Submitted:
02 August 2024
Posted:
06 August 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bahceci, S.; Kuyum Töz, P.; Celebi Celik, F.; Can, D. A Different Starting Line for Allergic March: Food Protein-Induced Allergic Proctocolitis. Allergol. Immunopathol. (Madr.) 2023, 51, 40–45. [Google Scholar] [CrossRef] [PubMed]
- Meyer, R.; Chebar Lozinsky, A.; Fleischer, D.M.; Vieira, M.C.; Du Toit, G.; Vandenplas, Y.; Dupont, C.; Knibb, R.; Uysal, P.; Cavkaytar, O.; et al. Diagnosis and Management of Non-IgE Gastrointestinal Allergies in Breastfed Infants—An EAACI Position Paper. Allergy 2020, 75, 14–32. [Google Scholar] [CrossRef] [PubMed]
- Burris, A.D.; Burris, J.; Järvinen, K.M. Cow’s Milk Protein Allergy in Term and Preterm Infants: Clinical Manifestations, Immunologic Pathophysiology, and Management Strategies. NeoReviews 2020, 21, e795–e808. [Google Scholar] [CrossRef]
- Ohtsuka, Y.; Shimizu, T.; Shoji, H.; Kudo, T.; Fujii, T.; Wada, M.; Sato, H.; Aoyagi, Y.; Haruna, H.; Nagata, S.; et al. Neonatal Transient Eosinophilic Colitis Causes Lower Gastrointestinal Bleeding in Early Infancy. J. Pediatr. Gastroenterol. Nutr. 2007, 44, 501–505. [Google Scholar] [CrossRef] [PubMed]
- Jang, H.-J.; Kim, A.S.; Hwang, J.-B. The Etiology of Small and Fresh Rectal Bleeding in Not-Sick Neonates: Should We Initially Suspect Food Protein-Induced Proctocolitis? Eur. J. Pediatr. 2012, 171, 1845–1849. [Google Scholar] [CrossRef] [PubMed]
