Submitted:
23 June 2024
Posted:
24 June 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Data source
2.2. Statistical analysis
2.2.1. Trends assessment: Joinpoint regression
2.2.2. Association and impact evaluation: LASSO regression
3. Results
3.1. Joinpoint regression findings
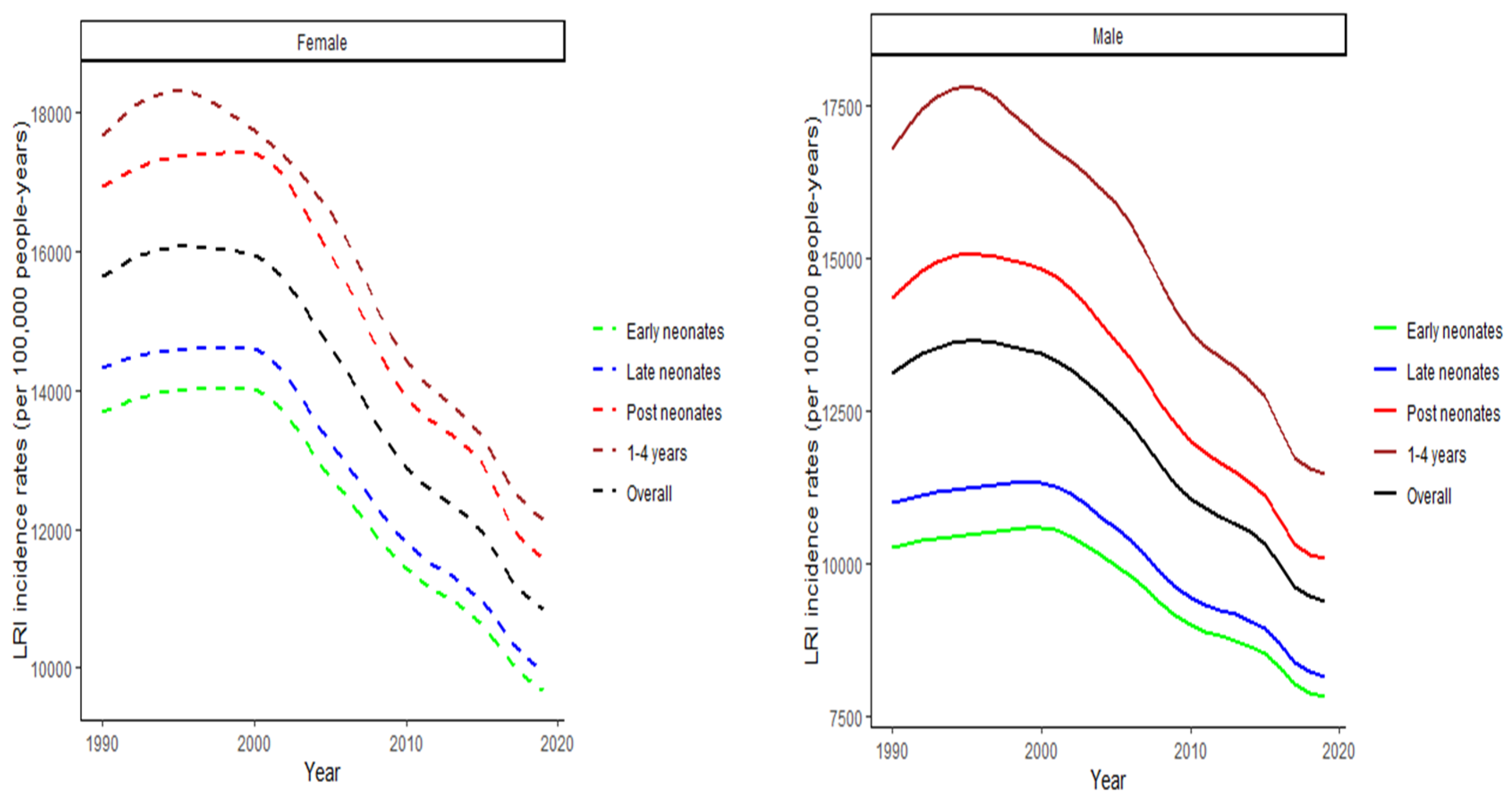
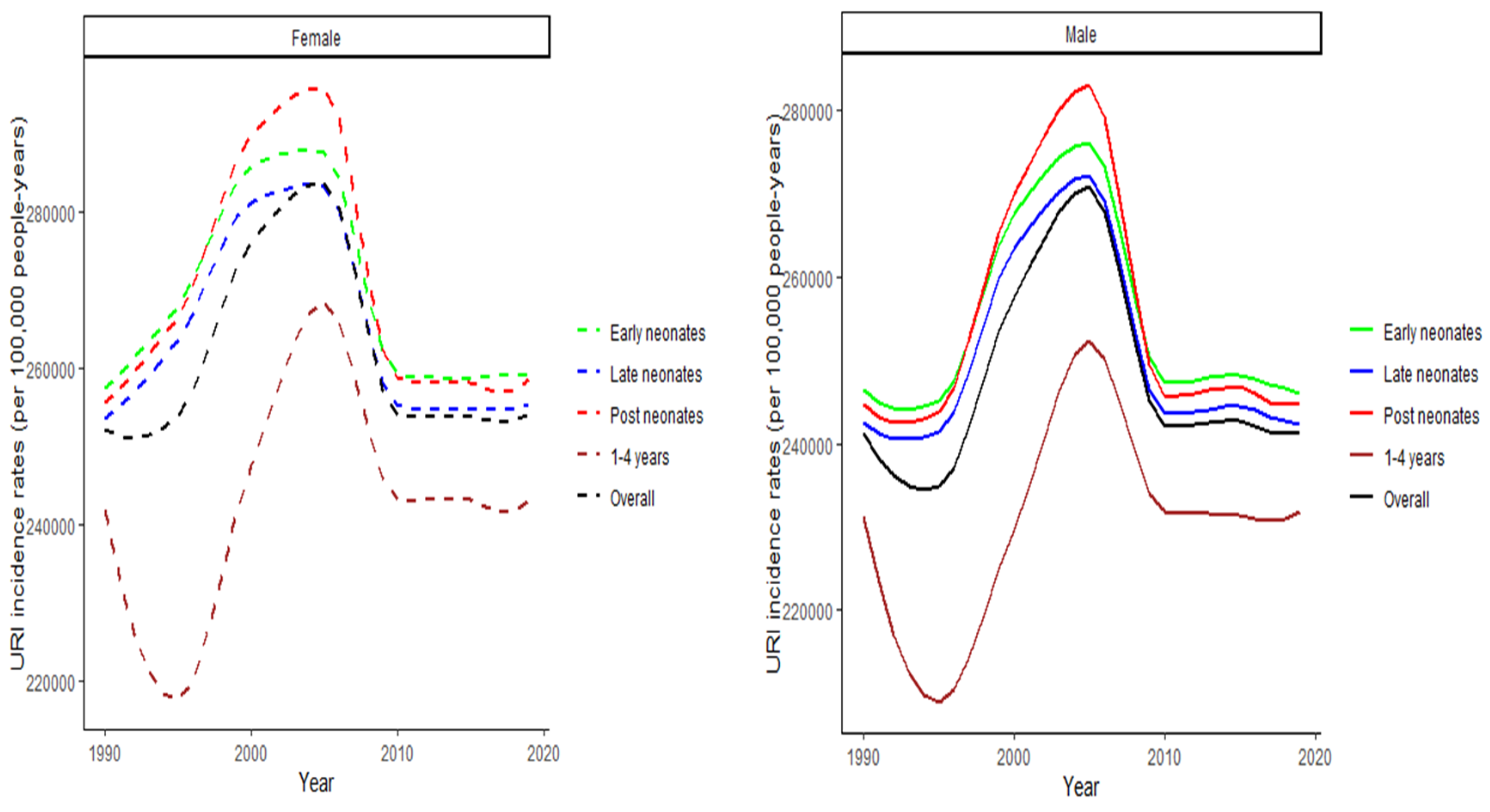
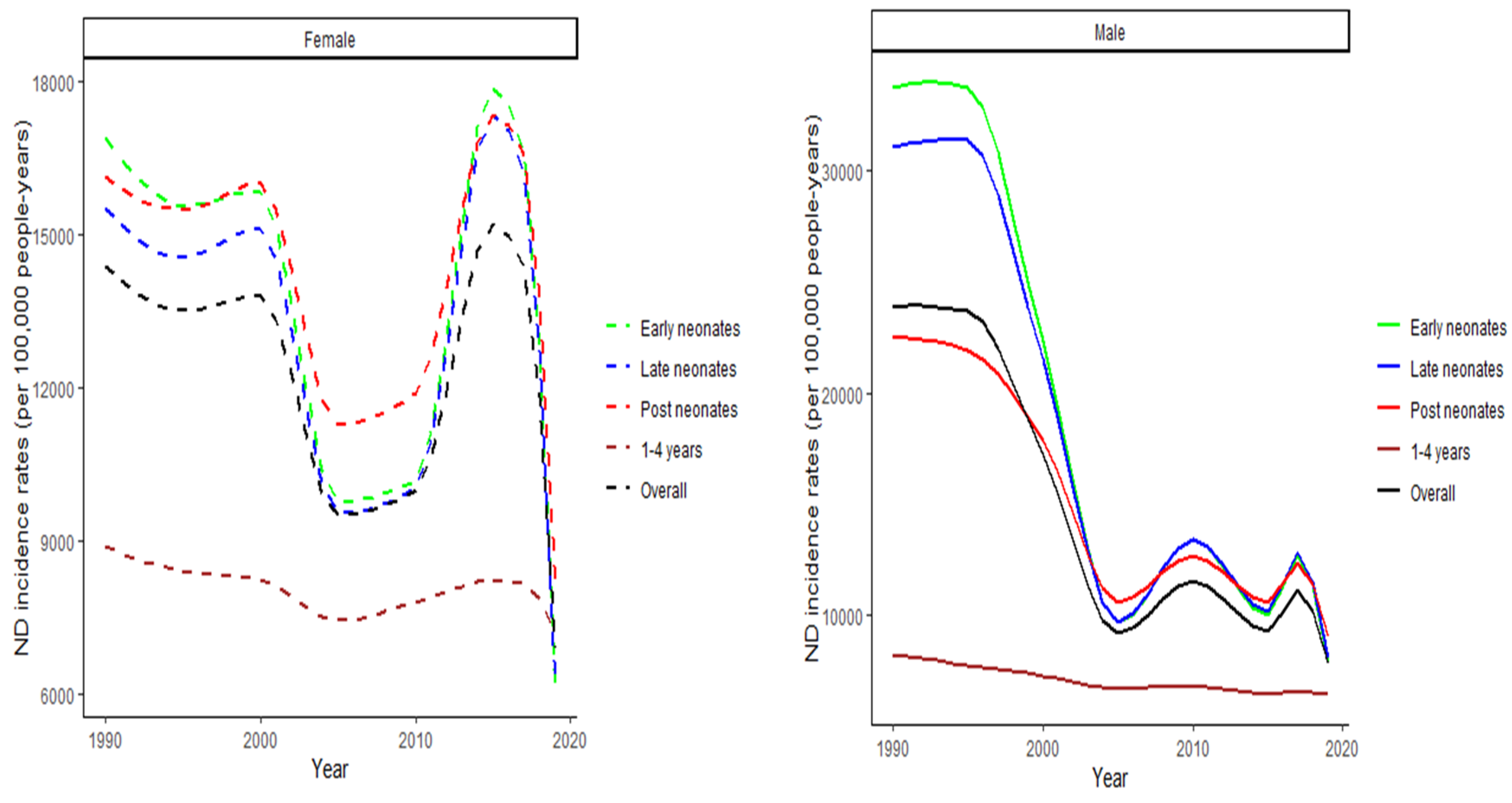
| LRI | URI | ND | ||
| Variables | Period | AAPC (95% CI) | AAPC (95% CI) | AAPC (95% CI) |
| Female | ||||
| Early neonates (0-6 days) | 1990-2019 | -1.2* (-1.3, -1.1) | 0.0 (0.0, 0.1) | -3.1* (-3.8, -2.3) |
| Late neonates (7-27 days) | 1990-2019 | -1.3* (-1.3, -1.2) | 0.0 (0.0, 0.1) | -2.8* (-3.5, -2.0) |
| Post neonates (28-364 days) | 1990-2019 | -1.3* ( -1.5, -1.2) | 0.0 (-0.1, 0.1) | -2.1* (-2.7, -1.5) |
| 1-4 years | 1990-2019 | -1.3* ( -1.4, -1.2) | 0.0 (-0.1, 0.1) | -0.7* (-0.8, -0.6) |
| Overall | 1990-2019 | -1.3* (-1.4, -1.2) | 0.0 (-0.0, 0.1) | -2.2* (-2.9, -1.6) |
| Male | ||||
| Early neonates (0-6 days) | 1990-2019 | -1.0* (-1.0, -0.9) | 0.0 (-0.1, 0.1) | -4.9* (-6.1, -3.6) |
| Late neonates (7-27 days) | 1990-2019 | -1.0* (-1.1, -1.0) | 0.0 (-0.1, 0.1) | -4.5* (-5.7, -3.3) |
| Post neonates (28-364 days) | 1990-2019 | -1.2* (-1.4, -1.1) | 0.0 (-0.1, 0.2) | -3.1* (-3.8, -2.4) |
