Submitted:
22 July 2024
Posted:
23 July 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Blood Sample Collection
2.3. Statistical Analysis
3. Results
3.1. Comparison of Uncomplicated and Complicated Patient Groups
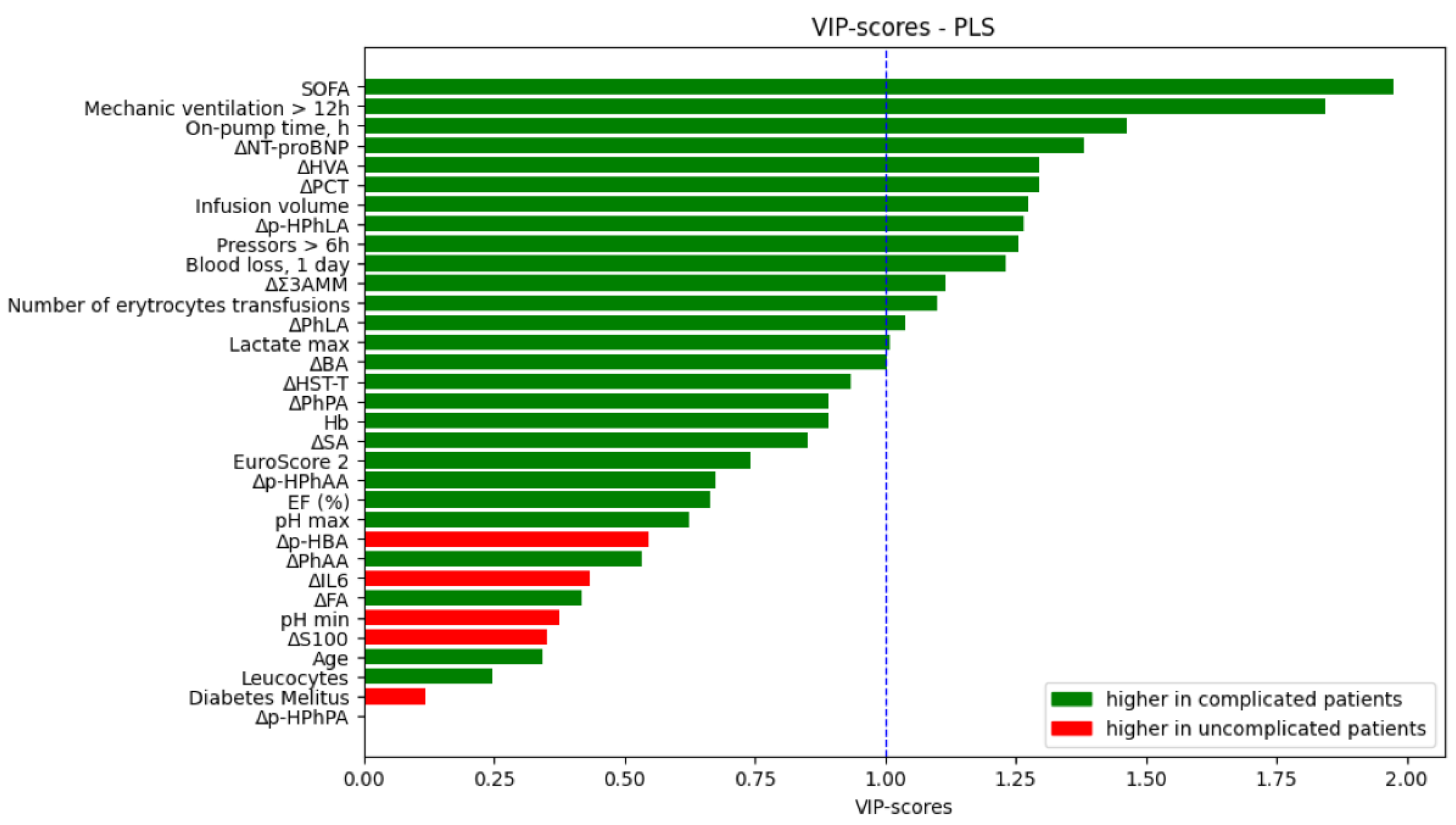
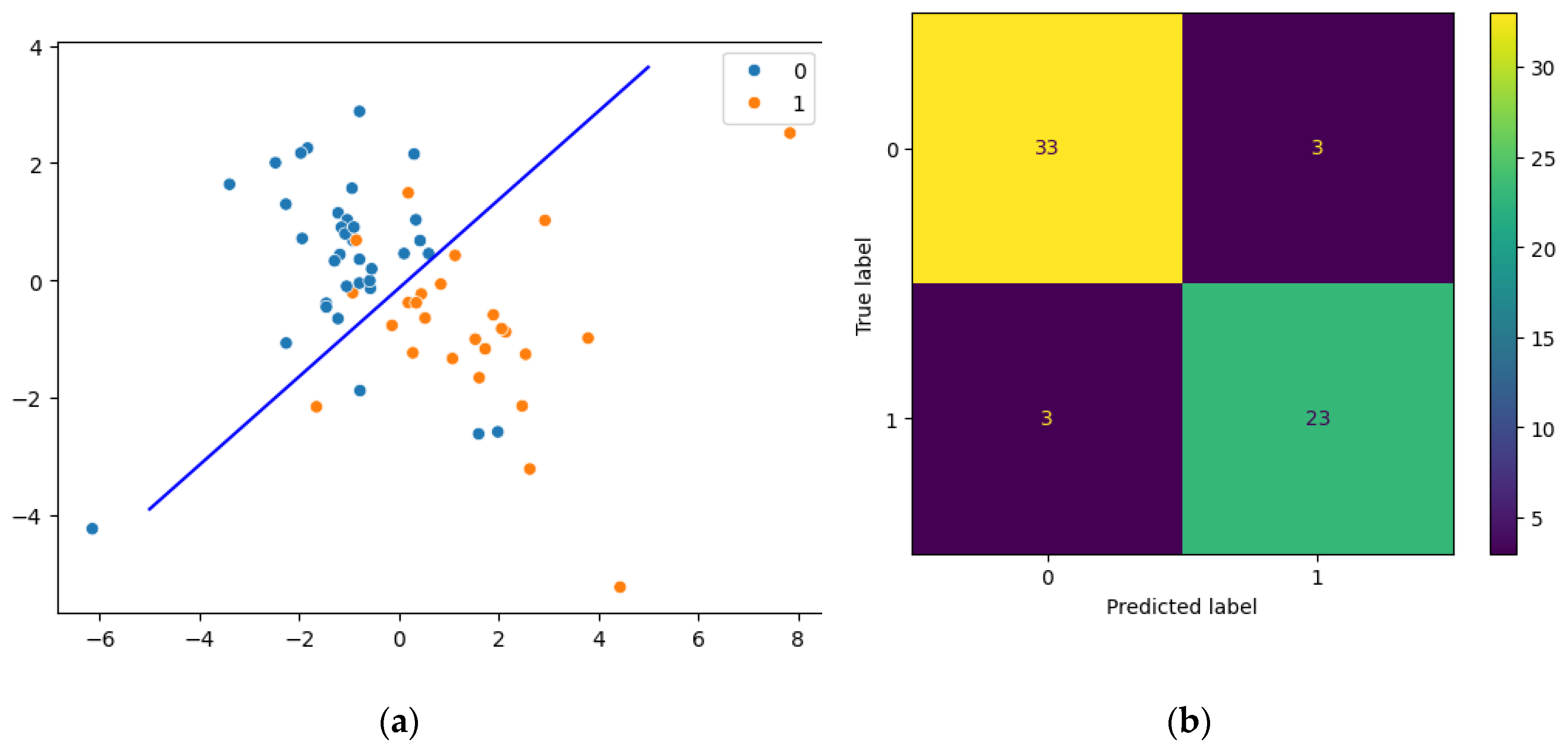
3.2. Models for the Prognosis of the Postoperative Complications
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Crawford, T.C.; Magruder, J.T.; Grimm, J.C.; Suarez-Pierre, A.; Sciortino, C.M.; Mandal, K.; Zehr, K.J.; Conte, J. V.; Higgins, R.S.; Cameron, D.E.; et al. Complications After Cardiac Operations: All Are Not Created Equal. Ann. Thorac. Surg. 2017, 103, 32–40. [Google Scholar] [CrossRef] [PubMed]
- Montrief, T.; Koyfman, A.; Long, B. Coronary artery bypass graft surgery complications: A review for emergency clinicians. Am. J. Emerg. Med. 2018, 36, 2289–2297. [Google Scholar] [CrossRef] [PubMed]
- Lazzeri, C.; Valente, S.; Chiostri, M.; Gensini, G.F. Clinical significance of Lactate in acute cardiac patients. World J. Cardiol. 2015, 7, 483. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Li, H.-Y.; Hu, X.-M.; Zhang, Y.; Zhang, S.-Y. Current understanding of gut microbiota alterations and related therapeutic intervention strategies in heart failure. Chin. Med. J. (Engl). 2019, 132, 1843–1855. [Google Scholar] [CrossRef]
- Kavsak, P.A.; Belley-Cote, E.P.; Whitlock, R.P.; Lamy, A. Cardiac troponin testing in cardiac surgery. Expert Rev. Cardiovasc. Ther. 2023, 21, 729–731. [Google Scholar] [CrossRef] [PubMed]
- Gowda, G.N.; Zhang, S.; Gu, H.; Asiago, V.; Shanaiah, N.; Raftery, D. Metabolomics-based methods for early disease diagnostics. Expert Rev. Mol. Diagn. 2008, 8, 617–633. [Google Scholar] [CrossRef] [PubMed]
- Cui, H.; Shu, S.; Li, Y.; Yan, X.; Chen, X.; Chen, Z.; Hu, Y.; Chang, Y.; Hu, Z.; Wang, X.; et al. Plasma Metabolites-Based Prediction in Cardiac Surgery-Associated Acute Kidney Injury. J. Am. Heart Assoc. 2021, 10. [Google Scholar] [CrossRef] [PubMed]
