Submitted:
30 August 2024
Posted:
30 August 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Epithelial Wavefront Analysis
Clinical Examination
Statistical Analysis
3. Results
4. Discussion
5. Conclusions
- This study introduces a novel and easy-to-use biomarker, suitable for discrimination between healthy and EBMD eyes: the epithelial wavefront error.
- This study provides evidence of smoothing of the corneal epithelium and reduction of epithelial wavefront error after PTK
Author Contributions
Funding
Conflicts of Interest
References
- Weiss, J.S., et al., IC3D Classification of Corneal Dystrophies-Edition 3. Cornea, 2024. 43(4): p. 466-527. [CrossRef]
- Møller, H.U. and J.S. Weiss, IC3D classification of corneal dystrophies. Dev Ophthalmol, 2011. 48: p. 1-8. [CrossRef]
- Weiss, J.S., et al., IC3D classification of corneal dystrophies--edition 2. Cornea, 2015. 34(2): p. 117-59. [CrossRef]
- Brown, N. and A. Bron, Recurrent erosion of the cornea. Br J Ophthalmol, 1976. 60(2): p. 84-96.
- Laibson, P.R., Recurrent corneal erosions and epithelial basement membrane dystrophy. Eye Contact Lens, 2010. 36(5): p. 315-7.
- Gupta, P.K., et al., Prevalence of ocular surface dysfunction in patients presenting for cataract surgery evaluation. J Cataract Refract Surg, 2018. 44(9): p. 1090-1096.
- Boutboul, S., et al., A subset of patients with epithelial basement membrane corneal dystrophy have mutations in TGFBI/BIGH3. Hum Mutat, 2006. 27(6): p. 553-7.
- Watson, S.L. and V. Leung, Interventions for recurrent corneal erosions. Cochrane Database Syst Rev, 2018. 7(7): p. Cd001861. [CrossRef]
- Adams, C., et al., [Phototherapeutic keratectomy for epithelial basement membrane dystrophy : Impact of excimer laser systems used on the changes of visual acuity, refraction and astigmatism]. Ophthalmologie, 2022. 119(9): p. 945-951.
- Ohman, L. and P. Fagerholm, The influence of excimer laser ablation on recurrent corneal erosions: a prospective randomized study. Cornea, 1998. 17(4): p. 349-52.
- Maini, R. and M.S. Loughnan, Phototherapeutic keratectomy re-treatment for recurrent corneal erosion syndrome. Br J Ophthalmol, 2002. 86(3): p. 270-2. [CrossRef]
- Goerlitz-Jessen, M.F., P.K. Gupta, and T. Kim, Impact of epithelial basement membrane dystrophy and Salzmann nodular degeneration on biometry measurements. J Cataract Refract Surg, 2019. 45(8): p. 1119-1123.
- Yeu, E., O. Hashem, and H. Sheha, Treatment of Epithelial Basement Membrane Dystrophy to Optimize the Ocular Surface Prior to Cataract Surgery. Clin Ophthalmol, 2022. 16: p. 785-795.
- Bellucci, C., et al., Acuity and Quality of Vision in Eyes with Epithelial Basement Membrane Dystrophy after Regular Pseudophakia. J Clin Med, 2023. 12(3).
- Pérez-Santonja, J.J., et al., Severe corneal epithelial sloughing during laser in situ keratomileusis as a presenting sign for silent epithelial basement membrane dystrophy. J Cataract Refract Surg, 2005. 31(10): p. 1932-7.
- Buffault, J., et al., Assessment of corneal epithelial thickness mapping in epithelial basement membrane dystrophy. PLoS One, 2020. 15(11): p. e0239124.
- Levy, A., et al., Corneal Epithelial Thickness Mapping in the Diagnosis of Ocular Surface Disorders Involving the Corneal Epithelium: A Comparative Study. Cornea, 2022. 41(11): p. 1353-1361.
- Canto-Cerdan, M., et al., Corneal Epithelium Thickness and Refractive Changes After Myopic Laser Corneal Refractive Surgery. J Refract Surg, 2022. 38(9): p. 602-608.
- World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. Jama, 2013. 310(20): p. 2191-4.