| 1-4 years | 1990-2019 | -1.3* (-1.5, -1.2) | 0.0 (-0.1, 0.1) | -0.9* (-0.9, -0.8) |
| Overall | 1990-2019 | -1.2* (-1.4, -1.0) | 0.0 (-0.1, 0.2) | -3.8* (-4.7, -2.8) |
3.1. LASSO regression outcomes
| Variables | β1 | β2 | β3 | β4 | β5 | β6 | β7 | β8 | β9 | R2 (%) | MSE |
| Female | |||||||||||
| LRI | |||||||||||
| Early neonates | -0.01 | 0.14 | 0.29 | 0.60 | N/A | N/A | 0.10 | N/A | -0.01 | 99.90 | 0.006 |
| Late neonates | -0.01 | 0.14 | 0.34 | 0.57 | N/A | N/A | 0.09 | N/A | -0.00 | 99.90 | 0.007 |
| Post neonates | -0.08 | 0.07 | 0.43 | 0.53 | N/A | N/A | 0.01 | N/A | -0.04 | 99.90 | 0.006 |
| 1-4 years | -0.07 | 0.24 | 0.52 | 0.10 | N/A | 0.09 | N/A | -0.07 | 99.91 | 0.006 | |
| Overall | -0.08 | 0.02 | 0.24 | 0.62 | N/A | N/A | 0.11 | N/A | -0.06 | 99.91 | 0.005 |
| URI | |||||||||||
| Early neonates | -0.92 | 0.06 | 0.17 | 0.51 | -0.54 | 0.33 | N/A | -0.29 | 0.23 | 99.90 | 0.007 |
| Late neonates | -0.92 | 0.05 | 0.19 | 0.49 | -0.54 | 0.33 | -0.01 | -0.29 | 0.22 | 99.90 | 0.007 |
| Post neonates | -0.89 | N/A | 0.26 | 0.32 | -0.61 | 0.48 | -0.05 | -0.32 | 0.17 | 99.87 | 0.008 |
| 1-4 years | -0.44 | N/A | 0.09 | 0.16 | -1.33 | 1.13 | -0.39 | -.058 | 0.37 | 99.49 | 0.036 |
| Overall | -0.88 | N/A | 0.11 | 0.42 | -0.87 | 0.67 | -0.08 | -0.42 | 0.26 | 99.84 | 0.011 |
| ND | |||||||||||
