Submitted:
25 September 2024
Posted:
26 September 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Fundamentals of Biomaterials
2. Method of Fabrication of Biomaterials
3. Sustainability in Biomaterials
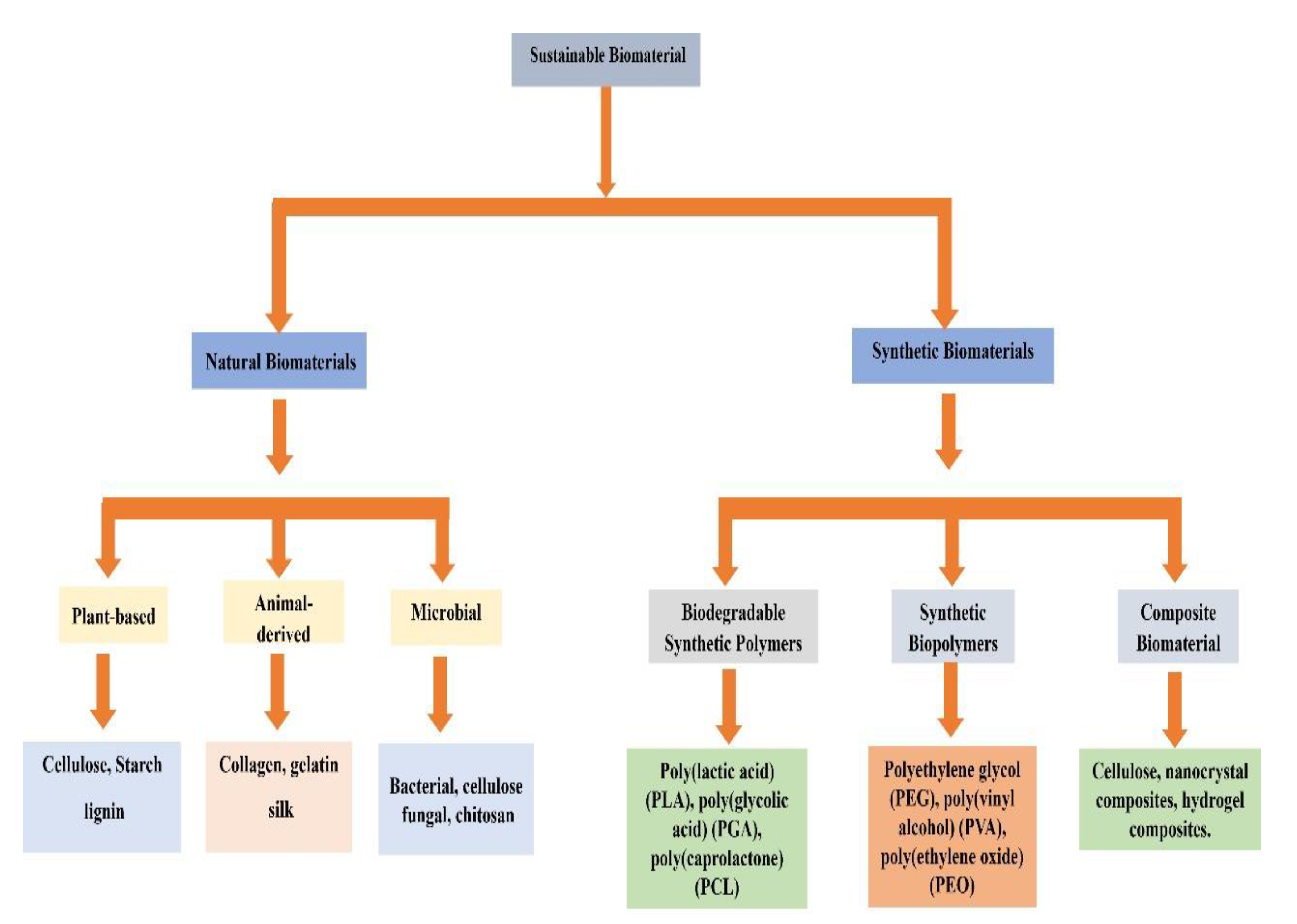
4. Natural Biomaterials
1. Synthetic Biomaterials from Renewable Resources
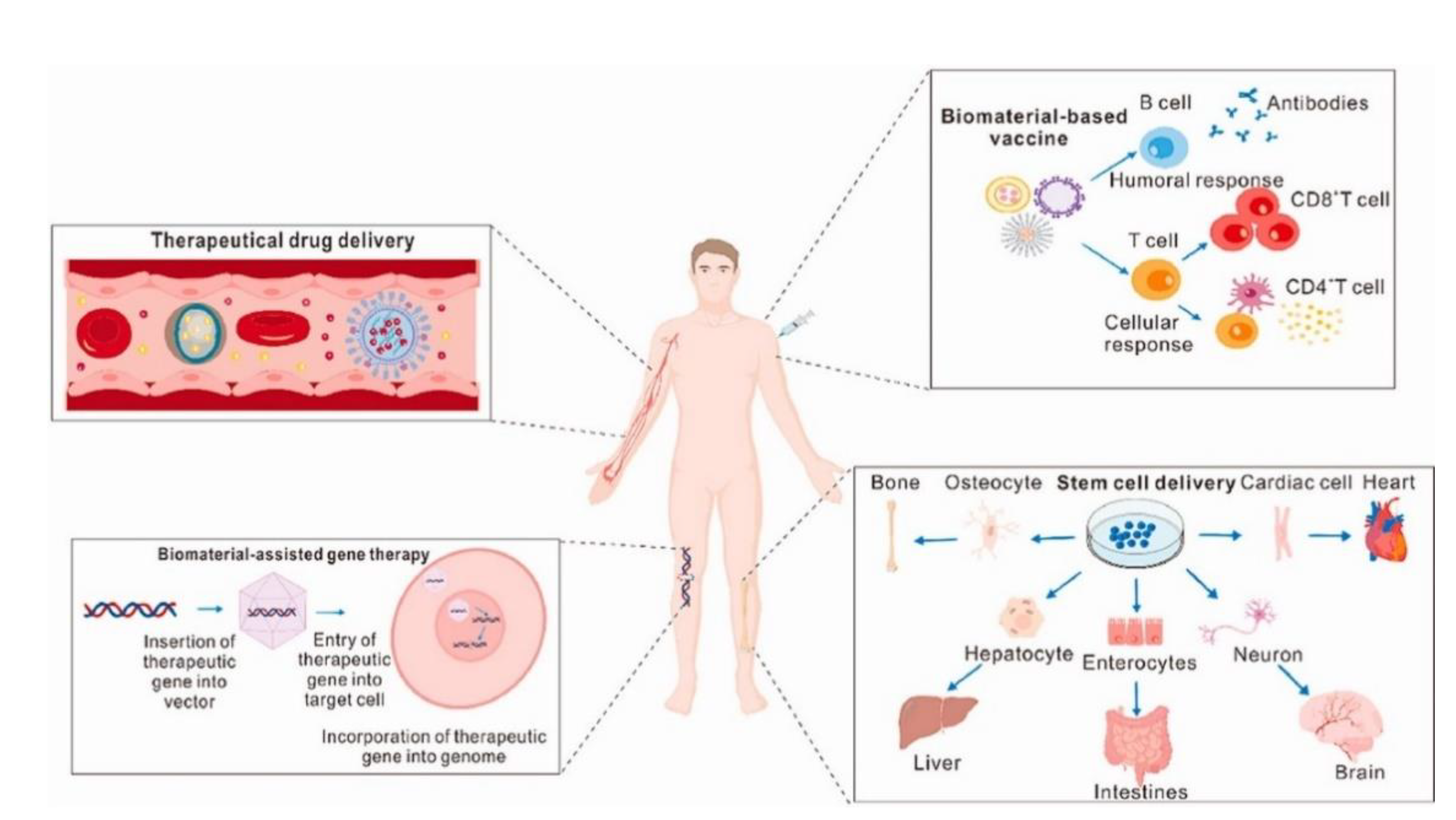
2. Applications of Sustainable Biomaterials in Pharmaceutics
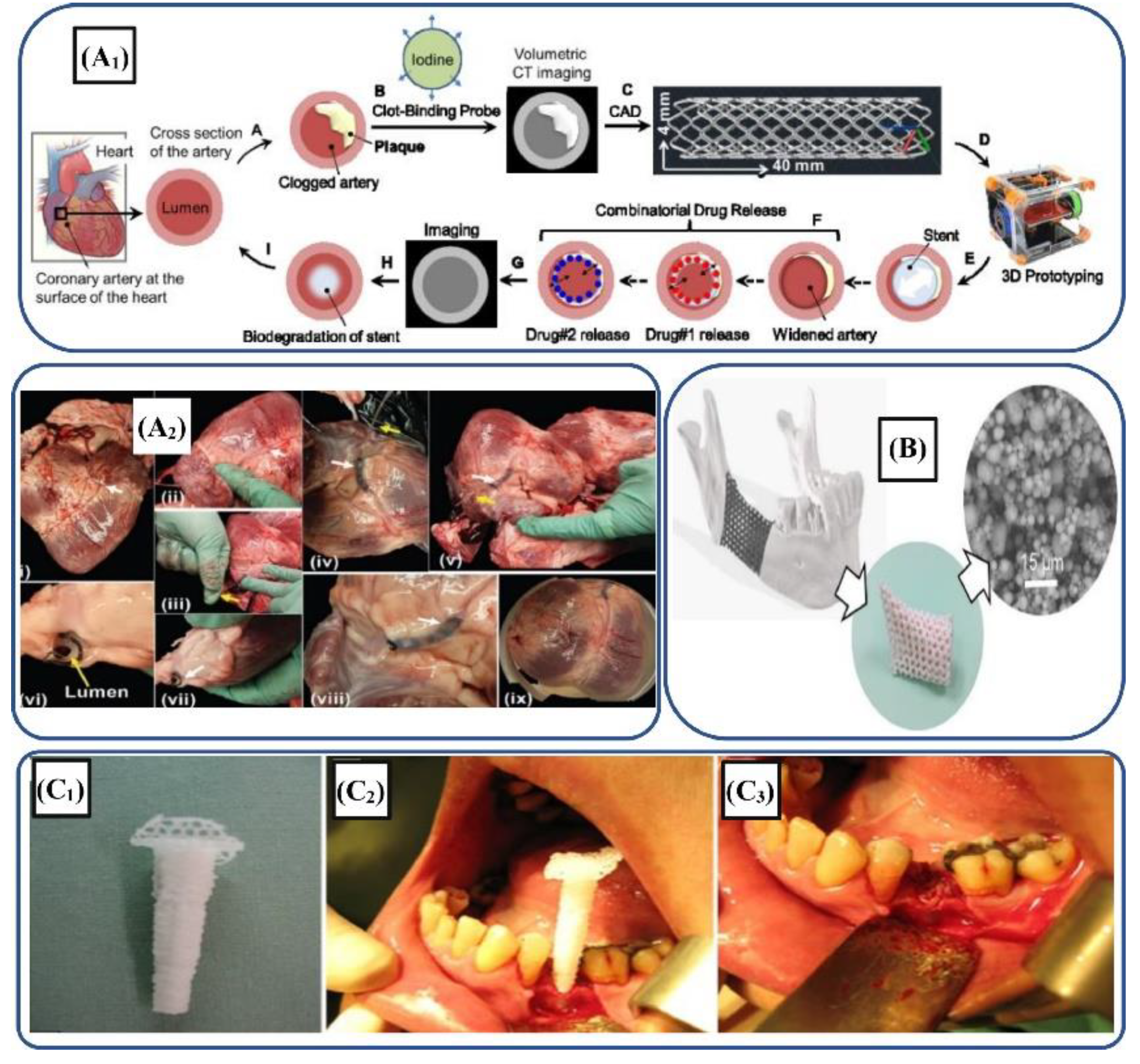
8. Applications of Sustainable Biomaterials in Medical devices
8. Cell Toxicity of Sustainable Biomaterials
10. Future Perspectives and Challenges
11. Conclusion
Ethical consideration
Funding
Data availability statement
Acknowledgments
Abbreviations
| BSEM | Backscattered Electron Microscopy |
| AM | Additive Manufacturing |
| PLA | Polylactic Acid |
| PHAs | Polyhydroxyalkanoates |
| PGA | Polyglycolic Acid |
| PHB | Polyhydroxybutyrate |
| PHBV | Poly(3-hydroxybutyrate-co-3-hydroxyvalerate |
| PLLA | Poly(L-lactic acid) |
| PDLLA | Poly(D,L- lactic acid) |
| PLGA | Poly(lactic –co-glycolic acid) |
| PEG | Polyethylene glycol |
| ECM | Extracellular Matrix |
| NRU | Neutral Red Uptake |
| MTT | (3-[4,5-dimethyl2-thiazolyl]-2,5-diphenyl tetrazolium bromide |
References
- Rezvani Ghomi E, Khalili S, Nouri Khorasani S, Esmaeely Neisiany R, Ramakrishna S: Wound dressings: Current advances and future directions. J Appl Polym Sci. 2019, 136:47738. [CrossRef]
- Al Rashid A, Khan SA, G. Al-Ghamdi S, Koç M: Additive manufacturing of polymer nanocomposites: Needs and challenges in materials, processes, and applications. J Mater Res Technol. 2021, 14:910–41. [CrossRef]
- Tümer EH, Erbil HY. Extrusion-Based 3D Printing Applications of PLA Composites: A Review. Coatings. 2021; 11(4):390. [CrossRef]
- Arif ZU, Khalid MY, Noroozi R, et al.: Additive manufacturing of sustainable biomaterials for biomedical applications. Asian J Pharm Sci. 2023, 18:100812. [CrossRef]
- Huang Z, Shao G, Li L: Micro/nano functional devices fabricated by additive manufacturing. Prog Mater Sci. 2023, 131:101020. [CrossRef]
- Zhang Y, Lim CT, Ramakrishna S, Huang Z-M: Recent development of polymer nanofibers for biomedical and biotechnological applications. J Mater Sci Mater Med. 2005, 16:933–46. [CrossRef]
- Alizadeh-Osgouei M, Li Y, Wen C: A comprehensive review of biodegradable synthetic polymer-ceramic composites and their manufacture for biomedical applications. Bioact Mater. 2019, 4:22–36. [CrossRef]
- Azuraini MJ, Vigneswari S, Huong K-H, Khairul WM, H.P.S. AK, Ramakrishna S, Amirul A-AA. Surface Modification of Sponge-like Porous Poly(3-hydroxybutyrate-co-4-hydroxybutyrate)/Gelatine Blend Scaffolds for Potential Biomedical Applications. Polymers. 2022; 14(9):1710. [CrossRef]
- Qiu S, Zhou Y, Waterhouse GIN, Gong R, Xie J, Zhang K, Xu J: Optimizing interfacial adhesion in PBAT/PLA nanocomposite for biodegradable packaging films. Food Chem. 2021, 334:127487. [CrossRef]
- 10. Giubilini A, Bondioli F, Messori M, Nyström G, Siqueira G. Advantages of Additive Manufacturing for Biomedical Applications of Polyhydroxyalkanoates. Bioengineering. 2021; 8(2):29. [CrossRef]
- Abbasian M, Massoumi B, Mohammad-Rezaei R, Samadian H, Jaymand M: Scaffolding polymeric biomaterials: Are naturally occurring biological macromolecules more appropriate for tissue engineering? Int J Biol Macromol. 2019, 134:673–94. [CrossRef]
- Mohanty AK, Wu F, Mincheva R, et al.: Sustainable polymers. Nat Rev Methods Primer. 2022, 2:.
- Biswas MC, Jony B, Nandy PK, et al.: Recent Advancement of Biopolymers and Their Potential Biomedical Applications. J Polym Environ. 2022, 30:51–74. [CrossRef]
