Submitted:
30 October 2024
Posted:
31 October 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods &Materials
- Cancer Care Ontario resources
- The Right Time for the Pap Test brochure
- Videos from Ontario Health: Hamilton FHT
- Negative Results: Participants with negative results received a letter from the research team, advising them to follow provincial guidelines and undergo routine screening in five years. If a primary care provider’s contact information was provided, they also received a notification.
- Positive Results: Participants with positive results received a letter advising them to follow up with their primary care provider for a Pap test. A member of the research team also called them directly. If a primary care provider’s contact information was provided, they were sent a letter.
3. Data Analysis
4. Results
4.1. Section A: Participants Socio-Demographic and Clinical Characteristics
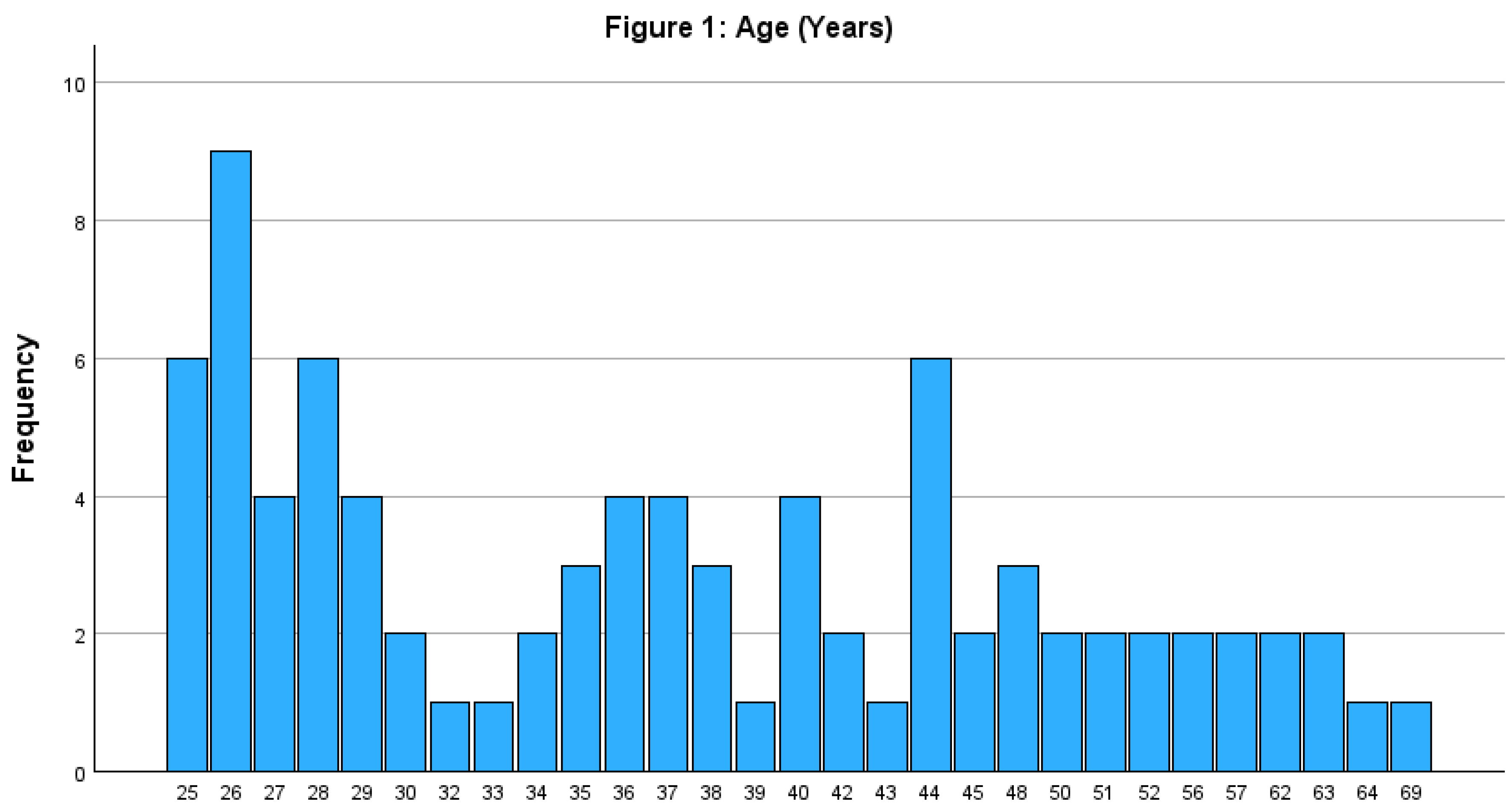
4.1.1. Sociodemographic Characteristics
4.1.2. Clinical Characteristics
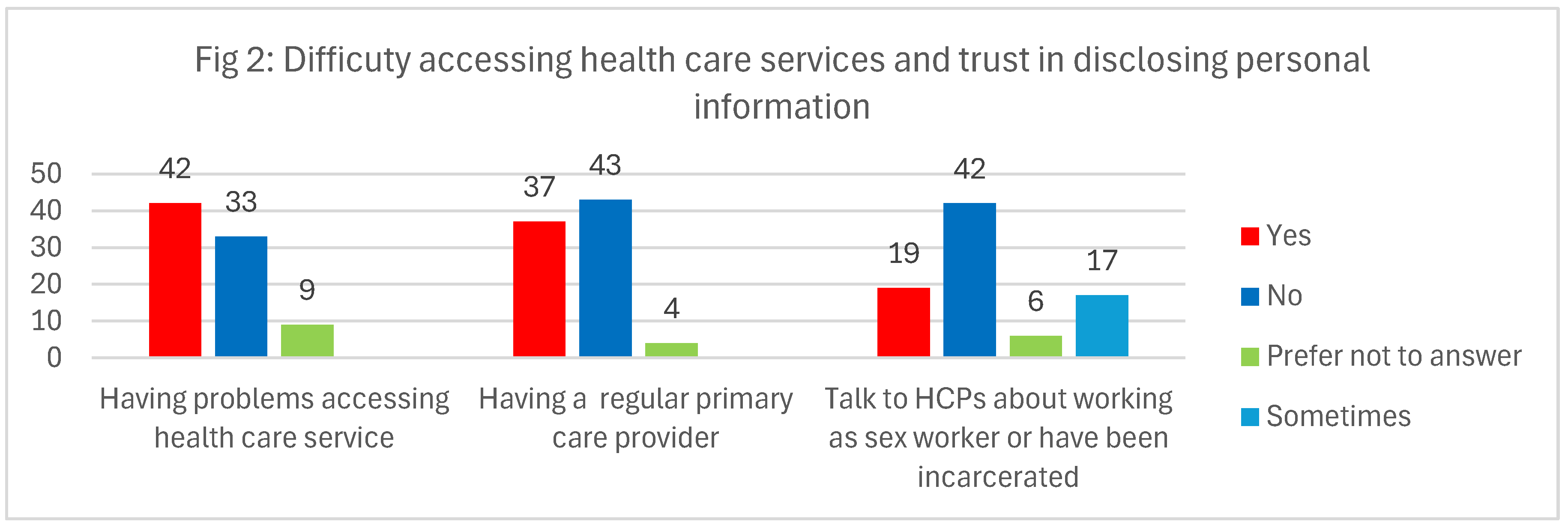
4.2. Section B: Access to Health Services
4.3. Section C. Perceived Risk of Encountering Cervical Cancer
4.4. Section D. Knowledge of Cervical Cancer and Screening
4.4.1. Cervical Cancer
4.4.2. Pap-Test
4.4.3. HPV Screening
4.5. Section E. Perceived Stigma During Medical Encounters or Other Social Interactions