| Early neonates | -1.30 | 0.14 | -1.83 | 2.80 | -0.70 | -1.64 | 0.22 | -1.71 | 0.57 | 99.05 | 0.068 |
| Late neonates | -1.33 | 0.21 | -1.55 | 2.73 | -0.65 | -1.77 | 0.00 | -1.69 | 0.60 | 98.93 | 0.077 |
| Post neonates | -1.42 | 0.16 | -1.97 | 3.35 | -0.62 | -1.95 | 0.01 | -1.65 | 0.68 | 99.05 | 0.068 |
| 1-4 years | -0.28 | 0.25 | -0.69 | 1.98 | -0.17 | -1.29 | N/A | -0.72 | 0.43 | 99.71 | 0.020 |
| Overall | -1.29 | 0.18 | -1.57 | 2.83 | -0.61 | -1.78 | 0.01 | -1.61 | 0.60 | 99.04 | 0.069 |
| Variables | β1 | β2 | β3 | β4 | β5 | β6 | β7 | β8 | β9 | R2 (%) | MSE |
| Male | |||||||||||
| LRI | |||||||||||
| Early neonates | -0.10 | 0.05 | 0.34 | 0.64 | -0.02 | N/A | N/A | N/A | -0.06 | 99.91 | 0.006 |
| Late neonates | -0.08 | 0.08 | 0.40 | 0.57 | N/A | N/A | N/A | N/A | -0.04 | 99.90 | 0.006 |
| Post neonates | -0.08 | N/A | 0.07 | 0.68 | 0.00 | 0.00 | 0.19 | N/A | -0.10 | 99.90 | 0.006 |
| 1-4 years | 0.04 | N/A | 0.26 | N/A | 0.08 | 0.26 | 0.38 | N/A | -0.22 | 99.82 | 0.011 |
| Overall | -0.08 | 0.02 | 0.24 | 0.62 | N/A | N/A | 0.11 | N/A | -0.06 | 99.91 | 0.005 |
| URI | |||||||||||
| Early neonates | -1.09 | -0.17 | 0.14 | 0.72 | -0.93 | 0.50 | -0.33 | -0.47 | 0.30 | 99.77 | 0.016 |
| Late neonates | -1.08 | -0.17 | 0.16 | 0.70 | -0.93 | 0.51 | -0.33 | -0.47 | 0.30 | 99.77 | 0.020 |
