Obesity represents an important threat to national and global public health in terms of prevalence, incidence and economic burden [
1]. Over the past four decades, the worldwide prevalence of obesity has almost tripled [
2]. It was estimated in 2014, more than 2.1 billion people, nearly 30% of the global population, were overweight or obese and 5% of the deaths worldwide were attributable to obesity. If this trend continues, almost half of the world’s adult population will be overweight or obese by 2030 [
3].
The United States of America has one of the highest rates of obesity in the world, with over 40% of adults were estimated to have obesity in 2017–2018 [
4]. The prevalence of obesity in Europe is almost so high and increasing over time. In 2019, 52.7% of the adult EU members was overweight defined as a body mass index (BMI) of ≥25 kg/m
2, of which 16.3% could be classified as obese (BMI ≥30 kg/m
2)[
5].
Compared with people without obesity, people living with obesity have an increased risk of morbidity and excess mortality as well, because of the co-morbidities associated with obesity. Obesity is linked to more than 250 genetic variants and a wide array of clinical conditions, including diseases of the circulatory, endocrine, digestive, neurological, dermatological, musculoskeletal, respiratory, and genitourinary systems, infectious, and malignant diseases, more frequent injuries [
1].
Many of previous studies found that obesity induces higher healthcare costs due to treatment of obesity-related diseases and complications. Different methods are used to calculate the real economic burden. Cost-of-illness (COI) is the method most commonly used to estimate the economic costs which are divided into three components: direct, indirect, and intangible costs. The
direct medical costs are associated with treating obesity itself and the medical costs for treating those diseases for which excess body weight are a risk factor. Hospital care, physician outpatient visits, nursing home, hospice, rehabilitation, specialist and other health professional care, diagnostic tests, prescription drugs, and other medical supplies belong to this group.