- Naderi H, Matin MM, Bahrami AR: Review paper: critical issues in tissue engineering: biomaterials, cell sources, angiogenesis, and drug delivery systems. J Biomater Appl. 2011, 26:383–417. [CrossRef]
- Campoccia D, Montanaro L, Arciola CR: A review of the biomaterials technologies for infection-resistant surfaces. Biomaterials. 2013, 34:8533–54. [CrossRef]
- Pradhan D, Sukla LB: Thin film of Yttria stabilised zirconia on NiO using vacuum cold spraying process for solid oxide fuel cell. Int J Nano Biomater. 2017, 7:38. [CrossRef]
- Abraham AK, G SV: Materials, design and manufacturing technologies for orthopaedic biomaterials: A review. Trends Biomater Artif Organs. 2015, 29:258–61.
- Stoddart A, Cleave V: The evolution of biomaterials. Nat Mater. 2009, 8:444–5. [CrossRef]
- Parker JB, Griffin MF, Spielman AF, Wan DC, Longaker MT: Exploring the Overlooked Roles and Mechanisms of Fibroblasts in the Foreign Body Response. Adv Wound Care. 2023, 12:85–96. [CrossRef]
- Sheikh Z, Najeeb S, Khurshid Z, Verma V, Rashid H, Glogauer M: Biodegradable Materials for Bone Repair and Tissue Engineering Applications. Materials. 2015, 8:5744–94. [CrossRef]
- Zybutz MD, Laurell L, Rapoport DA, Rutger Persson G: Treatment of intrabony defects with resorbable materials, non-resorbable materials and flap debridement. J Clin Periodontol. 2000, 27:169–78. [CrossRef]
- Sheikh Z, Najeeb S, Khurshid Z, Verma V, Rashid H, Glogauer M. Biodegradable Materials for Bone Repair and Tissue Engineering Applications. Materials. 2015; 8(9):5744-5794. [CrossRef]
- Prakasam M, Locs J, Salma-Ancane K, Loca D, Largeteau A, Berzina-Cimdina L. Biodegradable Materials and Metallic Implants-A Review. J Funct Biomater. 2017 Sep 26;8(4):44. [CrossRef]
- Biswal T, BadJena SK, Pradhan D: Sustainable biomaterials and their applications: A short review. Mater Today Proc. 2020, 30:274–82. [CrossRef]
- Sathiyavimal S, Vasantharaj S, LewisOscar F, Selvaraj R, Brindhadevi K, Pugazhendhi A: Natural organic and inorganic–hydroxyapatite biopolymer composite for biomedical applications. Prog Org Coat. 2020, 147:105858. [CrossRef]
- Huang Z-M, Zhang Y-Z, Kotaki M, Ramakrishna S: A review on polymer nanofibers by electrospinning and their applications in nanocomposites. Compos Sci Technol. 2003, 63:2223–53. [CrossRef]
- Roshandel M, Dorkoosh F: Cardiac tissue engineering, biomaterial scaffolds, and their fabrication techniques. Polym Adv Technol. 2021, 32:2290–305. [CrossRef]
- Mani MP, Sadia M, Jaganathan SK, et al.: A review on 3D printing in tissue engineering applications. J Polym Eng. 2022, 42:243–65. [CrossRef]
- Zhang C, Li Y, Kang W, Liu X, Wang Q: Current advances and future perspectives of additive manufacturing for functional polymeric materials and devices. SusMat. 2021, 1:127–47. [CrossRef]
- Udayakumar GP, Muthusamy S, Selvaganesh B, et al.: Biopolymers and composites: Properties, characterization and their applications in food, medical and pharmaceutical industries. J Environ Chem Eng. 2021, 9:105322. [CrossRef]
- Visco A, Scolaro C, Facchin M, Brahimi S, Belhamdi H, Gatto V, Beghetto V: Agri-Food Wastes for Bioplastics: European Prospective on Possible Applications in Their Second Life for a Circular Economy. Polymers. 2022, 14:2752. [CrossRef]
- Agnieray H, Glasson JL, Chen Q, Kaur M, Domigan LJ: Recent developments in sustainably sourced protein-based biomaterials. Biochem Soc Trans. 2021, 49:953–64. [CrossRef]
- Lefèvre T, Auger M: Spider silk inspired materials and sustainability: perspective. Mater Technol. 2016, 1–16. [CrossRef]
- Pesode P, Barve S, Wankhede SV, Ahmad A: Sustainable Materials and Technologies for Biomedical Applications. Adv Mater Sci Eng. 2023, 2023:e6682892. [CrossRef]