- Miceli Sopo, S.; Monaco, S.; Bersani, G.; Romano, A.; Fantacci, C. Proposal for Management of the Infant with Suspected Food Protein-induced Allergic Proctocolitis. Pediatr. Allergy Immunol. 2018, 29, 215–218. [Google Scholar] [CrossRef] [PubMed]
- Koksal, B.T.; Barıs, Z.; Ozcay, F.; Yilmaz Ozbek, O. Single and Multiple Food Allergies in Infants with Proctocolitis. Allergol. Immunopathol. (Madr.) 2018, 46, 3–8. [Google Scholar] [CrossRef]
- Senocak, N.; Ertugrul, A.; Ozmen, S.; Bostanci, I. Clinical Features and Clinical Course of Food Protein—Induced Allergic Proctocolitis: 10-Year Experience of a Tertiary Medical Center. J. Allergy Clin. Immunol. Pract. 2022, 10, 1608–1613. [Google Scholar] [CrossRef] [PubMed]
- Morita, Y.; Iwakura, H.; Ohtsuka, H.; Kohno, Y.; Shimojo, N. Milk Allergy in the Neonatal Intensive Care Unit: Comparison between Premature and Full-Term Neonates. Asia Pac. Allergy 2013, 3, 35–41. [Google Scholar] [CrossRef]
- Florquin, M.; Eerdekens, A. What Is Known About Cow’s Milk Protein Allergy in Preterm Infants? Breastfeed. Med. 2023, 18, 767–778. [Google Scholar] [CrossRef]
- D’Auria, E.; Cocchi, I.; Monti, G.; Sartorio, M.U.A.; Daniele, I.; Lista, G.; Zuccotti, G.V. Food Protein–Induced Enterocolitis Syndrome in Preterm Newborns. Pediatr. Allergy Immunol. 2022, 33, e13676. [Google Scholar] [CrossRef] [PubMed]