Indirect costs include the value of the time lost from employment or other productive activities, costs of personal contribution of the family members and friends.
Intangible costs are those associated with the pain and suffering from obesity itself, and from those diseases for which obesity is a contributing factor. Because of the difficulty of assigning a monetary value to physical or emotional suffering, this component has not been usually included in the total costs of obesity. The COI method has been used to derive two sets of estimates related to the economic costs of obesity: the
prevalence based and
incidence based costs estimates [
6,
7,
8,
9,
10,
11].
The
total medical cost of each obesity-related diseases used in studies are based on the attributable risk approach is obtained from few published studies rather than being estimated directly by the authors of those studies [
12].
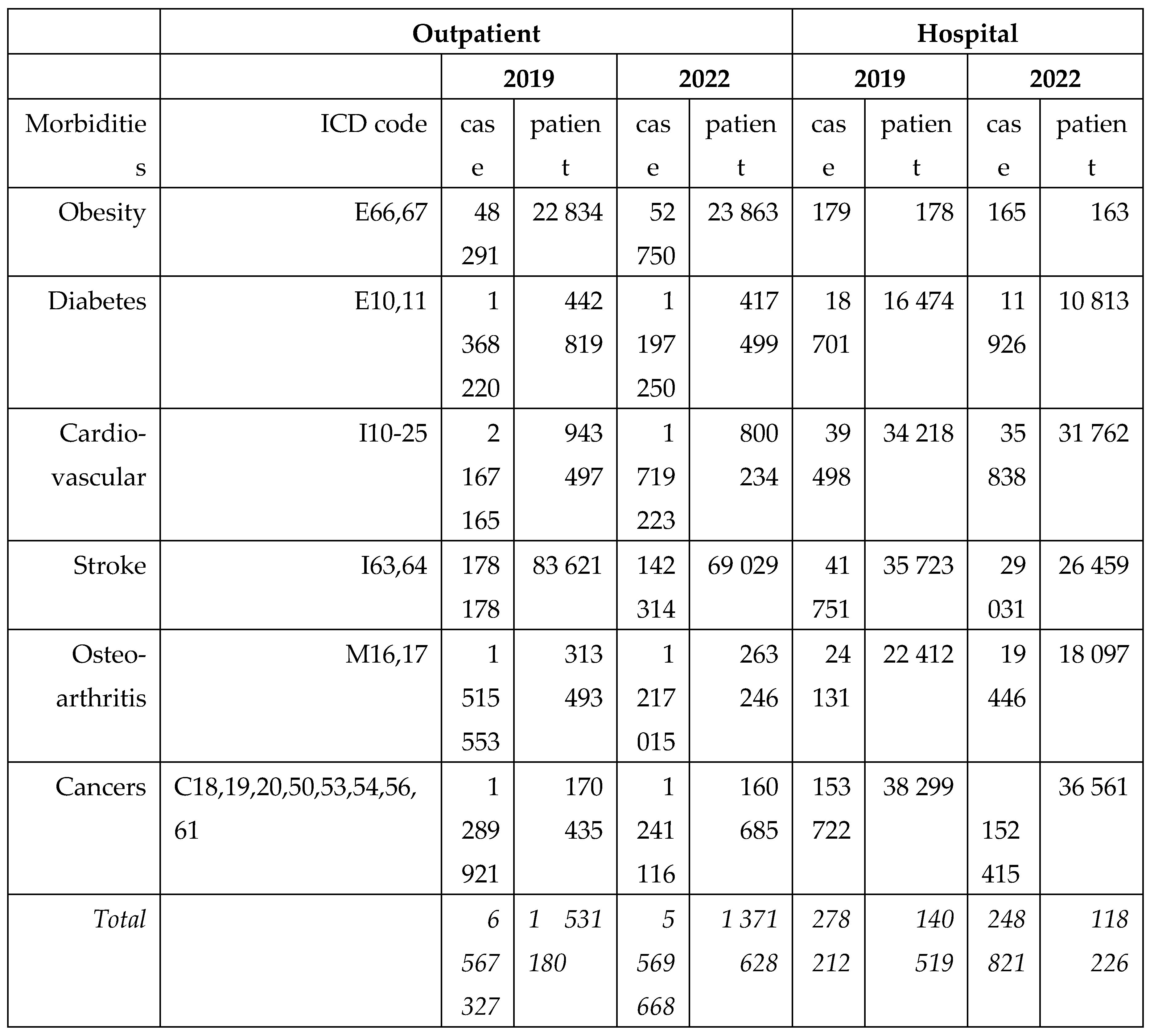
Based on the prevalence data in Canada in 2004, overall 45% of hypertension, 39% of type II diabetes, 35% of gallbladder disease, 23% of coronary artery diseases (CAD), 19% of osteoarthritis, 11% of stroke, 22% of endometrial cancer, 12% of postmenopausal breast cancer, and 10% of colon cancer could be attributed to obesity [
7]. Obesity is reported to be one of the strongest lifestyle-related factors for developing type II diabetes with relative risk (RR) 17 by women and 23 by men, is associated with hypertension with RR ranging from 2.2 to 5.7, can lead to coronary disease (RR=1,4) and is also associated with an increased risk of both ischemic and haemorrhagic stroke. People with obesity have a predisposition to cholelythiasis (RR=1.9) and to osteoarthritis in weight-bearing joints such as knee (RR= 6) and hip (RR=4) [
10,
12].
As obesity is a growing problem in most countries, Hungary being no exception. In 2015 the overall prevalence rate of overweight and obesity among adult men was 40% and 32%, respectively, while both overweight and obesity occurred in 32% of women. In 1988 obesity was registered by only 12% of men and by 18% of women [
13]. National public health care expenditures in 2013 were evaluated in our previous study, focusing to the expenditures of diabetes and hypertension only [
14].