- Moshood TD, Nawanir G, Mahmud F, Mohamad F, Ahmad MH, AbdulGhani A: Sustainability of biodegradable plastics: New problem or solution to solve the global plastic pollution? Curr Res Green Sustain Chem. 2022, 5:100273. [CrossRef]
- López-Castro LF, Solano-Charris EL. Integrating Resilience and Sustainability Criteria in the Supply Chain Network Design. A Systematic Literature Review. Sustainability. 2021; 13(19):10925. [CrossRef]
- Troy E, Tilbury MA, Power AM, Wall JG: Nature-Based Biomaterials and Their Application in Biomedicine. Polymers. 2021, 13:3321. [CrossRef]
- Bhat S, Kumar A: Biomaterials and bioengineering tomorrow’s healthcare. Biomatter. 2013, 3:e24717. [CrossRef]
- Liu S, Yu J-M, Gan Y-C, et al.: Biomimetic natural biomaterials for tissue engineering and regenerative medicine: new biosynthesis methods, recent advances, and emerging applications. Mil Med Res. 2023, 10:16. [CrossRef]
- Bodin A, Concaro S, Brittberg M, Gatenholm P: Bacterial cellulose as a potential meniscus implant. J Tissue Eng Regen Med. 2007, 1:406–8. [CrossRef]
- Yang X, Lu Z, Wu H, Li W, Zheng L, Zhao J: Collagen-alginate as bioink for three-dimensional (3D) cell printing based cartilage tissue engineering. Mater Sci Eng C. 2018, 83:195–201. [CrossRef]
- Liu S, Huang D, Hu Y, et al.: Sodium alginate/collagen composite multiscale porous scaffolds containing poly(ε-caprolactone) microspheres fabricated based on additive manufacturing technology. RSC Adv. 10:39241–50. [CrossRef]
- Zarrintaj P, Manouchehri S, Ahmadi Z, Saeb MR, Urbanska AM, Kaplan DL, Mozafari M: Agarose-based biomaterials for tissue engineering. Carbohydr Polym. 2018, 187:66–84. [CrossRef]
- Davison-Kotler E, Marshall WS, García-Gareta E: Sources of Collagen for Biomaterials in Skin Wound Healing. Bioengineering. 2019, 6:56. [CrossRef]
- Kato Y, Onishi H, Machida Y: Application of Chitin and Chitosan Derivatives in the Pharmaceutical Field. Curr Pharm Biotechnol. 4:303–9.
- Fujita M, Kinoshita M, Ishihara M, et al.: Inhibition of vascular prosthetic graft infection using a photocrosslinkable chitosan hydrogel. J Surg Res. 2004, 121:135–40. [CrossRef]
- 47. Alexandru Mihai Grumezescu, Valentina Grumezescu; Materials for Biomedical Engineering: Bioactive Materials, Properties, and Applications - 1st Edition | Elsevier Shop. Accessed: March 26, 2024. [Google Scholar]
- Elzoghby AO: Gelatin-based nanoparticles as drug and gene delivery systems: Reviewing three decades of research. J Controlled Release. 2013, 172:1075–91. [CrossRef]
- Husain S, Al-Samadani KH, Najeeb S, Zafar MS, Khurshid Z, Zohaib S, Qasim SB: Chitosan Biomaterials for Current and Potential Dental Applications. Materials. 2017, 10:602. [CrossRef]
- Fadilah NIM, Phang SJ, Kamaruzaman N, et al.: Antioxidant Biomaterials in Cutaneous Wound Healing and Tissue Regeneration: A Critical Review. Antioxidants. 2023, 12:787. [CrossRef]
- Kumar Gupta G, De S, Franco A, Balu AM, Luque R: Sustainable Biomaterials: Current Trends, Challenges and Applications. Molecules. 2015, 21:48. [CrossRef]
- Moshood TD, Nawanir G, Mahmud F, Mohamad F, Ahmad MH, AbdulGhani A: Sustainability of biodegradable plastics: New problem or solution to solve the global plastic pollution? Curr Res Green Sustain Chem. 2022, 5:100273. [CrossRef]
- Hou W, Miyazaki S, Takada M, Komai T: Sustained release of indomethacin from chitosan granules. Chem Pharm Bull (Tokyo). 1985, 33:3986–92. [CrossRef]
- Dash M, Chiellini F, Ottenbrite RM, Chiellini E: Chitosan—A versatile semi-synthetic polymer in biomedical applications. Prog Polym Sci. 2011, 36:981–1014. [CrossRef]