- Feng, Y., et al., Epithelial Thickness Mapping in Keratoconic Corneas: Repeatability and Agreement Between CSO MS-39, Heidelberg Anterion, and Optovue Avanti OCT Devices. J Refract Surg, 2023. 39(7): p. 474-480.
- Mason, S.J. and N.E. Graham, Areas beneath the relative operating characteristics (ROC) and relative operating levels (ROL) curves: Statistical significance and interpretation. Quarterly Journal of the Royal Meteorological Society, 2002. 128(584): p. 2145-2166.
- Thiele, C. and G. Hirschfeld, cutpointr: Improved Estimation and Validation of Optimal Cutpoints in R. Journal of Statistical Software, 2021. 98(11): p. 1 - 27.
- Shajari, M., et al., Katarakt- und Linsenchirurgie. 2022: Springer Berlin Heidelberg.
- Tobalem, S., et al., Myopic outcomes after excimer laser phototherapeutic keratectomy (PTK). J Fr Ophtalmol, 2021. 44(1): p. 35-40.
- Grauvogl, V., et al., [Phototherapeutic keratectomy for recurrent corneal erosion of various epithelial origins: influence of depth of ablation on pachymetry and refraction]. Ophthalmologe, 2022.
- Kepez Yildiz, B., et al., Changes in Higher-Order Aberrations After Phototherapeutic Keratectomy for Subepithelial Corneal Infiltrates After Epidemic Keratoconjunctivitis. Cornea, 2017. 36(10): p. 1233-1236.
- Wilson, S.E., Bowman's layer in the cornea- structure and function and regeneration. Exp Eye Res, 2020. 195: p. 108033.
- Eghrari, A.O., S.A. Riazuddin, and J.D. Gottsch, Overview of the Cornea: Structure, Function, and Development. Prog Mol Biol Transl Sci, 2015. 134: p. 7-23.