4.6. Section F: HPV-SS Uptake and Perceived Motivators and Barriers
4.6.1. HPV-SS Uptake
4.6.2. Perceived Motivators for Utilizing HPV Self-Sampling
4.6.3. Potential Barriers in Using HPV-SS
4.7. Section G: Reasons for Not Opting for HPV-SS
5. Discussion
6. Conclusion
Author Contributions
Funding
Data Availability
Acknowledgments
Competing interests
Abbreviations
| CC: Cervical cancer |
| Greater Toronto Area: GTA |
| HPV: Human papillomavirus |
| HPV-SS: Human papillomavirus Self-Sampling |
| Pap test: Papanicolaou test |
| RA: Research Associate |
| STIs: Sexually transmissible/transmitted infections |
| UNS: Under or never screened |
References
- Canadian Cancer Society - The annual report – Canadian Cancer Statistics 2023. p. 20. https://cdn.cancer.ca/-/media/files/research/cancer-statistics/2023-statistics/2023_pdf_en.pdf?rev=7e0c86ef787d425081008ed22377754d&hash=DBD6818195657364D831AF0641C4B45C&_gl=1*120rhkl*_gcl_au*ODg5OTY4NDgyLjE3MTMyMTQ2NTAC.
- Canadian Cancer Society, Risk factors for Cervical Cancer. https://cancer.ca/en/cancer-information/cancer-types/cervical/risks.
- Canadian Cancer Society, Cervical Cancer Statistics. https://cancer.ca/en/cancer-information/cancer-types/cervical/statistics.
- Cervical Screening: Cancer Care Ontario; https://www.cancercareontario.ca/en/types-of-cancer/cervical/screening.
