Submitted:
22 August 2024
Posted:
23 August 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Statistical Analysis
3. Results
3.1. Clinical and Demographic Characteristics before and after the Onset of COVID-19
3.2. Attendance Rates before and after the Onset of COVID-19
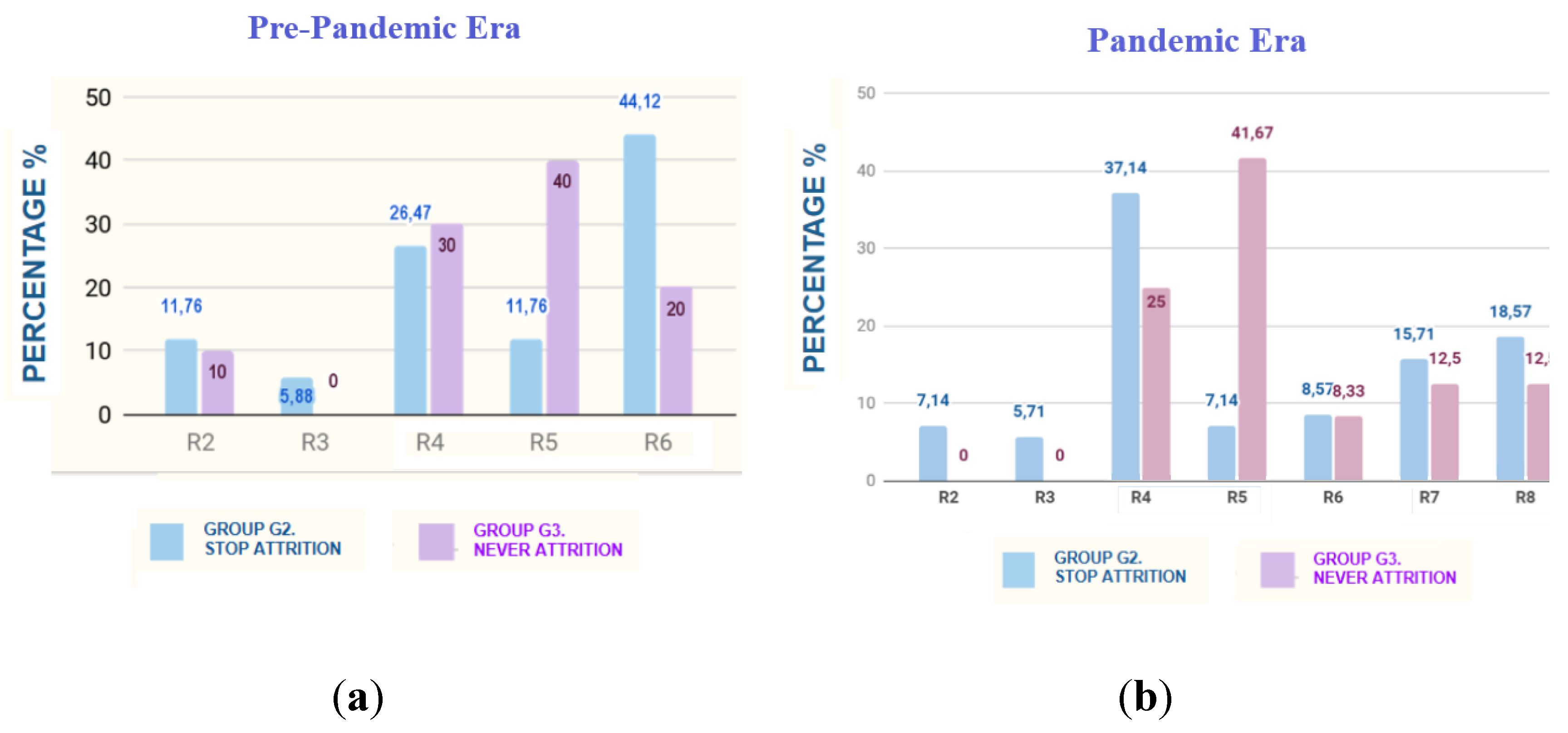
3.2.1. Reasons for Non-Attendance
3.2.2. Comparisons between Groups before the Onset of COVID-19
3.2.3. Comparisons between Groups after the Onset of COVID-19
3.2.4. Multiple Regression Analysis
4. Discussion
4.1. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
References
- Blencowe H, Cousens S, Oestergaard MZ, Chou D, Moller AB, Narwal R, et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. The Lancet. 2012 Jun;379(9832):2162–72. [CrossRef]
- World Health Organization. Preterm birth [Internet]. 2023 [cited 2023 May 28]. Available from: https://www.who.int/news-room/fact-sheets/detail/preterm-birth.
