Submitted:
07 August 2024
Posted:
08 August 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Initial Analysis of Surface Roughness and Color
2.2. Simulated Toothbrushing
2.3. Analysis of Roughness and Color after Simulated Brushing
2.4. Microtensile Test
2.5. Data Analysis
3. Results
4. Discussion
5. Conclusions
- -
- All the tested resin composites exhibited an increase in Ra following the abrasion protocol. The TNF and Constic SARFs had the highest Ra values;
- -
- The resin composites demonstrated similar color stability following simulated brushing;
- -
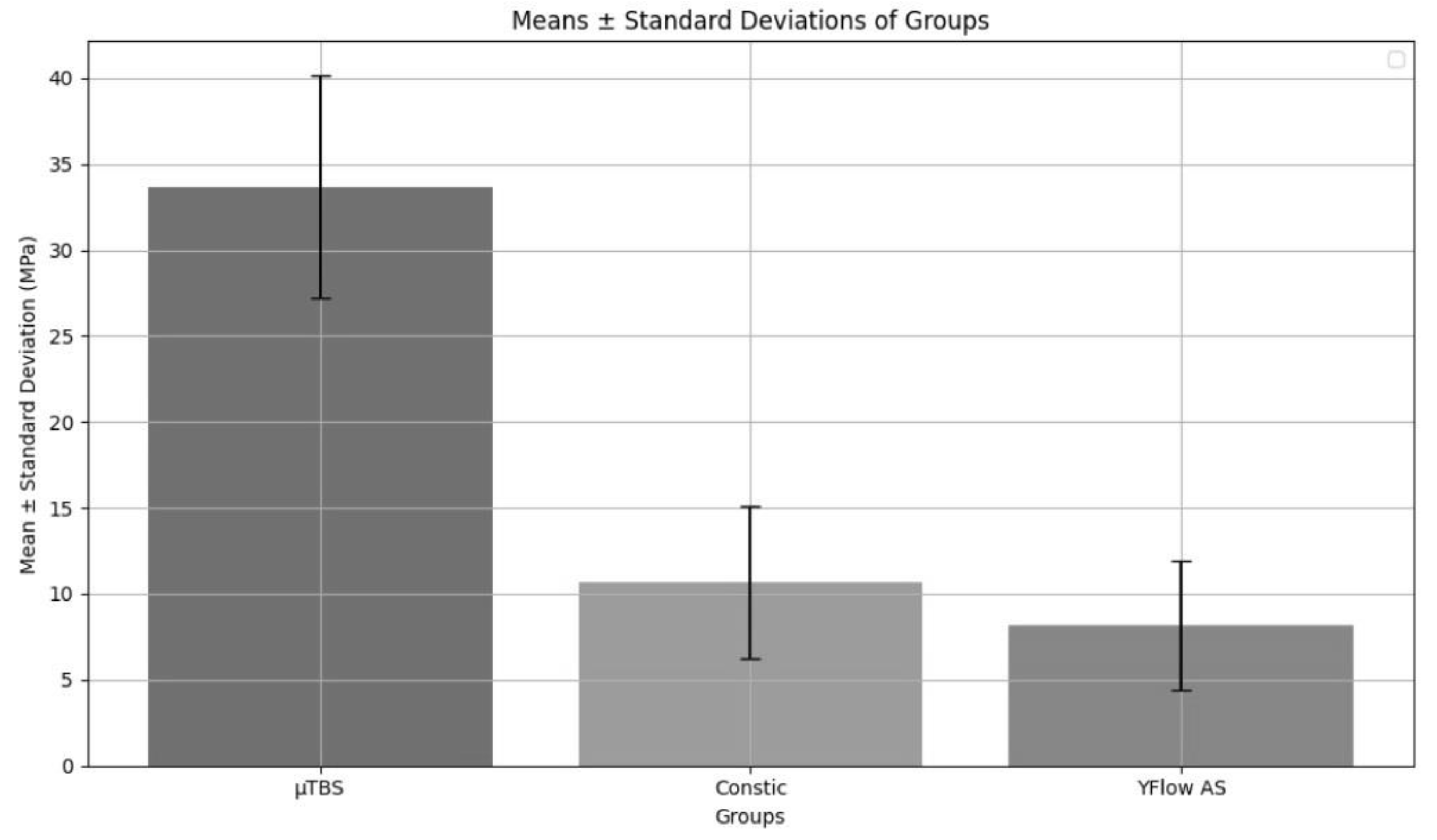
- SARFs exhibit weaker μTBS than CFR utilizing an adhesive system.