- Tripp, B.A.; Dillon, S.T.; Yuan, M.; Asara, J.M.; Vasunilashorn, S.M.; Fong, T.G.; Metzger, E.D.; Inouye, S.K.; Xie, Z.; Ngo, L.H.; et al. Targeted metabolomics analysis of postoperative delirium. Sci. Rep. 2021, 11, 1521. [Google Scholar] [CrossRef] [PubMed]
- Gregory, A.J.; Noss, C.D.; Chun, R.; Gysel, M.; Prusinkiewicz, C.; Webb, N.; Raymond, M.; Cogan, J.; Rousseau-Saine, N.; Lam, W.; et al. Perioperative Optimization of the Cardiac Surgical Patient. Can. J. Cardiol. 2023, 39, 497–514. [Google Scholar] [CrossRef]
- Gong, Y.; Li, T.; Liu, Q.; Wang, X.; Deng, Z.; Cheng, L.; Yu, B.; Liu, H. Analysis of differential metabolites in serum metabolomics of patients with aortic dissection. BMC Cardiovasc. Disord. 2024, 24, 1–10. [Google Scholar] [CrossRef]
- Dodd, D.; Spitzer, M.H.; Van Treuren, W.; Merrill, B.D.; Hryckowian, A.J.; Higginbottom, S.K.; Le, A.; Cowan, T.M.; Nolan, G.P.; Fischbach, M.A.; et al. A gut bacterial pathway metabolizes aromatic amino acids into nine circulating metabolites. Nature 2017, 551, 648–652. [Google Scholar] [CrossRef]
- Lu, X.; Liu, J.; Zhou, B.; Wang, S.; Liu, Z.; Mei, F.; Luo, J.; Cui, Y. Microbial metabolites and heart failure: Friends or enemies? Front. Microbiol. 2022, 13. [Google Scholar] [CrossRef]
- Chernevskaya, E.A.; Getsina, M.L.; Cherpakov, R.A.; Sorokina, E.A.; Shabanov, A.K.; Moroz, V. V.; Beloborodova, N. V. Sepsis-Associated Metabolites and Their Biotransformation by Intestinal Microbiota. Gen. Reanimatol. 2023, 19, 4–12. [Google Scholar] [CrossRef]
- Beloborodova, N.; Pautova, A.; Grekova, M.; Yadgarov, M.; Grin, O.; Eremenko, A.; Babaev, M. Microbiota Metabolism Failure as a Risk Factor for Postoperative Complications after Aortic Prosthetics. Biomedicines 2023, 11, 1335. [Google Scholar] [CrossRef]
- Chernevskaya, E.; Zuev, E.; Odintsova, V.; Meglei, A.; Beloborodova, N. Gut Microbiota as Early Predictor of Infectious Complications before Cardiac Surgery: A Prospective Pilot Study. J. Pers. Med. 2021, 11, 1113. [Google Scholar] [CrossRef]