| Post neonates | -0.92 | -0.04 | 0.24 | 0.27 | -0.90 | 0.74 | -0.24 | -0.55 | 0.27 | 99.71 | 0.020 |
| 1-4 years | -0.47 | -0.11 | 0.34 | N/A | -1.04 | 1.00 | -0.73 | -0.51 | 0.39 | 99.49 | 0.036 |
| Overall | -0.90 | -0.09 | 0.23 | 0.37 | -1.03 | 0.79 | -0.39 | -0.56 | 0.33 | 99.68 | 0.022 |
| ND | |||||||||||
| Early neonates | 0.41 | 0.37 | -0.16 | 0.32 | 0.49 | -0.32 | 0.55 | 0.00 | 0.11 | 99.73 | 0.018 |
| Late neonates | 0.43 | 0.43 | -0.39 | 0.47 | 0.45 | -0.31 | 0.65 | -0.04 | 0.15 | 99.73 | 0.019 |
| Post neonates | 0.18 | 0.26 | -0.76 | 1.21 | 0.30 | -0.51 | 0.64 | -0.04 | 0.23 | 99.76 | 0.016 |
| 1-4 years | 0.31 | N/A | N/A | 0.28 | 0.11 | N/A | 0.53 | N/A | N/A | 99.69 | 0.022 |
| Overall | 0.37 | 0.18 | -1.57 | 2.83 | -0.61 | -1.78 | 0.01 | -1.61 | 0.60 | 99.04 | 0.069 |
4. Discussion
5. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AAPC | average annual percent change |
| AUD | alcohol usage disorders |
| APC | annual percentage of change |
| CI | confidence interval |
| GBD | global burden of disease |
| GD | gynecological diseases |
| GHDx | global health data exchange |
| HB | hepatitis B |
| HCE | heat and cold exposure |
| HIV/AIDS | human immunodeficiency virus/acquired immunodeficiency syndrome |
| IHME | institute of health metrics and evaluation |
| LASSO | least absolute shrinkage and selection operator |