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Josic, U.; D'Alessandro, C.; Miletic, V.; Maravic, T.; Mazzitelli, C.; Jacimovic, J.; et al. Clinical longevity of direct and indirect posterior resin composite restorations: An updated systematic review and meta-analysis. Dent. Mater. 2023, 39, 1085–1094. [Google Scholar] [CrossRef]
- Pilcher, L.; Pahlke, S.; Urquhart, O.; O'Brien, K.K.; Dhar, V.; Fontana, M.; et al. Direct materials for restoring caries lesions: Systematic review and meta-analysis—a report of the American Dental Association Council on Scientific Affairs. J Am Dent Assoc (2023), 154, e1-e98. Erratum in: J. Am. Dent. Assoc 2023, 154.
- Perdigão, J.; Araujo, E.; Ramos, R.Q.; Gomes, G.; Pizzolotto, L. Adhesive dentistry: Current concepts and clinical considerations. J. Esthet. Restor. Dent. 2021, 33, 51–68. [Google Scholar] [CrossRef] [PubMed]
- Stewart, C.A.; Finer, Y. Biostable, antidegradative and antimicrobial restorative systems based on host-biomaterials and microbial interactions. Dent. Mater. 2019, 35, 36–52. [Google Scholar] [CrossRef]
- Zhou, X.; Huang, X.; Li, M.; Peng, X.; Wang, S.; Zhou, X.; et al. Development and status of resin composite as dental restorative materials. J. App Pol. Sci. 2019, 136, 48180. [Google Scholar] [CrossRef]
- Pinna, R.; Usai, P.; Filigheddu, E.; Garcia-Godoy, F.; Milia, E. The role of adhesive materials and oral biofilm in the failure of adhesive resin restorations. Am. J. Dent. 2017, 30, 285–292. [Google Scholar]
- Şişmanoğlu, S. Efficiency of self-adhering flowable resin composite and different surface treatments in composite repair using a universal adhesive. Niger. J. Clin. Pract. 2019, 22, 1675–1679. [Google Scholar] [CrossRef] [PubMed]
- Kalola, A.V.; Sreejith, S.U.; Kanodia, S.; Parmar, A.; Iyer, J.V.; Parmar, G.J. Comparative clinical evaluation of a self-adhering flowable composite with conventional flowable composite in Class I cavity: An in vivo study. J. Conserv. Dent. 2022, 25, 156–160. [Google Scholar]
- Wadhwa, S.; Nayak, U.A.; Kappadi, D.; Prajapati, D.; Sharma, R.; Pawar, A. Comparative Clinical Evaluation of Resin-based Pit and Fissure Sealant and Self-adhering Flowable Composite: An In Vivo Study. Int. J. Clin. Pediatr. Dent. 2018, 11, 430–434. [Google Scholar]