- McCormick MC, Litt JS, Smith VC, Zupancic JAF. Prematurity: An Overview and Public Health Implications. Annu Rev Public Health. 2011 Apr 21;32(1):367–79. [CrossRef]
- Litt JS, Campbell DE. High-Risk Infant Follow-Up After NICU Discharge. Clin Perinatol. 2023 Mar;50(1):225–38. [CrossRef]
- Spittle A, Treyvaud K. The role of early developmental intervention to influence neurobehavioral outcomes of children born preterm. Semin Perinatol. 2016 Dec;40(8):542–8. [CrossRef]
- Patra K, Greene MM, Perez B, Silvestri JM. Neonatal high-risk follow-up clinics: How to improve attendance in very low birth weight infants. EJ Neonatal Res. 2014;4(1):3–12.
- McGowan EC, Vohr BR. Neurodevelopmental Follow-up of Preterm Infants. Pediatr Clin North Am. 2019 Apr;66(2):509–23. [CrossRef]
- Purdy IB, Melwak MA. Who Is at Risk? High-Risk Infant Follow-up. Newborn Infant Nurs Rev. 2012 Dec;12(4):221–6. [CrossRef]
- Orton J, Spittle A, Doyle L, Anderson P, Boyd R. Do early intervention programmes improve cognitive and motor outcomes for preterm infants after discharge? A systematic review: Early Intervention for Preterm Infants. Dev Med Child Neurol. 2009 Nov;51(11):851–9. [CrossRef]
- LW, Anderson PJ, Battin M, Bowen JR, Brown N, Callanan C, et al. Long term follow up of high risk children: who, why and how? BMC Pediatr. 2014 Dec;14(1):279. [CrossRef]
- Ayala L, Winter S, Byrne R, Fehlings D, Gehred A, Letzkus L, et al. Assessments and Interventions for Spasticity in Infants With or at High Risk for Cerebral Palsy: A Systematic Review. Pediatr Neurol. 2021 May;118:72–90. [CrossRef]
- Kuppala VS, Tabangin M, Haberman B, Steichen J, Yolton K. Current state of high-risk infant follow-up care in the United States: results of a national survey of academic follow-up programs. J Perinatol. 2012;32(4):293–8. [CrossRef]
- Tang B. The State of Neonatal Follow-Up Programs. In: Needelman H, Jackson BJ, editors. Follow-Up for NICU Graduates: Promoting Positive Developmental and Behavioral Outcomes for At-Risk Infants [Internet]. Cham: Springer International Publishing; 2018 [cited 2024 Jun 12]. p. 337–41. Available from. [CrossRef]
- Vohr BR, O’Shea M, Wright LL. Longitudinal multicenter follow-up of high-risk infants: why, who, when, and what to assess. Semin Perinatol. 2003 Aug 1;27(4):333–42. [CrossRef]
- Bhutta AT, Cleves MA, Casey PH, Cradock MM, Anand KJS. Cognitive and Behavioral Outcomes of School-Aged Children Who Were Born Preterm: A Meta-analysis. JAMA. 2002 Aug 14;288(6):728. [CrossRef]
- Maitre NL, Duncan AF. Neurologic and Developmental Outcomes of High-Risk Neonates. Clin Perinatol. 2023 Mar;50(1):xxi–xxii. [CrossRef]
- Perenyi A, Katz J, Flom P, Regensberg S, Sklar T. Analysis of compliance, morbidities and outcome in neurodevelopmental follow-up visits in urban African-American infants at environmental risk. J Dev Orig Health Dis. 2010 Dec;1(6):396–402. [CrossRef]
- Tang B, Lee H, Gray E, Gould J, Hintz S. Programmatic and Administrative Barriers to High-Risk Infant Follow-Up Care. Am J Perinatol. 2018 Aug;35(10):940–5. [CrossRef]
- Ballantyne M, Stevens B, Guttmann A, Willan AR, Rosenbaum P. Transition to Neonatal Follow-up Programs: Is Attendance a Problem? J Perinat Neonatal Nurs. 2012;26(1):90–8. [CrossRef]
- Harmon SL, Conaway M, Sinkin RA, Blackman JA. Factors associated with neonatal intensive care follow-up appointment compliance. Clin Pediatr (Phila). 2013;52(5):389–96. [CrossRef]