- Pautova, A.K.; Burnakova, N.A.; Beloborodova, N. V.; Revelsky, A.I. Simultaneous Determination of Aromatic, Short-Chain Fatty and Dicarboxylic Acids in Blood Serum and Cerebrospinal Fluid by Gas Chromatography–Mass Spectrometry. J. Anal. Chem. 2023, 78, 1942–1954. [Google Scholar] [CrossRef]
- Wiredu, K.; O’Connor, S.; Naseem, H.; Brauer, B.L.; Kettenbach, A.N.; Frost, H.R.; Shaefi, S.; Gerber, S.A. Intraoperative plasma proteomic changes in cardiac surgery: In search of biomarkers of post-operative delirium. PROTEOMICS – Clin. Appl. 2023, 17, e2200066. [Google Scholar] [CrossRef]
- Ruslyakova, I.A.; Belyakov, K.S.; Abdulrazakov, A.A.; Marinin, V.A. Predictors of Complications Related to Cardiac Ablation for Atrial Arrhythmias. Gen. Reanimatol. 2024, 20, 4–14. [Google Scholar] [CrossRef]
- Gonenc, A.; Hacışevki, A.; Griffiths, H.R.; Torun, M.; Bakkaloglu, B.; Simsek, B. Free radical reaction products and antioxidant capacity in beating heart coronary artery surgery compared to conventional bypass. Biochem. 2011, 76, 677–685. [Google Scholar] [CrossRef]
- Li, Q.; Lv, H.; Chen, Y.; Shen, J.; Shi, J.; Zhou, C. Development and validation of a machine learning predictive model for perioperative myocardial injury in cardiac surgery with cardiopulmonary bypass. J. Cardiothorac. Surg. 2024, 19, 384. [Google Scholar] [CrossRef]
- Turagam, M.K.; Mirza, M.; Werner, P.H.; Sra, J.; Kress, D.C.; Tajik, A.J.; Jahangir, A. Circulating Biomarkers Predictive of Postoperative Atrial Fibrillation. Cardiol. Rev. 2016, 24, 76–87. [Google Scholar] [CrossRef] [PubMed]
- Forner, J.; Schupp, T.; Weidner, K.; Rusnak, J.; Jawhar, S.; Dulatahu, F.; Brück, L.M.; Behnes, M.; Hoffmann, U.; Bertsch, T.; et al. Cardiac Troponin I Reveals Diagnostic and Prognostic Superiority to Aminoterminal Pro-B-Type Natriuretic Peptide in Sepsis and Septic Shock. J. Clin. Med. 2022, 11, 6592. [Google Scholar] [CrossRef]