- Ghebre RG, Grover S, Xu MJ, Chuang LT, Simonds H. Cervical cancer control in HIV-infected women: past, present and future. Gynecologic oncology reports. 2017 Aug 1;21:101-8. [CrossRef]
- Cohen PA, Jhingran A, Oaknin A, Denny L. Cervical cancer. The Lancet. 2019 Jan 12;393(10167):169-82.
- Roura E, Castellsague X, Pawlita M, Travier N, Waterboer T, Margall N, Bosch FX, De Sanjosé S, Dillner J, Gram IT, Tjønneland A. Smoking as a major risk factor for cervical cancer and pre-cancer: Results from the EPIC cohort. International journal of cancer. 2014 Jul 15;135(2):453-66. [CrossRef]
- Brenner DR, Gillis JL, Demers A, Ellison LF, Billette JM, Zhang SX, Liu J, Woods, RR, Finley C, Fitzgerald N, Saint-Jacques N, Shack L, Turner D, for the Canadian Cancer Statistics Advisory Committee. Projected estimates of cancer in Canada in 2024. CMAJ 2024 May 13;196:E615-23. [CrossRef]
- Vahabi, M., Lofters, A, Kim, E., Wong, J., Ellison,L, Graves, E, Glazier R.H. (2017).Breast cancer screening among women from Muslim-majority countries in Ontario, Canada. Preventive Medicine, 105:176-183. Published online September 13, 2017. [CrossRef]
- Vahabi, M., Lofters, A. (2018). HPV self-sampling: A promising approach to reduce cervical cancer screening disparities in Canada, Current Oncology, Special issue (HPV self-sampling in promoting cervical cancer screening), 25 (1):13-18, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5832271/. http://doi.org/10.3747/co.25.3845.