- Powell, G.K. Enterocolitis in Low-Birth-Weight Infants Associated with Milk and Soy Protein Intolerance. J. Pediatr. 1976, 88, 840–844. [Google Scholar] [CrossRef] [PubMed]
- Coviello, C.; Rodriquez, D.C.; Cecchi, S.; Tataranno, M.L.; Farmeschi, L.; Mori, A.; Buonocore, G. Different Clinical Manifestation of Cow’s Milk Allergy in Two Preterm Twins Newborns. J. Matern. Fetal Neonatal Med. 2012, 25, 132–133. [Google Scholar] [CrossRef] [PubMed]
- Cai, N.; Liao, W.; Chen, Z.; Tao, M.; Chen, S. The Mean Platelet Volume Combined with Procalcitonin as an Early Accessible Marker Helps to Predict the Severity of Necrotizing Enterocolitis in Preterm Infants. Int. J. Gen. Med. 2022, 15, 3789–3795. [Google Scholar] [CrossRef] [PubMed]
- Mukhopadhyay, D.; Weaver, L.; Tobin, R.; Henderson, S.; Beeram, M.; Newell-Rogers, M.K.; Perger, L. Intrauterine Growth Restriction and Prematurity Influence Regulatory T Cell Development in Newborns. J. Pediatr. Surg. 2014, 49, 727–732. [Google Scholar] [CrossRef] [PubMed]
- Lahl, K.; Loddenkemper, C.; Drouin, C.; Freyer, J.; Arnason, J.; Eberl, G.; Hamann, A.; Wagner, H.; Huehn, J.; Sparwasser, T. Selective Depletion of Foxp3+ Regulatory T Cells Induces a Scurfy-like Disease. J. Exp. Med. 2007, 204, 57–63. [Google Scholar] [CrossRef] [PubMed]