| Epithelial thickness | EBMD (n = 32) |
Control group (n = 32) |
p-value* |
|---|---|---|---|
| Mean (µm) |
58 ± 9 Range 46 to 87 |
51 ± 3 Range 45 to 60 |
< 0.001 |
| Min (µm) |
40 ± 8 Range 26 to 64 |
43 ± 5 Range 35 to 56 |
0.03 |
| Max (µm) |
70 ± 12 Range 53 to 101 |
57 ± 5 Range 52 to 74 |
< 0.001 |
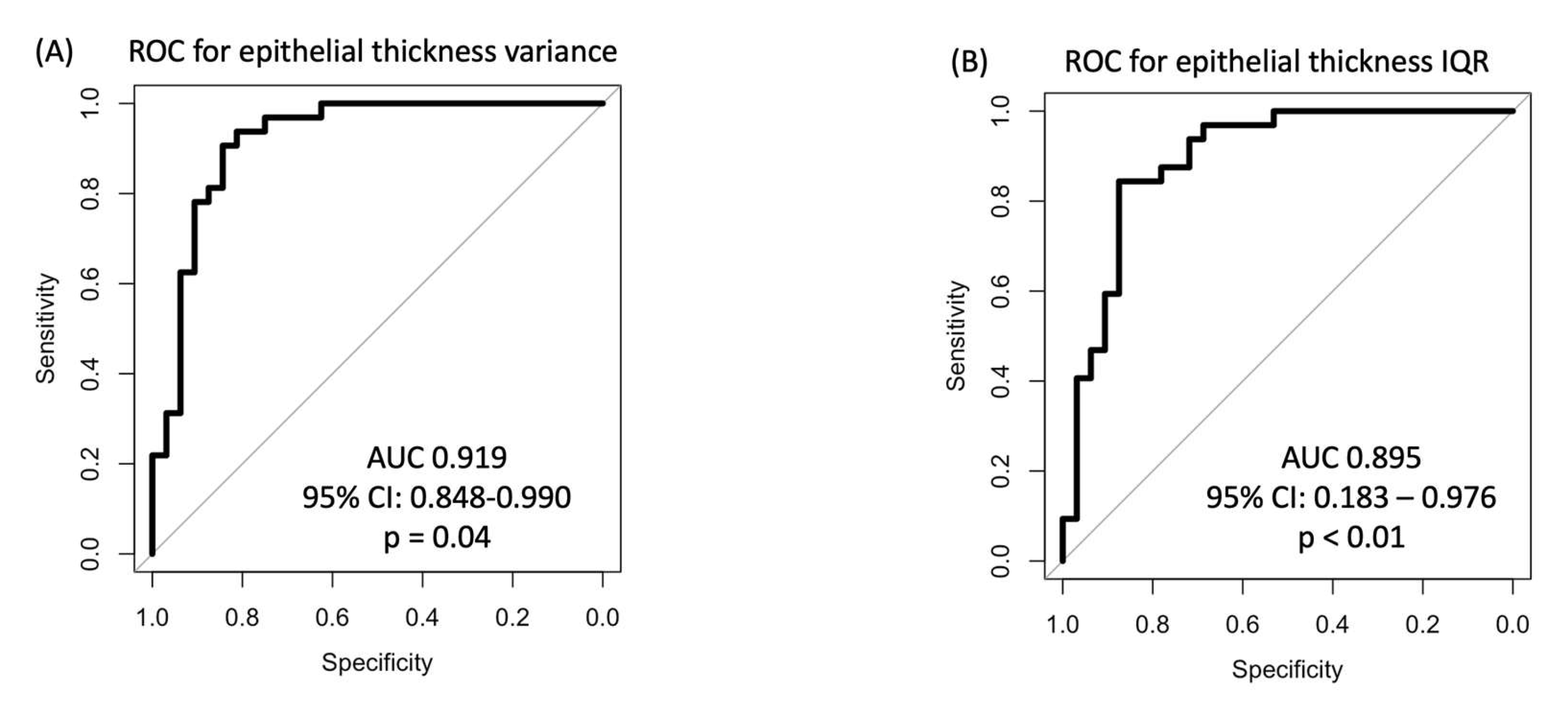
| IQR (µm) |
11 ± 7 Range 1 to 28 |
3 ± 2 Range 1 to 10 |
< 0.001 |
| Variance (µm2) |
60 ± 57 Range 3 to 224 |
8 ± 6 Range 1 to 29 |
< 0.001 |
| WFE components | EBMD (n = 32) |
Control group (n = 32) |
p-value* |
|---|---|---|---|
| Spherical WFE (D) |
-0.85 ± 1.00 Range -3.45 to 0.81 |
-0.07 ± 0.31 Range -0.51 to 0.79 |
< 0.001 |