- Hayashi, K.; Ishii, R.; Takamizawa, T.; Aoki, R.; Muto, R.; Suda, S.; et al. Influence of etching mode on bonding performance of self-adhesive flowable resin composites to bovine teeth. Dent. Mater. J. 2024, 43, 338–345. [Google Scholar] [CrossRef] [PubMed]
- Jordehi, A.Y.; Shahabi, M.S.; Akbari, A. Comparison of self-adhering flowable composite microleakage with several types of bonding agent in class V cavity restoration. Dent. Res. J. 2019, 16, 257–263. [Google Scholar] [PubMed] [PubMed Central]
- Sachdeva, P.; Goswami, M.; Singh, D. Comparative evaluation of shear bond strength and nanoleakage of conventional and self-adhering flowable composites to primary teeth dentin. Contemp. Clin. Dent. 2016, 7, 326–331. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Brueckner, C.; Schneider, H.; Haak, R. Shear Bond Strength and Tooth-Composite Interaction With Self-Adhering Flowable Composites. Oper. Dent. 2017, 42, 90–100. [Google Scholar] [CrossRef] [PubMed]
- Abdelraouf, R.M.; Mohammed, M.; Abdelgawad, F. Evaluation of Shear-Bond-Strength of Dental Self-Adhering Flowable Resin-Composite versus Total-Etch One to Enamel and Dentin Surfaces: An In-Vitro Study. Open Access Maced. J. Med. Sci. 2019, 7, 2162–2166. [Google Scholar] [CrossRef]
- Sibai, N.; El Mourad, A.; Al Suhaibani, N.; Al Ahmadi, R.; Al Dosary, S. Shear bond strength of self-adhesive flowable resin composite. Inter. J. Dent. 2022, v2022, 6280624. [Google Scholar] [CrossRef]
- Sachdeva, P.; Goswami, M.; Singh, D. Comparative evaluation of shear bond strength and nanoleakage of conventional and self-adhering flowable composites to primary teeth dentin. Contemp. Clin. Dent. 2016, 7, 326–331. [Google Scholar] [PubMed]
- Elraggal, A.; Raheem, I.A.; Holiel, A.; Alhotan, A.; Alshabib, A.; Silikas, N.; et al. Bond Strength, Microleakage, Microgaps, and Marginal Adaptation of Self-adhesive Resin Composites to Tooth Substrates with and without Preconditioning with Universal Adhesives. J. Adhes. Dent, 2024, 26, 53–64. [Google Scholar]
- Monteiro, B.; Spohr, A.M. Surface Roughness of Composite Resins after Simulated Toothbrushing with Different Dentifrices. J. Int. Oral. Health. 2015, 7, 1–5. [Google Scholar] [PubMed] [PubMed Central]