- Dingle, B.M.; Liu, Y.; Fatheree, N.Y.; Min, J.; Rhoads, J.M.; Tran, D.Q. FoxP3+ Regulatory T Cells Attenuate Experimental Necrotizing Enterocolitis. PLoS ONE 2013, 8, e82963. [Google Scholar] [CrossRef]
- Pacella, I.; Di Chiara, M.; Prota, R.; De Luca, C.; Cardillo, A.; Potenza, E.; Grimaldos, A.P.; Pinna, V.; Piconese, S.; Terrin, G. Reduction in Regulatory T Cells in Preterm Newborns Is Associated with Necrotizing Enterocolitis. Pediatr. Res. 2023, 94, 1789–1796. [Google Scholar] [CrossRef] [PubMed]
- Steinborn, A.; Engst, M.; Haensch, G.M.; Mahnke, K.; Schmitt, E.; Meuer, S.; Sohn, C. Small for Gestational Age (SGA) Neonates Show Reduced Suppressive Activity of Their Regulatory T Cells. Clin. Immunol. 2010, 134, 188–197. [Google Scholar] [CrossRef]
- Salvatore, S.; Folegatti, A.; Ferrigno, C.; Pensabene, L.; Agosti, M.; D’Auria, E. To Diet or Not to Diet This Is the Question in Food-Protein-Induced Allergic Proctocolitis (FPIAP)—A Comprehensive Review of Current Recommendations. Nutrients 2024, 16, 589. [Google Scholar] [CrossRef]
- Cordova, J.; Sriram, S.; Patton, T.; Jericho, H.; Gokhale, R.; Weinstein, D.; Sentongo, T. Manifestations of Cow’s-Milk Protein Intolerance in Preterm Infants. J. Pediatr. Gastroenterol. Nutr. 2016, 62, 140–144. [Google Scholar] [CrossRef] [PubMed]