- Bavare, A.; Rissmiller, B.; Devaraj, S.; Guffey, D.; Rajapakshe, D.; Weiner, H.; Caldarone, C.; Shekerdemian, L. Perioperative Procalcitonin in Predicting Infection in Children Undergoing Surgical Procedures. J. Surg. Res. 2021, 258, 332–338. [Google Scholar] [CrossRef] [PubMed]
- Stephens, E.H.; Epting, C.L.; Backer, C.L.; Wald, E.L. Hyperlactatemia: An Update on Postoperative Lactate. World J. Pediatr. Congenit. Hear. Surg. 2020, 11, 316–324. [Google Scholar] [CrossRef] [PubMed]
- Zhizhin, K.Y.; Turyshev, E.S.; Pautova, A.K.; Beloborodova, N. V.; Kuznetsov, N.T. Methodology for the determining aromatic monocarboxylic acids as products of phenylalanine and tyrosine metabolism: current advances and trends. Russ. Chem. Rev. 2024, 93, RCR5119. [Google Scholar] [CrossRef]
- Jia, T.; Xu, K.; Bai, Y.; Lv, M.; Shan, L.; Li, W.; Zhang, X.; Li, Z.; Wang, Z.; Zhao, X.; et al. Machine-learning predictions for acute kidney injuries after coronary artery bypass grafting: a real-life muticenter retrospective cohort study. BMC Med. Inform. Decis. Mak. 2023, 23, 270. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Li, L.; Li, Y.; Zeng, Z. Machine learning model-based risk prediction of severe complications after off-pump coronary artery bypass grafting. Adv. Clin. Exp. Med. 2022, 32, 185–194. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Chen, L.; Yao, G.; Yang, W.; Yang, K.; Xiong, C. Novel Blood Cytokine-Based Model for Predicting Severe Acute Kidney Injury and Poor Outcomes After Cardiac Surgery. J. Am. Heart Assoc. 2020, 9, 18004. [Google Scholar] [CrossRef]
- van Dijk, W.B.; Leeuwenberg, A.M.; Grobbee, D.E.; Siregar, S.; Houterman, S.; Daeter, E.J.; de Vries, M.C.; Groenwold, R.H.H.; Schuit, E.; Bramer, S.; et al. Dynamics in cardiac surgery: trends in population characteristics and the performance of the EuroSCORE II over time. Eur. J. Cardio-Thoracic Surg. 2023, 64, 301. [Google Scholar] [CrossRef]
- Schoe, A.; Bakhshi-Raiez, F.; de Keizer, N.; van Dissel, J.T.; de Jonge, E. Mortality prediction by SOFA score in ICU-patients after cardiac surgery; comparison with traditional prognostic–models. BMC Anesthesiol. 2020, 20, 65. [Google Scholar] [CrossRef]