- Malavasi, C.V.; Macedo, E.M.; Souza, K.D.A.C.; Rego, G.F.; Schneider, L.F.; et al. Surface Texture and Optical Properties of Self-Adhering Composite Materials after Toothbrush Abrasion. J. Contemp. Dent. Pract. 2015, 16, 775–782. [Google Scholar] [CrossRef] [PubMed]
- Lai, G.; Zhao, L.; Wang, J.; Kunzelmann, K.H. Surface properties and color stability of dental flowable composites influenced by simulated toothbrushing. Dent. Mater. J. 2018, 37, 717–724. [Google Scholar] [CrossRef]
- Jefferies, S.R. Abrasive finishing and polishing in restorative dentistry: a state-of-the-art review. Dent. Clin. North. Am. 2007, 51, 379–397. [Google Scholar] [CrossRef] [PubMed]
- Elraggal, A.; Raheem, I.A.; Holiel, A.; Alhotan, A.; Alshabib, A.; Silikas, N.; Watts, D.C.; Alharbi, N.; Afifi, R.R. Bond Strength, Microleakage, Microgaps, and Marginal Adaptation of Self-adhesive Resin Composites to Tooth Substrates with and without Preconditioning with Universal Adhesives. J. Adhes. Dent. 2024, 26, 53–64. [Google Scholar] [PubMed]
- Faggion, C.M., Jr. Guidelines for reporting pre-clinical in vitro studies on dental materials. J. Evid. Based Dent. Pract. 2012, 12, 182–189. [Google Scholar] [CrossRef]
- Delgado, A.H.; Sauro, S.; Lima, A.F.; Loguercio, A.D.; Della Bona, A.; Mazzoni, A. RoBDEMAT: A risk of bias tool and guideline to support reporting of preclinical dental materials research and assessment of systematic reviews. J. Dent. 2022, 127, 104350. [Google Scholar] [CrossRef] [PubMed]
- Arai, Y.; Kurokawa, H.; Takamizawa, T.; Tsujimoto, A.; Saegusa, M.; Yokoyama, M.; et al. Evaluation of structural coloration of experimental flowable resin composites. J. Esthet. Restor. Dent. 2021, 33, 284–293. [Google Scholar] [CrossRef] [PubMed]
- Durand, L.B.; Ruiz-López, J.; Perez, B.G.; Ionescu, A.M.; Carrillo-Pérez, F.; Ghinea, R.; et al. Color, lightness, chroma, hue, and translucency adjustment potential of resin composites using CIEDE2000 color difference formula. J. Esthet. Restor. Dent. 2021, 33, 836–843. [Google Scholar] [CrossRef]
- Sharma, G.; Wu, W.; Dalal, E.N. The CIEDE2000 color-difference formula: Implementation notes, supplementary test data, and mathematical observations. Color. Res. App. 2005, 30, 21–30. [Google Scholar] [CrossRef]