| LMIC | low- and middle-income countries |
| LRI | lower respiratory infections |
| M | malaria |
| MD | maternal disorders |
| N/A | not applicable |
| ND | nutritional deficiency |
| SDGs | sustainable development goals |
| TB | tuberculosis infection |
| URI | upper respiratory infections |
| USA | united states of America |
| VIF | variance inflation factors |
| WB | world bank |
References
- Dasaraju PV, Liu C. Infections of the Respiratory System. In: Baron S, editor. Medical Microbiology. 4th edition. Galveston (TX): University of Texas Medical Branch at Galveston; 1996. Chapter 93.
- Lewandowicz-Uszyńska A, Pasternak G, Pentoś K. Immunoglobulin G deficiency in children with recurrent respiratory infections with and without history of allergy. Adv Exp Med Biol. 2021;1289:63–70. [CrossRef]
- Pasternak G, Lewandowicz-Uszyńska A, Pentoś K. Disorders of humoral immunity in children with IgG subclass deficiency and recurrent respiratory infections. Adv Exp Med Biol. (2018) 1108:99–106. [CrossRef]
- Kiani AK, Dhuli K, Donato K, Aquilanti B, Velluti V, Matera G, Iaconelli A, Connelly ST, Bellinato F, Gisondi P, Bertelli M. Main nutritional deficiencies. J Prev Med Hyg 2022;63(suppl.3):E93-E101. [CrossRef]