- Meyer, Z.C.; Schreinemakers, J.M.J.; de Waal, R.A.L.; van der Laan, L. Searching for predictors of surgical complications in critically ill surgery patients in the intensive care unit: a review. Surg. Today 2015, 45, 1091–1101. [Google Scholar] [CrossRef] [PubMed]
- Cho, H.; Jung, J.-Y.; Yoon, H.-K.; Yang, S.-M.; Lee, H.-J.; Kim, W.H.; Jung, C.-W.; Suh, K.-S. Serum neutrophil gelatinase-associated lipocalin and lactate level during surgery predict acute kidney injury and early allograft dysfunction after liver transplantation. Sci. Rep. 2023, 13, 8643. [Google Scholar] [CrossRef] [PubMed]
| Parameter | Reference values/Concentrations of metabolites in donors | All patients (n=62) |
Uncomplicated group (n=36) |
Complicated group (n=26) |
Uncomp. vs comp., p-value | All patients vs donors, p-value |
|---|---|---|---|---|---|---|
| Age, years | - | 62 (57,67) | 61 (57,67) | 63 (56,67) | 0.62 | - |
| Sex (males), n, % | - | 44, 71% | 13, 36% | 5, 19% | 0.15* | - |
| Diabetes Mellitus, n, % | - | 10, 16.1% | 6, 16.7% | 4, 15.4% | 0.72* | - |
| EF (%) | - | 60 (49,63) | 58 (48,63) | 60 (51,66) | 0.33 | - |
| EuroScore 2 | - | 0.91 (0.75,1.16) | 0.94 (0.78,1.08) | 0.90 (0.71,1.35) | 0.84 | - |
| Hemoglobin, g/l | 110-160 | 114.5 (107.0,125.5) | 113.0 (107.0,124.5) | 118.0 (103.3,125.5) | 0.89 | ns |
| Leucocytes, 109 | 4-9 | 16.10 (13.50,19.87) | 16.20 (13.65,18.54) | 15.98 (12.56,20.62) | 0.85 | ** |
| Vasopressors > 6h | - | 45, 72.6% | 22, 61.1% | 23, 88.5% | 0.02* | - |
| Mechanic ventilation> 12h | - | 9, 14.5% | 0, 0% | 9, 34,6% | 0.001* | - |
| Lactate max, mmol/l | <2 | 5.17 (3.54,7.08) | 4.84 (3.46,6.08) | 5.85 (3.94,7.94) | 0.07 | ** |
| Infusion volume, ml | - | 5928 (5175,6897) | 5560 (4822,6425) | 6825 (5888,7600) | 0.001 | - |
| On-pump time, h | - | 85.50 (76.25,108.75) | 78.50 (67.50,98.50) | 102.00 (85.00,129.75) | 0.001 | - |
| рН max | 7.35-7.45 | 7.47 (7.45,7.50) | 7.47 (7.44,7.49) | 7.49 (7.45,7.50) | 0.21 | ns |