- Zhang Y, Zhang M: Microstructural and mechanical characterization of chitosan scaffolds reinforced by calcium phosphates. J Non-Cryst Solids. 2001, 282:159–64. [CrossRef]
- Peng T, Gibula P, Yao K, Goosen MFA: Role of polymers in improving the results of stenting in coronary arteries. Biomaterials. 1996, 17:685–94. [CrossRef]
- Kılıçay E, Demirbilek M, Türk M, Güven E, Hazer B, Denkbas EB: Preparation and characterization of poly(3-hydroxybutyrate-co-3-hydroxyhexanoate) (PHBHHX) based nanoparticles for targeted cancer therapy. Eur J Pharm Sci. 2011, 44:310–20. [CrossRef]
- Chen L, Li X, Li L, Guo S: Acetylated starch-based biodegradable materials with potential biomedical applications as drug delivery systems. Curr Appl Phys. 2007, 7:e90–3. [CrossRef]
- Chen L, Li X, Li L, Guo S: Acetylated starch-based biodegradable materials with potential biomedical applications as drug delivery systems. Curr Appl Phys. 2007, 7:e90–3. [CrossRef]
- Park S-B, Lih E, Park K-S, Joung YK, Han DK: Biopolymer-based functional composites for medical applications. Prog Polym Sci. 2017, 68:77–105. [CrossRef]
- Caldas M, Santos AC, Veiga F, Rebelo R, Reis RL, Correlo VM: Melanin nanoparticles as a promising tool for biomedical applications – a review. Acta Biomater. 2020, 105:26–43. [CrossRef]
- Freitas AAR, Ribeiro AJ, Santos AC, et al.: Sterculia striata gum as a potential oral delivery system for protein drugs. Int J Biol Macromol. 2020, 164:1683–92. [CrossRef]
- Hussain Z, Katas H, Mohd Amin MCI, Kumolosasi E, Buang F, Sahudin S: Self-assembled polymeric nanoparticles for percutaneous co-delivery of hydrocortisone/hydroxytyrosol: An ex vivo and in vivo study using an NC/Nga mouse model. Int J Pharm. 2013, 444:109–19. [CrossRef]
- Md S, Kuldeep Singh JKA, Waqas M, et al.: Nanoencapsulation of betamethasone valerate using high pressure homogenization-solvent evaporation technique: optimization of formulation and process parameters for efficient dermal targeting. Drug Dev Ind Pharm. 2019, 45:323–32. [CrossRef]
- Dadashzadeh A, Imani R, Moghassemi S, Omidfar K, Abolfathi N: Study of hybrid alginate/gelatin hydrogel-incorporated niosomal Aloe vera capable of sustained release of Aloe vera as potential skin wound dressing. Polym Bull. 2020, 77:387–403. [CrossRef]
- Szekalska M, Sosnowska K, Tomczykowa M, Winnicka K, Kasacka I, Tomczyk M: In vivo anti-inflammatory and anti-allergic activities of cynaroside evaluated by using hydrogel formulations. Biomed Pharmacother. 2020, 121:109681. [CrossRef]
- Salehi M, Ehterami A, Farzamfar S, Vaez A, Ebrahimi-Barough S: Accelerating healing of excisional wound with alginate hydrogel containing naringenin in rat model. Drug Deliv Transl Res. 2021, 11:142–53. [CrossRef]
- Han X, Alu A, Liu H, Shi Y, Wei X, Cai L, Wei Y: Biomaterial-assisted biotherapy: A brief review of biomaterials used in drug delivery, vaccine development, gene therapy, and stem cell therapy. Bioact Mater. 2022, 17:29–48. [CrossRef]
- Sun G, Zhang X, Shen Y-I, et al.: Dextran hydrogel scaffolds enhance angiogenic responses and promote complete skin regeneration during burn wound healing. Proc Natl Acad Sci. 2011, 108:20976–81. [CrossRef]
- Li Z, Song J, Zhang J, et al.: Topical application of silk fibroin-based hydrogel in preventing hypertrophic scars. Colloids Surf B Biointerfaces. 2020, 186:110735. [CrossRef]
- Dong M, Mao Y, Zhao Z, Zhang J, Zhu L, Chen L, Cao L: Novel fabrication of antibiotic containing multifunctional silk fibroin injectable hydrogel dressing to enhance bactericidal action and wound healing efficiency on burn wound: In vitro and in vivo evaluations. Int Wound J. 2021, 19:679–91. [CrossRef]