- Gómez-Polo, C.; Portillo Muñoz, M.; Lorenzo Luengo, M.C.; Vicente, P.; Galindo, P.; Martín Casado, A.M. Comparison of the CIELab and CIEDE2000 color difference formulas. J. Prosthet. Dent. 2016, 115, 65–70. [Google Scholar] [CrossRef]
- Turssi, C.P.; Binsaleh, F.; Lippert, F.; Bottino, M.C.; Eckert, G.J.; Moser, E.A.S.; et al. Interplay between toothbrush stiffness and dentifrice abrasivity on the development of noncarious cervical lesions. Clin. Oral. Investig. 2019, 23, 3551–3556. [Google Scholar] [CrossRef]
- Orellana, N.; Ramírez, R.; Roig, M.; Giner, L.; Mercade, M.; Durán, F.; et al. Comparative study of the microtensile bond strength of three different total etch adhesives with different solvents to wet and dry dentin (in vitro test). Acta Odontol. Latinoam. 2009, 22, 47–56. [Google Scholar]
- Yuan, H.; Li, M.; Guo, B.; Gao, Y.; Liu, H.; Li, J. Evaluation of Microtensile Bond Strength and Microleakage of a Self-adhering Flowable Composite. J. Adhes. Dent. 2015, 17, 535–543. [Google Scholar] [CrossRef] [PubMed]
- Bolme, J.; Gjerdet, N.R.; Laegreid, T. Effect of saliva contamination on the bond strength of single-step and three-step adhesive systems. Eur. J. Oral. Sci. 2022, 130, e12838. [Google Scholar] [CrossRef]
- Guler, S.; Unal, M. The Evaluation of Color and Surface Roughness Changes in Resin based Restorative Materials with Different Contents After Waiting in Various Liquids: An SEM and AFM study. Microsc. Res. Tech. 2018, 81, 1422–1433. [Google Scholar] [CrossRef]
- AlHumaid, J.; Al Harbi, F.A.; ElEmbaby, A.E. Performance of Self-adhering Flowable Composite in Class V Restorations: 18 Months Clinical Study. J. Contemp. Dent. Pract. 2018, 19, 785–791. [Google Scholar] [PubMed]
- Costa, R.T.F.; Pellizzer, E.P.; Vasconcelos, B.C.D.E.; Gomes, J.M.L.; Lemos, C.A.A.; de Moraes, S.L.D. Surface roughness of acrylic resins used for denture base after chemical disinfection: A systematic review and meta-analysis. Gerodontology. 2021, 38, 242–251. [Google Scholar] [CrossRef] [PubMed]
- Sanal, F.A.; Kilinc, H. Evaluating Ceramic Repair Materials in Terms of Bond Strength and Color Stability. Int J Prosthodont. 2020, 33, 536–545. [Google Scholar] [CrossRef] [PubMed]