- Brady JM, Pouppirt N, Bernbaum J, D’Agostino JA, Gerdes M, Hoffman C, et al. Why do children with severe bronchopulmonary dysplasia not attend neonatal follow-up care? Parental views of barriers. Acta Paediatr. 2018 Jun;107(6):996–1002. [CrossRef]
- Swearingen C, Simpson P, Cabacungan E, Cohen S. Social disparities negatively impact neonatal follow-up clinic attendance of premature infants discharged from the neonatal intensive care unit. J Perinatol. 2020 May;40(5):790–7. [CrossRef]
- DeMauro SB, Bellamy SL, Fernando M, Hoffmann J, Gratton T, Schmidt B, et al. Patient, Family, and Center-Based Factors Associated with Attrition in Neonatal Clinical Research: A Prospective Study. Neonatology. 2019;115(4):328–34. [CrossRef]
- Duarte ED, Tavares TS, Cardoso IVL, Vieira CS, Guimarães BR, Bueno M. Factors associated with the discontinuance of outpatient follow-up in neonatal units. Rev Bras Enferm. 2020;73(3):e20180793. [CrossRef]
- Ballantyne M, Benzies K, Rosenbaum P, Lodha A. Mothers’ and health care providers’ perspectives of the barriers and facilitators to attendance at Canadian neonatal follow-up programs. Child Care Health Dev. 2015 Sep;41(5):722–33. [CrossRef]
- Hintz SR, Gould JB, Bennett MV, Lu T, Gray EE, Jocson MAL, et al. Factors Associated with Successful First High-Risk Infant Clinic Visit for Very Low Birth Weight Infants in California. J Pediatr. 2019 Jul;210:91-98.e1. [CrossRef]
- Ballantyne M, Stevens B, Guttmann A, Willan AR, Rosenbaum P. Maternal and infant predictors of attendance at Neonatal Follow-Up programmes. Child Care Health Dev. 2014;40(2):250–8. [CrossRef]
- Kim NH, Youn YA, Cho SJ, Hwang JH, Kim EK, Kim EAR, et al. The predictors for the non-compliance to follow-up among very low birth weight infants in the Korean neonatal network. Gurgel RQ, editor. PLOS ONE. 2018 Oct 1;13(10):e0204421. [CrossRef]
- Nehra V, Pici M, Visintainer P, Kase JS. Indicators of compliance for developmental follow-up of infants discharged from a regional NICU. J Perinat Med. 2009;37(6):677–81. [CrossRef]
- Tuczyńska M, Matthews-Kozanecka M, Baum E. Accessibility to Non-COVID Health Services in the World During the COVID-19 Pandemic: Review. Front Public Health. 2021 Dec 16;9:760795. [CrossRef]
- De Biase S, Cook L, Skelton DA, Witham M, ten Hove R. The COVID-19 rehabilitation pandemic. Age Ageing. 2020 Aug 24;49(5):696–700. [CrossRef]
- Kondilis E, Tarantilis F, Benos A. Essential public healthcare services utilization and excess non-COVID-19 mortality in Greece. Public Health. 2021 Sep;198:85–8. [CrossRef]
- Roberton T, Carter ED, Chou VB, Stegmuller AR, Jackson BD, Tam Y, et al. Early estimates of the indirect effects of the COVID-19 pandemic on maternal and child mortality in low-income and middle-income countries: a modelling study. Lancet Glob Health. 2020 Jul;8(7):e901–8. [CrossRef]
- Erdei C, Liu CH. The downstream effects of COVID-19: a call for supporting family wellbeing in the NICU. J Perinatol. 2020 Sep;40(9):1283–5. [CrossRef]
- Fazzi E, Galli J. New clinical needs and strategies for care in children with neurodisability during COVID-19. Dev Med Child Neurol. 2020 Jul;62(7):879–80. [CrossRef]
- Fraiman YS, Edwards EM, Horbar JD, Mercier CE, Soll RF, Litt JS. Racial Inequity in High-Risk Infant Follow-Up Among Extremely Low Birth Weight Infants. Pediatrics. 2023 Feb 1;151(2):e2022057865. [CrossRef]
