Submitted:
22 December 2024
Posted:
23 December 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Results
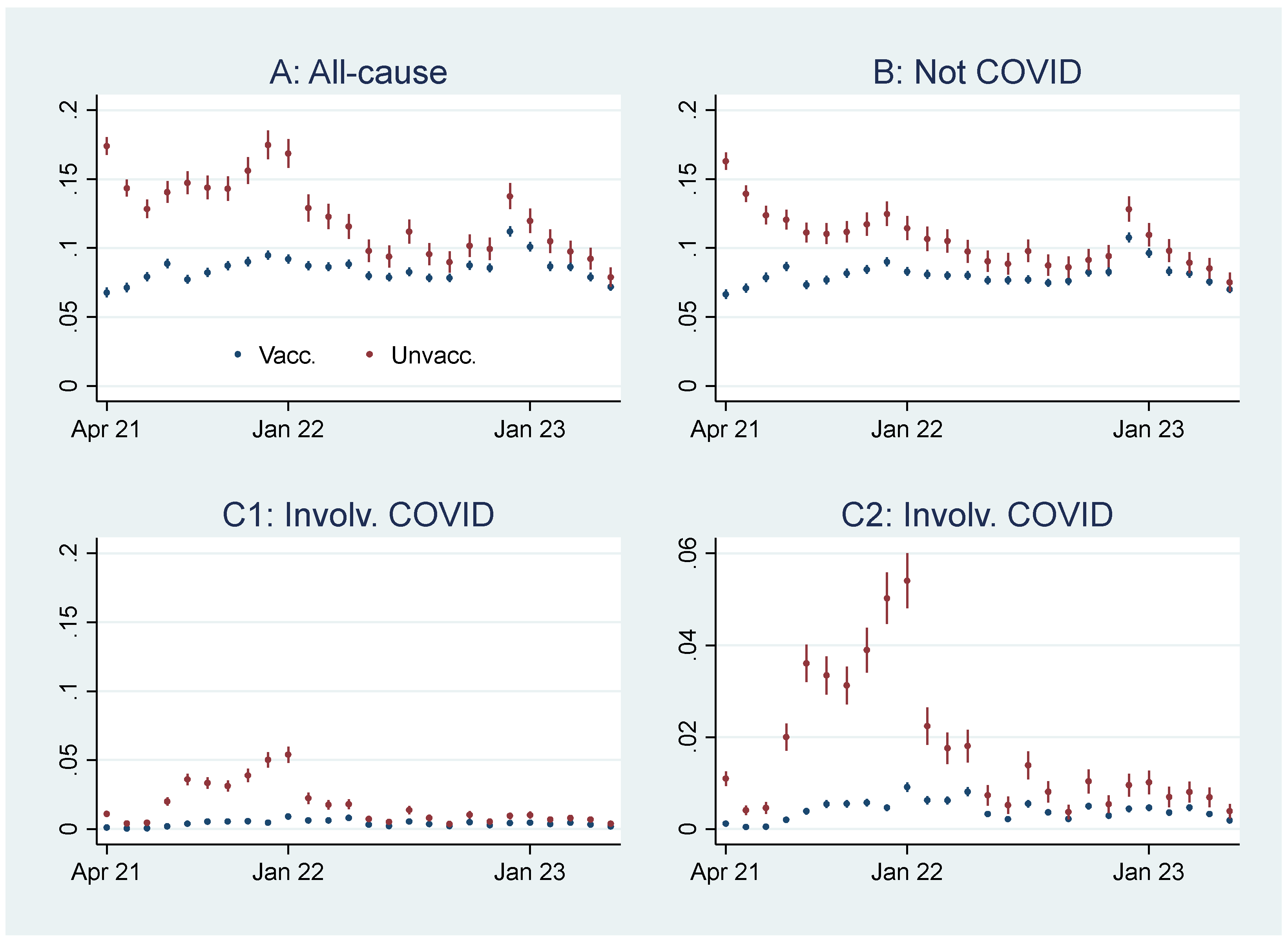
Initial Mortality Probability Analyses
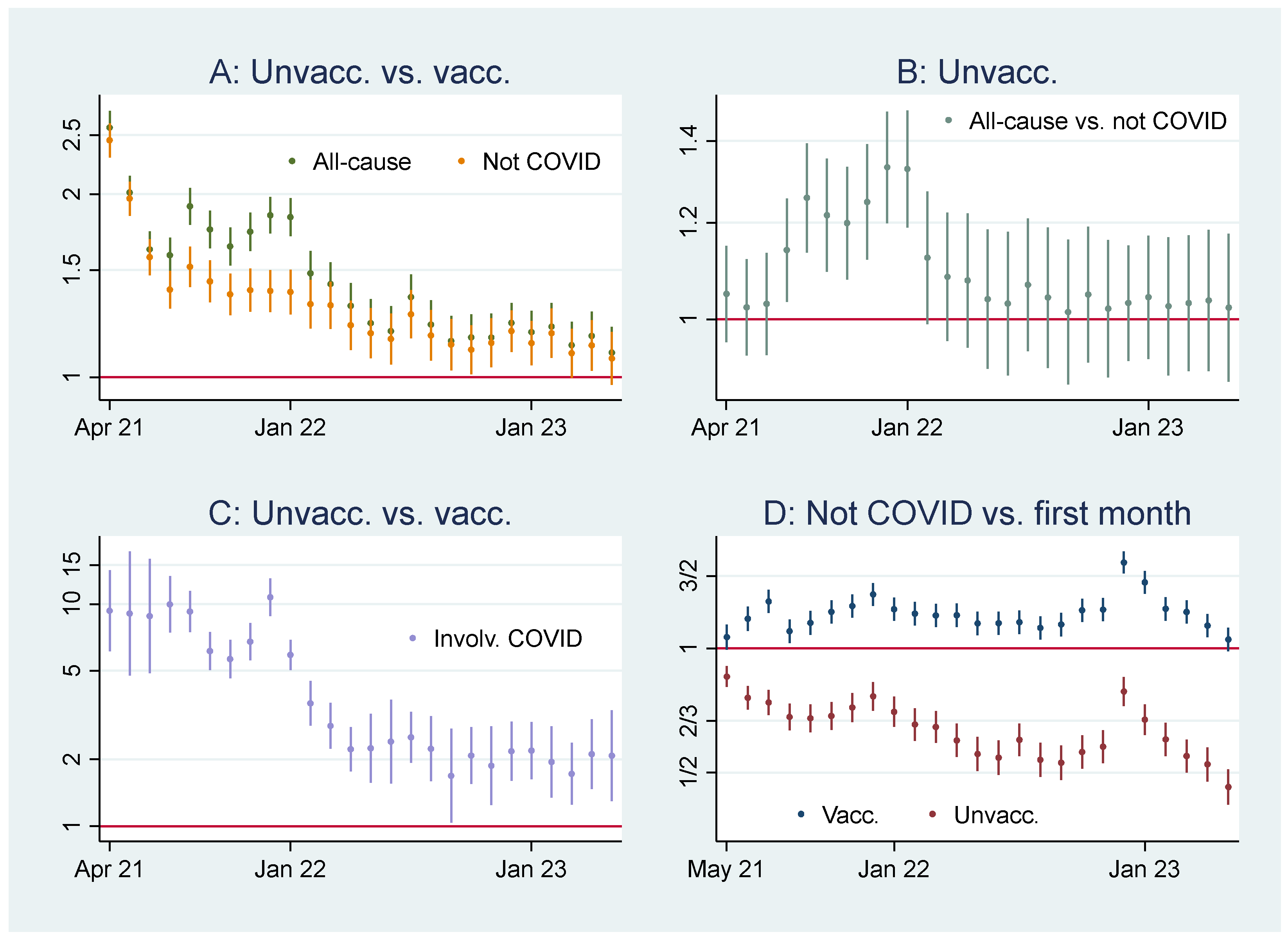
Odds Ratio Analyses
How Odds Ratios and Probability Analyses Indicate Declining Health among Vaccinated
Discussion
Methods
Notes
- Vertical axes in Figure 2 are log-transformed using the natural logaritm.