- Chuang, S. -L.; Hayes, P.J.; Ogundipe, E.; Haddad, M.; MacDonald, T.T.; Fell, J.M. Cow’s Milk Protein-specific T-helper Type I/II Cytokine Responses in Infants with Necrotizing Enterocolitis. Pediatr. Allergy Immunol. 2009, 20, 45–52. [Google Scholar] [CrossRef] [PubMed]
- Chinnappan, A.; Sharma, A.; Agarwal, R.; Thukral, A.; Deorari, A.; Sankar, M.J. Fortification of Breast Milk With Preterm Formula Powder vs Human Milk Fortifier in Preterm Neonates: A Randomized Noninferiority Trial. JAMA Pediatr. 2021, 175, 790. [Google Scholar] [CrossRef] [PubMed]
| FPIAP (16) | Transient haematochezia (9) | NEC (18) | |
|---|---|---|---|
| Mean gestational age | 34.38 ±3.19 weeks | 35.1 ± 4.47 | 31 ± 4 |
| Twin pregnancies | 8 (50%) (4/8 BC, 4/8 MC) |
6 | 12 (66%) |
| Birth weight | 1680 g | 1539 g | 1606 |
| CesareanSection | 13 (81,3%) | 7 (77%) | 17 (94%) |
| Days of onset | 16 | 27 | 11,1 |
| SGA/IUGR | 6 (37,5%) | 2 (22%) | 3 (16%) |
| FEF beforehematochezia | 7 (43,8%) | 4 (44%) | 6 (33%) |
| Familiarity | 5 (31,2%) | 1 (11%) | 0 |
| Protein fortification milk | 4 (25%) | 1 (11%) | 2 (1,1%) |
| Hemoglobin | 13,8 | 14,1 | 13,6 |
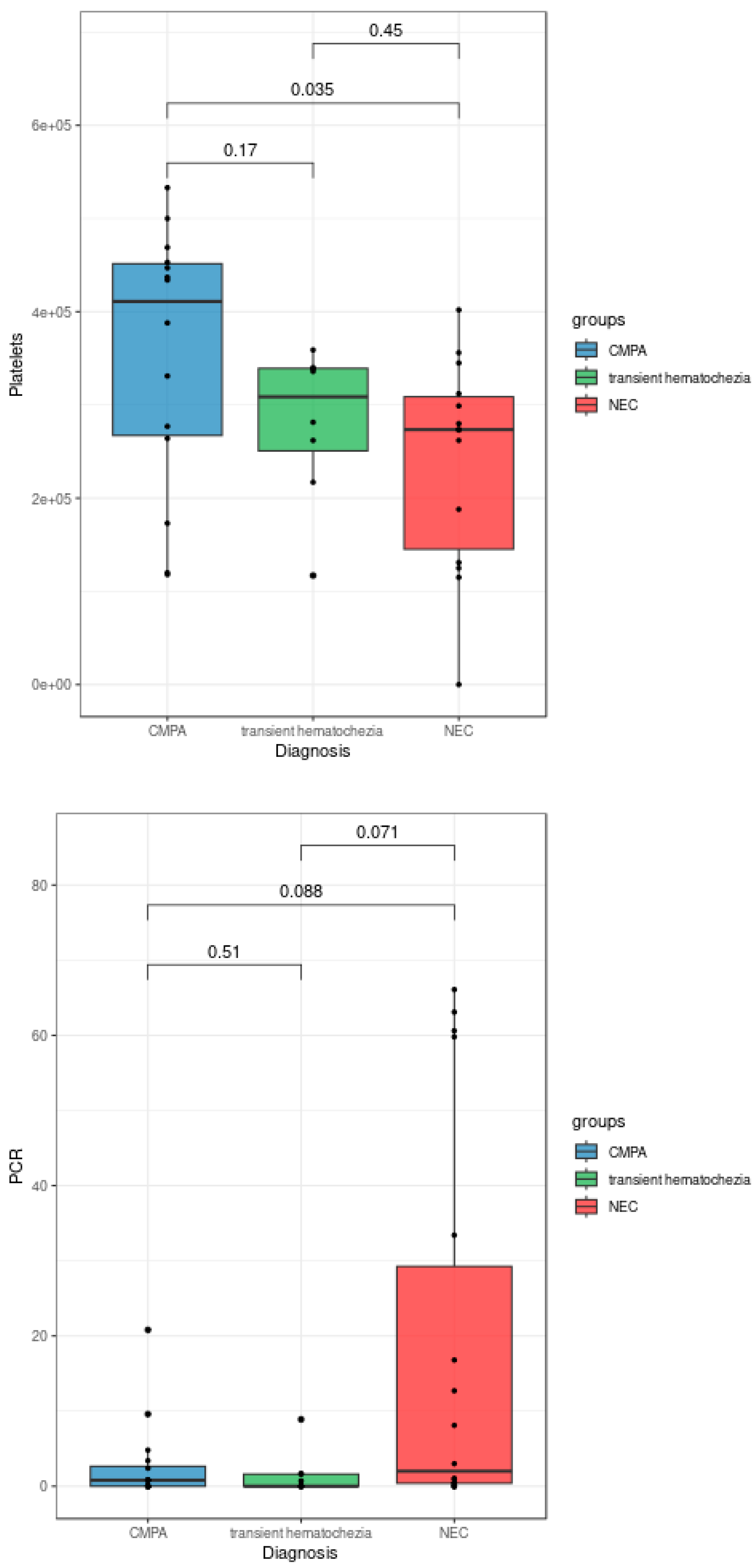
| Platelets | 353.142 | 281.428 | 240.142 |
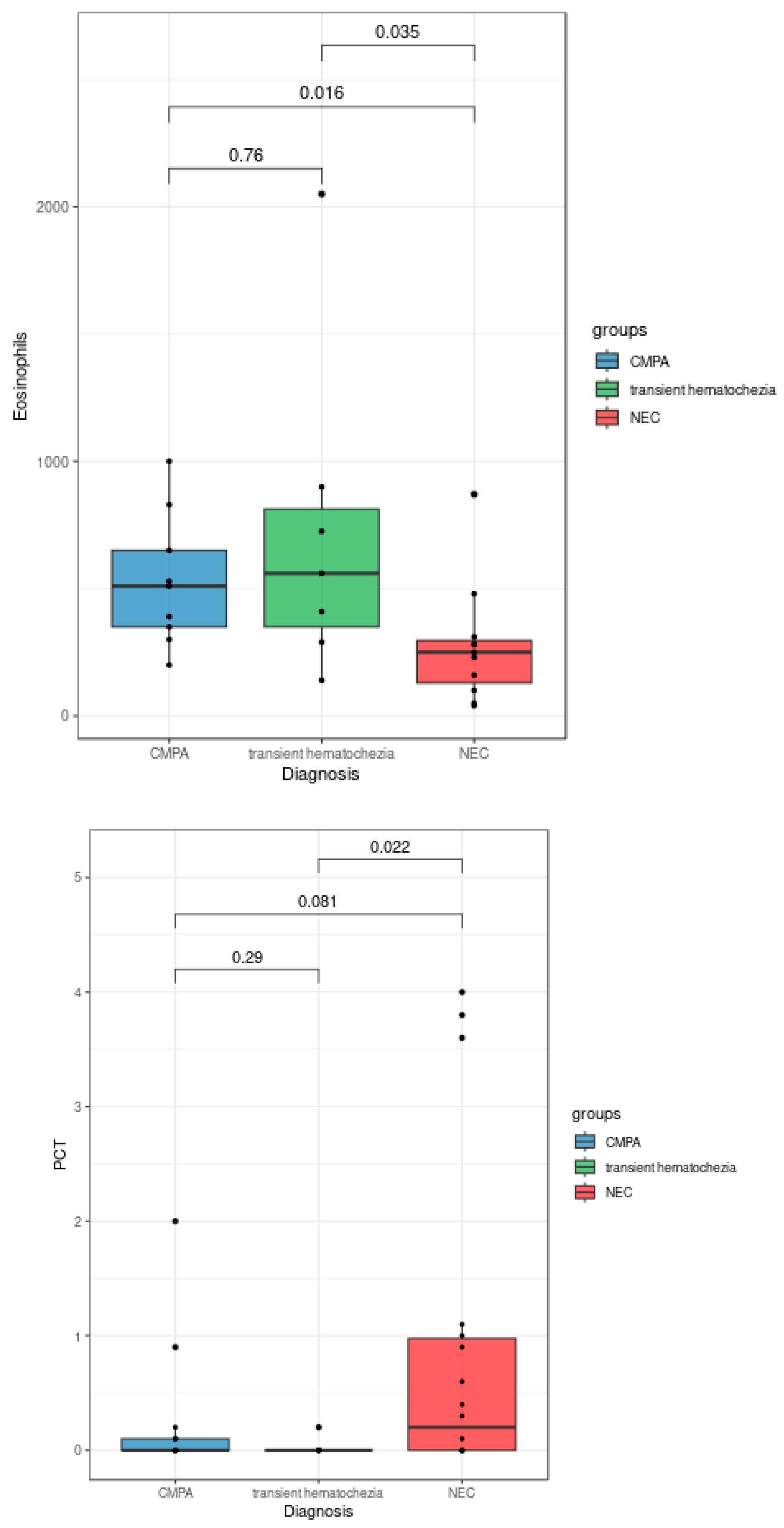
| CRP | 3,8 | 1,6 | 27,2 |
| White blood cells | 9982 | 11.192 | 11962 |
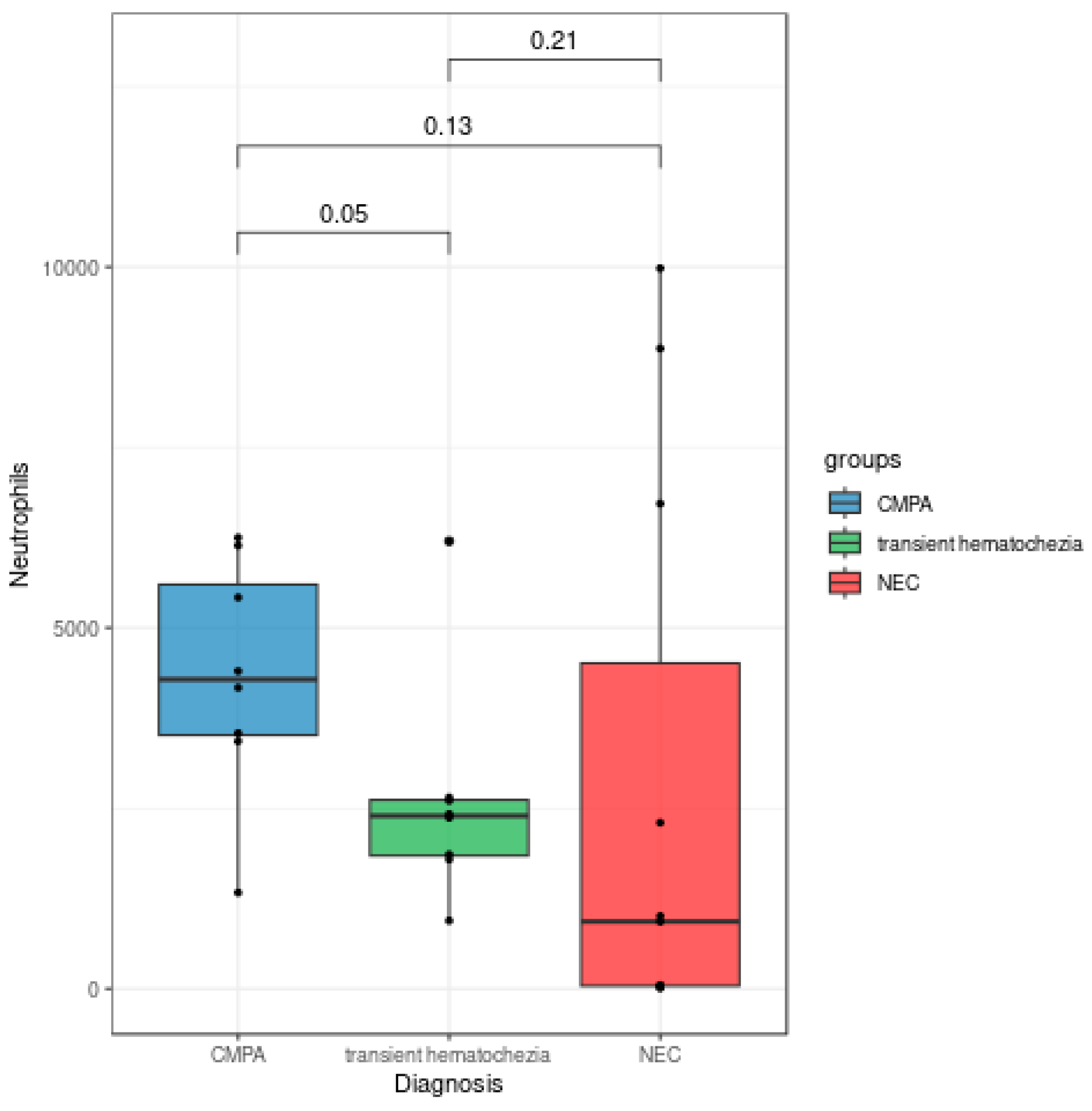
| Neutrophils | 4335 | 2604 | 2724 |
| Eosinophils | 405 | 725 | 277 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




