Submitted:
04 December 2024
Posted:
06 December 2024
You are already at the latest version
Abstract
The mechanism of menstrual-disturbance post-COVID-19 vaccination is subtle. Although direct interactions with molecular vaccines per se is reported, albeit the indirect stimulants, factors, patient demographics involved are not clear. Stress and uterine dysbiosis are largely overlooked despite the similar neurochemicals to that in the gut-brain-axis. Thus, more surveillance on women’s responses post-vaccination are needed. We aimed to survey the increasing trends in women’s menstrual disturbance post-pandemic vaccination for frequency, potential factors, patients’ demographics, and vaccine types involved using a self-administered web-based online public question-naire sent to different regions of Saudi Arabia. We collected data on 1372 women who developed menstrual ir-regularity after vaccination and used statistical analysis to examine and identify associated factors. In 1372 females; 61.1% (n=838) aged 19-29 years, 94.2% (n = 1292) Saudi citizens, 66.4% (n=911) graduates, 70% (n=965) were single, and only 15% (n=205) had chronic diseases. About 96.5% (n=1285) of 97% (n=1332) had two doses, mostly Pfizer's first and second doses (82% and 78, respectively) while ~3.5% (n=47) had one. No acute COVID infection appeared. The majority (77%; n=1057) reported no issues pre-vaccination except 23%(n=315) of whom 43% (n=135) reported worsening issues post-vaccination. However, 47.2% (n=629) complained only post-vaccination particularly after dose-2 (59% (n=370). These were mostly multiple simultaneously occurring issue in 75% (n=471) on cycle-timing disruptions the rest were low frequencies of decreased blood, missed periods, increased blood volume, pain, or increased bleeding. Potential reasons were fear, stress, mental health, and/or emotional problems in 51% (n=674), while 53% (n = 701) were worried about the pandemic. Although proportional differences between age-groups were significant (P =0.05), the relative frequency was highest in ages 30-39 (51%). Significant proportional differences in groups of (Pfizer, Moderna, Oxford, Don't know) occurred in outcomes post first (0.047) and second (0.049) doses. However, relative frequencies of outcomes were higher in Pfizer and Moderna. Logistic regression revealed postgraduate [OR=2.11 (0.98-4.72), P = 0.015) employment [OR=2.18 (0.95-4.86), P = 0.049]and Pfizer vaccine [OR = 2.09 (0.96-4.10), P= 0.029] two doses [OR=3.21(1.23-5.21), P = 0.030] as significant predictors. Mental health and emotional factors such as fear, worries, and emotional problems that triggered stress were also associated [OR=1.78 (0.76-3.21), P=0.033]. However, all other variables were not associated with menorrhea disturbances. Thus, menstrual disturbance was significantly associated with vaccina-tions. Fear, stress, mental health, worries about the pandemic, and/or emotional problems were the major reasons reported. Apart from direct viral interactions, these findings are consistent with the emerging evidence on indirect stress- and microbiome-induced stimulations. This is plausible in the absence of significant factors related to old-age, chronic diseases, and lifestyle-behaviors. These findings have significant implications in women’s health, gender-based interpretation, and vaccine improvement strategies. Future vertical studies on cortisol response and the consequence of uterine-dysbiosis in manipulating immune-response is warranted.
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Sample Size and Sampling Procedure
2.3. Data Collection Tool and Interpretations of Patients’ Responses
2.4. Ethics Approval
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- COVID-19 cases | WHO COVID-19 dashboard. Available online: https://data.who.int/dashboards/covid19/cases?n=c (accessed on 29 February 2024).