- Lofters, A., Kopp, A., Vahabi, M., Glazier R.H. (2019) Understanding Those Overdue For Cancer Screening By Five Years Or More: A Retrospective Cohort Study In Ontario, Canada. Preventive Medicine. 26(10):1493-1499. [CrossRef]
- Wong, J. Vahabi, M., Miholjcic, J., Tan, V., Owino, M., Li, A., Poon, M. (2018). Knowledge of HPV/cervical cancer and acceptability of HPV self-sampling among women living with HIV: A scoping review. Current Oncology, Special issue (HPV self-sampling in promoting cervical cancer screening), 25 (1): e73-e82. [CrossRef]
- Lofters, A., Vahabi, M., Kim, E., Ellison, L, Graves, E, Glazier R.H. (2017) Cervical cancer screening among women from Muslim majority countries in Ontario, Canada. Cancer Epidemiology, Biomarkers & Prevention, 26(10):1493-9. [CrossRef]
- McDonald, J.T., Kennedy, S. (2007). Cervical cancer screening by immigrant and minority women in Canada. Journal of Immigrant Minority Health, 9: 323-334. [CrossRef]
- Ross, L. E., Sterling, A., Dobinson, C., Logie, C. H., & D'Souza, S. (2021). Access to sexual and reproductive health care among young adult sex workers in Toronto, Ontario: a mixed-methods study. CMAJ Open, 9(2), E482–E490. [CrossRef]
- Duff, P., Ogilvie, G., Shoveller, J., Amram, O., Chettiar, J., Nguyen, P., Dobrer, S., Montaner, J., & Shannon, K. (2016). Barriers to Cervical Screening Among Sex Workers in Vancouver. American Journal of Public Health (1971), 106(2), 366–373. [CrossRef]
- Sex work in Canada: the public health perspective. Ottawa: Canadian Public Health Association; 2014. Available: www.cpha.ca/sites/default/files/assets/policy/sex-work_e.pdf.(accessed 2022 Dec. 15).
- UNAIDS welcomes the decision by the Northern Territory of Australia to decriminalize sex work [news release]. Geneva: UNAIDS; 2019. Available: www.unaids.org/en/resources/presscentre/pressreleaseandstatementarchive/2019/december/decision-northern-territory-australia-decriminalize-sex-work.(accessed 2022 Dec. 5).
- Lazarus, L., Deering, K. N., Nabess, R., Gibson, K., Tyndall, M. W., & Shannon, K. (2012). Occupational stigma as a primary barrier to health care for street-based sex workers in Canada. Culture, Health & Sexuality, 14(2), 139–150. [CrossRef]
- Benoit, C., Jansson, S. M., Smith, M., & Flagg, J. (2018). Prostitution Stigma and Its Effect on the Working Conditions, Personal Lives, and Health of Sex Workers. The Journal of Sex Research, 55(4-5), 457–471. [CrossRef]
- Saslaw, D., Solomon, D., Lawson, H.W., Killackey, M., Kulasingam, S.L., Cain, J. et al., (2012). American Cancer Society, American Society for Colposcopy and Cervical Pathology, and American for Clinical Pathology Screening guidelines for the prevention and early detection of cervical cancer. American Journal of Pathology, 137(4): 516-542.
- Petignant, P., Vassilakos, P. (2012). Is it time to introduce HPV self-sampling for primary cervical cancer screening? Journal of National Cancer Institute, 104(3): 166-167.
- Agorastos, T., Sotiriadis, A., Chatzigeorgiou, K. (2010). Can HPV testing replace the Pap smear? Annals of the New York Academy of Sciences, 1205: 51-56.
- Bhatla, N., Dar, L., Patro, A.R., Kumar, P., Kriplani, A., Gulati, A, et Al., (2009). Can human papilliomavirus DNA testing of self-collected vaginal samples compares with physician-collected cervical samples and cytology for cervical cancer screening in developing countries? Cancer Epidemiology, 33(6): 446-450.
- Schiffman, M., Wentzensen, N., Wacholders, S., Kinney, W., Gage,J.C., Castle, P.E. (2011). Human papilliomavirus testing in the prevention of cervical cancer, Journal of National Cancer Institute, 103(5): 368-383.
- Wright, T.C., (2007). Cervical cancer screening in the 21st century: Is it time to retire the Pap smear? Clinical Obstetrics & Gynecology, 50(2): 313-323.