- The ORs in Graph C, Figure 2, were significant (95% CIs) during the whole period, which can be due to (i) vaccine protection and (ii) unvaccinated having inferior health at the outset. But as the ORs were only about fifth since Feb 22 compared to the first months, explanation (ii) is more likely during that period.
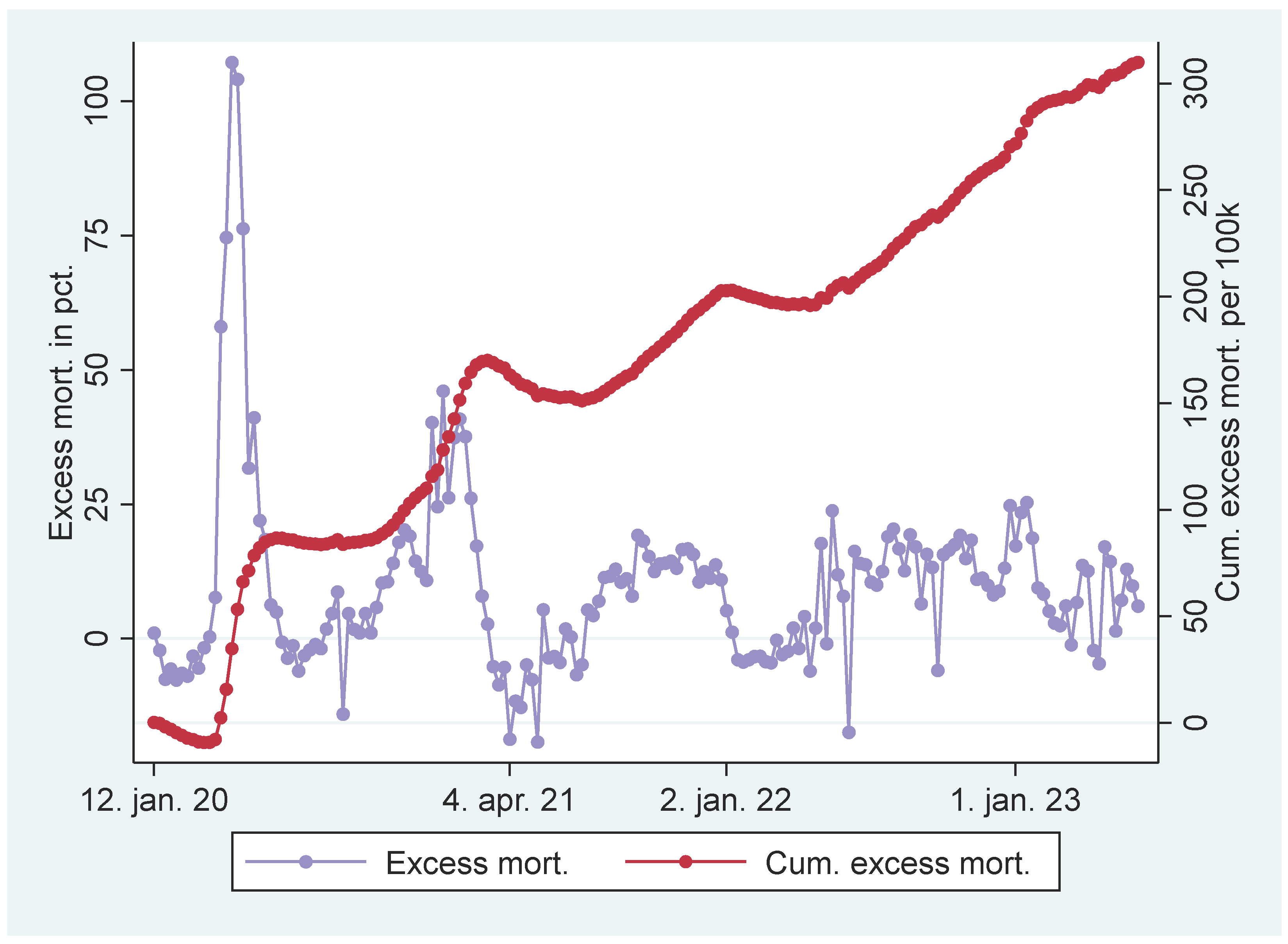
- Assuming that the excess mortality among the unvaccinated segment before Apr 21 was a percent, one may assume that it was a*b percent among the vaccinated segment, where 0<b<1. One may assume b<1 because the vaccinated segment had relatively good health at the outset [1], and one may assume 0<b because there were, nonetheless, people vulnerable to COVID-19 among them. I.e., a*b was lower than a but still higher than zero. According to the reasoning, one should expect a decline in mortality among vaccinated during the study period due to previous excess mortality, but not necessarily as marked as observed among unvaccinated. Alternatively, one may argue the opposite as among the vaccinated segment, “some very comorbid patients [in care homoes] got vaccine side effects that probably accelerated an already progressing death process” ([23], p. 3 - my translation from Norwegian).
- People in England under 70 years old but clinically extremely vulnerable were prioritized vaccination with those aged between 70-74 [18]. Hence, they were prioritized early.