- David, C.; Cuevas-Suárez, C.E.; de Cardoso, G.C.; Isolan, C.P.; de Moraes, R.R.; da Rosa, W.; et al. Characterization of Contemporary Conventional, Bulk-fill, and Self-adhesive Resin Composite Materials. Oper. Dent. 2022, 47, 392–402. [Google Scholar] [CrossRef] [PubMed]
- Peterson, J.; Rizk, M.; Hoch, M.; Wiegand, A. Bonding performance of self-adhesive flowable composites to enamel, dentin and a nanohybrid composite. Odontology 2018, 106, 171–180. [Google Scholar] [CrossRef]
- Makishi, P.; Pacheco, R.R.; Sadr, A.; Shimada, Y.; Sumi, Y.; Tagami, J.; et al. Assessment of Self-Adhesive Resin Composites: Nondestructive Imaging of Resin-Dentin Interfacial Adaptation and Shear Bond Strength. Microsc. Microanal. 2015, 21, 1523–1529. [Google Scholar] [CrossRef]
- Cengiz, T.; Ünal, M. Comparison of microtensile bond strength and resin-dentin interfaces of two self-adhesive flowable composite resins by using different universal adhesives: Scanning electron microscope study. Microsc. Res. Tech. 2019, 82, 1032–1040. [Google Scholar] [CrossRef]
- Mine, A.; De Munck, J.; Van Ende, A.; Poitevin, A.; Matsumoto, M.; Yoshida, Y.; et al. Limited interaction of a self-adhesive flowable composite with dentin/enamel characterized by TEM. Dent. Mater. 2017, 33, 209–217. [Google Scholar] [CrossRef]
- Temel, U.B.; Van Ende, A.; Van Meerbeek, B.; Ermis, R.B. Bond strength and cement-tooth interfacial characterization of self-adhesive composite cements. Am. J. Dent. 2017, 30, 205–211. [Google Scholar] [PubMed]
- David, C.; Cardoso de Cardoso, G.; Isolan, C.P.; Piva, E.; Moraes, R.R.; Cuevas-Suarez, C.E. Bond strength of self-adhesive flowable composite resins to dental tissues: A systematic review and meta-analysis of in vitro studies. J. Prosthet. Dent. 2022, 128, 876–885. [Google Scholar] [CrossRef] [PubMed]

| Product | Manufacturer | Lot No. | Chemical composition | Technique |
|---|---|---|---|---|
| Tetric N Flow (TNF) | Ivoclar Vivadent, Barueri, SP, Brazil | Z020DP Z019WR |
Dimethacrylates (including TEGDMA), barium oxide, ytterbium trifluoride, highly dispersed silica and mixed oxides, pigments, catalysts, and stabilizers. | Apply the adhesive to the enamel and dentin, then insert the resin into the cavity using the incremental technique. Use increments between 1.5 and 2 mm thick, polymerizing each one for 20 seconds. The halogen light should have a minimum intensity of 500 mW/cm² and be kept as close as possible to the restoration, ensuring that the entire surface is reached. |