- Ogilvie, G., Krajden, M., Maginley, J., Isaac-Renton, J., Hislop,, G., Elwood-Martin, R., et al. (2007). Feasibility of self-collected of specimens for human papillomavirus testing in hard to reach women. Canadian Medical Association Journal, 177(5): 480-483. [CrossRef]
- Khoo, S. P., Lim, W. T., Rajasuriar, R., Nasir, N. H., Gravitt, P., & Woo, Y. L. (2021). The acceptability and preference of vaginal self-sampling for human papillomavirus (HPV) testing among a multi-ethnic Asian female population. Cancer Prevention Research, 14(1), 105-112. [CrossRef]
- Vahabi, M, Kithulegoda, N., Wong, J, Lofters, A.K., (2024) Knowledge and Attitudes towards cervical cancer screening and acceptability of HPV self-sampling (HPV-SS) among under or never screened racialized immigrant women in GTA, Ontario, Canada, Journal of Environmental Science and Public Health. 2024; 8(2), 32-48, . [CrossRef]
- Lofters A, Devotta K, Prakash V, Vahabi M. Understanding the Acceptability and Uptake of HPV Self-Sampling Amongst Women Under- or Never-Screened for Cervical Cancer in Toronto (Ontario, Canada): An Intervention Study Protocol. Int J Environ Res Public Health. 2021;18(17):9114. Published 2021 Aug 29. [CrossRef]
- Vahabi, M., Mishra, G., Pimple, S., Wong, J. P.H., Khan, M., Prakash, V., Anand, K., Narushima, M., Lofters, A.K. 2023, Effectiveness of family-centred sexual health education and HPV self-sampling in promoting cervical cancer screening among hard-to-reach Indian women in rural and tribal areas: a community-based pilot study. BMC Public Health 23, 671 (2023). [CrossRef]
- Nelson, E. J., Maynard, B. R., Loux, T., Fatla, J., Gordon, R., & Arnold, L. D. (2017). The acceptability of self-sampled screening for HPV DNA: a systematic review and meta-analysis. Sexually transmitted infections, 93(1), 56-61. [CrossRef]
- Mitchelle, S., Ogilvie, G., Steinberg, M., Sekikubo, M., Biryabarema, C., Money, D. (2011). Assessing women’s willingness to collect their own cervical samples for HPV testing as part of ASPIRE cervical cancer screening project in Uganda. International Journal of Gynecology & Obstetrics, 114(2): 111-115. [CrossRef]
- Ogilvie G, Krajden M, Maginley J, Isaac-Renton J, Hislop G, Elwood-Martin R, Sherlock C, Taylor D, Rekart M. Feasibility of self-collection of specimens for human papillomavirus testing in hard-to-reach women. CMAJ. 2007 Aug 28;177(5):480-3. [CrossRef]
- Zhao, F.H., Lewkowitz, A.K., Chen, F., Lin, M.J., Hu, S.Y., Zhang, X., et al. (2012). Pooled analysis of a self-sampling HPV DNA test as a cervical cancer primary screening method, Journal of National Cancer Institute, 104(3): 178-188. [CrossRef]
- Virtanen, A., Nieminen, P., Lustarinen, T., Anttila, A. (2011). Self-sample HPV tests as an intervention for non-attendees of cervical cancer screening in Finland :A randomized trial, Cancer Epidemiology Biomarkers & Prevention, 20(9): 1960-1969.
- Ogilvie, G., Partrick, D.M., Schulzer, M., Sellors, J.W., Petric, M., Chambers, K., et al. (2005). Diagnostic accuracy of self-collected vaginal specimens for human papillomavirus testing compared to clinician collected human papillomavirus specimens: A meta-analysis. Sexually Transmitted Infection, 81 (3): 207-2012.
- Fernandes B, Dworkin S, Bunzeluk K, Turner D, Baldry L, Coulter L, et al. Elimination of cervical cancer in Canada: exploring invitation strategies for HPV self-sampling among under screened women [Poster Presentation]. ICSN 2023, Turin, Italy. 2023.