- Saudagar, V.; Patil, S.; Goh, S.; Pothiawala, S. Vigilance Regarding Immune Thrombocytopenic Purpura after COVID-19 Vaccine. Ir J Med Sci 2022, 191, 919. [Google Scholar] [CrossRef]
- Rodríguez Quejada, L.; Toro Wills, M. F.; Martínez-Ávila, M. C.; Patiño-Aldana, A. F. Menstrual Cycle Disturbances after COVID-19 Vaccination. Womens Health (Lond) 2022, 18. [Google Scholar] [CrossRef]
- Baena-García, L.; Aparicio, V. A.; Molina-López, A.; Aranda, P.; Cámara-Roca, L.; Ocón-Hernández, O. Premenstrual and Menstrual Changes Reported after COVID-19 Vaccination: The EVA Project. Womens Health (Lond) 2022, 18. [Google Scholar] [CrossRef] [PubMed]
- Trogstad, L.; Laake, I.; Robertson, A. H.; Mjaaland, S.; Caspersen, I. H.; Juvet, L. K.; Magnus, P.; Blix, K.; Feiring, B. Heavy Bleeding and Other Menstrual Disturbances in Young Women after COVID-19 Vaccination. Vaccine 2023, 41, 5271–5282. [Google Scholar] [CrossRef]
- Farland, L. V.; Khan, S. M.; Shilen, A.; Heslin, K. M.; Ishimwe, P.; Allen, A. M.; Herbst-Kralovetz, M. M.; Mahnert, N. D.; Pogreba-Brown, K.; Ernst, K. C.; Jacobs, E. T. COVID-19 Vaccination and Changes in the Menstrual Cycle among Vaccinated Persons. Fertil Steril 2023, 119, 392–400. [Google Scholar] [CrossRef] [PubMed]
- Rastegar, T.; Feryduni, L.; Fakhraei, M. COVID-19 Vaccine Side Effects on Menstrual Disturbances among Iranian Women. New Microbes New Infect 2023, 53. [Google Scholar] [CrossRef]
- Kareem, R.; Sethi, M. R.; Inayat, S.; Irfan, M. The Effect of COVID-19 Vaccination on the Menstrual Pattern and Mental Health of the Medical Students: A Mixed-Methods Study from a Low and Middle-Income Country. PLoS One 2022, 17. [Google Scholar] [CrossRef] [PubMed]
- Alghamdi, A. N.; Alotaibi, M. I.; Alqahtani, A. S.; Al Aboud, D.; Abdel-Moneim, A. S. BNT162b2 and ChAdOx1 SARS-CoV-2 Post-Vaccination Side-Effects Among Saudi Vaccinees. Front Med (Lausanne) 2021, 8. [Google Scholar] [CrossRef] [PubMed]
- Shabu, A.; Nishtala, P. S. Safety Outcomes Associated with the Moderna COVID-19 Vaccine (MRNA-1273): A Literature Review. Expert Rev Vaccines 2023, 22, 393–409. [Google Scholar] [CrossRef] [PubMed]