| Constic | DMG, Hambug, Germany) | 232801 | Barium glass in a matrix of dental resins based on Bis-GMA. EBADMA, UDMA, HEMA, TEGDMA, HDMA, MDP. Pigments, additives, and catalyst. Filler volume: 66% by weight = 43% by volume. The range of variation of inorganic filler particles is from 0.02 to 2.3 µm. | After preparation, clean the tooth with water spray and then dry it with oil-free air spray. A superficially moist layer should remain. Apply the material to the cavity surface by pressing the syringe and rub for 25 seconds to form a thin layer (0.5 mm). Remove any excess if necessary and light-cure for 20 seconds. Then, apply increments of up to 2 mm and light-cure each one for 20 seconds. |
| Yflow SA | Yller Biomateriais, Pelotas, RS, Brazil | 00009968 | Methacrylate monomers, acid monomers, inorganic fillers, pigments, initiators, and stabilizers. | After dental cleaning, attach the applicator tip to the syringe and dispense the product directly into the preparation. Place the resin in increments of up to 2 mm and light-cure for 40 seconds. |
| Colgate Cavity Protection |
Colgate-Palmolive Industry and Commerce Ltd., New York, USA |
1500 ppm of Fluoride, Calcium Carbonate, Sodium Lauryl Sulfate, Sodium Saccharin, Tetrasodium Pyrophosphate, Sodium Silicate, Polyethylene Glycol, Sorbitol, Carboxymethyl Cellulose, Methylparaben, Propylparaben, Aromatic Composition, and Water. Contains Sodium Monofluorophosphate - MFP® |
| Groups | Before | After | p |
|---|---|---|---|
| TNF | 0,101 ± 0,019 | 0,316 ± 0,070 | 0,005* |
| Constic | 0,111 ± 0,019 | 0,702 ± 0,282 | 0,005* |
|
Yflow AS p |
0,131 ± 0,053 0.051 |
0,184 ± 0,065 <0,001* |
0,012* |
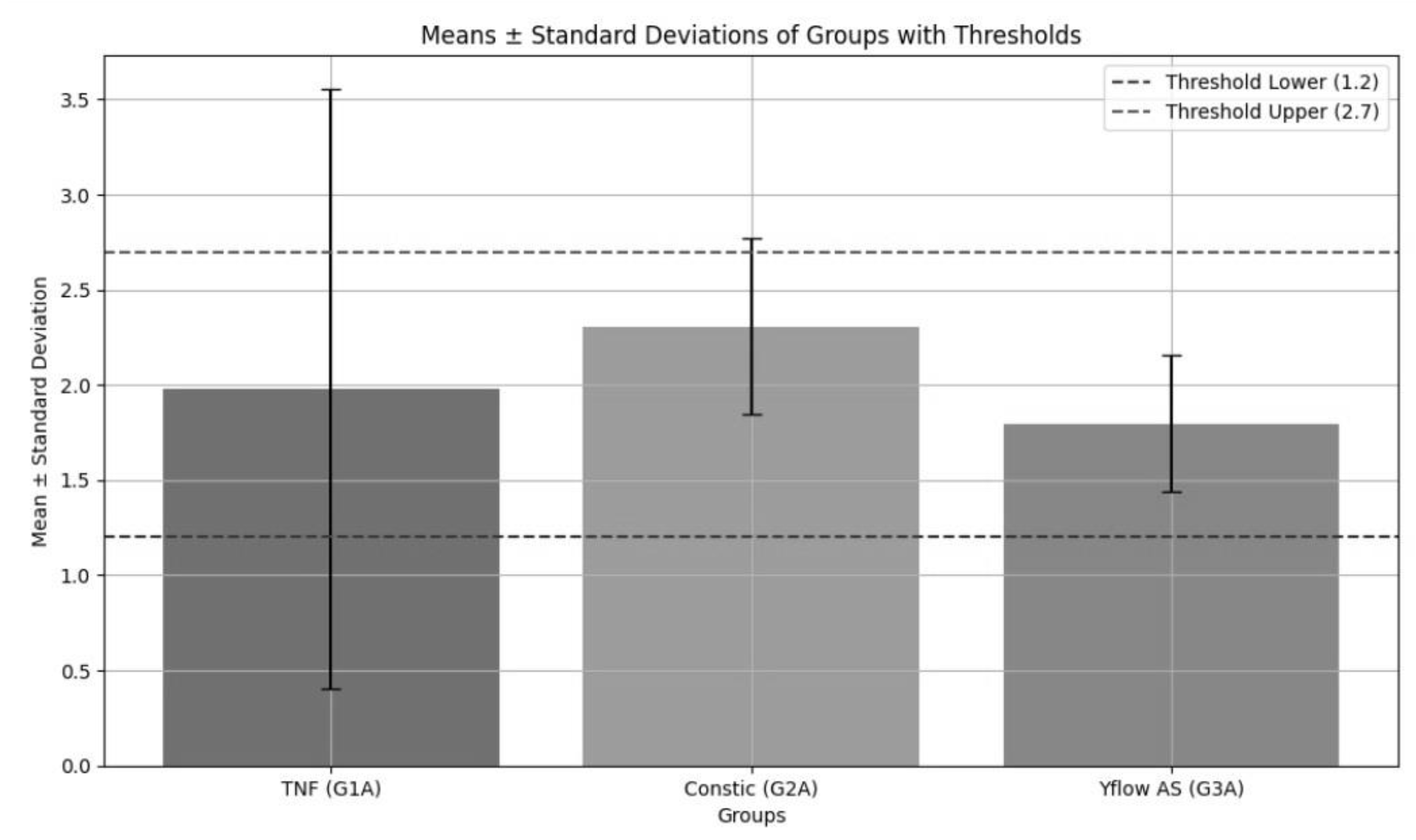
| Groups | Mean ± dp |
|---|---|
| TNF | 1,977 ± 1,575 |
| Constic | 2,307 ± 0,464 |
| Yflow AS | 1,798 ± 0,356 |
| p | 0.080 |
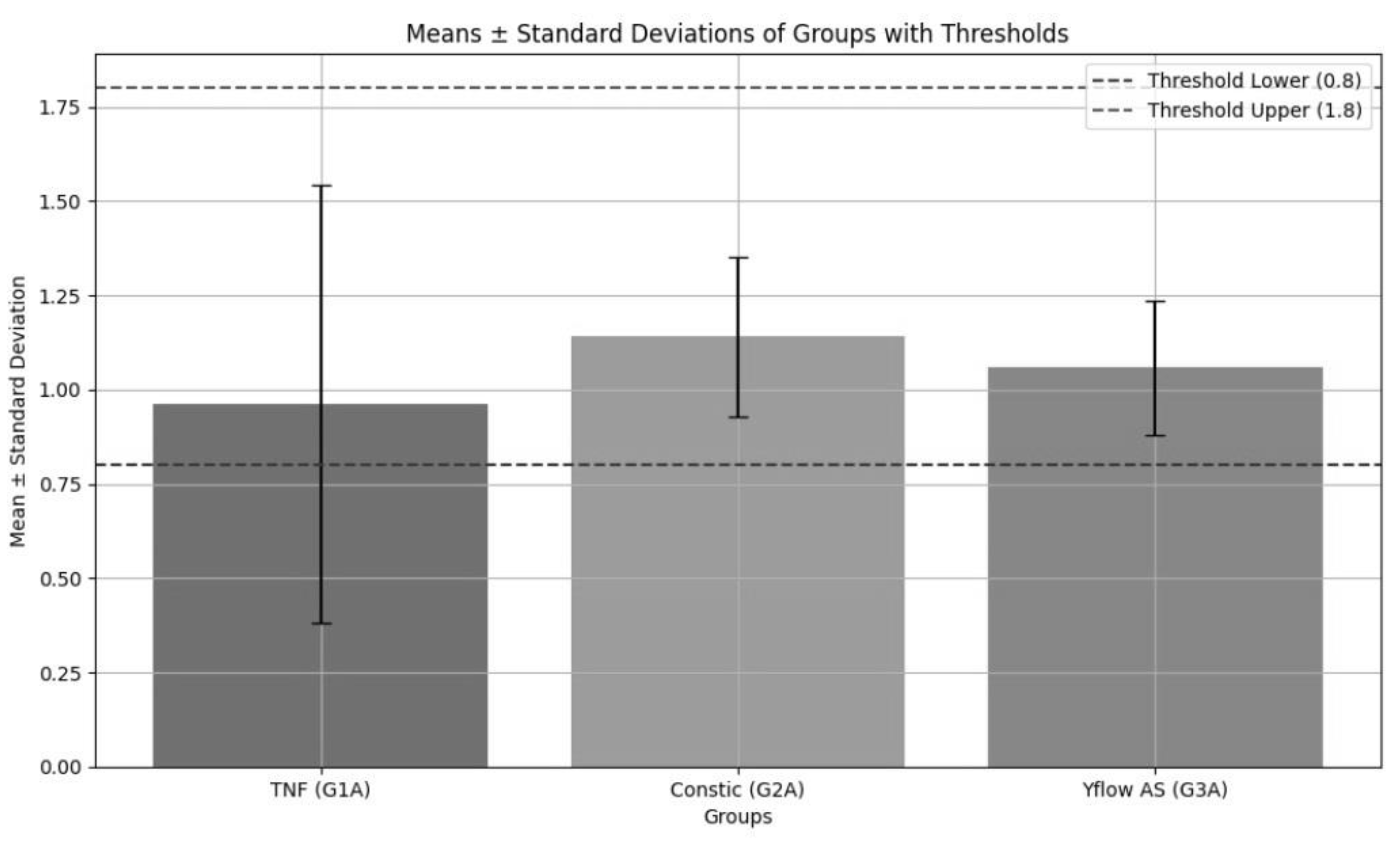
| Groups | Mean ± dp |
|---|---|
| TNF | 0,962 ± 0,580 |
| Constic | 1,140 ± 0,213 |
| Yflow AS | 1,058 ± 0,177 |
| p | 0.144 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