- Jalili F, O'Conaill C, Templeton K, Lotocki R, Fischer G, Manning L, Cormier K, Decker K. Assessing the impact of mailing self-sampling kits for human papillomavirus testing to unscreened non-responder women in Manitoba. Current Oncology. 2019 Jun;26(3):167-172. [CrossRef]
- Devotta, K., Vahabi, M., Prakash, V., Lofters, AK. 2023, Implementation of a Cervical Cancer Screening Intervention for Under- or Never-Screened Women in Ontario, Canada: Understanding the Acceptability of HPV Self-Sampling. Current Oncology. 30(7):6786-6804. [CrossRef]
- ICO/IARC Information Center on HPV and Cancer. Canada: Human Papillomavirus and related Cancer , Fact sheet 2023. https://hpvcentre.net/statistics/reports/CAN_FS.pdf.
- Kerrigan D, Kennedy CE, Morgan-Thomas R, Reza-Paul S, Mwangi P, Win KT, McFall A, Fonner VA, Butler J. A community empowerment approach to the HIV response among sex workers: effectiveness, challenges, and considerations for implementation and scale-up. Lancet. 2015 Jan 10;385(9963):172-85.
- Province to close 5 Toronto supervised drug consumption sites, CBC, https://www.cbc.ca/news/canada/toronto/toronto-supervised-injection-sites-ontario-restrictions-1.7299398.
| # of years | Frequency | Percent |
|---|---|---|
| Less than 1 year | 7 | 9.2 |
| 1-3 years | 21 | 27.6 |
| 3-4 years | 12 | 15.8 |
| 5-9 years | 15 | 19.7 |
| 10+ years | 16 | 21.1 |
| Prefer not to answer | 5 | 6.6 |
| Total | 76 | 100.0 |
| Types | Frequency | Percent |
|---|---|---|
| An agency escort | 8 | 9.5 |
| A fetish worker (i.e., Pro-Domme/sub) | 18 | 21.4 |
| An independent escort | 44 | 52.4 |
| A massage parlour attendant | 9 | 10.7 |
| An outdoor worker | 18 | 21.4 |
| Working for someone else (i.e., pimp, a manager) | 9 | 10.7 |
| A stripper | 12 | 14.3 |
| A porn performer | 6 | 7.1 |
| A sugar baby | 31 | 36.9 |
| A webcam host | 19 | 22.6 |
| Survival sex work: (sex work in exchange for basic needs/necessities (e.g., for food, shelter/housing, transportation, substances and/or medication or things you needed) | 25 | 29.8 |
Other- Please specify
|
2 | 2.4 |
| Prefer not to answer | 4 | 6.6 |
| Type of Employment | Frequency | Percent |
|---|---|---|
| House cleaner/nanny | 3 | 3.6 |
| Work in a bar, restaurant, or shack | 3 | 3.6 |
| Work in a public business | 7 | 8.3 |
| Work for a private business | 1 | 1.2 |
| Dancer or performance arts | 7 | 8.3 |
| Other (online sex work, sex work & bartending, PSW, Cam girl, sugar baby, harm reduction worker, student, community services) | 21 | 25.0 |
| Unemployed | 40 | 47.6 |
| Prefer not to answer | 2 | 2.4 |
| Total | 84 | 100.0 |
| Having engaged in sexual intercourse | |
| 84 (100) | |
| Age at first sexual intercourse | |
| 16 years old or less | 41 (48.8 ) |
| Over 16 years old | 39 (46.4) |
| Prefer not to answer | 4 (4.8) |
| Total | 84 (100) |
| Number of partners in the past 3 months | |
| 1 | 26 (31.0) |
| 2-5 | 29 (34.5) |
| 6-9 | 10 (11.9) |
| 10 or more | 11 (13.1) |