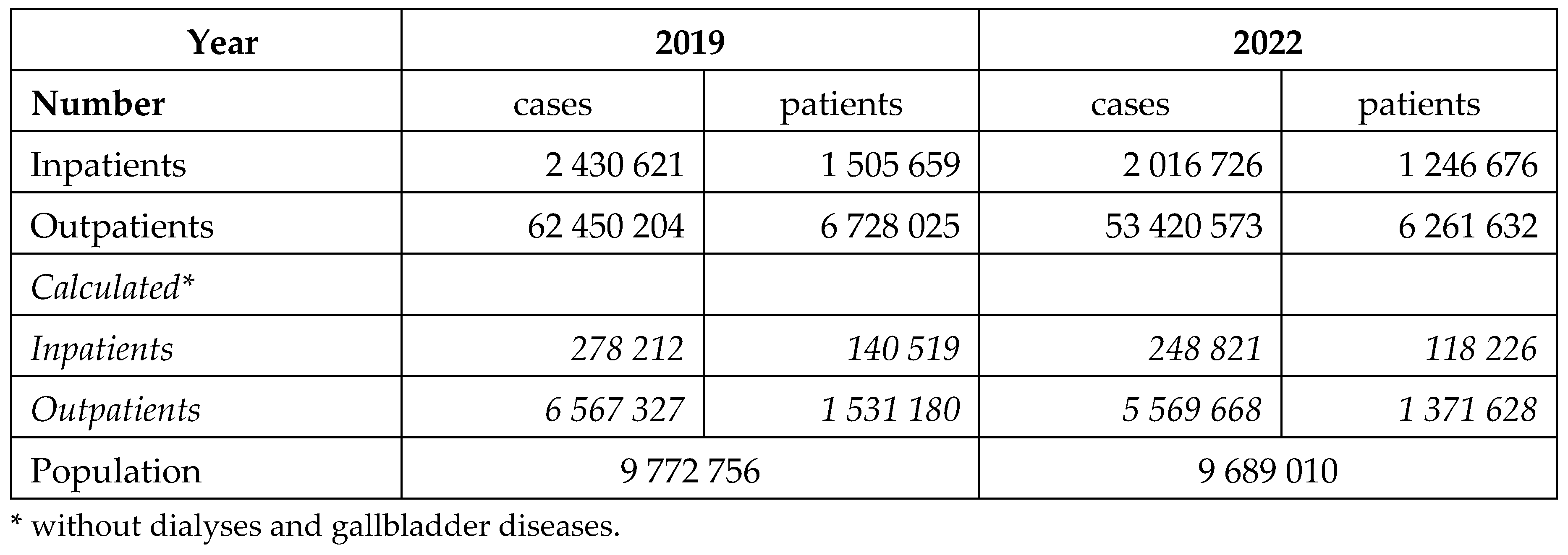
The Hungarian National Health Insurance Fund (NHIF-Hungarian acronym: NEAK) is the only health-care financing agency in a single-payer social-insurance system, managed by the government. All the public inpatient (hospitals) and outpatient (secondary/specialist) health care providers have to report their activities on monthly basis to the NHIF.