- Oryan A, Jalili M, Kamali A, Nikahval B: The concurrent use of probiotic microorganism and collagen hydrogel/scaffold enhances burn wound healing: An in vivo evaluation. Burns. 2018, 44:1775–86. [CrossRef]
- Yoon DS, Lee Y, Ryu HA, et al.: Cell recruiting chemokine-loaded sprayable gelatin hydrogel dressings for diabetic wound healing. Acta Biomater. 2016, 38:59–68. [CrossRef]
- Pawar V, Maske P, Khan A, Ghosh A, Keshari R, Bhatt M, Srivastava R: Responsive Nanostructure for Targeted Drug Delivery. J Nanotheranostics. 2023, 4:55–85. [CrossRef]
- Malhotra N, Joshi M, Dey S, Sahoo R, Verma S, Asish K: Recent trends in chronic pain medicine. Indian J Anaesth. 2023, 67:123–9. [CrossRef]
- Gu X, Carroll Turpin MA, Romero-Ortega MI: Biomaterials and Regenerative Medicine in Pain Management. Curr Pain Headache Rep. 2022, 26:533–41. [CrossRef]
- Makadia HK, Siegel SJ. Poly Lactic-co-Glycolic Acid (PLGA) as Biodegradable Controlled Drug Delivery Carrier. Polymers. 2011; 3(3):1377-1397. [CrossRef]
- Trucillo P, Campardelli R, Reverchon E. Liposomes: From Bangham to Supercritical Fluids. Processes. 2020; 8(9):1022. [CrossRef]
- Tønnesen HH, Karlsen J: Alginate in drug delivery systems. Drug Dev Ind Pharm. 2002, 28:621–30. [CrossRef]
- Tao F, Ma S, Tao H, et al.: Chitosan-based drug delivery systems: From synthesis strategy to osteomyelitis treatment – A review. Carbohydr Polym. 2021, 251:117063. [CrossRef]
- How KN, Yap WH, Lim CLH, Goh BH, Lai ZW: Hyaluronic Acid-Mediated Drug Delivery System Targeting for Inflammatory Skin Diseases: A Mini Review. Front Pharmacol. 2020, 11. [CrossRef]
- Sun S, Cui Y, Yuan B, et al.: Drug delivery systems based on polyethylene glycol hydrogels for enhanced bone regeneration. Front Bioeng Biotechnol. 2023, 11:1117647. [CrossRef]
- Haimhoffer Á, Rusznyák Á, Réti-Nagy K, et al.: Cyclodextrins in Drug Delivery Systems and Their Effects on Biological Barriers. Sci Pharm. 2019, 87:33. [CrossRef]
- Wang J, Li B, Qiu L, Qiao X, Yang H: Dendrimer-based drug delivery systems: history, challenges, and latest developments. J Biol Eng. 2022, 16:18. [CrossRef]
- Rancan F, Papakostas D, Hadam S, et al.: Investigation of Polylactic Acid (PLA) Nanoparticles as Drug Delivery Systems for Local Dermatotherapy. Pharm Res. 2009, 26:2027–36. [CrossRef]
- Chaudhuri A, Ramesh K, Kumar DN, Dehari D, Singh S, Kumar D, Agrawal AK: Polymeric micelles: A novel drug delivery system for the treatment of breast cancer. J Drug Deliv Sci Technol. 2022, 77:103886. [CrossRef]
- Pattanashetti NA, Heggannavar GB, Kariduraganavar MY: Smart Biopolymers and their Biomedical Applications. Procedia Manuf. 2017, 12:263–79. [CrossRef]
- Bello AB, Kim D, Kim D, Park H, Lee S-H: Engineering and Functionalization of Gelatin Biomaterials: From Cell Culture to Medical Applications. Tissue Eng Part B Rev. 2020, 26:164–80. [CrossRef]
- Wachol-Drewek Z, Pfeiffer M, Scholl E: Comparative investigation of drug delivery of collagen implants saturated in antibiotic solutions and a sponge containing gentamicin. Biomaterials. 1996, 17:1733–8. [CrossRef]
- Tenchov R, Bird R, Curtze AE, Zhou Q: Lipid Nanoparticles─From Liposomes to mRNA Vaccine Delivery, a Landscape of Research Diversity and Advancement. ACS Nano. 2021, 15:16982–7015. [CrossRef]
- Patel N, Davis Z, Hofmann C, Vlasak J, Loughney JW, DePhillips P, Mukherjee M: Development and Characterization of an In Vitro Cell-Based Assay to Predict Potency of mRNA–LNP-Based Vaccines. Vaccines. 2023, 11:1224. [CrossRef]
- Liang Z, Zhu H, Wang X, et al.: Adjuvants for Coronavirus Vaccines. Front Immunol. 2020, 11:. [CrossRef]
- Elmowafy E, Abdal-Hay A, Skouras A, Tiboni M, Casettari L, Guarino V: Polyhydroxyalkanoate (PHA): applications in drug delivery and tissue engineering. Expert Rev Med Devices. 2019, 16:467–82. [CrossRef]