| Cylindrical WFE (D) |
-0.75 ± 0.36 Range -1.69 to -0.28 |
-0.45 ± 0.11 Range -0.75 to -0.34 |
< 0.001 |
| Spherical aberration RMS (µm) |
0.32 ± 0.30 Range 0.00 to 1.13 |
0.09 ± 0.06 Range 0.01 to 0.22 |
< 0.001 |
| Coma RMS (µm) |
0.55 ± 0.36 Range 0.08 to 1.23 |
0.14 ± 0.09 Range 0.02 to 0.38 |
< 0.001 |
| Trefoil RMS (µm) |
0.38 ± 0.38 Range 0.04 to 2.21 |
0.12 ± 0.06 Range 0.01 to 0.29 |
< 0.001 |
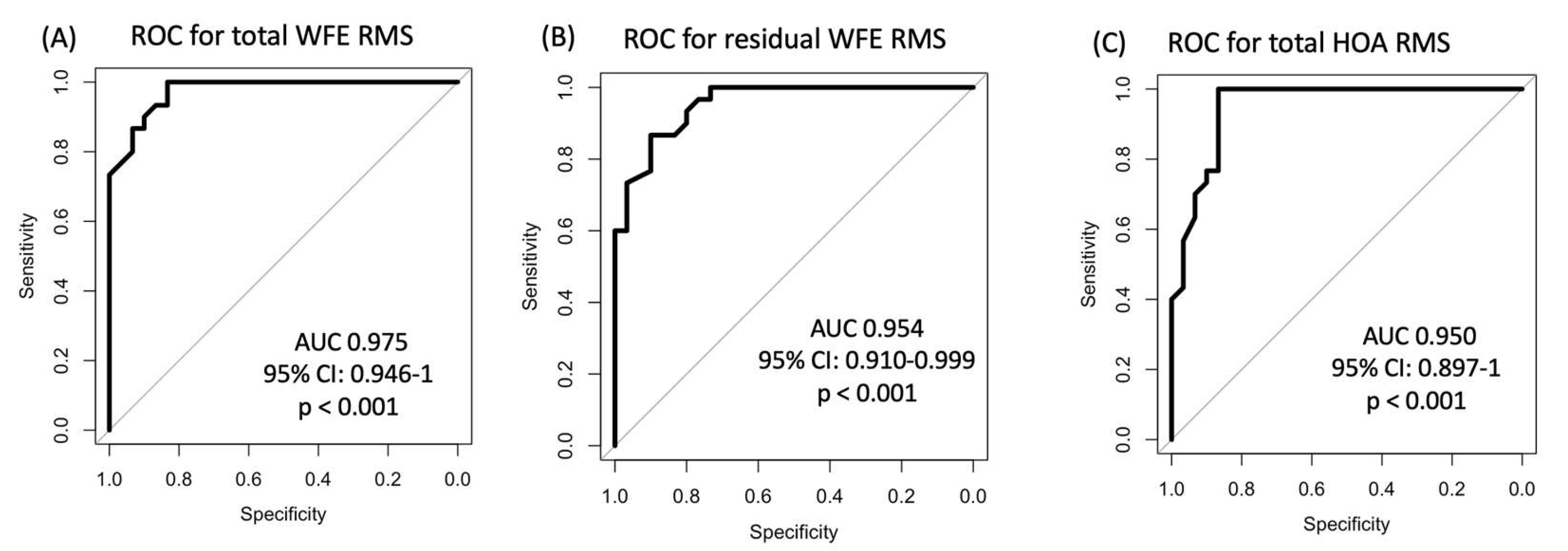
| Total HOAs RMS (µm) |
1.12 ± 0.63 Range 0.28 to 2.91 |
0.33 ± 0.10 Range 0.17 to 0.52 |
< 0.001 |
| Total WFE RMS (µm) |
2.14 ± 1.20 Range 0.73 to 4.78 |
0.62 ± 0.20 Range 0.26 to 1.07 |
< 0.001 |
| Residual WFE RMS (µm) |
0.88 ± 0.66 Range 0.25 to 3.49 |
0.27 ± 0.09 Range 0.15 to 0.48 |
< 0.001 |