- Meo, S. A.; Bukhari, I. A.; Akram, J.; Meo, A. S.; Klonoff, D. C. COVID-19 Vaccines: Comparison of Biological, Pharmacological Characteristics and Adverse Effects of Pfizer/BioNTech and Moderna Vaccines. Eur Rev Med Pharmacol Sci 2021, 25, 1663–1679. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Mateus, J.; Coelho, C. H.; Dan, J. M.; Moderbacher, C. R.; Gálvez, R. I.; Cortes, F. H.; Grifoni, A.; Tarke, A.; Chang, J.; Escarrega, E. A.; Kim, C.; Goodwin, B.; Bloom, N. I.; Frazier, A.; Weiskopf, D.; Sette, A.; Crotty, S. Humoral and Cellular Immune Memory to Four COVID-19 Vaccines. Cell 2022, 185, 2434–2451.e17. [Google Scholar] [CrossRef] [PubMed]
- Yadav, T.; Kumar, S.; Mishra, G.; Saxena, S. K. Tracking the COVID-19 Vaccines: The Global Landscape. Hum Vaccin Immunother 2023, 19. [Google Scholar] [CrossRef]
- Benner, M.; Ferwerda, G.; Joosten, I.; van der Molen, R. G. How Uterine Microbiota Might Be Responsible for a Receptive, Fertile Endometrium. Hum Reprod Update 2018, 24, 393–415. [Google Scholar] [CrossRef] [PubMed]
- Winters, A. D.; Romero, R.; Gervasi, M. T.; Gomez-Lopez, N.; Tran, M. R.; Garcia-Flores, V.; Pacora, P.; Jung, E.; Hassan, S. S.; Hsu, C. D.; Theis, K. R. Does the Endometrial Cavity Have a Molecular Microbial Signature? Sci Rep 2019, 9. [Google Scholar] [CrossRef] [PubMed]
- Pelzer, E. S.; Willner, D.; Buttini, M.; Huygens, F. A Role for the Endometrial Microbiome in Dysfunctional Menstrual Bleeding. Antonie van Leeuwenhoek, International Journal of General and Molecular Microbiology 2018, 111, 933–943. [Google Scholar] [CrossRef] [PubMed]
- Maher, M.; O’ Keeffe, A.; Phelan, N.; Behan, L. A.; Collier, S.; Hevey, D.; Owens, L. Female Reproductive Health Disturbance Experienced During the COVID-19 Pandemic Correlates With Mental Health Disturbance and Sleep Quality. Front Endocrinol (Lausanne) 2022, 13, 838886. [Google Scholar] [CrossRef] [PubMed]
- Phelan, N.; Behan, L. A.; Owens, L. The Impact of the COVID-19 Pandemic on Women’s Reproductive Health. Front Endocrinol (Lausanne) 2021, 12. [Google Scholar] [CrossRef] [PubMed]