- Chaikof EL, Matthew H, Kohn J, Mikos AG, Prestwich GD, Yip CM: Biomaterials and Scaffolds in Reparative Medicine. Ann N Y Acad Sci. 2002, 961:96–105. [CrossRef]
- Song W, Lima AC, Mano JF: Bioinspired methodology to fabricate hydrogel spheres for multi-applications using superhydrophobic substrates. Soft Matter. 2010, 6:5868–71. [CrossRef]
- Hassan N, Verdinelli V, Ruso JM, Messina PV: Assessing structure and dynamics of fibrinogen films on silicon nanofibers: towards hemocompatibility devices. Soft Matter. 2012, 8:6582–92. [CrossRef]
- Misra SK, Ostadhossein F, Babu R, et al.: 3D-Printed Multidrug-Eluting Stent from Graphene-Nanoplatelet-Doped Biodegradable Polymer Composite. Adv Healthc Mater. 2017, 6:1700008. [CrossRef]
- Dienel KEG, Van Bochove B, Seppälä JV: Additive Manufacturing of Bioactive Poly(trimethylene carbonate)/β-Tricalcium Phosphate Composites for Bone Regeneration. Biomacromolecules. 2020, 21:366–75. [CrossRef]
- Goh BT, Teh LY, Tan DBP, Zhang Z, Teoh SH: Novel 3 D polycaprolactone scaffold for ridge preservation – a pilot randomised controlled clinical trial. Clin Oral Implants Res. 2015, 26:271–7. [CrossRef]
- Reddy N, Reddy R, Jiang Q: Crosslinking biopolymers for biomedical applications. Trends Biotechnol. 2015, 33:362–9. [CrossRef]
- Wróblewska-Krepsztul J, Rydzkowski T, Michalska-Pożoga I, Thakur VK: Biopolymers for Biomedical and Pharmaceutical Applications: Recent Advances and Overview of Alginate Electrospinning. Nanomaterials. 2019, 9:404. [CrossRef]
- Gagliardi A, Giuliano E, Venkateswararao E, Fresta M, Bulotta S, Awasthi V, Cosco D: Biodegradable Polymeric Nanoparticles for Drug Delivery to Solid Tumors. Front Pharmacol. 2021, 12:601626. [CrossRef]
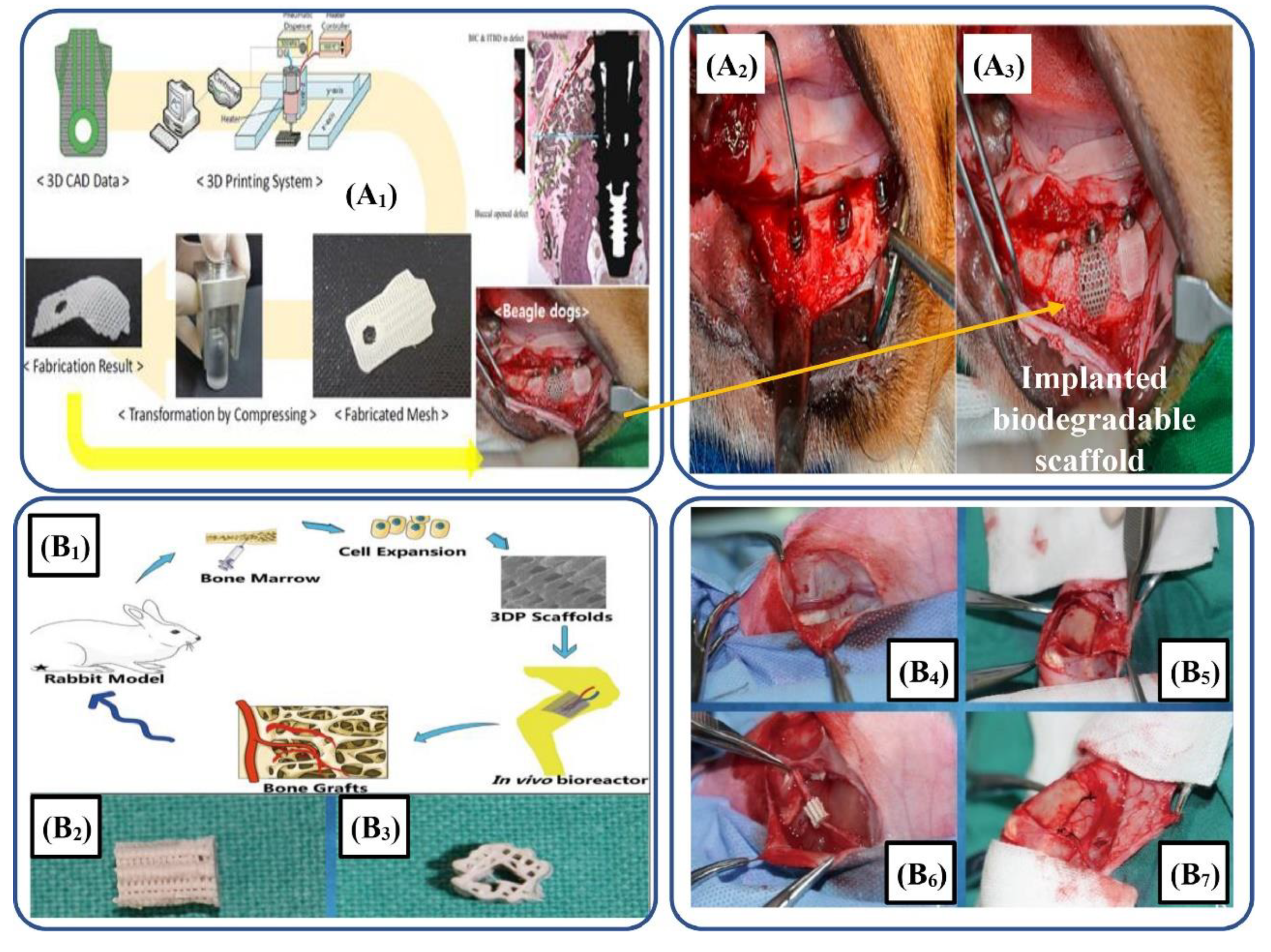
- Shim J-H, Won J-Y, Sung S-J, Lim D-H, Yun W-S, Jeon Y-C, Huh J-B. Comparative Efficacies of a 3D-Printed PCL/PLGA/β-TCP Membrane and a Titanium Membrane for Guided Bone Regeneration in Beagle Dogs. Polymers. 2015; 7(10):2061-2077. [CrossRef]
- Zhang H, Mao X, Zhao D, et al.: Three dimensional printed polylactic acid-hydroxyapatite composite scaffolds for prefabricating vascularized tissue engineered bone: An in vivo bioreactor model. Sci Rep. 2017, 7:15255. [CrossRef]
- Tripathi D, Rastogi K, Tyagi P, et al.: Comparative Analysis of Collagen and Chitosan-based Dressing for Haemostatic and Wound Healing Application. AAPS PharmSciTech. 2021, 22:76. [CrossRef]
- Álvarez-Castillo E, Aguilar JM, Bengoechea C, López-Castejón ML, Guerrero A: Rheology and Water Absorption Properties of Alginate–Soy Protein Composites. Polymers. 2021, 13:1807. [CrossRef]
- Jensen G, Holloway JL, Stabenfeldt SE: Hyaluronic Acid Biomaterials for Central Nervous System Regenerative Medicine. Cells. 2020, 9:2113. [CrossRef]
- Nelson DW, Gilbert RJ: Extracellular matrix-mimetic hydrogels for treating neural tissue injury: a focus on fibrin, hyaluronic acid, and elastin-like polypeptide hydrogels. Adv Healthc Mater. 2021, 10:e2101329. [CrossRef]
- Grabska-Zielińska S, Sionkowska A: How to Improve Physico-Chemical Properties of Silk Fibroin Materials for Biomedical Applications?—Blending and Cross-Linking of Silk Fibroin—A Review. Materials. 2021, 14:1510. [CrossRef]
- Mahmood A, Patel D, Hickson B, DesRochers J, Hu X: Recent Progress in Biopolymer-Based Hydrogel Materials for Biomedical Applications. Int J Mol Sci. 2022, 23:1415. [CrossRef]
- Khaliq T, Sohail M, Minhas MU, et al.: Self-crosslinked chitosan/κ-carrageenan-based biomimetic membranes to combat diabetic burn wound infections. Int J Biol Macromol. 2022, 197:157–68. [CrossRef]