Hospital services (inpatient care) are financed through the implementation of a system similar to the American Diagnosis Related Groups (DRG). The diagnoses as a reason for hospitalisation are recorded and reported. The main diagnosis serves as a basement for financing, modified with registered co-morbidities, duration of the treatment and other factors. In the outpatient care, a German fee-for-service point system is used for financing.
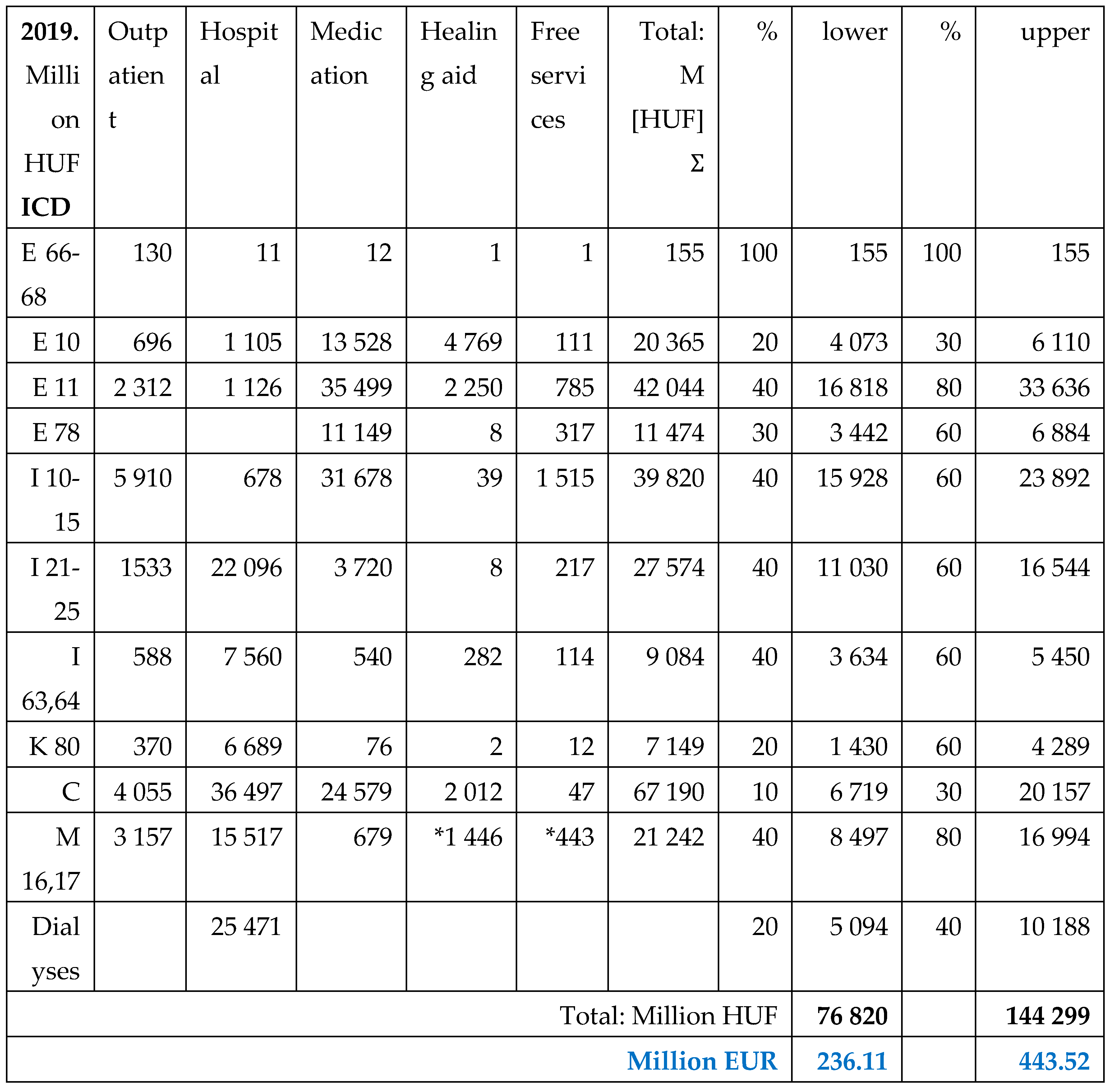
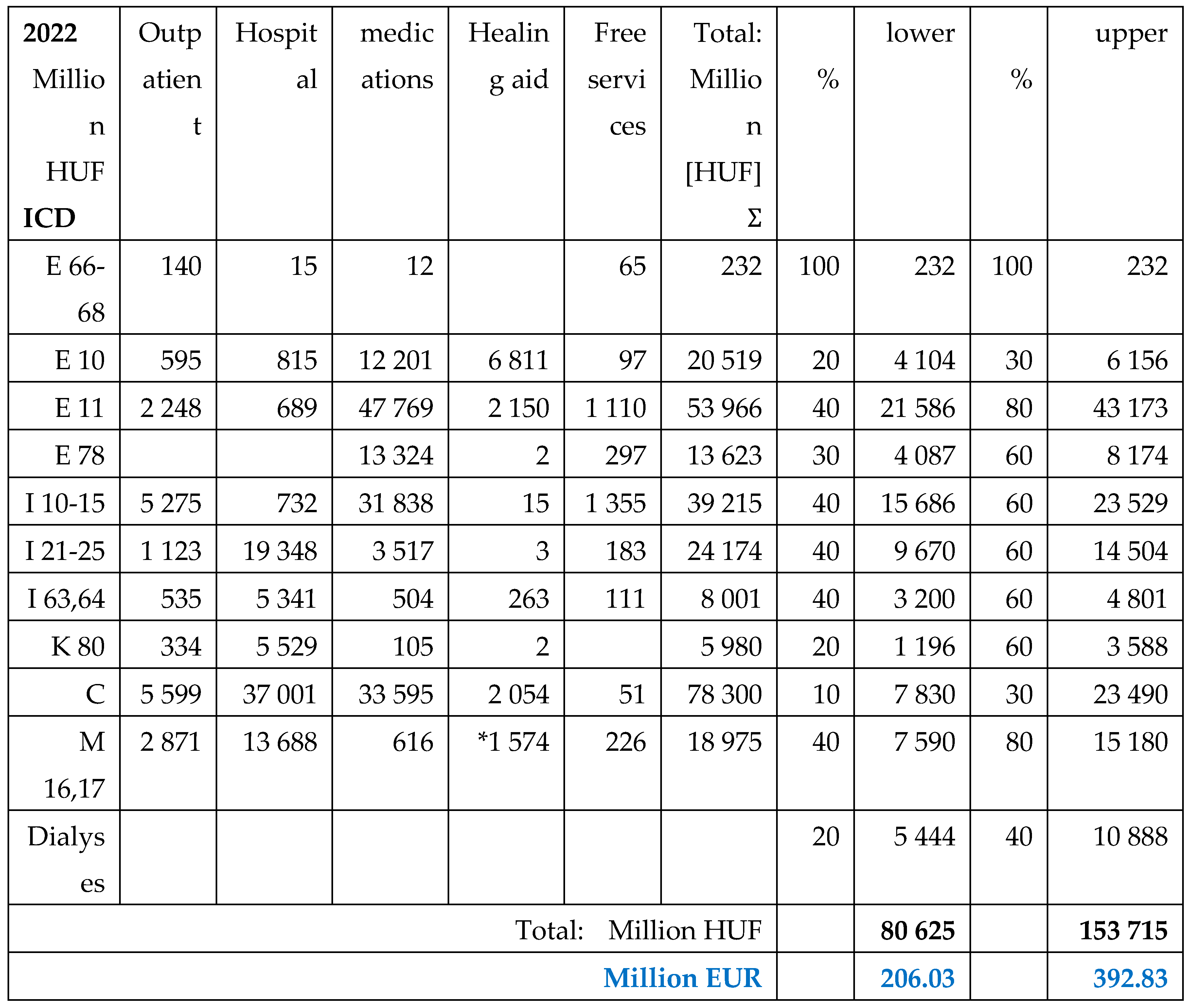
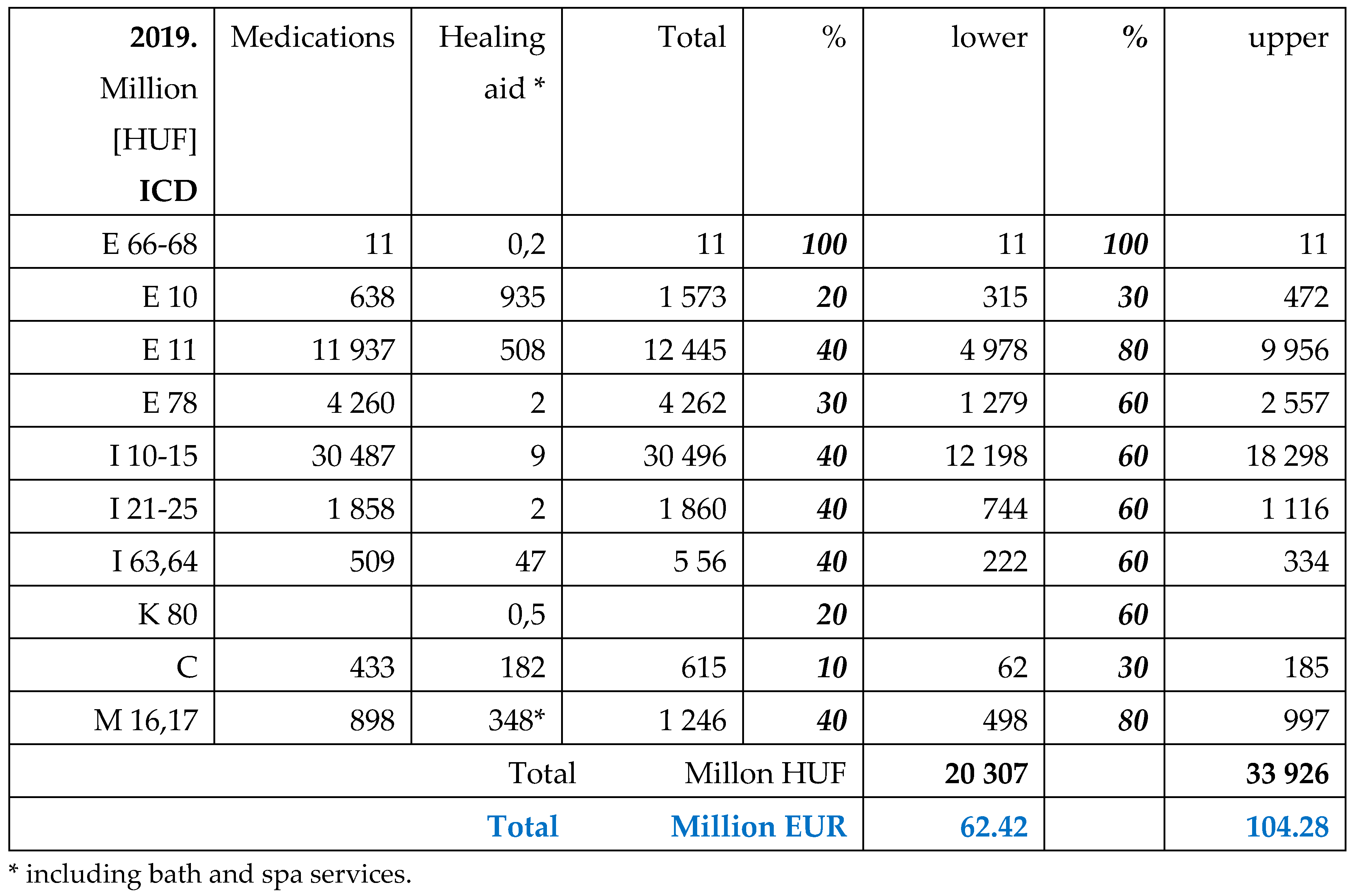
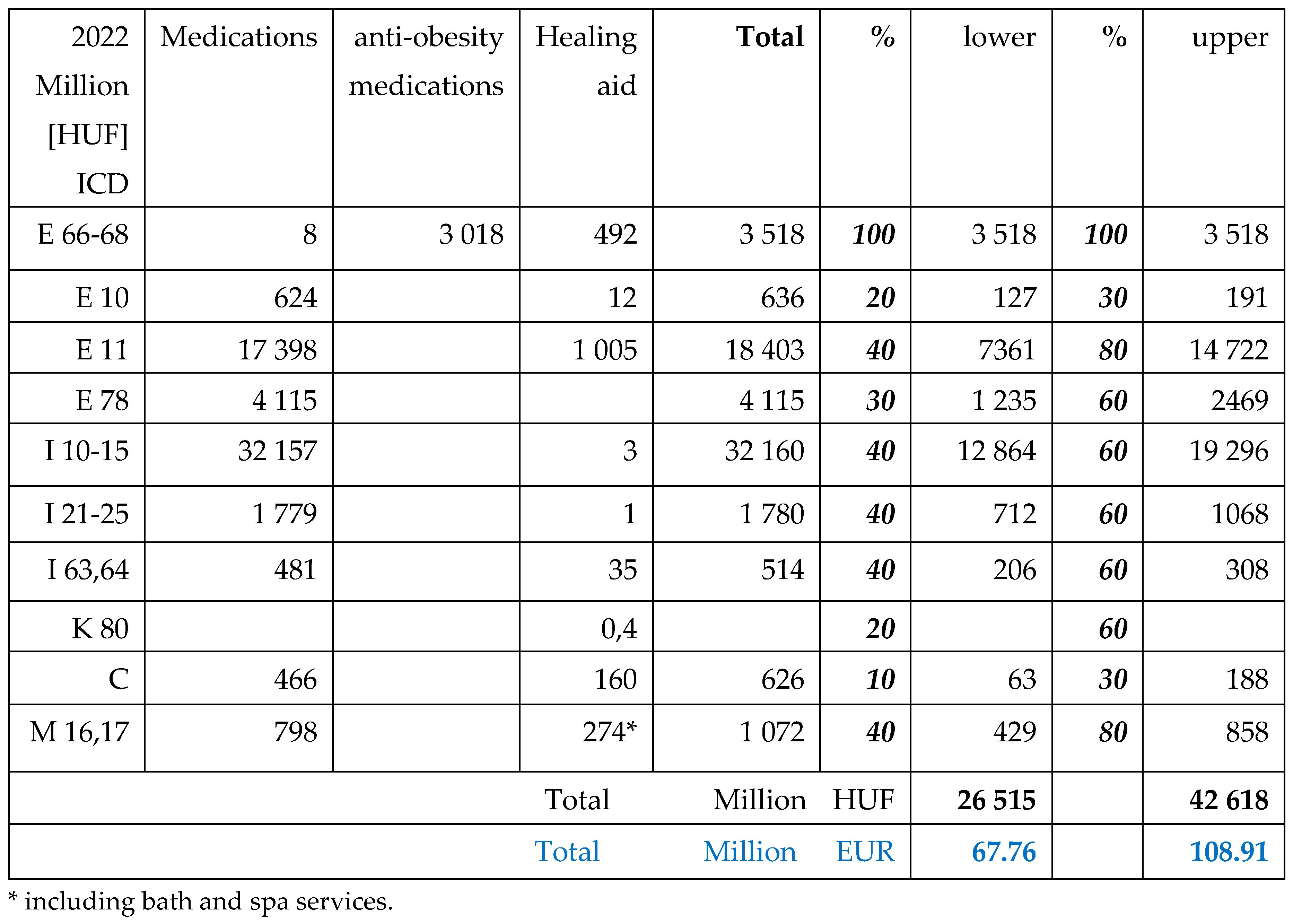
Prescribed drugs are partially reimbursed by NHIF. Its ratio depends from the type of morbidities (almost 100% for cancer patients, less for insulin’s) and 25-75% for other medications, except over-the counter (OTC) products. Medications dedicated for only obesity treatment did not get any reimbursement, even surgical (metabolic, bariatric) procedures.