- To exemplify, in Apr 2021, the age-standardized all-cause mortality rate among “ever vaccinated”, defined as vaccinated in this study, was 812.7 per 100,000 person-years, which were 2,124,523 [5]. The expression (812.7/100,000)*2,124,523 gives 17,266 estimated deaths in an estimated population of 25,494,276, which was reached by multiplying 2,124,523 by 12. I.e., the age-standardized all-cause mortality probability among vaccinated in Ap 21 was 17,266 divided by 25,494,276, taking the value of .0068 percent. Similar estimations of all-cause mortality, mortality involving and not involving COVID-19, were carried out each month for vaccinated and unvaccinated.
Funding
Conflicts of Interest
References
- UK Office for National Statistics. Coronavirus (COVID-19) latest insights: Vaccines 2023. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/articles/coronaviruscovid19latestinsights/vaccines.
- King, G.; Nielsen, R. Why Propensity Scores Should Not Be Used for Matching. Political Analysis 2019, 27, 435–454. [Google Scholar] [CrossRef]
- Wysocki, A.C.; Lawson, K.M.; Rhemtulla, M. Statistical Control Requires Causal Justification. Advances in Methods and Practices in Psychological Science 2022, 5, 25152459221095823. [Google Scholar] [CrossRef]
- York, R. Control variables and causal inference: a question of balance. International Journal of Social Research Methodology 2018, 21, 675–684. [Google Scholar] [CrossRef]
- UK Office for National Statistics. Deaths by vaccination status, England 2023. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/datasets/deathsbyvaccinationstatusengland.
- Wakker, W. XLINCOM: Stata module to estimate multiple linear combinations of parameters. 2023.
- StataCorp. Version 17. College Station, TX StataCorp LP; 2021.