- Klavert J, van der Eerden BCJ: Fibronectin in Fracture Healing: Biological Mechanisms and Regenerative Avenues. Front Bioeng Biotechnol. 2021, 9:663357. [CrossRef]
- Microbial Polyhydroxyalkanoates Granules: An Approach Targeting Biopolymer for Medical Applications and Developing Bone Scaffolds - PMC. Accessed: , 2024. 14 March.
- Sarangthem V, Singh TD, Dinda AK: Emerging Role of Elastin-Like Polypeptides in Regenerative Medicine. Adv Wound Care. 2021, 10:257–69. [CrossRef]
- Sellappan LK, Anandhavelu S, Doble M, Perumal G, Jeon J-H, Vikraman D, Kim H-S: Biopolymer film fabrication for skin mimetic tissue regenerative wound dressing applications. Int J Polym Mater Polym Biomater. 2022, 71:196–207. [CrossRef]
- Varma K, Gopi S: Chapter 7 - Biopolymers and their role in medicinal and pharmaceutical applications. In: Thomas S, Gopi S, Amalraj A, eds. Biopolymers and their Industrial Applications. Elsevier; 2021. 175–91. [CrossRef]
- Mao J, Zhao L, De Yao K, Shang Q, Yang G, Cao Y. Study of novel chitosan-gelatin artificial skin in vitro. J Biomed Mater Res A. 2003 Feb 1;64(2):301-8. [CrossRef]
- Little CJ, Bawolin NK, Chen X: Mechanical Properties of Natural Cartilage and Tissue-Engineered Constructs. Tissue Eng Part B Rev. 2011, 17:213–27. [CrossRef]
- Kulinets I: 1 - Biomaterials and their applications in medicine. In: Amato SF, Ezzell RM, eds. Regulatory Affairs for Biomaterials and Medical Devices. Woodhead Publishing; 2015. 1–10. [CrossRef]
- Deng M, Kumbar SG, Wan Y, Toti US, Allcock HR, Laurencin CT: Polyphosphazene polymers for tissue engineering: an analysis of material synthesis, characterization and applications. Soft Matter. 2010, 6:3119–32. [CrossRef]
- Schatzlein, AG. Non-viral vectors in cancer gene therapy: principles and progress. Anticancer Drugs. 2001 Apr;12(4):275-304. [CrossRef]
- Kumar N, Langer RS, Domb AJ: Polyanhydrides: an overview. Adv Drug Deliv Rev. 2002, 54:889–910. [CrossRef]
- Leong KW, Kost J, Mathiowitz E, Langer R: Polyanhydrides for controlled release of bioactive agents. Biomaterials. 1986, 7:364–71. [CrossRef]
- Torres MP, Determan AS, Anderson GL, Mallapragada SK, Narasimhan B: Amphiphilic polyanhydrides for protein stabilization and release. Biomaterials. 2007, 28:108–16. [CrossRef]
- Varma K, Gopi S: Biopolymers and their role in medicinal and pharmaceutical applications. In: Biopolymers and their Industrial Applications. Elsevier; 2021. 175–91. [CrossRef]
- Yang X, Zhao K, Chen G-Q: Effect of surface treatment on the biocompatibility of microbial polyhydroxyalkanoates. Biomaterials. 2002, 23:1391–7. [CrossRef]
- Ciapetti G, Granchi D, Savarino L, Cenni E, Magrini E, Baldini N, Giunti A: In vitro testing of the potential for orthopedic bone cements to cause apoptosis of osteoblast-like cells. Biomaterials. 2002, 23:617–27. [CrossRef]
- Lee WK, Park KD, Keun Han D, Suh H, Park J-C, Kim YH: Heparinized bovine pericardium as a novel cardiovascular bioprosthesis. Biomaterials. 2000, 21:2323–30. [CrossRef]
- Rundén-Pran E, Mariussen E, El Yamani N, Elje E, Longhin EM, Dusinska M: The colony forming efficiency assay for toxicity testing of nanomaterials—Modifications for higher-throughput. Front Toxicol. 2022, 4:983316. [CrossRef]
- Kumar Gupta G, De S, Franco A, Balu AM, Luque R: Sustainable Biomaterials: Current Trends, Challenges and Applications. Molecules. 2015, 21:48. [CrossRef]
- Dutta V, Verma R, Gopalkrishnan C, Yuan M-H, Batoo KM, Jayavel R, Chauhan A, Lin K-YA, Balasubramani R, Ghotekar S. Bio-Inspired Synthesis of Carbon-Based Nanomaterials and Their Potential Environmental Applications: A State-of-the-Art Review. Inorganics, 1: 10(10).