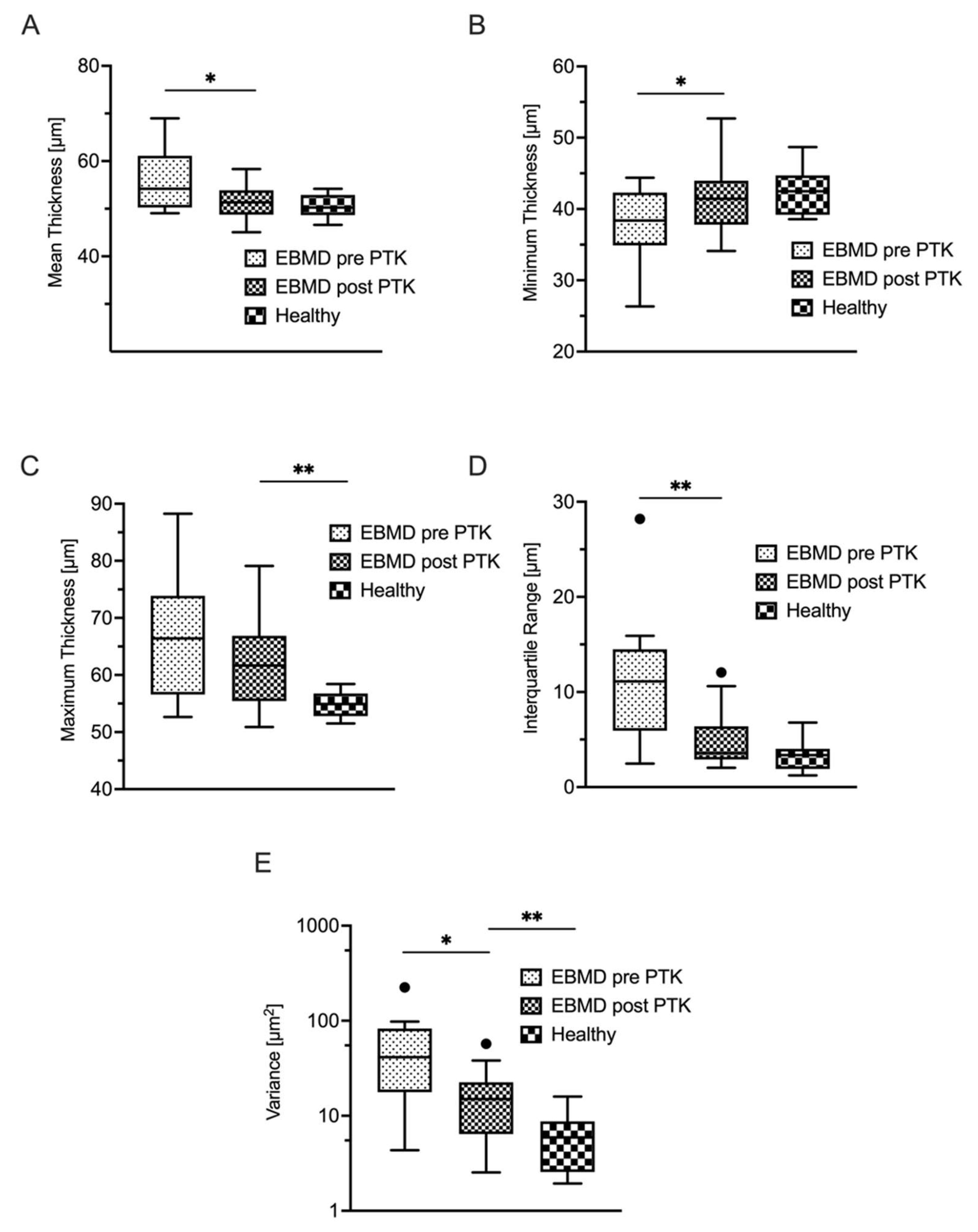
| Epithelial thickness | Pre-PTK (n = 17) |
Post-PTK (n = 17) |
p-value* |
|---|---|---|---|
| Mean (µm) |
56 ± 7 Range 49 to 69 |
52 ± 4 Range 45 to 58 |
0.03 |
| Min (µm) |
38 ± 5 Range 26 to 44 |
42 ± 5 Range 35 – 53 |
0.02 |
| Max (µm) |
67 ± 11 Range 53 to 88 |
62 ± 8 Range 51 to 79 |
0.10 |
| IQR (µm) |
11 ± 7 Range 3 to 28 |
5 ± 3 Range 2 to 12 |
< 0.01 |
| Variance (µm2) |
56 ± 54 Range 4 to 224 |
18 ± 15 Range 3 to 57 |
0.01 |
| WFE components | Pre-PTK (n = 17) |
Post-PTK (n = 17) |
p-value* |
|---|---|---|---|
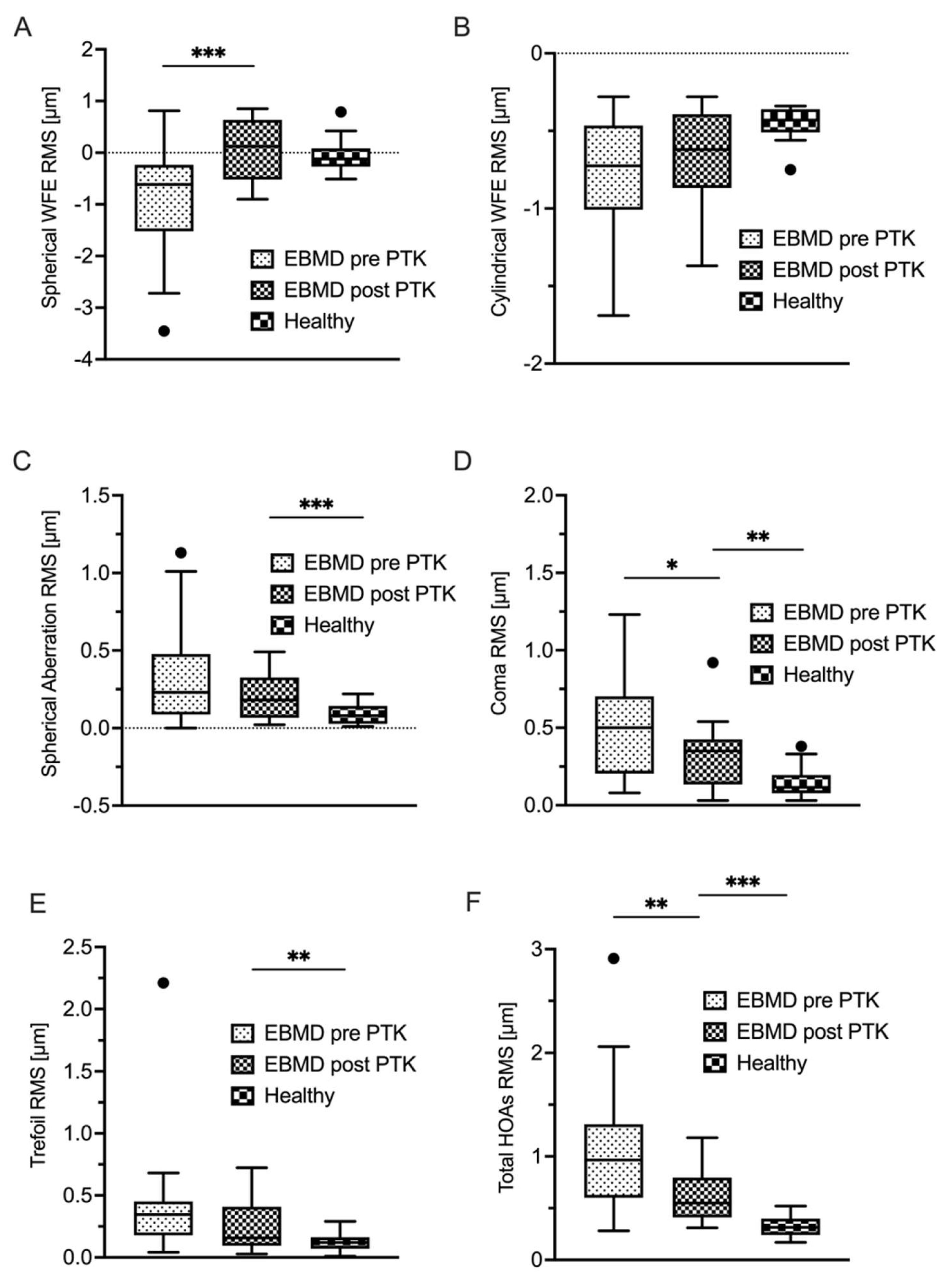
| Spherical WFE (D) |
-1.00 ± 0.96 Range -3.61 to -0.10 |
0.07 ± 0.57 Range -0.90 to 0.85 |
< 0.001 |
| Cylindrical WFE (D) |
0.69 ± 0.38 Range -1.31 to -0.28 |