- Nazzal, W.; Al-Maqati, T. N.; Almulhim, M. A.; Alsulmi, E. S.; Alotaibi, J. F.; AlBahrani, S.; Alsuhaibani, O.; Alenezi, E. H.; Albusaili, S.; Alharbi, A.; Alqahtani, A.; Alahmari, F.; Alshahrani, A.; Al Otaibi, D. A.; Alfaifi, A. H.; Madkhali, O. A. Saudi Women’s Perception of the Effect of COVID-19 Infection and Vaccination on Menstrual Cycle Length. Womens Health Rep (New Rochelle) 2024, 5, 495–502. [Google Scholar] [CrossRef]
- Ozimek, N.; Velez, K.; Anvari, H.; Butler, L.; Goldman, K. N.; Woitowich, N. C. Impact of Stress on Menstrual Cyclicity During the Coronavirus Disease 2019 Pandemic: A Survey Study. J Womens Health 2022, 31, 84–90. [Google Scholar] [CrossRef] [PubMed]
- Tripathy, S.; Preethika, A.; Sajeetha Kumari, R.; Anuradha, M.; Mohapatra, S. The Potential Impact of COVID-19 on Women’s Reproductive and Mental Health: A Questionnaire Study. J Obstet Gynaecol (Lahore) 2022, 42, 3328–3335. [Google Scholar] [CrossRef] [PubMed]
- Bruinvels, G.; Blagrove, R. C.; Goldsmith, E.; Shaw, L.; Martin, D.; Piasecki, J. How Lifestyle Changes during the COVID-19 Global Pandemic Affected the Pattern and Symptoms of the Menstrual Cycle. Int J Environ Res Public Health 2022, 19. [Google Scholar] [CrossRef] [PubMed]
- Barsom, S. H.; Mansfield, P. K.; Koch, P. B.; Gierach, G.; West, S. G. Association between Psychological Stress and Menstrual Cycle Characteristics in Perimenopausal Women. Womens Health Issues 2004, 14, 235–241. [Google Scholar] [CrossRef] [PubMed]
- Haji Seyed Javadi, S. A.; Shafikhani, A. A. Anxiety and Depression in Patients with Gastroesophageal Reflux Disorder. Electron Physician 2017, 9, 5107–5112. [Google Scholar] [CrossRef] [PubMed]
- Sibelli, A.; Chalder, T.; Everitt, H.; Workman, P.; Windgassen, S.; Moss-Morris, R. A Systematic Review with Meta-Analysis of the Role of Anxiety and Depression in Irritable Bowel Syndrome Onset. Psychol Med 2016, 46, 3065–3080. [Google Scholar] [CrossRef]
- Duran-Pinedo, A. E.; Solbiati, J.; Frias-Lopez, J. The Effect of the Stress Hormone Cortisol on the Metatranscriptome of the Oral Microbiome. NPJ Biofilms Microbiomes 2018, 4. [Google Scholar] [CrossRef]
