant) |
1 | 1 (70) | P | LN / VI LN / IV |
8.2 13.2 |
3 |
| Pt No7 (34/F) |
intermediate | T3b(m) N1a M0 |
PTC (tall-cell variant) |
1 | 2 (300) | P | LN / VI (delphian) | 8 | 4 |
| Pt No8 (27/F) |
intermediate | T2 N1a M0 |
PTC (classical variant) |
1 | 2 (150) | P | LN / III | 11.5 | 11 |
| Patients | Pre-RFA volume (ml) | Pre-RFA Tg (ng/ml) or anti-Tg |
Post-RFA volume (ml) | Post-RFA Tg (ng/ml) or anti-Tg |
Time (months) |
VRR (%) |
|---|---|---|---|---|---|---|
| Pt No1 | lesion 1.1: 0.4 lesion 1.2: 0.2 |
0.2 | 0 0.01 |
<0.1 | 12 | 100 95 |
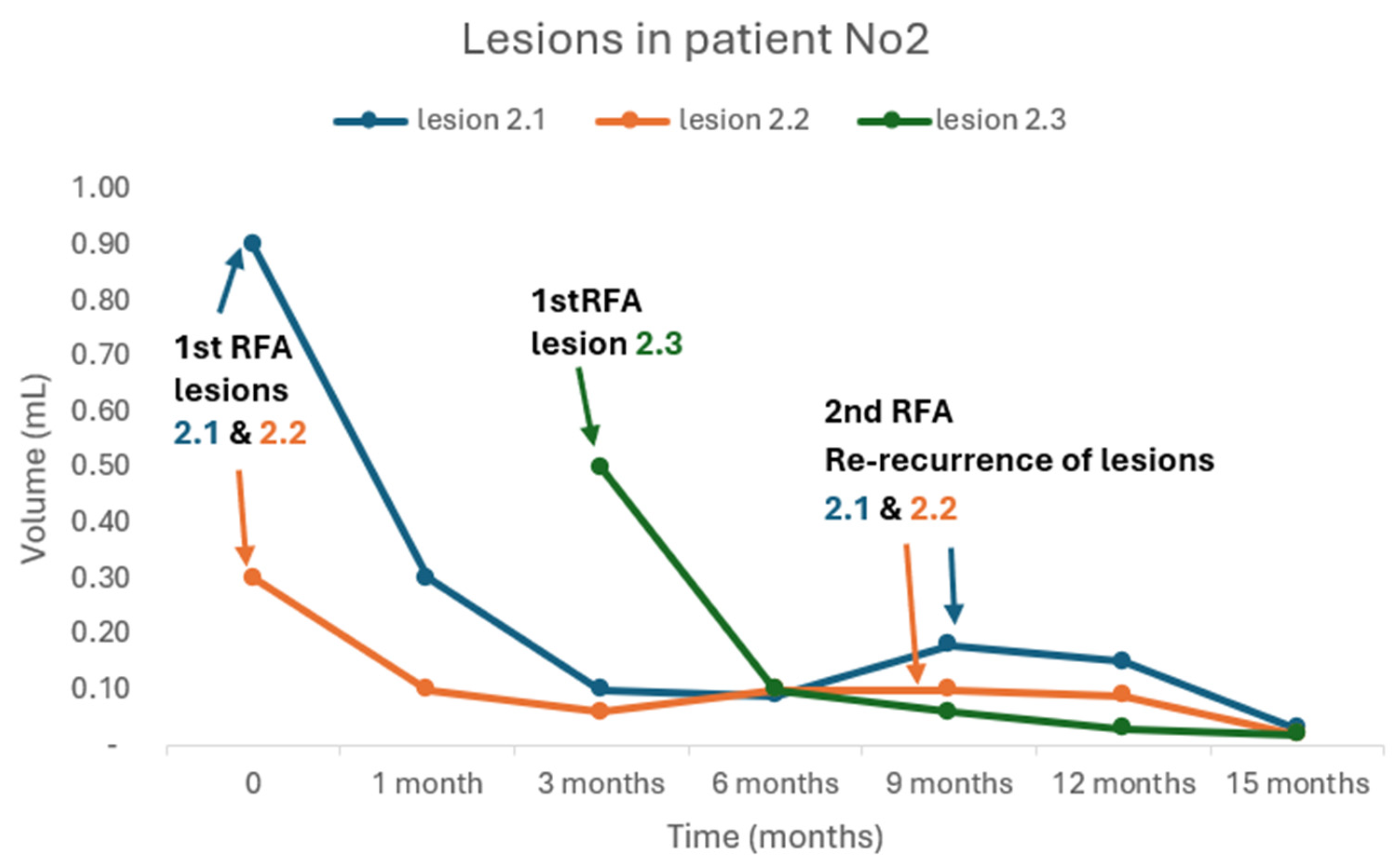
| Pt No2 | lesion 2.1: 0.9 lesion 2.2: 0.3 |
9.97 | 0.03 0.02 |
0.2 0.2 |
15 | 96 93 |
| lesion 2.3: 0.5† | 6.2 | 0.03 | 0.2 | 12 | 94 | |
| Pt No3 | lesion 3.1: 0.5 lesion 3.2: 0.2 |
88* | 0 0.01 |
40* | 21 | 100 95 |
| Pt No4 | 0.14 | 5.8 | 0.01 | 0.5 | 24 | 93 |
| Pt No5 | lesion 5.1: 0.4 lesion 5.1: 0.2 |
1.2 | 0.02 0.01 |
0.28 | 6 | 95 95 |
| Pt No6 | lesion 6.1: 0.12 lesion 6.2: 0.24 |
0.21 | 0.01 0.02 |
<0.1 | 18 | 92 92 |
| Pt No7 | 0.09 | 0.9 | 0.02 | 0.2 | 6 | 78 |
| Pt No8 | 0.23 | 4.9* | 0.03 | 3.5* | 4 | 87 |
| Pre-RFA Median (IQR) |
Post-RFA Median (IQR) |
p | |
| Volume (mL) | 0.24 | 0.02 | 0.001 |
| Thyroglobulin (ng/mL) | 1.05 | 0.2 | 0.028 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