- Fuller MG, Lu T, Gray EE, Jocson MAL, Barger MK, Bennett M, et al. Rural Residence and Factors Associated with Attendance at the Second High-Risk Infant Follow-up Clinic Visit for Very Low Birth Weight Infants in California. Am J Perinatol. 2023 Apr;40(05):546–56. [CrossRef]
- Attar MA, Gates MR, Iatrow AM, Lang SW, Bratton SL. Barriers to Screening Infants for Retinopathy of Prematurity after Discharge or Transfer from a Neonatal Intensive Care Unit. J Perinatol. 2005 Jan 1;25(1):36–40. [CrossRef]
- Panda S, Somu R, Maitre N, Levin G, Singh AP. Impact of the Coronavirus Pandemic on High-Risk Infant Follow-Up (HRIF) Programs: A Survey of Academic Programs. Children. 2021 Oct 6;8(10):889.Roberts HJ, Harris RM, Krehbiel. [CrossRef]
- C, Banks B, Jackson B, Needelman H. Examining disparities in the long term follow-up of Neonatal Intensive Care Unit graduates in Nebraska, U.S.A. J Neonatal Nurs. 2016 Oct;22(5):250–6. [CrossRef]
- Watson L, Woods CW, Cutler A, DiPalazzo J, Craig AK. Telemedicine Improves Rate of Successful First Visit to NICU Follow-up Clinic. Hosp Pediatr. 2023 Jan 1;13(1):3–8. [CrossRef]
- Caporali C, Pisoni C, Naboni C, Provenzi L, Orcesi S. Challenges and opportunities for early intervention and neurodevelopmental follow-up in preterm infants during the COVID-19 pandemic. Child Care Health Dev. 2021 Jan;47(1):140–1. [CrossRef]
- Christner LP, Irani S, McGowan C, Dabaja E, Dejong C, Attar MA. Previous missed visits and independent risk of loss to follow-up in the high-risk neonatal follow-up clinic. Early Hum Dev. 2023 Aug;183:105813. [CrossRef]
| Reasons for Νon-Attendance (R) | Categorization |
|---|---|
| R1 | Lack of health insurance |
| R2 | Accessibility (distance of the clinic from the permanent residence / lack of means of transport / change of residence / moving (to another region / country) / bad weather |
| R3 | Loaded parental / family work schedule |
| R4 | Obstacles related to hospital services (Limited availability during clinic hours / Difficulty with parking / Long waiting time / Bad communication with the secretariat / Disappointment from the experience at the hospital. Change (cancellation or postponement) either after consultation (with the Hospital / with Papageorgiou's doctors) or at the initiative of the parents, closed outpatient clinics due to COVID-19 |
| R5 | Negligence - Absence of Specific Reason |
| R6 | Assessment by the parents that monitoring / FU appointment was unnecessary |
| R7 | Health issues / Death in the family |
| R8 | Fear of diseases exposure (to COVID-19 or other diseases) / Difficulties due to Covid-19 (“Because only one parent was allowed to accompany ” or difficulty with Rapid Tests) |
| Characteristics | Pre-Pandemic Era (n=573) |
Pandemic Era (n=564) |
p | OR and 95% CI |
|---|---|---|---|---|
| Gender (Male)a | 315 (54.97) | 283 (50.18) | 0.1091 | 0.82 (0.65-1.04) |
| Birth weight (gr)a | 2090 (1620-2830) | 1830 (1430-2490) | 0.0005 | NA |
| Gestational age (weeks)a | 34.6 (32-37.3) | 33.1 (31.4-35.7) | 0.0003 | NA |
| Age of mothera | 32 (29-38) | 33 (29-38) | 0.3454 | NA |
| Multiparitya | 1 (1-2) | 1 (1-2) | 0.4379 | NA |
| Multiple Gestationb | 104 (34.9) | 137 (34.25) | 0.8724 | 0.97 (0.71-1.33) |
| Small for Gestational Age (SGA)b | 72 (25.09) | 80 (20.89) | 0.2256 | 0.79 (0.55-1.13) |
| Gestational Hypertensionb | 30 (11.03) | 55 (14.82) | 0.1947 | 1.4 (0.87-2.26) |