- Yildiz, E.; Timur, B.; Guney, G.; Timur, H. Does the SARS-CoV-2 MRNA Vaccine Damage the Ovarian Reserve? Medicine 2023, 102, E33824. [Google Scholar] [CrossRef]
- Conti, P.; Younes, A. Coronavirus COV-19/SARS-CoV-2 Affects Women Less than Men: Clinical Response to Viral Infection. J Biol Regul Homeost Agents 2020, 34, 339–343. [Google Scholar] [CrossRef]
- Turke, P. W. Five Reasons COVID-19 Is Less Severe in Younger Age-Groups. Evol Med Public Health 2021, 9, 113. [Google Scholar] [CrossRef] [PubMed]
- Fish, E. N. The X-Files in Immunity: Sex-Based Differences Predispose Immune Responses. Nat Rev Immunol 2008, 8, 737. [Google Scholar] [CrossRef] [PubMed]
- Baker, J. M.; Chase, D. M.; Herbst-Kralovetz, M. M. Uterine Microbiota: Residents, Tourists, or Invaders? Front Immunol 2018, 9. [Google Scholar] [CrossRef]
- Said, K. B.; Al-Otaibi, A.; Aljaloud, L.; Al-Anazi, B.; Alsolami, A.; Alreshidi, F. S. The Frequency and Patterns of Post-COVID-19 Vaccination Syndrome Reveal Initially Mild and Potentially Immunocytopenic Signs in Primarily Young Saudi Women. Vaccines (Basel) 2022, 10, 1015. [Google Scholar] [CrossRef]
- Foster, J. A.; Rinaman, L.; Cryan, J. F. Stress & the Gut-Brain Axis: Regulation by the Microbiome. Neurobiol Stress 2017, 7, 124–136. [Google Scholar] [CrossRef]
- Nazir, M.; Asghar, S.; Rathore, M. A.; Shahzad, A.; Shahid, A.; Ashraf Khan, A.; Malik, A.; Fakhar, T.; Kausar, H.; Malik, J. Menstrual Abnormalities after COVID-19 Vaccines: A Systematic Review. [CrossRef]
- Meringer, H.; Mehandru, S. Gastrointestinal Post-Acute COVID-19 Syndrome. Nat Rev Gastroenterol Hepatol 2022, 19, 345. [Google Scholar] [CrossRef] [PubMed]
- Creed, F. Risk Factors for Self-Reported Irritable Bowel Syndrome With Prior Psychiatric Disorder: The Lifelines Cohort Study. J Neurogastroenterol Motil 2022, 28, 442–453. [Google Scholar] [CrossRef] [PubMed]
- Yarandi, S. S. Overlapping Gastroesophageal Reflux Disease and Irritable Bowel Syndrome: Increased Dysfunctional Symptoms. World J Gastroenterol 2010, 16, 1232. [Google Scholar] [CrossRef] [PubMed]