| pH min | 7.35-7.45 | 7.33 (7.29,7.36) | 7.33 (7.29,7.36) | 7.33 (7.29,7.35) | 0.40 | ns |
| SOFA on the 1st day | - | 4 (3,6) | 4 (2,4) | 6 (4,6) | 0.001 | - |
| Number of erythrocytes transfusions | - | 1 (0,2) | 1 (0,2) | 2 (1,3) | 0.03 | - |
| Blood loss on the 1st day, ml | - | 1275 (1050,1400) | 1200 (1050,1300) | 1350 (1075,1487) | 0.04 | - |
| Before surgery (point 0) | ||||||
| BA_0, µmol/l | <0.5 (<0.5,<0.5) | 1.8 (1.3,2.4) | 1.7 (1.3,2.3) | 2.1 (1.5,2.6) | 0.13 | 0.001 |
| PhAA_0, µmol/l | <0.5 (<0.5,0.6) | 0.9 (0.6,1.2) | 1.0 (0.6,1.5) | 0.9 (0.6,1.0) | 0.24 | 0.001 |
| PhPA_0, µmol/l | <0.5 (<0.5,0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,0.5) | <0.5 (<0.5,<0.5) | 0.33 | 0.75 |
| PhLA_0, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.85 | 0.79 |
| p-HBA_0, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.19 | 0.03 |
| p-HPhAA_0, µmol/l | <0.5 (<0.5,<0.5) | 0.7 (0.5,1.0) | 0.7 (0.5,1.1) | 0.6 (0.5,0.9) | 0.45 | 0.001 |
| p-HPhPA_0, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 1.00 | 1 |
| HVA_0, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.74 | 0.13 |
| p-HPhLA_0, µmol/l | 1.2 (1.0,1.6) | 1.2 (1.0,1.4) | 1.2 (1.0,1.4) | 1.2 (1.1,1.4) | 0.72 | 0.37 |
| Σ3AMM_0, µmol/l | 1.9 (1.5,2.2) | 2.1 (1.8,2.7) | 2.1 (1.8,2.8) | 2.0 (1.7,2.5) | 0.55 | 0.04 |
| SA_0, µmol/l | 4.8 (4.4,6.0) | 20.2 (17.0,25.2) | 19.9 (16.9,25.8) | 20.7 (17.6,24.0) | 0.86 | 0.001 |
| FA_0, µmol/l | 1.3 (1.1,1.5) | 1.7 (1.5,2.1) | 1.7 (1.4,2.1) | 1.7 (1.5,2.4) | 0.93 | 0.001 |
| IL6_0, pg/ml | <7 | 9.0 (6.8,13.6) | 9.5 (7.0,13.6) | 8.7 (6.2,14.2) | 0.75 | ns |
| PCT_0, ng/ml | <0.5 | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.59 | ns |
| NT-proBNP_0, pg/ml | <300 | 564.8 (216.0,883.0) | 478.3 (213.7,790.3) | 625.2 (239.8,883.0) | 0.72 | ns |
| S100_0, pg/ml | <0.5 | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.27 | ns |
| HST-T_0, pg/ml | <0.5 | 24.2 (16.2,40.3) | 29.2 (16.5,45.3) | 22.5 (15.6,30.4) | 0.16 | ns |