| Prefer not to answer | 8 (9.5) |
| Total | 84 (100.0) |
| Condom use during sex | |
| Always | 10 11.9 |
| Usually | 22 (26.2) |
| Sometimes | 27 (32.1) |
| Rarely | 11 (13.1) |
| Never | 10 (11.9) |
| Prefer not to answer | 4 (4.8) |
| Total | 84 (100.0) |
| Being diagnosed with Sexually transmitted infections (STIs) | |
| Yes | 43 (51.2) |
| No | 35 (41.7) |
| Don’t Know | 4 (4.8) |
| Preferred not to answer | 2 (2.4) |
| Total | 84 (100.0) |
| STIs | |
| Chlamydia | 20 (23.8) |
| Hepatitis | 3 (3.6) |
| Herpes | 7 (8.3) |
| Gonorrhea | 9 (10.7) |
| Syphilis, | 8 (9.5) |
| HIV/AIDS | 8 (9.5) |
| Pelvic inflammatory diseases | 3 (3.6) |
| Other STIs (genital wart, HPV) | 11 (13.1) |
| Abnormal discharge from vagina/ sore or ulcer near or on vagina/ pelvic pain in the past 6 months | |
| Yes | 20 (23.8%) |
| Number of participants who saw a health care provider for these problems | 8 (40%) |
| Number of people who were told to have a STI | 4 (50%) |
| Items | SD (%) | D (%) | Neutral (%) | A (%) | SA (%) | Mean | SD |
|---|---|---|---|---|---|---|---|
| 1. I do not seek healthcare because someone might learn that I am a sex worker or have been incarcerated | 16 (19.0) | 21 (25.0) |
21 (25.0) |
20 (23.8) |
6 (7.1) |
2.75 | 1.22 |
| 2. I have been denied health services or had someone keep me from receiving health services because I am a sex worker or have been incarcerated. | 13 (15.5) |
34 (40.5) |
15 (17.6) |
17 (20.2) |
5 (6) |
2.61 | 1.15 |
| 3. I have been verbally harassed when receiving health or social care because I am a sex worker or have been incarcerated. | 15 (17.9) |
22 (26.2) |
16 (19.0) |
20 (23.8) |
11 (13.1) |
2.88 | 1.32 |
| 4. I feel excluded from my friends and family because I am a sex worker or have been incarcerated. | 8 (9.5) |
17 (20.2) |
21 (25) |
24 (28.6) |
14 (16.7) |
3.23 | 1.23 |
| 5. Negative remarks or gossip was made by a family member about me because I am a sex worker or have been incarcerated. | 7 (8.3) |
15 (17.9) |
21 (25) |
22 (26.2) |
19 (22.6) |
3.37 | 1.25 |
| 6. Negative remarks or gossip was made by a healthcare worker about me because I am a sex worker or have been incarcerated. | 7 (8.3) |
25 (29.8) |
22 (26.2) |
17 (20.2) |
13 (15.5) |
3.05 | 1.21 |
| 7. Working as a sex worker or having a history of incarceration makes me feel that I do not have value. | 14 (16.7) |
18 (21.4) |
18 (21.4) |
16 (19.0) |
18 (21.4) |
3.07 | 1.40 |
| 8. People’s attitudes about sex workers or people who have been incarcerated make me feel worse about myself. | 10 (11.9) |
15 (17.9) |
16 (19.0) |
14 (16.7) |
27 (32.1) |
3.46 | 1.46 |
| 9. I work hard to keep my work as a sex worker or having been in prison a secret | 12 (14.3) |
12 (14.3) |
17 (20.2) |
17 (20.2) |
26 (31.0) |
3.39 | 1.42 |
| 10. It’s easier to avoid friendships than worry about telling others you are a sex worker. | 10 (11.9) |
15 (17.9) |
19 (22.6) |
20 (23.8) |
20 (23.8) |
3.30 | 1.33 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