- Martinson, M. L.; Lapham, J.; Ercin-Swearinger, H.; Teitler, J. O.; Reichman, N. E. Generational Shifts in Young Adult Cardiovascular Health? Millennials and Generation X in the United States and England. J Gerontol B Psychol Sci Soc Sci 2022, 77 (Suppl 2), S177. [Google Scholar] [CrossRef] [PubMed]
- Demir, O.; Sal, H.; Comba, C. Triangle of COVID, Anxiety and Menstrual Cycle. J Obstet Gynaecol (Lahore) 2021, 41, 1257–1261. [Google Scholar] [CrossRef]
- Hunter, P. R. Thrombosis after Covid-19 Vaccination. bmj. British Medical Journal Publishing Group 2021. [CrossRef] [PubMed]
| Characteristics (n=1372) | Frequency | Percent | |
|---|---|---|---|
| Age (years) | <18 | 216 | 15.7 |
| 19-29 | 838 | 61.1 | |
| 30-39 | 175 | 12.8 | |
| 40-50 | 143 | 10.4 | |
| Nationality | Non-Saudi | 80 | 5.8 |
| Saudi | 1292 | 94.2 | |
| Region | Central Region | 303 | 22.1 |
| Eastern Region | 402 | 29.3 | |
| Southern area | 73 | 5.3 | |
| Northern area | 305 | 22.2 | |
| Western Region | 289 | 21.1 | |
| Educational | No primary education | 7 | 0.5 |
| Elementary or Intermediate | 70 | 5.1 | |
| Secondary | 331 | 24.1 | |
| Graduate | 911 | 66.4 | |
| Postgraduate | 53 | 3.9 | |
| Employment status | Employed | 182 | 13.3 |
| House wife | 306 | 22.3 | |
| Retired | 25 | 1.8 | |
| Social status | Married | 407 | 29.7 |
| Single | 965 | 70.3 | |
| Chronic diseases | No | 1167 | 85.1 |
| Yes | 205 | 14.9 | |
| Type of Chronic diseases (n=205) | Cardiovascular disease | 3 | 1.5 |
| Blood diseases | 28 | 13.7 | |
| Diabetes | 15 | 7.3 | |
| Hypertension | 20 | 9.8 | |
| Kidney disease | 2 | 1.0 | |
| Respiratory system diseases | 33 | 16.1 | |
| Rheumatic diseases | 10 | 4.9 | |
| Liver diseases | 1 | .5 | |
| Other diseases | 60 | 29.3 | |
| Multiple diseases | 33 | 16.1 | |
| Medications | No | 1177 | 85.8 |
| Yes | 195 | 14.2 | |
| Type of medications used (n=195) | Anti-hypertensive medications | 24 | 12.3 |
| Insulin | 22 | 11.3 | |
| Cardiovascular medications | 4 | 2.1 | |