| A day after surgery (point 1) | ||||||
| BA_1, µmol/l | <0.5 (<0.5,<0.5) | 1.4 (0.9,2.8) | 1.2 (0.9,2.1) | 1.6 (1.1,3.1) | 0.15 | 0.001 |
| PhAA_1, µmol/l | <0.5 (<0.5,0.60) | <0.5 (<0.5,0.5) | <0.5 (<0.5,0.5) | <0.5 (<0.5,<0.5) | 0.99 | 0.001 |
| PhPA_1, µmol/l | <0.5 (<0.5,0.52<0.) | 5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 1.00 | 0.001 |
| PhLA_1, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.96 | 0.001 |
| p-HBA_1, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.77 | 0.03 |
| p-HPhAA_1, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.49 | 0.001 |
| p-HPhPA_1, µmol/l | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 1.00 | 0.001 |
| HVA_1, µmol/l | <0.5 (<0.5,<0.5) | 1.6 (0.7,3.0) | 1.1 (<0.5,3.0) | 2.3 (1.1,3.3) | 0.06 | 0.001 |
| p-HPhLA_1, µmol/l | 1.3 (1.0,1.6) | 1.6 (1.3,2.4) | 1.6 (1.3,2.3) | 1.6 (1.3,2.4) | 0.56 | 0.001 |
| Σ3AMM_1, µmol/l | 1.9 (1.5,2.2) | 2.2 (1.8,3.3) | 2.4 (1.7,3.3) | 2.2 (1.8,3.2) | 0.98 | 0.001 |
| SA_1, µmol/l | 4.8 (4.4,5.9) | 16.2 (12.7,21.7) | 15.8 (12.2,20.0) | 16.9 (14.3,23.3) | 0.34 | 0.001 |
| FA_1, µmol/l | 1.3 (1.1,1.5) | 2.2 (1.5,3.8) | 2.2 (1.5,4.5) | 2.1 (1.8,3.4) | 0.91 | 0.001 |
| IL6_1, pg/ml | <7 | 67.6 (38.0,101.1) | 58.7 (34.8,102.8) | 76.4 (43.7,100.0) | 0.64 | ** |
| PCT_1, ng/ml | <0.5 | 3.3 (0.7,8.8) | 1.5 (<0.5,7.3) | 4.2 (1.1,16.8) | 0.06 | ** |
| NT-proBNP_1, pg/ml | <300 | 981.9 (608.9,1409.3) | 964.1 (468.8,1329.8) | 1181.5 (817.8,1878.8) | 0.13 | ** |
| S100_1, pg/ml | <0.5 | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | <0.5 (<0.5,<0.5) | 0.81 | ns |
| HST-T_1, pg/ml | <0.5 | 356.7 (202.4,614.0) | 261.9 (194.2,455.0) | 575.5 (216.9,745.5) | 0.03 | ** |
| Differences between point 1 and point 0 (Δ) | ||||||
| ΔBA, µmol/l | - | -0.3 (-2.5,1.9) | -0.4 (-2.0,1.3) | -0.2 (-3.0,2.5) | 0.89 | - |
| ΔPhAA, µmol/l | - | -0.8 (-1.4,-0.2) | -0.8 (-1.5,-0.1) | -0.7 (-1.2,-0.3) | 0.32 | - |
| ΔPhPA, µmol/l | - | 0.0 (-0.2,0.2) | 0.0 (-0.3,0.3) | 0.0 (-0.1,0.1) | 0.37 | - |