- Yue, T., Zhang, Q., Li, G., & Qin, H. (2022). Global Burden of Nutritional Deficiencies among Children under 5 Years of Age from 2010 to 2019. Nutrients, 14(13), 2685. [CrossRef]
- Tazinya, A.A., Halle-Ekane, G.E., Mbuagbaw, L.T. et al. Risk factors for acute respiratory infections in children under five years attending the Bamenda Regional Hospital in Cameroon. BMC Pulm Med 18, 7 (2018). [CrossRef]
- Ahinkorah, B.O., Seidu, AA., Budu, E. et al. Proximate, intermediate, and distal predictors of under-five mortality in Chad: analysis of the 2014–15 Chad demographic and health survey data. BMC Public Health 20, 1873 (2020). [CrossRef]
- World Bank. New World Bank country classifications by income level: 2022-2023. (2022). Retrieved in May 2023 from https://blogs.worldbank.org/opendata/new-world-bank-country-classifications-income-level-2022-2023.
- Save the Children, United Nations Children’s Fund (UNICEF), Chaque Souffle compte. A bout de souffle au Tchad. (2020) (Accessed in May 2023) from https://stoppneumonia.org/wp-content/uploads/2020/06/CHAD-FRENCH-2020.pdf.
- Nations Unies. Organization des Nations Unies (ONU) Info. Le taux de malnutrition des enfants alarmant dans l’ouest du Tchad. (2008). Retrieved in May 2023 from https://news.un.org/fr/story/2008/11/143522#:~:text=L'OCHA%20se%20fonde%20sur,sur%2010.000%20meurent%20de%20malnutrition (Accessed May 2023).