| Salbutamol | 11 | 5.6 | |
| Other medications | 107 | 54.9 | |
| Multiple medications | 27 | 13.8 | |
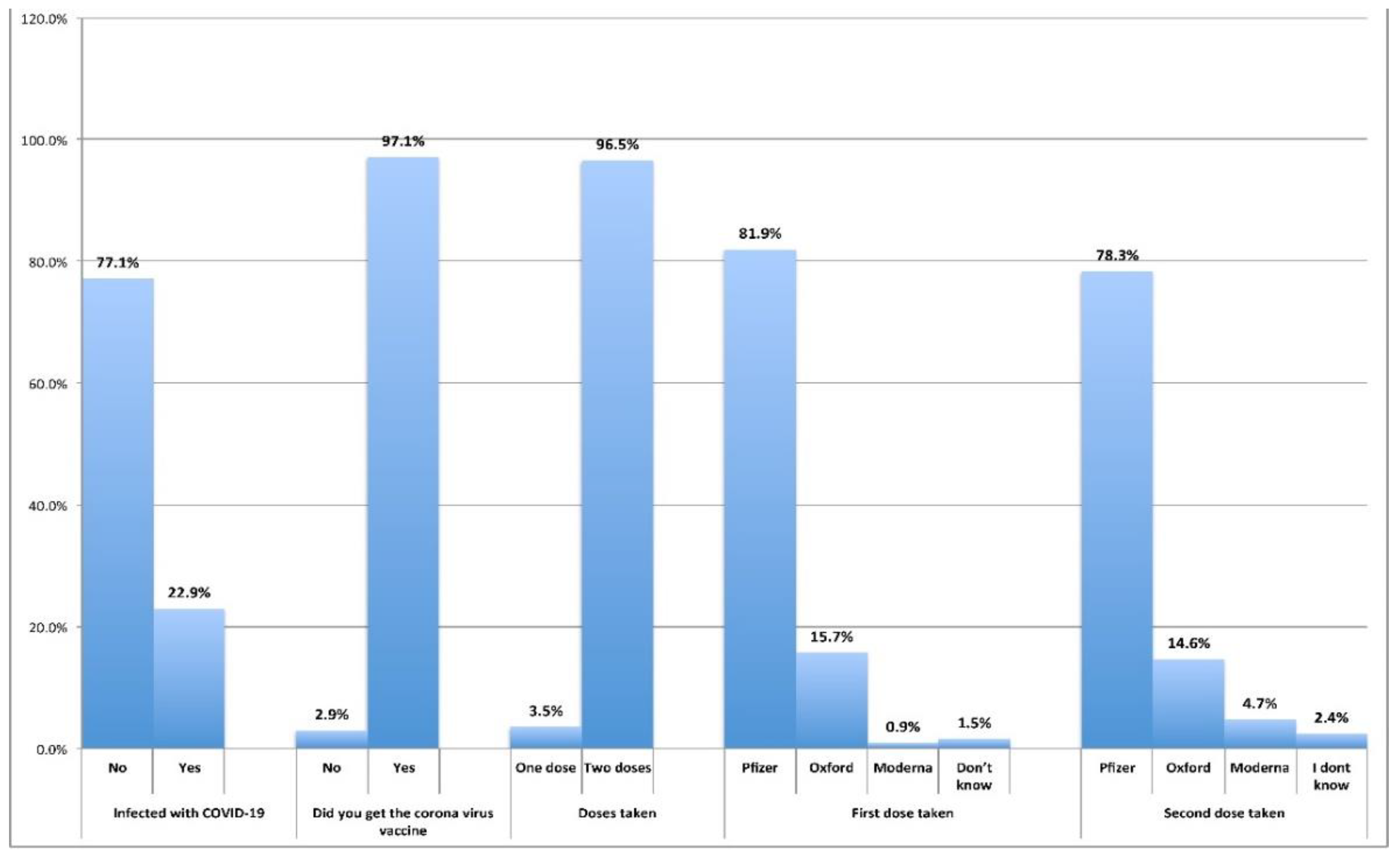
| N | % | ||
|---|---|---|---|
| Infected with SARS-CoV-2 | No | 1058 | 77.1 |
| Yes | 314 | 22.9 | |
| Received COVID-19 vaccine | No | 40 | 2.9 |
| Yes | 1332 | 97.1 | |
| Doses taken (n=1332) | One dose | 47 | 3.5 |
| Two doses | 1285 | 96.5 | |
| First dose taken (n=1332) |
Pfizer | 1091 | 81.9 |
| Oxford | 209 | 15.7 | |
| Moderna | 12 | 0.9 | |
| Don’t know | 20 | 1.5 | |
| Second dose taken (n=1285) |
Pfizer | 1006 | 78.3 |
| Oxford | 187 | 14.6 | |
| Moderna | 61 | 4.7 | |
| Don't know | 31 | 2.4 | |
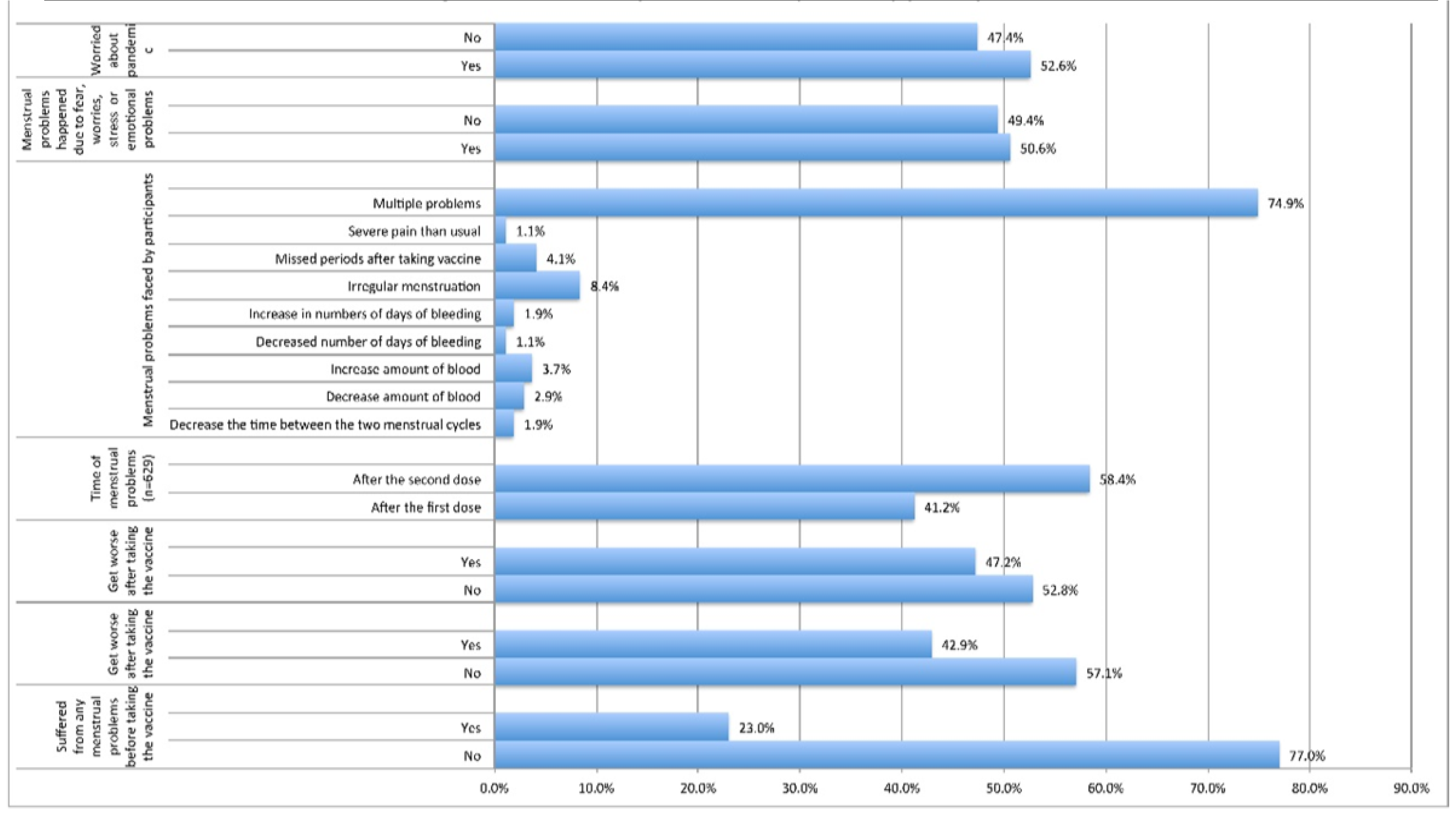
| N | % | ||
|---|---|---|---|
| Suffered from any menstrual problems before taking the vaccine (n=1332) | No | 1057 | 77.0 |
| Yes | 315 | 23.0 | |
| Get worse after taking the vaccine (n=315 of respondents said Yes) |
No | 180 | 57.1 |
| Yes | 135 | 42.9 | |
| Did you have any menstrual problems after taking the vaccine (n=1332) | No | 703 | 52.8 |
| Yes | 629 | 47.2 | |
| Time of menstrual problems (of n=629 who responded Yes to issues after vaccination) |
After the first dose | 259 | 41.2 |
| After the second dose | 370 | 58.8 | |
| Types of menstrual problems reported by participants (n=629) |
Decrease the time between the two menstrual cycles | 12 | 1.9 |
| Decrease amount of blood | 18 | 2.9 | |
| Increase amount of blood | 23 | 3.7 | |
| Decreased number of days of bleeding | 7 | 1.1 | |
| Increase in numbers of days of bleeding | 12 | 1.9 | |
| Irregular menstruation | 53 | 8.4 | |
| Missed periods after taking vaccine | 26 | 4.1 | |
| Severe pain than usual | 7 | 1.1 | |
| Simultaneous multiple menstrual problems | 471 | 74.9 | |
| Menstrual problems happened due to fear, worries, stress and or emotional problems (n=1332) | Yes | 674 | 50.6 |
| No | 658 | 49.4 | |
| Worried about pandemic (n=1332) | Yes | 701 | 52.6 |
| No | 631 | 47.4 | |
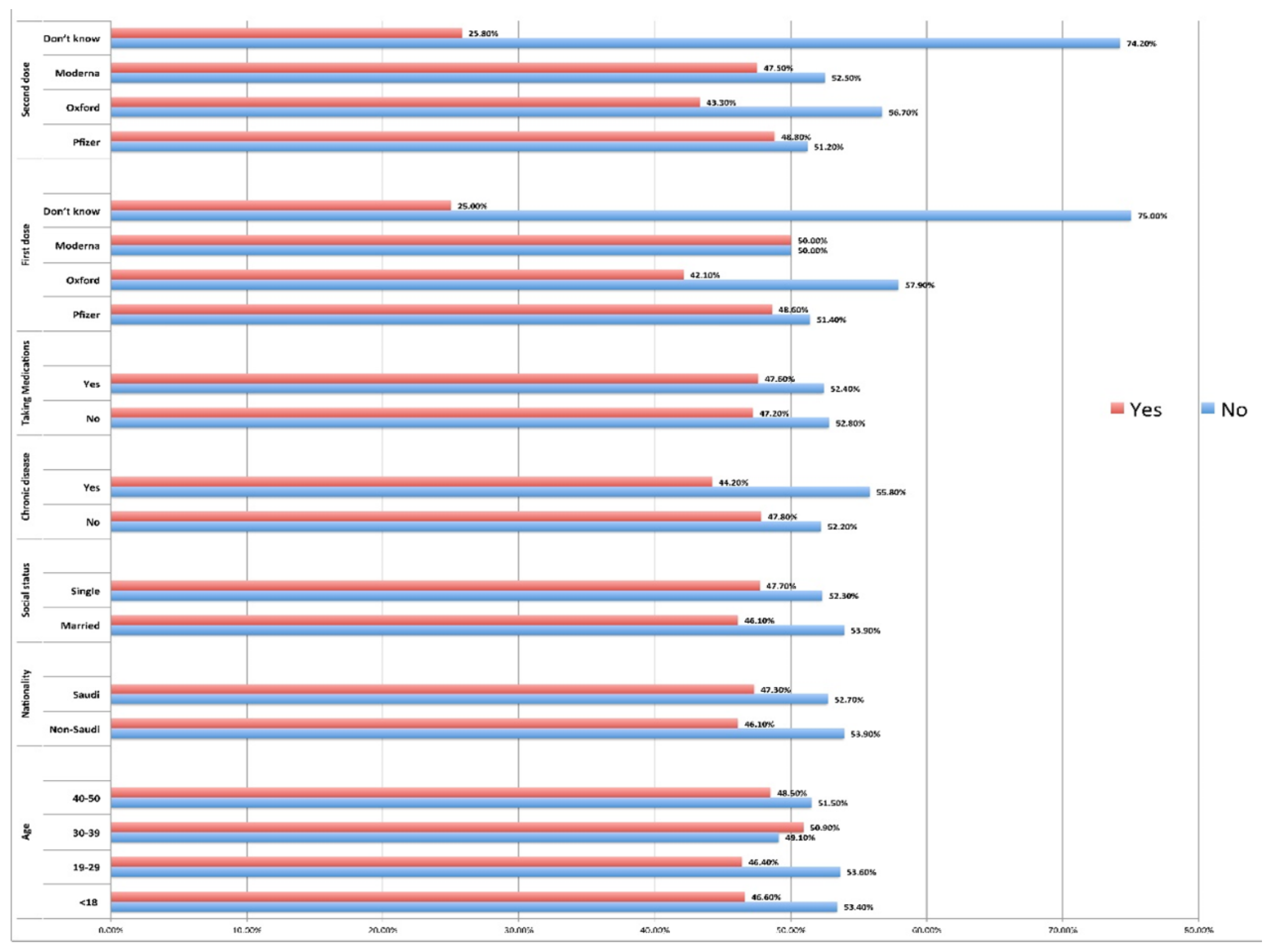
|
Menstrual problems after taking the vaccine* *(n) for each character = (yes+no) |