In the Hungarian health care system the
International Classification of Diseases (ICD-10) codes are still used [
15].
All public health care provision and reimbursement for medication are related to the social security number.
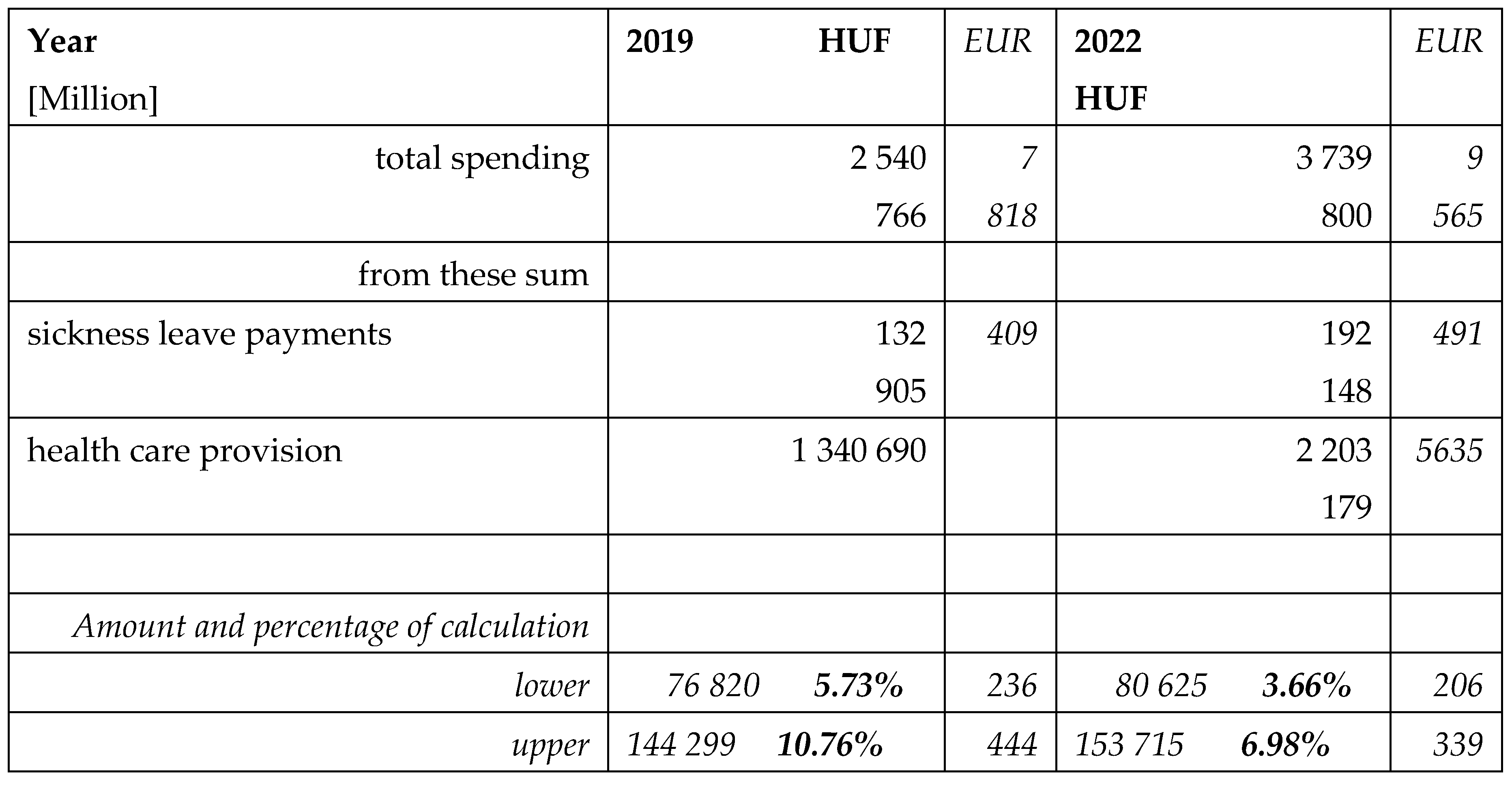
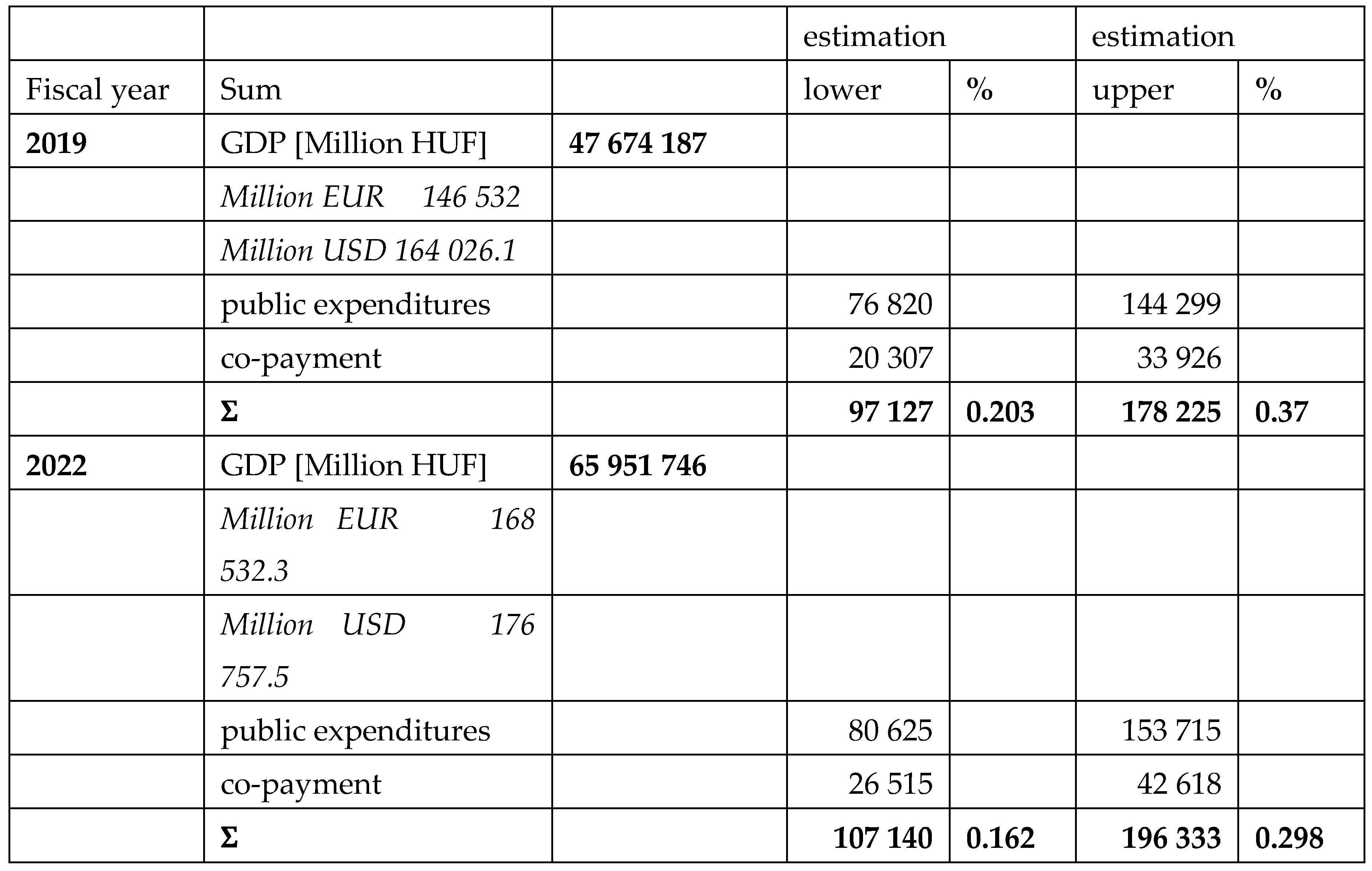
The aim of this study is to calculate the obesity related public expenditures in Hungary, to estimate the expenses and contribution of patients and to make a comprehensive evaluation about the financial data of the last year before the pandemic (2019) and the last available year 2022, after the post-pandemic recovery of the health care system.