- Warr, A. J., Pintye, J., Kinuthia, J., Drake, A. L., Unger, J. A., McClelland, R. S., Matemo, D., Osborn, L., & John-Stewart, G. (2019). Sexually transmitted infections during pregnancy and subsequent risk of stillbirth and infant mortality in Kenya: a prospective study. Sexually transmitted infections, 95(1), 60–66. [CrossRef]
- Arunda, M. O., Choudhry, V., Ekman, B., & Asamoah, B. O. (2016). Under-five mortality and maternal HIV status in Tanzania: analysis of trends between 2003 and 2012 using AIDS Indicator Survey data. Global health action, 9, 31676. [CrossRef]
- Yaya, S., Bishwajit, G., Okonofua, F., & Uthman, O. A. (2018). Under five mortality patterns and associated maternal risk factors in sub-Saharan Africa: A multi-country analysis. PloS one, 13(10), e0205977. [CrossRef]
- Marais B. J. (2011). Impact of tuberculosis on maternal and child health. The Journal of infectious diseases, 203(3), 304–305. [CrossRef]
- United Nations Economic Commission for Europe (UNECE). Indicator 3.2. 1 (b). Under-five mortality rate, deaths per 1,000 live births. Retrieved in May 2023 from https://w3.unece.org/SDG/en/Indicator?id=91.
- Global Burden of Disease Collaborative Network. Global Burden of Disease Study 2019 (GBD 2019) Results; Institute for Health Metrics and Evaluation (IHME): Seattle, WA, USA, 2020; Available online: Retrieved in April 2023 from http://ghdx.healthdata.org/gbd-results-tool.
- Terán JM, Sánchez-García E, Martínez-Carrión JM, Bogin B, Varea C. Use of Joinpoint regressions to evaluate changes over time in conscript height. Official Journal of the Human Biology Council. 2022, 34(1), e23572. [CrossRef]
- Zhang, Y., Liu, J., Han, X., Jiang, H., Zhang, L., Hu, J., Shi, L., & Li, J. (2022). Long-term trends in the burden of inflammatory bowel disease in China over three decades: A joinpoint regression and age-period-cohort analysis based on GBD 2019. Frontiers in public health, 10, 994619. [CrossRef]
- Zhu, B., Wang, Y., Zhou, W., Jin, S., Shen, Z., Zhang, H., Zhang, X., Ding, X., & Li, Y. (2022). Trend dynamics of gout prevalence among the Chinese population, 1990-2019: A joinpoint and age-period-cohort analysis. Frontiers in public health, 10, 1008598. [CrossRef]
- Qiu, H., Cao, S., & Xu, R. (2021). Cancer incidence, mortality, and burden in China: a time-trend analysis and comparison with the United States and United Kingdom based on the global epidemiological data released in 2020. Cancer communications (London, England), 41(10), 1037–1048. [CrossRef]
- Liu, X., Yu, C., Bi, Y., & Zhang, Z. J. (2019). Trends and age-period-cohort effect on incidence and mortality of prostate cancer from 1990 to 2017 in China. Public health, 172, 70–80. [CrossRef]
- Shrestha N. Detecting Multicollinearity in Regression Analysis. American Journal of Applied Mathematics and Statistics, 2020.
- Daoud JI. Multicollinearity and Regression Analysis. Journal of Physics: Conference Series. 2018, 949(1). [CrossRef]
- Murray L, Nguyen H, Lee YF, Remmenga MD, Smith DW. (2012). Variance Inflation Factors in Regression Models with Dummy Variables. Conference on Applied Statistics in Agriculture, 2012 (pp. 1-18).
- Cule E, Vineis P, De Iorio M. Significance testing in ridge regression for genetic data. BMC Bioinformatics. 2011, 12, 372. [CrossRef]
- Gelman A. Scaling regression inputs by dividing by two standard deviations. Statistics in Medicine. 2008, 27(15), 2865–2873. [CrossRef]
- Weaving D, Jones B, Ireton M, Whitehead S, Till K, Beggs CB. Overcoming the problem of multicollinearity in sports performance data: A novel application of partial least squares correlation analysis. PloS One. 2019, 14(2), e0211776.