- Nongbet A, Mishra AK, Mohanta YK, et al.: Nanofertilizers: A Smart and Sustainable Attribute to Modern Agriculture. Plants. 2022, 11:2587. [CrossRef]
- Xiang Y, Xin L, Hu J, Li C, Qi J, Hou Y, Wei X. Advances in the Applications of Graphene-Based Nanocomposites in Clean Energy Materials. Crystals. 2021; 11(1):47.
- R R, Philip E, Madhavan A, et al.: Advanced biomaterials for sustainable applications in the food industry: Updates and challenges. Environ Pollut. 2021, 283:117071. [CrossRef]
- Huzum B, Puha B, Necoara RM, et al.: Biocompatibility assessment of biomaterials used in orthopedic devices: An overview (Review). Exp Ther Med. 2021, 22:1315. [CrossRef]
| Serial No. | Biomaterial | Source | Application | Reference |
|---|---|---|---|---|
| 1 | Poly(lactic-co-glycolic acid) (PLGA) | lactic acid and glycolic acid | Microspheres, nanoparticles, implants | [77] |
| 2 | Liposomes | phospholipids | Targeted drug delivery, gene therapy | [78] |
| 3 | Alginate | algae | Controlled drug release, wound healing | [79] |
| 4 | Chitosan | chitin | Oral drug delivery, wound dressingsrazmak | [80] |
| 5 | Hyaluronic Acid (HA) | human body, particularly in connective tissues, joints, and skin | Ophthalmic, joint injections, skin creams | [81] |
| 6 | Polyethylene Glycol (PEG) | ethylene oxide | Nanoparticles, conjugates | [82] |
| 7 | Cyclodextrins | starch | Increasing drug solubility | [83] |
| 8 | Dendrimers | synthetic macromolecules | Targeted drug delivery, gene therapy | [84] |
| 9 | Polylactic Acid (PLA) | renewable resources | Nanoparticles, implants | [85] |
| 10 | Polymeric Micelles | renewable resources or petrochemical-derived sources | Solubilization and delivery of hydrophobic drugs | [86] |
| 11 | Poly(methoxyl ethylene glycolcaprolactonecomethacrylic acid-co-poly(ethylene glycol)methylethylenemethacrylate) | chemical synthesis | For oral drug delivery | [87] |
| 12 | Alginate and chemically modified carboxymethyl chitosan | Algae, chitin | For oral drug delivery | [87] |
| 13 | Gelatin | Bovine or porcine collagen | deliver anti-inflammatory, antibacterial, and antineoplastic agents | [88] |
| 14 | Nanocellulose | Drug delivery | [37] | |
| 15 | Collagen | Natural ECM or recombinant | Drug delivery | [89] |
| 16 | Lipid Nanoparticles (LNPs) | - | Deliver mRNA and other vaccine components efficiently. | [90] |
| 17 | Cell-Based Vaccines | - | Use cultured cells to produce antigens for vaccine development | [91] |
| 18 | Adjuvants (Aluminum salts) | - | Enhance immune response and vaccine efficacy | [92] |
| 19 | Polyhydroxyalkanoates (PHA) | Synthetic by various microorganisms | Drug delivery | [93] |
| 20 | Silk Fibroin | Silkworm | controlled release of therapeutics, including proteins, peptides, and small molecules. | [37] |
| Serial No. | Biomaterial | Source | Application | Reference |
|---|---|---|---|---|
| 1 | Collagen | Animal tissues skin,razmakBones | Surface coating for tissue culture plates | [105] |
| 2 | Alginate | Brown algae | Regenerative medicine, Tissue engineering | [106] |
| 3 | Hyaluronic acidrazmak | Rooster combs bacteria | Treatment and lubrication of damaged joints, Cutaneous and corneal wound healing | [107] |
| 4 | Fibrin | Blood plasma | Blood clotting, Wound healing, and tumor growth, Hemostatic agent, sealant, and surgical glue, Regenerative medicine | [108] |
| 5 | Silk fibroin | Silkworm silk | Bioengineering of tissues, Treatment of wounds, Bioengineering of tissues | [109] |
| 6 | Agarose | Red algae | Skeletal tissues regeneration, kidney and fibroblast encapsulation | [110] |
| 7 | Carrageenan | Red algae | Skeletal tissues regeneration, Cell delivery system | [111] |
| 8 | Fibronectin | Animal tissues | Wound healing, Cardiac repair, Bone regeneration | [112] |
| 9 | PHAs | Bacteria | Drug delivery systems, One tissue regeneration | [113] |
| 10 | Elastin | Animal tissues arteries | Soft-tissue reconstruction, Orthopedics and cell encapsulation | [114] |
| 11 | Keratin | Animal tissues | Cornea tissue engineering, Skin regeneration | [115] |
| 12 | Starch | Plants | Bone and cartilage regeneration,Spinal cord injury treatment | [116] |
| 13 | Gelatin | skin, bones, and connective tissues of animals, | Stem cell therapy | [117] |
| 14 | Polyester | petrochemicals | Fracture fixations, Tissue augmentation, Cartilage repair, Dental implants, Cardiac patches, Ear implants, Cartilage repair, Nerve repair | [118,119] |
| 15 | Polyphosphazenes | phosphorus and nitrogen-containing compounds | Delivery of vaccines, Gene delivery | [120,121] |
| 16 | Poly anhydrides | dicarboxylic acids | Drug delivery, Antigen delivery, Peptide delivery | [122,123,124] |
| 17 | Polyurethanes | petrochemicals | Medical devices, Drug delivery | [125] |
| 18 | Poly(n-isopropyl acrylamide-copropylacrylicacid-co-butyl acrylate) | Synthetic polymer, produced through chemical synthesis. | To improve angiogenesis in infracted myocardium | [87] |
| 19 | Poly(acrylamide)-g-carrageenan and sodium alginate | Carrageenan,razmakSodium Alginate | For colon-targeted delivery | [87] |
| 20 | Conjugated linoleic acid coupled with pluronic F-127, PLGA–PEG–PLGA | razmak- | Peritoneal dissemination of gastric cancer, Treatment of type II Diabetes | [87] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