| Gestational Diabetesb | 34 (13.08) | 127 (36.6) | <.0001 | 3.84 (2.52-5.85) |
| IntraUterine Growth Retardation (IUGR)b | 54 (19.85) | 94 (25.34) | 0.1078 | 1.37 (0.94-2) |
| Delivery mode: Cesarean Section (CS)b | 235 (80.48) | 317 (83.42) | 0.3607 | 0.82 (0.55-1.22) |
| Antenatal Steroid Administration (ASA)b | 62 (26.72) | 137 (37.53) | 0.0075 | 1.65 (1.15-2.36) |
| Respiratory Distress Syndromeb | 87 (29.49) | 173 (42.3) | 0.0005 | 1.75 (1.28-2.41) |
| Bronchopulmonary dysplasiab | 29 (9.83) | 44 (10.76) | 0.7092 | 1.11 (0.67-1.81) |
| Early onset sepsis (<=3 DOL)b | 35 (12.07) | 13 (3.32) | <.0001 | 0.25 (0.13-0.48) |
| Late onset sepsis (>3 DOL)b | 38 (13.1) | 73 (18.39) | 0.0742 | 1.49 (0.98-2.29) |
| Jaundiceb | 236 (64.13) | 277 (63.68) | 0.9412 | 0.98 (0.73-1.31) |
| Necrotizing Enterocolitisb | 6 (2.08) | 15 (3.87) | 0.2623 | 1.9 (0.73-4.95) |
| Retinopathy of Prematurityb | 7 (2.45) | 8 (2.04) | 0.7941 | 0.83 (0.3-2.31) |
| Number of visitsa | 1 (1-4) | 2 (1-3) | 0.8534 | NA |
| Nationality (Foreign)b | 64 (11.17) | 67 (11.88) | 0.7114 | 0.93 (0.65-1.34) |
| Characteristics | G1 group (n=451) | G2 group (n=66) | G3 group (n=53) | G1 vs G2 | G1 vs G3 | ||
|---|---|---|---|---|---|---|---|
| p | OR (95% CI) | p | OR (95% CI) | ||||
| Number of visitsa | 2 (1-5) | 2 (1-3) | 0 (0-0) | 0.329605 | NA | <.0001 | NA |
| Birth weight (gr)a | 2115 (1620-2835) |
1750 (1355-2400) | 2282.5 (1917.5-3290) | 0.008906 | NA | 0.026459 | NA |
| Gestational age (weeks)a | 34.6 (32.1-37.1) | 32.9 (29.7-35.6) | 36.3 (33-38.3) | 0.002245 | NA | 0.010815 | NA |
| Antenatal Steroid Administration (ASA)b | 43 (29.25) | 14 (30.44) | 3 (8.11) | 0.86 | 1.06 (0.51-2.18) | 0.0097 | 4.76 (1.37-16.67) |
| Multiparitya | 1 (1-2) | 1 (1-2) | 2 (1-2.5) | 0.422272 | NA | 0.000098662 | NA |
| Multiple Gestationb | 71 (38.17) | 22 (37.93) | 9 (17.31) | 1 | 0.99 (0.54-1.82) | 0.0047 | 2.94 (1.35-6.25) |
| Jaundiceb | 169 (67.33) | 43 (69.36) | 23 (43.4) | 0,8796 | 1.1 (0.6-2) | 0.0016 | 2.70 (1.47-5) |
| Respiratory Distress Syndromeb | 54 (29.67) | 23 (38.98) | 8 (15.38) | 0.2005 | 1.51 (0.82-2.79) | 0.0493 | 2.33 (1.02-5.26) |
| Nationality (Foreign)b | 42 (9.31) | 9 (13.64) | 13 (24.53) | 0.2706 | 0.65 (0.3-1.41 | 0.0037 | 3.13 (1.56-6.25) |
| Characteristics | G1 group (n=451) | G2 group (n=66) | G3 group (n=53) | G1 vs G2 | G1 vs G3 | ||
|---|---|---|---|---|---|---|---|
| p | OR (95% CI) | p | OR (95% CI) | ||||
| Number of visitsa | 2 (1-4) | 2 (1-3) | 0 (0-0) | 0.000627 | NA | 0.05 | NA |
| Birth weight (gr)a | 1830 (1420-2430) | 1710 (1410-2250) | 2142.5 (1600-2660) | 0.304486 | NA | 0.037274 | NA |
| Gestational age (weeks)a | 33.3 (31.1-36) | 32.4 (30.9-34.7) | 34.4 (33-37.4) | 0.144974 | NA | 0.003007 | NA |
| Multiparitya | 1 (1-2) | 2 (1-2) | 2 (1-3) | 0.198001 | NA | 0.009142 | NA |
| Jaundiceb | 183 (68.03) | 76 (63.87) | 18 (38.3) | 0.4833 | NA | 0.0001 | 3.45 (1.82-6.67) |
| Late onset sepsis (>3 DOL)b | 37 (16.02) | 34 (28.33) | 2 (4.35) | 0.01 | 0.48 (0.28-0.82) | 0.0372 | 4.17 (0.97-16.67) |
| Necrotizing Enterocolitisb | 6 (2.64) | 9 (7.76) | 0 (0) | 0.0467 | 0.32 (0.11-0.93) | 0.5936 | NA |
| Respiratory Distress Syndromeb | 108 (44.81) | 53 (44.17) | 12 (25) | 1 | NA | 0.0155 | 2.44 (1.2-5) |
| Hours of workb | 40 (20-40) | 40 (0-40) | 17.5 (0-40) | 0.273635 | NA | 0.023946 | NA |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