| ΔPhLA, µmol/l | - | 0.0 (-0.2,0.2) | 0.0 (-0.3,0.3) | 0.0 (-0.2,0.2) | 0.65 | - |
| Δp-HBA, µmol/l | - | 0.0 (-0.8,0.8) | 0.0 (-0.9,0.9) | 0.0 (-0.5,0.5) | 0.28 | - |
| Δp-HPhAA, µmol/l | - | -0.6 (-1.8,0.7) | -0.7 (-2.1,0.7) | -0.5 (-1.4,0.3) | 0.22 | - |
| Δp-HPhPA, µmol/l | - | 0.0 (0.0,0.0) | 0.0 (0.0,0.0) | 0.0 (0.0,0.0) | 0.99 | - |
| ΔHVA, µmol/l | - | 1.7 (-2.4,5.8) | 1.1 (-2.4,4.7) | 2.3 (-2.2,6.7) | 0.08 | - |
| Δp-HPhLA, µmol/l | - | 0.5 (-0.3,1.3) | 0.4 (-0.2,1.1) | 0.6 (-0.3,1.5) | 0.20 | - |
| ΔΣ3AMM, µmol/l | - | 0.3 (-1.2,1.9) | 0.0 (-1.5,1.5) | 0.7 (-0.8,2.2) | 0.03 | - |
| ΔSA, µmol/l | - | -4.4 (-16.3,7.6) | -4.9 (-15.8,5.9) | -2.3 (-14.9,10.4) | 0.29 | - |
| ΔFA, µmol/l | - | 0.5 (-8.7,9.7) | 0.4 (-11.0,11.7) | 0.5 (-4.2,5.3) | 0.96 | - |
| ΔIL6, pg/ml | - | 60.8 (-28.6,150.1) | 51.6 (-31.2,134.4) | 69.3 (-28.4,167.0) | 0.97 | - |
| ΔPCT, ng/ml | - | 3.6 (-11.6,18.8) | 1.5 (-4.2,7.1) | 4.9 (-16.2,25.9) | 0.01 | - |
| ΔNT-proBNP, pg/ml | - | 493.6 (-1878.4,2865.7) | 264.4 (-871.4,1400.1) | 720.6 (-2547.1,3988.3) | 0.01 | - |
| ΔS100, pg/ml | - | 0.0 (-0.3,0.3) | 0.0 (-0.2,0.2) | 0.0 (-0.4,0.5) | 0.67 | - |
| ΔHST-T, pg/ml | - | 390.7 (47.8,733.6) | 247.0 (-106.4,600.4) | 569.5 (270.4,868.6) | 0.01 | - |
| Models | ROC-AUC (95% CI) |
Sensitivity (95% CI) |
Specificity (95% CI) |
|---|---|---|---|
| Multivariate models | |||
| All data | 0.75 (0.74, 0.76) | 0.74 (0.72, 0.75) | 0.77 (0.75, 0.78) |
| Clinical data | 0.71 (0.69, 0.72) | 0.68 (0.66, 0.69) | 0.74 (0.72, 0.75) |
| Metabolites and biomarkers | 0.60 (0.57, 0.63) | 0.73 (0.70, 0.75) | 0.47 (0.44, 0.51) |
| Univariate models | |||
| SOFA | 0.76 (0.71, 0.82) | 0.69 (0.63, 0.76) | 0.83 (0.79, 0.88) |
| Lactate | 0.71 (0.65, 0.78) | 0.76 (0.71, 0.82) | 0.67 (0.59, 0.74) |
| ΔΣ3AMM | 0.70 (0.63, 0.77) | 0.62 (0.54, 0.70) | 0.78 (0.72, 0.83) |
| Δp-HPhLA | 0.69 (0.62, 0.76) | 0.88 (0.85, 0.91) | 0.50 (0.42, 0.58) |
| EuroScore2 | 0.59 (0.51, 0.67) | 0.52 (0.44, 0.60) | 0.67 (0.60, 0.74) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