-0.68 ± 0.34 Range -1.37 to -0.28 |
0.36 |
| Spherical aberration RMS (µm) |
0.29 ± 0.34 Range 0.00 to 1.13 |
0.20 ± 0.16 Range 0.02 to 0.49 |
0.14 |
| Coma RMS (µm) |
0.53 ± 0.39 Range 0.08 to 1.23 |
0.32 ± 0.22 Range 0.03 to 0.92 |
0.03 |
| Trefoil RMS (µm) |
0.30 ± 0.15 Range 0.04 to 0.55 |
0.25 ± 0.20 Range 0.03 to 0.72 |
0.11 |
| Total HOAs RMS (µm) | 0.62 ± 0.51 Range 0.28 to 2.06 |
0.63 ± 0.26 Range 0.31 to 1.18 |
< 0.01 |
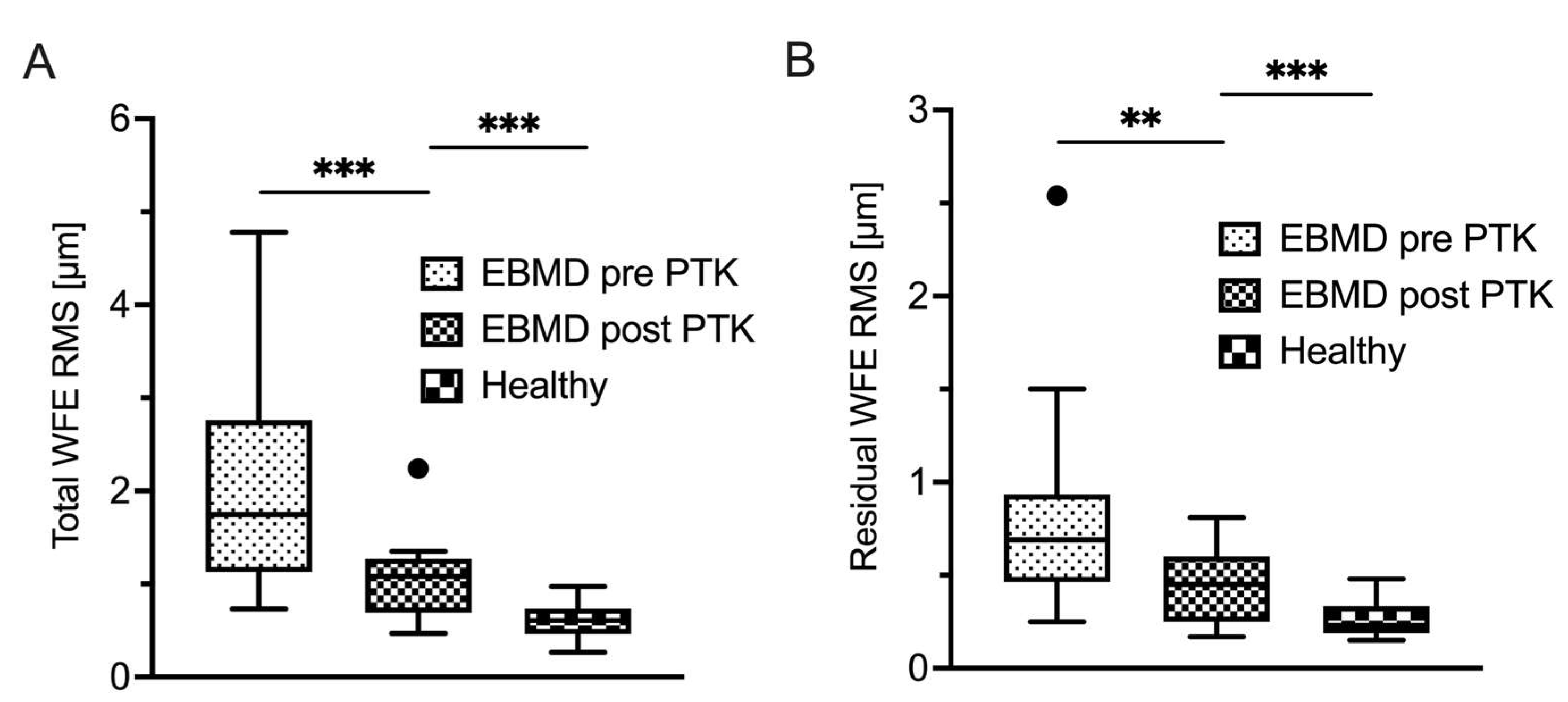
| Total WFE RMS (µm) |
2.04 ± 1.17 Range 0.73 to 4.70 |
1.07 ± 0.41 Range 0.47 to 2.24 |
< 0.001 |
| Residual WFE RMS (µm) |
0.72 ± 0.35 Range 0.25 to 1.50 |
0.46 ± 0.20 Range 0.17 to 0.81 |
< 0.01 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