p value | |||
| No | Yes | |||
| Age | 12-18 | 109 | 95 | 0.05 |
| 53.4% | 46.6% | |||
| 19-29 | 439 | 380 | ||
| 53.6% | 46.4% | |||
| 30-39 | 85 | 88 | ||
| 49.1% | 50.9% | |||
| 40-50 | 70 | 66 | ||
| 51.5% | 48.5% | |||
| Nationality | Non-Saudi | 41 | 35 | 0.833 |
| 53.9% | 46.1% | |||
| Saudi | 662 | 594 | ||
| 52.7% | 47.3% | |||
| Social status | Married | 214 | 183 | 0.592 |
| 53.9% | 46.1% | |||
| Single | 489 | 446 | ||
| 52.3% | 47.7% | |||
| Chronic disease | No | 593 | 542 | 0.351 |
| 52.2% | 47.8% | |||
| Yes | 110 | 87 | ||
| 55.8% | 44.2% | |||
| Taking medication | No | 605 | 540 | 0.913 |
| 52.8% | 47.2% | |||
| Yes | 98 | 89 | ||
| 52.4% | 47.6% | |||
| First dose | Pfizer (n=1091) |
561 | 530 | 0.047 |
| 51.4% | 48.6% | |||
| Oxford (n = 209) |
121 | 88 | ||
| 57.9% | 42.1% | |||
| Moderna (n = 12) |
6 | 6 | ||
| 50.0% | 50.0% | |||
| I don’t know (n = 20) |
15 | 5 | ||
| 75.0% | 25.0% | |||
| Second dose | Pfizer | 515 | 491 | 0.049 |
| 51.2% | 48.8% | |||
| Oxford | 106 | 81 | ||
| 56.7% | 43.3% | |||
| Moderna | 32 | 29 | ||
| 52.5% | 47.5% | |||
| I don’t know | 23 | 8 | ||
| 74.2% | 25.8% | |||
| Dependent variable = menorrhea disturbances | Odd’s Ratio | 95% confidence interval | p value | |
|---|---|---|---|---|
| Age(=19-29years) | 2.07 | 0.66 | 6.50 | 0.209 |
| Nationality | 0.57 | 0.25 | 1.29 | 0.181 |
| Region | 1.17 | 0.62 | 2.19 | 0.624 |
| Education=Postgraduate | 2.11 | 0.98 | 4.72 | 0.015 |
| Employment | 2.18 | 0.95 | 4.86 | 0.049 |
| Social status | 1.76 | 0.94 | 3.31 | 0.076 |
| Chronic diseases | 0.91 | 0.47 | 1.74 | 0.781 |
| Medications | 0.95 | 0.65 | 1.39 | 0.775 |
| Type of vaccine taken= Pfizer | 2.09 | 0.96 | 4.10 | 0.029 |
| Doses taken= 2 doses | 1.59 | 0.74 | 3.29 | 0.014 |
| Suffered from any menstrual problems before taking vaccine | 0.91 | 0.45 | 2.21 | 0.412 |
| Menstrual problems occurred after the second dose | 3.21 | 1.23 | 5.21 | 0.030 |
| Period is affected by fear, worries, stress, or any emotional problems | 1.78 | 0.76 | 3.21 | 0.033 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