- Lopez-Doriga Ruiz, P.; Gunnes, N.; Michael Gran, J.; Karlstad, Ø.; Selmer, R.; Dahl, J.; et al. Short-term safety of COVID-19 mRNA vaccines with respect to all-cause mortality in the older population in Norway. Vaccine 2023, 41, 323–332. [Google Scholar] [CrossRef] [PubMed]
- Haas, E.J.; Angulo, F.J.; McLaughlin, J.M.; Anis, E.; Singer, S.R.; Khan, F.; et al. Impact and effectiveness of mRNA BNT162b2 vaccine against SARS-CoV-2 infections and COVID-19 cases, hospitalisations, and deaths following a nationwide vaccination campaign in Israel: an observational study using national surveillance data. Lancet 2021, 397, 1819–1829. [Google Scholar] [CrossRef]
- Bernal, J.L.; Andrews, N.; Gower, C.; Robertson, C.; Stowe, J.; Tessier, E.; et al. Effectiveness of the Pfizer-BioNTech and Oxford-AstraZeneca vaccines on covid-19 related symptoms, hospital admissions, and mortality in older adults in England: test negative case-control study. Bmj-British Medical Journal 2021, 373. [Google Scholar]
- Watson, O.J.; Barnsley, G.; Toor, J.; Hogan, A.B.; Winskill, P.; Ghani, A.C. Global impact of the first year of COVID-19 vaccination: a mathematical modelling study. The Lancet Infectious Diseases 2022. [Google Scholar] [CrossRef] [PubMed]
- Nordstrom, P.; Ballin, M.; Nordstrom, A. Risk of infection, hospitalisation, and death up to 9 months after a second dose of COVID-19 vaccine: a retrospective, total population cohort study in Sweden. Lancet 2022, 399, 814–823. [Google Scholar] [CrossRef]
- Alessandria, M.; Malatesta, G.; Di Palmo, G.; Cosentino, M.; Donzelli, A. All-cause mortality according to COVID-19 vaccination status: An analysis of the UK office for National statistics public data. F1000Research 2024, 13, 886. [Google Scholar] [CrossRef]
- Fraiman, J.; Erviti, J.; Jones, M.; Greenland, S.; Whelan, P.; Kaplan, R.M.; Doshi, P. Serious adverse events of special interest following mRNA COVID-19 vaccination in randomized trials in adults. Vaccine 2022, 40, 5798–5805. [Google Scholar] [CrossRef]
- Mostert, S.; Hoogland, M.; Huibers, M.; Kaspers, G. Excess mortality across countries in the Western World since the COVID-19 pandemic: ’Our World in Data’ estimates of 20 to December 2022. BMJ Public Health 2024, 2, e000282. [Google Scholar] [CrossRef]
- Faksova, K.; Walsh, D.; Jiang, Y.; Griffin, J.; Phillips, A.; Gentile, A.; et al. COVID-19 vaccines and adverse events of special interest: A multinational Global Vaccine Data Network (GVDN) cohort study of 99 million vaccinated individuals. Vaccine 2024, 42, 2200–2211. [Google Scholar] [CrossRef]
- Aarstad, J. Deaths among young people in England increased significantly in 10 of 11 weeks after COVID-19 vaccination and doubled in three. Excli j. 2024, 23, 908–911. [Google Scholar]
- UK Office for National Statistics. UK COVID-19 vaccines delivery plan 2021. Available online: https://www.gov.uk/government/publications/uk-covid-19-vaccines-delivery-plan/uk-covid-19-vaccines-delivery-plan.
- UK Office for National Statistics. Weekly COVID-19 age-standardised mortality rates by vaccination status, England: methodology 2021. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/methodologies/weeklycovid19agestandardisedmortalityratesbyvaccinationstatusenglandmethodology.
- UK Office for National Statistics. Impact of registration delays on mortality statistics in England and Wales: 2022 2024. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/articles/impactofregistrationdelaysonmortalitystatisticsinenglandandwales/latest.
- Williams, R. Using the margins command to estimate and interpret adjusted predictions and marginal effects. Stata Journal 2012, 12, 308–331. [Google Scholar] [CrossRef]
- Knol, M.J.; Pestman, W.R.; Grobbee, D.E. The (mis)use of overlap of confidence intervals to assess effect modification. Eur J Epidemiol. 2011, 26, 253–254. [Google Scholar] [CrossRef]
- Wyller, T.B.; Kittang, B.R.; Ranhoff, A.H.; Harg, P.; Myrstad, M. Dødsfall i sykehjem etter covid-19-vaksine. Tidsskrift for Den norske legeforening 2021, 141, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Our World in Data. Coronavirus (COVID-19) Vaccinations 2024. Available online: https://ourworldindata.org/covid-vaccinations.
- UK Office for National Statistics. Excess mortality within England: 2023 data - statistical commentary 2024 [.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