- van Egmond MB, Spini G, van der Galien O, IJpma A, Veugen T, Kraaij W, Sangers A, Rooijakkers T, Langenkamp P, Kamphorst B, van de L'Isle N, Kooij-Janic M. Privacy-preserving dataset combination and Lasso regression for healthcare predictions. BMC Medical Informatics and Decision Making. 2021, 21(1), 266. [CrossRef]
- Tibshirani R. Regression Shrinkage and Selection via the Lasso. Journal of the Royal Statistical Society: Series B (Methodological). 1996, 58, 267-288. [CrossRef]
- United Nations Children’s Fund (UNICEF). UNICEF Chad Humanitarian Situation Report No. 3 for 1 July to September 2022. (2022). Retrieved in June 2023 from https://reliefweb.int/report/chad/unicef-chad-humanitarian-situation-report-no-3-1-july-30-september-2022?gclid=Cj0KCQjwkqSlBhDaARIsAFJANkhoafrw0kO7wZMOsjr2mx0dk2YvUPgc0LiqlH-eh_AwCgjX1D13rPYaApoVEALw_wcB.
- D. Manoufi, W.C. Kabore, C.N. Yahannon, A. Dumont, V. Ridde, Amélioration de l’offre et de la demande de soins de santé maternelle et infantile au Tchad : une étude quasi-expérimentale, Revue d'Épidémiologie et de Santé Publique, Volume 69, Issue 4, 2021,Pages 193-203, ISSN 0398-7620. [CrossRef]
- Simen-Kapeu, A., Bogler, L., Weber, A. C., Ntambi, J., Zagre, N. M., Vollmer, S., & Ekpini, R. E. (2021). Prevalence of diarrhoea, acute respiratory infections, and malaria over time (1995-2017): A regional analysis of 23 countries in West and Central Africa. Journal of global health, 11, 13008. [CrossRef]
- Hammond, A., Halliday, A., Thornton, H. V., & Hay, A. D. (2021). Predisposing factors to acquisition of acute respiratory tract infections in the community: a systematic review and meta-analysis. BMC infectious diseases, 21(1), 1254. [CrossRef]
- Cortes-Ramirez, J., Wilches-Vega, J.D., Paris-Pineda, O.M., Ayurzana, L., & Sly, P.D. (2021). Environmental risk factors associated with respiratory diseases in children with socioeconomic disadvantage. Heliyon, 7(4), e06820. [CrossRef]
- Vilcins, D., Sly, P.D., & Jagals, P. (2018). Environmental risk factors associated with child stunting: A systematic Review of the literature. Annals of Global Health, 84(4), 551-562. [CrossRef]
- Khalid N, Aslam Z, Kausar F, Irshad H, Anwer P (2017) Maternal Malnutrition and Its Kick on Child Growth: An Alarming Trim for Pakistan. J Food Nutr Popul Health Vol.1 No.3:24.
- Kim, S., Choe, SA. & Cho, SI. Harmful alcohol use among mothers of under-five child: findings from the Panel Study on Korean Children. BMC Women's Health 21, 159 (2021). [CrossRef]
- Colleen O’Leary, David Lawrence, Katherine Hafekost, Stephen R. Zubrick, Carol Bower; Maternal Alcohol-Use Disorder and Child Outcomes. Pediatrics March 2020; 145 (3): e20191574. 10.1542/peds.2019-1574.
- Tse, K. Y., Ho, L. F., & Lao, T. (2005). The impact of maternal HBsAg carrier status on pregnancy outcomes: a case-control study. Journal of hepatology, 43(5), 771–775. [CrossRef]
- Kuehn, L., & McCormick, S. (2017). Heat Exposure and Maternal Health in the Face of Climate Change. International journal of environmental research and public health, 14(8), 853. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




